Substantial evidence has accumulated in support of the hypothesis that elevated cholesterol
|
|
|
- Rosa Malone
- 5 years ago
- Views:
Transcription
1 NEUROLOGICAL REVIEW Cholesterol Level and Statin Use in Alzheimer Disease II. Review of Human Trials and Recommendations Nina E. Shepardson, MS; Ganesh M. Shankar, MD, PhD; Dennis J. Selkoe, MD Substantial evidence has accumulated in support of the hypothesis that elevated cholesterol levels increase the risk of Alzheimer disease (AD). As a result, much work has investigated the potential use of lipid-lowering agents, particularly, as preventive or therapeutic agents for AD. Although epidemiology and preclinical statin research (described in part I of this review) have generally supported an adverse role of high cholesterol levels regarding AD, human studies of (reviewed herein) show highly variable outcomes, making it difficult to draw firm conclusions. We identify several confounding factors among the human studies, including differing blood-brain barrier permeabilities among, the stage in AD at which were administered, and the drugs pleiotropic metabolic effects, all of which contribute to the substantial variability observed to date. We recommend that future human studies of this important therapeutic topic (1) take the blood-brain barrier permeabilities of into account when analyzing results, (2) include specific analyses of the effects on low- and highdensity lipoprotein cholesterol, and, most important, (3) conduct statin treatment trials solely in patients with mild AD, who have the best chance for disease modification. Arch Neurol. 2011;68(11): Author Affiliations: Center for Neurologic Diseases, Department of Neurology, Brigham and Women s Hospital and Harvard Medical School (Ms Shepardson and Drs Shankar and Selkoe), and Department of Neurological Surgery, Massachusetts General Hospital (Dr Shankar), Boston, Massachusetts. In part I of this review, 1 we examined the epidemiological and neuropathological literature relevant to the relationship between cholesterol levels and Alzheimer disease (AD) risk and preclinical studies of lipid-lowering agents (LLAs) as potential therapeutic or preventive agents. In this second segment, we appraise the human studies of this topic and find substantial variability in outcomes. We then address whether the complex and inconsistent trial results to date may be explained in part by differential abilities of to cross the blood-brain barrier (BBB) and several other confounding factors. Our review reveals that the principal basis for reported differences in the effects of LLAs across studies is the highly variable relationship between the initiation of statin therapy and the time of onset and the severity of AD. These and other findings herein lead us to recommend a set of specific criteria for conducting muchneeded clinical trials of the potentially important effects of cholesterol level regulation on AD incidence and progression. STUDY SELECTION We performed an unbiased search of the PubMed database for relevant studies in the English language, without regard to publication date. Additional studies were identified by citations in the resultant studies and also by the recommendation of the coauthors or consultants (identified in the Acknowledgments section). We included all articles that provided well-controlled studies and clearly interpretable conclusions about this topic. Studies of the effects of in human subjects were required to include at least 50 persons, and human studies examining LLAs were required to specify the drugs being investigated. 1385
2 OBSERVATIONAL STUDIES A number of observational studies in human subjects bolster the hypothesis that may be able to mitigate the course of AD or reduce the probability of it (Table 1). A case-control study by Jick and colleagues 5 found that people older than 50 years who were taking had a lower risk of dementia. An examination of patients older than 60 years demonstrated that patients taking lovastatin and/or pravastatin sodium had a lower AD risk compared with the general population or patients taking other medications for hypertension or heart disease. 9 In a study of postmenopausal women younger than 80 years with heart disease, subjects taking had better scores on the modified Mini-Mental State Examination and were less likely to be cognitively impaired. 11 Wolozin and colleagues 10 found that simvastatin treatment significantly reduced the risk of dementia and Parkinson disease. A study of elderly Mexican Americans reported that statin treatment was associated with a reduced risk of dementia and cognitive impairment without frank dementia. 3 Similarly, participants in the Rotterdam epidemiological study were less likely to develop AD if they were taking, an effect that was not dependent on the apolipoprotein E (ApoE) genotype. 4 Other studies have examined the effects of cholesterollowering treatment on subjects who had already been given a diagnosis of AD. A neuropathological assessment by Li et al 6 concluded that, although statin users did not have lower scores on the Consortium to Establish a Registry for Alzheimer s Disease (CERAD) instrument (a quantitative scale of amyloid plaque pathological features) than nonusers, they had lower Braak stages (a quantitative scale of neurofibrillary tangle and neuritic pathological features). Furthermore, study subjects using were less likely to have typical AD-type neuropathology, which the authors defined as abraakstageofatleastiv(maximumscore, VI) andacerad score of at least moderate (maximum score, severe). Not all observational studies conclude that are beneficial in the setting of AD (Table 1). When a large cohort (4895 for prevalent dementia and 3308 for incident dementia) of elderly people was surveyed for overall dementia or AD and the use of (an aggregate of lovastatin, simvastatin, cerivastatin sodium, atorvastatin calcium, pravastatin, and fluvastatin sodium) in 1995 to 1997 and again in 1998 to 2000, statin use at the initial visit and at follow-up visits did not correlate with the risk of any dementia or AD during the period between the 2 visits, although statin use was less common among those who already had dementia at the initial visit. 12 Another study found that statin treatment of patients 65 years or older did not affect their risk of AD or other forms of dementia, and this result did not change when more lipophilic (lovastatin, simvastatin, or cerivastatin) and less lipophilic (atorvastatin, pravastatin, or fluvastatin) drugs were separately. 8 Wolozin et al, 10 who showed a protective effect with simvastatin, failed to find such an effect with lovastatin. Arvanitakis et al 2 reported that, although statin users were less likely to be demented at the time of death, statin use did not affect AD risk or cognitive ability. RANDOMIZED CONTROLLED TRIALS As with the human observational studies described in the preceding subsections, the results of randomized controlled trials in AD patients have been contradictory (Table 2). Administering a controlled-release form of lovastatin to nondemented subjects has been shown to decrease serum -amyloid (A ) levels in a dose-dependent manner 14 (Figure 1).Sparksetal 17 observeddifferencesbetweenatorvastatin users and nonusers on the cognitive subscale of the Alzheimer Disease Assessment Scale at 6 months and on the Geriatric Depression Scale at 12 months. However, large double-blind randomized controlled trials of pravastatin 16 and simvastatin 15 with mean follow-up ranging from 3.2 to 5.0 years were unable to demonstrate a protective effect, and the study by Sparks et al 17 did not find an effect on the Mini- Mental State Examination, Neuropsychiatric Inventory, or Alzheimer Disease Cooperative Study Activities of Daily Living Scale. Most recently, a randomized controlled trial found that cognitive decline in patients who already had mild to moderate AD was unaltered by a 72-week administration of atorvastatin. 13 Overall, we interpret these various studies to indicate that have not yet been shown to influence the course of AD in controlled trials. EFFECTS OF NONSTATIN LLAs Some observational studies have examined the effects of nonstatin LLA compounds (Table 1). Yaffe et al 11 examined a combination of niacin, cholestyramine resin, and other nonspecified compounds and did not find these to be effective at preventing cognitive impairment in postmenopausal women without dementia. Fibrates (a group of amphipathic carboxylic acids used for hypercholesterolemia treatment) were also reported to be ineffective for dementia or AD protection 4,5,8,12 (although Masse et al 7 found them to be efficacious), as were cholestyramine and nicotinic acid 12 and a combination of niacin, bile acid sequestrants, and probucol. 8 DIFFERING BBB PERMEABILITIES AMONG THE STATINS The substantial variability in outcomes of the diverse human studies reviewed in the preceding paragraphs makes it difficult to ascertain whether could have a beneficial role in preventing or treating AD (Tables 1 and 2). One possible reason for the inconsistency is that, to potentially affect the course of AD, any prospective treatment must be able to pass through the BBB and enter the brain. In this respect, all are not created equal; some have a much greater capacity to cross the BBB than others, but this is not always commented on by authors in interpreting their studies. Differences in BBB permeability among the various (Table 3) were recognized while investigating why some, when prescribed as a treatment for hypercholesterolemia, had a higher incidence of neurological adverse effects than others. Lovastatin, but not fluvastatin, efficiently crossed a monolayer of bovine brain microvessel endothelial cells (a model for the BBB) and was detected in the brain extracts of rats receiving the compound. 18 In 1386
3 Table 1. Human Observational Studies of the Efficacy of LLAs for the Treatment and Prevention of AD and Dementia Source Arvanitakis et al, Cramer et al, Haag et al, Jick et al, Li et al, Masse et al, Rea et al, Wolozin et al Wolozin et al Yaffe et al Zandi et al, Statins SIM, LOV, ATOR, PRA, and FLU together and in more- and less-lipophilic groups ATOR, CER, FLU, LOV, PRA, ROS, and SIM together LLAs Used ATOR, CER, FLU, PRA, ROS, and SIM together and in lipophilic and hydrophilic groups; SIM and PRA also separately ATOR, CER, FLU, PRA, and SIM together SIM, LOV, PRA, and ATOR together Unspecified LOV, SIM, CER, ATOR, PRA, and FLU together and in more- and less-lipophilic groups LOV, PRA, LOV PRA, and SIM separately ATOR, LOV, and SIM separately SIM, ATOR, LOV, PRA, and FLU together LOV, SIM, CER, ATOR, PRA, and FLU together None Others Study Size a Disease Severity Length of Follow-up 929 Clinical evaluations of living patients; 262 postmortem neuropathological examinations Incident 12 y Risk of Outcome Measures AD; composite of cognitive test scores; neuropathology None 1021 Subjects Incident 5 y Risk of dementia or cognitive impairment without dementia Fibrates, bile acid binding resins, and nicotinic acid Fibrates, gemfibrozil, colestipol hydrochloride, cholestyramine, acipimox, niacin, and nicotinic acid 6992 Subjects Incident Varied; mean, 9.2 y Risk of AD 1364 Subjects Incident 6 y Risk of dementia None 110 Subjects Incident 12 y Incidence of dementia; Braak stages; CERAD scores Fibrates and unspecified other LLAs Fibrates; niacin, bile acid sequestrants, and probucol together Other drugs for heart disease treatment 342 Subjects Mild to moderate Varied; mean, 34.8 mo 2798 Subjects Incident Varied; median, 5 y Subjects Unspecified NA (retrospective) None Subjects Incident NA (retrospective) Cholestyramine resin and niacin Fibrates, cholestyramine, and nicotinic acid Rate of decline in MMSE scores Risk of dementia, AD, and/or vascular dementia Prevalence of AD Risk of dementia Effectiveness Yes for amyloid pathological changes; no for risk of AD, cognitive ability, and global AD pathological changes Yes Yes for all, lipophilic, and hydrophilic ; no for other LLAs Yes for ; no for other LLAs No for incidence of dementia and CERAD scores; yes for Braak stages Yes for all LLAs together and fibrates; no for and other LLAs No Yes for LOV, PRA, and LOV PRA; no for others Yes for LOV; no for SIM and ATOR 1037 Subjects Incident 4 y MMSE-m scores Yes for ; no for other LLAs 4895 (Unspecified severity); 3308 (incident) Unspecified, incident 3 y Likelihood of preexisting dementia or AD; risk of dementia or AD Yes for for preexisting dementia or AD); no for for risk of dementia or AD; no for other LLAs BBB Permeability Yes for LOV and SIM; no for PRA; mixed for LOV PRA Yes for LOV and SIM; disputed for ATOR Abbreviations: AD, Alzheimer disease; ATOR, atorvastatin calcium; BBB, blood-brain barrier; CER, cerivastatin sodium; CERAD, Consortium to Establish a Registry for Alzheimer Disease; FLU, fluvastatin sodium; LLAs, agents to lower lipid levels; LOV, lovastatin; NA, not available; PRA, pravastatin sodium; ROS, rosuvastatin calcium; SIM, simvastatin; MMSE-m, modified Mini-Mental State Examination; a Cohort studies and case-control studies are included. Study size represents the number of participants who completed the study, unless otherwise noted. 1387
4 Table 2. Randomized Controlled Trials of the Efficacy of LLAs for the Treatment and Prevention of AD and Dementia Source LLA Used Study Size a Disease Severity Length of Follow-up Outcome Measures Effectiveness Feldman et al, ATOR 449 b Mild to moderate 80 wk ADAS-cog, CGIC scores No Disputed Friedhoff et al, LOV 94 c None d 12 wk Serum A levels Yes Yes SIM e Incident Varied; mean, 5 y TICS-m scores No Yes Heart Protection Study Collaborative Group, Shepherd et al, PRA 4351 f Incident Varied; mean, 3.2 y MMSE, picture-word learning, Stroop color word, letter digit coding, Barthel, and instrumental activities of daily living tests Sparks et al, ATOR 46 g Mild to moderate 1 y ADAS-cog, CGIC, MMSE, GDS, NPI, and ADCS-ADL tests No Yes for ADAS-cog at 6 mo and GDS at 12 mo; no for others BBB Permeability No Disputed Abbreviations: A, -amyloid; AD, Alzheimer disease; ADAS-cog, cognitive subscale of Alzheimer Disease Assessment Scale; ADCS-ADL, Alzheimer Disease Cooperative Study Activities of Daily Living; CGIC, Clinical Global Impression of Change; GDS, Geriatric Depression Scale; NPI, Neuropsychiatric Inventory; TICS-m, modified Telephone Interview for Cognitive Status. For other abbreviations, see Table 1. a Represents the number of participants who completed the study, unless otherwise noted. b Represents the number of participants who completed the study. The modified intent-to-treat value was 614. c Represents the number of participants for whom the authors were able to obtain usable serum samples. One hundred sixty participants completed the study. d Listed as none instead of incident because the authors did not evaluate incidence of dementia. e Represents the number of participants who completed the study. The intent-to-treat value was f Represents the number of participants who completed the study. The authors intent-to-treat value was g Represents the number of participants who completed the study. The number of participants considered to have evaluable data by the authors was P =.02 P =.03 Table 3. Blood-Brain Barrier Permeability of Major Statins Change in Serum Aβ Levels, % Placebo (n = 15) 10 (n = 20) 20 (n = 19) 40 (n = 20) 60 (n = 20) Dose of Controlled-Release Lovastatin, mg Name Permeability Proprietary Names Atorvastatin calcium Disputed Lipitor, Torvast, Caduet (with amlodipine besylate) Cerivastatin sodium Disputed Lipobay, Baycol (both withdrawn) Fluvastatin sodium No Lescol, Lescol XL Lovastatin Yes Mevacor, Altocor, Altoprev, Advicor (with niacin) Pravastatin sodium No Pravachol, Selektine, Lipostat Rosuvastatin No Crestor calcium Simvastatin Yes Zocor, Lipex, Vytorin (with ezetimible), Simcor (with niacin) Figure 1. Effect of controlled-release lovastatin on serum -amyloid (A ) levels. Administering lovastatin to nondemented participants leads to a decrease in serum A levels. Open bars represent mean (SEM); solid bars, median. Reproduced from Friedhoff et al 14 with permission from Cambridge Journals. another study, 19 lovastatin and simvastatin had much higher BBB permeability coefficients than did pravastatin (Figure 2). Like pravastatin, rosuvastatin calcium has a limited ability to cross the BBB. 20 The evidence on atorvastatin and cerivastatin is mixed; some researchers reported that they cross the BBB effectively (ie, Kandiah and Feldman 21 for atorvastatin and Knopp 22 for cerivastatin), whereas others did not (ie, Knopp 22 for atorvastatin and Kandiah and Feldman 21 for cerivastatin). What is responsible for this disparity in BBB permeability among the? One key determinant is lipophilicity. Lovastatin and simvastatin are much more lipophilic than pravastatin, 23 whereas fluvastatin falls somewhere in between. 24 Also, fluvastatin is negatively charged and so would be repelled by the anionic microdomains in the plasma membranes of BBB endothelial cells. 18 Different transport mechanisms may also play a role; simvastatin and lovastatin appear to cross the BBB via passive diffusion, whereas pravastatin relies on an active transport system, for which it may have a low affinity. 25 This variation in the biochemical properties of provides an important clue as to why some studies may have shown a beneficial effect of statin treatment on dementia and AD whereas others have not. However, because several investigators 2,4,8 found that the lipophilicity of did not affect their usefulness as preventive agents for AD, other factors must also be taken into account. Among these are the methodology and design of statin studies and the pleiotropic effects of. 1388
5 METHODOLOGICAL AND DESIGN ISSUES The data on the variability of BBB penetration across (Table 3) provide a potentially important explanation for the inconsistency in outcome. Some studies focus on a statin that does not cross the BBB well, or they aggregate data from penetrant and nonpenetrant drugs (Tables 1 and 2). With substantial variation in BBB permeability among, it becomes difficult to reconcile the conflicting findings in the literature. Also, some studies base their conclusions for as a whole on the analysis of a single drug. Various methodological issues are also likely to contribute to the inconsistency. In their review, Kandiah and Feldman 21 identified as particularly important (1) the distinction between preexisting and incident AD, (2) the time of statin use vs the time of cognitive assessment, (3) the dose of the statin, (4) the duration of statin use, (5) the duration of observation, (6) the conflation of AD with other forms of dementia (a major concern), (7) patient adherence to the statin prescription regimen, and (8) whether vascular risk factors were controlled. In accord with that review, 21 the authors of primary studies have often discussed such methodological concerns relevant to the evaluation of their experimental results. Solomon et al, 26 for example, discussed survival bias as one of the difficulties in studying the relationship between cholesterol levels and AD. Statin dosage and brain penetration were alluded to by Meske et al 27 as potential confounding factors in various epidemiological studies; that is, negative results may be due to not reaching a therapeutic concentration in the brain. The importance of dosage was stressed in an elegant study conducted by Ostrowski et al, 28 which found, that although simvastatin and lovastatin can affect Rho and Rab family proteins, applying a physiologically relevant concentration of the statin would influence some members of these protein families but not others. Those authors postulate that Rab- and Rho-dependent effects overlap at high statin doses, whereas Rho-dependent effects dominate at lower doses. Indication bias (in which a drug is prescribed to treat a condition that is associated with the variable of interest) and cessation bias (in which some of the observed protective effects of a drug may be due to patients stopping the drug therapy after being diagnosed as having a condition) have also been suggested as problems that may occur in statin studies. 29 Another potential pitfall is the question of whether those who are in generally good health are more likely to be prescribed, resulting in a misleading apparent effect of these drugs on disease prevention or treatment. This was addressed by Rockwood et al, 29 who found that there was no association between self-reported health and LLA use. On the contrary, there was an association between LLA use and other vascular risk factors, indicating that LLAs are not more likely to be used by healthier people. The period during which a study was conducted may be a particularly important factor. After finding protective effects for lovastatin and pravastatin but not simvastatin, Wolozin et al 9 pointed out that simvastatin was (at the time) a relatively new drug, so prescribing patterns may have been different than for the other 2 compounds studied. In another study, Wolozin and colleagues 10 chose not to assess fluvastatin because the number of people taking it increased drastically during the course of the study, which they believed introduced a confounding variable. The time in the patient s life at which measurements are taken may also be critical. Yaffe et al 11 mentioned that dementia might alter a patient s diet or metabolism, thus having an effect on lipid levels, and part I of this article 1 emphasized that studies conducted in middle vs old age reach different conclusions about the relationship between cholesterol levels and dementia risk. Permeability, µl/cm Lovastatin Lovastatin acid Simvastatin Simvastatin acid Pravastatin Sucrose Time, min Figure 2. Permeability of different across the blood-brain barrier. Reproduced from Saheki et al 19 with permission from Springer Science Business Media. The statistical power of a study is a major issue to consider. Li et al 6 expressed concern that the crude, semiquantitative CERAD scale may not have very high power to detect relationships between statin use and AD pathological characteristic. Arvanitakis et al 2 indicated that their study was limited in statistical power, which could account for the observed lack of correlation between statin use and overall AD brain pathological features or tangle immunoreactivity. Difficulties can arise when only a small percentage of even a large initial cohort develop AD during the course of the study, making it problematic to detect the potential effects of therapeutic interventions on outcome. Another confounding factor is the fact that an AD patient s ApoE genotype may affect not only AD risk but also the effectiveness of as an AD prevention or treatment. In one study, people with the ApoE4 allele saw less benefit (in terms of cholesterol levels) from statin treatment than those with the E2 or E3 alleles. 30 Although a detailed discussion of the potential effects of ApoE is not within the purpose of this review, some trials of have taken ApoE genotype into account, 4 and the mechanism by which the ApoE genotype might influence AD risk continues to be the subject of intense research (eg, Morris et al 31 and Belinson et al 32 ). PLEIOTROPIC EFFECTS OF STATINS Statins have other effects on physiology and metabolism besides lowering cholesterol levels, some of which could independently affect AD risk. For example, can alter the expression of genes related to cell growth, signaling, trafficking, and apoptosis. 33 Here, too, we see differences among the. In the study by Johnson- Anuna et al, genes were affected by simvastatin, 26 by lovastatin, and only 21 by pravastatin. Rosuvastatin, atorvastatin, and simvastatin have all been found to increase the expression and activity of endothelial nitric oxide synthase in mice. 34 Furthermore, treatment of normocholesterolemic, spontaneously hypertensive rats with a physiologically relevant dose of atorvastatin mediated a host of beneficial effects. It lowered blood pressure, enhanced carbachol-induced vasodilation, inhibited angiotensin II induced vasoconstriction, decreased the production of superoxide in blood vessel walls, lowered messenger RNA and protein expression of angiotensin type 1 receptor, and reduced messenger 1389
6 A B C PM FL-APP APPsβ C99 Aβ APPsα C83 Reduced trafficking Normal trafficking Endosome β-secretase γ-secretase α-secretase TGN Golgi ER Figure 3. Cholesterol- vs isoprenoid-dependent effects of statin treatment in cells. A, Normal cholesterol and isoprenoid levels with normal amyloid precursor protein (APP) export and endocytosis. B, When isoprenoid (but not cholesterol) levels are reduced by treatment with a statin in the presence of mevalonate, APP export is reduced and -amyloid (A ) accumulates intracellularly. C, By contrast, when cholesterol levels are depleted by statin treatment in the absence of mevalonate, -secretase processing of APP is enhanced, which in turn leads to less A being secreted. ER indicates endoplasmic reticulum; FL, full-length; PM, plasma membrane; and TGN, trans-golgi network. Reproduced from Cole et al 36 with permission from the American Society for Biochemistry and Molecular Biology. RNA expression of the nicotinamide adenine dinucleotide phosphate oxidase subunit p22phox. 35 Although the mechanisms behind these effects are largely unknown, the authors speculated that they may involve downstream isoprenoids, some of which are important for posttranslational modification of other proteins. In any event, the broad spectrum of actions of some or most means that any effect they have on AD incidence or course (or on preclinical measures, such as degree of A pathological features) may not necessarily relate to their cholesterol level lowering effects per se. One potential effect of statin treatment deserves special mention. Inhibition of hydroxymethylglutaryl CoA reductase activity interferes with the isoprenylation of other proteins, impairing their functions and causing a wide variety of downstream effects. Isoprenylation is important in protein trafficking and signaling and in cytoskeletal structure. If are added to cells in the presence of mevalonate, cholesterol synthesis will still be blocked, but isoprenylation can continue unimpeded. This gives researchers a way to separately analyze the cholesterol- and isoprenoid-dependent effects of. Using this strategy, Cole et al 36 concluded that low isoprenoid levels inhibit the passage of amyloid precursor protein through the secretory pathway, leading various processing products to accumulate intracellularly. Low cholesterol levels, meanwhile, may inhibit receptor-mediated endocytosis of amyloid precursor protein. The authors hypothesized that the following 2 largely separate pools of A exist: an intracellular pool that is mainly affected by isoprenoids and a secreted pool that is mainly influenced by cholesterol (Figure 3). In summary, the diverse potential roles for cholesterol in aspects of AD pathogenesis have led to numerous studies evaluating LLAs such as for potential therapeutic effects. Based on all available studies, appear to hold greater promise than other classes of LLAs. However, individual differ in ways that could affect their efficacy with respect to AD. The conflation of with other LLAs, the disparities among in their respective BBB permeabilities, and the differences in biochemical effects among these drugs are all likely to contribute to the unfortunate variability in study outcomes observed to date. RECOMMENDATIONS FOR FUTURE RESEARCH Most of the laboratory studies discussed in part I of this review 1 converge on a model suggesting that increased cholesterol levels promote A formation and accumulation in the brain. However, the human epidemiological studies (also in part I) are difficult to bring together with similar conviction. Throughout this second part of our review, we have found reconciling the many human LLA studies difficult because of (1) the different biochemical properties of the and other LLAs used in the studies, (2) the myriad points of cholesterol level measurements (see part I) and 1390
7 statin administration (Tables 1 and 2), (3) the inconsistent use of biomarker and cognitive end points, and (4) the methodological challenges of observing complex human populations, especially regarding the conflation of AD with vascular dementia. Based on these observations, we can make several urgent recommendations for future studies investigating the potential link between statin use and AD risk or progression. First, the characteristics of the LLAs should be more explicitly defined (particularly their permeability across the BBB), and BBB-permeant compounds should be assessed nonpermeant ones. This step will help clarify whether BBB permeability governs how a statin modifies the incidence and progression of AD. Second, future cohort studies should focus on investigating the effects of cholesterol levels and statin use in the presymptomatic or very mild symptomatic stages of AD and their contribution to modifying the risk of frank AD, and they should assess low- and high-density lipoprotein cholesterol separately. We consider this point of evaluating in individuals with mild (or earlier) AD to be particularly salient. Because of the progressive nature of AD neuropathological changes, measurement and modulation of cholesterol levels in moderate or late stages of the disease, when significant neurological injury has accrued, may show little or no effect. Third, an agreed-upon set of biomarkers in serum and cerebrospinal fluid (particularly A 42, tau, and phospho-tau levels), brain imaging (including amyloid imaging by positron emission tomography, which has only recently become available), and cognitive measures (such as the cognitive subscale of the Alzheimer Disease Assessment Scale and, preferably, more sophisticated and specific tests of verbal and episodic memory) should be uniformly applied to future epidemiology studies and clinical trials. Fourth, given the complex spectrum of nonvascular dementias that includes mild cognitive impairment and AD, the common binary distinction between demented and nondemented individuals is insufficient. Available diagnostic modalities (including assays of cerebrospinal fluid A 42 and tau and amyloid imaging by positron emission tomography) should generally be sufficient to define the probable pathological basis of a dementia. Fifth, there are many complexities in this area of clinical research that could also be explored in well-controlled animal models to give the field a clearer picture of what occurs mechanistically in the brain when are administered. These issues include whether the concentration of typically administered to human patients is sufficient to interfere with isoprenylation and, importantly, to what extent the BBB is damaged in individuals with mild AD and how this might affect the penetration of cholesterol and into the brain. To evaluate more rigorously than heretofore the potential efficacy of for AD, we propose a prospective epidemiological cohort study designed and conducted by several experts coming together that begins with subject recruitment in late middle age and includes comprehensive assessment and follow-up using the biomarkers and clinical assessments we have listed in the previous paragraph. It is our hope that such research can untangle the complex factors discussed herein that have precluded a clear answer to the overarching question of whether, such widely prescribed and generally safe drugs in our society, represent viable therapeutic or preventive agents for the most common cause of progressive cognitive failure in older humans. Accepted for Publication: April 6, Correspondence: Dennis J. Selkoe, MD, Center for Neurologic Diseases, Department of Neurology, Brigham and Women s Hospital and Harvard Medical School, HIM Room 730, 77 Avenue Louis Pasteur, Boston, MA (dselkoe@rics.bwh.harvard.edu). Author Contributions: Dr Selkoe had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Shankar and Selkoe. Acquisition of data: Shepardson and Shankar. Analysis and interpretation of data: Shepardson, Shankar, and Selkoe. Drafting of the manuscript: Shepardson and Shankar. Critical revision of the manuscript for important intellectual content: Shepardson and Selkoe. Statistical analysis: Shankar. Obtained funding: Selkoe. Administrative, technical, and material support: Selkoe. Study supervision: Shankar and Selkoe. Financial Disclosure: Dr Selkoe is a founding scientist and consultant of Elan PLC. Funding/Support: This study was supported by grant AG06173 from the National Institutes of Health (Dr Selkoe). Role of the Sponsor: The funding organization had no role in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, or approval of the manuscript. Additional Contributions: Francine Grodstein, ScD, of the Harvard School of Public Health and Benjamin Wolozin, MD, PhD, of the Boston University School of Medicine provided insightful comments and suggestions on an earlier draft of this article and did not receive financial compensation for their contributions. REFERENCES 1. Shepardson NE, Shankar GM, Selkoe DJ. Cholesterol level and statin use in Alzheimer disease, I: review of epidemiological and preclinical studies. Arch Neurol. 2011;68(10): Arvanitakis Z, Schneider JA, Wilson RS, et al. Statins, incident Alzheimer disease, change in cognitive function, and neuropathology. Neurology. 2008;70 (19, pt 2): Cramer C, Haan MN, Galea S, Langa KM, Kalbfleisch JD. Use of and incidence of dementia and cognitive impairment without dementia in a cohort study. Neurology. 2008;71(5): Haag MD, Hofman A, Koudstaal PJ, Stricker BH, Breteler MM. Statins are associated with a reduced risk of Alzheimer disease regardless of lipophilicity: the Rotterdam Study. J Neurol Neurosurg Psychiatry. 2009;80(1): Jick H, Zornberg GL, Jick SS, Seshadri S, Drachman DA. Statins and the risk of dementia. Lancet. 2000;356(9242): Li G, Larson EB, Sonnen JA, et al. Statin therapy is associated with reduced neuropathologic changes of Alzheimer disease. Neurology. 2007;69(9): Masse I, Bordet R, Deplanque D, et al. Lipid lowering agents are associated with a slower cognitive decline in Alzheimer s disease. J Neurol Neurosurg Psychiatry. 2005;76(12): Rea TD, Breitner JC, Psaty BM, et al. Statin use and the risk of incident dementia: the Cardiovascular Health Study. Arch Neurol. 2005;62(7): Wolozin B, Kellman W, Ruosseau P, Celesia GG, Siegel G. Decreased prevalence of Alzheimer disease associated with 3-hydroxy-3-methyglutaryl coenzyme A reductase inhibitors. Arch Neurol. 2000;57(10): Wolozin B, Wang SW, Li NC, Lee A, Lee TA, Kazis LE. Simvastatin is associated 1391
8 with a reduced incidence of dementia and Parkinson s disease. BMC Med. July 19, 2007;5:20. doi: / Yaffe K, Barrett-Connor E, Lin F, Grady D. Serum lipoprotein levels, statin use, and cognitive function in older women. Arch Neurol. 2002;59(3): Zandi PP, Sparks DL, Khachaturian AS, et al; Cache County Study Investigators. Do reduce risk of incident dementia and Alzheimer disease? the Cache County Study. Arch Gen Psychiatry. 2005;62(2): Feldman HH, Doody RS, Kivipelto M, et al; LEADe Investigators. Randomized controlled trial of atorvastatin in mild to moderate Alzheimer disease: LEADe. Neurology. 2010;74(12): Friedhoff LT, Cullen EI, Geoghagen NSM, Buxbaum JD. Treatment with controlledrelease lovastatin decreases serum concentrations of human -amyloid (A ) peptide. Int J Neuropsychopharmacol. 2001;4(2): Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360(9326): Shepherd J, Blauw GJ, Murphy MB, et al; PROSPER Study Group; PROspective Study of Pravastatin in the Elderly at Risk. Pravastatin in elderly individuals at risk of vascular disease (PROSPER): a randomised controlled trial. Lancet. 2002; 360(9346): Sparks DL, Sabbagh MN, Connor DJ, et al. Atorvastatin for the treatment of mild to moderate Alzheimer disease: preliminary results. Arch Neurol. 2005;62(5): Guillot F, Misslin P, Lemaire M. Comparison of fluvastatin and lovastatin bloodbrain barrier transfer using in vitro and in vivo methods. J Cardiovasc Pharmacol. 1993;21(2): Saheki A, Terasaki T, Tamai I, Tsuji A. In vivo and in vitro blood-brain barrier transport of 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase inhibitors. Pharm Res. 1994;11(2): Nezasa KI, Higaki K, Matsumura T, et al. Liver-specific distribution of rosuvastatin in rats: comparison with pravastatin and simvastatin. Drug Metab Dispos. 2002;30(11): Kandiah N, Feldman HH. Therapeutic potential of in Alzheimer s disease. J Neurol Sci. 2009;283(1-2): Knopp RH. Drug treatment of lipid disorders. N Engl J Med. 1999;341(7): Serajuddin AT, Ranadive SA, Mahoney EM. Relative lipophilicities, solubilities, and structure-pharmacological considerations of 3-hydroxy-3-methylglutarylcoenzyme A (HMG-CoA) reductase inhibitors pravastatin, lovastatin, mevastatin, and simvastatin. J Pharm Sci. 1991;80(9): Hamelin BA, Turgeon J. Hydrophilicity/lipophilicity: relevance for the pharmacology and clinical effects of HMG-CoA reductase inhibitors. Trends Pharmacol Sci. 1998;19(1): Tsuji A, Saheki A, Tamai I, Terasaki T. Transport mechanism of 3-hydroxy-3- methylglutaryl coenzyme A reductase inhibitors at the blood-brain barrier. J Pharmacol Exp Ther. 1993;267(3): Solomon A, Kåreholt I, Ngandu T, et al. Serum cholesterol changes after midlife and late-life cognition: twenty-one-year follow-up study. Neurology. 2007;68 (10): Meske V, Albert F, Richter D, Schwarze J, Ohm TG. Blockade of HMG-CoA reductase activity causes changes in microtubule-stabilizing protein tau via suppression of geranylgeranylpyrophosphate formation: implications for Alzheimer s disease. Eur J Neurosci. 2003;17(1): Ostrowski SM, Wilkinson BL, Golde TE, Landreth G. Statins reduce amyloid- production through inhibition of protein isoprenylation. J Biol Chem. 2007; 282(37): Rockwood K, Kirkland S, Hogan DB, et al. Use of lipid-lowering agents, indication bias, and the risk of dementia in community-dwelling elderly people. Arch Neurol. 2002;59(2): Carmena R, Roederer G, Mailloux H, Lussier-Cacan S, Davignon J. The response to lovastatin treatment in patients with heterozygous familial hypercholesterolemia is modulated by apolipoprotein E polymorphism. Metabolism. 1993; 42(7): Morris JC, Roe CM, Xiong C, et al. APOE predicts amyloid- but not tau Alzheimer pathology in cognitively normal aging. Ann Neurol. 2010;67(1): Belinson H, Kariv-Inbal Z, Kayed R, Masliah E, Michaelson DM. Following activation of the amyloid cascade, apolipoprotein E4 drives the in vivo oligomerization of amyloid- resulting in neurodegeneration. J Alzheimers Dis. 2010;22 (3): Johnson-Anuna LN, Eckert GP, Keller JH, et al. Chronic administration of alters multiple gene expression patterns in mouse cerebral cortex. J Pharmacol Exp Ther. 2005;312(2): Laufs U, Gertz K, Dirnagl U, Böhm M, Nickenig G, Endres M. Rosuvastatin, a new HMG-CoA reductase inhibitor, upregulates endothelial nitric oxide synthase and protects from ischemic stroke in mice. Brain Res. 2002;942(1-2): Wassmann S, Laufs U, Bäumer AT, et al. HMG-CoA reductase inhibitors improve endothelial dysfunction in normocholesterolemic hypertension via reduced production of reactive oxygen species. Hypertension. 2001;37(6): Cole SL, Grudzien A, Manhart IO, Kelly BL, Oakley H, Vassar R. Statins cause intracellular accumulation of amyloid precursor protein, beta-secretase-cleaved fragments, and amyloid beta-peptide via an isoprenoid-dependent mechanism. J Biol Chem. 2005;280(19):
Statins and Cognition A Focus on Mechanisms
 Statins and Cognition A Focus on Mechanisms Note: Deleted copyrighted graphs/tables are described In red text and source references are provided Disclosures: SPARCL Steering Committee and past consultant
Statins and Cognition A Focus on Mechanisms Note: Deleted copyrighted graphs/tables are described In red text and source references are provided Disclosures: SPARCL Steering Committee and past consultant
Use of statins and incidence of dementia and cognitive impairment without dementia in a cohort study
 Use of statins and incidence of dementia and cognitive impairment without dementia in a cohort study Fn1 C. Cramer, PhD M.N. Haan, DrPH S. Galea, MD, DrPH K.M. Langa, MD, PhD J.D. Kalbfleisch, PhD Address
Use of statins and incidence of dementia and cognitive impairment without dementia in a cohort study Fn1 C. Cramer, PhD M.N. Haan, DrPH S. Galea, MD, DrPH K.M. Langa, MD, PhD J.D. Kalbfleisch, PhD Address
Association of statin use with risk of dementia: A meta-analysis of prospective cohort studies
 bs_bs_banner Geriatr Gerontol Int 2013; 13: 817 824 REVIEW ARTICLE Association of statin use with risk of dementia: A meta-analysis of prospective cohort studies Yu Song, 1 Hongwei Nie, 2 * Yong Xu, 1
bs_bs_banner Geriatr Gerontol Int 2013; 13: 817 824 REVIEW ARTICLE Association of statin use with risk of dementia: A meta-analysis of prospective cohort studies Yu Song, 1 Hongwei Nie, 2 * Yong Xu, 1
STATIN UTILIZATION MANAGEMENT CRITERIA
 STATIN UTILIZATION MANAGEMENT CRITERIA DRUG CLASS: HMG Co-A Reductase Inhibitors & Combinations Agents which require prior review: Advicor (niacin extended-release/lovastatin) Crestor (rosuvastatin)(5mg,10mg,
STATIN UTILIZATION MANAGEMENT CRITERIA DRUG CLASS: HMG Co-A Reductase Inhibitors & Combinations Agents which require prior review: Advicor (niacin extended-release/lovastatin) Crestor (rosuvastatin)(5mg,10mg,
ORIGINAL CONTRIBUTION. Atorvastatin for the Treatment of Mild to Moderate Alzheimer Disease
 ORIGINAL CONTRIBUTION Atorvastatin for the Treatment of Mild to Moderate Alzheimer Disease Preliminary Results D. Larry Sparks, PhD; Marwan N. Sabbagh, MD; Donald J. Connor, PhD, PhD; Jean Lopez, MSN,
ORIGINAL CONTRIBUTION Atorvastatin for the Treatment of Mild to Moderate Alzheimer Disease Preliminary Results D. Larry Sparks, PhD; Marwan N. Sabbagh, MD; Donald J. Connor, PhD, PhD; Jean Lopez, MSN,
During the last 2 decades, evidence has accumulated that a high cholesterol level may
 NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD Cholesterol Level and Statin Use in Alzheimer Disease I. Review of Epidemiological and Preclinical Studies Nina E. Shepardson, MS; Ganesh M. Shankar,
NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD Cholesterol Level and Statin Use in Alzheimer Disease I. Review of Epidemiological and Preclinical Studies Nina E. Shepardson, MS; Ganesh M. Shankar,
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Caduet) Reference Number: CP.CPA.237 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Caduet) Reference Number: CP.CPA.237 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy
CLINICAL TRIALS SECTION EDITOR: IRA SHOULSON, MD. Statin Use and the Risk of Incident Dementia
 CLINICAL TRIALS SECTION EDITOR: IRA SHOULSON, MD Statin Use and the Risk of Incident Dementia The Cardiovascular Health Study Thomas D. Rea, MD, MPH; John C. Breitner, MD; Bruce M. Psaty, MD, PhD; Annette
CLINICAL TRIALS SECTION EDITOR: IRA SHOULSON, MD Statin Use and the Risk of Incident Dementia The Cardiovascular Health Study Thomas D. Rea, MD, MPH; John C. Breitner, MD; Bruce M. Psaty, MD, PhD; Annette
How would you manage Ms. Gold
 How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
Corporate Medical Policy Genetic Testing for Alzheimer s Disease
 Corporate Medical Policy Genetic Testing for Alzheimer s Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alzheimers_disease 8/2010 10/2017 10/2018 10/2017
Corporate Medical Policy Genetic Testing for Alzheimer s Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alzheimers_disease 8/2010 10/2017 10/2018 10/2017
Association of statin use with cognitive decline in elderly African Americans
 Association of statin use with cognitive decline in elderly African Americans S.J. Szwast, MD H.C. Hendrie, MB, ChB, DSc K.A. Lane, MS S. Gao, PhD S.E. Taylor, MA F. Unverzagt, PhD J. Murrell, PhD M. Deeg,
Association of statin use with cognitive decline in elderly African Americans S.J. Szwast, MD H.C. Hendrie, MB, ChB, DSc K.A. Lane, MS S. Gao, PhD S.E. Taylor, MA F. Unverzagt, PhD J. Murrell, PhD M. Deeg,
It is the policy of health plans affiliated with PA Health & Wellness that Vytorin is medically necessary when the following criteria are met:
 Clinical Policy: Ezetimibe and Simvastatin (Vytorin) Reference Number: PA.CP.PMN.77 Effective Date: 02.01.17 Last Review Date: 07.18 Revision Log Description Ezetimibe/simvastatin (Vytorin ) contains ezetimibe,
Clinical Policy: Ezetimibe and Simvastatin (Vytorin) Reference Number: PA.CP.PMN.77 Effective Date: 02.01.17 Last Review Date: 07.18 Revision Log Description Ezetimibe/simvastatin (Vytorin ) contains ezetimibe,
Drug Class Review HMG-CoA Reductase Inhibitors (Statins) and Fixed-dose Combination Products Containing a Statin
 Drug Class Review HMG-CoA Reductase Inhibitors (Statins) and Fixed-dose Combination Products Containing a Statin Final Report Update 5 November 2009 This report reviews information about the comparative
Drug Class Review HMG-CoA Reductase Inhibitors (Statins) and Fixed-dose Combination Products Containing a Statin Final Report Update 5 November 2009 This report reviews information about the comparative
ALZHEIMER S DISEASE FACTOIDS & STATISTICS
 ALZHEIMER S DISEASE FACTOIDS & STATISTICS ~ 4 million affected in US alone 6-8% if 65+ years old, 30-50% if 80+ By 2030, in US >65 million people >65+ (---> ~14 million with AD) AD is one of the top 10
ALZHEIMER S DISEASE FACTOIDS & STATISTICS ~ 4 million affected in US alone 6-8% if 65+ years old, 30-50% if 80+ By 2030, in US >65 million people >65+ (---> ~14 million with AD) AD is one of the top 10
ATP IV: Predicting Guideline Updates
 Disclosures ATP IV: Predicting Guideline Updates Daniel M. Riche, Pharm.D., BCPS, CDE Speaker s Bureau Merck Janssen Boehringer-Ingelheim Learning Objectives Describe at least two evidence-based recommendations
Disclosures ATP IV: Predicting Guideline Updates Daniel M. Riche, Pharm.D., BCPS, CDE Speaker s Bureau Merck Janssen Boehringer-Ingelheim Learning Objectives Describe at least two evidence-based recommendations
( Diabetes mellitus, DM ) ( Hyperlipidemia ) ( Cardiovascular disease, CVD )
 005 6 69-74 40 mg/dl > 50 mg/dl) (00 mg/dl < 00 mg/dl(.6 mmol/l) 30-40% < 70 mg/dl 40 mg/dl 00 9 mg/dl fibric acid derivative niacin statin fibrate statin niacin ( ) ( Diabetes mellitus,
005 6 69-74 40 mg/dl > 50 mg/dl) (00 mg/dl < 00 mg/dl(.6 mmol/l) 30-40% < 70 mg/dl 40 mg/dl 00 9 mg/dl fibric acid derivative niacin statin fibrate statin niacin ( ) ( Diabetes mellitus,
Antihyperlipidemic Drugs
 Antihyperlipidemic Drugs Hyperlipidemias. Hyperlipoproteinemias. Hyperlipemia. Hypercholestrolemia. Direct relationship with acute pancreatitis and atherosclerosis Structure Lipoprotein Particles Types
Antihyperlipidemic Drugs Hyperlipidemias. Hyperlipoproteinemias. Hyperlipemia. Hypercholestrolemia. Direct relationship with acute pancreatitis and atherosclerosis Structure Lipoprotein Particles Types
Quality ID #438: Statin Therapy for the Prevention and Treatment of Cardiovascular Disease National Quality Strategy Domain: Effective Clinical Care
 Quality ID #438: Statin Therapy for the Prevention and Treatment of Cardiovascular Disease National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID #438: Statin Therapy for the Prevention and Treatment of Cardiovascular Disease National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Simvastatin 40 mg equivalent
 Simvastatin 40 mg equivalent medications equivalent to Simvastatin is available on the Drugs.com website. Simvastatin (Zocor ): 10 mg : Equivalent Dosages - 3: Atorvastatin (Lipitor. 40 mg : Equivalent
Simvastatin 40 mg equivalent medications equivalent to Simvastatin is available on the Drugs.com website. Simvastatin (Zocor ): 10 mg : Equivalent Dosages - 3: Atorvastatin (Lipitor. 40 mg : Equivalent
ORIGINAL CONTRIBUTION. Serum Lipoprotein Levels, Statin Use, and Cognitive Function in Older Women
 ORIGINAL CONTRIBUTION Serum Lipoprotein Levels, Statin Use, and Cognitive Function in Older Women Kristine Yaffe, MD; Elizabeth Barrett-Connor, MD; Feng Lin, MS; Deborah Grady, MD Background: Few strategies
ORIGINAL CONTRIBUTION Serum Lipoprotein Levels, Statin Use, and Cognitive Function in Older Women Kristine Yaffe, MD; Elizabeth Barrett-Connor, MD; Feng Lin, MS; Deborah Grady, MD Background: Few strategies
The Primary Care Guide To Understanding The Role Of Diabetes As A Risk Factor For Cognitive Loss Or Dementia In Adults
 The Primary Care Guide To Understanding The Role Of Diabetes As A Risk Factor For Cognitive Loss Or Dementia In Adults. Introduction Glucose intolerance is common in older individuals and this metabolic
The Primary Care Guide To Understanding The Role Of Diabetes As A Risk Factor For Cognitive Loss Or Dementia In Adults. Introduction Glucose intolerance is common in older individuals and this metabolic
Statins and newly diagnosed diabetes
 DOI:10.1111/j.1365-2125.2004.02142.x British Journal of Clinical Pharmacology Statins and newly diagnosed diabetes Susan S. Jick & Brian D. Bradbury Boston Collaborative Drug Surveillance Program, 11 Muzzey
DOI:10.1111/j.1365-2125.2004.02142.x British Journal of Clinical Pharmacology Statins and newly diagnosed diabetes Susan S. Jick & Brian D. Bradbury Boston Collaborative Drug Surveillance Program, 11 Muzzey
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
Anti Hyperlipidemic Drugs. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Anti Hyperlipidemic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Lipoproteins Macromolecular complexes in the blood that transport lipids Apolipoproteins
Anti Hyperlipidemic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Lipoproteins Macromolecular complexes in the blood that transport lipids Apolipoproteins
Clinical Policy: Ezetimibe (Zetia) Reference Number: CP.PMN.78 Effective Date: Last Review Date: 02.19
 Clinical Policy: (Zetia) Reference Number: CP.PMN.78 Effective Date: 02.01.17 Last Review Date: 02.19 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Zetia) Reference Number: CP.PMN.78 Effective Date: 02.01.17 Last Review Date: 02.19 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Cholesterol Management Roy Gandolfi, MD
 Cholesterol Management 2017 Roy Gandolfi, MD Goals Interpreting cholesterol guidelines Cholesterol treatment in diabetics Statin use and side effects therapy Reporting- Comparison data among physicians
Cholesterol Management 2017 Roy Gandolfi, MD Goals Interpreting cholesterol guidelines Cholesterol treatment in diabetics Statin use and side effects therapy Reporting- Comparison data among physicians
Cholesterol. Medicines To Help You
 Medicines To Help You Cholesterol Use this guide to help you talk to your doctor, pharmacist, or nurse about your cholesterol medicines. The guide lists all of the FDA-approved products now available to
Medicines To Help You Cholesterol Use this guide to help you talk to your doctor, pharmacist, or nurse about your cholesterol medicines. The guide lists all of the FDA-approved products now available to
Clinical Policy: Pitavastatin (Livalo), Ezetimibe/Simvastatin (Vytorin 10/10 mg) Reference Number: CP.CPA.62 Effective Date:
 Clinical Policy: Pitavastatin (Livalo), Ezetimibe/Simvastatin (Vytorin 10/10 mg) Reference Number: CP.CPA.62 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Revision Log See
Clinical Policy: Pitavastatin (Livalo), Ezetimibe/Simvastatin (Vytorin 10/10 mg) Reference Number: CP.CPA.62 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Commercial Revision Log See
The Impact of the Use of Statins on the Prevalence of Dementia and the Progression of Cognitive Impairment
 Journal of Gerontology: MEDICAL SCIENCES 2002, Vol. 57A, No. 7, M414 M418 Copyright 2002 by The Gerontological Society of America The Impact of the Use of Statins on the Prevalence of Dementia and the
Journal of Gerontology: MEDICAL SCIENCES 2002, Vol. 57A, No. 7, M414 M418 Copyright 2002 by The Gerontological Society of America The Impact of the Use of Statins on the Prevalence of Dementia and the
Cholesterol targets and therapy Thomas C. Andrews, MD, FACC
 Cholesterol targets and therapy Thomas C. Andrews, MD, FACC 2 Statins in secondary prevention Still first line therapy! First line therapy: high intensity statin Dose individualized based on baseline LDL
Cholesterol targets and therapy Thomas C. Andrews, MD, FACC 2 Statins in secondary prevention Still first line therapy! First line therapy: high intensity statin Dose individualized based on baseline LDL
Pharmacy Drug Class Review
 Pharmacy Drug Class Review January 22, 2014 Authored By: Christina Manciocchi, Pharm.D. BCACP Disclaimer: Specific agents may have variations Edited By: Richard J. Kraft, Pharm.D.BCPS NEW CHOLESTEROL GUIDELINES
Pharmacy Drug Class Review January 22, 2014 Authored By: Christina Manciocchi, Pharm.D. BCACP Disclaimer: Specific agents may have variations Edited By: Richard J. Kraft, Pharm.D.BCPS NEW CHOLESTEROL GUIDELINES
APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES
 APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES Main systematic reviews secondary studies on the general effectiveness of statins in secondary cardiovascular prevention (search date: 2003-2006) NICE.
APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES Main systematic reviews secondary studies on the general effectiveness of statins in secondary cardiovascular prevention (search date: 2003-2006) NICE.
ANTIHYPERLIPIDEMIA. Darmawan,dr.,M.Kes,Sp.PD
 ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Plasma Levels of -Amyloid (1-4), -Amyloid (1-42), and Total -Amyloid Remain Unaffected in Adult Patients With Hypercholesterolemia After Treatment With Statins Kina Höglund, MSc;
ORIGINAL CONTRIBUTION Plasma Levels of -Amyloid (1-4), -Amyloid (1-42), and Total -Amyloid Remain Unaffected in Adult Patients With Hypercholesterolemia After Treatment With Statins Kina Höglund, MSc;
Lipid Management Step Therapy Criteria with Medical Diagnoses Option*
 Lipid Management Step Therapy Criteria with Medical Diagnoses Option* * Medical diagnoses are required for implementation of this option. Program may be implemented with the following options: Option One
Lipid Management Step Therapy Criteria with Medical Diagnoses Option* * Medical diagnoses are required for implementation of this option. Program may be implemented with the following options: Option One
Diabetes Mellitus and Dementia. Andrea Shelton & Adena Zadourian
 Diabetes Mellitus and Dementia Andrea Shelton & Adena Zadourian Abstract Diabetes mellitus increases the risk for developing dementia...but there is inconsistency with the subtypes of dementia Diabetes
Diabetes Mellitus and Dementia Andrea Shelton & Adena Zadourian Abstract Diabetes mellitus increases the risk for developing dementia...but there is inconsistency with the subtypes of dementia Diabetes
Mild Cognitive Impairment
 Mild Cognitive Impairment Victor W. Henderson, MD, MS Departments of Health Research & Policy (Epidemiology) and of Neurology & Neurological Sciences Stanford University Director, Stanford Alzheimer s
Mild Cognitive Impairment Victor W. Henderson, MD, MS Departments of Health Research & Policy (Epidemiology) and of Neurology & Neurological Sciences Stanford University Director, Stanford Alzheimer s
Delirium, Apo-E status, and AD CSF biomarkers
 Delirium, Apo-E status, and AD CSF biomarkers Zhongcong Xie, M.D., Ph.D. Geriatric Anesthesia Research Unit Department of Anesthesia, Critical Care and Pain Medicine Massachusetts General Hospital Harvard
Delirium, Apo-E status, and AD CSF biomarkers Zhongcong Xie, M.D., Ph.D. Geriatric Anesthesia Research Unit Department of Anesthesia, Critical Care and Pain Medicine Massachusetts General Hospital Harvard
Evidence for benefit of statins to modify cognitive decline and risk in Alzheimer s disease
 Geifman et al. Alzheimer's Research & Therapy (2017) 9:10 DOI 10.1186/s13195-017-0237-y RESEARCH Open Access Evidence for benefit of statins to modify cognitive decline and risk in Alzheimer s disease
Geifman et al. Alzheimer's Research & Therapy (2017) 9:10 DOI 10.1186/s13195-017-0237-y RESEARCH Open Access Evidence for benefit of statins to modify cognitive decline and risk in Alzheimer s disease
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Vytorin) Reference Number: CP.PMN.77 Effective Date: 02.01.17 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Vytorin) Reference Number: CP.PMN.77 Effective Date: 02.01.17 Last Review Date: 02.18 Line of Business: Commercial, Medicaid Revision Log See Important Reminder at the end of this policy
Platelet Amyloid Precursor Protein Processing: A Biomarker for Alzheimer s Disease.
 Platelet Amyloid Precursor Protein Processing: A Biomarker for Alzheimer s Disease. Roger N. Rosenberg, MD Alzheimer s Disease Center University of Texas Southwestern Medical Center at Dallas Disclosures:
Platelet Amyloid Precursor Protein Processing: A Biomarker for Alzheimer s Disease. Roger N. Rosenberg, MD Alzheimer s Disease Center University of Texas Southwestern Medical Center at Dallas Disclosures:
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Reference Number: CP.HNMC.05 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: Reference Number: CP.HNMC.05 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy for important
Diseases & Conditions
 http://my.clevelandclinic.org Diseases & Conditions About Cholesterol-Lowering Drugs Some people have a genetic predisposition to high blood cholesterol levels. These people may need drug therapy in addition
http://my.clevelandclinic.org Diseases & Conditions About Cholesterol-Lowering Drugs Some people have a genetic predisposition to high blood cholesterol levels. These people may need drug therapy in addition
Doctor discussion guide:
 Doctor discussion guide: MAnaging Cholesterol Bring this printout to your next doctor s appointment. It will help you and your doctor work together to set goals for treatment, evaluate the success of your
Doctor discussion guide: MAnaging Cholesterol Bring this printout to your next doctor s appointment. It will help you and your doctor work together to set goals for treatment, evaluate the success of your
B. Patient has not reached the percentage reduction goal with statin therapy
 Managing Cardiovascular Risk: The Importance of Lowering LDL Cholesterol and Reaching Treatment Goals for LDL Cholesterol The Role of the Pharmacist Learning Objectives 1. Review the role of lipid levels
Managing Cardiovascular Risk: The Importance of Lowering LDL Cholesterol and Reaching Treatment Goals for LDL Cholesterol The Role of the Pharmacist Learning Objectives 1. Review the role of lipid levels
Statins in the Treatment of Type 2 Diabetes Mellitus: A Systematic Review.
 ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 1 Statins in the Treatment of Type 2 Diabetes Mellitus: A Systematic Review. C ANYANWU, C NOSIRI Citation C ANYANWU, C NOSIRI.
ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 1 Statins in the Treatment of Type 2 Diabetes Mellitus: A Systematic Review. C ANYANWU, C NOSIRI Citation C ANYANWU, C NOSIRI.
Doctor discussion guide:
 Bring this printout to your next doctor s appointment. It will help you and your doctor work together to set goals for treatment, evaluate the success of your treatment, and reduce your risk of side effects.
Bring this printout to your next doctor s appointment. It will help you and your doctor work together to set goals for treatment, evaluate the success of your treatment, and reduce your risk of side effects.
Joslin Diabetes Center Advances in Diabetes and Thyroid Disease 2013 Consensus and Controversy in Diabetic Dyslipidemia
 Consensus and Controversy in Diabetes and Dyslipidemia Om P. Ganda MD Director, Lipid Clinic Joslin diabetes Center Boston, MA, USA CVD Outcomes in DM vs non- DM 102 Prospective studies; 698, 782 people,
Consensus and Controversy in Diabetes and Dyslipidemia Om P. Ganda MD Director, Lipid Clinic Joslin diabetes Center Boston, MA, USA CVD Outcomes in DM vs non- DM 102 Prospective studies; 698, 782 people,
Fact Sheet Alzheimer s disease
 What is Alzheimer s disease Fact Sheet Alzheimer s disease Alzheimer s disease, AD, is a progressive brain disorder that gradually destroys a person s memory and ability to learn, reason, make judgements,
What is Alzheimer s disease Fact Sheet Alzheimer s disease Alzheimer s disease, AD, is a progressive brain disorder that gradually destroys a person s memory and ability to learn, reason, make judgements,
Mild Cognitive Impairment (MCI)
 October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
1.* Dosage. A. Adults
 3-Hydroxy-3-Methylglutaryl Coenzyme A (HMG-CoA) Reductase Inhibitors [Developed, November 1994; Revised, October 1996; September 1997; September 1998; October 1999; November 1999; August 2000; September
3-Hydroxy-3-Methylglutaryl Coenzyme A (HMG-CoA) Reductase Inhibitors [Developed, November 1994; Revised, October 1996; September 1997; September 1998; October 1999; November 1999; August 2000; September
Apolipoprotein E and cholesterol metabolism in the pathogenesis and treatment of Alzheimer s disease
 94 Review TRENDS in Molecular Medicine Vol.9 No.3 March 2003 Apolipoprotein E and cholesterol metabolism in the pathogenesis and treatment of Alzheimer s disease Judes Poirier McGill Centre for Studies
94 Review TRENDS in Molecular Medicine Vol.9 No.3 March 2003 Apolipoprotein E and cholesterol metabolism in the pathogenesis and treatment of Alzheimer s disease Judes Poirier McGill Centre for Studies
Chapter 1. Introduction
 The older people get, the bigger the chance of losing cognitive abilities and ultimately to develop dementia. Increasing age is the largest known risk factor of dementia, with a prevalence of 1% in people
The older people get, the bigger the chance of losing cognitive abilities and ultimately to develop dementia. Increasing age is the largest known risk factor of dementia, with a prevalence of 1% in people
High ( 50%) Restrictions mg 20-40mg PA; TS ⱡ 15 ⱡ
 MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Cholesterol P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular REVIEW HISTORY: 5/16, 5/15, 2/14, 5/12, LOB AFFECTED: Medi-Cal
MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Cholesterol P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular REVIEW HISTORY: 5/16, 5/15, 2/14, 5/12, LOB AFFECTED: Medi-Cal
Supplement Table 2. Categorization of Statin Intensity Based on Potential Low-Density Lipoprotein Cholesterol Reduction
 Supplement: Tables Supplement Table 1. Study Eligibility Criteria Supplement Table 2. Categorization of Statin Intensity Based on Potential Low-Density Lipoprotein Cholesterol Reduction Supplement Table
Supplement: Tables Supplement Table 1. Study Eligibility Criteria Supplement Table 2. Categorization of Statin Intensity Based on Potential Low-Density Lipoprotein Cholesterol Reduction Supplement Table
Biomarkers for Alzheimer s disease
 Biomarkers for Alzheimer s Disease Henrik Zetterberg, MD, PhD Professor of Neurochemistry The Sahlgrenska Academy, University of Gothenburg 1 Alzheimer s disease 2 Neuropathological criteria for Alzheimer
Biomarkers for Alzheimer s Disease Henrik Zetterberg, MD, PhD Professor of Neurochemistry The Sahlgrenska Academy, University of Gothenburg 1 Alzheimer s disease 2 Neuropathological criteria for Alzheimer
Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States
 Bull. Natl. Inst. Health Sci., 123 Notes # Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States Journal of American Medical Association (JAMA) Statin HMG
Bull. Natl. Inst. Health Sci., 123 Notes # Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States Journal of American Medical Association (JAMA) Statin HMG
Learning Objectives. Patient Case
 Joseph Saseen, Pharm.D., FASHP, FCCP, BCPS Professor and Vice Chair, Department of Clinical Pharmacy University of Colorado Anschutz Medical Campus Learning Objectives Identify the 4 patient populations
Joseph Saseen, Pharm.D., FASHP, FCCP, BCPS Professor and Vice Chair, Department of Clinical Pharmacy University of Colorado Anschutz Medical Campus Learning Objectives Identify the 4 patient populations
Antihyperlipidemic drugs
 Antihyperlipidemic drugs The clinically important lipoproteins are LDL low density lipoprotein, VLDL very low density lipoprotein, HDL high density lipoprotein. Hyperlipidemia may caused 1. by individual
Antihyperlipidemic drugs The clinically important lipoproteins are LDL low density lipoprotein, VLDL very low density lipoprotein, HDL high density lipoprotein. Hyperlipidemia may caused 1. by individual
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη
 Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
Month/Year of Review: September 2013 Date of Last Review: February 2012
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
PATIENT INFORMATION. Medicine To Treat: C ardiac Diseases. Lipid-Lowering Medicines. Statins Fibrates Fat Binding Agents Nicotinic Acid Group
 PATIENT INFORMATION Medicine To Treat: C ardiac Diseases Lipid-Lowering Medicines Statins Fibrates Fat Binding Agents Nicotinic Acid Group ABOUT YOUR MEDICINE Your doctor has just prescribed for you: Medicine
PATIENT INFORMATION Medicine To Treat: C ardiac Diseases Lipid-Lowering Medicines Statins Fibrates Fat Binding Agents Nicotinic Acid Group ABOUT YOUR MEDICINE Your doctor has just prescribed for you: Medicine
Pravastatin conversion to atorvastatin
 P ford residence southampton, ny Pravastatin conversion to atorvastatin Pravastatin official prescribing information for healthcare professionals. Includes: indications, dosage, adverse reactions, pharmacology
P ford residence southampton, ny Pravastatin conversion to atorvastatin Pravastatin official prescribing information for healthcare professionals. Includes: indications, dosage, adverse reactions, pharmacology
Clinical Policy: Lomitapide (Juxtapid) Reference Number: ERX.SPA.170 Effective Date:
 Clinical Policy: (Juxtapid) Reference Number: ERX.SPA.170 Effective Date: 01.11.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Juxtapid) Reference Number: ERX.SPA.170 Effective Date: 01.11.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
ORIGINAL INVESTIGATION. Screening for Statin-Related Toxicity. The Yield of Transaminase and Creatine Kinase Measurements in a Primary Care Setting
 ORIGINAL INVESTIGATION Screening for Statin-Related Toxicity The Yield of Transaminase and Creatine Kinase Measurements in a Primary Care Setting C. Christopher Smith, MD; Lana I. Bernstein, MD; Roger
ORIGINAL INVESTIGATION Screening for Statin-Related Toxicity The Yield of Transaminase and Creatine Kinase Measurements in a Primary Care Setting C. Christopher Smith, MD; Lana I. Bernstein, MD; Roger
The current state of healthcare for Normal Aging, Mild Cognitive Impairment, & Alzheimer s Disease
 The current state of healthcare for Normal Aging, g, Mild Cognitive Impairment, & Alzheimer s Disease William Rodman Shankle, MS MD FACP Director, Alzheimer s Program, Hoag Neurosciences Institute Neurologist,
The current state of healthcare for Normal Aging, g, Mild Cognitive Impairment, & Alzheimer s Disease William Rodman Shankle, MS MD FACP Director, Alzheimer s Program, Hoag Neurosciences Institute Neurologist,
Drug Class Review on HMG-CoA Reductase Inhibitors (Statins)
 Drug Class Review on HMG-CoA Reductase Inhibitors () Final Report June 2004 Mark Helfand, MD, MPH Susan Carson, MPH Cathy Kelley, PharmD Oregon Evidence-based Practice Center Oregon Health & Science University
Drug Class Review on HMG-CoA Reductase Inhibitors () Final Report June 2004 Mark Helfand, MD, MPH Susan Carson, MPH Cathy Kelley, PharmD Oregon Evidence-based Practice Center Oregon Health & Science University
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema
 The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
Antihyperlipidemic Drugs
 Antihyperlipidemic Drugs Lipid disorders: Disorders of lipid metabolism are manifest by elevation of the plasma concentrations of the various lipid and lipoprotein fractions (total and LDL cholesterol,
Antihyperlipidemic Drugs Lipid disorders: Disorders of lipid metabolism are manifest by elevation of the plasma concentrations of the various lipid and lipoprotein fractions (total and LDL cholesterol,
Effect of statins on the mortality of patients with ischaemic heart disease: population based cohort study with nested case control analysis
 752 CARDIOVASCULAR MEDICINE Effect of statins on the mortality of patients with ischaemic heart disease: population based cohort study with nested case control analysis J Hippisley-Cox, C Coupland... Heart
752 CARDIOVASCULAR MEDICINE Effect of statins on the mortality of patients with ischaemic heart disease: population based cohort study with nested case control analysis J Hippisley-Cox, C Coupland... Heart
A Review: Atherosclerosis & its treatment
 73 Review Article A Review: Atherosclerosis & its treatment Yogesh K. Patil* Department of Pharmacology, Shree Mahavir Institute of Pharmacy, Nashik, Maharashtra, India *yogesh_kpatil85@yahoo.co.in ABSTRACT
73 Review Article A Review: Atherosclerosis & its treatment Yogesh K. Patil* Department of Pharmacology, Shree Mahavir Institute of Pharmacy, Nashik, Maharashtra, India *yogesh_kpatil85@yahoo.co.in ABSTRACT
In 2001, the National Cholesterol Education Program
 At a Glance Practical Implications p 330 Author Information p 333 Full text and PDF www.ajpblive.com Lipid Management When Converting Fluvastatin to Pravastatin: Medication Use Evaluation Original Research
At a Glance Practical Implications p 330 Author Information p 333 Full text and PDF www.ajpblive.com Lipid Management When Converting Fluvastatin to Pravastatin: Medication Use Evaluation Original Research
The All Wales Medicine Strategy Group (AWMSG) is asked to support implementation of the following prescribing indicators.
 ENCLOSURE 5 APPENDIX 1 Paper presented to AWMSG in June 2006 AWPAG considered comments recorded in AWMSG minutes in July 2006 Paper subsequently updated and brought back to AWMSG for endorsement This paper
ENCLOSURE 5 APPENDIX 1 Paper presented to AWMSG in June 2006 AWPAG considered comments recorded in AWMSG minutes in July 2006 Paper subsequently updated and brought back to AWMSG for endorsement This paper
SUPPLEMENTARY APPENDIX
 Type 2 diabetes as a risk factor for dementia in women compared with men: a pooled analysis of 23 million people and more than 100,000 cases of dementia SUPPLEMENTARY APPENDIX Supplementary Methods Newcastle
Type 2 diabetes as a risk factor for dementia in women compared with men: a pooled analysis of 23 million people and more than 100,000 cases of dementia SUPPLEMENTARY APPENDIX Supplementary Methods Newcastle
Novel Therapeutic Strategies in Lipid Management: Lowering LDL C to Improve Patient Outcomes
 Novel Therapeutic Strategies in Lipid Management: Lowering LDL C to Improve Patient Outcomes Rajat Deo, MD, MTR Assistant Professor of Medicine Division of Cardiology University of Pennsylvania April 25,
Novel Therapeutic Strategies in Lipid Management: Lowering LDL C to Improve Patient Outcomes Rajat Deo, MD, MTR Assistant Professor of Medicine Division of Cardiology University of Pennsylvania April 25,
8/14/2018. The Evolving Concept of Alzheimer s Disease. Epochs of AD Research. Diagnostic schemes have evolved with the research
 The Evolving Concept of Alzheimer s Disease David S. Geldmacher, MD, FACP Warren Family Endowed Chair in Neurology Department of Neurology UAB School of Medicine Epochs of AD Research Epoch Years Key Event
The Evolving Concept of Alzheimer s Disease David S. Geldmacher, MD, FACP Warren Family Endowed Chair in Neurology Department of Neurology UAB School of Medicine Epochs of AD Research Epoch Years Key Event
Management of Post-transplant hyperlipidemia
 Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Cholesterol-Lowering Drugs And Alzheimer S Disease
 Future Lipidology ISSN: 1746-0875 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/tlip19 Cholesterol-Lowering Drugs And Alzheimer S Disease Gunter P Eckert, Walter E Müller & Gibson W.
Future Lipidology ISSN: 1746-0875 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/tlip19 Cholesterol-Lowering Drugs And Alzheimer S Disease Gunter P Eckert, Walter E Müller & Gibson W.
Clinical Policy: Mipomersen (Kynamro) Reference Number: ERX.SPA.171 Effective Date:
 Clinical Policy: (Kynamro) Reference Number: ERX.SPA.171 Effective Date: 01.11.17 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Kynamro) Reference Number: ERX.SPA.171 Effective Date: 01.11.17 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Statins, Risk of Dementia, and Cognitive Function: Secondary Analysis of the Ginkgo Evaluation of Memory Study
 Statins, Risk of Dementia, and Cognitive Function: Secondary Analysis of the Ginkgo Evaluation of Memory Study Kerstin Bettermann, MD, PhD,* Alice M. Arnold, PhD, Jeff Williamson, MD, Stephen Rapp, PhD,x
Statins, Risk of Dementia, and Cognitive Function: Secondary Analysis of the Ginkgo Evaluation of Memory Study Kerstin Bettermann, MD, PhD,* Alice M. Arnold, PhD, Jeff Williamson, MD, Stephen Rapp, PhD,x
Original paper. Abstract. Abdullah S. Asia 1*, Al-Mahdi A. Modar 2, Hadi M. Ali 3
 Original paper Frequency Of Potential Adverse Effects Of A Semisynthetic Statin (Simvastatin) Compared To A Synthetic Statin (Atorvastatin) Used To Reduce Cardiovascular Risk For Patients In Basra 1*,
Original paper Frequency Of Potential Adverse Effects Of A Semisynthetic Statin (Simvastatin) Compared To A Synthetic Statin (Atorvastatin) Used To Reduce Cardiovascular Risk For Patients In Basra 1*,
How to use statins in patients with chronic liver disease
 REVIEW CME CREDIT MARK W. RUSSO, MD Center for the Study of Hepatitis C, Division of Gastroenterology and Hepatology, Weill Cornell Medical College, New York, NY IRA M. JACOBSON, MD Center for the Study
REVIEW CME CREDIT MARK W. RUSSO, MD Center for the Study of Hepatitis C, Division of Gastroenterology and Hepatology, Weill Cornell Medical College, New York, NY IRA M. JACOBSON, MD Center for the Study
CHOLESTEROL REDUCING MEDICATIONS. Five Main Categories. 1. Statins 2. Fibrates 3. Resins 4. Niacin 5. Cholesterol absorption inhibitor
 Page 1 of 5 PHA-GEN-002-2004 CHOLESTEROL REDUCING MEDICATIONS Five Main Categories 1. Statins 2. Fibrates 3. Resins 4. Niacin 5. Cholesterol absorption inhibitor Statins Also called HMG-CoA reductase inhibitors
Page 1 of 5 PHA-GEN-002-2004 CHOLESTEROL REDUCING MEDICATIONS Five Main Categories 1. Statins 2. Fibrates 3. Resins 4. Niacin 5. Cholesterol absorption inhibitor Statins Also called HMG-CoA reductase inhibitors
Drugs for Dyslipidemias
 Drugs for Dyslipidemias HMG CoA reductase inhibitors (statins): atorvastatin, lovastatin, pravastatin, simvastatin Bile acid-binding resins: cholestyramine, colestipol, colesevelam Fibric acid derivatives
Drugs for Dyslipidemias HMG CoA reductase inhibitors (statins): atorvastatin, lovastatin, pravastatin, simvastatin Bile acid-binding resins: cholestyramine, colestipol, colesevelam Fibric acid derivatives
Mild Cognitive Impairment Symposium January 19 and 20, 2013
 Highlights of Biomarker and Clinical Outcomes in Recent AD Treatment Trials Stephen Salloway, MD, MS Professor of Neurology and Psychiatry Alpert Medical School, Brown University Mild Cognitive Impairment
Highlights of Biomarker and Clinical Outcomes in Recent AD Treatment Trials Stephen Salloway, MD, MS Professor of Neurology and Psychiatry Alpert Medical School, Brown University Mild Cognitive Impairment
Critical Review. Cholesterol and Alzheimer s Disease: A Still Poorly Understood Correlation
 IUBMB Life, 64(12): 931 935, December 2012 Critical Review Cholesterol and Alzheimer s Disease: A Still Poorly Understood Correlation Roberta Ricciarelli 1 *, Elisa Canepa 1, Barbara Marengo 1, Umberto
IUBMB Life, 64(12): 931 935, December 2012 Critical Review Cholesterol and Alzheimer s Disease: A Still Poorly Understood Correlation Roberta Ricciarelli 1 *, Elisa Canepa 1, Barbara Marengo 1, Umberto
The Effects of HMG-CoA Reductase Inhibitors in the Prevention of Dementia in the Elderly Population
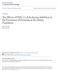 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 The Effects of HMG-CoA Reductase Inhibitors in the Prevention of Dementia
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 The Effects of HMG-CoA Reductase Inhibitors in the Prevention of Dementia
Section Editor Steven T DeKosky, MD, FAAN Kenneth E Schmader, MD
 Prevention of dementia Author Daniel Press, MD Michael Alexander, MD Section Editor Steven T DeKosky, MD, FAAN Kenneth E Schmader, MD Deputy Editor Janet L Wilterdink, MD Last literature review version
Prevention of dementia Author Daniel Press, MD Michael Alexander, MD Section Editor Steven T DeKosky, MD, FAAN Kenneth E Schmader, MD Deputy Editor Janet L Wilterdink, MD Last literature review version
Pharmacology Challenges: Managing Statin Myalgia
 Clinical Case: RM is a 50 year-old African American woman with a past medical history of type diabetes, dyslipidemia, hypertension and peripheral arterial disease. She had been prescribed simvastatin 80
Clinical Case: RM is a 50 year-old African American woman with a past medical history of type diabetes, dyslipidemia, hypertension and peripheral arterial disease. She had been prescribed simvastatin 80
Data Alert. Vascular Biology Working Group. Blunting the atherosclerotic process in patients with coronary artery disease.
 1994--4 Vascular Biology Working Group www.vbwg.org c/o Medical Education Consultants, LLC 25 Sylvan Road South, Westport, CT 688 Chairman: Carl J. Pepine, MD Eminent Scholar American Heart Association
1994--4 Vascular Biology Working Group www.vbwg.org c/o Medical Education Consultants, LLC 25 Sylvan Road South, Westport, CT 688 Chairman: Carl J. Pepine, MD Eminent Scholar American Heart Association
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Statin Therapy Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Statin Therapy Prime Therapeutics will review Prior Authorization requests. Prior Authorization
Statin Therapy Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Statin Therapy Prime Therapeutics will review Prior Authorization requests. Prior Authorization
Coronary heart disease is the leading cause of death in
 PHARMACOLOGY NOTES Ezetimibe (Zetia): a new type of lipid-lowering agent JIGNA PATEL, PHARMD CANDIDATE, VALERIE SHEEHAN, PHARMD, AND CHERYLE GURK-TURNER, RPH Coronary heart disease is the leading cause
PHARMACOLOGY NOTES Ezetimibe (Zetia): a new type of lipid-lowering agent JIGNA PATEL, PHARMD CANDIDATE, VALERIE SHEEHAN, PHARMD, AND CHERYLE GURK-TURNER, RPH Coronary heart disease is the leading cause
Statin Use, Incident Dementia
 Original Report: Mental Health Statin Use, Incident Dementia and Alzheimer Disease in Elderly African Americans Hugh C. Hendrie, MBChB, DSc; Ann Hake, MD; Kathleen Lane, MS; Christianna Purnell, BA; Frederick
Original Report: Mental Health Statin Use, Incident Dementia and Alzheimer Disease in Elderly African Americans Hugh C. Hendrie, MBChB, DSc; Ann Hake, MD; Kathleen Lane, MS; Christianna Purnell, BA; Frederick
Medical evidence suggests that
 COMBINATION THERAPY TO ACHIEVE LIPID GOALS David G. Robertson, MD* ABSTRACT Coronary heart disease (CHD) remains the leading cause of death in the United States despite recent advances in treatment and
COMBINATION THERAPY TO ACHIEVE LIPID GOALS David G. Robertson, MD* ABSTRACT Coronary heart disease (CHD) remains the leading cause of death in the United States despite recent advances in treatment and
THE ROLE OF ACTIVITIES OF DAILY LIVING IN THE MCI SYNDROME
 PERNECZKY 15/06/06 14:35 Page 1 THE ROLE OF ACTIVITIES OF DAILY LIVING IN THE MCI SYNDROME R. PERNECZKY, A. KURZ Department of Psychiatry and Psychotherapy, Technical University of Munich, Germany. Correspondence
PERNECZKY 15/06/06 14:35 Page 1 THE ROLE OF ACTIVITIES OF DAILY LIVING IN THE MCI SYNDROME R. PERNECZKY, A. KURZ Department of Psychiatry and Psychotherapy, Technical University of Munich, Germany. Correspondence
Neuroinflammation in preclinical AD: in vivo evidence
 Neuroinflammation in preclinical AD: in vivo evidence Barbara Bendlin, PhD Assistant Professor UW-Madison Dept. of Medicine, Geriatrics bbb@medicine.wisc.edu Overview Background Preclinical effects of
Neuroinflammation in preclinical AD: in vivo evidence Barbara Bendlin, PhD Assistant Professor UW-Madison Dept. of Medicine, Geriatrics bbb@medicine.wisc.edu Overview Background Preclinical effects of
4/24/15. AHA/ACC 2013 Guideline Key Points
 Review of the ACC/AHA 2013 Guidelines Anita Ralstin, MS, CNS, CNP Next Step Health Consultant, LLC 1! Discuss the rationale for the change in lipid guidelines and how that affects the decision to implement
Review of the ACC/AHA 2013 Guidelines Anita Ralstin, MS, CNS, CNP Next Step Health Consultant, LLC 1! Discuss the rationale for the change in lipid guidelines and how that affects the decision to implement
A mong the 20 leading prescription
 Safety and Statins: Pharmacologic and Clinical Perspectives Michael B. Bottorff, PharmD A mong the 20 leading prescription drugs in the United States, 3 agents atorvastatin (Lipitor), simvastatin (Zocor),
Safety and Statins: Pharmacologic and Clinical Perspectives Michael B. Bottorff, PharmD A mong the 20 leading prescription drugs in the United States, 3 agents atorvastatin (Lipitor), simvastatin (Zocor),
Dyslipedemia New Guidelines
 Dyslipedemia New Guidelines New ACC/AHA Prevention Guidelines on Blood Cholesterol November 12, 2013 Mohammed M Abd El Ghany Professor of Cardiology Cairo Universlty 1 1 0 Cholesterol Management Pharmacotherapy
Dyslipedemia New Guidelines New ACC/AHA Prevention Guidelines on Blood Cholesterol November 12, 2013 Mohammed M Abd El Ghany Professor of Cardiology Cairo Universlty 1 1 0 Cholesterol Management Pharmacotherapy
