Orthognathic and Orthodontic Treatments for TMJ-osteoarthritis with Jaw Deformity
|
|
|
- Rosamond Russell
- 5 years ago
- Views:
Transcription
1 Orthognathic and Orthodontic Treatments for TMJ-osteoarthritis with Jaw Deformity Eiji TANAKA, DDS, PhD 1, Shinya HORIUCHI, DDS, PhD 2 and Shingo KURODA, DDS, PhD 3 Introduction TMJ disorders TMDs as reported in the early dental literature 1 3 and by Costen 4 in the early medical literature, first promoted TMJ anatomical misalignment as a new and separate source of facial pain. Nowadays, TMDs are characterized by intra-articular morphologic abnormalities, such as traumatic, degenerative and/or inflammatory arthritic pathology, and developmental, congenital and neoplastic processes. A review of 18 epidemiologic studies published in the 1980s reported prevalence rates ranging from 16 to 59 for reported symptoms and 33 to 86 for clinical signs 5, although 3 to 7 of the adult population have sought care for TMD-related pain and dysfunction 6. The most common joint pathology affecting the TMJ is degenerative joint disease, also known as osteoarthrosis or osteoarthritis OA. Mejersjö, et al. 7 reported that 11 of 93 TMD patients had symptoms of TMJ-OA, whereas 50 of the joints 71 of the patients revealed radiographic signs of TMJ structural changes. Furthermore, an epidemiological study, using cephalometrically corrected tomograms, showed that minimal flattening of the condyle and/or eminence was seen in 35 of TMJs in asymptomatic persons no internal derangement 8. More advanced osseous changes were not seen, therefore, it was concluded that minimal flattening was probably of no clinical significance. However, once the breakdown in the joint starts, TMJ-OA can be crippling, leading to a variety of morphological and functional deformities 9. Increased awareness and interest in TMDs, while part of a general trend in dentistry, represents a change in emphasis in orthodontics toward treating more adults 10. At present, more than 30 of all orthodontic patients are adults. By enlarging the scope of their treatment population, orthodontists have already been treating patients who are part of the group most likely to suffer from TMDs. Therefore, orthodontics is part of the interdisciplinary TMJ care team. This paper outlines some basic concepts in the management of TMJ-OA. We propose an orthodontic approach to TMJ- OA from our own clinical experiences, which shows the potential of orthodontics to contribute to TMJ-OA managements. Definition and etiology of TMJ-OA Unlike rheumatoid arthritis, TMJ-OA has a noninflammatory origin 9. The pathological process is characterized by deterioration and abrasion of articular cartilage and local thickening and remodeling of the underlying bone 9. These changes are frequently accompanied by the superimposition of secondary inflammatory changes. Therefore, mechanicallyinduced OA may better reflect TMJ-OA. It was suggested that OA may be a final common pathway for several joint conditions, including inflammatory, endocrine, metabolic, developmental and biomechanical disorders 9. Typical symptoms in TMJ- OA patients are crepitus, TMJ pain, and restriction of mandibular movements, especially mouth opening movement. The characteristic radiographic sign of TMJ-OA is dysfunctional remodeling on the mandibular condyle and articular eminence surfaces with osteophyte formation. OA has been generally regarded as inevitably progressive once it has become clinically symptomatic.
2 Fig. 1 Schematic illustration of the concept of mandibular condylar resorption. TMJ-OA is initiated from mandibular condylar cartilage degradation. Fig. 1 shows a schematic illustration of the concept of mandibular condylar cartilage degradation 11, 12. Under normal conditions, functional loading in the TMJ is essential to functional bone remodeling and metabolism. This loading is absolutely necessary for growth, development and maintenance of the TMJ. However, if the loading is excessive or abnormal, or if the host adaptive capacity decreases due to aging and systematic disease, functional overloading can facilitate hypoxia in the TMJ which mediates the destructive processes associated with OA as an autocrine factor. The induction of vascular endothelial growth factor VEGF in OA-cartilage by functional overloading is linked to activation of the hypoxia-inducing factor, HIF-1, leading to hypoxia in the joint tissue Furthermore, VEGF regulates the production of MMPs and TIMPs which are among the effectors of extracellular matrix remodeling. Overloading also causes collapse of joint lubrication as a result of the degradation of hyaluronic acid by free radicals 12. The regulation of hyaluronic acid production is controlled by various pro-inflammatory cytokines. As a result, TMJ overloading is one of the key factors in the onset and progression of OA. Functional overloading can lead to physical disruption of cells, impaired cellular function, transient ischemia of cell population and neurogenic irritants 16. As a result, joint tissues may collapse Fig. 2. If the collapse occurs in one side of the TMJ, the mandible shifts laterally, resulting in mandibular asymmetry. If the collapse occurs in both TMJs, condylar resorption produces morphologic collapse of the TMJ component and a subsequent decrease in the ramus height, resulting in progressive mandibular retrusion with anterior open bite. Management of TMJ-OA Management of TMJ-OA may be divided into noninvasive, minimally invasive, invasive or surgical modalities, and salvage modalities in end-stage disease. The decision to surgically manage any TMJ arthritic condition must be based on an evaluation of the patient s response to non-invasive management, the patient s mandibular form and function, and the effect the condition has on the patient s quality of life 17. The management goals in TMJ-OA should be: 1. Decreasing joint pain, swelling and reflex masticatory muscle spasm/pain 2. Increasing joint function 3. Preventing further joint damage 4. Preventing disability and disease related morbidity Using a classification scheme based on clinical signs
3 Fig. 2 Samples of MR images in severe TMJ-OA patients: Condylar re sorption and avascular necrosis. and symptoms and imaging, modified from that developed by Steinbrocker, et al. 18 and Kent, et al. 19, this paper presents an evidence-based discussion on the management of TMJ-OA. 1. Non-invasive management modalities 1 Occlusal splint In the clinic, occlusal splints are the most common method of treating pain associated with the TMJ. Occlusal splints are an effective device to protect the TMJ from involuntary overloading, and to reduce the muscle hyperactivity and articular strain due to bruxism. In a controlled study on the effects of occlusal splint therapy in individuals with severe TMJ-OA, a reduction of clinical signs was seen 20. However, a critical evaluation of splint therapy has not yet been conducted due to a lack of evidence, and its clinical effectiveness in relieving pain seems modest compared with that of pain treatment methods in general 21. None of the occlusal adjustment studies provided evidence supporting the use of this treatment method. 2 Medications Non-steroidal anti-inflammatory NSAID agents such as ibuprofen should be used on a time contingent basis to take advantage of their pharmacokinetics. Muscle relaxants may be helpful to control the reflex masticatory muscle spasm/pain Orthotics Oral orthotics, while assisting in the control of parafunctional habits in many patients, also can provide relief from masticatory muscle spasm/pain and, along with a soft diet, will decrease the loads delivered across the TMJ articulation under function. 4 Physical therapy Physical therapeutic modalities act as counter irritants to reduce inflammation and pain. Superficial warm and moist heat or localized cold may relieve pain sufficiently to permit exercise. Therapeutic exercises are designed to increase muscle strength, reduce joint contractures and maintain a functional range of motion. Active and passive jaw movements, manual therapy techniques, and relaxation techniques were used in the management of 20 consecutive TMJ-OA patients. After treatment mean 46 days, pain at rest was reduced by 80 and there was no impairment in 37 of cases Minimally invasive modalities 1 Hyaluronate HA HA, comprising of synovial fluid in normal subjects 24, is one of the principal components determining its rheological properties. It has been
4 demonstrated that injection of HA into joints improves mobility and suppresses pain and inflammation 25, 26. In double blind studies in other joints after 2 months, HA has been shown to provide significantly better results than saline 27, 28. These results were sustained for 1 year. However, the effectiveness of HA injection into the TMJ remains controversial, and so HA has not yet been approved as a safe and effective medication in the management of arthritic disease in the TMJ by the United States Food and Drug Administration. 2 Corticosteroids Intra-articular injections of corticosteroids are of limited use in other joints of the body 29. The main limitations of repeated intra-articular steroid injections are the risks of infection and the destruction of articular cartilage, tendon or ligament attachments. Repeated intra-articular corticosteroid injections have been implicated in the chemical condylectomy phenomenon in the TMJ 30, Arthrocentesis Nitzan, et al. 32 demonstrated that arthrocentesis is a rapid and safe procedure that may result in the TMJ-OA returning to a functional state. Failure of arthrocentesis 32 suggested that painful limitation of TMJ function might be the result of fibrous adhesions or osteophytes that require arthrotomy for management. 4 Arthroscopy The value of TMJ arthroscopy may be in the early diagnosis and management of arthritic processes affecting the TMJ, especially early-stage arthritic disease, to avoid the complications of open bite and ankylo - sis 33, 34. However, late-stage marked fibrosis or ankylosis makes arthroscopy impossible and contra indicates its usefulness. 3. Invasive surgical modalities Bone and joint procedures 1 Arthroplasty Henny, et al. 35 described this procedure high condylar shave as a limited removal of the damaged articular surface of the condyle, which maintains the height of the ramus, the articular disc and the surrounding soft tissue including the lateral pterygoid muscle attachment. Its use was advocated in cases with severe, unremitting OA pain. 2 Autogenous hemiarthroplasty A number of different autogenous tissues have been advocated as a replacement for the TMJ disc 36, however, the literature on the use of the vascularized local temporalis muscle flap appears to present the most applicable data to the management of the arthritic TMJ Osteotomy Although successful outcomes have been reported using orthognathic surgical procedures to manage maxillofacial skeletal discrepancies with signs and symptoms of TMD 39, the treatment outcomes after orthognathic surgery depend on the presurgical TMJ condition. Patients with active TMJ disease and either concomitant or resultant maxillofacial skeletal discrepancies, treated only with orthognathic surgery, often have poor outcomes and significant relapse This implies that patients with presurgical TMJ symptoms requiring mandibular advancement appear to be at increased risk of condylar resorption. Pre-existing TMJ pathologies, with or without symptoms that can lead to unfavorable orthognathic surgery outcomes, include: internal derangements, progressive condylar resorption, condylar hyperplasia, osteochondroma, congenital deformities, and non-salvageable joints 44. Since the TMJs are the foundation of orthognathic surgery, the resultant pathology offers a poor base upon which to build any maxillofacial functional and skeletal reconstruction in conditions where there are gross erosive changes in the articulating components of both the fossa and condyle resulting in loss of vertical height. Furthermore, the degenerative and osteolytic changes that the joint components are undergoing in these conditions make these components of the TMJ highly susceptible to failure under the new functional loading resulting from orthognathic surgical repositioning of the maxillofacial skeleton. Meanwhile, Wolford, et al. 46 reported 12 young patients with active idiopathic condylar resorption who underwent combined TMJ disc repositioning and stabilization with the Mitek anchor Mitek Surgical Products Inc., Westwood, MA and bimaxillary orthognathic surgery followed for 33 months with stable skeletal and occlusal results as well as significant pain relief. Morales-Ryan, et al. 47 also evaluated 44 young idiopathic condylar resorption patients, 10 of whom underwent bimaxillary orthognathic surgery but no TMJ surgery and 34 of whom underwent the management recommended by Wolford, et al. 46. The former 10 patients followed for 37 months were
5 reported as having statistically significant relapse due to progressive condylar resorption, whereas the other 34 patients followed for 25.5 months had no statistically significant relapse due to progressive condylar resorption. Recently, Goncalves, et al. 48 reported 35 patients with degenerative joint disease who underwent combined TMJ disc repositioning and stabilization with the Mitek anchor and orthognathic surgery followed for 31 months with stable skeletal and occlusal results as well as significant pain relief, while 16 patients with preoperative TMJ disc displacement who underwent double-jaw surgery and no TMJ intervention experienced significant relapse. Taken together, maxillomandibular advancement with counterclockwise rotation of the occlusal plane is a stable procedure for patients with healthy TMJs and for patients undergoing simultaneous TMJ disc repositioning using the Mitek anchor technique. However, the patients who had presurgical TMJ symptoms but underwent only orthognathic surgery demonstrated a statistically significant rate of skeletal relapse related to condylar remodeling and resorption. In Japan, surgical disc-repositioning using the Mitek anchor technique is not popular compared with in America. Therefore, orthognathic surgery is not strongly recommended for patients with progressive mandibular retrusion involved in TMJ-OA. 4 Osseodistraction Van Strijen, et al. 49 reported a case of idiopathic condylar resorption 1 year following distraction osteogenesis to advance the mandible in a 15-year-old male. While there was associated post-distraction trauma in this case, the authors advised that since osteoclastic activity in the TMJ has been reported after gradual distraction of the mandible, distraction osteogenesis may make its own contribution to TMJ-OA and idiopathic condylar resorption. Van Strijen, et al. 49 suggested that in the future, patients being considered for surgical management of mandibular hypoplasia should be critically evaluated for any traumatic, functional or metabolic risk factors for OA and condylar resorption. Based on the experience reported in the literature, it is recommended that maxillofacial skeletal discrepancies resulting from active or advanced arthritic TMJ disease should be most predictably managed utilizing the orthopedic principles of total joint replacement, which has been safely and effectively used for over four decades in other joints for these conditions. 4. Salvage procedures - total joint replacement In the TMJ, alloplastic reconstruction has been discussed at length 50, 51. All of these authors agree that when the mandibular condyle is extensively damaged, degenerated or lost, as in arthritic conditions, replacement with either autogenous graft or alloplastic implant is an acceptable approach to achieve optimal symptomatic and functional improvement. Long-term follow-up studies have included patients with diagnoses consistent with low- and high-inflammatory arthritic TMJs in their total alloplastic reconstruction datasets 17, At present, based on the available published clinical data, alloplastic TMJ reconstruction may be most successful for the reconstruction of patients with high-inflammatory TMJ arthritis, for management of reankylosis and loss of posterior mandibular vertical dimension as the result of pathology, or for ablative mandibular surgery in adults. Orthodontic approach to TMJ-OA By using orthognathic surgery, maxillomandibular advancement with counterclockwise rotation in skeletal mandibular retrusion and the resultant anterior open bite can provide significant improvements in both occlusion and facial esthetics. However, as described above, orthognathic surgery might not improve TMD in patients with active TMD symptoms. In addition, orthognathic surgery requires surgical invasion with postoperative discomfort and risks. It is true that morphologic collapse of the joint component by TMJ-OA induces a decrease in the ramus height, leading to a clockwise rotation of the mandible and anterior open bite. These characteristics appear to cause TMJ overloading. From the results of finite element model analysis, the open bite condition can induce larger stress in the TMJ compared with normal occlusion 56. Furthermore, clockwise rotation of the mandible, which is a main characteristic of skeletal open bite, leads to a synergistic increase of the TMJ stress during clenching 56. This indicates that improvement of mandibular clockwise rotation may be essential for the treatment of acquired open bite with TMJ-OA, resulting in the reduction of TMJ overloading. Kuroda, et al. 57, 58 reported that molar intrusion using implant anchorage was quite useful to improve both
6 Fig. 3 Treatment mechanism for mandibular retrusion with anterior open bite involved in condylar resorption. occlusion and facial esthetics in severe anterior open bite patients with a skeletal Class II jaw relationship, because of mandibular counterclockwise rotation and the resultant relatively forward movement of the mandible. In their case reports, the mandibular plane was rotated more than 5 by the molar intrusion, nevertheless the patients after orthodontic treatment did not have any functional problems. These procedures are far less invasive for the patient than a LeFort I osteotomy for maxillary impaction or a mandibular set-forward osteotomy. Therefore, we suggest orthodontic treatment for patients with OA-associated condylar resorption and either concomitant or resultant maxillofacial skeletal discrepancies such as mandibular retrusion and anterior open bite with molar intrusion, which not only has a beneficial effect on esthetic appearance and occlusion, but also results in TMJ improvement Fig. 3. As a result of counterclockwise rotation of the mandible caused by molar intrusion, the condyle is repositioned, and functional adaptation in circumoral musculature can be achieved. However, it has been difficult to achieve these skeletal improvements by traditional orthodontic mechanics Treatment with implant anchorage for molar intrusion might become a new therapeutic approach for anterior open bite patients with TMD. In our experience, long-term follow-up at least 5 years after orthodontic treatment confirmed no or minimal relapse of mandibular clockwise rotation and anterior open bite and recurrences of TMD symptoms. Conclusions Growing evidence suggests that like OA in other joints, overloading may be assumed to be an initiating factor for a series of degenerative changes in the TMJ- OA, such as condylar resorption, the subsequent decrease in mandibular ramus height, mandibular clockwise rotation, progressive mandibular retrusion, and anterior open bite. To date, many treatment modalities for TMJ-OA have been reported, while the treatment outcomes depend on the preoperative TMJ conditions. Therefore, it is essential to understand the pathogenesis of TMJ-OA and current clinical treatment to develop a good as new treatment remedy for TMJ- OA, including the orthodontic approach. References 1 Wright, W.H.: Deafness as influenced by malposition of the jaws, J Natl Dent Assoc, , Monson, G.S.: Occlusion as applied to crown and bridge work, J Natl Dent Assoc, , Gysi, A. : Studies on the leverage problem of the mandible, Dent Digest, , , , Costen, J.B.: A syndrome of ear and sinus symp-
7 toms dependent upon disturbed function of the temporomandibular joint, Ann Otol Rhinol Laryngol, , Carlsson, G.E., et al. : Epidemiology of temporomandibular disorders. In: Temporomandibular Disorders and Related Pain Conditions Sessle BJ, Bryant PS, Dionne RA, eds.. Seattle: Seattle Press, Carlsson, G.E. : Epidemiology and treatment need for temporomandibular disorders, J Orofac Pain, , Mejersjö, C., et al.: Radiography of the temporomandibular joint in the mandibular joint in female patients with TMJ pain or sysfunction, Acta Radiol, , Brooks, S.L., et al.: Prevalence of osseous changes in the temporomandibular joint of asymptomatic persons without internal derangement, Oral Surg Oral Med Oral Pathol, , Zarb, G.A., et al. : Temporomandibular disorders: Osteoarthritis, J Orofac Pain, , Solberg, W.K.: Current concepts on the development of TMJ dysfunction. In : Developmental Aspects of Temporomandibular Joint Disorders Carlson DS, McNamara JA, Ribbens KA, eds.. Michigan : Center for Human Growth and Development, pp 37 47, Kuroda, S., et al.: Biomechanical and biochemical characteristics of the mandibular condylar cartilage, Osteoarthritis Cartilage, , Tanaka, E., et al.: Degenerative disorders of the Temporomandibular Joint: Etiology, diagnosis, and treatment, J Dent Res, , Aoyama, J., et al.: Immunolocalization of vascular endothelial growth factor in rat condylar cartilage during postnatal development, Histochem Cell Biol, , Shirakura, M., et al. : Activation of the hypoxiainducible factor-1 in overloaded temporomandibular joint, and induction of osteoclastogenesis, Biochem Biophys Res Commun, , Tanaka, E., et al.: Vascular endothelial growth factor plays an important autocrine/paracrine role in the progression of osteoarthritis, Histochem Cell Biol, , Arnett, G.W., et al.: Progressive mandibular retrusion-idiopathic condylar resorption. Part I, Am J Orthod Dentofacial Orthop, , Mercuri, L.G.: Surgical management of TMJ arthritis. In: TMDs, An Evidence-Based Approach to Diagnosis and Treatment Laskin DM, Greene CS, Hylander WL, eds.. Chicago: Quintessence, pp , Steinbrocker, O., et al.: Therapeutic criteria in rheumatoid arthritis, JAMA, , Kent, J.N., et al.: Experience with polymer glenoid fossa prosthesis for partial or total temporomandibular joint reconstruction, J Oral Maxillofac Surg, , Kuttila, M., et al. : Efficiency of occlusal appliance therapy in secondary otalgia and temporomandibular disorders, Acta Odontol Scnad, , Forssell, H., et al.: Application of principles of evidence-based medicine to occlusal treatment for temporomandibular disorders: are there lessons to be learned? J Orofac Pain, , Dionne, R.A. : Pharmacologic Approaches. In: TMDs, An Evidence-Based Approach to Diagnosis and Treatment Laskin DM, Greene CS, Hylander WL, eds.. Chicago: Quintessence, pp , Nicolakis, P., et al.: An investigation of the effectiveness of exercise and manual therapy in treating symptoms of TMJ osteoarthritis, Cranio, , Sundblad, L.: Glycosaminoglycans and glycoproteins in synovial fluid. In: The amino sugars. The chemistry and biology of compounds containing amino sugars Balazs EA, Jeanloz RW, eds.. New York, Academic Press, pp , Wobig, M., et al.: The role of elastoviscosity in the efficacy of viscosupplementation for osteoarthritis of the knee: a comparison of hylan G-F 20 and a lower-molecular-weight hyaluronan, Clin Ther, , Mabuchi, K., et al.: Molecular weight independence of the effect of additive hyaluronic acid on the lubricating characteristics in synovial joints with experimental deterioration, Clin Biomech, , Dougados, M., et al.: High molecular weight sodium hyaluronate Hyalectin in osteoarthritis of the knee: a 1 year placebo-controlled trial, Osteoarthritis Cartilage, , Lohmander, L.S., et al.: Intra-articular hyaluronan injections in the treatment of osteoarthritis on the knee: a randomized, double blind, placebo controlled trial. Hyaluronan Multicentre Trial Group, Ann Rheum Dis, , Gray, R.G., et al.: Intra-articular corticosteroids. An updated assessment, Clin Orthop Relat Res, , Moskowitz, R., et al.: Experimentally induced corticosteroid arthropathy, Arthritis Rheum, , Toller, P.: Use and misuse of intra-articular corticosteriods in the treatment of TMJ pain, Proc Soc Med, , Nitzan, D.W., et al.: The use of arthrocentesis for the treatment of osteoarthritic temporomandibular joints, J Oral Maxillofac Surg, , Gynther, G.W., et al.: Efficacy of arthroscopic lysis and lavage in patients with temporomandibular joint symptoms associated with generalized osteoarthritis or rheumatoid arthritis, J Oral Maxillofac Surg, , 1998.
8 34 Murakami, K.: Arthroscopy of the temporomandibular joint. In : Modern Practice in Orthognathic and Reconstructive Surgery Bell WH, ed.. Philadelphia: Saunders Co., pp , Henny, F.A., et al. : Condylectomy for the persistently painful temporomandibular joint, J Oral Surg, , Albert, T.W., et al.: Temporalis muscle flap for reconstruction of the temporomandibular joint, Oral Maxillofac Clin NA, , Brusati, R., et al. : The temporalis muscle flap in temporomandibular joint surgery, J Craniomaxillofac Surg, , Pogrel, M.A., et al.: The role of a temporalis fascia and muscle flap in temporomandibular joint surgery. J Oral Maxillofac Surg, Magnusson, T., et al.: Function of the masticatory system in 20 patients with mandibular hypo- or hyperplasia after correction by a sagittal split osteotomy, Int J Oral Maxillofac Surg, , Kerstens, H.C., et al.: Condylar atrophy and osteoarthrosis after bimaxillary surgery, Oral Surg Oral Med Oral Pathol, , Crawford, J.G., et al.: Stability after reoperation for progressive condylar resorption after orthognathic surgery : report of seven cases, J Oral Maxillofac Surg, , De Clercq, C.A., et al.: Condylar resorption in orthognathic surgery: a retrospective study, Int J Adult Orthod Orthognath Surg, , Moore, K.E., et al.: The contributing role of condylar resorption to skeletal relapse following mandibular advancement surgery: report of five cases, J Oral Maxillofac Surg, , Wolford, L.M., et al. : Temporomandibular joint reconstruction of the complex patient with the Techmedica custom-made total joint prosthesis, J Oral Maxillofac Surg, , Wolford, L.M., et al.: Changes in temporomandibular joint dysfunction after orthognathic surgery, J Oral Maxillofac Surg, , Wolford, L.M., et al.: Idiopathic condylar resorption: diagnosis, treatment protocol, and outcomes, Am J Orthodont Dentofacial Orthop, , Morales-Ryan, C.A., et al. : Idiopathic condylar resorption: Outcome assessment of TMJ disc repositioning and orthognathic surgery, J Oral Maxillofac Surg, 60 S53, Goncalves, J.R., et al.: Postsurgical stability of counterclockwise maxillomandibular advancement surgery : Affect of articular disc repositioning, J Oral Maxillofac Surg, , van Strijen, P.J., et al.: Condylar resorption following distraction osteogenesis: a case report, J Oral Maxillofac Surg, , Donlon, W.C.: Total Temporomandibular Joint Reconstruction. Oral Maxillofac Surg Clin NA vol. 12, Philadelphia, Saunders Co., McBride, K.L. : Total temporomandibular joint reconstruction. In : Controversies in Oral and Maxillofacial Surgery Worthington P, Evans JR, eds.. Philadelphia : Saunders Co., pp , Mercuri, L.G., et al.: Long-term follow-up of the CAD/CAM patient fitted total temporomandibular joint reconstruction system, J Oral Maxillofac Surg, , Mercuri, L.G., et al.: Long-term outcomes after total alloplastic temporomandibular joint reconstruction following exposure to failed materials, J Oral Maxillofac Surg, , Mercuri, L.G.: A rationale for total alloplastic temporomandibular joint reconstruction in the management of idiopathic/progressive condylar resorption, J Oral Maxillofac Surg, , Mercuri, L.G., et al.: Considerations for the use of alloplastic temporomandibular joint replacement in the growing patient, J Oral Maxillofac Surg, , Tanaka, E., et al.: Influences of occlusal and skeletal discrepancies on biomechanical environment in the TMJ during maximum clenching : an analytic approach with the finite element method, J Oral Rehabil, , Kuroda, S., et al. : Severe anterior open-bite case treated using titanium screw anchorage, Angle Orthod, , Kuroda, S., et al.: Anterior open bite with temporomandibular disorder treated with titanium screw anchorage : evaluation of morphological and functional improvement, Am J Orthod Dentofacial Orthop, , Kuroda, S., et al.: Long-term stability of conservative orthodontic treatment in a patient with rheumatoid arthritis and severe condylar resorption, Am J Orthod Dentofacial Orthop, , Tanaka, E., et al. : An adult case of TMJ osteoarthrosis treated with splint therapy and the subsequent orthodontic occlusal reconstruction: adaptive change of the condyle during the treatment, Am J Orthod Dentofacial Orthop, , Tanaka, E., et al.: An adult case of skeletal open bite with a large lower anterior facial height, Angle Orthod, , 2005.
TMJ Parametro Classico
 TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
Concomitant Temporomandibular Joint and Orthognathic Surgery
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
A Rare Case of Cheerleader Syndrome, Case Report
 47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study
 The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ)
 Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Corporate Medical Policy
 Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Purpose: To review the evolution of Temporomandibular joint TMJ surgery together with the biological evidence for surgical disease
 Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
TMJ Joint Replacement System
 TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
Temporomandibular Joint (TMJ) Disorder Surgery
 Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0156 Temporomandibular Joint (TMJ) Disorder Surgery Table of Contents Related Coverage Resources
Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0156 Temporomandibular Joint (TMJ) Disorder Surgery Table of Contents Related Coverage Resources
Temporomandibular joint reconstruction with alloplastic prosthesis: the outcomes of four cases
 Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Nomenclature and classification of temporomandibular joint disorders Stegenga, Boudewijn
 University of Groningen Nomenclature and classification of temporomandibular joint disorders Stegenga, Boudewijn Published in: Journal of Oral Rehabilitation DOI: 10.1111/j.1365-2842.2010.02146.x IMPORTANT
University of Groningen Nomenclature and classification of temporomandibular joint disorders Stegenga, Boudewijn Published in: Journal of Oral Rehabilitation DOI: 10.1111/j.1365-2842.2010.02146.x IMPORTANT
Arthrogenous disorders of the TMJ
 Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Arthrocentesis and viscosupplementation as treatment modalities for arthralgia of the temporomandibular joint Vos, Lukas Matthijs
 University of Groningen Arthrocentesis and viscosupplementation as treatment modalities for arthralgia of the temporomandibular joint Vos, Lukas Matthijs IMPORTANT NOTE: You are advised to consult the
University of Groningen Arthrocentesis and viscosupplementation as treatment modalities for arthralgia of the temporomandibular joint Vos, Lukas Matthijs IMPORTANT NOTE: You are advised to consult the
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report
 Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Y. H. SHEN*, Y. K. CHEN & S. Y. CHUANG Departments of *Oral and Maxillofacial Surgery, Oral Pathology. Introduction. Case report
 Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
Q2Q3 Reza Movahed, DMD a, *, Larry Wolford, DMD b,c. oralmaxsurgery.theclinics.com KEYWORDS KEY POINTS
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
Osteochondroma of the mandibular condyle cured by conservative resection
 Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
@ CIC Edizioni Internazionali. TMJ inferior compartment arthroplasty procedure through a 25-year follow-up (functional arthroplasty) Original article
 Original article TMJ inferior compartment arthroplasty procedure through a 25-year follow-up (functional arthroplasty) Piero Cascone 1 Valerio Ramieri 1 Paolo Arangio 1 Valentino Vellone 1 Achille Tarsitano
Original article TMJ inferior compartment arthroplasty procedure through a 25-year follow-up (functional arthroplasty) Piero Cascone 1 Valerio Ramieri 1 Paolo Arangio 1 Valentino Vellone 1 Achille Tarsitano
Topic: Orthognathic Surgery Date of Origin: October 5, Section: Surgery Last Reviewed Date: December 2013
 Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
TMJ UNDERSTANDING SYNDROME SPECIAL REPORT By Paul R. White, D.D.S. Special Report: Understanding TMJ Syndrome
 SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Postoperative Evaluation on SSRO performed by Short Lingual Osteotomy and IVRO
 140 J Meikai Dent Med 43 2, 140 147, 2014 Short Lingual Osteotomy SSRO IVRO 1 1 1 1 1 1 2 2 1 2 1 1 2 SSRO SSRO IVRO SSRO short lingual osteotomy SL SL IVRO SL 4 6 IVRO SL IVRO SL 1 IVRO SL short lingual
140 J Meikai Dent Med 43 2, 140 147, 2014 Short Lingual Osteotomy SSRO IVRO 1 1 1 1 1 1 2 2 1 2 1 1 2 SSRO SSRO IVRO SSRO short lingual osteotomy SL SL IVRO SL 4 6 IVRO SL IVRO SL 1 IVRO SL short lingual
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani. Background & Etiology
 Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Post-graduate Student, Department of Oral and Maxillofacial Radiology, School of Dentistry, Isfahan University of Medical Sciences, Isfahan, Iran
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.53824 http://dx.doi.org/10.4317/jced.53824 Evaluation of orthognathic surgery on articular disc position and temporomandibular
Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.53824 http://dx.doi.org/10.4317/jced.53824 Evaluation of orthognathic surgery on articular disc position and temporomandibular
Stability and Relapse in Orthognathic Surgery
 Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
Artigo Original / Original Article
 Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 02 SURGICAL - ORTHODONTIC TREATMENT OF CLASS II DIVISION 1 MALOCCLUSION IN AN ADULT PATIENT: A CASE REPORT Amit Dahiya 1,Minakshi
Definition and History of Orthodontics
 In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
pc oral surgery international
 pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
Original Article. Articular disc displacement in mandibular asymmetry patients. Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma
 J Med Dent Sci ; : 8 Original Article Articular disc displacement in mandibular asymmetry patients Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma Orthodontic Science, Department of Orofacial
J Med Dent Sci ; : 8 Original Article Articular disc displacement in mandibular asymmetry patients Boonsiva Buranastidporn, Masataka Hisano and Kunimichi Soma Orthodontic Science, Department of Orofacial
Modified T-Plate Interpositional Arthroplasty for Temporomandibular Joint Ankylosis: A New and Versatile Option
 Original rticle Modified T-Plate Interpositional rthroplasty for Temporomandibular Joint nkylosis: New and Versatile Option Imran hmad, Mohd ltaf Mir, Lalit Mohan ariar Department of Plastic and Reconstructive
Original rticle Modified T-Plate Interpositional rthroplasty for Temporomandibular Joint nkylosis: New and Versatile Option Imran hmad, Mohd ltaf Mir, Lalit Mohan ariar Department of Plastic and Reconstructive
Arthritis of the Shoulder
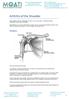 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion patients
 ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.139 pissn 22347550 eissn 22345930 Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion
ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.139 pissn 22347550 eissn 22345930 Clinical evaluation of temporomandibular joint disorder after orthognathic surgery in skeletal class II malocclusion
The Temporomandibular joint: Anatomy, Mechanics, Pathology. Aditya Bahel, DO
 The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
A jaw exerciser for fibrous ankylosis of the temporomandibular joint
 418 Australian Dental Journal, December, 1985 Volume 30, No. 6 A jaw exerciser for fibrous ankylosis of the temporomandibular joint M. Darveniza, M.D.Sc., F.R.A.C.D.S. Lecturer in Operative Dentistry,
418 Australian Dental Journal, December, 1985 Volume 30, No. 6 A jaw exerciser for fibrous ankylosis of the temporomandibular joint M. Darveniza, M.D.Sc., F.R.A.C.D.S. Lecturer in Operative Dentistry,
TMJ Concepts Related Articles
 Page 1 of 14 1 2 3 4 5 6 7 8 9 10 Henry CH, Wolford LM: Treatment outcomes for temporomandibular joint reconstruction after Proplast-Teflon implant failure. J Oral Maxillofac Surg 51:352-358, 1993 Wolford
Page 1 of 14 1 2 3 4 5 6 7 8 9 10 Henry CH, Wolford LM: Treatment outcomes for temporomandibular joint reconstruction after Proplast-Teflon implant failure. J Oral Maxillofac Surg 51:352-358, 1993 Wolford
Simultaneous gap arthroplasty and intraoral distraction and secondary contouring surgery for unilateral temporomandibular joint ankylosis
 Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital,
 Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries
 JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y
 TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
Rheumatoid arthritis is a chronic inflammatory
 CASE REPORT Long-term stability of conservative orthodontic treatment in a patient with rheumatoid arthritis and severe condylar resorption Shingo Kuroda, a Yasuko Kuroda, b Yuko Tomita, c and Eiji Tanaka
CASE REPORT Long-term stability of conservative orthodontic treatment in a patient with rheumatoid arthritis and severe condylar resorption Shingo Kuroda, a Yasuko Kuroda, b Yuko Tomita, c and Eiji Tanaka
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty
 Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study
 Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
DEGENERATIVE DISEASE OF THE TEMPOROMANDIBULAR JOINT IN YOUNG PERSONS. Introduction
 British Journal of Oral Surgery 17 (1979-80), 17-26 DEGENERATIVE DISEASE OF THE TEMPOROMANDIBULAR JOINT IN YOUNG PERSONS HUGH Ocus, B.D.s., F.D.S. Basingstoke District Hospital Summary. The majority of
British Journal of Oral Surgery 17 (1979-80), 17-26 DEGENERATIVE DISEASE OF THE TEMPOROMANDIBULAR JOINT IN YOUNG PERSONS HUGH Ocus, B.D.s., F.D.S. Basingstoke District Hospital Summary. The majority of
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery (AAOMS ParCare 2017) TEMPOROMANDIBULAR JOINT SURGERY
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 Parameters of Care: Clinical Practice Guidelines
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 Parameters of Care: Clinical Practice Guidelines
Appropriate Management of Temporomandibular Disorders in the Elderly
 Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
Journal of Advanced Medical and Dental Sciences of Scientific Research and Studies
 Journal of Advanced Medical and Dental Sciences Research @Society of Scientific Research and Studies Journal home page: www.jamdsr.com doi: 10.21276/jamdsr UGC approved journal no. 63854 (e) ISSN Online:
Journal of Advanced Medical and Dental Sciences Research @Society of Scientific Research and Studies Journal home page: www.jamdsr.com doi: 10.21276/jamdsr UGC approved journal no. 63854 (e) ISSN Online:
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature:
 CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient with facial asymmetry
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Osteoarthrosis of Temporomandibular Joint Related to the Defects of Posterior Dentition: A Retrospective Study
 176) Prague Medical Report / Vol. 117 (2016) No. 4, p. 176 184 Osteoarthrosis of Temporomandibular Joint Related to the Defects of Posterior Dentition: A Retrospective Study Jitka Levorová, Vladimír Machoň,
176) Prague Medical Report / Vol. 117 (2016) No. 4, p. 176 184 Osteoarthrosis of Temporomandibular Joint Related to the Defects of Posterior Dentition: A Retrospective Study Jitka Levorová, Vladimír Machoň,
A Clinical Study of Efficacy of Hydrocortisone Compared With Hyaluronic Acid After Arthrocentesis In TMJ Disorders
 ORIGINAL RESEARCH A Clinical Study of Efficacy of Hydrocortisone Compared With Hyaluronic Acid After Arthrocentesis In TMJ Disorders Pavan Kumar B 1, Haripriya Chari 2, Mohan AP 3, Brahmaji Rao J 4 Quick
ORIGINAL RESEARCH A Clinical Study of Efficacy of Hydrocortisone Compared With Hyaluronic Acid After Arthrocentesis In TMJ Disorders Pavan Kumar B 1, Haripriya Chari 2, Mohan AP 3, Brahmaji Rao J 4 Quick
Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology
 TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
Orthodontic-Surgical Treatment of a Rare Case of Aplasia of the Mandibular Condyles
 report imedpub Journals http://www.imedpub.com Orthodontic-Surgical Treatment of a Rare of Aplasia of the Mandibular Condyles Vanessa Castro 1, Lucas SE 2, Daniel SC 3, Jesus do PC 4, Antonio Irineu TN
report imedpub Journals http://www.imedpub.com Orthodontic-Surgical Treatment of a Rare of Aplasia of the Mandibular Condyles Vanessa Castro 1, Lucas SE 2, Daniel SC 3, Jesus do PC 4, Antonio Irineu TN
Ankle Arthritis and Ankle Replacement
 Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
Clinical Policy Title: Temporomandibular joint disorder
 Clinical Policy Title: Temporomandibular joint disorder Clinical Policy Number: 14.02.02 Effective Date: September 1, 2013 Initial Review Date: May 13, 2013 Most Recent Review Date: May 1, 2018 Next Review
Clinical Policy Title: Temporomandibular joint disorder Clinical Policy Number: 14.02.02 Effective Date: September 1, 2013 Initial Review Date: May 13, 2013 Most Recent Review Date: May 1, 2018 Next Review
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY
 PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence
 Case Report DOI: 10.18231/2455-6750.2017.0022 A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence Shruti Sambyal 1,*, Ajit D. Dinkar 2, Bhanu Pratap Singh 3, Atul Chauhan
Case Report DOI: 10.18231/2455-6750.2017.0022 A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence Shruti Sambyal 1,*, Ajit D. Dinkar 2, Bhanu Pratap Singh 3, Atul Chauhan
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS. FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy
 MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch
 Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina Zepa
 Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 32-36, 2009 Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina
Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 32-36, 2009 Three-dimensional evaluation of TMJ parameters in Class II and Class III patients Zane Krisjane, Ilga Urtane, Gaida Krumina, Katrina
Qestions often arise regarding the appropriate
 CLINICAL REVIEW C E Considerations for orthognathic surgery during growth, Part 1: Mandibular deformities Larry M. Wolford, DMD, a Spiro C. Karras, DDS, b and Pushkar Mehra, DMD c Dallas, Tex Management
CLINICAL REVIEW C E Considerations for orthognathic surgery during growth, Part 1: Mandibular deformities Larry M. Wolford, DMD, a Spiro C. Karras, DDS, b and Pushkar Mehra, DMD c Dallas, Tex Management
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S.
 THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
Chapter 79: Temporomandibular Joint Disorders. Daniel M. Laskin
 Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Condylar Degeneration and Diseases Local and Systemic Etiologies
 Condylar Degeneration and Diseases Local and Systemic Etiologies David M. Sarver,* Sridhar Janyavula,** and Randy Q. Cron*** The temporomandibular joint condyle is susceptible to developing a variety of
Condylar Degeneration and Diseases Local and Systemic Etiologies David M. Sarver,* Sridhar Janyavula,** and Randy Q. Cron*** The temporomandibular joint condyle is susceptible to developing a variety of
TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE
 TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE Khushboo Singh, MDS 1, Dr. Sujata Mohanty, MDS 2, Mahesh Verma, MDS, MBA, PhD 3, Sunita Gupta, MDS, MBA (HCA) 4, Sujoy Ghosh, MDS 5, and Meera Choudhary,
TRIFID MANDIBULAR CONDYLE: REPORT OF A RARE CASE Khushboo Singh, MDS 1, Dr. Sujata Mohanty, MDS 2, Mahesh Verma, MDS, MBA, PhD 3, Sunita Gupta, MDS, MBA (HCA) 4, Sujoy Ghosh, MDS 5, and Meera Choudhary,
4 2 Osteoarthritis 1
 Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
The future of health is digital
 Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
Changes in the temporomandibular joint after mandibular lengthening with different rates of distraction
 Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
THE RELATION BETWEEN TMJ OSTEOARTHRITIS AND THE INADEQUATELY SUPPORTED OCCLUSION
 THE RELATION BETWEEN TMJ OSTEOARTHRITIS AND THE INADEQUATELY SUPPORTED OCCLUSION Ra ed Al-Sadhan, BDS, MS, Diplomat American Board of Oral and Maxillofacial Radiology. Assistant Professor, Department of
THE RELATION BETWEEN TMJ OSTEOARTHRITIS AND THE INADEQUATELY SUPPORTED OCCLUSION Ra ed Al-Sadhan, BDS, MS, Diplomat American Board of Oral and Maxillofacial Radiology. Assistant Professor, Department of
Review Article A 5 Year Retrospective Study on the Clinical Outcomes of Performing Arthrocentesis in Basildon Hospital
 Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Postoperative mandibular stability after orthognathic surgery in patients with mandibular protrusion and mandibular deviation
 Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Effect of orthognathic surgery on the temporomandibular joint in patients with anterior open bite
 Behnam Aghabeigi, PhD, FDSRCS, FFDRCSI Former Visiting Resident Currently Clinical Lecturer Eastman Dental Institute London, United Kingdom David Hiranaka, MD, DMD Former Chief Resident Massachusetts General
Behnam Aghabeigi, PhD, FDSRCS, FFDRCSI Former Visiting Resident Currently Clinical Lecturer Eastman Dental Institute London, United Kingdom David Hiranaka, MD, DMD Former Chief Resident Massachusetts General
Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement
 Original Article Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement Beom-Seok Moon a ; Il-Hyung Yang b ; Sug-Joon Ahn c ABSTRACT Introduction:
Original Article Dentofacial characteristics of women with oversized mandible and temporomandibular joint internal derangement Beom-Seok Moon a ; Il-Hyung Yang b ; Sug-Joon Ahn c ABSTRACT Introduction:
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Orthodontics-surgical combination therapy for Class III skeletal malocclusion
 [Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
[Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
For nongrowing patients with skeletal Class II
 CASE REPORT Treatment of anterior open bite and multiple missing teeth with lingual fixed appliances, double jaw surgery, and dental implants Min-Ho Jung, a Un-Bong Baik, b and Sug-Joon Ahn c Seoul, Korea
CASE REPORT Treatment of anterior open bite and multiple missing teeth with lingual fixed appliances, double jaw surgery, and dental implants Min-Ho Jung, a Un-Bong Baik, b and Sug-Joon Ahn c Seoul, Korea
KJLO. A Sequential Approach for an Asymmetric Extraction Case in. Lingual Orthodontics. Case Report INTRODUCTION DIAGNOSIS
 KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
MDJ Stabilization Splint (Night Guard, Mouth Guard) Vol.:6 No.:2 2009
 MDJ Stabilization Splint (Night Guard, Mouth Guard) Comparative Research Dr. Kais George Zia B.D.S, M.Sc, Ph.D. Abstract This research compares between the effect of flexible and hard stabilization splint
MDJ Stabilization Splint (Night Guard, Mouth Guard) Comparative Research Dr. Kais George Zia B.D.S, M.Sc, Ph.D. Abstract This research compares between the effect of flexible and hard stabilization splint
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder
 Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
