Environmental Medicine Article
|
|
|
- Ashlynn Colleen Kennedy
- 5 years ago
- Views:
Transcription
1 Article Respiratory Morbidity in Office Workers in a Water-Damaged Building Jean M. Cox-Ganser, 1 Sandra K. White, 1 Rebecca Jones, 1 Ken Hilsbos, 1 Eileen Storey, 2 Paul L. Enright, 1 Carol Y. Rao, 1 and Kathleen Kreiss 1 1 Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, Morgantown, West Virginia, USA; 2 University of Connecticut Health Center, Farmington, Connecticut, USA We conducted a study on building-related respiratory disease and associated social impact in an office building with water incursions in the northeastern United States. An initial questionnaire had 67% participation (888/1,327). Compared with the U.S. adult population, prevalence ratios were for wheezing, lifetime asthma, and current asthma, 3.3 for adult-onset asthma, and 3.4 for symptoms improving away from work (p < 0.05). Two-thirds (66/103) of the adult-onset asthma arose after occupancy, with an incidence rate of 1.9/1,000 person-years before building occupancy and 14.5/1,000 person-years after building occupancy. We conducted a second survey on 140 respiratory cases, 63 subjects with fewer symptoms, and 44 comparison subjects. Healthrelated quality of life decreased with increasing severity of respiratory symptoms and in those with work-related symptoms. Symptom status was not associated with job satisfaction or how often jobs required hard work. Respiratory health problems accounted for one-third of sick leave, and respiratory cases with work-related symptoms had more respiratory sick days than those without work-related symptoms (9.4 vs. 2.4 days/year; p < 0.01). Abnormal lung function and/or breathing medication use was found in 67% of respiratory cases, in 38% of participants with fewer symptoms, and in 11% of the comparison group (p < 0.01), with similar results in never-smokers. Postoccupancy-onset asthma was associated with less atopy than preoccupancy-onset asthma. Occupancy of the water-damaged building was associated with onset and exacerbation of respiratory conditions, confirmed by objective medical tests. The morbidity and lost work time burdened both employees and employers. Key words: building-related symptoms, hypersensitivity pneumonitis, indoor environment, occupational asthma, office workers, quality of life, sarcoidosis, sick leave. Environ Health Perspect 113: (2005). doi: /ehp.7559 available via [Online 20 January 2005] As part of a program to study occupational respiratory disease in the nonindustrial environment, we investigated building-related respiratory health in the employees of a large 20-story office building in the northeastern United States. Since the mid-1990s, the building had leaked through the roof, around windows, and through sliding doors of terraces. The upper floors had suffered the most water damage and mold contamination. During investigation of these problems, the building was found to be operating at a negative pressure with respect to the outdoors, which could exacerbate water incursion through the building envelope. Furthermore, there had been plumbing leaks on many floors which had damaged interior walls. The first major construction activity related to water incursion began in 2000, with repair of roof copings and brick caulking. From 2000 to 2002, cubicle partitions and carpets were cleaned, wetted carpet and stained wallboard replaced, wallpaper and underlying mold removed from bathrooms, upgrades to the air handling system made, and windows caulked. In 2002, permanent repairs on the building exterior, including roof replacement, began to prevent water incursion. Building occupants had reported health conditions that they considered building related. Symptom onset spanned several years, with an increase in symptoms and frequency of complaints beginning in the fall of Sentinel cases of postoccupancy-onset asthma, hypersensitivity pneumonitis (HP), and sarcoidosis had been diagnosed, and the persons affected had been relocated to another facility. HP is an immune-regulated granulomatous disease that has been associated with fungal contamination, and it has been found to coexist with asthma in damp office buildings (Arnow et al. 1978; Kreiss 1989; Hoffman et al. 1993; Jarvis and Morey 2001). Sarcoidosis is an immune-regulated granulomatous disease of unknown etiology. In this article we report evidence of excesses of respiratory symptoms and physician diagnosis of asthma in the occupants of the water-damaged building as well as verification of self-reported respiratory illness with objective testing. We also describe the burden of illness in terms of absences, use of breathing medications, and health-related quality of life. Methods and Materials Study design and population. In September 2001, we offered a questionnaire to all 1,327 employees working in the building. The questionnaire was administered to groups of approximately 50 employees at a time, using schedules prepared by management. During each group session, National Institute for Occupational Safety and Health (NIOSH) staff described the purpose of the survey and the consent process and read the questions aloud from overhead transparencies as the participants completed them. By completing the questionnaire, the participants were indicating consent to take part in the survey. The questionnaire comprised sections on demographics; symptoms (upper and lower respiratory, systemic, headache, and difficulty concentrating) in the last 4 weeks and 12 months, and in relation to being in the building; physician diagnosis of asthma, HP, and sarcoidosis, with dates of diagnosis; smoking history; and work history in the building. The completed questionnaires were electronically scanned into a database and hand-checked for quality control. We used the September questionnaire to identify a group of employees who had worked in the building for at least 1 year and who met either an epidemiologic case definition for lower respiratory illness or a comparison group definition. The respiratory case definition was three or more of five lower respiratory symptoms (wheeze/whistling in the chest, chest tightness, shortness of breath, coughing, awakening by attack of breathing difficulty) occurring weekly over the past month; or at least two of three symptoms consistent with HP (shortness of breath when hurrying on level ground or walking up a slight hill, fever and chills, flulike achiness or achy joints) occurring weekly over the past month; or current asthma with postoccupancy physician diagnosis, or physician-diagnosed HP or sarcoidosis. The comparison group definition was none of the respiratory case lower respiratory or HP-like symptoms in the past year and none of the respiratory case diagnoses. We invited the 202 employees who met the case definition and the 154 employees who met the comparison group definition to participate in a questionnaire and medical testing survey in June During the site visit, an additional 15 employees asked to take part in the survey. All participants provided written informed consent (approved by the NIOSH Address correspondence to J.M. Cox-Ganser, National Institute for Occupational Safety and Health, Suite H- 2800, 1095 Willowdale Rd., Morgantown, WV USA. Telephone: (304) Fax: (304) jjc8@cdc.gov The authors declare they have no competing financial interests. Received 8 September 2004; accepted 19 January Environmental Health Perspectives VOLUME 113 NUMBER 4 April
2 Cox-Ganser et al. Human Subjects Review Board). We used results of the June questionnaire to reclassify participants into the respiratory case or comparison groups. Participants who reported lower respiratory or systemic symptoms but who did not meet the criteria of a respiratory case formed a third, fewer symptoms group. Questionnaire. Participants completed an interviewer-administered computer-based questionnaire. The June 2002 questionnaire included sections on demographics, work history, health and symptom history, physician diagnoses, smoking, home environment, and job stress and satisfaction as used in the U.S. Environmental Protection Agency (EPA) Building Assessment Survey and Evaluation (BASE) study (U.S. EPA 1994), and healthrelated quality of life from the SF-12 (Medical Outcomes Study, Short Form; Ware et al. 1996). We included questions on the use of beta-agonist and corticosteroid inhalers, overthe-counter breathing medications, and other asthma medications in the previous 4 weeks, as well as oral corticosteroid use in the previous 12 months, adapted from an asthma-severity score module (Blanc et al. 1996). To help with recall, participants were asked to bring to their testing session a list of the medications that they were taking for breathing problems. Spirometry. Qualified technicians followed standard guidelines for spirometry (American Thoracic Society 1995). We compared the test results to expected values for a healthy, nonsmoking person of the same age, height, sex, and race using spirometry reference values and 95% normal confidence intervals (CIs) generated from the third National Health and Nutrition Examination Survey (NHANES III) (Hankinson et al. 1999). Abnormal test results were categorized as having a pattern of obstruction, restriction, or a mixed pattern of both airways obstruction and a low forced vital capacity (FVC) (American Thoracic Society 1995). We defined airways obstruction as a low forced expiratory volume in 1 sec (FEV 1 ) to FVC ratio (FEV 1 /FVC%) with low FEV 1. We defined restriction as a low FVC and normal FEV 1 /FVC%. Methacholine challenge testing. To detect bronchial hyperresponsiveness (BHR), we performed methacholine challenge testing Table 1. Demographics of 888 participants in the September 2001 questionnaire survey. Proportion Characteristic or measure Female (%) 59 Age [years (mean ± SD)] 46 ± 9 Race (%) White 74 Black 19 Hispanic 6 Building occupancy [years (mean ± SD)] 6 ± 2 Current smoker (%) 14 Never smoker (%) 62 (MCT) using standardized techniques (Crapo et al. 2000) with 0.125, 0.5, 2, 8, and 32 mg/ml methacholine. Five breaths of nebulized methacholine were administered for each dose, with FEV 1 measured 30 and 90 sec later. If FEV 1 dropped > 20% of the baseline value, no further methacholine was given. We report methacholine dose as PC 20, which is the provocative concentration of methacholine that causes an interpolated 20% decline in FEV 1 from the baseline. We defined BHR as a PC 20 of 4.0 mg/ml, and borderline BHR as a PC 20 between 4.1 and 16.0 mg/ml (Crapo et al. 2000). Bronchodilator testing. In subjects with baseline FEV 1 < 70% of the predicted value, MCT was not performed, but a bronchodilator test was performed to detect any reversible bronchoconstriction. Two puffs of a beta-agonist were administered via metered dose inhaler and were followed by spirometry. We defined reversibility as a 12% and 200 ml FEV 1 improvement after bronchodilator administration (American Thoracic Society 1991). Allergen skin prick testing. We applied extracts of seven common indoor and outdoor allergens and three mold mixes using the GreerPIK system (Greer Laboratories, Lenoir, NC): dust mite mix (Dermatophagoides farinae and D. pteronyssinus), German cockroach (Blattella germanica), cat hair, seven grass mix, ragweed mix, common weed mix, Eastern eight tree mix, Dematiaceae mix (outdoor molds: Alternaria tenuis, Cladosporium herbarum, Helminthosporium sativum, Pullularia pullulans, Spondylocladium atrovirens, Curvularia spicifera), Aspergillus mix, and Penicillium mix. The negative control was 50% glycerin in water, and histamine served as a positive control. For each wheal, the mean diameter (average of the length and width) at 15 min was calculated. We defined a positive reaction as an average diameter at least 3 mm larger than the negative control and > 25% of the average diameter of the positive control. For the purposes of this study, atopy was defined as at least one positive skin test on allergy testing, using a total of seven common antigen extracts (excluding the mold mixes). Data analysis. We compared the prevalence rates of respiratory symptoms and self-reported medical diagnoses observed in the building occupants during the September 2001 survey to the U.S. adult prevalence rates obtained from NHANES III [National Center for Health Statistics (NCHS) 1996], the 2001 data for Connecticut from the Behavioral Risk Factor Surveillance System (BRFSS) (National Center for Chronic Disease Prevention and Health Promotion Behavioral Risk Factor Surveillance System 2001), and data for occupants of 41 office buildings with no known indoor environmental problems (Apte et al. 2000). For comparisons with NHANES III, we used indirect standardization for race (black, Hispanic, white), sex, age (17 39 years of age versus years of age), and cigarette smoking status (current, former, or never smoker). For comparisons with BRFSS, we standardized for sex. We derived 95% CIs using a method that assumes that the observed data are from a Poisson distribution (Kahn 1989). To estimate incidence density rates of physician-diagnosed adult-onset asthma, for each participant we calculated person-time at risk for two time periods: from 16 years of age to building occupancy and from building occupancy to the September 2001 survey date. For subjects with physician-diagnosed adult-onset asthma, time at risk ended on the date of diagnosis. Time at risk for each participant was summed to give person-years at risk. Participants with childhood asthma did not contribute any time at risk. We used SAS software (version 8.02; SAS Institute Inc. Cary, NC) to analyze the data. Chi-square tests were used in statistical analysis of two-way classification tables. We used the Cochran-Mantel-Haenszel test in analysis of differences between proportions after adjustment for smoking, and we used the Cochran-Armitage test in analysis for linear trends in proportions. We used the SAS GLM procedure to model number of days lost and Duncan s multiple range test for multiple means comparisons. Results September 2001 Survey Participation. Participation was 67% (888/1,327) in the cross-sectional questionnaire study. Participants were predominantly Table 2. Comparison of health outcomes prevalences with NHANES III (NCHS 1996). Building Prevalence Standardized questions prevalence [% (n)] ratio 95% CI Asthma ever 17.7 (143/810) Asthma current 12.8 (103/804) Wheezing or whistling in your chest in the last 12 months 35.9 (291/811) Stuffy, itchy, or runny nose in the last 12 months a 79.3 (643/811) Watery, itchy eyes in the last 12 months 63.4 (510/804) Wheezing, nose, or eye symptoms better on days off work 72.1 (468/649) The prevalence ratios were adjusted for age, sex, race, and smoking category; missing information on these characteristics led to comparisons based on fewer than the total 888 participants. a Our question included sneezing. 486 VOLUME 113 NUMBER 4 April 2005 Environmental Health Perspectives
3 Respiratory morbidity in office workers white, in their mid-forties, former or never smokers, who had been working in the building for about 6 years (Table 1). We had demographic and participation information on the 689 employees working for one of the two building tenant organizations. These employees had a mean age of 45 years, and 74% were white, 19% were black, and 53% were female. There was 76% participation among these employees. Comparison between participants and nonparticipants showed no differences in mean age or race. There were proportionately more females among participants than among nonparticipants (57% vs. 40%, p < 0.01). Excess respiratory symptoms and physiciandiagnosed asthma. In comparisons with the U.S. adult population, prevalence ratios ranged from 2.2 to 2.5 for wheezing, lifetime asthma, and current asthma (p < 0.05; Table 2). Nasal and eye symptoms were more prevalent in the building occupants than lower-respiratory symptoms, but were less elevated compared to U.S. adults (prevalence ratios 1.5 and 1.6, respectively, p < 0.05). The building occupants reported wheeze, nasal, or eye symptoms that improved when they were away from work at 3.4 times the rate of the U.S. population (p < 0.05). Compared to the state adult population, prevalence ratios were 1.4 (95% CI, ) for lifetime asthma, and 1.5 (95% CI, ) for current asthma. A majority (60 70%) of participants with wheeze, chest tightness, shortness of breath, or cough in the last 4 weeks reported an improvement in symptoms when away from the building. Prevalence ratios for work-related lower respiratory symptoms compared to U.S. office workers were elevated and ranged from 2.7 to 4.7 (p < 0.05; Table 3). Adult onset asthma prevalence and incidence. The prevalence of adult-onset asthma was 12% (103/865). A comparison to the U.S. adult population gave a prevalence ratio of 3.3 (95%, CI ). Two-thirds (66/103) of the adult-onset asthma occurred after occupancy of the building. An analysis of adultonset asthma incidence density was conducted based on 19,173 person-years at risk before building occupancy and 4,564 person-years at risk after building occupancy. We found incidences of 1.9 per 1,000 person-years in the period before building occupancy and 14.5 per 1,000 person-years in the period after building occupancy. The incidence rate ratio was 7.5, indicating a large increase in asthma incidence in the period after building occupancy. Asthma symptom severity and exacerbation. The participants with postoccupancyonset, physician-diagnosed asthma had a higher mean value for the sum of cough, wheeze, chest tightness, and shortness of breath occurring once or more per week in the last 4 weeks than any other participants (p < 0.05). There was also a significant trend (p < 0.01) in prevalence of lower respiratory symptoms that improved when away from the building: 52% of those with postoccupancy-onset asthma, 41% of those with adult preoccupancy-onset asthma, 27% of those with childhood asthma, and 23% of those with no physician-diagnosed asthma (Table 4). HP and sarcoidosis. Eight participants reported HP, five with postoccupancy-onset and one with preoccupancy-onset HP (two people did not give diagnosis dates). Sarcoidosis was reported by six participants, three with postoccupancy onset, and two with preoccupancy onset (one person did not give a date of diagnosis). Fever and chills were reported as occurring once or more in the last 4 weeks by 9%, flulike achiness or achy joints by 22%, and excessive fatigue by 29% of participants. A work-related pattern was noted by 22% of those with fever and chills, by 30% of those with flulike achiness or achy joints, and by 52% of those with excessive fatigue. June 2002 Survey Participation. There were 248 participants in the June 2002 survey. Participation was higher among the invited employees meeting the respiratory case definition in September 2001 (142/202; 70%) than among the comparison group invitees (91/154; 59%). Based on the June 2002 questionnaire results, there were 140 participants in the respiratory case group, 63 participants in the fewer symptoms group, and 44 participants in the comparison group. One participant had missing questionnaire information and could not be classified. A little more than half of those asymptomatic in September 2001 reported symptoms 9 months later, with 17% achieving respiratory case status, and 38% falling into the fewer symptoms group. In contrast, a majority (81%) of those meeting the respiratory case definition in September 2001 still met this definition 9 months later, 17% fell into the intermediate group, and 2% became asymptomatic. The demographics of the June 2002 participants stratified by respiratory status are given in Table 5. There were more females and more current smokers in the respiratory case group. Lung function tests, breathing medication use, and reported respiratory health. Respiratory cases had the highest proportions of abnormal breathing tests and breathing medication use; the fewer symptoms group had the next highest; and the comparison group had the lowest proportions of these two outcomes (Tables 6 and 7). Test results indicated more obstruction than restriction, and the respiratory cases had a trend for a higher prevalence of obstruction than the other participants. BHR was higher in the two groups with symptoms than in the comparison group, but this finding was not significantly different. Table 3. The prevalence of work-related lower respiratory symptoms that occurred frequently in the previous 4 weeks, compared to U.S. office workers. Prevalence (%) Prevalence ratio a 95% CI Wheezing Coughing attacks Chest tightness Shortness of breath a The prevalence of the 888 study participants compared with results from 41 nonproblem buildings (Apte et al. 2000). Table 4. Mean number of lower respiratory symptoms and prevalence of work-related symptoms in the last 4 weeks by asthma status and onset period. Preoccupancy Postoccupancy- adult-onset Childhood-onset No reported onset asthma asthma asthma asthma Number of lower respiratory 1.7 ± 1.6 A 1.1 ± 1.3 B 0.7 ± 1.3 B,C 0.5 ± 0.9 C symptoms (mean ± SD) a Work-related lower 34/66 (52) 15/37 (41) 8/30 (27) 169/731 (23) respiratory symptoms [n (%)] Lower respiratory symptoms include wheeze, cough, chest tightness, and shortness of breath. a Means with the same letter are not significantly different at α = 0.05, using Duncan's multiple-range test. Cochran- Armitage trend test p < Table 5. Demographics of June 2002 participants by respiratory symptom status. Respiratory case Fewer symptoms Comparison group (n = 140) group (n = 63) group (n = 44) Female (%) Age [years (mean ± SD)] 47 ± 8 46 ± 9 46 ± 8 Occupancy duration [years (mean ± SD)] 7 ± 2 7 ± 2 7 ± 2 Current smoker (%) Never smoker (%) Due to missing values, age and duration of occupancy in respiratory case group are based on 137 participants. For age, n = 62 in the fewer symptoms group and n = 42 in the comparison group. p = by Chi-square test on sex. Environmental Health Perspectives VOLUME 113 NUMBER 4 April
4 Cox-Ganser et al. We found very little breathing medication use reported by the comparison group as compared to almost half of the respiratory cases. Analyses on the never-smokers showed similar trends, with a prevalence of abnormal lung function tests and medication use combined of 71% for respiratory cases, 30% for participants with fewer symptoms, and 12% for the comparison group. Quality of life. We compared responses to health-related quality-of-life questions among the three symptom status groups. We found statistically significant trends for increasing impairment in health-related quality of life with increasing severity of respiratory symptoms. The largest differences were seen for reported physical limitations (Figure 1). Within the respiratory case and the fewer symptoms groups, we found statistically significant poorer health-related quality of life in relation to the presence of work-related symptoms, except for general health status (Figure 2). Similar results were found for health-related quality of life and postoccupancy symptom onset, except that statistical differences were seen for limitations in climbing stairs, physical health-limiting s, and physical health limiting the kind of activities. Job stress/dissatisfaction. There were no statistical differences among symptom status groups for responses on job satisfaction or how often a person was required to work hard. Being very or somewhat satisfied with their job was reported by 87% of respiratory cases, 90% of the group with fewer symptoms and 93% of the comparison group. Being required to work hard frequently or very often was reported by 51% of respiratory cases, 62% of the intermediate group, and 45% of the comparison group. Work days lost. The number of days off work in the last 12 months due to respiratory problems was significantly associated with symptom status (p < 0.01). The respiratory cases had missed a mean of 6.9 days as compared to 1.7 days for the group with fewer symptoms and 2.0 days for the asymptomatic group. We found that 34% of respiratory cases had 6 days of respiratory sick leave, compared to 11% of the fewer symptoms group and 4.7% of the asymptomatic comparison group (p < 0.01). In contrast, there was no statistically significant difference between the three groups for nonrespiratory sick leave. The respiratory cases lost a mean of 4.5 days, the group with fewer symptoms lost 7.5 days, and the asymptomatic group lost 4.1 days due to nonrespiratory conditions. The number of respiratory sick days was similar for symptomatic participants regardless of whether the onset was pre- or postoccupancy. A large effect was seen for having respiratory symptoms that improved away from the building. Respiratory cases with work-related respiratory symptoms had more respiratory sick days than those with symptoms that did not improve away from the building (9.4 vs. 2.4, p < 0.01). In the group with fewer symptoms, those with work-related respiratory symptoms had more respiratory sick leave than those with symptoms with no work-related pattern (3.7 vs. 1.1, p < 0.05). We estimated sick days over the past year for respiratory conditions and total sick leave for building occupants by applying the mean work days missed for the three symptom groups to the number of participants in those categories from the September 2001 questionnaire (816 participants had adequate data). Respiratory health problems accounted for 34% of sick leave days (2,490/7,402). The respiratory case group represented 25% of the September 2001 participants but contributed 56% (1,401/2,490) of the respiratory sick leave days. Using the mean of 2 days of respiratory sick leave reported by the comparison group as a non building-related baseline for building occupants gives an estimated 858 days of excess respiratory sick leave (2,490 1,632). Thus, up to 12% (858/7,402) of the preceding 12 months of employee sick leave days might have been attributable to buildingrelated effects. Breathing medication use. We looked at the prevalence of the use of asthma-controller medications (inhaled corticosteroids, cromolyn, nedocromil, oral antileukotrienes) and reliever medications (short-acting beta-agonists and ipratropium bromide) in the last 4 weeks in participants with physician-diagnosed asthma for comparison with a national sample of 1,788 U.S. adults with current asthma Table 7. Medication usage and combined medication usage and abnormal lung function [% (n)] stratified by symptom status in June Respiratory Fewer Comparison cases group a symptoms group Any medication for breathing problems 46 (65/140) 13 (8/63) 2 (1/44) Oral steroids 21 (29/140) 8 (5/63) 2 (1/44) Inhaled steroids 19 (27/140) 2 (1/63) 0 (0/44) Beta-agonists 28 (39/140) 2 (1/63) 0 (0/44) Positive for any medication for breathing problems or 67 (83/124) 38 (21/55) 11 (4/37) an abnormal lung function test a Across all rows there were significant Cochran-Armitage trend tests (p < 0.01); the significant differences by symptom status remained after adjusting for smoking category (Cochran-Mantel-Haenszel tests; p < 0.01). Table 6. Breathing test results for participants, stratified by symptom status in June Variable Respiratory cases group Fewer symptoms group Comparison group Spirometry testing [% (n)] a Abnormal 24 (31/131) b 13 (8/62) 7 (3/42) Obstructed or mixed 15 (20/131) 6 (4/62) 7 (3/42) Restriction (low FVC) 8 (11/131) 6 (4/62) 0 (0/42) Percent predicted FEV 1 (mean ± SD) 92 ± 16 c 96 ± ± 12 Percent predicted FVC (mean ± SD) 94 ± 14 d 97 ± ± 11 Methacholine challenge testing [% (n)] Abnormal (< 16 mg/ml) 19 (19/99) 20 (10/51) 6 (2/36) < 4 mg/ml (BHR) 6 (6/99) 8 (4/51) 0 (0/36) > 4 and < 16 mg/ml (borderline BHR) 13 (13/99) 12 (6/51) 6 (2/36) Bronchodilator testing positive [% (n)] 18 (2/11) ND ND Abnormal methacholine challenge or bronchodilator tests [% (n)] 19 (21/110) 20 (10/51) 6 (2/36) Any abnormal lung function test [% (n)] e 39 (44/114) f 29 (16/55) 11 (4/37) ND, not done. a Two invalid tests by the symptomatic participants were not included. b Across the row there was a significant Cochran-Armitage trend test (p < 0.01); the significant differences by symptom status remained after adjusting for smoking category (Cochran-Mantel-Haenszel test; p < 0.05). c In a linear regression model adjusting for smoking category, there was a significant effect of symptom status (p < 0.01); the group meeting the respiratory case definition had a lower mean percent predicted FEV 1 than either of the other two groups. d In a linear regression model adjusting for smoking category, there was a significant effect of symptom status (p < 0.01); the group that met the respiratory case definition had a lower mean percent predicted FVC than the asymptomatic group. e Participants who had either a negative spirometry or a negative methacholine/bronchodilator test and who had not done the other tests were excluded. f Across the row there was a significant Cochran-Armitage trend test (p < 0.01); the significant differences by symptom status remained after adjusting for smoking category (Cochran-Mantel-Haenszel test; p < 0.01). 488 VOLUME 113 NUMBER 4 April 2005 Environmental Health Perspectives
5 Respiratory morbidity in office workers (Adams et al. 2002; Fuhlbrigge et al. 2002) using two-sample tests of proportions. Use of an asthma controller was reported by 39% of our study group versus 21% of U.S. asthma cases overall (p < 0.01). The prevalence of 39% asthma-controller use was marginally higher (p = 0.07) than the value of 29% reported for U.S. cases with severe persistent symptoms in the last 4 weeks. Reliever use was reported by 50% of our group versus 63% of U.S. cases (p < 0.05). Skin prick allergy tests. Over half of the participants met the definition for atopy. There was no statistical difference in the prevalence of atopy among the respiratory case group, the group with fewer symptoms, and the comparison group. However, preoccupancy-onset asthma was associated with a higher prevalence of atopy (p < 0.05). The results of individual skin prick allergen tests showed that persons with preoccupancy-onset asthma had a higher prevalence of positive reactions to cat, dust mites, and weed mix (p < 0.01) as well as to cockroach allergens (p < 0.05). We found that the postoccupancy-onset asthma cases had the lowest reaction to the mold mixes (p = 0.05; Figure 3). Discussion Physician-diagnosed asthma and respiratory symptoms occurred in excess among our study participants and was confirmed by an excessive rate of airway obstruction and BHR. Studies of building occupants with known health concerns are subject to reporting bias. In our study, in addition to reported symptoms Percentage General health fair to poor Respiratory cases group Fewer symptoms group Comparison group Emotional health has limited the kind of activities Emotional health has limited Physical health has limited the kind of activities Physical health has limited Limited in climbing stairs Limited in moderate activity Figure 1. Quality-of-life comparisons among symptom groups. p < 0.01, Cochran-Armitage trend test. and physician diagnoses, we examined measures of respiratory disease, including medication use and medical tests. Two-thirds of those classified as respiratory cases based on symptoms or physician diagnoses had objective pulmonary function abnormalities or used prescription medications for breathing difficulties (given with the goal of normalizing lung function). The higher rate of lung function abnormalities and breathing medication use in the participants reporting respiratory symptoms validates the symptom reports. The majority (60 70%) of participants with respiratory symptoms reported a workrelated pattern, implying a building-related exposure. The 7% overall prevalence of workrelated wheeze was higher than the 2 4% in studies of nonproblem buildings (Apte et al. 2000) and higher than the 2 6% found in studies of problem buildings (Malkin et al. 1996). In the 9-month interval between the building-wide questionnaire survey and the nested case control survey, more than half (55%) of the comparison group chosen because they had no lower respiratory or systemic symptoms in September 2001 had become symptomatic, including 17% who were classified as respiratory cases. Improvement was rare in September 2001 cases (17%), suggesting a continued effect of building occupancy on respiratory health. Some of this response pattern may be attributable to overreporting due to general concern about water incursions and sentinel cases with health effects, but such Percentage General health fair to poor Symptoms better away from work No work-related symptoms Emotional health has limited the kind of activities Emotional health has limited Physical health has limited the kind of activities Physical health has limited Figure 2. Quality of life in the respiratory case group and the fewer symptoms group, stratified by work-relatedness of symptoms. p < 0.05 and p < 0.01, Chi-square test. Limited in climbing stairs Limited in moderate activity concerns had been present since before the September 2001 survey. The estimated incidence of physiciandiagnosed, adult-onset asthma among the study participants (1.9 per 1,000 person-years) before building occupancy was within the range of other estimates for adults, for example, 2.1 per 1,000 person-years (McWhorter et al. 1989), 3.8 per 1,000 person-years (Sama et al. 2003), and about 1 per 1,000 personyears (Reed 1999). In contrast, after building occupancy, incidence rose 7.5 times to 14.5 per 1,000 person-years, consistent with the symptoms that developed in the previously asymptomatic comparison group. The burden of respiratory problems in this population was reflected in substantial respiratory sick leave attributable to building occupancy (estimated at 12% of total). The presence of work-related respiratory symptoms was positively associated with respiratory sick leave, but time of symptom onset was not, suggesting that having a work-related pattern to respiratory symptoms was a larger determinant of respiratory sick leave than whether the symptoms arose before or after building occupancy. The proportion of our study respiratory cases with 6 days of respiratory sick leave was 34%. In comparison, a population study of 1,788 adults with asthma in the United States found that 11% of participants had 6 days of sick leave in the past year related to their asthma (Fuhlbrigge et al. 2002). In our Percentage skin prick positive Grasses No reported asthma Pre occupancy-onset asthma Post occupancy-onset asthma Trees Ragweed Roach Figure 3. Allergy skin test results by asthma diagnosis. p < 0.05 and p < 0.01, Chi-square test. Weeds Dust mites Cat Atopic Molds Environmental Health Perspectives VOLUME 113 NUMBER 4 April
6 Cox-Ganser et al. study, respiratory cases had a mean of 6.9 respiratory sick days, compared to 4.4 annual work absences because of breathing problems among Canadian asthmatics (Ungar and Coyte 2000). In the Canadian study more productivity was lost due to a decrease in level of functioning at work on days when breathing problems were worse than usual than due to days off work. Although we have no estimate of productivity loss due to a decrease in functioning at work for our study participants, the high prevalence of work-related symptom exacerbation suggests a substantial decrease in productivity might have occurred. High respiratory morbidity was also indicated by the high use of asthma-controller medication and the decreased prevalence of quick-relief medications. This pattern of medication use is consistent with persistent asthma associated with daily work-related exacerbation. We found strong associations between respiratory symptom status and lower healthrelated quality of life, confirming the social burden of respiratory morbidity in building occupants. In contrast, we found no relation between job stress, job satisfaction, or perceived work burdens with symptom status; this is consistent with the findings of another investigation of building-related respiratory disease (Jarvis and Morey 2001) and reduces the likelihood that disgruntled employees in a problem building exaggerate their symptoms. The specific etiology and mechanisms of the respiratory disease in this building remain undefined. The skin prick test results for immediate hypersensitivity responses to common aeroallergens were unexpected. Preoccupancyonset asthma was associated with atopy, as anticipated [National Asthma Education and Prevention Program (NAEPP) 1997; Peden 2000]. However, postoccupancy-onset asthma cases had much lower prevalence of IgEmediated allergen skin-test positivity (atopy). Perhaps the airway inflammation was not driven by an IgE mechanism. It is possible that nonbiologic irritant exposures were present, and furthermore, although molds have allergenic properties (Lander et al. 2001), the development of asthma in damp/moldy conditions may not be IgE mediated (Douwes et al. 2003; Savilahti et al. 2001). The rarity of clusters of HP in the general population points to a work-related etiology for the cluster in the building occupants. The recent Institute of Medicine report on damp indoor spaces and health found sufficient evidence for an association between mold or other agents in damp indoor environments and upper respiratory tract symptoms, cough, wheeze, asthma symptoms in sensitized persons, and HP in susceptible persons (Institute of Medicine 2004). The cluster of sarcoidosis raises concern that this granulomatous lung disease was misdiagnosed HP (Forst and Abraham 1993) or has overlapping environmental causes (Kucera et al. 2003). The major limitation of the present study is the possible influence of participation bias. We had a 67% participation in our September 2001 survey, and differences in health status of participants and nonparticipants could have led to overestimation of symptom and asthma prevalence, particularly since women were more likely to be participants. Using the most conservative approach, we compared minimum possible prevalences among the entire building population to the external reference populations. We still found excesses of asthma and symptoms in comparison to the U.S. population and to office workers in buildings not known to have indoor environmental problems (data not shown), but we found no differences in asthma prevalence in comparison to the state population. Counterbalancing possible response bias among those occupants who participated in our study is our finding of gradients of nonsubjective tests and reported medication use in relation to symptom intensity. In conclusion, the present study contributes to the growing literature that waterdamaged buildings can be associated with work-related respiratory disease. This investigation documents the considerable respiratory illness, adverse effects on quality of life, and absenteeism that have placed personal, social, and economic burdens on many employees and their employers. Building-related respiratory disease warrants increased public health, medical research, and policy attention. REFERENCES Adams RJ, Fuhlbrigge A, Guilbert T, Lozano P, Martinez F Inadequate use of asthma medication in the United States: results of the Asthma in America national population survey. J Allergy Clin Immunol 110: American Thoracic Society Lung function testing: selection of reference values and interpretative strategies. Am Rev Respir Dis 144: American Thoracic Society Standardization of Spirometry, 1994 Update. Am J Respir Crit Care Med 152: Apte MG, Fisk WJ, Daisey JM Associations between indoor CO 2 concentrations and sick building syndrome symptoms in US office buildings: an analysis of the BASE study data. Indoor Air 10: Arnow PM, Fink JN, Schlueter DP, Barboriak JJ, Mallison G, Said SI, et al Early detection of hypersensitivity pneumonitis in office workers. Am J Med 64: Blanc PDM, Cisternas MM, Smith SB, Yelin EHP Asthma, employment status, and disability among adults treated by pulmonary and allergy specialists. Chest 109: Crapo RO, Casaburi R, Coates AL, Enright PL, Hankinson JL, Irvin CG, et al Guidelines for methacholine and exercise challenge testing Am J Respir Crit Care Med 161: Douwes J, Thorne P, Pearce N, Heederik D Bioaerosol health effects and exposure assessment: progress and prospects. Ann Occup Hyg 47: Forst LS, Abraham J Hypersensitivity pneumonitis presenting as sarcoidosis. Br J Ind Med 50: Fuhlbrigge AL, Adams RJ, Guilbert TW, Grant E, Lozano P, Janson SL, et al The burden of asthma in the United States level and distribution are dependent on interpretation of the National Asthma Education and Prevention Program guidelines. Am J Respir Crit Care Med 166: Hankinson JL, Odencrantz JR, Fedan KB Spirometric reference values from a sample of the general US population. Am J Respir Crit Care Med 159: Hoffman RE, Wood RC, Kreiss K Building-related asthma in Denver office workers. Am J Public Health 83: Institute of Medicine. Damp Indoor Spaces and Health Washington, DC:National Academy Press. Jarvis JQ, Morey PR Allergic respiratory disease and fungal remediation in a building in a subtropical climate. Appl Occup Environ Hyg 16: Kahn HA, Sempos CT Statistical Methods in Epidemiology. New York:Oxford University Press. Kreiss K The epidemiology of building-related complaints and illness. Occup Med 4: Kucera GP, Rybicki BA, Kirkey KL, Coon SW, Major ML, Maliarik MJ, et al Occupational risk factors for sarcoidosis in African-American siblings. Chest 123: Lander F, Meyer HW, Norn S Serum IgE specific to indoor moulds, measured by basophil histamine release, is associated with building-related symptoms in damp buildings. Inflamm Res 50: Malkin R, Wilcox T, Sieber WK The National Institute for Occupational Safety and Health indoor environmental evaluation experience. Part two: symptom prevalence. Appl Occup Environ Hyg 11: McWhorter WP, Polis MA, Kaslow RA Occurrence, predictors, and consequences of adult asthma in NHANESI and follow-up survey. Am Rev Respir Dis 139: NAEPP Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma. NIH Publication no Washington, DC:National Asthma Education and Prevention Program. National Center for Chronic Disease Prevention and Health Promotion Behavioral Risk Factor Surveillance System. Prevalence Data. Available: gov/brfss/. [accessed 12 March 2004]. NCHS Third National Health and Nutrition Examination Survey, , NHANES III Laboratory Data File. Public use data file documentation no (CD ROM). Hyattsville, MD:National Center for Health Statistics. Peden DB Development of atopy and asthma: candidate environmental influences and important periods of exposure. Environ Health Perspect 108(suppl 3): Reed CE The natural history of asthma in adults: the problem of irreversibility. J Allergy Clin Immunol 103: Sama SR, Hunt PR, Cirillo CI, Marx A, Rosiello RA, Henneberger PK, et al A longitudinal study of adult-onset asthma incidence among HMO members. Environ Health 2:10. Available: [accessed 22 February 2005]. Savilahti R, Uitti J, Roto P, Laippala P, Husman T Increased prevalence of atopy among children exposed to mold in a school building. Allergy 56: U.S. EPA A Standardized EPA Protocol for Characterizing Indoor Air Quality in Large Buildings. Washington, DC:U. S. Environmental Protection Agency, Office of Research and Development and Office of Air and Radiation. Ungar WJ, Coyte PC Measuring productivity loss days in asthma patients. Health Econ 9: Ware J Jr, Kosinski M, Keller SD A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care 34: VOLUME 113 NUMBER 4 April 2005 Environmental Health Perspectives
NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS
 NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS Jean Cox-Ganser, Ph.D. Division of Respiratory Disease Studies The findings and conclusions in this presentation are those of the author
NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS Jean Cox-Ganser, Ph.D. Division of Respiratory Disease Studies The findings and conclusions in this presentation are those of the author
Pathology of Asthma Epidemiology
 Asthma A Presentation on Asthma Management and Prevention What Is Asthma? A chronic disease of the airways that may cause Wheezing Breathlessness Chest tightness Nighttime or early morning coughing Pathology
Asthma A Presentation on Asthma Management and Prevention What Is Asthma? A chronic disease of the airways that may cause Wheezing Breathlessness Chest tightness Nighttime or early morning coughing Pathology
Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece
 Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece Christos Lionis and Leda Chatzi, Clinic of Social and Family Medicine, School of Medicine, University of Crete,
Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece Christos Lionis and Leda Chatzi, Clinic of Social and Family Medicine, School of Medicine, University of Crete,
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province
 Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Facts about Stachybotrys chartarum and Other Molds
 Facts about Stachybotrys chartarum and Other Molds I heard about "toxic molds" that grow in homes and other buildings. Should I be concerned about a serious health risk to me and my family? (/mold/stachy.htm#q1)
Facts about Stachybotrys chartarum and Other Molds I heard about "toxic molds" that grow in homes and other buildings. Should I be concerned about a serious health risk to me and my family? (/mold/stachy.htm#q1)
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
An Overview of Asthma - Diagnosis and Treatment
 An Overview of Asthma - Diagnosis and Treatment Definition of Asthma: Asthma is a common chronic disease of children and adults. Nationally, more than 1 in 14 Americans report having asthma and as many
An Overview of Asthma - Diagnosis and Treatment Definition of Asthma: Asthma is a common chronic disease of children and adults. Nationally, more than 1 in 14 Americans report having asthma and as many
ImmunoCAP. Specific IgE blood test
 Allergy- Specific IgE blood test provides clinicians with an accurate and convenient method of helping to rule in or rule out allergy in patients with allergy-like symptoms. Allergy- Positive About Allergy-
Allergy- Specific IgE blood test provides clinicians with an accurate and convenient method of helping to rule in or rule out allergy in patients with allergy-like symptoms. Allergy- Positive About Allergy-
Asthma for Primary Care: Assessment, Control, and Long-Term Management
 Asthma for Primary Care: Assessment, Control, and Long-Term Management Learning Objectives After participating in this educational activity, participants should be better able to: 1. Choose the optimal
Asthma for Primary Care: Assessment, Control, and Long-Term Management Learning Objectives After participating in this educational activity, participants should be better able to: 1. Choose the optimal
your triggers? Information about a simple lab test that lets you Know Your IgE.
 What your are CAT DANDER DUST MITE triggers? Knowing if you have allergic triggers can help you manage your symptoms. Know yours and take control. OAK Information about a simple lab test that lets you
What your are CAT DANDER DUST MITE triggers? Knowing if you have allergic triggers can help you manage your symptoms. Know yours and take control. OAK Information about a simple lab test that lets you
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
O ccupational asthma (OA) is the most commonly
 58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma
 Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma Magnitude of Asthma - India Delhi Childhood asthma: 10.9% Adults: 8% Other Cities 3 to 18% Chhabra SK et al Ann Allergy Asthma
Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma Magnitude of Asthma - India Delhi Childhood asthma: 10.9% Adults: 8% Other Cities 3 to 18% Chhabra SK et al Ann Allergy Asthma
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Diagnosis, Treatment and Management of Asthma
 Diagnosis, Treatment and Management of Asthma Asthma is a complex disorder characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness, and an underlying inflammation.
Diagnosis, Treatment and Management of Asthma Asthma is a complex disorder characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness, and an underlying inflammation.
ASTHMA IN THE PEDIATRIC POPULATION
 ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
Bronchial asthma. E. Cserháti 1 st Department of Paediatrics. Lecture for english speaking students 5 February 2013
 Bronchial asthma E. Cserháti 1 st Department of Paediatrics Lecture for english speaking students 5 February 2013 Epidemiology of childhood bronchial asthma Worldwide prevalence of 7-8 and 13-14 years
Bronchial asthma E. Cserháti 1 st Department of Paediatrics Lecture for english speaking students 5 February 2013 Epidemiology of childhood bronchial asthma Worldwide prevalence of 7-8 and 13-14 years
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
The Asthma Guidelines: Diagnosis and Assessment of Asthma
 The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene
 Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
Mould Allergy. Patient Information
 Mould Allergy Patient Information Mould allergy An allergy is a condition which manifests as an exaggerated defence reaction of the body to allergens. Mould allergies are caused by the spores or fungal
Mould Allergy Patient Information Mould allergy An allergy is a condition which manifests as an exaggerated defence reaction of the body to allergens. Mould allergies are caused by the spores or fungal
Improving the Management of Asthma to Improve Patient Adherence and Outcomes
 Improving the Management of Asthma to Improve Patient Adherence and Outcomes Robert Sussman, MD Atlantic Health System Overlook Medical Center Asthma Remains a Serious Health Risk in the US Every day in
Improving the Management of Asthma to Improve Patient Adherence and Outcomes Robert Sussman, MD Atlantic Health System Overlook Medical Center Asthma Remains a Serious Health Risk in the US Every day in
Does rhinitis. lead to asthma? Does sneezing lead to wheezing? What allergic patients should know about the link between allergic rhinitis and asthma
 Does rhinitis lead to asthma? Does sneezing lead to wheezing? What allergic patients should know about the link between allergic rhinitis and asthma For a better management of allergies in Europe Allergy
Does rhinitis lead to asthma? Does sneezing lead to wheezing? What allergic patients should know about the link between allergic rhinitis and asthma For a better management of allergies in Europe Allergy
This is a cross-sectional analysis of the National Health and Nutrition Examination
 SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
Asthma: diagnosis and monitoring
 Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Potential Health Effects of Mold Exposure in Buildings
 Potential Health Effects of Mold Exposure in Buildings Objective: To present information about health hazard concerns associated with mold assessment and remediation projects. 1 Emerging Science The medical
Potential Health Effects of Mold Exposure in Buildings Objective: To present information about health hazard concerns associated with mold assessment and remediation projects. 1 Emerging Science The medical
Connecting Health & Housing: Asthma and the Home. Presented by: The California-Nevada Public Health Training Center
 Connecting Health & Housing: Asthma and the Home Presented by: The California-Nevada Public Health Training Center Funded by Grant #UB6HP20202 from the Health Resources and Services Administration, U.S.
Connecting Health & Housing: Asthma and the Home Presented by: The California-Nevada Public Health Training Center Funded by Grant #UB6HP20202 from the Health Resources and Services Administration, U.S.
Asthma and IAQ. Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst
 Asthma and IAQ Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst Division of Adolescent and School Health Centers for Disease Control and Prevention Asthma is a Major Public Health Problem
Asthma and IAQ Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst Division of Adolescent and School Health Centers for Disease Control and Prevention Asthma is a Major Public Health Problem
Asthma. Guide to Good Health. Healthy Living Guide
 Asthma Guide to Good Health Healthy Living Guide Asthma Chronic Fatigue Syndrome (CFS) Chronic Obstructive Pulmonary Disease (COPD) Coronary Artery Disease (CAD) Depression Hyperlipidemia Hypertension
Asthma Guide to Good Health Healthy Living Guide Asthma Chronic Fatigue Syndrome (CFS) Chronic Obstructive Pulmonary Disease (COPD) Coronary Artery Disease (CAD) Depression Hyperlipidemia Hypertension
National Asthma Educator Certification Board Detailed Content Outline
 I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
SCREENING AND PREVENTION
 These protocols are designed to implement standard guidelines, based on the best evidence, that provide a consistent clinical experience for AHC II Integrated Clinical Delivery Network patients and allow
These protocols are designed to implement standard guidelines, based on the best evidence, that provide a consistent clinical experience for AHC II Integrated Clinical Delivery Network patients and allow
Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma?
 Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Asthma in the Athlete
 Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Asthma in Pediatric Patients. DanThuy Dao, D.O., FAAP. Disclosures. None
 Asthma in Pediatric Patients DanThuy Dao, D.O., FAAP Disclosures None Objectives 1. Discuss the evaluation and management of asthma in a pediatric patient 2. Accurately assess asthma severity and level
Asthma in Pediatric Patients DanThuy Dao, D.O., FAAP Disclosures None Objectives 1. Discuss the evaluation and management of asthma in a pediatric patient 2. Accurately assess asthma severity and level
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma and Air Pollution
 Asthma and Air Pollution Health Effects Workshop Nov. 6, 2008 Joann Held with thanks to: Dave Brown Asthma and Airways Asthma Physiology A chronic disease that affects airways. The inside walls of airways
Asthma and Air Pollution Health Effects Workshop Nov. 6, 2008 Joann Held with thanks to: Dave Brown Asthma and Airways Asthma Physiology A chronic disease that affects airways. The inside walls of airways
Michael S. Blaiss, MD
 Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine Division of Clinical Immunology and Allergy University of Tennessee Health Science Center Memphis, Tennessee Speaker s Bureau: AstraZeneca,
Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine Division of Clinical Immunology and Allergy University of Tennessee Health Science Center Memphis, Tennessee Speaker s Bureau: AstraZeneca,
Science in the News: Asthma
 Science in the News: Asthma Spring has returned to the United States. The sky is blue, the grass is green and many plants are flowering. Spring can be a beautiful time of year. But it is especially troublesome
Science in the News: Asthma Spring has returned to the United States. The sky is blue, the grass is green and many plants are flowering. Spring can be a beautiful time of year. But it is especially troublesome
Repeated Aerosol Exposure to Small Doses of Allergen A Model for Chronic Allergic Asthma
 Repeated Aerosol Exposure to Small Doses of Allergen A Model for Chronic Allergic Asthma S. HASAN ARSHAD, ROBERT G. HAMILTON, and N. FRANKLIN ADKINSON, Jr. Department of Medicine, Division of Allergy and
Repeated Aerosol Exposure to Small Doses of Allergen A Model for Chronic Allergic Asthma S. HASAN ARSHAD, ROBERT G. HAMILTON, and N. FRANKLIN ADKINSON, Jr. Department of Medicine, Division of Allergy and
Asthma and Vocal Cord Dysfunction
 Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Abstract INTRODUCTION. Keywords: atopic asthma, children, fungus sensitization ORIGINAL ARTICLE
 ORIGINAL ARTICLE Fungus Sensitizations: Specific IgE to 4 Different Fungi among Asthmatic Children in North Taiwan Yu-Ting Yu, Shyh-Dar Shyur, Hwai-Chih Yang, Szu-Hung Chu, Yu-Hsuan Kao, Hou-Ling Lung,
ORIGINAL ARTICLE Fungus Sensitizations: Specific IgE to 4 Different Fungi among Asthmatic Children in North Taiwan Yu-Ting Yu, Shyh-Dar Shyur, Hwai-Chih Yang, Szu-Hung Chu, Yu-Hsuan Kao, Hou-Ling Lung,
Speaker Disclosure. Identification and Diagnosis of Asthma. Definition of Asthma. Objectives 11/9/2017
 Speaker Disclosure Identification and Diagnosis of Asthma Isabel L. Virella Lowell, MD, Associate Professor, Pulmonology and Sleep Medicine, University of Alabama at Birmingham Isabel Virella-Lowell, MD
Speaker Disclosure Identification and Diagnosis of Asthma Isabel L. Virella Lowell, MD, Associate Professor, Pulmonology and Sleep Medicine, University of Alabama at Birmingham Isabel Virella-Lowell, MD
You Can Control Your Asthma
 asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network
 Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Asthma Pathophysiology and Treatment. John R. Holcomb, M.D.
 Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
(Asthma) Diagnosis, monitoring and chronic asthma management
 Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
THE ROLE OF INDOOR ALLERGEN SENSITIZATION AND EXPOSURE IN CAUSING MORBIDITY IN WOMEN WITH ASTHMA
 Online Supplement for: THE ROLE OF INDOOR ALLERGEN SENSITIZATION AND EXPOSURE IN CAUSING MORBIDITY IN WOMEN WITH ASTHMA METHODS More Complete Description of Study Subjects This study involves the mothers
Online Supplement for: THE ROLE OF INDOOR ALLERGEN SENSITIZATION AND EXPOSURE IN CAUSING MORBIDITY IN WOMEN WITH ASTHMA METHODS More Complete Description of Study Subjects This study involves the mothers
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Clinical Practice Guideline: Asthma
 Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Asthma COPD Overlap (ACO)
 Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
2012 PENNSYLVANIA ASTHMA BURDEN REPORT
 2012 PENNSYLVANIA ASTHMA BURDEN REPORT Table Of Contents Introduction ----------------------------------------------------------------------------------------------------1 Methodology---------------------------------------------------------------------------------------------------2
2012 PENNSYLVANIA ASTHMA BURDEN REPORT Table Of Contents Introduction ----------------------------------------------------------------------------------------------------1 Methodology---------------------------------------------------------------------------------------------------2
Environmental Allergens. Allergies to Dust, Mold and Pollen. A Patient s Guide
 Environmental Allergens Allergies to Dust, Mold and Pollen A Patient s Guide Our environment, at home or outdoors, can be a potent source of allergens causing itchy, puffy and watery eyes, sneezing, a
Environmental Allergens Allergies to Dust, Mold and Pollen A Patient s Guide Our environment, at home or outdoors, can be a potent source of allergens causing itchy, puffy and watery eyes, sneezing, a
Wood Dust Exposure and Asthma in British Columbia Sawmill Workers
 Wood Dust Exposure and Asthma in British Columbia Sawmill Workers C.E. Peters, H.W. Davies, P.A. Demers University of British Columbia AIHce, Philadelphia, June 5 th, 2007 Background Asthma is the most
Wood Dust Exposure and Asthma in British Columbia Sawmill Workers C.E. Peters, H.W. Davies, P.A. Demers University of British Columbia AIHce, Philadelphia, June 5 th, 2007 Background Asthma is the most
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit)
 Line of Business: All Lines of Business Effective Date: August 16, 2017 Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit) This policy has been developed through review
Line of Business: All Lines of Business Effective Date: August 16, 2017 Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit) This policy has been developed through review
Public Dissemination
 1. THE ASTHMA CONDITION 9 18 3 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
1. THE ASTHMA CONDITION 9 18 3 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
In 2002, it was reported that 72 of 1000
 REPORTS Aligning Patient Care and Asthma Treatment Guidelines Eric Cannon, PharmD Abstract This article describes how the National Asthma Education and Prevention Program Guidelines for the Diagnosis and
REPORTS Aligning Patient Care and Asthma Treatment Guidelines Eric Cannon, PharmD Abstract This article describes how the National Asthma Education and Prevention Program Guidelines for the Diagnosis and
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Allergic Rhinitis: Effects on Quality of Life and Co-morbid Conditions
 Disclosures : Effects on Quality of Life and Co-morbid Conditions Nycomed Pharmaceutical Sepracor Pharmaceutical Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee
Disclosures : Effects on Quality of Life and Co-morbid Conditions Nycomed Pharmaceutical Sepracor Pharmaceutical Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee
Content Indica c tion Lung v olumes e & Lung Indica c tions i n c paci c ties
 Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES
 LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES WHAT ARE ALLERGIES? It s probably not something that you think about, but every time you open your mouth or inhale, tiny particles from the environment that
LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES WHAT ARE ALLERGIES? It s probably not something that you think about, but every time you open your mouth or inhale, tiny particles from the environment that
Avg PM10. Avg Low Temp
 Geography 532 Geography of Environmental Health Dr. Paul Marr Name: Ex 16- Seasonality, Time Delay, and Disease (10 pts) Below are asthma cases per month for the years 1992-1994. The table also includes
Geography 532 Geography of Environmental Health Dr. Paul Marr Name: Ex 16- Seasonality, Time Delay, and Disease (10 pts) Below are asthma cases per month for the years 1992-1994. The table also includes
Health Surveillance. Reference Documents
 Health Surveillance Trevor Smith Consultant Occupational Physician Reference Documents Control of Substances Hazardous to Health Regulations 2002 HSE Guidance Note MS25 Medical Aspects of Occupational
Health Surveillance Trevor Smith Consultant Occupational Physician Reference Documents Control of Substances Hazardous to Health Regulations 2002 HSE Guidance Note MS25 Medical Aspects of Occupational
A llergy is a common occupational hazard for workers
 766 ORIGINAL ARTICLE Incidence of allergy and allergy symptoms among workers exposed to laboratory animals L Elliott, D Heederik, S Marshall, D Peden, D Loomis... See end of article for authors affiliations...
766 ORIGINAL ARTICLE Incidence of allergy and allergy symptoms among workers exposed to laboratory animals L Elliott, D Heederik, S Marshall, D Peden, D Loomis... See end of article for authors affiliations...
The Compensation of Allergic Disease ALLSA Conference, September 2017
 The Compensation of Allergic Disease ALLSA Conference, September 2017 Dr Shahieda Adams MBChB MMed (Occ Med) PhD OCCUPATIONAL MEDICINE DIVISION School of Public Health and Family Medicine University of
The Compensation of Allergic Disease ALLSA Conference, September 2017 Dr Shahieda Adams MBChB MMed (Occ Med) PhD OCCUPATIONAL MEDICINE DIVISION School of Public Health and Family Medicine University of
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Jeffrey M. Davidson, M.D. Certified by the Board of Allergy and Immunology Clinical Professor, University of California San Francisco
 180 Montgomery Street, Suite 2370 San Francisco, CA 94104 Tel: (415) 433-6673 Fax: (415) 433.6063 www.mydrd.com Jeffrey M. Davidson, M.D. Certified by the Board of Allergy and Immunology Clinical Professor,
180 Montgomery Street, Suite 2370 San Francisco, CA 94104 Tel: (415) 433-6673 Fax: (415) 433.6063 www.mydrd.com Jeffrey M. Davidson, M.D. Certified by the Board of Allergy and Immunology Clinical Professor,
What are Allergy shots / SCIT?
 Allergy diagnosis must be made accurately with correct history and tests including the skin prick test and the blood test like immunocap / Phadiatop study. This once made will help decide the dose and
Allergy diagnosis must be made accurately with correct history and tests including the skin prick test and the blood test like immunocap / Phadiatop study. This once made will help decide the dose and
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
BOULDER MEDICAL CENTER, P.C.
 BOULDER MEDICAL CENTER, P.C. Dear Patient, We are pleased that you have chosen our clinic for your medical needs. Here are a few suggestions to make your visit with us a pleasant experience. Please arrive
BOULDER MEDICAL CENTER, P.C. Dear Patient, We are pleased that you have chosen our clinic for your medical needs. Here are a few suggestions to make your visit with us a pleasant experience. Please arrive
Eczema: also called atopic dermatitis; a chronic, itchy, scaly rash not due to a particular substance exposure
 Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
Clinical Study Report SLO-AD-1 Final Version DATE: 09 December 2013
 1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
COPD and environmental risk factors other than smoking. 14. Summary
 COPD and environmental risk factors other than smoking 14. Summary Author : P N Lee Date : 7 th March 2008 1. Objectives and general approach The objective was to obtain a good insight from the available
COPD and environmental risk factors other than smoking 14. Summary Author : P N Lee Date : 7 th March 2008 1. Objectives and general approach The objective was to obtain a good insight from the available
Revised Protocol: Criteria for Designating Substances as. Occupational Asthmagens on the AOEC List of. Exposure Codes
 Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
UNIT TWO: OVERVIEW OF SPIROMETRY. A. Definition of Spirometry
 UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
Looking for Answers to Asthma
 01 May 2012 MP3 at voaspecialenglish.com Looking for Answers to Asthma AP Asthmatics feel like something heavy is on their chest during an attack, as demonstrated in Geneva for World Asthma Day in 2009
01 May 2012 MP3 at voaspecialenglish.com Looking for Answers to Asthma AP Asthmatics feel like something heavy is on their chest during an attack, as demonstrated in Geneva for World Asthma Day in 2009
Prince Edward Island Asthma Trends
 Prince Edward Island Asthma Trends 2001-2011 November 2014 Population Health Assessment and Surveillance Unit, Chief Public Health Office, Department of Health and Wellness Dr. Carol McClure, Chronic Disease
Prince Edward Island Asthma Trends 2001-2011 November 2014 Population Health Assessment and Surveillance Unit, Chief Public Health Office, Department of Health and Wellness Dr. Carol McClure, Chronic Disease
Clinical Implications of Asthma Phenotypes. Michael Schatz, MD, MS Department of Allergy
 Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
The Impact of a Smoke-Free Ordinance on the Health and Attitudes of Bartenders
 The Impact of a Smoke-Free Ordinance on the Health and Attitudes of Bartenders Karen A. Palmersheim, PhD, MS a, Patrick L. Remington, MD, MPH b, David F. Gundersen, MPH c Abstract Introduction: This report
The Impact of a Smoke-Free Ordinance on the Health and Attitudes of Bartenders Karen A. Palmersheim, PhD, MS a, Patrick L. Remington, MD, MPH b, David F. Gundersen, MPH c Abstract Introduction: This report
A Collaboration of Community, University and City
 A Collaboration of Community, University and City Boston Housing Authority Boston Public Health Commission Boston University School of Public Health Committee for Boston Public Housing, Inc. Franklin Hill
A Collaboration of Community, University and City Boston Housing Authority Boston Public Health Commission Boston University School of Public Health Committee for Boston Public Housing, Inc. Franklin Hill
Morbidity from asthma has been increasing in. Asthma in the Elderly* Cockroach Sensitization and Severity of Airway Obstruction in Elderly Nonsmokers
 Asthma in the Elderly* Cockroach Sensitization and Severity of Airway Obstruction in Elderly Nonsmokers Linda Rogers, MD, FCCP; Cara Cassino, MD, FCCP; Kenneth I. Berger, MD, FCCP; Roberta M. Goldring,
Asthma in the Elderly* Cockroach Sensitization and Severity of Airway Obstruction in Elderly Nonsmokers Linda Rogers, MD, FCCP; Cara Cassino, MD, FCCP; Kenneth I. Berger, MD, FCCP; Roberta M. Goldring,
Most common chronic disease in childhood Different phenotypes:
 Dr. W. Wijnant Paediatric Pulmonology Steve Biko Academic Hospital Most common chronic disease in childhood Different phenotypes: Viral wheezer Multiple trigger wheezer Transient wheezer Persistent early
Dr. W. Wijnant Paediatric Pulmonology Steve Biko Academic Hospital Most common chronic disease in childhood Different phenotypes: Viral wheezer Multiple trigger wheezer Transient wheezer Persistent early
Key Facts About. ASTHMA
 Key Facts About. ASTHMA Asthma is a serious lung disease that can be frightening and disabling. The public is becoming increasingly aware that more people, especially children, are suffering and dying
Key Facts About. ASTHMA Asthma is a serious lung disease that can be frightening and disabling. The public is becoming increasingly aware that more people, especially children, are suffering and dying
ASTHMA CONTROL. Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms.
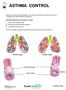 ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
UNDERSTANDING COPD MEDIA BACKGROUNDER
 UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
Integrated Cardiopulmonary Pharmacology Third Edition
 Integrated Cardiopulmonary Pharmacology Third Edition Chapter 13 Pharmacologic Management of Asthma, Chronic Bronchitis, and Emphysema Multimedia Directory Slide 7 Slide 12 Slide 60 COPD Video Passive
Integrated Cardiopulmonary Pharmacology Third Edition Chapter 13 Pharmacologic Management of Asthma, Chronic Bronchitis, and Emphysema Multimedia Directory Slide 7 Slide 12 Slide 60 COPD Video Passive
C.S. Ulrik *, V. Backer **
 Eur Respir J, 1996, 9, 1696 1700 DOI: 10.1183/09031936.96.09081696 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Increased bronchial responsiveness
Eur Respir J, 1996, 9, 1696 1700 DOI: 10.1183/09031936.96.09081696 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Increased bronchial responsiveness
Allergies and Asthma 5/21/2013. Objectives. Allergic Rhinitis (AR): Risk Factor for ASTHMA. Rhinitis and Asthma
 Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
Clinical Study Principal Components Analysis of Atopy-Related Traits in a Random Sample of Children
 International Scholarly Research Network ISRN Allergy Volume 2011, Article ID 170989, 4 pages doi:10.5402/2011/170989 Clinical Study Principal Components Analysis of Atopy-Related Traits in a Random Sample
International Scholarly Research Network ISRN Allergy Volume 2011, Article ID 170989, 4 pages doi:10.5402/2011/170989 Clinical Study Principal Components Analysis of Atopy-Related Traits in a Random Sample
Presented by the California Academy of Family Physicians 2013/California Academy of Family Physicians
 Family Medicine and Patient-Centered Asthma Care Presented by the California Academy of Family Physicians Faculty: Hobart Lee, MD Disclosures: Jeffrey Luther, MD, Program Director, Memorial Family Medicine
Family Medicine and Patient-Centered Asthma Care Presented by the California Academy of Family Physicians Faculty: Hobart Lee, MD Disclosures: Jeffrey Luther, MD, Program Director, Memorial Family Medicine
Allergies from A to Z
 Allergies from A to Z Rana T. Misiak, i MD Senior Staff Physician Henry Ford Health System Clinical Assistant Professor Wayne State University School of Medicine Objective To discuss the causes and treatment
Allergies from A to Z Rana T. Misiak, i MD Senior Staff Physician Henry Ford Health System Clinical Assistant Professor Wayne State University School of Medicine Objective To discuss the causes and treatment
Asthma Description. Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways.
 Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
