DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER
|
|
|
- Hilda Underwood
- 5 years ago
- Views:
Transcription
1 November 2015
2 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background Dysphagia Grading Dysphagia General Guidelines Modes of Managing Dysphagia Modified consistency diet Radiological or endoscopically placed nasogastric/nasojejunal feeding tube Radiologically inserted gastrostomy (RIG) Surgical gastrostomy or jejunostomy Self Expanding Metal Stent (SEMS) Radiotherapy +/- chemotherapy Chemotherapy alone Ablative therapies Brachytherapy Chemo-radiation versus SEMS Combined SEMS and radiotherapy +/- chemotherapy Treatment Options at Diagnosis Pre tissue diagnosis and staging At diagnosis Patient Selection and Preparation for Stent Principles of oesophageal stenting Technique of oesophageal stenting Complications of oesophageal stenting Management of recurrent dysphagia post stent insertion References... 9 Appendix 1: Patients Presenting With Malignant Dysphagia London Cancer Alliance
3 BACKGROUND 1 Median survival from the time of diagnosis of oesophageal cancer is in the order of 7-8 months and 1 year survival is 37% in the UK. 1 This is less if metastatic disease is present at diagnosis and is in the order of 4-6 months. Significant prolongation of survival can be achieved in suitable patients with chemotherapy or chemoradiation and surgery, with cure being possible for patients with resectable or limited disease. An initial audit of stenting practice from within the LCA raised the possibility that some patients were spending prolonged periods being unable to swallow. This guideline is an attempt to deal with this issue. Dysphagia is one of the most distressing symptoms of oesophageal carcinoma. Dysphagia not only interferes with quality of life and nutrition, but increases the risk of aspiration pneumonia. Owing to short life expectancy once diagnosed, it is important that treatments for dysphagia can be delivered promptly and should ideally relieve dysphagia rapidly and durably. None of the methods for palliation of this symptom are ideal, and there are no clear answers as to the best approach. 2,3,4 Treatment can be categorised as palliative supportive, palliative active (chemo+/-radiation) and curative chemo+/-radiation followed by surgery or primary surgery. The approach to dysphagia depends on which treatment approach is being adopted and to some extent by tumour type and location. For adenocarcinoma and squamous cancers affecting the lower third of the oesophagus, initial chemotherapy followed by surgery is the preferred option in operable cases. For squamous tumours affecting the upper 2/3 of the oesophagus, definitive treatment tends to be radical chemoradiation. 2 The following dysphagia grading scale is used for this guidance. Dysphagia grade scale (Mellow and Pinkas, Knyrim et al.1993) 0 = able to eat normal diet/no dysphagia 1 = able to swallow some solid foods 2 = able to swallow only semi solid foods 3 = able to swallow liquids only 4 = unable to swallow anything/total dysphagia 3
4 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 3 All patients with dysphagia scores of 1 or more must be seen by a dietician for nutritional assessment and appropriate support, advice and dietary counselling. All patients should be counselled about what to do and who to contact if their dysphagia worsens. Decisions on treatment pathway should be taken within 1 week of diagnosis so that the appropriate management of dysphagia can be decided upon. The patient should always be consulted about the options for treatment of their dysphagia, and their preferences taken into consideration when deciding optimum management. Dysphagia score and an assessment of symptoms of dysphagia should occur at each clinical contact with the patient. A stent should be inserted within 5 working days of decision to stent. All patients should be given appropriate post stent dietary advice and counselling by a dietician. All patients in whom the stent crosses the gastro-oesophageal junction should be prescribed proton pump inhibitors (PPIs) Modified consistency diet All patients requiring a modified consistency diet should receive advice from a dietician, and a speech and language therapist if required. Advice on soft/pureed/liquidised diets, nourishing fluids and oral nutritional supplements can be provided. 4.2 Radiologically or endoscopically placed nasogastric/nasojejunal feeding tube A feeding tube, which is passed under direct vision, is usually a temporary measure, used when an improvement in dysphagia is anticipated, e.g. before starting chemotherapy or before surgery. 4.3 Radiologically inserted gastrostomy (RIG) A feeding tube placed in the stomach under radiological guidance (RIG) will allow adequate delivery of nutrition and drug administration whilst undergoing other treatments. This approach does not restore swallowing. It is contra-indicated in surgical candidates as it may compromise the stomach for use as a gastric conduit at surgery when the stomach is anastomosed to the oesophageal remnant. Note that an oesophageal stricture is a contra-indication for percutaneous endoscopic gastrostomy (PEG) tube insertion. 4.4 Surgical gastrostomy or jejunostomy This may be considered for patients where RIG insertion is technically difficult or if the patient is likely to undergo surgery. The tube is inserted by surgeons (usually) or sometimes by radiologists. The patient will require a general anaesthetic. 4
5 MODES OF MANAGING DYSPHAGIA 4.5 Self Expanding Metal Stent (SEMS) These are inserted endoscopically or radiologically. They improve dysphagia rapidly and reliably, but have relatively high rates of mid-term failure as high as 20-30% by 3 months after insertion. Failure due to migration or tumour ingrowth can usually be dealt with by further straightforward intervention with serious complications being rare. Around 60% or more of stents will migrate by 10 weeks if concurrent chemo/radiation is given, particularly if there is a tumour response to treatment. Modern double layer partially covered metal stents show some advantage as regards migration but are not designed to be removed. SEMS are not ideal in non-circumferential soft tumours or in tumours within 2cm of the upper oesophageal sphincter because of globus sensation. Stents which cross the gastro-oesophageal junction are associated additionally with the problem of reflux which can be troublesome. 3 Stents interfere with radiotherapy planning and also make surgery more difficult. 4.6 Radiotherapy +/- chemotherapy Radiotherapy with or without chemotherapy is relatively slow to access it can be up to 10 weeks after referral until treatment begins and slow to take effect, but provides durable relief of symptoms. There is some survival advantage and chance of long-term cure associated with chemo-radiation in locally advanced but non-metastatic disease. It is the definitive curative treatment for squamous carcinomas in the upper third of the oesophagus. 4.7 Chemotherapy alone Most patients in the LCA with metastatic disease receive chemotherapy alone. This is less efficacious at palliating dysphagia than radiotherapy, but 50% of patients have significant relief of dysphagia within 2 weeks avoiding the necessity for stenting. 4.8 Ablative therapies Laser and alcohol injection are useful in selected cases with relative short strictures and for patients with high obstruction. Dilatation is not recommended. 4.9 Brachytherapy This is not currently available in the LCA, but it has been shown to provide superior relief of dysphagia compared to stenting for patients surviving more than 3 months, although no prolongation of survival has been shown Chemo-radiation versus SEMS There have been only limited comparisons of SEMS and radiotherapy +/- chemotherapy in the palliation of dysphagia in metastatic oesophageal cancer in the literature. In one such study in which radiotherapy was delivered both by external beam and brachytherapy, immediate palliation by oesophageal stenting was achieved in 85% of subjects but with a 20% failure rate by 10 weeks, compared to 50% being adequately palliated by radiotherapy within 2 weeks of starting treatment and 90% remaining palliated by 10 weeks Combined SEMS and radiotherapy +/- chemotherapy According to a recent American Gastroenterology Association (AGA) position statement, this cannot currently be recommended, but can be considered on a case by case basis owing to a lack of evidence. Limited evidence suggests that fully covered metal stents can be safely removed 4 weeks after initiating treatment. This maximises the benefit to swallowing and minimises the risk of stent migration. 5
6 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER Pre tissue diagnosis and staging For patients with dysphagia who have an oesophageal stricture, the nature of which is unknown, the options for relieving dysphagia (if dysphagia score 4) are insertion of removable SEMS (risk of migration) or insertion of nasogastric or nasojejunal feeding tube (less complicated though difficult to manage in community and risk of tube misplacement). All patients should be referred to a dietician. 5.2 At diagnosis Curative intent i.e. surgery or chemotherapy +/- radiation prior to possible surgery For patients with lower third tumours likely to undergo surgery there are two options. The first option is to insert a fully covered metal stent if there is grade 3 or 4 dysphagia and the patient is struggling to maintain adequate nutrition and fluid intake. This stent should be removed 4 weeks after beginning chemotherapy. The second option is to provide nutritional support by NG feeding managed in the community. Patient preference will play an important role in this decision. For squamous cell tumours in the upper 2/3 of the oesophagus, chemo-radiation is the definitive treatment and surgery is less likely. These patients should have a gastrostomy (or jejunostomy where appropriate) in preference to a stent Palliative active treatment with chemotherapy in patients with metastatic disease A permanent partially covered metal stent should be inserted for grade 4 dysphagia at diagnosis or at any stage of treatment, or grade 3 or 4 dysphagia after 2 cycles of chemotherapy. Radiotherapy can also be considered in early stage disease in a patient unsuitable for radical treatment for other reasons like age or co-morbidity, in which case stenting can be avoided. However for grade 3 or 4 dysphagia owing to the slow onset of relief from radiotherapy, a temporary covered metal stent should be inserted with a view to removal 4 weeks after beginning treatment Palliative supportive treatment anticipated survival is short or age or comorbidities preclude chemotherapy If dysphagia score 3 or 4 strong consideration should be given to insertion of a partially covered metal stent During treatment with chemotherapy Lack of adequate response of dysphagia to score 2 or better after the second cycle of chemotherapy should lead to either placement of a stent or RIG and early provision of radiotherapy During treatment with radiotherapy Lack of response 4 weeks after initiation of radiotherapy should lead to early endoscopy and either dilatation of benign looking strictures, stenting if malignant looking, or other treatments if inflammatory looking strictures. 6
7 PATIENT SELECTION AND PREPARATION FOR STENT After treatment with chemotherapy and/or radiotherapy as the only intended treatment All patients with dysphagia score 3 and above should be endoscoped if anticipated survival is greater than 30 days. If appearances suggest malignant rather than benign change they should be stented. If appearances suggest benign changes, initial dilatation may be performed. Patients with grade 4 dysphagia in whom it is not possible to provide nutrition in any other way and expected survival is more than 3 months should be considered for total parental nutrition. These cases are rare but do occur. 6 Ideally patients should have an expected survival of more than 30 days although this does depend on individual circumstances. The patient must be able to lie flat for the procedure without developing hypoxia. Clotting should be checked and corrected if INR>1.5. British Society of Gastroenterology (BSG) guidelines on antiplatelet medication and anticoagulants should be followed oesophageal stent insertion should be considered a high bleeding risk procedure. If it is decided the patient is not medically fit for oesophageal stent or patient preference precludes insertion of stent, a referral to palliative care should be made. Palliative care team should also be involved if patients experience other symptoms. The first point of contact for arranging an oesophageal stent should be the UGI cancer diagnostic team at the hospital where the cancer was originally diagnosed. Patients should be nil by mouth at least 6 hours prior to the procedure. 6.1 Principles of oesophageal stenting Proximal oesophageal stricture. Ultraflex stent may be better suited for placing an oesophageal stent in the cervical oesophagus. Proximal releasing stent and special cervical stents are available. These stents usually require endoscopic and fluoroscopic control. Dilatation and laser therapy are not recommended due to associated risk of complications. In a study by Macdonald et al 9, 28% patients had throat pain when stent was within 1.5cm of upper oesophageal sphincter (UOS) while none had throat pain at 2cm. Patients can have a globus sensation if stent was placed within 4cm UOS although this did not require stent removal. Mid and distal oesophageal stricture. Various stents including Flamingo, Ultraflex, Niti S double stent, or Z stent can be used. Dilatation provides short term relief and is associated with a risk of perforation. Very tight strictures may need dilatation to allow for deployment of oesophageal stent. For tumours at GO junction, stents with anti-reflux valve (Hanaro stent, Choo stent, Dua Z stent, Bona stent) or Umbrella stent can be used. For extrinsic compression of oesophagus, covered or uncovered metal stents can be deployed. These strictures should not be dilated. Biodegradable stents (Ella BD) take weeks to disintegrate. Advantage is to let the stent dissolve in the stomach if it migrates, although it is more difficult to deploy these stents and they need hand loading before deploying. 7
8 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 6.2 Technique of oesophageal stenting Oesophageal stents are inserted through a trans-oral approach using either fluoroscopic guidance, endoscopy or a combination of the above. The fluoroscopy alone approach is easy and quick. However, some endoscopists prefer the combined use of endoscopic and fluoroscopic guidance especially in hospitals where an established experienced radiological service is not available. The procedure is typically performed under conscious sedation with a combination of an opiate (i.e. pethidine 25-50mg or fentanyl µm) and a sedative (i.e. midazolam 2-6 mg). The patient is usually positioned in the left lateral decubitus position as this enables optimal identification of the gastroesophageal junction (GEJ). However, if the patient is unable to tolerate this position, the procedure can be performed in the supine position. A right anterior oblique view enables accurate stent placement at the GEJ. A tilting table allows for the head to be placed in a raised position to decrease the risk of aspiration during the procedure. A 260cm guidewire is passed through a 6Fr sheath (goldprobe or a double lumen catheter) and under endoscopic vision the wire is threaded through the stricture. Once the wire is deemed to be in the stomach, it is removed and iodinated contrast injected to confirm visualisation of gastric rugal folds. The catheter is then passed over the wire back into the stomach. The length and tightness of stricture can be estimated by slowly withdrawing the sheath while injecting contrast till the stricture is delineated. An alternative method is to pass a balloon over the guidewire into the stomach, inflating the balloon and withdrawing the balloon till it impacts at the distal end of the stricture. A fluoroscopic image should also be taken to look for landmarks (ribs/vertebrae or diaphragm.). An external metal clip can be placed on the skin to visualise the positioning of the stent relative to the stricture. Alternatively lipiodiol can be injected above the proximal end though it dissipates rapidly and may be difficult to use as a landmark. A stent that is at least 3-4 cm longer than the stricture is recommended to account for stent shortening and to ensure satisfactory stent coverage across the lesion. This ensures 1-2 cm cephalic and caudal coverage of the lesion. It is recommended that placement of the stent is performed so that two thirds of the stent is placed cranial (proximal) to the stricture. This is to reduce the possibility of stent migration. Oesophageal stricture pre-dilatation is not advised due to the risk of perforation but can be performed in cases of tight stenosis to allow for stent delivery. In such cases, gentle dilatation, usually with a mm oesophageal radial balloon, may be performed. In patients with tight strictures requiring pre-dilatation, if dilatation is not performed prior to stent insertion, then it can be done post stenting. A chest X-ray is usually performed post procedure to rule out perforation. After stent placement, if the stricture is not tight, post dilatation is not usually required, as the stent gradually expands to its nominal diameter in hours. Covered part of the stent is usually 18mm in diameter which flares to 26mm at proximal and distal ends (although the sizes can vary depending on the type of stent used). 6.3 Complications of oesophageal stenting 10 Bleeding (3-8%) Chest pain (12-14%) Migration (<6% for bare and 25-32% for covered) Tumour ingrowth in bare SEMS (17-36%) Fistulation (2.8%) Perforation (<1%) Reflux (3.7%) 8
9 REFERENCES Post procedural pain is common and adequate analgesia should be provided. Occasionally stents have to be removed because of the pain. Haemorrhage can also occur and stenting should be avoided in haemorrhagic tumours where radiotherapy is preferred. Perforation can be managed by successful deployment of the stent. 3 Stent migration can usually be managed endoscopically/radiologically. In many cases the migrated stents produce no clinical problems. Surgery for migrated stents causing obstruction is relatively rare. 6 What is not known about is the experience of patients with dysphagia and the proportion of time spent with severe dysphagia from diagnosis until their death. 6.4 Management of recurrent dysphagia post stent insertion Causes of recurrent dysphagia after stent insertion can include stent blockage due to food bolus (can be removed endoscopically) or due to tumour at the proximal or distal end of stent. For the distal overgrowth, a second overlapping stent can be deployed or laser can be used if the lesion is nodular. For proximal overgrowth, a second overlapping stent can be deployed if there is enough clearance at the superior end. If there is inadequate clearance, laser therapy can be tried. In either situation, a RIG or surgical jejunostomy may be required. Other causes can be tracheo-oesophageal fistula (treated by deploying an overlapping covered stent) or stent migration (re-stenting may be required). 7 1 Coupland VH, Allum W, Blazeby JM et al. Incidence and survival of oesophageal and gastric cancer in England between 1998 and 2007, a population-based study. BMC Cancer. 2012; 12: Hanna WC, Andersham M, Roberge D et al. What is the optimal management of dysphagia in metastatic oesophageal adenocarcinoma? Current Oncology. 2012; 19: Prateek Sharma MD, Richard Kozarek MD and the Practice Parameters Committee of the American College of Gastroenterology. Role of oesophageal stents in benign and malignant disease. Am J Gastroenterol. 2010; 105: Blazeby JM, Griffin SM, Cunningham D et al. Guidelines for the management of oesophageal and gastric cancer. Gut. 2011; 60: Philips P, North DA, Scoggins C et al. Gastric-esophageal stenting for malignant dysphagia: results of prospective clinical trial evaluation of long-term gastroesophageal reflux and quality of life-related symptoms. J Am Coll Surg. 2015; 221(1): Park JH, Song HY, Shin JH et al. Migration of retrievable expandable metallic stents inserted for malignantesophageal strictures: incidence, management, and prognostic factors in 332 patients. Am J Roentgenol. 2015; 204(5): Dai Y, Li C, Xie Y et al. Interventions for dysphagia in oesophageal cancer. Cochrane Database of Systematic Reviews. 2014, Issue Homs MY et al. (2004) Single-dose brachytherapy versus metal stent placement for the palliation of dysphagia from oesophageal cancer: multicenter, randomised trial. Lancet 364: Macdonald S, Edwards RD and Moss JG. Patient tolerance of cervical oesophageal metallic stents. J Vasc Interv Radiol. 2000; 11(7) : Parthipun A, Diamantopoulos A, Shaw A et al. Self expanding metal stents in palliative malignant oesophageal dydphagia. Ann Palliat Med. 2014; 3(2):
10 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER All patients - dietician review Pre diagnosis: removable stent/ng feeding tube for grade 4 dysphagia Diagnosis made and treatment plan decided Curative intent Palliative active treatment (metastatic disease) Local disease unsuitable for curative treatment Palliative supportive Squamous cancer upper 2/3 for grade 3 or 4 dysphagia. Gastro/jejunostomy or NG tube managed in the community Lower third tumours for grade 3 or 4 dysphagia: removable stent for removal 4/52 after beginning Rx or NG tube managed in the community Insert partially covered stent for grade 4 dysphagia at diagnosis. Dysphagia score grade 3 or 4 after 2 nd cycle of chemotherapy insert SEMS or consider radiotherapy Consider palliative radiotherapy or partially covered stent for dysphagia score grade 3 or 4 Metastatic or advanced disease, consider partially covered SEMS if dysphagia score grade 3 or 4 and expected survival >30 days or patient preference 10
Endoscopic Palliation of Malignant Dysphagia
 Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Colonic Metal Stents MAKING A DIFFERENCE TO HEALTH
 Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Douglas G. Adler MD. ACG Regional Postgraduate Course - Nashville, TN Copyright 2013 American College of Gastroenterology
 Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications
 Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Esophageal Stenosis Treatment by Interventional Radiology: Indications, Techniques and complications Poster No.: C-0437 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Leyva Vásquez-Caicedo,
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Is a Metallic Stent Useful for Non Resectable Esophageal Cancer?
 Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
Original article INTRODUCTION
 Diseases of the Esophagus (2007) 20, 466 470 DOI: 10.1111/j.1442-2050.2007.00696.x Blackwell Publishing Asia Original article Superiority of anti-reflux stent compared with conventional stents in the palliative
Diseases of the Esophagus (2007) 20, 466 470 DOI: 10.1111/j.1442-2050.2007.00696.x Blackwell Publishing Asia Original article Superiority of anti-reflux stent compared with conventional stents in the palliative
ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE
 22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
NICE guideline Published: 24 January 2018 nice.org.uk/guidance/ng83
 Oesophago-gastric cancer: assessment and management in adults NICE guideline Published: 24 January 18 nice.org.uk/guidance/ng83 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Oesophago-gastric cancer: assessment and management in adults NICE guideline Published: 24 January 18 nice.org.uk/guidance/ng83 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Type of intervention Palliative care. Economic study type Cost-effectiveness analysis.
 Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
Oesophageal and gastric stents Patient Information leaflet
 Oesophageal and gastric stents Patient Information leaflet Why have you been given this leaflet? This leaflet has been written to help you understand why it has been recommended that you have a stent.
Oesophageal and gastric stents Patient Information leaflet Why have you been given this leaflet? This leaflet has been written to help you understand why it has been recommended that you have a stent.
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Oesophageal Stent insertion
 Oesophageal Stent insertion What is an Oesophageal Stent? Patients with a blockage in their oesophagus or stomach that cannot be relieved by an operation may be offered the option of having an oesophageal
Oesophageal Stent insertion What is an Oesophageal Stent? Patients with a blockage in their oesophagus or stomach that cannot be relieved by an operation may be offered the option of having an oesophageal
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent
 Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
Clinical evaluation of treating an advanced esophageal carcinoma by using membrane-covered metallic stent Xu meidong, Yao liqing, Zhong yunshi et al. Department of Endoscopy Center, Zhongshan Hospital,
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser
 16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
Swallowing, nutrition and PEG feeding: deciding, doing and managing
 Swallowing, nutrition and PEG feeding: deciding, doing and managing Swallowing in MND Dysphagia disruption in the swallowing process In MND can be variable depending on type Bulbar MND - faster progression
Swallowing, nutrition and PEG feeding: deciding, doing and managing Swallowing in MND Dysphagia disruption in the swallowing process In MND can be variable depending on type Bulbar MND - faster progression
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
ESOPHAGEAL CANCER. Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds
 ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
The following slides are from a. presentation given by. H. Worth Boyce, M.D. on. Specialized Studies on Diseases of the Esophagus.
 The following slides are from a presentation given by H. Worth Boyce, M.D. on Endoscopic Lumen Restoration at the 8 th OESO World Organization for Specialized Studies on Diseases of the Esophagus. Endoscopic
The following slides are from a presentation given by H. Worth Boyce, M.D. on Endoscopic Lumen Restoration at the 8 th OESO World Organization for Specialized Studies on Diseases of the Esophagus. Endoscopic
The role of esophageal brachytherapy
 Esophageal cancer is combination with surgery (stents) or EBRT a better solution? Razvan Galalae, MD, PhD Associate Professor, Medical Faculty, Christian Albrecht University Kiel, Germany, and Head of
Esophageal cancer is combination with surgery (stents) or EBRT a better solution? Razvan Galalae, MD, PhD Associate Professor, Medical Faculty, Christian Albrecht University Kiel, Germany, and Head of
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Colorectal stenting. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
17. Oesophagus. Upper gastrointestinal cancer
 110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
Patient information for Oesophago-gastroduodenoscopy
 Patient information for Oesophago-gastroduodenoscopy Full name of procedure: Oesophago-gastro-duodenoscopy Short name: OGD, gastroscopy or endoscopy Reason for procedure: The gastroscope is a narrow telescope
Patient information for Oesophago-gastroduodenoscopy Full name of procedure: Oesophago-gastro-duodenoscopy Short name: OGD, gastroscopy or endoscopy Reason for procedure: The gastroscope is a narrow telescope
Recanalisation of urethral strictures with new-generation temporary covered biocompatible metal endoprostheses
 Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up
 Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up Neil A. Christie, MD, Percival O. Buenaventura, MD, Hiran C. Fernando, MD, Ninh
Results of Expandable Metal Stents for Malignant Esophageal Obstruction in 100 Patients: Short-Term and Long-Term Follow-up Neil A. Christie, MD, Percival O. Buenaventura, MD, Hiran C. Fernando, MD, Ninh
MICRO-TECH Oesophagus stents.
 MICRO-TECH. Nitinol stents. Reliable bypassing of stenoses in the area of the digestive or respiratory tract places high demands on a stent. As one of the leading international manufacturers, MICRO-TECH
MICRO-TECH. Nitinol stents. Reliable bypassing of stenoses in the area of the digestive or respiratory tract places high demands on a stent. As one of the leading international manufacturers, MICRO-TECH
Endoscopy Unit Pyloric and Duodenal Stent insertion
 Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
Self-expanding metallic stent placement with an exaggerated 5-cm proximal tumor covering for palliation of esophageal cancer
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 Self-expanding metallic stent placement with an exaggerated 5-cm proximal tumor covering for palliation of esophageal cancer Mehdi Tahiri, Pasquale
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 Self-expanding metallic stent placement with an exaggerated 5-cm proximal tumor covering for palliation of esophageal cancer Mehdi Tahiri, Pasquale
Surgery for Gastric and Oesophageal Cancer
 Surgery for Gastric and Oesophageal Cancer Trends in cancer mortality, England and Wales SMR base 1980 Oesophago-Gastric Cancer The National Problem 5 th commonest malignancy 4 th commonest cause of death
Surgery for Gastric and Oesophageal Cancer Trends in cancer mortality, England and Wales SMR base 1980 Oesophago-Gastric Cancer The National Problem 5 th commonest malignancy 4 th commonest cause of death
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Department of Thoracic Medicine, Chang Gung Memorial Hospital, Lin-Kuo Branch, Chang Gung Medical Foundation; Abstract
 DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
Fluoroscopically Guided Balloon Dilation for Benign Anastomotic Stricture in the Upper Gastrointestinal Tract
 Fluoroscopically Guided alloon ilation for enign nastomotic Stricture in the Upper Gastrointestinal Tract Jin Hyoung Kim, M Ji Hoon Shin, M Ho-Young Song, M benign anastomotic stricture is a common complication
Fluoroscopically Guided alloon ilation for enign nastomotic Stricture in the Upper Gastrointestinal Tract Jin Hyoung Kim, M Ji Hoon Shin, M Ho-Young Song, M benign anastomotic stricture is a common complication
Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula
 European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
Jejunostomy after oesophagectomy, how and why I do it
 Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting
 Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting Mary Mc Clenaghan Advanced Specialist Head and Neck Dietitian, South London Community Head and Neck Team,
Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting Mary Mc Clenaghan Advanced Specialist Head and Neck Dietitian, South London Community Head and Neck Team,
Iraqi JMS. Expandable Metal Esophageal Stent Deployment in Patients with Malignant Dysphagia
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 1681-6579 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq Expandable Metal Esophageal Stent Deployment in Patients
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 1681-6579 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq Expandable Metal Esophageal Stent Deployment in Patients
The CREST Trial. Funded by Cancer Research UK and developed by the National Cancer Research Institute
 The CREST Trial A randomised phase III study of stenting as a bridge to surgery in obstructing colorectal cancer. Results of the UK ColoRectal Endoscopic Stenting Trial (CREST). Funded by Cancer Research
The CREST Trial A randomised phase III study of stenting as a bridge to surgery in obstructing colorectal cancer. Results of the UK ColoRectal Endoscopic Stenting Trial (CREST). Funded by Cancer Research
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
Gastroscopy and dilatation/stent insertion
 Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Having a radiologically inserted gastrostomy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers
 Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study
 E89 Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study Authors Institution Agnes N. Reijm, Paul Didden, Marco
E89 Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study Authors Institution Agnes N. Reijm, Paul Didden, Marco
Esophageal Stents What, Why, When and How?
 Esophageal Stents What, Why, When and How? Motility Noon Conference Bill Kessler February 1, 2017 Disclosure Research support from Merit Medical, Inc. Objectives Background Indications Techniques and What?
Esophageal Stents What, Why, When and How? Motility Noon Conference Bill Kessler February 1, 2017 Disclosure Research support from Merit Medical, Inc. Objectives Background Indications Techniques and What?
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience
 GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
Biodegradable esophageal stents in benign and malignant strictures a single center experience
 E618 THIEME Biodegradable esophageal stents in benign and malignant strictures a single center experience Authors Institution Dimitrios E. Sigounas, Sandeep Siddhi, John N. Plevris Centre for Liver & Digestive
E618 THIEME Biodegradable esophageal stents in benign and malignant strictures a single center experience Authors Institution Dimitrios E. Sigounas, Sandeep Siddhi, John N. Plevris Centre for Liver & Digestive
Esophageal Cancer. What is esophageal cancer?
 Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery?
 Ulster Med J 2019;88(1):10-14 Grand Rounds Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery? Jennifer E Tham 1, Benjamin Tharian 2, Patrick B Allen 1, Gary Spence 1, Tony
Ulster Med J 2019;88(1):10-14 Grand Rounds Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery? Jennifer E Tham 1, Benjamin Tharian 2, Patrick B Allen 1, Gary Spence 1, Tony
Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer
 Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer Authors: Eduardo Rodrigues-Pinto, Pedro Pereira, Todd H. Baron, Guilherme Macedo DOI: 10.17235/reed.2018.5323/2017
Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer Authors: Eduardo Rodrigues-Pinto, Pedro Pereira, Todd H. Baron, Guilherme Macedo DOI: 10.17235/reed.2018.5323/2017
Intra-gastric balloon procedure. Information for patients Sheffield Centre for Weight Loss Surgery
 Intra-gastric balloon procedure Information for patients Sheffield Centre for Weight Loss Surgery Introduction The intra-gastric balloon is designed to provide short term weight loss therapy. It is a temporary
Intra-gastric balloon procedure Information for patients Sheffield Centre for Weight Loss Surgery Introduction The intra-gastric balloon is designed to provide short term weight loss therapy. It is a temporary
Head and neck cancer - patient information guide
 Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
PERCUTANEOUS BILIARY DRAINAGE
 PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
E09 PEG. Expires end of March 2018 VITALITY.CO.UK
 VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
Thrombolysis and thrombectomy
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Thrombolysis and thrombectomy This information sheet explains about how a blood is diagnosed and the various forms
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Thrombolysis and thrombectomy This information sheet explains about how a blood is diagnosed and the various forms
Pexact gastrostomy. GI Unit. Patient Information Leaflet
 Pexact gastrostomy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are considering having a Pexact gastrostomy. It gives information about what this is, what the procedure
Pexact gastrostomy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are considering having a Pexact gastrostomy. It gives information about what this is, what the procedure
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW
 PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
Oral anti-thrombotic therapy-management in patients requiring endoscopy
 Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Gastro-Oesophageal Reflux Disease Information Sheet
 Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
ANGIOPLASTY AND STENTING
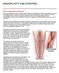 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Observations on oesophageal length
 Thorax (1976), 31, 284. Observations on oesophageal length G. J. KALLOOR, A. H. DESHPANDE, and J. LEIGH COLLIS The Queen Elizabeth Hospital, Birmingham Kalloor, G. J., Deshpande, A. H., and Leigh Colfis,
Thorax (1976), 31, 284. Observations on oesophageal length G. J. KALLOOR, A. H. DESHPANDE, and J. LEIGH COLLIS The Queen Elizabeth Hospital, Birmingham Kalloor, G. J., Deshpande, A. H., and Leigh Colfis,
Patient Information Having a Fistuloplasty or Venoplasty
 Patient Information Having a Fistuloplasty or Venoplasty Renal Department Introduction This leaflet is intended to provide you with information about having a fistuloplasty. What is a fistuloplasty or
Patient Information Having a Fistuloplasty or Venoplasty Renal Department Introduction This leaflet is intended to provide you with information about having a fistuloplasty. What is a fistuloplasty or
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey
 Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
Pediatric ER Half-day Rounds October 12, 2011 Dr. Karen Bailey Objectives to identify various enteral and vascular access lines what do they look like? indications & contraindications proper placement
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
Home Enteral Nutrition: What happens after discharge? Niamh Maher Senior Dietitian HSE Dublin North East
 Home Enteral Nutrition: What happens after discharge? Niamh Maher Senior Dietitian HSE Dublin North East Nutrition Support Study Day April 25 th 2012 Home enteral nutrition (HEN) Enteral tube feeding is
Home Enteral Nutrition: What happens after discharge? Niamh Maher Senior Dietitian HSE Dublin North East Nutrition Support Study Day April 25 th 2012 Home enteral nutrition (HEN) Enteral tube feeding is
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Achalasia and Laparoscopic Heller Myotomy
 1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE
 July 2015 Issue No.17 DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE www.sghgroup.com JEDDAH RIYADH MEDINA ASEER HAIL SANAA DUBAI CAIRO Definitions Over View and General Facts General Key facts! Worldwide
July 2015 Issue No.17 DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE www.sghgroup.com JEDDAH RIYADH MEDINA ASEER HAIL SANAA DUBAI CAIRO Definitions Over View and General Facts General Key facts! Worldwide
Oesophageal, gastric and duodenal stents
 Oesophageal, gastric and duodenal stents Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Oesophageal, gastric and duodenal stents Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Intraluminal brachytherapy in oesophageal cancer: defining its role and introducing the technique
 Review paper Educational Activity Intraluminal brachytherapy in oesophageal cancer: defining its role and introducing the technique Sebastian Lettmaier, MD, Vratislav Strnad, MD, Prof. Department of Radiation
Review paper Educational Activity Intraluminal brachytherapy in oesophageal cancer: defining its role and introducing the technique Sebastian Lettmaier, MD, Vratislav Strnad, MD, Prof. Department of Radiation
EXPANDABLE METAL STENTS FOR INOPERABLE OESOPHAGEAL CANCER
 EXPANDABLE METAL STENTS FOR INOPERABLE OESOPHAGEAL CANCER A West Midlands Health Technology Assessment Collaboration report Authors: Roger Gajraj, SpR in Public Health, West Midlands Training Scheme David
EXPANDABLE METAL STENTS FOR INOPERABLE OESOPHAGEAL CANCER A West Midlands Health Technology Assessment Collaboration report Authors: Roger Gajraj, SpR in Public Health, West Midlands Training Scheme David
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA
 Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
