Prescribing Formulary. 7 th Edition April 2010
|
|
|
- Ruth Dixon
- 5 years ago
- Views:
Transcription
1 Prescribing Formulary 7 th Edition April 2010
2 Somerset Primary Care Trust - Primary Care Formulary 7 th Edition April 2010 Introduction This formulary has been developed and reviewed by the Somerset PCT Medicines Management team, in liaison with Secondary Care NHS Trusts. It is intended to guide evidence-based and cost-effective prescribing across Somerset. Key points to note with regard to the formulary are: It is intended to only cover first and in some cases second-line drug choices (other than where stated) in uncomplicated patients It is expected that practices will find the options provided are appropriate for the treatment of most new patients It is acknowledged that patients who are intolerant / unresponsive to formulary drugs, may require alternatives which are non-formulary It is anticipated that medication reviews will provide an opportunity to transfer appropriate patients from non-formulary to formulary drugs New products will by default be non-formulary initially and prescribers are thus asked to refrain from prescribing new drugs until they have been assessed and approved for addition to the formulary either by the Prescribing Forum or Drugs and Therapeutics Committee. Drugs which are classified as amber under the County Prescribing Group Traffic Lights Scheme are not generally included in the formulary, as they should be initiated by an appropriate specialist and only prescribed by GPs where there are arrangements for shared care The formulary is primarily aimed at prescribing for adults, guidance on prescribing for children can be found in the BNF for Children It is acknowledged that to be effective the formulary needs to be accessible and thus an electronic rather than paper format is preferred by many. To aid decision support at the point of prescribing, this formulary will therefore be made available on general practice clinical systems. It is expected that this formulary will then be set as the default for all users within practices, including partners, retained doctors, locums and non-medical prescribers. It is proposed to review the formulary at approximately six-monthly intervals, in light of emerging evidence, product availability and pricing. Prices quoted in this edition are taken from the April 2010 editions of the Drug Tariff and Chemist & Druggist monthly price list. By rationalising the choice of drugs prescribed in Primary Care through adoption of the formulary, and by improving liaison with Secondary Care, it is hoped that prescribing across the Somerset health community can become more rational, cost-effective and seamless. In further support of this objective, the Out of Hours formulary and Somerset Traffic Lights Scheme are reproduced as appendices to this document. Somerset PCT Medicines Management Team April 2010 We believe the information in this document is correct at the time of production. Please notify the Medicines Management Team of any errors. geoffrey.howard@somerset.nhs.uk Team Administrator Introduction Page 1
3 ADMISSION AND DISCHARGE PROCESSES Poor communication of information at transition points is responsible for as many as 50% of all medication errors and up to 20% of adverse drug events in hospital. Practices should have a process for medicines reconciliation before admission and after discharge from secondary care and a means of identifying patients at high risk of medicines related adverse events. NPC recommends a minimum dataset of information: From Primary to Secondary Care From Secondary to Primary care Complete patient details The presenting condition plus co-morbidities A list of all the medicines currently prescribed for the patient with indications Any OTC medicines or supplements the patient takes Dose, frequency and route of all the medicines listed An indication of any medicines that are not intended to be continued (eg.acute prescriptions) Known allergies Complete patient details The diagnosis of the presenting condition plus comorbidities Dose, frequency and route of all the medicines listed Medicines stopped and started, with reasons Length of courses where appropriate Details of increasing or decreasing regimes Known allergies Known previous side effects Suggestions for Drug Monitoring in Adults in Primary Care The monitoring parameters cited in the formulary are derived from a range of guideline and other reference sources and expert opinion and must therefore be considered suggestions only. Adherence to them will not ensure a successful outcome in every case. The ultimate judgement regarding a particular clinical result must be made by the doctor in light of the clinical data presented by the patient and the diagnostic and treatment options available. Admission and discharge processes Page 2
4 Contents BNF Therapeutic Chapter Page(s) Gastro-intestinal system 8 14 Helicobacter pylori eradication 10 Guidance on assessing dehydration in children under 5 years 11 Cardiovascular system Hypertension guidance Hypertension Guidance flowchart 23 Heart Failure Guidance Heart Failure prescribing Guidelines flowchart 28 Primary Care Guidelines for the Treatment of Chronic Stable Angina Pectoris 30 Management of anti-coagulant induced haemorrhage 33 Lipid-Regulation Guidance Primary Prevention in CVD (based on NICE CG 67) 36 Secondary Prevention of CVD (based on NICE CG 67) 37 Summary of drug-statin interations 38 Respiratory System COPD Guidance Top tips for COPD management 51 Table of contents Page 3
5 BNF Therapeutic Chapter Page(s) Central Nervous System Analgesia Opioid conversion table 63 Neuropathic pain Summary of NICE Guidance CG 96: Neuropathic pain 64 Migraine Drugs used in substance dependance Smoking Cessation Opioid dependence 71 Treatment of infection Influenza vaccines 76 Management of infection guidance Upper respiratory tract infections 77 Lower respiratory tract infections 78 Menigitis 78 Urinary tract infections 78 Gastro-intestinal tract infections 79 Genital tract infections 79 Skin / soft tissue infections 80 Methicillin Resistant Staphylococcus aureus (MRSA) decolonistation policy 81 Table of contents Page 4
6 BNF Therapeutic Chapter Page(s) Endocrine system Diabetes Summary chart for the treatment of diabetes 83 Insulin therapy in diabetes guidance 84 Blood glucose monitoring guidance 91 Thyroid and anti-thyroid drugs 92 Corticosteroids 92 Sex hormones Hormone replacement therapy Male sex hormones and antagonists 95 Drugs affecting bone metabolism Summary of NICE TAG 160: Primary Prevention of Osteoporosis 98 Summary of NICE TAG 161: Secondary Prevention of Osteoporosis 100 Gynaecology and urinary tract disorders Contraceptives Emergency hormonal contraception 105 Treatment of erectile dysfunction 108 Malginant disease and immunosuppression 109 Prostate cancer & Gonadorelin analogues 109 Somerset Prescribing Forum statement on endometriosis & fibroids 109 Table of contents Page 5
7 BNF Therapeutic Chapter Page(s) Nutrition and blood Musculo-skeletal and joint diseases Non-steroidal anti-inflammatory drugs (NSAIDs) 112 Rubefacients and topical NSAIDs 114 Gout 115 Guidance on the management of osteoarthritis (OA) Eye Ear, nose and oropharynx Nasal allergy Decolonisation of nasal MRSA 122 Skin Emollients Topical corticosteroids Acne Anti-infective skin preparations 130 Anaesthesia 131 Antagonists for central and respiratory depression 131 Borderline substances 132 Food supplements 132 Gluten-free foods 132 Table of contents Page 6
8 BNF Therapeutic Chapter Page(s) Appendices Appendix 1: Dorset & Somerset Out-of-hours Formulary Summary of supply of medicines in the OOH period 138 Urgent Care Service Formulary Somerset Community Pharmacies holding Palliative Care Drugs List of Palliative Care Drugs held by Community Pharmacies 157 Appendix 2: Somerset Traffic Lights System Guidance (June 2010 revision.) Intoduction Classification definitions 161 Alphabetical list of drugs with Traffic Light status Format of Shared Care agreements 227 Pro-forma for request of Traffic light status of drugs 229 Table of contents Page 7
9 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments BNF Chapter 1: Gastro-intestinal Detailed guidance on dyspepsia is provided by NICE: "Dyspepsia - management of dyspepsia in adults in primary care" (Aug'04) Antacids Magnesium trisilicate Suspension: 0.91 (200ml) Alginates Asilone Suspension: 1.95 (500ml) Peptac Aniseed and peppermint flavour Liquid: 1.95 (500ml) Gastrocote Suspension: 2.67 (500ml) Tablets: 3.51 (100) Inexpensive, but contains 3mmol Sodium per 5ml so should be avoided in patients where Sodium intake restriction is desirable. Available OTC A combination of Magnesium and Aluminium antacids, plus an antiflatulent, also low in Sodium. Available OTC Contains 3.1mmol of Sodium per 5ml so should be avoided in patients where restriction of Sodium intake is desirable. Available OTC Gastrocote liquid contains 1.8mmol of Sodium per 5ml and may therefore be more appropriate than Peptac in patients where restriction of Sodium intake is desirable. Gastrocote tablets contain 1mmol Sodium per tablet. Both suspension and tablets available OTC Gaviscon Advance is NOT due to its relatively high cost 5.21 per 500ml. H2RA and PPI are more cost effective choices. Antispasmodics Mebeverine 135mg: 7.08 (100) Avoid prescribing as Colofac IBS as this is the OTC pack and more expensive. H2- Receptor antagonists Ranitidine 150mg: 1.99 (60) 300mg: 2.23 (30) Ranitidine is as first line treatment for mildmoderate GORD in the majority of patients. Ranitidine is available OTC, but only as 75mg tablets Gastro-intestinal System Page 8
10 Therapeutic Area Formulary Choices Cost for 28 unless stated Proton Pump Inhibitors First line NB. Refer to NICE guidance on use of PPIs Lansoprazole capsules 15mg: mg: 2.78 Omeprazole capsules 10mg: mg: 2.04 Second line Pantoprazole tablets 20mg: mg: 4.34 Rationale for decision / comments Based on licensed indications and availability of both as generics omeprazole and lansoprazole are now considered joint first line PPIs and the need to use other PPIs should therefore be limited. Avoid prescribing Lansoprazole orodispersible tablets (Zoton FasTabs) as the cost is greater than generic capsules, except as an alternative to costly special liquid formulations. Avoid prescribing Omeprazole dispersible tablets (Losec MUPS ), as they cost about five times more than generic capsules, except as an alternative to costly special liquid formulations and where lansoprazole orodispersible tablets are not an acceptable alternative. Where Omeprazole 20mg once-daily is not effective, increasing dose to 2x20mg daily (not 1x40mg) or using Lansoprazole 30mg daily is. Included second line for circumstances where tablet formulation is essential. Gastro-intestinal System Page 9
11 Therapeutic Area Formulary Choices Cost for 28 unless stated HP Eradication First line: or Second line: Acute diarrhoea PPI (as opposite) + Metronidazole + Clarithromycin all for 7 days PPI (as opposite) + Amoxicillin + Clarithromycin all for 7 days See opposite or seek specialist advice 400mg BD 250mg BD 1g BD 500mg BD Rationale for decision / comments Helicobacter pylori eradication is indicated in GU, DU and MALT lymphoma, whereas evidence of value in GORD and NUD is inconsistent. Recommended PPI regimes for H. pylori eradication are either Omeprazole capsules 20mg bd or Lansoprazole capsules 30mg bd. The combination of a PPI + Clarithromycin and Metronidazole is now a as first line therapy for H. pylori eradication. However the use of Clarithromycin or Metronidazole should be avoided if they have been used in the previous year for the treatment of any other infections as this significantly increases the likelihood of H Pylori being resistant. NB. Different doses of Clarithromycin indicated in the two regimes. Where patients require a second course of eradication, a regime should be chosen which does not include antibiotics given previously, see BNF for guidance or seek specialist advice. Avoid anti-motility agents in children. See page 11 for assessment of dehydration in under 5s NICE CG84 Oral rehydration Electrolade 1.33 (6 sachet) 4.99 (20 sachet) Available as multipack containing mixed flavours, less expensive than Dioralyte. Available OTC. Antimotility agents Loperamide capsules 2mg: 1.23 (30) Available OTC as generic loperamide, various own-brand products and as Imodium. Codeine 15mg: mg tablets: 1.51 Just 3 days of codeine containing medicines can lead to addiction The PCT strongly recommends that prescribers discuss the risk of addiction when initiating new patients on any opioid containing medication and that this discussion is recorded in the patient notes. Watch for increasing frequency of requests for prescriptions Gastro-intestinal System Page 10
12 Signs (face-to-face assessments) Symptoms (remote and face-to-face assessments) Assessing dehydration in children under 5 years for use during remote and face-to-face assessments Adapted from Diarrhoea and vomiting in children (NICE clinical guideline 84). The quick reference guide and full guidance are available from: No clinically detectable dehydration Appears well Alert and responsive Increasing severity of dehydration Clinical dehydration may indicate children at increased risk of progression to shock Appears to be unwell or deteriorating Altered responsiveness (for example, irritable, lethargic) Normal urine output Decreased urine output Clinical shock (one or more signs/symptoms present. (-) features do not specifically indicate shock Decreased level of consciousness Skin colour unchanged Skin colour unchanged Pale or mottled skin Warm extremities Warm extremities Cold extremities Alert and responsive Altered responsiveness (for example, irritable, lethargic) Decreased level of consciousness Skin colour unchanged Skin colour unchanged Pale or mottled skin Warm extremities Warm extremities Cold extremities Eyes not sunken Sunken eyes Moist mucous membranes (except after a drink) Dry mucous membranes (except for mouth breather') Normal heart rate Tachycardia Tachycardia Normal breathing pattern Tachypnoea Tachypnoea Normal peripheral pulses Normal peripheral pulses Weak peripheral pulses Normal capillary refill time Normal capillary refill time Prolonged capillary refill time Normal skin turgor Reduced skin turgor Normal blood pressure Normal blood pressure Hypotension (decompensated shock) Risk Factors for Dehydration: Children younger than 1 year, especially those younger than 6 months infants who were of low birth weight children who have passed six or more diarrhoeal stools in the past 24 hours children who have vomited three times or more in the past 24 hours children who have not been offered or have not been able to tolerate supplementary fluids before presentation infants who have stopped breastfeeding during the illness children with signs of malnutrition. X Box 1 x Suspect hypernatraemic dehydration if there are any of the following: jittery movements increased muscle tone hyperreflexia convulsions drowsiness or coma. Laboratory investigations: Do not routinely perform blood biochemistry. Measure plasma sodium, potassium, urea, creatinine and glucose concentrations if: intravenous fluid therapy is required or there are symptoms or signs suggesting hypernatraemia. Measure venous blood acid base status and chloride concentration if shock is suspected or confirmed. Interpret symptoms and signs taking into account risk factors for dehydration (see box 1). Page 11
13 Therapeutic Area Formulary Choices Cost for 28 unless stated Chronic diarrhoea First line: or Second line: Mesalazine as Mesren Mesalazine as Pentasa Mesalazine as Mezavant 400mg tablets: (90) 500mg tablets (100) 1200mg tablets: (60) Bulk-forming laxatives Ispaghula Husk Generic 3.5g sachets: 2.12 (30) Stimulant laxatives Senna 7.5mg tablets: 2.77 (60) 7.5mg/5ml SF liquid: 2.69 (500ml) Glycerin suppositories 1g: 1.02 (12) 2g: 1.02 (12) 4g: 1.69 (12) Rationale for decision / comments In line with national guidance it is that Mesalazine is prescribed by brand name. Where 400mg tablets are required Mesren tablets are as first line as they are considered to be bioequivalent to the original product Asacol but at a lower cost. For all mesalazine preparations monitor renal function as in SPC. Where 500mg tablets are required Pentasa tablets are. Asacol 800mg tablets are not because of three times daily dose regime Consultant initiation only. All patients to have evaluation of renal function prior to initiation and at least twice yearly whilst on treatment. Available OTC. 3.4g sachets (e.g. Regulan ) are more expensive at 2.44 per 30 Available OTC. Glycerin suppository sizes: 1g = infant 2g = child 4g = adult All available OTC Gastro-intestinal System Page 12
14 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments Osmotic laxatives Pre-op Bowel Cleansing Solutions Peripheral opioidreceptor antagonist Lactulose 3.35g/5ml solution Macrogol as Laxido Orange or Laxido Natural N/A Methylnaltrexone Injection 12mg/0.6ml 3.15 (500ml) Takes 2 to 3 days to exert effect, prn use ineffective; should be taken with additional fluid. Therapeutic dose for adults 15ml twice daily. Available OTC. For the treatment of constipation in people with IBS laxatives should be considered (but not lactulose). NICE CG 61 Sachets: 5.34 (30) (pack 1) (pack 7) Rectal soothing agents Anusol Cream: 2.02 (23g) Ointment: 2.02 (25g) Suppositories: 1.90 (12) Course of treatment for chronic constipation not normally > 2 weeks. May be repeated if necessary. For extended use, see summary of product characteristics. Efficacy requires adequate fluid intake. Contains Na +, care in patients with hypertension / heart failure. Laxido replaces Movicol as lower cost brand equivalent. Bowel cleansing medicine may modify the absorption of regularly prescribed medications. Urea and Electrolytes shou;d be checked in all patients to minimise the risk of electrolyte imbalance particularly patients taking the following medications: Diuretics, corticosteroids, cardiac glycosides, NSAIDs, tricyclics, SSRIa, antipsychotics, carbamazepine. See NPSA Alert and local guidelines for details. Opioid-induced constipation in terminally ill patients, when response to other laxatives is inadequate..used in addition to existing laxative therapy. Not licensed for use in any other circumstance. Available as cream, ointment and suppositories. Available OTC. Gastro-intestinal System Page 13
15 Therapeutic Area Formulary Choices Cost for 28 unless stated Rectal corticosteroids Scheriproct Ointment: 3.00 (30g) Suppositories: 1.41 (12) Preparations for Anal Fissure Rectogesic (Glyceryl Trinitrate Ointment 0.4%) Ointment: (30g) Rationale for decision / comments Scheriproct is over the traditionally widely used Proctosedyl, as the latter is one of the most costly preparations of its type at per tube. Glyceryl Trinitrate for the management of anal fissure should be prescribed as Rectogesic, which is the only available licensed product for this indication. Prescriptions for other strengths will require the dispensing of specials which are unlicensed, often have a short shelf life and usually cost in excess of 100 per pack. Maximum duration of use: 8 weeks All external preparations of diltiazem unlicensed specials and are non-formulary. Gastro-intestinal System Page 14
16 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments BNF Chapter 2: Cardiovascular System Given the wide overlap between many drug groups and clinical indications and vice-versa, the indications for which each drug is included in the formulary are clearly stated in the comments section. Recommendations and local guidelines for the management of specified cardiovascular conditions are provided as inserts. Hypertension page Hypertension Guidance flowchart page 23 Heart Failure page Primary Care Guidelines for the Treatment of Chronic Stable Angina Pectoris page 30 Management of anticoagulant induce haemorrhage page 33 DH statement on cholesterol targets page 36 Primary Prevention of CVD guidance page 36 Secondary Prevention of CVD guidance page 37 Drug statin interactions table page Positive Inotropic Drugs Cardiac Glycosides Digoxin 62.5mcg: mcg: mcg: 1.30 Digoxin is included in the formulary for use: Atrial Fibrillation: but not paroxysmal AF Heart Failure: where patients condition is worsening or severe (due to LVSD) despite ACEIs, B-Blockers and diuretics. Monitoring requirements are for U&Es 12 monthly. Digoxin levels are only required if toxicity is suspected or during dose adjustments. Cardiovascular system Page 15
17 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments 2.3 Anti-arrhythmic drugs Drugs for arrythmias Amiodarone 100mg: mg: 2.86 Treatment should only be initiated by hospital specialist and only for the treatment of severe rhythm disorders not responding to other therapies. Prescribing at initial loading dose should be limited to 2 weeks. Amiodarone therapy requires monitoring of: LFTs and TFTs at baseline and then every 6 months. Ophthalmic examination at baseline and then twelvemonthly The long half-life of Amiodarone means the therapeutic and adverse effects persist for long periods after discontinuation of therapy WARNING Do not exceed Simvastatin 20mg in patients taking Amiodarone and monitor lipid levels to ensure lowest dose necessary of atorvastatin is used. 2.2 Diuretics Thiazides and related diuretics Bendroflumethiazide 2.5mg tablets: 0.91 Bendroflumethiazide is included in the formulary for: Hypertension. in line with NICE guidance. Bendroflumethiazide 2.5mg daily is considered the optimal dose for hypertension, higher doses offer little or no additional antihypertensive effect but cause more hyponatraemia and hypokalaemia, and have effects on glucose tolerance, lipid and uric acid metabolism Heart failure: Bendroflumethiazide may have a limited role in mild heart failure or where patients are intolerant of loop diuretics. Cardiovascular system Page 16
18 Therapeutic Area Formulary Choices Cost for 28 unless stated Loop Diuretics Furosemide 20mg tablets: mg tablets: 0.95 Aldosterone Antagonists Spironolactone 25mg tablets: mg tablets: 2.33 Rationale for decision / comments Furosemide is included in the formulary for use Heart Failure: to provide relief of symptoms Hypertension: Whilst the antihypertensive effects of Furosemide are not as pronounced as those of Bendroflumethiazide, it may have a role in the management of hypertension, where there is intolerance or a C/I to standard therapies, or where BP remains suboptimally controlled despite standard therapies. Spironolactone is included in the formulary for : Heart failure: for patients with NHYA Grade III-IV who remain symptomatic despite optimisation of therapies such as ACE inhibitors and Beta-blockers. Spironolactone is the aldosterone antagonist of choice in this situation; Eplenerone is considered an alternative only for specialist initiation. Hypertension: where there is intolerance or a C/I to standard therapies, or where BP remains sub-optimally controlled despite standard therapies. Regular monitoring (maintenance): U&E at 6, 9 & 12 months, thereafter every 6 months. Cardiovascular system Page 17
19 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments 2.4 Beta-adrenoreceptor antagonist drugs NB. Evidence suggests the combination of Beta-blocker and Thiazide increases risk of Type 2 DM and this is generally considered to be dose related. Recent evidence-based guidance for angina states that beta-blockers should be the first line therapy for the long-term prevention of angina. Beta-blockers are no longer preferred as routine therapy for hypertension Beta-blockers Atenolol 25mg: mg: mg: 1.01 Bisoprolol 1.25mg: mg: mg: mg: mg: mg: 1.33 Metoprolol 50mg: mg: 1.69 Atenolol is included in the formulary for: Hypertension: in line with NICE guidance. Atenolol dose for hypertension should not normally exceed 50mg daily. Angina: for prophylaxis of symptoms, some additional benefit may be obtained by increasing the dose to 100mg. Bisoprolol is included in the formulary for: Heart failure: Where a beta-blocker is indicated for heart failure, Bisoprolol is first line drug, initiated at 1.25mg and titrated according to guidelines. Hypertension: in line with NICE guidance. Alternative to Atenolol or Metoprolol Angina: as alternative to Metoprolol Post-MI: as alternative to Metoprolol Metoprolol is included in the formulary for: Hypertension: in line with NICE guidance. Alternative to Atenolol or Bisoprolol Angina: as alternative to Bisoprolol Post-MI: as alternative to Bisoprolol Cardiovascular system Page 18
20 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments 2.5 Renin-Angiotensin System Drugs and other antihypertensives ACE inhibitors ACE Inhibitors (ACEIs) should be used in line with NICE / PCT guidance for hypertension and heart failure. All should be prescribed in a single daily dose where possible. Lisinopril and Ramipril are the first line options. Monitoring requirements U+Es at baseline, repeated 1-2 weeks after each dose increase for heart failure and after final dose increase in hypertension, annually thereafter. Patients exhibiting ACE cough on first choice ACE should trial a second choice ACE before an ARB. Lisinopril 2.5mg: mg: mg: mg: 1.39 or Ramipril capsules 1.25mg: mg: mg: mg: 1.59 Enalapril 2.5mg; mg: mg: mg: 1.39 Lisinopril is included in the formulary for: Hypertension: in line with NICE guidance. Usual dose range 2.5mg -20mg daily. May be commenced at dose of 10mg daily in patients without renal impairment and not on diuretics. Post-MI: titrated to 5-10mg daily if possible Heart failure: as guidelines, titrated to 35mg if possible Diabetic nephropathy: initially 2.5mg once daily, adjusted to achieve sitting diastolic BP of < 75mmHg in normotensive IDDM and < 90mm Hg in hypertensive NIDDM, usual range 10-20mg once daily Ramipril is included in the formulary for: Hypertension: in line with NICE guidance. Dose range 1.25mg to 10mg daily Post-MI: titrated to 10mg daily if possible Heart failure: as guidelines, titrated to 10mg if possible Enalapril is only included in the formulary for existing stabilised patients Cardiovascular system Page 19
21 Therapeutic Area Formulary Choices Cost for 28 unless stated Angiotensin Receptor Blocker (ARBs) Rationale for decision / comments ARBs should only be used in patients with persistent troublesome ACEI induced cough (between 2% - 10% patients MeReC Mar 10 20, 2). ACEIs have a better evidence base and are more costeffective. ARBs should be used in line with NICE / PCT guidance for hypertension and heart failure. Patients exhibiting ACE cough on first choice ACE should trial a second choice ACE before an ARB. Dual therapy ACE+ARB is not. First line: Candesartan 2mg: 3.39 (7) 4mg: mg: mg: mg: Second line: Losartan 25mg: Following consideration of available evidence at Somerset Prescribing Forum March 2010 it was agreed that generic versions of losartan may be used for all indications 50mg: mg: Third line: Valsartan 40mg: 4.11 (7) 80mg: mg: Candesartan is included in the formulary for: Hypertension: (where intolerant to ACEI) in line with NICE guidance, dose range 2-16mg daily Heart failure: (where intolerant to ACEI) as per guidelines, titrated to 32mg daily if possible. Losartan is included in the formulary for: Hypertension: (where intolerant to ACEI and to Candesartan) in line with NICE guidance, dose range mg once daily Renal protection in Type 2 DM with Nephropathy: (where intolerant to ACEI) initially 50mg daily, increased after one month to 100mg daily according to blood pressure Chronic heart failure (>60 yrs; ACE intolerant; LVEF <40% & clinically stable). Patients with heart failure who have been stabilised with an ACE inhibitor should not be switched to losartan. Initially 12.5mg, titrated at weekly intervals to usual maintenance dose of 50mg, as tolerated by patient. Valsartan is only included in the formulary for: Post-MI: (where intolerant to ACEI) initially 20mg bd, titrated to 160mg bd where tolerated Not included for hypertension Cardiovascular system Page 20
22 Therapeutic Area Formulary Choices Cost for 28 unless stated Centrally acting antihypertensive drugs Methyldopa 125mg: (56) 250mg: 6.83 (56) 500mg: (56) Moxonidine 200mcg: mcg: mcg: 6.30 Alpha-blockers Doxazosin 1mg: mg: mg: 1.72 as Doxadura brand 1mg: mg: mg: 1.47 Rationale for decision / comments Methyldopa is included in the formulary for: Hypertension in pregnancy Moxonidine is included in the formulary for: Hypertension: as an add-on option if BP cannot be controlled on routine antihypertensive drugs Doxazosin is included in the formulary for: Hypertension: Note that Doxazosin should not be used as a first line antihypertensive. The ALLHAT trial showed doxazosin monotherapy resulted in an 80% increase in heart failure and 26% increase in stroke compared to low dose diuretic therapy. Alpha-blockers may however be a useful as an add-on option if BP cannot be controlled on other drugs and in patients with co-existing BPH. Benign prostatic hyperplasia: See section 7 NB. Doxazosin MR (Cardura XL ) tablets are specifically not for maintenance in hypertension and maximum licensed dose for other indications is 8mg. Stabilised hypertensive patients on Doxazosin MR tablets should be switched to standard 4mg tablets: Doxazosin MR 4mg one daily > Doxazosin 4mg one daily Doxazosin MR 8mg one daily > Doxazosin 4mg two daily Cardiovascular system Page 21
23 Hypertension If patient has Diabetes or CVD follow specific relevant NICE Clinical Guideline NHS Somerset recommends practices follow the revised joint NICE/BHS guidance on management of hypertension. NB: All usual contra-indications apply - see BNF / SmPC for details. Key points of the new NICE guidance are as follows: Step 1: > 55 years or African/Caribbean patients of any age Thiazide-type diuretic (e.g. Bendroflumethiazide 2.5mg) or calcium channel blocker (e.g Amlodipine) < 55 years ACE Inhibitor (e.g. Ramipril or Lisinopril ) Step 2: Add second drug ACE + Calcium Channel Blocker or ACE + Thiazide type diuretic ( if intolerant to ACE ~5 % an ARB can be used (e.g. Candesartan) Step 3: Add third drug to make the combination ACE + Calcium channel blocker + Thiazide-type Diuretic NB. Only dihydropyridine CCBs should be combined with a beta-blocker (i.e. not Diltiazem or Verapamil) Step 4: Add fourth drug or Further diuretic therapy or Alpha blocker (plain doxazosin) Beta-blocker Consider seeking specialist advice Beta-blockers should not usually be withdrawn if a patient has a compelling indication for being treated with one eg symptomatic angina or previous MI. Cardiovascular system Page 22
24 No HYPERTENSION GUIDANCE FLOWCHART No Clinical consultation No Review within 5 years clinic BP raised? 3. Yes Diabetes? No Previous CHD? Offer lifestyle advice 4. Measure BP on two further occasions 5. Hypertension? 6. Yes Offer a formal CV Risk assessment 7. Secondary hypertension 8. No Criterion for drug therapy? 9 No Yes Yes Review within 1 year 12. Offer care according to national guidance 1. Offer care according to national guidance 2. Yes Offer to begin or step up drug therapy 10. Yes Specialist referral BP criterion met 11. Yes Review within 1 year 13. No 1. See the NICE clinical guideline 66 Management of type 2 diabetes 2. See the NICE clinical guideline 48 MI: Secondary Prevention. 3. Raised blood pressure (BP) > 140/90 mmhg (BP > 140/90 means either or both systolic and diastolic exceed threshold). Take a second confirmatory reading at the end of the consultation. Take a standing reading in patients with symptoms of postural hypotension. 4. Explain the potential consequences of raised BP. Promote healthy diet regular exercise and smoking cessation. 5. Ask the patient to return for at least two subsequent clinics at monthly intervals, assessing BP under the best conditions available. 6. Hypertension: persistent raised BP > 140/90 mmhg at the last two visits. 7. Cardiovascular (CV) risk assessment may identify other modifiable risk factors and help explain the value of BP lowering and other treatment Risk charts and calculators are less valid in patients with cardiovascular disease (CVD) or on treatment. 8. Refer patients with signs and symptoms of secondary hypertension to a specialist. Refer patients with malignant hypertension or suspected phaeochromocytoma for immediate investigation. 9. Offer treatment for: (A) BP >160/100 mmhg; or (B) BP >140/90 mmhg and 10- year risk of CVD >20% or existing target organ damage. Consider other treatments for raised cardiovascular risk including lipid lowering and antiplatelet therapies. 10. As needed, add drugs in the order shown on p BP <140/90 mmhg or further treatment is inappropriate or declined. 12. Check BP, reassess CV risk and discuss lifestyle. 13. Review patient care: medication, symptoms and lifestyle. Cardiovascular system Page 23
25 Prescribing Guidelines for HEART FAILURE This guidance is not intended to replace the full NICE guidance on Chronic Heart Failure (October 2003), but provides primary care prescribers with a summary of key points relevant in practice. AIMS To relieve symptoms To improve exercise tolerance To reduce incidence of acute exacerbations To reduce hospitalisations To reduce mortality Angiotensin Converting Enzyme (ACE) Inhibitors Evidence shows that an ACE Inhibitor given at an adequate dose generally achieves these aims; therefore an ACE inhibitor is for ALL patients with asymptomatic left ventricular dysfunction or symptomatic heart failure (unless contra- indicated). ACE inhibitor treatment should be titrated up to the highest licensed dose which is tolerated where possible. Start with a low dose, double dose at not less than 2 weeks. GPs considering initiating ACE inhibitor therapy should consider specialist supervision and/or particularly careful monitoring for those: receiving multiple or high dose diuretics (Furosemide 80mg or equivalent) with hypovolaemic with hyponatraemia (<130mmol/l) with pre-existing hypotension (systolic < 90mm Hg) with unstable heart failure with renal impairment (creatinine > 150mmol/l) receiving high-dose vasoldilator therapy aged 70 years or more NB: A small dose of an ACE inhibitor is better than no ACE at all. Because of the risk of hypotension, especially in patients with hypovolaemia, consideration should be given to withholding or reducing the dose of diuretics for 24 hours prior to commencement of the ACE inhibitor. Cardiovascular system Page 24
26 PCT Formulary ACE inhibitors: LISINOPRIL initially 2.5-5mg od, titrated to 30-35mg od or RAMIPRIL initially 2.5mg od, titrated to 10mg od Where possible all these ACE inhibitors should be used in a single daily dose to aid compliance and cost-effectiveness. Angiotensin Receptor Blockers (ARBs) The weight of evidence supporting use of ARBs in heart failure is not as robust as it is for use of ACE inhibitors and therefore an ARB can only be for those patients who are intolerant of ACE inhibitor therapy due to intractable cough. On the basis of the currently available evidence, Candesartan and losartan are the only ARBs licensed for use in heart failure. PCT Formulary ARB: CANDESARTAN The triple combination of Valsartan, ACE inhibitor and beta-blocker should be avoided, based on current evidence. As with ACE inhibitors it is to exert particular care when using ARBs in the patient groups who are at greater risk of problems and consideration given to specialist input where appropriate. Dual Therapy: In heart failure, dual RAS blockade was associated with more hypotension, worsening renal function and hyperkalaemia than ACE therapy alone. Not. Diuretics A diuretic is usually required by most patients with heart failure to reduce symptoms of fluid overload, reduce hospitalisation due to acute exacerbation and increase exercise tolerance. In most patients this will be a loop diuretic: PCT Formulary loop diuretic: FUROSEMIDE 20mg each morning, titrated according to symptomatic response A thiazide diuretic may be of benefit in patients with mild heart failure and good renal function; however thiazides are ineffective in patients with poor renal function. PCT Formulary thiazide diuretic: BENDROFLUMETHIAZIDE 2.5mg each morning If diuresis with one diuretic is insufficient, a combination of loop diuretic and thiazide may be tried. Cardiovascular system Page 25
27 Metolazone may provide useful additional efficacy, but the risk of profound diuresis and electrolyte disturbance, requires use with great caution and frequent monitoring. Where used, it is to commence at very low dose e.g. 2.5mg daily. Spironolactone For patients with moderate to severe heart failure who are already receiving an ACE Inhibitor, a diuretic and in some cases a beta-blocker; low dose spironolactone has been shown to reduce both symptoms and mortality. PCT formulary recommendation: SPIRONOLACTONE initially 25mg each morning, reducing to 12.5mg daily or 25mg alternate days if necessary Although the doses of Spironolactone for use in heart failure are much lower than those used for ascites, there is still a significant risk of electrolyte disturbance. Close monitoring of serum creatinine and potassium is required, for example, baseline, 2 and 4 weeks after commencement and monthly thereafter. Beta-blockers All patients with any grade of stable heart failure should be prescribed a beta-blocker for life-long treatment if tolerated and not contra indicated. Beta-blocker therapy should be initiated by those experienced in the management of heart failure and should commence at a very low dose and titrated up by doubling doses at intervals of not less than two weeks. Symptoms may deteriorate initially, calling for adjustment of concomitant therapy, such as temporary increase in dose of diuretics. Bisoprolol is the PCT formulary beta-blocker for heart failure, based on the CIBIS trials, once a day dosing and costeffectiveness. PCT Formulary beta-blocker for heart failure: BISOPROLOL initially 1.25mg once daily, titrated according to response and tolerability to 10mg once daily Where an alternative to Bisoprolol is required, for example where there is intolerance or concern that unopposed beta-blockade may be undesirable; Carvedilol should be considered as the appropriate alternative beta-blocker for heart-failure patients. There is also a stronger evidence base for Carvedilol in those patients with higher grades of heart failure and its use may be preferred in this situation. Prescribers should be aware that Carvedilol requires twice-daily dosing and the implications of this for compliance with therapy should be taken into account when selecting a beta-blocker for heart failure. Although doses of beta-blockers should be titrated to the maximum tolerated, a small dose of a beta-blocker is better than no beta-blocker at all. For those patients with well controlled hypertension or angina, already prescribed an alternative beta-blocker which is not licensed for heart failure (e.g. Atenolol) who then go on to develop heart failure should not automatically have their beta-blocker changed. However, if symptoms worsen despite concurrent ACE inhibitor and diuretic therapy consideration should be given to switching the beta-blocker to one which is licensed, as above. Cardiovascular system Page 26
28 Digoxin Digoxin is appropriate for patients with atrial fibrillation and any degree of heart failure. It is also for those with worsening or severe heart-failure due to LV systolic dysfunction who remain symptomatic despite treatment with an ACE Inhibitor, a diuretic and a beta blocker. Digoxin may improve symptoms, exercise tolerance and reduce hospitalisations. Digoxin has not been shown to reduce mortality. Hypokalaemia predisposes to Digoxin toxicity so careful monitoring of U&Es is required, especially where patients are also prescribed loop or thiazide diuretics, especially if an ACE inhibitor, ARB or Spironolactone is not prescribed. PCT formulary recommendation: Calcium channel blockers DIGOXIN 62.5mcg mcg once daily - higher doses are rarely appropriate in heart failure which is not associated with AF. No Calcium Channel Blocker is licensed for the treatment of heart failure. The use of calcium channel blockers with a direct effect on cardiac contractility i.e. Verapamil or Diltiazem should be specifically avoided in heart failure. For those patients who develop heart failure whilst prescribed a long-acting dihydropyridine calcium channel blocker e.g. Nifedipine MR (Coracten), Felodipine MR (Felotens), Lercanidipine or Amlodipine (Amlostin) for hypertension or angina, it may be appropriate to re-assess the risks and benefits of continuing with such therapy. In this situation, Amlodipine is supported by evidence that it does not worsen heart failure, similar evidence does not currently exist for other dihydropyridines. Where continuation of a dihydropyridine calcium channel blocker is considered essential for control of hypertension or angina, this may be justified where use of other therapies such as beta-blocker, ACE inhibitor and diuretic has been optimised. Cardiovascular system Page 27
29 Cardiovascular system Page 28
30 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments 2.6 Nitrates, Calcium Channel Blockers and Potassium Channel Activators Nitrates ISMN First line: ISMN second line: Glyceryl Trinitrate (GTN) spray Isosorbide Mononitrate Standard tablets Sustained-release tablets 40mg MR as Isotard XL 60mg MR as Tardisc XL 400mcg spray 200 dose: 2.63 (180 dose) as brand Nitromin 10mg: 1.18 (56) 20mg: 1.18 (56) 40mg: 1.65 (56) 40mg: mg: 3.50 Glyceryl trinitrate is included in the formulary for: Angina: for as required use for relief of symptoms Note that GTN tablets are now significantly more costly than spray Isosorbide Mononitrate is included in the formulary for: Angina: for prophylaxis of symptoms as monotherapy where intolerance or C/I to use of a beta-blocker or rate-limiting CCB. As combination therapy with beta-blocker or CCB where monotherapy provides insufficient control. First line is to prescribe standard Isosorbide mononitrate tablets asymmetrically to ensure a nitrate free period is maintained to reduce nitrate tolerance e.g. 20mg bd at 6-8am and 2-4pm. If patients cannot comply with this regime, MR preparations should be prescribed as the brand Isotard XL for 40mg and Tardisc XL for 60mg and only given once-daily to reduce nitrate tolerance. Where Isosorbide mononitrate has been added to provide symptom control pending angioplasty or CABG, consideration should be given to cautious withdrawal after successful completion of and recovery from the procedure ISOSORBIDE DINITRATE is NON-FORMULARY Except where initiated by a specialist for left ventricular failure Cardiovascular system Page 29
31 C o n s i d e r f o r R e v a s c u l a r i z a t i o n C o n s i d e r f o r R e v a s c u l a r i z a t i o n Primary Care Guidelines for the Treatment of Chronic Stable Angina Pectoris Intermediate short-term relief Short-acting sublingual spray or buccal nitrate prn Stable angina for medical management Disp Aspirin 75mg od (+/- PPI) Contraindication (e.g. proven allergy to aspirin) Clopidogrel 75mg od (stop PPI) Statin Simvastatin 40mg. Target cholesterol as per any co-morbidity (eg diabetes) and relevant NICE guidance ACE (Ramipril or Lisinopril) in proven CVD Intolerant or interaction - reduce to lower dose simvastatin if NICE target achievable Or change statin to Pravastatin 40mg or Atorvastatin. If further intolerance then Rosuvastain or (due to lack of evidence final option is Ezetimibe Treatment aimed at relief of symptoms Beta-blocker post-mi Beta-blocker (bisoprolol) no prior MI Symptoms not controlled Add calcium antagonist (amlodipine) Symptoms not controlled Intolerant (e.g. fatigue) or contraindication Intolerant Consider initiating Diltiazem (Slozem) or Verapamil (stop beta blocker) consider reduce dose of statin Add Calcium antagonist (Amlodipine) Symptoms not controlled Add long acting nitrate (Isotard XL) Symptoms not controlled Add long acting nitrate (Isotard XL) Intolerant Add Nicorandil Symptoms not controlled Symptoms not controlled Add Nicorandil Symptoms not controlled Stop Nicorandil add Ranolazine (at reduced dose if Rx Diltiazem or Verapamil) may need to reduce simvastatin dose Stop Nicorandil and Ivabradine add Ranolazine may need to reduce simvastatin dose Add Ivabradine Symptoms not controlled Cardiovascular system Page 30
32 Therapeutic Area Formulary Choices Cost for 28 unless stated Calcium channel blockers - Dihydropyridines First line: Amlodipine 5mg: mg: 1.43 as Amlostin brand 5mg: mg: 1.13 Second line: Felodipine MR 2.5mg: mg: mg: 5.66 as Felotens brand 5mg: mg: 5.10 Rationale for decision / comments NB. Avoid short-acting dihydropyridines in BP and CHD. Amlodipine is now first line, with Felodipine MR as a second line option for: Hypertension: in line with NICE guidance Angina: as monotherapy where intolerance or C/I to use of a beta-blocker or rate-limiting CCB. As combination therapy with beta-blocker where monotherapy provides insufficient control. NB: When prescribing Amlodipine generically, this should be as plain Amlodipine. Prescriptions for Amlodipine besilate will result in the supply of Istin and incur significantly greater costs. Cardiovascular system Page 31
33 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments Calcium channel blockers rate limiting Potassium Channel Activators Diltiazem MR as Slozem 120mg: mg: mg: mg: 8.50 Verapamil 40mg: 1.70 (84) 80mg: 2.07 (84) and Verapamil MR as Half Securon SR or Securon SR 120mg SR: mg SR: 5.66 Nicorandil 10mg: 7.71 (60) 20mg: (60) Diltiazem MR (as Slozem ) is included in the formulary for: Angina: as monotherapy where intolerance or C/I to use of a beta-blocker. In combination with a beta-blocker where monotherapy provides insufficient control. - NB. caution required due to risk of bradycardia and heart-block. Hypertension: in line with NICE guidance NB. Prescribing Diltiazem MR as the formulary preferred Slozem brand ensures continuity of supply, as nationally. Verapamil is included in the formulary for: Angina: as monotherapy where intolerance or C/I to use of a beta-blocker. Hypertension: in line with NICE guidance. NB. Verapamil should not be combined with a beta-blocker for any indication due to high risk of bradycardia and heart-block Where Nicorandil has been added for symptom control pending angioplasty or CABG, strong consideration should be given to cautious withdrawal after successful completion of and recovery from the procedure Cardiovascular system Page 32
34 Therapeutic Area Formulary Choices Cost for 28 unless stated Rationale for decision / comments 2.8 Anticoagulant Drugs Oral anticoagulants Warfarin as Marevan Management of patients on Warfarin should be in line with the National Enhanced Service specification. Refer to National Patient Safety Agency (NPSA) guidance on safe practices around use of anticoagulants. 0.5mg tablets: mg tablets: mg tablets (GENERIC): mg tablets: 0.31 Warfarin is included in the formulary for the following indications (with target INRs): Atrial fibrillation: target INR 2.5 Treatment of deep-vein thrombosis and pulmonary embolism: target INR 2.5 Recurrent deep-vein thrombosis and pulmonary embolism: target INR 3.5 Mechanical prosthetic heart valves: target INR dependent on type and location of valve. Generally a target INR of 3 is for mechanical aortic valves and a target INR of 3.5 for mechanical mitral valves The brand Marevan is to ensure consistency of pack & colour for the patient and is available in 0.5mg strength. Management of haemorrhage: haemorrhage is the main adverse effect of all oral anticoagulants. Checking the INR and omitting doses is essential, if the anticoagulant is stopped but not reversed, the INR should be checked again after 2 to 3 days to ensure that it is falling. The following recommendations apply to patients taking Warfarin and are based on the result of the INR and whether there is major or minor bleeding: Major bleeding: stop Warfarin; give Phytomenadione (Vitamin K 1 ) 5-10mg by slow intra-venous injection; give prothrombin complex concentrate (factirs II, VII, IX and X) 30-50units/kg (or if no concentrate available) fresh frozen plasma 15ml/kg. INR> 8.0, no bleeding or minor bleeding: stop Warfarin, re-start when INR < 5. If there are other risk factors for bleeding, give Phytomenadione (Vitamin K 1 ) 500mcg by slow intra-venous injection or 5mg by mouth, (for partial reversal of anticoagulation give smaller oral doses of Phytomenadione e.g. 0.5mg 2.5mg, using the intravenous p reparation orally); repeat dose of Phytomenadione if INR still too high after 24 hours. See Chapter 9 for details of Phytomenadione preparations on the formulary. Cardiovascular system Page 33
Prescribing Formulary. 6 th Edition October 2009
 Prescribing Formulary 6 th Edition October 2009 Somerset Primary Care Trust - Primary Care Formulary 6th Edition October 2009 Introduction This formulary has been developed and reviewed by the Somerset
Prescribing Formulary 6 th Edition October 2009 Somerset Primary Care Trust - Primary Care Formulary 6th Edition October 2009 Introduction This formulary has been developed and reviewed by the Somerset
Younger adults with a family history of premature artherosclerotic disease should have their cardiovascular risk factors measured.
 Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Appendix 2A - Guidance on Management of Hypertension Measurement of blood pressure All adults from 40 years should have blood pressure measured as part of opportunistic cardiovascular risk assessment.
Chapter 2 - Cardiovascular System. Primary Care Prescribing Formulary - Preferred Drug Choices
 Chapter 2 - Cardiovascular System Primary Care Prescribing Formulary - Preferred Drug Choices Drug group Drug choice Comments/notes Cardiac glycosides Thiazide diuretics Loop diuretics Aldosterone antagonist
Chapter 2 - Cardiovascular System Primary Care Prescribing Formulary - Preferred Drug Choices Drug group Drug choice Comments/notes Cardiac glycosides Thiazide diuretics Loop diuretics Aldosterone antagonist
BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM. 1 April 13
 BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM 1 BNF 1.1 ANTACIDS Mucogel and Peptac are effective antacids and are available over the counter Gaviscon / Gaviscon Advance are available over the counter First
BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM 1 BNF 1.1 ANTACIDS Mucogel and Peptac are effective antacids and are available over the counter Gaviscon / Gaviscon Advance are available over the counter First
Chapter 2 ~ Cardiovascular system
 Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
Heart Failure Clinician Guide JANUARY 2018
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Chapter / Section / Drug
 2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
Heart Failure Clinician Guide JANUARY 2016
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Heart Failure (HF) - Primary Care Flow Charts. Pre diagnosis Symptoms or signs suggestive of HF
 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts. Symptoms or signs suggestive of HF. Pre diagnosis. Refer to the Heart Failure Clinic at VHK for
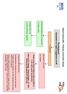 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
CARDIAC REHABILITATION PROGRAMME:- MEDICATION
 CARDIAC REHABILITATION PROGRAMME:- MEDICATION AIM OF THIS SESSION Understand the reasons for taking your medications, Discuss the common side effects associated with these medications - knowing when to
CARDIAC REHABILITATION PROGRAMME:- MEDICATION AIM OF THIS SESSION Understand the reasons for taking your medications, Discuss the common side effects associated with these medications - knowing when to
Management of Hypertension
 Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM
 BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM 1 ANTACIDS Maalox and Peptac are effective antacids that can be bought Over the Counter for self-limiting symptoms. Choice Product Cost Effective Options &Comments
BNF CHAPTER 1: GASTRO-INTESTINAL SYSTEM 1 ANTACIDS Maalox and Peptac are effective antacids that can be bought Over the Counter for self-limiting symptoms. Choice Product Cost Effective Options &Comments
Hypertension (JNC-8)
 Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
STANDARD treatment algorithm mmHg
 STANDARD treatment algorithm 130-140mmHg (i) At BASELINE, If AVERAGE SBP 1 > 140mmHg If on no antihypertensive drugs: Start 1 drug: If >55 years old / Afro-Caribbean: Calcium channel blocker (CCB) 2 If
STANDARD treatment algorithm 130-140mmHg (i) At BASELINE, If AVERAGE SBP 1 > 140mmHg If on no antihypertensive drugs: Start 1 drug: If >55 years old / Afro-Caribbean: Calcium channel blocker (CCB) 2 If
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
Volume 6; Number 1 January 2012 NICE CLINICAL GUIDELINE 127: HYPERTENSION CLINICAL MANAGEMENT OF PRIMARY HYPERTENSION IN ADULTS (AUGUST 2011)
 Volume 6; Number 1 January 2012 NICE CLINICAL GUIDELINE 127: HYPERTENSION CLINICAL MANAGEMENT OF PRIMARY HYPERTENSION IN ADULTS (AUGUST 2011) What s new in hypertension? NICE has issued an updated Clinical
Volume 6; Number 1 January 2012 NICE CLINICAL GUIDELINE 127: HYPERTENSION CLINICAL MANAGEMENT OF PRIMARY HYPERTENSION IN ADULTS (AUGUST 2011) What s new in hypertension? NICE has issued an updated Clinical
HEART FAILURE SUMMARY. and is associated with significant morbidity and mortality. the cornerstone of heart failure treatment.
 HEART FAILURE SUMMARY + Heart Failure is a condition affecting a large number of Irish people and is associated with significant morbidity and mortality. + ACE inhibitors, in combination with diuretics,
HEART FAILURE SUMMARY + Heart Failure is a condition affecting a large number of Irish people and is associated with significant morbidity and mortality. + ACE inhibitors, in combination with diuretics,
Hypertension diagnosis (see detail document) Diabetic. Target less than 130/80mmHg
 Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Shared Care Guideline Metolazone for fluid management in CKD (Adults)
 Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update)
 Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
NHS Kent and Medway Medicines Management. Dronedarone (Multaq ) Shared Care Guideline For Prescribing
 NHS Kent and Medway Medicines Management Dronedarone (Multaq ) Shared Care Guideline For Prescribing Issue No: 2 Review Date (If Applicable): Accountable Officer: Heather Lucas Contact Details: 01233 618158
NHS Kent and Medway Medicines Management Dronedarone (Multaq ) Shared Care Guideline For Prescribing Issue No: 2 Review Date (If Applicable): Accountable Officer: Heather Lucas Contact Details: 01233 618158
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
STOPP START Toolkit Supporting Medication Review in the Older Person
 STOPP START Toolkit Supporting Medication Review in the Older Person STOPP: Screening Tool of Older People s potentially inappropriate Prescriptions START: Screening Tool to Alert doctors to Right (appropriate,
STOPP START Toolkit Supporting Medication Review in the Older Person STOPP: Screening Tool of Older People s potentially inappropriate Prescriptions START: Screening Tool to Alert doctors to Right (appropriate,
Cardiology. Self Learning Package. Module 5: Pharmacology: Treatment of Acute Coronary. Prevention
 Cardiology Self Learning Package Module 5: Pharmacology: Treatment of Acute Coronary Syndromes, Module 5: Pharmacology: Hyperlipidaemia, Treatment of Acute Coronary Hypertension, Symdrome, Hyperlipidaemia,
Cardiology Self Learning Package Module 5: Pharmacology: Treatment of Acute Coronary Syndromes, Module 5: Pharmacology: Hyperlipidaemia, Treatment of Acute Coronary Hypertension, Symdrome, Hyperlipidaemia,
BNF CHAPTER 1: GASTROINTESTINAL
 BNF CHAPTER 1: GASTROINTESTINAL 1.1 DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE For symptomatic relief of hyperacidity, peptic ulcers, oesophagitis and acid reflux, liquids usually act faster than
BNF CHAPTER 1: GASTROINTESTINAL 1.1 DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE For symptomatic relief of hyperacidity, peptic ulcers, oesophagitis and acid reflux, liquids usually act faster than
Formulary and Prescribing Guidelines
 Formulary and Prescribing Guidelines SECTION 3: TREATMENT OF BIPOLAR AFFECTIVE DISORDER This section provides information regarding the pharmacological management of Bipolar affective disorder in secondary
Formulary and Prescribing Guidelines SECTION 3: TREATMENT OF BIPOLAR AFFECTIVE DISORDER This section provides information regarding the pharmacological management of Bipolar affective disorder in secondary
1/4/18. Heart Failure Guideline Review and Update. Disclosure. Pharmacist Objectives. Pharmacy Technician Objectives. What is Heart Failure?
 Disclosure Heart Failure Guideline Review and Update I have had no financial relationship over the past 12 months with any commercial sponsor with a vested interest in this presentation. Natalie Beiter,
Disclosure Heart Failure Guideline Review and Update I have had no financial relationship over the past 12 months with any commercial sponsor with a vested interest in this presentation. Natalie Beiter,
Hypertension Update. Objectives 4/28/2015. Beverly J. Mathis, D.O. OOA May 2015
 Hypertension Update Beverly J. Mathis, D.O. OOA May 2015 Objectives Learn new recommendations for BP treatment goals Approach to hypertension in the office Use of hypertensive drugs, and how to tailor
Hypertension Update Beverly J. Mathis, D.O. OOA May 2015 Objectives Learn new recommendations for BP treatment goals Approach to hypertension in the office Use of hypertensive drugs, and how to tailor
7/7/ CHD/MI LVH and LV dysfunction Dysrrhythmias Stroke PVD Renal insufficiency and failure Retinopathy. Normal <120 Prehypertension
 Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
SHARED CARE GUIDELINE
 SHARED CARE GUIDELINE Title: Lithium Treatment in Adults aged 18-65 years Scope: Pennine Care NHS Foundation Trust NHS Bury NHS Oldham NHS Heywood, Middleton and Rochdale NHS Stockport NHS Tameside & Glossop
SHARED CARE GUIDELINE Title: Lithium Treatment in Adults aged 18-65 years Scope: Pennine Care NHS Foundation Trust NHS Bury NHS Oldham NHS Heywood, Middleton and Rochdale NHS Stockport NHS Tameside & Glossop
Appendix C Factors to consider when choosing between anticoagulant options and FAQs
 Appendix C Factors to consider when choosing between anticoagulant options and FAQs Choice of anticoagulant for non-valvular* atrial fibrillation: Clinical decision aid Patients should already be screened
Appendix C Factors to consider when choosing between anticoagulant options and FAQs Choice of anticoagulant for non-valvular* atrial fibrillation: Clinical decision aid Patients should already be screened
Patient details GP details Specialist details Name GP Name Dr Specialist Name Dr R. Horton
 Rationale for Initiation, Continuation and Discontinuation (RICaD) Sacubitril/Valsartan (Entresto) For the treatment of symptomatic heart failure with reduced ejection fraction (NICE TA388) This document
Rationale for Initiation, Continuation and Discontinuation (RICaD) Sacubitril/Valsartan (Entresto) For the treatment of symptomatic heart failure with reduced ejection fraction (NICE TA388) This document
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
NHS GRAMPIAN MEDICAL TREATMENT GUIDELINES FOR CHRONIC HEART FAILURE (CHF) DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION (LVSD)
 NHS GRAMPIAN MEDICAL TREATMENT GUIDELINES FOR CHRONIC HEART FAILURE (CHF) DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION (LVSD) MANAGED CLINICAL NETWORK FOR CHRONIC HEART FAILURE November 2006 Review date:
NHS GRAMPIAN MEDICAL TREATMENT GUIDELINES FOR CHRONIC HEART FAILURE (CHF) DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION (LVSD) MANAGED CLINICAL NETWORK FOR CHRONIC HEART FAILURE November 2006 Review date:
5mg/5mL Liquid 25mg Tablets 50mg Tablets 100mg Tablets 50mg/5mL Suspension Special standardise strength 25mg Tablets
 Chapter 2- Cardiovascular Category Drug name Strength / dose / form BCU 2.1 Positive Inotropic drugs 2.1.1 Cardiac Digoxin 62.5 microgram Tablets Glycosides 125 microgram Tablets 250 microgram Tablets
Chapter 2- Cardiovascular Category Drug name Strength / dose / form BCU 2.1 Positive Inotropic drugs 2.1.1 Cardiac Digoxin 62.5 microgram Tablets Glycosides 125 microgram Tablets 250 microgram Tablets
Summary/Key Points Introduction
 Summary/Key Points Introduction Scope of Heart Failure (HF) o 6.5 million Americans 20 years of age have HF o 960,000 new cases of HF diagnosed annually o 5-year survival rate for HF is ~50% Classification
Summary/Key Points Introduction Scope of Heart Failure (HF) o 6.5 million Americans 20 years of age have HF o 960,000 new cases of HF diagnosed annually o 5-year survival rate for HF is ~50% Classification
Dorset Health Technologies Forum SHARED CARE GUIDELINE FOR PRESCRIBING EPLERENONE (INSPRA )
 INDICATION SHARED CARE GUIDELINE FOR PRESCRIBING EPLERENONE (INSPRA ) Eplerenone is an aldosterone antagonist licensed to be used in addition to standard therapy including beta-blockers, to reduce the
INDICATION SHARED CARE GUIDELINE FOR PRESCRIBING EPLERENONE (INSPRA ) Eplerenone is an aldosterone antagonist licensed to be used in addition to standard therapy including beta-blockers, to reduce the
Frimley Health Area Prescribing Committee
 Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
Dose. Route. Units. Given. Special situations. Dose. Route. Units. Given. Special situations
 Chapter 3 Cardiology Georgia Woodfield ASPIRIN FONDAPARINUX 300 once only in acute MI 75 in primary/ secondary prevention of thrombus formation and thromboembolic disease or PR; can also be given via nasogastric
Chapter 3 Cardiology Georgia Woodfield ASPIRIN FONDAPARINUX 300 once only in acute MI 75 in primary/ secondary prevention of thrombus formation and thromboembolic disease or PR; can also be given via nasogastric
Primary Care Constipation Guidelines. Version 1 November 2016
 Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression
 SHARED CARE PROTOCOL AND INFORMATION FOR GPS Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression Version:
SHARED CARE PROTOCOL AND INFORMATION FOR GPS Drug Name: Lithium Clinical Indications: Treatment and prophylaxis of mania; bipolar disorder; augmentation therapy in treatment resistant depression Version:
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Medication Reviews within Care Homes. Catherine Armstrong
 Medication Reviews within Care Homes Catherine Armstrong What is a Medication Review? A structured, critical examination of a patient s medicines with the objective of reaching an agreement with the patient
Medication Reviews within Care Homes Catherine Armstrong What is a Medication Review? A structured, critical examination of a patient s medicines with the objective of reaching an agreement with the patient
Therapeutic options for adult patients unable to take solid oral dosage forms (Adapted from UKMi Q&A for use in Northern Ireland) Sep 2015
 Therapeutic options for adult patients unable to take solid oral dosage forms (Adapted from UKMi Q&A 294.3 for use in Northern Ireland) Sep 2015 BNF 1.3.5 Proton pump inhibitors Lansoprazole orodispersible
Therapeutic options for adult patients unable to take solid oral dosage forms (Adapted from UKMi Q&A 294.3 for use in Northern Ireland) Sep 2015 BNF 1.3.5 Proton pump inhibitors Lansoprazole orodispersible
Prescribing in the Elderly. Dr Alison Macrae and Dr Debbie Vest GPST2 Drs in Psychiatry
 Prescribing in the Elderly Dr Alison Macrae and Dr Debbie Vest GPST2 Drs in Psychiatry 24 th September 2014 Objectives Understand the significance of polypharmacy in the elderly Become familiar with the
Prescribing in the Elderly Dr Alison Macrae and Dr Debbie Vest GPST2 Drs in Psychiatry 24 th September 2014 Objectives Understand the significance of polypharmacy in the elderly Become familiar with the
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
ANTI- HYPERTENSIVE AGENTS
 CLINICAL ANTI- HYPERTENSIVE AGENTS Jacqueline van Schoor, MPharm, BSc (Hons) Amayeza Info Centre Hypertension represents a major public health concern. It affects about a billion people worldwide and is
CLINICAL ANTI- HYPERTENSIVE AGENTS Jacqueline van Schoor, MPharm, BSc (Hons) Amayeza Info Centre Hypertension represents a major public health concern. It affects about a billion people worldwide and is
Mycophenolate Mofetil (MMF)
 SCG: For Transplant patients The following guidelines are designed to provide information relating to mycophenolate mofetil and to outline the responsibilities of the primary and secondary care teams in
SCG: For Transplant patients The following guidelines are designed to provide information relating to mycophenolate mofetil and to outline the responsibilities of the primary and secondary care teams in
Chapter 1 Gastro-Intestinal System
 Chapter 1 page number 1 Chapter 1 Gastro-Intestinal System First line drugs Drugs recommended in both primary and secondary care Second line drugs Alternatives (often in specific conditions) in both primary
Chapter 1 page number 1 Chapter 1 Gastro-Intestinal System First line drugs Drugs recommended in both primary and secondary care Second line drugs Alternatives (often in specific conditions) in both primary
Heart Failure. Dr. William Vosik. January, 2012
 Heart Failure Dr. William Vosik January, 2012 Questions for clinicians to ask Is this heart failure? What is the underlying cause? What are the associated disease processes? Which evidence-based treatment
Heart Failure Dr. William Vosik January, 2012 Questions for clinicians to ask Is this heart failure? What is the underlying cause? What are the associated disease processes? Which evidence-based treatment
Type 2 Diabetes. Stopping Smoking. Consider referral to smoking cessation. Consider referring for weight management advice.
 Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
Type 2 Diabetes Stopping Smoking Consider referral to smoking cessation BMI > 25 kg m² Set a weight loss target of a 5-10% reduction Consider referring for weight management advice Control BP to
Cardiovascular system
 Contents: Cardiovascular system 1. Hypertension 2 2. Hypertensive crises 4 3. Heart failure acute 5 4. Heart failure (chronic management) 6 5. Acute chest pain, angina and acute coronary syndromes (including
Contents: Cardiovascular system 1. Hypertension 2 2. Hypertensive crises 4 3. Heart failure acute 5 4. Heart failure (chronic management) 6 5. Acute chest pain, angina and acute coronary syndromes (including
Hypertension Update Warwick Jaffe Interventional Cardiologist Ascot Hospital
 Hypertension Update 2008 Warwick Jaffe Interventional Cardiologist Ascot Hospital Definition of Hypertension Continuous variable At some point the risk becomes high enough to justify treatment Treatment
Hypertension Update 2008 Warwick Jaffe Interventional Cardiologist Ascot Hospital Definition of Hypertension Continuous variable At some point the risk becomes high enough to justify treatment Treatment
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF CHRONIC HEART FAILURE with left ventricular systolic dysfunction
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF CHRONIC HEART FAILURE with left ventricular systolic dysfunction o o o o o All heart failure patients with LVSD should be considered for
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF CHRONIC HEART FAILURE with left ventricular systolic dysfunction o o o o o All heart failure patients with LVSD should be considered for
ESC Guidelines for the Diagnosis and Treatment of Acute and Chronic Heart Failure
 Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
Cardiovascular Health Practice Guideline Outpatient Management of Coronary Artery Disease 2003
 Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
Heart Failure: Guideline-Directed Management and Therapy
 Heart Failure: Guideline-Directed Management and Therapy Guideline-Directed Management and Therapy (GDMT) was developed by the American College of Cardiology and American Heart Association to define the
Heart Failure: Guideline-Directed Management and Therapy Guideline-Directed Management and Therapy (GDMT) was developed by the American College of Cardiology and American Heart Association to define the
What in the World is Functional Medicine?
 What in the World is Functional Medicine? An Introduction to a Systems Based Approach of Chronic Disease Meneah R Haworth, FNP-C Disclosure v I am a student of the Institute for Functional Medicine. They
What in the World is Functional Medicine? An Introduction to a Systems Based Approach of Chronic Disease Meneah R Haworth, FNP-C Disclosure v I am a student of the Institute for Functional Medicine. They
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Antihypertensive drugs: I. Thiazide and other diuretics:
 Clinical assessment of hypertensive patient: You have to take history regarding the presence of other risk factors for CAb like diabetes mellitus, smoking, etc. Take history whether the patient takes medications
Clinical assessment of hypertensive patient: You have to take history regarding the presence of other risk factors for CAb like diabetes mellitus, smoking, etc. Take history whether the patient takes medications
Incidental Findings; Management of patients presenting with high BP. Phil Swales
 Incidental Findings; Management of patients presenting with high BP Phil Swales Consultant Physician Acute & General Medicine University Hospitals of Leicester NHS Trust Objectives The approach to an incidental
Incidental Findings; Management of patients presenting with high BP Phil Swales Consultant Physician Acute & General Medicine University Hospitals of Leicester NHS Trust Objectives The approach to an incidental
PHARMACOLOGICAL PROBLEMS
 PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests
 www.bpac.org.nz keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests Why do we monitor patients taking diuretics and what do we monitor? Monitoring a person on
www.bpac.org.nz keyword: diuretics Drug monitoring Monitoring diuretics in primary care 2 March 2009 best tests Why do we monitor patients taking diuretics and what do we monitor? Monitoring a person on
Report generated from MPH Formulary provided by FormularyComplete (www.pharmpress.com). Accessed Formulary Status. TA Number.
 Report generated from MPH provided by Complete (www.pharmpress.com). Accessed 15 01 2016 Title Status Section TA Number TA Link Alu-Cap simeticone->aluminium- and magnesium-containing antacids->aluminium
Report generated from MPH provided by Complete (www.pharmpress.com). Accessed 15 01 2016 Title Status Section TA Number TA Link Alu-Cap simeticone->aluminium- and magnesium-containing antacids->aluminium
Medicines for high blood pressure
 Patient Information: Medicines Medicines for high blood pressure Health & care information you can trust The Information Standard Certified Member Working together for better patient information What is
Patient Information: Medicines Medicines for high blood pressure Health & care information you can trust The Information Standard Certified Member Working together for better patient information What is
ACE. Inhibitors. Quiz feedback
 ACE Inhibitors Quiz feedback bpac nz better medicin e bpac nz Quiz feedback, ACE inhibitors, 2006 Best Practice Advocacy Centre ACE inhibitors quiz feedback bpac nz Development Team: Rachael Clarke Sonia
ACE Inhibitors Quiz feedback bpac nz better medicin e bpac nz Quiz feedback, ACE inhibitors, 2006 Best Practice Advocacy Centre ACE inhibitors quiz feedback bpac nz Development Team: Rachael Clarke Sonia
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Berkshire West Area Prescribing Committee Guidance
 Guideline Name Berkshire West Area Prescribing Committee Guidance Date of Issue: September 2015 Review Date: September 2017 Date taken to APC: 2 nd September 2015 Date Ratified by GP MOC: Guidelines for
Guideline Name Berkshire West Area Prescribing Committee Guidance Date of Issue: September 2015 Review Date: September 2017 Date taken to APC: 2 nd September 2015 Date Ratified by GP MOC: Guidelines for
Cardiovascular drugs
 chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
Core Safety Profile. Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg. Date of FAR:
 Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005
 VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
Guidelines for the Management of Chronic Non-Malignant Pain (CNMP) in Primary Care (not including neuropathic pain (NeP).
 Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) North East Hampshire & Farnham CCG and Crawley, Horsham & Mid-Sussex CCG Guidelines for the
Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) North East Hampshire & Farnham CCG and Crawley, Horsham & Mid-Sussex CCG Guidelines for the
Section 3, Lecture 2
 59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
Coronary Artery Disease (CAD) Clinician Guide SEPTEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Coronary Artery Disease (CAD) Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide is based on the 2017 KP National Coronary Artery Disease
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Coronary Artery Disease (CAD) Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide is based on the 2017 KP National Coronary Artery Disease
Difficult to Treat Hypertension
 Difficult to Treat Hypertension According to Goldilocks JNC 8 Blood Pressure Goals (2014) BP Goal 60 years old and greater*- systolic < 150 and diastolic < 90. (Grade A)** BP Goal 18-59 years old* diastolic
Difficult to Treat Hypertension According to Goldilocks JNC 8 Blood Pressure Goals (2014) BP Goal 60 years old and greater*- systolic < 150 and diastolic < 90. (Grade A)** BP Goal 18-59 years old* diastolic
Patient Profile. Patient s details Initials: IF Age: 40 Gender: Male. Weight: 139.7kg Height: 510 metres BMI: >47
 Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Hypertension Clinical case scenarios for primary care
 Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
Hypertension Clinical case scenarios for primary care Implementing NICE guidance August 2011 NICE clinical guideline 127 What this presentation covers Five clinical case scenarios, including: presentation
Inverclyde CHP Protected Learning Event- Heart Failure
 Inverclyde CHP Protected Learning Event- Heart Failure 14:00 14:05 14:05 14:20 14:20 14:30 14:30 15:10 15:10 15:30 15:30 15:50 15:50 16:05 16:05 16:35 Welcome & Introduction Paul Forsyth (HF Pharmacist)
Inverclyde CHP Protected Learning Event- Heart Failure 14:00 14:05 14:05 14:20 14:20 14:30 14:30 15:10 15:10 15:30 15:30 15:50 15:50 16:05 16:05 16:35 Welcome & Introduction Paul Forsyth (HF Pharmacist)
Clinical Assessment Tool
 Clinical Assessment Tool Child with Suspected Gastroenteritis 0-5 Years Diarrhoea is defined as the passage of three or more loose/watery stools per day, the most common cause of diarrhoea in children
Clinical Assessment Tool Child with Suspected Gastroenteritis 0-5 Years Diarrhoea is defined as the passage of three or more loose/watery stools per day, the most common cause of diarrhoea in children
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF<40%
 Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Essential Shared Care Agreement: Lithium
 Ref No. E042 Essential Shared Care Agreement: Lithium Please complete the following details: Patient s name, address, date of birth Treatment (indication, dose regimen, brand name) Monitoring (proposed
Ref No. E042 Essential Shared Care Agreement: Lithium Please complete the following details: Patient s name, address, date of birth Treatment (indication, dose regimen, brand name) Monitoring (proposed
CLINICAL PROTOCOL THE PREVENTION OF FATALITIES FROM MEDICATION LOADING DOSES
 National Patient Safety Alert RRR018 Preventing Fatalities From Medication Loading Doses (November 2010) MMCP05 CLINICAL PROTOCOL THE PREVENTION OF FATALITIES FROM MEDICATION LOADING DOSES INTRODUCTION
National Patient Safety Alert RRR018 Preventing Fatalities From Medication Loading Doses (November 2010) MMCP05 CLINICAL PROTOCOL THE PREVENTION OF FATALITIES FROM MEDICATION LOADING DOSES INTRODUCTION
Medications and your Heart. RBCH Foundation Trust
 Medications and your Heart RBCH Foundation Trust Today I will try and cover Confusing cocktail of drugs? What are they for? How do I take them? What if I forget to take them? What are common side effects?
Medications and your Heart RBCH Foundation Trust Today I will try and cover Confusing cocktail of drugs? What are they for? How do I take them? What if I forget to take them? What are common side effects?
Royal Wolverhampton Hospital Adult Lipid Lowering Therapy Guidelines Lipid Lowering Therapy for the Prevention of Cardiovascular Disease
 Royal Wolverhampton Hospital Adult Lipid Lowering Therapy Guidelines 1 This guideline is intended to assist rational and cost-effective prescribing of lipid regulating medications across both primary and
Royal Wolverhampton Hospital Adult Lipid Lowering Therapy Guidelines 1 This guideline is intended to assist rational and cost-effective prescribing of lipid regulating medications across both primary and
Cardiovascular Clinical Practice Guideline Pilot Implementation
 Cardiovascular Clinical Practice Guideline Pilot Implementation Pharmacologic Management of Chronic Heart Failure Sept 15, 2004 Angela Allerman, PharmD, BCPS DoD Pharmacoeconomic Center Promoting high
Cardiovascular Clinical Practice Guideline Pilot Implementation Pharmacologic Management of Chronic Heart Failure Sept 15, 2004 Angela Allerman, PharmD, BCPS DoD Pharmacoeconomic Center Promoting high
Management of Hypertension. Ahmed El Hawary MD Suez Canal University
 Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
GASTRO-INTESTINAL SYSTEM 1.1 Dyspepsia and gastro-oesophageal reflux disease
 Original Date of issue: 05/04/07 Last eviewed: 08/03/2013 Version: 5 Page 1 of 11 GASTO-INTESTINAL SYSTEM 1.1 Dyspepsia and gastro-oesophageal reflux disease 1.1.1 Antacids and simeticone Magnesium Trisilicate
Original Date of issue: 05/04/07 Last eviewed: 08/03/2013 Version: 5 Page 1 of 11 GASTO-INTESTINAL SYSTEM 1.1 Dyspepsia and gastro-oesophageal reflux disease 1.1.1 Antacids and simeticone Magnesium Trisilicate
CORLANOR (ivabradine) oral tablet
 CORLANOR (ivabradine) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
CORLANOR (ivabradine) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
Chapter 1 Gastro-Intestinal System
 Chapter 1 page number 1 Chapter 1 Gastro-Intestinal System First line drugs Drugs recommended in both primary and secondary care Second line drugs Alternatives (often in specific conditions) in both primary
Chapter 1 page number 1 Chapter 1 Gastro-Intestinal System First line drugs Drugs recommended in both primary and secondary care Second line drugs Alternatives (often in specific conditions) in both primary
Paediatric Directorate
 Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Mid Essex Locality Guideline for Management of Adult Acute and Chronic Non-Cancer Pain in Primary care
 Guideline for Management of Adult Acute and Chronic Non-Cancer Pain in Primary care If possible patients should be assessed using a simple visual analogue scale VAS to determine the most appropriate stage
Guideline for Management of Adult Acute and Chronic Non-Cancer Pain in Primary care If possible patients should be assessed using a simple visual analogue scale VAS to determine the most appropriate stage
Dr Narender Goel MD (Internal Medicine and Nephrology) Financial Disclosure: None, Conflict of Interest: None
 Dr Narender Goel MD (Internal Medicine and Nephrology) drnarendergoel@gmail.com Financial Disclosure: None, Conflict of Interest: None 12 th December 2013, New York Visit us at: http://kidneyscience.info/
Dr Narender Goel MD (Internal Medicine and Nephrology) drnarendergoel@gmail.com Financial Disclosure: None, Conflict of Interest: None 12 th December 2013, New York Visit us at: http://kidneyscience.info/
Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127
 Hypertension in adults: diagnosis and management Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Hypertension in adults: diagnosis and management Clinical guideline Published: 24 August 2011 nice.org.uk/guidance/cg127 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
The ADDITION Study: A study about screening for diabetes. Screening Case Report Form
 ADDITION Study, Leicester Participant Identification Label: Date: / / The ADDITION Study: A study about screening for diabetes Screening Case Report Form You will need to have the following things done
ADDITION Study, Leicester Participant Identification Label: Date: / / The ADDITION Study: A study about screening for diabetes Screening Case Report Form You will need to have the following things done
