En bloc spondylectomy has been developed and. Late instrumentation failure after total en bloc spondylectomy. Clinical article
|
|
|
- Christal Norton
- 5 years ago
- Views:
Transcription
1 J Neurosurg Spine 15: , 2011 Late instrumentation failure after total en bloc spondylectomy Clinical article Morio Matsumoto, M.D., 1 Kota Watanabe, M.D., 2 Takashi Tsuji, M.D., 1 Ken Ishii, M.D., 1 Masaya Nakamura, M.D., 1 Kazuhiro Chiba, M.D., 1 and Yoshiaki Toyama, M.D. 1 1 Department of Orthopaedic Surgery; and 2 Department of Advanced Therapy for Spine and Spinal Cord Disorders, Keio University, Tokyo, Japan Object. The object of this study was to investigate failures after spinal reconstruction following total en bloc spondylectomy (TES), related factors, and sequelae arising from such failures in patients with malignant spinal tumors. Methods. Fifteen patients (12 males and 3 females, with a mean age of 46.5 years) with malignant spinal tumors who underwent TES and survived for more than 1 year were included in this analysis (mean follow-up 41.5 months). Seven patients had primary tumors, including giant cell tumors in 4 patients, chordoma in 2, and Ewing sarcoma in 1. Eight patients had metastatic tumors, including thyroid cancer in 6 and renal cell cancer and malignant fibrous histiocytoma in 1 patient each. Seven patients without prominent paravertebral extension of the tumor were treated using a posterior approach alone, and 8 patients who exhibited prominent anterior or anterolateral extension of the tumors into the thoracic or abdominal cavity were treated using a combined anterior and posterior approach. Spinal reconstruction after tumor resection was performed using a combination of anterior structural support and posterior instrumentation. The relationship between instrumentation failure and clinical and radiographic factors, including age, sex, history of previous surgery, preoperative radiotherapy, tumor histology, tumor level, surgical approach, number of resected vertebrae, rod diameter, number of instrumented vertebrae, and cage subsidence, was investigated. Results. Six patients (40%) with spinal instrumentation failure were identified: rod breakage occurred in 3 patients, and breakage of both the rod and the cage, combined cage breakage and screw back-out, and endplate fracture arising from cage subsidence occurred in 1 patient each. All of these patients experienced acute or chronic back pain, but only 1 patient with a tumor recurrence experienced neurological deterioration upon instrumentation failure. Cage subsidence ( 5 mm), preoperative irradiation, and the number of instrumented vertebrae ( 4 vertebrae) were significantly related to late instrumentation failure. Conclusions. Late instrumentation failure was a frequent complication after TES. Although patients with instrumentation failure experienced back pain, the neurological sequelae were not catastrophic. For prevention, meticulous preparation of the graft site and a longer posterior fixation should be considered. (DOI: / SPINE10813) Key Words total en bloc spondylectomy instrumentation failure spinal tumor En bloc spondylectomy has been developed and used for the marginal resection of malignant spinal tumors, allowing for the local treatment of tumors with acceptable perioperative morbidity and yielding good neurological recovery in patients with preoperative neurological deficits. 1,3,6,8 12,14,16 Tomita et al. 15 described a TES technique via a posterior-only approach and using his original T-saw. This aggressive surgical procedure is Abbreviation used in this paper: TES = total en bloc spondylectomy. indicated for patients with spinal tumors, including primary malignant tumors, benign but aggressive tumors (such as giant cell tumors), and metastatic tumors with curable primary lesions. After en bloc resection of the tumors, the spinal column is totally separated, and, especially in patients with tumors extending to surrounding structures such as the paravertebral muscles and ribs, combined resection of the surrounding structures is required, making the spine extremely unstable. To restabilize the spine, robust reconstruction of the 3 spinal columns is necessary using spinal instrumentation. 320 J Neurosurg: Spine / Volume 15 / September 2011
2 Late instrumentation failure Spinal instability resulting from the failure of spinal reconstruction after TES can lead to serious sequelae, including severe pain and neurological deterioration. Because TES is indicated for patients with a long life expectancy, 15 such patients may face a greater risk of suffering from instrumentation failure during a later stage of follow-up than the patients with a shorter life expectancy, who usually undergo palliative intralesional resection surgery. Late instrumentation failure can be caused by the lack of biological osseous fusion, but patients who undergo TES suffer from many factors unfavorable to osseous fusion, including postoperative instability of the spine, a decrease in blood supply due to wide dissection of the surrounding soft tissues, radiation, chemotherapy, and so forth. Therefore, we can hypothesize that those patients may have a high rate of instrumentation failure due to a lack of solid osseous fusion during a long-term follow-up period. Although several case studies examining TES have been reported, 1,3,8 12,14,16 to our knowledge, there are few published accounts of late instrumentation failure and the resulting sequelae after TES. The purpose of the present study was to investigate instrumentation failure after TES and subsequent spinal reconstruction, related factors, and the sequelae arising from instrumentation failure in patients with a postoperative survival period longer than 1 year. Methods Patient Characteristics Between 1997 and 2009, 22 patients with primary or metastatic spinal tumors underwent a TES at our institute. Of these, 15 patients (68.2%) survived for more than 1 year after the procedure and were included in the present analysis (Table 1). These 15 patients consisted of 12 men and 3 women, with a mean age of 46.5 years (range years). The mean follow-up period was 41.5 months (range months). At the final follow-up, 13 patients were alive without evidence of disease, and 2 patients had died of disease associated with tumor recurrence at 24 and 57 months after TES. Seven patients had primary tumors, including giant cell tumors in 4 patients, chordoma in 2, and Ewing sarcoma in 1. Eight patients had metastatic tumors including thyroid cancer in 6 and renal cell cancer and malignant fibrous histiocytoma in 1 patient each. The thoracic spine was involved in 7 patients, and the thoracolumbar spine and lumbar spine were involved in 4 patients each. Total en bloc spondylectomy was indicated for patients with metastatic tumors based on the scoring system proposed by Tomita et al. 15 This system consists of 3 prognostic factors including malignancy grade of primary lesion (slow growth, 1 point; moderate growth, 2 points; and rapid growth, 4 points), visceral metastases (no metastasis, 0 points; treatable metastasis, 2 points; and untreatable metastasis, 4 points), and bone metastases (solitary or isolated, 1 point; and multiple, 2 points). The resultant score ranges between 2 and 10. Total en bloc spondylectomy was indicated for patients with a Tomita score 4. Five of the patients with metastatic tumors had a Tomita score of 2, and 3 had a Tomita score of 3. Three patients had previously undergone intralesional palliative surgery that resulted in a recurrence. Neurological status before surgery, evaluated using the Frankel classification, 5 was Grade C (motor useless) TABLE 1: Summary of demographic characteristics in 15 patients who underwent TES* Case No. Age (yrs), Sex Tumor Type Tomita Score Histology Involved Vertebrae Previous Op FU (mos) Recurrence Prognosis Frankel Grade Preop FU 1 48, F primary GCT T3 5 Y 72 N NED C E 2 28, M primary GCT L1 2 Y 75 N NED D D 3 32, M primary Ewing sarcoma L-2 N 57 Y DOD (57) C D 4 42, M primary chordoma L-4 N 24 Y DOD (24) D D 5 35, M primary GCT T-12 N 26 N NED E C 6 22, M primary chordoma L-2 N 15 N CDF E E 7 32, M primary GCT T8 10 N 12 N CDF E E 8 42, M metastasis 2 thyroid T8 10 N 96 N CDF C E 9 57, M metastasis 3 thyroid T12 L1 N 31 N CDF C D 10 52, M metastasis 2 thyroid T-12 N 36 N CDF E E 11 56, F metastasis 2 thyroid T-4 Y 26 N NED D E 12 64, M metastasis 2 thyroid T-4 N 25 N CDF C D 13 62, M metastasis 3 RCC T-3 N 36 N CDF C D 14 63, M metastasis 3 MFH T11 L1 N 26 N CDF E E 15 60, F metastasis 2 thyroid T-10 N 74 N CDF E E * CDF = continuously disease free; DOD = died of disease; FU = follow-up; GCT = giant cell tumor; MFH = malignant fibrous histiocytoma; NED = no evidence of disease; N = no; RCC = renal cell carcinoma; Y = yes. Tomita score applies to metastatic tumors, not primary tumors. Number in parentheses indicates the number of months between surgery and death. J Neurosurg: Spine / Volume 15 / September
3 M. Matsumoto et al. in 6 patients, Grade D (motor useful) in 3, and Grade E (recovery or normal) in 6. At the final follow-up, neurological status was Grade C in 1 patient, Grade D in 6, and Grade E in 8. Surgical Procedures Prior to surgery, 13 patients underwent preoperative embolization of the feeding arteries, 3 had received radiation therapy, and 2 had received chemotherapy (Table 2). Seven patients without prominent paravertebral tumor extension were treated using a posterior approach alone, as described by Tomita et al., 14,16 and the other 8 patients, who exhibited prominent anterior or anterolateral extension of the tumors into the thoracic or abdominal cavity, were treated using a combined anterior and posterior approach with the anterior release of tumors from the surrounding vascular and visceral structures and ligation of segmental vessels, followed by en bloc resection of the tumor and surrounding tissues via a posterior approach. The number of resected vertebrae was 1 in 9 patients, 2 in 2 patients, and 3 in 4 patients. Spinal reconstruction after tumor resection was performed using a combination of anterior structural support and posterior instrumentation. For the anterior structural support, a titanium mesh cage packed with morcelized local bone, ribs, or iliac crest without tumor contamination was used in 13 patients, and a polymethylmethacrylate block or expandable titanium cage was used in 1 patient each. For the posterior instrumentation, pedicle screw systems with or without hooks were utilized in 14 patients, and a Luque rod was used in 1 patient. Study Analyses The relationships between instrumentation failure and clinical and radiographic factors were investigated using a chi-square test. The analyzed factors were age (< 60 or 60 years), sex, history of previous surgery, preoperative chemotherapy, preoperative radiotherapy, tumor histology (primary or metastatic), tumor level (thoracic, thoracolumbar, or lumbar), surgical approach (posterior only or combined anterior and posterior), number of resected vertebrae (single or multiple), rod diameter (5.5 vs 6.35 mm), number of instrumented vertebrae, and cage subsidence (< 5 or 5 mm). The cage subsidence was measured on radiographs taken immediately after surgery and at the follow-up by using measurement software loaded on the picture archiving and communication system (Fuji Film). For statistical analyses, the statistical software PASW Statistics17 (SPSS, Inc.) was used, and a p value < 0.05 was considered statistically significant. Results Instrumentation Failure Six patients (40%) with spinal instrumentation failure were identified (Table 3). The failure was noted an average of 28.3 months (range 6 42 months) after TES. The instrumentation failures included rod breakage in 3 patients and breakage of both the rod and the cage, cage breakage and screw back-out, and endplate fracture arising from cage subsidence in 1 patient each. All 6 patients experienced back pain, which was acute and severe enough in 3 patients to require a visit to an emergency department; moderate pain was reported by 3 patients during a regular postoperative follow-up examination. Only 1 patient with a tumor recurrence experienced neurological deterioration at the time of instrumentation failure. This patient (Case 4) had a recurrence of a chordoma at L-3 that led to mild paraparesis (Frankel Grade D). Four patients underwent revision surgery, whereas 2 patients refused further surgery. The revision surgeries included TABLE 2: Details of treatment in 15 patients who underwent TES* Case No. Preop Radiation Preop Chemo Embolization Surgical Approach No. of Resected Vertebra No. of Instrumented Vertebra Upper Lower Rod Diameter (mm) Anchor Cage Type 1 N N Y posterior PS mesh 2 N N Y combined PS + hook expandable 3 Y Y Y posterior PS mesh 4 Y N N combined PS mesh 5 N N Y combined PS mesh 6 N N Y combined PS mesh 7 N N Y combined PS mesh 8 Y N Y posterior PS + hook mesh 9 N N Y combined PS mesh 10 N N Y combined PS + hook mesh 11 N N Y posterior PS mesh 12 N N Y posterior PS + hook mesh 13 N N N posterior sublaminar cement 14 N Y Y combined PS mesh 15 N N Y posterior PS mesh * Chemo = chemotherapy; PS = pedicle screw. 322 J Neurosurg: Spine / Volume 15 / September 2011
4 Late instrumentation failure TABLE 3: Instrumentation failure and revision in 15 patients who underwent TES Case No. Failure Cage Subsidence Failure Mode 1 2 Duration Btwn TES & Failure (mos) Revision Method of Revision Op 1 N N 2 N Y 3 Y Y rod breakage cage breakage 42 N 4 Y Y cage breakage L-5 screw pull-out 28 Y extension of fusion level by 1 level above & below 5 N N 6 N N 7 N N 8 Y Y cage sinking 6 Y cage removal, vascularized rib & autologous fibula graft 9 N N 10 Y Y rod breakage 38 N 11 N N 12 N N 13 N N 14 Y Y rod breakage 23 Y rod replacement 15 Y Y rod breakage 33 Y rod replacement the replacement of broken 5.5-mm rods with 6.35-mm rods in 2 patients, the rostral and caudal extension of the instrumentation in a patient with cage breakage and screw back-out, and the replacement of a dislodged cage by an autologous fibula and vascularized rib in a patient with an endplate fracture. Factors Related to Instrumentation Failure Cage subsidence ( 5 mm; p = 0.001), preoperative radiation (p = 0.018), and the number of instrumented vertebrae (p = 0.018) were significantly related to late instrumentation failure (Table 4). All 6 patients with instrumentation failure exhibited obvious cage subsidence of 5 mm. All 3 patients who had received preoperative radiation (mean dosage 50 Gy) experienced instrumentation failure, whereas only 3 of the 12 patients without preoperative radiation experienced instrumentation failure. The 3 patients with preoperative radiation also demonstrated cage subsidence. All 3 patients with 4 instrumented vertebrae experienced instrumentation failure, whereas only 3 of the 12 patients with 5 had failure. None of the other factors, including age, sex, history of previous surgery, preoperative chemotherapy, tumor histology, tumor level, surgical approach, number of resected vertebrae, or rod diameter (5.5 vs 6.35 mm) was significantly related to late instrumentation failure. Case 1 Illustrative Cases J Neurosurg: Spine / Volume 15 / September 2011 History and Examination. This 42-year-old man with a thyroid cancer metastasis at T8 10 underwent TES via a posterior-only approach (Fig. 1). He had progressive paraplegia (Frankel Grade C) at the time of surgery; he had undergone radiation treatment previously, but this therapy had failed to prevent neurological deterioration. Operation. After en bloc resection of the inferior half of T-8, the entirety of T-9, the superior three-fourths of T-10, and the right 9th rib, the spine was reconstructed using a titanium mesh cage and posterior instrumentation. Postoperative Course. Seven months after the surgery, the patient experienced severe back pain, although he had improved neurologically and was ambulatory. A radiological investigation revealed that he had a fracture of the remaining T-10 endplate. His reconstruction was revised by removal of the cage followed by grafts from an autologous fibula and vascularized rib. Although a late infection developed requiring hardware removal 7 years later, he had obtained a solid bony fusion without any signs of recurrence or neurological deficits at that time. Case 5 Examination. This 63-year-old man presented with a malignant fibrous histiocytoma metastasis at T-11, T-12, and L-1. Operation. He underwent TES from T-11 to L-1 via a combined anterior and posterior approach (Fig. 2). The surgery and recovery were uneventful. Postoperative Course. At 23 months after TES, severe back pain developed and the patient visited the emergency department, where breakage of the bilateral rods was noted on radiography. The patient was neurologically intact. Radiographs and a sagittal reconstruction CT showed cage subsidence and a gap between the inhomo- 323
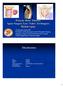
5 M. Matsumoto et al. Fig. 1. Case 1. Images obtained in a 42-year-old man with a thyroid cancer metastasis at T-8 to T-10. A: Enhanced sagittal T1-weighted MR image showing tumor involvement at T-8, T-9, and T-10. B: Enhanced axial T1-weighted MR image at T-9 showing tumor involvement of the T-9 vertebral body and right lamina and extending into the spinal canal. C: Postoperative radiograph showing a titanium cage placed on the inferior one-fourth of the T-10 vertebral body. D: Radiograph showing the resected specimen including the lower one-third of the T-8 vertebral body, the entire T-9 vertebral body, the right lamina, and the upper three-fourths of the T-10 vertebral body. E: Radiograph showing cage subsidence with fracture of the lower endplate. F: Coronal CT scan showing a cage replaced with autologous fibula and vascularized rib. geneous graft bone in the cage and the vertebral bodies. He underwent revision surgery during which the broken 5.5-mm rods were replaced with 6.35-mm rods, resulting in relief of the back pain. During the revision surgery, a compressive force was applied to the cage via the upper and lower vertebrae. Discussion The overall rate of late instrumentation failure after TES was 40% in this study, suggesting that such an event is not a rare complication associated with TES. However, the sequelae associated with such a failure were not catastrophic; that is, they were not associated with severe neurological deterioration, although all of the patients with failed instrumentation did experience moderate to severe back pain. One of the factors related to late instrumentation failure was the number of instrumented vertebrae. Boriani et al. 3 reported on the morbidity of en bloc resection of spinal tumors in 134 patients. These authors found posterior instrumentation failure with anterior column reconstruction in 7% of the patients. They attributed this failure to a posterior fixation that was too short. Failure of the anterior constructs was not observed. A biomechanical study by Disch et al., 4 who used a thoracolumbar en bloc spondylectomy model, demonstrated that multilevel posterior fixation resulted in better stability than did short posterior fixation with an anterolateral plate. In the present study as well, a short construct extending 2 levels above and below the point of fixation always failed. Considering these findings, fixation should be extended to 3 levels above and below the resected vertebrae. Although the rod diameter was not a significant risk factor for failure, a 6.35-mm rod may be more useful for securely holding an unstable spine than a 5.5-mm rod. Cage subsidence was also significantly associated with instrumentation failure. Because TES is, so to speak, the worst-case scenario in terms of spinal stability, a robust anterior support is essential for regaining spine stability. Cage subsidence leads to the failure of load sharing in the anterior column, resulting in an increased load im- 324 J Neurosurg: Spine / Volume 15 / September 2011
6 Late instrumentation failure Fig. 2. Case 5. Images obtained in a 63-year-old man with a malignant fibrous histiocytoma metastasis at T-11, T-12, and L-1. A: Sagittal T2-weighted MR image showing prominent ventral extension of the tumor. B: Enhanced MR image showing the tumor extending from T-11 to L-1. C: Radiograph showing the marked upper subsidence of the cage and rod breakage. D: Radiograph obtained after the revision surgery, showing broken rods replaced with 6.35-mm rods. E: Sagittal reformatted CT scan showing the cage subsidence and the nonhomogeneous graft bone inside the cage. posed on the posterior instrumentation. Cage subsidence may develop because of the fragility of the vertebral bodies, the condition of the interface between the cage and the graft site, or the failure of osseous fusion between the grafted autologous bone in the cage and the vertebral bodies. 7,13 Lim et al. 7 examined the relationship between the biomechanical strength and the condition of the graft-endplate in an anterior cervical fusion model. They conducted a destructive compression test on specimens with different endplate conditions and found that the load that produced failure in specimens with an intact endplate was significantly greater than that producing failure in specimens with no endplate. Togawa et al. 13 conducted a histological study of the contents of clinically failed interbody cages retrieved from human patients. These authors found a relatively high prevalence of hyaline and fibrocartilage in the cages and stressed the importance of graft and graft-site preparation for bone-graft incorporation. J Neurosurg: Spine / Volume 15 / September 2011 As reported in these studies, graft-site preparation is a critical factor for preventing cage subsidence. As shown in the patient in Case 1, cutting more than half of the vertebral bodies may lead to a weak and insufficient graft site for the cage. In such cases, the excisional line should be extended to the disc space above or below the involved vertebral body so that the cage can be placed on the bony endplates with better mechanical strength. Because irradiation is known to have a negative impact on bone quality and strength, 2 preoperative radiation can be a risk factor for cage subsidence and successive instrumentation failure. Therefore, the oncological need for preoperative irradiation should be weighed against successful TES without instrumentation failure. For patients expected to have a long survival period, measures for achieving solid osseous fusion should be considered, including the placement of an autologous vascularized or nonvascularized strut graft as an adjunct to the placement of a titanium cage. 325
7 M. Matsumoto et al. TABLE 4: Factors associated with instrumentation failure Parameter (no. of patients) No. of Patients (%) p Value age in yrs 0.63 <60 (11) 4 (36.4) 60 (4) 2 (50.0) sex 0.79 M (12) 5 (41.7) F (3) 1 (33.3) history of previous op 0.79 Y (3) 1 (33.3) N (12) 5 (41.7) preop chemo Y (2) 2 (100.0) N (13) 4 (30.8) radiotherapy 0.018* Y (3) 3 (100.0) N (12) 12 (25.0) histology of tumor 0.40 primary (7) 2 (28.6) metastatic (8) 4 (50.0) level of tumors 0.70 thoracic (7) 2 (28.6) thoracolumbar (4) 2 (50.0) lumbar (4) 2 (50.0) surgical approach 0.83 posterior only (7) 3 (42.9) combined (8) 3 (37.5) no. of resected vertebrae (9) 4 (44.4) 2 (2) 0 (0) 3 (4) 2 (50.0) rod diameter in mm (6) 3 (50.0) 6.35 (9) 3 (33.3) no. of instrumented vertebrae 0.018* 2 (3) 3 (100.0) 3 (12) 3 (25.0) cage subsidence 0.001* Y (7) 6 (85.7) N (8) 0 (0.0) * Statistically significant. The present study has several limitations, including its retrospective design, small sample size, and diversity of tumor histologies and surgical methods. And because of these limitations, we were not able to fully identify factors related to the achievement of biological osseous fusion, which is essential to successful long-term results after TES. We must improve the statistical power with a multicenter study to elucidate those factors. Nonetheless, this is the first case study to describe in detail late instrumentation failure, the resulting sequelae, and the related factors after TES. The information obtained from this study may contribute to the improvement of reconstruction methods after TES. Conclusions Late instrumentation failure was a frequent complication after TES. Although patients with instrumentation failure experienced back pain, the neurological sequelae were not catastrophic. For prevention, meticulous preparation of the graft site and a longer posterior fixation should be considered. Disclosure Drs. Matsumoto and Watanabe are paid consultants for Medtronic Sofamor Danek Japan. Author contributions to the study and manuscript preparation include the following. Conception and design: Matsumoto, Chiba. Acquisition of data: Matsumoto, Watanabe, Tsuji, Ishii, Nakamura. Analysis and interpretation of data: Matsumoto. Drafting the article: Matsumoto. Critically revising the article: Matsumoto. Statistical analysis: Matsumoto. Study supervision: Chiba, Toyama. References 1. Abe E, Kobayashi T, Murai H, Suzuki T, Chiba M, Okuyama K: Total spondylectomy for primary malignant, aggressive benign, and solitary metastatic bone tumors of the thoracolumbar spine. J Spinal Disord 14: , Alsaadi G, Quirynen M, Komárek A, van Steenberghe D: Impact of local and systemic factors on the incidence of late oral implant loss. Clin Oral Implants Res 19: , Boriani S, Bandiera S, Donthineni R, Amendola L, Cappuccio M, De Iure F, et al: Morbidity of en bloc resections in the spine. Eur Spine J 19: , Disch AC, Schaser KD, Melcher I, Luzzati A, Feraboli F, Schmoelz W: En bloc spondylectomy reconstructions in a biomechanical in-vitro study. Eur Spine J 17: , Frankel HL, Hancock DO, Hyslop G, Melzak J, Michaelis LS, Ungar GH, et al: The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia. I. Paraplegia 7: , Liljenqvist U, Lerner T, Halm H, Buerger H, Gosheger G, Winkelmann W: En bloc spondylectomy in malignant tumors of the spine. Eur Spine J 17: , Lim TH, Kwon H, Jeon CH, Kim JG, Sokolowski M, Natarajan R, et al: Effect of endplate conditions and bone mineral density on the compressive strength of the graft-endplate interface in anterior cervical spine fusion. Spine (Phila Pa 1976) 26: , Matsumoto M, Ishii K, Takaishi H, Nakamura M, Morioka H, Chiba K, et al: Extensive total spondylectomy for recurrent giant cell tumor in the thoracic spine. Case report. J Neurosurg Spine 6: , Melcher I, Disch AC, Khodadadyan-Klostermann C, Tohtz S, Smolny M, Stöckle U, et al: Primary malignant bone tumors and solitary metastases of the thoracolumbar spine: results by management with total en bloc spondylectomy. Eur Spine J 16: , Murakami H, Kawahara N, Demura S, Kato S, Yoshioka K, Tomita K: Neurological function after total en bloc spondylectomy for thoracic spinal tumors. Clinical article. J Neurosurg Spine 12: , Roy-Camille R, Saillant G, Mazel CH, Monpierre H: Total vertebrectomy as treatment of malignant tumors of the spine. Chir Organi Mov 75 (1 Suppl):94 96, J Neurosurg: Spine / Volume 15 / September 2011
8 Late instrumentation failure 12. Sakaura H, Hosono N, Mukai Y, Ishii T, Yonenobu K, Yoshikawa H: Outcome of total en bloc spondylectomy for solitary metastasis of the thoracolumbar spine. J Spinal Disord Tech 17: , Togawa D, Bauer TW, Lieberman IH, Sakai H: Lumbar intervertebral body fusion cages: histological evaluation of clinically failed cages retrieved from humans. J Bone Joint Surg Am 86-A:70 79, Tomita K, Kawahara N, Baba H, Tsuchiya H, Nagata S, Toribatake Y: Total en bloc spondylectomy for solitary spinal metastases. Int Orthop 18: , Tomita K, Kawahara N, Kobayashi T, Yoshida A, Murakami H, Akamaru T: Surgical strategy for spinal metastases. Spine (Phila Pa 1976) 26: , Tomita K, Toribatake Y, Kawahara N, Ohnari H, Kose H: Total en bloc spondylectomy and circumspinal decompression for solitary spinal metastasis. Paraplegia 32:36 46, 1994 Manuscript submitted November 17, Accepted May 5, Please include this information when citing this paper: published online June 3, 2011; DOI: / SPINE Address correspondence to: Morio Matsumoto, M.D., Department of Orthopaedic Surgery, Keio University, Shinanomachi 35, Shinjuku-ku, Tokyo # , Japan. morio@sc.itc.keio. ac.jp. J Neurosurg: Spine / Volume 15 / September
Risk factors of instrumentation failure after multilevel total en bloc spondylectomy
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Risk factors of instrumentation failure after multilevel total en bloc spondylectomy Katsuhito Yoshioka 1), Hideki Murakami 1), Satoru Demura 1), Satoshi
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Risk factors of instrumentation failure after multilevel total en bloc spondylectomy Katsuhito Yoshioka 1), Hideki Murakami 1), Satoru Demura 1), Satoshi
ONCOLOGY LETTERS 11: , 2016
 1778 Therapy for thoracic lumbar and sacral vertebrae tumors using total spondylectomy and spine reconstruction through posterior or combined anterior posterior approaches PINGLIN YANG, XIJING HE, HAOPENG
1778 Therapy for thoracic lumbar and sacral vertebrae tumors using total spondylectomy and spine reconstruction through posterior or combined anterior posterior approaches PINGLIN YANG, XIJING HE, HAOPENG
CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT
 Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Extensive total spondylectomy for recurrent giant cell tumor in the thoracic spine
 J Neurosurg Spine 6:600 605, 2007 Extensive total spondylectomy for recurrent giant cell tumor in the thoracic spine Case report MORIO MATSUMOTO, M.D., 1 KEN ISHII, M.D., 2 HIRONARI TAKAISHI, M.D., 2 MASAYA
J Neurosurg Spine 6:600 605, 2007 Extensive total spondylectomy for recurrent giant cell tumor in the thoracic spine Case report MORIO MATSUMOTO, M.D., 1 KEN ISHII, M.D., 2 HIRONARI TAKAISHI, M.D., 2 MASAYA
PRIMARY STUDIES EN BLOC VERSUS DEBULKING
 PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
Case Report Four-Rod Stabilization of Severely Destabilized Lumbar Spine Caused by Metastatic Tumor
 Volume 2013, Article ID 254684, 6 pages http://dx.doi.org/10.1155/2013/254684 Case Report Four-Rod Stabilization of Severely Destabilized Lumbar Spine Caused by Metastatic Tumor Isao Shibuya, Koichi Sairyo,
Volume 2013, Article ID 254684, 6 pages http://dx.doi.org/10.1155/2013/254684 Case Report Four-Rod Stabilization of Severely Destabilized Lumbar Spine Caused by Metastatic Tumor Isao Shibuya, Koichi Sairyo,
Healing of Autologous Bone in a Titanium Mesh Cage Used in Anterior Column Reconstruction After Total Spondylectomy
 Healing of Autologous Bone in a Titanium Mesh Cage Used in Anterior Column Reconstruction After Total Spondylectomy SPINE Volume 27, Number 13, pp E329 E333 2002, Lippincott Williams & Wilkins, Inc. Tomoyuki
Healing of Autologous Bone in a Titanium Mesh Cage Used in Anterior Column Reconstruction After Total Spondylectomy SPINE Volume 27, Number 13, pp E329 E333 2002, Lippincott Williams & Wilkins, Inc. Tomoyuki
Osteosarcoma of the spine: surgical treatment and outcomes
 Feng et al. World Journal of Surgical Oncology 2013, 11:89 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Osteosarcoma of the spine: surgical treatment and outcomes Dapeng Feng 1, Xinghai Yang
Feng et al. World Journal of Surgical Oncology 2013, 11:89 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Osteosarcoma of the spine: surgical treatment and outcomes Dapeng Feng 1, Xinghai Yang
En bloc spondylectomy for spinal metastases: a review of techniques
 Neurosurg Focus 15 (5):Article 6, 2003, Click here to return to Table of Contents En bloc spondylectomy for spinal metastases: a review of techniques KEVIN C. YAO, M.D., STEFANO BORIANI, M.D., ZIYA L.
Neurosurg Focus 15 (5):Article 6, 2003, Click here to return to Table of Contents En bloc spondylectomy for spinal metastases: a review of techniques KEVIN C. YAO, M.D., STEFANO BORIANI, M.D., ZIYA L.
Frozen recapping laminoplasty: a new technique to treat spinal tumor
 EUROSPINE 2018 19-21 September, Barcelona, Spain Frozen recapping laminoplasty: a new technique to treat spinal tumor Noritaka Yonezawa, Hideki Murakami, Satoru Demura, Satoshi Kato, Katsuhito Yoshioka,
EUROSPINE 2018 19-21 September, Barcelona, Spain Frozen recapping laminoplasty: a new technique to treat spinal tumor Noritaka Yonezawa, Hideki Murakami, Satoru Demura, Satoshi Kato, Katsuhito Yoshioka,
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach
 Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Infections and metastatic disease of the lumbar
 An Original Study Lumbar Extracavitary Corpectomy With a Single Stage Circumferential Arthrodesis: Surgical Technique and Clinical Series Kern Singh, MD, and Daniel K. Park, MD Abstract Circumferential
An Original Study Lumbar Extracavitary Corpectomy With a Single Stage Circumferential Arthrodesis: Surgical Technique and Clinical Series Kern Singh, MD, and Daniel K. Park, MD Abstract Circumferential
Surgical Treatment of Spine Surgery Experience Primary Spinal Neoplasms ( ) Ziya L. Gokaslan, MD, FACS Approximately 3500 spine tumor
 Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Review Article Chondrosarcoma of the Mobile Spine and Sacrum
 Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Survival Rate and Neurological Outcome after Operation for Advanced Spinal Metastasis (Tomita s Classification Type 4)
 Original Article DOI 10.3349/ymj.2009.50.5.689 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(5): 689-696, 2009 Survival Rate and Neurological Outcome after Operation for Advanced Spinal Metastasis
Original Article DOI 10.3349/ymj.2009.50.5.689 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(5): 689-696, 2009 Survival Rate and Neurological Outcome after Operation for Advanced Spinal Metastasis
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion and Posterior Instrumentation
 Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Treatment of Tumors of the Spine
 Hiroshima J. Med. Sci. Vol.46, No.4, 5~, December, 997 HIJM 46-7 5 Treatment of Tumors of the Spine Toshifumi OZAKI*, Henry HALM, Ulrich LILJENQVIST and Winfried WINKELMANN Department of Orthopaedics,
Hiroshima J. Med. Sci. Vol.46, No.4, 5~, December, 997 HIJM 46-7 5 Treatment of Tumors of the Spine Toshifumi OZAKI*, Henry HALM, Ulrich LILJENQVIST and Winfried WINKELMANN Department of Orthopaedics,
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked Response to Molecular Target Drugs
 Case Reports in Orthopedics Volume 2013, Article ID 916501, 4 pages http://dx.doi.org/10.1155/2013/916501 Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked
Case Reports in Orthopedics Volume 2013, Article ID 916501, 4 pages http://dx.doi.org/10.1155/2013/916501 Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked
Vertebrectomy and anterior reconstruction for the treatment of spinal metastases
 Acta Orthop. Belg., 2005, 71, 459-466 ORIGINAL STUDY Vertebrectomy and anterior reconstruction for the treatment of spinal metastases Thorsten ERNSTBERGER, Tanja BRÜNING, Friedhelm KÖNIG From Georg August
Acta Orthop. Belg., 2005, 71, 459-466 ORIGINAL STUDY Vertebrectomy and anterior reconstruction for the treatment of spinal metastases Thorsten ERNSTBERGER, Tanja BRÜNING, Friedhelm KÖNIG From Georg August
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine
 Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Advantages of MISS. Disclosures. Thoracolumbar Trauma: Minimally Invasive Techniques. Minimal Invasive Spine Surgery 11/8/2013.
 3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
Modern management in vertebral metastasis
 43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
Complications analysis of posterior vertebral column resection in 40 patients with spinal tumors
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 8: 1539-1544, 2014 Complications analysis of posterior vertebral column resection in 40 patients with spinal tumors YU FAN 1*, YU XIA 2*, HONG ZHAO 1, JIANGUO ZHANG
EXPERIMENTAL AND THERAPEUTIC MEDICINE 8: 1539-1544, 2014 Complications analysis of posterior vertebral column resection in 40 patients with spinal tumors YU FAN 1*, YU XIA 2*, HONG ZHAO 1, JIANGUO ZHANG
Evaluation of prognostic scoring systems for bone metastases using single center data
 MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Predictive value of pedicle involvement with MRI in spine metastases
 /, Vol. 7, No. 38 Predictive value of pedicle involvement with MRI in spine metastases Wang Mi Liu 1,*, Rong Xing 1,*, Chong Bian 1, Yun Liang 1, Libo Jiang 1, Chen Qian 1, Jian Dong 1 1 Department of
/, Vol. 7, No. 38 Predictive value of pedicle involvement with MRI in spine metastases Wang Mi Liu 1,*, Rong Xing 1,*, Chong Bian 1, Yun Liang 1, Libo Jiang 1, Chen Qian 1, Jian Dong 1 1 Department of
Palliative transpedicular partial corpectomy without anterior vertebral reconstruction in lower thoracic and thoracolumbar junction spinal metastases
 Chang et al. Journal of Orthopaedic Surgery and Research (2015) 10:113 DOI 10.1186/s13018-015-0255-z RESEARCH ARTICLE Palliative transpedicular partial corpectomy without anterior vertebral reconstruction
Chang et al. Journal of Orthopaedic Surgery and Research (2015) 10:113 DOI 10.1186/s13018-015-0255-z RESEARCH ARTICLE Palliative transpedicular partial corpectomy without anterior vertebral reconstruction
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
The frequency of tumors is increasing and metastases. Spinal Oncologic Reconstruction ABSTRACT
 WScJ 3: 176-183, 2010 Spinal Oncologic Reconstruction Cem Copuroglu, Erol Yalniz Department of Orthopaedics and Traumatology, School of Medicine, Trakya University, Edirne, Turkey ABSTRACT The frequency
WScJ 3: 176-183, 2010 Spinal Oncologic Reconstruction Cem Copuroglu, Erol Yalniz Department of Orthopaedics and Traumatology, School of Medicine, Trakya University, Edirne, Turkey ABSTRACT The frequency
Solitary vertebral metastasis of primary clear cell carcinoma of the liver: a case report and review of literature
 Case Report Solitary vertebral metastasis of primary clear cell carcinoma of the liver: a case report and review of literature Karthikeyan Maharajan 1, Hwee Weng Dennis Hey 2, Ivan Tham 3, Thomas Paulraj
Case Report Solitary vertebral metastasis of primary clear cell carcinoma of the liver: a case report and review of literature Karthikeyan Maharajan 1, Hwee Weng Dennis Hey 2, Ivan Tham 3, Thomas Paulraj
Comparison of clinical, radiological and functional outcome of short segment V/S long segment posterior fixation of tuberculosis of spine
 2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
GIZA Surgical Technique
 GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases-
 Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Traumatic thoracic spinal fracture dislocation with minimal or no cord injury
 J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
Vertebral body fractures after transpsoas interbody fusion procedures
 The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
CASE REPORT. Utility of a 3-dimensional full-scale NaCl model for rib strut grafting for anterior fusion for cervicothoracic kyphosis
 Nagoya J. Med. Sci. 77. 525 ~ 530, 2015 CASE REPORT Utility of a 3-dimensional full-scale NaCl model for rib strut grafting for anterior fusion for cervicothoracic kyphosis Kazuyoshi Kobayashi 1, Shiro
Nagoya J. Med. Sci. 77. 525 ~ 530, 2015 CASE REPORT Utility of a 3-dimensional full-scale NaCl model for rib strut grafting for anterior fusion for cervicothoracic kyphosis Kazuyoshi Kobayashi 1, Shiro
The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar Spine Fractures In A Rural Tertiary Care Centre Without Help Of Image Intensifier
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 4, Issue 6 (Jan.- Feb. 2013), PP 36-40 The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 4, Issue 6 (Jan.- Feb. 2013), PP 36-40 The Neurologic Outcome Of Posterior Fixation Of Thoraco- Lumbar
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Ning Liu, MD, 1,3 and Kirkham B. Wood, MD 1,2
 TECHNICAL NOTE J Neurosurg Spine 26:368 373, 2017 Multiple-hook fixation in revision spinal deformity surgery for patients with a previous multilevel fusion mass: technical note and preliminary outcomes
TECHNICAL NOTE J Neurosurg Spine 26:368 373, 2017 Multiple-hook fixation in revision spinal deformity surgery for patients with a previous multilevel fusion mass: technical note and preliminary outcomes
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony
 Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
Malignant metastatic tumors of the upper cervical
 J Neurosurg Spine 21:886 891, 2014 AANS, 2014 Treatment of C-2 metastatic tumors with intraoperative transoral or transpedicular vertebroplasty and occipitocervical posterior fixation Clinical article
J Neurosurg Spine 21:886 891, 2014 AANS, 2014 Treatment of C-2 metastatic tumors with intraoperative transoral or transpedicular vertebroplasty and occipitocervical posterior fixation Clinical article
VLIFT System Overview. Vertebral Body Replacement System
 VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS
 STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium
 Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis
 Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Research Article Structural Femoral Shaft Allografts for Anterior Spinal Column Reconstruction in Osteoporotic Spines
 BioMed Research International Volume 2016, Article ID 8681957, 9 pages http://dx.doi.org/10.1155/2016/8681957 Research Article Structural Femoral Shaft Allografts for Anterior Spinal Column Reconstruction
BioMed Research International Volume 2016, Article ID 8681957, 9 pages http://dx.doi.org/10.1155/2016/8681957 Research Article Structural Femoral Shaft Allografts for Anterior Spinal Column Reconstruction
Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis
 J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using a posterior-anterior approach: a case report
 Shimada et al. Journal of Medical Case Reports 2013, 7:9 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using
Shimada et al. Journal of Medical Case Reports 2013, 7:9 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY).
 SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES
 AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation
 The Spine Journal 6 (2006) 330 334 Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation Gregory P. Lekovic, MD, PhD, JD, Eric M. Horn, MD, PhD, Curtis A. Dickman, MD* Division
The Spine Journal 6 (2006) 330 334 Distraction injury to thoracic spine treated with thoracoscopic dual-rod fixation Gregory P. Lekovic, MD, PhD, JD, Eric M. Horn, MD, PhD, Curtis A. Dickman, MD* Division
Spinal Metastases From Myxoid Liposarcoma Warrant Screening With Magnetic Resonance Imaging
 1815 Spinal Metastases From Myxoid Liposarcoma Warrant Screening With Magnetic Resonance Imaging Joseph H. Schwab, MD 1 Patrick J. Boland, MD 1 Cristina Antonescu, MD 2 Mark H. Bilsky, MD 3 John H. Healey,
1815 Spinal Metastases From Myxoid Liposarcoma Warrant Screening With Magnetic Resonance Imaging Joseph H. Schwab, MD 1 Patrick J. Boland, MD 1 Cristina Antonescu, MD 2 Mark H. Bilsky, MD 3 John H. Healey,
Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity. Department of Spine, General Hospital of Lanzhou Command, Gansu, China
 Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Tumeurs Malignes du Rachis
 DESC de Chirurgie Pédiatrique Session de Mars 2008 - PARIS Tumeurs Malignes du Rachis G. BOLLINI We will exclude from this presentation the tumor involving the sacrum which are particular entities more
DESC de Chirurgie Pédiatrique Session de Mars 2008 - PARIS Tumeurs Malignes du Rachis G. BOLLINI We will exclude from this presentation the tumor involving the sacrum which are particular entities more
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma
 Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Leiomyosarcoma is a malignant soft tissue sarcoma. Outcomes after surgery for spinal metastatic leiomyosarcoma. Clinical article
 J Neurosurg Spine 17:432 437, 2012 Outcomes after surgery for spinal metastatic leiomyosarcoma Clinical article John E. Ziewacz, M.D., M.P.H., Darryl Lau, B.A., Frank La Marca, M.D., and Paul Park, M.D.
J Neurosurg Spine 17:432 437, 2012 Outcomes after surgery for spinal metastatic leiomyosarcoma Clinical article John E. Ziewacz, M.D., M.P.H., Darryl Lau, B.A., Frank La Marca, M.D., and Paul Park, M.D.
Metastatic Disease of the Proximal Femur
 CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Radiotherapy for Patients with Symptomatic Intramedullary Spinal Cord Metastasis
 J. Radiat. Res., 52, 641 645 (2011) Regular Paper Radiotherapy for Patients with Symptomatic Intramedullary Spinal Cord Metastasis Haruko HASHII 1,4 *, Masashi MIZUMOTO 1,4 *, Ayae KANEMOTO 1,4, Hideyuki
J. Radiat. Res., 52, 641 645 (2011) Regular Paper Radiotherapy for Patients with Symptomatic Intramedullary Spinal Cord Metastasis Haruko HASHII 1,4 *, Masashi MIZUMOTO 1,4 *, Ayae KANEMOTO 1,4, Hideyuki
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
ASJ. Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic and Koch s Spine. Asian Spine Journal.
 Asian Spine Journal 786 Rohit Anilbhai Clinical Thaker Studyet al. http://dx.doi.org/10.4184/asj.2014.8.6.786 Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic
Asian Spine Journal 786 Rohit Anilbhai Clinical Thaker Studyet al. http://dx.doi.org/10.4184/asj.2014.8.6.786 Study of Vertebral Body Replacement with Reconstruction Spinal Cages in Dorsolumbar Traumatic
Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention
 Moderator: Dr. P.S. Chandra Dr. Dr Deepak Gupta Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention A precise, comprehensive, ideal
Moderator: Dr. P.S. Chandra Dr. Dr Deepak Gupta Classification? Classification system should be: Comprehensive Usable Accurate Predictable Able to guide intervention A precise, comprehensive, ideal
Surgical Technique INTERSOMATIC CERVICAL CAGE
 R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
of thoracolumbar angular kyphosis.
 spine clinical article J Neurosurg Spine 23:42 48, 2015 Expanded eggshell procedure combined with closing-opening technique (a modified vertebral column resection) for the treatment of thoracic and thoracolumbar
spine clinical article J Neurosurg Spine 23:42 48, 2015 Expanded eggshell procedure combined with closing-opening technique (a modified vertebral column resection) for the treatment of thoracic and thoracolumbar
Case Report. Takaki Inoue 1), Sumihisa Orita 1) *, Hiroto Kamoda 2), Yoshihiro Sakuma 1)
 Chiba Medical J. 93E:53 ~ 57,2017 Case Report Successful revision enforcement surgery for postoperative implant failure in a patient with combined anteroposterior fixation after total en bloc spondylectomy:
Chiba Medical J. 93E:53 ~ 57,2017 Case Report Successful revision enforcement surgery for postoperative implant failure in a patient with combined anteroposterior fixation after total en bloc spondylectomy:
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy and fusion
 Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture
 779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
