Prognostic and Predictive Value of KRAS Mutations in Advanced Non-Small Cell Lung Cancer
|
|
|
- Marybeth Carson
- 5 years ago
- Views:
Transcription
1 Prognostic and Predictive Value of KRAS Mutations in Advanced Non-Small Cell Lung Cancer Jong-Mu Sun., Deok Won Hwang., Jin Seok Ahn, Myung-Ju Ahn, Keunchil Park* Division of Hematology-Oncology, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Abstract Clinical implications of KRAS mutations in advanced non-small cell lung cancer remain unclear. We retrospectively evaluated the prognostic and predictive value of KRAS mutations in patients with advanced NSCLC. Among 484 patients with available results for both KRAS and EGFR mutations, 39 (8%) had KRAS and 182 (38%) EGFR mutations, with two cases having both mutations. The median overall survivals for patients with KRAS mutations, EGFR mutations, or both wild types were 7.7, 38.0, and 15.0 months, respectively (P,0.001). The KRAS mutation was an independent poor prognostic factor in the multivariate analysis (hazard ratio = 2.6, 95% CI: ). Response rates and progression-free survival (PFS) for the pemetrexed-based regimen in the KRAS mutation group were 14% and 2.1 months, inferior to those (28% and 3.9 months) in the KRAS wild type group. KRAS mutation tended to be associated with inferior treatment outcomes after gemcitabine-based chemotherapy, while there was no difference regarding taxane-based regimen. Although the clinical outcomes to EGFR tyrosine kinase inhibitors (TKIs) seemed to be better in patients with KRAS wild type than those with KRAS mutations, there was no statistical difference in response rates and PFS according to KRAS mutation status when EGFR mutation status was considered. Two patients with both KRAS and EGFR mutations showed partial response to EGFR TKIs. Although G12D mutation appeared more frequently in never smokers, there was no difference in clinical outcomes according to KRAS genotypes. These results suggested KRAS mutations have an independent prognostic value but a limited predictive role for EGFR TKIs or cytotoxic chemotherapy in advanced NSCLC. Citation: Sun J-M, Hwang DW, Ahn JS, Ahn M-J, Park K (2013) Prognostic and Predictive Value of KRAS Mutations in Advanced Non-Small Cell Lung Cancer. PLoS ONE 8(5): e doi: /journal.pone Editor: Olga Y. Gorlova, The University of Texas M. D. Anderson Cancer Center, United States of America Received February 15, 2013; Accepted April 18, 2013; Published May 28, 2013 Copyright: ß 2013 Sun et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Funding: This work was supported by Korean Health 21 R&D Project, Ministry of Health & Welfare, Korea, grant A The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Competing Interests: The authors have declared that no competing interests exist. * kpark@skku.edu. These authors contributed equally to this work. Introduction Non-small cell lung cancer (NSCLC) is a leading cause of cancer-related mortality despite intensive anticancer treatment and improvement of clinical modalities seen in the recent decades. In order to provide more individualized therapy for NSCLC, a great effort has been made, targeting against several signaling pathways which include epidermal growth factor receptor (EGFR). The clinical activity of EGFR targeting agent, tyrosine kinase inhibitor (TKI) such as gefitinib and erlotinib, is closely associated with EGFR mutation status in NSCLC, and the clinical relevance of EGFR mutations as a positive predictive factor for EGFR TKI therapy has been well documented [1 5]. Like EGFR mutations, KRAS mutations are frequently appearing genetic changes in NSCLC, found in 15% to 30% of NSCLC among Western patients, although the frequency is lower in Asian patients [6 11]. However, the clinical implications of KRAS mutations remain unclear. Although some studies previously identified the KRAS mutation as a poor prognostic factor in NSCLC [12 14], others have failed to reproduce those results [6,8,15 17]. In addition, KRAS mutation has been proposed as a mechanism of primary resistance to EGFR TKI [18], and many studies demonstrated poor clinical outcomes to EGFR TKIs in patients with NSCLC harboring KRAS mutation [7,9,19,20]. However, the analysis of the predictive role of KRAS mutation for EGFR TKI therapy can be confounded by EGFR mutation status [21]. Therefore, the predictive value of KRAS mutation for EGFR TKI therapy should be analyzed with EGFR mutation status being considered. The inconsistent results regarding the prognostic and predictive values of KRAS mutations are in part caused by the heterogeneity and the small size of study population. In addition, many previous studies were performed in the patients with completely resected lung cancer, making it difficult to find small, but significant impacts of a biomarker on survival or treatment outcomes after chemotherapy. Interestingly, KRAS mutations were recently suggested as sensitizing tumors to pemetrexed, possibly by upregulation of a microrna that can downregulate KRAS [22]. This observation may be significant since, if it is true, it could affect how patients are selected in the clinical trials investigating new targeting agents for the KRAS pathway as well as how patients are treated in clinical practice. The purpose of this study was to evaluate whether there is any difference in the treatment outcomes to various types of chemotherapeutic regimens according to the KRAS mutation status and also to investigate the prognostic role of this biomarker. PLOS ONE 1 May 2013 Volume 8 Issue 5 e64816
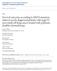
2 Patients and Methods Patients and data collection The study population included patients who were histologically diagnosed of advanced NSCLC at Samsung Medical Center between January 2006 and January Among them, patients who received palliative chemotherapy and had tumors known for both KRAS and EGFR mutation status were included in this study. Baseline characteristics and clinical outcomes for the administered chemotherapeutic regimens consisting of first- to third-line chemotherapy were retrospectively reviewed. Smoking status was defined as never (,100 lifetime cigarettes), former (quit $1 year before diagnosis), or current smokers (quit,1 year before diagnosis). The amount of smoking was categorized as zero, 30 pack-years or less, and more than 30 pack-years. Chemotherapeutic regimens were categorized into 4 types: pemetrexed-based, gemcitabine-based, taxane-based (paclitaxel or docetaxel) regimens, and EGFR TKI (gefitinib or erlotinib). The response outcome to chemotherapy was defined based on Response Evaluation Criteria Evaluation in Solid Tumors (RECIST). The study was approved by the Institutional Review Board of Samsung Medical Center. The requirement of informed consent was waived as the study was based in the retrospective analyses of existing administrative and clinical data. EGFR and KRAS mutation testing Tumor specimens for all patients in this study were obtained from diagnostic or surgical procedures. The mutational analyses of EGFR (exons 18 21) and KRAS (exons 2, 3) were performed by directional sequencing of polymerase chain reaction (PCR) fragments amplified with genomic DNA from paraffin-embedded tissue. PCR was performed in a 20 ml volume containing 100 ng of template DNA, 10 x PCR buffer; 0.25 mmdntps, 10 pmol primers and 1.25 U Taq DNA polymerase (intron, Korea). PCR products were electrophoresed on 2% agarose gels and were purified with a QIAquick PCR purification kit (QIAGEN, Hilden, Germany). Bidirectional sequencing was performed using the BigDye Terminator v 1.1 kit (Applied Biosystems, Foster City, CA, USA) on an ABI 3130xl genetic analyzer (Applied Biosystems, Foster City, CA, USA). Statistical analysis The relationship between KRAS or EGFR mutations with other clinicopathologic characteristics was analyzed with x 2 tests. The logistic regression model was used in the multivariate analysis. The difference in response rates after each chemotherapeutic regimen according to KRAS or EGFR mutation status was analyzed with x 2 tests. Overall survival (OS) and progression-free survival (PFS) were measured from the day of diagnosis of advanced lung cancer and from the start day of each chemother- Figure 1. Flow chart of study population. In total, 484 patients with advanced NSCLC with valid results for both KRAS/EGFR mutation status and chemotherapy were included. There were 39 KRAS mutations, 182 EGFR mutations, 265 both wild types. Interestingly, two patients had tumors simultaneously harboring both KRAS and EGFR mutations. doi: /journal.pone g001 PLOS ONE 2 May 2013 Volume 8 Issue 5 e64816
3 apeutic regimen, respectively, and were analyzed by Kaplan- Meier estimates and log-rank test. A multivariate analysis was carried out using Cox s regression analysis to assess the independent prognostic role of each clinicopathologic factor. In addition, OS according to the different types of KRAS mutations were analyzed to determine potential prognostic differences based on KRAS genotypes. Statistical analyses were performed using SPSS 19.0 (SPSS Inc. Chicago, IL), and statistical significance was considered to be P#0.05. Results Distributions of KRAS and EGFR mutations During the study period, 1,824 patients were newly diagnosed of advanced NSCLC at Samsung Medical Center. Among them, 664 (36%) patients were referred for KRAS or EGFR mutation tests. However, only EGFR mutations were tested in 112 patients, neither KRAS nor EGFR mutation test could not be done in 32 patients due to small amount of tumor DNA, and 11 cases who were not tested for both exon 19 and 21 EGFR mutations were classified as unknown mutation status. Consequently, both KRAS and EGFR mutation results were available in 509 patients. We further excluded 25 cases with advanced NSCLC who had not received palliative chemotherapy in our hospital. As a result, 484 patients with advanced NSCLC were included into the analysis (Fig. 1). KRAS mutations were detected in tumors from 39 (8%) and EGFR in 182 (38%) patients. Two tumors simultaneously had mutations for both KRAS and EGFR (G12V/deletion in exon 19, G12D/L858R). Most KRAS mutations (95%) appeared in codon 12 (13 G12D, 10 G12V, nine G12C, three G12A, one G12S, and one G12K) with one mutation in each codon 13 (G13D) and codon 61 (Q61H). Most EGFR mutations (88%) were typical mutations (103 deletions in exon 19 and 61 L858R mutations in exon 21). The other EGFR mutations were as below: 11 mutations in exon 20 (G796S, S768I, V786M, three duplications, and five insertions), six mutations in exon 18 (three G719A, two S720F, and one G719S), and one L747P mutation in exon 19. The distribution of KRAS mutations was significantly different by smoking status and the amount of smoking in the univariate analysis (Table 1). In the multivariate analysis, the current smoking status was significantly associated with higher KRAS mutation rates (Odds ratio = 2.7; 95% CI: ). Although several clinical characteristics such as sex, histology, smoking status, the amount of smoking were associated with EGFR mutation status in the univariate analysis, only adenocarcinoma was found to be an independent predictor for EGFR mutations (Odds ratio = 5.4, 95% CI: ). Prognostic value of KRAS mutations With median time to follow-up of 30 months, 312 death events were documented. The OS according to clinical characteristics are shown in table 2. In the univariate analysis, women, younger patients (,65 years), never smokers, and patients with adenocarcinoma, relapsed disease after curative operation, KRAS wild type tumors, and EGFR mutation tumors were associated with longer survival. In the multivariate analysis, KRAS mutations (Hazard ratio [HR] = 2.6, 95% CI: ) and stage IV (HR = 1.8, 95% CI: ) were independent predictors of poor prognosis, and EGFR mutations was an independent good prognostic factor (HR = 0.4, 95% CI: ). To evaluate the relationship between KRAS and EGFR mutations in the survival analysis, patients were divided into three groups: KRAS mutations, EGFR mutations, and both wild type groups. Two patients with both KRAS and EGFR mutations were excluded from this analysis. The survival curves of the three groups were well separated (Fig. 2). The median OS for patients with KRAS mutations, EGFR mutations, or both wild types were Table 1. Demographics of Patients with KRAS or EGFR mutation. Factors All cases KRAS mutation EGFR mutation No. No. (%) P No. (%) P All cases (8) 182 (38) Sex Men (9) (27),0.001 Women (7) 106 (52) Age (years), (5) (42) 0.14 $55,, (11) 61 (39) $ (9) 46 (31) Histology Adenocarcinoma (9) (41),0.001 Squamous cell carcinoma 45 1 (2) 5 (11) Others Smoking status Never smoker (6) (50),0.001 Ex-smoker (6) 16 (28) Current smoker (16) 19 (22) Smoking amount (pack-year) Zero (6) (50), , # (5) 40 (32) (14) 25 (20) Clinical stage IIIB 24 2 (8) (21) 0.16 IV (8) 134 (38) Postoperative relapse (9) 43 (42) doi: /journal.pone t001 PLOS ONE 3 May 2013 Volume 8 Issue 5 e64816
4 Table 2. Overall survival by clinical characteristics. Number Median OS (months) P (univariate) Sex Men ,0.001 Women Age (years) $ ,0.001, Smoking status Never ,0.001 Former Current Histology Adenocarcinoma ,0.001 Squamous cell carcinoma Others Clinical stage IIIB IV Postoperative relapse KRAS mutation Yes ,0.001 No EGFR mutations Yes No Abbreviation, OS: overall survival. doi: /journal.pone t , 38.0, and 15.0 months, respectively (P,0.001). The difference in survival among three groups was also seen among patients with adenocarcinoma with median OS of 7.7, 38.0, and 16.1 months, respectively (P,0.001), on the other hand, it was not significant in patients with squamous cell carcinoma due to small number of patients with KRAS mutation (n = 1) or EGFR mutation (n = 5), (Fig. S1). The statistical significance was also maintained in the comparison of OS between the KRAS mutation and KRAS wild type groups among patients with EGFR wild type tumors (P,0.001). Predictive value of KRAS mutations for chemotherapy In total, 321, 275, 112, and 288 patients received pemetrexed-, gemcitabine-, taxane-based regimens, and EGFR TKI, respectively, as the first-, second-, or third-line chemotherapy. The clinical outcomes after each chemotherapeutic regimen according to KRAS mutation status are shown in table 3. The response rates and PFS for the pemetrexed-based regimen in the KRAS mutation group were 14% and 2.1 months, respectively which were lower than those (28% and 3.9 months) in the KRAS wild type group. Even when the pemetrexed-based regimen was divided into pemetrexed monotherapy and pemetrexed plus platinum chemotherapy, clinical outcomes in the KRAS mutation group were inferior to those in the KRAS wild type group. In particular, there was no response to pemetrexed monotherapy in 13 KRAS mutation tumors. For the gemcitabine-based regimen, patients with KRAS mutation showed lower response rates (18% vs. 36%) and shorter PFS (2.4 vs. 4.2 months) than those with KRAS wild type. For the taxane-based regimen, however there was no difference in treatment outcomes according to KRAS mutation status. Even when the treatment outcomes were analyzed in each line of chemotherapy (the first-, second-, or third-line), their associations with KRAS mutation status showed similar trends.while the response rate to EGFR TKI was 56% in the KRAS wild type group, response in the KRAS mutation group was observed only in two (14%) patients (P = 0.002), both of whom had simultaneous EGFR mutations as well as KRAS mutations. The two patients (one with a G12V/deletion in exon 19 and the other with a G12D/L858R mutation) showed partial response to erlotinib and gefitinib with PFS of 17.7 and 7.1 months, respectively. The PFS for EGFR TKI were 1.6 and 7.0 months in the KRAS mutation and wild type groups, respectively (P = 0.003). When the predictive role of KRAS mutations was analyzed among patients with EGFR wild type tumors, the range Figure 2. Overall survival by KRAS and EGFR mutation status. The median overall survivals were 38.0, 7.7, and 15.0 months in the groups of EGFR mutation, KRAS mutation, and both wild types, respectively. doi: /journal.pone g002 PLOS ONE 4 May 2013 Volume 8 Issue 5 e64816
5 Table 3. Response Rates and Progression-free Survival by KRAS Mutation Status. Total No. KRAS mutation KRAS WT P Pemetrexed-based regimen 321 No Response rate 14% 28% 0.12 PFS (months) Pemetrexed monotherapy 166 No Response rate 0 19% 0.08 PFS (months) Pemetrexed plus platinum 155 No Response rate 27% 38% 0.39 PFS (months) First-line pemetrexed 152 No Response rate 25% 38% 0.3 PFS (months) Second-line pemetrexed 107 No Response rate 0 25% 0.07 PFS (months) Third-line pemetrexed 62 No Response rate 0 10% 0.64 PFS (months) Gemcitabine-based regimen 275 No Response rate 18% 36% 0.09 PFS (months) Gemcitabine monotherapy 38 No Response rate 0 13% 0.36 PFS (months) Gemcitabine plus platinum 237 No Response rate 25% 39% 0.25 PFS (months) First-line gemcitabine 238 No Response rate 22% 40% 0.14 PFS (months) Second-line gemcitabine 19 No Response rate 0 6% 0.73 PFS (months) Third-line gemcitabine 18 No Response rate 0 13% 0.6 PFS (months) Taxane-based regimen 112 No Response rate 27% 27% 0.98 PFS (months) Taxane monotherapy 48 No Response rate 20% 9% 0.46 PFS (months) Taxane plus platinum 64 No Response rate 33% 41% 0.7 PFS (months) First-line taxane 52 No Response rate 40% 49% 0.7 PFS (months) Second-line taxane 38 No PLOS ONE 5 May 2013 Volume 8 Issue 5 e64816
6 Table 3. Cont. Total No. KRAS mutation KRAS WT P Response rate 20% 12% 0.63 PFS (months) Third-line taxane 22 No Response rate 0 5% 0.82 PFS (months) EGFR TKI 288 No Response rate 14%* 56% PFS (months) First-line TKI 42 No Response rate N/A 62% N/A PFS (months) N/A 8.7 N/A Second-line TKI 188 No Response rate 25%* 62% 0.04 PFS (months) Third-line TKI 58 No Response rate 0% 31% 0.11 PFS (months) EGFR TKI in EGFR WT group 125 No Response rate 0 18% 0.11 PFS (months) Abbreviation, WT: wild type, PFS: progression-free survival, N/A: not applicable. *Two patients, who showed partial response to TKI in the KRAS mutation group, were also positive for EGFR mutations. doi: /journal.pone t003 of differences in response rates (0% vs. 18%, P = 0.12) and PFS (1.4 vs. 1.8 months, P = 0.09) between the KRAS mutation and wild type groups decreased into the insignificant levels. The clinical outcomes after EGFR TKI were strikingly different according to EGFR mutation status: response rates (83% vs. 16%, P,0.001) and PFS (11.8 vs. 1.8 months, P,0.001) in the EGFR mutation versus wild type groups. However, when it was analyzed Figure 3. Overall survival according to different types of KRAS mutations. There were ten G12V, 13 G12D, nine G12C, and seven others including three G12A, one G12S, one G12K, one G13D, and one Q61H. doi: /journal.pone g003 after EGFR mutations being divided into typical (deletion in exon 19 and L858R) and atypical mutations, only two (G719A, G796S) out of 18 patients with atypical mutations achieved objective response to EGFR TKI. Clinical outcomes according to KRAS mutation types While 62% (8/13) of patients with G12D type were never smokers, only 27% of patients with other KRAS mutation types were never smokers (P = 0.04). When the OS was analyzed after grouping the patients according to four types of KRAS mutations (G12D, G12V, G12C, and the other), the median OS were not different among four groups with the values of 8.1, 9.6, 7.7, and 5.5 months, respectively (P = 0.12), (Fig. 3). In addition, there was no difference in PFS for EGFR TKI therapy according to the KRAS genotypes (P = 0.73). Regarding the response for pemetrexed-based chemotherapy, there was one response (11%, respectively) in each of nine G12V and G12D mutations, zero in seven of G12C, and two responses in the other types. Discussion The present study shows that KRAS mutations are an independent predictor of poor prognosis in patients with advanced NSCLC. However, KRAS mutation status has no role in predicting the clinical outcomes after cytotoxic chemotherapy and is at most a weak predictor regarding EGFR TKI therapy when EGFR mutation status is also considered. Since KRAS mutation was first found in human lung cancer in 1984 [23], much effort has been expended to evaluate its clinical implication. A meta-analysis identified KRAS mutations as a negative prognostic factor [13]. In addition, it was shown that OS PLOS ONE 6 May 2013 Volume 8 Issue 5 e64816
7 in the KRAS mutation group was significantly poorer than those in the EGFR mutation or in both wild groups with completely resected lung adenocarcinoma [14]. However, a LACE-bio study, which included 1543 patients who had been enrolled into four randomized trials of adjuvant chemotherapy for completely resected NSCLC, recently suggested that KRAS mutations have no prognostic role in patients with completely resected NSCLC [17]. Among many studies with contradictory results, the present study has the merits with a well identified homogeneous study population, analysis controlling for EGFR mutation status, the relatively adequate sample size, and comprehensive analysis on prognostic and predictive values. While there is no definite relationship between KRAS mutation status and EGFR monoclonal antibody (cetuximab) in advanced NSCLC [10], whether KRAS mutations can predict EGFR TKI response has been contentious. Although many studies noted poorer clinical outcomes after EGFR TKI therapy in the KRAS mutation group compared in the KRAS wild type group [7,9,18,20], that was refuted by findings that KRAS mutation status has no effect on clinical outcomes to EGFR TKI therapy in analysis of patients with EGFR wild types [21]. In our study, although KRAS mutation seemed to predict EGFR TKI responsiveness (KRAS mutation vs. KRAS wild type: 14% vs. 56%, P = 0.002) in the entire study population including patients with or without EGFR mutation, the predicting power of KRAS mutations decreased when EGFR mutation status was also considered. An interesting observation is that there were 20 responses (18%) in 113 patients with both KRAS and EGFR wild type tumors, while there was no response in 12 patients with KRAS mutation and EGFR wild type tumors. The noticeable responses to EGFR TKI in the EGFR wild group could in part be explained by the relatively low sensitivity of direct sequencing EGFR mutation test as noted in a previous study [24]. It suggests that the KRAS mutations have a role as negative selection biomarker for EGFR TKI therapy when the sensitivity of the EGFR mutation test is relatively low. The irrelevance of KRAS mutations to EGFR TKI responsiveness was directly demonstrated from two cases with both KRAS and EGFR mutations in our study. These two patients achieved durable objective response with EGFR TKIs. The tissues for KRAS and EGFR mutation tests were biopsied at the time of diagnosis; therefore the mutations were de novo in these two patients. Although KRAS and EGFR mutations are known to be mutually exclusive, several episodic cases with both mutations were reported [7,21,25]. However, to the best of our knowledge, the clinical outcomes to EGFR TKI in patients with tumors harboring both mutations have been unknown and our study presents the first report of these findings. In addition to EGFR TKI, the clinical outcomes to other cytotoxic chemotherapeutic regimens could not be predicted by KRAS mutation status. Contrary to the preclinical data reporting that tumors with KRAS mutations, at least the specific genotype such as G12C, would be more sensitive to pemetrexed [22,26], patients with KRAS mutations showed inferior treatment outcomes to the pemetrexed-based regimen compared with those with KRAS wild types, irrespective of KRAS genotypes. In addition, KRAS mutations tended to be associated with poor References 1. Mok TS, Wu YL, Thongprasert S, Yang CH, Chu DT, et al. (2009) Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma. N Engl J Med 361: Maemondo M, Inoue A, Kobayashi K, Sugawara S, Oizumi S, et al. (2010) Gefitinib or chemotherapy for non-small-cell lung cancer with mutated EGFR. N Engl J Med 362: treatment outcomes to gemcitabine-based chemotherapy. The overall poor treatment outcomes in the KRAS mutation group to chemotherapeutic regimens seemed to be caused by the negative prognostic value rather than by the negative predictive value of KRAS mutations for specific regimens. It is hypothesized that different KRAS mutations may have different epidemiologic data, sensitivity to chemotherapy, and survival outcomes. Consistent with a previous report [27], G12D genotype was common in never smokers compared with other genotypes in the present study. Although patients with KRAS genotypes such as G12V or G12C were reported to have poor survival outcome with G12D in previous studies [28,29], the survival outcomes were not different according to KRAS genotypes in our study. However, the clinical implication of different genotypes is hard to be determined in the present study due to the small sample size. The present study has several limitations. First, this retrospective study included a cohort who had been tested for KRAS and EGFR mutations in clinical practice which consisted of more women and never smokers. Although this selection bias of the study population could explain the relatively low KRAS mutation rate in our data, the difference from the true value may be small when considering low KRAS mutation rate in Asian population [8]. Secondly, we reviewed chemotherapeutic regimens which were administered as the first-, second-, and third-line therapy. As a result, it was possible that the treatment outcomes after various regimens could be affected by the lines of chemotherapy. However, even when it was analyzed in each line of chemotherapy, the relationship between treatment outcomes and KRAS mutation status was not changed as shown in table 3. Therefore, we do not suspect the heterogeneity of chemotherapy lines had any effects on the analysis of predictive role of KRAS mutations. This study identified KRAS mutations as an independent prognostic marker but as having a limited role in predicting the treatment outcomes after EGFR TKI or cytotoxic chemotherapy. Based on our observations, patients with KRAS mutant NSCLC could be categorized as a specific group characterized as having poor prognosis without remarkable outcomes to any chemotherapeutic regimen. Although it has not been yet proved clinically, development of agents to inhibit KRAS pathway has been actively pursued [30 32]. Further efforts are urgently needed to improve the clinical outcomes of patients with KRAS mutant NSCLC. Supporting Information Figure S1 Overall survival by KRAS mutation status in patients with adenocarcinoma (a) and squamous cell carcinoma (b). The difference in survival was significant among patients with adenocarcinoma, on the other hand, it was not significant in patients with squamous cell carcinoma. (TIF) Author Contributions Conceived and designed the experiments: JMS KP. Performed the experiments: JMS DWH KP. Analyzed the data: JMS DWH. Contributed reagents/materials/analysis tools: JMS JSA MJA KP. Wrote the paper: JMS KP. 3. Mitsudomi T, Morita S, Yatabe Y, Negoro S, Okamoto I, et al. (2010) Gefitinib versus cisplatin plus docetaxel in patients with non-small-cell lung cancer harbouring mutations of the epidermal growth factor receptor (WJTOG3405): an open label, randomised phase 3 trial. Lancet Oncol 11: Zhou CC, Wu YL, Chen GY, Feng JF, Liu XQ, et al. (2011) Erlotinib versus chemotherapy as first-line treatment for patients with advanced EGFR PLOS ONE 7 May 2013 Volume 8 Issue 5 e64816
8 mutation-positive non-small-cell lung cancer (OPTIMAL, CTONG-0802): a multicentre, open-label, randomised, phase 3 study. Lancet Oncol 12: Rosell R, Carcereny E, Gervais R, Vergnenegre A, Massuti B, et al. (2012) Erlotinib versus standard chemotherapy as first-line treatment for European patients with advanced EGFR mutation-positive non-small-cell lung cancer (EURTAC): a multicentre, open-label, randomised phase 3 trial. Lancet Oncol 13: Schiller JH, Adak S, Feins RH, Keller SM, Fry WA, et al. (2001) Lack of prognostic significance of p53 and K-ras mutations in primary resected nonsmall-cell lung cancer on E4592: a Laboratory Ancillary Study on an Eastern Cooperative Oncology Group Prospective Randomized Trial of Postoperative Adjuvant Therapy. J Clin Oncol 19: Eberhard DA, Johnson BE, Amler LC, Goddard AD, Heldens SL, et al. (2005) Mutations in the epidermal growth factor receptor and in KRAS are predictive and prognostic indicators in patients with non-small-cell lung cancer treated with chemotherapy alone and in combination with erlotinib. J Clin Oncol 23: Shigematsu H, Lin L, Takahashi T, Nomura M, Suzuki M, et al. (2005) Clinical and biological features associated with epidermal growth factor receptor gene mutations in lung cancers. J Natl Cancer Inst 97: Massarelli E, Varella-Garcia M, Tang X, Xavier AC, Ozburn NC, et al. (2007) KRAS mutation is an important predictor of resistance to therapy with epidermal growth factor receptor tyrosine kinase inhibitors in non-small-cell lung cancer. Clin Cancer Res 13: O Byrne KJ, Gatzemeier U, Bondarenko I, Barrios C, Eschbach C, et al. (2011) Molecular biomarkers in non-small-cell lung cancer: a retrospective analysis of data from the phase 3 FLEX study. Lancet Oncol 12: Douillard JY, Shepherd FA, Hirsh V, Mok T, Socinski MA, et al. (2010) Molecular predictors of outcome with gefitinib and docetaxel in previously treated non-small-cell lung cancer: data from the randomized phase III INTEREST trial. J Clin Oncol 28: Slebos RJ, Kibbelaar RE, Dalesio O, Kooistra A, Stam J, et al. (1990) K-ras oncogene activation as a prognostic marker in adenocarcinoma of the lung. N Engl J Med 323: Mascaux C, Iannino N, Martin B, Paesmans M, Berghmans T, et al. (2005) The role of RAS oncogene in survival of patients with lung cancer: a systematic review of the literature with meta-analysis. Br J Cancer 92: Marks JL, Broderick S, Zhou Q, Chitale D, Li AR, et al. (2008) Prognostic and therapeutic implications of EGFR and KRAS mutations in resected lung adenocarcinoma. J Thorac Oncol 3: Tsao MS, Aviel-Ronen S, Ding K, Lau D, Liu N, et al. (2007) Prognostic and predictive importance of p53 and RAS for adjuvant chemotherapy in non smallcell lung cancer. J Clin Oncol 25: Butts CA, Ding K, Seymour L, Twumasi-Ankrah P, Graham B, et al. (2010) Randomized phase III trial of vinorelbine plus cisplatin compared with observation in completely resected stage IB and II non-small-cell lung cancer: updated survival analysis of JBR-10. J Clin Oncol 28: Shepherd FA, Bourredjem A, Brambilla E, Domerg C, Douillard JY, et al. (2012) Prognostic and predictive effects of KRAS mutation subtype in completely resected non-small cell lung cancer (NSCLC): A LACE-bio study. ASCO Meeting Abstracts 30: Pao W, Wang TY, Riely GJ, Miller VA, Pan Q, et al. (2005) KRAS mutations and primary resistance of lung adenocarcinomas to gefitinib or erlotinib. PLoS Med 2: e Linardou H, Dahabreh IJ, Kanaloupiti D, Siannis F, Bafaloukos D, et al. (2008) Assessment of somatic k-ras mutations as a mechanism associated with resistance to EGFR-targeted agents: a systematic review and meta-analysis of studies in advanced non-small-cell lung cancer and metastatic colorectal cancer. Lancet Oncol 9: Mao C, Qiu LX, Liao RY, Du FB, Ding H, et al. (2010) KRAS mutations and resistance to EGFR-TKIs treatment in patients with non-small cell lung cancer: a meta-analysis of 22 studies. Lung Cancer 69: Jackman DM, Miller VA, Cioffredi LA, Yeap BY, Janne PA, et al. (2009) Impact of epidermal growth factor receptor and KRAS mutations on clinical outcomes in previously untreated non-small cell lung cancer patients: results of an online tumor registry of clinical trials. Clin Cancer Res 15: Moran DM, Trusk P, Shell SA, Camidge DR, Doebele RC, et al. (2012) Abstract LB-449: KRAS mutation and amplification status predicts sensitivity to antifolate therapies in non-small-cell lung cancer. Cancer Research 72: LB Santos E, Martin-Zanca D, Reddy EP, Pierotti MA, Della Porta G, et al. (1984) Malignant activation of a K-ras oncogene in lung carcinoma but not in normal tissue of the same patient. Science 223: Querings S, Altmuller J, Ansen S, Zander T, Seidel D, et al. (2011) Benchmarking of mutation diagnostics in clinical lung cancer specimens. PLoS One 6: e Zhu CQ, da Cunha Santos G, Ding K, Sakurada A, Cutz JC, et al. (2008) Role of KRAS and EGFR as biomarkers of response to erlotinib in National Cancer Institute of Canada Clinical Trials Group Study BR.21. J Clin Oncol 26: Garassino MC, Marabese M, Rusconi P, Rulli E, Martelli O, et al. (2011) Different types of K-Ras mutations could affect drug sensitivity and tumour behaviour in non-small-cell lung cancer. Ann Oncol 22: Riely GJ, Kris MG, Rosenbaum D, Marks J, Li A, et al. (2008) Frequency and distinctive spectrum of KRAS mutations in never smokers with lung adenocarcinoma. Clin Cancer Res 14: Ihle NT, Byers LA, Kim ES, Saintigny P, Lee JJ, et al. (2012) Effect of KRAS oncogene substitutions on protein behavior: implications for signaling and clinical outcome. J Natl Cancer Inst 104: Keohavong P, DeMichele MA, Melacrinos AC, Landreneau RJ, Weyant RJ, et al. (1996) Detection of K-ras mutations in lung carcinomas: relationship to prognosis. Clin Cancer Res 2: Riely GJ, Johnson ML, Medina C, Rizvi NA, Miller VA, et al. (2011) A phase II trial of Salirasib in patients with lung adenocarcinomas with KRAS mutations. J Thorac Oncol 6: Gilmartin AG, Bleam MR, Groy A, Moss KG, Minthorn EA, et al. (2011) GSK (JTP-74057) is an inhibitor of MEK activity and activation with favorable pharmacokinetic properties for sustained in vivo pathway inhibition. Clin Cancer Res 17: Davies BR, Logie A, McKay JS, Martin P, Steele S, et al. (2007) AZD6244 (ARRY ), a potent inhibitor of mitogen-activated protein kinase/ extracellular signal-regulated kinase kinase 1/2 kinases: mechanism of action in vivo, pharmacokinetic/pharmacodynamic relationship, and potential for combination in preclinical models. Mol Cancer Ther 6: PLOS ONE 8 May 2013 Volume 8 Issue 5 e64816
EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence
 102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
RESEARCH ARTICLE. Ryosuke Hirano 1, Junji Uchino 1 *, Miho Ueno 2, Masaki Fujita 1, Kentaro Watanabe 1. Abstract. Introduction
 RESEARCH ARTICLE Low-dose Epidermal Growth Factor Receptor (EGFR)- Tyrosine Kinase Inhibition of EGFR Mutation-positive Lung Cancer: Therapeutic Benefits and Associations Between Dosage, Efficacy and Body
RESEARCH ARTICLE Low-dose Epidermal Growth Factor Receptor (EGFR)- Tyrosine Kinase Inhibition of EGFR Mutation-positive Lung Cancer: Therapeutic Benefits and Associations Between Dosage, Efficacy and Body
Frequency of Epidermal Growth Factor Mutation Status and Its Effect on Outcome of Patients with Adenocarcinoma of the Lung
 Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective
 Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients
 (2017) 1(1): 16-24 Mini Review Open Access Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients Chao Pui I 1,3, Cheng Gregory 1, Zhang Lunqing 2, Lo Iek
(2017) 1(1): 16-24 Mini Review Open Access Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients Chao Pui I 1,3, Cheng Gregory 1, Zhang Lunqing 2, Lo Iek
Original Article. Abstract
 Japanese Journal of Clinical Oncology, 2015, 45(7) 670 676 doi: 10.1093/jjco/hyv054 Advance Access Publication Date: 15 April 2015 Original Article Original Article Efficacy of chemotherapy after first-line
Japanese Journal of Clinical Oncology, 2015, 45(7) 670 676 doi: 10.1093/jjco/hyv054 Advance Access Publication Date: 15 April 2015 Original Article Original Article Efficacy of chemotherapy after first-line
Changing demographics of smoking and its effects during therapy
 Changing demographics of smoking and its effects during therapy Egbert F. Smit MD PhD. Dept. Pulmonary Diseases, Vrije Universiteit Medical Centre, Amsterdam, The Netherlands Smoking prevalence adults
Changing demographics of smoking and its effects during therapy Egbert F. Smit MD PhD. Dept. Pulmonary Diseases, Vrije Universiteit Medical Centre, Amsterdam, The Netherlands Smoking prevalence adults
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Survival outcome according to KRAS mutation status in newly diagnosed patients with stage IV non-small cell
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Survival outcome according to KRAS mutation status in newly diagnosed patients with stage IV non-small cell
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW. Erlotinib for the third or fourth-line treatment of NSCLC January 2012
 Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Introduction ORIGINAL ARTICLE
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival analysis of patients with advanced non-small cell lung cancer receiving tyrosine kinase inhibitor (TKI) treatment: A multi-center retrospective
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival analysis of patients with advanced non-small cell lung cancer receiving tyrosine kinase inhibitor (TKI) treatment: A multi-center retrospective
Personalized maintenance therapy in advanced non-small cell lung cancer
 China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
EGFR mutations in early-stage and advanced-stage lung adenocarcinoma: Analysis based on large-scale data from China
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE EGFR s in early-stage and advanced-stage lung adenocarcinoma: Analysis based on large-scale data from China Can Pi 1,2*, Chong-Rui Xu 2*, Ming-feng Zhang
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE EGFR s in early-stage and advanced-stage lung adenocarcinoma: Analysis based on large-scale data from China Can Pi 1,2*, Chong-Rui Xu 2*, Ming-feng Zhang
Yan Zhang 1*, Zheng Wang 2*, Xuezhi Hao 1, Xingsheng Hu 1, Hongyu Wang 1, Yan Wang 1, Jianming Ying 3. Original Article. Abstract
 Original Article Clinical characteristics and response to tyrosine kinase inhibitors of patients with non-small cell lung cancer harboring uncommon epidermal growth factor receptor mutations Yan Zhang
Original Article Clinical characteristics and response to tyrosine kinase inhibitors of patients with non-small cell lung cancer harboring uncommon epidermal growth factor receptor mutations Yan Zhang
Test Category: Prognostic and Predictive. Clinical Scenario
 Use of Epidermal Growth Factor Receptor (EGFR) Mutation Analysis in Patients with Advanced Non-Small-Cell Lung Cancer (NSCLC) to Determine Erlotinib Use as First-line Therapy Test Category: Prognostic
Use of Epidermal Growth Factor Receptor (EGFR) Mutation Analysis in Patients with Advanced Non-Small-Cell Lung Cancer (NSCLC) to Determine Erlotinib Use as First-line Therapy Test Category: Prognostic
Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007
 Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007 Bruce E. Johnson, MD Dana-Farber Cancer Institute, Brigham and Women s Hospital, and Harvard
Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007 Bruce E. Johnson, MD Dana-Farber Cancer Institute, Brigham and Women s Hospital, and Harvard
Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease Treated with High-Dose Radiotherapy
 Lung Cancer International Volume 2012, Article ID 587424, 6 pages doi:10.1155/2012/587424 Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease
Lung Cancer International Volume 2012, Article ID 587424, 6 pages doi:10.1155/2012/587424 Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease
Ludger Sellmann 1, Klaus Fenchel 2, Wolfram C. M. Dempke 3,4. Editorial
 Editorial Improved overall survival following tyrosine kinase inhibitor treatment in advanced or metastatic non-small-cell lung cancer the Holy Grail in cancer treatment? Ludger Sellmann 1, Klaus Fenchel
Editorial Improved overall survival following tyrosine kinase inhibitor treatment in advanced or metastatic non-small-cell lung cancer the Holy Grail in cancer treatment? Ludger Sellmann 1, Klaus Fenchel
Mutation and prognostic analyses of PIK3CA in patients with completely resected lung adenocarcinoma
 Cancer Medicine ORIGINAL RESEARCH Open Access Mutation and prognostic analyses of PIK3CA in patients with completely resected lung adenocarcinoma Zhengbo Song 1,2, Xinmin Yu 1 & Yiping Zhang 1,2 1 Department
Cancer Medicine ORIGINAL RESEARCH Open Access Mutation and prognostic analyses of PIK3CA in patients with completely resected lung adenocarcinoma Zhengbo Song 1,2, Xinmin Yu 1 & Yiping Zhang 1,2 1 Department
Introduction. pissn , eissn Open Access. Original Article
 pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 215;47(4):63-637 Original Article http://dx.doi.org/1.4143/crt.214.244 Open Access Pemetrexed Singlet Versus Nonpemetrexed-Based Platinum Doublet as Second-Line
pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 215;47(4):63-637 Original Article http://dx.doi.org/1.4143/crt.214.244 Open Access Pemetrexed Singlet Versus Nonpemetrexed-Based Platinum Doublet as Second-Line
Adenocarcinoma of the lung is the leading cause of cancerrelated
 ORIGINAL ARTICLE Prognostic and Therapeutic Implications of EGFR and KRAS Mutations in Resected Lung Adenocarcinoma Jenifer L. Marks, MD,* Stephen Broderick, MD, Qin Zhou, MA, Dhananjay Chitale, MD, Allan
ORIGINAL ARTICLE Prognostic and Therapeutic Implications of EGFR and KRAS Mutations in Resected Lung Adenocarcinoma Jenifer L. Marks, MD,* Stephen Broderick, MD, Qin Zhou, MA, Dhananjay Chitale, MD, Allan
Epidermal growth factor receptor mutation and pattern of brain metastasis in patients with nonsmall cell lung cancer
 ORIGINAL ARTICLE Korean J Intern Med 218;33:168-175 https://doi.org/1.394/kjim.215.158 Epidermal growth factor receptor mutation and pattern of brain metastasis in patients with nonsmall cell lung cancer
ORIGINAL ARTICLE Korean J Intern Med 218;33:168-175 https://doi.org/1.394/kjim.215.158 Epidermal growth factor receptor mutation and pattern of brain metastasis in patients with nonsmall cell lung cancer
MOLECULAR AND CLINICAL ONCOLOGY 4: , 2016
 774 Elevated levels of plasma lactate dehydrogenase is an unfavorable prognostic factor in patients with epidermal growth factor receptor mutation positive non small cell lung cancer, receiving treatment
774 Elevated levels of plasma lactate dehydrogenase is an unfavorable prognostic factor in patients with epidermal growth factor receptor mutation positive non small cell lung cancer, receiving treatment
EGFR inhibitors in NSCLC
 Suresh S. Ramalingam, MD Associate Professor Director of Medical Oncology Emory University i Winship Cancer Institute EGFR inhibitors in NSCLC Role in 2nd/3 rd line setting Role in first-line and maintenance
Suresh S. Ramalingam, MD Associate Professor Director of Medical Oncology Emory University i Winship Cancer Institute EGFR inhibitors in NSCLC Role in 2nd/3 rd line setting Role in first-line and maintenance
K-Ras signalling in NSCLC
 Targeting the Ras-Raf-Mek-Erk pathway Egbert F. Smit MD PhD Dept. Pulmonary Diseases Vrije Universiteit VU Medical Centre Amsterdam, The Netherlands K-Ras signalling in NSCLC Sun et al. Nature Rev. Cancer
Targeting the Ras-Raf-Mek-Erk pathway Egbert F. Smit MD PhD Dept. Pulmonary Diseases Vrije Universiteit VU Medical Centre Amsterdam, The Netherlands K-Ras signalling in NSCLC Sun et al. Nature Rev. Cancer
Page: 1 of 27. Molecular Analysis for Targeted Therapy of Non-Small-Cell Lung Cancer
 Last Review Status/Date: December 2014 Page: 1 of 27 Non-Small-Cell Lung Cancer Description Over half of patients with non-small-cell lung cancer (NSCLC) present with advanced and therefore incurable disease,
Last Review Status/Date: December 2014 Page: 1 of 27 Non-Small-Cell Lung Cancer Description Over half of patients with non-small-cell lung cancer (NSCLC) present with advanced and therefore incurable disease,
Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients: Patient Characteristics and Type of Chemotherapy
 SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
Shaohua Cui, Liwen Xiong, Yuqing Lou, Huangping Shi, Aiqin Gu, Yizhuo Zhao, Tianqing Chu, Huimin Wang, Wei Zhang, Lili Dong, Liyan Jiang
 Original Article Factors that predict progression-free survival in Chinese lung adenocarcinoma patients treated with epidermal growth factor receptor tyrosine kinase inhibitors Shaohua Cui, Liwen Xiong,
Original Article Factors that predict progression-free survival in Chinese lung adenocarcinoma patients treated with epidermal growth factor receptor tyrosine kinase inhibitors Shaohua Cui, Liwen Xiong,
Lihong Ma 1 *, Zhengbo Song 2 *, Yong Song 1, Yiping Zhang 2. Original Article
 Original Article MET overexpression coexisting with epidermal growth factor receptor mutation influence clinical efficacy of EGFR-tyrosine kinase inhibitors in lung adenocarcinoma patients Lihong Ma 1
Original Article MET overexpression coexisting with epidermal growth factor receptor mutation influence clinical efficacy of EGFR-tyrosine kinase inhibitors in lung adenocarcinoma patients Lihong Ma 1
Comparison of Gefitinib versus Docetaxel in Patients with Pre-Treated Non-Small Cell Lung Cancer (NSCLC)
 J Lung Cancer 2009;8(2):61-66 Comparison of Gefitinib versus Docetaxel in Patients with Pre-Treated Non-Small Cell Lung Cancer (NSCLC) More effective treatments in first, second, and third-line of metastatic
J Lung Cancer 2009;8(2):61-66 Comparison of Gefitinib versus Docetaxel in Patients with Pre-Treated Non-Small Cell Lung Cancer (NSCLC) More effective treatments in first, second, and third-line of metastatic
PRACTICE GUIDELINE SERIES
 ELLIS et al. PRACTICE GUIDELINE SERIES The role of the epidermal growth factor receptor tyrosine kinase inhibitors as therapy for advanced, metastatic, and recurrent nonsmall-cell lung cancer: a Canadian
ELLIS et al. PRACTICE GUIDELINE SERIES The role of the epidermal growth factor receptor tyrosine kinase inhibitors as therapy for advanced, metastatic, and recurrent nonsmall-cell lung cancer: a Canadian
First line erlotinib for NSCLC patients not selected by EGFR mutation: keep carrying the TORCH or time to let the flame die?
 Perspective First line erlotinib for NSCLC patients not selected by EGFR mutation: keep carrying the TORCH or time to let the flame die? Jared Weiss Multidisciplinary Thoracic Oncology Program, Lineberger
Perspective First line erlotinib for NSCLC patients not selected by EGFR mutation: keep carrying the TORCH or time to let the flame die? Jared Weiss Multidisciplinary Thoracic Oncology Program, Lineberger
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC. Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy
 PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
Improving outcomes for NSCLC patients with brain metastases
 Improving outcomes for NSCLC patients with brain metastases Martin Schuler West German Cancer Center, Essen, Germany In Switzerland, afatinib is approved as monotherapy for patients with non-small cell
Improving outcomes for NSCLC patients with brain metastases Martin Schuler West German Cancer Center, Essen, Germany In Switzerland, afatinib is approved as monotherapy for patients with non-small cell
ORIGINAL ARTICLE. Oncology and Translational Medicine DOI /s Abstract
 Oncology and Translational Medicine DOI 10.1007/s10330-018-0281-1 August 2018, Vol. 4, No. 4, P158 P162 ORIGINAL ARTICLE Treatment and survival status of patients with EGFR mutation-positive stage IV lung
Oncology and Translational Medicine DOI 10.1007/s10330-018-0281-1 August 2018, Vol. 4, No. 4, P158 P162 ORIGINAL ARTICLE Treatment and survival status of patients with EGFR mutation-positive stage IV lung
Thoracic and head/neck oncology new developments
 Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Additional clinical features of this patient include:
 *Not an actual patient. Challenge your knowledge of biomarker testing in advanced NSCLC. Consider this case study of disease progression following chemotherapy, with insightful commentary from Dr Edward
*Not an actual patient. Challenge your knowledge of biomarker testing in advanced NSCLC. Consider this case study of disease progression following chemotherapy, with insightful commentary from Dr Edward
Introduction. Methods. Patient and study design
 Original Article Continuation of gefitinib plus chemotherapy prolongs progressionfree survival in advanced non-small cell lung cancer patients who get acquired resistance to gefitinib without T790M mutations
Original Article Continuation of gefitinib plus chemotherapy prolongs progressionfree survival in advanced non-small cell lung cancer patients who get acquired resistance to gefitinib without T790M mutations
There has been a growing interest in lung cancer in neversmokers,
 ORIGINAL ARTICLE,, and Time of Diagnosis Are Important Factors for Prognosis Analysis of 1499 Never-Smokers with Advanced Non-small Cell Lung Cancer in Japan Tomoya Kawaguchi, MD,* Minoru Takada, MD,*
ORIGINAL ARTICLE,, and Time of Diagnosis Are Important Factors for Prognosis Analysis of 1499 Never-Smokers with Advanced Non-small Cell Lung Cancer in Japan Tomoya Kawaguchi, MD,* Minoru Takada, MD,*
Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Original Policy Date
 MP 2.04.34 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last
MP 2.04.34 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last
RESEARCH ARTICLE. EGFR Mutation Genotype Impact on the Efficacy of Pemetrexed in Patients with Non-squamous Non-small Cell Lung Cancer
 RESEARCH ARTICLE EGFR Mutation Genotype Impact on the Efficacy of Pemetrexed in Patients with Non-squamous Non-small Cell Lung Cancer Satoshi Igawa 1 *, Yuichi Sato 2, Mikiko Ishihara 1, Masashi Kasajima
RESEARCH ARTICLE EGFR Mutation Genotype Impact on the Efficacy of Pemetrexed in Patients with Non-squamous Non-small Cell Lung Cancer Satoshi Igawa 1 *, Yuichi Sato 2, Mikiko Ishihara 1, Masashi Kasajima
Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China Yu-Tao Liu, Xue-Zhi Hao, Jun-Ling Li, Xing-Sheng
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China Yu-Tao Liu, Xue-Zhi Hao, Jun-Ling Li, Xing-Sheng
Prognosis of recurrent non small cell lung cancer following complete resection
 1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
T he utility of epidermal growth factor receptor tyrosine kinase inhibitors (EGFR-TKIs) in metastatic nonsmall
 OPEN SUBJECT AREAS: NON-SMALL-CELL LUNG CANCER TARGETED THERAPIES Received 30 April 2014 Accepted 15 July 2014 Published 8 August 2014 Correspondence and requests for materials should be addressed to H.L.
OPEN SUBJECT AREAS: NON-SMALL-CELL LUNG CANCER TARGETED THERAPIES Received 30 April 2014 Accepted 15 July 2014 Published 8 August 2014 Correspondence and requests for materials should be addressed to H.L.
2 nd line Therapy and Beyond NSCLC. Alan Sandler, M.D. Oregon Health & Science University
 2 nd line Therapy and Beyond NSCLC Alan Sandler, M.D. Oregon Health & Science University Treatment options for advanced or metastatic (stage IIIb/IV) NSCLC Suitable for chemotherapy Diagnosis Unsuitable/unwilling
2 nd line Therapy and Beyond NSCLC Alan Sandler, M.D. Oregon Health & Science University Treatment options for advanced or metastatic (stage IIIb/IV) NSCLC Suitable for chemotherapy Diagnosis Unsuitable/unwilling
Kirsten rat sarcoma viral oncogene homolog (KRAS) mutation
 ORIGINAL ARTICLE KRAS Mutations in Advanced Nonsquamous Non Small- Cell Lung Cancer Patients Treated with First-Line Platinum- Based Chemotherapy Have No Predictive Value Wouter W. Mellema, MD,* Anne-Marie
ORIGINAL ARTICLE KRAS Mutations in Advanced Nonsquamous Non Small- Cell Lung Cancer Patients Treated with First-Line Platinum- Based Chemotherapy Have No Predictive Value Wouter W. Mellema, MD,* Anne-Marie
Correspondence should be addressed to Kumar Prabhash;
 Hindawi Chemotherapy Research and Practice Volume 2017, Article ID 8196434, 4 pages https://doi.org/10.1155/2017/8196434 Clinical Study Efficacy of Second-Line Pemetrexed-Carboplatin in EGFR-Activating
Hindawi Chemotherapy Research and Practice Volume 2017, Article ID 8196434, 4 pages https://doi.org/10.1155/2017/8196434 Clinical Study Efficacy of Second-Line Pemetrexed-Carboplatin in EGFR-Activating
Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors
 Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors Conor E. Steuer, MD Assistant Professor The Winship Cancer Institute of Emory University July 27, 2017 1 Lung Cancer One
Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors Conor E. Steuer, MD Assistant Professor The Winship Cancer Institute of Emory University July 27, 2017 1 Lung Cancer One
Lung cancer represents the leading cause of death from
 ORIGINAL ARTICLE Epidermal Growth Factor Receptor Tyrosine Kinase Inhibitors Beyond Progressive Disease A Retrospective Analysis for Japanese Patients with Activating EGFR Mutations Kenichi Nishie, MD,*
ORIGINAL ARTICLE Epidermal Growth Factor Receptor Tyrosine Kinase Inhibitors Beyond Progressive Disease A Retrospective Analysis for Japanese Patients with Activating EGFR Mutations Kenichi Nishie, MD,*
Targeted Agents as Maintenance Therapy. Karen Kelly, MD Professor of Medicine UC Davis Cancer Center
 Targeted Agents as Maintenance Therapy Karen Kelly, MD Professor of Medicine UC Davis Cancer Center Disclosures Genentech Advisory Board Maintenance Therapy Defined Treatment Non-Progressing Patients Drug
Targeted Agents as Maintenance Therapy Karen Kelly, MD Professor of Medicine UC Davis Cancer Center Disclosures Genentech Advisory Board Maintenance Therapy Defined Treatment Non-Progressing Patients Drug
Joachim Aerts Erasmus MC Rotterdam, Netherlands. Drawing the map: molecular characterization of NSCLC
 Joachim Aerts Erasmus MC Rotterdam, Netherlands Drawing the map: molecular characterization of NSCLC Disclosures Honoraria for advisory board/consultancy/speakers fee Eli Lilly Roche Boehringer Ingelheim
Joachim Aerts Erasmus MC Rotterdam, Netherlands Drawing the map: molecular characterization of NSCLC Disclosures Honoraria for advisory board/consultancy/speakers fee Eli Lilly Roche Boehringer Ingelheim
ORIGINAL ARTICLE. Received 4 August 2015; revised 16 November 2015; accepted 20 November Journal of Thoracic Oncology Vol. - No.
 ORIGINAL ARTICLE First-Line Pemetrexed plus Cisplatin followed by Gefitinib Maintenance Therapy versus Gefitinib Monotherapy in East Asian Never-Smoker Patients with Locally Advanced or Metastatic Nonsquamous
ORIGINAL ARTICLE First-Line Pemetrexed plus Cisplatin followed by Gefitinib Maintenance Therapy versus Gefitinib Monotherapy in East Asian Never-Smoker Patients with Locally Advanced or Metastatic Nonsquamous
East meets West: ethnic differences in epidemiology and clinical behaviors of lung cancer between East Asians and Caucasians
 East meets West: ethnic differences in epidemiology and clinical behaviors of lung cancer between East Asians and Caucasians The Harvard community has made this article openly available. Please share how
East meets West: ethnic differences in epidemiology and clinical behaviors of lung cancer between East Asians and Caucasians The Harvard community has made this article openly available. Please share how
Protocol. Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC)
 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) (20445) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) (20445) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
Supplementary Online Content
 Supplementary Online Content Kris MG, Johnson BE, Berry LD, et al. Using Multiplexed Assays of Oncogenic Drivers in Lung Cancers to Select Targeted Drugs. JAMA. doi:10.1001/jama.2014.3741 etable 1. Trials
Supplementary Online Content Kris MG, Johnson BE, Berry LD, et al. Using Multiplexed Assays of Oncogenic Drivers in Lung Cancers to Select Targeted Drugs. JAMA. doi:10.1001/jama.2014.3741 etable 1. Trials
Treatment of EGFR mutant advanced NSCLC
 Treatment of EGFR mutant advanced NSCLC Raffaele Califano Department of Medical Oncology The Christie and Manchester University Hospital Manchester, UK Outline Data on first-line Overcoming T790M mutation
Treatment of EGFR mutant advanced NSCLC Raffaele Califano Department of Medical Oncology The Christie and Manchester University Hospital Manchester, UK Outline Data on first-line Overcoming T790M mutation
Cheng-Zhi Zhou*, Yin-Yin Qin*, Zhan-Hong Xie, Jie-Xia Zhang, Ming Ou-Yang, Shi-Yue Li, Rong- Chang Chen
 Original Article Efficacy of third-line pemetrexed monotherapy versus pemetrexed combination with bevacizumab in patients with advanced EGFR mutation-positive lung adenocarcinoma Cheng-Zhi Zhou*, Yin-Yin
Original Article Efficacy of third-line pemetrexed monotherapy versus pemetrexed combination with bevacizumab in patients with advanced EGFR mutation-positive lung adenocarcinoma Cheng-Zhi Zhou*, Yin-Yin
Postoperative survival of EGFR-TKI-targeted therapy in non-small cell lung cancer patients with EGFR 19 or 21 mutations: a retrospective study
 Yang et al. World Journal of Surgical Oncology (2017) 15:197 DOI 10.1186/s12957-017-1251-z RESEARCH Open Access Postoperative survival of EGFR-TKI-targeted therapy in non-small cell lung cancer patients
Yang et al. World Journal of Surgical Oncology (2017) 15:197 DOI 10.1186/s12957-017-1251-z RESEARCH Open Access Postoperative survival of EGFR-TKI-targeted therapy in non-small cell lung cancer patients
AURA 3: the last word on chemotherapy as a control arm in EGFR mutant NSCLC?
 Editorial Page 1 of 5 AURA 3: the last word on chemotherapy as a control arm in EGFR mutant NSCLC? Terry L. Ng, D. Ross Camidge Division of Medical Oncology, Department of Medicine, University of Colorado
Editorial Page 1 of 5 AURA 3: the last word on chemotherapy as a control arm in EGFR mutant NSCLC? Terry L. Ng, D. Ross Camidge Division of Medical Oncology, Department of Medicine, University of Colorado
Editorial Process: Submission:10/27/2017 Acceptance:05/25/2018
 DOI:10.22034/APJCP.2018.19.7.1761 TKI by Liquid Biopsy RESEARCH ARTICLE Editorial Process: Submission:10/27/2017 Acceptance:05/25/2018 A Case-control Study Supporting the Use of Liquid Biopsy in the Targeted
DOI:10.22034/APJCP.2018.19.7.1761 TKI by Liquid Biopsy RESEARCH ARTICLE Editorial Process: Submission:10/27/2017 Acceptance:05/25/2018 A Case-control Study Supporting the Use of Liquid Biopsy in the Targeted
Review Article K-Ras Mutations in Non-Small-Cell Lung Cancer: Prognostic and Predictive Value
 International Scholarly Research Network ISRN Molecular Biology Volume 2012, Article ID 837306, 8 pages doi:10.5402/2012/837306 Review Article K-Ras Mutations in Non-Small-Cell Lung Cancer: Prognostic
International Scholarly Research Network ISRN Molecular Biology Volume 2012, Article ID 837306, 8 pages doi:10.5402/2012/837306 Review Article K-Ras Mutations in Non-Small-Cell Lung Cancer: Prognostic
ABSTRACT INTRODUCTION
 , Vol. 8 (5-6), May 2017 Phase I/II study of erlotinib, carboplatin, pemetrexed, and bevacizumab in chemotherapy-naïve patients with advanced non-squamous non-small cell lung cancer harboring epidermal
, Vol. 8 (5-6), May 2017 Phase I/II study of erlotinib, carboplatin, pemetrexed, and bevacizumab in chemotherapy-naïve patients with advanced non-squamous non-small cell lung cancer harboring epidermal
EGFR, Lung Cancer and Cytology. Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan.
 EGFR, Lung Cancer and Cytology Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan. It is histopathologically divided into two major sub-groups: Small
EGFR, Lung Cancer and Cytology Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan. It is histopathologically divided into two major sub-groups: Small
Osimertinib Activity in Patients With Leptomeningeal Disease From Non-Small Cell Lung Cancer: Updated Results From the BLOOM Study
 Osimertinib Activity in Patients With Leptomeningeal Disease From Non-Small Cell Lung Cancer: Updated Results From the BLOOM Study Abstract 9002 Yang JC, Kim DW, Kim SW, Cho BC, Lee JS, Ye X, Yin X, Yang
Osimertinib Activity in Patients With Leptomeningeal Disease From Non-Small Cell Lung Cancer: Updated Results From the BLOOM Study Abstract 9002 Yang JC, Kim DW, Kim SW, Cho BC, Lee JS, Ye X, Yin X, Yang
The epidermal growth factor receptor (EGFR) is a promising
 ORIGINAL ARTICLE Clinical Significance of Epidermal Growth Factor Receptor Gene Mutations on Treatment Outcome after First-line Cytotoxic Chemotherapy in Japanese Patients with Non-small Cell Lung Cancer
ORIGINAL ARTICLE Clinical Significance of Epidermal Growth Factor Receptor Gene Mutations on Treatment Outcome after First-line Cytotoxic Chemotherapy in Japanese Patients with Non-small Cell Lung Cancer
Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory
 2.04.45 Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date November 26, 2014 Original Policy Date November
2.04.45 Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date November 26, 2014 Original Policy Date November
Original Article. Abstract
 Original Article Survival difference between EGFR Del19 and L858R mutant advanced non-small cell lung cancer patients receiving gefitinib: a propensity score matching analysis Minglei Zhuo 1*, Qiwen Zheng
Original Article Survival difference between EGFR Del19 and L858R mutant advanced non-small cell lung cancer patients receiving gefitinib: a propensity score matching analysis Minglei Zhuo 1*, Qiwen Zheng
Uncommon EGFR mutations in a cohort of Chinese NSCLC patients and outcomes of first-line EGFR-TKIs and platinumbased
 Original Article Uncommon EGFR mutations in a cohort of Chinese NSCLC patients and outcomes of first-line EGFR-TKIs and platinumbased chemotherapy Jinpeng Shi 1*, Hui Yang 1*, Tao Jiang 1, Xuefei Li 2,
Original Article Uncommon EGFR mutations in a cohort of Chinese NSCLC patients and outcomes of first-line EGFR-TKIs and platinumbased chemotherapy Jinpeng Shi 1*, Hui Yang 1*, Tao Jiang 1, Xuefei Li 2,
ONCOLOGY LETTERS 8: , 2014
 ONCOLOGY LETTERS 8: 813-818, 2014 Investigation of the epidermal growth factor receptor mutation rate in non small cell lung cancer patients and the analysis of associated risk factors using logistic regression
ONCOLOGY LETTERS 8: 813-818, 2014 Investigation of the epidermal growth factor receptor mutation rate in non small cell lung cancer patients and the analysis of associated risk factors using logistic regression
IRESSA (Gefitinib) The Journey. Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca
 IRESSA (Gefitinib) The Journey Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca Overview The Drug The Biomarker and Clinical Trials Sampling Lessons Learned The
IRESSA (Gefitinib) The Journey Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca Overview The Drug The Biomarker and Clinical Trials Sampling Lessons Learned The
Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy
 Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy September 2008 This technology summary is based on information available at the time of research and a
Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy September 2008 This technology summary is based on information available at the time of research and a
Analysis of the outcome of young age tongue squamous cell carcinoma
 Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Molecular Targets in Lung Cancer
 Molecular Targets in Lung Cancer Robert Ramirez, DO, FACP Thoracic and Neuroendocrine Oncology November 18 th, 2016 Disclosures Consulting and speaker fees for Ipsen Pharmaceuticals, AstraZeneca and Merck
Molecular Targets in Lung Cancer Robert Ramirez, DO, FACP Thoracic and Neuroendocrine Oncology November 18 th, 2016 Disclosures Consulting and speaker fees for Ipsen Pharmaceuticals, AstraZeneca and Merck
Treatment of EGFR mutant advanced NSCLC
 Treatment of EGFR mutant advanced NSCLC Raffaele Califano Department of Medical Oncology The Christie and University Hospital of South Manchester, Manchester, UK Outline Data on first-line Overcoming T790M
Treatment of EGFR mutant advanced NSCLC Raffaele Califano Department of Medical Oncology The Christie and University Hospital of South Manchester, Manchester, UK Outline Data on first-line Overcoming T790M
Lung cancer remains the leading cause of cancer-related
 Original Article EGFR Mutation Impact on Definitive Concurrent Chemoradiation Therapy for Inoperable Stage III Adenocarcinoma Kosuke Tanaka, MD,* Toyoaki Hida, MD, PhD,* Yuko Oya, MD,* Tomoyo Oguri, MD,
Original Article EGFR Mutation Impact on Definitive Concurrent Chemoradiation Therapy for Inoperable Stage III Adenocarcinoma Kosuke Tanaka, MD,* Toyoaki Hida, MD, PhD,* Yuko Oya, MD,* Tomoyo Oguri, MD,
7/6/2015. Cancer Related Deaths: United States. Management of NSCLC TODAY. Emerging mutations as predictive biomarkers in lung cancer: Overview
 Emerging mutations as predictive biomarkers in lung cancer: Overview Kirtee Raparia, MD Assistant Professor of Pathology Cancer Related Deaths: United States Men Lung and bronchus 28% Prostate 10% Colon
Emerging mutations as predictive biomarkers in lung cancer: Overview Kirtee Raparia, MD Assistant Professor of Pathology Cancer Related Deaths: United States Men Lung and bronchus 28% Prostate 10% Colon
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? VEGF Is the Only Angiogenic Factor Present Throughout the Tumor Life Cycle
 Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
AHFS Final. line. Criteria Used in. combined. cisplatin. Strength. established was. Non-small Cell Lung. Cancer: of carboplatin and
 Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Prognostic Value of EGFR Mutation and ERCC1 in Patients with Non-Small Cell Lung Cancer Undergoing Platinum-Based Chemotherapy
 Prognostic Value of EGFR Mutation and ERCC1 in Patients with Non-Small Cell Lung Cancer Undergoing Platinum-Based Chemotherapy Fumie Yamashita 1, Koichi Azuma 1 *, Tsukasa Yoshida 1, Kazuhiko Yamada 1,
Prognostic Value of EGFR Mutation and ERCC1 in Patients with Non-Small Cell Lung Cancer Undergoing Platinum-Based Chemotherapy Fumie Yamashita 1, Koichi Azuma 1 *, Tsukasa Yoshida 1, Kazuhiko Yamada 1,
Surrogate endpoints for overall survival in advanced non small cell lung cancer patients with mutations of the epidermal growth factor receptor gene
 MOLECULAR AND CLINICAL ONCOLOGY 2: 731-736 Surrogate endpoints for overall survival in advanced non small cell lung cancer patients with mutations of the epidermal growth factor receptor gene REIKO YOSHINO
MOLECULAR AND CLINICAL ONCOLOGY 2: 731-736 Surrogate endpoints for overall survival in advanced non small cell lung cancer patients with mutations of the epidermal growth factor receptor gene REIKO YOSHINO
Personalized Medicine in Oncology and the Implication for Clinical Development
 THE POWER OFx Experts. Experienc e. Execution. Personalized Medicine in Oncology and the Implication for Clinical Development Jamal Gasmi MD, PhD, Medical Director, Medpace Introduction The notable success
THE POWER OFx Experts. Experienc e. Execution. Personalized Medicine in Oncology and the Implication for Clinical Development Jamal Gasmi MD, PhD, Medical Director, Medpace Introduction The notable success
GTS. Earn CME credits at
 Reflex testing of resected stage I through III lung adenocarcinomas for EGFR and KRAS mutation: Report on initial experience and clinical utility at a single center Sandra P. D Angelo, MD, Bernard Park,
Reflex testing of resected stage I through III lung adenocarcinomas for EGFR and KRAS mutation: Report on initial experience and clinical utility at a single center Sandra P. D Angelo, MD, Bernard Park,
Carmen Salvador-Coloma 1,2, David Lorente 1,2, Sarai Palanca 3, Javier Simarro 3, Nuria Mancheño 4, Juan Sandoval 5, Agustín Lahoz 5, Óscar Juan 2,5
 Original Article Early radiological response as predictor of overall survival in non-small cell lung cancer (NSCLC) patients with epidermal growth factor receptor mutations Carmen Salvador-Coloma 1,2,
Original Article Early radiological response as predictor of overall survival in non-small cell lung cancer (NSCLC) patients with epidermal growth factor receptor mutations Carmen Salvador-Coloma 1,2,
EGFR MUTATIONS: EGFR PATHWAY AND SELECTION OF FIRST-LINE THERAPY WITH TYROSINE KINASE INHIBITORS
 EGFR MUTATIONS: EGFR PATHWAY AND SELECTION OF FIRST-LINE THERAPY WITH TYROSINE KINASE INHIBITORS Federico Cappuzzo Istituto Clinico Humanitas IRCCS Rozzano-Italy The EGFR/HER Family Ligand binding domain
EGFR MUTATIONS: EGFR PATHWAY AND SELECTION OF FIRST-LINE THERAPY WITH TYROSINE KINASE INHIBITORS Federico Cappuzzo Istituto Clinico Humanitas IRCCS Rozzano-Italy The EGFR/HER Family Ligand binding domain
ABSTRACT. PERMANYER. J Cancerol. 2015;2:56-63
 www.journalofcancerology.com PERMANYER J Cancerol. 2015;2:56-63 JOURNAL OF CANCEROLOGY REVIEW ARTICLE Outcome of Patients with Lung Adenocarcinoma Harboring Common and Rare Epidermal Growth Factor Receptor
www.journalofcancerology.com PERMANYER J Cancerol. 2015;2:56-63 JOURNAL OF CANCEROLOGY REVIEW ARTICLE Outcome of Patients with Lung Adenocarcinoma Harboring Common and Rare Epidermal Growth Factor Receptor
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): November 26, 2013 Effective Date: July 24, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): November 26, 2013 Effective Date: July 24, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
REVIEWS. Personalized medicine in lung cancer: what we need to know. Tony S. K. Mok
 Personalized medicine in lung cancer: what we need to know Tony S. K. Mok Abstract Lung cancer is a complex and often fatal disease. The recent discovery of activating mutations in EGFR and fusion genes
Personalized medicine in lung cancer: what we need to know Tony S. K. Mok Abstract Lung cancer is a complex and often fatal disease. The recent discovery of activating mutations in EGFR and fusion genes
Overall survival with afatinib versus chemotherapy in patients with NSCLC harboring common EGFR
 Overall survival with afatinib versus chemotherapy in patients with NSCLC harboring common EGFR mutations: subgroup analyses by race/ethnicity in LUX-Lung 3 and LUX-Lung 6 Yi-Long Wu, 1 Lecia V Sequist,
Overall survival with afatinib versus chemotherapy in patients with NSCLC harboring common EGFR mutations: subgroup analyses by race/ethnicity in LUX-Lung 3 and LUX-Lung 6 Yi-Long Wu, 1 Lecia V Sequist,
Current outcomes of postrecurrence survival in patients after resection of non-small cell lung cancer
 Original Article Current outcomes of postrecurrence survival in patients after resection of non-small cell lung cancer Tetsuya Mizuno 1, Takaaki Arimura 1, Hiroaki Kuroda 1, Noriaki Sakakura 1, Yasushi
Original Article Current outcomes of postrecurrence survival in patients after resection of non-small cell lung cancer Tetsuya Mizuno 1, Takaaki Arimura 1, Hiroaki Kuroda 1, Noriaki Sakakura 1, Yasushi
Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases
 Original Article Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases Yuan-Yuan Lei 1,2, Jin-Ji Yang 2, Wen-Zhao Zhong 2, Hua-Jun Chen
Original Article Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases Yuan-Yuan Lei 1,2, Jin-Ji Yang 2, Wen-Zhao Zhong 2, Hua-Jun Chen
Dr R Corre : service de Pneumologie Hôpital Pontchaillou- CHU de Rennes Dr J.B Auliac : service de Pneumologie- Hôpital F. Quesnay CH Mantes la Jolie
 1. RESUME DE LA RECHERCHE PROMOTEUR INVESTIGATORS COORDONNATEURS GFPC (groupe français de pneumo-cancérologie) Dr R Corre : service de Pneumologie Hôpital Pontchaillou- CHU de Rennes Dr J.B Auliac : service
1. RESUME DE LA RECHERCHE PROMOTEUR INVESTIGATORS COORDONNATEURS GFPC (groupe français de pneumo-cancérologie) Dr R Corre : service de Pneumologie Hôpital Pontchaillou- CHU de Rennes Dr J.B Auliac : service
The discovery of targetable driver mutations in a subset of
 Original Article Clinical Characteristics and Course of 63 Patients with BRAF Mutant Lung Cancers Anya M. Litvak, MD,* Paul K. Paik, MD,* Kaitlin M. Woo, MS, Camelia S. Sima, MD, Matthew D. Hellmann, MD,*
Original Article Clinical Characteristics and Course of 63 Patients with BRAF Mutant Lung Cancers Anya M. Litvak, MD,* Paul K. Paik, MD,* Kaitlin M. Woo, MS, Camelia S. Sima, MD, Matthew D. Hellmann, MD,*
Exon 19 L747P mutation presented as a primary resistance to EGFR-TKI: a case report
 Case Report Exon 19 L747P mutation presented as a primary resistance to EGFR-TKI: a case report Yu-Ting Wang, Wei-Wei Ning, Jing Li, Jian-n Huang Department of Respiratory Medicine, the First ffiliated
Case Report Exon 19 L747P mutation presented as a primary resistance to EGFR-TKI: a case report Yu-Ting Wang, Wei-Wei Ning, Jing Li, Jian-n Huang Department of Respiratory Medicine, the First ffiliated
Cancer Cell Research 14 (2017)
 Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER. Virginie Westeel Chest Disease Department University Hospital Besançon, France
 PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5298-5303 Prognostic Value of Platelet to Lymphocyte Ratio in Patients with Non-Small Cell Lung Cancer Mohammad Sabry Elkady, Ghada
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5298-5303 Prognostic Value of Platelet to Lymphocyte Ratio in Patients with Non-Small Cell Lung Cancer Mohammad Sabry Elkady, Ghada
Lung cancer is the leading cause of cancer related death
 Original Article Bcl-2-Like Protein 11 Deletion Polymorphism Predicts Survival in Advanced Non Small-Cell Lung Cancer Jih-Hsiang Lee, MD,* Yu-Lin Lin, MD,* Wei-Hsun Hsu, MD,* Hsuan-Yu Chen, PhD, # Yeun-Chung
Original Article Bcl-2-Like Protein 11 Deletion Polymorphism Predicts Survival in Advanced Non Small-Cell Lung Cancer Jih-Hsiang Lee, MD,* Yu-Lin Lin, MD,* Wei-Hsun Hsu, MD,* Hsuan-Yu Chen, PhD, # Yeun-Chung
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 For Patients with Non-Small Cell Lung Cancer Page 1 of 14 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Epidermal Growth Factor Receptor Mutation Analysis
For Patients with Non-Small Cell Lung Cancer Page 1 of 14 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Epidermal Growth Factor Receptor Mutation Analysis
Molecular Testing in Lung Cancer
 Molecular Testing in Lung Cancer Pimpin Incharoen, M.D. Assistant Professor, Thoracic Pathology Department of Pathology, Ramathibodi Hospital Genetic alterations in lung cancer Source: Khono et al, Trans
Molecular Testing in Lung Cancer Pimpin Incharoen, M.D. Assistant Professor, Thoracic Pathology Department of Pathology, Ramathibodi Hospital Genetic alterations in lung cancer Source: Khono et al, Trans
The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line Chemotherapy for Advanced Non-small Cell Lung Cancer
 pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2015;47(4):638-644 Original Article http://dx.doi.org/10.4143/crt.2014.316 Open Access The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line
pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2015;47(4):638-644 Original Article http://dx.doi.org/10.4143/crt.2014.316 Open Access The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line
Erlotinib for the first-line treatment of EGFR-TK mutation positive non-small cell lung cancer
 ERRATUM Erlotinib for the first-line treatment of EGFR-TK mutation positive non-small cell lung cancer This report was commissioned by the NIHR HTA Programme as project number 11/08 Completed 6 th January
ERRATUM Erlotinib for the first-line treatment of EGFR-TK mutation positive non-small cell lung cancer This report was commissioned by the NIHR HTA Programme as project number 11/08 Completed 6 th January
