Some observations we are making
|
|
|
- Wilfred Young
- 5 years ago
- Views:
Transcription
1 Some observations we are making The audience is very smart and they know how to diagnose a neuropathy. There is a standard workup that all patients seem to get: B12, folate, RPR, TSH prior to them being referred to a neurologist. So the purpose of the talk will hopefully make the point of pitfalls in the diagnosis of neuropathy, how to think about diseases that mimic neuropathy and to expand your differential diagnosis and keep you interested with some challenging problems. Case 1: Burning and tingling in the legs How do we interpret this history? MD is an otherwise healthy 89 year old woman who complains of burning and tingling in her feet. She notices that this is worse when she walks a distance and it is worse at night when she lies flat on her back. How do we distinguish between neurogenic claudication vs. vascular claudication? How do we distinguish between the pain of a neuropathy vs. lumbosacral polyradiculopathy These two distinctions are important to make as it drives the workup in a different way Remember also that elderly patients may have multiple pathologies
2 Physical Examination She has excellent distal pulses and no risk factors for vascular disease She does have a known history for lumbar spinal stenosis There is no history of weight loss, night sweats and she has a normal diet. Physical examination of her legs demonstrates mild weakness of both EDB muscles. There is a distal length-dependent gradient of sensory hyperesthesia to light touch and pinprick to the level of the mid-calf. Joint position sense is impaired at the toes and there is mildly diminished vibration sense. Workup Blood work demonstrates normal B12 and MMA levels Normal blood sugar and an % HgBA1C of 5.0 SPEP: Monoclonal Gammopathy: Abnormal band in the Gamma Region identified as IgM Lambda (915mg/dl) which is 6% of total protein. There were no Bence Jones Proteins in the urine MGUS: Monoclonal gammopathy of uncertain signficance Common in the general population and occur in 10% of patients with peripheral neuropathy. Initial workup is to look for Bence Jones Proteins in the urine, a skeletal survey and a consult with a hematologist. Annual SPEP as there is a transformation rate of 1% per year to a symptomatic plasma cell disorder. High risk factors for transformation include: M protein of 15g/l or greater Elevated free light chain ratio (ratio of kappa to lambda free light chains) Non IgG protein Hematological Disorders associated with paraproteinemias Overrepresentation of IgM paraprotein in patients with neuropathy Paraproteinemic Neuropathies Paraproteinemic Neuropathies Mauermann, Michelle L. CONTINUUM: Lifelong Learning in Neurology. 20(5, Peripheral Nervous System Disorders): , October Mauermann, Michelle L. CONTINUUM: Lifelong Learning in Neurology. 20(5, Peripheral Nervous System Disorders): , October Copyright 2016 American Academy of Neurology. Published by Lippincott Williams & Wilkins. 16 Copyright 2016 American Academy of Neurology. Published by Lippincott Williams & Wilkins. 17
3 Neuropathy Patterns and Type of Neuropathy Associated with multiple myeloma Treatment options Symptomatic relief: Anticonvulsants Tricyclic antidepressants SSRI s MGUS: First repeat SPEP at 6 months and then annually If IGA and Ig M paraproteinemia (less motor weakness and if sensory ataxia) consider IVIG, plasmapheresis or even Rituximab (anticd20 activity). Paraproteinemic Neuropathies Mauermann, Michelle L. CONTINUUM: Lifelong Learning in Neurology. 20(5, Peripheral Nervous System Disorders): , October Waldenstroms: per hematology, treatment is directed at bulky disease Myeloma: Neuropathy largely induced by treatment: Bortezomib (70%), Thalidomide (58-81%) POEMS Syndrome: Demyelinating polyneuropathy treated with plasma exchange, IVIG and radiation to the solitary plamacytoma Copyright 2016 American Academy of Neurology. Published by Lippincott Williams & Wilkins. 18 Case 2 presentation A 45-year-old teacher presented with a 6-month history of progressive bilateral foot, right thigh, and left face paresthesia. She denied loss of vision, diplopia, dysarthria, dysphagia, incontinence, limb weakness, or balance difficulty. She was recently diagnosed with hypertension and started on atenolol. She has a longstanding history of Type 1 diabetes (onset in her early 30 s), well controlled with an A1C of 7.2. She was married with three children. She drank socially and did not smoke. She had a family history of Type 1 diabetes and ovarian cancer. Case presentation Physical examination was remarkable for reduced sensation to pinprick in the V2 distribution of the left face and reduced sensation to pinprick in the right thigh and foot. The remainder of the neurologic examination was normal. MRI of the brain was normal. Electrodiagnostic testing of the legs, including bilateral sural and superficial peroneal responses, was normal. Blink reflex responses were normal. So what would you do next? Skin biopsy revealed normal right distal leg intraepidermal nerve fiber density and reduced right thigh intraepidermal nerve fiber density.
4 Is this just a small fiber neuropathy related to Diabetes? Complete blood count and metabolic profile normal Hemoglobin A 1c 7.2 Lyme disease, angiotensin converting enzyme, anti Hu antibodies, HIV, antinuclear antibodies, erythrocyte sedimentation rate, C reactive protein, doublestranded DNA, SS A, SS B, and gliadin IgA were normal. Serum gliadin immunoglobulin (Ig) G and transglutaminase antibody levels were elevated. Duodenal biopsy revealed severe villous flattening, crypt hyperplasia, and intraepithelial lymphocytosis. Comment: This patient has a length-independent small fiber sensory polyneuropathy, which is confirmed by a decreased intraepidermal nerve fiber density. Lonstanding association of Type 1 diabetes and celiac disease A diagnosis of celiac disease (gluten-sensitive enteropathy) is suspected based upon the elevated gliadin IgG and transglutaminase antibodies and is confirmed by the duodenal biopsy findings. Celiac neuropathy may occur in patients without gastrointestinal complaints. Case 3 CS is an 18 year old college freshman with a history of Type 1 diabetes since the age of 5. Her diabetes is well controlled with an insulin pump and she is very vigilant. She reports worsening pain in her feet with tingling and numbness and is worried about diabetic neuropathy. Pertinent Physical Examination of her feet She has high arches (pes cavus) There is mild weakness of foot and toe dorsiflexion. She is areflexic in her legs There is a stocking glove loss (to her mid calf) involving pinprick, light touch, cold, joint position and vibration sense Her gait is high stepping and she has a positive Romberg. Single Gene Causes of CMT Hereditary Neuropathy Type 1 Pathology Mode of Inheritance Proportion of CMT CMT1 Abnormal myelin AD ~50% What would you do next? CMT2 Axonopathy AD ~20-40% Intermediate form Combination of myelin and axonopathy AD Rare CMT4 Either myelinopathy or axonopathy AR Rare CMTX Axonopathy with secondary myelin changes X-linked ~10-20%
5 Segmental duplication in area containing PMP 22 gene on 1 chromosome 17 Occurs with abnormal alignment during meiotic crossing over Leads to total of 3 copies of PMP 22 gene Treatment options for neuropathy: Big discussion General principles Try to treat the underlying cause (30% of the time we will find a treatable cause) If medication related, will have to stop the medicine if possible (difficult decision with chemotherapy). Stop all alcohol Avoid narcotics Multimodal therapy: Tricyclics, Anticonvulsants, SNRI s etc Symptomatic treatment Systemic treatment for demyelinating neuropathies: plasmapheresis, IVIG Orthopedic supports: AFO s, podiatry, foot orthotics, aqua therapy Case 4: Sudden ascending weakness and rash WR is a 67 year old man with a history of coronary artery disease who underwent a cardiac catheterization at a hospital in New Hampshire. Approximately 5 months later, he felt ill and complained of a rash that developed over his legs. He quickly developed weakness in his legs and was unable to support his weight. He was diagnosed with Hepatitis C, which was contracted by contaminated needles during his cardiac catheterization procedure. He had been tested for Hep C following a blood transfusion 6 months prior to the cardiac catheterization. Additional history: He noted weakness in his legs while walking his dog. He had difficulty getting up out of a chair. He fell many times. He has trouble with his memory. He also has trouble now holding a pen. Things got worse, but the rash on the legs together with the weakness prompted him to be transferred from the outside hospital. Neurological Examination There was weakness in the intrinsic muscles of his hands There was marked weakness of his iliospoas, hamstrings and quadriceps bilaterally (4/5). There is severe weakness of both EHL muscles and he has bilateral foot drop and flail ankles. There is asymmetric median sensory loss distribution to pinprick in the hands and he has stepwise loss to pinprick in the legs. He has absent joint position sense and vibration sense. There are no reflexes attainable in his legs. How do we put the examination together with the rash?
6 Localization of his neurological findings Global weakness, all muscles involved Areflexia Step wise sensory loss Multiple nerves: Median, common peroneal MONONEURITIS MULTIPLEX Neuropathology Small vessel vasculitis involving vessels of the epineurium with fibrinoid necrosis and apoptotic debris within the vessel wall Vasculitic Neuropathy: Mechanism of Injury Vasculitic Neuropathy: Clinical Presentation Acute or subacute symptom onset Chief Concerns: Pain Deep aching pain = poorly localized (attrib to acute ischemia) Cutaneous burning pain hours-days later Painful sensory/sensorimotor neuropathy Mononeuritis multiplex (sometimes confluent) and asymmetric polyneuropathy = most common neurological manifestations Initial symptoms generally in lower limbs, feet Associated Symptoms: migratory arthralgias, myalgias, respiratory symptoms, weight loss, abdominal pain Autonomic dysfunction Uncommon Vasculitic Neuropathy: Investigation CSF Most helpful to evaluate for mimickers SERUM CBC, chem-7 SPEP Hep B + C, HIV, lyme Cryoglobulins and test rheumatoid factor which binds to an epitope +/- complement levels (if suspect cryo or SLE) ESR, CRP, ANA, RF, ACE ANCA Final Diagnosis Cryoglobulinemic Vasculitis secondary to acute Hepatitis C
Jonathan Katz, MD CPMC
 Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017
 A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
The Internist s Approach to Neuropathy
 The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
PERIPHERAL NERVE WORKUP FORM (PNW)
 PERIPHERAL NERVE WORKUP FORM (PNW) The Peripheral Nerve Workup Form (PNW) has to be filled out at the time a new patient is enrolled into the PNRR study. Only testing conducted within 36 months of visit
PERIPHERAL NERVE WORKUP FORM (PNW) The Peripheral Nerve Workup Form (PNW) has to be filled out at the time a new patient is enrolled into the PNRR study. Only testing conducted within 36 months of visit
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
Diabetic Neuropathy. Nicholas J. Silvestri, M.D.
 Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
sensory nerves, motor nerves, autonomic nerves
 damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic: long term, begins subtly
damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic: long term, begins subtly
Peripheral neuropathy (PN)
 Peripheral neuropathy (PN) damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic:
Peripheral neuropathy (PN) damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic:
PERIPHERAL NEUROPATHIES
 PERIPHERAL NEUROPATHIES DIAGNOSIS AND TREATMENT Stefanie Geisler, MD Assistant Professor Neuromuscular Division Department of Neurology Washington University Saint Louis Financial disclosures Funding:
PERIPHERAL NEUROPATHIES DIAGNOSIS AND TREATMENT Stefanie Geisler, MD Assistant Professor Neuromuscular Division Department of Neurology Washington University Saint Louis Financial disclosures Funding:
Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy
 Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy Causes of chronic polyneuropathy Signs and symptoms Large fiber modalities Ataxia esp. in the dark Are you ok in the shower
Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy Causes of chronic polyneuropathy Signs and symptoms Large fiber modalities Ataxia esp. in the dark Are you ok in the shower
ACUTE AND CHRONIC NEUROPATHIES
 ACUTE AND CHRONIC NEUROPATHIES American College of Osteopathic Internists Internal Medicine Board Review Course 2018 April 25-29, 2018 Marriott Chicago Downtown Chicago, Illinois Scott Spradlin D.O.,FACP,FACOI
ACUTE AND CHRONIC NEUROPATHIES American College of Osteopathic Internists Internal Medicine Board Review Course 2018 April 25-29, 2018 Marriott Chicago Downtown Chicago, Illinois Scott Spradlin D.O.,FACP,FACOI
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Doc, DO I Have Neuropathy?
 Doc, DO I Have Neuropathy? Stanley Jones P. Iyadurai, MSc, PhD, MD Assistant Professor of Neurology Neuromuscular Division, Department of Neurology The Ohio State University Wexner Medical Center Case
Doc, DO I Have Neuropathy? Stanley Jones P. Iyadurai, MSc, PhD, MD Assistant Professor of Neurology Neuromuscular Division, Department of Neurology The Ohio State University Wexner Medical Center Case
Symptomatic pain treatments (carbamazepine and gabapentin) were tried and had only a transient and incomplete effect on the severe pain syndrome.
 Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Immune Mediated Neuropathies
 Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
PART IV: NEUROPATHIC PAIN SYNDROMES JILL SINDT FEBRUARY 7, 2019
 PART IV: NEUROPATHIC PAIN SYNDROMES JILL SINDT FEBRUARY 7, 2019 NEUROPATHIC PAIN PAIN ARISING AS DIRECT CONSEQUENCE OF A LESION OR DISEASE AFFECTING THE SOMATOSENSORY SYSTEM AFFECTS 3-8% OF POPULATION
PART IV: NEUROPATHIC PAIN SYNDROMES JILL SINDT FEBRUARY 7, 2019 NEUROPATHIC PAIN PAIN ARISING AS DIRECT CONSEQUENCE OF A LESION OR DISEASE AFFECTING THE SOMATOSENSORY SYSTEM AFFECTS 3-8% OF POPULATION
Diabetic Neuropathy WHAT IS DIABETIC NEUROPATHY?
 Diabetic Neuropathy WHAT IS DIABETIC NEUROPATHY? D iabetic neuropathy is actually a group of nerve diseases. All of these disorders affect the peripheral nerves, that is, the nerves that are outside the
Diabetic Neuropathy WHAT IS DIABETIC NEUROPATHY? D iabetic neuropathy is actually a group of nerve diseases. All of these disorders affect the peripheral nerves, that is, the nerves that are outside the
DISCLOSURES. UCSF Continuing Medical Education Neuropathy Pearls. Overview. Neuropathy terminology. Topics to be covered:
 UCSF Continuing Medical Education DISCLOSURES Nothing to Disclose Laura K. Rosow, MD Overview Topics to be covered: Neuropathy definitions, terminology Evaluation of the patient with neuropathy History
UCSF Continuing Medical Education DISCLOSURES Nothing to Disclose Laura K. Rosow, MD Overview Topics to be covered: Neuropathy definitions, terminology Evaluation of the patient with neuropathy History
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Numbness in right leg icd 10
 Search Search Numbness in right leg icd 10 A list of the most commonly used ICD -9 codes in Physical Medicine & Rehabilitation and Pain Management clinics. ICD - 10 codes will be slowly added over time.
Search Search Numbness in right leg icd 10 A list of the most commonly used ICD -9 codes in Physical Medicine & Rehabilitation and Pain Management clinics. ICD - 10 codes will be slowly added over time.
Disclosures. Objectives. Clinical Scenario. Four Common Neurological Problems: An Update for /25/2009. None
 Four Common Neurological Problems: An Update for 2009 Disclosures Vanja Douglas, M.D. Clinical Instructor UCSF Department of Neurology, Neurohospitalist Program None Objectives Learn an approach to the
Four Common Neurological Problems: An Update for 2009 Disclosures Vanja Douglas, M.D. Clinical Instructor UCSF Department of Neurology, Neurohospitalist Program None Objectives Learn an approach to the
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of
 Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Power Line to your Line to your Circuit Line to the station neighborhood house breaker living room. Outlet lamp Lamp with socket, Light bulb
 IMC 606 Neuroscience and Behavior Module Dr. Margaret Paroski Analysis of Sensory Lesions You walk into your living room and turn on the lamp. But no light comes on. What would you do? You would probably
IMC 606 Neuroscience and Behavior Module Dr. Margaret Paroski Analysis of Sensory Lesions You walk into your living room and turn on the lamp. But no light comes on. What would you do? You would probably
Four Common Neurological Problems: An Update for Vanja Douglas, M.D. Clinical Instructor UCSF Department of Neurology, Neurohospitalist Program
 Four Common Neurological Problems: An Update for 2009 Vanja Douglas, M.D. Clinical Instructor UCSF Department of Neurology, Neurohospitalist Program Disclosures None Objectives Learn an approach to the
Four Common Neurological Problems: An Update for 2009 Vanja Douglas, M.D. Clinical Instructor UCSF Department of Neurology, Neurohospitalist Program Disclosures None Objectives Learn an approach to the
Radiculopathy and Polyneuropathy
 Objectives Radiculopathy and Polyneuropathy Jeffrey W. Ralph, MD Jeffrey.Ralph@ucsf.edu UCSF Department of Neurology Advances in Internal Medicine May 24 and June 28, 2012 Radiculopathy Anatomy & Signs
Objectives Radiculopathy and Polyneuropathy Jeffrey W. Ralph, MD Jeffrey.Ralph@ucsf.edu UCSF Department of Neurology Advances in Internal Medicine May 24 and June 28, 2012 Radiculopathy Anatomy & Signs
Evaluating an Apparent Unprovoked First Seizure in Adults
 Evaluating an Apparent Unprovoked First Seizure in Adults Case Presentation A 52 year old woman is brought to the emergency room after a witnessed seizure. She was shopping at the local mall when she was
Evaluating an Apparent Unprovoked First Seizure in Adults Case Presentation A 52 year old woman is brought to the emergency room after a witnessed seizure. She was shopping at the local mall when she was
Evaluation of Tingling and Numbness in the Upper Extremities
 Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
POEMS syndrome. This Infosheet explains what POEMS syndrome is, how it is diagnosed and how it is treated and managed.
 POEMS syndrome This Infosheet explains what POEMS syndrome is, how it is diagnosed and how it is treated and managed. What is POEMS syndrome? POEMS syndrome is a rare type of plasma cell disorder that
POEMS syndrome This Infosheet explains what POEMS syndrome is, how it is diagnosed and how it is treated and managed. What is POEMS syndrome? POEMS syndrome is a rare type of plasma cell disorder that
Disclosures. Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies. None
 Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Wartenberg s migrant sensory neuritis: a prospective follow-up study
 J Neurol (2010) 257:1344 1348 DOI 10.1007/s00415-010-5530-7 ORIGINAL COMMUNICATION Wartenberg s migrant sensory neuritis: a prospective follow-up study Abraham C. J. Stork Marjon F. G. van der Meulen W.-Ludo
J Neurol (2010) 257:1344 1348 DOI 10.1007/s00415-010-5530-7 ORIGINAL COMMUNICATION Wartenberg s migrant sensory neuritis: a prospective follow-up study Abraham C. J. Stork Marjon F. G. van der Meulen W.-Ludo
NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1
 267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
FootHuggers Comfort Socks have been found to help people suffering with: Peripheral Neuropathy
 FootHuggers Comfort Socks have been found to help people suffering with: Peripheral Neuropathy Peripheral Neuropathy - Peripheral neuropathy is a term used to describe disorders of your peripheral nervous
FootHuggers Comfort Socks have been found to help people suffering with: Peripheral Neuropathy Peripheral Neuropathy - Peripheral neuropathy is a term used to describe disorders of your peripheral nervous
Is Small-Fiber Neuropathy Killing You?
 Is Small-Fiber Neuropathy Killing You? Presented By: Dr. Greg Fors, DC, DIBCN Board-certified Neurologist (IBCN) Author of the Best-Selling Why We Hurt Maybe Its Small Fiber Sensory NEUROPATHY! Do you
Is Small-Fiber Neuropathy Killing You? Presented By: Dr. Greg Fors, DC, DIBCN Board-certified Neurologist (IBCN) Author of the Best-Selling Why We Hurt Maybe Its Small Fiber Sensory NEUROPATHY! Do you
Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis)
 Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis) Goal: To enhance skills in assessing an article related to diagnostic testing in terms of validity and applying results to
Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis) Goal: To enhance skills in assessing an article related to diagnostic testing in terms of validity and applying results to
THICK AS THIEVES: A CURIOUS CASE OF SJOGREN S SYNDROME. Sophie Wojcik, Dr Murray Baron PGY5 Rheumatology McGill University Friday May 11 th 2018
 THICK AS THIEVES: A CURIOUS CASE OF SJOGREN S SYNDROME Sophie Wojcik, Dr Murray Baron PGY5 Rheumatology McGill University Friday May 11 th 2018 DISCLOSURES! No relevant disclosures MRS H! 34 y.o. woman,
THICK AS THIEVES: A CURIOUS CASE OF SJOGREN S SYNDROME Sophie Wojcik, Dr Murray Baron PGY5 Rheumatology McGill University Friday May 11 th 2018 DISCLOSURES! No relevant disclosures MRS H! 34 y.o. woman,
Nerve Site Latency ms Amplitude mv Distance mm Conduction Velocity m/s
 Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
Painful Diabetic Neuropathy Effective Management. Ketan Dhatariya Consultant in Diabetes NNUH
 Painful Diabetic Neuropathy Effective Management Ketan Dhatariya Consultant in Diabetes NNUH Neuropathic Pain Prevalence varies between 10 and 90% depending on classification Accounts for 50-75% of non-traumatic
Painful Diabetic Neuropathy Effective Management Ketan Dhatariya Consultant in Diabetes NNUH Neuropathic Pain Prevalence varies between 10 and 90% depending on classification Accounts for 50-75% of non-traumatic
Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies
 138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
Charcot-Marie-Tooth Disease (CMT) Sometimes known as Hereditary Motor and Sensory neuropathy (HMSN) or Peroneal Muscular Atrophy (PMA)
 Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy
 Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Clinical Aspects of Peripheral Nerve and Muscle Disease. Roy Weller Clinical Neurosciences University of Southampton School of Medicine
 Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
AII-type: Select the most appropriate answer
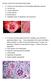 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
JMSCR Vol 04 Issue 12 Page December 2016
 JMSCR Vol 04 Issue 12 Page 14551-14556 December 2016 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i12.42
JMSCR Vol 04 Issue 12 Page 14551-14556 December 2016 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i12.42
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A RARE NEUROLOGICAL PRESENTATION OF SLE. Dr Yoganand M N Dr Prithvi P Nayak
 A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
2/17/2011. Two months after symptom onset, she began experiencing episodic vertigo and unsteadiness that was provoked by riding in the car.
 A young woman with blurry vision and an abnormal brain MRI Ellen M. Mowry, MD, MCR UCSF Multiple Sclerosis Center Recent Advances in Neurology February 16, 2011 History of Presenting Illness A 27-year-old,
A young woman with blurry vision and an abnormal brain MRI Ellen M. Mowry, MD, MCR UCSF Multiple Sclerosis Center Recent Advances in Neurology February 16, 2011 History of Presenting Illness A 27-year-old,
Peripheral Nerve Disorders - P a g e 1. Introduction
 Peripheral Nerve Disorders - P a g e 1 Introduction The peripheral nerves connect the central nervous system (the brain and the spinal cord) to the periphery (the sensory receptors and muscles). An illness
Peripheral Nerve Disorders - P a g e 1 Introduction The peripheral nerves connect the central nervous system (the brain and the spinal cord) to the periphery (the sensory receptors and muscles). An illness
Jo Abraham MD Division of Nephrology University of Utah
 Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
AN INTERESTING CASE OF PROGRESSIVE QUADRIPARESIS DR SHILPA
 AN INTERESTING CASE OF PROGRESSIVE QUADRIPARESIS DR SHILPA CASE: A 50yr old female, homemaker, hailing from Mandya, Chief complaints 1. Weakness of left upper limb since 9months. 2. Weakness of right upper
AN INTERESTING CASE OF PROGRESSIVE QUADRIPARESIS DR SHILPA CASE: A 50yr old female, homemaker, hailing from Mandya, Chief complaints 1. Weakness of left upper limb since 9months. 2. Weakness of right upper
A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging
 61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
DIAGNOSIS OF DIABETIC NEUROPATHY
 DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure
 Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny. Section 1: Today s Date: Date of Birth: Age:
 Baylor Physical Medicine and Rehabilitation NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny Dear Patient: Please complete this questionnaire before you come for your appointment. Be sure to call us as soon
Baylor Physical Medicine and Rehabilitation NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny Dear Patient: Please complete this questionnaire before you come for your appointment. Be sure to call us as soon
DSS-1. No financial disclosures
 DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
peripheral neuropathy peripheral neuropathy neuropathy peripheral neuropathy neuropathic foot heel Bilateral foot pain Bilateral heel pain bilateral
 Peripheral neuropathy (PN) is damage to or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health. The 2018 edition of ICD-10-CM G62.9. Auditory
Peripheral neuropathy (PN) is damage to or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health. The 2018 edition of ICD-10-CM G62.9. Auditory
PNS and ANS Flashcards
 1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
Pain Drawing. Name: Today s Date: How were you referred to the office: Visual Analog Scale
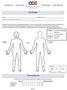 Pain Drawing Name: Today s Date: How were you referred to the office: Please be sure to fill this out as accurately as possible. This will become part of your permanent medical record and will be used
Pain Drawing Name: Today s Date: How were you referred to the office: Please be sure to fill this out as accurately as possible. This will become part of your permanent medical record and will be used
Lec-14 د.خالد نافع. Medicine. Multiple Myeloma
 Fifth stage Lec-14 د.خالد نافع Medicine 24/4/2016 Multiple Myeloma Plasma cell myeloma Variants Non - secretory myeloma Indolent myeloma Smouldering myeloma Plasma cell leukaemia Plasmacytoma - Solitary
Fifth stage Lec-14 د.خالد نافع Medicine 24/4/2016 Multiple Myeloma Plasma cell myeloma Variants Non - secretory myeloma Indolent myeloma Smouldering myeloma Plasma cell leukaemia Plasmacytoma - Solitary
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital
 Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
A Practical Approach to Peripheral Neuropathy
 A Practical Approach to Peripheral Neuropathy Michelle L. Mauermann M.D. Associate Professor of Neurology Mayo Clinic, Rochester MN 2017 MFMER slide-1 Disclosures None 2017 MFMER slide-2 Learning Objectives
A Practical Approach to Peripheral Neuropathy Michelle L. Mauermann M.D. Associate Professor of Neurology Mayo Clinic, Rochester MN 2017 MFMER slide-1 Disclosures None 2017 MFMER slide-2 Learning Objectives
ESI - Utilization Review Case Presentation
 ESI - Utilization Review Case Presentation Request for ESI Hx & PE 31 y/o F parts warehouse stocker DOI: 2008 MOI: felt tightness in legs and shoulders reaching into a shelf to move a product from one
ESI - Utilization Review Case Presentation Request for ESI Hx & PE 31 y/o F parts warehouse stocker DOI: 2008 MOI: felt tightness in legs and shoulders reaching into a shelf to move a product from one
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nerve_fiber_density_testing 2/2010 10/2016 10/2017 10/2016 Description of Procedure or Service Skin biopsy
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nerve_fiber_density_testing 2/2010 10/2016 10/2017 10/2016 Description of Procedure or Service Skin biopsy
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
NEW SPINE PATIENT. Date Seen: Blood Pressure: Pulse: Weight: Height: O 2. How long (days, weeks, or years) has this complaint/problem been going on?
 ROOM #: NEW SPINE PATIENT Date Seen: Blood Pressure: Pulse: Weight: Height: O 2 Sats: For office use only above this line. Patient Name: Referring Physician: Date of Birth: Age: Insurance Carrier: Present
ROOM #: NEW SPINE PATIENT Date Seen: Blood Pressure: Pulse: Weight: Height: O 2 Sats: For office use only above this line. Patient Name: Referring Physician: Date of Birth: Age: Insurance Carrier: Present
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Ahmed Abbas, Mark Cook, Liong Hiew Fu, Alistair Lewthwaite, Colin Shirley, Yusuf A. Rajabally
 2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 4, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 4 Tuesday, September 15, 2015 MHD I, Session 4, STUDENT Copy Page 2 Resource for cases: Robbins Basic Pathology, Chapter
MHD I, Session 4, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 4 Tuesday, September 15, 2015 MHD I, Session 4, STUDENT Copy Page 2 Resource for cases: Robbins Basic Pathology, Chapter
Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
 doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy
 Lepr Rev (2008) 79, 441 446 CASE REPORT Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy JIANPING SHEN*, GUOCHENG ZHANG*, RONGDE YANG**, TINGYING HU** & MIN ZHOU*
Lepr Rev (2008) 79, 441 446 CASE REPORT Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy JIANPING SHEN*, GUOCHENG ZHANG*, RONGDE YANG**, TINGYING HU** & MIN ZHOU*
e) None of the above e) None of the above
 Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Muscle Pathology Surgical Pathology Unknown Conference. November, 2008 Philip Boyer, M.D., Ph.D.
 Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Subacute combined degeneration of the spinal cord following recreational nitrous oxide use
 Subacute combined degeneration of the spinal cord following recreational nitrous oxide use Jae Park Hui Mei Cheng Royal Perth Hospital, Perth Western Australia Australia Background and aim Subacute combined
Subacute combined degeneration of the spinal cord following recreational nitrous oxide use Jae Park Hui Mei Cheng Royal Perth Hospital, Perth Western Australia Australia Background and aim Subacute combined
Multiple Myeloma 101: Understanding Your Labs
 Multiple Myeloma 101: Understanding Your Labs Tim Wassenaar MD MS Hematologist, Director of Clinical Trials UW Cancer Center at ProHealth Care None Disclosures Outline Define hematopoiesis WBCs, RBCs,
Multiple Myeloma 101: Understanding Your Labs Tim Wassenaar MD MS Hematologist, Director of Clinical Trials UW Cancer Center at ProHealth Care None Disclosures Outline Define hematopoiesis WBCs, RBCs,
Polyneuropathy has an estimated FAMILY PRACTICE
 For mass reproduction, content licensing and permissions contact Dowden Health Media. THE JOURNAL OF An easy approach to evaluating peripheral neuropathy Ask what, where, when, and in what setting to narrow
For mass reproduction, content licensing and permissions contact Dowden Health Media. THE JOURNAL OF An easy approach to evaluating peripheral neuropathy Ask what, where, when, and in what setting to narrow
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center
 Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
Lactic Acidosis and Ascending Neuromuscular Syndrome. Mina Hosseinipour, M.D, MPH. University of North Carolina Project, Lilongwe Malawi
 Lactic Acidosis and Ascending Neuromuscular Syndrome Mina Hosseinipour, M.D, MPH. University of North Carolina Project, Lilongwe Malawi Introduction ART is rapidly scaling up in resource poor countries
Lactic Acidosis and Ascending Neuromuscular Syndrome Mina Hosseinipour, M.D, MPH. University of North Carolina Project, Lilongwe Malawi Introduction ART is rapidly scaling up in resource poor countries
BRAIN STEM CASE HISTORIES CASE HISTORY VII
 463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD
 Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Preview of the Medifocus Guidebook on: Peripheral Neuropathy Updated January 5, 2019
 Preview of the Medifocus Guidebook on: Peripheral Neuropathy Updated January 5, 2019 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Peripheral Neuropathy. It is intended primarily
Preview of the Medifocus Guidebook on: Peripheral Neuropathy Updated January 5, 2019 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Peripheral Neuropathy. It is intended primarily
WILLIAM K MONTGOMERY, MD
 WILLIAM K MONTGOMERY, MD Knee and Hip Joint Replacement Specialist New Patient Questionnaire NAME: DOB: / / AGE: Your Primary Care Physician: Phone Number: Referring Physician: Phone Number: Are you a
WILLIAM K MONTGOMERY, MD Knee and Hip Joint Replacement Specialist New Patient Questionnaire NAME: DOB: / / AGE: Your Primary Care Physician: Phone Number: Referring Physician: Phone Number: Are you a
Neuropathy, Radiculopathy & Myelopathy. Jean D. Francois, MD Neurology & Neurophysiology
 Neuropathy, Radiculopathy & Myelopathy Jean D. Francois, MD Neurology & Neurophysiology Purpose and Objectives PURPOSE Avoid Confusing Certain Key Neurologic Concepts OBJECTIVES Objective 1: Define & Identify
Neuropathy, Radiculopathy & Myelopathy Jean D. Francois, MD Neurology & Neurophysiology Purpose and Objectives PURPOSE Avoid Confusing Certain Key Neurologic Concepts OBJECTIVES Objective 1: Define & Identify
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Thank you to: L Magy, L Richard, N Couade, F Maquin
 «Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
«Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
The signs and symptoms of diabetic neuropathy vary, depending on the type of neuropathy and which nerves are affected.
 DIABETIC NEUROPATHY Overview Diabetic neuropathy is a type of nerve damage that can occur if you have diabetes. High blood sugar (glucose) can injure nerve fibers throughout your body, but diabetic neuropathy
DIABETIC NEUROPATHY Overview Diabetic neuropathy is a type of nerve damage that can occur if you have diabetes. High blood sugar (glucose) can injure nerve fibers throughout your body, but diabetic neuropathy
