9/25/2014. Medical Issues (Restrictive processes) Medical Issues (Obstructive processes) Respiratory Emergencies (Class 10)
|
|
|
- Rodger Woods
- 5 years ago
- Views:
Transcription
1 1 2 3 Respiratory Emergencies (Class 10) Respiratory distress accounts for approximately 60% of all ambulance calls There are greater than 300,000 deaths annually due to respiratory emergencies All respiratory problems impact at least 1 of 3 things: Ventilation (mechanical movement of air into and out of the lungs Diffusion (distribution of air throughout the alveoli) Perfusion (distribution of blood throughout the capillary beds of the lungs Three basic forms of respiratory problems Restrictive processes Obstructive processes Miscellaneous 4 Medical Issues (Restrictive processes) 5 Problems that limit lung volume Usually due to structural defects in chest wall or diseases of the lung tissue itself that minimizes lung volume Scoliosis Kyphosis Can also be caused by disesases of the lung tissue itself Pulmonary fibrosis Medical Issues (Obstructive processes) Problems that interfere with the ability to move air into and/or out of the lungs Usually due to behaviors or chronic diseases that damages the air passages and/or alveoli Smoking Environmental exposures One of the most common reasons for ambulance calls Bronchitis 1
2 Definition Inflammation of the respiratory epithelium (mucosa) Causes Exposure to irritants or infectious agents Cigarette smoke Air pollution Workplace exposure (becoming increasingly more rare due to worker safety regulations)» Dry cleaners» Industry Bacteria Viruses 12 Physiology Irritated mucosa Thickened mucosa Excessive mucous production Goblet cell Fibrous scarring Decreased ciliary action Signs and symptoms Productive cough At least three consecutive months for at least two consecutive years Usually in the morning Increases with seasonal change Dyspnea Exertional Resting (severe cases) Obesity (blue bloaters) Rales, rhonchi and wheezing Emphysema (COPD) Definition Numerous processes occurring in the lung as a result of continual airway irritation Causes Chronic bronchitis due to Cigarette smoke» Active» Passive Air pollution Workplace exposure (becoming increasingly more rare due to worker safety regulations) 2
3 » Industry» Dry cleaners Pathology Irritated & thickened mucosa Excessive mucous production Goblet cells Eventual goblet cell death Unusual to see completely "dry" emphysema patient Fibrous scarring Decreased ciliary action Cell death Prone to infection Loss of elasticity Pathology (cont.) Mucous plugs Retains CO 2 Distal airway collapse Retains CO 2 Confluency Decreases surface area Bullae formation CO 2 Narcosis Medulla (normally senses CO 2 ) Tolerance Chemoreceptors (senses O 2 ) High O 2 decreases drive to breath Respiratory arrest results if O 2 too high Signs and symptoms Initial productive cough, becoming more of a dry cough as disease progresses Dyspnea Resting Exertional (greater dyspnea) Patients typically end up living in one room having a bathroom and almost always on the ground floor Tachypnea Tripod posturing Retractions 3
4 Pursed lipped breathing 24 Signs and symptoms COPD personality Restless Anxious Irritable Angry Skin color usually remains pink ( Pink Puffers ) Barrel chest Rales Spontaneous pneumothorax for both chronic bronchitis and COPD Establish responsiveness Airway Positioning Modified jaw thrust Chin lift Adjuncts as needed Nasal airway Oral airway PTL Usually mechanical device not required Suction as needed Breathing Assist and supplement breathing as necessary, artificial ventilation as necessary Breathing patient Low flow O 2» 24% venturi mask (best)» Nasal cannula at 1-2 LPM DO NOT WITHHOLD OXYGEN IF PATIENT HAVING SIGNIFICANT BREATHING PROBLEMS Allow patient to use inhaler as prescribed Consider use of CPAP Non-breathing patient 100% O 2 by bag-valve-mask Assist with pre-prescribed Albuterol nebulizer 2.5 mg/3ml normal saline with 6LPM oxygen Circulation 4
5 Check and maintain appropriate pulse IV normal saline TKO (may use INT) Patient positioning Fowler's Semi-Fowler's Supine for CPR or airway management NPO (non per os) Frequent vital signs Emergency transport, if necessary 29 Asthma Definition - bronchospasm Causes Allergens Irritants Stress Exertion Physiology Irritated mucosa Thickened mucosa Excessive mucous production Bronchospasm Narrowed lumen Sustained contraction Episodic Signs and symptoms Dyspnea Sudden Resting Exertional Non-productive cough Tachypnea Tachycardia Retractions Wheezing and perhaps rales Cyanosis Low SpO2 95% or less Establish responsiveness Airway Positioning 5
6 Modified jaw thrust Chin lift Adjuncts as needed Nasal airway Oral airway PTL Usually mechanical device not required Suction as necessary Breathing Breathing patient High flow O 2 Non-rebreathing mask (best) Nasal cannula at 10 LPM as a last resort Bag-valve-mask assembled and ready»begin ventilations if SpO2 less than 90% even if patient is breathing on his/her own Assist with pre-prescribed metered dose inhaler Consider CPAP Non-breathing patient 100% O 2 by bag-valve-mask Assist with pre-prescribed Albuterol nebulizer 2.5 mg/3ml normal saline with 6LPM oxygen Consider epinephrine injection for patients in extreme distress who don t respond to inhaled medications MUST HAVE APPROVAL OF MEDICAL CONTROL Circulation Check and maintain appropriate pulse IV normal saline TKO (may use INT) Patient positioning Fowler's Semi-Fowler's Supine for CPR or airway management NPO (non per os) Frequent vital signs Emergency transport, if necessary Status Asthmaticus Definition Extended attacks Rapid, recurrent attacks Treatment Same as above Will probably have to bag the patient 6
7 36 Pneumoconiosis Definition Inflammatory response due to particulate matter lodging in lung tissue Pathology Inflammation Fibrous scarring Emphysematous changes Types Black lung or Coal Miner s disease (coal dust) White lung (cotton fibers) Farmer's lung (dust) Signs & symptoms & treatment Same as COPD Medical Issues (Miscellaneous problems) 39 Pneumonia Definition Infection of deep lung tissues Causes Bacteria Virus Frequency Very common in geriatric patients Very common in immuno-compromised patients AIDS Organ transplant patients Common cause of death in geriatric patients Signs and symptoms Fever Chest pain upon deep breathing or coughing Altered mental status Dyspnea Cough Tachypnea Tachycardia Wheezing, rales and perhaps rhonchi Cyanosis Low SpO2 7
8 95% or less Establish responsiveness Airway Positioning Modified jaw thrust Chin lift Adjuncts as needed Nasal airway Oral airway PTL Usually mechanical device not required Suction as necessary Breathing Breathing patient High flow O 2 Non-rebreathing mask (best) Nasal cannula at 10 LPM as a last resort Consider CPAP Non-breathing patient 100% O 2 by bag-valve-mask Circulation Check and maintain appropriate pulse IV normal saline TKO (may use INT) Patient positioning Fowler's Semi-Fowler's Supine for CPR or airway management NPO (non per os) Frequent vital signs Emergency transport, if necessary Hyperventilation Syndrome (Tachypnea) Definition Excessive rate and depth of breathing Excessive loss of CO 2 Causes Psychological Fright and anxiety Metabolic DKA 8
9 Signs and symptoms Tachypnea Rate greater than 20/min Usually 30 to 40/min Tingling Hands Feet Face Cramping Fingers Toes Anxiety Nervousness Restlessness Vertigo (unusual) Chest pain (unusual) Calm patient Slow breathing techniques Inhale slowly Hold breath Count to thousand five Exhale slowly Count to thousand five Repeat Rebreathing USE ONLY AT DIRECTION OF MEDICAL CONTROL Paper bag Partial rebreathing mask No O 2 Full or semi-fowler's position Transport Pulmonary embolism Definition Clot in arteries or capillary beds of the lungs Causes Immobility Recent surgery Childbirth Birth control pill use Signs and symptoms Sudden unexpected dyspnea without obvious cause Sharp, stabbing chest pain 9
10 Hemoptysis Tachypnea Retractions Cyanosis Atypical chest pain Establish responsiveness Airway Positioning Modified jaw thrust Chin lift Adjuncts as needed Nasal airway Oral airway Double lumen airway Suction as necessary Breathing Breathing patient High flow O 2 Non-rebreathing mask (best) Nasal cannula at 6 LPM as a last resort Bag-valve-mask assembled and ready Non-breathing patient 100% O 2 by bag-valve-mask Circulation Check and maintain appropriate pulse IV normal saline TKO (may use INT) Patient positioning Fowler's or Semi-Fowler's if breathing Supine for CPR or airway management NPO (non per os) Frequent vital signs Emergency transport Pulmonary edema Definition Abnormal accumulation of interstitial fluid in the lungs 10
11 Causes Congestive heart failure Pneumonia Smoke inhalation Further discussion in cardiac emergencies lecture Always consider CPAP!! CPAP (Continuous Positive Airway Pressure) Increased pressure in the airways designed to keep them open Pursed-lipped breathing is self-cpap Now considered standard of care Indications Patient awake and able to follow commands Systolic pressure >90 mmhg Ability to maintain airway CPAP (Cont.) Two or more of the following: Respiratory rate > 25/min O2 saturation < 94% Use of accessory muscles (expiration becomes a muscular act) Contraindications Cardiac or respiratory arrest Pneumothorax Agonal breathing Typical starting pressure is 5 cm H 2 0 Open 0 2 regulator WIDE 57 CPAP Machine 58 Medical or Trauma Issues 59 Simple pneumothorax Air between visceral and parietal pleura May be caused by trauma or medical problem Assessment Dyspnea Absent or decreased breath sounds on affected side 11
12 Trachea MAY deviate toward injured side when patient inhales Simple pneumothorax (Cont.) Treatment Airway with Spinal Precautions Manual immobilization Ask patient to remain motionless Adjuncts as needed» Nasal airway» Oral airway» PTL Breathing High flow oxygen» Non-rebreathing mask» 15 LPM Bag-valve-mask assembled and ready Assist and supplement breathing as necessary Artificial ventilation as necessary Simple pneumothorax (Cont.) Circulation Stop Major Hemorrhage IV normal saline TKO» 20 cc/kg bolus if hypotension present Spinal precautions NPO (non per os) Frequent vital signs Emergency transport, if necessary 63 Trauma Issues 64 Sucking chest wound Movement of air through open chest wall wound Always causes pneumothorax Assessment Most rib fracture signs and symptoms Open chest wall laceration or puncture Air movement through wound Whistling Bubbling Foaming 12
13 "Spurting" with breathing, not pulse Pneumothorax signs and symptoms Sucking chest wound (Cont.) Treatment Airway with Spinal Precautions Manual immobilization Ask patient to remain motionless Adjuncts as needed» Nasal airway» Oral airway» PTL Breathing High flow oxygen» Non-rebreathing mask» 15 LPM Bag-valve-mask assembled and ready Assist and supplement breathing as necessary Artificial ventilation as necessary Circulation Check and maintain a central pulse Stop major hemorrhage IV normal saline TKO» 20 cc/kg bolus if hypotension present Sucking chest wound (Cont.) Treatment (Cont.) Close the sucking wound Occlusive dressing» Aluminum foil» Vaseline gauze» Plastic wrap Close on exhalation Sterility Three sides to avoid tension pneumothorax Patient positioning Fowler's, if no spinal injury Semi-Fowler's, if no spinal injury Supine for CPR Spinal precautions NPO (non per os) Frequent vital signs and monitoring Observe for the development of a tension pneumothorax 13
14 Emergency transport Tension pneumothorax Pressurized air between visceral and parietal pleura Usually caused by trauma Tension pneumothorax (Cont.) Assessment Dyspnea Absent or decreased breath sounds on affected side Narrowed pulse pressure Moves air poorly even with adequate airway Tracheal deviation AWAY from the injured side (LATE SIGN) Jugular vein distention (LATE SIGN) Unilaterally toward injury Bilateral as tension increases Tension pneumothorax Treatment Airway with Spinal Precautions Manual immobilization Ask patient to remain motionless Adjuncts as needed» Nasal airway» Oral airway» PTL Breathing High flow oxygen» Non-rebreathing mask» 15 LPM Bag-valve-mask assembled and ready» Assist and supplement breathing as necessary» Artificial ventilation as necessary Circulation Check and maintain a central pulse IV normal saline TKO» 20 cc/kg bolus if hypotension present 14
15 78 79 Tension pneumothorax (Cont.) Treatment (Cont.) If tension pneumothorax is due to a sucking chest wound, open the sucking wound Raise the occlusive dressing Allow pressure to escape Reclose the sucking wound» Close on exhalation Patient positioning Fowler's, if no spinal injury Semi-Fowler's, if no spinal injury Shock precautions Spinal precautions NPO (non per os) Frequent vital signs and monitoring Observe for the redevelopment of a tension pneumothorax Emergency transport Hemothorax Blood between visceral and parietal pleura Usually caused by trauma Assessment Dyspnea Absent or decreased breath sounds on affected side Shock may be present Flat neck veins Treatment Same as pneumothorax Patients are usually extremely difficult to ventilate Treat for shock Pneumo-hemothorax Blood and air between visceral and parietal pleura Usually caused by trauma Assessment Dyspnea Absent or decreased breath sounds on affected side Shock may be present Treatment Same as pneumothorax Treat for shock Pulmonary Contusion 75% of chest trauma patients also have pulmonary contusion (bruising of the lung). 15
16 The bruising results in alveolar edema, alveolar hemorrhage and atelectasis (deflation of the alveoli) This causes hypoxia and hypercarbia due to poor perfusion and reduced gas exchange in the affected area (ventilation/perfusion mismatch) Most common potentially life-threatening pulmonary injury Assessment Small movements of the stethoscope identify areas of present then absent breath sounds Treatment High flow oxygen Medications Metered Dose Inhaler (MDI) Nebulizer (Small Volume Nebulizer/SVN) Bronchiodilator Albuterol (Proventil, Ventolin, Bronkosol, Alupent, Metaprel, etc) Description A commonly prescribed bronchiodilator in pre-hospital care, Albuterol is administered with a small volume nebulizer, or metered dose inhaler. Actions Causes bronchiodilation with minimal side effects, reduces airway resistance, and duration is approximately five hours. Indications Exhibits signs and symptoms of respiratory emergency (Bronchial asthma or signs and symptoms of respiratory distress; reversible bronchospasm associated with chronic bronchitis and cases of emphysema). Third drug for anaphylaxis. Has physician prescribed inhaler or nebulizer medication, and Specific authorization by medical direction. Contraindications Patients with a known hypersensitivity to the drug. Inability of patient to use device However, nebulizers are occasionally used with a mask. Inhaler/nebulization medication is not prescribed for the patient. No permission from medical direction. 16
17 Patient has already met maximum prescribed dose prior to your arrival. Precautions Palpitations, anxiety, nausea, and dizziness may be seen. Monitor vital signs Use caution when administering to patients with history of cardiovascular disease or hypertension. Side effects Increased pulse rate. May increase systolic pressure. Tremors. Nervousness Dosage Nebulizer Amount of medication or duration of treatment based upon medical direction's order or physician's order based upon consultation with the patient Typical order is 2.5 mg of the drug placed in 3 ml of normal saline for inhalation and administered by a nebulizer running at the flow rate established in the nebulizer s manufacturer s recommendations until appropriate mist is achieved (usually about six liters per minute). Metered Dose Inhaler Shake inhaler vigorously several times and administer to the patient upon deep inhalation. The patient should hold their breath as long as comfortably possible (at least 10 seconds or more) to assure more effective distribution of medication. Number of inhalations based upon medical direction's order or physician's order based upon consultation with the patient. Route Inhalation only Infant & child considerations Use of handheld inhalers is very common in children Retractions are more commonly seen in children than adults Cyanosis is a late finding in children Very frequent coughing may be present rather than wheezing in some children Emergency care with usage of handheld inhalers is the same if the indications for usage of inhalers are met by the ill child Skills Metered Dose Inhaler Administration Skills Manual pages 15 & 16 Video Skills Nebulized Medication Administration 17
18 Skills Manual pages 17 & 18 Video 95 18
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Respiratory System Anatomy Respiratory system: all the structures that contribute to
 1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 16. Objectives. Objectives. Respiratory Emergencies
 Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Respiratory Emergencies
 29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 15 - Respiratory Emergencies
 1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
STS: Circulatory/Pulmonary
 STS: Circulatory/Pulmonary September 27, 2017 You have a 50 y/o male who is complaining of excruciating pain in his chest. You find him sitting down on a bench, arms in a tripod position, breathing heavily.
STS: Circulatory/Pulmonary September 27, 2017 You have a 50 y/o male who is complaining of excruciating pain in his chest. You find him sitting down on a bench, arms in a tripod position, breathing heavily.
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Topics. Seattle/King County EMT-B Class. Pharmacology: Chapter 10. Respiratory Emergencies: Chapter 11. Cardiovascular Emergencies: Chapter 12
 Seattle/King County EMT-B Class Topics 1 Pharmacology: Chapter 10 Respiratory Emergencies: Chapter 11 Cardiovascular Emergencies: Chapter 1 1 Pharmacology 1 General Pharmacology You will be responsible
Seattle/King County EMT-B Class Topics 1 Pharmacology: Chapter 10 Respiratory Emergencies: Chapter 11 Cardiovascular Emergencies: Chapter 1 1 Pharmacology 1 General Pharmacology You will be responsible
WESTCHESTER REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE
 WESTCHESTER REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE POLICY STATEMENT Supercedes/Updates: New No. 04-02 Date: April 19, 2004 Re: EMT-B Administration of Nebulized Albuterol Pages: 3 Administration
WESTCHESTER REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE POLICY STATEMENT Supercedes/Updates: New No. 04-02 Date: April 19, 2004 Re: EMT-B Administration of Nebulized Albuterol Pages: 3 Administration
The Respiratory System
 The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Goal of the Respiratory Assessment. Two Parts of the Respiratory Assessment
 The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
HASPI Medical Anatomy & Physiology 14b Lab Activity
 HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
ALCO Regulations. Protocol pg. 47
 For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
This activity should be used to motivate students to learn about the significance and concerns associated with patients in respiratory emergencies.
 Pre-Lecture I. You Are the Provider Time: 10 Minutes Small Group Activity/Discussion The You are the Provider case study is discussed within the PowerPoint presentation for this chapter. The instructor
Pre-Lecture I. You Are the Provider Time: 10 Minutes Small Group Activity/Discussion The You are the Provider case study is discussed within the PowerPoint presentation for this chapter. The instructor
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
UNIT TERMINAL OBJECTIVE
 UNIT TERMINAL OBJECTIVE 5-1 At the end of this unit, the EMT-Enhanced student will be able to utilize the assessment findings to formulate a field impression and implement the treatment plan for the patient
UNIT TERMINAL OBJECTIVE 5-1 At the end of this unit, the EMT-Enhanced student will be able to utilize the assessment findings to formulate a field impression and implement the treatment plan for the patient
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Respiratory Distress/Failure - General
 Respiratory Distress/Failure - General Criteria: Dyspnea WITHOUT a clear etiology O 2 V/S and SpO 2 (with and without Oxygen therapy if possible) Blood glucose analysis: if less than 80 mg/dl, refer to
Respiratory Distress/Failure - General Criteria: Dyspnea WITHOUT a clear etiology O 2 V/S and SpO 2 (with and without Oxygen therapy if possible) Blood glucose analysis: if less than 80 mg/dl, refer to
February EMS Training: Pulmonary Emergencies. Used with permission of Silver Cross EMS System
 February EMS Training: Pulmonary Emergencies Used with permission of Silver Cross EMS System Goals Review airway anatomy and physiology for adults and pediatrics Review issues and techniques in airway
February EMS Training: Pulmonary Emergencies Used with permission of Silver Cross EMS System Goals Review airway anatomy and physiology for adults and pediatrics Review issues and techniques in airway
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Acute respiratory failure
 Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Phases of Respiration
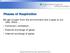 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Anatomy. The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs.
 Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Chronic Obstructive Pulmonary Disease (COPD) Copyright 2014 by Mosby, an imprint of Elsevier Inc.
 Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Acute Respiratory Disorders. and How to Assess them: Diagnostics
 Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Why do you breathe? What is oxygen used for? Where does CO2 come from?
 RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
EMS Subspecialty Certification Review Course
 EMS Subspecialty Certification Review Course 1.3.1 1.3.1.1 Shortness of Breath 1.3.1.1.1 Use of portable non invasive ventilation devices 1.3.1.1.2 Field Identification of COPD 1.3.1.1.3 Assisted Ventilation
EMS Subspecialty Certification Review Course 1.3.1 1.3.1.1 Shortness of Breath 1.3.1.1.1 Use of portable non invasive ventilation devices 1.3.1.1.2 Field Identification of COPD 1.3.1.1.3 Assisted Ventilation
7/12/2014. Cardiovascular Emergencies (Class 11)
 1 2 3 4 5 6 7 8 9 Cardiovascular Emergencies (Class 11) Review Circulatory System Anatomy and Physiology Blood flow through the heart Regular anatomy of the heart Electrical anatomy of the heart Arteriosclerosis/atherosclerosis
1 2 3 4 5 6 7 8 9 Cardiovascular Emergencies (Class 11) Review Circulatory System Anatomy and Physiology Blood flow through the heart Regular anatomy of the heart Electrical anatomy of the heart Arteriosclerosis/atherosclerosis
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Chapter 10. Objectives. Objectives 01/09/2013. Airway Management, Artificial Ventilation, and Oxygenation
 Chapter 10 Airway Management, Artificial Ventilation, and Oxygenation Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Chapter 10 Airway Management, Artificial Ventilation, and Oxygenation Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 5 Respiratory Disorders. TEXT ASSIGNMENT Paragraphs 5-1 through 5-17. LESSON OBJECTIVES After completing this lesson, you should be able to: 5-1. Identify the characteristics,
LESSON ASSIGNMENT LESSON 5 Respiratory Disorders. TEXT ASSIGNMENT Paragraphs 5-1 through 5-17. LESSON OBJECTIVES After completing this lesson, you should be able to: 5-1. Identify the characteristics,
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Appendix E Choose the sign or symptom that best indicates severe respiratory distress.
 Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Condensed version.
 I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
Chronic Obstructive Pulmonary Disease
 Scope of Problem Chronic Obstructive Pulmonary Disease Marianne J. Davies, RN, MSN, APRN Yale University School of Medicine Yale Comprehensive Cancer Center Nevada Cancer Institute 2005 Hospitalizations
Scope of Problem Chronic Obstructive Pulmonary Disease Marianne J. Davies, RN, MSN, APRN Yale University School of Medicine Yale Comprehensive Cancer Center Nevada Cancer Institute 2005 Hospitalizations
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition)
 2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
Cough Associated with Bronchitis
 Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Nursing Process Focus: Patients Receiving Salmeterol (Serevent)
 Prior to administration: Assess for presence/history of chronic asthma, exercise induced asthma, acute asthma attacks, and acute upper airway obstruction. Assess respiratory rate and lung sounds, pulse
Prior to administration: Assess for presence/history of chronic asthma, exercise induced asthma, acute asthma attacks, and acute upper airway obstruction. Assess respiratory rate and lung sounds, pulse
Care of the Patient with a Respiratory Disorder
 Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
Appendix D An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires:
 Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
Chronic Obstructive Pulmonary Disease
 Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Respiratory diseases in Ostrołęka County
 Respiratory diseases in Ostrołęka County 4400 persons underwent examination 950 persons were given referrals to more detailed investigation 600 persons were examined so far The results of more detailed
Respiratory diseases in Ostrołęka County 4400 persons underwent examination 950 persons were given referrals to more detailed investigation 600 persons were examined so far The results of more detailed
Pulmo-Park Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D
 Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Medical NREMT-PTE. NREMT Paramedic Trauma Exam.
 Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Medical NREMT-PTE NREMT Paramedic Trauma Exam https://killexams.com/pass4sure/exam-detail/nremt-pte Question: 41 Which of the following most accurately describes the finding of jugular venous distension
Atrovent Administration
 Atrovent Administration ICEMA Training 2007 Sherri Shimshy RN OBJECTIVES Describe the pharmacology of Atrovent Identify the indications for use of Atrovent in the Adult Population Identify the indications
Atrovent Administration ICEMA Training 2007 Sherri Shimshy RN OBJECTIVES Describe the pharmacology of Atrovent Identify the indications for use of Atrovent in the Adult Population Identify the indications
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Pulmonary Emergencies. Lower Airway Structures Trachea Bronchial tree Primary bronchi Secondary bronchi Bronchioles Alveoli Lungs
 Pulmonary Emergencies Lower Airway Structures Trachea Bronchial tree Primary bronchi Secondary bronchi Bronchioles Alveoli Lungs Pulmonary Surfactant Thin film that coats alveoli Prevents alveoli from
Pulmonary Emergencies Lower Airway Structures Trachea Bronchial tree Primary bronchi Secondary bronchi Bronchioles Alveoli Lungs Pulmonary Surfactant Thin film that coats alveoli Prevents alveoli from
