BJUI. Active surveillance of small renal masses offers short-term oncological efficacy equivalent to radical and partial nephrectomy
|
|
|
- Amice Harrington
- 5 years ago
- Views:
Transcription
1 BJUI Active surveillance of small renal masses offers short-term oncological efficacy equivalent to radical and partial nephrectomy Nilay Patel, David Cranston, M. Zeeshan Akhtar, Caroline George, Andrew Jones, Aaron Leiblich, Andrew Protheroe and Mark Sullivan Department of Urology, Churchill Hospital, Headington, Oxford, UK Accepted for publication 20 December 2011 Study Type Therapy (case series) Level of Evidence 4 OBJECTIVE To compare the oncological outcomes of active surveillance (AS), radical nephrectomy (RN) and partial nephrectomy (PN) in the management of T1a small renal masses (SRMs). What s known on the subject? and What does the study add? Active surveillance of small renal masses has traditionally been reserved for elderly patients deemed unfit for surgery or ablation. There is increasing evidence showing the safety of active surveillance in the management of small renal masses. In this retrospective study we compared outcomes for patients with small renal masses managed with active surveillance, radical nephrectomy and partial nephrectomy. We showed that active surveillance was safe and appeared as effective as immediate surgery in the management of small renal tumours. RESULTS CONCLUSIONS PATIENTS AND METHODS At present AS is used in the treatment of SRMs in elderly patients with multiple co-morbidities or in those who decline surgery. We identified all patients with T1a SRMs managed with RN, PN or AS. Retrospective data were collected from patient case records with survival data and cause of death cross-referenced with the Oxford Cancer Intelligence Unit. A total of 202 patients with 234 T1a SRMs (solid or Bosniak IV) were identified; 71 patients were managed with AS, 41 with an RN and 90 by PN. Over a median follow-up of 34 months the mean growth rate on AS was 0.21 cm/ year with 53% of SRMs managed with AS showing negative or zero growth. No statistically significant difference was observed in overall (OS) and cancer-specific (CSS) survival for AS, RN and PN (AS-CSS 98.6%, AS-OS 83%; RN-CSS 92.6%, RN-OS 80.4%; PN-CSS 96.6%, PN-OS 90.0%). Active surveillance of SRMs offers oncological efficacy equivalent to surgery in the short/intermediate term. The results of this study support a multicentre prospective randomized controlled trial designed to compare the oncological efficacy of AS and surgery. KEYWORDS active surveillance, renal carcinoma, small mass INTRODUCTION The incidence of renal cancer has been increasing in Europe and the USA since the 1980s [ 1 3 ]. An increase in the use of cross-sectional imaging over this period has resulted in a downward stage migration at presentation with an increasing proportion of patients presenting with small renal masses (SRM) < 4 cm in size [ 4 6 ]. Increased detection rates of early stage disease have resulted in increased rates of surgery for SRMs, the benefits of which remain unclear. There are conflicting reports on improvements in mortality rates for renal cancer over the past few years [ 5,7 ], suggesting that increased detection and earlier treatment may not necessarily be improving the survival of patients with T1a renal cancer. Numerous treatment options have been available to patients presenting with SRMs inclding radical nephrectomy (RN), partial nephrectomy (PN), ablative therapies (cryotherapy, radiofrequency ablation, high-intensity focused ultrasound) and active surveillance (AS). The current guidelines for the treatment of T1 renal cancer from the AUA and the European Association of Urology have suggested performing a PN whenever possible in the surgically fit patient [ 8,9 ]. A recent study from the USA has shown the increased use of nephron-sparing techniques over the past decade; however, in 2007 only 32.2% of T1 renal masses were managed with a PN, 57.7% with an RN, 6.8% with ablative therapy and 3.3% with AS [ 10 ]. A significant number of SRMs are diagnosed as incidental tumours often in elderly 2012 doi: /j x x 1
2 PATEL ET AL. patients. As life expectancy continues to improve, the number of patients with incidentally detected renal masses is likely to increase further, as will the number of patients being offered surgical intervention. There is increasing evidence to suggest that surgical intervention may not be needed in all SRMs because the risk of metastases and death from RCC is low regardless of treatment modality [ 11 ]. Active surveillance has traditionally been reserved for the treatment of SRMs in elderly patients with multiple co-morbidities or in those who decline surgery. It has not been proposed as the treatment of choice in young fit patients because of the small but real risk of developing incurable metastatic disease while on surveillance. In this paper we present the results of a single-centre retrospective audit in which we compared the oncological outcomes of AS, PN and RN in the management of SRMs. The main objective of the study being to determine if there is adequate evidence to support a randomized trial and to inform any proposed trial design of potential inclusion/exclusion criteria and triggers for intervention. METHODS We used our local Cancer Research Uro-Onocology Database [ 12 ] to identify all patients that presented to our department between 1 January 2005 and 31 December 2010 with suspected T1 renal tumours. Upon presentation, each patient was definitively staged with either a triple-phase CT scan of the chest and abdomen or a dedicated renal MRI scan. All images were reviewed by a urological surgeon and a uro-radiologist. Patients were subsequently counselled regarding their treatment options, which included RN (open or laparoscopic), PN (open, laparoscopic or robotic), ablative therapy (cryotherapy, radiofrequency ablation or high-intensity frequency ultrasound) and AS. The choice of treatment was based on tumour characteristics and patient factors, including age, associated co-morbidities and overall surgical risk. Predefined selection criteria for each treatment option had not been established at the commencement of this study. We only included patients with solid enhancing or cystic enhancing T1a small renal masses managed by RN, PN or AS. T1a Active Surveillance No. of patients 71 Sex Male 52 Female 19 Number of masses 93 Nature of masses Solid enhancing 76 Cystic enhancing 17 Biopsy Yes 7 Renal cell carcinoma 2 Oncocytoma 2 Non diagnostic 3 No 86 Mean annual growth rate (cm/year) 0.21 Mean duration of follow-up (months) 34 Mean growth rate (cm/year) All patients 0.21 Positive growth 0.35 Mean growth rates (cm/year) All patients 0.21 Negative or zero growth, n (%) 49 (53) cm/year, n (%) 19 (21) cm/year, n (%) 13 (14) > 0.5 cm/year, n (%) 11 (12) Positive growth 0.35 Patients progressing to intervention, n / N (%) 14/71 (19.7) Increase in size, n (%) 9 (64) Patient choice, n (%) 4 (29) Change in diagnosis, n (%) 1 (7) A follow-up surveillance protocol for patients managed with AS had not been prospectively established before this study. Patient assessment and follow-up were dependent upon individual physician preferences. Patients were followed up with CT, MRI or ultrasound scans of the abdomen and chest every 3 6 months. Routine percutaneous renal biopsy of T1 lesions has not been part of our practice. Patients on AS were advised to have definitive treatment if their tumours grew to > 4 cm in maximal diameter or had rapid tumour growth rates. Patients managed with an RN or PN were followed up postoperatively every 6 12 months with a CT scan of the chest and abdomen. Retrospective data were collected from patient case records including; radiological tumour characteristics at presentation, radiological tumour characteristics during follow-up, surgical pathology, incidence of local and metastatic recurrence and survival. Renal masses were staged according to the 2009 TNM classification for kidney tumours. Survival data and cause of death were cross-referenced with the Oxford Cancer Intelligence Unit. Statistical analysis was performed using Microsoft E XCEL and G RAPH P AD P RISM 4; using the following tests; chi squared, Student s t test and Kaplan Meier curves. RESULTS TABLE 1 Demographics and outcomes of patients managed with active surveillance A total of 71 patients with 93 small renal masses < 4 cm in maximal diameter (76 solid, 17 enhancing cystic Bosniak IV) were managed with AS ( Table 1 ). Four patients with a total of seven tumours were known to have Von Hippel Lindau disease. The mean age of patients on AS was 71.9 years (24 93) with a mean tumour size at presentation of 2.2 cm. The mean duration of follow-up was 34 months
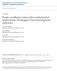
3 A C T I V E S U R V E I L L A N C E O F S M A L L R E N A L M A S S E S FIG. 1. A waterfall plot illustrating the annual growth rate for each small renal mass managed with active surveillance. The dashed line represents a growth rate of 0.5 cm/year. This could be used as a trigger for intervention for patients being managed with active surveillance. Growth rate, cm/yr Patient Number Over this period the average annual growth rate for all 93 tumours was 0.21 cm/year. A percutaneous renal biopsy was performed in 7/93 (7.5%) tumours of which two showed renal carcinoma, two oncocytoma and three were non-diagnostic. We observed that 49/93 (53%) masses had negative or zero growth during the course of their follow-up. Tumours that did increase in size were observed to have variable growth rates: cm/year, 19/93 (21%); cm/year, 13/93 (14%); > 0.5 cm/year, 11/93 (12%) ( Fig. 1 ). Overall 14/71 (19.7%) patients managed with AS subsequently went on to receive definitive therapy; RN (2/14), PN (7/14), radiofrequency ablation (3/14) and high-intensity focused ultrasound (2/14). The trigger for intervention in these patients was an increase in size (9/14), patient choice (4/14) and a change in radiological diagnosis (1/14). The annual growth rate for patients that went on to receive treatment after a period of surveillance was significantly higher than those that remained on AS (0.32 cm/year vs 0.14 cm/year, P < 0.05). The mean time from commencement of AS to delayed intervention was 29 months. Metastatic progression was observed in only one patient of 71 (1.4%) managed with AS. This patient had a history of RCC and presented with two tumours within a solitary kidney, which measured 5.3 cm and 1.5 cm in maximal diameter. A total of 12 deaths occurred in the active surveillance cohort of which one was attributed to metastatic RCC, giving an overall survival (OS) rate of 83% and a cancer-specific survival (CSS) rate of 98.6%. Tumours 0 4 cm Tumours 4 7 cm Number of tumours Sex Male Female Operation Radical nephrectomy Partial nephrectomy Tumour characteristics Solid Solid (multifocal) 15 3 Cystic Tumour histology CCRCC CHROMO 8 5 ONCO 10 6 PAP PAP PAP 1 & SPINDLE 0 1 Tumour stage T1a T1b 0 67 T3a T3b 0 1 Furhman grade I 12 7 II III IV 3 7 x 10 6 Surgical margin Negative Positive 10 (PN = 9; RN = 1) 1 (RN = 1) Patients managed with AS and deferred definitive treatment had an OS rate of 78.5% and a CSS rate of 100%. Surgical pathology data were available in 9/14 patients, with no statistically significant upstaging of disease after a period of active surveillance; T1a, 6/8; T3a, 2/8. Pathology data were not available for the five patients who underwent tumour ablation. Over the study period, 131 patients with 141 SRMs < 4 cm in size were managed surgically by either a radical nephrectomy (43 patients) or a partial nephrectomy (98 patients). Over the same period 102 patients with T1b tumours were also managed with extirpative surgery ( Table 2 ). Four patients with six tumours with known Von Hippel Lindau disease underwent surgery for T1a tumours. TABLE 2 Patient demographics and pathological features of T1 tumours managed with surgery PN, partial nephrectomy; RN, radical nephrectomy. Patients managed with AS were significantly older than those managed with either RN or PN (mean age, AS 71.9 years, RN 65.4 years, PN 58.9 years; P < 0.05). There were no statistically significant differences in tumour size between the three treatment groups (AS 2.2 cm, RN 2.66 cm, PN 2.67 cm) ( Table 3 ). Local recurrence within the renal remnant or renal bed after surgery was observed in 2/41 patients after an RN and 7/90 patients after a PN (7.7%). Four of the seven patients who developed local recurrences after PN had multifocal disease and 2/7 had positive surgical margins. Positive surgical margins were noted in 10/141 (7%) SRMs (PN 9, RN 1); of whom only 2/10 went on to develop a local recurrence and 1/10 went on to develop metastatic disease. Metastatic progression was observed after surgery in 15/131 patients (11.4%). Of these patients,
4 PATEL ET AL. TABLE 3 Comparison of patient characteristics and oncological outcomes for patients with T1 renal masses managed with Active Surveillance (AS), Radical Nephrectomy (RN) and Partial Nephrectomy (PN) Variable < 4 cm AS < 4 cm RN < 4 cm PN < 4 cm surgery > 4 cm surgery No. of patients Mean age (years) Mean tumour size (cm) Mean follow-up (months) Local recurrence, n / N (%) N/A 2/41 (4.8) 7/90 (7.7) 10/131 (7.6) 5/102 (4.9) Metastatic progression, n / N (%) 1/71 (1.5) 4/41 (9.7) 11/90 (12.2) 15/131 (11.4) 18/102 (17.6) Overall survival, n / N (%) 59/71 (83) 33/41 (80.4) 81/90 (90.0) 113/131 (87.0) 85/102 (83.8) Cancer-specific survival, n / N (%) 70/71 (98.6) 38/41 (92.6) 87/90 (96.6) 125/131 (95.4) 95/102 (93.1) 8/15 had clear-cell RCC, 1/15 type 1 papillary RCC, 3/15 type 2 papillary RCC and 1/15 chromophobe RCC; 11/15 T1a, 4/15 T3a/b; G1/2 4/15, G3/4 11/15; mean size 2.36 cm ( ). Overall 114/131 patients managed with surgery were alive, equating to an 87.0% OS rate and a 95.4% CSS rate. Kaplan Meier curves comparing oncological outcomes for AS, RN and PN showed no statistically significant difference in OS or CSS between the groups ( Fig. 2 ). A sub-group analysis compared outcomes of AS and surgery in patients over the age of 70. In total, 60 tumours in 47 patients were managed with surveillance and 43 with surgery (PN 23, RN 20). No statistically significant difference was seen in the OS or CSS rate (surgery, 76.7% OS, 97.6% CSS; AS, 76.5% OS, 97.8% CSS). Surgical pathology was reviewed for all patients who underwent surgery for a T1 renal mass. The incidence of high-risk locally advanced disease (stage T3a) was significantly higher in patients with tumours 4 7 cm in maximal diameter than those with tumours < 4 cm in maximal diameter ( < 4 cm 11/141 (7.8%); > 4 cm 38/102 (37.3%), P < 0.001) ( Fig. 3 ). A similar difference was observed for tumours cm in size: /36 (25%); < 3.5 cm 8/105 (7.6%); P < These differences were not replicated when comparing smaller tumours; /40 (5%); < 3.0 6/76 (7.8%); P > DISCUSSION In this study we compared oncological outcomes for patients with T1a SRMs managed by either AS, RN or PN. The study has a number of inherent weaknesses; it is a retrospective single-centre study, the three treatment arms have unmatched patient characteristics that can introduce case selection bias between surgery and active surveillance, there is a low diagnostic biopsy rate for the active surveillance group and a lack of predetermined criteria for intervention in the AS group. Despite these weaknesses much can be gleaned from the results of this study. One of the main aims of this study was to evaluate the oncological safety of AS in comparison with surgical intervention. This was initially evaluated by determining the natural history of the SRMs within the study cohort. We observed an average growth rate for SRMs < 4 cm in size of 0.21 cm/year (mean follow-up 34 months). This compares with data from the pooled analysis by Smaldone et al. [ 13 ], which showed that T1a tumours have a growth rate of 0.31 cm/ year. Jewett et al. [ 14 ] noted an annual growth rate of 0.13 cm/year for T1a masses in the prospective Canadian Small Renal Mass Trial. Numerous studies have previously shown variability in the growth rates of T1 renal masses. In our experience 53% of T1a SRMs showed zero or negative growth and none of the patients subsequently developed metastatic disease. Other studies have shown that 23 36% of T1 SRMs have zero or negative growth rates [ ]. The pooled analysis of 880 patients with SRMs by Smaldone et al. [ 13 ] observed that metastatic progression was not observed in any patient who had negative or zero growth on follow-up, which is potentially of great importance when counselling patients being managed with AS. FIG. 2. Kaplan Meier curves comparing overall survival (OS) and cancer-specific survival (CSS) for all patients with T1a tumours managed with active surveillance (AS), radical nephrectomy (RN) and partial nephrectomy (PN). Percent survival Percent survival Months Months FIG. 3. Comparison of surgical pathology for T1 renal tumours. PN OS RN OS AS OS PN CSS RN CSS AS CSS 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% >4 cm <4 cm <3.5 < T3a (%) T1a (%)
5 A C T I V E S U R V E I L L A N C E O F S M A L L R E N A L M A S S E S Triggers for intervention for patients on an AS protocol are yet to be clearly defined in the management of SRMs. At present, rapid tumour growth and progression beyond a maximal size are the most commonly used triggers for intervention. The principle aim being to distinguish between high-risk tumours and low-risk SRMs. The identification of rapid growth rates in an active surveillance protocol for SRMs may act as a marker of aggressive disease in a similar way to that in which PSA doubling time is used in active surveillance protocols for prostate cancer. The use of growth rate in differentiating SRMs seems well founded, Smaldone et al. [ 13 ] showed that SRMs that progressed to metastatic disease had significantly higher growth rates than tumours that did not metastasize (0.8 cm/ year vs 0.4 cm/year). In our study, 12% of patients had an annual growth rate > 0.5 cm/year whereas 9% of patients showed an annual growth rate > 0.8 cm/year. Our data and that of Smaldone et al. [ 13 ] suggest that a linear growth rate of > 0.5 cm/year could be proposed as a trigger for intervention in an AS protocol. Use of the linear growth rate however may not be the most accurate means of assessing tumour growth as the linear growth rate is dependent upon tumour size at presentation. Evaluation of tumour volume may be a more sensitive means of assessing tumour burden and risk. Jewett et al. [ 14 ] used a doubling of tumour volume within 12 months as a trigger for progression in their prospective observation study. It is unclear which of these approaches is better at identifying high-risk disease. Tumour size beyond a predetermined limit such as 4 cm is often used alongside growth rate as the trigger for intervention for patients on AS. Our study justifies this approach, as we showed that tumours > 4 cm in size had significantly higher rates of high-risk disease (T3a) than tumours < 4 cm in size ( > 4 cm 37% vs < 4 cm 7.8%). Our study suggested that the trigger point should be lowered to 3.5 cm as a significant proportion of patients with cm tumours have T3a disease (25%). Others have suggested a trigger point as low as 3 cm, because tumours > 3 cm are associated with increased aggressive potential [ 17 ]. During the course of our study 14/71 (19%) patients went on to receive definitive therapy for their SRMs. Other groups have reported intervention rates of between 4.5 and 45.4% [ 13,14,18 20 ], most of these studies did not report predetermined intervention criteria for patients on AS. As would be expected the tumours of our patients who underwent definitive treatment had higher annual growth rates than tumours of patients who continued on AS (0.32 cm/year vs 0.14 cm/year, P < 0.05) an observation mirrored by Smaldone et al. [ 13 ]. Delayed intervention did not appear to adversely affect surgical approach or oncological outcome. Patients who went on to receive definitive treatment in our study were managed with nephron-sparing surgery in 85% of cases. There was no upstaging of disease or there were no adverse oncological outcomes in contrast to patients managed with surgery initially. Having determined the natural history of SRMs managed with AS we subsequently compared the oncological outcomes of tumours < 4 cm in size treated with AS, RN or PN. In our series only 1/71 patients managed with AS developed metastatic RCC (1.4%). In this patient it was unclear if the T1a SRM was the cause of the metastatic disease because the patient had a history of renal cancer and a synchronous T1b tumour within his remaining kidney. Interestingly metastatic disease occurred more frequently after surgery than after active surveillance (AS 1/71, RN 4/41, PN 12/90), though this may be a result of increased tumour size in both surgery groups and the potential for benign pathology in the non-biopsied AS group. Metastatic progression rates for T1a SRMs managed with AS are reported to be between 1 and 2% [ 13,14,21 ]. Kunkle et al. [ 11 ] performed a meta-analysis of oncological outcomes for over 6000 SRMs and concluded that no significant differences were detected in the incidence of metastatic progression regardless of whether lesions were excised, ablated or observed. No significant differences in CSS rates at a mean follow-up of 34 months were observed when comparing the outcomes of SRMs treated with AS, RN or PN. Evaluation of the overall survival rates suggested a benefit in favour of PN, although this was not significant (AS 83%, RN 80%, PN 90%). These are striking observations when it is considered that most AS patients are enrolled to surveillance on account of significant co-morbidities. Numerous groups have shown an overall survival benefit of PN over RN in the treatment of the SRMs [ ], an effect that may be attributable to the significantly greater incidence of chronic kidney disease after RN [ 25 ]. Our work and other recent studies have started to show the safety of AS as a treatment modality for SRMs. It is becoming increasingly clear that all SRMs do not need immediate surgical treatment. Many SRMs are incidental low-grade, low-risk tumours akin to Gleason 6 prostate cancer and are unlikely to result in the development of metastatic disease or cancer-related death. As a consequence, to treat all SRMs may be over-treatment and may unnecessarily expose patients to the perioperative risks of surgery and the long-term risks of chronic kidney disease and cardiovascular disease [ 25 ]. Further research in the diagnostic work up of patients may help to identify high-risk SRMs that are more likely to progress or metastasize. An example of clinically applicable advances in imaging is the R.E.N.A.L. nephrometry scoring system which has recently been shown to predict malignancy and high-grade pathology [ 26 ]. The ability to accurately identify vascular invasion (T3a) may be of particular importance in identifying patients suitable for AS. The past few years has seen a significant increase in the use of percutaneous renal biopsies in the diagnostic setting. Routine renal biopsy results in an 80% diagnostic rate with minimal associated complications [ 27,28 ]. The importance of renal biopsies may increase with the development and adoption of biomarkers that may help to personalize treatment of SRMs [ 27,29 ]. The results of this study support the development of a multi-centre prospective randomized controlled trial comparing active surveillance with delayed intervention versus immediate partial nephrectomy or ablation. The randomized controlled trial would aim to determine the oncological efficacy of these differing approaches in patients with biopsy-proven RCC. We would propose recruiting patients over 70 years of age as our study and that of Lane et al. [ 30 ] has shown the safety of AS in patients older than years. Based on our results we would propose intervention when tumours
6 PATEL ET AL. being managed with AS are > 3.5 cm in size or have growth rates > 0.5 cm/year or show doubling of tumour volume in less than 12 months. CONFLICT OF INTEREST None declared. REFERENCES 1 Ferlay J, Parkin DM, Steliarova- Foucher E. Estimates of cancer incidence and mortality in Europe in Eur J Cancer 2010 ; 46 : Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin 2011 ; 61 : Mathew A, Devesa SS, Fraumeni JF, Chow W-H. Global increases in kidney cancer incidence, Eur J Cancer Prev 2002 ; 11 : Cooperberg MR, Mallin K, Ritchey J, Villalta JD, Carroll PR, Kane CJ. Decreasing size at diagnosis of stage 1 renal cell carcinoma: analysis from the National Cancer Data Base, 1993 to J Urol 2008 ; 179 : Hollingsworth JM, Miller DC, Daignault S, Hollenbeck BK. Rising incidence of small renal masses: a need to reassess treatment effect. J Natl Cancer Inst 2006 ; 98 : Kane CJ, Mallin K, Ritchey J, Cooperberg MR, Carroll PR. Renal cell cancer stage migration: analysis of the National Cancer Data Base. Cancer 2008 ; 113 : Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ. Cancer statistics, CA Cancer J Clin 2009 ; 59 : Campbell SC, Novick AC, Belldegrun A et al. Guideline for management of the clinical T1 renal mass. J Urol 2009 ; 182 : Ljungberg B, Cowan NC, Hanbury DC et al. EAU guidelines on renal cell carcinoma: the 2010 update. Eur Urol 2010 ; 58 : Cooperberg MR, Mallin K, Kane CJ, Carroll PR. Treatment trends for stage I renal cell carcinoma. J Urol 2011 ; 186 : Kunkle DA, Egleston BL, Uzzo RG. Excise, ablate or observe: the small renal mass dilemma a meta-analysis and review. J Urol 2008 ; 179 : ; discussion Charlesworth PJS, Kilbey N, Taylor M et al. Automated uro-oncology data collection: the Cancer Research Uro-Oncology Database. BJU Int 2010 ; 105 : Smaldone MC, Kutikov A, Egleston BL et al. Small renal masses progressing to metastases under active surveillance: a systematic review and pooled analysis. Cancer 2011 ; 118 : Jewett MAS, Mattar K, Basiuk J et al. Active surveillance of small renal masses: progression patterns of early stage kidney cancer. Eur Urol 2011 ; 60 : Crispen PL, Viterbo R, Boorjian SA, Greenberg RE, Chen DYT, Uzzo RG. Natural history, growth kinetics, and outcomes of untreated clinically localized renal tumors under active surveillance. Cancer 2009 ; 115 : Kunkle DA, Crispen PL, Chen DYT, Greenberg RE, Uzzo RG. Enhancing renal masses with zero net growth during active surveillance. J Urol 2007 ; 177 : ; discussion Remzi M, Ozsoy M, Klingler HC et al. Are small renal tumors harmless? Analysis of histopathological features according to tumors 4 cm or less in diameter. J Urol 2006 ; 176 : Haramis G, Mues AC, Rosales JC et al. Natural history of renal cortical neoplasms during active surveillance with follow-up longer than 5 years. Urology 2011 ; 77 : Rosales JC, Haramis G, Moreno J et al. Active surveillance for renal cortical neoplasms. J Urol 2010 ; 183 : Kouba E, Smith A, McRackan D, Wallen EM, Pruthi RS. Watchful waiting for solid renal masses: insight into the natural history and results of delayed intervention. J Urol 2007 ; 177 : ; discussion Chawla SN, Crispen PL, Hanlon AL, Greenberg RE, Chen DYT, Uzzo RG. The natural history of observed enhancing renal masses: meta-analysis and review of the world literature. J Urol 2006 ; 175 : Kates M, Badalato GM, Pitman M, McKiernan JM. Increased risk of overall and cardiovascular mortality after radical nephrectomy for renal cell carcinoma 2 cm or less. J Urol 2011 ; 186 : Huang WC, Elkin EB, Levey AS, Jang TL, Russo P. Partial nephrectomy versus radical nephrectomy in patients with small renal tumors is there a difference in mortality and cardiovascular outcomes? J Urol 2009 ; 181 : ; discussion Thompson RH, Boorjian SA, Lohse CM et al. Radical nephrectomy for pt1a renal masses may be associated with decreased overall survival compared with partial nephrectomy. J Urol 2008 ; 179 : ; discussion Huang WC, Levey AS, Serio AM et al. Chronic kidney disease after nephrectomy in patients with renal cortical tumours: a retrospective cohort study. Lancet Oncol 2006 ; 7 : Kutikov A, Smaldone MC, Egleston BL et al. Anatomic features of enhancing renal masses predict malignant and high-grade pathology: a preoperative nomogram using the RENAL Nephrometry score. Eur Urol 2011 ; 60 : Ph é V, Yates DR, Renard-Penna R, Cussenot O, Roupret M. Is there a contemporary role for percutaneous needle biopsy in the era of small renal masses? BJU Int 2012 ; 109 : Leveridge MJ, Finelli A, Kachura JR et al. Outcomes of small renal mass needle core biopsy, nondiagnostic percutaneous biopsy, and the role of repeat biopsy. Eur Urol 2011 ; 60 : Yates DR, Roupret M. Small renal mass and low-risk prostate cancer: any more for active surveillance? Eur Urol 2011 ; 60 : Lane BR, Abouassaly R, Gao T et al. Active treatment of localized renal tumors may not impact overall survival in patients aged 75 years or older. Cancer 2010 ; 116 : Correspondence: Nilay Patel, Department of Urology, Churchill Hospital, Old Road, Headington, Oxford OX3 7LJ, UK. n1laysp@googl .com Abbreviations : SRM, small renal mass ; RN, radical nephrectomy ; PN, partial nephrectomy ; AS, active surveillance ; OS, overall survival ; CSS, cancer-specific survival
What is the role of partial nephrectomy in the context of active surveillance and renal ablation?
 What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
Canadian Guidelines for Management of the Small Renal Mass (SRM)
 Canadian Guidelines for Management of the Small Renal Mass (SRM) Michael A.S. Jewett*, Ricardo Rendon, Louis Lacombe, Pierre I. Karakiewicz, Simon Tanguay, Wes Kassouf, Mike Leveridge, Ilias Cagiannos,
Canadian Guidelines for Management of the Small Renal Mass (SRM) Michael A.S. Jewett*, Ricardo Rendon, Louis Lacombe, Pierre I. Karakiewicz, Simon Tanguay, Wes Kassouf, Mike Leveridge, Ilias Cagiannos,
WHAT IS THE ROLE OF ACTIVE SURVEILLANCE
 WHAT IS THE ROLE OF ACTIVE SURVEILLANCE IN THE CONTEXT OF RENAL ABLATION AND PARTIAL NEPHRECTOMY? Alessandro Volpe University of Eastern Piedmont Novara, Italy RCC INCIDENCE SEER DATABASE (1975-2006) RCC
WHAT IS THE ROLE OF ACTIVE SURVEILLANCE IN THE CONTEXT OF RENAL ABLATION AND PARTIAL NEPHRECTOMY? Alessandro Volpe University of Eastern Piedmont Novara, Italy RCC INCIDENCE SEER DATABASE (1975-2006) RCC
Who are Candidates for Laparoscopic or Open Radical Nephrectomy. Arieh Shalhav
 Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Patient Selection for Ablative Therapies. Adrian D Joyce Leeds UK
 Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
BJUI. Solitary solid renal mass: can we predict malignancy?
 BJUI Solitary solid renal mass: can we predict malignancy? Philippe Violette, Samuel Abourbih, Konrad M. Szymanski, Simon Tanguay, Armen Aprikian, Keith Matthews, Fadi Brimo * and Wassim Kassouf Divisions
BJUI Solitary solid renal mass: can we predict malignancy? Philippe Violette, Samuel Abourbih, Konrad M. Szymanski, Simon Tanguay, Armen Aprikian, Keith Matthews, Fadi Brimo * and Wassim Kassouf Divisions
ACTIVE SURVEILLANCE FOR RENAL MASSES: Where are we in 2016?
 ACTIVE SURVEILLANCE FOR RENAL MASSES: Where are we in 2016? Phillip M. Pierorazio, MD Assistant Professor of Urology and Oncology Brady Urological Institute Sidney Kimmel Cancer Center Johns Hopkins Hospital
ACTIVE SURVEILLANCE FOR RENAL MASSES: Where are we in 2016? Phillip M. Pierorazio, MD Assistant Professor of Urology and Oncology Brady Urological Institute Sidney Kimmel Cancer Center Johns Hopkins Hospital
Renal biopsy is mandatory for every small renal mass
 Renal biopsy is mandatory for every small renal mass Ben Challacombe Consultant Urologist The Urology Centre Guy s and St. Thomas Hospital NHS Foundation Trust Oncocytoma High Risk Partial converted to
Renal biopsy is mandatory for every small renal mass Ben Challacombe Consultant Urologist The Urology Centre Guy s and St. Thomas Hospital NHS Foundation Trust Oncocytoma High Risk Partial converted to
Renal Mass Biopsy: Needed Now More than Ever
 Renal Mass Biopsy: Needed Now More than Ever Stuart G. Silverman, MD, FACR Professor of Radiology Harvard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
Renal Mass Biopsy: Needed Now More than Ever Stuart G. Silverman, MD, FACR Professor of Radiology Harvard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
Indications For Partial
 Indications For Partial Nephrectomy Christopher G. Wood, M. D., FACS Professor and Deputy Chairman Douglas E. Johnson, M. D. Endowed Professorship in Urology Department of Urology The University of Texas
Indications For Partial Nephrectomy Christopher G. Wood, M. D., FACS Professor and Deputy Chairman Douglas E. Johnson, M. D. Endowed Professorship in Urology Department of Urology The University of Texas
Key Words: kidney; carcinoma, renal cell; renal insufficiency; nephrectomy; mortality
 Comparative Effectiveness for Survival and Renal Function of Partial and Radical Nephrectomy for Localized Renal Tumors: A Systematic Review and Meta-Analysis Simon P. Kim, R. Houston Thompson, Stephen
Comparative Effectiveness for Survival and Renal Function of Partial and Radical Nephrectomy for Localized Renal Tumors: A Systematic Review and Meta-Analysis Simon P. Kim, R. Houston Thompson, Stephen
RAPN. in T1b Renal Masses? A. Mottrie. G. Denaeyer, P. Schatteman, G. Novara
 RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
Contemporary Role of Renal Mass Biopsy
 Contemporary Role of Renal Mass Biopsy Jeffrey K. Mullins, MD Director Urologic Oncology CHI Memorial Chattanooga Urology Associates September 8, 2018 Disclosures I, Jeffrey Mullins, do not have a financial
Contemporary Role of Renal Mass Biopsy Jeffrey K. Mullins, MD Director Urologic Oncology CHI Memorial Chattanooga Urology Associates September 8, 2018 Disclosures I, Jeffrey Mullins, do not have a financial
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Review Article Surveillance for the Management of Small Renal Masses
 Hindawi Publishing Corporation Advances in Urology Volume 2008, Article ID 196701, 6 pages doi:10.1155/2008/196701 Review Article Surveillance for the Management of Small Renal Masses Mehmet Ozsoy, Tobias
Hindawi Publishing Corporation Advances in Urology Volume 2008, Article ID 196701, 6 pages doi:10.1155/2008/196701 Review Article Surveillance for the Management of Small Renal Masses Mehmet Ozsoy, Tobias
RENAL Nephrometry Scoring System: The Radiologist s Perspective
 Genitourinary Imaging Clinical Perspective Parsons et al. Nephrometry Score Genitourinary Imaging Clinical Perspective Rosaleen B. Parsons 1 Daniel Canter 2 Alexander Kutikov 3 Robert G. Uzzo 3 Parsons
Genitourinary Imaging Clinical Perspective Parsons et al. Nephrometry Score Genitourinary Imaging Clinical Perspective Rosaleen B. Parsons 1 Daniel Canter 2 Alexander Kutikov 3 Robert G. Uzzo 3 Parsons
ELECTIVE PARTIAL NEPHRECTOMY FOR T1B RCC. Vitaly Margulis MD. Associate Professor of Urology
 ELECTIVE PARTIAL NEPHRECTOMY FOR T1B RCC Vitaly Margulis MD Associate Professor of Urology NEPHRON SPARING SURGERY WHY? MAXIMIZING NEPHRON MASS SAVES LIVES ELECTIVE PARTIAL NEPHRECTOMY IF: TECHNICALLY
ELECTIVE PARTIAL NEPHRECTOMY FOR T1B RCC Vitaly Margulis MD Associate Professor of Urology NEPHRON SPARING SURGERY WHY? MAXIMIZING NEPHRON MASS SAVES LIVES ELECTIVE PARTIAL NEPHRECTOMY IF: TECHNICALLY
Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes
 Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes Ryan M. Hegg, Grant D. Schmit,* Stephen A. Boorjian, Robert J. McDonald, A. Nicholas Kurup,
Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes Ryan M. Hegg, Grant D. Schmit,* Stephen A. Boorjian, Robert J. McDonald, A. Nicholas Kurup,
St. Dominic s Annual Cancer Report Outcomes
 St. Dominic s 2017 Annual Cancer Report Outcomes Cancer Program Practice Profile Reports (CP3R) St. Dominic s Cancer Committee monitors and ensures that patients treated at St. Dominic Hospital receive
St. Dominic s 2017 Annual Cancer Report Outcomes Cancer Program Practice Profile Reports (CP3R) St. Dominic s Cancer Committee monitors and ensures that patients treated at St. Dominic Hospital receive
Metastatic Potential in Renal Cell Carcinomas =7 cm: Swedish Kidney Cancer Quality Register Data
 EUROPEAN UROLOGY 60 (2011) 975 982 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Eric C. Umbreit and R. Houston Thompson on pp.
EUROPEAN UROLOGY 60 (2011) 975 982 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Eric C. Umbreit and R. Houston Thompson on pp.
Renal Mass Biopsy Should be Used for Most SRM - PRO
 Renal Mass Biopsy Should be Used for Most SRM - PRO Tony Finelli, MD, MSc, FRCSC Head, Division of Urology GU Site Lead, Princess Margaret Cancer Center GU Cancer Lead, Cancer Care Ontario Associate Professor,
Renal Mass Biopsy Should be Used for Most SRM - PRO Tony Finelli, MD, MSc, FRCSC Head, Division of Urology GU Site Lead, Princess Margaret Cancer Center GU Cancer Lead, Cancer Care Ontario Associate Professor,
Comparison of radiographic and pathologic sizes of renal tumors
 ORIGINAL Article Vol. 39 (2): 189-194, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.06 Comparison of radiographic and pathologic sizes of renal tumors Wei Chen, Linhui Wang, Qing Yang, Bing
ORIGINAL Article Vol. 39 (2): 189-194, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.06 Comparison of radiographic and pathologic sizes of renal tumors Wei Chen, Linhui Wang, Qing Yang, Bing
ablativi Vincenzo Ficarra Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine
 Sorveglianza attiva e trattamenti ablativi Vincenzo Ficarra Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine Risk of mortality in RCC patients Kutikov A. et al. J Clin Oncol 2010;
Sorveglianza attiva e trattamenti ablativi Vincenzo Ficarra Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine Risk of mortality in RCC patients Kutikov A. et al. J Clin Oncol 2010;
Is renal cryoablation becoming an effective alternative to partial nephrectomy?
 Is renal cryoablation becoming an effective alternative to partial nephrectomy? J GARNON 1, G TSOUMAKIDOU 1, H LANG 2, A GANGI 1 1 department of interventional radiology 2 department of urology University
Is renal cryoablation becoming an effective alternative to partial nephrectomy? J GARNON 1, G TSOUMAKIDOU 1, H LANG 2, A GANGI 1 1 department of interventional radiology 2 department of urology University
Overall Survival and Development of Stage IV Chronic Kidney Disease in Patients Undergoing Partial and Radical Nephrectomy for Benign Renal Tumors
 EUROPEAN UROLOGY 64 (2013) 600 606 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alexander Kutikov, Marc C. Smaldone and Robert
EUROPEAN UROLOGY 64 (2013) 600 606 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alexander Kutikov, Marc C. Smaldone and Robert
Original Article - Urological Oncology
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.7.446 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.7.446&domain=pdf&date_stamp=2014-07-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.7.446 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.7.446&domain=pdf&date_stamp=2014-07-16
Small renal masses: Toward more rational treatment
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will discuss the treatments for small renal masses, including nephron-sparing options ANIL A. THOMAS, MD Glickman Urological and Kidney Institute, Cleveland
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will discuss the treatments for small renal masses, including nephron-sparing options ANIL A. THOMAS, MD Glickman Urological and Kidney Institute, Cleveland
Salvage surgery after energy ablation for renal masses
 Salvage surgery after energy ablation for renal masses Jose A. Karam, Christopher G. Wood, Zachary R. Compton, Priya Rao*, Raghunandan Vikram, Kamran Ahrar and Surena F. Matin Departments of Urology, *Pathology,
Salvage surgery after energy ablation for renal masses Jose A. Karam, Christopher G. Wood, Zachary R. Compton, Priya Rao*, Raghunandan Vikram, Kamran Ahrar and Surena F. Matin Departments of Urology, *Pathology,
Partial versus radical nephrectomy for pt1a renal cancer in Serbia
 JBUON 2016; 21(6): 1449-1453 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Partial versus radical nephrectomy for pt1a renal cancer in Serbia
JBUON 2016; 21(6): 1449-1453 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Partial versus radical nephrectomy for pt1a renal cancer in Serbia
GUIDELINES ON RENAL CELL CARCINOMA
 GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
Comparison of Partial and Radical Nephrectomy for pt1b Renal Cell Carcinoma
 www.kjurology.org DOI:10.4111/kju.2010.51.9.596 Urological Oncology Comparison of Partial and Radical Nephrectomy for pt1b Renal Cell Carcinoma Jong Min Kim, Phil Hyun Song, Hyun Tae Kim, Tong Choon Park
www.kjurology.org DOI:10.4111/kju.2010.51.9.596 Urological Oncology Comparison of Partial and Radical Nephrectomy for pt1b Renal Cell Carcinoma Jong Min Kim, Phil Hyun Song, Hyun Tae Kim, Tong Choon Park
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute
 Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
Clinical Study The Role of Pathology in Small Renal Mass Laparoscopic Cryoablation
 Advances in Urology Volume 2012, Article ID 539648, 6 pages doi:10.1155/2012/539648 Clinical Study The Role of Pathology in Small Renal Mass Laparoscopic Cryoablation B. W. Lagerveld, 1 H. van Dekken,
Advances in Urology Volume 2012, Article ID 539648, 6 pages doi:10.1155/2012/539648 Clinical Study The Role of Pathology in Small Renal Mass Laparoscopic Cryoablation B. W. Lagerveld, 1 H. van Dekken,
Active surveillance for clinically localized renal tumors: An updated review of current indications and clinical outcomes
 bs_bs_banner International Journal of Urology (2015) 22, 432 438 doi: 10.1111/iju.12734 Review Article Active surveillance for clinically localized renal tumors: An updated review of current indications
bs_bs_banner International Journal of Urology (2015) 22, 432 438 doi: 10.1111/iju.12734 Review Article Active surveillance for clinically localized renal tumors: An updated review of current indications
Vincenzo Ficarra 1,2,3. Associate Editor BJU International
 Partial Nephrectomy for RCC Vincenzo Ficarra 1,2,3 1 Director Department of Urology University of Udine, Italy 2 Associate Editor BJU International 3 Scientific Director OLV Robotic Surgery Institute,
Partial Nephrectomy for RCC Vincenzo Ficarra 1,2,3 1 Director Department of Urology University of Udine, Italy 2 Associate Editor BJU International 3 Scientific Director OLV Robotic Surgery Institute,
Optimal Treatment of ct1b Renal Mass in Patient with Normal GFR: a Role for Radical Nephrectomy?
 Optimal Treatment of ct1b Renal Mass in Patient with Normal GFR: a Role for Radical Nephrectomy? Steven C. Campbell, MD, PhD Program Director, Vice Chairman Department of Urology Center for Urologic Oncology
Optimal Treatment of ct1b Renal Mass in Patient with Normal GFR: a Role for Radical Nephrectomy? Steven C. Campbell, MD, PhD Program Director, Vice Chairman Department of Urology Center for Urologic Oncology
Comparison of Long-Term Results After Nephron-Sparing Surgery and Radical Nephrectomy in Treating 4- to 7-cm Renal Cell Carcinoma
 :3-8 3 Comparison of Long-Term Results After Nephron-Sparing Surgery and Radical Nephrectomy in Treating 4- to 7-cm Renal Cell Carcinoma Daimantas Milonas, Giedrius Skulčius, Ruslanas Baltrimavičius, Stasys
:3-8 3 Comparison of Long-Term Results After Nephron-Sparing Surgery and Radical Nephrectomy in Treating 4- to 7-cm Renal Cell Carcinoma Daimantas Milonas, Giedrius Skulčius, Ruslanas Baltrimavičius, Stasys
Research Article Practice Trends in the Surgical Management of Renal Tumors in an Academic Medical Center in the Past Decade
 ISRN Endoscopy Volume 2013, Article ID 945853, 5 pages http://dx.doi.org/10.5402/2013/945853 Research Article Practice Trends in the Surgical Management of Renal Tumors in an Academic Medical Center in
ISRN Endoscopy Volume 2013, Article ID 945853, 5 pages http://dx.doi.org/10.5402/2013/945853 Research Article Practice Trends in the Surgical Management of Renal Tumors in an Academic Medical Center in
Canadian Urological Association guidelines for followup of patients after treatment of nonmetastatic
 Canadian Urological Association guidelines for followup of patients after treatment of nonmetastatic renal cell carcinoma Wassim Kassouf, Leonardo L. Monteiro, Darrel E. Drachenberg, Adrian S. Fairey,
Canadian Urological Association guidelines for followup of patients after treatment of nonmetastatic renal cell carcinoma Wassim Kassouf, Leonardo L. Monteiro, Darrel E. Drachenberg, Adrian S. Fairey,
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018
 Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Surveillance Strategies in Kidney Cancer: When is Enough? Role of Survivorship Clinic in Long-Term Follow-Up of Kidney Cancer
 Surveillance Strategies in Kidney Cancer: When is Enough? Role of Survivorship Clinic in Long-Term Follow-Up of Kidney Cancer Brandon Manley, MD Assistant Member, Genitourinary Oncology Department of Genitourinary
Surveillance Strategies in Kidney Cancer: When is Enough? Role of Survivorship Clinic in Long-Term Follow-Up of Kidney Cancer Brandon Manley, MD Assistant Member, Genitourinary Oncology Department of Genitourinary
AUA Guidelines Renal Mass and Localized Kidney Cancer
 AUA Guidelines Renal Mass and Localized Kidney Cancer Steven C. Campbell, MD, PhD Chair AUA Guidelines Panel Professor Surgery, Vice Chair, Program Director Department of Urology Glickman Urological and
AUA Guidelines Renal Mass and Localized Kidney Cancer Steven C. Campbell, MD, PhD Chair AUA Guidelines Panel Professor Surgery, Vice Chair, Program Director Department of Urology Glickman Urological and
Minimal invasive treatment of small renal masses
 Minimal invasive treatment of small renal masses Financial disclosure: Advisor and proctor: BTG Ole Graumann, MD, PhD, Associate Professor Dep. of Radiology, Odense University Hospital Head of Radiology
Minimal invasive treatment of small renal masses Financial disclosure: Advisor and proctor: BTG Ole Graumann, MD, PhD, Associate Professor Dep. of Radiology, Odense University Hospital Head of Radiology
The Incidental Renal Mass in the Primary Care Setting
 The Incidental Renal Mass in the Primary Care Setting Adele M. Caruso, MSN, CRNP Adult Nurse Practitioner The Perelman School of Medicine at the University of Pennsylvania Abstract There are approximately
The Incidental Renal Mass in the Primary Care Setting Adele M. Caruso, MSN, CRNP Adult Nurse Practitioner The Perelman School of Medicine at the University of Pennsylvania Abstract There are approximately
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 2 JANUARY 0 200 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Evaluating Overall Survival and Competing Risks of Death in Patients With Localized Renal Cell Carcinoma Using
VOLUME 28 NUMBER 2 JANUARY 0 200 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Evaluating Overall Survival and Competing Risks of Death in Patients With Localized Renal Cell Carcinoma Using
Vincenzo Ficarra. Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine
 Best Papers on Kidney Cancer Vincenzo Ficarra Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine Uro-oncological oncological topics Renal Tumor biopsy Positive Surgical Margins after
Best Papers on Kidney Cancer Vincenzo Ficarra Direttore Clinica di Urologia Azienda Ospedaliera Universitaria di Udine Uro-oncological oncological topics Renal Tumor biopsy Positive Surgical Margins after
Guidelines on Renal Cell
 Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
Clinical/Surgical trials that will change my practice
 Clinical/Surgical trials that will change my practice Mr Jim M Adshead Herts and Beds Urological Cancer Centre, Lister Hospital What s changed and where do I feel we are clutching at straws? Regional Specialist
Clinical/Surgical trials that will change my practice Mr Jim M Adshead Herts and Beds Urological Cancer Centre, Lister Hospital What s changed and where do I feel we are clutching at straws? Regional Specialist
Management, pathology and outcomes of Bosniak category IIF and III cystic renal lesions
 World J Urol (2015) 33:295 300 DOI 10.1007/s00345-014-1301-x ORIGINAL ARTICLE Management, pathology and outcomes of Bosniak category IIF and III cystic renal lesions Peter Weibl Milan Hora Boris Kollarik
World J Urol (2015) 33:295 300 DOI 10.1007/s00345-014-1301-x ORIGINAL ARTICLE Management, pathology and outcomes of Bosniak category IIF and III cystic renal lesions Peter Weibl Milan Hora Boris Kollarik
Partial Nephrectomy Is Associated with Improved Overall Survival Compared to Radical Nephrectomy in Patients with Unanticipated Benign Renal Tumours
 EUROPEAN UROLOGY 58 (2010) 293 298 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Partial Nephrectomy Is Associated with Improved Overall Survival Compared to
EUROPEAN UROLOGY 58 (2010) 293 298 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Partial Nephrectomy Is Associated with Improved Overall Survival Compared to
Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia
 original research Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia Dong Soo Park, MD; * Jin Ho Hwang, MD; * Moon Hyung
original research Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia Dong Soo Park, MD; * Jin Ho Hwang, MD; * Moon Hyung
RCC in ADPKD / CKD / ESRD
 RCC in ADPKD / CKD / ESRD FOIU 2018 David A. Goldfarb, MD,FACS Professor of Surgery, Cleveland Clinic Lerner College of Medicine Glickman Urological and Kidney Institute Cleveland Clinic, Cleveland, Ohio
RCC in ADPKD / CKD / ESRD FOIU 2018 David A. Goldfarb, MD,FACS Professor of Surgery, Cleveland Clinic Lerner College of Medicine Glickman Urological and Kidney Institute Cleveland Clinic, Cleveland, Ohio
Renal cryoablation versus robot-assisted partial nephrectomy: Washington University long-term experience
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 12-16-2013 Renal cryoablation versus robot-assisted partial nephrectomy: Washington University long-term experience
Washington University School of Medicine Digital Commons@Becker Open Access Publications 12-16-2013 Renal cryoablation versus robot-assisted partial nephrectomy: Washington University long-term experience
Surgical Management of Renal Cancer. David Nicol Consultant Urologist
 Surgical Management of Renal Cancer David Nicol Consultant Urologist Roles of Surgery 1. Curative intervention localised disease 2. Symptomatic control advanced disease 3. Augmentation of efficacy of systemic
Surgical Management of Renal Cancer David Nicol Consultant Urologist Roles of Surgery 1. Curative intervention localised disease 2. Symptomatic control advanced disease 3. Augmentation of efficacy of systemic
EUROPEAN UROLOGY 61 (2012)
 EUROPEAN UROLOGY 61 (2012) 1156 1161 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alvin C. Goh and Inderbir S. Gill on pp. 1162
EUROPEAN UROLOGY 61 (2012) 1156 1161 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alvin C. Goh and Inderbir S. Gill on pp. 1162
The role of cytoreductive. nephrectomy in elderly patients. with metastatic renal cell. carcinoma in an era of targeted. therapy
 The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
ACTIVE SURVEILLANCE OF RCTs
 . JOURNAL COMPILATION 2010 BJU INTERNATIONAL Mini Reviews T1 RENAL CORTICAL TUMOURS CUTRESS ET AL. BJUI BJU INTERNATIONAL Update on the management of T1 renal cortical tumours Mark L. Cutress, Hari L.
. JOURNAL COMPILATION 2010 BJU INTERNATIONAL Mini Reviews T1 RENAL CORTICAL TUMOURS CUTRESS ET AL. BJUI BJU INTERNATIONAL Update on the management of T1 renal cortical tumours Mark L. Cutress, Hari L.
Robotic Partial Nephrectomy Versus Laparoscopic Cryoablation for the Small Renal Mass
 EUROPEAN UROLOGY 61 (2012) 899 904 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Jose A. Karam and Christopher G. Wood on pp.
EUROPEAN UROLOGY 61 (2012) 899 904 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Jose A. Karam and Christopher G. Wood on pp.
Small Renal Mass Guidelines. Clif Vestal, MD USMD Arlington, Texas
 Small Renal Mass Guidelines Clif Vestal, MD USMD Arlington, Texas Evaluation/Diagnosis 1. Obtain high quality, multiphase, cross-sectional abdominal imaging to optimally characterize/stage the renal mass.
Small Renal Mass Guidelines Clif Vestal, MD USMD Arlington, Texas Evaluation/Diagnosis 1. Obtain high quality, multiphase, cross-sectional abdominal imaging to optimally characterize/stage the renal mass.
Treatment of Patients With Small Renal Masses: A Survey of the American Urological Association
 Treatment of Patients With Small Renal Masses: A Survey of the American Urological Association Rodney H. Breau,*, Paul L. Crispen,* Sarah M. Jenkins, Michael L. Blute and Bradley C. Leibovich From the
Treatment of Patients With Small Renal Masses: A Survey of the American Urological Association Rodney H. Breau,*, Paul L. Crispen,* Sarah M. Jenkins, Michael L. Blute and Bradley C. Leibovich From the
Research Article Multifocal Renal Cell Carcinoma: Clinicopathologic Features and Outcomes for Tumors 4cm
 Hindawi Publishing Corporation Advances in Urology Volume 28, Article ID 51891, 7 pages doi:1.1155/28/51891 Research Article Renal Cell Carcinoma: Clinicopathologic Features and Outcomes for Tumors 4cm
Hindawi Publishing Corporation Advances in Urology Volume 28, Article ID 51891, 7 pages doi:1.1155/28/51891 Research Article Renal Cell Carcinoma: Clinicopathologic Features and Outcomes for Tumors 4cm
Renal Masses in Patients with Known Extrarenal Primary Primary Cancer Primary Primary n Met Mets s RCC Beni L mphoma Lung Breast Others
 The Importance of Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston, MA The Importance of
The Importance of Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston, MA The Importance of
Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma
 ONCOLOGY LETTERS 9: 125-130, 2015 Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma KEIICHI ITO 1, KENJI SEGUCHI 1, HIDEYUKI SHIMAZAKI 2, EIJI TAKAHASHI
ONCOLOGY LETTERS 9: 125-130, 2015 Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma KEIICHI ITO 1, KENJI SEGUCHI 1, HIDEYUKI SHIMAZAKI 2, EIJI TAKAHASHI
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
Comparison of Glomerular Filtration Rate (GFR) (RCC)
 Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-323X) Vol. 3(10) pp. 467-471, October, 2015 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2015 Merit
Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-323X) Vol. 3(10) pp. 467-471, October, 2015 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2015 Merit
Cancer. Description. Section: Surgery Effective Date: October 15, 2016 Subsection: Original Policy Date: September 9, 2011 Subject:
 Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Research Article Cancer Characteristics and Current Treatments of Patients with Renal Cell Carcinoma in Sweden
 BioMed Research International Volume 2015, Article ID 456040, 5 pages http://dx.doi.org/10.1155/2015/456040 Research Article Cancer Characteristics and Current Treatments of Patients with Renal Cell Carcinoma
BioMed Research International Volume 2015, Article ID 456040, 5 pages http://dx.doi.org/10.1155/2015/456040 Research Article Cancer Characteristics and Current Treatments of Patients with Renal Cell Carcinoma
SAMPLING OF POST NEPHRECTOMY CANCER CARE (5)
 SAMPLING OF POST NEPHRECTOMY CANCER CARE (5) Universally recognized post-nephrectomy cancer treatment. Sampling: National Comprehensive Cancer Network (NCCN) NCCN Clinical Practice Guidelines in Oncology
SAMPLING OF POST NEPHRECTOMY CANCER CARE (5) Universally recognized post-nephrectomy cancer treatment. Sampling: National Comprehensive Cancer Network (NCCN) NCCN Clinical Practice Guidelines in Oncology
Anatomic Features of Enhancing Renal Masses Predict Malignant and High-Grade Pathology: A Preoperative Nomogram Using the RENAL Nephrometry Score
 EUROPEAN UROLOGY 60 (2011) 241 248 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Brian F. Chapin and Christopher G. Wood on pp.
EUROPEAN UROLOGY 60 (2011) 241 248 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Brian F. Chapin and Christopher G. Wood on pp.
Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy for pathologic T1a lesions
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy
RENAL CANCER GUIDELINES
 Greater Manchester and Cheshire Cancer Network RENAL CANCER GUIDELINES Agreed by Urology CSG: July 2010 Review Date: July 2012 Renal Cancer Guidelines 1. Introduction 1.1 Kidney cancer accounts for 3%
Greater Manchester and Cheshire Cancer Network RENAL CANCER GUIDELINES Agreed by Urology CSG: July 2010 Review Date: July 2012 Renal Cancer Guidelines 1. Introduction 1.1 Kidney cancer accounts for 3%
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense?
 Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
RENAL CANCER. Dr. Giandomenico Roviello. Oncologia Medica Ospedale San Donato Arezzo
 RENAL CANCER Dr. Giandomenico Roviello Oncologia Medica Ospedale San Donato Arezzo Abstracts Abstract Number: 433. Cryoablation of ct1 renal masses in the healthy patient: Early outcomes from Mayo Clinic.
RENAL CANCER Dr. Giandomenico Roviello Oncologia Medica Ospedale San Donato Arezzo Abstracts Abstract Number: 433. Cryoablation of ct1 renal masses in the healthy patient: Early outcomes from Mayo Clinic.
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation. Basics. What is Percutaneous Ablation? Where are your kidneys?
 Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Carcinoma renale (I): Posters Review. Elena Verzoni Oncologia Medica 1 SS.Oncologia Genitourinaria Fondazione IRCCS Istituto Nazionale Tumori Milano
 Carcinoma renale (I): Posters Review Elena Verzoni Oncologia Medica 1 SS.Oncologia Genitourinaria Fondazione IRCCS Istituto Nazionale Tumori Milano Agenda: Best Posters in Localized RCC Surgery: CN (#
Carcinoma renale (I): Posters Review Elena Verzoni Oncologia Medica 1 SS.Oncologia Genitourinaria Fondazione IRCCS Istituto Nazionale Tumori Milano Agenda: Best Posters in Localized RCC Surgery: CN (#
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
King s Research Portal
 King s Research Portal DOI: 10.1016/j.ijsu.2016.11.096 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Kasivisvanathan,
King s Research Portal DOI: 10.1016/j.ijsu.2016.11.096 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Kasivisvanathan,
Florida Cancer Specialist & Research Institute, Sebastian and Vero Beach, Fl, USA 3
 Evaluation of Perioperative Outcomes and Renal Function after Robotic Assisted Laparoscopic Partial Nephrectomy Off/On Clamp: Comparison of ct1a versus ct1b Renal Masses Hugo H Davila 1-4*, Raul E Storey
Evaluation of Perioperative Outcomes and Renal Function after Robotic Assisted Laparoscopic Partial Nephrectomy Off/On Clamp: Comparison of ct1a versus ct1b Renal Masses Hugo H Davila 1-4*, Raul E Storey
Radical Nephrectomy for Renal Cell Carcinoma Its Contemporary Role Related to Histologic Type, Tumor Size, and Nodal Status: A Retrospective Study
 AJCP /ORIGINAL ARTICLE Radical Nephrectomy for Renal Cell Carcinoma Its Contemporary Role Related to Histologic Type, Tumor Size, and Nodal Status: A Retrospective Study Kamran M. Mirza, MD, PhD, Jerome
AJCP /ORIGINAL ARTICLE Radical Nephrectomy for Renal Cell Carcinoma Its Contemporary Role Related to Histologic Type, Tumor Size, and Nodal Status: A Retrospective Study Kamran M. Mirza, MD, PhD, Jerome
Debate: Lymphadenectomy is Important in mrcc, CON P. Mulder, M.D., Ph.D. JJ. Patard, MD, Ph.D.
 Debate: Lymphadenectomy is Important in mrcc, CON P. Mulder, M.D., Ph.D. JJ. Patard, MD, Ph.D.. Eighth European International Kidney Cancer Symposium Budapest 03-04 May 2013 The role of LND In organ confined
Debate: Lymphadenectomy is Important in mrcc, CON P. Mulder, M.D., Ph.D. JJ. Patard, MD, Ph.D.. Eighth European International Kidney Cancer Symposium Budapest 03-04 May 2013 The role of LND In organ confined
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
State-of-the-art: vision on the future. Urology
 State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
Freeze, Fry or Cut. Jennifer A. Linehan, MD Associate Professor Urologic Oncology John Wayne Cancer Institute 2/9/2018
 Freeze, Fry or Cut Jennifer A. Linehan, MD Associate Professor Urologic Oncology John Wayne Cancer Institute 2/9/2018 Disclosures Consultant for UroGen Pharma. REDEFINING WHAT SURGEONS SEE Bay Area-based
Freeze, Fry or Cut Jennifer A. Linehan, MD Associate Professor Urologic Oncology John Wayne Cancer Institute 2/9/2018 Disclosures Consultant for UroGen Pharma. REDEFINING WHAT SURGEONS SEE Bay Area-based
Hyperechoic renal masses
 Hyperechoic renal masses Jean-Yves Meuwly, MD Department of Diagnostic and Interventional Radiology, University Hospital Lausanne, Switzerland Department of Diagnostic and Interventional Radiology Renal
Hyperechoic renal masses Jean-Yves Meuwly, MD Department of Diagnostic and Interventional Radiology, University Hospital Lausanne, Switzerland Department of Diagnostic and Interventional Radiology Renal
Manchester Cancer. Guidelines for the management of renal cancer
 Guidelines for the management of renal cancer Approved by the urology pathway board September 2014 To be reviewed September 2016 Renal Cancer Guidelines 1. Introduction 1.1 Kidney cancer accounts for 3%
Guidelines for the management of renal cancer Approved by the urology pathway board September 2014 To be reviewed September 2016 Renal Cancer Guidelines 1. Introduction 1.1 Kidney cancer accounts for 3%
Clinical Study A Single Surgeon s Experience with Open, Laparoscopic, and Robotic Partial Nephrectomy
 International Scholarly Research Notices, Article ID 430914, 5 pages http://dx.doi.org/10.1155/2014/430914 Clinical Study A Single Surgeon s Experience with Open, Laparoscopic, and Robotic Partial Nephrectomy
International Scholarly Research Notices, Article ID 430914, 5 pages http://dx.doi.org/10.1155/2014/430914 Clinical Study A Single Surgeon s Experience with Open, Laparoscopic, and Robotic Partial Nephrectomy
Recent Developments in Research on Kidney Cancer: Highlights from Urological and Oncological Congresses in 2007
 european urology supplements 7 (2008) 494 507 available at www.sciencedirect.com journal homepage: www.europeanurology.com Recent Developments in Research on Kidney Cancer: Highlights from Urological and
european urology supplements 7 (2008) 494 507 available at www.sciencedirect.com journal homepage: www.europeanurology.com Recent Developments in Research on Kidney Cancer: Highlights from Urological and
concordance indices were calculated for the entire model and subsequently for each risk group.
 ; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
Pathologic Characteristics of Solitary Small Renal Masses. Can They Be Predicted by Preoperative Clinical Parameters?
 Anatomic Pathology / Pathology of Small Renal Masses Pathologic Characteristics of Solitary Small Renal Masses Can They Be Predicted by Preoperative Clinical Parameters? Tom DeRoche, MD, 1 Esteban Walker,
Anatomic Pathology / Pathology of Small Renal Masses Pathologic Characteristics of Solitary Small Renal Masses Can They Be Predicted by Preoperative Clinical Parameters? Tom DeRoche, MD, 1 Esteban Walker,
Controversies in Prostate Cancer Screening
 Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Lymphadenectomy in RCC: Yes, No, Clinical Trial?
 Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy
 Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy Joshua J. Meeks, Marc Walker*, Melanie Bernstein, Matthew Kent and James A. Eastham Urology Service, Department of Surgery and
Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy Joshua J. Meeks, Marc Walker*, Melanie Bernstein, Matthew Kent and James A. Eastham Urology Service, Department of Surgery and
Understanding the risk of recurrence after primary treatment for prostate cancer. Aditya Bagrodia, MD
 Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Clinical Symptoms Predict Poor Overall Survival in Chronic-dialysis Patients with Renal Cell Carcinoma Associated with End-stage Renal Disease
 Jpn J Clin Oncol 2014;44(11)1096 1100 doi:10.1093/jjco/hyu117 Advance Access Publication 19 August 2014 Clinical Symptoms Predict Poor Overall Survival in Chronic-dialysis Patients with Renal Cell Carcinoma
Jpn J Clin Oncol 2014;44(11)1096 1100 doi:10.1093/jjco/hyu117 Advance Access Publication 19 August 2014 Clinical Symptoms Predict Poor Overall Survival in Chronic-dialysis Patients with Renal Cell Carcinoma
Sommerakademie Munich, June
 Active surveillance: Shrinking the grey zone Sommerakademie Munich, June 30 2016 Active surveillance Overview of 20 year history Laurence Klotz, MD, CM Professor of Surgery Sunnybrook Heatlh Sciences Centre
Active surveillance: Shrinking the grey zone Sommerakademie Munich, June 30 2016 Active surveillance Overview of 20 year history Laurence Klotz, MD, CM Professor of Surgery Sunnybrook Heatlh Sciences Centre
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
Directness Consistency Precision Reporting Bias
 responsible for the accuracy and presentation of the material. Supplemental Table. Strength of evidence for primary. Key Outcomes* Studies (N) Study limitations Directness Consistency Precision Reporting
responsible for the accuracy and presentation of the material. Supplemental Table. Strength of evidence for primary. Key Outcomes* Studies (N) Study limitations Directness Consistency Precision Reporting
Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors
 Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors Grant D. Schmit,* R. Houston Thompson, Anil N. Kurup, Adam J.
Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors Grant D. Schmit,* R. Houston Thompson, Anil N. Kurup, Adam J.
