Use of panel tests in place of single gene tests in the cancer genetics clinic
|
|
|
- Ambrose Henderson
- 5 years ago
- Views:
Transcription
1 Clin Genet 2015: 88: Printed in Singapore. All rights reserved CLINICAL GENETICS doi: /cge Short Report se of panel tests in place of single gene tests in the cancer genetics clinic Yorczyk A, Robinson LS, Ross TS. se of panel tests in place of single gene tests in the cancer genetics clinic. Clin Genet 2015: 88: The Authors. Clinical Genetics published by John Wiley & Sons A/S. Published by John Wiley & Sons Ltd., 2014 Improved technology has made it possible to test for mutations within multiple genes simultaneously. It is not clear when these gene panels should be used in the hereditary cancer setting. These analyses were intended to guide panel testing criteria. Offering hereditary panel testing as a first and final, single-tier, option was explored. A two-tiered approach, in which panel testing is offered reflexively following stricter criteria, was then applied to the same data. Within our cohort of 105 patients, the single-tier approach was associated with a higher mutation detection rate (6.7% vs 3.8%) and variant of uncertain significance (VS) rate (0.94 vs 0.23 average per person) compared to a two-tiered approach. Of the VSs also identified in other patients by another lab, 53% were classified differently between laboratories. Individuals reporting African American race had more VSs compared to other ancestry groups (p = 0.001). The test cost for a single-tier test was 21% more than a two-tiered approach. Single-tier panel testing was associated with higher mutation and VS rates, and there is inconsistent classification of the VS/low penetrant genes between laboratories. Conflict of interest The authors report no conflicts of interest. A. Yorczyk a,b, L.S. Robinson a,b and T.S. Ross a,b a Department of Cancer Genetics, niversity of Texas Southwestern Medical Center s Harold Simmons Comprehensive Cancer Center, Dallas, TX, SA and b Department of Cancer Genetics, niversity of Texas Southwestern Medical Center s Moncrief Cancer Institute, Fort Worth, TX, SA Key words: hereditary cancer next-generation sequencing panel testing Corresponding author: Theodora S. Ross, Department of Cancer Genetics, T Southwestern Medical Center, 5323 Harry Hines Blvd, MC 8852, Dallas, TX , SA. Tel.: ; fax: ; theo.ross@utsouthwestern.edu Received 17 May 2014, revised and accepted for publication 18 August 2014 Individuals with hereditary predispositions to cancer are at an increased risk to develop specific cancers compared to the general population. Next-generation sequencing (NGS) has allowed for the ability to analyze multiple genes simultaneously in panel tests at a reduced cost compared to Sanger sequencing (1, 2). Recently, we gained the ability to apply NGS technology to diagnose hereditary cancer syndromes accurately (3). Two-tiered strategies for incorporating hereditary cancer panels into a testing algorithm have been proposed (4, 5). This involves initial testing for genes with higher penetrance such as BRCA1/2 and reflexing to hereditary panels upon return of a negative results based on the level of risk and consideration of other syndromes (5). As part of the early phase for the panel test offered by Myriad Genetics, select providers were given the opportunity to offer a single, multi-cancer gene panel test at no extra cost to patients meeting specific criteria for hereditary breast and colon cancer testing. sing these data, we assessed the benefits and limitations of single-tier hereditary cancer panel testing, compared to the previously proposed two-tiered approach (5). The mutation rates, variant of undetermined significance (VS) rates, and test costs were compared between the two approaches. Materials and methods The panel test used, MyRisk, in the single-tier option included 25 genes; APC, ATM, BARD1, BMPR1A, BRCA1, BRCA2, BRIP1, CDH1, CDK4, CDKN2A, CHEK2, EPCAM, MLH1, MSH2, MSH6, MTYH, NBN, PALB2, PMS2, PTEN, RAD51C, RAD51D, SMAD4, STK11, and TP53. Patients were eligible for the panel test as a first-tier test at no extra cost if they The Authors. Clinical Genetics published by John Wiley & Sons A/S. Published by John Wiley & Sons Ltd. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs License, which permits use and distribution in any medium, provided the original work is properly cited, the use is non-commercial and no modifications or adaptations are made.
2 se of panel tests in the cancer genetics clinic 468 new patients seen by a genetic 370 underwent hereditary testing 98 did not meet criteria for testing or were unable to undergo testing for other reasons 318 qualified for BRCA1 or BRCA2 gene testing, or Lynch syndrome testing 52 patients underwent hereditary testing, but did not qualify for BRCA1or BRCA2 gene testing, or Lynch syndrome testing 301 underwent germline testing 17 underwent Lynch syndrome tumor testing that was either negative or guided gene-specific testing 132 underwent the hereditary cancer panel test offered by Myriad Genetics 169 excluded 143 patients did not undergo hereditary panel testing 26 patients underwent testing through a different laboratory 27 tests were either not resulted in time or were cancelled 105 tests results were returned for study participation Fig. 1. Details of patient accrual. All patients evaluated in our cancer genetics clinics during the fall of 2013 were offered panel testing if they qualified for BRCA1/2 or Lynch Syndrome testing. met their health insurance criteria for BRCA1/2 or Lynch syndrome gene testing. Patients were excluded from this multi-cancer syndrome panel if they underwent prior BRCA1/2 or Lynch syndrome gene testing, required a saliva sample, or needed a quick turn-around time. All patients meeting these criteria were offered the hereditary multi-cancer panel test and genetic counseling. Although the original goal was to analyze the first 100 results, 6 results were received on the final day, so 105 patients were included (Fig. 1). Following this single-tier approach, a review was performed to determine deleterious mutation rates and VSs rates. Genetics also provided their interpretations of the VSs identified in these patients. The significance of the average differences in the number of VSs between ancestry categories were evaluated using a one-way anova statistical test. sing the data from the same patient cohort, mutation and VS rates that would have resulted if the patient population had undergone a stricter, two-tiered approach were calculated based on the criteria originally proposed by Mauer et al. (Table S1, Supporting Information) (5). We also compared the costs of the single-tier method to a two-tiered method. The client prices for various NGS cancer panels, BRCA gene testing, and Lynch syndrome gene testing were averaged. The prices from nine clinical labs were used to determine average cost per person of the single-tier and two-tiered methods. Results From September through November 2013, 468 patients were seen for genetic counseling (Fig. 1). Of these, 370 elected to proceed with genetic testing, and
3 Yorczyk et al. Table 1. Deleterious mutations detected using single-tier method vs two-tier method Actionable mutations reported in our cohort by single-tier panel testing Mutation detected using single-tier (panel-only) method Mutation detected using two-tiered method Mutation detected in the first tier Mutation detected in the reflexive second tier APC c.3920t>a (I1307K) Yes No No BRCA1 c t>g Yes Yes n/a BRCA1 c t>g Yes Yes n/a BRCA2 c.9302del Yes Yes n/a BRCA2 del exons Yes Yes n/a CHEK2 c.1555c>t Yes No No EPCAM 3 term del Yes No No qualified for BRCA1/2 testing and/or Lynch syndrome testing. Of these, 17 had previous colon tumor testing that either obviated the need for germline testing or guided gene-specific testing. Of the remaining 301 patients, a total of 169 patients did not have the panel test because they met Myriad s exclusion criteria (see Materials and Methods) or they had panel testing through another lab (n = 26). A total of 132 patients (44%) underwent panel testing by Myriad Genetics and the first 105 test results were evaluated. Of the 105 study patients, 100 (95.2%) were female. Seventeen patients (16.2%) reported African American, two (1.9%) Ashkenazi Jewish, three (2.9%) Asian, thirteen (12.4%) Hispanic, Latin American, or Caribbean, six (5.7%) Native American, and 72 (68.6%) European descent. A total of 61 (58%) had a current or prior cancer diagnosis. sing the hereditary cancer panel as a single-tier test for individuals who met BRCA1/2 or Lynch syndrome testing criteria, seven individuals (6.7%) were reported to have a deleterious or suspected deleterious mutation. These were within APC, BRCA1/2, CHEK2, orepcam gene (Table 1). The seven mutation patients met NCCN guidelines for BRCA1/2 gene testing. One of these mutations (APC c.3920t>a) was classified as suspected deleterious. We next analyzed our data using a two-tiered method (Table S1) in which the most likely hereditary cancer syndrome is tested first then reflexing to panel if no mutation was detected. Four (3.8%) of the seven mutations would have been detected (all BRCA1/2) (Table 1). Of the 105 patients examined, 32 patients would have been recommended for a second-tier, reflex panel test following the criteria from Mauer et al. (Table S1) (5). No additional mutations would have been detected in the second tier in our cohort based on these criteria. The single-tier panel test approach increased our detection rate to 6.7% from 3.8% where three additional reported mutations (APC, CHEK2, and EPCAM), were detected. The family and medical history were not characteristic of the predicted phenotypes associated with these genes. sing the single-tier approach, 74 unique VSs were called by Myriad where each panel gene had a VSs at least once in this cohort (Table S2). We compared the interpretation of these variants with another laboratory, Genetics. Of the 74 VSs found in the study, observed and interpreted 32 of them. Of these 32 VSs, 17 (53%) were classified differently by (Table 2). One of the six deleterious mutations, the well-studied APC alteration (p.i1307k) would have been classified as a pathogenic mutation with reduced penetrance by Genetics. This difference reflects the considerable debate about the clinical significance of this mutation. Thirteen of the Myriad VSs would have been reported as polymorphisms by Genetics, and three of the VSs would have been classified as likely benign. One variant reported by Myriad (CHEK2 c.470>t) would have been reported as a moderate penetrance mutation with a comment regarding variant specific risks. Thirty-three VSs reported by Myriad were not yet classified by at the time of data collection and nine intronic variants would not have been reported by. sing the single-tier approach, 99 VSs (0.94 per person) were detected overall (Table S3). If a stricter, two-tiered approach had been applied, only 24 VSs (0.23 per person) would have been detected. As expected, those who reported African American ethnicity had statistically higher rate of VSs compared to other ethnicities (p = 0.001). sing the average cost of hereditary panels from various labs, the cost of a single-tier, panel-only test would have been $4099 per person, or an estimated $430,425 for all 105 patients. Had a two-tiered approach been used instead, $2190 would have been spent per person on the first-tier test, and $3392, would have been spent in test charges per person upon completion of the second tier ($356,244 in total) (Table S3). The cost of the single-tier hereditary panel test was therefore 21% higher compared to the stricter two-tiered approach. Discussion As the cancer genetic community is moving to NGS panel testing, there are still many unanswered questions. By analyzing our cohort of patients that had initial panel testing against published two-tiered testing criteria, we found that more mutations would be found, but at a higher test cost. In addition, the types of mutations found were not always expected based on the family 280
4 se of panel tests in the cancer genetics clinic Table 2. The VSs and mutations reported by Myriad Genetics were not all interpreted the same by Genetics at the time of test report a Myriad VS APC c.1145g>a APC c.4336g>a APC c.6670a>g APC c.721g>a APC c.8161c>t ATM c.1132a>g ATM c.1430a>g ATM c.1464g>t ATM c.1516g>t ATM c.1810c>t ATM c.186-7c>t ATM c.2289t>a ATM c.2362a>c ATM c.2442c>a ATM c.320g>a ATM c.334g>a ATM c.4388t>g ATM c a>g ATM c.6088a>g ATM c.6919c>t BARD1 c.1216c>g BARD1 c.1738g>a BARD1 c.1793c>a BARD1 c.776a>g BARD1 c.899c>t BMPR1A c A>G BRCA1 c.2346t>a BRIP1 c.151g>a BRIP1 c.205g>a BRIP1 c.258_269del BRIP1 c.2873t>a BRIP1 c.890a>g CDH1 c c>g CDH1 c.688-4t>c CDK4 c.776c>t CDKN2A c.-25c>t CDKN2A c.-2g>a CDKN2A c.316g>a CDKN2A c.369t>a CDKN2A c.430c>t CHEK2 c.1510g>c CHEK2 c.382c>a CHEK2 c.410g>a CHEK2 c.442a>g CHEK2 c.470t>c CHEK2 c.707t>c CHEK2 c.715g>a MLH1 c.1245t>g MLH1 c.2217t>g MLH1 c.2239c>t MLH1 c.-25t>c MSH2 c.1004c>g MSH2 c c>a MSH6 c.1028c>t MSH6 c G>A MTYH c.1450g>a MTYH c.821g>a VS VS VS VS VS VS VS VS b VS VS VS VS Table 2. Continued Myriad VS MTYH c.925c>t NBN c.1489a>g NBN c.1882g>a NBN c G>A NBN c.680t>c PALB2 c.2816t>g PMS2 c.1438g>c PTEN c _802-14del RAD51C c.146-8a>g RAD51C c.431t>c RAD51C c.790g>a RAD51D c.362a>g RAD51D c.698a>g SMAD4 c.1573a>g STK11 c.835g>a TP53 c.1079g>c TP53 c.97-6c>t Myriad mutations APC c.3920t>a b BRCA1 c t>g BRCA2 c.9302del BRCA2 del exons CHEK2 c.1555c>t EPCAM 3 term del VS VS VS c, deleterious/suspected deleterious mutation;, not reported; = polymorphism; = unknown; = variant likely benign. a Intronic alterations beyond ± 5 are only reported by Genetics if they are pathogenic or likely pathogenic mutations. b reported as suspected deleterious ; test report describes fold increased risk for colon cancer. c Reduced penetrance. history and are not well-defined in terms of their clinical significance. In our population, we found an APC mutation (I1307K) in a male non-jewish breast cancer patient, with a mother and grandfather with late onset colon cancer. Thus, the APC gene mutation could help to explain the colon cancer in his family and would not have been detected with two-tiered testing. Another woman with breast cancer at 39 was found to have a CHEK2 c.1555c>t mutation. Her father reportedly had colon cancer at age 46 and a maternal uncle had colon cancer at age 65. The patient did not meet previously proposed criteria (5) for two-tiered testing following negative BRCA1/2 gene testing, nor did she meet criteria previously outlined for CHEK2 gene testing (5). The third mutation, EPCAM 3 term del, was found in a 54-year-old unaffected female who had a family history of breast and ovarian cancer, but no colon cancer. This mutation was not expected based on the family history. It is possible that these patients had incorrectly documented their family histories (6). Offering first-tier panel testing, which includes genes tertiary on the differential, could prevent inaccurate, or even limited, family histories from restricting testing options. 281
5 Yorczyk et al. One of the unexpected findings in our study was the differences between labs classifications of the 74 unique VSs reported by Myriad. Of the 32 variants interpreted by both and Myriad, 17 (53%) were classified differently between the labs. Each lab has a different process for determining the significance of variants, and clinicians need to be aware of these inconsistencies. Sharing information on variant classifications will improve patient care by speeding up the VSs reclassification process. Another challenge of panel testing is the high VSs rate. Individuals of African American ancestry comprised 16.2% of our cohort and had a greater VS frequency compared to those of other ancestries (p = 0.001). Panel testing will certainly result in the detection of moderate penetrance genes, such as ATM and CHEK2. No consensus on recommendations for management or surveillance exists for lower-penetrant genes (3, 7), nor for individuals found to have multiple mutations of moderate penetrance (7). There is also an issue of finding unexpected mutations, such as the EPCAM mutation in our cohort. Clinicians need to counsel patients about unexpected genetic findings or findings that may not affect the management. Of the seven initially reported deleterious mutation or suspected deleterious mutation carriers, six (5.7%) were clinically actionable. The remaining variant, APC c.3920t>a (I1307K) was reported as suspected deleterious by Myriad Genetics with special interpretation that indicated a lower penetrance than standard loss of function APC mutations. Literature review indicates controversy over whether this mutation is associated with a lower penetrance (1.5 to 1.9-fold increased non-polyposis colon cancer risk) (8) or no increased risk (9), thus leading to different interpretations by different laboratories. Single-tier panel test cost was on average $4099 per person, compared to $3392 per person for a two-tiered test. Thus, it was $707 more per person, or $74,235 altogether, to increase the detection rate by 2.9%, and to detect 75% more mutations in our cohort of 105 individuals. This is approximately the cost of treatment for one cancer. Although this is not a complete cost analysis, it appears that offering panel testing as a single-tier test would be cost-effective given the higher detection rate and the elimination of the costs associated with a return to clinic for further testing. Conclusion This is the first analysis that compares the outcomes of a single-tier, panel-only approach to the outcomes that would have resulted using a two-tiered approach. se of a single-tier approach led to clinical reports of three deleterious mutations that would have otherwise gone undetected. There was also a higher VSs rate in the single-tier approach. Similarly, both provider and patient should be aware of the potential to find lower-penetrant mutations for which management recommendations may or may not exist. There was also variability in the interpretation of VSs and lower-penetrant genes between laboratories; data-sharing would help reduce these inconsistencies. The increased diagnosis rate with first-tier hereditary cancer panel testing suggests that this strategy should be discussed with all patients, as the benefits may outweigh the risks and costs for different patients. Supporting Information Additional supporting information may be found in the online version of this article at the publisher s web-site. Acknowledgements We thank Myriad Genetics for the opportunity to perform this study with their MyRisk test. We also thank Genetics, especially Laura Panos and Jill Dolinsky and their colleagues. Finally, we are grateful to the staff of the T Southwestern Genetics group and Marion-Stewart Thomas for her administrative assistance. References 1. Walsh T, Lee MK, Casadei S et al. Detection of inherited mutations for breast and ovarian cancer using genomic capture and massively parallel sequencing. Proc Natl Acad Sci S A 2010: 107: Ku CS, Cooper DN, Iacopetta B et al. Integrating next-generation sequencing into the diagnostic testing of inherited cancer predisposition. Clin Genet 2013: 83: Domchek SM, Bradbury A, Garber JE et al. Multiplex genetic testing for cancer susceptibility: out on the high wire without a net? J Clin Oncol 2013: 31: Walsh T, Casadei S, Lee MK et al. Mutations in 12 genes for inherited ovarian, fallopian tube, and peritoneal carcinoma identified by massively parallel sequencing. Proc Natl Acad Sci S A 2011: 108: Mauer CB, Pirzadeh-Miller SM, Robinson LD et al. The integration of next-generation sequencing panels in the clinical cancer genetics practice: an institutional experience. Genet Med 2014: 16: Murff HJ, Spigel DR, Syngal S. Does this patient have a family history of cancer? An evidence-based analysis of the accuracy of family cancer history. JAMA 2004: 292: National Comprehensive Cancer Network (NCCN) I: Genetic/Familial High-Risk Assessment: Breast and Ovarian, version Woodage T, King SM, Wacholder S et al. The APCI1307K allele and cancer risk in a community-based study of Ashkenazi Jews. Nat Genet 1998: 20: Strul H, Barenboim E, Leshno M et al. The I1307K adenomatous polyposis coli gene variant does not contribute in the assessment of the risk for colorectal cancer in Ashkenazi Jews. Cancer Epidemiol Biomarkers Prev 2003: 12:
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
Why Test for Hereditary Cancer in Preventive Care?
 Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
The Next Generation of Hereditary Cancer Testing
 The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
A Patient s Guide to Hereditary Cancer. Is Hereditary Cancer Testing Right for You?
 A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
Learn your genetic risk for the most common hereditary cancers.
 Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
Germline Testing for Hereditary Cancer with Multigene Panel
 Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective
 Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
Hereditary Cancer Products
 Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer
 GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
Myriad Financial Assistance Program (MFAP)
 Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
The benefit of. knowing. Genetic testing for hereditary cancer. A patient support guide
 The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing.
 Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
A guide to genetic testing for hereditary cancers
 Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Genetic Testing for BRCA1 and BRCA2 Genes
 Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Assessment and Management of Genetic Predisposition to Breast Cancer. Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18
 Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
GYNplus. genetic testing for hereditary ovarian and/or uterine cancer
 GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
Genetic testing and pancreatic disease
 Genetic testing and pancreatic disease February 2 d, 2018 Yale Pancreas Symposium 2018: Multidisciplinary Management of Pancreatic Cancer Xavier Llor, M.D., PhD. Associate Professor of Medicine Co-Director,
Genetic testing and pancreatic disease February 2 d, 2018 Yale Pancreas Symposium 2018: Multidisciplinary Management of Pancreatic Cancer Xavier Llor, M.D., PhD. Associate Professor of Medicine Co-Director,
CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION
 CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION CentoCancer our most comprehensive oncogenetics panel for hereditary mutations Hereditary pathogenic variants confer an increased risk of developing
CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION CentoCancer our most comprehensive oncogenetics panel for hereditary mutations Hereditary pathogenic variants confer an increased risk of developing
Genetic Testing for BRCA1 and BRCA2 Genes
 Genetic Testing f BRCA1 and BRCA2 Genes MP9478 Covered Service: Pri Authization Required: Additional Infmation: Yes when meets criteria below Yes--as shown below Pre and post-test genetic counseling is
Genetic Testing f BRCA1 and BRCA2 Genes MP9478 Covered Service: Pri Authization Required: Additional Infmation: Yes when meets criteria below Yes--as shown below Pre and post-test genetic counseling is
Understanding Your Positive Result. A guide to understanding your risk and taking action
 Understanding Your Positive Result A guide to understanding your risk and taking action 2017 Myriad Genetics, Inc. 320 Wakara Way, Salt Lake City, Utah 84108 PH: 1-800-469-7423 FX: 801-584-3615 1 PART
Understanding Your Positive Result A guide to understanding your risk and taking action 2017 Myriad Genetics, Inc. 320 Wakara Way, Salt Lake City, Utah 84108 PH: 1-800-469-7423 FX: 801-584-3615 1 PART
Genetic Testing: who, what, why?
 Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Variant Reclassification in a Clinical Cohort: A Decade of Experience
 Variant Reclassification in a Clinical Cohort: A Decade of Experience Jacqueline Mersch, MS, CGC 1, Nichole Brown, MS, CGC 1, Sara Pirzadeh Miller, MS, CGC 1, Erin Mundt, MS, CGC 2, Hannah C. Cox, PhD
Variant Reclassification in a Clinical Cohort: A Decade of Experience Jacqueline Mersch, MS, CGC 1, Nichole Brown, MS, CGC 1, Sara Pirzadeh Miller, MS, CGC 1, Erin Mundt, MS, CGC 2, Hannah C. Cox, PhD
Managing Moderate Penetrance
 Managing Moderate Penetrance Thomas Slavin, MD, FACMG Assistant Clinical Professor, Department of Medical Oncology, Division of Clinical Cancer Genetics Program Member, Cancer Control and Population Sciences
Managing Moderate Penetrance Thomas Slavin, MD, FACMG Assistant Clinical Professor, Department of Medical Oncology, Division of Clinical Cancer Genetics Program Member, Cancer Control and Population Sciences
Are you at risk of Hereditary Cancer? Your Guide to the Answers
 Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Genetics and Cancer Care. Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP
 Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
Multigene Panel Testing for Hereditary Cancer Risk
 Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers
 POLICY: PG0067 ORIGINAL EFFECTIVE: 07/30/02 LAST REVIEW: 01/25/18 MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers GUIDELINES This policy does not certify benefits or authorization of benefits,
POLICY: PG0067 ORIGINAL EFFECTIVE: 07/30/02 LAST REVIEW: 01/25/18 MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers GUIDELINES This policy does not certify benefits or authorization of benefits,
BRCAplus. genetic testing for hereditary breast cancer
 BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
Clinical Cancer Genetics
 Clinical Cancer Genetics Lisen Axell, MS, CGC University of Colorado Cancer Center Individuals with cancer Making surgical decisions (lump vs. mast) Making treatment decisions (XRT) Concerns for additional
Clinical Cancer Genetics Lisen Axell, MS, CGC University of Colorado Cancer Center Individuals with cancer Making surgical decisions (lump vs. mast) Making treatment decisions (XRT) Concerns for additional
Genetic testing for hereditary cancer
 Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES GENETIC CANCER SUSCEPTIBILITY PANELS USING NEXT GENERATION SEQUENCING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program
PROVIDER POLICIES & PROCEDURES GENETIC CANCER SUSCEPTIBILITY PANELS USING NEXT GENERATION SEQUENCING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
The Role of genetic Testing for Inherited Prostate Cancer Risk
 FOIU July 2018 The Role of genetic Testing for Inherited Prostate Cancer Risk Leonard G. Gomella, MD Chairman, Department of Urology Sidney Kimmel Cancer Center Thomas Jefferson University Philadelphia,
FOIU July 2018 The Role of genetic Testing for Inherited Prostate Cancer Risk Leonard G. Gomella, MD Chairman, Department of Urology Sidney Kimmel Cancer Center Thomas Jefferson University Philadelphia,
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain
 Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain Why Would We Consider Genetic Testing in Patients With Ovarian Cancer?
Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain Why Would We Consider Genetic Testing in Patients With Ovarian Cancer?
Genetics & Precision Medicine Cancer Care
 Genetics & Precision Medicine Cancer Care Johnathan M. Lancaster, MD PhD Chief Medical Officer Myriad Genetics Copyright 2015 Myriad Genetics, Inc., all rights reserved. www.myriad.com. Precision Medicine
Genetics & Precision Medicine Cancer Care Johnathan M. Lancaster, MD PhD Chief Medical Officer Myriad Genetics Copyright 2015 Myriad Genetics, Inc., all rights reserved. www.myriad.com. Precision Medicine
6/8/17. Genetics 101. Professor, College of Medicine. President & Chief Medical Officer. Hereditary Breast and Ovarian Cancer 2017
 Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Proactive Patient Paves the Way for Genetic Testing of Eight Family Members
 CASE STUDY Proactive Patient Paves the Way for Genetic Testing of Eight Family Members Quick Summary Samar Mohite * was diagnosed with colon adenocarcinoma at the age of 49 years. Genetic counselling was
CASE STUDY Proactive Patient Paves the Way for Genetic Testing of Eight Family Members Quick Summary Samar Mohite * was diagnosed with colon adenocarcinoma at the age of 49 years. Genetic counselling was
Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary?
 May 16, 2016 Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary? Presenter: Emily Kuchinsky, MS, CGC 1 Experiences with Genetic Testing Adverse Events in Cancer Genetic Testing:
May 16, 2016 Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary? Presenter: Emily Kuchinsky, MS, CGC 1 Experiences with Genetic Testing Adverse Events in Cancer Genetic Testing:
Medical Policy Manual. Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer. Date of Origin: January 27, 2011
 Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
Identification of patients suggestive of hereditary breast and ovarian cancer syndrome that warrants further professional evaluation.
 Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention
 patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime types
patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime types
Cancer Survivorship Symposium Cancer and Heredity January 16, Jeanne P. Homer, MS Licensed Certified Genetic Counselor
 Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Objectives. Genetics in Cancer Treatment and Prevention. Genes
 Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
GENETIC TESTING FOR HEREDITARY CANCER
 UnitedHealthcare Oxford Clinical Policy GENETIC TESTING FOR HEREDITARY CANCER Policy Number: DIAGNOSTIC 004.27 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
UnitedHealthcare Oxford Clinical Policy GENETIC TESTING FOR HEREDITARY CANCER Policy Number: DIAGNOSTIC 004.27 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
A pathogenic mutation was identified in the BRCA1 gene.
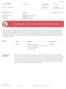 Hereditary Cancer Risk Test ORDERING PHYSICIAN Dr. Jenny Jones Sample Medical Group 123 Main St. Sample, CA SPECIMEN Type: Saliva Barcode: 223 234234 2343 Collected: Apr 13, 2016 Received: Apr 14, 2016
Hereditary Cancer Risk Test ORDERING PHYSICIAN Dr. Jenny Jones Sample Medical Group 123 Main St. Sample, CA SPECIMEN Type: Saliva Barcode: 223 234234 2343 Collected: Apr 13, 2016 Received: Apr 14, 2016
CASE STUDY. Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members. Introduction. Patient Profile.
 CASE STUDY Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members Introduction Most cancers are caused by genetic damage resulting from random mutations and exposure to
CASE STUDY Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members Introduction Most cancers are caused by genetic damage resulting from random mutations and exposure to
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center
 Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
UW359 Ovary 3c 3 Serous Recurrent 68 BRCA1 816delGT BRCA1 del exon 1-2. UW417 Ovary 3c 3 Serous Primary 38 BRCA1 1675delA
 Supplementary Table 1. Cases with deleterious germline mutations, somatic HR mutations, and somatic PTEN mutations. ID Site Stage Grade Histology Tumor Age Germline mutation(s) a Somatic HR mutation(s)
Supplementary Table 1. Cases with deleterious germline mutations, somatic HR mutations, and somatic PTEN mutations. ID Site Stage Grade Histology Tumor Age Germline mutation(s) a Somatic HR mutation(s)
Genetic Testing for Familial Gastrointestinal Cancer Syndromes. C. Richard Boland, MD La Jolla, CA January 21, 2017
 Genetic Testing for Familial Gastrointestinal Cancer Syndromes C. Richard Boland, MD La Jolla, CA January 21, 2017 Disclosure Information C. Richard Boland, MD I have no financial relationships to disclose.
Genetic Testing for Familial Gastrointestinal Cancer Syndromes C. Richard Boland, MD La Jolla, CA January 21, 2017 Disclosure Information C. Richard Boland, MD I have no financial relationships to disclose.
NGS for Cancer Predisposition
 NGS for Cancer Predisposition Colin Pritchard MD, PhD University of Washington Dept. of Lab Medicine AMP Companion Society Meeting USCAP Boston March 22, 2015 Disclosures I am an employee of the University
NGS for Cancer Predisposition Colin Pritchard MD, PhD University of Washington Dept. of Lab Medicine AMP Companion Society Meeting USCAP Boston March 22, 2015 Disclosures I am an employee of the University
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2
 GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
CASE STUDY. Mutation-Specific Testing: Eligibility for PARP Inhibitor Therapy Established. Introduction. Patient Profile.
 CASE STUDY Mutation-Specific Testing: Eligibility for PARP Introduction Genetic testing is an emergent diagnostic technique that can provide specific and actionable inputs to the management of cancer therapy.
CASE STUDY Mutation-Specific Testing: Eligibility for PARP Introduction Genetic testing is an emergent diagnostic technique that can provide specific and actionable inputs to the management of cancer therapy.
Disclosure. Gynecologic Cancer Genetics. Audience response. Audience response. What was the result? 47%
 Disclosure Cancer Genetics I have served as a moderator for an advisory board to Genentech Lee-may Chen, M.D. Professor Department of Obstetrics, Gynecology, & Reproductive Sciences UCSF Obstetrics and
Disclosure Cancer Genetics I have served as a moderator for an advisory board to Genentech Lee-may Chen, M.D. Professor Department of Obstetrics, Gynecology, & Reproductive Sciences UCSF Obstetrics and
Yes when meets criteria below. Dean Health Plan covers when Medicare also covers the benefit.
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
CASE STUDY. Germline Test for Mother and Follow up Testing for Daughter: Assessment of Hereditary Cancer Risk. Introduction.
 CASE STUDY Germline Test for Mother and Follow up Testing for Daughter: Assessment of Hereditary Cancer Risk Introduction Germline cancer risk assessment tests are well-prescribed tests from Strand Life
CASE STUDY Germline Test for Mother and Follow up Testing for Daughter: Assessment of Hereditary Cancer Risk Introduction Germline cancer risk assessment tests are well-prescribed tests from Strand Life
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER SYNDROME BRCA1 BRCA2
 SYNDROME BRCA1 BRCA2 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
SYNDROME BRCA1 BRCA2 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Genetic Cancer Susceptibility Panels Using Next Generation Sequencing
 Genetic Cancer Susceptibility Panels Using Next Generation Sequencing Policy Number: 2.04.93 Last Review: 7/2017 Origination: 7/2013 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City
Genetic Cancer Susceptibility Panels Using Next Generation Sequencing Policy Number: 2.04.93 Last Review: 7/2017 Origination: 7/2013 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer
 Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
Hereditary Aspects of Pancreatic Cancer
 Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Genetic Determinants, Risk Assessment and Management
 Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017
 Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
HEREDITY & CANCER: Breast cancer as a model
 HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
The Value of Panel Testing in Inherited Breast Cancer Risk Assessment. Rodney J. Scott Division of Molecular Medicine
 The Value of Panel Testing in Inherited Breast Cancer Risk Assessment Rodney J. Scott Division of Molecular Medicine Mutation Detection Next Generation DNA sequencing has revolutionised mutation detection
The Value of Panel Testing in Inherited Breast Cancer Risk Assessment Rodney J. Scott Division of Molecular Medicine Mutation Detection Next Generation DNA sequencing has revolutionised mutation detection
Hereditary Breast and Ovarian Cancer Rebecca Sutphen, MD, FACMG
 Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Inherited Cancer Genomics and Prevention:
 Inherited Cancer Genomics and Prevention: How much cancer risk is inherited? Clinical utility of germline genetic testing in precision prevention and targeted therapy Kenneth Offit MD MPH Chief, Clinical
Inherited Cancer Genomics and Prevention: How much cancer risk is inherited? Clinical utility of germline genetic testing in precision prevention and targeted therapy Kenneth Offit MD MPH Chief, Clinical
Supplementary Online Content
 Supplementary Online Content Pearlman R, Frankel WL, Swanson B, et al. Prevalence and spectrum of germline cancer susceptibility gene mutations among patients with early-onset colorectal cancer. JAMA Oncol.
Supplementary Online Content Pearlman R, Frankel WL, Swanson B, et al. Prevalence and spectrum of germline cancer susceptibility gene mutations among patients with early-onset colorectal cancer. JAMA Oncol.
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T. Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics
 GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
TGL clinical User Guide
 TGL clinical User Guide The Institute of Cancer Research Brookes Lawley Building 15 Cotswold Road Sutton, Surrey SM2 5NG Page 1 of 7 TGL clinical This document describes the services provided by TGL clinical
TGL clinical User Guide The Institute of Cancer Research Brookes Lawley Building 15 Cotswold Road Sutton, Surrey SM2 5NG Page 1 of 7 TGL clinical This document describes the services provided by TGL clinical
GeneticsNow TM. A Guide to Testing Hereditary Conditions in Women & Men. Patient & Physician Information
 GeneticsNow TM A Guide to Testing Hereditary Conditions in Women & Men Patient & Physician Information How can BRCA status affect your health? Everyone has BRCA1 and BRCA2 genes. However, sometimes the
GeneticsNow TM A Guide to Testing Hereditary Conditions in Women & Men Patient & Physician Information How can BRCA status affect your health? Everyone has BRCA1 and BRCA2 genes. However, sometimes the
Consensus Guideline on Hereditary Genetic Testing for Patients With and Without Breast Cancer
 Consensus Guideline on Hereditary Genetic Testing for Patients With and Without Breast Cancer Purpose: To outline an approach to hereditary cancer genetic testing for patients with and without breast cancer
Consensus Guideline on Hereditary Genetic Testing for Patients With and Without Breast Cancer Purpose: To outline an approach to hereditary cancer genetic testing for patients with and without breast cancer
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian
 Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014
 COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
Policy Specific Section: Medical Necessity and Investigational / Experimental. October 15, 1997 October 9, 2013
 Medical Policy Genetic Testing for Hereditary Breast and/or Ovarian Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date:
Medical Policy Genetic Testing for Hereditary Breast and/or Ovarian Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date:
patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention
 patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime
patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime
Genetic Testing for Lynch Syndrome
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
Hereditary Cancer Risk Assessment for Gynecological Cancers. FarrNezhatMD.com
 Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
Moderate Penetrance Variants Associated With Breast Cancer in Individuals at High Breast Cancer Risk
 Moderate Penetrance Variants Associated With Breast Cancer in Individuals at High Breast Cancer Risk Policy Number: 2.04.126 Last Review: 3/2018 Origination: 3/2017 Next Review: 3/2019 Policy Blue Cross
Moderate Penetrance Variants Associated With Breast Cancer in Individuals at High Breast Cancer Risk Policy Number: 2.04.126 Last Review: 3/2018 Origination: 3/2017 Next Review: 3/2019 Policy Blue Cross
The Role of Genetics in Ovarian Cancer Screening. Dawn DeLozier, Ph.D. Medical Geneticist, SAMC Associate Professor UCSF-Fresno
 The Role of Genetics in Ovarian Cancer Screening Dawn DeLozier, Ph.D. Medical Geneticist, SAMC Associate Professor UCSF-Fresno How Much Breast and Ovarian Cancer Is Hereditary? 15%-20% 5%-10% Breast Cancer
The Role of Genetics in Ovarian Cancer Screening Dawn DeLozier, Ph.D. Medical Geneticist, SAMC Associate Professor UCSF-Fresno How Much Breast and Ovarian Cancer Is Hereditary? 15%-20% 5%-10% Breast Cancer
Prior Authorization. Additional Information:
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Consensus Guideline on Genetic Testing for Hereditary Breast Cancer
 Consensus Guideline on Genetic Testing for Hereditary Breast Cancer Purpose: To outline recommendations for genetic testing that medical professionals can use to assess hereditary risk for breast cancer
Consensus Guideline on Genetic Testing for Hereditary Breast Cancer Purpose: To outline recommendations for genetic testing that medical professionals can use to assess hereditary risk for breast cancer
Family Assessment. Objectives. Comprehensive Family History Important Inexpensive Underutilized genetic tool
 Besides the BRCA genes, what else to consider in hereditary breast and ovarian cancer? Laurie M. Connors DNP, APNG, FNP-BC, AGN-BC Objectives Evaluate personal & family history to assess risk for hereditary
Besides the BRCA genes, what else to consider in hereditary breast and ovarian cancer? Laurie M. Connors DNP, APNG, FNP-BC, AGN-BC Objectives Evaluate personal & family history to assess risk for hereditary
OvaNext. patient guide. genetic testing for hereditary breast, ovarian, and uterine cancer
 patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
BRCA1 & BRCA2: CANCER RISK & GENETIC TESTING IAP ID 2013 NAIR HOSPITAL, MUMBAI
 BRCA1 & BRCA2: CANCER RISK & GENETIC TESTING IAP ID 2013 NAIR HOSPITAL, MUMBAI DR KIRTI CHADHA MD (Path), PDCC (Oncopath & Oncohemat) CONSULTANT SURGICAL PATHOLOGIST NATIONAL COORDINATOR,SURGICAL PATHOLOGY
BRCA1 & BRCA2: CANCER RISK & GENETIC TESTING IAP ID 2013 NAIR HOSPITAL, MUMBAI DR KIRTI CHADHA MD (Path), PDCC (Oncopath & Oncohemat) CONSULTANT SURGICAL PATHOLOGIST NATIONAL COORDINATOR,SURGICAL PATHOLOGY
Forward Looking Statements
 Forward Looking Statements Some of the information presented here today may contain projections or other forward-looking statements regarding future events or the future financial performance 15M Patient
Forward Looking Statements Some of the information presented here today may contain projections or other forward-looking statements regarding future events or the future financial performance 15M Patient
THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES
 THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES Denise Uyar, MD Associate Professor OB/GYN Chief Gynecologic Oncology Medical College of Wisconsin April 12, 2019 NO DISCLOSURES
THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES Denise Uyar, MD Associate Professor OB/GYN Chief Gynecologic Oncology Medical College of Wisconsin April 12, 2019 NO DISCLOSURES
Reference #: SYS-PC-VPCI-CG-002. Origination Date: June 2012 Next Review Date: April 2019 Effective Date: April 2016
 Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Using the Bravo Liquid-Handling System for Next Generation Sequencing Sample Prep
 Using the Bravo Liquid-Handling System for Next Generation Sequencing Sample Prep Tom Walsh, PhD Division of Medical Genetics University of Washington Next generation sequencing Sanger sequencing gold
Using the Bravo Liquid-Handling System for Next Generation Sequencing Sample Prep Tom Walsh, PhD Division of Medical Genetics University of Washington Next generation sequencing Sanger sequencing gold
BRCA Precertification Information Request Form
 BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
Page 1 of 8 TABLE OF CONTENTS
 Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Evaluation of BRCA1/2 and homologous recombination defects in ovarian cancer and impact on clinical outcomes
 Evaluation of BRCA1/2 and homologous recombination defects in ovarian cancer and impact on clinical outcomes Melinda S. Yates, PhD Department of Gynecologic Oncology & Reproductive Medicine University
Evaluation of BRCA1/2 and homologous recombination defects in ovarian cancer and impact on clinical outcomes Melinda S. Yates, PhD Department of Gynecologic Oncology & Reproductive Medicine University
DNA Genetic Cancer Risk Test. Test Report
 Test Report CONTENTS SECTION 1 1-1. Customer Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Cancers / Tumors Tested SECTION 2 2-1. About the Test 2-2. References 1 CL0040-1_B
Test Report CONTENTS SECTION 1 1-1. Customer Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Cancers / Tumors Tested SECTION 2 2-1. About the Test 2-2. References 1 CL0040-1_B
Genetic Testing Today: What Genes Can Tell Us. Living Beyond Breast Cancer Conference Kara N. Maxwell, MD, PhD University of Pennsylvania
 Genetic Testing Today: What Genes Can Tell Us Living Beyond Breast Cancer Conference Kara N. Maxwell, MD, PhD University of Pennsylvania Overview of talk PART 1: Overview of Genetics PART 2: BRCA1/2 PART
Genetic Testing Today: What Genes Can Tell Us Living Beyond Breast Cancer Conference Kara N. Maxwell, MD, PhD University of Pennsylvania Overview of talk PART 1: Overview of Genetics PART 2: BRCA1/2 PART
So, now, that we have reviewed some basics of cancer genetics I will provide an overview of some common syndromes.
 Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Multi-gene panel testing for hereditary cancer predisposition in unsolved high-risk breast and ovarian cancer patients
 Breast Cancer Res Treat (207) 63:383 390 DOI 0.007/s0549-07-48-0 BRIEF REPORT Multi-gene panel testing for hereditary cancer predisposition in unsolved high-risk breast and ovarian cancer patients Beth
Breast Cancer Res Treat (207) 63:383 390 DOI 0.007/s0549-07-48-0 BRIEF REPORT Multi-gene panel testing for hereditary cancer predisposition in unsolved high-risk breast and ovarian cancer patients Beth
Accepted Manuscript. Utility of Genetic Testing in Persons with Multiple Colorectal Polyps. Natalia Khalaf, MD, MPH, Niloy Jewel Samadder, MD, MS
 Accepted Manuscript Utility of Genetic Testing in Persons with Multiple Colorectal Polyps Natalia Khalaf, MD, MPH, Niloy Jewel Samadder, MD, MS PII: S1542-3565(19)30259-9 DOI: https://doi.org/10.1016/j.cgh.2019.03.007
Accepted Manuscript Utility of Genetic Testing in Persons with Multiple Colorectal Polyps Natalia Khalaf, MD, MPH, Niloy Jewel Samadder, MD, MS PII: S1542-3565(19)30259-9 DOI: https://doi.org/10.1016/j.cgh.2019.03.007
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 AWARD NUMBER: W81XWH-13-1-0421 TITLE: The Fanconi Anemia BRCA Pathway as a Predictor of Benefit from Bevacizumab in a Large Phase III Clinical Trial in Ovarian Cancer PRINCIPAL INVESTIGATOR: Elizabeth
AWARD NUMBER: W81XWH-13-1-0421 TITLE: The Fanconi Anemia BRCA Pathway as a Predictor of Benefit from Bevacizumab in a Large Phase III Clinical Trial in Ovarian Cancer PRINCIPAL INVESTIGATOR: Elizabeth
