All medically accepted Prior authorization applies to new starts only excluded from Part D. 12 months
|
|
|
- Hilary Powers
- 6 years ago
- Views:
Transcription
1 2018 Cigna-HealthSpring Prior Authorization Criteria Drug Name Excluded Prior Authorization Product Age Prescriber Coverage Covered Uses Exclusion Criteria Required Medical Information Other Criteria Drug Type Description Group Restrictions Restrictions Duration Criteria ABELCET Antifungals, Polyene 6 months B vs D coverage determination ABRAXANE Abraxane BvsD coverage determination ACETYLCYSTEINE ACITRETIN Acitretin Documentation of diagnosis Use of Actemra is considered medically necessary for the treatment of rheumatoid arthritis (RA) when BOTH of the following criteria are met: 1) inadequate response, intolerance, or contraindication to at Documentation of diagnosis and past medication least one disease-modifying anti-rheumatic drug (DMARD) (i.e., ACTEMRA Actemra history. Methotrexate (MTX) Azathioprine, gold, Hydroxychloroquine, Penicillamine, Sulfasalazine and 2) failure, contraindication or intolerance to Enbrel or Humira. B vs D coverage determination required for Actemra IV. ACTIMMUNE Actimmune ACYCLOVIR SODIUM ADAGEN IMMUNE STIMULANT S Documentation of diagnosis ADEMPAS ADEMPAS ADRUCIL AFINITOR Afinitor is considered medically necessary for the treatment of patients Documentation of diagnosis and past medication Afinitor with advanced renal cell carcinoma after failure of treatment with history Sutent (sunitinib) OR Nexavar (sorafenib). AFINITOR DISPERZ Afinitor is considered medically necessary for the treatment of patients Documentation of diagnosis and past medication Afinitor with advanced renal cell carcinoma after failure of treatment with history Sutent (sunitinib) OR Nexavar (sorafenib). ALBUTEROL SULFATE ALDURAZYME Enzyme Replacement/ Modifiers Documentation of diagnosis ALECENSA Molecular Inhibitors ALIMTA Alimta BvsD coverage determination ALIQOPA Antineoplastics, Monoclonal Antibodies B vs D coverage determination ALORA (MAPD plans) Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age risedronate, raloxifene, and Prolia.
2 Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, ALORA (PDP SECURE and HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the PDP SECURE EXTRA) Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age raloxifene, and Prolia. Alosetron will not be approved ALOSETRON for use in men, as safety and Alosetron HYDROCHLORIDE efficacy in men has not been established. ALOXI (Non-formulary for PDP Secure, PDP Secureauthorization only Extra) ALUNBRIG Molecular Inhibitors AMBISOME Antifungals, Polyene 6 months B vs D coverage determination AMIFOSTINE AMINOSYN AMINOSYN 7%/ELECTROLYTES AMINOSYN 8.5%/ELECTROLYTES AMINOSYN II AMINOSYN II 8.5%/ELECTROLYTES AMINOSYN M AMINOSYN-HBC AMINOSYN-PF AMINOSYN-PF 7% AMINOSYN-RF Automatic AMITRIPTYLINE HCL approval if HRM - the continued use of the HRM (high risk med) with member is less Tricyclic an explanation of the specific benefit established than 65 years of through the Antidepressant with the medication and how that benefit outweighs age. Prior s the potential risk, AND the physician will continue authorization to monitor for side effects. required for age 65 or older. AMPHOTERICIN B Antifungals, Polyene 6 months B vs D coverage determination AMPYRA Ampyra is considered medically necessary for patients with multiple Ampyra Documentation of diagnosis sclerosis with medical documentation of impaired walking ability. ANABOLIC ANADROL-50 STEROIDS, Documentation of diagnosis ANDROGENS ANABOLIC ANDROXY STEROIDS, Documentation of diagnosis ANDROGENS APOKYN Apokyn APREPITANT
3 ARALAST NP For initial treatment of anemia, documentation of Hemoglobin less than 10, transferrin saturation greater than 20%, and ferritin levels greater than 100 obtained over the last 3 months. For ARANESP ALBUMIN HEMATOPOI reauthorizations, approvals granted if Hemoglobin FREE ETICS does not exceed 10-12g/dL or approvals granted if Hemoglobin does not exceed 10-13g/dL for the 6 months B vs D coverage determination indication of reduction of allogeneic red cell transfusions in patients undergoing elective, noncardiac, nonvascular surgery. Documentation of diagnosis of Cryopyrin- Associated Periodic Syndromes (CAPS), including 12 years of age ARCALYST Arcalyst B vs D coverage determination Familial Cold Auto-inflammatory Syndrome and older (FCAS) and Muckle-Wells Syndrome (MWS) ARMODAFINIL Nonamphetamine Documentation of diagnosis and sleep study for the Central diagnosis of sleep apnea or narcolepsy Nervous ARZERRA System Agents with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of ASCOMP/CODEINE Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age IMMUNE ASTAGRAF XL SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED IMMUNE ATGAM SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED AVASTIN Antineoplastics, Monoclonal Antibodies B vs D coverage determination AVONEX Patient must have failure, contraindication or intolerance to two of the Immunomodula following: Avonex, Betaseron and Copaxone before Rebif will be tors authorized. AVONEX PEN Patient must have failure, contraindication or intolerance to two of the Immunomodula following: Avonex, Betaseron and Copaxone before Rebif will be tors authorized. AZACITIDINE IMMUNE AZASAN SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED IMMUNE AZATHIOPRINE SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED BANZEL Banzel Documentation of diagnosis
4 BAVENCIO Antineoplastics, Monoclonal Antibodies B vs D coverage determination BELEODAQ Beleodaq B vs D coverage determination BENDEKA The patient must be receiving one standard therapy for SLE with any of the following: corticosteroids, hydroxychloroquine, The patient must have a positive autoantibody test immunosuppressives (cyclophosphamide, azathioprine, (i.e., anti-nuclear antibody [ANA] greater than or BENLYSTA BENLYSTA mycophenolate, methotrexate, cyclosporine) or nonsteroidal anti equal to 1:80 and/or anti-double-stranded DNA inflammatory drugs AND there must be an absence of severe active [anti-dsdna] greater than or equal to 30 IU/ml) lupus nephritis or severe active central nervous system lupus before Benlysta is authorized. B vs D coverage determination. the continued use of the HRM (high risk med) with an explanation of the specific benefit established with the medication and how that benefit outweighs the potential risk, AND the physician will continue Automatic to monitor for side effects, AND the physician has approval if documented that the patient has tried and failed two member is less Safer alternatives depend on indication. For Parkinsonism, safer BENZTROPINE HRM - (2) safer formulary alternatives if two are available than 65 years of alternatives are: Carbidopa/Levodopa, Pramipexole, Ropinirole, through the MESYLATE Benztropine or provided clinical rationale why two safer age. Prior Bromocriptine, Amantadine, and Selegiline. For extrapyramidal formulary alternatives are not appropriate for the authorization symptoms, a safer alternative is: Amantadine. patient. If only one (1) safer formulary alternative required for age is available, then only that particular medication 65 or older. would need to be documented as tried and failed or clinical rationale provided as to why that one safer formulary alternative is not appropriate for the patient. BESPONSA Antineoplastics, Monoclonal Antibodies B vs D coverage determination BETASERON Patient must have failure, contraindication or intolerance to two of the Immunomodula following: Avonex, Betaseron and Copaxone before Rebif will be tors authorized. BICNU BLEOMYCIN SULFATE BORTEZOMIB Velcade BvsD coverage determination BOSULIF Molecular Inhibitors BUDESONIDE BUPHENYL BUPHENYL Buprenorphin e-1 mo or 6 mo if BUPRENORPHINE HCL preg/hypersen Opioid Agonist- All FDA-approved The use of buprenorphine for maintenance therapy should be limited to sitive to Antagonist Documentation of opioid dependence. patients who have experienced a hypersensitivity reaction to naloxone naloxone. Analgesics or require buprenorphine during pregnancy. Zubsolv, Subox, and bup/nalox-6 mo Buprenorphin e-1 mo or 6 mo if preg/hypersen Opioid Agonist- All FDA-approved The use of buprenorphine for maintenance therapy should be limited to BUPRENORPHINE sitive to Antagonist Documentation of opioid dependence. patients who have experienced a hypersensitivity reaction to naloxone HCL/NALOXONE HCL naloxone. Analgesics or require buprenorphine during pregnancy. Zubsolv, Subox, and bup/nalox-6 mo
5 BUSULFAN BUSULFEX with the medication and how that benefit outweighs member is less HRM - BUTALBITAL/ACETAMIN the potential risk, AND the physician will continue than 65 years of Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. OPHEN/CAFFEINE to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age with the medication and how that benefit outweighs member is less BUTALBITAL/ACETAMIN HRM - the potential risk, AND the physician will continue than 65 years of OPHEN/CAFFEINE/CODEI Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. to monitor for side effects, AND the physician has age. Prior NE Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age with the medication and how that benefit outweighs member is less HRM - BUTALBITAL/ASPIRIN/C the potential risk, AND the physician will continue than 65 years of Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. AFFEINE to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age with the medication and how that benefit outweighs member is less HRM - BUTALBITAL/ASPIRIN/C the potential risk, AND the physician will continue than 65 years of Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. AFFEINE/CODEINE to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age CABOMETYX Molecular Inhibitors CALQUENCE Molecular Inhibitors Onychomycos is (fingernails only) - 2mo. For the treatment of tinea versicolor or pityriasis, use of oral CANCIDAS Antifungals, Onychomycos ketoconazole or a topical antifungal agent is required prior to the use Superficial and is (toenails) - of Itraconazole. For candidiasis infections (unless specified C. Systemic 3mo. All glabrata or C. krusei) use of fluconazole is required prior to the use of other itraconazole. indications - 12mo with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of CAPACET Butalbital through the Safer alternatives are: naproxen sodium and ibuprofen. to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age
6 CAPRELSA Caprelsa Documentation of diagnosis CARBAGLU CARBAGLU CARBOPLATIN CARNITOR Onychomycos is (fingernails only) - 2mo. For the treatment of tinea versicolor or pityriasis, use of oral CASPOFUNGIN ACETATE Antifungals, Onychomycos ketoconazole or a topical antifungal agent is required prior to the use Superficial and is (toenails) - of Itraconazole. For candidiasis infections (unless specified C. Systemic 3mo. All glabrata or C. krusei) use of fluconazole is required prior to the use of other itraconazole. indications - 12mo CAYSTON CAYSTON 7 years and older CEREZYME Hormonal CHORIONIC Agents, GONADOTROPIN Gonadotropins Documentation of diagnosis CINRYZE The patient must have a history of more than one severe event per month and have failure, contraindication or intolerance to one Cinryze Patient must have a confirmed diagnosis of HAE. conventional therapy for HAE prophylaxis such as aminocaproic acid, danazol or tranexamic acid. B vs D coverage determination. CISPLATIN CLADRIBINE CLINIMIX 2.75%/DEXTROSE 5% CLINIMIX 4.25%/DEXTROSE 10% CLINIMIX 4.25%/DEXTROSE 20% CLINIMIX 4.25%/DEXTROSE 25% CLINIMIX 4.25%/DEXTROSE 5% CLINIMIX 5%/DEXTROSE 15% CLINIMIX 5%/DEXTROSE 20% CLINIMIX 5%/DEXTROSE 25% CLINIMIX E 2.75%/DEXTROSE 10% CLINIMIX E 4.25%/DEXTROSE 10% CLINIMIX E 4.25%/DEXTROSE 25% CLINIMIX E 5%/DEXTROSE 25% CLINISOL SF 15% CLOFARABINE Automatic CLOMIPRAMINE HCL approval if HRM - the continued use of the HRM (high risk med) with member is less Tricyclic an explanation of the specific benefit established than 65 years of through the Antidepressant with the medication and how that benefit outweighs age. Prior s the potential risk, AND the physician will continue authorization to monitor for side effects. required for age 65 or older. COMETRIQ Molecular Inhibitors
7 Patient must have failure, contraindication or intolerance to two of the Immunomodula COPAXONE following: Avonex, Betaseron and Copaxone before Rebif will be tors authorized. 1.) Blood pressure less than 90/50 mmhg. 2.) Sick sinus syndrome, sinoatrial block, or 3rd degree AV block, unless a The patient must have a diagnosis of chronic heart failure with left functioning demand pacemaker Documentation of diagnosis, previous use of a beta- ventricular ejection fraction less than or equal to 35%, normal sinus CORLANOR CORLANOR is present. 3.) Resting heart blocker, LVEF, sinus rhythm, resting HR, and rhythm with resting heart rate greater than or equal to 70 beats per rate less than 60 bpm prior to blood pressure minute, and either be on maximally tolerated doses of beta-blockers or treatment. 4.) Pacemaker have a contraindication to beta-blocker use. dependence (heart rate maintained exclusively by the pacemaker). COSMEGEN COTELLIC Molecular Inhibitors CROMOLYN SODIUM Automatic approval if HRM - the continued use of the HRM (high risk med) with member is less CYCLOBENZAPRINE Skeletal an explanation of the specific benefit established than 65 years of through the HCL Muscle with the medication and how that benefit outweighs age. Prior Relaxants the potential risk, AND the physician will continue authorization to monitor for side effects. required for age 65 or older. CYCLOPHOSPHAMIDE IMMUNE CYCLOSPORINE SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED IMMUNE SUPPRESSAN CYCLOSPORINE TS - MODIFIED TRANSPLAN B vs D coverage determination T RELATED CYRAMZA Antineoplastics, Monoclonal Antibodies B vs D coverage determination CYSTARAN CYSTARAN CYTARABINE CYTARABINE AQUEOUS DACARBAZINE DALIRESP Phosphodiester ase Type 4 (PDE4) Inhibitors DAPTOMYCIN DARZALEX Antineoplastics, Monoclonal Antibodies B vs D coverage determination DAUNORUBICIN HCL DEXRAZOXANE DEXTROSE 10%/NACL 0.45% DEXTROSE 5% /ELECTROLYTE #48 VIAFLEX
8 DEXTROSE 10% DEXTROSE 10%/NACL 0.2% DEXTROSE 2.5%/NACL 0.45% DEXTROSE 20% DEXTROSE 25% DEXTROSE 30% DEXTROSE 40% DEXTROSE 5%/LACTATED RINGERS DEXTROSE 50% DIGITEK with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of through the Digoxin to monitor for side effects, AND the physician has age. Prior documented that the patient has tried and failed authorization digoxin 0.125mg daily or provided clinical required for age rationale as to why the lower dose is not 65 or older. appropriate for the patient. DIGOX with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of through the Digoxin to monitor for side effects, AND the physician has age. Prior documented that the patient has tried and failed authorization digoxin 0.125mg daily or provided clinical required for age rationale as to why the lower dose is not 65 or older. appropriate for the patient. DIGOXIN with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of through the Digoxin to monitor for side effects, AND the physician has age. Prior documented that the patient has tried and failed authorization digoxin 0.125mg daily or provided clinical required for age rationale as to why the lower dose is not 65 or older. appropriate for the patient. with the medication and how that benefit outweighs member is less DIPYRIDAMOLE (only HRM - Platelet the potential risk, AND the physician will continue than 65 years of Safer alternatives are: Clopidogrel, Warfarin, Jantoven, and covered on PDP Secure, PDP Modifying through the to monitor for side effects, AND the physician has age. Prior aspririn/dipyridamole. Secure-Extra) Agents documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age DOCEFREZ DOCETAXEL
9 Automatic DOXEPIN HCL approval if HRM - the continued use of the HRM (high risk med) with member is less Tricyclic an explanation of the specific benefit established than 65 years of through the Antidepressant with the medication and how that benefit outweighs age. Prior s the potential risk, AND the physician will continue authorization to monitor for side effects. required for age 65 or older. DOXORUBICIN HCL DOXORUBICIN HCL LIPOSOME DRONABINOL Dronabinol Documentation of diagnosis 6 months B vs D coverage determination ELAPRASE Enzyme Replacement/ Modifiers Documentation of diagnosis ELIGARD Pituitary Hormones ELITEK EMEND EMPLICITI Documentation of diagnosis and current medication Empliciti is approved with concurrent use of dexamethasone and Empliciti regimen lenalidomide. B vs D coverage determination. Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy ENBREL Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade.
10 Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy ENBREL MINI Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade. Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy ENBREL SURECLICK Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade. ENGERIX-B IMMUNE ENVARSUS XR SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED 12 weeks, EPCLUSA Documentation from the medical record of based on For genotype 1, 4, 5 and 6, clinical information must be provided diagnosis including genotype, current medication indication and EPCLUSA confirming the patient is not a candidate for Harvoni before Epclusa regimen, HCV-RNA levels, history of previous established will be authorized. HCV therapies and presence/absence of cirrhosis. treatment guidelines EPIRUBICIN HCL ERBITUX Antineoplastics, Monoclonal Antibodies B vs D coverage determination
11 ERGOLOID MESYLATES with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of Antidementia through the to monitor for side effects, AND the physician has age. Prior Agents documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age Safer alternatives are: donepezil, galantamine and rivastigmine. ERIVEDGE Erivedge ERWINAZE ESBRIET Diagnosis confirmed by 1.) in patients without Other known causes of surgical lung biopsy: Usual interstitial pneumonia interstitial lung disease e.g., All FDA-approved (UIP) pattern on high resolution computed domestic and occupational ESBRIET tomography (HRCT) is indicative of IPF or 2.) in environmental exposures, excluded from part D. patients with surgical lung biopsy: The biopsy connective tissue disease, and pattern is diagnostic of IPF or the combination of drug toxicity. HRCT and biopsy pattern is indicative of IPF. Esbriet will be used as monotherapy. ESGIC with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of Butalbital through the to monitor for side effects, AND the physician has age. Prior Combinations documented that the patient has tried and failed two authorization (2) safer formulary alternatives or provided clinical required for age Safer alternatives are: naproxen sodium and ibuprofen. ESTRADIOL (MAPD plans) Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age risedronate, raloxifene, and Prolia. Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, ESTRADIOL (PDP HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms SECURE and PDP SECURE through the Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and EXTRA) documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age raloxifene, and Prolia. ETHYOL ETOPOSIDE EVOMELA EVOMELA B vs D coverage determination FABRAZYME FARYDAK FARYDAK FASLODEX FENTANYL CITRATE
12 Enrollment in the Transmucosal fentanyl products will only be covered with 16 years of age Transmucosal All FDA-approved Transmucosal documentation of breakthrough cancer pain. The patient must be FENTANYL CITRATE Documentation from the medical record of and older for Fentanyl Immediate- currently receiving and be tolerant to opioid therapy for persistent ORAL TRANSMUCOSAL diagnosis fentanyl citrate Citrate Release Fentanyl cancer pain. The patient must be enrolled in the TIRF REMS Access (lozenge/troche). (TIRF) REMS program. Access program FERRIPROX FERRIPROX FIRAZYR The patient must have a history of a moderate or severe attack (e.g., Firazyr Patient must have a confirmed diagnosis of HAE. airway swelling, severe abdominal pain, facial swelling, nausea and vomiting, painful facial distortion). FIRMAGON FLUDARABINE PHOSPHATE FLUOROURACIL FOLOTYN 1.) Pediatric patients or young 1.) Bone mineral density (BMD) by DEXA at hip Metabolic adults with open epiphyses. and spine. 2.) Confirmation of normal serum 2 years from FORTEO Bone Disease 2.) History of prior external alkaline phosphatase or provider statement that initiation of agents beam or implant radiation Paget s disease has been excluded. 3.) Treatment therapy involving the skeleton history Member has a history of at least one osteoporotic fracture while on Bisphosphonate Therapy OR Member meets BOTH of the following criteria: 1) Member has BMD screening results of -2.5 or below AND 2) Member has tried and or failed an oral bisphosphonate or SERM OR the member has documented intolerance, contraindication, or hypersensitivity to other osteoporosis therapies. FREAMINE HBC 6.9% FREAMINE III FYAVOLV (MAPD plans) Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age risedronate, raloxifene, and Prolia. Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, FYAVOLV (PDP SECURE HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the and PDP SECURE EXTRA) Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age raloxifene, and Prolia. FYCOMPA (Prior Authorization only required for PDP SECURE and PDP SECURE EXTRA) GAMMAKED GAMUNEX-C GANCICLOVIR FYCOMPA
13 As long as the patient requires GATTEX parenteral GATTEX nutrition and/or IV fluids, 3 months up to. GAZYVA Antineoplastics, Monoclonal Antibodies B vs D coverage determination GEMCITABINE GEMCITABINE HCL IMMUNE GENGRAF SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED GENOTROPIN Pituitary Hormones GENOTROPIN Pituitary MINIQUICK Hormones GILENYA Gilenya GILOTRIF Molecular Inhibitors GRANISETRON HCL HALAVEN Use of Halaven is considered medically necessary for the treatment of Documentation of prior treatment with an patients with metastatic breast cancer who have previously received at Halaven anthracycline and a taxane. least two chemotherapeutic regimens for the treatment of metastatic disease. B vs D coverage determination. 12 to 24 HARVONI weeks based Documentation from the medical record of on indication diagnosis including genotype, HCV RNA viral HARVONI and levels prior to treatment, history of previous HCV established therapies, and presence/absence of cirrhosis. treatment guidelines IMMUNE HECORIA SUPPRESSAN TS - TRANSPLAN B vs D coverage determination T RELATED HEPATAMINE HERCEPTIN Antineoplastics, Monoclonal Antibodies B vs D coverage determination HETLIOZ Documentation that patient is totally blind and HETLIOZ lacks light perception
14 Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy HUMIRA Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade. Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or HUMIRA PEDIATRIC Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy CROHNS DISEASE Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) STARTER PACK Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade.
15 Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy HUMIRA PEN Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade. Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or HUMIRA PEN-CROHNS Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy DISEASESTARTER Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade.
16 Use of Humira, Enbrel, or Remicade is considered medically necessary for the treatment of: 1.) Rheumatoid Arthritis in patients that have tried and failed methotrexate OR at least 2 alternative disease modifying antirheumatic drugs (DMARDs). 2.) Juvenile Rheumatoid Arthritis in patients that have tried and failed at least 2 DMARDs. 3.) Ankylosing Spondylitis in patients that have tried and failed at least 1 non-steroidal anti-inflammatory drug (NSAID), corticosteroid, OR sulfasalazine. 4.) Plaque Psoriasis in patients that have: a.) moderate to severe chronic disease, b.) minimum body surface area (BSA) involvement of greater than or equal to 5% OR involvement of the palms, soles, head, neck or genitalia, c.) tried and failed at least 1 topical agent (topical steroid, calcipotriene, or HUMIRA PEN-PSORIASIS Immune Documentation of diagnosis and past medication tazarotene), AND d.) tried and failed at least 1 systemic therapy STARTER Suppressants history (cyclosporine, methotrexate, or acitretin) OR phototherapy. 5.) Psoriatic Arthritis in patients with active disease. In addition, use of Humira or Remicade is considered medically necessary for the treatment of: 1.) Moderate to severe Crohn s Disease in patients that have tried and failed at least 2 of the following: immunomodulators, corticosteroids, or aminosalicylates. 2.) Treatment of moderately to severely active ulcerative colitis in patients who have had inadequate response to at least 2 of the following: corticosteroids, sulfasalazine, mesalamine, azathioprine, 6-mercaptopurine. Use of Humira will also be considered medically necessary for the treatment of hidradenitis suppurativa and uveitis. Use of Remicade will also be considered medically necessary for the treatment of fistulizing Crohn's disease. B vs D coverage determination required for Remicade. HYDROXYP HYDROXYPROGESTERO ROGESTERO NE CAPROATE NE B vs D coverage determination IBRANCE Molecular Inhibitors ICLUSIG Molecular Inhibitors IDARUBICIN HCL IDHIFA Molecular Inhibitors IFOSFAMIDE ILARIS Ilaris B vs D coverage determination IMATINIB MESYLATE Molecular Inhibitors IMBRUVICA Molecular Inhibitors IMFINZI Antineoplastics, Monoclonal Antibodies B vs D coverage determination Automatic IMIPRAMINE HCL approval if HRM - the continued use of the HRM (high risk med) with member is less Tricyclic an explanation of the specific benefit established than 65 years of through the Antidepressant with the medication and how that benefit outweighs age. Prior s the potential risk, AND the physician will continue authorization to monitor for side effects. required for age 65 or older. IMOVAX RABIES (H.D.C.V.) Height standard deviation score must be less than or equal to -3.0 AND the basal IGF-1 score must be below the lower limits of normal Documentation of diagnosis. Documentation of lab Insulin-Like for the reporting lab AND the patient must have a normal or elevated INCRELEX data reflecting height standard deviation score, Growth Factor growth hormone level (excluding patients with growth hormone gene basal IGF-1 score, and growth hormone level. deletion) AND epiphyses must be confirmed as open in patients greater than or equal to 10 years of age. Molecular INLYTA Inhibitors
17 INTRALIPID IPRATROPIUM BROMIDE IPRATROPIUM BROMIDE/ALBUTEROL SULFATE IRESSA Molecular Inhibitors IRINOTECAN IRINOTECAN HCL ISTODAX Use of Istodax is considered medically necessary for the treatment of Documentation of diagnosis and past medication Istodax cutaneous T-cell lymphoma in patients that have tried and failed at history least 1 prior therapy. B vs D coverage determination. ISTODAX (OVERFILL) Use of Istodax is considered medically necessary for the treatment of Documentation of diagnosis and past medication Istodax cutaneous T-cell lymphoma in patients that have tried and failed at history least 1 prior therapy. B vs D coverage determination. Onychomycos is (fingernails only) - 2mo. For the treatment of tinea versicolor or pityriasis, use of oral ITRACONAZOLE Antifungals, Onychomycos ketoconazole or a topical antifungal agent is required prior to the use Superficial and is (toenails) - of Itraconazole. For candidiasis infections (unless specified C. Systemic 3mo. All glabrata or C. krusei) use of fluconazole is required prior to the use of other itraconazole. indications - 12mo IXEMPRA KIT JAKAFI Molecular Inhibitors Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, JEVANTIQUE LO (MAPD HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms through the plans) Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age risedronate, raloxifene, and Prolia. Safer alternatives to the estrogen high risk medications depend on the with the medication and how that benefit outweighs member is less indication. For Hot Flashes, safer alternatives are: Depo-Estradiol, JEVANTIQUE LO (PDP HRM - the potential risk, AND the physician will continue than 65 years of SSRIs, venlafaxine, gabapentin, and Femring. For Vaginal Symptoms SECURE and PDP SECURE through the Estrogens to monitor for side effects, AND the physician has age. Prior of menopause, safer alternatives are: Premarin Cream, Estring, and EXTRA) documented that the patient has tried and failed two authorization Femring. For Bone Density, safer alternatives are: alendronate, (2) safer formulary alternatives or provided clinical required for age raloxifene, and Prolia. JEVTANA Jevtana BvsD coverage determination KABIVEN KADCYLA Antineoplastics, Monoclonal Antibodies B vs D coverage determination KALYDECO 2 years of age Patients with cystic fibrosis CF mutation test documenting patient has one and older for (CF) who are homozygous for mutation in the CFTR gene that is responsive to KALYDECO packets. 6 years the F508del mutation in the ivacaftor based on clinical and/or in vitro assay of age and older CFTR gene. data. for tablets. KCL 0.075%/D5W/NACL 0.45% KCL 0.15%/D5W/ NACL 0.3%
18 KCL 0.15%/D5W/NACL 0.2% KCL 0.15%/D5W/NACL 0.225% KCL 0.15%/D5W/NACL 0.45% KCL 0.15%/D5W/NACL 0.9% KCL 0.3%/D5W/NACL 0.45% KCL 0.3%/D5W/NACL 0.9% KEYTRUDA Antineoplastics, Monoclonal Antibodies B vs D coverage determination Treatment of rheumatoid arthritis (RA) in adults and when the following criteria are met: inadequate response, intolerance, or For RA: 18 years contraindication to at least one disease-modifying anti-rheumatic drug KINERET KINERET and older (DMARD) (i.e., methotrexate (MTX), azathioprine, gold, hydroxychloroquine, penicillamine, sulfasalazine) AND the patient has had failure, contraindication, or intolerance to Enbrel or Humira. KISQALI Molecular Inhibitors Molecular KISQALI FEMARA 200 DOSE Inhibitors Molecular KISQALI FEMARA 400 DOSE Inhibitors Molecular KISQALI FEMARA 600 DOSE Inhibitors KORLYM KORLYM KUVAN Kuvan Documentation of diagnosis KYPROLIS LACTATED RINGERS LACTATED RINGERS VIAFLEX with the medication and how that benefit outweighs member is less LANOXIN (only covered on HRM - the potential risk, AND the physician will continue than 65 years of PDP Secure, PDP Secure- through the Digoxin to monitor for side effects, AND the physician has age. Prior Extra) documented that the patient has tried and failed authorization digoxin 0.125mg daily or provided clinical required for age rationale as to why the lower dose is not 65 or older. appropriate for the patient. with the medication and how that benefit outweighs member is less HRM - the potential risk, AND the physician will continue than 65 years of LANOXIN PEDIATRIC through the Digoxin to monitor for side effects, AND the physician has age. Prior documented that the patient has tried and failed authorization digoxin 0.125mg daily or provided clinical required for age rationale as to why the lower dose is not 65 or older. appropriate for the patient. Antineoplastics LARTRUVO, Monoclonal B vs D coverage determination Antibodies Molecular LENVIMA 10 MG DAILY DOSE Inhibitors
19 Molecular LENVIMA 14 MG DAILY DOSE Inhibitors Molecular LENVIMA 18 MG DAILY DOSE Inhibitors Molecular LENVIMA 20 MG DAILY DOSE Inhibitors Molecular LENVIMA 24 MG DAILY DOSE Inhibitors Molecular LENVIMA 8 MG DAILY DOSE Inhibitors LETAIRIS Letairis Documentation of diagnosis LEUKINE Colony stimulating factors Documentation of diagnosis. 6 months LEUPROLIDE ACETATE Pituitary Hormones For the FDA-labeled indication of post-herpetic neuralgia, no additional criteria are required to be met. For diabetic neuropathic pain: the patient must have previous use and inadequate response or Lidocaine LIDOCAINE intolerance to any ONE medication that is FDA-labeled for diabetic Patch peripheral neuropathy, including (but not limited to) duloxetine and Lyrica. For cancer related neuropathic pain (including treatmentrelated neuropathy), no additional criteria are required to be met. LIPOSYN III LONSURF LONSURF LUMIZYME Lumizyme Documentation of diagnosis B vs D coverage determination LUPRON DEPOT (4- Pituitary MONTH) Hormones LUPRON DEPOT (6- Pituitary MONTH) Hormones LUPRON DEPOT MG Pituitary (3-MONTH) Hormones LUPRON DEPOT 22.5 MG Pituitary (3-MONTH) Hormones LUPRON DEPOT 3.75 MG Pituitary (1-MONTH) Hormones LUPRON DEPOT 7.5 MG Pituitary (1-MONTH) Hormones LUPRON DEPOT-PED (1- Pituitary MONTH) Hormones LUPRON DEPOT-PED (3- Pituitary MONTH) Hormones LYNPARZA Molecular Inhibitors MAGNESIUM SULFATE IN D5W MAGNESIUM SULFATE INJ MAGNESIUM SULFATE IV
2018 Cigna-HealthSpring Prior Authorization Criteria
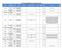 2018 Cigna-HealthSpring Prior Authorization Criteria Drug Name Prior Authorization Type Description Product Group Covered Uses Exclusion Criteria Required Medical Information Age Restrictions Prescriber
2018 Cigna-HealthSpring Prior Authorization Criteria Drug Name Prior Authorization Type Description Product Group Covered Uses Exclusion Criteria Required Medical Information Age Restrictions Prescriber
Age Restrictions. Prescriber Restrictions. Documentation of diagnosis and past medication history.
 2018 Cigna-HealthSpring Authorization Criteria - - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO) Drug Name Authorization
2018 Cigna-HealthSpring Authorization Criteria - - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO) Drug Name Authorization
1 P a g e. Systemic Juvenile Idiopathic Arthritis (SJIA) (1.3) Patients 2 years of age and older with active systemic juvenile idiopathic arthritis.
 LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
Circle Yes or No Y N. [If no, skip to question 7.] 2. Does the patient have a diagnosis of ulcerative colitis? Y N. [If no, skip to question 4.
![Circle Yes or No Y N. [If no, skip to question 7.] 2. Does the patient have a diagnosis of ulcerative colitis? Y N. [If no, skip to question 4. Circle Yes or No Y N. [If no, skip to question 7.] 2. Does the patient have a diagnosis of ulcerative colitis? Y N. [If no, skip to question 4.](/thumbs/85/91758188.jpg) 06/01/2016 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Humira (MI88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
06/01/2016 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Humira (MI88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
Product Group Covered Uses Exclusion Criteria Required Medical Information Age Restrictions
 2016 Cigna-HealthSpring Criteria - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO) (Updated November 2016) Drug Name Type
2016 Cigna-HealthSpring Criteria - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO) (Updated November 2016) Drug Name Type
ABRAXANE. Products Affected. Prior Authorization Criteria 2019 Secure-Essential PDP 5 Tier Last Updated: 10/01/2018. Abraxane
 Prior Authorization 2019 Secure-Essential PDP 5 Tier Last Updated: 10/01/2018 ABRAXANE Abraxane PA Details Age Other B vs D coverage determination 1 ACITRETIN Acitretin PA Details Documentation of diagnosis.
Prior Authorization 2019 Secure-Essential PDP 5 Tier Last Updated: 10/01/2018 ABRAXANE Abraxane PA Details Age Other B vs D coverage determination 1 ACITRETIN Acitretin PA Details Documentation of diagnosis.
HARVARD PILGRIM HEALTH CARE RECOMMENDED MEDICATION REQUEST GUIDELINES HUMIRA PEDIATRIC
 Generic Brand HICL GCN Exception/Other ADALIMUMAB HUMIRA 24800 HUMIRA PEDIATRIC GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the patient currently taking Humira? If
Generic Brand HICL GCN Exception/Other ADALIMUMAB HUMIRA 24800 HUMIRA PEDIATRIC GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the patient currently taking Humira? If
2. Is the patient responding to Remicade therapy? Y N
 09/29/2015 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Remicade (MI88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
09/29/2015 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Remicade (MI88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
ABRAXANE. Products Affected. Prior Authorization Criteria 2019 Secure-Extra PDP 6 Tier Last Updated: 12/2018. Abraxane
 Prior Authorization 2019 Secure-Extra PDP 6 Tier Last Updated: 12/2018 ABRAXANE Abraxane PA Details Age Other B vs D coverage determination 1 ACITRETIN Acitretin PA Details Documentation of diagnosis.
Prior Authorization 2019 Secure-Extra PDP 6 Tier Last Updated: 12/2018 ABRAXANE Abraxane PA Details Age Other B vs D coverage determination 1 ACITRETIN Acitretin PA Details Documentation of diagnosis.
HARVARD PILGRIM HEALTH CARE RECOMMENDED MEDICATION REQUEST GUIDELINES
 Generic Brand HICL GCN Exception/Other CERTOLIZUMAB PEGOL CIMZIA 35554 GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the request for a patient with a diagnosis of moderate
Generic Brand HICL GCN Exception/Other CERTOLIZUMAB PEGOL CIMZIA 35554 GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the request for a patient with a diagnosis of moderate
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
2. Has the patient had a response to treatment? Y N. 3. Does the patient have a diagnosis of rheumatoid arthritis (RA)? Y N
 12/21/2016 Prior Authorization Aetna Better Health of West Virginia Humira (WV88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
12/21/2016 Prior Authorization Aetna Better Health of West Virginia Humira (WV88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
ADALIMUMAB Generic Brand HICL GCN Exception/Other ADALIMUMAB HUMIRA GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW)
 Generic Brand HICL GCN Exception/Other ADALIMUMAB HUMIRA 24800 GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Does the patient have a diagnosis of moderate to severe rheumatoid
Generic Brand HICL GCN Exception/Other ADALIMUMAB HUMIRA 24800 GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Does the patient have a diagnosis of moderate to severe rheumatoid
Humira (adalimumab) DRUG.00002
 Humira (adalimumab) DRUG.00002 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Humira 10 mg/0.2 ml syringe Humira pediatric Crohn s Disease starter pack 40 mg/0.8 ml
Humira (adalimumab) DRUG.00002 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Humira 10 mg/0.2 ml syringe Humira pediatric Crohn s Disease starter pack 40 mg/0.8 ml
Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases
 Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy
Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy
Drug Name Tier Drug Name Tier
 Drug Name Tier Drug Name Tier ABELCET 100 MG/20 ML VIAL 4 ACETYLCYSTEINE 10% VIAL 2 ACETYLCYSTEINE 20% VIAL 2 ACYCLOVIR 1,000 MG/20 ML VIAL 2 ACYCLOVIR 500 MG/10 ML VIAL 2 ADRUCIL 500 MG/10 ML VIAL 2 ALBUTEROL
Drug Name Tier Drug Name Tier ABELCET 100 MG/20 ML VIAL 4 ACETYLCYSTEINE 10% VIAL 2 ACETYLCYSTEINE 20% VIAL 2 ACYCLOVIR 1,000 MG/20 ML VIAL 2 ACYCLOVIR 500 MG/10 ML VIAL 2 ADRUCIL 500 MG/10 ML VIAL 2 ALBUTEROL
ACTIMMUNE. Products Affected Actimmune Prior Authorization Criteria Effective: 06/01/2016 Updated 06/2016
 2016 Prior Authorization Effective: 06/01/2016 Updated 06/2016 ACTIMMUNE Products Affected Actimmune Other 1 ADAGEN Products Affected Adagen Other Contraindicated in bone marrow transplantation and in
2016 Prior Authorization Effective: 06/01/2016 Updated 06/2016 ACTIMMUNE Products Affected Actimmune Other 1 ADAGEN Products Affected Adagen Other Contraindicated in bone marrow transplantation and in
ACTIMMUNE. Products Affected Actimmune Prior Authorization Criteria Effective: 11/01/2016 Updated 11/2016
 2016 Prior Authorization Effective: 11/01/2016 Updated 11/2016 ACTIMMUNE Products Affected Actimmune PA Details Age Other 1 ADAGEN Products Affected Adagen PA Details Age Other Contraindicated in bone
2016 Prior Authorization Effective: 11/01/2016 Updated 11/2016 ACTIMMUNE Products Affected Actimmune PA Details Age Other 1 ADAGEN Products Affected Adagen PA Details Age Other Contraindicated in bone
First Name. Specialty: Fax. First Name DOB: Duration:
 Prescriber Information Last ame: First ame DEA/PI: Specialty: Phone - - Fax - - Member Information Last ame: First ame Member ID umber DOB: - - Medication Information: Drug ame and Strength: Diagnosis:
Prescriber Information Last ame: First ame DEA/PI: Specialty: Phone - - Fax - - Member Information Last ame: First ame Member ID umber DOB: - - Medication Information: Drug ame and Strength: Diagnosis:
8-MOP. Products Affected
 2018 First Choice VIP Care Plus Document: 2018 Prior Authorization Formulary ID: 18395 Last Updated: 10/2018 Effective Date: 11-01-2018 8-MOP 8-MOP Age must be a dermatologist or an oncologist. 1 ABILIFY
2018 First Choice VIP Care Plus Document: 2018 Prior Authorization Formulary ID: 18395 Last Updated: 10/2018 Effective Date: 11-01-2018 8-MOP 8-MOP Age must be a dermatologist or an oncologist. 1 ABILIFY
Infliximab/Infliximab-dyyb DRUG.00002
 Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Remicade (infliximab) DRUG.00002
 Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Cyltezo (adalimumab-adbm) CG-DRUG-64, CG-DRUG-65
 Market DC Cyltezo (adalimumab-adbm) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Cyltezo (adalimumab-adbm) 40 mg/0.8 ml prefilled syringe #* ^ Approval Duration 1 year
Market DC Cyltezo (adalimumab-adbm) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Cyltezo (adalimumab-adbm) 40 mg/0.8 ml prefilled syringe #* ^ Approval Duration 1 year
3. Did the patient show evidence of remission by week 8 of Humira Y N therapy?
 09/23/2015 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
09/23/2015 Prior Authorization AETA BETTER HEALTH OF MICHIGA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG CG-DRUG-64
 Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG.00002 CG-DRUG-64 Override(s) Prior Authorization *Washington Medicaid See State Specific Mandates Medications Inflectra
Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG.00002 CG-DRUG-64 Override(s) Prior Authorization *Washington Medicaid See State Specific Mandates Medications Inflectra
Subject: Remicade (Page 1 of 5)
 Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
ABIRATERONE. Products Affected Abiraterone Acetate
 Prior Authorization 2019 Arizona -H0354 -Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO), Cigna-HealthSpring Alliance (HMO) Last Updated:
Prior Authorization 2019 Arizona -H0354 -Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna-HealthSpring Preferred Plus (HMO), Cigna-HealthSpring Alliance (HMO) Last Updated:
CIMZIA (certolizumab pegol)
 Pre - PA Allowance None Prior-Approval Requirements Age Diagnoses 18 years of age or older Patient must have ONE of the following: 1. Moderate to severe Crohn s Disease (CD) a. Inadequate response, intolerance
Pre - PA Allowance None Prior-Approval Requirements Age Diagnoses 18 years of age or older Patient must have ONE of the following: 1. Moderate to severe Crohn s Disease (CD) a. Inadequate response, intolerance
INFLIXIMAB Remicade (infliximab), Inflectra (infliximab-dyyb), Ixifi* (infliximabqbtx), Renflexis (infliximab-abda)
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following: 6 years of age or older 1. Moderate to severe Crohn s disease (CD) a. Patient has fistulizing disease
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following: 6 years of age or older 1. Moderate to severe Crohn s disease (CD) a. Patient has fistulizing disease
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 01/01/2017 Updated: 11/2016
 2017 Prior Authorization Effective: 01/01/2017 Updated: 11/2016 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
2017 Prior Authorization Effective: 01/01/2017 Updated: 11/2016 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 11/01/2017 Updated 11/2017
 2017 Prior Authorization Effective: 11/01/2017 Updated 11/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
2017 Prior Authorization Effective: 11/01/2017 Updated 11/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
ACTEMRA. Cigna Medicare Rx (PDP) 2014 Cigna Medicare Rx Secure-Xtra Plan (PDP) Formulary. Products Affected Actemra. Prior Authorization Criteria
 Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure-Xtra Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure-Xtra Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Prior Authorization Conditions for Approval of Humira (adalimumab) Website Form Submit request via: Fax
 Prior Authorization Conditions for Approval of Humira (adalimumab) Website Form www.highmarkhealthoptions.com Submit request via: Fax - 1-855-476-4158 All requests for Humira (adalimumab) require a prior
Prior Authorization Conditions for Approval of Humira (adalimumab) Website Form www.highmarkhealthoptions.com Submit request via: Fax - 1-855-476-4158 All requests for Humira (adalimumab) require a prior
1. Background: Infliximab is administered parenterally; therefore, it is not covered under retail pharmacy benefits.
 Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
ACTHAR HP GEL PA MEDICATION(S) H.P. ACTHAR. COVERED USES All FDA-approved indications not otherwise excluded from Part D. EXCLUSION CRITERIA N/A
 ACTHAR HP GEL PA H.P. ACTHAR Criteria for approval are ALL of the following: 1. ONE of: A. Diagnosis of infantile spasm OR B. Diagnosis of multiple sclerosis AND i. Patient is experiencing an acute exacerbation
ACTHAR HP GEL PA H.P. ACTHAR Criteria for approval are ALL of the following: 1. ONE of: A. Diagnosis of infantile spasm OR B. Diagnosis of multiple sclerosis AND i. Patient is experiencing an acute exacerbation
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 04/01/2017 Updated 04/2017
 2017 Prior Authorization Effective: 04/01/2017 Updated 04/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
2017 Prior Authorization Effective: 04/01/2017 Updated 04/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 03/01/2017 Updated 03/2017
 2017 Prior Authorization Effective: 03/01/2017 Updated 03/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
2017 Prior Authorization Effective: 03/01/2017 Updated 03/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
UnitedHealthcare Pharmacy Clinical Pharmacy Programs
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1041-8 Program Prior Authorization/Notification Medication Humira (adalimumab) P&T Approval Date 1/2007, 6/2008, 4/2009, 6/2009,
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1041-8 Program Prior Authorization/Notification Medication Humira (adalimumab) P&T Approval Date 1/2007, 6/2008, 4/2009, 6/2009,
C. Assess clinical response after the first three months of treatment.
 Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 01/01/2017 Updated 12/2016
 2017 Prior Authorization Effective: 01/01/2017 Updated 12/2016 ACTHAR GEL Products Affected H.p. Acthar PA Details Covered Uses All medically accepted indications not otherwise excluded from Part D. Age
2017 Prior Authorization Effective: 01/01/2017 Updated 12/2016 ACTHAR GEL Products Affected H.p. Acthar PA Details Covered Uses All medically accepted indications not otherwise excluded from Part D. Age
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 06/01/2017 Updated 06/2017
 2017 Prior Authorization Effective: 06/01/2017 Updated 06/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
2017 Prior Authorization Effective: 06/01/2017 Updated 06/2017 ACTHAR GEL Products Affected H.p. Acthar Covered Uses All medically accepted indications not otherwise excluded from Part D. Other Covered
Biologics for Autoimmune Diseases
 Biologics for Autoimmune Diseases Goal(s): Restrict use of biologics to OHP funded conditions and according to OHP guidelines for use. Promote use that is consistent with national clinical practice guidelines
Biologics for Autoimmune Diseases Goal(s): Restrict use of biologics to OHP funded conditions and according to OHP guidelines for use. Promote use that is consistent with national clinical practice guidelines
2. Does the patient have a diagnosis of ulcerative colitis or Crohn s? Y N
 Pharmacy Prior Authorization AETA BETTER HEALTH LOUISIAA (MEDICAID) Remicade (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
Pharmacy Prior Authorization AETA BETTER HEALTH LOUISIAA (MEDICAID) Remicade (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign
ACTHAR GEL. Products Affected H.p. Acthar Prior Authorization Criteria Effective: 07/01/2017 Updated 07/2017
 2017 Prior Authorization Effective: 07/01/2017 Updated 07/2017 ACTHAR GEL Products Affected H.p. Acthar PA Details Covered Uses All medically accepted indications not otherwise excluded from Part D. Age
2017 Prior Authorization Effective: 07/01/2017 Updated 07/2017 ACTHAR GEL Products Affected H.p. Acthar PA Details Covered Uses All medically accepted indications not otherwise excluded from Part D. Age
Pharmacy Prior Authorization
 Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of: (2-3)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Amjevita (adalimumab-atto)
 *- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
*- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
Pharmacy Management Drug Policy
 SUBJECT: Cimzia (Certolizumab pegol) - for Ankylosing Spondylitis, Crohn s Disease, Psoriatic Arthritis and Rheumatoid Arthritis POLICY NUMBER: PHARMACY-07 EFFECTIVE DATE: 5/2009 LAST REVIEW DATE: 6/13/2018
SUBJECT: Cimzia (Certolizumab pegol) - for Ankylosing Spondylitis, Crohn s Disease, Psoriatic Arthritis and Rheumatoid Arthritis POLICY NUMBER: PHARMACY-07 EFFECTIVE DATE: 5/2009 LAST REVIEW DATE: 6/13/2018
ACTEMRA SC. Products Affected
 Advantra (HMO), Advantra (PPO), Advantra Advantage (HMO), Advantra Cares (HMO SNP), Advantra Choice (HMO), Advantra Freedom (PPO), Advantra Freedom Plus (PPO), Advantra Gold (PPO), Advantra Option 1 (HMO-POS),
Advantra (HMO), Advantra (PPO), Advantra Advantage (HMO), Advantra Cares (HMO SNP), Advantra Choice (HMO), Advantra Freedom (PPO), Advantra Freedom Plus (PPO), Advantra Gold (PPO), Advantra Option 1 (HMO-POS),
DRAFT. Therapeutic Class Code: D6A, S2J, S2M, S2Q, Z2U, Z2Z, S2Z, L1A, S2V, Z2V, D6K Therapeutic Class Description: Injectable Immunomodulators
 AFT Therapeutic Class Code: D6A, S2J, S2M, S2Q, Z2U, Z2Z, S2Z, L1A, S2V, Z2V, D6K Therapeutic Class Description: Injectable Immunomodulators Medication Generic Code Number(s) NDC Number(s) Actemra SQ 35486
AFT Therapeutic Class Code: D6A, S2J, S2M, S2Q, Z2U, Z2Z, S2Z, L1A, S2V, Z2V, D6K Therapeutic Class Description: Injectable Immunomodulators Medication Generic Code Number(s) NDC Number(s) Actemra SQ 35486
Pharmacy Prior Authorization
 Pharmacy Prior Authorization MERC CARE PLA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
Pharmacy Prior Authorization MERC CARE PLA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
Pharmacy Management Drug Policy
 SUBJECT: Inflammatory Conditions Clinical Review Prior Authorization (CRPA) Rx and Medical Drugs POLICY NUMBER: PHARMACY-73 EFFECTIVE DATE: 01/01/2018 LAST REVIEW DATE: 06/11/2018 If the member s subscriber
SUBJECT: Inflammatory Conditions Clinical Review Prior Authorization (CRPA) Rx and Medical Drugs POLICY NUMBER: PHARMACY-73 EFFECTIVE DATE: 01/01/2018 LAST REVIEW DATE: 06/11/2018 If the member s subscriber
PRIOR AUTHORIZATION PROTOCOLS
 PRIOR AUTHORIZATION PROTOCOLS How do I request an exception to the Central Health Plan s Formulary? You can ask Central Health Plan to make an exception to our coverage rules. There are several types of
PRIOR AUTHORIZATION PROTOCOLS How do I request an exception to the Central Health Plan s Formulary? You can ask Central Health Plan to make an exception to our coverage rules. There are several types of
ANTIDEPRESSANTS. Details. Step Therapy 2018 Last Updated: 8/21/2018
 ANTIDEPRESSANTS EMSAM PATCH 24 HOUR 12 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 6 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 9 MG/24HR TRANSDERMAL FETZIMA CAPSULE EXTENDED RELEASE 24 HOUR 120 MG ORAL FETZIMA
ANTIDEPRESSANTS EMSAM PATCH 24 HOUR 12 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 6 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 9 MG/24HR TRANSDERMAL FETZIMA CAPSULE EXTENDED RELEASE 24 HOUR 120 MG ORAL FETZIMA
Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65
 Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
Stelara. Stelara (ustekinumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
PA Criteria. Prior Authorization Group ACITRETIN Drug Names. ACITRETIN Covered Uses
 PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
Covered Uses: All FDA-approved indications not otherwise excluded from Part D
 ACNE PRODUCTS Epiduo Tretinoin Exclusion Criteria: Esthetic purposes Required Medical Information: 1) Diagnosis: acne vulgaris Age Restrictions: N/A Prescription Order Restrictions: N/A TSA 2018 Platino
ACNE PRODUCTS Epiduo Tretinoin Exclusion Criteria: Esthetic purposes Required Medical Information: 1) Diagnosis: acne vulgaris Age Restrictions: N/A Prescription Order Restrictions: N/A TSA 2018 Platino
ANTIDEPRESSANTS. Details. Step Therapy 2017 Last Updated: 5/23/2017
 ANTIDEPRESSANTS EMSAM PATCH 24 HOUR 12 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 6 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 9 MG/24HR TRANSDERMAL FETZIMA CAPSULE EXTENDED RELEASE 24 HOUR 120 MG FETZIMA CAPSULE
ANTIDEPRESSANTS EMSAM PATCH 24 HOUR 12 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 6 MG/24HR TRANSDERMAL EMSAM PATCH 24 HOUR 9 MG/24HR TRANSDERMAL FETZIMA CAPSULE EXTENDED RELEASE 24 HOUR 120 MG FETZIMA CAPSULE
Somavert ALL FDA-APPROVED INDICATIONS NOT OTHERWISE EXCLUDED FROM PART D.
 ACROMEGALY THERAPY Somatuline Depot subcutaneous syringe 120 mg/0.5 ml, 60 mg/0.2 ml, 90 mg/0.3 ml Somavert Age Other ALL FDA-APPROVED INDICATIONS NOT OTHERWISE PATIENT PROGRESS NOTES, DOCUMENTATION OF
ACROMEGALY THERAPY Somatuline Depot subcutaneous syringe 120 mg/0.5 ml, 60 mg/0.2 ml, 90 mg/0.3 ml Somavert Age Other ALL FDA-APPROVED INDICATIONS NOT OTHERWISE PATIENT PROGRESS NOTES, DOCUMENTATION OF
intolerance to, contraindication to, or therapeutic failure on a minimum 3 month trial of Inflectra*
 What s New Medical Pharmaceutical Policy March 2018 Updates MBP 5.0 Remicade (infliximab), Inflectra (infliximab-dyyb), Renflexis (infliximab-abda)- Updated policy Remicade (infliximab), Inflectra (infliximab-dyyb)
What s New Medical Pharmaceutical Policy March 2018 Updates MBP 5.0 Remicade (infliximab), Inflectra (infliximab-dyyb), Renflexis (infliximab-abda)- Updated policy Remicade (infliximab), Inflectra (infliximab-dyyb)
PRIOR AUTHORIZATION PROTOCOLS
 2018 PRIOR AUTHORIZATION PROTOCOLS How do I request an exception to the Imperial Health Plan s Formulary? You can ask Imperial Health Plan to make an exception to our coverage rules. There are several
2018 PRIOR AUTHORIZATION PROTOCOLS How do I request an exception to the Imperial Health Plan s Formulary? You can ask Imperial Health Plan to make an exception to our coverage rules. There are several
1. Does the patient have a diagnosis of moderate to severe polyarticular juvenile idiopathic arthritis (PJIA)?
 Humira (adalimumab) Medication Request Form (MRF) for Healthy Indiana Plan (HIP) and Hoosier Healthwise (HHW) FAX TO: (858) 790-7100 c/o MedImpact Healthcare Systems, Inc. Attn: Prior Authorization Department
Humira (adalimumab) Medication Request Form (MRF) for Healthy Indiana Plan (HIP) and Hoosier Healthwise (HHW) FAX TO: (858) 790-7100 c/o MedImpact Healthcare Systems, Inc. Attn: Prior Authorization Department
3. Has the patient shown improvement in signs and symptoms of the disease? Y N
 Pharmacy Prior Authorization MERC CARE (MEDICAID) Renflexis (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
Pharmacy Prior Authorization MERC CARE (MEDICAID) Renflexis (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
Drugs That Require Prior Authorization (PA) Before Being Approved for Coverage
 Drugs That Require Prior Authorization (PA) Before Being Approved for Coverage You will need authorization by AvMed Medicare before filling prescriptions for the drugs listed below. AvMed Medicare will
Drugs That Require Prior Authorization (PA) Before Being Approved for Coverage You will need authorization by AvMed Medicare before filling prescriptions for the drugs listed below. AvMed Medicare will
ACNE AGENTS_NVT Chinese Community Health Plan Senior Select Program (HMO SNP)
 ACNE AGENTS_NVT adapalene topical cream adapalene topical gel Avita tretinoin tretinoin microspheres topical gel Age Other 1 ADAGEN_NVT Adagen Age Other 2 ADCIRCA_NVT 2017 Adcirca Diagnosis confirmed by
ACNE AGENTS_NVT adapalene topical cream adapalene topical gel Avita tretinoin tretinoin microspheres topical gel Age Other 1 ADAGEN_NVT Adagen Age Other 2 ADCIRCA_NVT 2017 Adcirca Diagnosis confirmed by
HARVARD PILGRIM HEALTH CARE RECOMMENDED MEDICATION REQUEST GUIDELINES
 Generic Brand HICL GCN Exception/Other GOLIMUMAB SIMPONI 22533, 22536, 34697, 35001 ROUTE = SUBCUTANE. GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the request for a
Generic Brand HICL GCN Exception/Other GOLIMUMAB SIMPONI 22533, 22536, 34697, 35001 ROUTE = SUBCUTANE. GUIDELINES FOR USE INITIAL CRITERIA (NOTE: FOR RENEWAL CRITERIA SEE BELOW) 1. Is the request for a
PA Criteria. Prior Authorization Group Drug Names Covered Uses
 PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications
PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications
ACITRETIN. EnvisionRxPlus 2018 Formulary Prior Authorization Criteria. Products Affected. acitretin
 ACITRETIN acitretin Age Other Severely impaired liver or kidney function. Chronic abnormally elevated blood lipid values. Concomitant use of methotrexate or tetracyclines. Pregnancy. Females of child-bearing
ACITRETIN acitretin Age Other Severely impaired liver or kidney function. Chronic abnormally elevated blood lipid values. Concomitant use of methotrexate or tetracyclines. Pregnancy. Females of child-bearing
CARE N CARE HEALTH PLAN
 ACTIMMUNE CARE N CARE HEALTH PLAN ACTIMMUNE Covered Uses All FDA-approved indications not otherwise excluded from Part D. Age This criteria applies to New Starts only. 1 ADAGEN ADAGEN Covered Uses All
ACTIMMUNE CARE N CARE HEALTH PLAN ACTIMMUNE Covered Uses All FDA-approved indications not otherwise excluded from Part D. Age This criteria applies to New Starts only. 1 ADAGEN ADAGEN Covered Uses All
ADCIRCA. Tribute 2017 Formulary 2017 Prior Authorization Criteria. Products Affected. Adcirca
 ADCIRCA Adcirca All FDA approved indications not otherwise excluded from Part D. Concomitant administration of riociguat with a specific PDE5 inhibitor (eg, sildenafil, tadalafil, vardenafil) Treatment
ADCIRCA Adcirca All FDA approved indications not otherwise excluded from Part D. Concomitant administration of riociguat with a specific PDE5 inhibitor (eg, sildenafil, tadalafil, vardenafil) Treatment
BENEFIT CHANGES TO NBPDP
 Bulletin #789 June 15, 2010 BENEFIT CHANGES TO NBPDP This update to the New Brunswick Prescription Drug Program (NBPDP) Formulary is effective June 15, 2010. Included in this bulletin: Regular Benefit
Bulletin #789 June 15, 2010 BENEFIT CHANGES TO NBPDP This update to the New Brunswick Prescription Drug Program (NBPDP) Formulary is effective June 15, 2010. Included in this bulletin: Regular Benefit
2018 Prior Authorization Criteria Updated 10/2017 Effective 01/01/2018
 ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications not
ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications not
Prior Authorization Criteria ACTIMMUNE
 Prior Authorization ACTIMMUNE ACTIMMUNE Covered Uses All FDA-approved indications not otherwise excluded from Part D. Age Effective 01/01/2019 Page 1 of 150 ADEMPAS Prior Authorization ADEMPAS Covered
Prior Authorization ACTIMMUNE ACTIMMUNE Covered Uses All FDA-approved indications not otherwise excluded from Part D. Age Effective 01/01/2019 Page 1 of 150 ADEMPAS Prior Authorization ADEMPAS Covered
PA Criteria. Prior Authorization Group Drug Names Covered Uses
 PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
2018 Prior Authorizations (List of Prior Authorizations)
 Prior Authorization Last Updated: April 24, 2018 Effective Date: May 1, 2018 2018 Prior Authorizations (List of Prior Authorizations) PLEASE READ CAREFULLY: THIS DOCUMENT CONTAINS INFORMATION ABOUT THE
Prior Authorization Last Updated: April 24, 2018 Effective Date: May 1, 2018 2018 Prior Authorizations (List of Prior Authorizations) PLEASE READ CAREFULLY: THIS DOCUMENT CONTAINS INFORMATION ABOUT THE
SAMPLE IgE: ESR: CRP: # Joints: %BSA: Height: Weight: BMI:
 Please Note: Medical Necessity Prior Authorization may be overrided for both formulary coverage and benefit design restrictions. They are issued at the full discretion of the benefit manager. PRIOR AUTHORIZATION
Please Note: Medical Necessity Prior Authorization may be overrided for both formulary coverage and benefit design restrictions. They are issued at the full discretion of the benefit manager. PRIOR AUTHORIZATION
What prescribers need to know
 HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
Biologic Immunomodulators Prior Authorization with Quantity Limit Program Summary
 Biologic Immunomodulators Prior Authorization with Quantity Limit Program Summary Biologic Immunomodulators Prior Authorization with Quantity Limit (with a preferred option) OBJECTIVE The intent of the
Biologic Immunomodulators Prior Authorization with Quantity Limit Program Summary Biologic Immunomodulators Prior Authorization with Quantity Limit (with a preferred option) OBJECTIVE The intent of the
PA Criteria Prior Authorization Group Drug Names Covered Uses
 PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications
PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals. ACTIMMUNE ACTIMMUNE All FDA-approved indications
2015 PRIOR AUTHORIZATION CRITERIA TABLE OF CONTENTS ACTHAR HP GEL... 8 ADCIRCA... 9 AFINITOR AFINITOR DISPERZ AMITIZA...
 2015 PRIOR AUTHORIZATION CRITERIA TABLE OF CONTENTS ACTHAR HP GEL... 8 ADCIRCA... 9 AFINITOR... 77 AFINITOR DISPERZ... 77 AMITIZA... 10 amitriptyline... 48 AMPYRA... 11 ANADROL-50... 14 RODERM... 17 ROGEL...
2015 PRIOR AUTHORIZATION CRITERIA TABLE OF CONTENTS ACTHAR HP GEL... 8 ADCIRCA... 9 AFINITOR... 77 AFINITOR DISPERZ... 77 AMITIZA... 10 amitriptyline... 48 AMPYRA... 11 ANADROL-50... 14 RODERM... 17 ROGEL...
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Clinical Policy: Etanercept (Enbrel) Reference Number: PA.CP.PHAR.250 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid
 Clinical Policy: (Enbrel) Reference Number: PA.CP.PHAR.250 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Enbrel ) is tumor necrosis
Clinical Policy: (Enbrel) Reference Number: PA.CP.PHAR.250 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Enbrel ) is tumor necrosis
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of:
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
PA Criteria. Prior Authorization Group ACITRETIN Drug Names. ACITRETIN Covered Uses
 PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
PA Criteria Prior Authorization Group ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of nonmelanoma skin cancers in high risk individuals, Lichen planus,
All FDA-approved indications not otherwise excluded from Part D, mycosis fungoides, Sezary syndrome, atopic dermatitis.
 PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals, Lichen planus, Keratosis follicularis
PA Criteria ACITRETIN ACITRETIN All FDA-approved indications not otherwise excluded from Part D, prevention of non-melanoma skin cancers in high risk individuals, Lichen planus, Keratosis follicularis
Medicare Advantage Plans
 Medicare Advantage Plans 2017 Prior Authorization and Step Therapy Updated: November 4, 2016 Health First Health Plans is an HMO plan with a Medicare Contract. Enrollment in Health First Health Plans depends
Medicare Advantage Plans 2017 Prior Authorization and Step Therapy Updated: November 4, 2016 Health First Health Plans is an HMO plan with a Medicare Contract. Enrollment in Health First Health Plans depends
ACTIMMUNE. HEALTHTEAM ADVANTAGE 2018 Prior Authorization Criteria. Products Affected ACTIMMUNE
 ACTIMMUNE HEALTHTEAM ADVANTAGE ACTIMMUNE Age This criteria applies to New Starts only. Effective 07/01/2018 1 ADAGEN ADAGEN Age Severe thrombocytopenia. Use in preparation for or in support of bone marrow
ACTIMMUNE HEALTHTEAM ADVANTAGE ACTIMMUNE Age This criteria applies to New Starts only. Effective 07/01/2018 1 ADAGEN ADAGEN Age Severe thrombocytopenia. Use in preparation for or in support of bone marrow
Inflectra Frequently Asked Questions
 Inflectra Frequently Asked Questions 1. What is the funding status of Inflectra (infliximab)? Earlier in 2016, Inflectra (infliximab) was added to the Ontario Drug Benefit (ODB) Formulary as a Limited
Inflectra Frequently Asked Questions 1. What is the funding status of Inflectra (infliximab)? Earlier in 2016, Inflectra (infliximab) was added to the Ontario Drug Benefit (ODB) Formulary as a Limited
Clinical Policy: Ustekinumab (Stelara) Reference Number: ERX.SPMN.167
 Clinical Policy: (Stelara) Reference Number: ERX.SPMN.167 Effective Date: 10/16 Last Review Date: 12/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Stelara) Reference Number: ERX.SPMN.167 Effective Date: 10/16 Last Review Date: 12/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
