The current perspective of low grade myelodysplastic syndrome in children
|
|
|
- Quentin Green
- 5 years ago
- Views:
Transcription
1 Int J Hematol (2016) 103: DOI /s PROGRESS IN HEMATOLOGY Pediatric MDS/MPN The current perspective of low grade myelodysplastic syndrome in children Daisuke Hasegawa 1 Received: 5 January 2016 / Revised: 16 February 2016 / Accepted: 16 February 2016 / Published online: 3 March 2016 The Japanese Society of Hematology 2016 Abstract Myelodysplastic syndrome (MDS) without increased blasts, i.e., low-grade MDS, is the most common subtype of pediatric MDS and has characteristics different from adult form of the disease. Although histological findings of bone marrow (BM) biopsies suggest that lowgrade MDS is a morphologically distinctive entity, a subset of pediatric low-grade MDS may clinically overlap with aplastic anemia (AA), such as high likelihood of hypocellular marrow and normal karyotype. In addition, children with low-grade MDS are as likely to respond to immunosuppressive therapy as those with AA, which indicates that a part of these disorders might share a common pathogenesis, that is, T cell-mediated inhibition of hematopoiesis. In contrast, a small part of children with low-grade MDS experience disease progression to advanced MDS. Given that the clinical courses of pediatric low-grade MDS are heterogeneous, assessing prognostic values of clinical, morphological, histological and cytogenetic findings is critical. Thus far, monosomy 7 and multilineage dysplasia have been suggested as prognostic factors that could predict disease progression. Treatment strategy will be optimized based on more precise prognostic factors. In the future, molecular findings may also help prognostification in children with hypoplastic BM disorders. Keywords Myelodysplastic syndrome Refractory cytopenia of childhood Immunosuppressive therapy Hematopoietic stem cell transplantation * Daisuke Hasegawa hase dai@umin.net 1 Department of Pediatrics, St. Luke s International Hospital, 9 1, Akashi cho, Chuo ku, Tokyo , Japan Introduction Myelodysplastic syndrome (MDS) is a term defined as a group of clonal hematopoietic stem cell disorders characterized by cytopenia, dysplasia in any one of the myeloid lineages, ineffective hematopoiesis and a varying propensity to transform into acute myeloid leukemia (AML). MDS is uncommon in children compared to the elderly, and several differences between MDS in children and adults have been identified, such as the rarity of refractory anemia with ringed sideroblasts and MDS associated with del(5q) chromosome [1]. In addition, pediatric MDS can evolve from inherited bone marrow failure syndromes (IBMFS) such as Fanconi anemia (FA). Considering these differences, a pediatric approach to the diagnosis and management of MDS was proposed in 2003 [1] and was incorporated into the 4th edition of the World Health Organization (WHO) classification in 2008 [2]. This classification mentioned unique characteristics of pediatric MDS without increased blasts, i.e., low-grade MDS. For example, neutropenia and thrombocytopenia are more likely to be the presenting manifestation in children in contrast to adults who often present with isolated anemia [3]. Children with low-grade MDS frequently show hypocellular marrow [3]. Consequently, refractory cytopenia of childhood (RCC) was introduced as a provisional entity in the 2008 WHO classification [2]. It is recommended that children who meet the criteria for refractory cytopenia with multilineage dysplasia (RCMD) be considered as RCC until the prognostic significance of a multilineage dysplasia is clarified in children [2]. This review overviews the clinical, morphological and pathobiological characteristics of low-grade MDS in childhood and discusses appropriate management and treatment
2 The current perspective of low-grade myelodysplastic syndrome in children 361 strategy. Current problems concerning the concept of RCC are also addressed. Clinical characteristics Pediatric MDS is an uncommon disorder accounting for 5 10 % of all hematological malignancies in childhood [1]. Of those, low-grade MDS is the most common subtype. From February 2009 to October 2013, 1000 children who were suspected of having MDS, myeloproliferative neoplasms and bone marrow (BM) failure were prospectively registered into the Japanese Society of Pediatric Hematology/Oncology database and underwent the central review of morphology and histology [4]. Of those, 339 and 24 children were diagnosed with de novo low-grade MDS and refractory anemia with excess blasts (RAEB), respectively (Fig. 1). This indicated that the annual incidence of de novo MDS in Japan was 78 cases, more than 90 % of which were classified as low-grade MDS. Low-grade MDS is diagnosed in all age groups with median age at diagnosis ranging from 6 to 12 years from three representative reports (Table 1) [3, 5, 6]. Boys and girls are equally affected. Children usually present with symptoms related to cytopenias such as bleeding tendency, infection and pallor. Some children have no clinical symptoms and can be diagnosed by chance. Cytopenias are generally milder in low-grade MDS than aplastic anemia (AA). A Japanese prospective registry revealed normal karyotype in 41 out of 65 children (65 %) with low-grade MDS, whereas monosomy 7 was found in only 5 (8 %) [5]. Morphology and histology The 2008 WHO classification defines RCC as a childhood MDS characterized by persistent cytopenia with <5 % blasts in the BM, <2 % blasts in the peripheral blood (PB) and dysplastic changes in two or three lineages or exceeding 10 % in one single lineage [2]. BM cellularity was reduced in about half of the children with low-grade MDS [3, 5]. In children, cytopenias with decrease of BM cellularity might be caused by various underlying disorders, including AA, IBMFS and other hematological and nonhematological disorders [7]. Morphological abnormalities may also be found in these disorders. Of those, AA and Total ( ) 1,000 Bone marrow failure 570 AA 137 RCC 236 RCMD 103 Neutropenia 3% Thrombocytopenia 5% Anemia Others Hepatitis-related 38 PNH 3 IBMFS 53 Advanced MDS / AML 97 MPN 12% BMF 5 RAEB 24 Therapy-related 21 AA-related 1 Advanced MDS/AML 10% IBMFS-related 5 De novo AML 32 Down syndrome-related 14 MPN 116 Anemia 68 Thrombocytopenia 51 Neutropenia 26 Others 72 Hepatitis PNH 1% RCMD 18% IBMF 9% AA 24% RCC 41% Fig. 1 Distribution of patients with myelodysplastic syndrome, myeloproliferative neoplasms and bone marrow failure in Japan. One thousand patients prospectively underwent the central review of morphology and histology from February 2009 to October This data was provided by the courtesy of Dr. Asahito Hama
3 362 D. Hasegawa Table 1 Clinical and hematological findings of low-grade MDS in childhood Reference Kardos et al. [3] Hasegawa et al. [5] Hama et al. [6] RCC RCMD Age at diagnosis a (years) 8.3 ( ) 7.8 ( ) 6 (1 16) 12 (2 16) Male/female 30/37 34/31 51/40 19/15 Neutrophils a ( 10 9 /L) 0.9 (0 6.7) 0.9 ( ) 0.95 (0 3.1) 1.0 ( ) Hemoglobin a (g/dl) 9.5 ( ) 7.6 ( ) 7.3 (2.5 11) 8.6 ( ) Reticulocyte a, b 1.0 % (0 6.7 %) 49.0 ( ) 35 (1 91) 55 (7.6 99) MCV a (fl) 98 (80 140) ( ) NA NA Platelet a ( 10 9 /L) 65 (0 450) 35 (3 403) 28 (2 73) 19 (1 68) MCV mean corpuscular volume, NA not available, RCC refractory cytopenia of childhood, RCMD refractory cytopenia with multilineage dysplasia a Median (range) b Reticulocyes were indicated in percentage by Kardos, whereas in absolute numbers ( 10 9 /L) by other two reports Fig. 2 Representative pictures of bone marrow (BM) biopsies obtained from patients with pediatric low-grade MDS (AS-D naphthol chloroacetate esterase stain with Giemsa staining). a, b BM specimens of hypocellular refractory cytopenia of childhood; c, d those of hypercellular refractory cytopenia with multilineage dysplasia. a Patchy distribution of erythropoiesis accompanied by sparsely distributed granulopoiesis, in an otherwise adipocytic BM. b Immature erythroid precursors form one or several islands. c Immature erythropoiesis and granulopoiesis are distributed diffusely. d Left-shifted erythroid and myeloid cells are increased. These pictures were provided by the courtesy of Dr. Masafumi Ito IBMFS are the most common and important differential diagnoses of low-grade MDS, however, the clinical and histopathological distinction between these three disorders is challenging. Since hematopoietic cells in hypocellular low-grade MDS are often distributed in a patchy pattern (Fig. 2a), information obtained from aspiration cytology
4 The current perspective of low-grade myelodysplastic syndrome in children 363 is limited [7, 8]. Therefore, BM biopsies, which mirror the topography and cellularity of the local hematopoiesis, should be performed at least twice to diagnose hypoplastic BM disorders in children [2, 7, 8]. Patchy erythropoiesis with impaired maturation, accompanied by sparsely distributed granulopoiesis, in an otherwise adipocytic BM is characteristic of hypoplastic low-grade MDS (Fig. 2b) [2, 7, 8]. Megakaryocytes are markedly decreased or absent. Immunohistochemistry is mandatory for the detection of micromegakaryocytes. A subset of children with low-grade MDS shows normo- or hypercellular BM, in which hematopoietic cells are diffusely distributed and dysplasia may be prominent (Fig. 2c, d). Since IBMFS, such as FA and dyskeratosis congenital (DC), show overlapping morphological features with lowgrade MDS and AA, IBMFS has to be excluded by careful past medical and family history, and thorough physical examination. Several laboratory studies, such as chromosome breakage test and telomere length assay, should be considered in the differential diagnosis of hypoplastic BM disorders, because children without any phenotypic features can be diagnosed with IBMFS. In fact, Yoshimi et al. [9] reported that FA and DC were found in patients with hypo- or normocellular RCC with a prevalence of 14 and 2 %, respectively. Pathobiology Intrinsic defects in hematopoietic stem cell caused by acquired cytogenetic and genetic abnormalities are thought as hallmark features of adult MDS. Recently, the molecular basis has been comprehensively addressed in a large cohort of MDS and AA in adults [10, 11]; however, molecular pathogenesis of pediatric MDS is still largely unknown except that spliceosome mutations are found to be rare in pediatric MDS [12]. Given that immunosuppressive therapy (IST) is effective in some children with low-grade MDS as well as MDS in adults or AA [13 15], a part of these disorders might share a common pathogenesis, that is, T cell-mediated inhibition of hematopoiesis. Indeed, T cell oligoclonality was identified in 40 % of RCC patients [16]. Minor paroxysmal nocturnal hemoglobinuria clones, which are thought to be a predictor of favorable response to IST, were also detected in 41 % of RCC patients [17]. These findings suggest that pathogenesis attributes to activated T cells in a subset of children with low-grade MDS. Management and treatment strategy The analysis of treatment outcome of 65 cases with lowgrade MDS revealed heterogeneity in the clinical courses [5]. Approximately, a third of the patients remained stable for long periods without IST or hematopoietic stem cell transplantation (HSCT), whereas eight of 65 patients suffered from progressive disease. Kardos et al. [3] reported that monosomy 7 significantly correlated with progression to advanced MDS. Because patients whose disease progressed before HSCT fared significantly worse, those with monosomy 7 as well as complex karyotype were encouraged to be transplanted as soon as possible. Those who suffer from transfusion dependency or severe neutropenia may also be candidates for HSCT if suitable donor is available. Because transplant-related mortality is the major cause of treatment failure in children with low-grade MDS [18], reduced-intensity conditioning (RIC) regimen is an attractive option [19, 20]; however, it remains to be established whether RIC is an appropriate regimen for children with low-grade MDS with multilineage dysplasia, hypercellularity, or unfavorable karyotype. If children with low-grade MDS without unfavorable karyotype require therapeutic intervention but suitable donor is unavailable, IST may be an advisable option. IST consisting of antithymocyte globulin (ATG) and cyclosporine has proven to be effective in a subset of children with low-grade MDS, with response rate ranging from 30 to 70 % [5, 6, 14, 15, 21]. Some patients with chromosomal abnormalities or multilineage dysplasia were also reported to respond to IST [5, 6, 14, 15, 21]. However, patients who received IST remain at risk of clonal evolution and relapse, and the long-term failure-free survival rate was estimated as only % [5, 21]. As reliable biomarkers that can predict response have not yet identified, candidates for IST should be selected with utmost caution. Controversies and future directions RCC seems a morphologically distinctive entity, but its clinical relevance has been challenged. Forester et al. [22] performed retrospective analysis of children previously diagnosed with AA and found that histologic diagnosis of RCC did not predict IST failure or clonal evolution. Hama et al. also argued that morphological classification (AA, RCC and RCMD) did not correlate with IST response or clonal evolution in the retrospective analysis. Although some clinical features of RCC may overlap with AA, these results should be interpreted with cautions, since they retrospectively analyzed a cohort of patients who had been diagnosed with AA. Another controversial point in the concept of RCC is significance of multilineage dysplasia, which correlated with deterioration of cytopenia during the watchful observation period and disease progression in our analysis [5]. To select patients who would fail IST, experience clonal evolution and require HSCT at the early phase
5 364 D. Hasegawa of the disease, comprehensive prospective study assessing prognostic values of clinical, morphological, histological and cytogenetic findings and predefined treatment assignment will be needed. In the future, molecular findings may also help prognostification in children with hypoplastic BM disorders [23]. Acknowledgments The author would like to thank Ms. Y Imanishi for preparing and refining the patients data, and Drs. S Kojima, A Hama, K Nozawa and M Ito for central review of specimens. The author also thanks Dr. A Manabe for valuable advice. Compliance with ethical standards Conflict of interest The author declares no conflict of interest. References 1. Hasle H, Niemeyer CM, Chessells JM, Baumann I, Bennett JM, Kerndrup G, et al. A pediatric approach to the WHO classification of myelodysplastic and myeloproliferative diseases. Leukemia. 2003;17: Baumann I, Niemeyer CM, Bennett JM. Childhood myelodysplastic syndrome. In: Swerdlow SH, et al., editors. World Health Organization classification of tumours of haematopoietic and lymphoid tissues. 4th ed. Lyon: IARC Press; p Kardos G, Baumann I, Passmore SJ, Locatelli F, Hasle H, Schultz KR, et al. Refractory anemia in childhood: a retrospective analysis of 67 patients with particular reference to monosomy 7. Blood. 2003;102: Hama A, Manabe A, Hasegawa D, Nozawa K, Okuno Y, Irie M, et al. Central morphology review of childhood bone marrow failure in Japan. Blood. 2014;124:1604 [abstract]. 5. Hasegawa D, Chen X, Hirabayashi S, Ishida Y, Watanabe S, Zaike Y, et al. Clinical characteristics and treatment outcome in 65 cases with refractory cytopenia of childhood defined according to the WHO 2008 classification. Br J Haematol. 2014;166: Hama A, Takahashi Y, Muramatsu H, Ito M, Narita A, Kosaka Y, et al. Comparison of long-term outcomes between children with aplastic anemia and refractory cytopenia of childhood who received immunosuppressive therapy with antithymocyte globulin and cyclosporine. Haematologica. 2015;100: Niemeyer CM, Baumann I. Classification of childhood aplastic anemia and myelodysplastic syndrome. Hematol Am Soc Hematol Educ Progr. 2011;2011: Baumann I, Führer M, Behrendt S, Campr V, Csomor J, Furlan I, et al. Morphological differentiation of severe aplastic anaemia from hypocellular refractory cytopenia of childhood: reproducibility of histopathological diagnostic criteria. Histopathology. 2012;61: Yoshimi A, Niemeyer C, Baumann I, Schwarz-Furlan S, Schindler D, Ebell W, et al. High incidence of Fanconi anaemia in patients with a morphological picture consistent with refractory cytopenia of childhood. Br J Haematol. 2013;160: Haferlach T, Nagata Y, Grossmann V, Okuno Y, Bacher U, Nagae G, et al. Landscape of genetic lesions in 944 patients with myelodysplastic syndromes. Leukemia. 2014;28: Yoshizato T, Dumitriu B, Hosokawa K, Makishima H, Yoshida K, Townsley D, et al. Somatic mutations and clonal hematopoiesis in aplastic anemia. N Engl J Med. 2015;373: Hirabayashi S, Flotho C, Moetter J, Heuser M, Hasle H, Gruhn B, et al. Spliceosomal gene aberrations are rare, coexist with oncogenic mutations, and are unlikely to exert a driver effect in childhood MDS and JMML. Blood. 2012;119:e Sloand EM, Rezvani K. The role of the immune system in myelodysplasia: implications for therapy. Semin Hematol. 2008;45: Yoshimi A, Baumann I, Fuhrer M, Bergsträsser E, Göbel U, Sykora KW, et al. Imunosuppressive therapy with anti-thymocyte globulin and cyclosporine A in selected children with hypoplastic refractory cytopenia. Haematologica. 2007;92: Hasegawa D, Manabe A, Yagasaki H, Ohtsuka Y, Inoue M, Kikuchi A, et al. Treatment of children with refractory anemia: the Japanese childhood MDS Study Group Trial (MDS99). Pediatr Blood Cancer. 2009;53: Aalbers AM, van den Heuvel-Eibrink MM, Baumann I, Beverloo HB, Driessen GJ, Dworzak M, et al. T-cell receptor Vβ skewing frequently occurs in refractory cytopenia of childhood and is associated with an expansion of effector cytotoxic T cells: a prospective study by EWOG-MDS. Blood Cancer J. 2014;4:e Aalbers AM, van der Velden VH, Yoshimi A, Fischer A, Noellke P, Zwaan CM, et al. The clinical relevance of minor paroxysmal nocturnal hemoglobinuria clones in refractory cytopenia of childhood: a prospective study by EWOG-MDS. Leukemia. 2014;28: Starý J, Locatelli F, Niemeyer CM. Stem cell transplantation for aplastic anemia and myelodysplastic syndrome. Bone Marrow Transpl. 2005;35(Suppl 1):S Strahm B, Locatelli F, Bader P, Ehlert K, Kremens B, Zintl F, et al. Reduced intensity conditioning in unrelated donor transplantation for refractory cytopenia in childhood. Bone Marrow Transpl. 2007;40: Inagaki J, Fukano R, Kurauchi K, Noguchi M, Tanioka S, Okamura J. Hematopoietic stem cell transplantation in children with refractory cytopenia of childhood: single-center experience using high-dose cytarabine containing myeloablative and aplastic anemia oriented reduced-intensity conditioning regimens. Biol Blood Marrow Transpl. 2015;21: Yoshimi A, van den Heuvel-Eibrink MM, Baumann I, Schwarz S, Simonitsch-Klupp I, de Paepe P, et al. Comparison of horse and rabbit antithymocyte globulin in immunosuppressive therapy for refractory cytopenia of childhood. Haematologica. 2014;99: Forester CM, Sartain SE, Guo D, Harris MH, Weinberg OK, Fleming MD, et al. Pediatric aplastic anemia and refractory cytopenia: a retrospective analysis assessing outcomes and histomorphologic predictors. Am J Hematol. 2015;90: Patel B, Hirsch C, Clemente M, Sekeres M, Makishima H, Maciejewski JP. Genetic and molecular characterization of myelodysplastic syndromes and related myeloid neoplasms. Int J Hematol. 2015;101:213 8.
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed
 MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
Overview of Aplastic Anemia. Overview of Aplastic Anemia. Epidemiology of aplastic anemia. Normal hematopoiesis 10/6/2017
 Overview of Aplastic Anemia Overview of Aplastic Anemia Peter Westervelt, MD, PhD Professor of Medicine Chief, BMT/Leukemia Section Washington University School of Medicine Epidemiology Normal hematopoiesis
Overview of Aplastic Anemia Overview of Aplastic Anemia Peter Westervelt, MD, PhD Professor of Medicine Chief, BMT/Leukemia Section Washington University School of Medicine Epidemiology Normal hematopoiesis
The histopathology of bone marrow failure in children
 Journal of clinical and experimental hematopathology Vol. 58 No.2, 68-86, 2018 JC lin EH xp ematopathol Review Article The histopathology of bone marrow failure in children Hideto Iwafuchi Bone marrow
Journal of clinical and experimental hematopathology Vol. 58 No.2, 68-86, 2018 JC lin EH xp ematopathol Review Article The histopathology of bone marrow failure in children Hideto Iwafuchi Bone marrow
Classification of Childhood Aplastic Anemia and Myelodysplastic Syndrome
 APLASTIC ANEMIA:BONE MARROW FAILURE Classification of Childhood Aplastic Anemia and Myelodysplastic Syndrome Charlotte M. Niemeyer 1 and Irith Baumann 2 1 University Medical Center Freiburg, Freiburg,
APLASTIC ANEMIA:BONE MARROW FAILURE Classification of Childhood Aplastic Anemia and Myelodysplastic Syndrome Charlotte M. Niemeyer 1 and Irith Baumann 2 1 University Medical Center Freiburg, Freiburg,
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
MDS: Who gets it and how is it diagnosed?
 MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Policy Specific Section:
 Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
myelodysplastic syndrome MDS MDS MDS
 myelodysplastic syndrome MDS MDS 15 10 3 2004 15 MDS 400 2 65 61 70 MDS MDS 1 1 2 3 3 4 1 4 2 3 4 MDS 1982 Bennett French- American-BritishFAB 1 2 WHO 1999 3 2001 4 2002 Vardiman MDS 5 2WHO FAB refractory
myelodysplastic syndrome MDS MDS 15 10 3 2004 15 MDS 400 2 65 61 70 MDS MDS 1 1 2 3 3 4 1 4 2 3 4 MDS 1982 Bennett French- American-BritishFAB 1 2 WHO 1999 3 2001 4 2002 Vardiman MDS 5 2WHO FAB refractory
Outline. What is aplastic anemia? 9/19/2012. Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options
 Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
Border between aplastic anemia and myelodysplastic syndrome
 Int J Hematol (2013) 97:558 563 DOI 10.1007/s12185-013-1324-x PROGRESS IN HEMATOLOGY Advances in the management of acquired aplastic anemia (AA) Border between aplastic anemia and myelodysplastic syndrome
Int J Hematol (2013) 97:558 563 DOI 10.1007/s12185-013-1324-x PROGRESS IN HEMATOLOGY Advances in the management of acquired aplastic anemia (AA) Border between aplastic anemia and myelodysplastic syndrome
Table 1: biological tests in SMD
 Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
Myelodysplastic Syndrome: Let s build a definition
 1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
Changes to the 2016 WHO Classification for the Diagnosis of MDS
 Changes to the 2016 WHO Classification for the Diagnosis of MDS Welcome to Managing MDS. I am Dr. Ulrich Germing, and today, I will provide highlights from the 14th International Symposium on MDS in Valencia,
Changes to the 2016 WHO Classification for the Diagnosis of MDS Welcome to Managing MDS. I am Dr. Ulrich Germing, and today, I will provide highlights from the 14th International Symposium on MDS in Valencia,
The function of the bone marrow. Living with Aplastic Anemia. A Case Study - I. Hypocellular bone marrow failure 5/14/2018
 The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
9/9/2015 HISTORY & EPIDEMIOLOGY. Objectives. Textbook Definition of Aplastic anemia (AA) Epidemiology. History
 Objectives Aplastic Anemia: Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Amy E. DeZern, MD, MHS Assistant Professor of Oncology and Medicine The Johns Hopkins University School
Objectives Aplastic Anemia: Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Amy E. DeZern, MD, MHS Assistant Professor of Oncology and Medicine The Johns Hopkins University School
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification
 What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
Myelodysplastic and myeloproliferative disorders of childhood
 PEDIATRIC HEMATOLOGIC MALIGNANCIES Myelodysplastic and myeloproliferative disorders of childhood Henrik Hasle Department of Pediatrics, Aarhus University Hospital, Aarhus, Denmark Myelodysplastic syndrome
PEDIATRIC HEMATOLOGIC MALIGNANCIES Myelodysplastic and myeloproliferative disorders of childhood Henrik Hasle Department of Pediatrics, Aarhus University Hospital, Aarhus, Denmark Myelodysplastic syndrome
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression
 Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
SESSION 1 Reactive cytopenia and dysplasia
 SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
Aplastic Anemia: Understanding your Disease and Treatment Options
 Aplastic Anemia: Understanding your Disease and Treatment Options No financial relationships or commercial interest related to the content of this presentation Josh Sasine, MD, PhD Hematopoietic Cell Transplant
Aplastic Anemia: Understanding your Disease and Treatment Options No financial relationships or commercial interest related to the content of this presentation Josh Sasine, MD, PhD Hematopoietic Cell Transplant
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Severe Aplastic Anemia in Children and Adolescents. Brigitte Strahm 21. April 2018
 Severe Aplastic Anemia in Children and Adolescents Brigitte Strahm 21. April 2018 Acquired Aplastic Anemia in children What is aquired aplastic anemia? Camitta, Blood 1976 How A.L.G. acts is unknown, but
Severe Aplastic Anemia in Children and Adolescents Brigitte Strahm 21. April 2018 Acquired Aplastic Anemia in children What is aquired aplastic anemia? Camitta, Blood 1976 How A.L.G. acts is unknown, but
Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled. in EWOG-MDS Studies
 Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled in EWOG-MDS Studies EWOG-MDS Consensus Conference Freiburg, October 25/26, 2016 These guidelines
Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled in EWOG-MDS Studies EWOG-MDS Consensus Conference Freiburg, October 25/26, 2016 These guidelines
7/13/2017. PreventionGenetics. How are genes associated with bone marrow failure?
 Personalized Medicine: tic Testing and the Implications for Future Therapies Preventiontics Michael Chicka, PhD, Molecular ticist, Preventiontics Founded in 2004 in Marshfield Wisconsin by Dr. Jim Weber
Personalized Medicine: tic Testing and the Implications for Future Therapies Preventiontics Michael Chicka, PhD, Molecular ticist, Preventiontics Founded in 2004 in Marshfield Wisconsin by Dr. Jim Weber
Review of Aplastic Anemia Guidelines. Seiji Kojima MD. PhD.
 Review of Aplastic Anemia Guidelines Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific Blood
Review of Aplastic Anemia Guidelines Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific Blood
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Session II: Summary. Robert P Hasserjian, MD Professor of Pathology Massachusetts General Hospital and Harvard Medical School
 Session II: Summary Robert P Hasserjian, MD Professor of Pathology Massachusetts General Hospital and Harvard Medical School Disclosure of speaker s interests (Prefix and Last Name) (Potential) conflict
Session II: Summary Robert P Hasserjian, MD Professor of Pathology Massachusetts General Hospital and Harvard Medical School Disclosure of speaker s interests (Prefix and Last Name) (Potential) conflict
Therapeutic Advances in Treatment of Aplastic Anemia. Seiji Kojima MD. PhD.
 Therapeutic Advances in Treatment of Aplastic Anemia Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific
Therapeutic Advances in Treatment of Aplastic Anemia Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific
Myelodysplastic Syndrome Case 158
 Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
June 11, Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI
 June 11, 2018 Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI 53713 policycomments@wpsic.com RE: Draft Local Coverage Determination: MolDX: MDS FISH (DL37772) Dear Dr. Noel Thank you for the opportunity
June 11, 2018 Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI 53713 policycomments@wpsic.com RE: Draft Local Coverage Determination: MolDX: MDS FISH (DL37772) Dear Dr. Noel Thank you for the opportunity
A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes.
 Protocol Synopsis Study Title A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes. Short Title European MDS
Protocol Synopsis Study Title A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes. Short Title European MDS
RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165
 RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165 Sebastian J. Sasu, M.D. UCLA Medical Center, Hematopathology Los Angeles, CA and Saint John s s Health Center Santa Monica, CA Clinical History
RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165 Sebastian J. Sasu, M.D. UCLA Medical Center, Hematopathology Los Angeles, CA and Saint John s s Health Center Santa Monica, CA Clinical History
Myelodysplastic syndromes
 Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Myelodysplastic scoring system with flow cytometry. G Detry B Husson
 Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Aplastic Anemia. is a bone marrow failure disease 9/19/2017. What you need to know about. The 4 major components of blood
 What you need to know about Aplastic Anemia Stuart Goldberg MD Aplastic Anemia is a bone marrow failure disease The bone marrow is the factory that makes blood The 4 major components of blood Red Blood
What you need to know about Aplastic Anemia Stuart Goldberg MD Aplastic Anemia is a bone marrow failure disease The bone marrow is the factory that makes blood The 4 major components of blood Red Blood
Comparison of horse and rabbit anti-thymocyte globulin in immunosuppressive therapy for refractory cytopenia of childhood
 Published Ahead of Print on October 25, 2013, as doi:10.3324/haematol.2013.095786. Copyright 2013 Ferrata Storti Foundation. Comparison of horse and rabbit anti-thymocyte globulin in immunosuppressive
Published Ahead of Print on October 25, 2013, as doi:10.3324/haematol.2013.095786. Copyright 2013 Ferrata Storti Foundation. Comparison of horse and rabbit anti-thymocyte globulin in immunosuppressive
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
ACCME/Disclosures. History. Hematopathology Specialty Conference Case #4 4/13/2016
 Hematopathology Specialty Conference Case #4 Sherrie L. Perkins MD, PhD University of Utah ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose
Hematopathology Specialty Conference Case #4 Sherrie L. Perkins MD, PhD University of Utah ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood
 Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood V. TOULIATOU 1, A. KOLIALEXI 1, G.TH. TSANGARIS 2, M. MOSCHOVI 3, S.
Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood V. TOULIATOU 1, A. KOLIALEXI 1, G.TH. TSANGARIS 2, M. MOSCHOVI 3, S.
Outline. Case Study 5/17/2010. Treating Lower-Risk Myelodysplastic Syndrome (MDS) Tapan M. Kadia, MD Department of Leukemia MD Anderson Cancer Center
 Treating Lower-Risk Myelodysplastic Syndrome (MDS) Tapan M. Kadia, MD Department of Leukemia MD Anderson Cancer Center Outline Case Study What is lower-risk MDS? Classification systems Prognosis Treatment
Treating Lower-Risk Myelodysplastic Syndrome (MDS) Tapan M. Kadia, MD Department of Leukemia MD Anderson Cancer Center Outline Case Study What is lower-risk MDS? Classification systems Prognosis Treatment
Shall young patients with severe aplastic anemia without donors receive BMT from alternative source of HCT? Elias Hallack Atta, MD, PhD
 Shall young patients with severe aplastic anemia without donors receive BMT from alternative source of HCT? Elias Hallack Atta, MD, PhD Declaração de Conflito de Interesse Declaro que possuo conflito de
Shall young patients with severe aplastic anemia without donors receive BMT from alternative source of HCT? Elias Hallack Atta, MD, PhD Declaração de Conflito de Interesse Declaro que possuo conflito de
3/31/2014. New Directions in Aplastic Anemia Treatment: What s on the Horizon? Objectives
 New Directions in Aplastic Anemia Treatment: What s on the Horizon? AA & MDS International Foundation Living with, MDS, or PNH Patient and Family Conferences in 2014 April 5, 2014 Objectives To provide
New Directions in Aplastic Anemia Treatment: What s on the Horizon? AA & MDS International Foundation Living with, MDS, or PNH Patient and Family Conferences in 2014 April 5, 2014 Objectives To provide
MYELODYSPLASTIC SYNDROME. Vivienne Fairley Clinical Nurse Specialist Sheffield
 MYELODYSPLASTIC SYNDROME Vivienne Fairley Clinical Nurse Specialist Sheffield MDS INCIDENCE 1/100,000/YEAR 3,250/YEAR MEDIAN AGE 70 MDS HYPO OR HYPERCELLULAR BONE MARROW BLOOD CYTOPENIAS (EARLY STAGES
MYELODYSPLASTIC SYNDROME Vivienne Fairley Clinical Nurse Specialist Sheffield MDS INCIDENCE 1/100,000/YEAR 3,250/YEAR MEDIAN AGE 70 MDS HYPO OR HYPERCELLULAR BONE MARROW BLOOD CYTOPENIAS (EARLY STAGES
Ferrata Storti Foundation
 ARTICLES Introduction Refractory cytopenia of childhood (RCC) is a provisional entity of the pediatric myelodysplastic syndrome (MDS) in the WHO classification and is characterized by persistent cytopenia
ARTICLES Introduction Refractory cytopenia of childhood (RCC) is a provisional entity of the pediatric myelodysplastic syndrome (MDS) in the WHO classification and is characterized by persistent cytopenia
MDS - Diagnosis and Treatments. Dr Helen Enright, Adelaide and Meath Hospital Dr Catherine Flynn, St James Hospital
 MDS - Diagnosis and Treatments Dr Helen Enright, Adelaide and Meath Hospital Dr Catherine Flynn, St James Hospital Overview What is myelodysplasia? Symptoms Diagnosis and prognosis Myelodysplasia therapy
MDS - Diagnosis and Treatments Dr Helen Enright, Adelaide and Meath Hospital Dr Catherine Flynn, St James Hospital Overview What is myelodysplasia? Symptoms Diagnosis and prognosis Myelodysplasia therapy
Treatment of low risk MDS
 Treatment of low risk MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu International Prognostic Scoring
Treatment of low risk MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu International Prognostic Scoring
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Ordering Physician CLIENT,CLIENT. Collected REVISED REPORT
 HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
Supplementary Appendix
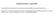 Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION
 ORIGINAL ARTICLES NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION Ilina Micheva 1, Rosen Rachev 1, Hinco Varbanov 1, Vladimir
ORIGINAL ARTICLES NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION Ilina Micheva 1, Rosen Rachev 1, Hinco Varbanov 1, Vladimir
INHERITED PANCYTOPENIA SYNDROMES Fanconi anemia Shwachman-Diamond syndrome Dyskeratosis congenita Congenital amegakaryocytic thrombocytopenia
 The Pancytopenias The Inherited Pancytopenias Pancytopenia refers to a reduction below normal values of all 3 peripheral blood component: leukocytes, platelets, and erythrocytes. Pancytopenia requires
The Pancytopenias The Inherited Pancytopenias Pancytopenia refers to a reduction below normal values of all 3 peripheral blood component: leukocytes, platelets, and erythrocytes. Pancytopenia requires
Aplastic Anemia: Current Thinking
 Aplastic Anemia: Current Thinking ANDREW C. DIETZ, MD, MSCR PEDIATRIC BLOOD AND MARROW TRANSPLANTATION CHILDREN S HOSPITAL LOS ANGELES, UNIVERSITY OF SOUTHERN CALIFORNIA Outline Ø What is Aplastic Anemia?
Aplastic Anemia: Current Thinking ANDREW C. DIETZ, MD, MSCR PEDIATRIC BLOOD AND MARROW TRANSPLANTATION CHILDREN S HOSPITAL LOS ANGELES, UNIVERSITY OF SOUTHERN CALIFORNIA Outline Ø What is Aplastic Anemia?
Review Article. MYELODYSPLASIA IN CHILDHOOD Shantaraman. K
 MYELODYSPLASIA IN CHILDHOOD Shantaraman. K Review Article Abstract: Myelodysplasia is a heterogenous group of disorders that was earlier described as preleukemia, refractory anemia with excess of blasts,
MYELODYSPLASIA IN CHILDHOOD Shantaraman. K Review Article Abstract: Myelodysplasia is a heterogenous group of disorders that was earlier described as preleukemia, refractory anemia with excess of blasts,
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
How I treat acquired aplastic anemia
 How I treat acquired aplastic anemia Phillip Scheinberg and Neal S. Young Blood Volume 120(6):1185-1196 August 9, 2012 2012 by American Society of Hematology Symptoms, Signs, and Lab Findings Bruising,
How I treat acquired aplastic anemia Phillip Scheinberg and Neal S. Young Blood Volume 120(6):1185-1196 August 9, 2012 2012 by American Society of Hematology Symptoms, Signs, and Lab Findings Bruising,
Year 2002 Paper two: Questions supplied by Jo 1
 Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Disclosers Updates: Management of Aplastic Anemia and Congenital Marrow Failure 5/9/2017
 2017 Updates: Management of Aplastic Anemia and Congenital Marrow Failure Sachit Patel, MD Department of Pediatrics Division of Hematology-Oncology Blood and Marrow Transplantation Disclosers None 1 Objectives:
2017 Updates: Management of Aplastic Anemia and Congenital Marrow Failure Sachit Patel, MD Department of Pediatrics Division of Hematology-Oncology Blood and Marrow Transplantation Disclosers None 1 Objectives:
YEREVAN STATE MEDICAL UNIVERSITY DEPARTMENT OF HEMATOLOGY COURSE DESCRIPTION HEMATOLOGY
 1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
 Preface In recent years, the pathogenesis of hematological disorders in children has been clarified, which has led to remarkable progress in the treatment outcome for these disorders. In particular, molecular
Preface In recent years, the pathogenesis of hematological disorders in children has been clarified, which has led to remarkable progress in the treatment outcome for these disorders. In particular, molecular
CASE 106. Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation
 CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Etiology. Definition MYELODYSPLASTIC SYNDROMES. De novo. Secondary MDS (10 years earlier than primary) transformation
 MYELODYSPLASTIC SYNDROMES Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics The University of Texas M.D. Anderson Cancer Center Houston, Texas No relevant COIs to
MYELODYSPLASTIC SYNDROMES Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics The University of Texas M.D. Anderson Cancer Center Houston, Texas No relevant COIs to
Aplastic Anemia Pathophysiology and Approach to Therapy
 Aplastic Anemia Pathophysiology and Approach to Therapy BSMCON 2018 Dr. Syed Ghulam Mogni Mowla MBBS, FCPS, FACP Introduction Aplastic anaemia (AA) is the paradigm of the human bone marrow failure syndromes
Aplastic Anemia Pathophysiology and Approach to Therapy BSMCON 2018 Dr. Syed Ghulam Mogni Mowla MBBS, FCPS, FACP Introduction Aplastic anaemia (AA) is the paradigm of the human bone marrow failure syndromes
Should we still use Camitta s criteria for severe aplastic anemia?
 VOLUME 47 ㆍ NUMBER 2 ㆍ June 2012 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Should we still use Camitta s criteria for severe aplastic anemia? Hyun Hwa Yoon, Seok Jae Huh, Ji Hyun Lee, Suee Lee,
VOLUME 47 ㆍ NUMBER 2 ㆍ June 2012 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Should we still use Camitta s criteria for severe aplastic anemia? Hyun Hwa Yoon, Seok Jae Huh, Ji Hyun Lee, Suee Lee,
DISCLOSURE Luca Malcovati, MD. No financial relationships to disclose
 ICUS, CCUS and CHIP Luca Malcovati, MD Department of Molecular Medicine, University of Pavia Medical School, & Department of Hematology Oncology, IRCCS Policlinico S. Matteo Foundation, Pavia, Italy DISCLOSURE
ICUS, CCUS and CHIP Luca Malcovati, MD Department of Molecular Medicine, University of Pavia Medical School, & Department of Hematology Oncology, IRCCS Policlinico S. Matteo Foundation, Pavia, Italy DISCLOSURE
Novità nelle MDS. Matteo G Della Porta. Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy
 Novità nelle MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu Outline ARCH Predictive value of somatic
Novità nelle MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu Outline ARCH Predictive value of somatic
Bor-Sheng Ko. Hematology Division, Department of Internal Medicine, National Taiwan University Hospital
 Bor-Sheng Ko Hematology Division, Department of Internal Medicine, National Taiwan University Hospital On behalf of Members of Aplastic Anemia Consensus Meeting Diagnosis and classification: Treatment
Bor-Sheng Ko Hematology Division, Department of Internal Medicine, National Taiwan University Hospital On behalf of Members of Aplastic Anemia Consensus Meeting Diagnosis and classification: Treatment
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Better Prognosis for Patients With Del(7q) Than for Patients With Monosomy 7 in Myelodysplastic Syndrome
 Better Prognosis for Patients With Del(7q) Than for Patients With Monosomy 7 in Myelodysplastic Syndrome Iris Cordoba, MD 1 ; José R. González-Porras, MD 1 ; Benet Nomdedeu, MD 2 ; Elisa Luño, MD 3 ; Raquel
Better Prognosis for Patients With Del(7q) Than for Patients With Monosomy 7 in Myelodysplastic Syndrome Iris Cordoba, MD 1 ; José R. González-Porras, MD 1 ; Benet Nomdedeu, MD 2 ; Elisa Luño, MD 3 ; Raquel
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal 1 0.
 Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Long-term outcome of isolated thrombocytopenia accompanied by hypocellular marrow
 VOLUME 46 ㆍ NUMBER 2 ㆍ June 2011 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Long-term outcome of isolated thrombocytopenia accompanied by hypocellular marrow Gak-Won Yun 1, Young-Jun Yang 1, Ik-Chan
VOLUME 46 ㆍ NUMBER 2 ㆍ June 2011 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Long-term outcome of isolated thrombocytopenia accompanied by hypocellular marrow Gak-Won Yun 1, Young-Jun Yang 1, Ik-Chan
Supplemental Material. The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia
 Supplemental Material The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia Torsten Haferlach, 1 Anna Stengel, 1 Sandra Eckstein, 1 Karolína
Supplemental Material The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia Torsten Haferlach, 1 Anna Stengel, 1 Sandra Eckstein, 1 Karolína
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
Cynthia Fata, MD, MSPH 6/23/15
 Cynthia Fata, MD, MSPH 6/23/15 Clinical case presentation Introduction to thrombopoietin Development of thrombopoietic agents Clinical Indications Eltrombopag use in aplastic anemia Future uses 33 yo F
Cynthia Fata, MD, MSPH 6/23/15 Clinical case presentation Introduction to thrombopoietin Development of thrombopoietic agents Clinical Indications Eltrombopag use in aplastic anemia Future uses 33 yo F
Impact of Comorbidity on Quality of Life and Clinical Outcomes in MDS
 Current Therapeutic and Biologic Advances in MDS A Symposium of The MDS Foundation ASH 2014 Impact of Comorbidity on Quality of Life and Clinical Outcomes in MDS Peter Valent Medical University of Vienna
Current Therapeutic and Biologic Advances in MDS A Symposium of The MDS Foundation ASH 2014 Impact of Comorbidity on Quality of Life and Clinical Outcomes in MDS Peter Valent Medical University of Vienna
Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome
 Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
Long-term risk of cancer development in adult patients with idiopathic aplastic anemia after treatment with anti-thymocyte globulin
 Published Ahead of Print on July 13, 2017, as doi:10.3324/haematol.2017.171215. Copyright 2017 Ferrata Storti Foundation. Long-term risk of cancer development in adult patients with idiopathic aplastic
Published Ahead of Print on July 13, 2017, as doi:10.3324/haematol.2017.171215. Copyright 2017 Ferrata Storti Foundation. Long-term risk of cancer development in adult patients with idiopathic aplastic
Case Presentation. Attilio Orazi, MD
 Case Presentation Attilio Orazi, MD Weill Cornell Medical College/ NYP Hospital Department of Pathology and Laboratory Medicine New York, NY United States History 60 year old man presented with anemia
Case Presentation Attilio Orazi, MD Weill Cornell Medical College/ NYP Hospital Department of Pathology and Laboratory Medicine New York, NY United States History 60 year old man presented with anemia
Hepatitis-Associated Aplastic Anemia. Kazuko KUDO and Seiji KOJIMA Department of Pediatrics, Nagoya University Graduate School of Medicine
 Hepatitis-Associated Aplastic Anemia Kazuko KUDO and Seiji KOJIMA Department of Pediatrics, Nagoya University Graduate School of Medicine Abstract We retrospectively analysed the clinical outcome of 85
Hepatitis-Associated Aplastic Anemia Kazuko KUDO and Seiji KOJIMA Department of Pediatrics, Nagoya University Graduate School of Medicine Abstract We retrospectively analysed the clinical outcome of 85
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
MUD HSCT as first line Treatment in Idiopathic SAA. Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK
 MUD HSCT as first line Treatment in Idiopathic SAA Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK No Financial Disclosures Guidelines for management of aplastic anaemia British
MUD HSCT as first line Treatment in Idiopathic SAA Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK No Financial Disclosures Guidelines for management of aplastic anaemia British
APPROACH TO MYELODYSPLASTIC SYNDROMES IN THE ERA OF PRECISION MEDICINE
 APPROACH TO MYELODYSPLASTIC SYNDROMES IN THE ERA OF PRECISION MEDICINE Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics Department of Hematopathology The University
APPROACH TO MYELODYSPLASTIC SYNDROMES IN THE ERA OF PRECISION MEDICINE Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics Department of Hematopathology The University
2007 Workshop of SH/EAHP. Session 5 Therapy-related myeloid neoplasms
 2007 Workshop of SH/EAHP Session 5 Therapy-related myeloid neoplasms Classification: Key issues MDS vs. AML-M6 MDS vs. MDS/MPD Genetically defined entities Relevance of morphologic classification Clinical
2007 Workshop of SH/EAHP Session 5 Therapy-related myeloid neoplasms Classification: Key issues MDS vs. AML-M6 MDS vs. MDS/MPD Genetically defined entities Relevance of morphologic classification Clinical
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Myelodysplastic syndromes: 2018 update on diagnosis, risk-stratification and management
 Received: 2 October 2017 Accepted: 2 October 2017 DOI: 10.1002/ajh.24930 ANNUAL CLINICAL UPDATES IN HEMATOLOGICAL MALIGNANCIES Myelodysplastic syndromes: 2018 update on diagnosis, risk-stratification and
Received: 2 October 2017 Accepted: 2 October 2017 DOI: 10.1002/ajh.24930 ANNUAL CLINICAL UPDATES IN HEMATOLOGICAL MALIGNANCIES Myelodysplastic syndromes: 2018 update on diagnosis, risk-stratification and
Pathophysiology 7/18/2012 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA
 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
Bone marrow failure. By Zahraa Nasooh Al_Saaty
 Bone marrow failure By Zahraa Nasooh Al_Saaty Pancytopenia : Pancytopenia describes a reduction in the blood count of all the major cell lines-red cells,white cell and platelets. It has several causes
Bone marrow failure By Zahraa Nasooh Al_Saaty Pancytopenia : Pancytopenia describes a reduction in the blood count of all the major cell lines-red cells,white cell and platelets. It has several causes
Overview of guidelines on iron chelation therapy in patients with myelodysplastic syndromes and transfusional iron overload
 Int J Hematol (2008) 88:24 29 DOI 10.1007/s12185-008-0118-z PROGRESS IN HEMATOLOGY Transfusional iron overload and iron chelation therapy Overview of guidelines on iron chelation therapy in patients with
Int J Hematol (2008) 88:24 29 DOI 10.1007/s12185-008-0118-z PROGRESS IN HEMATOLOGY Transfusional iron overload and iron chelation therapy Overview of guidelines on iron chelation therapy in patients with
Myelodysplastic Syndromes: WHO 2008
 Myelodysplastic Syndromes: WHO 2008 Attilio Orazi, M.D., FRCPath. (Engl.) Weill Medical College of Cornell University New York, NY Congresso Nazionale SIE - Società Italiana di Ematologia - MIC Milano
Myelodysplastic Syndromes: WHO 2008 Attilio Orazi, M.D., FRCPath. (Engl.) Weill Medical College of Cornell University New York, NY Congresso Nazionale SIE - Società Italiana di Ematologia - MIC Milano
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Let s Look at Our Blood
 Let s Look at Our Blood Casey O Connell, MD Associate Professor of Clinical Medicine Jane Anne Nohl Division of Hematology Keck School of Medicine of USC 10,000,000,000 WBCs/day Bone Marrow: The Blood
Let s Look at Our Blood Casey O Connell, MD Associate Professor of Clinical Medicine Jane Anne Nohl Division of Hematology Keck School of Medicine of USC 10,000,000,000 WBCs/day Bone Marrow: The Blood
