Protocols 9-12 MMR mutation carrier guidelines Frequently asked questions
|
|
|
- Maximilian Maxwell
- 6 years ago
- Views:
Transcription
1 Protocols 9-12 MMR mutation carrier guidelines Frequently asked questions Last updated: 10/02/2015 Q: Where have the general population cancer risks been taken from? The risk figures for the general population in UK have been calculated by the Cancer Research UK Statistical Information Team, and are based on UK cancer incidence data for The risk figures represent cancer risk up to the age of 64yrs. Q: How accurate are the lifetime cancer risk figures? These figures are risks for an average carrier and do not represent a definitive risk for an individual carrier. The data provided are taken from retrospective studies reporting lifetime cancer risks in cohorts of mutation carriers selected and/or unselected for family history. Please note that lifetime risk refers to the cancer risks up to 70 years and are therefore comparable to the population risks discussed above. The figures include data from studies corrected and uncorrected for ascertainment bias. The figures have been condensed to present the data in a practical format for use in clinic, and represent the best approximation of lifetime cancer risks for an individual. The principal aim of the figures is for use during the genetic counselling process, where many carriers find more qualitative discussion most helpful. Q: What cancer types are currently considered part of the LS tumour spectrum? The LS tumour spectrum is defined by the Amsterdam I criteria (colorectal cancer), Amsterdam II criteria (addition of endometrium, small bowel, ureter or renal pelvis cancers), and the revised Bethesda guidelines (addition of stomach, ovarian, pancreas, bladder, biliary tract, brain, sebaceous gland adenomas and keratocanthoma). See background document Lynch Syndrome evaluation and investigation. Q: Why is the range of lifetime risk of colorectal and endometrial cancer so broad? The range for lifetime colorectal and endometrial cancer risk for MMR mutation carriers reflects the range of risk figures derived from retrospective studies which have been corrected (using statistical methods or by excluding index cases) and uncorrected for ascertainment bias. The lower figure in the range is taken from studies corrected for ascertainment bias, in which MMR mutation carriers were identified in cases selected (clinic-based) and unselected (population-based) for family history. The upper figure in the range is taken from uncorrected (clinic-based) studies of large, multiple case families identified through Lynch Syndrome registries. The majority of these carriers will have been referred to family cancer clinics on the basis of clinical criteria (e.g. Amsterdam criteria I/II). Most families seen in Genetics have some family history. The most appropriate risk figure may be selected by assessing family history. The lower risk figures represent the best approximate risk for Amsterdam-negative families, and the upper risk figures represent the best approximate risk for Amsterdam-positive families. Q: Why are the same cancer risks figures not used for all MMR mutation carriers? Increasingly, multiple studies suggest that the phenotypic spectrum and cancer risks differ substantially between MMR carriers. From the data, MLH1 and MSH2 carriers generally FAQ - Protocols 9-12 Page 1 of 7
2 have higher lifetime risks of cancer compared to MSH6 and PMS2 carriers. The only inconsistency in the data is endometrial cancer risks, which has been demonstrated to be highest in MSH6 carriers by some studies. The data also suggest that PMS2 and MSH6 carriers are at low risk of minor LS-related cancers. But some caution is warranted, as cancer risks have been less well defined in these carriers, particularly PMS2 carriers. Q: How should I manage an EPCAM deletion carrier? EPCAM deletion carriers should have equivalent management to MSH2 mutation carriers, as EPCAM deletions cause Lynch syndrome through epigenetic silencing of MSH2 in EPCAM-expressing tissues. From the limited data, EPCAM deletion carriers have similar lifetime risks of colorectal cancer to MSH2 carriers, but the risk of endometrial cancer has been reported to be significantly lower (although still above 10% threshold). This may be in part due to the tissue-specific MSH2 deficiency caused by EPCAM deletions, but there is still uncertainty regarding the risks of minor cancers in deletion carriers. Q: Are prostate and breast cancer considered part of the tumour spectrum of MMR carriers? Prostate and breast cancer are not currently considered part of the LS tumour spectrum. Both of these cancers are very common in the general population. Further studies are required to include these cancer types as part of the Lynch syndrome spectrum. Q: Are tumours with an MMR-deficient phenotype part of the LS tumour spectrum? Many rare cancer types have been reported in MMR carriers, with evidence of MMR deficiency (loss of MMR protein straining on IHC and/or MSI) being demonstrated for various sites such as adrenocortical adenocarcinoma, thyroid carcinoma, and sarcomas. However, there is insufficient data that MMR carriers have increased lifetime risk for these cancer types, and therefore they are not currently considered part of the LS tumour spectrum. Should a MMR-deficient phenotype be identified in a non-ls spectrum tumour, the family history should be evaluated for other evidence of a LS phenotype Q: What is the clinical phenotype of Muir-Torre Syndrome? Muir-Torre syndrome (MTS) is characterised by the coexistence of at least one sebaceous skin tumour (sebaceous adenomas and carcinomas) or keratocanthoma (neoplasm of the hair follicle) and one or more visceral malignancies (most commonly colorectal cancers). Most reported MTS diagnoses have been in MSH2 carriers, with a few reported in MLH1 mutation carriers. Q: Why are lifetime risk figures for sebaceous tumours not given in the protocols? There are no risk figures available for sebaceous tumours in MMR carriers. However, there is data available regarding the frequency of Muir-Torre syndrome among Lynch pedigrees. The frequency of MTS is estimated to range from 1 to 9%. Q: What is the clinical phenotype of Turcot Syndrome? Turcot syndrome is a clinical description characterised by the coexistence of colorectal cancer and brain tumours. This syndrome is genetically heterogeneous and can been seen in MMR carriers (associated with glioblastomas) or APC carriers (associated with medulloblastomas). Q: What is Constitutional MMR Deficiency Syndrome? This is the term given to individuals who carry biallelic germline mutations in the MMR genes. This syndrome is characterised by café au lait spots, early (in childhood and teenage years) onset of colorectal cancers or other LS-related cancers, oligopolyposis in the small bowel and/or colon, brain tumours, and haematological malignancies. FAQ - Protocols 9-12 Page 2 of 7
3 Q: What types of colorectal cancers do MMR carriers get? Colorectal cancers can be of any histological subtype but there are several characterised associations. Colorectal cancers in MMR carriers are predominantly located in the proximal colon (60 70% in LS, 30% in sporadic CRC), and are often mucinous and poorly differentiated. Colorectal cancers in carriers have a reported MSI frequency of ~85 to 90%. Diploid tumours and signet-ring cancers also seem to be common in carriers. Q: What types of colorectal adenomas do MMR carriers get? Colonic adenomas in MMR carriers tend to be larger and more severely dysplastic than in sporadic cases and most show MSI or loss of immunohistochemical staining of the MMR proteins. Q: What types of endometrial cancers do MMR carriers get? There is no consistent evidence of a significant difference in histological subtypes of endometrial cancers between MMR carriers and the general population. Endometrial cancers in carriers and the general population are predominantly endometrioid subtype (~80%), with non-endometrioid subtypes (e.g. clear cell, serous) accounting for the remaining cases. Q: What types of ovarian cancers do MMR carriers get? Ovarian cancers in MMR carriers can be of any histological subtypes but there are some recognised patterns. Ovarian cancers in MMR carriers are predominantly epithelial nonserous cancer subtypes, particularly endometrioid carcinoma. An excess of clear cell histology subtypes may also be seen in carriers. Ovarian cancers in MMR carriers typically present at an earlier stage (FIGO I/II ~ 80%), compared to sporadic and BRCA-related ovarian cancers (FIGO I/II~33%). Q: What types of gastric cancers do MMR carriers get? Gastric cancers in MMR carriers are predominantly intestinal subtype (~ 80%) with diffuse subtype (13%) accounting for most of the remaining cases. Gastric cancers in carriers have a high degree of MSI. The frequency of BRAF-V600E mutations is low in sporadic and Lynch-related gastric cancers, and therefore this cannot be used to selected individuals for genetic testing. Q: What types of small bowel cancers do MMR carriers get? Small bowel cancers in carriers are predominantly located in the duodenum (~43%) and jejunum (~37%); and only ~7% are located in the ileum. Small bowel cancers in MMR carriers have been shown to have a high degree of MSI (95% compared to ~13% sporadic cases). Q: What types of urinary tract cancers do MMR carriers get? MMR carriers can get any type of urinary tract cancer, but there is a predominance of urothelial cancers (ureter and renal pelvis) in carriers. The histology of these urothelial cancers is similar to that of sporadic cancers. There is conflicting data in regards to the incidence of bladder cancers in carriers. Studies have reported high frequencies of MSI for urothelial tumours in LS that clearly exceed frequencies for corresponding sporadic tumours. Q: Why do we recommend a later starting age of colonoscopic surveillance for MSH6 and PMS2 carriers? From the available data, the average age of CRC onset is somewhat later in MSH6 and PMS2 mutation carriers (54yrs and 59yrs) compared to MLH1 and MSH2 carriers (44yrs and 45yrs). By age 50yrs the cumulative risk of CRC was not reported to exceed 2% for PMS2 carriers and 3% for MSH6 carriers. Based on this evidence, and the risks associated with colonoscopy, it would seem appropriate to offer MSH6 and PMS2 mutation carriers, surveillance starting from the age of 30yrs. However, some MSH6 and FAQ - Protocols 9-12 Page 3 of 7
4 PMS2 carriers may still wish to start colonoscopy at the age of 25yrs. This can be arranged, but the above should be articulated to mutation carriers. Q: What ovarian screening is available to carriers? Ovarian screening is not recommended for MMR carriers, as no ovarian screening modality (including trans-vaginal ultrasound or CA-125 measurement), has demonstrated improved survival for carriers. Q: What endometrial screening is available to carriers? Endometrial screening is not recommended for MMR carriers, as no endometrial screening modality (including trans-vaginal ultrasound or hysteroscopy, or endometrial sampling) has demonstrated improved survival for carriers. Q: What urinary tract screening is available to carriers? Urinary tract screening is not recommended for MMR carriers, as no urinary tract screening modality (including renal ultrasound or urine cytology) has demonstrated improved survival for carriers Q: What gastric screening is available to MMR carriers? Gastric screening is not recommended for MMR carriers, as no gastric screening modality (upper GI endoscopy), has demonstrated improved survival for MMR carriers. The available data also demonstrates that the lifetime risk of gastric cancer is relatively low (<10%) for MMR mutation carriers, with the incidence of gastric cancer now declining in Western countries. Q: Why is Helicobacter pylori screening and eradication recommended? Infection with Helicobacter pylori is an important risk factor for gastric cancer. It causes chronic gastritis, which may lead to gastric atrophy and intestinal metaplasia. These are the main histological precursors to gastric cancer. The available data suggests that searching for and eradicating H pylori reduces the incidence of gastric cancer in asymptomatic individuals. Q: When should I discuss Helicobacter pylori screening and eradication with MMR carriers? Helicobacter pylori screening and eradication can be discussed and offered to MLH1 and MSH2 carriers. PSM2 and MSH6 carriers have significantly lower lifetime risk of gastric cancer, and therefore should only be offered Helicobacter pylori screening and eradication if they have at least one first or second degree relative with gastric cancer. Q: Who will organise Helicobacter pylori screening? A letter should be sent to the patient s GP to organise H pylori screening. NICE recommends that the C urea breath or stool antigen tests be used to screen for H pylori in general practice. Both tests are highly reliable for diagnosis and can be used to assess the success of eradication therapy in positive individuals. Q: Who will prescribe Helicobacter pylori eradication therapy? Helicobacter pylori eradication therapy will be prescribed by the patient s GP if required. There are several treatment regimens. Typically regimens include one-week triple therapy regimen with a proton pump inhibitor (e.g. omeprazole) plus two antibiotics (e.g. amoxicillin and clarithromycin). Q: What symptoms should be discussed with carriers? The importance of symptom awareness should be discussed with all MMR carriers. The following symptoms should be discussed: FAQ - Protocols 9-12 Page 4 of 7
5 Colorectal: bleeding from the back passage (rectum), blood in stools, change in normal bowel habits to diarrhoea or looser stools, lasting longer than 4 to 6 weeks, unexplained weight loss, abdominal pain, and fatigue. Endometrial: Vaginal bleeding after the menopause, heavy periods, bleeding between menstrual cycles, and vaginal discharge. Ovarian: Symptoms can be quite vague, but include pain in the lower abdomen or side, feeling bloated, abdominal swelling, abdominal pain, abnormal vaginal bleeding (post menopausally or in between cycles), back pain, and constipation. Urinary tract: Blood in urine, mass in abdomen, weight loss, fatigue, persistent pain in side, urinary frequency or urgency. Gastric: persistent indigestion, feeling full early, pain or difficulty with swallowing, fatigue, dark tarry stools, nausea. Q: What is the risk of a metachronous colorectal cancer? The risk of a second colorectal cancer remains substantial after a partial colectomy. The risk of developing a metachronous colorectal cancer in MMR carriers has been reported by a study to be 16% (95% CI 10% to 25%) at 10 years, 41% (95% CI 30% to 52%) at 20 years and 62% (95% CI 50% to 77%) at 30 years after segmental colectomy. This data does have some limitations, as detailed information about the surveillance protocol (e.g. interval and quality) was unavailable, which may result in upwardly biased metachronous cancer risks. It is also unclear what factors influenced the choice of surgery. Q: What surgical options are there for colorectal cancer? All carriers with a newly diagnosed colorectal cancer should be offered the opportunity to discuss different surgical options (partial vs. subtotal colectomy) with their surgical team, and should be aware that carriers whose first colon cancer is treated with more extensive colonic resection have a lower risk of metachronous colorectal cancer than those having less extensive colonic surgery. However, there is no data that suggests a survival benefit in carriers having more extensive surgery, and there is good evidence that colonoscopy is effective at preventing deaths by colon cancer in carriers. Other important issues carriers may like to consider are functional results of subtotal vs. partial colectomy, age, and personal preference. Q: When should I discuss aspirin chemoprevention with carriers? All MMR carriers who do not wish to take part in the CAPP3 study should be offered the option of taking low dose aspirin (75mg OD) from the age of 25yrs. Q: What benefits of aspirin chemoprevention should I discuss? MMR carriers should be made aware that aspirin (600mg) chemoprevention has been shown to reduce the overall number of colorectal cancer cases, and incidence of LS-related cancers in carriers. However, aspirin chemoprevention has not been shown to have an impact on mortality. Q: What side effects of chemoprevention should I discuss? Regular aspirin use is associated with an increased risk of gastrointestinal bleeding, (which is probably dose-dependent), and intracranial haemorrhage (1 in 10,000 per annum). Aspirin can also exacerbate asthma in certain individuals. Q: Are there any contraindications to chemoprevention? Aspirin should not be taken if pregnant or planning pregnancy in next 2 years Aspirin should not be taken by women who are breast feeding Aspirin should not be taken with other drugs that increase the risk of bleeding (e.g. NSAIDS, anticoagulant medication, steroids) FAQ - Protocols 9-12 Page 5 of 7
6 Aspirin should not be taken if carriers have a history of bleeding disorder, active peptic ulcer disease within the last 3 months, liver impairment, renal impairment, or poorly controlled hypertension. Aspirin should not be taken if carriers have known aspirin intolerance or hypersensitivity, including aspirin-sensitive asthma. Q: Why do we recommend risk-reducing hysterectomy for all MMR carriers? All female MMR carriers have been demonstrated to have a high (at least 10%) lifetime risk of developing endometrial cancer. A significant proportion of carriers who develop endometrial cancer will eventually die from their disease and there is significant morbidity associated with cancer-related treatment. There is also no proven, efficacious form of screening. Risk reduction hysterectomy has been demonstrated to reduce the endometrial cancer risk in MMR carriers by up to 100%. However, it has not been shown to improve survival in MMR carriers, which in part may be due to the relatively good prognosis associated with endometrial cancers in Lynch syndrome patients. Q: Why do we recommend risk-reducing bilateral salpingo-oophorectomy for MSH2 and MLH1 carriers? Data has consistently demonstrated a high (at least 10%) lifetime risk of ovarian cancers for MSH2 and MLH1 carriers. Risk reducing bilateral salpingo-oophorectomy is recommended for MSH2 and MLH1 carriers because the benefit/harm ratio is likely to be favourable. These carriers have a high lifetime risk of ovarian cancer, a significant proportion of carriers who develop ovarian cancer will eventually die of their disease, and there is significant morbidity associated with cancer-related treatment. There is also no proven, efficacious form of screening. Risk reducing BSO has been demonstrated to reduce the ovarian cancer risk in MMR carriers by up to 100% (not statistically significant due to low numbers). However, it has not been shown to improve survival in MMR carriers, which in part may be due to the relatively good prognosis associated with LS-related ovarian cancers (in comparison to sporadic or BRCA-related cancers). Q: Why do we not routinely recommend risk-reducing bilateral salpingooophorectomy for MSH6 and PMS2 carriers? Although the data is limited, it would appear that the lifetime risk of ovarian cancer for MSH6 and PMS2 carriers is significantly lower than MSH2 and MLH1 carriers. To date no studies have demonstrated a 10% or greater lifetime risk of ovarian cancers for MSH6 and PMS2 carriers. Therefore, risk reducing BSO is not routinely recommended in premenopausal MSH6 and PMS2 carriers, as based on the current evidence available, the benefit/harm ratio is likely to be unfavourable. Q: Are there any circumstances that we would discuss risk-reducing BSO with MSH6 and PMS2 carriers? Similar to non-carrier females, BSO may be discussed in MSH6 and PMS2 carriers who have two or more first or second-degree relatives with ovarian cancer. At least one should be a first-degree relative of the carrier. BSO may also be discussed with carriers undergoing hysterectomies post-menopausally, as the benefit/harm ratio is likely to be more favourable in this situation. Q: At what age should women undertake risk-reducing hysterectomy with or without BSO? For MLH1 and MSH2 carriers who have completed their families, it is appropriate to consider hysterectomy with BSO from 40yrs onwards, as the risk of endometrial and ovarian cancer increases from the age of 40yrs. FAQ - Protocols 9-12 Page 6 of 7
7 For MSH6 and PMS2 carriers who have completed their families it is appropriate to consider hysterectomy from 40yrs onwards, as the risk of endometrial cancer is not clinically significant below this age. For PMS2 carriers it may be reasonable to delay until the age of 45, as the risk of endometrial cancer does not increase until the age of 50. Obviously there are also many personal factors that may influence this decision, which should be taken into consideration. For example, sometimes women wish to consider surgery earlier because there have been younger-onset cases within their family. Q: What are the disadvantages of risk-reducing hysterectomy and bilateral salpingooophorectomy? The main adverse effects of prophylactic gynaecological surgery include colonoscopic surveillance becoming more difficult and painful, loss of fertility, and surgically-induced menopause (if surgery is performed pre-menopausally). Menopausal symptoms include hot flushes, vaginal dryness, sexual dysfunction, sleep and cognitive disturbances. Premature menopause may also be associated with increased risk of osteoporosis and heart disease in later life. HRT should be used to minimise these effects and should be started in women who have not had breast cancer from time of surgery until 50 years (the approximate time of the natural menopause). Carriers should be made aware of the small risk of peritoneal carcinoma that remains following BSO. Carriers should also be made aware that surgery is associated with a small risk of morbidity and mortality. Q: What advice should be given to carriers regarding the investigation of urinary tract cancer symptoms? All MMR carriers should be advised that if they develop symptoms suggestive of urinary tract cancer, such as haematuria (blood in urine), that they should contact their GPs immediately for further investigations. Although, it is appropriate to exclude other more common causes of urinary tract symptoms (e.g. infection), it is important that GP have a low threshold for referring carriers onward for a urological opinion. This should be clearly articulated to carriers. Q: What lifestyle advice should be given to MMR carriers? Smoking and a high BMI have been demonstrated to increase the risk of adenomas and colorectal cancer in MMR carriers. Therefore carriers should be advised to maintain a healthy weight and refrain from smoking. Q: How should I manage an individual in whom a predictive test is negative? A negative predictive test is when an individual is found to not carry the mutation that has been shown to be responsible for the LS-related cancers in their family. On the basis of current knowledge such individuals should be returned to population bowel screening. FOB kits are sent out biennially to individuals aged 60yrs. Individuals with abnormal results are offered colonoscopy. See for more details. Risk reducing hysterectomy or BSO is not recommended. Q: How do I manage a MMR negative family? Please see Protocols 7-8. Q: What should I do if there is a variant of unclear significance? report to vus@icr.ac.uk and discuss case at multi-disciplinary team meeting. FAQ - Protocols 9-12 Page 7 of 7
FAQ-Protocol 3. BRCA mutation carrier guidelines Frequently asked questions
 ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
Content. Diagnostic approach and clinical management of Lynch Syndrome: guidelines. Terminology. Identification of Lynch Syndrome
 of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
Mr Chris Wakeman. General Surgeon University of Otago, Christchurch. 12:15-12:40 Management of Colorectal Cancer
 Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
Guidelines on Genetic Evaluation and Management of Lynch Syndrome: A Consensus Statement by the US Multi-Society Task Force on Colorectal Cancer
 s on Genetic Evaluation and Management of Lynch Syndrome: A Consensus Statement by the US Multi-Society Task Force on Colorectal Cancer Francis M. Giardiello, MD, 1 John I. Allen, 2 Jennifer E. Axilbund,
s on Genetic Evaluation and Management of Lynch Syndrome: A Consensus Statement by the US Multi-Society Task Force on Colorectal Cancer Francis M. Giardiello, MD, 1 John I. Allen, 2 Jennifer E. Axilbund,
Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Pr
 Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Professor Yong Loo Lin School of Medicine, National University
Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Professor Yong Loo Lin School of Medicine, National University
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document Molecular testing strategies for Lynch syndrome in The National Institute for Health
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document Molecular testing strategies for Lynch syndrome in The National Institute for Health
LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)!
 LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)! Kathryn Singh, MPH, MS, LCGC Associate Clinical Professor Assistant Director, Graduate Program in Genetic Counseling Division of Genetic and Genomic
LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)! Kathryn Singh, MPH, MS, LCGC Associate Clinical Professor Assistant Director, Graduate Program in Genetic Counseling Division of Genetic and Genomic
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By. Magnitude of the Problem. Magnitude of the Problem. Cardinal Features of Lynch Syndrome
 GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
Primary Care Approach to Genetic Cancer Syndromes
 Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Gynecologic Cancers are many diseases. Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine. Speaker Disclosure:
 Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Gynecologic Cancers are many diseases. Speaker Disclosure: Gynecologic Cancer Care in the Age of Precision Medicine. Controversies in Women s Health
 Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Controversies in Women s Health Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Controversies in Women s Health Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Hereditary Non Polyposis Colorectal Cancer(HNPCC) From clinic to genetics
 From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27
 Molecular testing strategies for Lynch syndrome in people with colorectal cancer Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27 NICE 2018. All rights reserved. Subject to Notice
Molecular testing strategies for Lynch syndrome in people with colorectal cancer Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27 NICE 2018. All rights reserved. Subject to Notice
Surgery to Reduce the Risk of Ovarian Cancer. Information for Women at Increased Risk
 Surgery to Reduce the Risk of Ovarian Cancer Information for Women at Increased Risk Centre for Genetics Education NSW Health 2017 The Centre for Genetics Education NSW Health Level 5 2C Herbert St St
Surgery to Reduce the Risk of Ovarian Cancer Information for Women at Increased Risk Centre for Genetics Education NSW Health 2017 The Centre for Genetics Education NSW Health Level 5 2C Herbert St St
GI Screening/Surveillance in Lynch Syndrome
 GI Screening/Surveillance in Lynch Syndrome M Appleyard Royal Brisbane and Women s Hospital Brisbane, Australia GI Disease and Lynch Syndrome What are risks of GI disease in Lynch? Who do we screen for
GI Screening/Surveillance in Lynch Syndrome M Appleyard Royal Brisbane and Women s Hospital Brisbane, Australia GI Disease and Lynch Syndrome What are risks of GI disease in Lynch? Who do we screen for
MSH6 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table
 MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes
 Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes Policy Number: 2.04.08 Last Review: 1/2014 Origination: 1/2004 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes Policy Number: 2.04.08 Last Review: 1/2014 Origination: 1/2004 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas
MLH1 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MLH1 Summary Cancer Risk Table
 MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer
 Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
Lynch Syndrome. Angie Strang, PGY2
 Lynch Syndrome Angie Strang, PGY2 Background Previously hereditary nonpolyposis colorectal cancer Autosomal dominant inherited cancer susceptibility syndrome Caused by defects in the mismatch repair system
Lynch Syndrome Angie Strang, PGY2 Background Previously hereditary nonpolyposis colorectal cancer Autosomal dominant inherited cancer susceptibility syndrome Caused by defects in the mismatch repair system
Hereditary Cancer Products
 Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Policy Specific Section: Medical Necessity and Investigational / Experimental. October 14, 1998 March 28, 2014
 Medical Policy Genetic Testing for Colorectal Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: October
Medical Policy Genetic Testing for Colorectal Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: October
PMS2 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table
 PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Management of dyspepsia and of Helicobacter pylori infection
 Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
BowelGene. How do I know if I am at risk? Families with hereditary bowel cancer generally show one or more of the following clues:
 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer
 GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
FAMILIAL COLORECTAL CANCER. Lyn Schofield Manager Familial Cancer Registry
 FAMILIAL COLORECTAL CANCER Lyn Schofield Manager Familial Cancer Registry Cancer in WA 2004 4000 3500 ASPR, rate per 100,000 3000 2500 2000 1500 1000 Male incidence Female incidence Male mortality Female
FAMILIAL COLORECTAL CANCER Lyn Schofield Manager Familial Cancer Registry Cancer in WA 2004 4000 3500 ASPR, rate per 100,000 3000 2500 2000 1500 1000 Male incidence Female incidence Male mortality Female
Understanding and Managing Lynch Syndrome
 Understanding and Managing Lynch Syndrome Princess Margaret For women who may have Lynch syndrome and their family members Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Understanding and Managing Lynch Syndrome Princess Margaret For women who may have Lynch syndrome and their family members Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Genetic Testing for Lynch Syndrome and Other Inherited Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Genetic Testing for Lynch Syndrome and Other
Genetic Testing for Lynch Syndrome and Other Inherited Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Genetic Testing for Lynch Syndrome and Other
Hereditary Cancer Update: What do GPOs need to know?
 Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
How common are mutations in the MSH2 gene? 1. Mutations that cause Lynch syndrome are rare found in approximately 1 in 370 individuals.
 The gene is a tumor suppressor gene. Tumor suppressor genes slow down cell division, repair DNA mistakes, or tell cells when to die. When they don't work properly, cells can grow out of control, which
The gene is a tumor suppressor gene. Tumor suppressor genes slow down cell division, repair DNA mistakes, or tell cells when to die. When they don't work properly, cells can grow out of control, which
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_colon_cancer 5/2004 8/2017 8/2018 8/2017 Description of Procedure or Service Genetic
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_colon_cancer 5/2004 8/2017 8/2018 8/2017 Description of Procedure or Service Genetic
GHUK BowelGene_2017.qxp_Layout 1 22/02/ :22 Page 3 BowelGene
 GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
6 Week Course Agenda. Today s Agenda. Ovarian Cancer: Risk Factors. Winning the War 11/30/2016 on Women s Cancer Gynecologic Cancer Prevention
 6 Week Course Agenda Winning the War 11/30/2016 on Women s Cancer Gynecologic Cancer Prevention Lee-may Chen, MD Director, Division of Gynecologic Oncology Professor Department of Obstetrics, Gynecology
6 Week Course Agenda Winning the War 11/30/2016 on Women s Cancer Gynecologic Cancer Prevention Lee-may Chen, MD Director, Division of Gynecologic Oncology Professor Department of Obstetrics, Gynecology
Lynch syndrome. 9 October 2015 Masato Yozu Middlemore Hospital, Auckland, New Zealand
 Lynch syndrome 9 October 2015 Masato Yozu Middlemore Hospital, Auckland, New Zealand History of Lynch syndrome Aldred ScoO Warthin, MD, PhD (1866-1931) The father of cancer geneycs (JAMA. 2005;294(17):2195-2202)
Lynch syndrome 9 October 2015 Masato Yozu Middlemore Hospital, Auckland, New Zealand History of Lynch syndrome Aldred ScoO Warthin, MD, PhD (1866-1931) The father of cancer geneycs (JAMA. 2005;294(17):2195-2202)
Tumori eredofamiliari: sorveglianza di donne ad alto rischio
 Tumori eredofamiliari: sorveglianza di donne ad alto rischio 14/01/2018 Dott Matteo Generali AUSL Modena Carpi U.O. Ostetricia e Ginecologia Screening for gynaecologic cancer in genetically predisposed
Tumori eredofamiliari: sorveglianza di donne ad alto rischio 14/01/2018 Dott Matteo Generali AUSL Modena Carpi U.O. Ostetricia e Ginecologia Screening for gynaecologic cancer in genetically predisposed
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory
 2.04.08 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date January 30, 2015 Original Policy Date October
2.04.08 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date January 30, 2015 Original Policy Date October
Sarah Burton. Lead Gynae Oncology Nurse Specialist Cancer Care Cymru
 Sarah Burton Lead Gynae Oncology Nurse Specialist Cancer Care Cymru Gynaecological Cancers Cervical Cancers Risk factors Presentation Early sexual activity Multiple sexual partners Smoking Human Papiloma
Sarah Burton Lead Gynae Oncology Nurse Specialist Cancer Care Cymru Gynaecological Cancers Cervical Cancers Risk factors Presentation Early sexual activity Multiple sexual partners Smoking Human Papiloma
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2018 Origination: 1/2004 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2018 Origination: 1/2004 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas
MANAGEMENT OF HIGH RISK BREAST PATIENTS DR PAMELA THOMPSON BREAST PHYSICIAN, FSH
 MANAGEMENT OF HIGH RISK BREAST PATIENTS DR PAMELA THOMPSON BREAST PHYSICIAN, FSH HIGH RISK MANAGEMENT OBJECTIVES Be alert to FHx Breast and/or Ovarian cancer Know how to perform a risk assessment Be aware
MANAGEMENT OF HIGH RISK BREAST PATIENTS DR PAMELA THOMPSON BREAST PHYSICIAN, FSH HIGH RISK MANAGEMENT OBJECTIVES Be alert to FHx Breast and/or Ovarian cancer Know how to perform a risk assessment Be aware
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Result Navigator Positive Test Result: MSH6
 Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Myriad Financial Assistance Program (MFAP)
 Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
Universal Screening for Lynch Syndrome
 Universal Screening for Lynch Syndrome St. Vincent/Ameripath protocol proposal Lynch syndrome (HNPCC) 1/35 individuals with colorectal cancer has Lynch syndrome Over half individuals are >50 at time of
Universal Screening for Lynch Syndrome St. Vincent/Ameripath protocol proposal Lynch syndrome (HNPCC) 1/35 individuals with colorectal cancer has Lynch syndrome Over half individuals are >50 at time of
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014
 COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
The Whys OAP Annual Meeting CCO Symposium September 20. Immunohistochemical Assessment Dr. Terence Colgan Mount Sinai Hospital, Toronto
 Immunohistochemical Assessment of Mismatch Repair Proteins in Endometrial Cancer: The Whys and How Terence J. Colgan, MD Head of Gynaecological Pathology, Mount Sinai Hospital, University of Toronto, Toronto.
Immunohistochemical Assessment of Mismatch Repair Proteins in Endometrial Cancer: The Whys and How Terence J. Colgan, MD Head of Gynaecological Pathology, Mount Sinai Hospital, University of Toronto, Toronto.
Gynaecological Oncology Cases
 Gynaecological Oncology Cases 1. Tamoxifen and the endometrium 2. Cancer and the older woman Dr Julie M Lamont Consultant Gynaecological Oncologist Epworth Freemasons Hospital 21 st April 2015 Mrs FS 66
Gynaecological Oncology Cases 1. Tamoxifen and the endometrium 2. Cancer and the older woman Dr Julie M Lamont Consultant Gynaecological Oncologist Epworth Freemasons Hospital 21 st April 2015 Mrs FS 66
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2019 Origination: 1/2004 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2019 Origination: 1/2004 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas
Figure 1: Consort diagram; the status of participants in the study
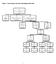 Figure : Consort diagram; the status of participants in the study Figure a. Time to first colorectal cancer in those randomized to aspirin compared with those randomized to aspirin placebo (AP). Kaplan-Meier
Figure : Consort diagram; the status of participants in the study Figure a. Time to first colorectal cancer in those randomized to aspirin compared with those randomized to aspirin placebo (AP). Kaplan-Meier
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER. Dr Abhijit Dixit. Family Health Clinical Genetics
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
FACT SHEET 49. What is meant by a family history of bowel cancer? What is bowel cancer? What causes bowel cancer?
 Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
Advice about familial aspects of breast cancer and epithelial ovarian cancer
 Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017
 Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122
 Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Pathology reports, related operative reports and consult letters must be provided with a request for assessment.
 Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Importance of Family History in Gynecologic Cancer Prevention. Objectives. Genetic Counselors. Angela Thompson, MS, CGC
 Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Genetic Testing for Inherited Susceptibility to Colon Cancer Page 1 of 24 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Genetic Testing for Inherited Susceptibility
Genetic Testing for Inherited Susceptibility to Colon Cancer Page 1 of 24 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Genetic Testing for Inherited Susceptibility
Proactive Patient Paves the Way for Genetic Testing of Eight Family Members
 CASE STUDY Proactive Patient Paves the Way for Genetic Testing of Eight Family Members Quick Summary Samar Mohite * was diagnosed with colon adenocarcinoma at the age of 49 years. Genetic counselling was
CASE STUDY Proactive Patient Paves the Way for Genetic Testing of Eight Family Members Quick Summary Samar Mohite * was diagnosed with colon adenocarcinoma at the age of 49 years. Genetic counselling was
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
GYNplus. genetic testing for hereditary ovarian and/or uterine cancer
 GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University
 COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
Lynch Syndrome. A Patient s Guide to Genetic Testing for Lynch Syndrome
 Lynch Syndrome A Patient s Guide to Genetic Testing for Lynch Syndrome What is Lynch Syndrome? Lynch syndrome is an inherited condition that increases your risk of developing colon cancer and other cancers
Lynch Syndrome A Patient s Guide to Genetic Testing for Lynch Syndrome What is Lynch Syndrome? Lynch syndrome is an inherited condition that increases your risk of developing colon cancer and other cancers
Serrated Polyps and a Classification of Colorectal Cancer
 Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
 Familial breast cancer: classification, care and managing breast cancer and related risks in people with a family history of breast cancer Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
Familial breast cancer: classification, care and managing breast cancer and related risks in people with a family history of breast cancer Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Classification of polyposis syndromes two major groups. Adenomatous polyposis syndromes. Hamartomatous polyposis syndromes
 Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
CA125 in the diagnosis of ovarian cancer: the art in medicine
 CA125 in the diagnosis of ovarian cancer: the art in medicine Dr Marcia Hall Consultant Medical Oncology Mount Vernon Cancer Centre Hillingdon Hospital Wexham Park Hospital Epidemiology Ovarian cancer
CA125 in the diagnosis of ovarian cancer: the art in medicine Dr Marcia Hall Consultant Medical Oncology Mount Vernon Cancer Centre Hillingdon Hospital Wexham Park Hospital Epidemiology Ovarian cancer
Familial Adenomatous Polyposis
 Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Page 1 of 8 TABLE OF CONTENTS
 Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
27
 26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
Yes when meets criteria below. Dean Health Plan covers when Medicare also covers the benefit.
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome
 Pathology Research International Volume 2012, Article ID 350309, 6 pages doi:10.1155/2012/350309 Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome Markku Aarnio Department
Pathology Research International Volume 2012, Article ID 350309, 6 pages doi:10.1155/2012/350309 Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome Markku Aarnio Department
Genetic Testing for Inherited Susceptibility to Colon Cancer; Including Microsatellite Instability Testing. Original Policy Date
 MP 2.04.06 Genetic Testing for Inherited Susceptibility to Colon Cancer; Including Microsatellite Instability Testing Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 2.04.06 Genetic Testing for Inherited Susceptibility to Colon Cancer; Including Microsatellite Instability Testing Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review
Familial Cancer Clinic Information Sheet. Surgery to prevent endometrial and ovarian cancer. in women with Lynch Syndrome
 Familial Cancer Clinic Institute for Women s Health 1 st Floor, Maple House 124 Tottenham Court Road W1T 7DN Telephone: 020 7380 6912 Fax: 020 7380 6929 Email: michelle.johnson@ucl.ac.uk Familial Cancer
Familial Cancer Clinic Institute for Women s Health 1 st Floor, Maple House 124 Tottenham Court Road W1T 7DN Telephone: 020 7380 6912 Fax: 020 7380 6929 Email: michelle.johnson@ucl.ac.uk Familial Cancer
A Review from the Genetic Counselor s Perspective
 : A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
: A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
X-Plain Ovarian Cancer Reference Summary
 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Colorectal Cancer Syndromes. Barbara Jung, MD AGAF Associate Professor and Chief University of Illinois at Chicago
 Colorectal Cancer Syndromes Barbara Jung, MD AGAF Associate Professor and Chief University of Illinois at Chicago Outline Colon cancer General Genetics, Risk, Screening Specific Syndromes, when to suspect,
Colorectal Cancer Syndromes Barbara Jung, MD AGAF Associate Professor and Chief University of Illinois at Chicago Outline Colon cancer General Genetics, Risk, Screening Specific Syndromes, when to suspect,
University Gynecologic Oncology Associates
 University Gynecologic Oncology Associates Medical History Form Date: Name: Date of Birth: / / GYNE HISTORY Age of first period? If you no longer have periods, at what age did they stop? Are you pregnant
University Gynecologic Oncology Associates Medical History Form Date: Name: Date of Birth: / / GYNE HISTORY Age of first period? If you no longer have periods, at what age did they stop? Are you pregnant
Management of higher risk of colorectal cancer. Huw Thomas
 Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy?
 Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy? Robert Benamouzig Service de Gastroentérologie Hôpital Avicenne Bobigny, France Aspirin and Colorectal carcinogenesis Aspirin
Is aspirin ready for colorectal cancer chemoprevention and adjuvant therapy? Robert Benamouzig Service de Gastroentérologie Hôpital Avicenne Bobigny, France Aspirin and Colorectal carcinogenesis Aspirin
Genetic Testing for Lynch Syndrome
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
number Done by Corrected by Doctor مها شوماف
 number 15 Done by Ali Yaghi Corrected by Waseem Alhaj Doctor مها شوماف 1 P a g e Epidemiology Epidemiology is the study of the incidence of a disease. It can give us information about the possible causes
number 15 Done by Ali Yaghi Corrected by Waseem Alhaj Doctor مها شوماف 1 P a g e Epidemiology Epidemiology is the study of the incidence of a disease. It can give us information about the possible causes
General Surgery Grand Grounds
 General Surgery Grand Grounds University of Colorado Health Sciences Center Case Presentation December 24, 2009 Adam Lackey, PGY-5 J.L. - 2111609 27 YO female with chief complaint of abdominal pain. PMHx:
General Surgery Grand Grounds University of Colorado Health Sciences Center Case Presentation December 24, 2009 Adam Lackey, PGY-5 J.L. - 2111609 27 YO female with chief complaint of abdominal pain. PMHx:
GI update. Common conditions and concerns my patients frequently asked about
 GI update Common conditions and concerns my patients frequently asked about Specific conditions I ll try to cover today 1. Colon polyps, colorectal cancer and colonoscopy 2. Crohn s disease 3. Peptic ulcer
GI update Common conditions and concerns my patients frequently asked about Specific conditions I ll try to cover today 1. Colon polyps, colorectal cancer and colonoscopy 2. Crohn s disease 3. Peptic ulcer
Colonic polyps and colon cancer. Andrew Macpherson Director of Gastroentology University of Bern
 Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Ovarian Cancer Causes, Risk Factors, and Prevention
 Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
National Medical Policy
 National Medical Policy Subject: Policy Number: Genetic Testing for Hereditary Nonpolyposis Colorectal Cancer (HNPCC) (Lynch Syndrome) NMP137 Effective Date*: April 2004 Updated: March 2017 This National
National Medical Policy Subject: Policy Number: Genetic Testing for Hereditary Nonpolyposis Colorectal Cancer (HNPCC) (Lynch Syndrome) NMP137 Effective Date*: April 2004 Updated: March 2017 This National
Coversheet for Network Site Specific Group Agreed Documentation
 Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
A Patient s Guide to risk assessment. Hereditary Colorectal Cancer
 A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
