is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
|
|
|
- Rodney Newman
- 5 years ago
- Views:
Transcription
1 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment of patients with oncologic diseases. The objectives of this session [are] to be able to discuss the role for surgery for both solid tumors and hematologic malignancies; to describe the various biopsy techniques, which are used including incisional biopsy, excisional biopsy, open biopsy, core biopsy as well as fine needle aspiration; and to discuss the complications of surgical intervention as well as the role for surgery in palliation and in patients with metastatic disease. So, traditionally surgery is the main modality for treatment of patients with solid tumors. It can be used both as a diagnostic means, a curative means and a palliative means, and we will discuss all those individually. For hematological malignancies, surgery is not traditionally a curative modality. It is more of a supportive modality. Surgery is used for venous access, not infrequently for decreasing the burden of disease by doing splenectomies in patients with leukemia or lymphoma, as well as doing biopsies in order to obtain diagnoses for patients with these disease processes. So, from a diagnostic standpoint, traditionally surgical biopsy was done by either incisional or excisional biopsy. Nowadays, open biopsies like incisional or excisional biopsy are much less common. We much more commonly use fine needle aspiration or FNA, core biopsies, or image-guided needle biopsies. Surgery has also traditionally been an important part of staging the patient. Laparoscopic staging was initially a --- was an initial use of laparoscopy in patients with cancer, most commonly in patients with gastric cancer or pancreatic cancer. However, as imaging modalities like CT scan, PET scan, and MRI have markedly improved over the last several years the use for --- the need for surgery in staging has decreased. And it is fairly uncommon that we do staging even using laparoscopic methods in patients with cancer nowadays. So, again the main purpose for surgery in patients with solid tumors is curative treatment. Most patients --- even patients understand that the best way to cure a tumor is to take it out. It is the only treatment modality that independently is able to provide cure for a large variety of solid tumors. The basic principles of surgical resection for cancer include the removal of all of the gross visible tumor. And this should be done with surrounding margin of normal tissue with a general rule of 2 cm being the accepted or the ideal amount of normal tissue around the tumor that we would like. In order to get that normal tissue around the tumor, it may require resection of adjacent organs. Not infrequently we have to evaluate margins at the time of surgery to be sure that not only all the macroscopic tumor is removed, but the microscopic tumor as well. We fairly liberally use intraoperative assessment, but depending --- but there are some restrictions that may help guide whether to use intra-operative assessment, because it
2 is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the margin or if that additional tissue would cause --- would inflict significant morbidity or potentially even mortality on the patient. So if you can t get any more margin, there is no reason to assess the margin. If you can get more tissue, then it makes sense to assess the margin while the patient is still asleep and in the operating room. The immediate pathologic evaluation may be required to be sure that the margin is free of tumor, and I think the most frequent setting we use this in is breast cancer, because, if we are doing a partial mastectomy, there is many times that we can take more tissue to be sure that there is a true microscopic negative margin. This can be difficult for the pathologist, because, if patients have gotten preoperative treatment either chemotherapy or radiation therapy, it can be much more difficult for them to be able to evaluate normal tissue from scar tissue from tumor tissue. Additionally, if patients have had previous surgeries, scar tissue can make frozen section more difficult to evaluate. So, it s not always easy for the pathologist to evaluate margins while the patient is asleep. Again, it can be very time consuming and also very expensive. The other important role for surgery, which falls into staging, is evaluation of the lymph node basins. That frequently is required as I said for staging, but sometimes is required for local control and in some cases even for cure of the patient when removing lymph nodes will improve the outcome. For intra-abdominal tumors like the stomach, the colon, or the pancreas, the normal resection falls along according to the vascular supply and drainage of that organ. For trunk or extremities, tumors in the trunk or extremities like, for example, the breast, there is an orderly drainage pattern, as you see here, from the area of the tumor to the lymph node basin. It is very frequent that these tumors will spread through the regional lymph nodes like in breast and melanoma. But there are some tumors that never --- very rarely metastasize to the lymph nodes, such as sarcoma and hepatocellular carcinoma and those tumors, because they rarely, so rarely metastasize to the lymph nodes, do not require a lymph node evaluation. How else can we evaluate lymph nodes if we know there are abnormal lymph nodes preoperatively? You can do a fine needle aspiration. You can do a core biopsy. You can do an excisional biopsy of the lymph node. You can do lymphatic mapping and sentinel lymph node biopsy, or you can do a formal lymph node dissection, and we will talk about each of these individually. So, fine needle aspiration is appropriate for evaluating abnormal appearing lymph nodes that are either present on physical exam, ultrasound, or other imaging methods. The problem with fine needle aspiration is it gives you only individual cells. So it can t tell you anything about the structure of the organ or whether there is invasion or not. It can help you to rule out metastatic disease. One other problem is that often you do not
3 have adequate amount of tissue for a complete pathologic evaluation of patients that have hematologic malignancies, so you may be able to get a preliminary evaluation, but not enough information to be able to do a definitive treatment plan. Again, it may not be enough tissue, because you are only getting individual cells, to get a complete histologic diagnosis. An excisional biopsy provides more tissue for pathologic evaluation. An excisional biopsy is a complete removal of the gross tumor. It is helpful in cases that are difficult to diagnose by needle biopsy, and for many hematologic malignancies, it is necessary to have the complete structure of the lymph node, for example, to be able to get a full pathologic evaluation. Lymphatic mapping and sentinel node biopsy is a procedure that now has been in practice for about 10 years. It is based on the fact that there is a reproducible orderly drainage of lymphatics in almost all cases from the primary tumor. And the first lymph node in that regional chain is called the sentinel lymph node. Because of this orderly drainage, the sentinel lymph node is that tumor --- that lymph node that is most likely to harbor metastatic tumor cells. It was originally described for patients with carcinoma of the penis, but has really become the standard of care for melanoma and invasive breast cancer. It is an extremely accurate staging tool. If there is no tumor in the sentinel lymph node then there is no need to do further nodal removal in those diseases. On the other hand, if there is a tumor in the sentinel lymph node, then it may be necessary to perform further evaluation of the remainder of the lymph node basin. That evaluation will be done by a formal lymph node dissection. And a lymph node dissection is removal of the majority of a lymph node basin. There are several purposes to a lymph node dissection. It provides local control for patients with --- that have metastases that have been documented in the sentinel lymph node. It gives more accurate staging, so you know the number of lymph nodes that are involved when --- or if a sentinel node biopsy does not work. There are times about 10% of --- less than 10% of the time that sentinel lymph node biopsy is not successful, where you cannot find the sentinel lymph node. So, you may need to do a lymph node dissection in order to be able to get an accurate lymph node evaluation. The difference between a sentinel lymph node biopsy and a lymph node --- a formal lymph node dissection is that there is a significant increase in the morbidity in post-op recovery with a formal lymph node dissection. The recovery is significantly longer and more morbid. Another area that we use surgery is after patients have received neoadjuvant treatment. Both chemotherapy and radiation therapy are often used in the neoadjuvant setting, sometimes even together. Initially, there was concern that the use of surgery after neoadjuvant treatment would increase morbidity and mortality, and in some cases that is true, especially after neoadjuvant radiation therapy. However, most studies have shown that, for the diseases that we use neoadjuvant radiation therapy, that risk --- that increase in morbidity is not prohibitive.
4 The purpose of neoadjuvant treatment is to reduce the tumor size and bulk. This tumor cytoreduction may allow for some patients to go from being unresectable to resectable. And we see that with chemoradiation for rectal cancer; we see it for patients with metastatic colorectal cancer to the liver, as two examples of diseases that, not infrequently we see good responses to neoadjuvant treatment and enough tumor cytoreduction to allow a change in surgical strategy. It also can reduce the extent of surgery, and this is a way that we increase organ preservation. And again, very classically this has been done in breast cancer. And it has allowed us to do breast conservation in patients who have large tumors by giving them pre-operative chemotherapy --- neoadjuvant chemotherapy. We can reduce the size of tumors and allow them to have partial mastectomies as opposed to total mastectomies. Additionally, it has been very clearly shown in a number of studies that we can increase the sphincter preservation rate in rectal cancer with neoadjuvant chemoradiation therapy, and that is solely because we decrease the bulk of the tumor, which allows the surgery to be a little easier and more readily accomplished in terms of being able to save the sphincters. Well, since we can make tumors smaller, the question often arises does it make sense to debulk tumors and take out part of tumors. In general, it is felt that tumor debulking is not indicated. It is unlikely to alter patient outcome in any solid tumor malignancy. And it is frequently associated with significant morbidity and mortality, because it is hard to define tissue planes when you are cutting through tumor or you are only taking out parts of tumor. The only disease where it has been shown to be beneficial to do tumor debulking is in patients with pseudomyxoma peritonei. In those patients, neoadjuvant --- I m sorry, tumor debulking has been shown in combination with intraperitoneal chemotherapy to both prolong survival and decrease ascites. There have been questions about the role for tumor debulking in ovarian cancer and carcinomatosis. In ovarian cancer, it is the other disease that has been really frequently evaluated, the role and the benefit of debulking surgery and intraperitoneal chemotherapy in ovarian cancer really remains controversial at this time. In patients with multifocal sarcomas throughout the abdominal cavity, so called sarcomatosis, there really has been no proven role of benefit in those patients to debulking tumors. In patients with carcinomatosis, for example, from gastric cancer and pancreatic cancer as well as colorectal cancer, again there has been no good proven role or benefit for debulking those patients and/or using intraperitoneal chemotherapy. Another important role for surgery is the palliation of patients with cancer. We really feel pretty strongly that surgical treatment should be reserved for the alleviation of symptoms. Reducing the bulk of tumor does not improve outcome or increase survival. So, the surgical dogma is you can t palliate something if there is nothing to palliate. So, if the patient is asymptomatic, you cannot improve that. You can only improve on somebody --- a patient s symptoms. So, if there are no symptoms, you can t palliate
5 them. It is probably one of the most difficult decisions to make in surgery, deciding whether the benefit of intervening palliatively from a surgical standpoint outweighs the cost and benefit of an invasive procedure. You have to take into account, there s pain that you introduce from a surgical procedure. Most likely, they will require a hospitalization. And the worse scenario is, if a patient develops a complication when you are doing palliation and has the ultimate worse outcome, even a death. So, though all of those are very difficult things to measure and predict, making it much more difficult --- making it a much more difficult decision as to when to do palliative surgery. Again, alleviating symptoms is the main role for palliation, and we feel strongly that we should use the least invasive methods possible to be able to alleviate those symptoms. So, for example, if you can do something endoscopically, it is better than doing something even laparoscopically, which is better than doing something with open surgery. The least surgery the better. So, for example, if a patient has an obstructing colon cancer, a stent placed endoscopically may relieve the obstruction and avoid a laparotomy or laparostomy or avoid a colostomy. Most patients would prefer not to have a colostomy bag even if they know it s terminal --- you know, part of their terminal event. It is very a difficult thing to convince a patient that a colostomy bag would be in their benefit. If patients are having pain, sometimes things like nerve blocks or regional anesthesia can be used for local control as opposed to resecting the tumor. Again, if you are not going to change the survival, putting a patient through a large operation that could have a large morbidity due to blood loss, functional debility, etc., would not be as big a benefit as if you could control the pain with either pain medication, nerve block, regional anesthesia, or some other less invasive procedure. Frequently, we are asked to help patients who have blockages of their intestinal tracts by placing gastrotomy tubes or feeding jejunostomy tubes. If those tubes can be placed percutaneously, either by endoscopic techniques or interventional radiology --- radiologic techniques, that s better than having the patient have to have an open laparotomy, which again requires more anesthetic time, possibly a hospitalization and the risk of more --- higher risk of complications. We have to understand that sometimes the best intervention may be no intervention. It may be that doing nothing may be the best thing in the palliative setting. Another frequent expanded role for surgery has been the role for surgery in patients with metastatic disease. And traditionally surgery was not felt to be indicated and certainly was not the first line of treatment for patients with metastatic disease, because it was felt that surgery alone, once the tumor has spread from its primary site, was not going to be curative. So why put a patient through a large, potentially painful, difficult recovery if you are not going to be curing the patient? And it was always felt that nonoperative treatment modalities should be considered before doing an operative intervention. When patients have multiple sites of disease, we really think that it is extremely rare that surgery could be of benefit in those patients. So, surgery should be limited to again palliation, as we already discussed. So, for example, if somebody has a bowel obstruction, relieving that bowel obstruction, surgery may be the only way to do that.
6 Patients with symptomatic brain metastasis, again surgery might be the only, or the best potential mechanism for treating those symptoms. On the other hand, when the patients have isolated metastatic disease, it is possible that a subset of those patients can be cured by resecting the metastatic disease. So, how do we know who to resect and who not to resect when there is metastatic disease? There is no good scientific data to say who should be resected and who should not be resected. We think that, if there is a period of stability or response while the patient is on systemic treatment, that might help predict who is going to benefit from resection. So, again with metastatic disease the best primary treatment is systemic treatment, chemotherapy or biologic therapy. If we see a response or the stabilization of tumor in those cases, then it may be that those patients have a favorable biology and will benefit by taking out the tumor then. So, some examples of situations where we use selective surgery for isolated metastatic disease are in patients with sarcoma who we see respond to chemotherapy. We might do resection of their lung metastasis. One of the most common things that we see is patients with colorectal cancer and liver metastasis. We used to say that the limit for a liver resection was for metastasis, and now we have kind of expanded that limit to we don t know what the upper limit should be. We think that, if patients are responding and their tumors are respectable, that they potentially could benefit from resection. There have been several studies to show that there is even a survival benefit in those --- that group of patients. So, if you see a response, or even a stabilization, because stabilization is a response, tumors don t necessarily just have to shrink. If the tumor stops growing that means it has responded to the treatment. So, if there is some sign of response to systemic treatment, resecting those tumors may be reasonable. And, again, in patients with brain metastasis for melanoma, another disease where we may be able to show benefit in both survival and outcome in those patients [is] by resecting that disease. One issue that I have alluded to several times is that surgery comes with potential downsides, and you can t do surgery without the potential of having complications. We really define surgery --- surgical complications into acute and chronic. Acute surgical complications are defined as those that occur within 30 days of the operation. They could be related to the anesthesia and the surgery, such as pneumonia, urinary tract infections, or venous thrombosis are some of the more common complications that we see in the early postoperative period. They may be related to surgery itself, like an abscess, a fistula, or bleeding. All of these are problematic, delay recovery, and even more significantly can potentially delay systemic or adjuvant systemic treatment or radiation treatment. Chronic complications are defined as those that occur or continue for more than 30 days after surgery, and some of the more common things we see are, for example, lymphedema after a lymph node dissection in the extremity. Not uncommonly we can see patients with pain syndromes when there is neurologic involvement of a tumor that has been resected. And then bowel and bladder dysfunction can happen after pelvic surgery, not uncommonly. There is not --- very frequently a change in bladder and
7 bowel habits after both bladder or rectal surgery, and those can be for the patient s entire lifetime, a different change in their bowel patterns or urinary patterns. So, in summary, surgery plays an important role in both the diagnosis, the staging, and the treatment of cancer, more so in solid tumors but also an important role in hematologic malignancies as well. In addition to rendering a patient disease free from their tumor, surgery may be beneficial in providing effective palliation for selected patients. Surgery can result in both acute and chronic complications. I would like to thank you for your time, and please do not hesitate to contact us if there should be any questions regarding this lecture. Thank you very much.
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Heated Intraperitoneal Chemotherapy (HIPEC) for Advanced Abdominal Cancers
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/heated-intraperitonealchemotherapy-hipec-for-advanced-abdominal-cancers/7091/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/heated-intraperitonealchemotherapy-hipec-for-advanced-abdominal-cancers/7091/
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
So, we already talked about that recognition is the key to optimal treatment and outcome.
 Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R
 Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R 2 0 1 2 Objectives Discuss Diagnostic and staging strategies in oncology Know
Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R 2 0 1 2 Objectives Discuss Diagnostic and staging strategies in oncology Know
What is Cancer? Petra Ketterl, MD Medical Oncology and Functional Medicine
 What is Cancer? Petra Ketterl, MD Medical Oncology and Functional Medicine What is Cancer? Layman s terms: cancer starts when cells grow out of control (in any place in the body) and crowd out normal cells
What is Cancer? Petra Ketterl, MD Medical Oncology and Functional Medicine What is Cancer? Layman s terms: cancer starts when cells grow out of control (in any place in the body) and crowd out normal cells
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies
 HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies Crescent City Cancer Update: GI and HPB Saturday September 24, 2016 George M. Fuhrman,
HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies Crescent City Cancer Update: GI and HPB Saturday September 24, 2016 George M. Fuhrman,
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS
 Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Case Scenario 1. Pathology report Specimen from mediastinoscopy Final Diagnosis : Metastatic small cell carcinoma with residual lymphatic tissue
 Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY
 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD
 STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
Pancreatic Cancer: Associated Signs, Symptoms, Risk Factors and Treatment Approaches
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/pancreatic-cancerassociated-signs-symptoms-and-risk-factors-and-treatment-approaches/9552/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/pancreatic-cancerassociated-signs-symptoms-and-risk-factors-and-treatment-approaches/9552/
General Information Key Points
 The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules
 Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules Case 1 72 year old white female presents with a nodular thyroid. This was biopsied in
Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules Case 1 72 year old white female presents with a nodular thyroid. This was biopsied in
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation *
 ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation * CS Tumor Size/Extension Evaluation 24842 12/11/2007: Q:
ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation * CS Tumor Size/Extension Evaluation 24842 12/11/2007: Q:
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominoperineal excision, of rectal cancer, 93 111 current controversies in, 106 109 extent of perineal dissection and removal of pelvic floor,
Note: Page numbers of article titles are in boldface type. A Abdominoperineal excision, of rectal cancer, 93 111 current controversies in, 106 109 extent of perineal dissection and removal of pelvic floor,
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Principles of Surgical Oncology. Winnie Achilles Tierklinik Hollabrunn Lastenstrasse Hollabrunn
 Principles of Surgical Oncology Winnie Achilles Tierklinik Hollabrunn Lastenstrasse 2 2020 Hollabrunn boexi@gmx.de The first surgery provides the best chance for a cure in an animal with a tumor Clinical
Principles of Surgical Oncology Winnie Achilles Tierklinik Hollabrunn Lastenstrasse 2 2020 Hollabrunn boexi@gmx.de The first surgery provides the best chance for a cure in an animal with a tumor Clinical
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Classification System
 Classification System A graduate of the Breast Oncology training program should be able to care for all aspects of disease and/or provide comprehensive management. When referring to a discipline of training
Classification System A graduate of the Breast Oncology training program should be able to care for all aspects of disease and/or provide comprehensive management. When referring to a discipline of training
COLORECTAL CANCER STAGING in 2010
 COLORECTAL CANCER STAGING in 2010 Robert A. Halvorsen, MD, FACR MCV Hospitals / VCU Medical Center Richmond, Virginia I do not have any relevant financial relationships with any commercial interests COLON
COLORECTAL CANCER STAGING in 2010 Robert A. Halvorsen, MD, FACR MCV Hospitals / VCU Medical Center Richmond, Virginia I do not have any relevant financial relationships with any commercial interests COLON
MS (General Surgery) Title (Plan of Thesis) (Session )
 S.No. 1. Outcome analysis of laparoscopic ventral hernia repair post mesh fixation : An observational study 2. A Clinico-Radiological study of Post-operative port site complications after elective laparoscopic
S.No. 1. Outcome analysis of laparoscopic ventral hernia repair post mesh fixation : An observational study 2. A Clinico-Radiological study of Post-operative port site complications after elective laparoscopic
Diagnostic Laparoscopy patient information from your surgeon & SAGES
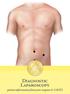 Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
X-Plain Pancreatic Cancer Reference Summary
 X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Different Types of Cancer
 Different Types of Cancer Cancer can originate almost anywhere in the body. Sarcomas (connective tissue) Ø arise from cells found in the supporting tissues of the body such as bone, cartilage, fat, connective
Different Types of Cancer Cancer can originate almost anywhere in the body. Sarcomas (connective tissue) Ø arise from cells found in the supporting tissues of the body such as bone, cartilage, fat, connective
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: SURGICAL ONCOLOGY 5-May-2013 DEVELOPED BY: Bruce
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: SURGICAL ONCOLOGY 5-May-2013 DEVELOPED BY: Bruce
A schematic of the rectal probe in contact with the prostate is show in this diagram.
 Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
(WG Whitfield Growden, MD; DR Diane Redington, CRNP)
 2795 Estates Drive Park City, UT 84060 TRANSCRIPT FOR VIDEO #4: D IAGNOSIS AND TREATMENT OF GYN CARCINOSARCOMA WITH DR. WHITFIELD GROWDEN Interview, Massachusetts General Hospital January 5, 2017 Produced
2795 Estates Drive Park City, UT 84060 TRANSCRIPT FOR VIDEO #4: D IAGNOSIS AND TREATMENT OF GYN CARCINOSARCOMA WITH DR. WHITFIELD GROWDEN Interview, Massachusetts General Hospital January 5, 2017 Produced
Evaluation of the Axilla Post Z-0011 Trial New Paradigm
 Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Oncology 101. Cancer Basics
 Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Surgical management and neoadjuvant chemotherapy for stage III-IV ovarian cancer
 Ovarian cancer Surgical management and neoadjuvant chemotherapy for stage III-IV ovarian cancer JM. Classe, R. Rouzier, O.Glehen, P.Meeus, L.Gladieff, JM. Bereder, F Lécuru Suitable candidates for neo-adjuvant
Ovarian cancer Surgical management and neoadjuvant chemotherapy for stage III-IV ovarian cancer JM. Classe, R. Rouzier, O.Glehen, P.Meeus, L.Gladieff, JM. Bereder, F Lécuru Suitable candidates for neo-adjuvant
Clinical indications for positron emission tomography
 Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Laparoscopic Resection Of Colon & Rectal Cancers. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Locally Advanced Colon Cancer. Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery
 Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
11/21/13 CEA: 1.7 WNL
 Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Patient Presentation. 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201
 Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
X-Plain Ovarian Cancer Reference Summary
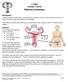 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
Breast Cancer. What is breast cancer?
 Scan for mobile link. Breast Cancer Breast cancer is a malignant tumor in or around breast tissue. It usually begins as a lump or calcium deposit that develops from abnormal cell growth. Most breast lumps
Scan for mobile link. Breast Cancer Breast cancer is a malignant tumor in or around breast tissue. It usually begins as a lump or calcium deposit that develops from abnormal cell growth. Most breast lumps
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Upper Tract Urothelial Carcinomas (UTUCs)
 Upper Tract Urothelial Carcinomas (UTUCs) Part II: UTUC Treatment Options November 14, 2017 Moderated by: Presented by: Gary D. Steinberg, MD University of Chicago Medical Center Ahmad Shabsigh, MD Ohio
Upper Tract Urothelial Carcinomas (UTUCs) Part II: UTUC Treatment Options November 14, 2017 Moderated by: Presented by: Gary D. Steinberg, MD University of Chicago Medical Center Ahmad Shabsigh, MD Ohio
Metastatic mechanism of spermatic cord tumor from stomach cancer
 Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
What you need to know about Radiation Therapy for Colorectal Cancer
 What you need to know about Radiation Therapy for Colorectal Cancer Questions and Answers CR Lund MSc MD FRCPC Radiation Oncologist Clinical Assistant Professor Overview I. Description of Radiation II.
What you need to know about Radiation Therapy for Colorectal Cancer Questions and Answers CR Lund MSc MD FRCPC Radiation Oncologist Clinical Assistant Professor Overview I. Description of Radiation II.
L impatto dell imaging sulla definizione della strategia terapeutica
 GISCoR L impatto dell imaging sulla definizione della strategia terapeutica M. Galeandro U.C. Radioterapia Oncologica ASMN-IRCCS Reggio Emilia 14 Novembre 2014 Rectal Cancer TNM AJCC-7 th edition 2010
GISCoR L impatto dell imaging sulla definizione della strategia terapeutica M. Galeandro U.C. Radioterapia Oncologica ASMN-IRCCS Reggio Emilia 14 Novembre 2014 Rectal Cancer TNM AJCC-7 th edition 2010
Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery
 Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery Goal The goal of the Breast Surgery rotation is to develop the knowledge, skills and attitudes necessary to evaluate,
Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery Goal The goal of the Breast Surgery rotation is to develop the knowledge, skills and attitudes necessary to evaluate,
What s New for 8 th Edition
 What s New for 8 th Edition KCR 2018 SPRING TRAINING Overview What s New New Chapters for 8 th Editions Chapters That Split in 8 th Edition Merged 8 th Edition Chapters Blanks vs Xs How to Navigate Through
What s New for 8 th Edition KCR 2018 SPRING TRAINING Overview What s New New Chapters for 8 th Editions Chapters That Split in 8 th Edition Merged 8 th Edition Chapters Blanks vs Xs How to Navigate Through
Decision making in surgical oncology- when to cut big, when to cut small
 Decision making in surgical oncology- when to cut big, when to cut small Simon T. Kudnig, BVSc, MVS, MS, FANZCVSc, Dipl. ACVS ACVS Founding Fellow in Surgical Oncology Animal Referral Hospital, Melbourne,
Decision making in surgical oncology- when to cut big, when to cut small Simon T. Kudnig, BVSc, MVS, MS, FANZCVSc, Dipl. ACVS ACVS Founding Fellow in Surgical Oncology Animal Referral Hospital, Melbourne,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
Disclosure. Acknowledgement. What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Rectal cancer imaging. None
 What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Pre-operative assessment of patients for cytoreduction and HIPEC
 Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Epithelial Ovarian Cancer
 Epithelial Ovarian Cancer GYNE/ONC Practice Guideline Dr. Alex Hammond Dr. Ian Kerr Dr. Akira Sugimoto Dr. Stephen Welch Kay Faroni Christine Gawlik Kerri Thornton Approval Date: This guideline is a statement
Epithelial Ovarian Cancer GYNE/ONC Practice Guideline Dr. Alex Hammond Dr. Ian Kerr Dr. Akira Sugimoto Dr. Stephen Welch Kay Faroni Christine Gawlik Kerri Thornton Approval Date: This guideline is a statement
Cancer , The Patient Education Institute, Inc. ocf80101 Last reviewed: 06/08/2016 1
 Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
COLON AND RECTAL CANCER
 COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Q: How do you clinically code the N if the nodes are stated to be positive on mammogram/us or other imaging? No biopsy of nodes was done.
 Q&A Breast Webinar Q: One of my investigators is interested in knowing when Oncotype DX data collection was implemented. That data is collected in SSFs 22 and 23. I remember that the SSFs for breast were
Q&A Breast Webinar Q: One of my investigators is interested in knowing when Oncotype DX data collection was implemented. That data is collected in SSFs 22 and 23. I remember that the SSFs for breast were
Workup of a Solid Liver Lesion
 Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
Liver Tumors. Prof. Dr. Ahmed El - Samongy
 Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Colon Cancer Surgery
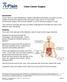 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Introduction. Growths in the prostate can be benign (not cancer) or malignant (cancer).
 This information was taken from urologyhealth.org. Feel free to explore their website to learn more. Another trusted website with good information is the national comprehensive cancer network (nccn.org).
This information was taken from urologyhealth.org. Feel free to explore their website to learn more. Another trusted website with good information is the national comprehensive cancer network (nccn.org).
Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer
 Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer PD Dr. med. Michel Adamina, MSc Department of Surgery Agenda Prerequisite for successful CRS HIPEC Planned
Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer PD Dr. med. Michel Adamina, MSc Department of Surgery Agenda Prerequisite for successful CRS HIPEC Planned
Please complete prior to the webinar. HOSPITAL REGISTRY WEBINAR FEMALE REPRODUCTIVE SYSTEM EXERCISES CASE 1: FEMALE REPRODUCTIVE
 Please complete prior to the webinar. HOSPITAL REGISTRY WEBINAR FEMALE REPRODUCTIVE SYSTEM EXERCISES PHYSICAL EXAMINATION CASE 1: FEMALE REPRODUCTIVE 3/5 Patient presents through the emergency room with
Please complete prior to the webinar. HOSPITAL REGISTRY WEBINAR FEMALE REPRODUCTIVE SYSTEM EXERCISES PHYSICAL EXAMINATION CASE 1: FEMALE REPRODUCTIVE 3/5 Patient presents through the emergency room with
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY
 DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation. Basics. What is Percutaneous Ablation? Where are your kidneys?
 Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Cancer Cases Treated and Results
 Cancer Cases Treated and Results Below are some of the cases, from more than 30 cases we have treated so far with good results. When reading the PET/CT scans, the picture on the left is before treatment,
Cancer Cases Treated and Results Below are some of the cases, from more than 30 cases we have treated so far with good results. When reading the PET/CT scans, the picture on the left is before treatment,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Breast Cancer. Excess Estrogen Exposure. Alcohol use + Pytoestrogens? Abortion. Infertility treatment?
 Breast Cancer Breast Cancer Excess Estrogen Exposure Nulliparity or late pregnancy + Early menarche + Late menopause + Cystic ovarian disease + External estrogens exposure + Breast Cancer Excess Estrogen
Breast Cancer Breast Cancer Excess Estrogen Exposure Nulliparity or late pregnancy + Early menarche + Late menopause + Cystic ovarian disease + External estrogens exposure + Breast Cancer Excess Estrogen
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
CT PET SCANNING for GIT Malignancies A clinician s perspective
 CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
Alison Douglass Gillian Lieberman, MD. November. Colon Cancer. Alison Douglass, Harvard Medical School Year III Gillian Lieberman, MD
 November Colon Cancer Alison Douglass, Harvard Medical School Year III Our Patient Mr. K. is a 67 year old man with no prior medical problems other than hemorrhoids which have caused occasional rectal
November Colon Cancer Alison Douglass, Harvard Medical School Year III Our Patient Mr. K. is a 67 year old man with no prior medical problems other than hemorrhoids which have caused occasional rectal
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital
 Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Low-grade appendiceal mucinous neoplasm (LAMN) High-grade appendiceal mucinous neoplasm (HAMN) Adenocarcinoma
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Low-grade appendiceal mucinous neoplasm (LAMN) High-grade appendiceal mucinous neoplasm (HAMN) Adenocarcinoma
DEPARTMENT OF ONCOLOGY ELECTIVE
 DEPARTMENT OF ONCOLOGY ELECTIVE 2015-2016 www.uwo.ca/oncology Oncology Elective Program Administrator: Ms. Kimberly Trudgeon Room A4-901C (Admin) LHSC London Regional Cancer Centre (Victoria Campus) Phone:
DEPARTMENT OF ONCOLOGY ELECTIVE 2015-2016 www.uwo.ca/oncology Oncology Elective Program Administrator: Ms. Kimberly Trudgeon Room A4-901C (Admin) LHSC London Regional Cancer Centre (Victoria Campus) Phone:
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Ines Buccimazza 16 TH UP CONTROVERSIES AND PROBLEMS IN SURGERY SYMPOSIUM
 BILATERAL MASTECTOMY IS NOT ROUTINELY JUSTIFIED IN PATIENTS WITH BILATERAL AXILLARY LYMPHADENOPATHY AND ONLY ONE DETECTABLE PRIMARY BREAST CANCER LESION SURGERY SYMPOSIUM Ines Buccimazza Breast Unit Department
BILATERAL MASTECTOMY IS NOT ROUTINELY JUSTIFIED IN PATIENTS WITH BILATERAL AXILLARY LYMPHADENOPATHY AND ONLY ONE DETECTABLE PRIMARY BREAST CANCER LESION SURGERY SYMPOSIUM Ines Buccimazza Breast Unit Department
Requirements for Abstracted Text
 Slide 1 Requirements for Abstracted Text Principles of Abstracting Lesson 3: Purpose of Text Slide 2 Available Text Fields Place of Diagnosis Immunotherapy Chemotherapy Hormone Therapy Other Therapy Radiation
Slide 1 Requirements for Abstracted Text Principles of Abstracting Lesson 3: Purpose of Text Slide 2 Available Text Fields Place of Diagnosis Immunotherapy Chemotherapy Hormone Therapy Other Therapy Radiation
What Is an Endoscopic Ultrasound (EUS)?
 ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
Cervical cancer presentation
 Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
COLON AND RECTAL CANCER
 No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
