Lab Guide 2018 Diagnostic Genomic Division(DGD)
|
|
|
- Charlene Johns
- 5 years ago
- Views:
Transcription
1 Lab Guide 2018 Diagnostic Genomic Division(DGD) Diagnostic Genomic Division DGD lab Guide Page 1 of 74
2 Cytogenetics Section Title ACUTE MYELOID LEUKEMIA PANEL BY FISH ITEM Days test is performed Turnaround time Acute Myelogenous Leukemia (AML) is a disorder of myeloid cells which were historically categorized by the myeloid cell lineage involved, several of which showed recurrent balanced chromosomal rearrangements resulting in the creation of novel fusion proteins. Recent reclassification (groups the recurrent rearrangements into a single category. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in AML with recurrent genetic abnormalities and in therapy-related AML. Recurrent abnormalities are observed in the majority of AML cases. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative In addition to morphology, several recurrent chromosomal abnormalities have been linked to specific subtypes of AML. The most common chromosome abnormalities associated with AML include t(8;21), t(15;17), inv(16), +8, t(6;9), t(8;16), t(1;22), t(9;22), t(3;5), and abnormalities of the MLL (KMT2A) gene at 11q23. The most common genes juxtaposed with MLL through translocation events Diagnostic Genomic Division DGD lab Guide Page 2 of 74
3 in AML include AFF1- t(4;11), MLTT4- t(6;11), MLLT3- t(9;11), MLLT10- t(10;11), CREBBP- t(11;16), ELLt(11;19p13.1), and MLLT1- t(11;19p13.3). AML can also evolve from myelodysplasia (MDS). Thus, the common chromosome abnormalities associated with MDS can also be identified in AML, which include: inv(3), - 5/5q-, -7/7q-, +8, 13q-, 17p-, 20q-, t(1;3), and t(3;21). In combination, the multiple recurrent chromosome abnormalities identified in patients with AML are observed in approximately 60% of diagnostic AML cases. Location Diagnostic Genomic Division DGD lab Guide Page 3 of 74
4 Title ALK BY FISH ITEM Days test is performed Turnaround time Location ALK gene rearrangement is observed in a small subset (3 7%) of non-small cell lung cancer (NSCLC) patients. The efficacy of crizotinib was shown in lung cancer patients harboring ALK rearrangement. Anaplastic lymphoma kinase (a receptor tyrosine kinase anaplastic lymphoma, CD246), is a transmembrane protein a member of the insulin-like tyrosine kinase receptor superfamily, encoded by the ALK gene on chromosome 2. In non-small-cell lung cancer patients, the inversion [Inv (2) (p21p23)] within the short arm of chromosome 2 is the most frequently described abnormality of the ALK gene, occurring in approximately 3 7% of lung adenocarcinoma patients. Type: Tissue Block/ Slide Container/Tube: Slides from Tissue block Volume: 1stained H&E slide - 4 unstained slides Ambient Sunday-Wednesday 7:00am-3:00PM 14 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative A positive result (ALK rearrangement identified) is detected when the percent of cells with an abnormality exceeds the normal cutoff for the ALK probe set. A positive result suggests rearrangement of the ALK locus and a tumor that may be responsive to ALK inhibitor therapy. A negative result suggests no rearrangement of the ALK gene region at 2p Diagnostic Genomic Division DGD lab Guide Page 4 of 74
5 Title B CELL ACUTE LYMPHOBLASTIC LEUKEMIA PANEL BY FISH ITEM Days test is performed Turnaround time B-Acute Lymphoblastic Leukemia (ALL) is a disorder of B lymphoblast that accounts for the vast majority of children with acute leukemia and a fraction of adults with acute leukemia. B-ALL is broadly categorized as either having recurrent genetic abnormalities or not; recurrent genetic abnormalities include both balanced translocations and aneuploidy (Swerdlow et al. 2008). This FISH panel is designed to detect the most common, and/or prognosticaly -significant abnormalities in B-ALL (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression. As an adjunct to conventional chromosome studies. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Diagnostic Genomic Division DGD lab Guide Page 5 of 74
6 Location B-ALL is broadly categorized as either having recurrent genetic abnormalities or not; recurrent genetic abnormalities include both balanced translocations and aneuploidy (Swerdlow et al. 2008). This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in B-ALL (Swerdlow et al. 2008) Diagnostic Genomic Division DGD lab Guide Page 6 of 74
7 Title BURKITT S LYMPHOMA PANEL BY FISH ITEM Days test is performed Turnaround time This small, multiprobe panel contributes to the distinction of Burkitt s from large B-cell lymphoma on problematic specimens demonstrating borderline morphologic or immunophenotypic features, limited sample volume, or zero to low probability for successful karyotyping. Burkitt s lymphoma characteristically demonstrates a very high Ki67 staining index, strong CD10, and positive bcl-6 staining with negative staining for bcl-2. Burkitt s lymphomas typically reveal MYC translocation partnered to Ig heavy or light chain genes in the background of an otherwise simple karyotype. Rarely, Burkitt s lymphomas may lack MYC translocation. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Burkitt s lymphomas typically reveal MYC translocation partnered to Ig heavy or light chain genes in the background of an otherwise simple karyotype. Rarely, Burkitt s lymphomas may lack MYC translocation. Among large B-cell lymphomas, MYC translocation is Diagnostic Genomic Division DGD lab Guide Page 7 of 74
8 demonstrated in a small but significant subset, almost always in the background of a complex karyotype, presumably representing secondarily acquired genetic change. Frequently, these MYC+ large B-cell lymphomas are also positive for BCL2 or BCL6 rearrangements. Incomplete clinical evidence suggests that MYC+ large B- cell lymphomas may benefit from Burkitt-like chemotherapeutic regimens. Location Diagnostic Genomic Division DGD lab Guide Page 8 of 74
9 Title CHROMOSOMAL MICROARRAY ANALYSIS ITEM Chromosomal Microarray Analysis is useful for the detection of DNA copy number gains and losses associated with unbalanced chromosomal aberrations. The utility of this technology for the detection of gains and losses in patients with intellectual disabilities, autism/asd, and/ or congenital anomalies has been well documented and chromosomal microarray analysis is now recommended as a first tier test for these indications. 1. Type: Whole blood/ Cord blood Container/Tube: EDTA- Lavender top Volume: 3-5 ml preferred, minimum 1ml 2. Type: Amniotic Fluid Container/Tube: ml Sterile falcon tube/ container Volume: 20 ml 3. Type: CVS, Skin Biopsy and POC Container /Tube: Sterile Container containing normal saline/sterile transport media Weight/Volume: 20-30mg of specimen Note: Cord blood, Amniotic Fluid, CVS and POC should be accompanied with maternal blood (3-5ml in lavender top tube) to rule out maternal cell contamination Ambient Days test is Sunday to Thursday 07:00 AM to 02:00 PM performed Turnaround Postnatal acgh: 4 weeks time Prenatal acgh: 2 weeks Postnatal NICU: Products of conception/fibroblasts: 7 days 6 weeks Array Comparative Genomic Hybridization using Surescan High Resolution Technology Diagnostic Genomic Division DGD lab Guide Page 9 of 74
10 Reference Value Rejection Criteria Performing Lab Location Negative Copy number variants are classified based on known, predicted, or possible pathogenicity and reported with interpretive comments detailing their potential or known significance Bldg, Hamad Bin Khalifa Medical City, Doha. Tel: Diagnostic Genomic Division DGD lab Guide Page 10 of 74
11 Title CHROMOSOME ANALYSIS CONSTITUTIONAL ITEM Chromosome analysis is the microscopic examination of chromosomes in dividing cells. Such analysis can detect changes in chromosomal number and structure. Deletions (eg, partial monosomy), duplications (eg, partial trisomy), and structural abnormalities such as translocations, inversions, and rings can be detected. These chromosomal changes may be associated with infertility, miscarriage, stillbirth, birth defects, intellectual disability, developmental delay, or abnormalities of sexual differentiation and development. 1. Type: Whole blood/ Cord blood Container/Tube: Sodium Heparin- Green top Volume: 3-5 ml preferred, minimum 2ml 2. Type: Amniotic Fluid Container/Tube: ml Sterile falcon tube/ container Volume: 20 ml 3. Type: CVS Container /Tube: Sterile Container containing normal saline/sterile transport media Weight/Volume: 20-30mg of specimen Note: Cord blood, Amniotic Fluid and CVS should be accompanied with maternal blood (3-5ml in lavender top tube) to rule out Maternal cell contamination. Ambient Sunday to Thursday 07:00 AM to 02:00 PM Days test is performed Turnaround Amniotic fluid: 14 days time CVS: Peripheral blood: 14 days 7-28 days Cell Culture with Mitogens followed by Chromosome Analysis Reference Value Negative Diagnostic Genomic Division DGD lab Guide Page 11 of 74
12 The numerical and structural abnormalities are reported as per An International System for Human Cytogenomic Nomenclature (ISCN). The report includes chromosomal findings, clinical significance, and recommendations for additional studies (eg, FISH and microarray) when indicated. Rejection Criteria Location Bldg, Hamad Bin Khalifa Medical City, Doha. Tel: Diagnostic Genomic Division DGD lab Guide Page 12 of 74
13 Title CHROMOSOME ANALYSIS HEMATO ONCLOGY ITEM Days test is performed Turnaround time Location Chromosome analysis is the microscopic examination of chromosomes in dividing cells and can be used for hemato-oncology specimens to determie and diagnose the acquired chromosomal changes that are related to multiple malignancy types. This study also assists in classification of different malignant hematological disorders, monitoring effect of treatment and knowing the remission status of disorders. 1. Type: Whole blood Container/Tube: Sodium Heparin- Green top Volume: 3-5 ml preferred, minimum 2ml 2. Type: Bone Marrow Container/Tube: ml of Bone marrow transport media/ container Volume: 10 ml Ambient Sunday to Thursday 07:00 AM to 02:00 PM 21 Days Cell Culture without/ with Mitogens followed by Chromosome Analysis Negative The numerical and structural abnormalities are reported as per An International System for Human Cytogenomic Nomenclature (ISCN). The report includes chromosomal findings, clinical significance, and recommendations for additional studies (eg, FISH and microarray) when indicated Diagnostic Genomic Division DGD lab Guide Page 13 of 74
14 Title CHRONIC LYMPHOCYTIC LEUKEMIA PANEL BY FISH ITEM Used for detecting a neoplastic clone associated with the common chromosome abnormalities seen in patients with chronic lymphocytic leukemia (CLL). Identifying and tracking known chromosome abnormalities in patients with CLL and tracking response to therapy. Distinguishing patients with 11;14 translocations who have leukemic phase of mantle cell lymphoma from patients who have CLL. Detecting patients with atypical CLL or other forms of lymphoma associated translocation between IGH/CCND1 and ATM, TP53, D13S319 or other partner genes. Days test is performed Turnaround time Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml, Child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative This FISH test detects an abnormal clone in approximately 70% of patients with indolent disease and >80% of patients who require treatment. At least 5% of patients referred for CLL FISH testing have translocations involving the IGH locus; approximately 66% of these patients have translocations that result in fusion of IGH/CCND1, Fusion Diagnostic Genomic Division DGD lab Guide Page 14 of 74
15 of IGH and CCND1 is associated with t(11;14)(q13;q32), The prognostic associations for chromosome abnormalities detected by this FISH assay are, from best to worst: 13q-, normal, +12, 6q-, 11q-, and 17p-. Location Diagnostic Genomic Division DGD lab Guide Page 15 of 74
16 Title CHRONIC MYELOGENOUS LEUKEMIA PANEL BY FISH ITEM Days test is performed Turnaround time Used for detecting a neoplastic clone associated with a BCR/ABL1 rearrangement in patients with chronic myeloid leukemia (CML). Tracking the percentage of nuclei with BCR/ABL1 rearrangement and response to therapy in patients with CML. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Fusion of BCR/ABL1 is observed in all patients with chronic myeloid leukemia (CML), in approximately 25% of adult patients with precursor B-cell acute lymphoblastic leukemia (B-ALL) and in 1% of patients with pediatric B- ALL. The chromosome mechanism resulting in BCR/ABL1 fusion is a t(9;22)(q34;q11.2) in approximately 85%, a complex 9;22 translocation with 1 or more additional chromosomes in approximately 15% and a chromosomally "cryptic" or insertional translocation in fewer than 1% of Diagnostic Genomic Division DGD lab Guide Page 16 of 74
17 patients. Location Diagnostic Genomic Division DGD lab Guide Page 17 of 74
18 Title Diffuse Large B Cell Lymphoma (DLBCL) PANEL BY FISH ITEM Days test is performed Turnaround time This probe panel detects specific structural chromosome abnormalities commonly associated with Diffuse Large B- cell Lymphoma. Routine chromosome analysis performed on all diagnostic samples and is recommended on all bone marrow specimens to exclude abnormalities not identified by the specified FISH probe(s). Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Diffuse Large B-Cell Lymphoma (DLBCL) is a lymphoid neoplasm, particularly involving large (microscopically) B cells. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in DLBCL, and may aid in discrimination between is Diagnostic Genomic Division DGD lab Guide Page 18 of 74
19 DLBCL and other lymphomas (Swerdlow et al. 2008) as well as uncovering double hit lymphomas (Aukema et 2011). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. al. Location Diagnostic Genomic Division DGD lab Guide Page 19 of 74
20 Title DUCHENNE MUSCULAR DYSTROPHY GENE ANALYSIS BY MICROARRAY ITEM Days test is performed Turnaround time Chromosomal Microarray Analysis is useful for the detection of Micro deletions and duplications in Duchenne Muscular Dystrophy (DMD) and Beckers Muscular Dystrohy (BMD) genes. DMD/BMD gene analysis by CMA can also help in determining the carrier status in family members at the risk of having DMD/BMD. 1. Type: Whole blood/ Cord blood Container/Tube: EDTA- Lavender top Volume: 3-5 ml preferred, minimum 1ml 2. Type: Amniotic Fluid Container/Tube: ml Sterile falcon tube/ container Volume: 20 ml 3. Type: CVS, Skin Biopsy and POC Container /Tube: Sterile Container containing normal saline/ Sterile transport media Weight/Volume: 20-30mg of specimen Note: Cord blood, Amniotic Fluid, CVS and POC should be accompanied with maternal blood (3-5ml in lavender top tube) to rule out maternal cell contamination Ambient Sunday to Thursday 07:00 AM to 02:00 PM 28 Days Array Comparative Genomic Hybridization using Surescan High Resolution Technology on OGT CytoSure Platform. Negative DMD/BMD gene analysis by microarray is useful for studying exonic copy number variations. Deletions account for approximately 65% of DMD mutations and 85% of BMD mutations. Duplications occur in approximately 6 10% of Diagnostic Genomic Division DGD lab Guide Page 20 of 74
21 males with either DMD or BMD. Location Diagnostic Genomic Division DGD lab Guide Page 21 of 74
22 Title EXTRA NODAL MZL PANEL BY FISH ITEM Days test is performed Turnaround time Marginal Zone Lymphoma (MZL) is comprised of two lymphoid neoplasms: extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma) and nodal MZL; the former is more common than the latter and affects the GI tract most commonly, whereas MZL affects peripheral lymph nodes predominately. The two may also be discriminated with the translocation probes listed below. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in MZL (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml, Child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Marginal zone lymphomas (MZL) are distinct B cell neoplasms with variable clinical presentations. The Diagnostic Genomic Division DGD lab Guide Page 22 of 74
23 clinicopathologic entities include extranodal marginal zone MALT lymphoma, nodal marginal zone lymphoma (MZL), and splenic marginal zone lymphoma (MZL). The Extra-nodal MZL FISH panel includes: MALT1 dual-fusion probe, to detect rearrangement 1) on chromosome 18. 2) IGH break-apart probe, to detect disruption of IGH (14q32). 3) BCL6 break-apart probe to detect disruption of BCL6 and/or trisomy 3. Location Diagnostic Genomic Division DGD lab Guide Page 23 of 74
24 Title FFPE LYMPHOMA PANEL BY FISH ITEM Days test is performed Turnaround time Location Useful for detecting a neoplastic clone associated with the common chromosome abnormalities seen in patients with various B-cell lymphomas. Tracking known chromosome abnormalities and response to therapy in patients with B- cell lymphomas. This targeted panel is appropriate when clinical and morphologic evaluation is most suggestive of a low-grade/small B-cell lymphoma, and high-grade lymphomas (such as large cell anaplastic and Burkitt s lymphoma) are not a diagnostic consideration. Type: Tissue Block/ Slide Container/Tube: Slides from Tissue block Volume: 1stained H&E slide - 6 unstained slides Ambient Sunday-Wednesday 7:00am-3:00PM 14 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative A neoplastic clone is detected when the percent of cells with an abnormality exceeds the normal reference range for any given probe. Detection of an abnormal clone is supportive of a diagnosis of a B-cell lymphoma. The specific abnormality detected may help subtype the neoplasm. The absence of an abnormal clone does not rule out the presence of a neoplastic disorder. Fixatives other than formalin (eg, Prefer, Bouin) may not be successful for FISH assays Diagnostic Genomic Division DGD lab Guide Page 24 of 74
25 Title FOLLICULAR LYMPHOMA PANEL BY FISH ITEM This assay is useful to diagnose follicular lymphoma (> 75%) and diffuse large cell lymphomas (25%). Translocation t (14; 18) (q32; Q21. 3) is assayed by FISH with probes from the regions IgH (14q32) and BCL2 (18q21. 3). Days test is performed Turnaround time Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative This FISH assay specifically detects the t(14;18)(q32;q21) involving the BCL2 and IGH chain genes. This translocation is present in over 90% of follicular lymphomas and in a significant minority (20-30%) of diffuse large B cell lymphomas. It is characterized by the aberrant juxtaposition of the BCL2 proto-oncogene on chromosome 18 with the immunoglobulin heavy chain gene on chromosome 14, resulting in constitutive overexpression of the BCL2 protein which ultimately leads to alterations in programmed cell death (i.e., apoptosis) and tumor cell proliferation. Evaluation for a t(14;18)(q32;q21) is of use in the diagnostic evaluation for Diagnostic Genomic Division DGD lab Guide Page 25 of 74
26 follicular lymphoma as well as in the evaluation of aggressive B cell lymphomas where Burkitt's lymphoma (BL), diffuse large B cell lymphoma (DLBCL), and the intermediate category are diagnostic considerations. In aggressive B cell lymphoma, the presence of a t(14;18)(q32;q21) in addition to a MYC rearrangement argues against the diagnosis of BL. The presence of a t(14;18)(q32;q21) is seen more often in DLBCLs of germinal center cell type and has been reported to be a poor prognostic factor in some studies. Location Diagnostic Genomic Division DGD lab Guide Page 26 of 74
27 Title HAIRY CELL LEUKEMIA PANEL BY FISH ITEM Days test is performed Turnaround time Used for detecting a neoplastic clone associated with the common chromosome abnormalities seen in patients with Hairy cell leukemia (HCL). Identifying and tracking known chromosome abnormalities in patients with HCL and tracking response to therapy. Distinguishing patients with 11;14 translocations who have leukemic phase of HCL. Detecting patients with atypical HCL/CLL or other forms of lymphoma associated translocation between IGH/CCND1 and CEP12,TP53,deletion or other partner genes Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Hairy cell leukemia (HCL) is a low grade B-cell lymphoproliferative disorder that typically presents with splenomegaly, cytopenias, and diffuse bone marrow infiltration. There have been few cases in the literature of HCL presenting as lymphomas in extra-nodal locations, such as soft tissues and bones without circulating leukemic cells, splenomegaly, or iliac crest bone marrow involvement. Panel includes testing for the abnormalities Diagnostic Genomic Division DGD lab Guide Page 27 of 74
28 using the probes listed: Location Diagnostic Genomic Division DGD lab Guide Page 28 of 74
29 Title HER2 GENE ANALYSIS BY FISH ITEM Days test is performed Turnaround time Location Used as a prognostic indicator for patients with both nodepositive and node-negative primary and metastatic breast cancer. Guiding therapy, as patients with HER2 amplification may be candidates for therapies that target the human epidermal growth factor receptor 2 (HER2) proteins (eg, trastuzumab [Herceptin], pertuzumab, lapatinib). Confirming the presence of HER2 amplification in cases with 2+ (low level) or 3+ (high level) HER2 overexpression by immunohistochemistry. Type: Tissue Container/Tube: Slides from Tissue block Volume: 1stained H&E slide - 2 unstained slide Ambient Sunday-Wednesday 7:00am-3:00PM 14 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative An interpretive report is provided. Results are interpreted utilizing the 2013 American Society of Clinical Oncology (ASCO)/College of American Pathologists (CAP) guidelines Diagnostic Genomic Division DGD lab Guide Page 29 of 74
30 Title HYPEREOSINOPHILIC SYNDROME PANEL BY FISH ITEM Days test is performed Turnaround time Useful in providing genetic information for patients with hypereosinophilic syndrome (HES) and systemic mast cell disease (SMCD) involving CHIC2 deletion. Identifying and tracking chromosome abnormalities and response to therapy. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Imatinib mesylate, a small molecule tyrosine kinase inhibitor from the 2-phenylaminopyrimidine class of compounds, has shown activity in the treatment of malignancies that are associated with the constitutive activation of a specific subgroup of tyrosine kinases. A novel tyrosine kinase, generated from fusion of the Fip1- like 1 (FIP1L1) gene to the PDGFRA gene, was identified in 9 of 16 patients (56%) with hypereosinophilic syndrome (HES). This fusion results from an approximate 800 kb interstitial chromosomal deletion that includes the cysteine-rich hydrophobic domain 2 (CHIC2) loci at 4q12. Diagnostic Genomic Division DGD lab Guide Page 30 of 74
31 FIP1L1-PDGFRA is a constitutively activated tyrosine kinase that transforms hematopoietic cells, and is a therapeutic target for imatinib in a subset of HES patients. Location Diagnostic Genomic Division DGD lab Guide Page 31 of 74
32 Title MANTLE CELL LYMPHOMA PANEL BY FISH ITEM Days test is performed Turnaround time The 11;14 translocation is frequently associated with mantle cell lymphoma and may be found in other hematologic tumors such as multiple myeloma, plasma cell leukemia and chronic lymphocytic leukemia. This translocation results in the fusion of the immunoglobulin heavy chain gene (IGH), located at chromosome region 14q32, with the cyclin D1 (CCND1) gene, and located at chromosome region 11q13. Fluorescence in situ hybridization (FISH) in interphase nuclei and in metaphase spreads will detect the translocation. Results of this FISH assay should be considered in context of routine chromosome analysis, when possible. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am- 3:00PM 07 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Mantle-cell lymphoma (MCL) has a poorer prognosis than other small B-cell lymphomas, thus a definitive diagnosis is essential. The t(11;14)(q13;q32) associated with MCL juxtaposes portions of CCND1 (11q13) and IGH (14q32), Diagnostic Genomic Division DGD lab Guide Page 32 of 74
33 cyclin D1. Thus we resulting in over-expression of use FISH with a highly sensitive two-colour fluorescence in situ hybridization (FISH) method to detect t(11;14)(q13;q32) in nuclei isolated from Bone marrow samples. Location Diagnostic Genomic Division DGD lab Guide Page 33 of 74
34 Title MARGINAL MALT LYMPHOMA PANEL BY FISH ITEM Days test is performed Turnaround time Marginal Zone Lymphoma (MZL) is comprised of two lymphoid neoplasms: extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma) and nodal MZL; the former is more common than the latter and affects the GI tract most commonly, whereas MZL affects peripheral lymph nodes predominately. The two may also be discriminated with the translocation probes listed below. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in MZL (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 07 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative MALT lymphoma is the extra-nodal presentation of marginal zone B-cell lymphomas (MZBCL). The most common anomalies in extra-nodal MZBCL of MALT type Diagnostic Genomic Division DGD lab Guide Page 34 of 74
35 include: The t(11;18)(q21;q21) / API2-MLT fusion, having a 20-50% incidence. The translocation is associated with low-grade MALT lymphoma of the stomach, and of the lung. Importantly, this translocation was associated with increased rates of persistent disease or recurrence after HP eradication therapy. The translocation t(14;18)(q32;q21)/igh-mlt1 fusion, leading to enhanced MLT1 expression may occur in 10-20% of all MALT lymphomas. It is associated with MALT lymphoma of the liver, skin, ocular adnexa, lung and salivary gland. It was not found in MALT lymphomas of the stomach, intestine, thyroid, or breast. Location Diagnostic Genomic Division DGD lab Guide Page 35 of 74
36 Title MARGINAL ZONE PANEL BY FISH ITEM Days test is performed Turnaround time Marginal Zone Lymphoma (MZL) is comprised of two lymphoid neoplasms: extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma) and nodal MZL; the former is more common than the latter and affects the GI tract most commonly, whereas MZL affects peripheral lymph nodes predominately. The two may also be discriminated with the translocation probes listed below. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in MZL (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Marginal zone lymphomas (MZL) are distinct B cell neoplasms with variable clinical presentations. The clinicopathologic entities include extra nodal marginal Diagnostic Genomic Division DGD lab Guide Page 36 of 74
37 zone MALT lymphoma, nodal marginal zone lymphoma (MZL), and splenic marginal zone lymphoma (MZL). The MZL FISH panel includes: 1) IGH/MALT1 dual-fusion probe, to detect t(14;18); and for trisomy 18. 2) IGH break-apart probe, to detect disruption of IGH (14q32). 3) BCL6 break-apart probe to detect disruption of BCL6 and/or trisomy 3. 4) IGH/CCND1dual-fusion probe, to detect t(11;14); and for trisomy 14. 5) BIRC3/MALT1 (aka API2/MALT1) dual-fusion probe, to detect t(11;18). Location Diagnostic Genomic Division DGD lab Guide Page 37 of 74
38 Title MULTIPLE MYELOMA PANEL BY FISH ITEM Days test is performed Turnaround time The MM-MGUS FISH panel is often used as an initial diagnosis/pre-treatment panel for the detection of FISH and chromosome aberrations useful in prognosis in plasma cell myeloma. As malignant plasma cells often have a low proliferation index, conventional cytogenetics frequently yields normal results. When this happens, interphase FISH studies can increase the abnormality detection rate. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambien t Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Multiple Myeloma (MM) belongs to a family of neoplasms involving clonal expansion of immunoglobulin secreting B- cells, often with bone marrow involvement, resulting in anemia and leukopenia. Additionally, bone lesions are often seen. This FISH panel is designed to detect the prognosticallysignificant most common, and/or Diagnostic Genomic Division DGD lab Guide Page 38 of 74
39 abnormalities in Multiple Myeloma and related plasma cell neoplasms (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. Fluorescence in situ hybridization (FISH) for multiple myeloma (MM), targeting 13q14, IGH, TP53, on plasma enriched cells. Location Diagnostic Genomic Division DGD lab Guide Page 39 of 74
40 Title MYELODYSPLASTIC SYNDOME PANEL BY FISH ITEM Days test is performed Turnaround time Myelodysplastic syndrome (MDS) describes a group of clonal haematopoietic disorders resulting in ineffective production of one or more of the myeloid cell lineages; risk for transformation to AML is increased. MDS may occur de novo or may arise as a secondary malignancy associated with treatment. This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in MDS (Swerdlow et al. 2008). FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, or when material is inadequate for chromosomal analysis. Chromosome analysis is recommended either as an initial test for MDS or at least in conjunction with FISH. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative FISH studies can provide confirmatory evidence of MDS and can be used to provide clinical prognostic or diagnostic information. Clonal cytogenetic abnormalities are more frequently observed in cases of secondary MDS Diagnostic Genomic Division DGD lab Guide Page 40 of 74
41 (80% of patients) than in primary MDS (40%-60% of patients). The common chromosomal abnormalities associated with MDS include: inv (3), -5/5q-, -7/7q-, +8, 13q-, and 20q-. These abnormalities can be observed singly or in concert. In addition, MLL (KMT2A) rearrangements, t(1;3) and t(3;21) are more frequently associatedwithsecondarymds. Conventional chromosome analysis is the gold standard for identification of the common, recurrent chromosome abnormalities in MDS. Location Diagnostic Genomic Division DGD lab Guide Page 41 of 74
42 Title MYELOPROLIFERATIVE NEOPLASMS PANEL BY FISH ITEM Days test is performed Turnaround time Myeloproliferative neoplasm panel is useful for detection of neoplastic clone that is associated with chromosome abnormalities observed in patients with MPN, to evaluate specimens in which standard cytogenetic analysis has been unsuccessful, to identify and track chromosome abnormalities for follow up of patients, and to evaluate response to therapy. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative The classic, more common MPNs include chronic myelogenous leukemia (CML), essential thrombocythemia (ET), polycythemia vera (PV), and primary myelofibrosis (PMF). Chronic eosinophilic leukemia, not otherwise specified (CEL, NOS), systemic mastocytosis (SM), chronic neutrophilic leukemia (CNL), and unclassifiable MPN are rare. MPNs typically occur in adults 50 to 70 years old and are uncommon in individuals <20 years old. Diagnostic Genomic Division DGD lab Guide Page 42 of 74
43 Frequently, the onset is insidious and the clinical course indolent. Patient complaints may include fatigue and lethargy, weight loss, abdominal discomfort, easy bruising, night sweats, and swollen, painful joints. Physical examination may reveal pallor, enlargement of the spleen or liver, and petechiae. Distinguishing between the MPNs is often difficult because of the overlap of clinical and laboratory findings. For example, most MPNs result in increased numbers of granulocytes, RBCs, and/or platelets. Each MPN begins with effective hematopoiesis resulting in circulating mature blood cells, but may result in marrow failure due to myelofibrosis, ineffective hematopoiesis, or progression to acute myeloid leukemia (AML). Location Diagnostic Genomic Division DGD lab Guide Page 43 of 74
44 Title PML/RARA(DF)t(15;17)(q22;q21.1) BY FISH ITEM Days test is performed Turnaround time Useful for detecting the chromosomal abnormalities associated with acute promyelocytic Leukemia (APL), t(15;17) fusion or PML/RARA gene fusion. Detection of residual or recurrent APL. Monitoring the level of promyelocytic leukemia/retinoic acid receptor alpha (PML/RARA) in APL patients. The disease is characterized by a chromosomal translocation involving the retinoic acid receptor-alpha gene on chromosome 17 (RARA). In 95% of cases of APL, retinoic acid receptor-alpha (RARA) gene on chromosome 17 is involved in a reciprocal translocation with the promyelocytic leukemia gene (PML) on chromosome 15, a translocation denoted as t(15;17)(q22;q12). The RAR receptor is dependent on retinoic acid for regulation of transcription. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Acute promyelocytic leukemia (APL) accounts for 5% to 10% of acute myeloid leukemia, and generally has a good Diagnostic Genomic Division DGD lab Guide Page 44 of 74
45 prognosis with current treatment protocols. APL cells contain a fusion gene comprised of the downstream sequences of the retinoic acid receptor alpha gene (RARA) fused to the promoter region and upstream sequences of one of several genes, the most common (>80%) being the promyelocytic leukemia gene (PML). The fusion gene is designated PML/RARA and may be seen in a karyotype as t(15;17)(q22;q12). FISH analysis of nonproliferating (interphase) cells can be used to detect the common chromosome abnormalities observed in patients with AML. The abnormalities have diagnostic and prognostic relevance and this testing can also be used to track response to therapy. Location Diagnostic Genomic Division DGD lab Guide Page 45 of 74
46 Title T CELL ACUTE LYMPHOBLASTIC LEUKEMIA PANEL BY FISH ITEM Days test is performed Turnaround time Used for detecting a neoplastic clone associated with the common chromosome abnormalities seen in patients with T-cell acute lymphoblastic leukemia (T-ALL). This FISH panel is designed to detect the most common, and/or prognostically-significant abnormalities in T-ALL. FISH studies are useful adjuncts to complete chromosome studies, particularly when following an abnormal clone, assessing relapse and progression, as an adjunct to conventional chromosome studies. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Specific genetic abnormalities are identified in the majority of cases of T-ALL, although many of the classic abnormalities are "cryptic" by conventional chromosome studies and must be identified by FISH studies. Each of the genetic subgroups are important to detect and can be critical prognostic markers. One predictive marker, amplification of the ABL1 gene region, has been identified in 5% of T-ALL, and these patients may be responsive to Diagnostic Genomic Division DGD lab Guide Page 46 of 74
47 targeted tyrosine kinase inhibitors. Location Diagnostic Genomic Division DGD lab Guide Page 47 of 74
48 Title T CELL LYMPHOMA PANEL BY FISH ITEM Days test is performed Turnaround time Useful for detecting a neoplastic clone associated with the common chromosome abnormalities seen in patients with various T-cell lymphomas. Tracking known chromosome abnormalities and response to therapy in patients with T- cell lymphoma Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative T-cell neoplasms are relatively uncommon, accounting for approximately 12% of all non-hodgkin lymphomas. There are several subtypes of T-cell neoplasms: T-cell acute lymphoblastic leukemia (T-ALL), T-cell prolymphocytic leukemia (T-PLL), T-cell large granular lymphocytic leukemia (T-LGL), anaplastic large cell lymphoma (ALCL), peripheral T-cell lymphoma, and various other cutaneous, nodal, and extranodal lymphoma subtypes. The 2 most prevalent lymphoma subtypes are unspecified peripheral T-cell lymphoma (3.7%) and ALCL (2.4%). T-cell neoplasms are among the most aggressive of all Diagnostic Genomic Division DGD lab Guide Page 48 of 74
49 hematologic and lymphoid neoplasms with the exception of ALCL, which is usually responsive to chemotherapy. Location Diagnostic Genomic Division DGD lab Guide Page 49 of 74
50 Title TRANSPLANTATION MONITORING BY FISH ITEM Days test is performed Turnaround time FISH studies can be used to detect chimerism for XX and XY cells to evaluate successful engraftment post-bone marrow transplant. Serial FISH chimerism studies are useful in monitoring these patients. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative In patients who underwent allogeneic hematopoietic stem cell transplantation, engraftment (chimerism) studies are used to evaluate the level of donor versus recipient cells in post-transplant peripheral blood or bone marrow specimens (and/ or specific sorted cell populations). In order to proceed with engraftment analysis, a pretransplant specimen is obtained from the recipient and from the donor. DNA from each pre-transplant specimen is extracted and stored for future comparison with posttransplant specimens from the recipient. X and Y chromosome status is used to quantify donor/recipient cells in sex mismatch transplants, allowing assessment of engraftment. Diagnostic Genomic Division DGD lab Guide Page 50 of 74
51 Location Diagnostic Genomic Division DGD lab Guide Page 51 of 74
52 Title WALDENSTROMS MACROGLOBULINEMIA BY FISH ITEM Days test is performed Turnaround time Waldenström s macroglobulinemia (WM) is an indolent and incurable B-cell neoplasm defined by the accumulation of lymphoplasmacytic cells in the bone marrow and characterized by the hypersecretion of monoclonal immunoglobulin M (IgM) protein.1 Representing 1 2% of hematologic cancers. Type: Blood/Leukemic Blood Container/Tube: Green top (sodium heparin) Volume: 2-6 ml (Varies depending on the (Adult ml,child - 2 ml, Infant - 2 ml) Type: Bone marrow Container/Tube: Bone Marrow Media Volume: 1-3 ml (Varies depending on the Ambient Sunday-Wednesday 7:00am-3:00PM 7 Days Interphase Fluorescence In situ Hybridization (ifish) study. Negative Initial cytogenetic studies reported chromosomal abnormalities in around 10 20% of patients with WM, spanning observations involving IGH (14q32) to trisomy 12 to deletion of 6q.FISH analyses has consistently indicated that IGH of immunoglobulin heavy chain (IgH) are infrequently detected in WM with IGH rearrangments. Diagnostic Genomic Division DGD lab Guide Page 52 of 74
53 Location Molecular Genetics Section: Acquired malignancies Haemato-Oncology: Quantitation BCR-ABL1 transcript levels Test BCR-ABL1 Quantitation Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days Real time PCR (ABI Quant Studio) quantitative analysis of cdna using Europe Against Cancer standardized primers and Qiagen-Ipsogen quantitation standards (Qiagen, Germany). Control Gene Transcript levels location Quantitative assessment of mutation burden in leukemia patients undergoing treatment with tyrosine kinase inhibitors. Bldg, Hamad Bin Khalifa Medical City, Doha. Tel: moleculargenetics@hamad.qa Diagnostic Genomic Division DGD lab Guide Page 53 of 74
54 BCR-ABL1 Characterisation Test BCR-ABL1 Breakpoint Characterisation Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days RT-PCR analysis of cdna following extraction of total RNA from blood/marrow Negative Diagnosis of Chronic Myeloid Leukemia location moleculargenetics@hamad.qa CALR MUTATION TESTING Test CALR MUTATION TESTING Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days PCR analysis of genomic DNA followed by fragment analysis for detection of size changes representative of somatic insertion/deletion mutations within exon 9 of the CALR gene. Wild Type Diagnosis of Myeloproliferative Neoplasm location moleculargenetics@hamad.qa Diagnostic Genomic Division DGD lab Guide Page 54 of 74
55 FLT3-itd MUTATION TESTING Test FLT3-itd MUTATION TESTING Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days PCR analysis of genomic DNA followed by fragment analysis for detection of size changes representative of somatic duplications within exons 14 & 15 of the FLT3 gene. Wild Type Diagnosis of Acute Myeloid Leukemia location moleculargenetics@hamad.qa Diagnostic Genomic Division DGD lab Guide Page 55 of 74
56 JAK2 V617F MUTATION TESTING Test JAK2 V617F MUTATION TESTING Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days Real time PCR (Lightcycler) semi quantitative analysis of genomic DNA using the MutaSearch detection kit (Qiagen, Germany). Wild Type Sequence Diagnosis of Myeloproliferative Disorder location moleculargenetics@hamad.qa NPM1 MUTATION TESTING Test NPM1 MUTATION TESTING Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days PCR analysis of genomic DNA followed by fragment analysis for detection of size changes representative of somatic duplications within exons 12 of the NPM1 gene. Wild Type Diagnosis of Acute Myeloid Leukemia location moleculargenetics@hamad.qa Diagnostic Genomic Division DGD lab Guide Page 56 of 74
57 Quantitation of PML-RARA transcript levels Test PML-RARA Quantitation Days Test is Performed Turnaround Time 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days Real time PCR (ABI Quant Studio) quantitative analysis of cdna using Europe Against Cancer standardized primers and Qiagen-Ipsogen quantitation standards (Qiagen, Germany). Control Gene Transcript levels location Quantitative assessment of mutation burden in Acute Promyelocytic leukemia patients undergoing treatment with targeted therapies moleculargenetics@hamad.qa Diagnostic Genomic Division DGD lab Guide Page 57 of 74
58 Immunoglobulin and T cell Receptor gene rearrangement Clonality Assessment HAEMATO ONCOLOGY Days Test is Performed Turnaround Time Immunoglobulin and T cell Receptor gene rearrangement Clonality Assessment 3-5mls Blood or Marrow in EDTA within 24 hours of the patient being bled. Ambient ( c) Batched Weekly 10 working days PCR analysis of genomic DNA followed by fragment analysis for detection of size changes representative of T and /or B cell clonality. Negative Diagnosis of Lymphoproliferative Disorders location Diagnostic Genomic Division Department of Laboratory Medicine & Pathology Third Floor -Qatar Rehabilitation Institute (QRI) Hamad Bin Khalifa Medical City (HBKM) Diagnostic Genomic Division DGD lab Guide Page 58 of 74
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Role of FISH in Hematological Cancers
 Role of FISH in Hematological Cancers Thomas S.K. Wan PhD,FRCPath,FFSc(RCPA) Honorary Professor, Department of Pathology & Clinical Biochemistry, Queen Mary Hospital, University of Hong Kong. e-mail: wantsk@hku.hk
Role of FISH in Hematological Cancers Thomas S.K. Wan PhD,FRCPath,FFSc(RCPA) Honorary Professor, Department of Pathology & Clinical Biochemistry, Queen Mary Hospital, University of Hong Kong. e-mail: wantsk@hku.hk
JAK2 V617F analysis. Indication: monitoring of therapy
 JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
MPL W515L K mutation
 MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
CYTOGENETICS INTRODUCTION SPECIAL INSTRUCTIONS ON SAMPLE COLLECTION AND HANDLING
 INTRODUCTION The Cytogenetics Laboratory offers a comprehensive array of chromosome investigations for cancers, constitutional abnormalities, and prenatal and postnatal diagnosis. Analyses are performed
INTRODUCTION The Cytogenetics Laboratory offers a comprehensive array of chromosome investigations for cancers, constitutional abnormalities, and prenatal and postnatal diagnosis. Analyses are performed
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms
 Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
GENETIC MARKERS IN LYMPHOMA a practical overview. P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute
 GENETIC MARKERS IN LYMPHOMA a practical overview P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute B and T cell monoclonalities Rearrangement of immunoglobin and TCR genes may help
GENETIC MARKERS IN LYMPHOMA a practical overview P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute B and T cell monoclonalities Rearrangement of immunoglobin and TCR genes may help
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
[COMPREHENSIVE GENETIC ASSAY PANEL ON
 2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
Significance of Chromosome Changes in Hematological Disorders and Solid Tumors
 Significance of Chromosome Changes in Hematological Disorders and Solid Tumors Size of Components of Human Genome Size of haploid genome 3.3 X 10 9 DNA basepairs Estimated genetic constitution 30,000
Significance of Chromosome Changes in Hematological Disorders and Solid Tumors Size of Components of Human Genome Size of haploid genome 3.3 X 10 9 DNA basepairs Estimated genetic constitution 30,000
Significance of Chromosome Changes in Hematological Disorders and Solid Tumors
 Significance of Chromosome Changes in Hematological Disorders and Solid Tumors Size of Components of Human Genome Size of haploid genome! Estimated genetic constitution! Size of average chromosome
Significance of Chromosome Changes in Hematological Disorders and Solid Tumors Size of Components of Human Genome Size of haploid genome! Estimated genetic constitution! Size of average chromosome
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Combinations of morphology codes of haematological malignancies (HM) referring to the same tumour or to a potential transformation
 Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
September 04, 2008
 27027 Tourney Road Valencia, CA 91355 800 421 7110 www.specialtylabs.com Test Updates September 04, 2008 Dear Valued Client: As you may be aware, in recent years there has been a tremendous challenge in
27027 Tourney Road Valencia, CA 91355 800 421 7110 www.specialtylabs.com Test Updates September 04, 2008 Dear Valued Client: As you may be aware, in recent years there has been a tremendous challenge in
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
TEST MENU TEST CPT CODES TAT. Chromosome Analysis Bone Marrow x 2, 88264, x 3, Days
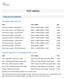 TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Molecular Diagnosis. Nucleic acid based testing in Oncology
 Molecular Diagnosis Nucleic acid based testing in Oncology Objectives Describe uses of NAT in Oncology Diagnosis, Prediction, monitoring. Genetics Screening, presymptomatic testing, diagnostic testing,
Molecular Diagnosis Nucleic acid based testing in Oncology Objectives Describe uses of NAT in Oncology Diagnosis, Prediction, monitoring. Genetics Screening, presymptomatic testing, diagnostic testing,
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Nucleic Acid Testing - Oncology. Molecular Diagnosis. Gain/Loss of Nucleic Acid. Objectives. MYCN and Neuroblastoma. Molecular Diagnosis
 Nucleic Acid Testing - Oncology Molecular Diagnosis Nucleic acid based testing in Oncology Gross alterations in DNA content of tumors (ploidy) Gain/Loss of nucleic acids Markers of Clonality Oncogene/Tumor
Nucleic Acid Testing - Oncology Molecular Diagnosis Nucleic acid based testing in Oncology Gross alterations in DNA content of tumors (ploidy) Gain/Loss of nucleic acids Markers of Clonality Oncogene/Tumor
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Fluorescence in-situ Hybridization (FISH) ETO(RUNX1T1)/AML1(RUNX1) or t(8;21)(q21.3;q22)
 PML/RARA t(15;17) Translocation Assay Result : nuc ish(pml 2)(RARA 2)[200] : 200/200(100%) interphase nuclei show normal 2O 2G signals for PML/RARA : is Negative for t(15;17)(q22;q21.1) 2 Orange 2 Green
PML/RARA t(15;17) Translocation Assay Result : nuc ish(pml 2)(RARA 2)[200] : 200/200(100%) interphase nuclei show normal 2O 2G signals for PML/RARA : is Negative for t(15;17)(q22;q21.1) 2 Orange 2 Green
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Canadian College of Medical Geneticists (CCMG) Cytogenetics Examination. May 4, 2010
 Canadian College of Medical Geneticists (CCMG) Cytogenetics Examination May 4, 2010 Examination Length = 3 hours Total Marks = 100 (7 questions) Total Pages = 8 (including cover sheet and 2 pages of prints)
Canadian College of Medical Geneticists (CCMG) Cytogenetics Examination May 4, 2010 Examination Length = 3 hours Total Marks = 100 (7 questions) Total Pages = 8 (including cover sheet and 2 pages of prints)
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Hematopathology Case Study
 www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
Addressing the challenges of genomic characterization of hematologic malignancies using microarrays
 Addressing the challenges of genomic characterization of hematologic malignancies using microarrays Sarah South, PhD, FACMG Medical Director, ARUP Laboratories Department of Pediatrics and Pathology University
Addressing the challenges of genomic characterization of hematologic malignancies using microarrays Sarah South, PhD, FACMG Medical Director, ARUP Laboratories Department of Pediatrics and Pathology University
Case #16: Diagnosis. T-Lymphoblastic lymphoma. But wait, there s more... A few weeks later the cytogenetics came back...
 Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Diagnostic Approach for Eosinophilia and Mastocytosis. Curtis A. Hanson, M.D.
 Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Hepatic Lymphoma Diagnosis An Algorithmic Approach
 Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
CYTOGENETICS Dr. Mary Ann Perle
 CYTOGENETICS Dr. Mary Ann Perle I) Mitosis and metaphase chromosomes A) Chromosomes are most fully condensed and clearly distinguishable during mitosis. B) Mitosis (M phase) takes 1 to 2 hrs and is divided
CYTOGENETICS Dr. Mary Ann Perle I) Mitosis and metaphase chromosomes A) Chromosomes are most fully condensed and clearly distinguishable during mitosis. B) Mitosis (M phase) takes 1 to 2 hrs and is divided
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation
 a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Molecular Hematopathology
 Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
LYMPHOMAS an overview of some subtypes of NHLs
 One of the confusing aspects of the lymphoid neoplasms concerns the use of the descriptive terms "leukemia" and "lymphoma." LYMPHOMAS an overview of some subtypes of NHLs Leukemia is used for lymphoid
One of the confusing aspects of the lymphoid neoplasms concerns the use of the descriptive terms "leukemia" and "lymphoma." LYMPHOMAS an overview of some subtypes of NHLs Leukemia is used for lymphoid
PhenoPath. Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA
 PhenoPath Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA C urrent diagnosis of B cell non-hodgkin lymphoma (B-NHL) is based on the 2008 WHO Classification of Tumours of Haematopoietic and Lymphoid
PhenoPath Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA C urrent diagnosis of B cell non-hodgkin lymphoma (B-NHL) is based on the 2008 WHO Classification of Tumours of Haematopoietic and Lymphoid
Use of MYC, BCL2 and BCL6 FISH for investigations of high grade B cell lymphoma
 Use of MYC, BCL2 and BCL6 FISH for investigations of high grade B cell lymphoma Dr Anthony Bench Haematopathology and Oncology Diagnostic Service Cambrıdge Unıversıty Hospitals NHS Foundatıon Trust Cambridge
Use of MYC, BCL2 and BCL6 FISH for investigations of high grade B cell lymphoma Dr Anthony Bench Haematopathology and Oncology Diagnostic Service Cambrıdge Unıversıty Hospitals NHS Foundatıon Trust Cambridge
HEMATOPATHOLOGY SERVICES
 HEMATOPATHOLOGY SERVICES Know what your patient s future holds, NOW. Driven by patient care, GoPath Laboratories has set a new standard for hematologic cancer testing. thick, 2 slides per probe minimum
HEMATOPATHOLOGY SERVICES Know what your patient s future holds, NOW. Driven by patient care, GoPath Laboratories has set a new standard for hematologic cancer testing. thick, 2 slides per probe minimum
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU
 Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Hypereosinophili c syndrome
 Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Methods used to diagnose lymphomas
 Institut für Pathologie Institut für Pathologie Methods used to diagnose lymphomas Prof. Dr.Med. Leticia Quintanilla-Fend Molecular techniques NGS histology Cytology AS-PCR Sanger seq. MYC Immunohistochemistry
Institut für Pathologie Institut für Pathologie Methods used to diagnose lymphomas Prof. Dr.Med. Leticia Quintanilla-Fend Molecular techniques NGS histology Cytology AS-PCR Sanger seq. MYC Immunohistochemistry
CLL Complete SM Report
 Reported: 02/01/2012 Σ CGI ID No:5 Client:r Client Address: CLINICAL DATA: Lymphoma No CBC results provided. CLL Complete SM Report FINAL DIAGNOSIS: CD19+ B cell lymphoma, ZAP-70 + (44%), with borderline
Reported: 02/01/2012 Σ CGI ID No:5 Client:r Client Address: CLINICAL DATA: Lymphoma No CBC results provided. CLL Complete SM Report FINAL DIAGNOSIS: CD19+ B cell lymphoma, ZAP-70 + (44%), with borderline
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
Welcome to Master Class for Oncologists. Session 3: 9:15 AM - 10:00 AM
 Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Molecular Hematopathology Leukemias I. January 14, 2005
 Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Template for Reporting Results of Monitoring Tests for Patients With Chronic Myelogenous Leukemia (BCR-ABL1+)
 Template for Reporting Results of Monitoring Tests for Patients With Chronic Myelogenous Leukemia (BCR-ABL1+) Version: CMLBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is
Template for Reporting Results of Monitoring Tests for Patients With Chronic Myelogenous Leukemia (BCR-ABL1+) Version: CMLBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
Small B-cell (Histologically Low Grade) Lymphoma
 Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
WBCs Disorders. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
Prepared by: Dr.Mansour Al-Yazji
 C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms
 Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Template web posting date: December 2014 Authors Todd W. Kelley, MD, FCAP University of Utah and ARUP Laboratories,
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Template web posting date: December 2014 Authors Todd W. Kelley, MD, FCAP University of Utah and ARUP Laboratories,
Understanding the Human Karyotype Colleen Jackson Cook, Ph.D.
 Understanding the Human Karyotype Colleen Jackson Cook, Ph.D. SUPPLEMENTAL READING Nussbaum, RL, McInnes, RR, and Willard HF (2007) Thompson and Thompson Genetics in Medicine, 7th edition. Saunders: Philadelphia.
Understanding the Human Karyotype Colleen Jackson Cook, Ph.D. SUPPLEMENTAL READING Nussbaum, RL, McInnes, RR, and Willard HF (2007) Thompson and Thompson Genetics in Medicine, 7th edition. Saunders: Philadelphia.
Pathology of the indolent B-cell lymphomas Elias Campo
 Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation
 Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
Oncology Cytogenetics Diagnostic Service - User Guide 2014
 Oncology Cytogenetics Diagnostic Service - User Guide 2014 Contact details Address: Cytogenetics Department 5 th Floor Tower Wing Guy s Hospital Great Maze Pond London SE1 9RT General enquiries 0207 188
Oncology Cytogenetics Diagnostic Service - User Guide 2014 Contact details Address: Cytogenetics Department 5 th Floor Tower Wing Guy s Hospital Great Maze Pond London SE1 9RT General enquiries 0207 188
Outline. Chromosomal analysis FISH. Chromosomal abnormalities in cancer. Clinical application of cytogenetics. Procedure Nomenclature
 Outline Chromosomal analysis Procedure Nomenclature FISH Procedure Probes Multicolor-FISH CGH Chromosomal abnormalities in cancer CML, MPD, MDS, AML, ALL, CLL, myeloma, lymphoma Clinical application of
Outline Chromosomal analysis Procedure Nomenclature FISH Procedure Probes Multicolor-FISH CGH Chromosomal abnormalities in cancer CML, MPD, MDS, AML, ALL, CLL, myeloma, lymphoma Clinical application of
Oncology Genetics: Cytogenetics and FISH 17/09/2014
 Oncology Genetics: Cytogenetics and FISH 17/09/2014 Chris Wragg Head of Oncology Genomics, BGL BGL Bristol Genetics Laboratory (BGL) CPA accredited Genetics laboratory serving a core population of 4-5million
Oncology Genetics: Cytogenetics and FISH 17/09/2014 Chris Wragg Head of Oncology Genomics, BGL BGL Bristol Genetics Laboratory (BGL) CPA accredited Genetics laboratory serving a core population of 4-5million
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms
 Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD
 HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
Haematology Probes for Multiple Myeloma
 Haematology Probes for Multiple Myeloma MULTIPLE MYELOMA Multiple myeloma (MM) is a plasma cell neoplasm, characterised by the accumulation of clonal plasma cells in the bone marrow and by very complex
Haematology Probes for Multiple Myeloma MULTIPLE MYELOMA Multiple myeloma (MM) is a plasma cell neoplasm, characterised by the accumulation of clonal plasma cells in the bone marrow and by very complex
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Genetic Testing Oncology
 Genetic Testing Oncology Policy Number: Original Effective Date: MM.02.010 05/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 05/01/2014 Section: Medicine Place(s) of Service:
Genetic Testing Oncology Policy Number: Original Effective Date: MM.02.010 05/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 05/01/2014 Section: Medicine Place(s) of Service:
