Debridement: treatment, options and selection.
|
|
|
- Elvin Payne
- 5 years ago
- Views:
Transcription
1 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher. To access the final edited and published work see Debridement: treatment, options and selection. Leanne Atkin, Lecturer/Practitioner, Department of Health Sciences, School of Human and Health Sciences, Institute of Skin Integrity and Infection Prevention, University of Huddersfield, Queensgate, Huddersfield, Yorkshire, HD1 3DH. Introduction Wound debridement, the removal of devitalised tissue, continues to be a cornerstone of wound management. There are many different methods of wound debridement, these are grouped into autolytic, surgical/sharp, mechanical and biological categories, each of which have specific advantages and disadvantages. The decision as to whether to debride a wound and which method(s) to choose is very individualised, therefore all practitioners involved in wound care must be competent at wound bed assessment and have an awareness of all debridement options available. This article will provide a brief overview of wound bed assessment, provide information about the decision process of whether to debride and describe different methods of wound debridement. Debridement The word debridement originated from France and means to remove constraints. Within wound care debridement refers to the removal of adherent, dead or contaminated tissue from the wound and is clearly separated from the act of wound cleansing which is defined as the removal of dirt, foreign material or metabolic waste, (Strohal, Apelqvist, & Dissemond, 2014). The presence of dead/devitalised tissue hinders wound healing, debridement provides the foundation for subsequent tissue growth, (O'Brien, 2003). Appropriate and early debridement accelerates wound healing, this in turn delivers additional benefits of improved quality of care, enhanced patient health and wellbeing and a reduction in treatment costs, (Wounds UK, 2013). The body s natural method of wound debridement is called autolysis, in acute wounds autolytic debridement occurs automatically. During the acute inflammatory state of wound healing neutrophils and macrophages clear devitalised tissue, cell debris or containments preparing the wound bed to allow healing to occur. However, in chronic wounds this autolytic process can be delayed due to increase levels of endotoxins released from damaged cells, (Broadus, 2013). Consequently debridement is often a common goal in the management of chronic wounds and has been included in many clinical guidelines from professional wound organisations such as European Wound Healing Society (Strohal et al., 2014) and Wounds UK (Wounds UK, 2013).
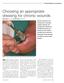
2 Wounds Assessment Generalist nurses remain the primary point of care for most patients with a wound, subsequently they play an important role in the clinical decision making regarding whether debridement is necessary, which method to use and whether a patient needs to be referred on to specialist services such as tissue viability, (Wounds UK, 2013). Therefore it is vital that all practitioners involved in wound care are able to confidently perform holistic wound assessment. Holistic assessment of the patient and the wound is needed to ensure accurate diagnosis of the underlying factors that could be the cause of the wound and to identity elements that could delay wound healing, (Cook, 2012). To ensure effective treatment of patients with wounds the diagnostic process should: Determine the cause of the wound Identify any co-morbidities/complications that may contribute to the wound or delay healing Assess the status of the wound including location and size, condition of wound bed, signs of increased bacterial load, level of exudate, and condition of peri wound skin Established appropriate aims of wound care (World Union of Wound Healing Societies, 2008; Wounds UK, 2013). Debridement is common practice in many wounds and it can be applied to any wound type, irrespective of origin and diagnosis. However, practitioners need to have a clear understanding of the underlying cause of the wound and whether healing is the realistic/appropriate goal, as in certain circumstances debridement may not be beneficial for the patient and in some instances could be detrimental. For example patients with peripheral arterial disease who develop distal gangrene (Figure 1), with dry gangrene it is more appropriate to leave these wounds without any dressings rather than promoting debridement. This is because in the debridement process levels of moisture at the wound bed will increase leading to increased risk of infection and due to the arterial disease this would expose the patient to an increased risk of amputation. In patients with peripheral arterial disease debridement should only be initiated by the specialist vascular team, ideally after adequate revascularisation has been established. Figure 1
3 When to debride? The type of tissue found in the wound bed often provides a clear indication as to whether debridement is required but other factors such as bio-burden, wound edges and condition of peri wound skin can also influence the decision of whether debridement is required. There are relatively few wounds where it is not safe to debride so long as the correct method of debridement is chosen, (Wounds UK, 2013). Where there is any evidence of slough (Figure 2), necrotic tissue or eschar (Figures 3 & 4) debridement of this non-viable tissue will aid to progress the wound towards healing. The presence of non-viable tissue will delaying wound healing as it hinders the formation of granulation tissue but it can also be a cause of bacterial growth increasing the risk of infection, (Broadus, 2013). Debridement may also assist in wound assessment or pressure ulcer categorisation as removing nonviable tissue, slough and excess exudate this will help to visualise the wound bed depth and condition more accurately, (Ousey & Cook, 2011). Figure 2 Figure 3
4 Figure 4 Debridement options Various factors influence the choice of method of debridement such as wound type, anatomical location, extent of devitalised tissue, pain, patient environment, resources and patient choice. Debridement may only need to be performed once but more commonly episodic or continual debridement may be required over a number of weeks, (Ousey & Cook, 2012). Therefore there needs to be consideration of the risk that the devitalised tissue presents to the patient to help determine the speed of debridement required. Wound debridement remains a generalist nursing skill and all practitioners involved in wound care need to be aware of the wide range of debridement options. However, certain methods of debridement, such as sharp debridement, can only be performed by clinicians with appropriate knowledge and clinical skills. Nevertheless, it is important that the most appropriate debridement method selected is based on it providing best outcomes for the patient and not merely limited to the skills of the practitioner. If the practitioner feels they do not have the knowledge/skills to perform the certain methods of debridement they should seek support from others or refer the patient on to someone with the requisite skills, such as specialist wound nurses. For many wounds more than one method of debridement may be required and currently there is no robust evidence favouring one method of debridement over another.
5 Methods of debridement commonly used in the United Kingdom (UK) include: Autolytic Larval Mechanical Sharp Surgical Autolytic Autolytic debridement is the most commonly used method of debridement, it refers to the use of the body s own enzymes and moisture to rehydrate, soften and liquefy devitalised tissue, (Gray et al., 2010). The majority of wound dressings, such as hydrogels, hydrocolloids, and hydrofibres, debride by the process of autolysis. Wound dressings facilitate debridement by either donating moisture or maintaining a moist wound environment which provides the optimal environment for the body s enzymes to break down the non-viable tissue. The advantages of autolytic debridement is that there is relatively little pain associate with this form of treatment, it is versatile, selective and requires minimal skill/training. Autolytic debridement is useful where there are small volumes or superficial slough, however it can be a slow process often taking weeks to achieve a clean wound bed, this slow rate of debridement may raise the potential for infection and maceration of the peri-wound skin, (Gray et al., 2010). Larval Larval therapy (maggots) is a form of biological debridement (Figure 5), the larvae of the greenbottle fly has been bred in sterile conditions for medical use for a number of years. The maggots debride by secreting a proteolytic enzyme which liquefies the dead tissue, once this tissue is dissolved the maggots then ingest the fluid neutralising any bacteria in their gut. They don t, as commonly believed, bite or chew the dead tissue. Other benefits of larvae therapy have been published including increased irrigation of the wound bed by the movement of the larvae stimulating exudate production (Sherman, 2002) and increased granulation growth rates through the changes in PH level on the wound bed increasing oxygenation and number of growth factors, (Wollina, Liebold, & Schmidt, 2002). Larval therapy offers a fast selective method of debridement but is not suitable for all wounds. The effectiveness solely relies on the survival of the larvae, so there needs to be consideration of whether they may be squashed, for instance if used on a heel of an active patient or if exudate levels are very high that they may drown. The application of loose maggots can be tricky and does require previous training, however, the marketing of bagged maggots has reduced the specialist skill level previously required. Not all patients accept the idea of maggots on their wound and detailed conversations with
6 the patient must take place prior to their application to ensure the patient is fully informed and consents to treatment. Figure 5 Mechanical Mechanical debridement refers to the physical removal of devitalised tissue, historically this was associated with the use of wet to dry gauze where the top of the wound was effectively ripped from the underlying structure, this non-discriminatory method resulted in damage to the healthy tissue and significant pain for the patient so has not been used for many decades within the UK. However, in recent years mechanical debridement is on the rise with the use of monofilament debridement pads (Debrisoft). Debrisoft is a single use, soft, polyester fibre pad which is wiped across the wound in either circular or vertical motions (depending on tissue type), dead cells and wound debris are caught within the fibres and removed from the wound bed, (Atkin, 2014). The advantages of debridement using Debrisoft is that is it easy to perform, requires little training, it is a fast effective method which causes no damage to the healthy underlying or surrounding tissue. Debrisoft has recently been
7 included in a technology appraisal conducted by the National Institute for Health and Care Excellence (NICE), (NICE, 2014). After reviewing the published evidence NICE supported the use of Debrisoft as an effective method of wound debridement which additionally could reduce costs of patient care in the community setting. NICE calculated that Debrisoft could save the National Health Service up to 484 per patient of completed debridement episode compared to standard practice, (NICE, 2014). However, effectiveness is dependent on tissue type; debridement with monofilament pads is not effective on dry eschar, hard necrotic tissue or thick dehydrated slough. Sharp Debridement Sharp debridement involves the removal of dead tissue with a scalpel, pair of scissors or forceps, in many cases the level of debridement is just above the level of viable tissue. Sharp debridement can only be performed by practitioners who have undergone appropriate training and who are able to prove competency in this area. In experienced hands sharp debridement is a fast, selective and effective means to remove de-vitalised tissue which it is often pain free for the patient. Surgical debridement Surgical debridement is the fastest and usually the most thorough method available, (Stephen-Haynes & Thompson, 2007). It is usually performed in an operating theatre and involves an anaesthetist and a surgical practitioner resulting in this being a high cost option. In many instances it results in a larger wound being created as surgical debridement is not as selective as some other methods, and frequently an element of viable tissue is also removed. Due to these issues surgical debridement tends to be reserved for patients with extensive tissue damage or those facing risk from increasing virulent infection such as diabetic foot ulceration or necrotising fasciitis. Conclusion Debridement is an integral part of wound management, the aim of debridement is to remove nonviable tissue allowing wound healing to occur. Many different methods of debridement are available each with their own specific advantages and disadvantages. Nurses based in community settings continue to provide the majority of wound care to patients, in order to deliver high quality care they need to be confident that they posess the required knowledge and skills to accurate assess the wound, to formulate appropriate aims of care and to select the most applicable method of debridement. Failure to select the most appropriate method of debridement may lead to delays in wound healing, increased costs and unnecessary patient suffering.
8 Reference List Atkin, L. (2014). Understanding methods of wound debridement. British Journal of Nursing, 23(12). Broadus, C. (2013). Debridement options: BEAMS made easy. Wound Care Advisor, 2(2), Cook, L. (2012). Wound Assessment. British journal of nursing (Mark Allen Publishing), 21(20a), 4-6. Gray, D., Acton, C., Chadwick, P., Fumarola, S., Leaper, D., Morris, C.,... Young, T. (2010). Consensus guidance for the use of debridement techniques in the UK. Wounds UK, 6(4). NICE. (2014). National Institute for Heath and Care Excellence medical technology guidance 17: The Debrisoft monofilament debridement pad for use in acute or chronic wounds.. O'Brien, J. (2003). Debridement: ethical, legal and practical considerations. British journal of community nursing, 8(Supplement 3), Ousey, K., & Cook, L. (2011). Understanding the importance of holistic wound assessment. Practice nursing, 22(6), Ousey, K., & Cook, L. (2012). Wound Assessment: made easy. Wounds UK, 8(2), 1-4. Sherman, R. A. (2002). Maggot versus conservative debridement therapy for the treatment of pressure ulcers. Wound Repair and Regeneration, 10, Stephen-Haynes, J., & Thompson, G. (2007). The different methods of wound debridement. British journal of community nursing, 12(sup3), S6-S16. Strohal, R., Apelqvist, J., & Dissemond, J. (2014). EWMA Document: Debridement: An updated overview and clarification of the principle role of debridement. Journal of wound care, 22(sup1), S1-S49. Wollina, U., Liebold, K., & Schmidt, W. (2002). Biosurgery supports granulation and debridement in chronic wounds - clinical data and remittance spectroscopy measurements. International Society Dermatology, 41, World Union of Wound Healing Societies. (2008). Principles of Best Practice: Diagnostics and Wounds. A consensus document Wounds UK. (2013). Effective debridement in a changing NHS: a UK consensus.
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014
 Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Appropriate targeted foot care of
 Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
Medical technology guidance
 NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS)
 CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
Debridement masterclass <KOL>
 Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Fundamentals Of Wound Management. Julie Hewish Senior Tissue Viability Nurse
 Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
DEBRIDEMENT. Four Methods of Debridement
 Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Consensus guidance for the use of debridement techniques in the UK
 Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Slough is a complex, generally fibrinous,
 Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
Haycocks and Chadwick (2012)
 SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Debridement within the context of the EWMA s debridement guidelines. Emil Schmidt WCNS SDHB - Otago
 Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Larval Debridement Therapy Making healing possible
 Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
Use of an outside force to remove nonviable. Wound Debridement Guide South West Regional Wound Care Program Last Updated March 12,
 Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Protocol for the Use of Sterile Larvae in Wound Management
 Protocol for the Use of Sterile Larvae in Wound Management Approved by: CHS Clinical Policy Group and Clinical Quality and Governance Committee On: 10 August 2009 Review Date: 31 July 2011 Directorate
Protocol for the Use of Sterile Larvae in Wound Management Approved by: CHS Clinical Policy Group and Clinical Quality and Governance Committee On: 10 August 2009 Review Date: 31 July 2011 Directorate
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT. Policy Number: 122
 TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
Workshop on Debridement
 MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus
 GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
Autolysis: mechanisms of action in the removal of devitalised tissue in wounds
 Autolysis: mechanisms of action in the removal of devitalised tissue in wounds Authors: Alan A. Rogers, Mark G. Rippon, Leanne Atkin, Karen Ousey Alan A. Rogers, Independent Wound Care Consultant, UK Mark
Autolysis: mechanisms of action in the removal of devitalised tissue in wounds Authors: Alan A. Rogers, Mark G. Rippon, Leanne Atkin, Karen Ousey Alan A. Rogers, Independent Wound Care Consultant, UK Mark
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing Jalal
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing Jalal
Tissue Viability. Autolysis: mechanisms of action in the removal of devitalised tissue. November In association with
 November 2016 In association with Tissue Viability Autolysis: mechanisms of action in the removal of devitalised tissue Leanne Atkin, Vascular Nurse Specialist/Lecturer Practitioner, Mid Yorks NHS Trust/University
November 2016 In association with Tissue Viability Autolysis: mechanisms of action in the removal of devitalised tissue Leanne Atkin, Vascular Nurse Specialist/Lecturer Practitioner, Mid Yorks NHS Trust/University
EWMA Educational Development Programme. Curriculum Development Project. Education Module. Wound Infection
 EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Making healing possible. Patients & Carers Guide Answers to your common questions
 Making healing possible Patients & Carers Guide Answers to your common questions If you are reading this, it is likely that you are considering larval therapy as part of a course of wound treatment. This
Making healing possible Patients & Carers Guide Answers to your common questions If you are reading this, it is likely that you are considering larval therapy as part of a course of wound treatment. This
Larval debridement therapy (LDT)
 Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
Understanding the importance of holistic wound assessment
 Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
AWMA MODULE ACCREDITATION. Module Seven: Conservative Sharp Wound Debridement
 AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
Wound Assessment & Treatment
 Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
This article is based on a symposium held
 Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Education Module. Use of Conservative Sharp Wound Debridement to Debride Necrotic Tissue in Wounds
 British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
MANAGEMENT OF DIABETIC WOUNDS : HEALTH CLINIC SETTING DR NORLIZAH PAIDI FAMILY MEDICINE SPECIALIST KLINIK KESIHATAN BANDAR MAS KOTA TINGGI JOHOR
 MANAGEMENT OF DIABETIC WOUNDS : HEALTH CLINIC SETTING DR NORLIZAH PAIDI FAMILY MEDICINE SPECIALIST KLINIK KESIHATAN BANDAR MAS KOTA TINGGI JOHOR OUTLINE DEFINITION FACTORS CONTRIBUTING TO WOUND DEVELOPMENT
MANAGEMENT OF DIABETIC WOUNDS : HEALTH CLINIC SETTING DR NORLIZAH PAIDI FAMILY MEDICINE SPECIALIST KLINIK KESIHATAN BANDAR MAS KOTA TINGGI JOHOR OUTLINE DEFINITION FACTORS CONTRIBUTING TO WOUND DEVELOPMENT
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Haemoglobin. Granulox: TOPICAL HAEMOGLOBIN
 QUICK GUIDE Haemoglobin Granulox: TOPICAL HAEMOGLOBIN OXYGEN AND WOUND HEALING 1 Oxygen is needed at all phases of wound healing Insufficient wound tissue oxygenation is a major risk factor for delayed
QUICK GUIDE Haemoglobin Granulox: TOPICAL HAEMOGLOBIN OXYGEN AND WOUND HEALING 1 Oxygen is needed at all phases of wound healing Insufficient wound tissue oxygenation is a major risk factor for delayed
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Healthcare Improvement Scotland
 Article Relevance of a Health Technology Assessment report: antimicrobial wound dressings for diabetic foot chronic wounds with local infection Lynne Watret, Alison Rodgers, Karen Macpherson, Susan Myles,
Article Relevance of a Health Technology Assessment report: antimicrobial wound dressings for diabetic foot chronic wounds with local infection Lynne Watret, Alison Rodgers, Karen Macpherson, Susan Myles,
8-5cover.qxd 11/14/2006 5:09 PM Page 1 $20.00 (US)
 $20.00 (US) CASE REPORT Peer Reviewed Wound Management in a Trumpeter Swan using Honey and a Sustained Release Ionic Silver Hydrogel Christoph Mans, med vet; Janet Sunohara-Neilson, MSc; Geraldine Higginson,
$20.00 (US) CASE REPORT Peer Reviewed Wound Management in a Trumpeter Swan using Honey and a Sustained Release Ionic Silver Hydrogel Christoph Mans, med vet; Janet Sunohara-Neilson, MSc; Geraldine Higginson,
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Effective Wound Healing: Getting Back to the Basics. Bill Richlen PT, WCC, DWC
 Effective Wound Healing: Getting Back to the Basics Bill Richlen PT, WCC, DWC What Is Happening Currently? There is a lack of education in current wound care principles and evidence-based practice We have
Effective Wound Healing: Getting Back to the Basics Bill Richlen PT, WCC, DWC What Is Happening Currently? There is a lack of education in current wound care principles and evidence-based practice We have
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE
 Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
ALLEVYN Life Advanced Foam Wound Dressings
 ALLEVYN Life Advanced Foam Wound Dressings ALLEVYN Life Dressings have a multi-layered design incorporating hydrocellular foam, a hyper-absorber lock away core and a masking layer that has been designed
ALLEVYN Life Advanced Foam Wound Dressings ALLEVYN Life Dressings have a multi-layered design incorporating hydrocellular foam, a hyper-absorber lock away core and a masking layer that has been designed
GUIDELINES FOR THE USE OF STERILE MAGGOT THERAPY IN WOUND MANAGEMENT
 GUIDELINES FOR THE USE OF STERILE MAGGOT THERAPY IN WOUND MANAGEMENT Aim To provide evidence based guidelines on the use of sterile maggots and management of patients receiving this therapy. Background
GUIDELINES FOR THE USE OF STERILE MAGGOT THERAPY IN WOUND MANAGEMENT Aim To provide evidence based guidelines on the use of sterile maggots and management of patients receiving this therapy. Background
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
BIOSORB GELLING FIBRE DRESSING. Key facts: In vitro evidence
 BIOSORB GELLING FIBRE DRESSING Key facts: In vitro evidence BIOSORB Gelling Fibre Dressing WHAT IS IT? BIOSORB Gelling Fibre Dressing is a soft, conformable non-woven dressing made from sodium carboxymethyl
BIOSORB GELLING FIBRE DRESSING Key facts: In vitro evidence BIOSORB Gelling Fibre Dressing WHAT IS IT? BIOSORB Gelling Fibre Dressing is a soft, conformable non-woven dressing made from sodium carboxymethyl
JoyTickle, Tissue Viability Nurse Specialist, Shropshire Community Health NHS Trust
 Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Currently, the NHS is facing the challenge of
 Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
SAMPLE. HLTEN406A Undertake basic wound care. Learner resource. HLT07 Health Training Package. Version 2
 HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Essity Internal. Taking the fear out of wound infection: conquering everyday issues
 Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Challenge your practice: venous leg ulcers
 Challenge your practice: venous leg ulcers evidencebased practice clinical judgement patient choice patient choice clinical judgement evidence-based practice clinical judgement patient choice practice
Challenge your practice: venous leg ulcers evidencebased practice clinical judgement patient choice patient choice clinical judgement evidence-based practice clinical judgement patient choice practice
