Updates to your prescription benefits
|
|
|
- Lindsey Park
- 5 years ago
- Views:
Transcription
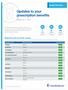
1 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill a prescription. Please reference this chart as you review the following updates. $ $$ $$$ Tier 1 Tiers 2 and 3 Tier 4 Your lowest-cost medications Your mid-range cost medications Your highest-cost medications Medications with new benefit coverage. The following medications were previously not covered under most benefit plans and are now eligible for coverage. Therapeutic Use Medication Name Tier Placement Allergies RyVent 4 Chest Pain GoNitro 4 Constipation Trulance 4 Dry Eye Disease Restasis MultiDose 4 Eye Pain/Inflammation BromSite 4 Hepatitis C Infections Mavyret Vosevi Daxbia Otovel 2 4 Migraines Ergomar 4 Oral Steroid LoCort ZonaCort 4 Osteoporosis Tymlos 3 Skin Conditions Micort-HC 2.5% cream Rhofade 4 Access Four-Tier Member Update Summary
2 Medications moving to a lower tier. The following medications are moving to a lower tier, making them more affordable. Therapeutic Use Medication Name Tier Placement Inflammatory Conditions Otezla 4 u 2 Pain Xtampza ER 3 u 2 Medications moving to a higher tier. Medications may move from a lower tier to a higher tier when they are more costly and have available lower-cost options. Therapeutic Use Acne Allergic Reactions Cancer Medication Name Differin 0.1% cream, gel, lotion* EpiPen (Brand Only)* EpiPen Jr (Brand Only)* Mekinist Tafinlar Tier Placement Lower-Cost Options 3 u 4 OTC Differin gel 2 u 4 epinephrine auto-injector (generic EpiPen) epinephrine auto-injector (generic EpiPen Jr) 2 u 3 Discuss with your doctor Contraceptive Natazia $0 u 2 $0 cost-share contraceptives Hepatitis C Daklinza Sovaldi 2 u 4 Discuss with your doctor Infections Albenza 2 u 4 OTC pyrantel pamoate Ciprodex otic 2 u 3 ofloxacin 0.3 % solution (generic Floxin Otic, Ocuflox) Osteoporosis Forteo 2 u 3 Discuss with your doctor Medications excluded from benefit coverage. We evaluate medications based on their total value, including how a medication works and how much it costs. When several medications work in the same way, we may choose to exclude the higher-cost option. Effective Jan. 1, 2018, the medications listed below may be excluded from coverage or subject to prior authorization (sometimes referred to as precertification) and/or trial/failure** of another medication(s). You should review your benefit plan documents and pharmacy benefit coverage for a full list of medications that are excluded or have programs or limits that apply. Therapeutic Use Medication Name Lower-Cost Options ADHD Strattera (Brand Only) atomoxetine (generic Strattera) Asthma/COPD AirDuo Respiclick (Brand Only) fluticasone/salmeterol powder for inhalation (generic AirDuo Respiclick), Advair Diskus/HFA, Breo Ellipta, Symbicort Cholesterol/Lipid Lowering Vytorin (Brand Only) simvastatin/ezetimibe (generic Vytorin) Diabetes*** Xultophy Soliqua * Medication is typically excluded from benefit coverage. ** Referred to as First Start in New Jersey. *** For Oxford plans, diabetic supplies and prescription medications may be subject to different cost-share arrangements. Please see your Summary of Benefits and Coverage (SBC) for specifics.
3 Therapeutic Use Medication Name Lower-Cost Options Duchenne Muscular Dystrophy Elevated Parathyroid Hormone Endocrine Disorders Emflaza Rayaldee Sandostatin (Brand Only) prednisone calcitriol (generic Rocaltrol), doxercalciferol (generic Hectorol), paricalcitol (generic Zemplar) octreotide (generic Sandostatin) Hepatitis B Baraclude tablets (Brand Only) entecavir tablet (generic Baraclude) Dutoprol metoprolol (generic Toprol-XL) plus hydrochlorothiazide High Blood Pressure Inderal LA (Brand Only) metoprolol extended-release/ propranolol extended-release capsule (generic Inderal LA) hydrochlorothiazide (Dutoprol metoprolol (generic Toprol-XL) plus hydrochlorothiazide Authorized Generic) Infections Vigamox (Brand Only) moxifloxacin ophthalmic solution (generic Viagamox) Influenza Tamiflu capsules (Brand Only) oseltamivir capsules (generic Tamiflu) Mental Health Opioid Induced Constipation Pain Parkinson's Disease Skin Conditions Pristiq (Brand Only) Prozac Weekly (Brand Only) Seroquel XR (Brand Only) Relistor tablet Arymo ER Opana ER Azilect (Brand Only) Cordran cream (Brand Only) Cordran lotion (Brand Only) desvenlafaxine extended-release tablet (generic Pristiq) fluoxetine capsules (generic Prozac) quetiapine extended-release (generic Seroquel XR) Movantik morphine sulfate extended-release tablet (generic MS Contin), Nucynta ER, Xtampza ER rasagiline (generic Azilect) flurandrenolide 0.05% cream (generic Cordran cream), hydrocortisone valerate 0.2% cream (generic Westcort cream), prednicarbate 0.1% cream (generic Dermatop cream) flurandrenolide 0.05% lotion (generic Cordran), triamcinolone acetonide 0.1% lotion (generic Kenalog lotion)
4 Prescription medications with over-the-counter equivalents.**** Prescription medications containing the same active ingredient available in an over-the-counter product may be excluded from coverage. Therapeutic Use Medication Name Lower-Cost Options Stroke & Heart Attack Prevention Yosprala OTC aspirin plus omeprazole (Prilosec), pantoprazole (Protonix) **** This is not applicable for plans written in New Jersey. For New York plans, a prescription drug product that is therapeutically equivalent to an over-the counter drug may be covered if it is determined to be medically necessary. Visit the member website listed on your health plan ID card to look up the price of drugs covered by your plan, find lower-cost options and more. For more information, call the toll-free phone number on the back of your health plan ID card to speak with a Customer Service respresentive. This document applies to commercial group members of UnitedHealthcare and Oxford New York and New Jersey plans. UnitedHealthcare is a registered trademark owned by UnitedHealth Group, Inc. All branded medications are trademarks or registered trademarks of their respective owners. Please note not all PDL updates apply to all groups depending on state regulation, riders and SPDs. Insurance coverage provided by or through UnitedHealthcare Insurance Company, UnitedHealthcare Insurance Company of New York, or Oxford Health Insurance, Inc. Oxford HMO products are underwritten by Oxford Health Plans (NJ), Inc. Administrative services provided by United HealthCare Services, Inc., UnitedHealthcare Service LLC, Oxford Health Plans LLC, or their affiliates. MT MS / United HealthCare Services, Inc. Access Four-Tier PDL Update Summary
5 Nondiscrimination notice and access to communication services UnitedHealthcare and Oxford do not discriminate on the basis of race, color, national origin, age, disability or sex in its health programs or activities. If you think you were treated unfairly because of your sex, age, race, color, disability or national origin, you can send a complaint to the Civil Rights Coordinator. Online: UHC_Civil_Rights@uhc.com Mail: Civil Rights Coordinator UnitedHealthcare Civil Rights Grievance P.O. Box Salt Lake City, UT You must send the complaint within 60 days of your experience. A decision will be sent to you within 30 days. If you disagree with the decision, you have 15 days to ask us to look at it again. If you need help with your complaint, please call the toll-free phone number listed on your ID card, TTY 711, Monday through Friday, 8 a.m. to 8 p.m. if you are a UnitedHealthcare member, or Monday through Friday, 8 a.m. to 6 p.m. if you are a member of an Oxford plan. You can also file a complaint with the U.S. Dept. of Health and Human Services. Online: Complaint forms are available at Phone: Toll free , (TDD) Mail: U.S. Dept. of Health and Human Services 200 Independence Avenue SW Room 509F, HHH Building Washington, D.C We provide free services to help you communicate with us, including letters in other languages or large print. Or, you can ask for an interpreter. To ask for help, please call the toll-free phone number listed on your ID card, TTY 711, Monday through Friday, 8 a.m. to 8 p.m. if you are a UnitedHealthcare member, or Monday through Friday, 8 a.m. to 6 p.m. if you are a member of an Oxford plan.
6
Updates to your prescription benefits
 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits
 Updates to your prescription benefits Effective January 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective January 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits
 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018
 Date: November 7, 2017 To: From: HPN/SHL Contracted Pharmacies and Providers Ryan Bitton, PharmD, MBA Senior Director, Pharmacy Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018 Effective
Date: November 7, 2017 To: From: HPN/SHL Contracted Pharmacies and Providers Ryan Bitton, PharmD, MBA Senior Director, Pharmacy Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018 Effective
Pharmacy Benefit Coverage Updates Jan. 1, 2018
 Pharmacy Benefit Coverage Updates Jan. 1, 2018 UnitedHealthcare routinely evaluates prescription benefit coverage to help ensure we offer members affordable and effective medication options. Medications
Pharmacy Benefit Coverage Updates Jan. 1, 2018 UnitedHealthcare routinely evaluates prescription benefit coverage to help ensure we offer members affordable and effective medication options. Medications
Updates to your prescription benefits
 Updates to your prescription benefits Effective July 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective July 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits
 Updates to your prescription benefits Effective July 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective July 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
$250 (Deductible does not apply to Tier 1 and Tier 2) $500 (Deductible does not apply to Tier 1 and Tier 2)
 Benefit Summary Outpatient Prescription Drug Illinois 5/50/100/250 Plan 455 Your Co-payment and/or Co-insurance is determined by the tier to which the Prescription Drug List (PDL) Management Committee
Benefit Summary Outpatient Prescription Drug Illinois 5/50/100/250 Plan 455 Your Co-payment and/or Co-insurance is determined by the tier to which the Prescription Drug List (PDL) Management Committee
Updates to your prescription benefits
 Updates to your prescription benefits Effective Jan. 1, 2019 Traditional Three-Tier PDL Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount
Updates to your prescription benefits Effective Jan. 1, 2019 Traditional Three-Tier PDL Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount
Updates to your prescription benefits
 Updates to your prescription benefits Effective January 1, 2019 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective January 1, 2019 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Health TALK. Heart smart. Plan to quit. Know your cholesterol numbers.
 Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day, or it could be the fi rst day of
Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day, or it could be the fi rst day of
Health TALK. Mammograms save lives. Plan to quit.
 Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day. Or it could be the fi rst day of
Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day. Or it could be the fi rst day of
Santa Clara Family Health Plan Cal MediConnect Plan (Medicare-Medicaid Plan) 2017 Drug List
 Upcoming Changes to Santa Clara Family Health Plan Cal MediConnect Plan (Medicare-Medicaid Plan) 2017 Drug List Updated 8/1/2017 Santa Clara Family Health Plan (SCFHP) Cal MediConnect Plan (Medicare-Medicaid
Upcoming Changes to Santa Clara Family Health Plan Cal MediConnect Plan (Medicare-Medicaid Plan) 2017 Drug List Updated 8/1/2017 Santa Clara Family Health Plan (SCFHP) Cal MediConnect Plan (Medicare-Medicaid
Health TALK. Toothache? Did you know?
 Health TALK SUMMER 2018 Did you know? About 618 people in the United States are killed by extreme heat every year. Heat-related illnesses happen when the body is not able to properly cool itself. Older
Health TALK SUMMER 2018 Did you know? About 618 people in the United States are killed by extreme heat every year. Heat-related illnesses happen when the body is not able to properly cool itself. Older
Health TALK. Toothache? KidsHealth
 Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
Health TALK. Toothache? Keep your coverage.
 Health TALK SUMMER 2018 VOLTEE PARA ESPAÑOL! Keep your coverage. You may have received a letter from the Mississippi Division of Medicaid. A special open enrollment process will begin July 1 through August
Health TALK SUMMER 2018 VOLTEE PARA ESPAÑOL! Keep your coverage. You may have received a letter from the Mississippi Division of Medicaid. A special open enrollment process will begin July 1 through August
Health TALK. Toothache? KidsHealth
 Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
2018 Preventive Schedule
 2018 Preventive Schedule Medicare-Covered Services PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat.
2018 Preventive Schedule Medicare-Covered Services PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat.
Tusculum College. Benefit Summary. $25 Copay. $25 Copay. after Deductible. 20% after Deductible 20% after Deductible
 Benefit Plan Features: Annual Deductible Benefit Summary Your Cost In-Network Individual/Family $750/$1500 Annual Out-of-Pocket Maximum Individual/Family $3500/$7000 4th Quarter Carry-over Covered Services
Benefit Plan Features: Annual Deductible Benefit Summary Your Cost In-Network Individual/Family $750/$1500 Annual Out-of-Pocket Maximum Individual/Family $3500/$7000 4th Quarter Carry-over Covered Services
2017 Preventive Schedule
 2017 Preventive Schedule PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The preventive guidelines
2017 Preventive Schedule PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The preventive guidelines
Health TALK. The right care. Register online!
 Health TALK SPRING 2019 VOLTEE PARA ESPAÑOL! Register online! You can get important information about your health plan anytime at myuhc.com/communityplan. At this secure site, you can view your ID card,
Health TALK SPRING 2019 VOLTEE PARA ESPAÑOL! Register online! You can get important information about your health plan anytime at myuhc.com/communityplan. At this secure site, you can view your ID card,
DRUG TESTING IN PAIN MANAGEMENT AND SUBSTANCE USE DISORDER(S) TREATMENT
 TREATMENT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
TREATMENT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
LARTRUVO (olaratumab)
 LARTRUVO (olaratumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
LARTRUVO (olaratumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Health TALK. Take charge. Health4Me TM. Prepare to see your provider.
 Health TALK SPRING 2018 Health4Me TM Do you have the UnitedHealthcare Health4Me mobile app? Health4Me has many of the same features as your secure member website, myuhc.com/communityplan. You can view
Health TALK SPRING 2018 Health4Me TM Do you have the UnitedHealthcare Health4Me mobile app? Health4Me has many of the same features as your secure member website, myuhc.com/communityplan. You can view
Pediatric Dental and Vision
 Individual & Family Plans (IFP) and Small Business Group (SBG) Health Net of California, Inc. (Health Net) Pediatric Dental and Vision Andre Hamil Health Net When you purchase a Health Net PureCare HSP
Individual & Family Plans (IFP) and Small Business Group (SBG) Health Net of California, Inc. (Health Net) Pediatric Dental and Vision Andre Hamil Health Net When you purchase a Health Net PureCare HSP
RELISTOR (methylnaltrexone bromide) INJECTION FOR SUBCUTANEOUS USE
 RELISTOR (methylnaltrexone bromide) INJECTION FOR SUBCUTANEOUS USE Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for
RELISTOR (methylnaltrexone bromide) INJECTION FOR SUBCUTANEOUS USE Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for
Department of Origin: Integrated Healthcare Services. Approved by: Chief Medical Officer Department(s) Affected: Date approved: 01/10/17
 Reference #: MP/D005 Page: 1 of 3 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MP/D005 Page: 1 of 3 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Calendar Year Deductible Annual Benefit Maximum. ADA Code Covered Services Member pays. n/a Office visit $5 per visit
 Blue Shield of California Dental HMO Plan Dental HMO Basic Benefit summary Effective January 1, 2018 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE
Blue Shield of California Dental HMO Plan Dental HMO Basic Benefit summary Effective January 1, 2018 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE
TYMLOS (abaloparatide)
 TYMLOS (abaloparatide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
TYMLOS (abaloparatide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Health TALK. Toothache? KidsHealth
 Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
Health TALK SUMMER 2018 KidsHealth UnitedHealthcare and KidsHealth have teamed up to provide advice you need, when you want it. Parents can get doctor-approved advice. Kids can fi nd fun health games and
Quarterly pharmacy formulary change notice
 Quarterly pharmacy formulary change notice The formulary changes listed in the table below were reviewed and approved at our second quarter 2018 Pharmacy and Therapeutics Committee meeting. Effective October
Quarterly pharmacy formulary change notice The formulary changes listed in the table below were reviewed and approved at our second quarter 2018 Pharmacy and Therapeutics Committee meeting. Effective October
PANCREATIC ISLET TRANSPLANT
 PANCREATIC ISLET TRANSPLANT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
PANCREATIC ISLET TRANSPLANT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
ORAL IMPLANT PROCEDURES
 ORAL IMPLANT PROCEDURES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
ORAL IMPLANT PROCEDURES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Pharmacy benefit guide
 FlexRx SM 5-Tier Pharmacy benefit guide 1 Welcome to FlexRx The NHP FlexRx SM program is built for choice, savings, and convenience with benefits including: Low-cost drug tier for many common medications
FlexRx SM 5-Tier Pharmacy benefit guide 1 Welcome to FlexRx The NHP FlexRx SM program is built for choice, savings, and convenience with benefits including: Low-cost drug tier for many common medications
MEDICAL COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 10/04/17 SECTION: DRUGS LAST REVIEW DATE: LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 BAVENCIO (avelumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
BAVENCIO (avelumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Dental Options 2018 BALTIMORE CITY PUBLIC SCHOOLS
 Dental Options 2018 BALTIMORE CITY PUBLIC SCHOOLS Contents Important Information for 2018... 1 Dental HMO (DHMO) Dental Plan... 2 Preferred Dental PPO (DPPO) Dental Plan... 3 Summary of Dental PPO Benefits...
Dental Options 2018 BALTIMORE CITY PUBLIC SCHOOLS Contents Important Information for 2018... 1 Dental HMO (DHMO) Dental Plan... 2 Preferred Dental PPO (DPPO) Dental Plan... 3 Summary of Dental PPO Benefits...
Smile SM Value 50/1500/No Ortho/MAC
 Blue Shield of California Dental PPO Plan Smile SM Value 50/1500/No Ortho/MAC Benefit summary Effective January 1, 2018 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A
Blue Shield of California Dental PPO Plan Smile SM Value 50/1500/No Ortho/MAC Benefit summary Effective January 1, 2018 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A
Quarterly pharmacy formulary change notice
 Provider Bulletin October 2018 Quarterly pharmacy formulary change notice The formulary changes listed in the table below apply to all Anthem HealthKeepers Plus patients. The changes listed in the table
Provider Bulletin October 2018 Quarterly pharmacy formulary change notice The formulary changes listed in the table below apply to all Anthem HealthKeepers Plus patients. The changes listed in the table
GENETIC TESTING FOR PREDICTING RISK OF NONFAMILIAL BREAST CANCER
 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
GENETIC TESTING FOR TAMOXIFEN TREATMENT
 GENETIC TESTING FOR TAMOXIFEN TREATMENT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
GENETIC TESTING FOR TAMOXIFEN TREATMENT Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
01/10/17. Replaces Effective Policy Dated: Amino Acid Based Elemental Formula (AABF) 09/28/15 Reference #: MP/A003 Page: 1 of 3
 Reference #: MP/A003 Page: 1 of 3 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MP/A003 Page: 1 of 3 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
ENDOBRONCHIAL ULTRASOUND FOR DIAGNOSIS AND STAGING OF LUNG CANCER
 CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
High-Cost Drug Exclusions
 PHARMACY SERVICES High-Cost Exclusions The high cost medications listed below are excluded from coverage because lower cost similar alternatives are available. To help you get the best health benefit at
PHARMACY SERVICES High-Cost Exclusions The high cost medications listed below are excluded from coverage because lower cost similar alternatives are available. To help you get the best health benefit at
ALPHA1-PROTEINASE INHIBITORS
 ALPHA1-PROTEINASE INHIBITORS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
ALPHA1-PROTEINASE INHIBITORS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
Smile SM Deluxe Gold 50/1500/Ortho/U85
 Blue Shield of California Dental PPO Plan Smile SM Deluxe Gold 50/1500/Ortho/U85 Benefit summary Effective January 1, 2017 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS
Blue Shield of California Dental PPO Plan Smile SM Deluxe Gold 50/1500/Ortho/U85 Benefit summary Effective January 1, 2017 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS
Calendar Year Deductible Annual Benefit Maximum. ADA Code Covered Services Member pays
 An independent member of the Blue Shield Association A50861-SG (1/19) Dental HMO Plan Dental HMO Standard Benefit summary Effective January 1, 2019 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
An independent member of the Blue Shield Association A50861-SG (1/19) Dental HMO Plan Dental HMO Standard Benefit summary Effective January 1, 2019 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
IMMUNE CELL FUNCTION ASSAY
 IMMUNE CELL FUNCTION ASSAY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
IMMUNE CELL FUNCTION ASSAY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 HYDROXYPROGESTERONE THERAPY Makena (hydroxyprogesterone caproate injection) Hydroxyprogesterone caproate compound Hydroxyprogesterone caproate injection with benzyl benzoate and the preservative benzyl
HYDROXYPROGESTERONE THERAPY Makena (hydroxyprogesterone caproate injection) Hydroxyprogesterone caproate compound Hydroxyprogesterone caproate injection with benzyl benzoate and the preservative benzyl
Quarterly pharmacy formulary change notice
 MEDICAID PROVIDER BULLETIN October 2018 The formulary changes listed in the table below were reviewed and approved at the second-quarter 2018 Pharmacy and Therapeutics Committee meeting. Effective October
MEDICAID PROVIDER BULLETIN October 2018 The formulary changes listed in the table below were reviewed and approved at the second-quarter 2018 Pharmacy and Therapeutics Committee meeting. Effective October
FYI ONLY Generic Name. Generics available. zoledronic acid N/A
 Criteria Document: Reference #: PC/A011 Page 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community
Criteria Document: Reference #: PC/A011 Page 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community
Tusculum College. Benefit Summary Option/Quote: 2. 30% after Deductible. $35 Copay. 30% after Deductible
 Benefit Plan Features: Annual Deductible Effective Date: 4/1/2018 Network: S Benefit Summary Option/Quote: 2 Your Cost In-Network Individual/Family $1250/$2500 Annual Out-of-Pocket Maximum Tusculum College
Benefit Plan Features: Annual Deductible Effective Date: 4/1/2018 Network: S Benefit Summary Option/Quote: 2 Your Cost In-Network Individual/Family $1250/$2500 Annual Out-of-Pocket Maximum Tusculum College
2019 Formulary Update
 MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
Health TALK. Heart smart. Plan to quit. Know your cholesterol numbers.
 Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day. Or it could be the fi rst day of
Health TALK FALL 2018 VOLTEE PARA ESPAÑOL! Plan to quit. Every November, the Great American Smokeout asks everyone to quit smoking. You can quit for just that one day. Or it could be the fi rst day of
HEMATOPOIETIC CELL TRANSPLANTATION FOR EPITHELIAL OVARIAN CARCINOMA
 CARCINOMA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
CARCINOMA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
REQUEST FOR MEDICARE PRESCRIPTION DRUG COVERAGE DETERMINATION This form may be sent to us by mail or fax:
 REQUEST FOR MEDICARE PRESCRIPTION DRUG COVERAGE DETERMINATION This form may be sent to us by mail or fax: Address: Fax Number: Anthem Blue Cross Cal MediConnect Plan 1-844-493-9213 Medicare Prior Authorization
REQUEST FOR MEDICARE PRESCRIPTION DRUG COVERAGE DETERMINATION This form may be sent to us by mail or fax: Address: Fax Number: Anthem Blue Cross Cal MediConnect Plan 1-844-493-9213 Medicare Prior Authorization
MOLECULAR TESTING IN THE MANAGEMENT OF PULMONARY NODULES
 MOLECULAR TESTING IN THE MANAGEMENT OF PULMONARY NODULES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
MOLECULAR TESTING IN THE MANAGEMENT OF PULMONARY NODULES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
RADIOFREQUENCY ABLATION OF PRIMARY OR METASTATIC LIVER TUMORS
 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Smile SM Plus 50/1500/Ortho/MAC
 Dental PPO Plan Smile SM Plus 50/1500/Ortho/MAC Benefit summary Effective January 1, 2019 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF
Dental PPO Plan Smile SM Plus 50/1500/Ortho/MAC Benefit summary Effective January 1, 2019 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF
MEMBER GRIEVANCES AND APPEALS PROCEDURES
 MEMBER GRIEVANCES AND APPEALS PROCEDURES We value our members. We want you to let us know right away if you are not happy with our health plan. This includes if you have any questions, complaints or problems
MEMBER GRIEVANCES AND APPEALS PROCEDURES We value our members. We want you to let us know right away if you are not happy with our health plan. This includes if you have any questions, complaints or problems
FlexRx 6-Tier. SM Pharmacy Benefit Guide
 FlexRx 6-Tier SM Pharmacy Benefit Guide Welcome to FlexRx The AllWays Health Partners FlexRx SM program is built for choice, savings, and convenience with benefits including: Low-cost drug tier for many
FlexRx 6-Tier SM Pharmacy Benefit Guide Welcome to FlexRx The AllWays Health Partners FlexRx SM program is built for choice, savings, and convenience with benefits including: Low-cost drug tier for many
PARSABIV (etelcalcetide)
 PARSABIV (etelcalcetide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
PARSABIV (etelcalcetide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
INTRAVITREAL IMPLANTS
 INTRAVITREAL IMPLANTS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
INTRAVITREAL IMPLANTS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
GENETIC TESTING FOR KRAS, NRAS AND BRAF VARIANT ANALYSIS IN METASTATIC COLORECTAL CANCER
 METASTATIC COLORECTAL CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
METASTATIC COLORECTAL CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
BLINCYTO (blinatumomab)
 BLINCYTO (blinatumomab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
BLINCYTO (blinatumomab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
MEDICAL COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 12/19/17 SECTION: MEDICINE LAST REVIEW DATE: LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 MEDICAL FOODS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
MEDICAL FOODS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
SOMATULINE DEPOT (lanreotide acetate)
 SOMATULINE DEPOT (lanreotide acetate) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
SOMATULINE DEPOT (lanreotide acetate) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
ENTYVIO (vedolizumab)
 ENTYVIO (vedolizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
ENTYVIO (vedolizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 XOLAIR (omalizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
XOLAIR (omalizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Dental Plus of Idaho THE POLICY PROVIDES DENTAL BENEFITS ONLY.
 Dental Plus of Idaho THE POLICY PROVIDES DENTAL BENEFITS ONLY. Form No. 005DPID(1/18) The Dental Plus of Idaho plan is a managed care dental policy and is underwritten by: Willamette Dental of Idaho, Inc.
Dental Plus of Idaho THE POLICY PROVIDES DENTAL BENEFITS ONLY. Form No. 005DPID(1/18) The Dental Plus of Idaho plan is a managed care dental policy and is underwritten by: Willamette Dental of Idaho, Inc.
APOKYN (apomorphine hydrochloride)
 APOKYN (apomorphine hydrochloride) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
APOKYN (apomorphine hydrochloride) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
2019 PHARMACY DIRECTORY
 2019 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2019 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
EXAMPLE ONLY. RxBIN Issuer (80840) ID NAME Drew Zehnder. Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030
 Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030 00001 RxBIN 004336 RxPCN ADV RxGRP RX3151 Issuer (80840) 9151014609 ID NAME 111111111 Drew Zehnder Present this Prescription Card to fill your
Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030 00001 RxBIN 004336 RxPCN ADV RxGRP RX3151 Issuer (80840) 9151014609 ID NAME 111111111 Drew Zehnder Present this Prescription Card to fill your
2017 Preventive Schedule
 2017 Preventive Schedule PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The preventive guidelines
2017 Preventive Schedule PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The preventive guidelines
Health New England (HNE) is making some changes to your Plan, most of which become effective July 1, 2015.
 April 17, 2015 FULLY FUNDED PLANS ONLY RE: Semi-Annual Notice of Changes Dear HNE Member: Health New England (HNE) is making some changes to your Plan, most of which become effective July 1, 2015. I have
April 17, 2015 FULLY FUNDED PLANS ONLY RE: Semi-Annual Notice of Changes Dear HNE Member: Health New England (HNE) is making some changes to your Plan, most of which become effective July 1, 2015. I have
Part D Pharmacy. An Independent Licensee of the Blue Cross Blue Shield Association ( )
 Part D Pharmacy 1 An Independent Licensee of the Blue Cross Blue Shield Association 044507 (12-21-2017) New MA pharmacy partner We ve selected CVS Caremark to manage our part D pharmacy benefits Providence
Part D Pharmacy 1 An Independent Licensee of the Blue Cross Blue Shield Association 044507 (12-21-2017) New MA pharmacy partner We ve selected CVS Caremark to manage our part D pharmacy benefits Providence
Drug List exclusions for Blue Cross commercial plans
 Drug List exclusions for Blue Cross commercial plans The drugs shown below aren t covered on the commercial Blue Cross Blue Shield of Michigan drug lists. In most cases, if you fill a prescription for
Drug List exclusions for Blue Cross commercial plans The drugs shown below aren t covered on the commercial Blue Cross Blue Shield of Michigan drug lists. In most cases, if you fill a prescription for
PROTEOMIC TESTING FOR SYSTEMIC THERAPY IN NON-SMALL-CELL LUNG CANCER
 CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Step Therapy Criteria
 Tier 5 Formulary Step Therapy 2016 Updated: 05/24/2016 Effective: 06/01/2016 What is Step Therapy? Some prescription drugs require step therapy (ST). In some cases, the plan requires you to first try certain
Tier 5 Formulary Step Therapy 2016 Updated: 05/24/2016 Effective: 06/01/2016 What is Step Therapy? Some prescription drugs require step therapy (ST). In some cases, the plan requires you to first try certain
CIMZIA (certolizumab pegol)
 CIMZIA (certolizumab pegol) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
CIMZIA (certolizumab pegol) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 NUCALA (mepolizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
NUCALA (mepolizumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Drug Formulary Update, April 2017 Commercial and State Programs
 Drug Formulary Update, April 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, April 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
FECAL ANALYSIS IN THE DIAGNOSIS OF INTESTINAL DYSBIOSIS
 FECAL ANALYSIS IN THE DIAGNOSIS OF INTESTINAL DYSBIOSIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
FECAL ANALYSIS IN THE DIAGNOSIS OF INTESTINAL DYSBIOSIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
Generics. Lead with. P r e s c r i p t i o n S t e p T h e r a p y P r o g r a m
 Lead with Generics P r e s c r i p t i o n S t e p T h e r a p y P r o g r a m WWW.BCBSLA.COM 04HQ3972 5/09 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Service & Indemnity
Lead with Generics P r e s c r i p t i o n S t e p T h e r a p y P r o g r a m WWW.BCBSLA.COM 04HQ3972 5/09 Blue Cross and Blue Shield of Louisiana incorporated as Louisiana Health Service & Indemnity
STELARA (ustekinumab)
 STELARA (ustekinumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
STELARA (ustekinumab) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Drug Formulary Update, January 2017 Commercial and State Programs
 Drug Formulary Update, January 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, January 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
01/26/17. Replaces Effective Policy Dated: Autism Spectrum Disorders in Children: Assessment 01/19/16 and Evaluation Reference #: MP/A005 Page 1 of 4
 Reference #: MP/A005 Page 1 of 4 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MP/A005 Page 1 of 4 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
2019 Drug List Negative Changes
 2019 Drug List Negative Changes Updated 03/26/2019 If you are taking a drug that is removed from the formulary (also known as the Drug List), we will tell you. We will also tell you if we add any restrictions
2019 Drug List Negative Changes Updated 03/26/2019 If you are taking a drug that is removed from the formulary (also known as the Drug List), we will tell you. We will also tell you if we add any restrictions
MYLOTARG (gemtuzumab ozogamicin)
 MYLOTARG (gemtuzumab ozogamicin) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
MYLOTARG (gemtuzumab ozogamicin) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
MULTIMARKER SERUM TESTING RELATED TO OVARIAN CANCER
 MULTIMARKER SERUM TESTING RELATED TO OVARIAN CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
MULTIMARKER SERUM TESTING RELATED TO OVARIAN CANCER Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
INTRAPERITONEAL CHEMOTHERAPY, CYTOREDUCTION
 INTRAPERITONEAL CHEMOTHERAPY, CYTOREDUCTION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
INTRAPERITONEAL CHEMOTHERAPY, CYTOREDUCTION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
Amitriptyline Hydrochloride Heart Health & BP Amlodipine Besylate 5mg Norvasc Antibiotics Amoxicillin 500 mg Amoxil
 Antiviral Acyclovir 400mg Zovirax Asthma Advair Diskus Diskus 250/50 Fluticasone/Salmeterol Asthma Albuterol Sulfate 2.5 mg/3 ml Proventil Arthritis and Pain Allendronate Sodium 70 mg Fosamax Arthritis
Antiviral Acyclovir 400mg Zovirax Asthma Advair Diskus Diskus 250/50 Fluticasone/Salmeterol Asthma Albuterol Sulfate 2.5 mg/3 ml Proventil Arthritis and Pain Allendronate Sodium 70 mg Fosamax Arthritis
Amitriptyline Hydrochloride Heart Health & BP Amlodipine Besylate 5mg Norvasc Antibiotics Amoxicillin 500 mg Amoxil
 School Corp Formulary Antiviral Acyclovir 400mg Zovirax Asthma Advair Diskus Diskus 250/50 Fluticasone/Salmeterol Asthma Albuterol Sulfate 2.5 mg/3 ml Proventil Arthritis and Pain Allendronate Sodium 70
School Corp Formulary Antiviral Acyclovir 400mg Zovirax Asthma Advair Diskus Diskus 250/50 Fluticasone/Salmeterol Asthma Albuterol Sulfate 2.5 mg/3 ml Proventil Arthritis and Pain Allendronate Sodium 70
2018 Preventive Schedule Effective 1/1/2018
 2018 Preventive Schedule Effective 1/1/2018 PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The
2018 Preventive Schedule Effective 1/1/2018 PLAN YOUR CARE: KNOW WHAT YOU NEED AND WHEN TO GET IT Preventive or routine care helps us stay well or finds problems early, when they are easier to treat. The
PURPOSE: The intent of this policy is to provide guidelines for coverage of dental procedures under the medical benefit.
 Integrated Reference #: MP/D009 Page 1 of 4 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc.
Integrated Reference #: MP/D009 Page 1 of 4 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc.
Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017
 Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017 DRUG LIST CHANGES Based on the availability of new prescription medications and Prime s National Pharmacy and Therapeutics Committee
Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017 DRUG LIST CHANGES Based on the availability of new prescription medications and Prime s National Pharmacy and Therapeutics Committee
03/13/18. A. Symptoms lasting for greater than or equal to 12 months that have resulted to significant impairment in activities of daily living; and
 Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
