Bisphosphonate-induced Severe Hypocalcemia - A Case Report -
|
|
|
- Shona Parker
- 5 years ago
- Views:
Transcription
1 CASE REPORT Vol. 19, No. 2, 2012 Bisphosphonate-induced Severe Hypocalcemia - A Case Report - Won-Seok Do, Jin-Kyung Park, Myung-Il Park, Hyeong-Seok Kim, Sung-Ho Kim, Duk-Hyun Lee * Department of Internal Medicine, Daegu Fatima Hospital, Daegu, Korea = Abstract = Bisphosphonate generally seems to be safe, but hypocalcemia may occasionally develop in the course of bisphosphonate treatment. Hypocalcemia induced by bisphosphonate is usually mild and asymptomatic, but unrecognized or poorly treated hypocalcemia can lead to life-threatening state. A 78-year-old woman who had a history of hip arthroplasty and intravenous zoledronate treatment for femur neck fracture was presented to emergency department with altered mental status. It turned out that her symptom was due to severe hypocalcemia which was caused by intravenous zoledronate treatment. She also had renal dysfunction. She was treated by intravenous calcium gluconate and calcitriol administration. This case supports the need for evaluation of renal dysfunction, vitamin D deficiency and parathyroid gland dysfunction before bisphosphonate treatment and accurate monitoring of plasma calcium and creatinine levels. In addition, vitamin D and calcium supply during treatment with bisphosphonate is mandatory. [Journal of Bone Metabolism, 19(2): , 2012] Key Words: Bisphosphonates, Hypocalcemia, Osteoporosis INTRODUCTION Bisphosphonate is analogues of pyrophosphate compounds and inhibits bone absorption effectively by suppressing osteoclast. In addition, it is utilized in a wide range of treatments including postmenopausal osteoporosis, Paget's disease, cancer-related osteolysis and hypercalcemia. Although bisphosphonate is known to be safe mostly, side effects such as gastrointestinal side effects, flu-like syndrome, nephrotoxicity, osteonecrosis of the jaw and hypocalcemia can be problematic.[1] Recently, as elderly population increases due to increase of average life-expectancy, bisphosphonate utilization in purpose of prevention and treatment of osteoporotic fracture also tends to increase. Therefore, more attention needs to be paid regarding the side effects. Since the authors experienced a case of severe hypocalcemia after utilizing intravenous bisphosphonate in the treatment of osteoporosis, we would like to report the case with literature review. CASE A 78-year-old female patient who had loss of appetite, lethargy, disorientation, and speech disturbance for several Received: May 22, 2012, Revised: September 18, 2012, Accepted: October 17, 2012 * Address for Correspondence. Duk-Hyun Lee, Department of Internal Medicine, Daegu Fatima Hospital, , Sinam-dong, Dong-gu, Daegu, , Korea. Tel: , Fax: , dhlee@fatima.or.kr CC This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( 139
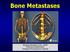
2 J Bone Metab Fig. 1. Measurement of bone mineral density in lumbar spine (left) and hip (right). BMD, bone mineral density. days came to our hospital in emergency room due to mental deterioration. About a month before the hospital visit, the patient had femur neck fracture caused by hitting on a table and then received hip arthroplasty under spinal anesthesia. At the time of the visit, blood pressure, body temperature, pulse rate, and respiratory rate were 120/70 mmhg, 36.5, 70 times/minute, and 20 times/minute, respectively, and the patient responded to pains but couldn't communicate. Brain magnetic resonance imaging (MRI) was carried out in order to check the occurrence of cerebrovascular event but acute lesion was not observed. Laboratory test showed the result of leukocyte count 6,530/μL, hemoglobin 11.3 g/dl, platelet count 197,000/μL, blood urea nitrogen 36.9 mg/dl (8-23), serum creatinine 3.67 mg/dl ( ), fractional excretion of sodium (FE Na ) 5.9%, serum albumin 3.3 g/dl ( ), sodium meq/l ( ), potassium 3.3 meq/l ( ), corrected calcium concentration 3.96 mg/ dl (9-11), phosphorus 2.5 mg/dl ( ), parathyroid hormone (PTH) pg/ml (12-88), ionized calcium 1.8 mg/dl (4-4.8), and magnesium 1.4 mg/dl ( ). The corrected calcium concentration was calculated utilizing equation of 'total calcium concentration in serum (mg/dl) + (0.8 (4.0 - serum albumin concentration [g/dl])'. On electrocardiography, corrected QT interval (519 msec) was prolonged, but Trousseau's phenomenon or Chvostek's sign was not exhibited. In the past medical history, no special diseases such as hypertension and diabetes were present and the patient was a non-smoker and a non-drinker. When the patient had femur neck fracture about a month ago, bone mineral density (BMD) was measured utilizing dualenergy X-ray absorptiometry (DXA; Hologic QDR-4500W; Hologic, Inc., Bedford, MA, USA). In result, osteoporosis was considered with T-scores of -3.9 and -3.4 in lumbar spine (L1-4) and hip, respectively (Fig. 1). Therefore, 5 mg of zoledronate (Aclasta ) was injected intravenously for 15 minutes on the day after the surgery and then calcium supplements were continuously being given until visiting the emergency room. In the blood test at the time of injecting zoledronate intravenously, serum creatinine concentration was 2.83 mg/dl and corrected calcium concentration was 140
3 Fig. 2. Changes in total serum calcium concentration with time. Time zero represents the time of patient's presentation with femur fracture. Bold arrow means the time of administration of zoledronate and empty arrow means the time of patient's presentation with hypocalcemia. 8.4 mg/dl. The patient was diagnosed intravenous zoledronateinduced hypocalcemia and then 20 ml of calcium gluconate (diluted in 100 ml of normal saline) and 1 μg/day of vitamin D (calcitriol, Bonky ) were started to inject intravenously. From the day after the intravenous injection of calcium, the patient showed gradual improvement in consciousness as well as lethargy and fatigue. However, in spite of continuous supplying of oral calcium carbonate, 3 g/day, and oral vitamin D, 0.5 μg/day, serum calcium concentration was not improved as much with 4.68 mg/dl of corrected calcium concentration in 2 weeks after the hospital visit. In the follow up examination performed in out-patient clinic after discharging from the hospital, serum creatinine concentration was 3.14 mg/dl and calcium concentration was 7.2 mg/dl (4 weeks after the symptom occurrence) and 9.3 mg/dl (4 months after the symptom occurrence) (Fig. 2). DISCUSSION Bisphosphonates are generally considered as safe drugs but, can be associated with laboratory abnormalities, particularly, elevated serum creatinine levels and hypocalcemia.[1] Sporadic episodes of acute and subacute renal failure have been reported, whereas hypocalcemia has not yet been the subject of detailed research. Theoretically, intravenous bisphosphonate guarantees 100% absorption without gastrointestinal adverse effects thereby advantageous over oral bisphosphonate. Particularly, zoledronate has gained popularity as an osteoporosis treatment since its injection time (15 minutes) is shorter than that of other intravenous bisphosphonates and the injection is performed only once a year. Maximum plasma concentrations of zoledronic acid are reached, as expected, at the end of the IV infusion. Blood levels then rapidly decline to less than 10% at four hours and to less than 1% at 24 hours after infusion. Half-life is known to be as long as 146 hours.[2] About 61% of the administered dose is taken up rapidly by bone tissue, tending to localize in areas of increased turnover rate, and is then slowly released back into the circulation. The remaining 39% is excreted unchanged via glomerular filtration by the kidneys. Zoledronic acid administration is not recommended in those with a creatinine clearance below 35 ml/min. There is no need to adjust the dose in patients who have a creatinine clearance of 35 ml/min or higher. Zoledronic acid does not inhibit the P450 enzyme, and there is therefore no interaction with other medications metabolized via cytochrome P450. However, caution should be exercised in patients on medications that have the potential of reducing the serum calcium level, such as loop diuretics and aminoglycosides, and potentially nephrotoxic medications, such as nonsteroidal anti-inflammatory drugs. In the literature, there is well-known direct association between the risk for renal failure and drug infusion time and dose. High-dose (8 mg i.v.) with a short infusion time (5 minutes) is strongly nephrotoxic. In contrast, using the recommended infusion time and dosage (15 minutes and 4 mg i.v., respectively), this drug showed a favorable renal safety profile, comparable with that of placebo.[3,4] Hypocalcemia is defined as a serum level of total calcium lower than 8.5 mg/dl (2.12 mmol/l). Calcium is mostly (99%) distributed in bone but serum calcium exists in three forms: (1) free or ionized calcium, the physiologically active form (50%); (2) calcium complexed to anions, including bicarbonate, lactate, phosphate, and citrate (10%); and (3) 141
4 J Bone Metab as calcium bound to plasma proteins (40%). Since approximately 80% of the protein-bound calcium fraction is associated with albumin, serum albumin can affect serum calcium level if the serum albumin is abnormally high or low. Therefore, in order to diagnose hypocalcemia accurately, serum albumin concentration should be measured first and then, based upon the measured albumin concentration calcium level should be corrected or biologically important ionized calcium concentration should be measured. Bisphosphonates are potent inhibitors of osteoclastic bone resorption. Such inhibition reduces calcium efflux from bone, which is normally followed by a transient period of slight hypocalcemia. Most patients do not become hypocalcemic because of compensatory mechanisms, the most important of which is increased secretion of PTH.[5] If serum calcium level decreases, formation of 1,25- dihydroxyvitamin D increases due to compensatory increase of PTH. Calcium reabsorption in distal renal tubule of kidney and calcium absorption in small intestine increase thereby preventing persistent hypocalcemia. Disease states that impair these compensatory mechanisms can potentially lead to hypocalcemia after bisphosphonate use. In other words, when surgical hypoparathyroidism, hypomagnesemic hypoparathyroidism, and pre-existing secondary hyperparathyroidism are present, it can cause restriction in compensatory increase of PTH. Hypocalcemia also occurs in case of vitamin D deficiency. Moreover, the clearance of bisphosphonates is reduced in patients with impaired renal function, possibly leading to greater delivery to bone remodeling sites and to prolonged antiresorptive action. In patients with severe renal dysfunction, the combination of retained bisphosphonate and impaired intestinal calcium absorption attributable to decreased production of 1,25- dihydroxyvitamin D could potentially exaggerate the risk of developing hypocalcemia. It has been known that the potency of bisphosphonate is somewhat involved as well.[5] The first case of bisphosphonate-associated symptomatic hypocalcemia was reported in 1987,[6] the case was associated with the use of pamidronate. And then reports of hypocalcemia associated with the use of alendronate[7] and risedronate[8] were followed. In the study performed by Conte et al.,[9] hypocalcemia was observed in 17% of patients out of 143 patients who were injected intravenously with pamidronate in order to treat bone metastasis of breast cancer, but all of them were asymptomatic. It is known that zoledronate is 100-1,000 times stronger than alendronate, risedronate, and pamidronate so that the risk of hypocalcemia is considered to be higher as well due to the strong effectiveness. There are several studies done investigating incidence of zoledronate-induced hypocalcemia. Saad et al.[4] reported that severe hypocalcemia was exhibited in 2% of the patients and Kohno et al.[10] reported high incidence (39%) of hypocalcemia but no severe cases were present. Lyles et al.[11] reported that only 0.3% patients showed hypocalcemia and considered that this might be due to vitamin D loading before the utilization of zoledronate. Impaired renal function and vitamin D deficiency are the most significant risk factors in hypocalcemia occurrence. Besides, hypoparathyroidism and hypomagnesemia were significant risk factors as well.[12] Furthermore, simultaneous injection of steroid, pre-existing hypocalcemia, and bone metastasis in more than 3 places had also reported as the risk factors of bisphosphonate-induced hypocalcemia.[13] In case of the patient in our study, PTH level was elevated already. Although serum 1,25-dihydroxyvitamin D level was not measured in advance but we can guess formation of 1,25-dihydroxyvitamin D must be reduced due to impaired renal function. Then, calcium absorption in small intestine also decreased. In result, the inadequate compensatory mechanism and prolonged action of bisphosphonate caused severe hypocalcemia regardless of oral calcium supply. Diagnosis and treatment of osteoporosis in patients with impaired renal function have not defined certainly yet. National Kidney Foundation (NKF)-Kidney Disease Outcomes Quality Initiative (K/DOQI) classifies chronic kidney disease (CKD) into 5 stages based upon degree of glomerular filtration rate (GFR) and recommends treatment and prognosis determination by each stage. Bone diseases are accompanied in many patients with CKD, called renal 142
5 osteodystrophy. Renal osteodystrophy is roughly classified into 3 types; 1) high turn-over diseases with main histological finding of osteitis fibrosa caused by hyperparathyroidism, 2) low turn-over diseases including osteomalacia caused by aluminum toxicity or adynamic bone disease caused by excessive suppression of PTH, and 3) a mixed type including characteristics of both osteitis fibrosa and osteomalacia.[14] It has been known that all three types can decrease BMD and increase the risk of fractures. Therefore, in diagnosis of osteoporosis in CKD patients with decreased BMD, renal osteodystrophy should be excluded by biochemical parameters and clinical aspects, however, bone biopsy should be performed to confirm the diagnosis. If osteoporosis is diagnosed only by using examination of BMD and treated with bisphosphonate, low turn-over bone diseases could be included and get worse thereby requesting more attention. In spite of concerns regarding the safety of bisphosphonate in CKD, some studies have also mentioned that utilization is too limited[15] because bisphosphonate is effective to decrease the risk of fractures in the patients with CKD and the frequency of side effects is quite low. Also, studies including CKD patients who had severely impaired renal function with 15 ml/min of GFR reported that alendronate[16] and risedronate[17] reduced the risk of fractures effectively without increase of side effects including nephrotoxicity. Although it is still controversial, given the multiple literatures regarding use of bisphosphonate in CKD patients with reduced BMD,[15,18,19] in CKD stage 1-3 patients without abnormal biochemical parameters, bisphosphonate can be used as it is for the treatment in patients with normal renal function because patients in these stages represent more frequent osteoporosis, rather than renal osteodystrophy and bisphosphonate is relatively safe. In case of CKD stage 4 and 5, there are not so many studies done and frequency of renal osteodystrophy is high in these stages so that condition of each patient should be evaluated with various perspectives in order to utilize bisphosphonate. Performing bone biopsy ahead of time is the best option. Mostly, for CKD stage 4 patients with high risk of fractures, oral drugs with recommended dosage can be given and intravenous drugs can be injected 2 times slower than that of recommended injection rate. For CKD stage 5 patients with fractures, dosage of oral drugs should be reduced by half of the recommended dosage and utilized for less than 3 years and the intravenous drugs should be injected 4 times slower than that of recommended rate. In the present case, the estimated GFR was 17 ml/min using equation of Modification of Diet in Renal Disease (MDRD) based upon serum creatinine measured at the time of femur fracture. Therefore, the patient corresponded to CKD stage 4 and high risk group since she was an elderly female patient with fracture. PTH level was pg/ml. It is difficult to classify renal osteodystrophy based upon clinical or biochemical aspects in general, however, studies reported that low turn-over disease such as adynamic bone disease is rare before CKD stage 5 and the case with less than 150 pg/ml of PTH is useful as a parameter of low turn-over disease (sensitivity 78.1%, specificity 76.2%).[20] Based upon these results, chance to have low turn-over diseases is considered to be low in this patient so bisphosphonate treatment can be considered. However, reduction in BMD of the patient in the present case is highly considered to be caused by renal osteodystrophy rather than simple osteoporosis. As the patient showed elevated PTH level, vitamin D concentration should have been measured in advance and vitamin D and calcium should have been given. Then, more attention should have been paid on drug selection and treatment determination. If treatment with oral drugs was considered or zoledronate was injected intravenously more than 2 times slower than that of the recommended injection rate of people with normal renal function, serious hypocalcemia could have been prevented. In conclusion, there has been no specific guideline established preventing the occurrence of hypocalcemia yet in spite of a wide range of bisphosphonate utilization. Given the many studies performed previously, when bisphosphonate is administered in the patients with osteoporosis, evaluation regarding renal function, presence or absence of vitamin D deficiency, parathyroid gland function, serum 143
6 J Bone Metab calcium, and levels of phosphorus and magnesium are needed in advance. Proper supply of calcium and vitamin D is requested in accordance with bisphosphonate injection and calcium and creatinine levels should be measured periodically. If hypocalcemia is suspicious, albumin concentration should be examined and then appropriate treatment should be carried out. In addition, when patients had impaired renal function, GFR is mandatory to calculate and the risk of fractures and presence or absence of renal osteodystrophy is required to be evaluated. Then, whether or not to inject bisphosphonate should be determined carefully. REFERENCES 1. Papapetrou PD. Bisphosphonate-associated adverse events. Hormones (Athens) 2009;8: Hamdy RC. Zoledronic acid: clinical utility and patient considerations in osteoporosis and low bone mass. Drug Des Devel Ther 2010;4: Rosen LS, Gordon D, Tchekmedyian S, et al. Zoledronic acid versus placebo in the treatment of skeletal metastases in patients with lung cancer and other solid tumors: a phase III, double-blind, randomized trial--the Zoledronic Acid Lung Cancer and Other Solid Tumors Study Group. J Clin Oncol 2003;21: Saad F, Gleason DM, Murray R, et al. A randomized, placebo-controlled trial of zoledronic acid in patients with hormone-refractory metastatic prostate carcinoma. J Natl Cancer Inst 2002;94: Peter R, Mishra V, Fraser WD. Severe hypocalcaemia after being given intravenous bisphosphonate. BMJ 2004;328: Jodrell DI, Iveson TJ, Smith IE. Symptomatic hypocalcaemia after treatment with high-dose aminohydroxypropylidene diphosphonate. Lancet 1987;1: Chesnut CH, 3rd, McClung MR, Ensrud KE, et al. Alendronate treatment of the postmenopausal osteoporotic woman: effect of multiple dosages on bone mass and bone remodeling. Am J Med 1995;99: Mortensen L, Charles P, Bekker PJ, et al. Risedronate increases bone mass in an early postmenopausal population: two years of treatment plus one year of follow-up. J Clin Endocrinol Metab 1998;83: Conte PF, Latreille J, Mauriac L, et al. Delay in progression of bone metastases in breast cancer patients treated with intravenous pamidronate: results from a multinational randomized controlled trial. The Aredia Multinational Cooperative Group. J Clin Oncol 1996;14: Kohno N, Aogi K, Minami H, et al. Zoledronic acid significantly reduces skeletal complications compared with placebo in Japanese women with bone metastases from breast cancer: a randomized, placebo-controlled trial. J Clin Oncol 2005;23: Lyles KW, Colón-Emeric CS, Magaziner JS, et al. Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 2007;357: Maalouf NM, Heller HJ, Odvina CV, et al. Bisphosphonateinduced hypocalcemia: report of 3 cases and review of literature. Endocr Pract 2006;12: Hanamura M, Iwamoto T, Soga N, et al. Risk factors contributing to the development of hypocalcemia after zoledronic acid administration in patients with bone metastases of solid tumor. Biol Pharm Bull 2010;33: Malluche H, Faugere MC. Renal bone disease 1990: an unmet challenge for the nephrologist. Kidney Int 1990;38: Courtney AE, Maxwell AP. Chronic kidney disease and bisphosphonate treatment: are prescribing guidelines unnecessarily restrictive? Postgrad Med J 2009;85: Jamal SA, Bauer DC, Ensrud KE, et al. Alendronate treatment in women with normal to severely impaired renal function: an analysis of the fracture intervention trial. J Bone Miner Res 2007;22: Miller PD, Roux C, Boonen S, et al. Safety and efficacy of risedronate in patients with age-related reduced renal function as estimated by the Cockcroft and Gault method: a pooled analysis of nine clinical trials. J Bone Miner Res 2005;20: Toussaint ND, Elder GJ, Kerr PG. Bisphosphonates in chronic kidney disease; balancing potential benefits and adverse effects on bone and soft tissue. Clin J Am Soc Nephrol 2009;4: Miller PD. The kidney and bisphosphonates. Bone 2011;49: 144
7 Couttenye MM, D'Haese PC, Deng JT, et al. High prevalence of adynamic bone disease diagnosed by biochemical markers in a wide sample of the European CAPD population. Nephrol Dial Transplant 1997;12:
Bone Disorders in CKD
 Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Metabolic Bone Disease Related to Chronic Kidney Disease
 Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Vol. 19, Bulletin No. 108 August-September 2012 Also in the Bulletin: Denosumab 120mg for Bone Metastases
 ה מ ר א פ הביטאון לענייני תרופות ISRAEL DRUG BULLETIN 19 years of unbiased and independent drug information P H A R x M A Vol. 19, Bulletin No. 108 August-September 2012 Also in the Bulletin: Denosumab
ה מ ר א פ הביטאון לענייני תרופות ISRAEL DRUG BULLETIN 19 years of unbiased and independent drug information P H A R x M A Vol. 19, Bulletin No. 108 August-September 2012 Also in the Bulletin: Denosumab
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Chapter 5: Evaluation and treatment of kidney transplant bone disease Kidney International (2009) 76 (Suppl 113), S100 S110; doi: /ki.2009.
 http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP
 Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
Horizon Scanning Technology Briefing. Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal. National Horizon Scanning Centre
 Horizon Scanning Technology Briefing National Horizon Scanning Centre Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal osteoporosis December 2006 This technology summary is based on information
Horizon Scanning Technology Briefing National Horizon Scanning Centre Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal osteoporosis December 2006 This technology summary is based on information
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
CKD-MBD CKD mineral bone disorder
 CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
Scottish Medicines Consortium
 Scottish Medicines Consortium zoledronic acid 5mg/100ml solution for infusion (Aclasta) No. (317/06) Novartis 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium zoledronic acid 5mg/100ml solution for infusion (Aclasta) No. (317/06) Novartis 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Bone Metastases. Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital
 Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Pharmacy Management Drug Policy
 Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
A Case of Cushing Syndrome Diagnosed by Recurrent Pathologic Fractures in a Young Woman
 A Case of Cushing Syndrome Diagnosed by Recurrent Pathologic Fractures in a Young Woman JY Han, et al CASE REPORT http://dx.doi.org/10.11005/jbm.2012.19.2.153 Vol. 19, No. 2, 2012 A Case of Cushing Syndrome
A Case of Cushing Syndrome Diagnosed by Recurrent Pathologic Fractures in a Young Woman JY Han, et al CASE REPORT http://dx.doi.org/10.11005/jbm.2012.19.2.153 Vol. 19, No. 2, 2012 A Case of Cushing Syndrome
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Effective Health Care
 Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Name of Policy: Zoledronic Acid (Reclast ) Injection
 Name of Policy: Zoledronic Acid (Reclast ) Injection Policy #: 355 Latest Review Date: May 2011 Category: Pharmacy Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
Name of Policy: Zoledronic Acid (Reclast ) Injection Policy #: 355 Latest Review Date: May 2011 Category: Pharmacy Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
Diagnosis and Treatment of Osteoporosis. Department of Endocrinology and Metabolism Ajou University School of Medicine.
 Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Spontaneous Non-Traumatic Stress Fractures in Bilateral Femoral Shafts in a Patient Treated with Bisphosphonates
 case report korean j intern med 2012;27:98-102 pissn 1226-3303 eissn 2005-6648 Spontaneous Non-Traumatic Stress Fractures in Bilateral Femoral Shafts in a Patient Treated with Bisphosphonates Dong Yeob
case report korean j intern med 2012;27:98-102 pissn 1226-3303 eissn 2005-6648 Spontaneous Non-Traumatic Stress Fractures in Bilateral Femoral Shafts in a Patient Treated with Bisphosphonates Dong Yeob
BONEFOS 800 mg. Bonefos adalah obat baru yang terdaftar tahun Informasi di bawah ini merupakan informasi update tahun 2008.
 Bonefos adalah obat baru yang terdaftar tahun 2007. Informasi di bawah ini merupakan informasi update tahun 2008. BONEFOS 800 mg Important information, please read carefully! Composition 1 tablet contains
Bonefos adalah obat baru yang terdaftar tahun 2007. Informasi di bawah ini merupakan informasi update tahun 2008. BONEFOS 800 mg Important information, please read carefully! Composition 1 tablet contains
Agents that Affect Bone & Mineral Homeostasis
 Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
What is Osteoporosis?
 What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016
 Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Osteoporosis and Chronic Kidney Disease: Diagnosis and Treatment Recommendations
 Osteoporosis and Chronic Kidney Disease: Diagnosis and Treatment Recommendations Nancy E. Lane, MD Director, Center for Musculoskeletal Health Endowed Professor of Medicine and Rheumatology University
Osteoporosis and Chronic Kidney Disease: Diagnosis and Treatment Recommendations Nancy E. Lane, MD Director, Center for Musculoskeletal Health Endowed Professor of Medicine and Rheumatology University
Bone Disease after Kidney Transplantation
 Bone Disease after Kidney Transplantation BTS March 2018 Dr Arif Khwaja PhD, FRCP Sheffield Kidney Institute Clinical case 47 year old female FSGS DBD 2007 egfr 25mls/min. Sirolimus, Azathioprine and prednisolone
Bone Disease after Kidney Transplantation BTS March 2018 Dr Arif Khwaja PhD, FRCP Sheffield Kidney Institute Clinical case 47 year old female FSGS DBD 2007 egfr 25mls/min. Sirolimus, Azathioprine and prednisolone
The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
CASE 1 WHY IS IT IMPORTANT TO TREAT? FACTS CONCERNS
 4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
GUIDELINES ON THE USE OF BISPHOSPHONATES IN PALLIATIVE CARE. November 2007(Amended July 2008)
 Yorkshire Palliative Medicine Clinical Guidelines Group GUIDELINES ON THE USE OF BISPHOSPHONATES IN PALLIATIVE CARE November 2007(Amended July 2008) Authors: Dr Kath Lambert and Dr Liz Brown, on behalf
Yorkshire Palliative Medicine Clinical Guidelines Group GUIDELINES ON THE USE OF BISPHOSPHONATES IN PALLIATIVE CARE November 2007(Amended July 2008) Authors: Dr Kath Lambert and Dr Liz Brown, on behalf
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience
 Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Bisphosphonates in the Management of. Myeloma Bone Disease
 Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Osteoporosis. Overview
 v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE. Lydia Au Geriatrics Ng Teng Fong Hospital
 OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE Lydia Au Geriatrics Ng Teng Fong Hospital LET S START WITH WHAT YOU WANT TO KNOW AND DO WITH A VERT FRACTURE Vertebral fractures Most common (550K
OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE Lydia Au Geriatrics Ng Teng Fong Hospital LET S START WITH WHAT YOU WANT TO KNOW AND DO WITH A VERT FRACTURE Vertebral fractures Most common (550K
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis Treatment Overview. Colton Larson RFUMS October 26, 2018
 Osteoporosis Treatment Overview Colton Larson RFUMS October 26, 2018 Burden of Disease Most common bone disease 9.9 million Americans + 43.1 million Americans have low bone mineral density (BMD) Stealthy
Osteoporosis Treatment Overview Colton Larson RFUMS October 26, 2018 Burden of Disease Most common bone disease 9.9 million Americans + 43.1 million Americans have low bone mineral density (BMD) Stealthy
Name of Policy: Boniva (Ibandronate Sodium) Infusion
 Name of Policy: Boniva (Ibandronate Sodium) Infusion Policy #: 266 Latest Review Date: April 2010 Category: Pharmacology Policy Grade: Active Policy but no longer scheduled for regular literature reviews
Name of Policy: Boniva (Ibandronate Sodium) Infusion Policy #: 266 Latest Review Date: April 2010 Category: Pharmacology Policy Grade: Active Policy but no longer scheduled for regular literature reviews
Management of postmenopausal osteoporosis
 Management of postmenopausal osteoporosis Yeap SS, Hew FL, Chan SP, on behalf of the Malaysian Osteoporosis Society Committee Working Group for the Clinical Guidance on the Management of Osteoporosis,
Management of postmenopausal osteoporosis Yeap SS, Hew FL, Chan SP, on behalf of the Malaysian Osteoporosis Society Committee Working Group for the Clinical Guidance on the Management of Osteoporosis,
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
OSTEOPOROSIS: PREVENTION AND MANAGEMENT
 OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Download slides:
 Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
DENOSUMAB (PROLIA & XGEVA )
 DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
Clinician s Guide to Prevention and Treatment of Osteoporosis
 Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
Zainab Al-dabi - Shahd Alqudah - Dr. Malik
 - 4 - Zainab Al-dabi - Shahd Alqudah - Dr. Malik 1 In the USA there are 10 million cases of osteoporosis, most of which belong to women, this represents 3-4% of the population which is a relatively high
- 4 - Zainab Al-dabi - Shahd Alqudah - Dr. Malik 1 In the USA there are 10 million cases of osteoporosis, most of which belong to women, this represents 3-4% of the population which is a relatively high
Kristen M. Nebel, DO PENN/ LGHP Geriatrics. Temple Family Medicine Review
 Kristen M. Nebel, DO PENN/ LGHP Geriatrics 10/3/17 Temple Family Medicine Review OBJECTIVES Define Revised 2017 American College of Physician Recommendations Screening, Prevention and Treatment Application
Kristen M. Nebel, DO PENN/ LGHP Geriatrics 10/3/17 Temple Family Medicine Review OBJECTIVES Define Revised 2017 American College of Physician Recommendations Screening, Prevention and Treatment Application
Posttransplant Bone Disease. Budapest 2007
 Posttransplant Bone Disease Budapest 2007 Post-transplant bone disease 7 10 % of kidney transplanted patients develope a fracture. The risk is higher in postmenopausal female transplanted patients. Diabetic,
Posttransplant Bone Disease Budapest 2007 Post-transplant bone disease 7 10 % of kidney transplanted patients develope a fracture. The risk is higher in postmenopausal female transplanted patients. Diabetic,
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
A Case of Acquired Fanconi Syndrome Induced by Zoledronic Acid
 CASE REPORT A Case of Acquired Fanconi Syndrome Induced by Zoledronic Acid Tetsuhiro Yoshinami, Toshinari Yagi, Daisuke Sakai, Naotoshi Sugimoto and Fumio Imamura Abstract A 61-year-old woman with metastatic
CASE REPORT A Case of Acquired Fanconi Syndrome Induced by Zoledronic Acid Tetsuhiro Yoshinami, Toshinari Yagi, Daisuke Sakai, Naotoshi Sugimoto and Fumio Imamura Abstract A 61-year-old woman with metastatic
Management of mineral and bone disorders in renal transplant recipients
 Nephrology 22, Suppl. 2 (2017) 65 69 Management of mineral and bone disorders in renal transplant recipients MATTHEW J DAMASIEWICZ 1,3 and PETER R EBELING 2,3,4 Departments of 1 Nephrology, and 2 Endocrinology,
Nephrology 22, Suppl. 2 (2017) 65 69 Management of mineral and bone disorders in renal transplant recipients MATTHEW J DAMASIEWICZ 1,3 and PETER R EBELING 2,3,4 Departments of 1 Nephrology, and 2 Endocrinology,
Head and Neck Endocrine Surgery
 Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
HOW I DO IT. Introduction. BARKIN J. How I Do It: Managing bone health in patients with prostate cancer. Can J Urol 2014;21(4):
 HOW I DO IT How I Do It: Managing bone health in patients with prostate cancer Jack Barkin, MD Department of Surgery, University of Toronto, Humber River Hospital, Toronto, Ontario, Canada BARKIN J. How
HOW I DO IT How I Do It: Managing bone health in patients with prostate cancer Jack Barkin, MD Department of Surgery, University of Toronto, Humber River Hospital, Toronto, Ontario, Canada BARKIN J. How
NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT
 NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF OSTEOPOROSIS: OVERVIEW Definitions Risk factors
NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF OSTEOPOROSIS: OVERVIEW Definitions Risk factors
Fragile Bones and how to recognise them. Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey
 Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Current and Emerging Strategies for Osteoporosis
 Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Overview. Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases. People Centred Positive Compassion Excellence
 Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Osteoporosis. Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective. Old Definition of Osteoporosis
 Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Guidelines and new evidence on CKD - MBD treatment
 Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
Guideline for the investigation and management of osteoporosis. for hospitals and General Practice
 Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
Bone Health in Celiac Disease. Partha S. Sinha MD, PhD October 29 th, 2017
 Bone Health in Celiac Disease Partha S. Sinha MD, PhD October 29 th, 2017 No Disclosures Objectives Recognize the mechanisms by which celiac disease can affect bone health Review what diagnostic tests
Bone Health in Celiac Disease Partha S. Sinha MD, PhD October 29 th, 2017 No Disclosures Objectives Recognize the mechanisms by which celiac disease can affect bone health Review what diagnostic tests
Clinical Study Effect of Zoledronic Acid on Bone Mineral Density in Men with Prostate Cancer Receiving Gonadotropin-Releasing Hormone Analog
 Hindawi Publishing Corporation Prostate Cancer Volume 2, Article ID 7664, 7 pages doi:.55/2/7664 Clinical Study Effect of Zoledronic Acid on Bone Mineral Density in Men with Prostate Cancer Receiving Gonadotropin-Releasing
Hindawi Publishing Corporation Prostate Cancer Volume 2, Article ID 7664, 7 pages doi:.55/2/7664 Clinical Study Effect of Zoledronic Acid on Bone Mineral Density in Men with Prostate Cancer Receiving Gonadotropin-Releasing
Controversies in Osteoporosis Management
 Controversies in Osteoporosis Management 2018 Northwest Rheumatism Society Meeting Portland, OR April 28, 2018 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Institute
Controversies in Osteoporosis Management 2018 Northwest Rheumatism Society Meeting Portland, OR April 28, 2018 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Institute
What is the right calcium balance?
 For patients with hypoparathyroidism What is the right calcium balance? Indications and Usage1 NATPARA is a parathyroid hormone indicated as an adjunct to calcium and vitamin D to control hypocalcemia
For patients with hypoparathyroidism What is the right calcium balance? Indications and Usage1 NATPARA is a parathyroid hormone indicated as an adjunct to calcium and vitamin D to control hypocalcemia
Case 4 Generalised bone pain
 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Misuse of Bisphosphonates. Dr Rukhsana Parvin Associate Professor Department of Medicine Enam Medical College & Hospital
 Misuse of Bisphosphonates Dr Rukhsana Parvin Associate Professor Department of Medicine Enam Medical College & Hospital Introduction Bisphosphonates are chemically stable analogues of pyrophosphate compounds.
Misuse of Bisphosphonates Dr Rukhsana Parvin Associate Professor Department of Medicine Enam Medical College & Hospital Introduction Bisphosphonates are chemically stable analogues of pyrophosphate compounds.
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
TREATMENT OF OSTEOPOROSIS
 TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
Elderly men with prostate cancer + ADT
 Elderly men with prostate cancer + ADT Background and Rationale ADT and Osteoporosis Proportion of Patients With Fractures 1-5 Yrs After Cancer Diagnosis 21 18 +6.8%; P
Elderly men with prostate cancer + ADT Background and Rationale ADT and Osteoporosis Proportion of Patients With Fractures 1-5 Yrs After Cancer Diagnosis 21 18 +6.8%; P
Zoledasta injection solution for infusion. 1-hydroxy-2-(1H-imidazol-1-yl)ethane-1,1-diphosphonic acid monohydrate
 Zoledasta injection solution for infusion NAME OF THE MEDICINE Zoledronic acid (as monohydrate) Chemical Name: 1-hydroxy-2-(1H-imidazol-1-yl)ethane-1,1-diphosphonic acid monohydrate Structural Formula:
Zoledasta injection solution for infusion NAME OF THE MEDICINE Zoledronic acid (as monohydrate) Chemical Name: 1-hydroxy-2-(1H-imidazol-1-yl)ethane-1,1-diphosphonic acid monohydrate Structural Formula:
Oral Alendronate Vs. Three-Monthly Iv Ibandronate In The Treatment Of Postmenopausal Osteoporosis
 Oral Alendronate Vs. Three-Monthly Iv Ibandronate In The Treatment Of Postmenopausal Osteoporosis Miriam Silverberg A. Study Purpose and Rationale More than 70% of fractures in people after the age of
Oral Alendronate Vs. Three-Monthly Iv Ibandronate In The Treatment Of Postmenopausal Osteoporosis Miriam Silverberg A. Study Purpose and Rationale More than 70% of fractures in people after the age of
Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss. A Publication of The Bone and Cancer Foundation
 Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss A Publication of The Bone and Cancer Foundation Contents This publication includes important information about
Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss A Publication of The Bone and Cancer Foundation Contents This publication includes important information about
Bone Densitometry Pathway
 Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Cinacalcet treatment in advanced CKD - is it justified?
 Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Assessment and Treatment of Osteoporosis Professor T.Masud
 Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Relationship between Decrease in Serum Sodium Level and Bone Mineral Density in Osteoporotic Fracture Patients
 J Bone Metab 2015;22:9-15 http://dx.doi.org/10.11005/jbm.2015.22.1.9 pissn 2287-6375 eissn 2287-7029 Original Article Relationship between Decrease in Serum Sodium Level and Bone Mineral Density in Osteoporotic
J Bone Metab 2015;22:9-15 http://dx.doi.org/10.11005/jbm.2015.22.1.9 pissn 2287-6375 eissn 2287-7029 Original Article Relationship between Decrease in Serum Sodium Level and Bone Mineral Density in Osteoporotic
Arizona Chapter AACE Paul D. Miller, M.D.
 Arizona Chapter AACE Paul D. Miller, M.D. Management of fractures in CKD and atypical subtrochanteric femur fractures September 2018 Paul D. Miller, M.D. Disclosures: Amgen (Consultant, Advisory Board,
Arizona Chapter AACE Paul D. Miller, M.D. Management of fractures in CKD and atypical subtrochanteric femur fractures September 2018 Paul D. Miller, M.D. Disclosures: Amgen (Consultant, Advisory Board,
Patients should receive supplemental calcium and vitamin D, if dietary intake is inadequate (see PRECAUTIONS).
 PRODUCT CIRCULAR Tablets Once Weekly 70 mg I. THERAPEUTIC CLASS Bisphosphonates are synthetic analogs of pyrophosphate that bind to the hydroxyapatite found in bone. is a bisphosphonate that acts as a
PRODUCT CIRCULAR Tablets Once Weekly 70 mg I. THERAPEUTIC CLASS Bisphosphonates are synthetic analogs of pyrophosphate that bind to the hydroxyapatite found in bone. is a bisphosphonate that acts as a
ACLASTA zoledronic acid
 1 ACLASTA zoledronic acid NAME OF THE MEDICINE The active ingredient of Aclasta is a bisphosphonate, zoledronic acid, or 1-hydroxy- 2-(1H-imidazol-1-yl)ethane-1,1-diphosphonic acid. Although zoledronic
1 ACLASTA zoledronic acid NAME OF THE MEDICINE The active ingredient of Aclasta is a bisphosphonate, zoledronic acid, or 1-hydroxy- 2-(1H-imidazol-1-yl)ethane-1,1-diphosphonic acid. Although zoledronic
Osteoporosis - New Guidelines. Michelle Glass B.Sc. (Pharm) June 15, 2011
 Osteoporosis - New Guidelines Michelle Glass B.Sc. (Pharm) June 15, 2011 Outline What is Osteoporosis? Who is at risk? What treatments are available? Role of the Pharmacy technician Definition of Osteoporosis
Osteoporosis - New Guidelines Michelle Glass B.Sc. (Pharm) June 15, 2011 Outline What is Osteoporosis? Who is at risk? What treatments are available? Role of the Pharmacy technician Definition of Osteoporosis
