HPV Vaccine Protein L1 Predicts Disease Outcome of High-Risk HPV+ Early Squamous Dysplastic Lesions
|
|
|
- Vivien Thompson
- 6 years ago
- Views:
Transcription
1 Anatomic Pathology / Predictive Value of HPV Protein L1 HPV Vaccine Protein L1 Predicts Disease Outcome of High-Risk HPV+ Early Squamous Dysplastic Lesions Henrik Griesser, MD, 1 Heinz Sander, MD, 2 Cindy Walczak, 2 and Ralf A. Hilfrich, PhD 3 Key Words: Cervical intraepithelial neoplasia; CIN; Papanicolaou smear; Human papillomavirus; HPV; HPV L1 capsid protein; Cytology; Biopsy; Prognostic biomarker CME/SAM Upon completion of this activity you will be able to: define the role of the L1 capsid protein in the life cycle of human papillomaviruses in squamous epithelium. outline the setting(s) in which L1 capsid staining may have a role in clinical management of patients with cervical squamous intraepithelial lesion. describe appropriate follow-up strategies for women with positive and negative nuclear staining for L1 capsid in cervical biopsies with squamous intraepithelial lesion. The ASCP is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians. The ASCP designates this educational activity for a maximum of 1 AMA PRA Category 1 Credit per article. This activity qualifies as an American Board of Pathology Maintenance of Certification Part II Self-Assessment Module. The authors of this article and the planning committee members and staff have no relevant financial relationships with commercial interests to disclose. Questions appear on p 973. Exam is located at Abstract Prediction of the clinical outcome of nonadvanced, early dysplastic lesions is one of the unresolved problems of cervical cancer screening programs. We examined the influence of human papillomavirus (HPV) L1 capsid protein detection in a randomized, prospective study of 187 high-risk HPV+ early dysplastic lesions during 36 to 46 months. The difference in the clinical outcome of the HPV L1 cases and the HPV L1+ cases was highly statistically significant (P <.0001) and independent of the classification of low-grade squamous intraepithelial lesion (mild dysplasia) and high-grade squamous intraepithelial lesion of the moderate dysplastic type. L1+ mild and moderate dysplasias, reflecting productive HPV infection, showed low malignant potential, justifying a wait-and-watch strategy to prevent overtreatment, especially in young women. L1 early dysplastic lesions, as nonproductive infections or precancerous lesions, have a high malignancy potential and close follow-up with colposcopy and histologic evaluation should be advised. Even with the vaccination era rising, human papillomavirus (HPV) will remain a major global health burden, inducing a range of malignant and benign diseases. Women, in particular, are experiencing the consequences of HPV infection, with about 500,000 new cases of invasive cervical cancers annually. 1 Cervical cancer screening programs for the detection of preinvasive cervical neoplasia are highly effective and caused a decline in the incidence of invasive cervical carcinomas. 2,3 As a result, cervical precancerous lesions are being diagnosed frequently, and the cost for treatment of low-grade intraepithelial lesions soared in recent years. 4 In young women, conizations are being performed frequently for high-grade lesions with a potentially negative impact on reproductive outcomes. To improve women s quality of life and health care resources, it would be most useful to have prognostic markers distinguishing patients who will experience progression of an early precursor lesion to cancer from patients who will not. 5 Such a risk assessment is equally important for borderline abnormalities such as atypical squamous cell of undetermined significance (ASC-US) and squamous intraepithelial lesion (SIL) of undetermined grade. Data from the ASCUS-LSIL Triage Study (ALTS) confirmed that HPV DNA testing is not a useful triage strategy in low-grade SIL (LSIL) cases 6 and that it is still unresolved whether cervical intraepithelial neoplasia grade 2 (CIN 2) represents low- or high-grade disease in individual lesions. Therefore, more specific tools are needed to identify women who are at risk for progressive lesions, ie, to discriminate HPV infection from real precancer. 7 Different reporting systems are used for Papanicolaou (Pap) smear diagnoses. Besides the original World Health Organization classification, 8 the Bethesda System (TBS) 9 is internationally accepted. In Germany, the Munich 840 Am J Clin Pathol 2009;132: Downloaded 840 from
2 Anatomic Pathology / Original Article Nomenclature II is being recommended, 10 which puts mild and moderate dysplasia in group IIID, with recommendation for cytologic follow-up and colposcopy. Germany s watch-andwait strategy offers the opportunity to investigate the clinical outcome of cytologically detected moderate dysplasia because independent of the reporting system, it is known that 10% of the mild and 20% of the moderate dysplastic lesions develop CIN 3+ lesions, but most of them regress spontaneously. 11,12 Many anogenital cancers, particularly squamous cell carcinoma of the cervix, are induced by epitheliotropic DNA tumor viruses, specifically the HPVs. 13 A large number of HPV types are known to infect the anogenital tract, but only a subset, the high-risk types, is frequently found in malignant lesions. 14 L1, or the major capsid protein, is 1 of 8 known HPVspecific proteins (E1, E2, E4, E5, E6, E7, L1, and L2). During the productive phase of the viral life cycle, the L1 capsid protein (together with L2, the minor capsid protein) is produced within the cytoplasm and translocated into the nucleus, immunochemically visible by a strong nuclear staining reaction in intermediate and superficial squamous epithelial cells. The viral DNA is encapsulated by 360 L1 capsid proteins to build new infectious viral particles that are released in the upper epithelial layer. 13 The presence of L1 capsid protein within the dysplastic cells, as evidenced by L1 capsid protein positive cases, is proof of a completed HPV life cycle. L1 capsid protein negative cases, however, have lost the ability to produce virions depending on squamous epithelial cell differentiation. In 2003, Melsheimer et al 15 reported that most of the high-risk HPV-associated LSILs express HPV L1 capsid protein, but most of the high-risk HPV-associated high-grade squamous intraepithelial lesions (HSILs) failed to synthesize HPV L1 capsid protein. It was suggested that a loss of viral L1 capsid protein, a major target of the immune response in HPV-infected SIL, could function as a prognostic marker for the development of CIN lesions. 15,16 We subsequently confirmed this in a retrospective study with a median follow-up of 22.8 months on 84 routinely performed Pap smears. We showed that high-risk HPV-associated mild to moderate dysplastic squamous lesions without immunochemically detectable HPV L1 capsid protein are significantly more likely to progress (76.4%) than are L1+ cases (23.6%). 17 Similar results regarding the prognostic relevance of HPV L1 capsid protein were obtained in different retrospective studies using cytology and biopsy specimens Materials and Methods Patients and Design In 2005, we started a randomized, prospective study with cytologic diagnoses according to TBS and the Munich nomenclature because the 2 main criticisms of our initial study 17 were its retrospective approach and the application of the Munich nomenclature only. On each working day, we recruited the first high-risk HPV+ mild or moderate dysplasia case (as defined by the World Health Organization classification) from the general screening population. A high-risk HPV association was confirmed with the Hybrid Capture II test (Digene/Qiagen, Hilden, Germany). The 211 conventional Pap smears and ThinPrep slides were independently classified (by H.G. and H.S.) according to the Second Munich Cytological Nomenclature (mild and moderate dysplasia as group IIID) and diagnosed according to TBS as LSIL (mild dysplasia) and HSIL (moderate dysplasia). Established cytologic criteria were applied to define mild and moderate dysplasia. 21 Informed consent from the patients was not necessary because the samples were received and analyzed anonymously and patients were treated according to the German Munich nomenclature with cytologic follow-up and colposcopy for mild and moderate dysplastic lesions. Follow-up smears were obtained at intervals of 3 to 6 months or annually after the first negative smear for intraepithelial lesions. A conization for treatment and/or histologic verification was performed if clinically indicated and with the patient s consent. Follow-up ended in December 2008, resulting in a follow-up period of 36 to 46 months. The clinical outcome was understood as possible remission, persistence, or progression of the lesion. Women having at least 2 consecutive smears negative for an intraepithelial lesion were considered to be in remission. Persistence was defined as the state in which mild and moderate dysplasia persisted cytologically during the whole follow-up period or as histologically CIN 1 or CIN 2. Progression was defined as a histologically confirmed CIN 3+ lesion because interrater and intraobserver reproducibility for CIN 3 histology is high and considerably better than that for CIN 2 histomorphology. 7 All histologic diagnoses were from conization specimens. The 2-sided Fisher exact test was used for data analysis. Immunochemical Studies At presentation, routinely processed conventional Pap smears and ThinPrep slides (Hologic, Bedford, MA) were immunochemically stained with the Cytoactiv Screening Set (Cytoimmun Diagnostics, Pirmasens, Germany), which detects the L1 capsid protein of all known HPV types. Staining was performed according to the manufacturer s protocol. In brief, slides were subjected to antigen unmasking by microwave treatment after unmounting without prior destaining. Cytoactiv screening antibody was applied to the slides and incubated for 30 minutes at room temperature, followed by incubation with the detection reagents for 10 minutes and AEC chromogen for 5 minutes. Downloaded from Am J Clin Pathol 2009;132:
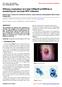
3 Griesser et al / Predictive Value of HPV Protein L1 After counterstaining with hematoxylin, slides were mounted with Aquatex (Merck, Darmstadt, Germany) and coverslipped. Stained slides were studied by light microscopy independently (by H.S. and H.G.). Slides with at least 1 epithelial cell with distinctly positive nuclear staining were scored as positive Image 1. This cutoff is recommended for the Cytoactiv assay and was used in all studies published so far, based on our initial work 17 showing that only the presence, not the amount of staining intensity of positive nuclei, correlated with the clinical course. Results The mean age of the 211 patients was 33.6 years (range, years). The mean was 34.8 years (range, years) for the LSIL group (n = 78 [37.0%]) and 32.9 years (range, years) for the HSIL group (n = 133 [63.0%]). Of the 211 high-risk HPV-associated early dysplastic lesions, 119 (56.4%) were L1 and 92 (43.6%) were L1+, with a profoundly different outcome between the 2 groups but independent of the classification as LSIL or HSIL. The mean age in the L1 group was 33.7 years (range, years) and 33.4 years (range, years) for the L1+ group. Of the 119 L1 cases, 36 (30.3%) were initially diagnosed as LSIL (mean age, 34.3 years) and 83 (69.7%) as HSIL (mean age, 33.4 years). Initially 42 (46%) of 92 L1+ cases were diagnosed as LSIL (mean age, 35 years) and 50 (54%) as HSIL (mean age, 32 years) Table 1. For data analysis, 187 cases with complete clinical records were included Table 2. Of 211 cases, 22 (5 HSIL and 17 LSIL) were lost during the follow-up period, and 2 HSIL L1 cases were excluded owing to inconsistencies in clinical records. Independent of the designation as LSIL or HSIL, 43 (61%) of 71 L1+ but only 6 (5.2%) of 116 L1 cases showed spontaneous remission of the lesion. In contrast, only 18 (25%) of 71 L1+ but 84 (72.4%) of 116 L1 cases progressed to CIN 3+, including 4 invasive carcinomas in the L1 HSIL cases only. The remission rate was highest among the L1+ LSIL (66% [21/32]) and HSIL cases (56% [22/39]) and lowest in the L1 LSIL (11% [4/36]) and HSIL (3% [2/80]) groups. In contrast, the rate of progression was highest in the L1 HSIL group (79% [63/80]), followed by the L1 LSIL (58% [21/36]), the L1+ HSIL (28% [11/39]), and the L1+ LSIL (22% [7/32]) groups. Table 1 Results of 211 Initially Recruited Cases by L1 Staining Result, LSIL/HSIL Grouping, and Age * LSIL HSIL Total L1 36 (30.3) 83 (69.7) 119 (56.4) Mean age (y) L1+ 42 (46) 50 (54) 92 (43.6) Mean age (y) Total 78 (37.0) 133 (63.0) 211 Mean age (y) HSIL, high-grade squamous intraepithelial lesion; LSIL, low-grade squamous intraepithelial lesion. * Data are given as number (percentage) unless otherwise indicated. A B Image 1 L1 capsid protein positive cases with strong nuclear staining. A, High-grade squamous intraepithelial lesion (moderate dysplasia) in a routinely performed Papanicolaou smear, overstained with Cytoactiv ( 400). B, Low-grade squamous intraepithelial lesion on a ThinPrep slide ( 400). 842 Am J Clin Pathol 2009;132: Downloaded 842 from
4 Anatomic Pathology / Original Article Table 2 Clinical Outcome of 187 High-Risk HPV+ Early Dysplastic Lesions by L1 Status and LSIL/HSIL * L1+ L1 Total LSIL HSIL Total LSIL HSIL Remission 43 (61) 21 (66) 22 (56) 6 (5.2) 4 (11) 2 (3) Persistence 10 (14) 4 (13) 6 (15) 26 (22.4) 11 (31) 15 (19) Progression 18 (25) 7 (22) 11 (28) 84 (72.4) 21 (58) 63 (79) Total No HPV, human papillomavirus; HSIL, high-grade squamous intraepithelial lesion; LSIL, low-grade squamous intraepithelial lesion. * Data are given as number (percentage) unless otherwise indicated. The L1 HSIL cases had a 2.8 times higher risk of progression than the L1+ HSIL cases and L1 LSIL cases a 2.6 times increased risk compared with L1+ LSIL. Within the 71 L1+ cases, only 18 (25%) progressed to CIN 3, and 10 lesions (14%; 2 CIN 1, 6 CIN 2, and 2 with cytologically persistent moderate dysplasia) were classified as stable disease. In detail, 22% of L1+ LSIL cases (7/32) and 28% of the L1+ HSIL cases (11/39) progressed. Of the 32 L1+ LSIL cases, 4 (13%; 2 CIN 1 and 2 CIN 2) were stable disease. Of the 39 L1+ HSIL cases, 6 (15%; 4 CIN 2 and 2 cytologically with persistent dysplasia) were stable disease. Of the 116 L1 cases, 84 were histologically CIN 3+ (72.4%), qualifying for progression, and 26 (22.4%; 10 CIN 1, 14 CIN 2, and 2 cytologically) were classified as stable disease. Of 36 L1 LSIL cases, 21 (58%) progressed to CIN 3, as did 63 (79%) of the 80 L1 HSIL cases. Of the 36 L1 LSIL cases, 11 (31%; 5 CIN 1, 5 CIN 2, and 1 cytologically LSIL) were confirmed as stable disease. Of the 80 L1 HSIL cases, 15 (19%) were confirmed as stable disease (5 CIN 1, 9 CIN 2, and 1 cytologically as moderate dysplasia). The difference in clinical outcome for the L1 cases and the L1+ cases was highly statistically significant (P <.0001) and independent of the classification of LSIL (mild dysplasia) and HSIL (moderate dysplasia). Analysis of the age-related clinical outcome of the women showed no statistically significant difference related to age younger than 30 years or 30 years and older. The mean duration from the initial L1 positively stained smear to the recognition of disease progression and to remission was 8.5 months (range, 1-13 months) and 7 months (range, 3-35 months), respectively Table 3. For L1 cases, the interval until progression was 6 months (range, 1-29 months) and was 6.4 months (range, 2-12 months) for remission. Discussion Prophylactic HPV vaccines using virus-like particles of the L1 capsid protein as the antigen are highly effective in preventing HPV-associated diseases. Among nonvaccinated and, possibly, vaccinated women (except for HPV types 16 and 18), high-risk HPVs as facultative but not obligatory pathogens are quite commonly detected. But owing to the low transformation capacity, progressive disease to cervical cancer occurs in only a minor fraction of infected people. This may be the reason that other markers seeking cellular transformation events have thus far failed to predict the outcome of nonadvanced dysplastic lesions. On the other hand, the presence of infiltrating T lymphocytes and macrophages in spontaneously regressing papillomas 22 and the increased incidence and progression of HPV infections in immunosuppressed patients emphasize the critical importance of cell-mediated immune responses in the resolution and control of HPV infections. 16,23 Therefore, we focused on one of the major HPV-associated stimuli of the immune system, the L1 capsid protein. Table 3 Time Until Remission or Progression * L1 L1+ Overall LSIL HSIL Overall LSIL HSIL Remission 6.4 (2-12) 7.5 (3-12) 2 7 (3-35) 6.5 (3-18) 9 (3-35) Progression 6 (1-29) 6 (1-29) 6 (1-20) 8.5 (1-13) 9 (6-13) 8 (1-13) HSIL, high-grade squamous intraepithelial lesion; LSIL, low-grade squamous intraepithelial lesion. * Data are given as mean (range) in months. Downloaded from Am J Clin Pathol 2009;132:
5 Griesser et al / Predictive Value of HPV Protein L1 Earlier studies 17,19 have shown that the immunochemical evaluation of HPV L1 status at presentation is valuable for predicting the outcome of early dysplastic lesions. HPV has developed several mechanisms to evade the innate immune response and delay the activation of the adaptive immune response. Despite its ability to impede host defense mechanisms, a successful immune response to genital HPV infection is established in almost all cases. But viral clearance can be delayed considerably because the HPV life cycle does not induce keratinocyte death and, especially in high-risk HPV infection, does not result in major proinflammatory signals. Hence, the time required for clearance of high-risk types, particularly HPV-16, averages 8 to 14 months, which is considerably longer than the 5 to 6 months needed for clearance of low-risk types. 24 Consequently, one could envision that in this setting an efficient transfer of antigen from HPV-infected keratinocytes to the antigen presenting cells (APCs) is not triggered. The only fully accessible antigen sources in the earlier stage of virally induced SIL are free viral particles consisting of 360 L1 capsid proteins released from the L1 capsid protein positive apical layers of keratinocytes during the productive phase at the end of the natural viral life cycle in HPV infection. To generate an effective virus-specific immune response, the virus particles have to be detected by the APCs of squamous epithelium, the Langerhans cells, or dendritic cells, which can be promoted by microlesions in the epithelial transformation zone. The activated APCs then migrate to the draining lymph node, process HPV antigens en route, and present these to naive T cells in the lymphatic tissue. The T cells should then differentiate into armed effector cells, migrate back to the site of infection, and destroy the infected keratinocytes, leading to a (spontaneous) remission of the lesion. 16 When such immunologic activation mechanisms are functional, they may be quite effective, since we found a remission of the lesion in about 61% of the cases within a period of 7 to 9 months, irrespective of the dysplasia being cytologically mild or moderate. That this process is not failsafe is evident in our finding that 25% of the L1+ cases in our study showed early progression to CIN 3 within 8.5 months, compared with 6 months for L1 cases. A block at any stage of the activation cascade, such as no or diminished antigen release, reduced numbers of APCs, or MHC incompatibility or deficiencies, may result in an ineffective immune response and failure to clear HPV, propagating a progression of the intraepithelial lesion. The short interval from detection of LSIL to the diagnosis of a CIN 3 lesion could also indicate that multiple dysplastic lesions and dysplasias of different grade coexist in the transformation zone, possibly reflecting a mixture of L1+ and L1 lesions with different progressive potentials. Looking for coexisting CIN 1/CIN 3 lesions, Negri et al 20 reported that about 70% (68.4%) of these CIN 1 lesions were already L1. It seems that this loss of L1 capsid protein synthesis is an early precancerous event, and CIN 3 lesions may evolve out of such L1 CIN 1 lesions. Since the capsid protein negative, L1 messenger RNA positive murine C3 cells can be destroyed by an L1-specific T-cell response, a beneficial effect of the presence of L1 capsid protein for the immune response could be postulated, even in coexisting L1 capsid protein negative dysplastic areas. Among the L1 cases in our study, this was an extremely rare event, with 5.2% of cases showing remission of the lesion. Reasons for the remission of these L1 cases are most likely expression levels below the detection limit of the immunochemical assay or a sampling error, with absence of L1-expressing cells in the sample. Persistence or progression of dysplasia was observed in 94.8% of the L1 cases, further emphasizing the importance of the HPV L1 capsid protein as major stimulus for the activation of the immune system and the clearance of dysplasia. The rapid progression of mild and moderate dysplasias to CIN 3 lesions within 6 months seems to support the notion that disease progression can be linked to a local immune system failure. L1, nonproductive HPV infection, as a precancerous event, eventually may lead to disturbed viral-cellular interaction, resulting in disorders of cell cycle regulation at transcriptional, translational, and genomic levels Taken together, the data from our prospective study confirmed our previously published findings using retrospective approaches and provide further evidence that immunochemical L1 capsid protein detection in situ is a highly useful prognostic tool in predicting the outcome of early dysplastic lesions, particularly LSIL and moderate dysplastic lesions, providing a better risk assessment than the detection of highrisk HPV DNA. We would like to emphasize that no significant prognostic difference between cytologically mild (LSIL) and moderate dysplastic lesions (part of the HSIL category) related to the L1 expression profile was evident in our study. Therefore, prognostic significance of immunochemical L1 detection can be postulated also for borderline lesions such as high-risk HPV+ ASC-US and SIL of undetermined grade or even moderate dysplasia as part of HSIL and the equivalent of CIN 2 biopsied lesions. L1+ mild and moderate dysplastic lesions, reflecting productive HPV infection, have a low risk of progression. L1 mild to moderate dysplastic lesions, as nonproductive infections or precancerous lesions, have a high progression potential, as high as expected for severe dysplasia and squamous carcinoma in situ. Close follow-up with colposcopy and histologic verification, therefore, should be advised for high-risk HPV+, L1 cases. Independent of the cytologic classifications used so far, we suggest determining the progressive potential of the 844 Am J Clin Pathol 2009;132: Downloaded 844 from
6 Anatomic Pathology / Original Article dysplastic lesions with an HPV L1 screening antibody and classifying L1 capsid protein positive cases as lesions with low malignant potential and L1, high-risk HPV+ cases as lesions with high malignant potential. From the 1 Center of Pathology and Cytodiagnostics, Cologne, Germany; 2 Cytology Laboratory Einbeck, Einbeck, Germany; and 3 Cytoimmun Diagnostics, Pirmasens, Germany. Address reprint requests to Dr Hilfrich: Cytoimmun Diagnostics, Delaware Avenue 1-3, Pirmasens, Germany. Dr Hilfrich is chief scientific officer of Cytoimmun Diagnostics, Pirmasens, Germany. References 1. Ferlay J, Bray F, Pisani P, et al. GLOBOCAN 2002: cancer incidence, mortality and prevalence worldwide. IARC CancerBase No. 5, Version 2.0. Lyon, France: IARC Press; Parkin DM, Bray FL, Devesa SS. Cancer burden in the year 2000: the global picture. Eur J Cancer. 2001;37: Becker N. Epidemiologic aspects of cancer screening in Germany. J Cancer Res Clin Oncol. 2003;129: Kurman RJ, Henson DE, Herbst AL, et al. Interim guidelines for management of abnormal cervical cytology. JAMA. 1994;271: Nucci MR, Castrillon DH, Bai H, et al. Biomarkers in diagnostic obstetrics and gynaecological pathology: a review. Adv Anat Pathol. 2003;10: The Atypical Squamous Cells of Undetermined Significance/ Low-Grade Squamous Intraepithelial Lesions Triage Study (ALTS) Group. Human papillomavirus testing for triage of women with cytological evidence of low-grade squamous intraepithelial lesions: baseline data from a randomized trial. J Natl Cancer Inst. 2000;92: Castle PE, Stoler MH, Solomon D, et al; for the ALTS Group. The relationship of community biopsy-diagnosed cervical intraepithelial neoplasia grade 2 to the quality control reviewed diagnosis: an ALTS report. Am J Clin Pathol. 2007;127: Riotton G, Christopherson WM, Lunt R. Cytology of the Female Genital Tract. Geneva, Switzerland: World Health Organization; International Histological Classification of Tumours; No Solomon D, Nayar R. The Bethesda System for Reporting Cervical Cytology. Definitions, Criteria and Explanatory Notes. New York, NY: Springer Verlag; Wagner D. Munich nomenclature II for gynaecologic cytodiagnosis. Acta Cytol. 1990;34: Cantor SB, Atkinson EN, Cardenas-Turanzas M, et al. Natural history of cervical intraepithelial neoplasia. Acta Cytol. 2005;49: Ostör A. Natural history of cervical intraepithelial neoplasia: a critical review. Int J Gynecol Pathol. 1993;12: zur Hausen H. Papillomaviruses and cancer: from basic studies to clinical application. Nat Rev Cancer. 2002;2: Munoz N, Bosch FX, de Sanjose S, et al. Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med. 2003;348: Melsheimer P, Kaul S, Dobeck S, et al. Immunocytochemical detection of human papillomavirus high risk type L1 capsid proteins in LSIL and HSIL as compared with detection of HPV L1 DNA. Acta Cytol. 2003;47: Stanley M. Immune response to human papillomavirus. Vaccine. 2006;24(suppl 1):S16-S Griesser H, Sander H, Hilfrich R, et al. Correlation of immunochemical detection of HPV L1 capsid protein in Pap smears with regression of high risk HPV positive mild/ moderate dysplasia. Anal Quant Cytol Histol. 2004;26: Rauber D, Mehlhorn G, Fasching PA, et al. Prognostic significance of the detection of the human papillomavirus L1 protein in smears of mild to moderate cervical intraepithelial lesions. Eur J Obstet Gynecol Reprod Biol. 2008;140: Hilfrich R, Hariri J. Prognostic relevance of HPV L1 capsid protein detection within mild to moderate dysplastic lesions of the cervix uteri in combination with a second biomarker p16. Anal Quant Cytol Histol. 2008;30: Negri G, Bellisano G, Zannoni GF, et al. p16 ink4a and HPV L1 immunohistochemistry is helpful for estimating the behavior of low-grade dysplastic lesions of the cervix uteri. Am J Surg Pathol. 2008;32: Voojis PG, van Aspert-van Erp AJM, Bulten J. Benign proliferative reactions, intraepithelial neoplasia, and invasive cancer of the uterine cervix. In: Bibbo M, Wilbur DC, eds. Comprehensive Cytopathology. 3rd ed. Philadelphia, PA: Saunders; 2008: Coleman N, Birley HD, Renton AM, et al. Immunological events in regressing genital warts. Am J Clin Pathol. 1994;102: Benton C, Shahidullah H, Hunter JAA. Human papillomavirus in the immunosuppressed. Papillomavirus Rep. 1992;3: Franco EL, Villa LL, Sobrinho JP, et al. Epidemiology of acquisition and clearance of cervical human papillomavirus infection in women from a high-risk area for cervical cancer. J Infect Dis. 1999;180: Choo KB, Lee HH, Pan CC, et al. Sequence duplication and internal deletion in the integrated human papillomavirus type 16 genome from cervical carcinoma. J Virol. 1998;62: Icenogle JP, Clancy KA, Lin SY. Sequence variation in the capsid protein genes of human papillomavirus type 16 and type 31. Virology. 1995;214: Yang R, Wheeler CM, Chen X, et al. Papillomavirus capsid mutation to escape dendritic cell dependent innate immunity in cervical cancer. J Virol. 2005;79: Downloaded from Am J Clin Pathol 2009;132:
Prognostic relevance of HPV L1 capsid. protein detection within mild and. moderate dysplastic lesions of the cervix
 Prognostic relevance of HPV L1 capsid protein detection within mild and moderate dysplastic lesions of the cervix uteri in combination with a second biomarker p16. Ralf Hilfrich, PhD, a ; Jalil Hariri,
Prognostic relevance of HPV L1 capsid protein detection within mild and moderate dysplastic lesions of the cervix uteri in combination with a second biomarker p16. Ralf Hilfrich, PhD, a ; Jalil Hariri,
HPV L1 capsid protein detection in high-risk human papillomavirus-positive cervical smears
 HPV L1 capsid protein detection in high-risk human papillomavirus-positive cervical smears Abstract Heunis N, BTech(MedTech), MT(HPCSA), SHP, SCY.CT(IAC), Laboratory Supervisor and Extraordinary Lecturer
HPV L1 capsid protein detection in high-risk human papillomavirus-positive cervical smears Abstract Heunis N, BTech(MedTech), MT(HPCSA), SHP, SCY.CT(IAC), Laboratory Supervisor and Extraordinary Lecturer
chapter 4. The effect of oncogenic HPV on transformation zone epithelium
 chapter 4. The effect of oncogenic HPV on transformation zone epithelium CHAPTER 1 All squamous cervical cancer (and probably all cervical adenocarcinoma) is associated with oncogenic HPV, and the absence
chapter 4. The effect of oncogenic HPV on transformation zone epithelium CHAPTER 1 All squamous cervical cancer (and probably all cervical adenocarcinoma) is associated with oncogenic HPV, and the absence
Human Papillomavirus
 Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
The Korean Journal of Cytopathology 13(1): 14-20, 2002
 13 1 The Korean Journal of Cytopathology 13(1): 14-20, 2002 : ASCUS 1941 Papanicolaou. The Bethesda System(TBS) 1) 1988, atypical squamous cells of undetermined significance(ascus), low-grade squamous
13 1 The Korean Journal of Cytopathology 13(1): 14-20, 2002 : ASCUS 1941 Papanicolaou. The Bethesda System(TBS) 1) 1988, atypical squamous cells of undetermined significance(ascus), low-grade squamous
HPV Testing & Cervical Cancer Screening:
 HPV Testing & Cervical Cancer Screening: Are they linked? By William Chapman, MD, FRCPC Screening for precursor lesions of cervical cancer by the Papanicolaou (Pap) smear has been one of the greatest success
HPV Testing & Cervical Cancer Screening: Are they linked? By William Chapman, MD, FRCPC Screening for precursor lesions of cervical cancer by the Papanicolaou (Pap) smear has been one of the greatest success
Biomed Environ Sci, 2015; 28(1): 80-84
 80 Biomed Environ Sci, 2015; 28(1): 80-84 Letter to the Editor Assessing the Effectiveness of a Cervical Cancer Screening Program in a Hospital-based Study* YANG Yi1, LANG Jing He1, WANG You Fang1, CHENG
80 Biomed Environ Sci, 2015; 28(1): 80-84 Letter to the Editor Assessing the Effectiveness of a Cervical Cancer Screening Program in a Hospital-based Study* YANG Yi1, LANG Jing He1, WANG You Fang1, CHENG
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines
 Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Detecting High-Grade Cervical Disease on ASC-H Cytology. Role of BD ProEx C and Digene Hybrid Capture II HPV DNA Testing
 Anatomic Pathology / BD ProEx C Use in ASC-H Cy t o l o g y Detecting High-Grade Cervical Disease on ASC-H Cytology Role of BD ProEx C and Digene Hybrid Capture II HPV DNA Testing Momin T. Siddiqui, MD,
Anatomic Pathology / BD ProEx C Use in ASC-H Cy t o l o g y Detecting High-Grade Cervical Disease on ASC-H Cytology Role of BD ProEx C and Digene Hybrid Capture II HPV DNA Testing Momin T. Siddiqui, MD,
HPV and Lower Genital Tract Disease. Simon Herrington University of Edinburgh, UK Royal Infirmary of Edinburgh, UK
 HPV and Lower Genital Tract Disease Simon Herrington University of Edinburgh, UK Royal Infirmary of Edinburgh, UK Conflict of interest/funding X None Company: Product royalties Paid consultant Research
HPV and Lower Genital Tract Disease Simon Herrington University of Edinburgh, UK Royal Infirmary of Edinburgh, UK Conflict of interest/funding X None Company: Product royalties Paid consultant Research
Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches.
 Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches. Fadi W. Abdul-Karim MD MEd. Professor of Pathology. Vice chair for education. Robert Tomsich Pathology and Lab Med
Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches. Fadi W. Abdul-Karim MD MEd. Professor of Pathology. Vice chair for education. Robert Tomsich Pathology and Lab Med
Clinicopathological Implications of Human Papilloma Virus (HPV) L1 Capsid Protein Immunoreactivity in HPV16-Positive Cervical Cytology
 Research Paper Ivyspring International Publisher International Journal of Medical Sciences 2014; 11(1):80-86. doi: 10.7150/ijms.5585 80 Clinicopathological Implications of Human Papilloma Virus (HPV) L1
Research Paper Ivyspring International Publisher International Journal of Medical Sciences 2014; 11(1):80-86. doi: 10.7150/ijms.5585 80 Clinicopathological Implications of Human Papilloma Virus (HPV) L1
PAP SMEAR by Dr.Shantha Krishnamurthy MD Senior Consultant Pathology Fortis Hospitals
 PAP SMEAR by Dr.Shantha Krishnamurthy MD Senior Consultant Pathology Fortis Hospitals Historical Named after George Papanicolaou, a Greek American Studied cervical epithelium in menstrual cycle of guinea
PAP SMEAR by Dr.Shantha Krishnamurthy MD Senior Consultant Pathology Fortis Hospitals Historical Named after George Papanicolaou, a Greek American Studied cervical epithelium in menstrual cycle of guinea
Understanding Your Pap Test Results
 Understanding Your Pap Test Results Most laboratories in the United States use a standard set of terms called the Bethesda System to report pap test results. Normal: Pap samples that have no cell abnormalities
Understanding Your Pap Test Results Most laboratories in the United States use a standard set of terms called the Bethesda System to report pap test results. Normal: Pap samples that have no cell abnormalities
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two
 Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
The Biology of HPV Infection and Cervical Cancer
 The Biology of HPV Infection and Cervical Cancer Kaitlin Sundling, M.D., Ph.D. Clinical Instructor Faculty Director, Cytotechnology Program Wisconsin State Laboratory of Hygiene and University of Wisconsin
The Biology of HPV Infection and Cervical Cancer Kaitlin Sundling, M.D., Ph.D. Clinical Instructor Faculty Director, Cytotechnology Program Wisconsin State Laboratory of Hygiene and University of Wisconsin
Cervical Dysplasia and HPV
 Cervical Dysplasia and HPV J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse HPV Double stranded DNA virus The HPV infect epithelial cells of the skin and mucous membranes Highest risk
Cervical Dysplasia and HPV J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse HPV Double stranded DNA virus The HPV infect epithelial cells of the skin and mucous membranes Highest risk
Update on HPV Testing. Robert Schlaberg, M.D., Dr. med., M.P.H. Assistant Professor, University of Utah Medical Director, ARUP Laboratories
 Update on HPV Testing Robert Schlaberg, M.D., Dr. med., M.P.H. Assistant Professor, University of Utah Medical Director, ARUP Laboratories Disclosures In accordance with ACCME guidelines, any individual
Update on HPV Testing Robert Schlaberg, M.D., Dr. med., M.P.H. Assistant Professor, University of Utah Medical Director, ARUP Laboratories Disclosures In accordance with ACCME guidelines, any individual
Table of Contents. 1. Overview. 2. Interpretation Guide. 3. Staining Gallery Cases Negative for CINtec PLUS
 Staining Atlas Table of Contents 1. Overview 1.1 Introduction 1.2 Role of p16 INK4a 1.3 Role of Ki-67 1.4 Molecular Pathogenesis 1.5 p16 INK4a Expression in Cervical Dysplasia 1.6 The Concept of CINtec
Staining Atlas Table of Contents 1. Overview 1.1 Introduction 1.2 Role of p16 INK4a 1.3 Role of Ki-67 1.4 Molecular Pathogenesis 1.5 p16 INK4a Expression in Cervical Dysplasia 1.6 The Concept of CINtec
Welcome. THE ROLE OF oncofish cervical ASSESSMENT OF CERVICAL DYSPLASIA. March 26, 2013
 THE ROLE OF oncofish cervical IN THE ASSESSMENT OF CERVICAL DYSPLASIA The phone lines will open, 15 minutes prior to the start of the webinar. Toll Free: 1-800-867-0864. Entry Code: 83956484. You may download
THE ROLE OF oncofish cervical IN THE ASSESSMENT OF CERVICAL DYSPLASIA The phone lines will open, 15 minutes prior to the start of the webinar. Toll Free: 1-800-867-0864. Entry Code: 83956484. You may download
Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines. June 2013
 Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines General Principles: Since its introduction in 1943, Papanicolaou (Pap) smear is widely
Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines General Principles: Since its introduction in 1943, Papanicolaou (Pap) smear is widely
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Garland SM, Hernandez-Avila M, Wheeler CM, et al. Quadrivalent
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Garland SM, Hernandez-Avila M, Wheeler CM, et al. Quadrivalent
Human Papillomaviruses and Cancer: Questions and Answers. Key Points. 1. What are human papillomaviruses, and how are they transmitted?
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Human Papillomaviruses
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Human Papillomaviruses
Should Anal Pap Smears Be a Standard of Care in HIV Management?
 Should Anal Pap Smears Be a Standard of Care in HIV Management? Gordon Dickinson, M.D., FACP Professor of Medicine and Chief Infectious Diseases, Miller School of Medicine Short Answer: NO But 15-20 HPV
Should Anal Pap Smears Be a Standard of Care in HIV Management? Gordon Dickinson, M.D., FACP Professor of Medicine and Chief Infectious Diseases, Miller School of Medicine Short Answer: NO But 15-20 HPV
Focus. International #52. HPV infection in High-risk HPV and cervical cancer. HPV: Clinical aspects. Natural history of HPV infection
 HPV infection in 2014 Papillomaviruses (HPV) are non-cultivable viruses with circular DNA. They can establish productive infections in the skin (warts) and in mucous membranes (genitals, larynx, etc.).
HPV infection in 2014 Papillomaviruses (HPV) are non-cultivable viruses with circular DNA. They can establish productive infections in the skin (warts) and in mucous membranes (genitals, larynx, etc.).
Study of Cervical Pap Smears in a Tertiary Hospital
 250 Original Study Study of Cervical Pap Smears in a Tertiary Hospital Sunita A. Bamanikar, Professor, Department of Pathology, Dadaso S. Baravkar, Resident Pathologist, Department of Pathology, Shirish
250 Original Study Study of Cervical Pap Smears in a Tertiary Hospital Sunita A. Bamanikar, Professor, Department of Pathology, Dadaso S. Baravkar, Resident Pathologist, Department of Pathology, Shirish
HUMAN PAPILLOMAVIRUS TESTING
 CLINICAL GUIDELINES For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS HUMAN PAPILLOMAVIRUS TESTING Policy Number: PDS - 016 Effective Date: October 1, 2018
CLINICAL GUIDELINES For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS HUMAN PAPILLOMAVIRUS TESTING Policy Number: PDS - 016 Effective Date: October 1, 2018
P16 et Ki67 Biomarkers: new tool for risk management and low grade intraepithelial lesions (LGSIL): be ready for the future.
 P16 et Ki67 Biomarkers: new tool for risk management and low grade intraepithelial lesions (LGSIL): be ready for the future. Mark H Stoler, MD University of Virginia Health System, Charlottesville, VA,
P16 et Ki67 Biomarkers: new tool for risk management and low grade intraepithelial lesions (LGSIL): be ready for the future. Mark H Stoler, MD University of Virginia Health System, Charlottesville, VA,
Colposcopy. Attila L Major, MD, PhD
 Colposcopy Attila L Major, MD, PhD Histology Colposcopy Cytology It has been estimated that annual Pap smear testing reduces a woman s chance of dying of cervical cancer from 4 in 1000 to about 5 in 10,000
Colposcopy Attila L Major, MD, PhD Histology Colposcopy Cytology It has been estimated that annual Pap smear testing reduces a woman s chance of dying of cervical cancer from 4 in 1000 to about 5 in 10,000
Pathology of the Cervix
 Pathology of the Cervix Thomas C. Wright Pathology of the Cervix Topics to Consider Burden of cervical cancer 1 Invasive Cervical Cancer Cervical cancer in world Second cause of cancer death in women Leading
Pathology of the Cervix Thomas C. Wright Pathology of the Cervix Topics to Consider Burden of cervical cancer 1 Invasive Cervical Cancer Cervical cancer in world Second cause of cancer death in women Leading
I have no financial interests in any product I will discuss today.
 Cervical Cancer Prevention: 2012 and Beyond George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics University of California,
Cervical Cancer Prevention: 2012 and Beyond George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics University of California,
He Said, She Said: HPV and the FDA. Audrey P Garrett, MD, MPH June 6, 2014
 He Said, She Said: HPV and the FDA Audrey P Garrett, MD, MPH June 6, 2014 Disclosure Speaker for Merck Gardasil Speaker for Hologic Thin Prep and Cervista Cervical Cancer Screening: 21 st century Dr. Papanicolaou
He Said, She Said: HPV and the FDA Audrey P Garrett, MD, MPH June 6, 2014 Disclosure Speaker for Merck Gardasil Speaker for Hologic Thin Prep and Cervista Cervical Cancer Screening: 21 st century Dr. Papanicolaou
News. Laboratory NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING TIMOTHY UPHOFF, PHD, DABMG, MLS (ASCP) CM
 Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Utilization of the Biomarkers to Improve Cervical Cancer Screening
 Utilization of the Biomarkers to Improve Cervical Cancer Screening Elena BERNAD Victor Babes University of Medicine and Pharmacy Timisoara, Romania Cervical cancer is at the second most common cancer in
Utilization of the Biomarkers to Improve Cervical Cancer Screening Elena BERNAD Victor Babes University of Medicine and Pharmacy Timisoara, Romania Cervical cancer is at the second most common cancer in
Making Sense of Cervical Cancer Screening
 Making Sense of Cervical Cancer Screening New Guidelines published November 2012 Tammie Koehler DO, FACOG The incidence of cervical cancer in the US has decreased more than 50% in the past 30 years because
Making Sense of Cervical Cancer Screening New Guidelines published November 2012 Tammie Koehler DO, FACOG The incidence of cervical cancer in the US has decreased more than 50% in the past 30 years because
HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests
 HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests Lee P. Shulman MD The Anna Ross Lapham Professor in Obstetrics and Gynecology and Chief, Division of Clinical Genetics Feinberg School
HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests Lee P. Shulman MD The Anna Ross Lapham Professor in Obstetrics and Gynecology and Chief, Division of Clinical Genetics Feinberg School
Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation?
 Anatomic Pathology / Monitoring HPV-16 Fractions in CIN Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation? Mary T. Galgano, MD, 1 Philip E. Castle, PhD, MPH, 2 Mark
Anatomic Pathology / Monitoring HPV-16 Fractions in CIN Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation? Mary T. Galgano, MD, 1 Philip E. Castle, PhD, MPH, 2 Mark
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma
 Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
HIV-infected men and women. Joel Palefsky, M.D. University of California, San Francisco
 Anal cytology and anal cancer in HIV-infected men and women. Joel Palefsky, M.D. University of California, San Francisco April 10, 2010 Disclosures Merck and Co: Research grant support, advisory boards
Anal cytology and anal cancer in HIV-infected men and women. Joel Palefsky, M.D. University of California, San Francisco April 10, 2010 Disclosures Merck and Co: Research grant support, advisory boards
STUDY OF EARLY DETECTION OF CERVICAL CANCER BY PAP S SMEAR IN SELECTED SETTING OF PUDUCHERRY
 STUDY OF EARLY DETECTION OF CERVICAL CANCER BY PAP S SMEAR IN SELECTED SETTING OF PUDUCHERRY *Thirumurugan. P, **Premila. E, ***Suresh Kanna. K *Associate Professor, Mother Theresa Post Graduate and Research
STUDY OF EARLY DETECTION OF CERVICAL CANCER BY PAP S SMEAR IN SELECTED SETTING OF PUDUCHERRY *Thirumurugan. P, **Premila. E, ***Suresh Kanna. K *Associate Professor, Mother Theresa Post Graduate and Research
TISSUE TUMOR MARKER EXPRESSION IN
 TISSUE TUMOR MARKER EXPRESSION IN NORMAL CERVICAL TISSUE AND IN CERVICAL INTRAEPITHELIAL NEOPLASIA, FOR WOMEN WHO ARE AT HIGH RISK OF HPV (HUMAN PAPILLOMA VIRUS INFECTION). Raghad Samir MD PhD Verksamhet
TISSUE TUMOR MARKER EXPRESSION IN NORMAL CERVICAL TISSUE AND IN CERVICAL INTRAEPITHELIAL NEOPLASIA, FOR WOMEN WHO ARE AT HIGH RISK OF HPV (HUMAN PAPILLOMA VIRUS INFECTION). Raghad Samir MD PhD Verksamhet
Study Number: Title: Rationale: Phase: Study Period Study Design: Centres: Indication Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Vasile Goldiş Western University of Arad, Faculty of Medicine, Obstetrics- Gynecology Department, Romania b
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Cervical Intraepithelial Neoplasia in the Dr. Salvator Vuia Clinical Obstetrics and Gynecology Hospital - Arad During the 2000-2009 Period Voicu
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Cervical Intraepithelial Neoplasia in the Dr. Salvator Vuia Clinical Obstetrics and Gynecology Hospital - Arad During the 2000-2009 Period Voicu
Performance of the Aptima High-Risk Human Papillomavirus mrna Assay in a Referral Population in Comparison with Hybrid Capture 2 and Cytology
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1071 1076 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.01674-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Performance
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1071 1076 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.01674-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Performance
Histopathology: Cervical HPV and neoplasia
 Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
Human Papillomavirus. Kathryn Thiessen, ARNP, ACRN The Kansas AIDS Education and Training Center The University of Kansas School of Medicine Wichita
 Human Papillomavirus Kathryn Thiessen, ARNP, ACRN The Kansas AIDS Education and Training Center The University of Kansas School of Medicine Wichita What is Genital HPV Infection Human papillomavirus is
Human Papillomavirus Kathryn Thiessen, ARNP, ACRN The Kansas AIDS Education and Training Center The University of Kansas School of Medicine Wichita What is Genital HPV Infection Human papillomavirus is
Cervical Cancer Screening. David Quinlan December 2013
 Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
Original Policy Date
 MP 2.04.03 Cervicography Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index Disclaimer
MP 2.04.03 Cervicography Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index Disclaimer
Cervical FISH Testing for Triage and Support of Challenging Diagnoses: A Case Study of 2 Patients
 Cervical FISH Testing for Triage and Support of Challenging Diagnoses: A Case Study of 2 Patients Richard Hopley, MD, Alexandra Gillespie, MD* Laboratory Medicine 47:1:52-56 CLINICAL HISTORY Patients:
Cervical FISH Testing for Triage and Support of Challenging Diagnoses: A Case Study of 2 Patients Richard Hopley, MD, Alexandra Gillespie, MD* Laboratory Medicine 47:1:52-56 CLINICAL HISTORY Patients:
New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology
 New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology United States and Canadian Academy of Pathology 102 nd Annual Meeting Baltimore, Maryland Christina S. Kong, M.D.
New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology United States and Canadian Academy of Pathology 102 nd Annual Meeting Baltimore, Maryland Christina S. Kong, M.D.
Long-Term Outcome and Relative Risk in Women With Atypical Squamous Cells of Undetermined Significance
 Anatomic Pathology / LONG-TERM OUTCOME WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Long-Term Outcome and Relative Risk in Women With Atypical Squamous Cells of Undetermined Significance Stephen
Anatomic Pathology / LONG-TERM OUTCOME WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Long-Term Outcome and Relative Risk in Women With Atypical Squamous Cells of Undetermined Significance Stephen
The Korean Journal of Cytopathology 15 (1) : 17-27, 2004
 5 The Korean Journal of Cytopathology 5 () : 7-7, / 5 / / (human papillomavirus, HPV), 6%, 5% HPV. HPV HPV. HPV HPV,,5 HPV HPV. HPV, 6 HPV. HPV HPV International Agency for Research on Cancer (IARC) HPV
5 The Korean Journal of Cytopathology 5 () : 7-7, / 5 / / (human papillomavirus, HPV), 6%, 5% HPV. HPV HPV. HPV HPV,,5 HPV HPV. HPV, 6 HPV. HPV HPV International Agency for Research on Cancer (IARC) HPV
No HPV High Risk Screening with Genotyping. CPT Code: If Result is NOT DETECTED (x3) If Results is DETECTED (Genotype reported)
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 117 August 6, 2013 HPV High Risk Screening with Genotyping Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Director, Molecular Pathology
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 117 August 6, 2013 HPV High Risk Screening with Genotyping Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Director, Molecular Pathology
Promoting Cervical Screening Information for Health Professionals. Cervical Cancer
 Promoting Cervical Screening Information for Health Professionals Cervical Cancer PapScreen Victoria Cancer Council Victoria 1 Rathdowne St Carlton VIC 3053 Telephone: (03) 635 5147 Fax: (03) 9635 5360
Promoting Cervical Screening Information for Health Professionals Cervical Cancer PapScreen Victoria Cancer Council Victoria 1 Rathdowne St Carlton VIC 3053 Telephone: (03) 635 5147 Fax: (03) 9635 5360
HPV AND CERVICAL CANCER
 HPV AND CERVICAL CANCER DR SANDJONG TIECHOU ISAAC DELON Postgraduate Training in Reproductive Health Research Faculty of Medicine, University of Yaoundé 2007 INTRODUCTION CERVICAL CANCER IS THE SECOND
HPV AND CERVICAL CANCER DR SANDJONG TIECHOU ISAAC DELON Postgraduate Training in Reproductive Health Research Faculty of Medicine, University of Yaoundé 2007 INTRODUCTION CERVICAL CANCER IS THE SECOND
Cancer Screening and Prevention: Eliminating Deaths from Cervical Cancer
 Cancer Screening and Prevention: Eliminating Deaths from Cervical Cancer 1 Learning Objectives Participant will understand the evolution of cervical cytology screening as well as current evidence-based
Cancer Screening and Prevention: Eliminating Deaths from Cervical Cancer 1 Learning Objectives Participant will understand the evolution of cervical cytology screening as well as current evidence-based
Evaluation of Low-Grade Squamous Intraepithelial Lesions, Cannot Exclude High-Grade Squamous Intraepithelial Lesions on Cervical Smear
 The Korean Journal of Pathology 2010; 44: 528-35 DOI: 10.4132/KoreanJPathol.2010.44.5.528 Evaluation of Low-Grade Squamous Intraepithelial Lesions, Cannot Exclude High-Grade Squamous Intraepithelial Lesions
The Korean Journal of Pathology 2010; 44: 528-35 DOI: 10.4132/KoreanJPathol.2010.44.5.528 Evaluation of Low-Grade Squamous Intraepithelial Lesions, Cannot Exclude High-Grade Squamous Intraepithelial Lesions
Objectives. I have no financial interests in any product I will discuss today. Cervical Cancer Screening Guidelines: Updates and Controversies
 Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
Cervical Precancer: Evaluation and Management
 TAJ June 2002; Volume 15 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Review fam Cervical Precancer: Evaluation and Management SM Khodeza Nahar Begum 1 Abstract Carcinoma of
TAJ June 2002; Volume 15 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Review fam Cervical Precancer: Evaluation and Management SM Khodeza Nahar Begum 1 Abstract Carcinoma of
The ABCs of TBS. A Novice's Guide to the Bethesda System
 CE U P D A T E W O M E N ' S HEALTH III Julia Woodruff Wildes, MD The ABCs of TBS A Novice's Guide to the Bethesda System This is the third and final article in a three-part series on women's health. The
CE U P D A T E W O M E N ' S HEALTH III Julia Woodruff Wildes, MD The ABCs of TBS A Novice's Guide to the Bethesda System This is the third and final article in a three-part series on women's health. The
Cervical Screening for Dysplasia and Cancer in Patients with HIV
 Cervical Screening for Dysplasia and Cancer in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute w w w.hivg uidelines.org Purpose of the Guideline Increase
Cervical Screening for Dysplasia and Cancer in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute w w w.hivg uidelines.org Purpose of the Guideline Increase
Atypical Glandular Cells of Undetermined Significance Outcome Predictions Based on Human Papillomavirus Testing
 Anatomic Pathology / ATYPICAL GLANDULAR CELLS AND HUMAN PAPILLOMAVIRUS Atypical Glandular Cells of Undetermined Significance Outcome Predictions Based on Human Papillomavirus Testing Jeffrey F. Krane,
Anatomic Pathology / ATYPICAL GLANDULAR CELLS AND HUMAN PAPILLOMAVIRUS Atypical Glandular Cells of Undetermined Significance Outcome Predictions Based on Human Papillomavirus Testing Jeffrey F. Krane,
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening
 Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Eradicating Mortality from Cervical Cancer
 Eradicating Mortality from Cervical Cancer Michelle Berlin, MD, MPH Vice Chair, Obstetrics & Gynecology Associate Director, Center for Women s Health June 2, 2009 Overview Prevention Human Papilloma Virus
Eradicating Mortality from Cervical Cancer Michelle Berlin, MD, MPH Vice Chair, Obstetrics & Gynecology Associate Director, Center for Women s Health June 2, 2009 Overview Prevention Human Papilloma Virus
HPV and Cervical Cancer, Screening and Prevention. John Ragsdale, MD July 12, 2018 CME Lecture Series
 HPV and Cervical Cancer, Screening and Prevention John Ragsdale, MD July 12, 2018 CME Lecture Series We have come a long Way Prevalence HPV in Young Adults in U.S HPV genotypes 55-60% of All cancers 20%
HPV and Cervical Cancer, Screening and Prevention John Ragsdale, MD July 12, 2018 CME Lecture Series We have come a long Way Prevalence HPV in Young Adults in U.S HPV genotypes 55-60% of All cancers 20%
SCCPS Scientific Committee Position Paper on HPV Vaccination
 SCCPS Scientific Committee Position Paper on HPV Vaccination Adapted from Joint Statement (March 2011) of the: Obstetrical & Gynaecological Society of Singapore (OGSS) Society for Colposcopy and Cervical
SCCPS Scientific Committee Position Paper on HPV Vaccination Adapted from Joint Statement (March 2011) of the: Obstetrical & Gynaecological Society of Singapore (OGSS) Society for Colposcopy and Cervical
I have no financial interests in any product I will discuss today.
 Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
Cervical Screening Results Leading to Detection of Adenocarcinoma in Situ of the Uterine Cervix
 DOI:10.31557/APJCP.2019.20.2.377 Cervical Screening Results Leading to Detecting Cervical AIS RESEARCH ARTICLE Editorial Process: Submission:09/27/2018 Acceptance:01/18/2019 Cervical Screening Results
DOI:10.31557/APJCP.2019.20.2.377 Cervical Screening Results Leading to Detecting Cervical AIS RESEARCH ARTICLE Editorial Process: Submission:09/27/2018 Acceptance:01/18/2019 Cervical Screening Results
CERVIX. MLS Basic histological diagnosis MLS HIST 422 Semester 8- batch 7 L12 : Dr. Ali Eltayb.
 CERVIX MLS Basic histological diagnosis MLS HIST 422 Semester 8- batch 7 L12 : Dr. Ali Eltayb. CERVIX Most cervical lesions are: Most are Cervicitis. cancers ( common in women worldwide). CERVICITIS Extremely
CERVIX MLS Basic histological diagnosis MLS HIST 422 Semester 8- batch 7 L12 : Dr. Ali Eltayb. CERVIX Most cervical lesions are: Most are Cervicitis. cancers ( common in women worldwide). CERVICITIS Extremely
PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE
 Arch Iranian Med 2005; 8 (3): 192 196 Original Article PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Fatemeh Ghaemmaghami MD *, Fereshteh Ensani MD**, Nadereh Behtash MD* Ebrahim
Arch Iranian Med 2005; 8 (3): 192 196 Original Article PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Fatemeh Ghaemmaghami MD *, Fereshteh Ensani MD**, Nadereh Behtash MD* Ebrahim
WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1
 WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1 HOW TO CITE THIS ARTICLE: G. J. Vani Padmaja. Well Woman Clinic-Screening Program for Cervical Carcinomas. Journal of Evolution
WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1 HOW TO CITE THIS ARTICLE: G. J. Vani Padmaja. Well Woman Clinic-Screening Program for Cervical Carcinomas. Journal of Evolution
Efficacy evaluation of a test CINtec p16ink4a in screening for cervical HPV infection
 Vol.1, No.3, 154-163 (2011) doi:10.4236/ojpm.2011.13020 Open Journal of Preventive Medicine Efficacy evaluation of a test CINtec p16ink4a in screening for cervical HPV infection Pafumi Carlo, Leanza Vito,
Vol.1, No.3, 154-163 (2011) doi:10.4236/ojpm.2011.13020 Open Journal of Preventive Medicine Efficacy evaluation of a test CINtec p16ink4a in screening for cervical HPV infection Pafumi Carlo, Leanza Vito,
A Cytologic/Histologic Review of 367 Cases. Original Article. Cancer Cytopathology August 25,
 Correlation Between Hybrid Capture II High-Risk Human Papillomavirus DNA Test Chemiluminescence Intensity From Cervical Samples With Follow-Up Histologic Results A Cytologic/Histologic Review of 367 Cases
Correlation Between Hybrid Capture II High-Risk Human Papillomavirus DNA Test Chemiluminescence Intensity From Cervical Samples With Follow-Up Histologic Results A Cytologic/Histologic Review of 367 Cases
Clinical Relevance of HPV Genotyping. A New Dimension In Human Papillomavirus Testing. w w w. a u t o g e n o m i c s. c o m
 Clinical Relevance of HPV Genotyping A New Dimension In Human Papillomavirus Testing Human Papillomavirus: Incidence HPV prevalence was 26.8% for women in US aged 14 59 yrs 1 20 million Americans are currently
Clinical Relevance of HPV Genotyping A New Dimension In Human Papillomavirus Testing Human Papillomavirus: Incidence HPV prevalence was 26.8% for women in US aged 14 59 yrs 1 20 million Americans are currently
Clinical Practice Guidelines June 2013
 Clinical Practice Guidelines June 2013 General Principles: The Papanicolaou (Pap) smear is widely credited with reducing mortality from cervical cancer, and remains the single best method for the early
Clinical Practice Guidelines June 2013 General Principles: The Papanicolaou (Pap) smear is widely credited with reducing mortality from cervical cancer, and remains the single best method for the early
PAP smear. (Papanicolaou Test)
 PAP smear (Papanicolaou Test) Is a screening test to prevent/ detect cancerous processes in endocervical canal It reduces the mortality caused by cervical cancer up to 80% M. Arbyn; et al. (2010). "European
PAP smear (Papanicolaou Test) Is a screening test to prevent/ detect cancerous processes in endocervical canal It reduces the mortality caused by cervical cancer up to 80% M. Arbyn; et al. (2010). "European
Cervical Cancer 4/27/2016
 Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical College of Wisconsin May 6, 2016 Cervical Cancer In US about
Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical College of Wisconsin May 6, 2016 Cervical Cancer In US about
1.Acute and Chronic Cervicitis - At the onset of menarche, the production of estrogens by the ovary stimulates maturation of the cervical and vaginal
 Diseases of cervix I. Inflammations 1.Acute and Chronic Cervicitis - At the onset of menarche, the production of estrogens by the ovary stimulates maturation of the cervical and vaginal squamous mucosa
Diseases of cervix I. Inflammations 1.Acute and Chronic Cervicitis - At the onset of menarche, the production of estrogens by the ovary stimulates maturation of the cervical and vaginal squamous mucosa
Cytyc Corporation - Case Presentation Archive - June 2003
 ThinPrep General Cytology History: Asymptomatic 35 Year Old Male Specimen type: Anal Cytology - This specimen was collected using a Dacron swab under proctoscopic visualization. This case was provided
ThinPrep General Cytology History: Asymptomatic 35 Year Old Male Specimen type: Anal Cytology - This specimen was collected using a Dacron swab under proctoscopic visualization. This case was provided
Outcome of Atypical Squamous Cells in Cervical Cytology: Follow-up Assessment by Loop Electrical Excision Procedure
 The Korean Journal of Pathology 2012; 46: 359-364 ORIGINAL ARTICLE Outcome of Atypical Squamous Cells in Cervical Cytology: Follow-up Assessment by Loop Electrical Excision Procedure Joon Seon Song Ilseon
The Korean Journal of Pathology 2012; 46: 359-364 ORIGINAL ARTICLE Outcome of Atypical Squamous Cells in Cervical Cytology: Follow-up Assessment by Loop Electrical Excision Procedure Joon Seon Song Ilseon
Dysplasia: layer of the cervical CIN. Intraepithelial Neoplasia. p16 immunostaining. 1, Cervical. Higher-risk, requires CIN.
 CLINICAL PRACTICE GUIDELINE Guideline Number: DHMP_DHMC_PG1015 Guideline Subject: Routine Cervical Cancer Screening Effective Date: 9/2018 Revision Date: 9/2019 Pages: 2 of 2 Quality Management Committee
CLINICAL PRACTICE GUIDELINE Guideline Number: DHMP_DHMC_PG1015 Guideline Subject: Routine Cervical Cancer Screening Effective Date: 9/2018 Revision Date: 9/2019 Pages: 2 of 2 Quality Management Committee
Update of the role of Human Papillomavirus in Head and Neck Cancer
 Update of the role of Human Papillomavirus in Head and Neck Cancer 2013 International & 12 th National Head and Neck Tumour Conference Shanghai, 11 13 Oct 2013 Prof. Paul KS Chan Department of Microbiology
Update of the role of Human Papillomavirus in Head and Neck Cancer 2013 International & 12 th National Head and Neck Tumour Conference Shanghai, 11 13 Oct 2013 Prof. Paul KS Chan Department of Microbiology
Cervical Testing and Results Management. An Evidenced-Based Approach April 22nd, Debora Bear, MSN, MPH
 Cervical Testing and Results Management An Evidenced-Based Approach April 22nd, 2010 Debora Bear, MSN, MPH Assistant Medical Director for Planned Parenthood of New Mexico, Inc. Burden of cervical cancer
Cervical Testing and Results Management An Evidenced-Based Approach April 22nd, 2010 Debora Bear, MSN, MPH Assistant Medical Director for Planned Parenthood of New Mexico, Inc. Burden of cervical cancer
Utility of Pap Smear in Cervical Screening in a Tertiary Care Hospital
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 319-323 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.039
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 319-323 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.039
ARTICLE IN PRESS. is not an effective triage test for women. women with high-grade squamous intraepithelial
 Research ONCOLOGY Amplification of the chromosome 3q26 region shows high negative predictive value for nonmalignant transformation of LSIL cytologic finding G. Reza Jalali, PhD; Thomas J. Herzog, MD; Bruce
Research ONCOLOGY Amplification of the chromosome 3q26 region shows high negative predictive value for nonmalignant transformation of LSIL cytologic finding G. Reza Jalali, PhD; Thomas J. Herzog, MD; Bruce
Woo Dae Kang, Ho Sun Choi, Seok Mo Kim
 Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
Profile Of Cervical Smears Cytology In Western Region Of Saudi Arabia
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 1 Number 2 Profile Of Cervical Smears Cytology In Western Region Of Saudi Arabia I Mansoor Citation I Mansoor. Profile Of Cervical Smears
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 1 Number 2 Profile Of Cervical Smears Cytology In Western Region Of Saudi Arabia I Mansoor Citation I Mansoor. Profile Of Cervical Smears
HPV Epidemiology and Natural History
 HPV Epidemiology and Natural History Rachel Winer, PhD, MPH Associate Professor Department of Epidemiology University of Washington School of Public Health rlw@uw.edu Human Papillomavirus (HPV) DNA virus
HPV Epidemiology and Natural History Rachel Winer, PhD, MPH Associate Professor Department of Epidemiology University of Washington School of Public Health rlw@uw.edu Human Papillomavirus (HPV) DNA virus
INTRODUCTION HUMAN PAPILLOMAVIRUS
 INTRODUCTION HUMAN PAPILLOMAVIRUS Professor Anna-Lise Williamson Institute of Infectious Disease and Molecular Medicine, University of Cape Town National Health Laboratory Service, Groote Schuur Hospital
INTRODUCTION HUMAN PAPILLOMAVIRUS Professor Anna-Lise Williamson Institute of Infectious Disease and Molecular Medicine, University of Cape Town National Health Laboratory Service, Groote Schuur Hospital
EU guidelines for reporting gynaecological cytology
 EU guidelines for reporting gynaecological cytology Amanda Herbert Guy s & St Thomas Foundation NHS Trust 5th EFCS Annual Tutorial, Trondheim, Norway 28 th May 1 st June 2012 EU guidelines aim to harmonize
EU guidelines for reporting gynaecological cytology Amanda Herbert Guy s & St Thomas Foundation NHS Trust 5th EFCS Annual Tutorial, Trondheim, Norway 28 th May 1 st June 2012 EU guidelines aim to harmonize
Altering Cervical Cancer s Trajectory. Mary S. Beattie, MD, MAS Medical Director, Women s Health BioOncology US Medical Affairs
 Altering Cervical Cancer s Trajectory Mary S. Beattie, MD, MAS Medical Director, Women s Health BioOncology US Medical Affairs Objectives and Agenda Objectives: Appreciate cervical cancer (CC) burden Understand
Altering Cervical Cancer s Trajectory Mary S. Beattie, MD, MAS Medical Director, Women s Health BioOncology US Medical Affairs Objectives and Agenda Objectives: Appreciate cervical cancer (CC) burden Understand
CINtec PLUS and the Pap smear: a co-testing alternative
 CINtec PLUS and the Pap smear: a co-testing alternative Rosemary Tambouret MD p16/ki67 (CINtec PLUS) and the Pap smear Rosemary Tambouret MD CINtec PLUS dual stain: p16 and Ki67 p16 is anti-proliferative
CINtec PLUS and the Pap smear: a co-testing alternative Rosemary Tambouret MD p16/ki67 (CINtec PLUS) and the Pap smear Rosemary Tambouret MD CINtec PLUS dual stain: p16 and Ki67 p16 is anti-proliferative
FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION
 Arch. Biol. Sci., Belgrade, 66 (4), 1653-1658, 2014 DOI:10.2298/ABS1404653M FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION IN WOMEN IN MONTENEGRO GORDANA MIJOVIĆ 1, TATJANA JOVANOVIĆ
Arch. Biol. Sci., Belgrade, 66 (4), 1653-1658, 2014 DOI:10.2298/ABS1404653M FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION IN WOMEN IN MONTENEGRO GORDANA MIJOVIĆ 1, TATJANA JOVANOVIĆ
SESSION J4. What's Next? Managing Abnormal PAPs in 2014
 37th Annual Advanced Practice in Primary and Acute Care Conference: October 9-11, 2014 2:45 SESSION J4 What's Next? Managing Abnormal PAPs in 2014 Session Description: Linda Eckert, MD Review current guidelines
37th Annual Advanced Practice in Primary and Acute Care Conference: October 9-11, 2014 2:45 SESSION J4 What's Next? Managing Abnormal PAPs in 2014 Session Description: Linda Eckert, MD Review current guidelines
Screening for Cervical Cancer: Demystifying the Guidelines DR. NEERJA SHARMA
 Screening for Cervical Cancer: Demystifying the Guidelines DR. NEERJA SHARMA Cancer Care Ontario Cervical Cancer Screening Goals Increase patient participation in cervical screening Increase primary care
Screening for Cervical Cancer: Demystifying the Guidelines DR. NEERJA SHARMA Cancer Care Ontario Cervical Cancer Screening Goals Increase patient participation in cervical screening Increase primary care
GUIDELINE FOR SCREENING FOR CERVICAL CANCER: REVISED
 GUIDELINE FOR SCREENING FOR CERVICAL CANCER: REVISED This guideline is a revised version of the guideline developed in February 2000, by the Cervical Cancer Screening Working Group. This revised version
GUIDELINE FOR SCREENING FOR CERVICAL CANCER: REVISED This guideline is a revised version of the guideline developed in February 2000, by the Cervical Cancer Screening Working Group. This revised version
Over-diagnoses in Cytopathology: Is histology the gold standard?
 Over-diagnoses in Cytopathology: Is histology the gold standard? Teresa M. Darragh, MD UCSF Departments of Pathology and Obstetrics, Gynecology & Reproductive Sciences Faculty Disclosures: Teresa M. Darragh,
Over-diagnoses in Cytopathology: Is histology the gold standard? Teresa M. Darragh, MD UCSF Departments of Pathology and Obstetrics, Gynecology & Reproductive Sciences Faculty Disclosures: Teresa M. Darragh,
Cytomorphologic Features According to HPV DNA Type in Histologically Proven Cases of the Uterine Cervix
 The Korean Journal of Pathology 2011; 45: 612-620 http://dx.doi.org/10.4132/koreanjpathol.2011.45.6.612 Cytomorphologic Features According to HPV DNA Type in Histologically Proven Cases of the Uterine
The Korean Journal of Pathology 2011; 45: 612-620 http://dx.doi.org/10.4132/koreanjpathol.2011.45.6.612 Cytomorphologic Features According to HPV DNA Type in Histologically Proven Cases of the Uterine
Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index
 DOI 10.1007/s00404-012-2569-y GYNECOLOGIC ONCOLOGY Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index Hadi Shojaei Fariba Yarandi Leila
DOI 10.1007/s00404-012-2569-y GYNECOLOGIC ONCOLOGY Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index Hadi Shojaei Fariba Yarandi Leila
A Study on Diagnostic Accuracy of Cervical Pap Smear by Correlating with Histopathology in a Tertiary Care Centre
 Original Article DOI: 10.21276/APALM.1878 A Study on Diagnostic Accuracy of Cervical Pap Smear by Correlating with Histopathology in a Tertiary Care Centre Rachana L Y, S.S. Hiremath*, Prabhu M H, S.S
Original Article DOI: 10.21276/APALM.1878 A Study on Diagnostic Accuracy of Cervical Pap Smear by Correlating with Histopathology in a Tertiary Care Centre Rachana L Y, S.S. Hiremath*, Prabhu M H, S.S
