CLINICAL PRACTICE ARTICLE Atypical presentations and treatment variations of pelvic congestion syndrome: A four patient case series
|
|
|
- Ashlynn Wiggins
- 5 years ago
- Views:
Transcription
1 CLINICAL PRACTICE ARTICLE Atypical presentations and treatment variations of pelvic congestion syndrome: A four patient case series David Greuner, Andrew Amorosso New York City Surgical Associates Surgical Group, New York, New York, 10022, USA, Arno Rotgans, Chris Hollingsworth, Adam Tonis v1 First published: N/A, N/A: N/A (doi: N/A) Latest published: N/A, N/A: N/A (doi: N/A) Open Peer Review Abstract This is a retrospective case review of four patients randomly selected from a pool of 43 patients who presented to our practice with historically atypical symptoms for pelvic congestion syndrome, and the treatment they received. These 43 patients were treated between June and December of Each patient presented with various atypical symptoms including chronic lower back pain, urinary frequency and incontinence, hip pain, tenesmus, and uncontrollable flatulence. Diagnostic abdominal and pelvic duplex ultrasound and fluoroscopic venography was performed on all patients with informed consent. The four selected patients for this study were all positive for pelvic venous reflux, pelvic venous insufficiency and ovarian/gonadal vein reflux and varicosities. All four of the patients selected in this retrospective study were examined at 1 week from date of intervention and again at 1 month from date of intervention. At the 1 week postoperative exam all four patients had experienced significant resolution of their symptoms, although all had residual congestion present on their right side. After re-intervention to treat right sided congestion via the right gonadal vein, at the 1 month postoperative exam all four patients had experienced an almost complete resolution of symptoms. Referee Status: AWAITING PEER REVIEW Discuss this article Comments (0) Corresponding author: Andrew Amorosso ( aamorosso@nycsurgical.net) How to cite this article: Greuner D, Amorosso A, Rotgans A et al. Atypical presentations and treatment variations of pelvic congestion syndrome: A four patient case series F1000Research, : (doi: $version.doi) Copyright: 2016 Greuner D et al. This is an open access article distributed under the terms of the Creative Commons Attribution Licence, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Grant information: The author(s) declared that no grants were involved in supporting this work. Competing interests: No competing interests were disclosed. First published: N/A, N/A: N/A (doi: N/A) F1000Research Page 1 of 7
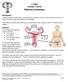
2 Introduction Pelvic congestion syndrome (PCS) presents as a constellation of symptoms all caused by the development of varicosities in veins typically drained by either the ovarian or internal iliac veins. Its typical presentation is one of noncyclical dull, aching pelvic pain, typically unilateral, and persisting for more than 6 months. It was present in all patients in our series. Other symptoms that are commonly associated with the condition include dysmenorrhea and dyspareunia, seen respectively in case 1 and 4, and to some degree in all patients in our series. Our experience has shown us that many authentic pelvic congestion syndrome diagnoses are being lost in a newfound reliance on cross sectional imaging as a diagnostic measure. We have found that to truly diagnose active pelvic congestion syndrome and treat the patient s correlating symptomatic disease, the gold standard diagnostic imaging modality is fluoroscopic venography. In the following four cases you will read about patients who presented at our practice with historically atypical symptoms for pelvic congestion. After our suspicions were confirmed with duplex sonography revealing ovarian vein reflux and/or pelvic varicosities each patient underwent a fluoroscopic venogram and the appropriate image guided treatment. Although all of these patients presented with symptoms that are not indicative of pelvic congestion, all patients did indeed have advanced pelvic congestion. When each patient was treated for their specific disease state in the pelvic congestion syndrome treatment spectrum all symptoms resolved. Our intention is that the documentation of this experience will help other clinicians in their vigilance to rule out pelvic congestion syndrome with fluoroscopic venography before starting patients on a long road to a differential diagnosis. Case 1: Hip pain A 61-year-old female with two children presented to our clinic with a chief complaint of left hip pain for 5 years, as well as pain in her lower back and pelvis, dysmenorrhea, and urinary frequency present for 2 years. Her hip pain was dull and aching in quality, though severe enough to interfere with exercise. She denied paresthesia radiating from her back down into either thigh, and she denied any history of prior trauma to the area. The patient had been seen both by orthopedists and pain management specialists, and both an MRI and a bone scan failed to pinpoint an etiology. She had taken non-steroidal anti-inflammatory drug (NSAID) regimens, systemic corticosteroids, and ultrasound-guided steroid injections without any improvement in her pain. The patient s past medical history was also notable for chronic venous insufficiency refractory to conservative and operative management, with endovenous thermal ablation therapy for the great saphenous veins in both legs. Three months after operative treatment, the patient reported continued pain, heaviness, fatigue, throbbing, cramping, and edema in both legs, aggravated by prolonged standing, and consistent with persistent chronic venous insufficiency. On physical examination, the lower extremities were remarkable for spider veins, reticular veins, varicose veins, and mild pigmentation in her ankles and calves. Infragluteal varices were present. There was some mild pitting edema present, around the ankle and calf bilaterally. A duplex sonogram was performed on both the pelvis and lower extremities. On sonographic examination of her pelvis, reflux was noted in her pelvic veins. In the legs, persistent reflux was noted in superficial veins in both legs. A fluoroscopic venogram was performed on the patient, with access obtained at the right common femoral vein. The study noted significant reflux in both internal iliac veins and reflux and stenosis in the left common iliac vein. Delayed washout of contrast was seen in the cross-pelvic collaterals of the tributaries off the internal iliac veins. Most notably, significant varicosities with delayed contrast washout were seen extending off the left ovarian vein (Figure 1) and communicating with the internal iliac veins. The varicose Figure 1. Pre-embolization fluoroscopic venogram showing reflux in ovarian vein. Page 2 of 7
3 circulation form the refluxing left gonadal vein included prominent lateral extension towards the left side of the patient. Embolization of the left ovarian vein and collaterals from both internal iliac veins was performed. Post-embolization venography performed immediately after demonstrated successful closure of these refluxing venous branches. The patient s post-procedure course was uneventful. When seen again in our clinic 8 days later, her symptoms were significantly improved. Her hip pain had almost completely resolved, and at her 4 week post-operative checkup the patient reports she is again able to exercise without any impediment. Case 2: Back pain A 34-year-old female with 3 children by Cesarean section presented with an 8 year history of back pain. The pain was described as a dull ache, which increased throughout the day and improved after long periods in a recumbent position. She denied any radiation of her pain down her thighs. She denied any history of trauma. She did however, note some increase in the severity of her pain with increases in temperature and around the time of her menses. She had been on NSAIDs and had multiple spinal manipulations with a chiropractor with no improvement in her symptoms. An MRI of the lumbar spine showed only a mild L4 disc protrusion, and a nerve conduction study (NCS) showed no evidence of lumbosacral radiculopathy. Upon further questioning, the patient noted a dull ache on the left side of her pelvis, and pain, cramping, and edema in both legs. As with her back pain, these symptoms would worsen with both daily activity and prolonged standing or sitting, and were worse on the left side. Her leg symptoms would improve slightly with leg elevation. On physical examination, the lower extremities were remarkable for varicose veins and mild pitting edema noted around the ankle and calf bilaterally. A duplex ultrasound examination was performed on the pelvis. A dilated left ovarian vein was visualized with 4.2 seconds of reflux. An initial fluoroscopic venogram was performed that demonstrated severe reflux in her internal iliac veins bilaterally, with cross-pelvic collateral circulation lying near the sacrum, and also showed significant dilatation and reflux in both a left primary and accessory ovarian vein, both terminating into large and dilated pelvic varicosities that communicated with the left internal iliac vein and the right internal iliac vein via cross-pelvic collaterals. An intravascular ultrasound (IVUS) catheter noted dilation of the right ovarian vein as well. Embolization of both left ovarian veins was performed using a polidocanol and gelfoam slurry. The patient was brought back to the radiology suite 2 weeks later for a repeat venogram. During this procedure, the pelvic varicosities extending off branches of the left internal iliac vein approaching the sacrum, were embolized with gelfoam slurry and detachable coils. Closure of the left ovarian vein from the prior procedure was confirmed with a left renal venogram, and a post-embolization venogram confirmed closure of the internal iliac varicosities. Roughly seven weeks after her two embolizations, the patient reported vast improvement in her symptoms on the left, both in her pelvis and in her back. She did, however, have persisting symptoms on her right side, and in addition noted post-coital tenderness that she was now noticing as some of her other discomfort was resolving. A follow-up sonogram demonstrated resolution of the left ovarian vein reflux, but significant reflux and varicosities on the right side of her pelvis consistent with right-sided pelvic congestion. At the 10 week mark from her initial treatment she has returned to the procedure suite for a third venogram with embolization of the right gonadal vein (Figure 2) and at the 12 week post-operative point has full resolution of her symptoms. Case 3: Tenesmus and uncontrollable flatulence A 42-year-old multiparous woman presented to our clinic with 8 years tenesmus, fecal incontinence, and uncontrollable flatulence. Figure 2. Fluoroscopic venography of ovarian vein showing reflux and varices. Page 3 of 7
4 These symptoms began shortly after the birth of her first child. The pregnancy was notable for a significant amount of pain and swelling in her legs and pelvis, and the vaginal delivery was assisted with an episiotomy. Although she had some improvement in her symptoms in the months after her pregnancy, she has since had 4 more pregnancies. Despite having Cesarean sections for her deliveries, each pregnancy has worsened her incontinence and overall bowel control, as well as her baseline control. She has been evaluated by gastroenterologists for the above problems, as well as for gas and bloating in her abdomen. She has undergone endoscopies and multiple imaging studies, and was diagnosed with Irritable Bowel Syndrome. Lastly, the patient had a history of hemorrhoids, which had bled on at least one occasion. In addition to her bowel symptoms, the patient reported problems with urinary frequency, dyspareunia, and pelvic heaviness, and ovarian pain. Her pain would worsen around the time of her menses. She has been followed by a gynecologist for these issues, which were attributed to endometriosis. Her obstetrician has also attributed her incontinence issues to the episiotomy and postpartum pelvic floor dysfunction, and had suggested a potential sacral nerve stimulator implant to help her. The patient also noted some cramping, heaviness, and swelling in both legs. These symptoms would worsen with daily activity, as well as with prolonged standing or sitting. She has had hemorrhoids and varicose veins over her perineum, and has had intermittent bleeding from both. For all these symptoms, and despite her extensive workup by both gastroenterologists and gynecologists, the patient had been unable to find any relief for her numerous problems. On physical examination, the lower extremities were remarkable for spider veins, varicose veins, prominent perineal veins, and vulvar varicosities. Mild pitting edema was noted as well. The abdomen was soft, with some ovarian tenderness on palpation. Duplex examination of the pelvis was performed. A collection of pelvic varicosities was seen surrounding the rectum. A diagnostic fluoroscopic venogram was performed using a right common femoral vein approach. Moderate reflux was noted in the common iliac veins and significant reflux noted in the internal iliac veins, with delayed contrast washout noted in several varices and cross-pelvic collaterals. The exam, however, was most notable for an immensely dilated left ovarian and accessory left ovarian vein. They were roughly mm in diameter, showing delayed contrast washout and collateralization with the internal iliac veins. A large and aneurysmal terminal branch of the vessels was noted to lie on the sigmoid colon. The left ovarian vein, its accessory, and its branches were embolized with a combination of gelfoam slurry and a 20mm detachable coil. Embolization of the internal iliac branches bilaterally was performed with gelfoam. Post-embolization venography performed immediately after embolization, demonstrated successful closure of all concerning branches. At 1 week out from her embolization, the patient has had almost complete resolution of both her flatulence and her tenesmus. At the 4 week post-operative mark she had improvement with her bladder control and dyspareunia as well. She has some residual pelvic pain, and will be returning for another diagnostic venogram with an intravascular ultrasound (IVUS) to assess the reflux in her common iliac veins. Case 4: Back pain A 36-year-old multiparous woman presented to our clinic for pain, cramping, and edema in both legs for roughly 5 years. Of note, she was having significant back pain as well, which she chose to disclose after experiencing relief following venogram with successful embolization of the left gonadal vein and collaterals from the refluxing internal iliac veins. In regard to her presenting complaint, her symptoms worsened over the course of the day and improved with leg elevation. They had shown no improvement with compression therapy and daily NSAIDs. Duplex sonography showed superficial venous reflux, which was ablated. Postoperative sonograms showed successful closure of each vein. Four months later, the patient experienced a relapse of her leg pain and cramping. A repeat sonogram was performed, which showed reopening of all previously ablated veins. A sonogram was performed on the pelvis, which showed 2.9 seconds of reflux in the left ovarian vein. On further questioning and examination, the patient was found to have pelvic pain and varicosities in her inguinal area, extending to the vulva, most prominently on the left. These varicosities had been a cause of dyspareunia for the patient for several years, beginning shortly after the birth of her third child. A diagnostic fluoroscopic venogram was performed from a right common femoral vein approach. Severe reflux was seen in the left internal iliac system, with cross-pelvic flow to the right side as well as retrograde contrast filling of the left ovarian vein. The left ovarian vein was almost as large as an iliac vein- roughly 14 to 16 mm in diameter. The left vein was embolized with a combination of polidocanol and gelfoam slurry. A post-procedure venogram was performed immediately after embolization and showed only moderate closure of the vein however, and intervention in the internal iliac system was thwarted due to vasospasm. A repeat venogram was performed 10 days later, again with a right common femoral vein approach. Reflux was still seen in the branches off both internal iliac veins. The left ovarian vein remained open and dilated, with delayed contrast washout. Embolization was again performed, this time on the left ovarian vein and on the collaterals extending from both internal iliac veins, using a combination of gelfoam slurry and a 13 mm detachable coil. Post-embolization venography immediately after coil placement showed successful closure of the refluxing veins. Visualization of the right iliac veins was performed using an IVUS catheter and showed no evidence of stenosis. Page 4 of 7
5 At 8 weeks out from our first intervention, the patient has had significant reduction in her pelvic pain. She also mentions finding reduction in back pain which she reported upon experiencing relief status-post venogram interventions with embolization. Discussion Pelvic congestion syndrome (PCS) presents as a constellation of symptoms all caused by the development of varicosities in veins typically drained by either the ovarian or internal iliac veins. Its typical presentation is one of noncyclical dull, aching pelvic pain, typically unilateral, and persisting for more than 6 months. It was present in all patients in our series. Other symptoms that are commonly associated with the condition include dysmenorrhea and dyspareunia, seen respectively in case 1 and 4, and to some degree in all patients in our series. PCS is also seen in association with lower extremity varicose veins. As many as 15 20% of patients with lower limb varicosities have demonstrated pelvic venous reflux on venogram or duplex ultrasound, with a 30% incidence among those patients with varicosities that have recurred after prior treatment 1. On physical examination, these patients may often have varicosities on the vulva, on or just beneath the buttocks, and on the upper thighs, particularly near the groin, owing to reflux from the pelvic veins communicating to the legs via the inferior gluteal and internal/ external pudental veins 2. In our series, cases 1 and 4 had reopening of veins previously closed by endovenous thermal ablations. Cases 1, 3, and 4 presented with either vulvar or infragluteal varices. It is important to remember that PCS affects its patients due to the local compression and consequent irritation and inflammation of organs in proximity to the engorged and swollen plexus of pelvic veins. Since these veins drain the bladder, vagina, uterus, rectum, and sacrum, PCS can be responsible for several atypical symptoms, depending on the organ compromised. Some form of bladder instability is not uncommon, and was seen in cases 1 and 3. Irritation of the lumbosacral nerves, although uncommon, can result in either back or hip pain. In our series, back pain was seen in cases 1 and 2. Hip pain was seen in case 1. The finding of hip pain is particularly rare, with only 2 other cases being reported in the literature 3. Pressure of these veins on the rectum, or perhaps reflux through collaterals feeding off a refluxing ovarian vein, can result in hemorrhoids, a finding seen in case 3. The finding of a dilated pelvic varicosity compressing the sigmoid colon and causing both tenesmus and uncontrollable flatulence in case 3 has never before been reported. As shown in our first three cases, this atypical presentation of PCS can be the predominant issue impacting the patient s quality of life. These atypical presentations are typically underdiagnosed, as seen by the extensive and ultimately unfruitful workups experienced by 3 of the 4 patients in our series. It is therefore important to maintain a low threshold for suspicion of PCS in any patient with symptoms that can be attributed to an organ in the pelvis. Our workup for suspected PCS begins with pelvic sonography. Although there has been literature championing the efficacy of either the CT venography (CTV) or more often the magnetic resonance venography (MRV), in our experience, both studies have had a lower diagnostic yield 4 6. Both imaging modalities require proper timing to catch the contrast in the pelvis during the venous phase, and are therefore very operator dependent. The studies also require the subject to be supine, a position that can compress ordinarily dilated pelvic veins. They are also expensive. In contrast, pelvic sonography is inexpensive, and can be performed with the patient upright, as the examiner looks for both dilated pelvic veins and flow reversal during Valsalva maneuvers 7. The operator-dependent nature inherent to sonography mandates valuable sonogram technicians with high levels of training and experience in finding and reporting pelvic reflux and varicosities. As with the CTV and MRV, the sonogram is also capable of ruling out other pelvic etiologies. Findings suggestive of PCS on ultrasound include ovarian veins >6 mm in diameter, the presence of dilated (>5 mm) arcuate veins crossing the uterine myometrium, and slow (<3 sm/sec) or reversed retrograde blood flow 2,6. Polycystic changes in the ovaries have also been seen in about 50% 4,6 of cases. Diagnostic venograms remain the gold standard in identifying PCS, and are indicated for all suspicious presentations, even, in the appropriate clinical setting, if the other studies are negative. It is a low risk procedure, and permits treatment and potential curing of the patient s symptoms at the same time. Evaluation of the left renal, bilateral ovarian, iliac, and internal iliac veins is performed, looking for dilatation and reflux. Venography findings include an ovarian vein diameter >5 mm, ovarian vein reflux, stagnation of contrast in the pelvic veins, contralateral reflux across the midline, and filling of vulvoperineal or thigh varices 2,4. If there is a question of a stenotic lesion in either the renal or iliac vein, pressures across the area in question can be measured, or an intravascular ultrasound can be placed. In all of our patients, pelvic venograms successfully identified the condition. In our clinic, we perform diagnostic venography with the patient awake. We begin our assessment at the most common site of pelvic reflux, the left ovarian vein. If reflux is present, we attempt to reproduce the patient s symptoms using high pressure contrast flushes in a 5 french sheath. If the venous distension created by the flush reproduces symptoms, and the anatomic distribution of the vessels distended corresponds to those symptoms, we embolize the vessel. Our preference in the ovarian vein is to use a combination of gelfoam or polidocanol for the terminal branches below the pelvic brim and an oversized (at least 150% of the diameter of the ovarian vein) coil in the ovarian vein, preferably near the ostia of any visualized ovarian collaterals, and no less than 4 mm from its confluence with the renal vein. After the treatment, we revisit the patient in roughly 1 week. If the patient is showing improvement, we repeat the pelvic sonogram to determine if any reflux remains. If reflux is noted, we perform a second venogram and embolization of pelvic varices fed by the refluxing internal iliac veins, and potentially the right ovarian vein if the patient s symptoms are significantly greater on the right. Our preference is to treat the internal iliac branches with either sclerotherapy or gelfoam alone, given the higher risk of coil Page 5 of 7
6 migration noted in this region. If the right ovarian vein is to be targeted, we consider a right internal jugular access to allow for easier cannulation. During this second procedure, we also employ an IVUS catheter to look for stenotic lesions. Pelvic reflux can frequently be secondary to anatomic anomalies resulting in downstream obstruction, such as compression of the left renal vein by the superior mesenteric artery (Nutcracker syndrome) 1,2,7, or compression of a left common iliac vein by a right common iliac artery (May-Thurner syndrome) 8. A May-Thurner s phenomenon can be present in as many as two-thirds of the general population 9. If any such lesions are identified, a full discussion with the patient regarding the anatomy affected by the stenosis, and the benefits and drawbacks of angioplasty alone versus stenting ensues. If the patient wishes to proceed, we return for a third venogram to treat the stenotic segments. For milder lesions ( 50% reduction in cross-sectional area), or for focal, short lesions caused by a localized vascular band or web, we attempt only an angioplasty. For a longer and more severe stenotic segment (> 50%), we prefer to both angioplasty and stent. As with our coils, our preference is to oversize our stents (roughly 4 mm greater than the average diameter of the non-stenotic venous segment). Our preference is to avoid stenting for as long as possible in women who intend to get pregnant and in patients with clotting disorders or prior DVTs, given the higher incidence of post-stent complications in these patient populations. Transcatheter embolization is currently regarded as the least invasive and most efficacious management option for PCS, with complete or partial symptom relief in % of patients 2,10. Apart from our preferences, a number of different approaches have been reported to affect closure of the refluxing veins, from simple coil embolization, to glue embolization, to combinations of sclerotherapy and coils. In studies using visual analog scale (VAS) pain scores to measure the extent of symptom relief, vast improvement was shown consistently, with mean scores of decreasing to scores of postoperatively. Depending on the initial severity, the symptoms can take as long as 9 13 months after therapy to resolve 10. Complications from the procedure are rare, being reported in % of patients, and consist of coil migration, vein perforation, local phlebitis, deep venous thrombosis, and contrast reactions 10. Patients may suffer from a brief period of flu-like symptoms within 72 hours of each embolization, but this consistently passes within 48 hours without need for intervention. Studies have also shown embolization to have no effect on the menstrual cycle or fertility 4. This is an important consideration, given that the predominance of PCS is in premenopausal women. With respect to the management of PCS secondary to stenotic vein lesions, endovenous stent placement is also safe and effective. In a review of multiple studies encompassing 1500 patients being treated for chronic iliac vein stenosis, stenting had a % patency rate for non-thrombotic disease and 74 89% patency rate for thrombotic disease at 3 to 5 years. Symptom relief was achieved in 86 94% of patients for pain, 66 89% for swelling, and 58 89% for healing of ulcers in the leg 11. Although these studies focused on the outcomes of patients suffering from venous insufficiency in the legs, it is not unreasonable to assume that treatment of the stenosis would similarly benefit patients with PCS, given that both ailments are due to venous obstruction causing congestion in communicating upstream veins. Among the 1500 patients reviewed, no deaths or pulmonary emboli were reported, and access site complications and significant bleeding, despite the larger sheaths required for the stents, occurred in only % 11. Given the effectiveness and safety of these procedures, our practice recommends aggressive management of patients whose symptoms and venogram findings suggest the presence of PCS. Conclusion Pelvic congestion syndrome is an underdiagnosed condition in premenopausal women that presents with a broad spectrum of symptoms that are often attributed to other pathologies. It is important to maintain a high level of suspicion in parous women wether the presenting symptoms are typical or atypical in nature. The complexity of the abdominal/pelvic venous vasculature in the premenopausal patient can distort accuracy and cloud the patients ability to properly articlutale symptoms. With modern advancements made in diagnostic imaging many clinicians feel MRV to be definitive in diagnosing pelvic congestion, but our experience has proven otherwise. Cross sectional imaging relies heavily on timing, patient immobility and technical skill level of the performing technologist and even then can still provide false positive reults 2,4,6. Our experience has shown us that fluoroscopic venography is the gold standard diagnostic imaging modality providing us with anatomical correlation as well as physiological confirmation of our suspicions. In this specific patient population a diagnostic venogram will go far in preventing patients with PCS from missing out on effective and low risk treatment. Consent Written informed consent for publication of their clinical details was obtained from each patient in this paper. Author contributions DG, AA, AR and CH all served as primary authors on this paper making substantial contributions to the design conception, acquisition, analysis and interpretation of the data for this paper. All four authors were substantially involved in the intellectual content drafting and subsequent revisions of this paper. All four authors gave approval for final version of this paper for publication and agree to be accountable for all aspects of the work therein. All authors ensure any questions related to the accuracy or integrity of any part of this work will be appropiately investigated and resolved. AT served as a scientific advisor for the entire duration of the data gathering phase of this research. AT also contributed through critically evaluating all drafts of this paper in the editing process. Competing interests No competing interests were disclosed. Grant information The author(s) declared that no grants were involved in supporting this work. Page 6 of 7
7 References 1. Lopez AJ: Female Pelvic Vein Embolization: Indications, Techniques, and Outcomes. Cardiovasc Intervent Radiol. 2015; 38(4): Free Full Text PubMed Abstract Publisher Full Text 2. Durham JD, Machan L: Pelvic congestion syndrome. Semin Intervent Radiol. 2013; 30(4): Free Full Text PubMed Abstract Publisher Full Text 3. Shelkey J, Huang C, Karpa K, et al.: Case report: pelvic congestion syndrome as an unusual etiology for chronic hip pain in 2 active, middle-age women. Sports Health. 2014; 6(2): PubMed Abstract Free Full Text 4. Bittles MA, Hoffer EK: Gonadal vein embolization: treatment of varicocele and pelvic congestion syndrome. Semin Intervent Radiol. 2008; 25(3): Free Full Text PubMed Abstract Publisher Full Text 5. Greiner M, Dadon M, Lemasle P, et al.: How does the patho-physiology influence the treatment of pelvic congestion syndrome and is the result long-lasting? Phlebology. 2012; 27(Suppl 1): PubMed Abstract Publisher Full Text 6. Ignacio EA, Dua R, Sarin S, et al.: Pelvic congestion syndrome: diagnosis and treatment. Semin Intervent Radiol. 2008; 25(4): Free Full Text PubMed Abstract Publisher Full Text 7. Liddle AD, Davies AH: Pelvic congestion syndrome: chronic pelvic pain caused by ovarian and internal iliac varices. Phlebology. 2007; 22(3): PubMed Abstract Publisher Full Text 8. Marsh P, Holdstock J, Harrison C, et al.: Pelvic vein reflux in female patients with varicose veins: comparison of incidence between a specialist private vein clinic and the vascular department of a National Health Service District General Hospital. Phlebology. 2009; 24(3): PubMed Abstract Publisher Full Text 9. Raju S, Darcey R, Neglén P: Unexpected major role for venous stenting in deep reflux disease. J Vasc Surg. 2010; 51(2): ; discussion 408. PubMed Abstract Publisher Full Text 10. Meissner MH, Gibson K: Clinical outcome after treatment of pelvic congestion syndrome: sense and nonsense. Phlebology. 2015; 30(1 Suppl): PubMed Abstract 11. Raju S: Best management options for chronic iliac vein stenosis and occlusion. J Vasc Surg. 2013; 57(4): PubMed Abstract Publisher Full Text Page 7 of 7
8 Flagship Office: 14 E 60 th Street, Suite 501 New York, NY Corporate Office: 555 Passaic Avenue West Caldwell, NJ P F About Pelvic Congestion Syndrome (PCS) What is Pelvic Congestion Syndrome? Pelvic Congestion Syndrome is a very common condition that is present in almost 50% of women with other forms of vein disease, including varicose veins. It also occurs in many people without a history of varicose veins, especially leaner people, or those that have lost a significant amount of weight or have had multiple pregnancies or abdominal surgery. Because vein disease does not begin in the legs, it actually begins at the top of the abdomen. Anything from the top of the abdomen down can be affected by vein disease because anything below that point is fighting against gravity to return back to the heart and is prone to pooling as a result. Typically however, vein disease in the abdomen and pelvis creates a very vague and varied presentation that is unique to each patient, and almost impossible to localize without an accurate map of anatomy, such as a venogram. How did I get Pelvic Congestion Syndrome? The risk factors for pelvic congestion include genetic issues, multiple pregnancies, and it seems to be more common in taller individuals. Smaller women also have a higher chance of having pelvic congestion after pregnancy, due to less room in their pelvis to accommodate a fetus, and more pressure on the veins as a result of pregnancy. There is also a form of pelvic congestion syndrome that occurs due to narrowing of veins upstream, causing the backing up of blood into the pelvis. The narrowing of veins, due to genetic or anatomic issues such as May Thurner Syndrome or Nutcracker syndrome, are commonly associated with pelvic congestion and often the patient requires treatment for both. 145 W Montauk Highway Hampton Bays, NY Northern Blvd Roslyn, NY South Pearl Street Pearl River, NY A L L P R O C E D U R E S A R E D O N E I N O U R S T A T E O F T H E A R T F A C I L I T Y
9 Flagship Office: 14 E 60 th Street, Suite 501 New York, NY Corporate Office: 555 Passaic Avenue West Caldwell, NJ P F What kind of symptoms does pelvic congestion cause? The symptoms of pelvic congestion are extremely varied and totally unique to the patient and their specific anatomy. Some of the more common presentations that we see regularly include abdominal bloating and distention, gassiness, abdominal pain, flatulence, urinary symptoms like pain during urination or the feeling that you need to urinate more frequently, severe menstrual pain and cramps, low back pain, hip pain, and pain during intercourse. Most often, but not always, the pain worsens throughout the day with standing and sitting, and alleviates somewhat with raising the legs. Very often, our patients report that they have undergone a workup for many other causes, from orthopedic or spinal disease to things like celiac disease or fibroids. Typically the workup has been unrevealing, as most practitioners do not think of PCS as a potential cause. So who needs treatment and how is it treated? In general, if the patient has positive ultrasound findings of blood pooling in the pelvis, as well as a history of abdominal and pelvic symptoms, we take the patient for a diagnostic venogram, which is a study done usually under local anesthesia, that allows us to clearly localize the anatomy, cause, and severity of blood pooling in the pelvis. We keep the patient awake preferentially so that they can understand the anatomy and why we do what we are doing, and in our experience this has helped tremendously with patient satisfaction. If we see blood pooling that correlates with the patients symptoms, we typically treat it at that time using material to help the blood clot in the pooling malfunctioning veins, similar to sclerotherapy on veins on the surface. This is called embolization. Depending on the size of the vein, a coil or plug may be needed to prevent recurrence. Treatment is very safe, benign, with almost no long term consequences or lifestyle alterations needed when done at the time of the venogram. Due to the very high success rate on alleviation of symptoms, as well as very low risk, we feel it is more important to treat findings when found rather than bring the patient back again for another procedure. Whether additional treatment is needed, which happens often, depends on other findings at the time of the venogram, which is a diagnostic test as well. 145 W Montauk Highway Hampton Bays, NY Northern Blvd Roslyn, NY South Pearl Street Pearl River, NY A L L P R O C E D U R E S A R E D O N E I N O U R S T A T E O F T H E A R T F A C I L I T Y
10 Flagship Office: 14 E 60 th Street, Suite 501 New York, NY Corporate Office: 555 Passaic Avenue West Caldwell, NJ P F What happens after treatment for PCS? After PCS treatment, usually several hours after, there is a vague feeling of mild to moderate pain that happens in the treated area. This may be accompanied by nausea and low-grade fever and loose stools, depending on anatomy. Most often it is described as an exacerbation of PMS type pain. This is a self-limited, well-recognized phenomenon called post-embolization syndrome. It typically mostly resolves on its own by the next day. After that, usually the patient s pre-operative symptoms are mostly gone. Sometimes, with more extensive disease, it takes up to two weeks to feel much better, but this is the exception rather than the rule. Very often there are residual symptoms somewhere else, due to continued blood pooling, which may require a different approach to treat, and we do this on a second visit if needed. Typically additional procedures are minor in comparison. What are the risks of treating my PCS? With any medical procedure, there is a theoretical risk of bleeding as well as infection. In addition, whenever endovascular procedures are performed, such as for PCS, some unique but very rare risks include the possibility of malposition or movement of devices, as well as damage to blood vessels and organs. In our experience at NYC Surgical our complication rate is far below that of most major academic institutions, far below the national average of less than 1 percent. Overall, the risk of these procedures is far lower than conventional surgery, but still present, and must be discussed. What is the prognosis after treatment? After treatment for PCS, the prognosis is excellent with very few full recurrences even long term. With any endovascular treatment, there is a small risk from side branches of recurrence that is easily treated with a minor procedure using local anesthesia only. Most often, we screen our post treatment patients annually to check for the long term durability of our repairs. 145 W Montauk Highway Hampton Bays, NY Northern Blvd Roslyn, NY South Pearl Street Pearl River, NY A L L P R O C E D U R E S A R E D O N E I N O U R S T A T E O F T H E A R T F A C I L I T Y
Michael Meuse, MD Vascular and Interventional Radiology
 Michael Meuse, MD Vascular and Interventional Radiology OBJECTIVES BACKGROUND PATHOPHYSIOLOGY SYMPTOM COMPLEX EVALUATION AND RX OPTIONS INDICATION FOR EMBOLOTHERAPY RESULTS 1857 Richet: Chronic pelvic
Michael Meuse, MD Vascular and Interventional Radiology OBJECTIVES BACKGROUND PATHOPHYSIOLOGY SYMPTOM COMPLEX EVALUATION AND RX OPTIONS INDICATION FOR EMBOLOTHERAPY RESULTS 1857 Richet: Chronic pelvic
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities
 250 JDMS 25:250-254 September/October 2009 Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities A Literature Review KATHLEEN WHEELOCK, RVT Pelvic congestion syndrome occurs
250 JDMS 25:250-254 September/October 2009 Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities A Literature Review KATHLEEN WHEELOCK, RVT Pelvic congestion syndrome occurs
Starting with deep venous treatment
 Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
The Evaluation & Treatment of Pelvic Venous Disorders
 The Evaluation & Treatment of Pelvic Venous Disorders Mark H. Meissner, MD Professor of Surgery University of Washington School of Medicine Seattle, Washington Pelvic Venous Disorders Pelvic Congestion
The Evaluation & Treatment of Pelvic Venous Disorders Mark H. Meissner, MD Professor of Surgery University of Washington School of Medicine Seattle, Washington Pelvic Venous Disorders Pelvic Congestion
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Duplex ultrasound is first-line imaging for all
 Our Protocol for Transabdominal Pelvic Vein Duplex Ultrasound A summary of s protocol for pelvic vein duplex ultrasonography, including equipment, patient positioning, ultrasound settings, and technique.
Our Protocol for Transabdominal Pelvic Vein Duplex Ultrasound A summary of s protocol for pelvic vein duplex ultrasonography, including equipment, patient positioning, ultrasound settings, and technique.
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Management of an Unusual Iliac Fossa Venous Plexus
 Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
Right Ovarian Vein Syndrome. Nasser Algharem, MD, FRCR, EBIR.
 Right Ovarian Vein Syndrome Nasser Algharem, MD, FRCR, EBIR. Disclosure Speaker name: Nasser Algharem... I do not have any potential conflict of interest Safi A 47-year-old multiparous woman who had conceived
Right Ovarian Vein Syndrome Nasser Algharem, MD, FRCR, EBIR. Disclosure Speaker name: Nasser Algharem... I do not have any potential conflict of interest Safi A 47-year-old multiparous woman who had conceived
Pelvic Congestion Syndrome Diagnosis and Treatment Hadjipolycarpou Andreas Vascular Surgery Clinic, Nicosia General Hospital Director Dr Ch.
 Pelvic Congestion Syndrome Diagnosis and Treatment Hadjipolycarpou Andreas Vascular Surgery Clinic, Nicosia General Hospital Director Dr Ch. Bekos Vascular Surgical Society of Cyprus @ LIVE Patra, 2018
Pelvic Congestion Syndrome Diagnosis and Treatment Hadjipolycarpou Andreas Vascular Surgery Clinic, Nicosia General Hospital Director Dr Ch. Bekos Vascular Surgical Society of Cyprus @ LIVE Patra, 2018
Selection and work up for the right patients suspected of deep venous disease
 Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
Pelvic Congestion Syndrome
 Pelvic Congestion Syndrome 1 Pelvic Congestion Syndrome (PCS) Condition and Symptom Background Condition Overview Urogynecological Symptoms 2 Non-cyclic pelvic pain affecting 39.1% of women at some point
Pelvic Congestion Syndrome 1 Pelvic Congestion Syndrome (PCS) Condition and Symptom Background Condition Overview Urogynecological Symptoms 2 Non-cyclic pelvic pain affecting 39.1% of women at some point
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction. Erin H. Murphy, MD Rane Center
 Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Image-Guided Approach to Treatment of Patients with Nonthrombotic
 Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Evaluation and Management of Pelvic Venous Disorders
 Evaluation and Management of Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Disorders University of Washington School of Medicine Seattle, WA Mark H. Meissner,
Evaluation and Management of Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Disorders University of Washington School of Medicine Seattle, WA Mark H. Meissner,
Chronic pelvic pain typically presents in young
 Endovascular Treatment of Pelvic Congestion Syndrome PCS remains underdiagnosed and undertreated, but recognizing this condition and providing endovascular treatment can benefit women with chronic pelvic
Endovascular Treatment of Pelvic Congestion Syndrome PCS remains underdiagnosed and undertreated, but recognizing this condition and providing endovascular treatment can benefit women with chronic pelvic
Hemorroids and pelvic venous congestion: venous embolization is it efficient and sufficient?
 Hemorroids and pelvic venous congestion: venous embolization is it efficient and sufficient? Milka GREINER MD American Hospital of Paris Hôpital Pitié-Salpêtrière Paris I do not have any potential conflict
Hemorroids and pelvic venous congestion: venous embolization is it efficient and sufficient? Milka GREINER MD American Hospital of Paris Hôpital Pitié-Salpêtrière Paris I do not have any potential conflict
US Imaging of pelvic congestion syndrome
 US Imaging of pelvic congestion syndrome Poster No.: C-1210 Congress: ECR 2015 Type: Educational Exhibit Authors: D. S. Baviskar, S. Baviskar; Abu Dhabi/AE Keywords: Pelvis, Vascular, Veins / Vena cava,
US Imaging of pelvic congestion syndrome Poster No.: C-1210 Congress: ECR 2015 Type: Educational Exhibit Authors: D. S. Baviskar, S. Baviskar; Abu Dhabi/AE Keywords: Pelvis, Vascular, Veins / Vena cava,
Pelvic venous insufficiency my best practice, warning and complications prevention
 Nice, June 1 st 2017 Pelvic venous insufficiency my best practice, warning and complications prevention O Hartung Dpt of Vascular Surgery CHU Nord, Marseille, FRANCE Pelvic venous insufficiency All manifestations
Nice, June 1 st 2017 Pelvic venous insufficiency my best practice, warning and complications prevention O Hartung Dpt of Vascular Surgery CHU Nord, Marseille, FRANCE Pelvic venous insufficiency All manifestations
LEFT RENAL VEIN COMPRESSION
 MANAGEMENT of LEFT RENAL VEIN COMPRESSION in PATIENTS PRESENTING LEFT GONADAL VEIN REFLUX J. LEAL MONEDERO, MD S. ZUBICOA EZPELETA, MD angiovascularlyz@gmail.com Hospital Ruber Internacional. Madrid Á.
MANAGEMENT of LEFT RENAL VEIN COMPRESSION in PATIENTS PRESENTING LEFT GONADAL VEIN REFLUX J. LEAL MONEDERO, MD S. ZUBICOA EZPELETA, MD angiovascularlyz@gmail.com Hospital Ruber Internacional. Madrid Á.
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View
 On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
Clinical case. Symptomatic anterior accessory great saphenous vein (AAGSV) reflux
 Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Corporate Medical Policy
 Corporate Medical Policy Ovarian, Internal Iliac and Gonadal Vein Embolization, Ablation and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ovarian_and_internal_iliac_vein_embolization
Corporate Medical Policy Ovarian, Internal Iliac and Gonadal Vein Embolization, Ablation and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ovarian_and_internal_iliac_vein_embolization
OHTAC Recommendation. Endovascular Laser Treatment for Varicose Veins. Presented to the Ontario Health Technology Advisory Committee in November 2009
 OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
Imaging, it s central role in planning and guiding intervention. Prof. Luis Izquierdo. MD, PhD, FEBVS
 Imaging, it s central role in planning and guiding intervention Prof. Luis Izquierdo. MD, PhD, FEBVS IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural
Imaging, it s central role in planning and guiding intervention Prof. Luis Izquierdo. MD, PhD, FEBVS IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural
History is Flawed. A New Paradigm for Abdominal & Pelvic Venous Disorders
 History is Flawed A New Paradigm for Abdominal & Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Medicine University of Washington School of Medicine Disclosures
History is Flawed A New Paradigm for Abdominal & Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Medicine University of Washington School of Medicine Disclosures
Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome. Original Policy Date
 MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Date: A. Venous Health History Form. Patient please complete questions Primary Care Physician:
 E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat?
 Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
2017 Florida Vascular Society
 Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Segmental GSV reflux
 Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Varicose Vein Information Sheet
 Neil Goldstein, MD Joseph Hewett, MD Board- Certified Physicians in Interventional, Diagnostic, and Vascular Radiology, Surgery, Vascular Surgery and Phlebology Varicose Vein Information Sheet PREVALENCE
Neil Goldstein, MD Joseph Hewett, MD Board- Certified Physicians in Interventional, Diagnostic, and Vascular Radiology, Surgery, Vascular Surgery and Phlebology Varicose Vein Information Sheet PREVALENCE
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Love your legs again Varicose Veins
 Love your legs again Varicose Veins Veins are the vessels that return blood to the heart once it has circulated through the body (as opposed to arteries, which carry oxygen-rich blood from the heart to
Love your legs again Varicose Veins Veins are the vessels that return blood to the heart once it has circulated through the body (as opposed to arteries, which carry oxygen-rich blood from the heart to
Nutcracker Syndrome. Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust
 Nutcracker Syndrome Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust Case 1: JB Referred at 17.9yrs with intermittent abdominal pain and few episodes of painless frank haematuria
Nutcracker Syndrome Dr Heena Kithany Specialty Registrar Dorset County Hospitals NHS Trust Case 1: JB Referred at 17.9yrs with intermittent abdominal pain and few episodes of painless frank haematuria
Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula
 EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
Proper Diagnosis of Venous Thromboembolism (VTE)
 Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment.
 Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment. Approximately 1 in 5 adult Americans suffer from superficial
Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment. Approximately 1 in 5 adult Americans suffer from superficial
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: MP.066.MH Last Review Date: 11/08/2018 Effective Date: 01/01/2019
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst PPO MedStar Health considers the treatment of Varicose
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst PPO MedStar Health considers the treatment of Varicose
Do ovarian cysts cause back pain
 Toggle navigation Do ovarian cysts cause back pain 10-3-2018 Ovarian Cysts - Symptoms. What. Since March 2017 had back pain radiating to groin and leg associated with. Ovarian Cysts - Causes. What was
Toggle navigation Do ovarian cysts cause back pain 10-3-2018 Ovarian Cysts - Symptoms. What. Since March 2017 had back pain radiating to groin and leg associated with. Ovarian Cysts - Causes. What was
FIND RELIEF FROM VARICOSE VEINS. VenaSeal Sapheon Closure System
 FIND RELIEF FROM VARICOSE VEINS VenaSeal Sapheon Closure System UNDERSTAND Varicose veins may be a sign of something more severe. Your doctor can help you understand if you have this condition. may cause
FIND RELIEF FROM VARICOSE VEINS VenaSeal Sapheon Closure System UNDERSTAND Varicose veins may be a sign of something more severe. Your doctor can help you understand if you have this condition. may cause
UNDERSTANDING VEIN PROBLEMS
 UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY
 RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
Date: A. Venous Health History Form. Patient please complete questions Primary Care Physician:
 E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
Disclosures. What is a Specialty Vein Clinic? Prevalence of Venous Disease. Management of Venous Disease: an evidence based approach.
 Management of Venous Disease: an evidence based approach Disclosures Ed Boyle, MD Andrew Jones, MD Dr. Ed Boyle and Dr. Andrew Jones disclose Grants/research support: Medtronic, BTG International, Clearflow,
Management of Venous Disease: an evidence based approach Disclosures Ed Boyle, MD Andrew Jones, MD Dr. Ed Boyle and Dr. Andrew Jones disclose Grants/research support: Medtronic, BTG International, Clearflow,
Chronic Iliocaval Venous Occlusive Disease
 none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES TREATMENT OF VARICOSE VEINS OF THE LOWER EXTREMITIES STAB PHLEBECTOMY AND SCLEROTHERAPY TREATMENT The primary purpose of this document is to assist providers enrolled in
PROVIDER POLICIES & PROCEDURES TREATMENT OF VARICOSE VEINS OF THE LOWER EXTREMITIES STAB PHLEBECTOMY AND SCLEROTHERAPY TREATMENT The primary purpose of this document is to assist providers enrolled in
Cases For Teaching Second Year Medical Students. Head and neck and neuroanatomy. 2- What is the anatomical explanation for her symptoms?
 Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Retrograde flow in the left ovarian vein is a shunt, not reflux
 Retrograde flow in the left ovarian vein is a shunt, not reflux Poster No.: C-0846 Congress: ECR 2013 Type: Scientific Exhibit Authors: R. Livsey; Brisbane/AU Keywords: Genital / Reproductive system female,
Retrograde flow in the left ovarian vein is a shunt, not reflux Poster No.: C-0846 Congress: ECR 2013 Type: Scientific Exhibit Authors: R. Livsey; Brisbane/AU Keywords: Genital / Reproductive system female,
FIND RELIEF FROM VARICOSE VEINS. VenaSeal Closure System
 FIND RELIEF FROM VARICOSE VEINS VenaSeal Closure System UNDERSTAND Varicose veins may be a sign of something more severe venous reflux disease Your doctor can help you understand if you have this condition.
FIND RELIEF FROM VARICOSE VEINS VenaSeal Closure System UNDERSTAND Varicose veins may be a sign of something more severe venous reflux disease Your doctor can help you understand if you have this condition.
Management of Post-Thrombotic Syndrome
 Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Recurrent Varicose Veins We All See Them
 We All See Them November 4, 2017 Austin, TX Arlington Heights, IL No conflicts Terminology REVAS REcurrent Varices After Surgery PREVAIT PREsence of Varices After Interventional Treatment Recurrent varices
We All See Them November 4, 2017 Austin, TX Arlington Heights, IL No conflicts Terminology REVAS REcurrent Varices After Surgery PREVAIT PREsence of Varices After Interventional Treatment Recurrent varices
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015
 Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
Patient assessment and strategy making for endovenous treatment
 Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery
 Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Varicose veins. Information for patients Sheffield Vascular Institute
 Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
The Use of Adjunctive Venography and Endovascular Manoeuvres In The Treatment of Saphenous Vein Insufficiency. A Prospective, Multi-centre Study
 The Use of Adjunctive Venography and Endovascular Manoeuvres In The Treatment of Saphenous Vein Insufficiency A Prospective, Multi-centre Study Ramon L. Varcoe, MBBS, MS, FRACS, PhD Associate Professor
The Use of Adjunctive Venography and Endovascular Manoeuvres In The Treatment of Saphenous Vein Insufficiency A Prospective, Multi-centre Study Ramon L. Varcoe, MBBS, MS, FRACS, PhD Associate Professor
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
X-Plain Ovarian Cancer Reference Summary
 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
A treatment option for varicose veins. enefit" Targeted Endovenous Therapy. Formerly known as the VNUS Closure procedure E 3 COVIDIEN
 A treatment option for varicose veins. enefit" Targeted Endovenous Therapy Formerly known as the VNUS Closure procedure E 3 COVIDIEN THE VENOUS SYSTEM ANATOMY The venous system is made up of a network
A treatment option for varicose veins. enefit" Targeted Endovenous Therapy Formerly known as the VNUS Closure procedure E 3 COVIDIEN THE VENOUS SYSTEM ANATOMY The venous system is made up of a network
Deep Venous Pathology. Eberhard Rabe Department of Dermatology University of Bonn Germany
 Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC
 Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Deep Vein Thrombosis
 Deep Vein Thrombosis Introduction Deep vein thrombosis (DVT) is a blood clot in a vein. This condition can affect men and women of any age and race. DVT is a potentially serious condition. If not treated,
Deep Vein Thrombosis Introduction Deep vein thrombosis (DVT) is a blood clot in a vein. This condition can affect men and women of any age and race. DVT is a potentially serious condition. If not treated,
Find From Varicose Veins. VenaSeal
 Find Relief From Varicose Veins VenaSeal Closure System Understand Varicose veins may be a sign of something more severe venous reflux disease. Your doctor can help you understand if you have this condition.
Find Relief From Varicose Veins VenaSeal Closure System Understand Varicose veins may be a sign of something more severe venous reflux disease. Your doctor can help you understand if you have this condition.
Vascular Surgery and Transplant Unit University of Catania. Pierfrancesco Veroux
 Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Non-Saphenous Vein Treatments. Jessica Ochs PA-C Albert Vein Institute Colorado Springs and Lone Tree, CO
 Non-Saphenous Vein Treatments Jessica Ochs PA-C Albert Vein Institute Colorado Springs and Lone Tree, CO I have no financial disclosures Types of Veins Treated Perforator Veins Tributary Veins Varicose
Non-Saphenous Vein Treatments Jessica Ochs PA-C Albert Vein Institute Colorado Springs and Lone Tree, CO I have no financial disclosures Types of Veins Treated Perforator Veins Tributary Veins Varicose
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre
 PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME
 Oxford UnitedHealthcare Oxford Clinical Policy EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME Policy Number: SURGERY 105.8 T2 Effective Date: November 1, 2018 Instructions for
Oxford UnitedHealthcare Oxford Clinical Policy EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME Policy Number: SURGERY 105.8 T2 Effective Date: November 1, 2018 Instructions for
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information
 Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
BC Vascular Surgery Day
 BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review
 ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
The Vascular Disease Almost No One Teaches But Should!!! Chronic Venous Insufficiency
 The Vascular Disease Almost No One Teaches But Should!!! Chronic Venous Insufficiency Thomas E. Eidson, DO Certified Venous Disease Specialist Board Certified Family Medicine Disclosure of Conflict of
The Vascular Disease Almost No One Teaches But Should!!! Chronic Venous Insufficiency Thomas E. Eidson, DO Certified Venous Disease Specialist Board Certified Family Medicine Disclosure of Conflict of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18
 INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
Determine the patients relative risk of thrombosis. Be confident that you have had a meaningful discussion with the patient.
 Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Ligation with Stripping
 Ligation with Stripping Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look? Vein problems
Ligation with Stripping Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look? Vein problems
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
The following are the objectives to be successfully completed by the IR fellow at the completion of training.
 GOALS and OBJECTIVES The following are the objectives to be successfully completed by the IR fellow at the completion of training. I. Patient Care Fellows must be able to provide patient care that is compassionate,
GOALS and OBJECTIVES The following are the objectives to be successfully completed by the IR fellow at the completion of training. I. Patient Care Fellows must be able to provide patient care that is compassionate,
Endovenous Laser Therapy INFORMATION & TREATMENT INSTRUCTIONS
 1324 Princess Street Kingston, ON K7M 3E2 Website: www.ucosmetic.com Email: nuyu@ucosmetic.com Phone: (613) 536-LASR (5277) Fax: (613) 536-5108 Dr. Kim Meathrel, MD, FRCSC, Plastic Surgeon, Associate Professor
1324 Princess Street Kingston, ON K7M 3E2 Website: www.ucosmetic.com Email: nuyu@ucosmetic.com Phone: (613) 536-LASR (5277) Fax: (613) 536-5108 Dr. Kim Meathrel, MD, FRCSC, Plastic Surgeon, Associate Professor
Patient Information. Venous Insufficiency and Varicose Veins
 Patient Information Venous Insufficiency and Varicose Veins What is a Varicose Vein? Gitter Vein Institute-revised 3/8/2016 2 Frequently Asked Questions What is the difference between varicose and spider
Patient Information Venous Insufficiency and Varicose Veins What is a Varicose Vein? Gitter Vein Institute-revised 3/8/2016 2 Frequently Asked Questions What is the difference between varicose and spider
Complex Iliocaval Reconstruction PNEC. Seattle WA. Bill Marston MD Professor, Div of Vascular Surgery University of N.
 Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Microphlebectomy for Varicose Veins
 Microphlebectomy for Varicose Veins Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look?
Microphlebectomy for Varicose Veins Understanding Problem Leg Veins Do your legs feel tired and achy at the end of the day? Have you stopped wearing shorts because you don t like the way your legs look?
n Make tremendous difference in patients lives: n Diagnosing or excluding disease and injury n Evaluating response to therapy
 Imaging: Choosing the Appropriate Exam Rob Milman, MD Austin Radiological Association What is a Radiologist? A physician who specializes in diagnosing and treating disease and injury by using medical imaging
Imaging: Choosing the Appropriate Exam Rob Milman, MD Austin Radiological Association What is a Radiologist? A physician who specializes in diagnosing and treating disease and injury by using medical imaging
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
AN UNCOMMON CAUSE OF MASSIVE HEMATURIA
 Originally Posted: August, 01, 2014 AN UNCOMMON CAUSE OF MASSIVE HEMATURIA Resident(s): Monzer Chehab, MD, Alexander Copelan MD Attending(s): Purushottam Dixit, MD Program/Dept(s): Oakland University William
Originally Posted: August, 01, 2014 AN UNCOMMON CAUSE OF MASSIVE HEMATURIA Resident(s): Monzer Chehab, MD, Alexander Copelan MD Attending(s): Purushottam Dixit, MD Program/Dept(s): Oakland University William
Deep Vein Thrombosis
 Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
