Intermountain Healthcare Bronchiolitis Update Intermountain Healthcare Pediatric Clinical Programs
|
|
|
- Lynne Aileen Williams
- 5 years ago
- Views:
Transcription
1 Intermountain Healthcare Bronchiolitis Update Intermountain Healthcare Pediatric Clinical Programs Updated 11/2008
2 Reviewed by: Intermountain Pediatric Education Team Intermountain Respiratory Therapy Team Anne Brenneman APRN, MS, CPNP Seasonal Outcomes Compiled by: Julie Ballard, BS, RRT
3 This Bronchiolitis Update Is Intended For: Physicians, Nurses, Respiratory Therapists and Other Healthcare Providers Who Care for Pediatric Patients Throughout Intermountain Healthcare. The important thing is not to stop questioning. Albert Einstein
4 Upon Completion of This Bronchiolitis Update, You Should Be Able To: Discuss the etiology, epidemiology, pathophysiology & management of RSV / Bronchiolitis Locate and utilize the Intermountain Newborn/Pediatric Bronchiolitis Protocol and Standardized Admit Orders (SAO) Discuss Seasonal Outcomes for your facility Pass the post-test as assigned The post test is available as an on-line test
5 Bronchiolitis Update Contents Definition of Bronchiolitis Epidemiology of RSV Pathophysiology Risk factors Clinical presentation Diagnosis Evaluation Intermountain protocol Therapy options Severe Bronchiolitis Prevention Discharge & followup Seasonal outcomes Articles
6 Definition of Bronchiolitis Common, acute, contagious respiratory illness of infants and young children that involves the lower respiratory tract Common causative agents include: Respiratory Syncytial virus (RSV) Parainfluenza types 1, 2, 3 Adenovirus Human Metapneumovirus (mpv) Rhinovirus Influenza types A, B Enterovirus
7 RSV is: RSV Epidemiology The most common cause of bronchiolitis Initially described over 100 years ago The leading cause of lower respiratory tract infections in infants and young children Infection spread by fomites and contact with infectious secretions Typically an upper respiratory tract infection in older children and adults A more severe illness in infants and small children, but infects all ages Duration of illness is 7-10 days Adults with RSV in one study had a mean work absence of 6 days
8 RSV Epidemiology Worldwide occurrence Peak incidence of RSV is in winter and early spring in the northern hemisphere, or rainy season in tropical climates Season is usually around 6 months (November April; Peak months are January & February) Most cases occur between 2-8 months of age /100 children are typically infected in the first year with most children demonstrating antibodies by 2nd - 3rd year of life 1-2% of all children are hospitalized
9 In one year: RSV Epidemiology 90, ,000 pediatric hospitalizations per year in the US Up to 510 deaths between * Mortality is 0.2-7% (depending upon risk factors; also some data was prior to current level of available ICU care) Recent data showed a 2-4% mortality in ICU patients * Shay DK, Holman, RC, et al. Bronchiolitis-Associated Mortality and Estimates of Respiratory Syncytial Virus-Associated Deaths among US Children J Infect Dis 2001; 183:16-22
10 RSV Epidemiology First-time infections are usually the most severe RSV can cause significant apnea via unknown mechanisms Apnea is the presenting symptom in approximately 20% of infants admitted to the hospital with RSV Infants at risk for developing apnea include: Premature infants < 32 wk gestational age Infants with a history of neonatal apnea Severe hypoxemia
11 Bronchiolitis Pathophysiology Obstruction of bronchioles Inflammation Edema Mucous Debris Increased airway resistance Hyperinflation Atelectasis V-Q mismatching Blood perfusing the lung is not exchanging gases due to atelectasis, mucous plugs, etc
12 Bronchiolitis Pathophysiology Infants are at highest risk due to small airways Recovery is slow Epithelium begins to regenerate in 3-5 days Cilia do not reappear for up to 2 weeks RSV may be shed by the nose for up to 21 days Cough may persist for weeks
13 Risk Factors for Developing Bronchiolitis Low birth weight, premature infants The younger the child, the higher the risk Lower socioeconomic group Crowded living conditions More than 2 children per bedroom Day care attendance Older siblings in preschool or school Being in a multiple birth set (eg. twins, triplets) Parental smoking
14 Risk Factors for Severe Disease* Prematurity Chronic lung disease, e.g. BPD Worse in the first 2 years of life Congenital heart disease Immunodeficiency states Symptomatic HIV disease, organ or bone marrow transplantation, elderly *Mortality is 3-5% in high-risk hospitalized patients and they tend to have more severe, protracted illness.
15 Bronchiolitis Clinical Progression Incubation period 2-5 days Infants fussy with some difficulty feeding Typically low-grade fever (less than 38.6º C or 101.4º f) Fever is usually gone by the time the family seeks medical care Over the next 2-5 days Increased coryza and congestion 60% of infections are confined to the upper airway Gradual progression to lower respiratory tract Cough, dyspnea, wheezing, feeding difficulties worsen
16 Bronchiolitis Commonly Reported Symptoms Increased work of breathing Fussiness, inability to sleep Cough, post-tussive emesis Poor feeding Decreased urine and stool output (or loose stool)
17 Bronchiolitis Common Physical Findings Fever C ( º F) Up to 20% of patients may have a higher temperature Occasionally infants < 1 month may be hypothermic (< 36.5 C) Tachypnea, tachycardia, increased work of breathing (nasal flaring, retractions, grunting) Coarse crackles, wheezing Cyanosis Otitis media (in up to 40% of cases) Mild conjunctivitis or pharyngitis Palpable liver from pulmonary hyperinflation
18 Bronchiolitis Diagnosis Diagnosis is based on clinical findings Age, seasonal occurrence, common symptoms and physical findings Viral diagnostic studies can be helpful For cohorting, SBI exclusion, differential diagnosis
19 Differential Diagnosis of Infant With Respiratory Distress Reactive airway disease/asthma Sepsis Croup, Pertussis Pneumonia aspiration, bacterial, other virus Foreign body aspiration Congenital structural anomaly, vascular ring Bronchomalacia, tracheomalacia Congenital lobar emphysema Tracheal ring Bronchial cleft cyst Cystic fibrosis Chronic aspiration Congenital heart disease Congestive heart failure and/or pulmonary edema
20 Bronchiolitis Evaluation O2 saturation Good indicator of severity and correlates well with degree of tachypnea but not with severity of wheezing or crackles At high elevation, O2 saturations 88% CR monitoring <3 months, apnea, high risk (h/o prematurity, BPD or underlying lung or heart disease), bronchiolitis score greater than 6. Consider CBG or ABG for severe respiratory distress or possible fatigue
21 Bronchiolitis-Evaluation Consider other lab studies in special situations: Full sepsis evaluation (CBC, blood culture, UA, urine culture, CSF studies and culture) for fever in infants < 90 days or those with toxic appearance (see Febrile Infant Protocol) Electrolytes, stool studies for dehydration or diarrhea
22 Bronchiolitis Evaluation Viral identification of nasal secretions Positive viral study can prevent more invasive workup in small infants and allows for cohorting of patients with the same viral diagnosis Rapid viral tests are available (during respiratory season) for RSV and Influenza, but if results are negative, proceed to DFA (direct fluorescent antibody) DFA commercial tests are available for RSV, Parainfluenza 1,2,3, Influenza A & B, Adenovirus, Human Metapneumovirus Sensitivity varies depending on how sample is obtained, and kit used. Most have a sensitivity of >90% Specificity generally >95% Viral culture is 60% sensitive but 100% specific
23 Bronchiolitis Evaluation Radiology-Chest X-Ray: Not routinely needed unless diagnosis uncertain Neither specific nor prognostic Typically shows hyperinflation, atelectasis, and 20-30% may show lobar infiltrates
24 Bronchiolitis Evaluation Indications for admission Toxic or septic appearance Respiratory distress Apnea Low O2 saturation on room air (<88%) Dehydration Risk factors for severe disease present
25 Risk Factors for Severe Disease* Prematurity Chronic lung disease, e.g. BPD Worse in the first 2 years of life Congenital heart disease Immunodeficiency states Symptomatic HIV disease, organ or bone marrow transplantation, elderly *Mortality is 3-5% in high-risk hospitalized patients and they tend to have more severe, protracted illness.
26 The Bronchiolitis Protocol Intended for inpatient management The protocol exists to create consistency among caregivers, emphasize effective treatments and reduce use of unnecessary therapies A team approach utilizes a standardized order set & the protocol Review Bronchiolitis Standardized Admit Orders (SAO) Review Bronchiolitis Newborn Pediatric Protocol
27 Bronchiolitis Protocol: Scoring Bronchiolitis score The score is an attempt to create consistency in assessment among caregivers The scoring system is not validated but inter-rater reliability has been demonstrated Intervention effectiveness is measured through rescoring after the intervention
28 Bronchiolitis Protocol: Bronchiolitis Score Score Respiratory Rate < 1 year > 1 year Wheeze Retractions 0 < 40 < 30 None None Expiration 1 location Insp/Exp 2 locations 3 > 65 > 45 Diminished > 3 locations 0-1= Normal 2-3=Mild 4-6=Moderate 7-9=Severe
29 Bronchiolitis Protocol: Inpatient Management The mainstay of therapy is supportive care Suctioning to assist with clearance of secretions Naso-pharyngeal (NP) suction with an 8 Fr. catheter, advanced into the hypopharynx BBG or bulb suction for nasal secretions for tight or bloody nares Oxygen to maintain saturations in the normal or desired range Hydration Oral intake, IV fluids and/or nasogastric tube Patients are usually made NPO if respiratory rate is > 65 BPM due to risk of aspiration
30 Bronchiolitis Protocol: Oxygen O2 therapy is indicated if saturations are <88%, or below goal saturation Nasal cannula administration preferred O2 humidified with bubbler can prevent irritation and bleeding of nares Room air trial every 4 hours when stable & sp02 flow rate of 0.1 liter/min for patient < 6 months, or.25 liter/min for patients 6-24 months Evaluate work of breathing carefully during weaning process
31 Bronchiolitis Protocol: Monitoring Cardiorespiratory monitoring is indicated for: Infants less than 3 months of age History of apnea or experiencing apnea Bronchiolitis score greater than 6 History of prematurity, BPD, or cardiorespiratory disease
32 Bronchiolitis Protocol: Suctioning Suctioning improves patient comfort and decreases work of breathing and may increase the ability to feed Indications for suctioning include: Increased work of breathing Increased retractions Decreased saturations or increased oxygen requirement Worsening bronchiolitis score Occasionally utilized if PO intake is marginal and it is thought that suctioning may help infant with troublesome secretions Patient is scored before and 15 minutes after suctioning
33 Suctioning Bronchiolitis Protocol: Suctioning Methods NP (nasopharyngeal) suction with an 8 Fr. catheter, advanced into the hypopharynx. May consider transition to BBG or bulb suction prior to discharge
34 Bronchiolitis Protocol: Isolation Droplet precautions Mask & gloves when entering room Gown, mask & gloves with patient contact When suctioning eye protection is a required precaution Hand hygiene before and after patient contact Cohort patients only with the same infectious agent
35 Bronchiolitis Protocol: Bronchodilator Trials A trial treatment of nebulized Albuterol or Racemic Epinephrine may be given and patient response evaluated: Steps include: Obtain baseline Bronchiolitis score Suction nasopharynx Obtain Bronchiolitis score 15 post sx Administer medication treatment Obtain Bronchiolitis score 15 post medication treatment A positive response = score decreases by at least one point Wheezing may become audible if breath sounds were diminished before treatment
36 Therapy Options: Bronchodilators Albuterol or other ß-agonists Meta-analyses reveal modest/short term improvement, inconclusive findings or no benefit Occasionally utilized in patients with recurrent wheezing or diagnosis of RAD Trial of nebulized albuterol may be considered in select patients (family history of asthma or personal history of multiple episodes of wheezing) Patient is scored before and 15 minutes after intervention
37 Therapy Options: Bronchodilators Racemic epinephrine Studies show some efficacy Stimulates alpha and beta receptors Vasoconstriction may decrease airway inflammation and mild bronchodilator effect Trial of nebulized epi may be considered if albuterol is ineffective Patient is scored before and 15 minutes after intervention CR monitoring recommended Concern for hypokalemia, hypertension, arrhythmia, tachycardia with use
38 Therapy Options: Steroids Multiple studies with varying results Some show effectiveness, some do not Randomized control trial (RCT) underway to determine if steroids administered in ED decrease admissions Occasionally utilized in patients with recurrent wheezing or diagnosis of RAD (reactive airway disease) or CLD (chronic lung disease) Not a component of the bronchiolitis protocol
39 Therapy Options: Antibiotics Serious bacterial co-infection unlikely in patients with known viral diagnosis (<1% association) Indicated for strong evidence of bacterial superinfection or otitis media Broad-spectrum antibiotics are used in infants 1-90 days in whom SBI (serious bacterial infection) is suspected and cultures are pending or in critically ill infants
40 Therapy Options: CPAP Non-invasive ventilation (CPAP or HFNC): May be used for infants who are tiring and have increasing respiratory insufficiency Help to maintain patency of the smaller airways preventing atelectasis
41 Management of Severe Bronchiolitis ICU care needed for the following: ABG or CBG showing respiratory acidosis and/or climbing PCO2 Severe distress not responding to conservative therapy (oxygen, suctioning, hydration, bronchodilators) Severe hypoxia requiring non-invasive ventilation Respiratory failure
42 Bronchiolitis Prevention Vaccines Attempts at developing a vaccine have yet to be successful. Presence of antibodies do not confer immunity Re-infection is common and, in vaccine studies, more severe
43 Bronchiolitis Prevention Palivizumab (Synagis) Monoclonal antibody against the F (fusion) protein of RSV Monthly IM injection, administered during peak RSV season Shown to decrease both risk for hospitalization (down 55%) and severity of subsequent infections Used in a very select patient population
44 Bronchiolitis Prevention Palivizumab (Synagis) indications: Refer to: Synagis order form for additional guidelines Infant < 24 months with chronic lung disease, CF or CHD Premature infants born at less than 28 weeks gestational age (WGA) Must be < 1 year old at the start of the RSV season Premature infants born at WGA Must be < 6 mos old at the start of the RSV season Infants born at WGA Must have additional risk factors with other criteria Infant received palivizumab (Synagis) one month previously
45 Bronchiolitis Discharge Discharge planning Consider discharge if patient: Has low and stable scores and no evidence of respiratory distress or cyanosis Tolerates room air or has a low, stable oxygen need Is able to maintain hydration with feeds Has clearly defined follow up care with primary care physician Caregivers should be reliable, have transportation, and have the ability to call for help
46 Bronchiolitis Discharge Plan for discharge with oxygen and any other equipment or supplies at least one day in advance Discharge teaching very important for parents Review Bronchiolitis Teaching Outline
47 Teach parents: Bronchiolitis Discharge Teaching To evaluate respiratory status, hydration, manage oxygen and other equipment To perform bulb or other suctioning, particularly prior to feedings To administer medications properly To understand when to call for assistance or seek medical care To understand hand washing, risk of irritants such as tobacco smoke, and avoidance of daycare while the child is ill Review Bronchiolitis Let s Talk About and provide a copy for the family
48 Bronchiolitis Follow up Care Follow up Contact with primary care physician is required before discharge Follow up in 2-3 days if stable and breathing easily without supplemental oxygen Follow up in 1-2 days if on oxygen or if patient has significant co-morbidities REMEMBER, patients can shed virus in their secretions for up to 21 days after the onset of symptoms, and the cough can last for weeks
49 Intermountain Healthcare Seasonal Outcomes To view Intermountain Healthcare outcomes, click on the above link and then select a link under Bronchiolitis Seasonal Outcomes
50 Articles American Academy of Pediatrics, Clinical Practice Guideline, Diagnosis and Mangement of Bronchiolitis, PEDIATRICS Volume 118, Number 4, October 2006 DeNicola, LK. Bronchiolitis. Emedicine article: Last Updated: December 11, 2006.
51 Articles Krilov LR. Respiratory Syncytial virus infection. Emedicine articles: Last Updated: March 24, 2006 Louden, M. Pediatrics, Bronchiolitis. Emedicine article: Article Last Updated: Nov 1, 2007.
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Discuss the benefits for developing an outpatient bronchiolitis clinic.
 Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Medical Center Discuss the benefits for developing an outpatient bronchiolitis clinic. 1 Definition Inflammation of the bronchioles
Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Medical Center Discuss the benefits for developing an outpatient bronchiolitis clinic. 1 Definition Inflammation of the bronchioles
PEDIATRIC RESPIRATORY ILLNESS MADE SIMPLE
 Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
Pediatric Bronchiolitis. Janie Robles, PharmD, AE-C Assistant Professor of Pharmacy Practice Pediatrics School of Pharmacy TTUHSC Lubbock, Texas
 This PowerPoint file is a supplement to the video presentation. Some of the educational content of this program is not available solely through the PowerPoint file. Participants should use all materials
This PowerPoint file is a supplement to the video presentation. Some of the educational content of this program is not available solely through the PowerPoint file. Participants should use all materials
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Video Cases in Pediatrics. Ran Goldman, MD BC Children s Hospital University of British
 Video Cases in Pediatrics Ran Goldman, MD BC Children s Hospital University of British Columbia @Dr_R_Goldman Bronchiolitis Viral infection of the lower respiratory tract characterized by acute inflammation,
Video Cases in Pediatrics Ran Goldman, MD BC Children s Hospital University of British Columbia @Dr_R_Goldman Bronchiolitis Viral infection of the lower respiratory tract characterized by acute inflammation,
BRONCHIOLITIS PEDIATRIC
 DEFINITION Bronchiolitis is typically defined as the first episode of wheezing in infants < 24 months of age. It is a viral illness of the lower respiratory tract that causes tachypnea, bronchospasm, and
DEFINITION Bronchiolitis is typically defined as the first episode of wheezing in infants < 24 months of age. It is a viral illness of the lower respiratory tract that causes tachypnea, bronchospasm, and
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Simulation 01: Two Year-Old Child in Respiratory Distress (Croup)
 Simulation 01: Two Year-Old Child in Respiratory Distress (Croup) Flow Chart Opening Scenario 2 year-old child in respiratory distress - assess Section 1 Type: IG audible stridor with insp + exp wheezing;
Simulation 01: Two Year-Old Child in Respiratory Distress (Croup) Flow Chart Opening Scenario 2 year-old child in respiratory distress - assess Section 1 Type: IG audible stridor with insp + exp wheezing;
PAEDIATRIC ACUTE CARE GUIDELINE. Bronchiolitis
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Bronchiolitis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Bronchiolitis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis. Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine
 Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Management of Bronchiolitis in Infants
 Co-issued by Paediatric Medicine and the Division of Paediatric Emergency Medicine. 1.0 Introduction Bronchiolitis is an acute inflammatory disease of the lower respiratory tract, resulting from obstruction
Co-issued by Paediatric Medicine and the Division of Paediatric Emergency Medicine. 1.0 Introduction Bronchiolitis is an acute inflammatory disease of the lower respiratory tract, resulting from obstruction
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
CONTAGIOUS COMMENTS Department of Epidemiology
 VOLUME XXX NUMBER 1 January 2015 CONTAGIOUS COMMENTS Department of Epidemiology Respiratory Season 2014 15 Kellie Rusin MLS (ASCP)CM MPH, Christine Robinson PhD, James Gaensbauer MD, MScPH, & the Respiratory
VOLUME XXX NUMBER 1 January 2015 CONTAGIOUS COMMENTS Department of Epidemiology Respiratory Season 2014 15 Kellie Rusin MLS (ASCP)CM MPH, Christine Robinson PhD, James Gaensbauer MD, MScPH, & the Respiratory
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
A Trust Guideline for the Management of. Bronchiolitis in Infants and Children under the age of 24 months
 A Clinical Guideline recommended Children s Assessment Unit (CAU), Buxton Ward, For use in: Children s Day Ward, Jenny Lind Out-patients Department, Accident and Emergency Department By: Medical and Nursing
A Clinical Guideline recommended Children s Assessment Unit (CAU), Buxton Ward, For use in: Children s Day Ward, Jenny Lind Out-patients Department, Accident and Emergency Department By: Medical and Nursing
All About RSV (Respiratory Syncytial Virus)
 All About RSV (Respiratory Syncytial Virus) A Guide for Parents What is RSV? RSV stands for respiratory syncytial virus, the most frequent cause of serious respiratory tract infections in infants and children
All About RSV (Respiratory Syncytial Virus) A Guide for Parents What is RSV? RSV stands for respiratory syncytial virus, the most frequent cause of serious respiratory tract infections in infants and children
PEDIATRIC RESPIRATORY SYNCYTIAL VIRUS (RSV) ALL THAT WHEEZES IS NOT ASTHMA
 PEDIATRIC RESPIRATORY SYNCYTIAL VIRUS (RSV) ALL THAT WHEEZES IS NOT ASTHMA Season changes here in Ohio can send the census numbers in our local P.I.C.U. s, N.I.C.U. s and Emergency Rooms through the roof.
PEDIATRIC RESPIRATORY SYNCYTIAL VIRUS (RSV) ALL THAT WHEEZES IS NOT ASTHMA Season changes here in Ohio can send the census numbers in our local P.I.C.U. s, N.I.C.U. s and Emergency Rooms through the roof.
Approach to Bronchiolitis
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Bronchiolitis. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Bronchiolitis. These podcasts are designed to give medical students an overview of key topics in pediatrics.
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
CONTAGIOUS COMMENTS Department of Epidemiology
 VOLUME XXVIII NUMBER 7 November/December 2013 CONTAGIOUS COMMENTS Department of Epidemiology Respiratory Season 2013 14 Kelly West MS, RN, CIC, Christine Robinson, PhD, & the Respiratory Season Planning
VOLUME XXVIII NUMBER 7 November/December 2013 CONTAGIOUS COMMENTS Department of Epidemiology Respiratory Season 2013 14 Kelly West MS, RN, CIC, Christine Robinson, PhD, & the Respiratory Season Planning
BRONCHIOLITIS. See also the PSNZ guideline - Wheeze & Chest Infections in infants under 1 year (www.paediatrics.org.nz)
 Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Bronchiolitis Update. Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch.
 www.bpac.org.nz keyword: bronchiolitis Bronchiolitis Update Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch Key Points: Bronchiolitis is the most
www.bpac.org.nz keyword: bronchiolitis Bronchiolitis Update Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch Key Points: Bronchiolitis is the most
BRONCHIOLITIS. Introduction
 BRONCHIOLITIS Introduction Bronchiolitis is the most common lower respiratory infection in infants and a leading cause of hospital admission in this age group. It is a viral infection and is most commonly
BRONCHIOLITIS Introduction Bronchiolitis is the most common lower respiratory infection in infants and a leading cause of hospital admission in this age group. It is a viral infection and is most commonly
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Bronchiolitis v.2.0: Criteria and Respiratory Score
 Bronchiolitis v.2.0: Criteria and Respiratory Score Executive Summary Test your knowledge Epidemiology, Pathophysiology & Natural History Inclusion Criteria Age
Bronchiolitis v.2.0: Criteria and Respiratory Score Executive Summary Test your knowledge Epidemiology, Pathophysiology & Natural History Inclusion Criteria Age
Diagnosis and Management of Bronchiolitis
 CLINICAL PRACTICE GUIDELINE Diagnosis and Management of Bronchiolitis Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of All Children Subcommittee on
CLINICAL PRACTICE GUIDELINE Diagnosis and Management of Bronchiolitis Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of All Children Subcommittee on
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Pulmonary
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
BPD. Neonatal/Pediatric Cardiopulmonary Care. Disease. Bronchopulmonary Dysplasia. Baby Jane
 1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
RESPIRATORY EMERGENCIES. Michael Waters MD April 2004
 RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
USAID Health Care Improvement Project. pneumonia) respiratory infections through improved case management (amb/hosp)
 Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Simulation 1: Two Year-Old Child in Respiratory Distress
 Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES
 PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086)
 Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Chapter 10 Respiratory System J00-J99. Presented by: Jesicca Andrews
 Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
PNEUMONIA IN CHILDREN. IAP UG Teaching slides
 PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Fever in neonates (age 0 to 28 days)
 Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Common Pediatric Respiratory Illness and Emergencies
 Common Pediatric Respiratory Illness and Emergencies Rob Cloutier, MD Assistant Professor Emergency Medicine & Pediatrics Oregon Health & Science University Overview Review key differences between pediatric
Common Pediatric Respiratory Illness and Emergencies Rob Cloutier, MD Assistant Professor Emergency Medicine & Pediatrics Oregon Health & Science University Overview Review key differences between pediatric
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
HealthStream Regulatory Script
 HealthStream Regulatory Script [Transmission-Based Precautions: Contact and Droplet] Version: [April 2005] Lesson 1: Introduction Lesson 2: Contact Precautions Lesson 3: Droplet Precautions Lesson 1: Introduction
HealthStream Regulatory Script [Transmission-Based Precautions: Contact and Droplet] Version: [April 2005] Lesson 1: Introduction Lesson 2: Contact Precautions Lesson 3: Droplet Precautions Lesson 1: Introduction
Guidelines and Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide
 Guidelines Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide Patient Selection Diagnoses Patient presents with one or more of the following signs or symptoms of respiratory distress:
Guidelines Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide Patient Selection Diagnoses Patient presents with one or more of the following signs or symptoms of respiratory distress:
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient
 Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Children s Hospital Discuss when foreign body aspiration
Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Children s Hospital Discuss when foreign body aspiration
A Pediatrician's Perspective: How to be prepared for life's little cold and fu misadventures! Kathleen Leach, MD October 12, 2010 Swarthmore College
 A Pediatrician's Perspective: How to be prepared for life's little cold and fu misadventures! Kathleen Leach, MD October 12, 2010 Swarthmore College About the speaker Dr. Leach is a primary care pediatrician
A Pediatrician's Perspective: How to be prepared for life's little cold and fu misadventures! Kathleen Leach, MD October 12, 2010 Swarthmore College About the speaker Dr. Leach is a primary care pediatrician
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Infant and Pediatric Influenza. Mike Czervinske RRT-NPS University of Kansas Medical Center
 Infant and Pediatric Influenza Mike Czervinske RRT-NPS University of Kansas Medical Center Influenza Infants and Influenza Acute infection of the respiratory tract Nose Throat Possibly lungs Pathophysiology
Infant and Pediatric Influenza Mike Czervinske RRT-NPS University of Kansas Medical Center Influenza Infants and Influenza Acute infection of the respiratory tract Nose Throat Possibly lungs Pathophysiology
Bronchiolitis: Systematic Review with 3 Decades of Experience in Resource-limited Setting
 Cronicon OPEN ACCESS EC PAEDIATRICS Review Article Bronchiolitis: Systematic Review with 3 Decades of Experience in Resource-limited Setting Suraj Gupte* Professor and Head, Postgraduate Department of
Cronicon OPEN ACCESS EC PAEDIATRICS Review Article Bronchiolitis: Systematic Review with 3 Decades of Experience in Resource-limited Setting Suraj Gupte* Professor and Head, Postgraduate Department of
Nursing care for children with respiratory dysfunction
 Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
BRONCHIOLITIS IN CHILDREN Register No: Status: Public
 BRONCHIOLITIS IN CHILDREN Type: Policy Register No: 09052 Status: Public Developed in response to: Safeguarding Children Every Child Matters CQC Fundamental Standard: 9, 12, 13 Consulted With Post/Committee/Group
BRONCHIOLITIS IN CHILDREN Type: Policy Register No: 09052 Status: Public Developed in response to: Safeguarding Children Every Child Matters CQC Fundamental Standard: 9, 12, 13 Consulted With Post/Committee/Group
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
MASTER SYLLABUS
 MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Provincial Clinical Knowledge Topic Bronchiolitis, Infant Emergency and Inpatient V 1.0
 Provincial Clinical Knowledge Topic Bronchiolitis, Infant Emergency and Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Provincial Clinical Knowledge Topic Bronchiolitis, Infant Emergency and Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Facilitator s Guide. Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama. Active Learning Module
 Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
URIs and Pneumonia. Elena Bissell, MD 10/16/2013
 URIs and Pneumonia Elena Bissell, MD 10/16/2013 Objectives Recognize and treat community acquired PNA in children/adults Discern between inpatient and outpatient treatment of PNA Recognize special populations/cases
URIs and Pneumonia Elena Bissell, MD 10/16/2013 Objectives Recognize and treat community acquired PNA in children/adults Discern between inpatient and outpatient treatment of PNA Recognize special populations/cases
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Acute respiratory failure
 Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Wheeze. Respiratory Tract Symptoms. Prof RJ Green Department of Paediatrics. Cough. Wheeze/noisy breathing. Acute. Tight chest. Shortness of breath
 Wheeze Prof RJ Green Department of Paediatrics Respiratory Tract Symptoms Cough Tight chest Wheeze/noisy breathing Shortness of breath Acute Chronic Respiratory rate Most important sign of respiratory
Wheeze Prof RJ Green Department of Paediatrics Respiratory Tract Symptoms Cough Tight chest Wheeze/noisy breathing Shortness of breath Acute Chronic Respiratory rate Most important sign of respiratory
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE
 Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
INFLUENZA WHAT YOU NEED TO KNOW ARE YOU SURE YOU USE THE RIGHT MEASURES TO PROTECT YOURSELF AGAINST THE FLU?
 INFLUENZA WHAT YOU NEED TO KNOW ARE YOU SURE YOU USE THE RIGHT MEASURES TO PROTECT YOURSELF AGAINST THE FLU? GET INFORMED! GET VACCINATED! GET PROTECTED! FLU VACCINE WHAT IS INFLUENZA? Seasonal influenza
INFLUENZA WHAT YOU NEED TO KNOW ARE YOU SURE YOU USE THE RIGHT MEASURES TO PROTECT YOURSELF AGAINST THE FLU? GET INFORMED! GET VACCINATED! GET PROTECTED! FLU VACCINE WHAT IS INFLUENZA? Seasonal influenza
FEVER. What is fever?
 FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
PATHOLOGY & PATHOPHYSIOLOGY
 PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF THE RESPIRATORY SYSTEM DISORDERS OF THE RESPIRATORY SYSTEM Disorders of the Respiratory System Infections Degenerative Tumours Immune Trauma Congenital Upper respiratory
PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF THE RESPIRATORY SYSTEM DISORDERS OF THE RESPIRATORY SYSTEM Disorders of the Respiratory System Infections Degenerative Tumours Immune Trauma Congenital Upper respiratory
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
CHILDREN S SERVICES. Patient information Leaflet BRONCHIOLITIS
 CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
I tri r n i si s c E t x ri r n i si s c
 Problems with Oxygenation Lemone and Burke Chapter 36-39 39 Objectives Review anatomy and physiology of respiratory system. Describe changes associated with aging. Review O2 delivery systems Explain maintenance
Problems with Oxygenation Lemone and Burke Chapter 36-39 39 Objectives Review anatomy and physiology of respiratory system. Describe changes associated with aging. Review O2 delivery systems Explain maintenance
9/18/2010. Diagnostic Tests Pulse Oximetry Monitor O2 sat Normal % CBC Infection present? Oxygen carrying capacity?
 3 4 5 6 Problems with Oxygenation Lemone and Burke Chapter 36-39 Objectives Review anatomy and physiology of respiratory system. Describe changes associated with aging. Review O delivery systems Explain
3 4 5 6 Problems with Oxygenation Lemone and Burke Chapter 36-39 Objectives Review anatomy and physiology of respiratory system. Describe changes associated with aging. Review O delivery systems Explain
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory System. Respiratory System Overview. Component 3/Unit 11. Health IT Workforce Curriculum Version 2.0/Spring 2011
 Component 3-Terminology in Healthcare and Public Health Settings Unit 11-Respiratory System This material was developed by The University of Alabama at Birmingham, funded by the Department of Health and
Component 3-Terminology in Healthcare and Public Health Settings Unit 11-Respiratory System This material was developed by The University of Alabama at Birmingham, funded by the Department of Health and
Pediatric Respiratory Infections
 Pediatric Respiratory Infections Brenda Kelly PharmD BCPS Residency Program Director Virginia Mason Memorial, Yakima, Washington brendakelly@yvmh.org Disclosure The presenter has no actual or potential
Pediatric Respiratory Infections Brenda Kelly PharmD BCPS Residency Program Director Virginia Mason Memorial, Yakima, Washington brendakelly@yvmh.org Disclosure The presenter has no actual or potential
Phases of Respiration
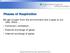 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Pulmonology Elective PL-1 Residents
 PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
RSV infection. Information about RSV and how you can reduce the risk of your child developing a severe infection.
 RSV infection Information about RSV and how you can reduce the risk of your child developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
RSV infection Information about RSV and how you can reduce the risk of your child developing a severe infection. What is RSV? RSV is one of the most common respiratory viruses and is spread easily. By
Bronchiolitis and its associated factors in pediatric hospital in Iraq, Diala (Albatool Teaching Hospital)
 International Journal of Advanced Research in Biological Sciences ISSN: 2348-8069 www.ijarbs.com DOI: 10.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 7-2018 Research Article DOI: http://dx.doi.org/10.22192/ijarbs.2018.05.07.021
International Journal of Advanced Research in Biological Sciences ISSN: 2348-8069 www.ijarbs.com DOI: 10.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 7-2018 Research Article DOI: http://dx.doi.org/10.22192/ijarbs.2018.05.07.021
