Use of Mycophenolate Mofetil in Dermatology
|
|
|
- Malcolm Mathews
- 6 years ago
- Views:
Transcription
1 eissn X 394X Review Use of Mycophenolate Mofetil in Dermatology Oya Oğuz, 1 MD, Sadiye Keskin, 2 * MD Address: 1Professor of Dermatology, Cerrahpaşa Medical Faculty, Istanbul University, Fatih, Istanbul, Turkey; 2 Resident, Cerrahpaşa Medical Faculty, Istanbul University, Fatih, Istanbul, Turkey bayraklilar@hotmail.com * Corresponding author: Sadiye Keskin, MD, Cerrahpaşa Medical Faculty, Istanbul University, Fatih, Istanbul, Turkey Published: J Turk Acad Dermatol 2007;1 (4): 71401r This article is available from: Key Words: mycophenolate mofetil, indications Abstract Background: In the past two decades, many new small molecules with immunosuppressive properties have been developed to prevent allograft rejection to be used particularly after organ transplantation. During clinical investigation in these conditions some of these substances have been observed to provide therapeutic efficacy in inflammatory skin disorders, as well. Recently, mycophenolate mofetil which is derived from mycophenolic acid has been proven to be available in various inflammatory and autoimmune disorders of the skin because of its antitumoral, antibacterial and immunosuppressive properties. In the past two decades, an increasing number of immunosupressive new agents have been developed to prevent allograft rejection in organ transplantation. Some of these agents have been used in dermatology, because they have also been observed to provide therapeutic efficacy in inflammatory skin disorders. One of these agents is mycophenolate mofetil. Mycophenolate mofetil is a morpholino ester derived of an old drug, mycophenolic asid, which had been isolated from cultures of Penicillium stoloniferum. Mycophenolic asid, which is a lipid-soluble, weak organic asid, was shown to have antibacterial, antiviral, antifungal, antitumoral and immunosupressive properties [1]. In 1975, mycophenolic asid was used in treatment of psoriatic patients in dermatology. These studies have no longer been available because of its long term risk of carcinogenicity and gastrointestinal adverse effects whereas mycophenolate mofetil, a derivate of mycophenolic acid has been introduced. This new formulation showed enhanced bioavailability, tolerability and efficacy [1, 2]. By 1995, MMF received US FDA approval for the prevention of acute renal allograft rejection and soon became recognized as an effective treatment option for immune-mediated skin diseases. Mechanism of Action Mycophenolate mofetil selectively and noncompetitively inhibits inosine monophosphate dehydrogenase in de novo pathway of purine synthesis. This enzyme facilitates the conversion of inosine monophosphate to xanthine monophosphate, an intermediate metabolite which takes place in the production of guanosine triphosphate. As mycophenolate mofetil results in the depletion of the guanosine nucleotides, it impairs RNA, DNA and protein synthesis [1]. Page 1 of 6
2 The purine bases, adenosine and guanosine, may be synthesized through two pathways: De novo purine synthesis pathway, or hypoxanthine-guanine phosphoribosyl transferase salvage pathway. As the lymphocytes lack the salvage pathway, mycophenolate mofetil may selectively inhibit lymphocyte proliferation and antibody formation. Consequently the other cells were not influenced by mycophenolate mofetil. Mycophenolate mofetil also prevents glycosylation of lymphocyte and monocyte glycoproteins that are involved in adhesion to endothelial cells. It may also inhibit the recruitment of leukocytes to sites of inflammation and impair antigen presentation [1]. Pharmacokinetics After oral ingestion, mycophenolate mofetil is hydrolyzed to its active metabolite, mycophenolic acid, by plasma esterases. Predominantly bound to albumin, mycophenolic acid has a bioavailability that approaches 94%. The peak concentration of the active metabolite that is obtained within minutes after oral administration, undergoes hepatic conjugation to its inactive glucuronide form. Approximately 87% of the drug is excreted by urine, 6% by feces and the remainder undergoes enterohepatic recirculation. Beta glucuronidase, found within the epidermis and gastrointestinal tract, can convert inactive glucuronide form to active form [1]. Safety MMF is generally well tolerated. Compared to other immunosuppressants, such as methotrexate, azathioprine and cyclosporine, the lack of hepatonephrotoxicity with mycophenolate mofetil offers an important therapeutic advantage. The most common side-effects involve gastrointestinal (nausea, diarrhea, abdominal cramps, constipation, vomiting and anorexia) and genitourinary symptoms (urgency, frequency, dysuria, hematuria and sterile pyuria). These occur in up to 36% and 40% of cases. Other reported adverse events include neurologic (headache, tinnitus and insomnia), cutaneous (exanthematous eruptions, acne and pedal edema), cardiorespiratory (dyspnea, cough, chest pain, palpitations and hypertension) and metabolic (hypercholesterolemia, hyperglycemia, hypophosphatemia and hypo/hyperkalemia) reactions. Severe leukopenia has been reported to occur in less than 3% of patients treated with mycophenolate mofetil. Infection rates with mycophenolate mofetil therapy are difficult to quantify in the dermatologic literature. Opportunistic infections occur in up to 40% of transplant patients treated with mycophenolate mofetil; however, the majority of these patients are also treated with other immunosuppressive agents. In addition to common bacterial and viral infections, patients are at increased risk for herpes simplex, herpes zoster, cytomegalovirus, candidiasis, cryptococcosis, aspergillosis, mucormycosis and Pneumocystis carinii pneumonia. The long-term risk of carcinogenicity with mycophenolate mofetil remains controversial. In the dermatologic literature, few malignancies have been reported in patients receiving mycophenolate mofetil or its prodrug, mycophenolic acid. Lymphoproliferative disease or lymphoma developed in 0.4% -1% of patients receiving mycophenolate mofetil. Non-melanoma skin cancer occurred in 1.6%-4.2% of patients, while other types of malignancy appeared in 0.7% -2.1% of patients. While there are no adequate studies on mycophenolate mofetil in pregnant women, the drug has been shown to be teratogenic in animals. Therefore, mycophenolate mofetil should be avoided during pregnancy (pregnancy risk C) [1]. Dosage The usual dose of mycophenolate mofetil ranges from 2-3g/day in adults. Mycophenolate mofetil should be administered as 600mg/m 2 per dose every 12 hours in the pediatric population. In order to prevent a disease flare, many clinicians would consider tapering MMF slowly. Dose of MMF reductions should be considered in patients with severe renal impairment [1]. Clinical Uses There exist a considerable number of reports and concerning the availability of mycophenolate mofetil in various dermatological disorders. These conditions are demonstrated in Table 1. Page 2 of 6
3 J Turk Acad Dermatol 2007; 1 (4): 71201r. Table 1. Dermatological Disorders in which Mycophenolate Mofetil may Exert Beneficial Effects Psoriasis Immunobullous diseases Pemphigus vulgaris Pemphigus foliaceus Paraneoplastic pemphigus Bullous pemphigoid Epidermolysis bullosa acquisita Linear IgA disease Connective tissue disease Systemic lupus erythematosus Discoid lupus erythematosus Dermatomyositis Wegener s granulomatosis Urticarial vasculitis Microscopic polyangiitis Takayasu s arteritis Lichen planus Pyoderma gangrenosum Idiopathic lobular panniculitis Dermatitis Atopic dermatitis Dyshidrotic dermatitis Chronic actinic dermatitis Graft-versus-host disease Sarcoidosis Cutaneous Crohn s disease Cutaneous lymphoma PSORIASIS Mycophenolate mofetil has been used in the treatment of psoriasis, since it suppressed pro-inflammatory cytokines and cytokines which stimulate keratinocyte proliferation and ICAM-1 (intercellular adhesion molecule-1) expression all of which are thought to be involved in the pathogenesis of psoriasis. Mycophenolate mofetil have been found more efficient especially in patients with chronic plaque psoriasis and erythrodermic psoriasis, while studies concerning results of treatment in pustular psoriasis are still lacking [2]. Mycophenolate mofetil was assessed in a clinical trial with 11 patients suffering from severe psoriasis. Oral mycophenolate mofetil was administered in doses of 1 g twice daily for 3 weeks and 0.5 g twice daily for 3 weeks. The clinical end point was a reduction in the psoriasis area and severity index (PASI). There was a reduction in PASI of 40% to 70% in 7 patients and of 25% to 39% in 3 patients within 3 weeks. After 6 weeks, there was a further improvement in 6 patients. The only side effect observed was muscle pain in 1 patient, which led to withdrawal from the study. The treatment was tolerated in all other patients without clinical and laboratory side effects. Thus, oral administration of 2 g mycophenolate mofetil per day has been shown to be safe and effective in the treatment of psoriasis [3, 4, 5, 6]. Because mycophenolate mofetil has been shown to provide therapeutic benefit in the treatment of rheumatoid arthritis, the drug was suggested to offer an alternative in the treatment of psoriatic arthritis. In a recent 10-week study, mycophenolate mofetil monotherapy (2 x 1 g daily) showed good tolerance and improvement in patients suffering from psoriatic arthritis [2, 3, 4]. Because adverse effects of cyclosporin, eight patients who had severe psoriasis were treated with mycophenolate mofetil where it has not been found as effective as cyclosporin, but suggested to be an alternative therapy in patients who could not tolerate cyclosporin because of its nephrotoxity [2, 7]. To summarize, mycophenolate mofetil is effective in the treatment of severe psoriasis, but more studies are still needed. IMMUNOBULLOUS DISEASES Oral mycophenolate mofetil was administered in 12 patients with pemphigus vulgaris, which had relapsed while they underwent treatment with azathioprine (1.5 2 mg/kg daily) and prednisolone (2 mg/kg daily). The patients received a combination therapy with mycophenolate mofetil (2 x1 g daily) and prednisolone (2 mg/kg daily). Eleven patients responded to the therapy and did not show any relapse of their disease, even after tapering the steroid dose. During the period of 9 to 12 months, none of the 11 patients showed recurrence of blistering lesions. Only 5 patients had mild gastrointestinal symptoms and 9 patients had mild lymphopenia [3]. In a patient with pemphigus vulgaris, mycophenolate mofetil (2 x1 g daily) led to a complete remission of skin lesions within 8 weeks, followed by a disease-free interval of 8 months during maintenance treatment [2, 3]. In 1996, the first report who has bullous pemphigoid that was treated with oral my- Page 3 of 6
4 cophenolate mofetil successfully has been demonstrated. After a 1-week treatment with 80 mg prednisolone daily, mycophenolate mofetil (2 x 1 g daily) was combined with prednisolone for 6 weeks and along with gradually tapered doses of prednisolone for a further 4 weeks, started as monotherapy for 10 months. During this treatment schedule no relapses occured [1]. Successful monotherapy with mycophenolate mofetil in bullous pemphigoid has been reported in two patients receiving 1 g mycophenolate mofetil twice daily. Resolution of the blisters was attained after 10 and 11 weeks, respectively, and there was no recurrence of blisters during 6 to 8 months of maintenance therapy [2, 3]. A patient with epidermolysis bullosa acquisita was successfully treated with mycophenolate mofetil. She received 1.5 g daily during the first week, 1 g daily for another 5 weeks, and 0.5 g for another 4 weeks. Thereafter, she was given 0.5 g mycophenolate mofetil every second day and remained without relapse of the disease for 6 months [3]. All these studies point out that mycophenolate mofetil is an effective agent and may be used in the treatment of immunobullous diseases. CONNECTIVE TISSUE DISEASES The efficacy of MMF in systemic lupus erythematosus has been clearly validated. Moreover, the cutaneous lesions of subacute cutaneous lupus erythematosus, chronic discoid lupus erythematosus and lupus perniosis have responded to MMF therapy. In a study evaluating effectiveness of MMF in 10 patients who had systemic lupus erythematosus by Gaubitz et al, mycophenolate mofetil was given gr daily to all patients and at the end of the study clinical healing have been achieved. Goya et al. have reported two patients who had palmoplantar discoid lupus erythematosus and were treated with mycophenolate mofetil successfully [2, 10]. Schanz et al. have reported two patients that had subacut cutaneous lupus erythematosus and were resistant to conventional therapy, but responded well to mycophenolate mofetil 2 gr/day [11]. Recently it has been reported to be effective in dermatomyositis, especially erythema and heliotropic rash improved with mycophenolate mofetil. 2 Other connective tissue disorders in which variable beneficial effects have been recorded are scleroderma, urticarial vasculitis, Takayasu's arteritis, microscopic polyangiitis, Wegener's granulomatosis, polyarteritis nodosa and Behçet's disease [1]. LICHEN PLANUS Mycophenolate mofetil has been used in some patients with lichen planus, since diffuse, hypertrophic, bullous and erosive forms of lichen planus are resistant to conventional therapy. 2gr daily mycophenolate mofetil was given to 2 patients with lichen planus that had diffuse and severely pruritic lesions and complete remission was achieved within 20 weeks [2]. PYODERMA GANGRENOSUM The management of pyoderma gangrenosum may be difficult and require prolonged treatment with systemic corticosteroids and/or other systemic immunosuppressants. There are some reports that have been shown that mycophenolate mofetil might be an effective treatment choice in pyoderma gangrenosum. Mycophenolate mofetil 2 g daily was given in combination with prednisolone and cyclosporine (200 mg daily) in a 68-year-old female patient suffering from severe and resistant ulcers due to pyoderma gangrenosum on the calves. This condition was controlled to some degree and additional topical treatment with autologous thrombocytic growth factor led to improvement of granulation and complete healing after 12 weeks. The patient was still disease free after 12 months [3]. In a 17-year-old male patient with severe recalcitrant pyoderma gangrenosum, healing was achieved with a combination of mycophenolate mofetil 2 g daily and cyclosporine (10 mg/kg daily), accompanied by negative-pressure dressings and split-skin grafts after 7 months of therapy. Complete remission was achieved after 10 months, and the doses of mycophenolate mofetil (2 x0.5 mg daily) and cyclosporine (150 mg daily) could be reduced [3, 12]. These case reports suggest that mycophe- Page 4 of 6
5 nolate mofetil is an alternative as part of a immunosuppressive combination therapy with cyclosporine and corticosteroid or cyclosporine alone in severe recalcitrant pyoderma gangrenosum. ERYTHEMA NODOSUM A case with erythema nodosum who had not responded to potassium iodide, azathioprine and indomethacine was reported to improve with mycophenolate mofetil 1g / day. Complete remission was achieved within 3 months [2]. IDIOPATHIC LOBULAR PANNICULITIS Idiopathic lobular panniculitis often requires prolonged treatment with high doses of systemic corticosteroids and/or immunosuppressants, such as cyclosporine, cyclophosphamide, methotrexate, or azathioprine. Mycophenolate mofetil (2 x1 g daily) was given in combination with prednisolone (2 mg/kg daily) in three patients who had not responded to a combination of prednisolone (2 mg/kg daily) with azathioprine (1.5 mg/kg daily) or to methotrexate (50 mg daily). Resolution of lesions and normalization of inflammatory blood parameters were achieved within 2 weeks. After discontinuation of the steroid treatment and reduction of mycophenolate mofetil to 2 x0.5 g daily, there was no relapse observed during the follow-up of 6 to 10 months [3]. DERMATITIS Two patients with severe atopic eczema who had not responded to conventional topical treatment or to systemic treatment with oral steroids, psoralen plus ultraviolet A (PUVA) photochemotherapy, or cyclosporine were treated with mycophenolate mofetil (1 g b.i.d) monotherapy. Clinical healing was reached within 2 to 4 weeks. The treatment was continued for another 4 weeks and was tolerated without side effects. During a follow -up of 12 weeks, no relapse was seen [2, 3]. In another study, 10 patients with severe atopic eczema were treated with oral mycophenolate mofetil at an initial dose of 2x0.5 g daily during the first week and 1g. b.i.d within 11 weeks. Compared with the baseline, the median scores for disease severity (SCORAD index) improved by 68% during treatment with mycophenolate mofetil. The median serum immunoglobulin E level decreased significantly after 12 weeks [3]. In another study mycophenolate mofetil 2x1 g /day was given to 10 patients with atopic eczema in a month and then 0.5g b.i.d mycophenolate mofetil was given within 20 weeks. Compared with the baseline, the median scores for disease severity (SCORAD index) improved by 74% during treatment with mycophenolate mofetil [1, 13].But in some of the studies, mycophenolate mofetil has not been found effective in the treatment of atopic eczema [14]. A patient with relapsing dyshidrotic eczema within corticosteroid therapy and was resistant to other therapeutic modalities including PUVA was treated with mycophenolate mofetil (1.5 mg b.i.d). Complete improvement was achieved within 4 weeks. The dose was reduced to 2 g/day and maintained for 12 months without recurrence of the eczema and therapy-related side effects [2, 3]. URTICARIA Since mycophenolate mofetil has been found to be effective in some patients with atopic eczema, 9 patients with urticaria who were resistant to antihistaminic agents and oral steoid, were treated with mycophenolate mofetil 2 g daily and pruritus was reduced and lesions were cleaned within 12 weeks. As a result, it has been concluded that mycophenolate mofetil may be used in patients with chronic idiopathic urticaria that is resistant to other conventional treatment, but more controlled studies are needed [15]. CHRONIC ACTINIC DERMATITIS Two patients with chronic actinic dermatitis who did not respond to conventional therapies including topical steroids, prednisolone, PUVA, azathioprine and cyclosporin and developed side effects, were treated with mycophenolate mofetil 1 and 2 g daily. After 6 weeks clinical improvement was observed. Consequently mycophenolate mofetil should be considered as an alternative treatment to conventional therapies for refractory chronic actinic dermatitis [2, 16]. GRAFT-VERSUS-HOST DISEASE (GVHD) Especially in pediatric ages, mycophenolate mofetil is an agent that can be selected in the treatment of GVHD. It is reported that mycophenolate mofetil and UVA-1 combina- Page 5 of 6
6 tion therapy is an alternative therapy in GVHD [2]. SARCOIDOSIS Kouba et al. have reported a patient with sarcoidosis who was treated with mycophenolate mofetil, hydroxychloroquin and prednisolone combination therapy. It is thought that mycophenolate mofetil could be an effective agent with other immunosuppressive agents in the treatment of sarcoidosis [2, 17]. CUTANEOUS CROHN S DISEASE Mycophenolate mofetil 1 g daily and thalidomide 200 mg daily combination therapy were given in a patient with perineal and metastatic cutaneous Crohn s disease that was resistant to azathioprine, methotrexate, prednisolone and FK-506, and reduction of lesions were achieved [2]. There is a variety of inflammatory skin disorders that have been shown to respond to oral mycophenolate mofetil either as monotherapy or in combination with systemic steroids and other immunosuppressants as steroid-sparing agents. Other systemic conditions with inflammatory or autoimmune pathogenesis which have cutaneous manifestations such as Behçet s disease or lymphoproliferative disorders may be targeted for future studies. References 1. Mydlarski PR. Mycophenolate mofetil: A dermatologic perspective. Skin Therapy Letter 2005; 10: 1-6. PMID: Altunay I. Dermatolojide mikofenolat mofetil. In: Dermatolojide Gelişmeler-6. Ed. Tüzün Y. Istanbul, Acamedia; 2007, pp Assmann T, Ruzicka T. New immunosuppressive drugs in dermatology (mycophenolate mofetil, tacrolimus): Unapproved uses, dosages, or indications. Clin Dermatol 2002; 20: PMID: Grundmann-Kollmann M, Mooser G, Schraeder P, Zollner T, Kaskel P, Ochsendorf F, Boehncke W, Kerscher M, Kaufmann R, Peter RU. Treatment of chronic plaque-stage psoriasis and psoriatic arthritis with mycophenolate mofetil. J Am Acad Dermatol 2000; 42: PMID: Tong DW, Walder BK. Widespread plaque psoriasis responsive to mycophenolate mofetil. Australas J Dermatol 1998; 40: PMID: Geilen CC, Arnold M, Orfanos CE. Mycophenolate mofetil as a systemic antipsoriatic agent: positive experience in 11 patients. Br J Dermatol 2001; 144: PMID: Davison SC. Morris-Jones R, Powles AV, Fry L. Change of treatment from cyclosporin to mycophenolate mofetil in severe psoriasis. Br J Dermatol 2000; 143: PMID: Williams JV, Marks JG, Billingsley EM. Use of mycophenolate mofetil in the treatment of paraneoplastic pemphigus. Br J Dermatol 2000; 142: PMID: Powell AM, Albert S, Al Fares S, Harman KE, Setterfield J, Bhogal B, Black MM. An evaluation of the usefulness of mycophenolate mofetil in pemghigus. Br J Dermatol 2003;149: PMID: Goyal S, Nousari HC. Treatment of resistant discoid lupus erythematosus of the palms and soles with mycophenolate mofetil. J Am Acad Dermatol 2001; 45: PMID: Schanz S, Ulmer A, Rassner G, Fierlbeck G. Successful treatment of subacute cutaneous lupus erythematosus with mycophenolate mofetil. Br J Dermatol 2002; 147: PMID: Gilmour E, Stewart DG. Severe recalcitrant pyoderma gangrenosum responding to a combination of mycophenolate mofetil with cyclosporin and complicated by a mononeuritis. Br J Dermatol 2001; 144: PMID: Grundmann-Kollmann M, Podda M, Ochsendorf F, Boehncke WH, Kaufmann R, Zollner TM. Mycophenolate mofetil is effective in the treatment of atopic dermatitis. Arch Dermatol 2001; 137: PMID: Murray ML, Cohen JB. Mycophenolate mofetil therapy for moderate to severe atopic dermatitis. Clin Dermatol 2006;32: PMID: Shahar E, Bergman R, Guttman-Yassky E, Pollack S. Treatment of severe chronic idiopathic urticaria with oral mycophenolate mofetil in patients not responding to antihistamines and/or corticosteroids. Int J Dermatol 2006; 45: PMID: Thomson MA, Stewart DG, Lewis HM. Chronic actinic dermatitis treated with mycophenolate mofetil. Br J Dermatol 2005; 152: PMID: Kouba DJ, Mimouni D, Rencic A, Nousari HC. Mycophenolate mofetil may serve as a steroid-sparing agent for sarcoidosis. Br J Dermatol 2003; 148: PMID: Page 6 of 6
Mycophenolate Mofetil
 Mycophenolate Mofetil Cynthia L. Chen, MD The Permanente Medical Group, Northern California Diablo Service Area February 17, 2018 January 23, 2018 2011 Kaiser Foundation Health Plan, Inc. For internal
Mycophenolate Mofetil Cynthia L. Chen, MD The Permanente Medical Group, Northern California Diablo Service Area February 17, 2018 January 23, 2018 2011 Kaiser Foundation Health Plan, Inc. For internal
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Mycophenolate in non-transplant disorders
 An initiative of NSW Clinical Pharmacologists & Pharmacists Funded by the NSW Department of Health Mycophenolate in non-transplant disorders (Includes review of therapeutic equivalence of mycophenolate
An initiative of NSW Clinical Pharmacologists & Pharmacists Funded by the NSW Department of Health Mycophenolate in non-transplant disorders (Includes review of therapeutic equivalence of mycophenolate
Autoimmune Diseases with Oral Manifestations
 Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Systemic Medications for the Dermatology Toolbox: Azathioprine
 Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
CELLCEPT Composition Properties Pharmacokinetics
 CELLCEPT Roche Composition Active ingredient: Mycophenolate mofetil. Capsules with 250 mg mycophenolate mofetil. Excipients: coloring agent E132, excipients for capsules. TABLETS with 500 mg mycophenolate
CELLCEPT Roche Composition Active ingredient: Mycophenolate mofetil. Capsules with 250 mg mycophenolate mofetil. Excipients: coloring agent E132, excipients for capsules. TABLETS with 500 mg mycophenolate
Dermatology GP Referral Guidelines
 Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Rayos Prior Authorization Program Summary
 Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Evolving therapies for posterior uveitis. Infliximab (Remicade) Infliximab: pharmacology. FDA-approved monoclonal antibody therapy Target
 Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Carolyn Bangert, MD Associated Dermatologists, PC
 Carolyn Bangert, MD Associated Dermatologists, PC Carolyn Bangert, MD Systemic Medications for the Dermatology Toolbox: Cyclosporine I have no relevant conflicts of interest with any companies. I will
Carolyn Bangert, MD Associated Dermatologists, PC Carolyn Bangert, MD Systemic Medications for the Dermatology Toolbox: Cyclosporine I have no relevant conflicts of interest with any companies. I will
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Post Transplant Immunosuppression: Consideration for Primary Care. Sameh Abul-Ezz, M.D., Dr.P.H.
 Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE. Drug: MYCOPHENOLATE MOFETIL/SODIUM Protocol number: CV 15
 Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: MYCOPHENOLATE MOFETIL/SODIUM Protocol number: CV 15 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: MYCOPHENOLATE MOFETIL/SODIUM Protocol number: CV 15 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION
SYNOPSIS (PROTOCOL WX17796)
 TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
Remicade (infliximab) DRUG.00002
 Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Infliximab/Infliximab-dyyb DRUG.00002
 Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Significance. Outline and Objectives. S007 Systemic Therapies for Medical Oncology
 S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG CG-DRUG-64
 Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG.00002 CG-DRUG-64 Override(s) Prior Authorization *Washington Medicaid See State Specific Mandates Medications Inflectra
Inflectra (infliximab-dyyb), Remicade (infliximab), Renflexis (infliximab-abda) DRUG.00002 CG-DRUG-64 Override(s) Prior Authorization *Washington Medicaid See State Specific Mandates Medications Inflectra
A case of bullous pemphigoid following pemphigus foliaceus
 #2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
#2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
DESCRIPTIONS FOR MED 3 ROTATIONS Dermatology A3S
 Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
Index. Angiosarcoma diagnosis, 47 lymphedema-related vs. non-lymphedemarelated, 48
 A Acneiform rash biopsy, 134 cetuximab, EGFR, 132 133 diagnosis, 131 patient history, 131 134 treatment, 134 135 Acne vulgaris, 109 AGA. See Androgenetic alopecia Alopecia areata, 148 American Joint Committee
A Acneiform rash biopsy, 134 cetuximab, EGFR, 132 133 diagnosis, 131 patient history, 131 134 treatment, 134 135 Acne vulgaris, 109 AGA. See Androgenetic alopecia Alopecia areata, 148 American Joint Committee
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis
 Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
CENTRAL NERVOUS SYSTEM VASCULITIS
 What is central nervous system (CNS) vasculitis? Central nervous system (CNS) vasculitis is among a family of rare disorders characterized by inflammation of the blood vessels, which restricts blood flow
What is central nervous system (CNS) vasculitis? Central nervous system (CNS) vasculitis is among a family of rare disorders characterized by inflammation of the blood vessels, which restricts blood flow
ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER
 European Medicines Agency Evaluation of Medicines for Human Use London, September 2006 Doc. Ref.: EMEA/381922/2006 ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER The Paediatric Working Party
European Medicines Agency Evaluation of Medicines for Human Use London, September 2006 Doc. Ref.: EMEA/381922/2006 ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER The Paediatric Working Party
Off-Label Dermatological Uses of Etanercept Treatment
 Review DOI: 10.6003/jtad.1593r1 Off-Label Dermatological Uses of Etanercept Treatment Belma Türsen, 1 MD, Ümit Türsen, 2 MD Address: 1 Mersin State Hospital, Department of Dermatology, 2 Mersin University,
Review DOI: 10.6003/jtad.1593r1 Off-Label Dermatological Uses of Etanercept Treatment Belma Türsen, 1 MD, Ümit Türsen, 2 MD Address: 1 Mersin State Hospital, Department of Dermatology, 2 Mersin University,
Manipulation of the Immune Response - Immunomodulation -
 Manipulation of the Immune Response - Immunomodulation - Janeway s Immunobiology, 9 th ed., 2017. Ivana Novak Nakir Immune system Immune system make components, cells and organs that act together to defend
Manipulation of the Immune Response - Immunomodulation - Janeway s Immunobiology, 9 th ed., 2017. Ivana Novak Nakir Immune system Immune system make components, cells and organs that act together to defend
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Treatment with steroids and immunosuppressants
 Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
D E R M A T O L O G Y
 We customize individual prescriptions for the specific needs of our patients. F E B R U A R Y 2 0 1 3 I N S I D E T H I S I S S U E : Psoriasis Vulgaris 2 Atopic Dermatitis 3 P R E S C R I P T I O N C
We customize individual prescriptions for the specific needs of our patients. F E B R U A R Y 2 0 1 3 I N S I D E T H I S I S S U E : Psoriasis Vulgaris 2 Atopic Dermatitis 3 P R E S C R I P T I O N C
Pediatric Pharmacotherapy
 Pediatric Pharmacotherapy A Monthly Review for Health Care Professionals of the Children's Medical Center Volume 4 Number 8, August 1998 Mycophenolate mofetil: Use in pediatrics Beth Ann Fullmer, R.Ph.,
Pediatric Pharmacotherapy A Monthly Review for Health Care Professionals of the Children's Medical Center Volume 4 Number 8, August 1998 Mycophenolate mofetil: Use in pediatrics Beth Ann Fullmer, R.Ph.,
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Rituximab in refractory autoimmune bullous diseases
 Clinical dermatology Review article doi: 10.1111/j.1365-2230.2006.02151.x Rituximab in refractory autoimmune bullous diseases E. Schmidt, N. Hunzelmann,* D. Zillikens, E.-B. Bröcker and M. Goebeler Departments
Clinical dermatology Review article doi: 10.1111/j.1365-2230.2006.02151.x Rituximab in refractory autoimmune bullous diseases E. Schmidt, N. Hunzelmann,* D. Zillikens, E.-B. Bröcker and M. Goebeler Departments
KEYTRUDA is also indicated in combination with pemetrexed and platinum chemotherapy for the
 FDA-Approved Indication for KEYTRUDA (pembrolizumab) in Combination With Carboplatin and Either Paclitaxel or Nab-paclitaxel for the Firstline Treatment of Patients With Metastatic Squamous Non Small Cell
FDA-Approved Indication for KEYTRUDA (pembrolizumab) in Combination With Carboplatin and Either Paclitaxel or Nab-paclitaxel for the Firstline Treatment of Patients With Metastatic Squamous Non Small Cell
Mycophenolate Mofetil (MMF)
 SCG: For Transplant patients The following guidelines are designed to provide information relating to mycophenolate mofetil and to outline the responsibilities of the primary and secondary care teams in
SCG: For Transplant patients The following guidelines are designed to provide information relating to mycophenolate mofetil and to outline the responsibilities of the primary and secondary care teams in
SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
Overview of New Approaches to Immunosuppression in Renal Transplantation
 Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
What prescribers need to know
 HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
RITUXAN (rituximab), NONONCOLOGIC USES
 RITUXAN (rituximab), NONONCOLOGIC USES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
RITUXAN (rituximab), NONONCOLOGIC USES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
New and emerging trends in the treatment of atopic dermatitis
 REVIEW New and emerging trends in the treatment of atopic dermatitis Christina M Gelbard 1 Adelaide A Hebert 1,2 1 Departments of Dermatology; 2 Pediatrics, University of Texas-Houston, Houston, TX, USA
REVIEW New and emerging trends in the treatment of atopic dermatitis Christina M Gelbard 1 Adelaide A Hebert 1,2 1 Departments of Dermatology; 2 Pediatrics, University of Texas-Houston, Houston, TX, USA
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research
 Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Corporate Medical Policy
 Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Announcing HUMIRA. Psoriasis Starter Package
 Announcing HUMIRA (adalimumab) Psoriasis Starter Package HUMIRA is indicated for the treatment of adult patients with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy
Announcing HUMIRA (adalimumab) Psoriasis Starter Package HUMIRA is indicated for the treatment of adult patients with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy
Table of Contents: Part 1 Medical Dermatology. Chapter 1 Acneiform Disorders. Acne. Acne Vulgaris. Pomade Acne. Steroid Acne
 Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
MYCOPHENOLATE MOFETIL In Renal Transplantation (prior to August 2004) and lupus nephritis/vasculitis
 Patient name Date of Birth DOCUMENT TO BE FILED IN NOTES AND SCANNED INTO ELECTRONIC RECORDS INTRODUCTION Mycophenolate Mofetil (Cellcept ) * is currently used first line as part of the triple immunosuppressant
Patient name Date of Birth DOCUMENT TO BE FILED IN NOTES AND SCANNED INTO ELECTRONIC RECORDS INTRODUCTION Mycophenolate Mofetil (Cellcept ) * is currently used first line as part of the triple immunosuppressant
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
Drug Class Prior Authorization Criteria Immune Globulins
 Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Narrow-band UVB PHOTOTHERAPY for Skin Diseases
 Narrow-band UVB PHOTOTHERAPY for Skin Diseases By Dr. Manal Bosseila Cairo University, Egypt HISTORICAL ASPECT In 1978: Irradiation cabin with broad band UVB tubes was introduced for psoriasis & uremic
Narrow-band UVB PHOTOTHERAPY for Skin Diseases By Dr. Manal Bosseila Cairo University, Egypt HISTORICAL ASPECT In 1978: Irradiation cabin with broad band UVB tubes was introduced for psoriasis & uremic
Primary Nephrotic Syndrome. Mao Jianhua, Department of Nephrology, The Children s Hospital of Zhejiang University School of Medicine
 Primary Nephrotic Syndrome Mao Jianhua, Department of Nephrology, The Children s Hospital of Zhejiang University School of Medicine Introduction Nephrotic syndrome is a group of symptoms including proteins
Primary Nephrotic Syndrome Mao Jianhua, Department of Nephrology, The Children s Hospital of Zhejiang University School of Medicine Introduction Nephrotic syndrome is a group of symptoms including proteins
AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE
 AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE Ron Feldman, MD, PhD Assistant Professor of Dermatology Emory University ron.j.feldman@emory.edu Disclosures I have no conflict of interest to
AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE Ron Feldman, MD, PhD Assistant Professor of Dermatology Emory University ron.j.feldman@emory.edu Disclosures I have no conflict of interest to
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE. Drug: AZATHIOPRINE Protocol number: CV 04
 Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: AZATHIOPRINE Protocol number: CV 04 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION LIVER
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: AZATHIOPRINE Protocol number: CV 04 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION LIVER
Proceedings of the Southern European Veterinary Conference - SEVC -
 Close this window to return to IVIS www.ivis.org Proceedings of the Southern European Veterinary Conference - SEVC - Sep. 30-Oct. 3, 2010, Barcelona, Spain Next SEVC Conference: Sep. 30-Oct. 2, 2011 -
Close this window to return to IVIS www.ivis.org Proceedings of the Southern European Veterinary Conference - SEVC - Sep. 30-Oct. 3, 2010, Barcelona, Spain Next SEVC Conference: Sep. 30-Oct. 2, 2011 -
1. Background: Infliximab is administered parenterally; therefore, it is not covered under retail pharmacy benefits.
 Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
PHARMACY POLICY STATEMENT Ohio Medicaid
 DRUG NAME BILLING CODE BENEFIT TYPE SITE OF SERVICE ALLOWED COVERAGE REQUIREMENTS LIST OF DIAGNOSES CONSIDERED NOT MEDICALLY NECESSARY PHARMACY POLICY STATEMENT Ohio Medicaid Enbrel (etanercept) Must use
DRUG NAME BILLING CODE BENEFIT TYPE SITE OF SERVICE ALLOWED COVERAGE REQUIREMENTS LIST OF DIAGNOSES CONSIDERED NOT MEDICALLY NECESSARY PHARMACY POLICY STATEMENT Ohio Medicaid Enbrel (etanercept) Must use
Management of Pyoderma Gangrenosum Mentoring in IBD XVII
 Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
Papular dermatitis: response to cyclosporin
 Journal of Dermatological Treatment (2000) 11, 253 257 2000 Journal of Dermatological Treatment. All rights reserved. ISSN 0954 6634 253 Papular dermatitis: response to cyclosporin E Alvarez, A Hendi,
Journal of Dermatological Treatment (2000) 11, 253 257 2000 Journal of Dermatological Treatment. All rights reserved. ISSN 0954 6634 253 Papular dermatitis: response to cyclosporin E Alvarez, A Hendi,
Humira. (adalimumab) Drug Update Slideshow NEW INDICATION
 Humira (adalimumab) NEW INDICATION Drug Update Slideshow Introduction Brand name: Humira Generic name: Adalimumab Pharmacological class: Tumor necrosis factor (TNF) blocker Strength and Formulation: 10mg/0.2mL,
Humira (adalimumab) NEW INDICATION Drug Update Slideshow Introduction Brand name: Humira Generic name: Adalimumab Pharmacological class: Tumor necrosis factor (TNF) blocker Strength and Formulation: 10mg/0.2mL,
Extracorporeal Photopheresis and Crohn s Disease. Jill Adamski MD, PhD Transfusion Medicine Department of Pathology
 Extracorporeal Photopheresis and Crohn s Disease Jill Adamski MD, PhD Transfusion Medicine Department of Pathology Outline 1. Crohn s Disease (CD) 2. Extracoporeal Photopheresis (ECP) 3. Pilot studies
Extracorporeal Photopheresis and Crohn s Disease Jill Adamski MD, PhD Transfusion Medicine Department of Pathology Outline 1. Crohn s Disease (CD) 2. Extracoporeal Photopheresis (ECP) 3. Pilot studies
0BCore Safety Profile. Pharmaceutical form(s)/strength: Cream 1% DK/H/PSUR/0009/005 Date of FAR:
 0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
Management of HBV in KidneyTransplanted Patients Dr.E.Nemati
 Management of HBV in KidneyTransplanted Patients Dr.E.Nemati Hepatitis B virus (HBV) infection Hepatitis B virus (HBV) infection confers a significantly negative impact on the clinical outcomes of kidney
Management of HBV in KidneyTransplanted Patients Dr.E.Nemati Hepatitis B virus (HBV) infection Hepatitis B virus (HBV) infection confers a significantly negative impact on the clinical outcomes of kidney
Combination Nonbiologic Therapy in Psoriasis. Sushil Tahiliani, MBBS, MD
 Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
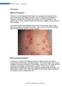 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
IMMUNOSUPPRESSIVE THERAPY: WHAT S NEW
 IMMUNOSUPPRESSIVE THERAPY: WHAT S NEW Dr. Andrew Mackin BVSc BVMS MVS DVSc FANZCVSc DipACVIM Professor of Small Animal Internal Medicine Mississippi State University College of Veterinary Medicine, Starkville,
IMMUNOSUPPRESSIVE THERAPY: WHAT S NEW Dr. Andrew Mackin BVSc BVMS MVS DVSc FANZCVSc DipACVIM Professor of Small Animal Internal Medicine Mississippi State University College of Veterinary Medicine, Starkville,
Contents. 3 Diagnostic Tests and Studies Introduction Examination... 27
 Contents 1 Normal Anatomy... 1 1.1 Introduction... 1 1.2 Surface Landmarks... 1 1.3 Oral Mucosa... 3 1.4 Tongue... 5 1.5 Floor of Mouth... 6 1.6 Palate... 6 1.7 Dentition... 7 1.8 Temporomandibular Joint...
Contents 1 Normal Anatomy... 1 1.1 Introduction... 1 1.2 Surface Landmarks... 1 1.3 Oral Mucosa... 3 1.4 Tongue... 5 1.5 Floor of Mouth... 6 1.6 Palate... 6 1.7 Dentition... 7 1.8 Temporomandibular Joint...
PUVATHERAPY tor PSORIASIS AND OTHER SKIN DISEASES
 PUVATHERAPY tor PSORIASIS AND OTHER SKIN DISEASES AN INITIAL REPORT by HILARY A. LAVERY and D. BURROWS Department of Dermatology, Royal Victoria Hospital, Belfast SUMMARY Fifty-two patients with severe
PUVATHERAPY tor PSORIASIS AND OTHER SKIN DISEASES AN INITIAL REPORT by HILARY A. LAVERY and D. BURROWS Department of Dermatology, Royal Victoria Hospital, Belfast SUMMARY Fifty-two patients with severe
INFLIXIMAB Remicade (infliximab), Inflectra (infliximab-dyyb), Renflexis (infliximab-abda)
 RATIONALE FOR INCLUSION IN PA PROGRAM Background Remicade, Renflexis and Inflectra are tumor necrosis factor (TNFα) blockers. Tumor necrosis factor is an endogenous protein that regulates a number of physiologic
RATIONALE FOR INCLUSION IN PA PROGRAM Background Remicade, Renflexis and Inflectra are tumor necrosis factor (TNFα) blockers. Tumor necrosis factor is an endogenous protein that regulates a number of physiologic
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Infliximab: A Treatment Option for Ulcerative Pyoderma Gangrenosum
 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/449955 Infliximab: A Treatment Option for Ulcerative Pyoderma Gangrenosum
To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/449955 Infliximab: A Treatment Option for Ulcerative Pyoderma Gangrenosum
Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial
 Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Pfizer Announces Modification To Ongoing Tofacitinib FDA Post- Marketing Requirement Study In Patients With Rheumatoid Arthritis
 February 19, 2019 Media Contact: Neha Wadhwa M: +1 212-733-2835 E: Neha.Wadhwa@pfizer.com Investor Contact: Charles Triano O: +1 212-733-3901 E: Charles.E.Triano@pfizer.com Pfizer Announces Modification
February 19, 2019 Media Contact: Neha Wadhwa M: +1 212-733-2835 E: Neha.Wadhwa@pfizer.com Investor Contact: Charles Triano O: +1 212-733-3901 E: Charles.E.Triano@pfizer.com Pfizer Announces Modification
Azathioprine in Dermatology
 Acta Dermatovenerol Croat 2007;15(4):264-268 REVIEW Azathioprine in Dermatology Ivana Bardek, Višnja Milavec-Puretić, Jasna Lipozenčić University Department of Dermatology and Venereology, Zagreb University
Acta Dermatovenerol Croat 2007;15(4):264-268 REVIEW Azathioprine in Dermatology Ivana Bardek, Višnja Milavec-Puretić, Jasna Lipozenčić University Department of Dermatology and Venereology, Zagreb University
TDM. Measurement techniques used to determine cyclosporine level include:
 TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
Appendix to Notification Letter for rituximab and eltrombopag dated 20 February 2014
 Appendix to Notification Letter for rituximab and eltrombopag dated 20 February 2014 The notification letter which contains details of the decision to widen the restriction criteria for rituximab and eltrombopag
Appendix to Notification Letter for rituximab and eltrombopag dated 20 February 2014 The notification letter which contains details of the decision to widen the restriction criteria for rituximab and eltrombopag
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Topical Immunomodulator Step Therapy Program
 Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
M0BCore Safety Profile
 M0BCore Safety Profile Active substance: Aciclovir Pharmaceutical form(s)/strength: Tablets 200, 400 or 800 mg Dispersible tablets 200, 400 or 800 mg Oral suspensions 200 mg or 400 mg per 5 ml. Freeze
M0BCore Safety Profile Active substance: Aciclovir Pharmaceutical form(s)/strength: Tablets 200, 400 or 800 mg Dispersible tablets 200, 400 or 800 mg Oral suspensions 200 mg or 400 mg per 5 ml. Freeze
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE. Drug: CICLOSPORIN Protocol number: CV 06
 Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: CICLOSPORIN Protocol number: CV 06 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: CICLOSPORIN Protocol number: CV 06 Indication: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS
Novel Therapies in Autoimmune Hepatitis
 Novel Therapies in Autoimmune Hepatitis Paul W. Rassam,MD Ass. Clinical Professor of Medicine Div. of Gastroenterology and Hepatology St George Hospital University Medical Center University of Balamand
Novel Therapies in Autoimmune Hepatitis Paul W. Rassam,MD Ass. Clinical Professor of Medicine Div. of Gastroenterology and Hepatology St George Hospital University Medical Center University of Balamand
The Benefits of Leflunomide
 Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
Name of Policy: Extracorporeal Photopheresis
 Name of Policy: Extracorporeal Photopheresis Policy #: 028 Latest Review Date: June 2014 Category: Therapy Policy Grade: A Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Extracorporeal Photopheresis Policy #: 028 Latest Review Date: June 2014 Category: Therapy Policy Grade: A Background/Definitions: As a general rule, benefits are payable under Blue Cross
Ciclosporin Microemulsion for Severe Atopic Dermatitis: Experience on Adolescents and Adults in Hong Kong
 ORIGINAL ARTICLES Ciclosporin Microemulsion for Severe Atopic Dermatitis: Experience on Adolescents and Adults in Hong Kong Drs. H. F. Ho, L.Y. Chong, K. M. Ho and W. K. Fung Social Hygiene Service (Dermatology),
ORIGINAL ARTICLES Ciclosporin Microemulsion for Severe Atopic Dermatitis: Experience on Adolescents and Adults in Hong Kong Drs. H. F. Ho, L.Y. Chong, K. M. Ho and W. K. Fung Social Hygiene Service (Dermatology),
Liver Transplant Immunosuppression
 Liver Transplant Immunosuppression Michael Daily, MD, MS, FACS Surgical Director, Kidney and Pancreas Transplantation University of Kentucky Medical Center Disclosures No financial disclosures I will be
Liver Transplant Immunosuppression Michael Daily, MD, MS, FACS Surgical Director, Kidney and Pancreas Transplantation University of Kentucky Medical Center Disclosures No financial disclosures I will be
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
GRANULOMATOSIS WITH POLYANGIITIS
 What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Rayos) Reference Number: CP.CPA.273 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Rayos) Reference Number: CP.CPA.273 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Revision Log See Important Reminder at the end of this policy for important
50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate).
 DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
Corticosteroids. Veterinary Pharmacology Endocrine System. University of Tehran Faculty of Veterinary Medicine Academic Year
 Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae
 H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE. Drug: TACROLIMUS Protocol number: CV 43
 Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: TACROLIMUS Protocol number: CV 43 Indications: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS.
Cardiff & Vale (C&V) UHB Corporate Medicines Management Group (c MMG) SHARED CARE Drug: TACROLIMUS Protocol number: CV 43 Indications: RENAL, PANCREAS OR COMBINED RENAL PANCREAS TRANSPLANTATION IN ADULTS.
