Personality Disorders and Retention in a Therapeutic Community for Substance Dependence
|
|
|
- Norma Blankenship
- 6 years ago
- Views:
Transcription
1 The American Journal on Addictions, 20: , 2011 Copyright C American Academy of Addiction Psychiatry ISSN: print / online DOI: /j x Personality Disorders and Retention in a Therapeutic Community for Substance Dependence Douglas B. Samuel, PhD, 1,2 Donna M. LaPaglia, PsyD, 1,3 Lisa M. Maccarelli, PhD, 4 Brent A. Moore, PhD, 1,5 Samuel A. Ball, PhD 1,5 1 Department of Psychiatry, Yale University School of Medicine, New Haven, Connecticut 2 VA New England MIRECC, West Haven, Connecticut 3 Substance Abuse Treatment Unit Yale University, New Haven, Connecticut 4 University of Pittsburgh Medical Center, Western Psychiatric Institute and Clinic, Pittsburgh, Pennsylvania 5 APT Foundation, New Haven, Connecticut Although therapeutic community (TC) treatment is a promising intervention for substance use disorders, a primary obstacle to successful treatment is premature attrition. Because of their prevalence within substance use treatment facilities, personality disorder (PD) diagnoses have been examined as predictors of treatment completion. Prior research on TC outcomes has focused almost exclusively on antisocial personality disorder (ASPD), and the results have been mixed. This study extends previous research by examining the impact of the 10 Axis II PDs on early (first 30 days) attrition as well as overall time to dropout in a 9-month residential TC. Survival analyses indicated that borderline was the only PD negatively related to overall program retention. In contrast, ASPD,aswellashistrionicPD,wererelatedtoveryearly attrition, but not to overall program retention. Early assessment and identification of at-risk individuals may improve treatment retention and outcome for TC treatment. (Am J Addict 2011:20: ) INTRODUCTION Therapeutic community (TC) treatment is a potentially effective psychosocial intervention for reducing substance use, criminality, unemployment, and other psychosocial problems experienced by addicted individuals. 1 Several large-scale studies 2 4 have found significant and sustained improvements following successful completion of a TC typically after 6 12 months of residential treatment. 5 These multisite studies indicate that the most stable predictor of positive treatment outcomes is retention in the treatment. 3 9 Unfortunately, it is common in intensive residen- Received July 14, 2010; revised September 21, 2010; accepted October 25, Address correspondence to Dr. Samuel, Department of Psychological Sciences, Purdue University, 703 Third St., West Lafayette, IN dbsamuel@purdue.edu. tial TCs for as many as 50% of residents to drop out within the first month and another 25 40% or more to drop out during subsequent months, often leaving as few as 10% of admissions who receive a moderately to maximally effective dose of this treatment modality. 10 Identification of factors associated with very early attrition and poor longer term retention is important to help recognize individuals who may be at high risk for poor outcomes and for whom additional intervention might be necessary. We evaluated the impact of the 10 Axis II personality disorders (PDs) on very early attrition (within the first 30 days) as well as overall time to dropout during a 9-month treatment program. PDs are the most common form of co-occurring psychiatric disorder found in TCs and the severe and persistent cognitive, emotional, interpersonal, and behavioral problems characterizing these disorders contribute to poor outcomes in substance abuse treatment as well as a variety of psychiatric disorders. 16 Median prevalence rates of Axis II disorders are especially high (70 80%) among drug-dependent persons treated in inpatient or residential settings. 17 Asystematic review of the literature 18 found that PDs, particularly antisocial personality disorder (ASPD) and borderline personality disorder (BPD), were consistently associated with risks for early dropout from all types of substance abuse treatment. Other studies have also documented poor outcomes for PDs in general, including their negative association with treatment completion in a large sample of homeless military veterans in a residential rehabilitation facility 24 and among a sample of 307 Norwegian drug abusers. 25 TCs were specifically designed to address the attitude, behavioral, criminogenic, and personality problems that characterize severe addiction and ASPD. As such, ASPD might be expected to have no appreciable impact on retention in an effectively run TC. However, studies evaluating retention among ASPD in TCs have been mixed. 555
2 Goldstein et al. 26 compared patients who met full criteria for ASPD (ie, adult criteria and evidence of conduct disorder in childhood) versus those who only displayed adult antisocial behavior. They found that the ASPD-diagnosed group had poorer retention for the longer (ie, 180 days) treatment program, but that the groups did not differ for the 90-day program. In contrast, Haller et al. 27 (1997) reported that ASPD was positively related to treatment retention in a sample of pregnant women. Messina and colleagues found that ASPD, diagnosed with either self-report inventory 28 or semi-structured interview 29 was unrelated to several outcome measures, including the completion of the 12-month TC. Most recently, Daughters et al. 30 reported that, while ASPD status did not predict retention on its own, the interaction of ASPD and court-mandated status did predict early attrition in a sample of 236 male TC patients. Considering these mixed findings for ASPD, continued study of its impact on TC retention would be helpful in supplementing and potentially clarifying the existing literature. Although a TC s highly structured, hierarchical social milieu, emphasizing positive and negative consequences, may be well suited to ASPD, such an intensive and confrontive peer pressure environment may not be an effective approach for PDs characterized by significant cognitive (eg, paranoid), emotional (eg, borderline), or interpersonal (eg, avoidant) vulnerability or rigidity. We are aware of only a few other studies that have evaluated PDs other than ASPD in relation to TC retention. Karterud et al. 31 evaluated 97 patients in a Norwegian day hospital TC and divided the patients into four diagnostic groups: borderline, schizotypal, other PD, and no PD. Borderline and schizotypal groups had greater rates of attrition than did the other PD or no PD groups. Fals-Stewart 32 also examined the MCMI-II 33 PD scales and found that schizoid and schizotypal scales were negatively related to length of stay within a TC, while histrionic and narcissistic scales were positively related. The current study attempted to address several gaps in the literature by conducting a more thorough evaluation of the relation between all 10 PDs and two measures of retention (ie, early attrition, defined as premature dropout within the first 30 days, and overall time to dropout from the 9-month treatment program). We chose these two frames because of their clinical relevance and because they corresponded to time frames chosen in prior research. We also addressed the limitations of previous research 31 which relied on unstructured clinical diagnoses, did not test all PDs, used a general index of retention (percent dropped out), and a lower intensity non-residential TC milieu. Although previous studies have been mixed, we predicted that ASPD would not be related to either very early attrition or overall time to dropout. However, we predicted that BPD and several Cluster A (paranoid, schizoid, schizotypal) and Cluster C (avoidant, obsessive-compulsive) PDs characterized by severe cognitive, emotional, and interpersonal vulnerabilities would be related to reduced retention. METHOD Participants We recruited adult and adolescent patients from a longterm residential TC treatment program for substance abuse located in an urban area in the Northeastern United States. For inclusion, patients had to be either adolescents (15 18 years; n = 49) or adults (19 65 years; n = 77) and have a lifetime DSM-IV substance abuse or dependence diagnosis. Seven additional patients provided informed consent, but were excluded based on inability to read or understand the consent or assessment forms based on the Slosson Oral Reading Test. 34 Patients with current suicidal or homicidal plans, severe medical illness, schizophrenia, or bipolar disorder were not eligible for admission to the residential program. Interested individuals provided consent and received the baseline packet of self-report materials from a research assistant. Participants received a $50 store gift card for completing the baseline assessment, $10 for month 1 5 assessments, $60 for the month 6 and $70 for month 9 assessments. This study was approved by the Institutional Review Board at the authors institution. Before combining results from the adolescents and adults, we carefully examined them for potential differences. Beyond age, t-tests and chi-square analyses did not indicate significant differences for racial or gender makeup. Significant differences were noted for lifetime substance diagnoses, with adults more likely to qualify for alcohol, opioid, and stimulant diagnoses while adolescents were more likely to be diagnosed with cannabis dependence. No differences were detected for lifetime rates of major depressive disorder or social phobia, but adults were more likely to have a diagnosis of posttraumatic stress disorder. Most importantly, chi-square analyses also did not detect significant differences in the diagnostic rate for any of the 10 PDs, which were the variables of interest in the current study. While diagnosis of PDs within DSM-IV is restricted to individuals over the age of 18, there is increasing evidence for the continuity of maladaptive personality functioning across this arbitrary threshold. 35,36 Additionally, the DSM-5 Personality and Personality Disorders Workgroup proposal 37 does not include an age requirement. Materials PDs were assessed using the Schedule for Nonadaptive and Adaptive Personality (SNAP). 38 The SNAP is a selfreport inventory that includes 375 items rated as true or false. It provides an assessment of three broad temperaments (ie, positive affect, negative affect, and disinhibition) as well as 12 maladaptive trait scales that assess aspects of personality pathology (eg, mistrust, aggression, and impulsivity). The SNAP also provides an assessment of the DSM-III-R 39 PDs, using some items that overlap with those included in the trait scales. These PD scales can be scored dimensionally (ie, summing the items) or can produce categorical variables for each diagnostic criterion 556 Personality Disorders Predicting Retention November December 2011
3 that can then be counted to determine whether the individual reaches the diagnostic threshold. Scores on the SNAP PD scales obtained stability coefficients over a 9-month interval ranging from.59 (schizotypal) to.84 (antisocial), with a median of.75 in a non-clinical sample. 40 SNAP PD scale scores have demonstrated validity when compared to semi-structured interview measures with a median convergent correlation of In addition, SNAP PD scores correlate strongly with scores from other self-report PD instruments with a median convergent value of.62 across the 10 PDs. 41 Finally, portions of the Structured Clinical Interview for DSM-IV (SCID) were administered for descriptive purposes. Procedures TC residents were approached about their interest in participating in research within 1 week of program admission. Eligible and interested residents provided informed consent and completed a baseline assessment which included the SNAP and then monthly and follow-up assessments during their participation in a randomized clinical trial of two active psychotherapies. All participants were admitted to the TC with a minimal length of stay of 9 months and typically by referral through the criminal justice or child protection systems. APT Residential Services Division embraces most of the core elements that have defined a TC. 42 The program involves a highly organized, staff-guided, self-help positive peer pressure process focused especially on changing attitudes, perceptions, and behaviors associated with drug use and criminality. Peers influence peers to promote learning and assimilation of social norms and skills. There are strict, explicit, behavioral norms with contingencies to promote self-control and responsibility. The first 30 days of treatment are spent in a semi-segregated orientation group program in which the rules and responsibilities are learned and residents are supported through their accommodation to this new milieu. The next 6 or more months are spent in the main TC program and then followed by 6 or more months in a higher status resident coordinator role or employment in the community during a reentry phase. Although community meetings and psychoeducational groups are important tools, peer encounter and other therapy groups are considered the core techniques aimed at change. These groups are meant to heighten each individual s awareness of specific attitudes or behavioral patterns that negatively affect the community and need to be changed for the individual to recover. All of these groups focus on changing cognitive, behavioral, and emotional processes that severely impede affiliation with the community and thus prevent socialization and maturation. In addition, there are an array of professional support services in place (group counseling, case management, medical care, psychiatric services, educational and vocational programming). Job or school functions are arranged in a hierarchy according to seniority and individual productivity such that progress leads to higher levels of management/coordination as well as additional privileges. This social organization reflects fundamental elements of the rehabilitative approach: self-help, trust in the community, responsible performance, honesty, hard work, tough love, and earned successes. These are conceptualized as necessary for long-term recovery from addiction. Data Analyses Although the primary result of interest was the impact of PDs on a 9-month TC program retention, attrition in the very early phase of treatment is a significant clinical problem for all addiction treatment modalities. Therefore, we also chose to evaluate the 30-day attrition because the first month (orientation phase) is a critical phase of adjustment to a TC where separate programming is provided and because this is the shortest duration used as an outcome variable in previous TC research. We first conducted univariate analyses using chi-square to evaluate early dropout and Kaplan-Meier survival analyses to evaluate days retained in treatment. For these univariate analyses, each diagnostic group was compared to the group without a PD diagnosis. In order to evaluate which predictors showed the strongest relationship we then conducted multivariate analyses by entering all diagnoses simultaneously. Binary logistic regression was used for early dropout and Cox regression survival analyses for treatment retention. Finally, because the field of PD research appears to be moving toward dimensional approaches for DSM-5, 37 we repeated the multivariate analyses using dimensional PD scores. For these analyses, the raw item scores for each SNAP scale were summed to create variables referred to as PD severity scores. Again, early dropout was evaluated using binary logistic regression and Cox regression was used for overall retention. RESULTS One hundred and twenty-six participants completed the baseline assessment and 17 (14%) dropped out before 30 days, and 81 of these participants (64%) did not complete the 9-month program. Although 270 days represented completion of the formal treatment, some patients remained in treatment for more than a year. Table 1 provides descriptive statistics on demographic variables as well as selected Axis I and Axis II PD diagnoses for the entire sample. Univariate Analyses We first examined the impact of any PD diagnosis, by comparing those meeting criteria for one or more PDs (n = 75) to those without any PD diagnosis (n = 51) on both early attrition and overall time to dropout. Five times as many patients with a PD diagnosis dropped out within the Samuel et al. November December
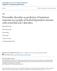
4 TABLE 1. Descriptive statistics for overall sample on demographic variables, SCID Axis I diagnoses, and SNAP Personality Disorder Diagnoses Overall Variable (n = 126) Gender (% male) 78.6 Race Caucasian (%) 55.6 African American (%) 27.6 Hispanic (%) 12.7 Other (%) 4.8 Age (M [SD]) 26.9 (10.3) Adult (%) 61.1 Lifetime substance diagnosis Alcohol (%) 69.7 Stimulant (%) 33.6 Opioid (%) 19.7 Cannabis (%) 37.7 Other (%) 5.7 Lifetime Axis I diagnosis Major depression (%) 38.5 Social phobia (%) 22.3 PTSD (%) 20.5 Personality disorder Paranoid (%) 20.6 Schizoid (%) 7.1 Schizotypal (%) 13.5 Antisocial (%) 31.0 Borderline (%) 25.4 Histrionic (%) 24.6 Narcissistic (%) 10.3 Avoidant (%) 23.0 Dependent (%) 13.5 Obsessive-compulsive (%) 3.2 SCID = Structured Clinical Interview for DSM-IV-Axis I; PTSD = posttraumatic stress disorder; SNAP = Schedule for Nonadaptive and Adaptive Personality. first 30 days compared to those without a PD diagnosis (see Table 2). Over the entire treatment, patients with any PD diagnosis completed significantly fewer days in treatment than those without a PD diagnosis. Chi-square results indicated that antisocial, histrionic, and paranoid PD diagnoses were significantly related to early attrition. However, when considering overall number of days in treatment, Kaplan- Meier analyses suggested that borderline, paranoid, and avoidant diagnoses were significantly predictive of shorter duration over the entire 9 months of treatment. Multivariate Analyses Seeking to better understand the unique contribution of each individual PD, we then entered the 10 PDs simultaneously into a binary logistic regression predicting the dichotomous variable of attrition within the first 30 days. Schizotypal diagnosis was excluded from the early attrition analyses because all 17 individuals meeting the criteria for schizotypal remained in the treatment at 30 days, providing no variability in the outcome. As with the univariate analyses, ASPD and histrionic were significantly predictive of early attrition. However, in contrast to the univariate findings, the impact of a paranoid diagnosis was nonsignificant when all the diagnoses were considered simultaneously (see Table 3). Multivariate analyses of days until dropout indicated that BPD was the only diagnosis that evidenced a significantly shorter stay over the 9- month treatment. Figure 1 presents the cumulative survival for those with and without a BPD diagnosis. Dimensional Scores Finally, in order to determine whether dimensional representations of these constructs would show comparable findings, we repeated the multivariate analyses using continuous measures of the PD constructs. A binary logistic regression on the early attrition variable showed that histrionic severity was significantly predictive of early attrition (Wald χ 2 = 5.0, OR = 1.58, 95% CI = ), while antisocial severity trended but was not significant (Wald χ 2 = 3.1, p =.08; OR = 1.20, 95% CI = ). Consistent with the categorical results above, a Cox proportional hazards regression indicated that borderline severity significantly predicted shorter treatment lengths, Wald χ 2 = 4.40, p <.05; H.R. = 1.21, 95% CI = DISCUSSION Although TCs are a promising treatment modality for severe addiction, criminality, unemployment, and other psychosocial problems, research has indicated that premature attrition is negatively associated with these long-term outcomes. 3 The existing literature has provided mixed findings with respect to ASPD and little information about the impact of other PDs on retention. In contrast with some other research 26 our findings replicate those of Messina and colleagues 28,29 who also reported that ASPD was unrelated to TC retention. Globally, the results of this study are consistent with previous findings in demonstrating that the presence of any PD is associated with worse retention in atc. 24,25 However, the effect appears to be more specific both in terms of specific diagnoses and treatment intervals. This study suggests that when considered in isolation, individuals with baseline diagnoses of BPD, avoidant, and paranoid PDs had significantly fewer days in treatment, compared to individuals without a PD diagnosis. However, when all 10 diagnoses were considered simultaneously only BPD remained significant, suggesting that it is most related to shorter duration, over the course of a 9-month treatment. Additionally, individuals with ASPD, histrionic, and paranoid PD diagnoses were significantly more likely than those without any diagnosis to drop out within the first 30 days 558 Personality Disorders Predicting Retention November December 2011
5 TABLE 2. Univariate analyses for SNAP PD diagnoses on early attrition and overall time to dropout Early attrition (<30 days) Overall time to dropout (270 days) Diagnostic group % Attrited Chi-square p Mean 95% CI Log-rank chi-square p Paranoid (26) Schizoid (9) Schizotypal (17) Antisocial (39) Borderline (32) Histrionic (31) Narcissistic (13) Avoidant (29) Dependent (17) OCPD (4) Any PD (75) No PD (51) Early dropout present chi-square analyses using Fisher s exact test (two-sided). Treatment completion analyses present results from Kaplan-Meier survival analysis with data right-censored at 270 days. Each diagnostic group was compared to the group without any PD diagnoses, provided on the lowest row. SNAP = Schedule for Nonadaptive and Adaptive Personality; PD = personality disorder; Mean = the mean number of days in treatment; CI = confidence interval; OCPD = obsessive-compulsive personality disorder; PD = personality disorder. Numbers in parentheses indicate the number of patients who met criteria for the PD. Values in boldface type indicate significance at p <.05. of treatment. Nonetheless, multivariate analyses (in which all diagnoses were entered at once) indicated that only the findings for ASPD and histrionic remained significant. It is perhaps interesting that, although BPD was the diagnosis with the shortest overall treatment duration, it was not significantly related to early attrition in the first 30 days. These findings indicate that individuals with high emotional reactivity (which characterizes BPD) are not prone to retention problems during the orientation phase of TC treatment when they are receiving highly structured psychoeducational group and individual meetings focused on adaptation to the program milieu. During these first 30 days, residents are also relatively segregated from the broader program population and stressors of peer confrontation and behavioral consequences. Our results suggest that BPD residents experience retention problems the longer that they are exposed to the more intensive environment of the regular TC program which can be characterized by affectively charged and interpersonally confrontive interactions with peers and staff. This type of demanding TC milieu contrasts with existing empirically supported treatments for BPD such as dialectical behavior therapy, 44 TABLE 3. Multivariate analyses of SNAP PD diagnoses on early attrition and overall time to dropout Early dropout (<30 days) Overall time to dropout (270 days) Wald chi-square OR 95% CI Wald chi-square HR 95% CI Paranoid Schizoid Schizotypal Antisocial Borderline Histrionic Narcissistic Avoidant Dependent OCPD Early attrition analyses present binary logistic regressions on presence of dropout at 30 days. Overall time to dropout analyses present Cox regression analyses for attrition over 9 months. SNAP = Schedule for Nonadaptive and Adaptive Personality; PD = personality disorder; OR = odds ratio; HR = hazard ratio; 95% CI = 95% confidence interval; OCPD = obsessive-compulsive PD. Values in boldface type indicate significance at p <.05. Schizotypal was excluded from early attrition analysis due to lack of variability in the outcome measure. Samuel et al. November December
6 FIGURE 1. Cox regression survival analysis for borderline personality disorder diagnosis. n = 126; Data right-censored at 270 days. which focuses explicitly on balancing change with empathic acceptance and validation of the individual. Research suggests that this type of treatment can increase retention and treatment outcomes for emotionally dysregulated and vulnerable patients. 45,46 Symptoms associated with BPD might not substantially interfere with the initial orientation to the TC model, but might interfere with the longer term effective utilization of the TC s core treatment processes. In this sense, the findings for BPD were almost completely opposite those for ASPD and histrionic as those PDs were both related to early attrition, but not to overall time spent in the TC. In contrast to BPD, the traits associated with ASPD, such as assertiveness, competitiveness, and tough-skinned independence, might lead to difficulty accepting the rules and regulations of the well-controlled environment. However, once the initial orientation period is over, those same traits might equip the individual for success within (or at least tolerance for) the confrontive TC atmosphere. The present findings for ASPD at the two time points might also explain its inconsistent relationship with TC completion in previous studies. The definition of treatment completion has varied greatly, from as few as 30 days 30 to as long as 12 months. 28 This wide range of intervals across studies as well as the fact that ASPD might present greater risks early in treatment suggests that, in addition to programmatic differences across TCs, the previous research might have been capturing temporal variation. The finding that histrionic PD is also associated with attrition within the first 30 days of treatment is somewhat more difficult to understand. Only one other study has examined the relationship between histrionic PD and TC completion and it suggested that histrionic scores were positively related to overall length of treatment. 32 Nonetheless, that study used a version of the MCMI 33 that researchers have suggested may assess only qualitative, and perhaps even adaptive, aspects of histrionic PD. 47 Histrionic is defined primarily by the need to be the center of attention and represented by traits such as exhibitionism. It is possible that such individuals also may not respond well to the early phases of TC orientation when they are segregated from the population and less able to engage the wider attention of all residents and staff. Nonetheless, the fact that this study is the first to report that histrionic PD might be related to early TC attrition should be interpreted cautiously until it can be further tested in additional studies. While the most robust findings were for BPD (in terms of overall treatment duration) and for ASPD and histrionic (in terms of attrition within the first 30 days), there were also other PDs that evidenced an increased risk for attrition. Notably, individuals diagnosed with paranoid PD completed fewer total days in treatment and were more likely to dropout within the first 30 days than individuals without a PD diagnosis. In both the cases, the findings for paranoid PD were not significant when considered simultaneously with the other PD diagnoses. This perhaps suggests that the effect of paranoid might be accounted for by its comorbidity with other disorders, rather than its unique variance. Similarly, individuals with an avoidant PD diagnosis spent significantly fewer days in treatment than individuals without any PD diagnoses, but this effect was 560 Personality Disorders Predicting Retention November December 2011
7 also not significant when considered in multivariate analyses. At a minimum these findings suggest that future studies of premature dropout should also consider paranoid and avoidant PD. Finally, it is important to note that the present findings were not specific to diagnostic status defined categorically (ie, presence vs. absence of the diagnosis) as analyses of dimensional scorings also obtained comparable results. This is particularly important as it appears increasingly likely that DSM-5 will incorporate a dimensional understanding of personality pathology. Within the currently available proposal 37 it appears that ASPD and BPD will continue to be included (although histrionic might be excluded) but will be rated along a continuum rather than categorically. If this model is indeed adopted, the dimensional results presented in this study might be most relevant to future researchers and clinicians. Clinical Implications A primary implication of this study is the importance of thorough personality assessment at the outset of treatment within a TC. Specifically, identification of those traits and behaviors characteristic of BPD and ASPD, as well as perhaps histrionic, paranoid, and avoidant PDs, is essential as they predicted different retention challenges. The current results suggest that ASPD should be identified quickly and that specific interventions be targeted toward these individuals to assist in their engagement and orientation to the TC atmosphere. The findings suggest that the risk for attrition for these individuals is greatest at the beginning of treatment and that the personality traits associated with ASPD might have a negligible (or even protective) effect once they integrate into the TC. Individuals with high standing on BPD, on the other hand, appear to be at no greater risk for very early attrition in programs that do not require immediate immersion into the treatment milieu. Nonetheless, the fact that BPD predicted attrition prior to program completion, suggests that a TC might not be the optimal choice of treatment for these individuals. Perhaps this initial early period (ie, first 30 days) can be utilized by identifying the individuals least likely to benefit from the TC and make programmatic adjustments or external referral to promote better treatment retention and outcome. Limitations This study provides data on the impact of PDs on TC retention at two different time points, but is not without limitations. While self-reports of PDs are the most common method of assessment within the research literature, semistructured interviews are considered to be the most valid method. 48 In addition, the version of the SNAP employed in this study assesses the DSM-III-R categories. Although the differences between the PD scales on the SNAP 34 and the SNAP-2 49 are relatively minor (typically only a few items were changed), the use of DSM-IV scales would be preferable. Finally, the initial sample size was larger than some previous examinations (eg, 97 patients 31 and 65 patients 25 ) but was also smaller than others (eg, 275 patients 28 ). Nonetheless, the low prevalence of some PDs within this sample perhaps reduced the ability to detect their impact on retention. This factor, combined with the gender imbalance typical of most TCs, prevented our evaluation of the effects of gender on retention for all PDs. Future studies that examine potential gender interactions would be particularly important for BPD and ASPD given the gender differences in these diagnoses. 50 CONCLUSIONS This was the first study to evaluate the categorical and dimensional representation of all 10 PDs in relation to two treatment retention milestones. Our results suggest that previously inconsistent findings for ASPD might be attributable to the length of the treatment interval used to define completion. Finally, this study also indicated that BPD negatively relates to long-term retention suggesting that other treatment modalities or approaches for emotionally dysregulated individuals might be preferable. Writing of this manuscript was supported by the Office of Academic Affiliations, Advanced Fellowship Program in Mental Illness Research and Treatment, Department of Veterans Affairs, Palo Alto, CA. This research was supported by grant DA14967 from the National Institute on Drug Abuse, Rockville, MD (Dr. Ball). Declaration of Interest The authors report no conflicts of interest. The authors alone are responsible for the content and writing of this paper. REFERENCES 1. De Leon G. Therapeutic communities. In: Galanter M, Kleber H, eds. Textbook of Substance Abuse Treatment, 3rd ed. Washington, DC: American Psychiatric Publishing; 2004: Simpson DD, Sells SB. Effectiveness of treatment for drug abuse: An overview of the DARP research program. Adv Alcohol Subst Abuse. 2002;2: Simpson DD, Joe GW, Brown BS. Treatment retention and follow-up outcomes in the Drug Abuse Treatment Outcome Study (DATOS). Psychol Addict Behav. 1997;11: Hubbard RL, Marsden ME, Rachal JV, et al. Drug Abuse Treatment: A National Study of Effectiveness. Chapel Hill, NC: University of North Carolina Press; Hubbard RL, Craddock SG, Flynn PM, et al. Psychol Addict Behav. 1997;11: Anglin MD, Hser YI. Treatment of drug abuse. In: Tonry M, Morris N, eds. Drugs and Crime: Crime and Justice: A Review of Research. Chicago, IL: University of Chicago Press; 1991: Condelli WS, Hubbard RL. Relationship between time spent in treatment and client outcomes from therapeutic communities. J Subst Abuse Treat. 1994;11: Samuel et al. November December
8 8. De Leon G. The Therapeutic Community: Study of Effectiveness. Treatment Research Monograph Series. DHHS Publication no (ADM) Rockville, MD: National Institute on Drug Abuse; Sacks S, Banks S, McKendrick K, et al. Modified therapeutic community for co-occurring disorders: A summary of four studies. J Subst Abuse Treat. 2008;34: Condelli WS. Domains of variables for understanding and improving retention in therapeutic communities. Int J Addict. 1994;29: De Leon G, Skodol A, Rosenthal MS. Phoenix House: Changes in psychopathological signs of resident drug addicts. Arch Gen Psychiatry. 1973;28: De Leon G. Psychopathology and substance abuse: What is being learned from research in therapeutic communities. J Psychoactive Drugs. 1989;21: Jainhill NG, De Leon G, Pinkham L. Psychiatric diagnoses among substance abusers in the therapeutic community. J Psychoactive Drugs. 1986;8: Sacks S, De Leon G, Balisteri E, et al. Modified therapeutic community for homeless mentally ill chemical abusers. J Subst Abuse Treat. 1999;15: Sacks JG, Levy NM. Objective personality changes in residents of a therapeutic community. Am J Psychiatry. 1979;136: Ansell EB, Grilo CM. Personality disorders. In: Hersen M, Turner SM, Beidel DC, eds. Adult Psychopathology and Diagnosis. Hoboken, NJ: Wiley; 2007: Verheul R, Ball S, van den Brink W. Substance abuse and personality disorders. In: Kranzler HR, Rounsaville BJ, eds. Dual Diagnosis and Treatment: Substance Abuse and Comorbid Medical and Psychiatric Disorders. New York: Marcel Dekker; 1998: Meier PS, Barrowclough C. Mental health problems: Are they or are they not a risk factor for dropout from drug treatment? A systematic review of the evidence. Drugs: Education, Policy, and Prevention. 2009;16: DeJong C, van den Brink W, Harteveld FM, et al. Personality disorders in alcoholics and drug addicts. Compr Psychiatry. 1993;34: Kosten TA, Kosten TR, Rounsaville BJ. Personality disorders in opiate addicts show prognostic specificity. J Subst Abuse Treat. 1989;6: Nace EP, Davis CW. Treatment outcome in substance abusing patients with a personality disorder. AmJAddict. 1993;2: Rounsaville BJ, Kosten TR, Weissman MM, et al. A 2.5 year follow-up of short-term interpersonal psychotherapy in methadone maintained opiate addicts. Compr Psychiatry. 1986;27: Thomas VH, Melchert TP, Banken JA. Substance dependence and personality disorders: Comorbidity and treatment outcome in an inpatient treatment population. J Stud Alcohol. 1999;60: Justus AN, Burling TA, Weingardt KR. Client predictors of treatment retention and completion in a program for homeless veterans. Subst Use Misuse. 2002;41: Ravndal E, Vaglum P, Lauritzen G. Completion of long-term inpatient treatment of drug abusers: A prospective study from 13 different units. Eur Addict Res. 2005;11: Goldstein RB, Powers SI, McCusker J, et al. Antisocial behavioral syndromes among residential drug abuse treatment clients. Drug Alcohol Depend. 1998;49: Haller DL, Knisley JS, Elswick RK, et al. Perinatal substance abusers: Factors influencing treatment retention. J Subst Abuse Treat. 1997;14: Messina N, Wish ED, Hoffman JA, et al. Antisocial personality disorder and TC treatment outcomes. Am J Drug Alcohol Abuse. 2002;28: Messina NP, Wish ED, Nemes S. Therapeutic community treatment for substance abusers with antisocial personality disorder. J Subst Abuse Treat. 1999;17: Daughters SB, Stipleman BA, Sargeant MN, et al. The interactive effects of antisocial personality disorder and court-mandated status on substance abuse treatment dropout. J Subst Abuse Treat. 2008;34: Karterud S, Vaglum S, Friis S, et al. Day hospital therapeutic community treatment for patients with personality disorders: An empirical evaluation of the containment function. J Nerv Ment Dis. 1992;180: Fals-Stewart W. Personality characteristics of substance abusers: An MCMI cluster typology of recreational drug users treated in a therapeutic community and its relationship to length of stay and outcome. J Pers Assess. 1992;59: Millon T, Millon C, Davis R. Millon Clinical Multiaxial Inventory: MCMI-III. Upper Saddle River, NJ: Pearson Assessments; Slosson R, Nicholson C. Slosson Oral Reading Test, rev. ed. SORT-R3. East Aurora, NY: Slosson Educational Publications; De Clercq B, De Fruyt F, Widiger TA. Integrating a developmental perspective in dimensional models of personality disorders. Clin Psychol Rev. 2009;29: Shiner RL. A developmental perspective on personality disorders: Lessons from research on normal personality development in childhood and adolescence. J Pers Disord. 2005;19: DSM-5 Personality Disorders Workgroup. Reformulation of personality disorders in DSM-5. Revisions/Pages/PersonalityandPersonalityDisorders.aspx. Accessed July 12, Clark LA. Manual for the Schedule for Nonadaptive and Adaptive Personality. Minneapolis, MN: University of Minnesota Press; American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders Revised, 3rd ed., revised. Washington, DC: American Psychiatric Association; Melley AH, Oltmanns TF, Turkheimer E. The Schedule for Nonadaptive and Adaptive Personality (SNAP): Temporal stability and predictive validity of the diagnostic scales. Assessment. 2002;9: Widiger TA, Boyd S. Assessing personality disorders. In: Butcher JN, ed. Oxford Handbook of Personality Assessment, 3rd ed. New York: Oxford University Press; 2009: De Leon G. Therapeutic communities: Is there an essential model. In: De Leon G, ed. Community as Method: Therapeutic Communities for Special Populations and Special Settings. Westport, CT: Praeger; 1997: First MB, Spitzer RL, Gibbon M, et al. Structured Clinical Interview for DSM-IV Axis I Disorders, Clinician Version (SCID-CV). Washington, DC: American Psychiatric Press; Linehan MM, Schmidt H, Dimeff LA, et al. Dialectical Behavior Therapy for patients with borderline personality disorder and drugdependence. AmJAddict. 1999;8: Bornalova MA, Daughters SB. How does Dialectical Behavior Therapy facilitate treatment retention among individuals with comorbid borderline personality disorder and substance use disorders. Clin Psychol Rev. 2007;27: Linehan MM, Dimeff LA, Reynolds SK, et al. Dialectical behavior therapy versus comprehensive validation therapy plus 12-step for the treatment of opioid dependent women meeting criteria for borderline personality disorder. Drug Alcohol Depend. 2002;67: Craig RJ. Overview and current status of the Millon Clinical Multiaxial Inventory. J Pers Assess. 1999;72: McDermut W, Zimmerman M. Assessment instruments and standardized evaluation. In: Bender D, Oldham J, Skodol A, eds. The American Psychiatric Publishing Textbook of Personality Disorders. Washington, DC: American Psychiatric Publishing; 2005: Clark LA, Simms LJ, Wu KD, et al. Manual for the Schedule for Nonadaptive and Adaptive Personality (SNAP-2). Minneapolis, MN: University of Minnesota Press; In press. 50. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Washington, DC: American Psychiatric Association; Personality Disorders Predicting Retention November December 2011
Five Factor Model Prototype Matching Scores: Convergence Within Alternative Methods
 Journal of Personality Disorders, 25(5), 571 585, 2011 2011 The Guilford Press Five Factor Model Prototype Matching Scores: Convergence Within Alternative Methods Douglas B. Samuel, PhD, Maryanne Edmundson,
Journal of Personality Disorders, 25(5), 571 585, 2011 2011 The Guilford Press Five Factor Model Prototype Matching Scores: Convergence Within Alternative Methods Douglas B. Samuel, PhD, Maryanne Edmundson,
Personality traits predict current and future functioning comparably for individuals with major depressive and personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. March, 2007 Personality traits predict current and future functioning comparably for individuals with major depressive and personality
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. March, 2007 Personality traits predict current and future functioning comparably for individuals with major depressive and personality
A Clinical Translation of the Research Article Titled Antisocial Behavioral Syndromes and. Additional Psychiatric Comorbidity in Posttraumatic Stress
 1 A Clinical Translation of the Research Article Titled Antisocial Behavioral Syndromes and Additional Psychiatric Comorbidity in Posttraumatic Stress Disorder among US Adults: Results from Wave 2 of the
1 A Clinical Translation of the Research Article Titled Antisocial Behavioral Syndromes and Additional Psychiatric Comorbidity in Posttraumatic Stress Disorder among US Adults: Results from Wave 2 of the
Comparing the temporal stability of self-report and interview assessed personality disorder.
 Purdue University Purdue e-pubs Department of Psychological Sciences Faculty Publications Department of Psychological Sciences 2011 Comparing the temporal stability of self-report and interview assessed
Purdue University Purdue e-pubs Department of Psychological Sciences Faculty Publications Department of Psychological Sciences 2011 Comparing the temporal stability of self-report and interview assessed
DIAGNOSIS OF PERSONALITY DISORDERS: SELECTED METHODS AND MODELS OF ASSESSMENT 1
 ROCZNIKI PSYCHOLOGICZNE/ANNALS OF PSYCHOLOGY 2017, XX, 2, 241 245 DOI: http://dx.doi.org/10.18290/rpsych.2017.20.2-1en AGNIESZKA POPIEL a BOGDAN ZAWADZKI b a SWPS University of Social Sciences and Humanities
ROCZNIKI PSYCHOLOGICZNE/ANNALS OF PSYCHOLOGY 2017, XX, 2, 241 245 DOI: http://dx.doi.org/10.18290/rpsych.2017.20.2-1en AGNIESZKA POPIEL a BOGDAN ZAWADZKI b a SWPS University of Social Sciences and Humanities
Treatment retention has served. Relationships Between Counseling Rapport and Drug Abuse Treatment Outcomes
 Relationships Between Counseling Rapport and Drug Abuse Treatment Outcomes George W. Joe, Ed.D. D. Dwayne Simpson, Ph.D. Donald F. Dansereau, Ph.D. Grace A. Rowan-Szal, Ph.D. Objective: This study examined
Relationships Between Counseling Rapport and Drug Abuse Treatment Outcomes George W. Joe, Ed.D. D. Dwayne Simpson, Ph.D. Donald F. Dansereau, Ph.D. Grace A. Rowan-Szal, Ph.D. Objective: This study examined
The traditional approach to. Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans
 Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Redefining personality disorders: Proposed revisions for DSM-5
 Interview Experts in personality disorders Web audio at CurrentPsychiatry.com Drs. Black and Zimmerman: How proposed changes to DSM-5 will affect researchers Online Only Redefining personality disorders:
Interview Experts in personality disorders Web audio at CurrentPsychiatry.com Drs. Black and Zimmerman: How proposed changes to DSM-5 will affect researchers Online Only Redefining personality disorders:
Diffusing the Stress in Financial Distress: The Intersection of Bankruptcy and Mental Health
 Diffusing the Stress in Financial Distress: The Intersection of Bankruptcy and Mental Health Moderator: Hon. Laura Taylor Swain (S.D. N.Y.), New York, NY Panelists: Prof. Richard A. Friedman, M.D., Weill
Diffusing the Stress in Financial Distress: The Intersection of Bankruptcy and Mental Health Moderator: Hon. Laura Taylor Swain (S.D. N.Y.), New York, NY Panelists: Prof. Richard A. Friedman, M.D., Weill
Personality disorders. Personality disorder defined: Characteristic areas of impairment: The contributions of Theodore Millon Ph.D.
 Personality disorders Personality disorder defined: An enduring maladaptive pattern of inner experience and outward behavior, involving impaired: (two or more of the following) sense of self emotional
Personality disorders Personality disorder defined: An enduring maladaptive pattern of inner experience and outward behavior, involving impaired: (two or more of the following) sense of self emotional
Douglas B. Samuel, Ph.D.
 Douglas B. Samuel, 1 Douglas B. Samuel, Ph.D. dbsamuel@purdue.edu Department of Psychological Sciences (765) 494-7559 Purdue University 703 Third Street West Lafayette, IN 47907 EDUCATION University of
Douglas B. Samuel, 1 Douglas B. Samuel, Ph.D. dbsamuel@purdue.edu Department of Psychological Sciences (765) 494-7559 Purdue University 703 Third Street West Lafayette, IN 47907 EDUCATION University of
Standardization of the Dutch MCMI-III: Specific problems associated with the use of base rates
 Standardization of the Dutch MCMI-III: Specific problems associated with the use of base rates Gina Rossi & Hedwig Sloore Corresponding author: Rossi Gina grossi@vub.ac.be Commission, July 6-8, 2006 Faculty
Standardization of the Dutch MCMI-III: Specific problems associated with the use of base rates Gina Rossi & Hedwig Sloore Corresponding author: Rossi Gina grossi@vub.ac.be Commission, July 6-8, 2006 Faculty
Prospective assessment of treatment use by patients with personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample
 Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans with comorbid axis I disorders
 Washington University School of Medicine Digital Commons@Becker Posters 2005: Alcoholism and Comorbidity 2005 Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans
Washington University School of Medicine Digital Commons@Becker Posters 2005: Alcoholism and Comorbidity 2005 Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans
GAP e comorbidità psichiatrica. Eugenio Aguglia. Università di Catania, Dipartimento di Medicina Clinica e Sperimentale
 GAP e comorbidità psichiatrica Eugenio Aguglia Università di Catania, Dipartimento di Medicina Clinica e Sperimentale The DSM 5 chapter Addictive Disorders includes gambling disorder as the sole condition
GAP e comorbidità psichiatrica Eugenio Aguglia Università di Catania, Dipartimento di Medicina Clinica e Sperimentale The DSM 5 chapter Addictive Disorders includes gambling disorder as the sole condition
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Personality Disorder: the clinical management of borderline personality disorder
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
Twelve-Month Test-Retest Reliability of the Structured Clinical Interview for DSM-III-R Personality Disorders in Cocaine-Dependent Patients
 Twelve-Month Test-Retest Reliability of the Structured Clinical Interview for DSM-III-R Personality Disorders in Cocaine-Dependent Patients Roger D. Weiss, Lisa M. Najavits, Larry R. Muenz, and Cathryn
Twelve-Month Test-Retest Reliability of the Structured Clinical Interview for DSM-III-R Personality Disorders in Cocaine-Dependent Patients Roger D. Weiss, Lisa M. Najavits, Larry R. Muenz, and Cathryn
Abstract. Comprehensive Psychiatry 48 (2007)
 Comprehensive Psychiatry 48 (2007) 329 336 www.elsevier.com/locate/comppsych Psychosocial impairment and treatment utilization by patients with borderline personality disorder, other personality disorders,
Comprehensive Psychiatry 48 (2007) 329 336 www.elsevier.com/locate/comppsych Psychosocial impairment and treatment utilization by patients with borderline personality disorder, other personality disorders,
Overview of. Treatment Outcome Studies from DATOS
 Drug Abuse Treatment Outcome (Funded by NIDA) Overview of Treatment Outcome from DATOS Charts Prepared & Released for Public Use by Dwayne Simpson (TCU), Robert Hubbard (NDRI-NC), Douglas Anglin (UCLA),
Drug Abuse Treatment Outcome (Funded by NIDA) Overview of Treatment Outcome from DATOS Charts Prepared & Released for Public Use by Dwayne Simpson (TCU), Robert Hubbard (NDRI-NC), Douglas Anglin (UCLA),
Douglas B. Samuel, Ph.D.
 Douglas B. Samuel, 1 Douglas B. Samuel, Ph.D. dbsamuel@purdue.edu Department of Psychological Sciences (765) 494-7559 Purdue University 703 Third Street West Lafayette, IN 47907 EDUCATION University of
Douglas B. Samuel, 1 Douglas B. Samuel, Ph.D. dbsamuel@purdue.edu Department of Psychological Sciences (765) 494-7559 Purdue University 703 Third Street West Lafayette, IN 47907 EDUCATION University of
Introduction to personality. disorders. University of Liverpool. James McGuire PRISON MENTAL HEALTH TRAINING WORKSHOP JUNE 2007
 PENAL REFORM INTERNATIONAL PRISON MENTAL HEALTH TRAINING WORKSHOP JUNE 2007 Introduction to personality disorders James McGuire University of Liverpool Session objectives To provide an overview of concepts
PENAL REFORM INTERNATIONAL PRISON MENTAL HEALTH TRAINING WORKSHOP JUNE 2007 Introduction to personality disorders James McGuire University of Liverpool Session objectives To provide an overview of concepts
A Structured Interview for the Assessment of the Five-Factor Model of Personality: Facet-Level Relations to the Axis II Personality Disorders
 A Structured Interview for the Assessment of the Five-Factor Model of Personality: Facet-Level Relations to the Axis II Personality Disorders Timothy J. Trull University of Missouri Columbia Thomas A.
A Structured Interview for the Assessment of the Five-Factor Model of Personality: Facet-Level Relations to the Axis II Personality Disorders Timothy J. Trull University of Missouri Columbia Thomas A.
PERSONALITY ASSESSMENT INVENTORY
 PERSONALITY ASSESSMENT INVENTORY TM The Personality Assessment Inventory (PAI) Revealed: Creation and Use of a Research Repository for the PAI Jennifer A. Greene, PhD Leslie Morey, PhD Introduction The
PERSONALITY ASSESSMENT INVENTORY TM The Personality Assessment Inventory (PAI) Revealed: Creation and Use of a Research Repository for the PAI Jennifer A. Greene, PhD Leslie Morey, PhD Introduction The
Estimates of the Reliability and Criterion Validity of the Adolescent SASSI-A2
 Estimates of the Reliability and Criterion Validity of the Adolescent SASSI-A 01 Camelot Lane Springville, IN 4746 800-76-056 www.sassi.com In 013, the SASSI Profile Sheets were updated to reflect changes
Estimates of the Reliability and Criterion Validity of the Adolescent SASSI-A 01 Camelot Lane Springville, IN 4746 800-76-056 www.sassi.com In 013, the SASSI Profile Sheets were updated to reflect changes
2014, Vol. 5, No. 2, /14/$12.00 DOI: /per BRIEF REPORT
 Personality Disorders: Theory, Research, and Treatment 2013 American Psychological Association 2014, Vol. 5, No. 2, 172 177 1949-2715/14/$12.00 DOI: 10.1037/per0000033 BRIEF REPORT The Convergence of Personality
Personality Disorders: Theory, Research, and Treatment 2013 American Psychological Association 2014, Vol. 5, No. 2, 172 177 1949-2715/14/$12.00 DOI: 10.1037/per0000033 BRIEF REPORT The Convergence of Personality
Twelve month test retest reliability of a Japanese version of the Structured Clinical Interview for DSM-IV Personality Disorders
 PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 575October 2003 1159 Japanese SCID-II A. Osone and S. Takahashi 10.1046/j.1323-1316.2003.01159.x Original Article532538BEES
PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 575October 2003 1159 Japanese SCID-II A. Osone and S. Takahashi 10.1046/j.1323-1316.2003.01159.x Original Article532538BEES
What to Measure in Client Behavior
 What to Measure in Client Behavior Alec Boros, Ph.D. Research Manager, Oriana House, Inc. Rebecca Fischbein, Ph.D. Research Specialist, Oriana House, Inc. Asli Buldum, M.A. Research Specialist, Oriana
What to Measure in Client Behavior Alec Boros, Ph.D. Research Manager, Oriana House, Inc. Rebecca Fischbein, Ph.D. Research Specialist, Oriana House, Inc. Asli Buldum, M.A. Research Specialist, Oriana
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
GIOCO D AZZARDO PATOLOGICO E COMORBIDITÀ PSICHIATRICHE
 Università degli Studi di Catania DIPARTIMENTO DI MEDICINA CLINICA E SPERIMENTALE AOU Policlinico-vittorio emanuele Catania U.O.P.I. di Psichiatria GIOCO D AZZARDO PATOLOGICO E COMORBIDITÀ PSICHIATRICHE
Università degli Studi di Catania DIPARTIMENTO DI MEDICINA CLINICA E SPERIMENTALE AOU Policlinico-vittorio emanuele Catania U.O.P.I. di Psichiatria GIOCO D AZZARDO PATOLOGICO E COMORBIDITÀ PSICHIATRICHE
Clinical experience suggests. Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders
 Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders Susanne Hörz, Dipl.-Psych., Ph.D. Mary C. Zanarini, Ed.D. Frances R. Frankenburg,
Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders Susanne Hörz, Dipl.-Psych., Ph.D. Mary C. Zanarini, Ed.D. Frances R. Frankenburg,
Managing Personality Disorders in Primary Care
 Managing Personality Disorders in Primary Care James A. Bourgeois, O.D., M.D. Learning Objectives At end of presentation, attendees will be able to: Classify personality disorders according to DSM-IV-TR
Managing Personality Disorders in Primary Care James A. Bourgeois, O.D., M.D. Learning Objectives At end of presentation, attendees will be able to: Classify personality disorders according to DSM-IV-TR
9 - SCREENING MEASURES FOR PERSONALITY DISORDERS
 ROMANIAN JOURNAL OF EXPERIMENTAL APPLIED PSYCHOLOGY VOL. 7, ISSUE 2 www.rjeap.ro DOI: 10.15303/rjeap.2016.v7i2.a9 9 - SCREENING MEASURES FOR PERSONALITY DISORDERS STELIANA RIZEANU Hyperion University of
ROMANIAN JOURNAL OF EXPERIMENTAL APPLIED PSYCHOLOGY VOL. 7, ISSUE 2 www.rjeap.ro DOI: 10.15303/rjeap.2016.v7i2.a9 9 - SCREENING MEASURES FOR PERSONALITY DISORDERS STELIANA RIZEANU Hyperion University of
Early Maladaptive Schemas And Personality. Disorder Symptoms An Examination In A Nonclinical
 Early Maladaptive Schemas And Personality Disorder Symptoms An Examination In A Non-clinical Sample Objective: This study examined whether some early maladaptive schema (EMS) domains, Results: Findings
Early Maladaptive Schemas And Personality Disorder Symptoms An Examination In A Non-clinical Sample Objective: This study examined whether some early maladaptive schema (EMS) domains, Results: Findings
Can my personality be a disorder?!
 Can my personality be a disorder?! Chapter 10- Personality Disorders What is Personality? There are many characteristics of personality: George is shy Karen is outgoing Missy is such a drama queen Jane
Can my personality be a disorder?! Chapter 10- Personality Disorders What is Personality? There are many characteristics of personality: George is shy Karen is outgoing Missy is such a drama queen Jane
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients. Centerstone Research Institute
 American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
Youth Using Behavioral Health Services. Making the Transition from the Child to Adult System
 Youth Using Behavioral Health Services Making the Transition from the Child to Adult System Allegheny HealthChoices Inc. January 2013 Youth Using Behavioral Health Services: Making the Transition from
Youth Using Behavioral Health Services Making the Transition from the Child to Adult System Allegheny HealthChoices Inc. January 2013 Youth Using Behavioral Health Services: Making the Transition from
MEDICAL POLICY EFFECTIVE DATE: 04/28/11 REVISED DATE: 04/26/12, 04/25/13, 04/24/14, 06/25/15, 06/22/16, 06/22/17
 MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
Can my personality be a disorder?!
 Can my personality be a disorder?! Chapter 11- Personality Disorders How would you describe your personality? A personality refers to a distinctive set of behavior patterns that make up our individuality..
Can my personality be a disorder?! Chapter 11- Personality Disorders How would you describe your personality? A personality refers to a distinctive set of behavior patterns that make up our individuality..
Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale
 Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale By: Thomas R Kwapil, Monica C. Mann and Michael L. Raulin Kwapil, T.R., Mann, M.C., & Raulin, M.L. (2002). Psychometric
Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale By: Thomas R Kwapil, Monica C. Mann and Michael L. Raulin Kwapil, T.R., Mann, M.C., & Raulin, M.L. (2002). Psychometric
Personality disorders. Eccentric (Cluster A) Dramatic (Cluster B) Anxious(Cluster C)
 Personality disorders Eccentric (Cluster A) Dramatic (Cluster B) Anxious(Cluster C) Personality Enduring pattern of perceiving, relating to and thinking about the environment and oneself in a wide range
Personality disorders Eccentric (Cluster A) Dramatic (Cluster B) Anxious(Cluster C) Personality Enduring pattern of perceiving, relating to and thinking about the environment and oneself in a wide range
Predictors of 2-year outcome for patients with borderline personality disorder
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. May, 2006 Predictors of 2-year outcome for patients with borderline personality disorder John G. Gunderson Maria T. Daversa Carlos
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. May, 2006 Predictors of 2-year outcome for patients with borderline personality disorder John G. Gunderson Maria T. Daversa Carlos
Dynamic Deconstructive Psychotherapy
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
Fabrizio Didonna, Paolo Zordan, Elena Prunetti, Denise Rigoni, Marzia Zorzi, Marco Bateni Unit for Anxiety and Mood Disorders Unit for Personality
 35th International Congress of SPR 16-19 June 2004 Roma - Italy Clinical features of obsessive symptoms in Borderline Personality Disorders and Obsessive Compulsive Disorders: Differences and overlapping
35th International Congress of SPR 16-19 June 2004 Roma - Italy Clinical features of obsessive symptoms in Borderline Personality Disorders and Obsessive Compulsive Disorders: Differences and overlapping
Universities of Leeds, Sheffield and York
 promoting access to White Rose research papers Universities of Leeds, Sheffield and York http://eprints.whiterose.ac.uk/ This is an author produced version of a paper published in Drug and Alcohol Review.
promoting access to White Rose research papers Universities of Leeds, Sheffield and York http://eprints.whiterose.ac.uk/ This is an author produced version of a paper published in Drug and Alcohol Review.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality disorder: the management and prevention of antisocial (dissocial) personality disorder 1.1 Short title Antisocial
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality disorder: the management and prevention of antisocial (dissocial) personality disorder 1.1 Short title Antisocial
Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group Treatment for Women in Secure Settings
 Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
COMORBIDITY OF ALCOHOL DEPENDENCE AND PERSONALITY DISORDERS: A COMPARATIVE STUDY
 Alcohol & Alcoholism Vol. 42, No. 6, pp. 618 622, 2007 Advance Access publication 31 August 2007 doi:10.1093/alcalc/agm050 COMORBIDITY OF ALCOHOL DEPENDENCE AND PERSONALITY DISORDERS: A COMPARATIVE STUDY
Alcohol & Alcoholism Vol. 42, No. 6, pp. 618 622, 2007 Advance Access publication 31 August 2007 doi:10.1093/alcalc/agm050 COMORBIDITY OF ALCOHOL DEPENDENCE AND PERSONALITY DISORDERS: A COMPARATIVE STUDY
The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders
 AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
9/12/2012 ALCOHOL AND DRUG USE, ASSOCIATED DISORDERS AND THEIR PSYCHIATRIC COMORBIDITIES IN U.S. ADULTS OBJECTIVES
 ALCOHOL AND DRUG USE, ASSOCIATED DISORDERS AND THEIR PSYCHIATRIC COMORBIDITIES IN U.S. ADULTS Risë B. Goldstein, Ph.D., M.P.H., Staff Scientist Laboratory of Epidemiology and Biometry Division of Intramural
ALCOHOL AND DRUG USE, ASSOCIATED DISORDERS AND THEIR PSYCHIATRIC COMORBIDITIES IN U.S. ADULTS Risë B. Goldstein, Ph.D., M.P.H., Staff Scientist Laboratory of Epidemiology and Biometry Division of Intramural
Personality Disorders. Mark Kimsey, M.D. March 8, 2014
 Personality Disorders Mark Kimsey, M.D. March 8, 2014 Objectives Understanding personality disorders using criteria from DSM-5. Learn approaches for separating personality disorders from other major illnesses.
Personality Disorders Mark Kimsey, M.D. March 8, 2014 Objectives Understanding personality disorders using criteria from DSM-5. Learn approaches for separating personality disorders from other major illnesses.
Course syllabus. Psychodynamic and cognitive-behavioral models of mental disorders.
 Course syllabus Course title Instructor s name Contact details Affiliation Course format Psychodynamic and cognitive-behavioral models of mental disorders. Agnieszka Chrzczonowicz Stępień, Ph.D. ag.chrzczonowicz@gmail.com
Course syllabus Course title Instructor s name Contact details Affiliation Course format Psychodynamic and cognitive-behavioral models of mental disorders. Agnieszka Chrzczonowicz Stępień, Ph.D. ag.chrzczonowicz@gmail.com
DBT Modification/ Intervention
 Table 2. Published Studies Examining Application of Inpatient DBT (alphabetical listing) Citation Inpatient Setting DBT Sample Comparison Sample DBT Modification/ Intervention Outcome Measures Results
Table 2. Published Studies Examining Application of Inpatient DBT (alphabetical listing) Citation Inpatient Setting DBT Sample Comparison Sample DBT Modification/ Intervention Outcome Measures Results
ORIGINAL ARTICLE. Introduction
 ORIGINAL ARTICLE (2009) 14, 1051 1066 & 2009 Nature Publishing Group All rights reserved 1359-4184/09 $32.00 www.nature.com/mp Sociodemographic and psychopathologic predictors of first incidence of DSM-IV
ORIGINAL ARTICLE (2009) 14, 1051 1066 & 2009 Nature Publishing Group All rights reserved 1359-4184/09 $32.00 www.nature.com/mp Sociodemographic and psychopathologic predictors of first incidence of DSM-IV
LOUISIANA MEDICAID PROGRAM ISSUED: 04/13/10 REPLACED: 03/01/93 CHAPTER 13: MENTAL HEALTH CLINICS SECTION13.1: SERVICES PAGE(S) 9 SERVICES
 SERVICES The clinic services covered under the program are defined as those preventive, diagnostic, therapeutic, rehabilitative, or palliative items or services that are furnished to an outpatient by or
SERVICES The clinic services covered under the program are defined as those preventive, diagnostic, therapeutic, rehabilitative, or palliative items or services that are furnished to an outpatient by or
Relationship Between Clinician Assessment and Self-Assessment of Personality Disorders Using the SWAP-200 and PAI
 Psychological Assessment Copyright 2007 by the American Psychological Association 2007, Vol. 19, No. 2, 225 229 1040-3590/07/$12.00 DOI: 10.1037/1040-3590.19.2.225 BRIEF REPORTS Relationship Between Clinician
Psychological Assessment Copyright 2007 by the American Psychological Association 2007, Vol. 19, No. 2, 225 229 1040-3590/07/$12.00 DOI: 10.1037/1040-3590.19.2.225 BRIEF REPORTS Relationship Between Clinician
Client Retention Paper. Scott J. Busby. Abilene Christian University
 Running head: CLIENT RETENTION PAPER Client Retention Paper Scott J. Busby Abilene Christian University CLIENT RETENTION PAPER 2 Introduction Client retention and attrition are concepts linked to the outcome
Running head: CLIENT RETENTION PAPER Client Retention Paper Scott J. Busby Abilene Christian University CLIENT RETENTION PAPER 2 Introduction Client retention and attrition are concepts linked to the outcome
Copyright American Psychological Association. Introduction
 Introduction Personality disorders (PDs) are commonly encountered in practice, but their management is challenging. Patients with these diagnoses can be described as the stepchildren of the mental health
Introduction Personality disorders (PDs) are commonly encountered in practice, but their management is challenging. Patients with these diagnoses can be described as the stepchildren of the mental health
Personality and Mental Health 5: (2011) Published online 19 December 2010 in Wiley Online Library (wileyonlinelibrary.com) DOI: /pmh.
 Personality and Mental Health 5: 12 28 (2011) Published online 19 December 2010 in Wiley Online Library (wileyonlinelibrary.com).152 Clinicians use of personality disorder models within a particular treatment
Personality and Mental Health 5: 12 28 (2011) Published online 19 December 2010 in Wiley Online Library (wileyonlinelibrary.com).152 Clinicians use of personality disorder models within a particular treatment
Overview of Treatment Engagement Findings from DATOS
 Drug Abuse Outcome Studies (Funded by NIDA) Overview of Engagement Findings from DATOS Charts Prepared & Released for Public Use by Dwayne Simpson (TCU), Robert Hubbard (NDRI-NC), Douglas Anglin (UCLA),
Drug Abuse Outcome Studies (Funded by NIDA) Overview of Engagement Findings from DATOS Charts Prepared & Released for Public Use by Dwayne Simpson (TCU), Robert Hubbard (NDRI-NC), Douglas Anglin (UCLA),
The Value of Engagement in Substance Use Disorder (SUD) Treatment
 The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
Assessing Outpatient Drug Abuse
 _ Articles Assessing Outpatient Drug Abuse Treatment Programs FRANK M. TIMS, ARTHUR M. HORTON, JR., BENNETT W. FLETCHER, and RICHARD H. PRICE Drug abuse is a major domestic health problem in the United
_ Articles Assessing Outpatient Drug Abuse Treatment Programs FRANK M. TIMS, ARTHUR M. HORTON, JR., BENNETT W. FLETCHER, and RICHARD H. PRICE Drug abuse is a major domestic health problem in the United
CLINICAL VS. BEHAVIOR ASSESSMENT
 CLINICAL VS. BEHAVIOR ASSESSMENT Informal Tes3ng Personality Tes3ng Assessment Procedures Ability Tes3ng The Clinical Interview 3 Defining Clinical Assessment The process of assessing the client through
CLINICAL VS. BEHAVIOR ASSESSMENT Informal Tes3ng Personality Tes3ng Assessment Procedures Ability Tes3ng The Clinical Interview 3 Defining Clinical Assessment The process of assessing the client through
Examining Criterion A: DSM-5 Level of Personality Functioning as Assessed through Life Story Interviews
 Washington University in St. Louis Washington University Open Scholarship Arts & Sciences Electronic Theses and Dissertations Arts & Sciences Winter 12-2016 Examining Criterion A: DSM-5 Level of Personality
Washington University in St. Louis Washington University Open Scholarship Arts & Sciences Electronic Theses and Dissertations Arts & Sciences Winter 12-2016 Examining Criterion A: DSM-5 Level of Personality
The University of Calgary Department of Psychology. Adult Psychopathology. Psychology 651 (L01) Fall 2005
 vw The University of Calgary Department of Psychology Adult Psychopathology Psychology 651 (L01) Fall 2005 Instructor: Candace Konnert, Ph.D., C.Psych. Lecture Location: Admin. 247B Phone: 220-4976 Lecture
vw The University of Calgary Department of Psychology Adult Psychopathology Psychology 651 (L01) Fall 2005 Instructor: Candace Konnert, Ph.D., C.Psych. Lecture Location: Admin. 247B Phone: 220-4976 Lecture
Neuroticism Behaviour Between Sportsmen And Non-Sportsmen - A Comparative Analysis
 IOSR Journal of Sports and Physical Education (IOSR-JSPE) e-issn: 2347-6737, p-issn: 2347-6745, Volume 3, Issue 5 (Sep. Oct. 216), PP 31-36 www.iosrjournals.org Neuroticism Behaviour Between Sportsmen
IOSR Journal of Sports and Physical Education (IOSR-JSPE) e-issn: 2347-6737, p-issn: 2347-6745, Volume 3, Issue 5 (Sep. Oct. 216), PP 31-36 www.iosrjournals.org Neuroticism Behaviour Between Sportsmen
TEACHING PLAN. Academic Year Subject: Abnormal Psychology Paper no: PSY 113
 Class: B.A. Third Year Subject: Abnormal Psychology Paper no: PSY 113 Periods per week: 04 s: (Total): 1 1.Abnormal Behavior in our times: i. What is abnormal Psychology?, What do we mean by Abnormal behavior?
Class: B.A. Third Year Subject: Abnormal Psychology Paper no: PSY 113 Periods per week: 04 s: (Total): 1 1.Abnormal Behavior in our times: i. What is abnormal Psychology?, What do we mean by Abnormal behavior?
OUTPATIENT TREATMENT WESTPORT, CONNECTICUT
 OUTPATIENT TREATMENT WESTPORT, CONNECTICUT ABOUT CLEARPOINT At Clearpoint, we focus on healing the whole person: mind, body, and spirit. Our comprehensive care methods set clients up for long-term success
OUTPATIENT TREATMENT WESTPORT, CONNECTICUT ABOUT CLEARPOINT At Clearpoint, we focus on healing the whole person: mind, body, and spirit. Our comprehensive care methods set clients up for long-term success
NIH Public Access Author Manuscript Psychol Assess. Author manuscript.
 NIH Public Access Author Manuscript The Impact of NEO PI-R Gender-Norms on the Assessment of Personality Disorder Profiles Douglas B. Samuel, Department of Psychiatry, Yale University School of Medicine
NIH Public Access Author Manuscript The Impact of NEO PI-R Gender-Norms on the Assessment of Personality Disorder Profiles Douglas B. Samuel, Department of Psychiatry, Yale University School of Medicine
The DSM-5 Draft: Critique and Recommendations
 The DSM-5 Draft: Critique and Recommendations Psychological Injury and Law ISSN 1938-971X Volume 3 Number 4 Psychol. Inj. and Law (2010) 3:320-322 DOI 10.1007/s12207-010-9091- y 1 23 Your article is protected
The DSM-5 Draft: Critique and Recommendations Psychological Injury and Law ISSN 1938-971X Volume 3 Number 4 Psychol. Inj. and Law (2010) 3:320-322 DOI 10.1007/s12207-010-9091- y 1 23 Your article is protected
Comparing Methods for Scoring Personality Disorder Types Using Maladaptive Traits in DSM-5
 486182ASMXXX10.1177/1073191113486182Assessment 20(3)Samuel et al. research-article2013 Article Comparing Methods for Scoring Personality Disorder Types Using Maladaptive Traits in DSM-5 Assessment 20(3)
486182ASMXXX10.1177/1073191113486182Assessment 20(3)Samuel et al. research-article2013 Article Comparing Methods for Scoring Personality Disorder Types Using Maladaptive Traits in DSM-5 Assessment 20(3)
Can my personality be a disorder?!
 Can my personality be a disorder?! Chapter 11- Personality Disorders 1 A personality refers to a distinctive set of behavior patterns that make up our individuality. Our personality consists of traits
Can my personality be a disorder?! Chapter 11- Personality Disorders 1 A personality refers to a distinctive set of behavior patterns that make up our individuality. Our personality consists of traits
Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities
 Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities By: Dr. Ehsane M. Gad M.B.B.Ch CABMSPsych. D.P.P Post-Fellow Aus. Consultant Child Psychiatry Childhood ADHD and emergence
Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities By: Dr. Ehsane M. Gad M.B.B.Ch CABMSPsych. D.P.P Post-Fellow Aus. Consultant Child Psychiatry Childhood ADHD and emergence
Relationships of Dissociative Disorders and Personality Traits in Opium Addicts on Methadone Treatment
 Abstract Relationships of Dissociative Disorders and Personality Traits in Opium Addicts on Methadone Treatment Alireza Ghafarinezhad MD 1, Ghodratollah Rajabizadeh MD 1, Vahid Shahriari MD 2 Original
Abstract Relationships of Dissociative Disorders and Personality Traits in Opium Addicts on Methadone Treatment Alireza Ghafarinezhad MD 1, Ghodratollah Rajabizadeh MD 1, Vahid Shahriari MD 2 Original
A Simplified Technique for Scoring DSM-IV Personality Disorders With the Five-Factor Model
 ASSESSMENT 10.1177/1073191105280987 Miller et al. / SCORING PERSONALITY DISORDERS WITH FFM A Simplified Technique for Scoring DSM-IV Personality Disorders With the Five-Factor Model Joshua D. Miller University
ASSESSMENT 10.1177/1073191105280987 Miller et al. / SCORING PERSONALITY DISORDERS WITH FFM A Simplified Technique for Scoring DSM-IV Personality Disorders With the Five-Factor Model Joshua D. Miller University
Long term predictive validity of diagnostic models for personality disorder: Integrating trait and disorder concepts
 Wesleyan University WesScholar Division III Faculty Publications Natural Sciences and Mathematics February 2012 Long term predictive validity of diagnostic models for personality disorder: Integrating
Wesleyan University WesScholar Division III Faculty Publications Natural Sciences and Mathematics February 2012 Long term predictive validity of diagnostic models for personality disorder: Integrating
Practical Tips for Dealing with Difficult People (or What Do I Do In The Real World?)
 Practical Tips for Dealing with Difficult People (or What Do I Do In The Real World?) Ronald Fraser, MD, CSPQ, FRCPC Associate Professor Department of Psychiatry McGill University Dalhousie University
Practical Tips for Dealing with Difficult People (or What Do I Do In The Real World?) Ronald Fraser, MD, CSPQ, FRCPC Associate Professor Department of Psychiatry McGill University Dalhousie University
CULTURE-SPECIFIC INFORMATION
 NAME: Sanctuary 0000: General Name Model Spelled Culture-Specific Information Out Information Engagement For which specific cultural group(s) (i.e., SES, religion, race, ethnicity, gender, immigrants/refugees,
NAME: Sanctuary 0000: General Name Model Spelled Culture-Specific Information Out Information Engagement For which specific cultural group(s) (i.e., SES, religion, race, ethnicity, gender, immigrants/refugees,
ABNORMAL PSYCHOLOGY. Psychological Disorders. Fast Track Chapter 11 (Bernstein Chapter 15)
 ABNORMAL PSYCHOLOGY Psychological Disorders Fast Track Chapter 11 (Bernstein Chapter 15) Introduction to Abnormal Psychology PSYCHOPATHOLOGY the study of the causes, symptoms, and development of psychological
ABNORMAL PSYCHOLOGY Psychological Disorders Fast Track Chapter 11 (Bernstein Chapter 15) Introduction to Abnormal Psychology PSYCHOPATHOLOGY the study of the causes, symptoms, and development of psychological
Available online at
 Available online at www.sciencedirect.com Comprehensive Psychiatry 49 (2008) 141 145 www.elsevier.com/locate/comppsych An examination of the factor structure of Diagnostic and Statistical Manual of Mental
Available online at www.sciencedirect.com Comprehensive Psychiatry 49 (2008) 141 145 www.elsevier.com/locate/comppsych An examination of the factor structure of Diagnostic and Statistical Manual of Mental
by Odd or Eccentric Behavior Paranoid Personality Disorder Pervasive suspiciousness Excessive mistrust of others No delusional thinking Overly sensiti
 Chapter Eleven: Personality Disorders PSY 440: Abnormal Psychology Dr. Rick Grieve Western Kentucky University Personality Disorders Personality Disorder Excessively rigid patterns of behavior or ways
Chapter Eleven: Personality Disorders PSY 440: Abnormal Psychology Dr. Rick Grieve Western Kentucky University Personality Disorders Personality Disorder Excessively rigid patterns of behavior or ways
Acute Stabilization In A Trauma Program: A Pilot Study. Colin A. Ross, MD. Sean Burns, MA, LLP
 In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
Evaluating the Co-morbidity of Major Depression Disorder and Personality Disorder in Year Old Women Referring to Outpatient Clinics
 Evaluating the Co-morbidity of Major Depression Disorder and Personality Disorder in 18-60 Year Old Women Referring to Outpatient Clinics Farrokh Lagha Alhooei 1, Omid Rezaei* 2, Behrooz Dolatshahi 3 1.
Evaluating the Co-morbidity of Major Depression Disorder and Personality Disorder in 18-60 Year Old Women Referring to Outpatient Clinics Farrokh Lagha Alhooei 1, Omid Rezaei* 2, Behrooz Dolatshahi 3 1.
Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting
 Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting Distinguishing features of DBT Implementing DBT within Drug Health Services RPAH Case Study Background to DBT Developed in early
Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting Distinguishing features of DBT Implementing DBT within Drug Health Services RPAH Case Study Background to DBT Developed in early
Students With Attention Deficit Hyperactivity Disorder
 On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
Adapting Dialectical Behavior. Therapy for Special Populations
 Adapting Dialectical Behavior Therapy for Special Populations Margaret Charlton, PhD, ABPP Aurora Mental Health Center Intercept Center 16905 E. 2nd Avenue Aurora, CO 80011 303-326-3748 MargaretCharlton@aumhc.org
Adapting Dialectical Behavior Therapy for Special Populations Margaret Charlton, PhD, ABPP Aurora Mental Health Center Intercept Center 16905 E. 2nd Avenue Aurora, CO 80011 303-326-3748 MargaretCharlton@aumhc.org
UNC-CH School of Social Work Clinical Lecture Series 10/17/2016
 UNC Chapel Hill School of Social Work Clinical Lecture Series DBT FOR ADOLESCENTS: WORKING WITH SUICIDAL, SELF-HARMING, AND EMOTIONALLY SENSITIVE YOUTH Lorie A. Ritschel, Ph.D. Assistant Professor, UNC
UNC Chapel Hill School of Social Work Clinical Lecture Series DBT FOR ADOLESCENTS: WORKING WITH SUICIDAL, SELF-HARMING, AND EMOTIONALLY SENSITIVE YOUTH Lorie A. Ritschel, Ph.D. Assistant Professor, UNC
HIBBING COMMUNITY COLLEGE COURSE OUTLINE
 HIBBING COMMUNITY COLLEGE COURSE OUTLINE COURSE NUMBER & TITLE: PSYC 1400: Abnormal Psychology CREDITS: 3 (3Lec 0 / Lab) PREREQUISITES: PSYC 1205: General Psychology CATALOG DESCRIPTION: Abnormal Psychology
HIBBING COMMUNITY COLLEGE COURSE OUTLINE COURSE NUMBER & TITLE: PSYC 1400: Abnormal Psychology CREDITS: 3 (3Lec 0 / Lab) PREREQUISITES: PSYC 1205: General Psychology CATALOG DESCRIPTION: Abnormal Psychology
Psychosis, Mood, and Personality: A Clinical Perspective
 Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment
 025-030_PB_V39N1_de_Haan.qxd 9/21/06 5:35 PM Page 25 ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment Reliability and Validity of the Yale-Brown
025-030_PB_V39N1_de_Haan.qxd 9/21/06 5:35 PM Page 25 ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment Reliability and Validity of the Yale-Brown
The Addiction Severity Index in Clinical Efficacy Trials of Medications for Cocaine Dependence
 The Addiction Severity Index in Clinical Efficacy Trials of Medications for Cocaine Dependence John S. Cacciola, Arthur I. Alterman, Charles P. O Brien, and A. Thomas McLellan INTRODUCTION The Addiction
The Addiction Severity Index in Clinical Efficacy Trials of Medications for Cocaine Dependence John S. Cacciola, Arthur I. Alterman, Charles P. O Brien, and A. Thomas McLellan INTRODUCTION The Addiction
SUD Requirements. Proprietary
 SUD Requirements Triage screening to determine eligibility and appropriateness (proper member placement) for admission and referral. A comprehensive bio-psychosocial evaluation must be completed prior
SUD Requirements Triage screening to determine eligibility and appropriateness (proper member placement) for admission and referral. A comprehensive bio-psychosocial evaluation must be completed prior
DSM-5 AND ASAM CRITERIA. Presented by Jaime Goffin, LCSW
 DSM-5 AND ASAM CRITERIA Presented by Jaime Goffin, LCSW MODULE 1: GOALS & OBJECTIVES What is your experience with using ASAM and DSM 5 criteria? What are your learning expectations for today? GOAL FOR
DSM-5 AND ASAM CRITERIA Presented by Jaime Goffin, LCSW MODULE 1: GOALS & OBJECTIVES What is your experience with using ASAM and DSM 5 criteria? What are your learning expectations for today? GOAL FOR
Background Paper: Shy Children. Briana Jackson. University of Pittsburgh. December 2011
 1 Background Paper: Shy Children Briana Jackson University of Pittsburgh December 2011 2 Shy Children Being shy is a highly occurring trait. It is seen in our family members, friends, partners, peers,
1 Background Paper: Shy Children Briana Jackson University of Pittsburgh December 2011 2 Shy Children Being shy is a highly occurring trait. It is seen in our family members, friends, partners, peers,
JC Sunnybrook HEALTH SCIENCES CENTRE
 Dear Referring Provider: Thank you for referring your patient to the Frederick W. Thompson Anxiety Disorders Centre at Sunnybrook Health Sciences Centre. The attached form will assist us in determining
Dear Referring Provider: Thank you for referring your patient to the Frederick W. Thompson Anxiety Disorders Centre at Sunnybrook Health Sciences Centre. The attached form will assist us in determining
Objectives. Why Anxiety? The Effect of Cranial Electrotherapy Stimulation (CES) on Anxiety Symptoms Following Opiate and Alcohol Withdrawal - An RCT
 The Effect of Cranial Electrotherapy Stimulation (CES) on Anxiety Symptoms Following Opiate and Alcohol Withdrawal - An RCT Janet Hutchison PhD ARNP- BC Adult Health, Addictions, Psychiatric mental Health
The Effect of Cranial Electrotherapy Stimulation (CES) on Anxiety Symptoms Following Opiate and Alcohol Withdrawal - An RCT Janet Hutchison PhD ARNP- BC Adult Health, Addictions, Psychiatric mental Health
