Chapter 2 Cancer and Genetic Counseling
|
|
|
- Abner Eaton
- 5 years ago
- Views:
Transcription
1 Chapter 2 Cancer and Genetic Counseling Brandie Heald and James M. Church Introduction All cancer is genetic. Cancer is a disease caused by an accumulation of genetic damage that interferes with the regulation of cell growth, differentiation, and death. Most cancer-causing genetic damage is acquired either due to environmental exposures, carcinogens, or chance. This type of genetic damage is somatic and does not present a risk to offspring. Accordingly, the majority of cancers occur sporadically. However, some cancers are familial, occurring as a cluster of similar cancers that occur within a family more frequently than expected by chance. These cancers do not follow a clearly hereditary pattern; they are thought to arise from shared genetic and environmental factors. Individuals within these families are at increased risk of developing the type of cancer found in their relatives. Finally, it is estimated that 5 10% of cancers are hereditary, occurring because of transmission of a genetic mutation in the germline. Individuals in these families are usually at increased risk for more than one type of cancer. Identification of a hereditary cancer syndrome is critical to help patients and their families understand what their lifetime risk of cancer is, help them to cope with the emotional response of knowing this risk, and develop a plan for management of this risk. The hereditary nature of some cancers has many implications for patients and families, implications that have become increasingly complex as genetic technology has become more sophisticated. Evaluation of a family history, explanation of the genetics of hereditary cancer syndromes, facilitation of genetic testing and discussion of the results, and advising about genetic discrimination and family planning are beyond the scope of the family practitioner or medical specialist. These are the roles of the genetic counselor. The purpose of this chapter is to describe the place of genetic counseling in the B. Heald (*) Genomic Medicine Institute and the Sanford R. Weiss Center for Hereditary Colorectal Neoplasio, Cleveland Clinic Foundation, Cleveland, OH 44195, USA leachb@ccf.org C.N. Ellis (ed.), Inherited Cancer Syndromes: Current Clinical Management, DOI / _2, Springer Science+Business Media, LLC
2 24 B. Heald and J.M. Church anagement of hereditary cancer, focusing on general principles that may be m applied to all syndromes. Background A gene is a particular segment of DNA that carries the biochemical code for a particular protein. Genes are packed into chromosomes, which are organized into 22 pairs of autosomes and one pair of sex chromosomes. All chromosomes are housed in the cell s nucleus. Each person receives one copy of each chromosome from each parent and therefore one copy of each gene from each parent. There is a huge amount of variation within human DNA enabling the existence of billions of unique human beings. Many genes are subtly different from one individual to another, accounting for much of the variation in our species. These variants are polymorphisms. Polymorphisms are alterations found in DNA in at least 1% of the population. Polymorphisms can be associated with a certain disease, but almost never do they cause the condition. Mutations are permanent, structural changes in a gene. They may be pathogenic (deleterious, causing disease), of unknown significance, or polymorphic. The redundancy in the genetic code means that not all mutations interfere with protein translation, and not all proteins made from a mutated gene are dysfunctional. Mutations can be somatic, randomly occurring in a cell. These types of mutations cannot be passed onto offspring. Other mutations occur in the germline. Germline mutations are present in every cell in the body, including the oocytes and spermatocytes, and can be passed onto offspring. An inherited germline mutation in a tumor suppressor gene is the most common way that cancer is transmitted within a family. Genetic Counseling A genetic counselor is a healthcare professional with training in medical genetics and counseling techniques. This is a rather young field of practice. However, within the past 10 years genetic counseling has been recognized by numerous professional societies as a critical element in the assessment and treatment of patients with or at risk for hereditary cancer syndromes [1 5]. Genetic counseling is a process of identification, education, facilitation, and psychosocial support for the patient and his or her family members. The National Society of Genetic Counselors states that the purpose of cancer genetic counseling is to educate clients about their chance of developing cancer, help them derive personal meaning form cancer genetic information, and empower them to make educated, informed decisions about genetic testing, cancer screening, and cancer prevention [6]. In addition to educating and empowering patients to
3 2 Cancer and Genetic Counseling 25 make decisions, genetic counselors also assess psychosocial issues that may arise for patients or their families while going through this process. Referring to a Genetic Counselor A referral is made to a genetic counselor to determine if a patient and his or her family is at risk for an inherited cancer syndrome and to facilitate suitable genetic testing. The referral is made because something in the patient s presentation, such as family history or disease phenotype, is suggestive of an inherited syndrome. General features of a hereditary cancer syndrome that may prompt a referral to a genetic counselor are listed in Table 2.1. Family history of cancer is an important risk factor that should be assessed by practitioners caring for patients with cancer. Over a 2-month period in six gastroenterology practices Dudley-Brown and Freivogel found that 26% of patients were at risk of a syndrome of hereditary colorectal cancer, establishing the absolute need for routine family histories [7]. In a less selected group, Mitchell et al. reported that almost 10% of patients had a first-degree relative with colorectal cancer and almost 30% has a first- or second-degree relative affected [8]. In the primary care office, or at the cancer specialist, the family history alone is usually enough to trigger a referral for genetic counseling. Sometimes hereditary cancer features are obscured by lack of knowledge, lack of accuracy, or small family size. Several studies in primary care, surgical, and oncologic practices show that family history of cancer is taken in a low percentage of cases [9 11]. Within a primary care setting one study showed that presence or absence of a family history of cancer was documented in 97.8% of patients records, but that insufficient information was available to perform a risk assessment in 69.5% of cases [12]. In another report, Mitchell et al. estimated that most patients underestimate their cancer family history, with a sensitivity of 57% for first-degree relatives and 27% for second-degree [13]. However, a family history screening question for colorectal cancer has anyone in your family ever had cancer or polyps of the colon or rectum was found to be over 90% accurate in a study of colorectal surgical patients subject to a thorough three-generation pedigree [9]. This question is therefore the bare minimum. Any positive answer should lead to a three-generation family tree with all cancers listed. Table 2.1 Hallmark feature of hereditary cancer syndromes Early age at cancer diagnosis (e.g. breast cancer before age 50) Multiple generation affected with cancer Multiple primary cancers in an individual Bilateral or multisynchronous cancers Clustering of genetically related cancer (e.g. uterine and colon cancer) Rare cancers (e.g. male with breast cancer) Known deleterious mutation present in the family
4 26 B. Heald and J.M. Church Occasionally, the disease phenotype is suggestive of inheritance. For example, the presence of more than 100 synchronous colorectal adenomas means a polyposis syndrome is present. Oligopolyposis, where patients have less than 100 but more than 10 synchronous adenomas, raises the possibilities of attenuated familial adenomatous polyposis and MuTYH-associated polyposis. Genetic counseling and genetic testing for a germline APC or MuTYH mutation is indicated for all these scenarios. Personal Medical History During a counseling session, information is collected on all major illnesses, surgical history, history of benign and malignant tumors, biopsy history, reproductive history, environmental exposures, and cancer surveillance [14]. For patients with a personal history of cancer, information is collected on the site and stage of the cancer, treatment and outcomes, and age at diagnosis. Cancer pathology is also a critical factor. As an example, in hereditary breast ovarian cancer syndrome it has been found that women with a triple negative cancer (negative for estrogenreceptor, progesterone-receptor, and HER2) are candidates for BRCA1 and BRCA2 testing, even in the absence of a family history of breast or ovarian cancer [15]. Family Medical History A genetic counselor is trained to obtain a detailed three- to four-generation family history. In taking the history, particular attention is paid to the site and pathology of the cancer, the stage of the cancer, treatment and outcomes, and age at diagnosis. Information is also collected about nonmalignant features of hereditary cancer syndromes. For example, when evaluating a family for Cowden syndrome, in addition to collecting family history of cancer, information is recorded about head circumference and benign dermatologic, thyroid, breast, and endometrial disease. Medical records and/or death certificates are typically requested in order to confirm the diagnoses within the family. For the genetic family history, it is also important to collect information on unaffected family members and deceased family members including age at death and cause of death. Information about ethnicity and consanguinity is also collected on all patients. For patients who have been adopted or have no information about their family medical history, counseling is based on the personal risk factors. Risk Assessment Once the personal medical and family history is obtained, a differential diagnosis is established. Various risk assessment models have been established for some of the more common syndromes such as hereditary breast ovarian cancer syndrome [16 21]
5 2 Cancer and Genetic Counseling 27 and hereditary non-polyposis colorectal cancer [22 26]. These models are used to quantify the risk of identifying a mutation in a patient. Upon this assessment, a testing strategy is devised. The patient is counseled on the disease(s) in question in a manner that is tailored to the patient s education level and focused on conveying the necessary information to make an informed decision regarding genetic testing. In addition to facilitating the patient s understanding of his or her own risks, the genetic counselor helps the patient to identify the family members who may be at risk. A list of the more common hereditary cancer syndromes and their inheritance is listed in Table 2.2. Almost all cancer syndromes follow an autosomal dominant inheritance pattern. This means that an affected individual has a 50% chance of Table 2.2 Syndromes of hereditary cancer Syndrome Ataxia telangiectasia Genes ATM Birt-Hogg-Dube syndrome Carney complex Familial adenomatous polyposis Familial malignant melanoma Familial paraganglioma syndrome Fanconi anemia BHD PRKRA1A APC TP16 SDHB SDHC SDHD FANCA FANCB FANCC FANCD FANCE FANCF FANCG FANCL PTCH BRCA1 BRCA2 CDH1 FH Gorlin syndrome Hereditary breast ovarian cancer Hereditary diffuse gastric cancer Hereditary leiomyomatosis and renal cell carcinoma Hereditary papillary renal cell carcinoma Hyperparathyroid-jaw tumor syndrome Juvenile polyposis syndrome Li-Fraumeni syndrome Lynch syndrome Multiple endocrine neoplasia 1 Multiple endocrine neoplasia 2 MuTYH-associated polyposis Neurofibromatosis type 1 Neurofibromatosis type 2 Peutz-Jehgers syndrome PTEN-hamartoma tumor syndrome Inheritance Recessive (only carriers at risk for cancer) Recessive Clinical testing available MET HPRT2 BMPRIA SMAD4 P53 hmlh1 hmsh2 hmsh6 hpms2 MEN1 RET MuTYH NF1 NF2 STK11 PTEN Recessive (continued)
6 28 B. Heald and J.M. Church Table 2.2 (continued) Syndrome Retinoblastoma Tuberous sclerosis complex Von Hippel Lindau disease Wilms tumor Xeroderma pigmentosa Genes RB1 TSC1 TSC2 VHL WT1 XPA ERCC3 XPC ERCC2 XPE ERCC4 ERCC5 Inheritance Recessive Clinical testing available passing on the pathogenic mutation to each pregnancy. There is also a 50% chance that the mutation would not be passed on. There are also a few hereditary cancer syndromes that follow an autosomal recessive pattern of inheritance. Autosomal recessive inheritance requires that both copies of the gene are mutated in order for the syndrome to manifest. When both parents are carriers of a mutated gene each offspring has a 25% chance of being unaffected, a 50% chance of also being a carrier, and a 25% chance of inheriting both mutated copies of the gene. In this case, that individual would be affected with the disease. Genetic Testing Genetic testing is an important part of the care of families with hereditary cancer syndromes. Ideally, testing is performed on a member of the family who has been diagnosed with cancer. Prior to ordering genetic testing, patients should be fully informed of the risks, benefits, and limitations of genetic testing. As part of this conversation, patients should be aware of the type of testing being ordered, the associated cost, and the turnaround time. Patients should be counseled about the outcomes of testing, and a plan should be established for how results will be disclosed. It is the role of a genetic counselor to ensure that all these issues are properly addressed with the patient. In 1997, Giardiello et al. showed what can happen when genetic counseling is not a part of genetic testing [27]. They reported on APC testing in 177 patients from 125 families during Only 18.6% (33 of 177) received genetic counseling before the test, and only 16.9% (28 of 166) provided written informed consent. The ordering physicians misinterpreted the test results 31.6% of the time. Finally, when the indications for testing were not those commonly used, the rate of positive results was only 2.3% (1 of 44). While these results are concerning, they apply to a relatively simple monogenic syndrome, with clear dominant inheritance, and penetrance close to 100%. Almost all other syndromes of hereditary cancer are more complex.
7 2 Cancer and Genetic Counseling 29 Clinical Versus Research Genetic Testing Important distinctions should be made between clinical and research genetic testing. Clinical genetic testing is used for diagnostic purposes and to guide medical management [28]. Within the United States, clinical testing must be preformed in a laboratory with Clinical Laboratory Improvement Amendments (CLIA) certification. CLIA certification requires that laboratory meets quality control and proficiency testing standards. This certification is a regulation of the Centers for Medical & Medicaid Services, which sets the precedent for other third party payers. There is a charge associated with clinical testing, and the majority of health insurance providers do cover some portion of genetic testing. Additionally, clinical test results are reported in writing. Research testing is done to develop a clinical test or gain a better understanding of a condition [28]. Typically, there is no cost to the patient for research testing as the investigator usually covers this. Research laboratories are neither required to have CLIA certification nor are they obligated to provide patients with the results of research genetic testing. If a patient does receive results from a research study, that information cannot be used to diagnose or manage the patient until it is confirmed in a laboratory with CLIA certification. Genetic Test Results For the first family member who undergoes genetic testing, there are three potential results: positive, negative, or uncertain. A positive result means that a deleterious mutation has been identified thus confirming that the patient has a hereditary cancer syndrome. This result can then be used to direct medical management for that patient and can be used to perform predictive testing for other family members. A negative result means that no mutation was identified. There are multiple explanations for this result. One explanation is that the patient does not have the genetic syndrome in question. A second explanation is that there are limitations of genetic testing technology. There is always a possibility that a mutation could be present within the gene that could not be detected with current genetic testing technology. Third, there could be a mutation in another gene that is responsible for the cancer in the family. Additionally, if the first person tested in the family is not someone who has been diagnosed with cancer, it is possible that a mutation is present in the family but that individual did not inherit the mutation. It is not possible to distinguish between these possibilities. Therefore, negative genetic test results do not necessarily rule out the possibility that a patient has a hereditary cancer syndrome. In the case of a negative genetic test result, the patient should be counseled that the likelihood that he or she has a hereditary cancer syndrome has been greatly reduced. Finally, a variant of uncertain significance could be identified. In this case, a genetic alteration has been identified but insufficient data exist in order to determine
8 30 B. Heald and J.M. Church if this mutation is pathogenic or polymorphic. In general, it is not recommended to perform predictive testing for at-risk family members for variants of uncertain significance. Predictive Genetic Testing The results of predictive testing are much more straightforward to interpret. Once a deleterious mutation is identified in a patient, single site testing for that mutation should be offered to all at-risk relatives. Any relative found to have the familyspecific deleterious mutation as has the hereditary cancer syndrome in question, that individual should then be offered increased cancer surveillance, chemoprevention, and/or prophylactic surgical options. If a relative is found not to have the family-specific mutation then he or she does not have the hereditary cancer syndrome in question and is at the general population risk to develop cancer. This is considered a true negative result. This individual should be offered general population cancer surveillance. Benefits of Genetic Testing Identification of a pathogenic mutation provides the patient with an explanation for their personal and/or family history of cancer, allows for medical management options to reduce the risk of developing a future cancer, and makes predictive testing available for family members. If a family member is found to have the family- specific mutation then he or she would be offered increased cancer surveillance and, potentially, prophylactic surgery to help reduce the risk of developing a cancer. Relatives who are affected can be diagnosed early, often before cancer has developed. If a relative is found not to carry the deleterious mutation then he or she would not need to undergo increased surveillance above the general population. This is perhaps the most important advantage of genetic testing, as without it everyone in the family must undergo surveillance as if they were affected. Affected patients can consider their status and the risk to their children in planning a family. Additionally, family planning options such as pre-implantation genetic diagnosis or prenatal testing could be considered if the family-specific mutation has been identified. Knowledge of the precise location of the mutation and the particular gene involved may allow for prediction of the clinical expression of the disease, and a tailored surveillance program. For example, multiple endocrine neoplasia (MEN) type 2B is the most aggressive form of MEN 2 and is associated with onset of medullary thyroid cancer in the teenage years, pheochromocytoma, and developmental defects. Greater than 95% of patients with MEN 2B have the mutation M918T in exon 15. Current consensus is that patients with this mutation undergo prophylactic thyroidectomy within the first six months of life [29].
9 2 Cancer and Genetic Counseling 31 Limitations of Genetic Testing The major limitation of genetic testing is the mutation detection frequency. With the exception of VHL gene testing, there is no genetic test for hereditary cancer syndromes that has a 100% mutation detection rate. However, the evolution of genetic testing, with increased sensitivity and mutation detection frequency, has been relatively quick over the last 10 years. While a patient may undergo genetic testing that is negative, or uninformative, it is likely that as sequencing and other genetic testing technologies, such as those to detect large deletions/duplications, are introduced, mutation negative patients will have their mutation found. In the case of Peutz-Jeghers syndrome, sequencing of STK11 will detect 39 69% of mutations. Until 2005, it was believed that a second susceptibility locus existed but then it was found that nearly 30% of patients have large deletions, which would not be detected using sequencing [30]. Now, with the incorporation of large deletion analysis, the deleterious mutation will be identified for the majority of patients with Peutz-Jeghers syndrome. Risks Associated with Genetic Testing Some patients and families may wish not to know their hereditary status. This fear of knowing is more common in hereditary syndromes without adequate treatment or interventions, such as Li-Fraumeni syndrome. Ideally, through the process of genetic counseling patients will gain an understanding of their cancer risk, strategies to help reduce this risk, and receive psychosocial support for coping with this result. There is also a possibility that through testing multiple family members nonpaternity could be uncovered. Additionally, patients could learn that they are not biologically related to their family members, as in cases of adoption. Finally, as long as genetic testing has been offered there has been a fear that the results will be used to influence decisions of employability or insurability. In practice, genetic discrimination is uncommon, and in many syndromes disease phenotype and family history make the diagnosis as clearly as the results of genetic testing. To date, there are no well-documented cases of insurance discrimination with regard to genetic information that have been reported. Further, the Health Insurance Portability and Accountability Act has a provision, which states that genetic testing information cannot be used as a pre-existing condition for patients who are in group health insurance plans. In May 2008, the Genetic Information Nondiscrimination Act (GINA) was signed into law. GINA prohibits United States insurance companies and employers from discriminating on the basis of genetic information. Genetic information is broadly defined as family history of a disease (up to a fourth-degree relative), genetic services, genetic test results, and participation in research involving genetics. In addition, under this law, insurers and employers are not allowed to request or demand a genetic test. The ability to obtain life and disability insurance are not protected by any laws.
10 32 B. Heald and J.M. Church Conclusion Diagnosing a hereditary cancer syndrome is essential for management of patients and their family members. To achieve the best outcome for patients, identification, assessment, diagnosis, and management requires a multidisciplinary team. A key member of the team is the genetic counselor. Genetic counselors are healthcare providers trained to obtain and evaluate medical and family histories; explain the genetics of hereditary cancer syndromes; facilitate genetic testing; interpret and discuss the results of genetic testing, and advise about genetic discrimination and family planning. References 1. Recommendations from the EGAPP Working Group: genetic testing strategies in newly diagnosed individuals with colorectal cancer aimed at reducing morbidity and mortality from Lynch syndrome in relatives. Genet Med 11, (2009). 2. Khatcheressian, J.L. et al. American Society of Clinical Oncology 2006 update of the breast cancer follow-up and management guidelines in the adjuvant setting. J Clin Oncol 24, (2006). 3. Lancaster, J.M. et al. Society of Gynecologic Oncologists Education Committee statement on risk assessment for inherited gynecologic cancer predispositions. Gynecol Oncol 107, (2007). 4. Murphy, C.D. et al. The American Cancer Society guidelines for breast screening with magnetic resonance imaging: an argument for genetic testing. Cancer 113, (2008). 5. Winawer, S. et al. Colorectal cancer screening and surveillance: clinical guidelines and rationale-update based on new evidence. Gastroenterology 124, (2003). 6. Trepanier, A. et al. Genetic cancer risk assessment and counseling: recommendations of the national society of genetic counselors. J Genet Couns 13, (2004). 7. Dudley-Brown, S. & Freivogel, M. Hereditary colorectal cancer in the gastroenterology clinic: how common are at-risk patients and how do we find them? Gastroenterol Nurs 32, 8 16 (2009). 8. Mitchell, R.J. et al. Accuracy of reporting of family history of colorectal cancer. Gut 53, (2004). 9. Church, J. & McGannon, E. Family history of colorectal cancer: how often and how accurately is it recorded? Dis Colon Rectum 43, (2000). 10. Lynch, H.T. et al. Who should be sent for genetic testing in hereditary colorectal cancer syndromes? J Clin Oncol 25, (2007). 11. Murff, H.J., Spigel, D.R. & Syngal, S. Does this patient have a family history of cancer? An evidence-based analysis of the accuracy of family cancer history. JAMA 292, (2004). 12. Tyler, C.V., Jr. & Snyder, C.W. Cancer risk assessment: examining the family physician s role. J Am Board Fam Med 19, (2006). 13. Mitchell, R.J. et al. Prevalence of family history of colorectal cancer in the general population. Br J Surg 92, (2005). 14. Schneider, K.A. Counseling About Cancer: Strategies for Genetic Counseling, 333 (WileyLiss, Inc., New York, 2002). 15. Young, S.R. et al. The prevalence of BRCA mutations among young women with triple-negative breast cancer. BMC Cancer 9, 86 (2009). 16. Berry, D.A., Parmigiani, G., Sanchez, J., Schildkraut, J. & Winer, E. Probability of carrying a mutation of breast-ovarian cancer gene BRCA1 based on family history. J Natl Cancer Inst 89, (1997).
11 2 Cancer and Genetic Counseling Couch, F.J. et al. BRCA1 mutations in women attending clinics that evaluate the risk of breast cancer. N Engl J Med 336, (1997). 18. Frank, T.S. et al. Clinical characteristics of individuals with germline mutations in BRCA1 and BRCA2: analysis of 10,000 individuals. J Clin Oncol 20, (2002). 19. Shattuck-Eidens, D. et al. BRCA1 sequence analysis in women at high risk for susceptibility mutations. Risk factor analysis and implications for genetic testing. JAMA 278, (1997). 20. Stoppa-Lyonnet, D. et al. BRCA1 sequence variations in 160 individuals referred to a breast/ ovarian family cancer clinic. Institut Curie Breast Cancer Group. Am J Hum Genet 60, (1997). 21. Tyrer, J., Duffy, S.W. & Cuzick, J. A breast cancer prediction model incorporating familial and personal risk factors. Stat Med 23, (2004). 22. Balmana, J. et al. Prediction of MLH1 and MSH2 mutations in Lynch syndrome. JAMA 296, (2006). 23. Barnetson, R.A. et al. Identification and survival of carriers of mutations in DNA mismatchrepair genes in colon cancer. N Engl J Med 354, (2006). 24. Chen, S. et al. Prediction of germline mutations and cancer risk in the Lynch syndrome. JAMA 296, (2006). 25. Marroni, F. et al. A genetic model for determining MSH2 and MLH1 carrier probabilities based on family history and tumor microsatellite instability. Clin Genet 69, (2006). 26. Wijnen, J.T. et al. Clinical findings with implications for genetic testing in families with clustering of colorectal cancer. N Engl J Med 339, (1998). 27. Giardiello, F.M. et al. The use and interpretation of commercial APC gene testing for familial adenomatous polyposis. N Engl J Med 336, (1997). 28. GeneTests. Medical Genetics Information Resource. (University of Seattle, Washington, ). 29. Brandi, M.L. et al. Guidelines for diagnosis and therapy of MEN type 1 and type 2. J Clin Endocrinol Metab 86, (2001). 30. Aretz, S. et al. High proportion of large genomic STK11 deletions in Peutz-Jeghers syndrome. Hum Mutat 26, (2005).
12
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Information for You and Your Family
 Information for You and Your Family What is Prevention? Cancer prevention is action taken to lower the chance of getting cancer. In 2017, more than 1.6 million people will be diagnosed with cancer in the
Information for You and Your Family What is Prevention? Cancer prevention is action taken to lower the chance of getting cancer. In 2017, more than 1.6 million people will be diagnosed with cancer in the
Clinical Cancer Genetics
 Clinical Cancer Genetics Lisen Axell, MS, CGC University of Colorado Cancer Center Individuals with cancer Making surgical decisions (lump vs. mast) Making treatment decisions (XRT) Concerns for additional
Clinical Cancer Genetics Lisen Axell, MS, CGC University of Colorado Cancer Center Individuals with cancer Making surgical decisions (lump vs. mast) Making treatment decisions (XRT) Concerns for additional
CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION
 CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION CentoCancer our most comprehensive oncogenetics panel for hereditary mutations Hereditary pathogenic variants confer an increased risk of developing
CentoCancer STRIVE FOR THE MOST COMPLETE INFORMATION CentoCancer our most comprehensive oncogenetics panel for hereditary mutations Hereditary pathogenic variants confer an increased risk of developing
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian
 Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
HEREDITY & CANCER: Breast cancer as a model
 HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
The benefit of. knowing. Genetic testing for hereditary cancer. A patient support guide
 The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
B Base excision repair, in MUTYH-associated polyposis and colorectal cancer, BRAF testing, for hereditary colorectal cancer, 696
 Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic testing for hereditary cancer
 Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
Are you at risk of Hereditary Cancer? Your Guide to the Answers
 Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Cancer Survivorship Symposium Cancer and Heredity January 16, Jeanne P. Homer, MS Licensed Certified Genetic Counselor
 Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention
 patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime
patient guide CancerNext-Expanded genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime
Hereditary Breast and Ovarian Cancer Rebecca Sutphen, MD, FACMG
 Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
BRCA 1/2. Breast cancer testing THINK ABOUT TOMORROW, TODAY
 BRCA 1/2 Breast cancer testing THINK ABOUT TOMORROW, TODAY 5 10% of patients with breast and/or ovarian cancer have a hereditary form1. For any individual carrying a mutation in BRCA1 or BRCA2, the lifetime
BRCA 1/2 Breast cancer testing THINK ABOUT TOMORROW, TODAY 5 10% of patients with breast and/or ovarian cancer have a hereditary form1. For any individual carrying a mutation in BRCA1 or BRCA2, the lifetime
Informed Consent Columbia Whole Genome or Whole Exome Sequencing
 Informed Consent Columbia Whole Genome or Whole Exome Sequencing Please read the following form carefully and discuss with your ordering physician before signing consent. This consent is intended for the
Informed Consent Columbia Whole Genome or Whole Exome Sequencing Please read the following form carefully and discuss with your ordering physician before signing consent. This consent is intended for the
Why Test for Hereditary Cancer in Preventive Care?
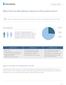 Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Neurogenetics Genetic Testing and Ethical Issues
 Neurogenetics Genetic Testing and Ethical Issues Grace Yoon, MD, FRCP(C) Divisions of Neurology and Clinical and Metabolic Genetics The Hospital for Sick Children Objectives 1) To recognize the ethical
Neurogenetics Genetic Testing and Ethical Issues Grace Yoon, MD, FRCP(C) Divisions of Neurology and Clinical and Metabolic Genetics The Hospital for Sick Children Objectives 1) To recognize the ethical
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
CANCER GENETICS PROVIDER SURVEY
 Dear Participant, Previously you agreed to participate in an evaluation of an education program we developed for primary care providers on the topic of cancer genetics. This is an IRB-approved, CDCfunded
Dear Participant, Previously you agreed to participate in an evaluation of an education program we developed for primary care providers on the topic of cancer genetics. This is an IRB-approved, CDCfunded
So, now, that we have reviewed some basics of cancer genetics I will provide an overview of some common syndromes.
 Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Genetic Determinants, Risk Assessment and Management
 Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017
 Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
6/8/17. Genetics 101. Professor, College of Medicine. President & Chief Medical Officer. Hereditary Breast and Ovarian Cancer 2017
 Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Genetic Testing for Familial Gastrointestinal Cancer Syndromes. C. Richard Boland, MD La Jolla, CA January 21, 2017
 Genetic Testing for Familial Gastrointestinal Cancer Syndromes C. Richard Boland, MD La Jolla, CA January 21, 2017 Disclosure Information C. Richard Boland, MD I have no financial relationships to disclose.
Genetic Testing for Familial Gastrointestinal Cancer Syndromes C. Richard Boland, MD La Jolla, CA January 21, 2017 Disclosure Information C. Richard Boland, MD I have no financial relationships to disclose.
Hereditary Gastric Cancer
 Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
DNA Genetic Cancer Risk Test. Test Report
 Test Report CONTENTS SECTION 1 1-1. Customer Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Cancers / Tumors Tested SECTION 2 2-1. About the Test 2-2. References 1 CL0040-1_B
Test Report CONTENTS SECTION 1 1-1. Customer Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Cancers / Tumors Tested SECTION 2 2-1. About the Test 2-2. References 1 CL0040-1_B
Germline Testing for Hereditary Cancer with Multigene Panel
 Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Reference #: SYS-PC-VPCI-CG-002. Origination Date: June 2012 Next Review Date: April 2019 Effective Date: April 2016
 Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
A guide to genetic testing for hereditary cancers
 Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Genetic Testing for Hereditary Cancer Susceptibility Syndromes
 Medical Coverage Policy Genetic Testing for Hereditary Cancer Susceptibility Syndromes Table of Contents Effective Date... 1/15/2018 Next Review Date... 7/15/2018 Coverage Policy Number... 0518 Related
Medical Coverage Policy Genetic Testing for Hereditary Cancer Susceptibility Syndromes Table of Contents Effective Date... 1/15/2018 Next Review Date... 7/15/2018 Coverage Policy Number... 0518 Related
Identification of patients suggestive of hereditary breast and ovarian cancer syndrome that warrants further professional evaluation.
 Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective
 Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
patient guide RenalNext genetic testing for hereditary kidney cancer Because knowing your risk can mean early detection and prevention
 patient guide RenalNext genetic testing for hereditary kidney cancer Because knowing your risk can mean early detection and prevention Know the Basics Risk factors for developing kidney cancer include
patient guide RenalNext genetic testing for hereditary kidney cancer Because knowing your risk can mean early detection and prevention Know the Basics Risk factors for developing kidney cancer include
BowelGene. How do I know if I am at risk? Families with hereditary bowel cancer generally show one or more of the following clues:
 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
Corporate Medical Policy
 Corporate Medical Policy Genetic Cancer Susceptibility Panels Using Next Generation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_cancer_susceptibility_panels_using_next_generation_sequencing
Corporate Medical Policy Genetic Cancer Susceptibility Panels Using Next Generation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_cancer_susceptibility_panels_using_next_generation_sequencing
Primary Care Approach to Genetic Cancer Syndromes
 Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Introduction to Evaluating Hereditary Risk. Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center
 Introduction to Evaluating Hereditary Risk Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center Objectives Describe genetic counseling and risk assessment Understand
Introduction to Evaluating Hereditary Risk Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center Objectives Describe genetic counseling and risk assessment Understand
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer
 GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
Hereditary Aspects of Pancreatic Cancer
 Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Pathology reports, related operative reports and consult letters must be provided with a request for assessment.
 Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014
 COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
Genetic Cancer Susceptibility Panels Using Next Generation Sequencing
 Genetic Cancer Susceptibility Panels Using Next Generation Sequencing Policy Number: 2.04.93 Last Review: 7/2017 Origination: 7/2013 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City
Genetic Cancer Susceptibility Panels Using Next Generation Sequencing Policy Number: 2.04.93 Last Review: 7/2017 Origination: 7/2013 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City
Learn your genetic risk for the most common hereditary cancers.
 Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
Does Cancer Run in Your Family?
 Does Cancer Run in Your Family? Nancie Petrucelli, MS, CGC Clinical Assistant Professor Certified Genetic Counselor/Coordinator Cancer Genetic Counseling Service Karmanos Cancer Institute Wayne State University
Does Cancer Run in Your Family? Nancie Petrucelli, MS, CGC Clinical Assistant Professor Certified Genetic Counselor/Coordinator Cancer Genetic Counseling Service Karmanos Cancer Institute Wayne State University
Hereditary Cancer Syndromes
 Hereditary Cancer Syndromes Nicoleta Voian, MD, MPH Director Clinical Genetics Service Roswell Park Cancer Institute Nicoleta.Voian@Roswellpark.org February 28, 2017 Common Genetics Terms Gene: A hereditary
Hereditary Cancer Syndromes Nicoleta Voian, MD, MPH Director Clinical Genetics Service Roswell Park Cancer Institute Nicoleta.Voian@Roswellpark.org February 28, 2017 Common Genetics Terms Gene: A hereditary
GHUK BowelGene_2017.qxp_Layout 1 22/02/ :22 Page 3 BowelGene
 GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
GYNplus. genetic testing for hereditary ovarian and/or uterine cancer
 GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GI EMERGENCIES Acute Abdominal Pain
 GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
11/29/2017. Genetics and Cancer ERICA L SILVER, MS, LCGC GENETIC COUNSELOR. Genetics 101. Transcription vs Translation
 Genetics and Cancer ERICA L SILVER, MS, LCGC GENETIC COUNSELOR Genetics 101 Transcription vs Translation 1 Carcinogenesis and Genetics Normal cell First mutation First mutation Second mutation Second mutation
Genetics and Cancer ERICA L SILVER, MS, LCGC GENETIC COUNSELOR Genetics 101 Transcription vs Translation 1 Carcinogenesis and Genetics Normal cell First mutation First mutation Second mutation Second mutation
Genetic Testing: who, what, why?
 Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Corporate Medical Policy
 Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
The Next Generation of Hereditary Cancer Testing
 The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
Introduction to Genetics
 Introduction to Genetics Table of contents Chromosome DNA Protein synthesis Mutation Genetic disorder Relationship between genes and cancer Genetic testing Technical concern 2 All living organisms consist
Introduction to Genetics Table of contents Chromosome DNA Protein synthesis Mutation Genetic disorder Relationship between genes and cancer Genetic testing Technical concern 2 All living organisms consist
Colorectal Cancer - Working in Partnership. David Baty Genetics, Ninewells Hospital
 Colorectal Cancer - Working in Partnership David Baty Genetics, Ninewells Hospital Genetics and Pathology National initiatives Colorectal cancer Inherited CRC Sporadic CRC The Liquid Biopsy The future?
Colorectal Cancer - Working in Partnership David Baty Genetics, Ninewells Hospital Genetics and Pathology National initiatives Colorectal cancer Inherited CRC Sporadic CRC The Liquid Biopsy The future?
Lynch Syndrome. Angie Strang, PGY2
 Lynch Syndrome Angie Strang, PGY2 Background Previously hereditary nonpolyposis colorectal cancer Autosomal dominant inherited cancer susceptibility syndrome Caused by defects in the mismatch repair system
Lynch Syndrome Angie Strang, PGY2 Background Previously hereditary nonpolyposis colorectal cancer Autosomal dominant inherited cancer susceptibility syndrome Caused by defects in the mismatch repair system
Hereditary Cancer Update: What do GPOs need to know?
 Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
Ovarian Cancer Causes, Risk Factors, and Prevention
 Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing.
 Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
What All of Us Should Know About Cancer and Genetics
 What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
OvaNext. patient guide. genetic testing for hereditary breast, ovarian, and uterine cancer
 patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
Family history of pancreatic cancer
 Family history of pancreatic cancer _ This fact sheet is for people who want to find out about the hereditary risk of pancreatic cancer. You can speak to our specialist nurses on our Support Line about
Family history of pancreatic cancer _ This fact sheet is for people who want to find out about the hereditary risk of pancreatic cancer. You can speak to our specialist nurses on our Support Line about
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD
 Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
ERN: GENTURIS Gene-c Tumour Risk Syndromes
 ERN: GENTURIS Gene-c Tumour Risk Syndromes Prof Nicoline Hoogerbrugge MD, PhD Coordinator Barcelona ESHG AIM of ERN GENTURIS Improving the iden@fica@on, diagnosis of a wide range of inherited syndromes
ERN: GENTURIS Gene-c Tumour Risk Syndromes Prof Nicoline Hoogerbrugge MD, PhD Coordinator Barcelona ESHG AIM of ERN GENTURIS Improving the iden@fica@on, diagnosis of a wide range of inherited syndromes
A Patient s Guide to Hereditary Cancer. Is Hereditary Cancer Testing Right for You?
 A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention
 patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime types
patient guide CancerNext genetic testing for hereditary cancer Because knowing your risk can mean early detection and prevention Know the Basics Cancer occurs in about 1 in 3 adults in their lifetime types
Hereditary Cancer Risk Assessment for Gynecological Cancers. FarrNezhatMD.com
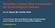 Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
CASE STUDY. Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members. Introduction. Patient Profile.
 CASE STUDY Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members Introduction Most cancers are caused by genetic damage resulting from random mutations and exposure to
CASE STUDY Germline Cancer Testing in A Proband: Extension of Benefits to Unaffected Family Members Introduction Most cancers are caused by genetic damage resulting from random mutations and exposure to
Whole Exome Sequencing (WES): Questions and Answers for Providers
 Whole Exome Sequencing (WES): Questions and Answers for Providers 1. What is Whole Exome Sequencing?... 2 2. What is the difference between Whole Exome Sequencing (WES) and Whole Exome Sequencing Plus
Whole Exome Sequencing (WES): Questions and Answers for Providers 1. What is Whole Exome Sequencing?... 2 2. What is the difference between Whole Exome Sequencing (WES) and Whole Exome Sequencing Plus
Cancer genetics
 Cancer genetics General information about tumorogenesis. Cancer induced by viruses. The role of somatic mutations in cancer production. Oncogenes and Tumor Suppressor Genes (TSG). Hereditary cancer. 1
Cancer genetics General information about tumorogenesis. Cancer induced by viruses. The role of somatic mutations in cancer production. Oncogenes and Tumor Suppressor Genes (TSG). Hereditary cancer. 1
Genetic Testing of Inherited Cancer Predisposition Genetic Testing - Oncology
 Genetic Testing of Inherited Cancer Predisposition Genetic Testing - Oncology Policy Number: Original Effective Date: MM.02.010 05/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Testing of Inherited Cancer Predisposition Genetic Testing - Oncology Policy Number: Original Effective Date: MM.02.010 05/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Célia DeLozier-Blanchet
 The Genetics Consultation in OB-GYN : Hereditary cancers Célia DeLozier-Blanchet Division of Medical Genetics, Geneva University Hospital It is probable that all cancers are genetic! genetic vs. hereditary
The Genetics Consultation in OB-GYN : Hereditary cancers Célia DeLozier-Blanchet Division of Medical Genetics, Geneva University Hospital It is probable that all cancers are genetic! genetic vs. hereditary
Policy Specific Section: Medical Necessity and Investigational / Experimental. October 14, 1998 March 28, 2014
 Medical Policy Genetic Testing for Colorectal Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: October
Medical Policy Genetic Testing for Colorectal Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: October
Multigene Panel Testing for Hereditary Cancer Risk
 Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes
 ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)!
 LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)! Kathryn Singh, MPH, MS, LCGC Associate Clinical Professor Assistant Director, Graduate Program in Genetic Counseling Division of Genetic and Genomic
LYNCH SYNDROME: IN YOUR FACE BUT LOST IN SPACE (MOUNTAIN)! Kathryn Singh, MPH, MS, LCGC Associate Clinical Professor Assistant Director, Graduate Program in Genetic Counseling Division of Genetic and Genomic
Result Navigator. Positive Test Result: STK11. After a positive test result, there can be many questions about what to do next. Navigate Your Results
 Result Navigator Positive Test Result: STK11 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: STK11 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
WELCOME. Taking Care of Your Health. April 30, 8 am to noon
 WELCOME Taking Care of Your Health April 30, 8 am to noon Cancer: Know Your Risk Emily Kuchinsky, MS, CGC, Certified Genetic Counselor Sporadic Cancer Lifetime Probability- Women Family Cluster Risk factors
WELCOME Taking Care of Your Health April 30, 8 am to noon Cancer: Know Your Risk Emily Kuchinsky, MS, CGC, Certified Genetic Counselor Sporadic Cancer Lifetime Probability- Women Family Cluster Risk factors
PMS2 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table
 PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Medical Policy Update
 Medical Policy Update Summer 2017 Highlights of recent medical policy revisions as well as any new medical policies approved by Prevea360 Health Plan s Medical Policy Committee are shown below. The Medical
Medical Policy Update Summer 2017 Highlights of recent medical policy revisions as well as any new medical policies approved by Prevea360 Health Plan s Medical Policy Committee are shown below. The Medical
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T. Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics
 GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
MSH6 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table
 MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
10/21/ New Release, Quest Diagnostics Nichols Institute, Valencia
 NEW TESTS Please Note: Not all test codes assigned to each assay are listed in the table of contents. Please refer to the complete listing on the page numbers indicated. Test Code Test Name Effective Date
NEW TESTS Please Note: Not all test codes assigned to each assay are listed in the table of contents. Please refer to the complete listing on the page numbers indicated. Test Code Test Name Effective Date
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
BRCAplus. genetic testing for hereditary breast cancer
 BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
Asingle inherited mutant gene may be enough to
 396 Cancer Inheritance STEVEN A. FRANK Asingle inherited mutant gene may be enough to cause a very high cancer risk. Single-mutation cases have provided much insight into the genetic basis of carcinogenesis,
396 Cancer Inheritance STEVEN A. FRANK Asingle inherited mutant gene may be enough to cause a very high cancer risk. Single-mutation cases have provided much insight into the genetic basis of carcinogenesis,
Yes when meets criteria below. Dean Health Plan covers when Medicare also covers the benefit.
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Importance of Family History in Gynecologic Cancer Prevention. Objectives. Genetic Counselors. Angela Thompson, MS, CGC
 Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Precision Medicine and Genetic Counseling : Is Yes always the correct answer?
 Precision Medicine and Genetic Counseling : Is Yes always the correct answer? Beverly M. Yashar, MS, PhD, CGC Director, Graduate Program in Genetic Counseling Professor, Department of Human Genetics. (yashar@umich.edu)
Precision Medicine and Genetic Counseling : Is Yes always the correct answer? Beverly M. Yashar, MS, PhD, CGC Director, Graduate Program in Genetic Counseling Professor, Department of Human Genetics. (yashar@umich.edu)
Objectives. Genetics in Cancer Treatment and Prevention. Genes
 Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
