Introduction. Yuichi Takano 1 Masatsugu Nagahama. Hiroki Mizukami 2 Jun-ichi Tanaka
|
|
|
- Veronica Anderson
- 5 years ago
- Views:
Transcription
1 Clin J Gastroenterol (2015) 8: DOI /s CASE REPORT Prolapse into the bile and expansive growth is characteristic behavior of mucinous cystic neoplasm of the liver: report of two cases and review of the literature Yuichi Takano 1 Masatsugu Nagahama 1 Eiichi Yamamura 1 Naotaka Maruoka 1 Hiroki Mizukami 2 Jun-ichi Tanaka 2 Nobuyuki Ohike 3 Hiroshi Takahashi 1 Received: 9 January 2015 / Accepted: 16 April 2015 / Published online: 8 May 2015 The Author(s) This article is published with open access at Springerlink.com Abstract Mucinous cystic neoplasm of the liver (MCN- L) is a very rare tumor whose detailed behavior is still unknown. We describe two cases of MCN-L that exhibited extremely interesting growth patterns, and discuss the characteristics of MCN-Ls. Both cases exhibited MCN-L that originated from the left hepatic lobe (Segment 4) and then prolapsed into the left hepatic and, resulting in obstructive jaundice due to expansive growth. Endoscopic retrograde cholangiopancreatographies showed the characteristic oval-shaped s in the bile s. Endoscopic ultrasound and intraal ultrasound were useful for differentiating the tumors from stones, since multiple septal formations were observed inside the tumors. A literature search revealed that, over the past 10 years, 15 cases of MCN-L (biliary s with ovarian-like stroma) that showed expansive growth in the bile had been reported. Prolapse into the bile and expansive growth appear to be characteristic behavior of MCN-L. In the future, additional data on more cases needs to be collected to further elucidate MCN-L pathophysiology. & Yuichi Takano yuichitakano1028@yahoo.co.jp Keywords Mucinous cystic neoplasm of the liver Biliary Ovarian-like stroma ERCP Abbreviations MCN-L Mucinous cystic neoplasm of the liver S4 of the Segment 4 of the liver liver ERCP Endoscopic retrograde cholangiopancreatography EUS Endoscopic ultrasound IDUS Intraal ultrasound OLS Ovarian-like stroma CA 19-9 Cancer antigen 19-9 CEA Carcinoembryonic antigen HBsAg Hepatitis B surface antigen HCVAb Hepatitis C virus antibody CT Computed tomography MRI Magnetic resonance imaging WHO World Health Organization IPNB Intraal papillary neoplasm of the bile IPMN Intraal papillary mucinous neoplasm MCN-P Mucinous cystic neoplasm of the pancreas HCC Hepatocellular carcinoma CCC Cholangiocellular carcinoma Division of Gastroenterology, Department of Internal Medicine, Showa University Fujigaoka Hospital, 1-30 Fujigaoka, Aoba-ku, Yokohama-shi, Yokohama, Kanagawa , Japan Department of Surgery, Showa University Fujigaoka Hospital, Yokohama, Kanagawa, Japan Department of Diagnostic Pathology, Showa University Fujigaoka Hospital, Yokohama, Kanagawa, Japan Introion Mucinous cystic neoplasm of the liver (MCN-L) is an extremely rare cyst-forming epithelial tumor. This unique neoplasm is commonly observed in middle-aged women and is usually characterized by having no communication with the
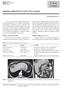
2 Clin J Gastroenterol (2015) 8: bile and rarely becoming malignant. Pathologically, the cyst wall is composed of mucin-producing cuboidal or columnar epithelium and is accompanied by ovarian-like stroma (OLS). However, detailed information on the behavior of MCN-L is lacking due to its rarity. Along with a review of the literature, we describe two cases of MCN-L that exhibited extremely interesting growth patterns, and consider the behavior of this tumor. Case presentation Case 1 A 57-year-old woman was admitted to the emergency room complaining of sudden abdominal pain and fever. Her vital signs were blood pressure 120/76 mmhg, heart rate 102 beats/min, and body temperature 38.2 C. Tenderness was noted from the epigastrium to the hypochondriac region, but neither muscular defense nor rebound tenderness was observed. Laboratory tests revealed elevated levels of hepato-biliary enzymes (T-bil: 2.7 mg/dl; GOT: 299 U/L; GPT: 535 U/L; ALP: 2459 U/L; c-gtp: 2054 U/L). Cancer antigen (CA) 19-9 levels were mildly increased (99.0 U/mL, normal = 0-37 U/mL) and carcinoembryonic antigen (CEA) levels were normal (^0.5 ng/ml, normal = ng/ml). Both the hepatitis B surface antigen (HBsAg) and the hepatitis C virus antibody (HCVAb) tests were negative, and the patient had no history of excessive alcohol consumption. Contrast abdominal computed tomography (CT) revealed a mm multi-locular cystic lesion with an internal septal formation in the left hepatic lobe (Segment 4: S4) (Fig. 1a). No nodular components, al invasion, or distant metastases were found. Magnetic resonance imaging (MRI) showed low signal intensities on T1- weighted images and high signal intensities on T2- weighted images inside the cystic lesion (Fig. 1b). The septal formation was connected to the left hepatic and, and spread of the tumor to the bile was suspected (Fig. 1c). Endoscopic retrograde cholangiopancreatography (ERCP) was performed, and no excretion of mucin from the papilla of Vater was observed. Cholangiography revealed an oval-shaped in the (Fig. 1d). There were no findings Fig. 1 a Contrast abdominal CT revealed a multi-locular cystic lesion in the left hepatic lobe (S4), with multiple septal formations (arrow). Intrahepatic bile s were dilated. b, c MRI showed high signal intensities on T2-weighted images of the components inside the cyst (arrow). The septal formation was connected to the left hepatic and (arrow), and thus the spread of the tumor into the bile was suspected. d ERCP revealed an oval-shaped that appeared to fill the (arrow). e Cholangioscopy enabled a direct observation of the tumor the. f EUS revealed that the tumor occupied the lumen of the, and many septal formations were observed
3 150 Clin J Gastroenterol (2015) 8: Fig. 2 a An incision was made in the, which was filled with the tumor (arrow). b A multi-locular cystic tumor was noted in the S4 liver segment, and had prolapsed into the left hepatic and indicating malignancy in the bile cytology. Cholangioscopy enabled a direct observation of the smooth tumor wall inside the (Fig. 1e). Endoscopic ultrasound (EUS) revealed that the tumor occupied the lumen of the, and many septal formations were observed (Fig. 1f). On the basis of the above findings, the patient was diagnosed with benign MCN-L that had prolapsed into the bile. The patient underwent a laparoscopy-assisted left lobectomy, a cholecystectomy, and a right hepaticojejunostomy. The patient progressed well following the surgical procedures and was discharged from the hospital 14 days postoperatively. Macroscopic findings indicated a multi-locular cystic tumor in S4 of the liver. It had prolapsed into the left hepatic and (Fig. 2a, b). Microscopic findings revealed that the cystic lesion was lined with mucinous cuboidal epithelium, and OLS was observed extensively in the cyst wall stroma (Fig. 3). The OLS was positive for both progesterone and estrogen receptors. A definitive diagnosis of MCN-L with low-grade dysplasia was therefore made. Case 2 A 26-year-old woman visited our hospital after being told by a family member that her eyes appeared yellow. Her vital signs were blood pressure 110/72 mmhg, heart rate 68 beats/min, and body temperature 36.2 C. She presented no tenderness in the abdominal region. Laboratory tests revealed elevated levels of hepato-biliary enzymes (T-bil: 4.1 mg/ml; GOT: 271 U/L; GPT: 394 U/L; ALP: 1568 U/L; c-gtp: 489 U/L). Tumor marker levels were normal (CA 19-9: 5.5 U/mL; CEA ^0.5 ng/ml). Both HBsAg and HCVAb were negative and the patient had no history of excessive alcohol consumption. Fig. 3 Microscopic findings revealed that the cystic lesion was lined with mucinous cuboidal epithelium, and OLS was observed extensively in the cyst wall stroma. MCN-L with low-grade dysplasia was diagnosed Contrast abdominal CT revealed a mm multilocular cystic lesion with internal septal formation in the left hepatic lobe (S4), but no nodular components were contained (Fig. 4a). No al invasion or distant metastases were found. MRI showed low signal intensities on T1-weighted images and high signal intensities on T2- weighted images inside the cyst (Fig. 4b). The septal formation was connected to the left hepatic and common bile, and thus the spread of the tumor to the bile was suspected (Fig. 4c). ERCP demonstrated no excretion of mucin from the papilla of Vater. Cholangiography revealed a in the upper bile, and the lower tip of the area was oval-shaped. Furthermore, stenosis of the left hepatic was observed (Fig. 4d). There were no findings indicating malignancy in the bile cytology. IDUS revealed the spread of the tumor to the left
4 Clin J Gastroenterol (2015) 8: Fig. 4 a Contrast abdominal CT revealed a cystic lesion with the septal formation in the left hepatic lobe (S4) (arrow). b, c MRI showed high signal intensities on T2-weighted images of the components of the cyst (arrow). The septal formations were connected to the left hepatic and (arrow). The spread of the tumor to the bile was suspected. d ERCP revealed a in the upper bile (arrow). The lower tip of the area was oval-shaped. Stenosis of the left hepatic was also observed. e IDUS revealed the spread of the tumor to the, with the septal formations inside the tumor hepatic and, with a number of septal formations inside the tumor (Fig. 4e). The patient was therefore diagnosed with non-malignant MCN-L and an extensive left lobectomy and right hepaticojejunostomy were performed. Examination of the resected specimen confirmed that the tumor originating from S4 of the liver had prolapsed into the left hepatic and (Fig. 5). Microscopic findings indicated that the cystic lesion was lined with mucinous cuboidal epithelium, and OLS was observed extensively in the cyst wall stroma (Fig. 6). The OLS was positive for both progesterone and estrogen receptors. MCN-L with low-grade dysplasia was diagnosed. Discussion The World Health Organization (WHO) classifies mucusproducing bile tumors of the liver into intraal papillary neoplasm of the bile (IPNB) or MCN-L [1]. These concepts were established as counterparts to intraal papillary mucinous neoplasm (IPMN) of the pancreas and mucinous cystic neoplasm of the pancreas (MCN-P). IPNBs become papillary inside the bile and secrete mucin in approximately one-third of all cases. They show communication with the bile and do not exhibit OLS. As in the case of IPMN of the pancreas, four phenotypes are known to exist pancreatobiliary, intestinal, oncocytic, and gastric. On the other hand, MCN-Ls are cyst-forming epithelial tumors that are composed pathologically of mucus-producing cuboidal or columnar epithelium. They usually have no communication with the bile and exhibit OLS. MCN-Ls have been traditionally called biliary s or biliary cystadenocarcinomas [2, 3]. The definitions of these tumors have been controversial; however, in recent years, OLS has been considered necessary for a MCN-L diagnosis, and therefore the disease concept is now being established. Thus, tumors that have been referred to as biliary s or biliary cystadenocarcinomas in previous reports could be classified into tumors with and without OLS. Most biliary cystic neoplasms that have been
5 152 Clin J Gastroenterol (2015) 8: Fig. 5 Examination of the resected specimen confirmed that the tumor originated from S4 of the liver. It had prolapsed into the left hepatic and (arrow) Fig. 6 Microscopic findings indicated that the cystic lesion was lined with mucinous cuboidal epithelium, and OLS was observed extensively in the cyst wall stroma. MCN-L with low-grade dysplasia was diagnosed reported previously as biliary s or cystadenocarcinomas without OLS are currently thought to be IPNBs [2, 4 8]. Based on the 2010 WHO classifications, biliary cystic neoplasm with OLS should be diagnosed as MCN-L. Zen et al. [9] investigated 54 cases of MCN-L and reported the following characteristics: MCN-Ls often occurred in the left hepatic lobe (72 %), the mean age of onset was 52.5 years, and they rarely developed in men (over 90 % of the patients were women). In addition, MCN-Ls are often large, with a mean size of 100 mm ( mm). There is little correlation with viral hepatitis, intrahepatic cholelithiasis, or liver cirrhosis, and malignancy is uncommon, with 1 out of 54 cases exhibiting micro-invasive carcinoma. Although rare, MCN-Ls have the potential to be malignant. Even for asymptomatic cases, surgery is generally preferable for MCN-L. MCN-Ps, the same type of tumor but located in the pancreas, are known to have relatively low malignant potential, but invasive carcinomas have been reported to account for approximately 10 % of cases [10]. Zen et al. suggested that both MCN-Ls and MCN-Ps exhibit low malignant potential; however, of the two, MCN-Ls exhibit lower malignant potential [9]. Preoperative differentiation of benign and malignant MCN-Ls is difficult. Previous reports of malignant MCN- Ls indicate nodular components with contrast enhancement effects within the cyst, al invasion, and metastasis to other organs [2, 11]. In our cases, contrast CT showed no nodules inside the cyst, no al invasion, and no metastasis to other organs. There were no findings indicating malignancy in the bile cytology. The above findings suggested the presence of benign MCN-L preoperatively. However, a definitive diagnosis can only be made based on postoperative pathological findings. Kubota et al. [12] investigated 119 cases of IPNB and 9 cases of MCN-L, all of which occurred in females, and most MCN-L cases were asymptomatic in comparison with the IPNB cases. They suggested that patients with IPNBs may be more likely to develop symptoms such as cholangitis and liver dysfunction due to communication with the bile. However, the tumors of the 2 patients in the present report had prolapsed into the bile and exhibited expansive growth. Obstructive jaundice was therefore observed. We searched the literature for MCN-L cases in which the tumor grew expansively in the bile over the past 10 years (from 2004 to 2014). In our literature search, we used the keywords biliary, biliary cystadenocarcinoma, and mucinous cystic neoplasm of the liver to search PubMed and extracted cases with growth in the bile. We only diagnosed cases with OLS as MCN-Ls and excluded cases that did not exhibit OLS or for which no mention of OLS was made. We also excluded any cases that were complicated by IPNB. As a result, 15 cases were extracted [13 27] and are listed in Table 1. The mean age of these patients was 44.5 years (25-62 years), all of the patients were female, and all showed the following symptoms: jaundice (9 patients), abdominal pain (9 patients), and liver dysfunction (2 patients); some patients had multiple symptoms. Tumor size was recorded in 11 of the 15 patients. The mean size was 49.5 mm (18-79 mm); the primary tumor sites included the left hepatic lobe (10 patients: 8 cases of S4, 1 case of S3, 1 case of unknown), the (3 patients), and the left hepatic (2 patients). The tumor
6 Clin J Gastroenterol (2015) 8: Table 1 Literature cases Reference number Age (years) Sex Symptoms Size Primary site of the tumor Development of the tumor ERC image Operation Pathological diagnosis F Jaundice 41 mm Common bile Common bile Oval-shaped F Recurrent episodes of obstructive jaundice F Epigastric pain and obstructive liver enzymes 45 mm Left lobe (S4) Left hepatic, 30 mm Left lobe (S4) Left hepatic Oval-shaped F Abdominal bloating 29 mm Left lobe (S4) Left hepatic, F Obstructive jaundice Left lobe (S4) Left hepatic, F Hypochondrial pain 55 mm Left lobe (S4) Left hepatic, F Dysuria and hyperpigmentation of urine Bile resection Cystadenoma of the Bile resection Biliary Oval-shaped Oval-shaped Left lobectomy, bile resection Hepatobiliary Left lobectomy, bile resection Biliary Left lobectomy, bile resection Biliary mucinous Left lobectomy Biliary Left hepatic Common bile Extended left lobectomy, bile resection F Upper abdominal pain 73 mm Left lobe (S4) Common bile Oval-shaped F Right hypochondrial pain, spontaneously remitted jaundice F Right hypochondrial pain, jaundice 55 mm Left lobe (S4) Left hepatic, Segmentectomy (left medial section), bile resection, cholecystectomy Extrahepatic Hepatobiliary Left lobectomy Biliary 50 mm Left lobe (S4) Left hepatic Left lobectomy, bile resection, cholecystectomy F Jaundice Common bile Common bile Oval-shaped F Abdominal pain, abnormal liver function tests F Hypochondrial pain, jaundice Left hepatic, Hepatobiliary Bile resection Biliary 18 mm Common bile Common bile Bile resection Biliary Left hepatic, Oval-shaped Bile resection Biliary F Epigastric pain, jaundice 70 mm Left lobe Left hepatic Left lobectomy Biliary F Abdominal pain, jaundice 79 mm Left lobe (S3) Left hepatic, Left lobectomy Biliary
7 154 Clin J Gastroenterol (2015) 8: spread to both the left hepatic and the in 7 patients, only the in 5 patients, and only the left hepatic in 3 patients. ERCP images were recorded for 7 patients. In all of the patients, the images revealed the same characteristic oval-shaped s in the bile, as seen in the 2 patients in our study. A hepatectomy and bile resection were performed to completely remove the lesions. Pathological examination indicated that none of tumors was malignant. The MCN-Ls that spread to and grew in the bile developed in patients who were younger than those described in the report by Zen et al., and the tumors tended to be smaller. This may have been because the spread of the tumors to the bile is more likely to cause symptoms, such as jaundice or cholangitis, leading to early detection. The characteristic oval-shaped s that are observed with ERCP may be extremely useful in diagnosing this tumor. The most common primary tumor site was S4 of the liver. The primary tumor site was also S4 of the liver in the 2 patients in our reports, suggesting that MCN-Ls that develop from this site may be prone to prolapse into the bile. This may be because the most common primary site of MCN-L is S4 of the liver [2], but it is potentially an interesting phenomenon. We hypothesize that because S4 of the liver is near the hepatic portal region and close to the relatively thick central side of the bile, the tumors originating from this site may be prone to prolapse into the bile. MCN-Ls in the 15 cases that we reviewed were all benign. Prolapse into the bile may be a finding which suggests that the tumor is benign. However, as malignant MCN-Ls are relatively uncommon, we have not reviewed enough cases to date to make such conclusions. In addition, we will discuss bile lesions of other liver tumors and compare them with MCN-L. Bile invasion of hepatocellular carcinomas (HCCs) is clinically rare, but reports suggest that it has been observed in 5 % of HCCs in autopsies [28]. Such cases exhibit irregular stenosis and exclusion of the bile. There are three main categories of cholangiocellular carcinoma (CCC): mass-forming (MF), perial infiltrative (IF), and intraal growth (IG). Of these, the IG type overlaps the IPNB concept proposed in recent years, with irregular papillary tumors developing in the bile. The frequency of the IG type is reported to be 4 % of CCC cases [29]. Papillary tumors are confirmed on cholangiography and cholangioscopy. Growth of other tumor-related lesions into the bile (focal nodular hyperplasia, hepatic adenoma, lymphoma, hepatoblastoma, and mesenchymal tumor) is exceptionally rare. The occurrence of MCN-Ls prolapsing into the bile is unclear as it is an extremely rare tumor. Prolapse into the bile has a strong impact, making it likely to be reported. Examination of further cases is required. In MCN- L, expansive growth is shown by prolapse into the bile so that the smooth, round tumor occupies the lumen of the bile. This development of the tumor, which is completely different from HCC invasion into the bile and the IG type of CCC, can be said to be a characteristic behavior of MCN-L. MCN-L is basically considered to be a non-invasive, benign tumor that does not grow invasively but grows expansively. This tumor can prolapse into the bile and then grow to fill the bile. ERCP can be used to confirm the characteristic oval-shaped in the bile. Even if the entire oval shape is not revealed, as in case 2, careful attention should be paid to the fact that the margins of the are oval. In addition, cholangioscopy, IDUS, and EUS are useful for differentiating these tumors from stones. We described 2 MCN-L cases that exhibited extremely interesting spread patterns. Prolapse into the bile and expansive growth may be a characteristic behavior of MCN-L. Additional data from more cases needs to be collected for further elucidation of MCN-L s pathophysiology. Disclosures Conflict of Interest: Yuichi Takano, Masatsugu Nagahama, Eiichi Yamamura, Naotaka Maruoka, Hiroki Mizukami, Jun-ichi Tanaka, Nobuyuki Ohike, and Hiroshi Takahashi declare that they have no conflict of interest. Human/Animal Rights: All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008(5). Informed Consent: Informed consent was obtained from all patients for being included in the study. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproion in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Nakanuma Y, Curado M-P, Franceschi S, et al. WHO classification of tumours of the digestive system. 4th ed. Lyon: WHO; p Zen Y, Pedica F, Patcha VR, et al. Mucinous cystic neoplasms of the liver: a clinicopathological study and comparison with intraal papillary neoplasms of the bile. Mod Pathol. 2011;24: Wheeler DA, Edmondson HA. Cystadenoma with mesenchymal stroma (CMS) in the liver and bile s. A clinicopathologic study of 17 cases, 4 with malignant change. Cancer. 1985;56: Nakanuma Y, Sasaki M, Ishikawa A, et al. Biliary papillary neoplasm of the liver. Histol Histopathol. 2002;17:
8 Clin J Gastroenterol (2015) 8: Li T, Ji Y, Zhi XT, et al. A comparison of hepatic mucinous cystic neoplasms with biliary intraal papillary neoplasms. Clin Gastroenterol Hepatol. 2009;7: Nakanuma Y, Zen Y, Harada K, et al. Tumorigenesis and phenotypic characteristics of mucin-producing bile tumors: an immunohistochemical approach. J Hepatobiliary Pancreat Sci. 2010;17: Lim JH, Zen Y, Jang KT, et al. Cyst-forming intraal papillary neoplasm of the bile s: description of imaging and pathologic aspects. Am J Roentgenol. 2011;197: Takanami K, Yamada T, Tsuda M, et al. Intraal papillary mucinous neoplasm of the bile s: multimodality assessment with pathologic correlation. Abdom Imaging. 2011;36: Zen Y, Jang KT, Ahn S, et al. Intraal papillary neoplasms and mucinous cystic neoplasms of the hepatobiliary system: demographic differences between Asian and Western populations, and comparison with pancreatic counterparts. Histopathology. 2014;65: Crippa S, Salvia R, Warshaw AL, et al. Mucinous cystic neoplasm of the pancreas is not an aggressive entity: lessons from 163 resected patients. Ann Surg. 2008;247: Vogt DP, Henderson JM, Chmielewski E. Cystadenoma and cystadenocarcinoma of the liver: a single center experience. J Am Coll Surg. 2005;200: Kubota K, Nakanuma Y, Kondo F, et al. Clinicopathological features and prognosis of mucin-producing bile tumor and mucinous cystic tumor of the liver: a multi-institutional study by the Japan Biliary Association. J Hepatobiliary Pancreat Sci. 2014;21: Shima Y, Horimi T, Shibuya Y, et al. Resected of the. J Hepatobiliary Pancreat Surg. 2004;11: Saravanan MN, Singh B, Ravindranath K, et al. Episodic jaundice due to an intrahepatic biliary with biliary stricture masquerading as hydatid cyst. Trop Gastroenterol. 2010;31: Vyas S, Markar S, Ezzat T, et al. Hepato-biliary with intraal extension: unusual cause of obstructive jaundice. J Gastrointest Cancer. 2012;43(1 Suppl): Rayapudi K, Schmitt T, Olyaee M. Filling on ERCP: biliary, a rare tumor. Case Rep Gastroenterol. 2013;7: Chandrasinghe PC, Liyanage C, Deen KI, et al. Obstructive jaundice caused by a biliary mucinous in a woman: a case report. J Med Case Rep. 2013;7: Siriwardana PN, Pathirana A. Episodic biliary obstruction due to an intrahepatic biliary : a case report. J Med Case Rep. 2009;3: Soochan D, Keough V, Wanless I, et al. Intra and extra-hepatic of the biliary. Review of literature and radiological and pathological characteristics of a very rare case. BMJ Case Rep doi: /bcr Abe Y, Kasuya K, Itoi T, et al. Hepatobiliary of the liver prolapsing into the extrahepatic bile (with video). Gastrointest Endosc. 2012;75: Yi B, Cheng QB, Jiang XQ, et al. A special growth manner of intrahepatic biliary. World J Gastroenterol. 2009;15: Harmouch T, Vullierme MP, Sauvanet A, et al. Hepatobiliary revealed by a jaundice: a case report. Case Rep Gastrointest Med. 2011;2011: Park JH, Lee DH, Kim HJ, et al. Unilocular extrahepatic biliary mimicking choledochal cyst: a case report. Korean J Radiol. 2004;5: Hennessey DB, Traynor O. Extrahepatic biliary with mesenchymal stroma: a true biliary? A case report. J Gastrointestin Liver Dis. 2011;20: Preetha M, Chung AY, Lim-Tan SK, et al. Intrahepatic biliary presenting with obstructive jaundice. Asian J Surg. 2004;27: Baudin G, Novellas S, Buratti MS, et al. Atypical MRI features of a biliary revealed by jaundice. Clin Imaging. 2006;30: Gonzalez M, Majno P, Terraz S, et al. Biliary revealed by obstructive jaundice. Dig Liver Dis. 2009;41:e Uka K, Aikata H, Takaki S, et al. Clinical features and prognosis of patients with extrahepatic metastases from hepatocellular carcinoma. World J Gastroenterol. 2007;13: Guglielmi A, Ruzzenente A, Campagnaro T, et al. Intrahepatic cholangiocarcinoma: prognostic factors after surgical resection. World J Surg. 2009;33:
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Intraductal papillary neoplasms in the bile ducts
 Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Trans-abdominal ultrasound features of the newly named intraductal papillary neoplasm of the bile duct
 Original Article on Translational Imaging in Cancer Patient Care Trans-abdominal ultrasound features of the newly named intraductal papillary neoplasm of the bile duct Xian-Shui Fu 1 *, Meng-Na He 2 *,
Original Article on Translational Imaging in Cancer Patient Care Trans-abdominal ultrasound features of the newly named intraductal papillary neoplasm of the bile duct Xian-Shui Fu 1 *, Meng-Na He 2 *,
Biliary tract tumors
 Short Course 2010 Annual Fall Meeting of the Korean Society for Pathologists Biliary tract tumors Joon Hyuk Choi, M.D., Ph.D. Professor, Department of Pathology, Yeungnam Univ. College of Medicine, Daegu,
Short Course 2010 Annual Fall Meeting of the Korean Society for Pathologists Biliary tract tumors Joon Hyuk Choi, M.D., Ph.D. Professor, Department of Pathology, Yeungnam Univ. College of Medicine, Daegu,
Clinical Features of Intraductal Papillary Neoplasm of the Bile Duct : Report of 3 Cases
 Jikeikai Med J 2016 ; 63 : 31-6 Case Report Clinical Features of Intraductal Papillary Neoplasm of the Bile Duct : Report of 3 Cases Naotake Funamizu 1, Fumitake Suzuki 1, Shuichi Fujioka 1, Tomoyoshi
Jikeikai Med J 2016 ; 63 : 31-6 Case Report Clinical Features of Intraductal Papillary Neoplasm of the Bile Duct : Report of 3 Cases Naotake Funamizu 1, Fumitake Suzuki 1, Shuichi Fujioka 1, Tomoyoshi
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
RESEARCH ARTICLE. Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation
 DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
Biliary Cystadenoma Causing Esophageal Varices
 https://doi.org/10.7180/kmj.2016.31.2.191 KMJ Case Report Biliary Cystadenoma Causing Esophageal Varices Sung Ju Kang, Tae Hee Lee, Min Gyu Seok, Hyo Jin Yun, Ye Seul Jang, Jun Hyun Byun Department of
https://doi.org/10.7180/kmj.2016.31.2.191 KMJ Case Report Biliary Cystadenoma Causing Esophageal Varices Sung Ju Kang, Tae Hee Lee, Min Gyu Seok, Hyo Jin Yun, Ye Seul Jang, Jun Hyun Byun Department of
Tanawat Pattarapuntakul *, Bancha Ovartlarnporn and Jaksin Sottisuporn
 Pattarapuntakul et al. Journal of Medical Case Reports (2018) 12:33 DOI 10.1186/s13256-017-1560-4 CASE REPORT Open Access Mucinous cystic neoplasm of the liver with extrahepatic growth presenting with
Pattarapuntakul et al. Journal of Medical Case Reports (2018) 12:33 DOI 10.1186/s13256-017-1560-4 CASE REPORT Open Access Mucinous cystic neoplasm of the liver with extrahepatic growth presenting with
X-Ray Corner. Imaging Approach to Cystic Liver Lesions. Pantongrag-Brown L. Solitary cystic liver lesions. Hepatic simple cyst (Figure 1)
 THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Biliary Papillomatosis: case report
 Chin J Radiol 2003; 28: 407-412 407 Biliary Papillomatosis: case report CHUN-LIN HUANG WEN-PIN CHEN YU-BUN NG JOSEPH HANG LEUNG Department of Medical Imaging, Chiayi Christian Hospital Biliary papillomatosis
Chin J Radiol 2003; 28: 407-412 407 Biliary Papillomatosis: case report CHUN-LIN HUANG WEN-PIN CHEN YU-BUN NG JOSEPH HANG LEUNG Department of Medical Imaging, Chiayi Christian Hospital Biliary papillomatosis
Filling Defect on ERCP: Biliary Cystadenoma, a Rare Tumor
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
HEPATO-BILIARY IMAGING
 HEPATO-BILIARY IMAGING BY MAMDOUH MAHFOUZ MD PROF.OF RADIOLOGY CAIRO UNIVERSITY mamdouh.m5@gmail.com www.ssregypt.com CT ABDOMEN Indications Patient preparation Patient position Scanogram Fasting 4-6 hours
HEPATO-BILIARY IMAGING BY MAMDOUH MAHFOUZ MD PROF.OF RADIOLOGY CAIRO UNIVERSITY mamdouh.m5@gmail.com www.ssregypt.com CT ABDOMEN Indications Patient preparation Patient position Scanogram Fasting 4-6 hours
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma. Judy Wyatt Dundee November 2010
 Cholangiocarcinoma Judy Wyatt Dundee November 2010 Making sense of cholangiocarcinoma Difficulties with diagnostic criteria How many entities within cholangiocarcinoma? Rapidly evolving Intrahepatic cholangiocarcinoma
Cholangiocarcinoma Judy Wyatt Dundee November 2010 Making sense of cholangiocarcinoma Difficulties with diagnostic criteria How many entities within cholangiocarcinoma? Rapidly evolving Intrahepatic cholangiocarcinoma
Case Reports. Intraductal Papillary Cholangiocarcinoma: Case Report and Review of the Literature INTRODUCTION CASE REPORT
 Case Reports Kongkam K, Rerknimitr R 45 Case Report and Review of the Literature Pradermchai Kongkam, M.D. Rungsun Rerknimitr, M.D. ABSTRACT A case of papillary cholangiocarcinoma is presented. A 64-year-old
Case Reports Kongkam K, Rerknimitr R 45 Case Report and Review of the Literature Pradermchai Kongkam, M.D. Rungsun Rerknimitr, M.D. ABSTRACT A case of papillary cholangiocarcinoma is presented. A 64-year-old
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1
 Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Case Report Cystic and Papillary Neoplasm at the Hepatic Hilum Possibly Originating in the Peribiliary Glands
 Case Reports in Pathology Volume 2016, Article ID 9130754, 7 pages http://dx.doi.org/10.1155/2016/9130754 Case Report Cystic and Papillary Neoplasm at the Hepatic Hilum Possibly Originating in the Peribiliary
Case Reports in Pathology Volume 2016, Article ID 9130754, 7 pages http://dx.doi.org/10.1155/2016/9130754 Case Report Cystic and Papillary Neoplasm at the Hepatic Hilum Possibly Originating in the Peribiliary
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary Mucinous Neoplasm
 Case Reports in Surgery Volume 2015, Article ID 816960, 4 pages http://dx.doi.org/10.1155/2015/816960 Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary
Case Reports in Surgery Volume 2015, Article ID 816960, 4 pages http://dx.doi.org/10.1155/2015/816960 Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
International Surgery Intrahepatic Biliary Intraductal Papillary Mucinous Neoplasm With Intermittent Jaundice: Case Report
 International Surgery Intrahepatic Biliary Intraductal Papillary Mucinous Neoplasm With Intermittent Jaundice: Case Report --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Keywords: Corresponding
International Surgery Intrahepatic Biliary Intraductal Papillary Mucinous Neoplasm With Intermittent Jaundice: Case Report --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Keywords: Corresponding
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Occult mucin-producing cholangiocarcinoma in situ: a rare clinical case with difficult tumour staging
 Kiriyama et al. Surgical Case Reports (2017) 3:6 DOI 10.1186/s40792-016-0283-x CASE REPORT Open Access Occult mucin-producing cholangiocarcinoma in situ: a rare clinical case with difficult tumour staging
Kiriyama et al. Surgical Case Reports (2017) 3:6 DOI 10.1186/s40792-016-0283-x CASE REPORT Open Access Occult mucin-producing cholangiocarcinoma in situ: a rare clinical case with difficult tumour staging
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Case Report Intrabiliary Hepatic Metastasis of Colorectal Carcinoma Mimicking Primary Cholangiocarcinoma: A Case Report and Review of the Literature
 Case Reports in Pathology Volume 2016, Article ID 4704781, 5 pages http://dx.doi.org/10.1155/2016/4704781 Case Report Intrabiliary Hepatic Metastasis of Colorectal Carcinoma Mimicking Primary Cholangiocarcinoma:
Case Reports in Pathology Volume 2016, Article ID 4704781, 5 pages http://dx.doi.org/10.1155/2016/4704781 Case Report Intrabiliary Hepatic Metastasis of Colorectal Carcinoma Mimicking Primary Cholangiocarcinoma:
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
CT Differentiation of Mucin- Producing Cystic Neoplasms of the Liver From Solitary Bile Duct Cysts
 Gastrointestinal Imaging Original Research Kim et al. CT of Hepatic Cystic Neoplasms and Cysts Gastrointestinal Imaging Original Research Hyoung Jung Kim 1 Eun Sil Yu 2 Jae Ho Byun 1 Seung-Mo Hong 2 Kyoung
Gastrointestinal Imaging Original Research Kim et al. CT of Hepatic Cystic Neoplasms and Cysts Gastrointestinal Imaging Original Research Hyoung Jung Kim 1 Eun Sil Yu 2 Jae Ho Byun 1 Seung-Mo Hong 2 Kyoung
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without papillotomy
 E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
Cystic Disease of the Liver Work Up and Management. Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center
 Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Overview. Disclosure. PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes. N. Volkan Adsay, MD
 PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes N. Volkan Adsay, MD Professor and Vice-Chair Director of Anatomic Pathology Emory University and Emory Winship Cancer Institute Atlanta,
PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes N. Volkan Adsay, MD Professor and Vice-Chair Director of Anatomic Pathology Emory University and Emory Winship Cancer Institute Atlanta,
FDG-PET Findings of Intraductal Oncocytic Papillary Neoplasms of the Pancreas: Two Case Reports
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case
 Rare disease Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case Diana Soochan,1 Valerie Keough,1 Ian Wanless,2
Rare disease Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case Diana Soochan,1 Valerie Keough,1 Ian Wanless,2
Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case
 Rare disease Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case Diana Soochan,1 Valerie Keough,1 Ian Wanless,2
Rare disease Intra and extra-hepatic cystadenoma of the biliary duct. Review of literature and radiological and pathological characteristics of a very rare case Diana Soochan,1 Valerie Keough,1 Ian Wanless,2
Hepatocellular carcinoma Cholangiocarcinoma. Jewels of hepatobiliary cancer imaging : what to look for? Imaging characteristics of HCC.
 Outline : Imaging Jewels Jewels of hepatobiliary cancer imaging : what to look for? Hepatocellular carcinoma Cholangiocarcinoma Surachate Siripongsakun, M.D. Chulabhorn Cancer Center Imaging characteristics
Outline : Imaging Jewels Jewels of hepatobiliary cancer imaging : what to look for? Hepatocellular carcinoma Cholangiocarcinoma Surachate Siripongsakun, M.D. Chulabhorn Cancer Center Imaging characteristics
Malignant Focal Liver Lesions
 Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case report
 Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Citation Acta medica Nagasakiensia. 1993, 38
 NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Aspect of Peripheral Chola Hepatectomy Cases Shimoyama, Takatoshi; Shimizu, Teru Kiyoomi; Azuma, Kohji; Shinkai, Kiy Terada, Ryusuke; Sasaki,
NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Aspect of Peripheral Chola Hepatectomy Cases Shimoyama, Takatoshi; Shimizu, Teru Kiyoomi; Azuma, Kohji; Shinkai, Kiy Terada, Ryusuke; Sasaki,
Endoscopic Resection of Ampullary Neuroendocrine Tumor
 CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016
 40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Pancreatic Cystic Lesions 원자력병원
 Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal papillary mucinous neoplasm (IPMN)
 Int Surg 2014;99:590 594 DOI: 10.9738/INTSURG-D-13-00134.1 Case Report Ruptured Intrahepatic Biliary Intraductal Papillary Mucinous Neoplasm in a Jehovah s Witness Patient Sangchul Yun 1, Dongho Choi 2
Int Surg 2014;99:590 594 DOI: 10.9738/INTSURG-D-13-00134.1 Case Report Ruptured Intrahepatic Biliary Intraductal Papillary Mucinous Neoplasm in a Jehovah s Witness Patient Sangchul Yun 1, Dongho Choi 2
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Imaging of liver and pancreas
 Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
R.Sotoudehmanesh, MD Professor of Gastroenterology Digestive Disease Research Institute Tehran University of Medical Sciences Pancreatobiliary
 R.Sotoudehmanesh, MD Professor of Gastroenterology Digestive Disease Research Institute Tehran University of Medical Sciences Pancreatobiliary /Advanced Endoscopy group Most common biliary malignancy and
R.Sotoudehmanesh, MD Professor of Gastroenterology Digestive Disease Research Institute Tehran University of Medical Sciences Pancreatobiliary /Advanced Endoscopy group Most common biliary malignancy and
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct
 CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Mucinous cystic neoplasms of the liver: a clinicopathological study and comparison with intraductal papillary neoplasms of the bile duct
 & 2011 USCAP, Inc. All rights reserved 0893-3952/11 $32.00 1079 Mucinous cystic neoplasms of the liver: a clinicopathological study and comparison with intraductal papillary neoplasms of the bile duct
& 2011 USCAP, Inc. All rights reserved 0893-3952/11 $32.00 1079 Mucinous cystic neoplasms of the liver: a clinicopathological study and comparison with intraductal papillary neoplasms of the bile duct
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CHOLANGIOCARCINOMA (CCA)
 CHOLANGIOCARCINOMA (CCA) Deepak Hariharan MD (Research), FRCS, Locum Consultant HPB Surgeon AIM Outline essential facts & principles Present 4 cases Discuss Challenges /Controversies INTRODUCTION Most
CHOLANGIOCARCINOMA (CCA) Deepak Hariharan MD (Research), FRCS, Locum Consultant HPB Surgeon AIM Outline essential facts & principles Present 4 cases Discuss Challenges /Controversies INTRODUCTION Most
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Invited Re vie W. Analytical histopathological diagnosis of small hepatocellular nodules in chronic liver diseases
 Histol Histopathol (1 998) 13: 1077-1 087 http://www.ehu.es/histoi-histopathol Histology and Histopathology Invited Re vie W Analytical histopathological diagnosis of small hepatocellular nodules in chronic
Histol Histopathol (1 998) 13: 1077-1 087 http://www.ehu.es/histoi-histopathol Histology and Histopathology Invited Re vie W Analytical histopathological diagnosis of small hepatocellular nodules in chronic
Primary Hepatic Undifferentiated Pleomorphic Sarcoma: CT and angiographic findings in two cases
 J Radiol Sci 2013; 38: 15-19 Primary Hepatic Undifferentiated Pleomorphic Sarcoma: CT and angiographic findings in two cases Jan-Wen Ku Ying-Chi Tseng Kuo-Luon Kung Hsien-Chang Shen Yen-Lin Huang Chi-Jen
J Radiol Sci 2013; 38: 15-19 Primary Hepatic Undifferentiated Pleomorphic Sarcoma: CT and angiographic findings in two cases Jan-Wen Ku Ying-Chi Tseng Kuo-Luon Kung Hsien-Chang Shen Yen-Lin Huang Chi-Jen
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Neoplasms of the Canine, Feline and Lemur Liver:
 Neoplasms of the Canine, Feline and Lemur Liver: Classification and Prognosis Annual Seminar of the French Society of Veterinary Pathology John M. Cullen VMD PhD DACVP North Carolina State University Primary
Neoplasms of the Canine, Feline and Lemur Liver: Classification and Prognosis Annual Seminar of the French Society of Veterinary Pathology John M. Cullen VMD PhD DACVP North Carolina State University Primary
Biliary cancers: imaging diagnosis. Study of 30 cases
 Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Management of Cholangiocarcinoma. Roseanna Lee, MD PGY-5 Kings County Hospital
 Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
A Case of Giant Mesenteric Cyst Originating from the Small Intestine
 Showa Univ J Med Sci 27 2, 125 129, June 2015 Case Report A Case of Giant Mesenteric Cyst Originating from the Small Intestine Takahiro UMEMOTO 1, Tetsuji WAKABAYASHI 1, Nobuyuki OHIKE 2, Ryuichi SEKINE
Showa Univ J Med Sci 27 2, 125 129, June 2015 Case Report A Case of Giant Mesenteric Cyst Originating from the Small Intestine Takahiro UMEMOTO 1, Tetsuji WAKABAYASHI 1, Nobuyuki OHIKE 2, Ryuichi SEKINE
Contemporary Imaging of Biliary Malignancy and Preoperative Evaluation
 Contemporary Imaging of Biliary Malignancy and Preoperative Evaluation Linda Pantongrag-Brown, MD Advanced Diagnostic Imaging, Ramathibodi Hospital, Bangkok, Thailand Malignancy of biliary tract Cholangiocarcinoma
Contemporary Imaging of Biliary Malignancy and Preoperative Evaluation Linda Pantongrag-Brown, MD Advanced Diagnostic Imaging, Ramathibodi Hospital, Bangkok, Thailand Malignancy of biliary tract Cholangiocarcinoma
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
Citation Acta medica Nagasakiensia. 1995, 40
 NAOSITE: Nagasaki University's Ac Title Author(s) Biliary Cystadenocarcinoma - Report Shimoyama, Takatoshi; Yasutake, Toh Hiroshi; Yamaguchi, Hiroyuki; Terad Sumida, Yorihisa; Hisano, Hiroshi; Hirano,
NAOSITE: Nagasaki University's Ac Title Author(s) Biliary Cystadenocarcinoma - Report Shimoyama, Takatoshi; Yasutake, Toh Hiroshi; Yamaguchi, Hiroyuki; Terad Sumida, Yorihisa; Hisano, Hiroshi; Hirano,
Hepato-Pancreatico-Biliary Surgery. Dr. Ankur J. Shah. MS, DNB, MNAMS, MRCSEd (UK), FRCS (UK)
 Hepato-Pancreatico-Biliary Surgery Dr. Ankur J. Shah MS, DNB, MNAMS, MRCSEd (UK), FRCS (UK) Consultant Hepato-Pancreatico-Biliary and Liver Transplant Surgeon Ansh Liver Clinic Prevention to Cure Address
Hepato-Pancreatico-Biliary Surgery Dr. Ankur J. Shah MS, DNB, MNAMS, MRCSEd (UK), FRCS (UK) Consultant Hepato-Pancreatico-Biliary and Liver Transplant Surgeon Ansh Liver Clinic Prevention to Cure Address
Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup Periods
 Oncology Volume 2009, Article ID 373465, 6 pages doi:10.1155/2009/373465 Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup
Oncology Volume 2009, Article ID 373465, 6 pages doi:10.1155/2009/373465 Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Hilar cholangiocarcinoma. Frank Wessels, Maarten van Leeuwen, UMCU utrecht
 Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
ENDOSCOPY IN COMPETITION DIAGNOSTICS. Dr. med. Dirk Hartmann Klinikum Ludwigshafen
 Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
BILIARY CYSTADENOMA OF LIVER.
 BILIARY CYSTADENOMA OF LIVER. K. Kuberan [1], G. Chandrasekar [1] Abstract Biliary cystadenoma is very rare non parasitic benign neoplasm of liver with less than 200 cases reported all over the world in
BILIARY CYSTADENOMA OF LIVER. K. Kuberan [1], G. Chandrasekar [1] Abstract Biliary cystadenoma is very rare non parasitic benign neoplasm of liver with less than 200 cases reported all over the world in
Evaluation of Liver Mass Lesions. American College of Gastroenterology 2013 Regional Postgraduate Course
 Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
D DAVID PUBLISHING. Groove Pancreatitis: A Case Report. 1. Introduction. 2. Case Report
 Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
