Vasectomy is the safest and most dependable
|
|
|
- Elijah Stephens
- 5 years ago
- Views:
Transcription
1 REVIEW NO-SCALPEL, NO-NEEDLE VASECTOMY MARA A. MONOSKI, PHILIP S. LI, NEIL BAUM, AND MARC GOLDSTEIN Vasectomy is the safest and most dependable method of permanent contraception available to men today. More than 500,000 vasectomies are performed in the United States and more than 55,000 in Canada each year. Of American married couples, 7% to 10% choose vasectomy as their form of birth control. This has made vasectomy the most common urologic procedure in North America. 1 3 Although vasectomy is a safe and simple procedure for those who are well-trained, it can be technically challenging. Most contemporary surgeons and urologists have never been formally educated on how to perform a conventional vasectomy through a 2 to 3-cm incision or the newer no-scalpel vasectomy made through a 2 to 3-mm puncture wound on the scrotum. Many are forced to learn the procedure by trial and error during or after their residency training. Therefore, many urologists develop their own techniques that stray from more superior methods that have fewer complications and lower failure rates and may be accomplished with little or no pain. Kendrick and associates 4 illustrated how vasectomy performed by inexperienced hands leads to an increased incidence of complications such as bleeding, hematoma and infection. We discuss the no-scalpel vasectomy and noneedle vasectomy, a unique and nearly painless technique for anesthetizing the scrotal skin and vas. Using a jet injector (MadaJet, Mada Medical Products, Carlstadt, NJ), the anesthetic solution is sprayed through the skin and around the vas using a high-pressure injector that patients have described as a gentle snap of a rubber band against From the Department of Urology and Center for Male Reproductive Medicine and Microsurgery, Cornell Institute for Reproductive Medicine, Weill Medical College of Cornell University, New York Presbyterian Hospital of Columbia and Cornell, New York, New York; Department of Urology, Tulane Medical School; and Department of Urology, Louisiana State University Medical School, New Orleans, Louisiana Reprint requests: Marc Goldstein, M.D., Department of Urology, Weill Medical College of Cornell University, New York Presbyterian Hospital of Columbia and Cornell, Box 580, 525 East 68th Street, New York, NY mgoldst@med. cornell.edu Submitted: November 10, 2005, accepted (with revisions): March 7, 2006 the scrotal skin. 1,5 The no-needle jet injection is a simple, effective, and safe technique that delivers excellent local anesthesia for vasectomy with high patient satisfaction. We believe this technique may reduce men s fear of the pain associated with the needle puncture involved in vasectomy and, in conjunction with the no-scalpel vasectomy, will likely enhance the popularity of vasectomy worldwide. HISTORY In 1974, Dr. Shunqiang Li developed the no-scalpel vasectomy in China. Goldstein et al. 6 performed the first no-scalpel vasectomy in the United States in 1985 and published their experience using this technique in Since then, millions of men have undergone no-scalpel vasectomy in the United States and Canada. No-scalpel vasectomy has become the technique of choice for surgeons in North America. 2 It has also been popularized worldwide because of its minimally invasive approach, which reduces the incision size, procedure time, pain, bleeding, and postoperative complications compared with conventional scalpel vasectomy. 2,3,6 11 Since 1975, more than 15 million men have undergone no-scalpel vasectomy with a 10-fold reduction in complications compared with standard vasectomy. 9 INDICATIONS AND CONTRAINDICATIONS It must first be determined whether vasectomy is an appropriate option for the patient. Information regarding the patient s age, reason for vasectomy, and relationship status should be documented. It is important to discuss with the patient alternative methods of contraception, risks of the procedure, which include failure, and possible complications such as bleeding and infection. The physician must ensure that the patient considers the procedure permanent and have him sign an informed consent form before undergoing vasectomy. 3,12,13 Men should also be encouraged to discuss this decision with their partner. On physical examination, the presence of bilateral vas deferens should be assessed. The testes should be examined for any masses, because men seeking vasectomies are in the age range for testic- 2006ELSEVIER INC. UROLOGY 68: 9 14, /06/$32.00 ALL RIGHTS RESERVED doi: /j.urology
2 ular cancer. This is also an opportunity for doctors to show men how to perform a testicular self-examination. 3 Certain conditions in which vasectomy should be delayed include active scrotal skin infections, epididymitis/orchitis, and balanitis because of the increased risk of postoperative infections. Men who have large varicoceles, hydroceles, or inguinal hernias may undergo vasectomy simultaneously with the repair of these other conditions. If an intrascrotal mass is present, a workup, including scrotal ultrasonography, must be performed before vasectomy to rule out malignancy. Caution should be used in men with a history of previous scrotal surgery and cryptorchidism, because it can be very difficult to locate the vas, making no-scalpel access more difficult. Men who have undergone prior varicocelectomy, especially with a non-artery-sparing or nonmicroscopic technique, are at risk of postvasectomy testicular atrophy if the testicular artery was ligated at varicocelectomy and they are dependent on the vasal artery for the blood supply to the testis. In these men, vasectomy should only be performed microsurgically, with preservation of the vasal (deferential) arteries and veins. Situations in which vasectomy should not be done include men with bleeding diatheses because they are at risk for hematomas, which can grow to frightening size. Young men or men who are not in permanent relationships should consider other forms of birth control. ANESTHESIA Until recently, anesthesia for vasectomy was administered into the scrotal skin and vas with a needle. However, the initial needle puncture is commonly the most anxiety-provoking aspect of the procedure for the patient. Now, a new and virtually painless application of anesthesia has been introduced that has revolutionized performance of vasectomy. 1,14 The purpose of no-needle jet injection, also called no-needle vasectomy, is to simplify the application of anesthesia for vasectomy, allay the fear of needles, and make vasectomy less painful. NEEDLE INJECTION The first steps are to shave the scrotum, secure the penis against the patient s lower abdomen, and prepare the surgical area with Betadine. The next step involves bringing one vas to the scrotal surface at the median raphe using the three-finger technique to stabilize the vas (Fig. 1A). For right-handed physicians, the left thumb is placed on the median raphe halfway between the base of the penis and the superior aspect of the testes. The left middle finger finds the vas on its posterior surface and brings it up to the median A C B Vas (2 to 3cc) FIGURE 1. (A) Three-finger technique to isolate vas from vessels in spermatic cord. (B) Local vasal nerve block: raise wheal at skin surface, inject 2 to 3 ml of anesthetic solution along vas approximately 2 to 3 cm proximal to vasectomy site. (C) Needle injection of anesthesia using three-finger technique. Parts A and B were modified, with permission, from Weiss RS, and Li PS: No-needle jet anesthetic technique for no-scalpel vasectomy. J Urol 173(5): , raphe so that it is caught between the thumb and middle finger (isolating it away from the rest of the testicular vessels in the spermatic cord). The index finger is then placed on the anterior surface of the vas proximal to where the other two fingers have the vas secured. The standard anesthesia technique for no-scalpel vasectomy is a local vasal nerve block using a needle injection with 1% to 2% lidocaine without epinephrine (Fig. 1B,C). Initially, a wheal is raised at the skin surface. Then, the needle is advanced deeply and proximally along the perivasal sheath while injecting 2 to 3 ml of anesthetic solution. We suggest a single injection instead of multiple injections to reduce the risk of injury to the testicular vessels and subsequent hematoma. 1,6,15 NO-NEEDLE JET INJECTION (NO-NEEDLE VASECTOMY) The jet injection technique uses an instrument that generates a high-pressure spray that forces anesthetic solution through the skin, vas, and surrounding vasal tissues providing complete anesthetic block of the vas (Fig. 2A). It provides near perfect, painless anesthesia, almost never requiring application of additional anesthetic. 1,5 Currently, MadaJet (US $568 to $662/set) is the brand used by our institution to perform no-needle vasectomy. Numerous jet injectors are available that are used in other fields of medicine. Some of these include the Syrijet Mark II (US $1649/set, Keystone Industries, Cherry Hill, NJ) and the Frenchmade DermoJet (US $550/set, Akra Dermojet, Pau, France). The Syrijet Mark II is primarily used by 10 UROLOGY 68 (1), 2006
3 A B Jet Injector (0.1cc) dentists and requires a special anesthetic cartridge. Currently, MadaJet is the most reliable and appropriate for vasectomy. No-needle jet injection has multiple advantages. 1 It is less traumatic to the tissues, uses only one tenth the volume of anesthetic solution (approximately 0.1 ml/spray), and has a much more profound and faster onset of action (seconds versus minutes). The incidence of hematoma using jet injection is very low and, in experienced hands, can be negligible. 1,16 This was illustrated by Weiss et al. 14 who had no hematomas develop after performing no-needle vasectomy on 1391 patients in All the components of the jet injector are autoclavable for proper sterilization. Approximately 4 to 5 ml of anesthetic solution is used to load the filling chamber. The jet injector assembly is affixed to the filling chamber. A spacer with a notch at the tip of the jet injector fits over the vas and allows enough distance for the spray of anesthesia to spread out in a cone-shaped distribution before and just after penetrating the skin. The instrument is then primed by pumping the lever and firing several times to ensure it is functioning properly. The patient is positioned and shaved as described previously. The right vas is grasped using the three-finger technique and brought to the surface of the scrotal skin at the median raphe. It is important to wear a finger protector over the middle finger of the nondominant hand behind the vas to prevent accidental injection of anesthesia through the scrotum into the practitioner s finger. This will only occur if the vas is not trapped in the groove of the injector. Normally, if the injection is properly directed into the vas wall, it will not penetrate through the posterior scrotal wall. C Vas Skin FIGURE 2. (A) Jet injector. (B) Jet injection of anesthesia along median raphe using three-finger technique. (C) Jet injection dispersion pattern. Part C was modified, with permission, from Weiss RS, and Li PS: Noneedle jet anesthetic technique for no-scalpel vasectomy. J Urol 173(5): , The skin over the median raphe only has to be swabbed with an alcohol pad before the administration of anesthesia. The groove in the spacer on the tip of the jet injector is placed firmly over the right vas on the median raphe at the junction of the upper one third and lower two thirds of the scrotum (Fig. 2B). Three sprays of anesthesia are applied along the left lateral aspect of the median raphe approximately 4 to 5 mm apart. Then, the left vas is brought to the same position at the median raphe, except that three injections are applied to the right lateral aspect of the median raphe adjacent to the previous injections. This crossed anesthesia along the median raphe gives a wider anesthetic field to the skin and underlying tissues and ensures patient comfort throughout the skin puncture and tissue manipulation during no-scalpel vasectomy. The jet injection is very effective because the anesthesia solution disperses in an inverted cone-shape distribution, affecting all the tissues to a depth of 4 to 4.5 mm from the skin surface (Fig. 2C). The anesthetic solution is quickly absorbed by the tissue around the vas, with much less trauma and pain than after needle injection. No skin wheal or local edema is present at the injection site, making no-scalpel vasectomy easier to perform. The injection sites are recognized by small blanched discolorations of the skin. Studies have been performed analyzing the pain scores involved in the application of anesthesia for vasectomy and the vasectomy itself. Using a visual analog scale, Weiss and Li 1 found that the average pain score for the jet injection of anesthesia was 1.71 of 10 (range 1 to 7.40, median 1.3). The average visual analog scale pain score for the vasectomy that was subsequently performed after jet injection was 0.66 of 10 (range 0 to 6.60, median 0.2). 1 The area is then prepared with Betadine and draped in standard surgical fashion. At this time, the tip of the jet injector should be soaked in a disinfectant solution (MadaCide is recommended by Mada Medical Products) to adequately sterilize it before its use on the next patient. SURGICAL PROCEDURE Vasectomy consists of two components: access to the vas and vasal occlusion. It is important to understand that the no-scalpel vasectomy is one method for gaining access to the vas and conventional vasectomy is another option. Once the vas is delivered out of the scrotum, the method of vasal occlusion can vary depending on physician preference. ACCESS TO THE VAS Conventional vasectomy involves making either bilateral transverse incisions high on the scrotum UROLOGY 68 (1),
4 or the preferred single vertical incision on the median raphe to expose the vas. At this point, any of the many techniques for vasal occlusion can be used. Once this has been accomplished, the scrotal incisions can either be left open if they are less than 1 cm long or closed with a few interrupted absorbable sutures. The no-scalpel vasectomy has been proved a superior method of gaining access to the vas compared with conventional vasectomy. It is an elegant technique for exposing the vas through a tiny puncture wound 2 to 3 mm in length, with negligible pain and trauma to the surrounding tissues. 3 Not only can it be performed faster, but the incidence of hematomas and infections is decreased and the postoperative recovery time is shorter. 17 The first step is to fix one of the vas against the scrotal skin at the median raphe using the threefinger technique. A ring-tipped fixation clamp is used to grasp the vas through the skin. One blade of a sharp, pointed, curved mosquito hemostat (dissecting forceps) is used to puncture through the scrotal skin for 5 mm or to the lumen of the vas. The instrument is removed, and both tips of the dissecting forceps are reinserted into the puncture site and spread transversely across the vas to strip the skin and vasal sheath away from the bare vas. After spreading the tissue on top of the vas adequately, one blade of the dissecting forceps is used to pierce the vas to the lumen. The blade inside the vas lumen is rotated 180 and then the vas is lifted up and out through the scrotal skin, at the same time releasing the ring clamp. This will allow the vas to be pulled up and out of the scrotal skin. The exposed vas is regrasped with the ring clamp to keep it from falling back into the scrotum. Approximately 1 cm of the vas is dissected free from its sheath longitudinally with the dissecting forceps. The vas is occluded using any of the techniques described below. The contralateral vas is brought through the same puncture site and is occluded using an identical approach. At the end of the procedure, it is necessary to inspect the ends of the vas and the wound for any bleeding to prevent hematoma formation. It is seldom necessary to close the puncture wound with sutures. It is merely compressed for 1 minute and then covered with antibiotic ointment. VAS OCCLUSION Numerous techniques for vasal occlusion exist and are used throughout the world. These include ligation of the vas with either suture or clips, excision of a segment of vas of various lengths, folding back the end of the vas onto itself, fascial interposition between the cut ends of the vas, and cautery of the lumen of the vas (thermal or electric). 10 These techniques have been used alone and in various combinations. However, it has been difficult to determine which method or combination of methods is truly most effective to prevent recanalization and vasectomy failure because of the heterogeneity of study design, surgical technique used, and assessment of results. 10 The method used most often worldwide is suture ligation and excision. This is especially true for economically challenged areas, because it is the simplest and quickest technique to perform, with the least amount of materials needed. 18 However, this technique used alone is the least effective and has a failure rate of approximately 1% to 5%. 2 This could be because of necrosis at the ends of the vas distal to the ligature, allowing recanalization to occur more easily. Some studies have shown that the addition of fascial interposition, in which the vasal sheath is pulled back over the cut end of the vas and secured in place, increases the effectiveness of vasal occlusion by ligation and excision. 10 Nevertheless, fascial interposition is a more complicated technique and increases the time needed to perform vasectomy. The most effective technique is thought to be cautery combined with fascial interposition. Data collected from multiple studies have shown a failure rate of 0% to 1.2%. 10 However, it has been debated whether thermal versus electric cautery is more effective. Several studies have suggested thermal cautery to be superior. One study in particular showed histologic proof of the ability of thermal cautery over electric cautery to occlude the vas, as evidenced by fewer cases of vasitis nodosa and spermatic granuloma. 19 Even with this information, the question remains whether cautery alone is better than ligation and excision. A recent survey of vasectomists in the United States looked at the use of different vasal occlusion methods specifically in America. The survey found that 70% used cautery to occlude the vas during vasectomy. The second most popular occlusion technique is ligation, used by approximately 60% of practitioners. Additionally, about one quarter of all vasectomists apply metal clips to the vas. 20 RESULTS AND COMPLICATIONS The most common complications associated with vasectomy are hematoma formation and infection. On average, 2% of conventional vasectomies are complicated by the formation of a hematoma postoperatively. 4 With the no-scalpel technique, the incidence of hematoma is less than 0.5%. Infection is a relatively rare occurrence when vasectomy is performed under sterile conditions. However, when it 12 UROLOGY 68 (1), 2006
5 does occur, it is usually associated with an underlying hematoma. 3 It is well documented that that the experience of the physician is the most important factor in the incidence of complications encountered after vasectomy. 4 Sperm granulomas form when sperm leak from the testicular side of the vas, leading to an inflammatory reaction. Some studies have shown that the formation of sperm granulomas can have a positive effect on patency rates in vasectomy reversals by decreasing the pressure-induced damage on the epididymis. 21 However, sperm granulomas can lead to unacceptably high recanalization and vasectomy failure rates. 3 Most pressure produced on the testicular side of the vas after occlusion is transmitted to the epididymis and efferent ductules, but not the seminiferous tubules. Minimal damage more distally in the system has been shown by electron microscopic studies of the testis, demonstrating areas of basal lamina thickening and spermatogenesis disruption. 22 However, Leydig cells remained normal, with no injury to their structure or function. 3 Several possible long-term effects associated with vasectomy include chronic testicular/epididymal pain, testicular dysfunction, vasitis nodosa, and chronic epididymal obstruction. 2 Approximately 1 in 1000 men will experience chronic testicular/epididymal pain postoperatively. 23 Possible treatments for this bothersome complication include vasectomy reversal, open-ended vasectomy, or even total epididymovasectomy. Systemic effects such as the development of antisperm antibodies can occur secondary to breakdown of the blood-testicular barrier. It has been postulated that the formation of immune complexes can occur, ultimately leading to atherosclerosis. However, multiple studies have failed to show the formation of these immune complexes or their deposition in vasectomized men. 2,3 There has also been a concern that vasectomy may increase the incidence of prostate and testicular cancer. This initial perception was probably a result of a selection bias because men undergoing vasectomy were seeing a urologist and were more likely to be screened, and therefore diagnosed, with urologic cancer. Many studies have shown this to be false. Men can be comfortable that vasectomy will not put them at a greater risk of genitourinary cancer. 3 Before a man can start having unprotected sex after vasectomy, he must be completely azoospermic. At least one to two semen analyses 4 to 6 weeks apart should be obtained 12 weeks after surgery. A repeat vasectomy should be performed if any motile sperm are found in the ejaculate 3 months after surgery. 2 OPPORTUNITIES AND MARKETING POTENTIAL Although no-scalpel vasectomy was introduced to the United States more than 20 years ago, many urologists still do not know how to perform this technique properly. Now, with the addition of noneedle vasectomy for the application of local anesthesia, there is a wonderful opportunity to provide men with a virtually painless and extremely effective form of permanent contraception. Vasectomy is an excellent opportunity for additional revenue for any urologist. Physicians can charge approximately U.S. $650 per vasectomy, which is commonly a cash-pay procedure compared with the U.S. $100 billed for a new level 3 patient visit. Vasectomy takes only 10 to 20 minutes to perform, resulting in a tremendous revenue/time ratio. If a physician can add five vasectomies a month by increased exposure on the Internet, this translates into a profit of U.S. $3000 to 4500/mo or US $40,000 to 55,000 annually. Another advantage to performing more vasectomy procedures is that urologists can increase their practice by additional patients and referrals from the patients friends and family with other urologic conditions. ACKNOWLEDGMENT. To Drs. Ronald Weiss and Doug Stein in pioneering the use and acceptance of no-scalpel and no-needle vasectomy and for sharing their experiences with us and to Dr. Ronald Weiss for allowing us to use some of his surgical images in Figures 1 and 2. REFERENCES 1. Weiss RS, and Li PS: No-needle jet anesthetic technique for no-scalpel vasectomy. J Urol 173: , Goldstein M: Surgical management of male infertility and other scrotal disorders, in Walsh PC, Retik AB, Vaughan ED, et al (Eds): Campbell s Urology, 8th ed. New York, WB Saunders, 2002, pp Schlegel PN, and Goldstein M: Vasectomy, in Goldstein M (Ed): Surgery of Male Infertility. New York, WB Saunders, 1995, pp Kendrick J, Gonzales B, Huber D, et al: Complications of vasectomies in the United States. J Fam Prac 25: , Wilson CL: No-needle anesthetic for no-scalpel vasectomy. Am Fam Physician 63: 1295, Li S, Goldstein M, Zhu J, et al: The no-scalpel vasectomy. J Urol 145: , Viladoms JM, and Li PS: Vasectomia sin Bisturi. Arch Esp Urol 47: , Kaza RM, Singh I, Singhal S, et al: An evaluation of the no-scalpel vasectomy technique. BJU Int 83: , Nirathpongporn A, Huber D, and Krieger JN: Noscalpel vasectomy at the King s birthday vasectomy festival. Lancet 335: , Labrecque M, Defresne C, Barone MA, et al: Vasectomy surgical techniques: a systematic review. BMC Med 2: 21 33, Skiver M, Skovsgaard F, and Miskowiak J: Conventional or Li vasectomy: a questionnaire study. BJU Int 79: , UROLOGY 68 (1),
6 12. Haws JM, and Feigin J: Vasectomy counseling. Am Fam Physician 52: , Schmidt SS: Vasectomy. Urol Clin North Am 14: , Weiss RS, Li PS, and Goldstein M: No-needle jet anesthetic technique for the no-scalpel vasectomy (abstract). Can J Urol 12: 2664, Li PS, Li SQ, Schlegel PN, et al: External spermatic sheath injection for vasal nerve block. Urology 39: , Weiss RS, and Li PS: No-needle jet anesthetic technique for the no-scalpel vasectomy (abstract). J Urol 173: , Sokal D, McMullen S, Gates D, et al: The male sterilization investigator team: a comparative study of the no scalpel and standard incision approaches to vasectomy in 5 countries. J Urol 162: , Labrecque M, Pile J, Sokal D, et al: Vasectomy surgical techniques in South and South East Asia. BMC Urol 5: 10 19, Schmidt SS, and Minckler TM: The vas after vasectomy: comparison of cauterization methods. Urology 40: , Haws JM, Morgan GT, Pollack AE, et al: Clinical aspects of vasectomies performed in the United States in Urology 52: , Silber SJ: Sperm granulomas and reversibility of vasectomy. Lancet 2: , Jarow JP, Budin RE, Dym M, et al: Quantitative pathological changes in the human testis after vasectomy. N Engl J Med 313: , McConaghy P, Paxton LD, and Loughlin V: Chronic testicular pain following vasectomy. Br J Urol 77: 328, UROLOGY 68 (1), 2006
Vasectomy for the Non-Vasectomist
 Vasectomy for the Non-Vasectomist Michel Labrecque MD PhD Department of Family and Emergency Medicine Laval University Quebec City Canada FMF 2014 Conflicts of Interests I perform vasectomy 25 000+ vasectomies
Vasectomy for the Non-Vasectomist Michel Labrecque MD PhD Department of Family and Emergency Medicine Laval University Quebec City Canada FMF 2014 Conflicts of Interests I perform vasectomy 25 000+ vasectomies
Surgical Approach and Occlusion of the Vasa
 From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth 5 Surgical Approach and Occlusion of the Vasa A lthough the no-scalpel technique is almost bloodless, an
From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth 5 Surgical Approach and Occlusion of the Vasa A lthough the no-scalpel technique is almost bloodless, an
No-Needle Anaesthesia for No-Scalpel Vasectomy: An Instructive Guide for Surgeons
 No-Needle Anaesthesia for No-Scalpel Vasectomy: An Instructive Guide for Surgeons Ronald S. Weiss, M.D. Philip S. Li, M.D. Copyright 2011 The Weiss Clinic, Ottawa, Canada www.vasectomystore.com www.vasectomy.ca
No-Needle Anaesthesia for No-Scalpel Vasectomy: An Instructive Guide for Surgeons Ronald S. Weiss, M.D. Philip S. Li, M.D. Copyright 2011 The Weiss Clinic, Ottawa, Canada www.vasectomystore.com www.vasectomy.ca
Introduction. Hands-On Training Recommended. From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth
 From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth Introduction The purpose of this guide is to provide physicians with an easy-to-use reference for learning
From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth Introduction The purpose of this guide is to provide physicians with an easy-to-use reference for learning
1. Pre-operative counseling:
 VASECTOMY UPDATE 2010 Dr. Armand Zini Associate Professor, Division of Urology, McGill University Montreal, Quebec Conflict of Interest: None 1. Pre-operative counseling: Vasectomy is a safe and effective
VASECTOMY UPDATE 2010 Dr. Armand Zini Associate Professor, Division of Urology, McGill University Montreal, Quebec Conflict of Interest: None 1. Pre-operative counseling: Vasectomy is a safe and effective
A comparative study of scalpel versus no scalpel vasectomy
 International Surgery Journal Patel HR et al. Int Surg J. 2018 May;5(5):1708-1712 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181406
International Surgery Journal Patel HR et al. Int Surg J. 2018 May;5(5):1708-1712 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181406
Vasectomy: The other form of sterilization
 Vasectomy: The other form of sterilization Grace Shih, MD MAS David Turok, MD MPH Willie Parker, MD MPH Reproductive Health September 2010 Disclosures David Turok receives research support from Duramed
Vasectomy: The other form of sterilization Grace Shih, MD MAS David Turok, MD MPH Willie Parker, MD MPH Reproductive Health September 2010 Disclosures David Turok receives research support from Duramed
Chapter 9. Summary & conclusion
 Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
An inexpensive yet realistic model for teaching vasectomy
 Surgical Technique Vol. 41 (2): 373-378, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.27 An inexpensive yet realistic model for teaching vasectomy Taylor M. Coe 1, John Curington 2 1 University
Surgical Technique Vol. 41 (2): 373-378, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.27 An inexpensive yet realistic model for teaching vasectomy Taylor M. Coe 1, John Curington 2 1 University
Vasectomy. Daniel Stulberg, MD University of New Mexico November 6, 2013
 Vasectomy Daniel Stulberg, MD University of New Mexico November 6, 2013 Goals Objectives Participants will Know the risks of vasectomy Know the benefits of vasectomy Understand the technique of no scalpel
Vasectomy Daniel Stulberg, MD University of New Mexico November 6, 2013 Goals Objectives Participants will Know the risks of vasectomy Know the benefits of vasectomy Understand the technique of no scalpel
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
THE PATIENT S GUIDE TO VASECTOMY
 The Vasectomy Decision This set of frequently asked questions is designed to help you understand what a vasectomy is, and whether it is the right form of birth control for you at this stage in your life.
The Vasectomy Decision This set of frequently asked questions is designed to help you understand what a vasectomy is, and whether it is the right form of birth control for you at this stage in your life.
INTRODUCTION METHODS. Hyun Joon Moon, MD, PhD
 Singapore Med J 2015; 56(4): 228-232 doi: 10.11622/smedj.2014191 A feasible ambulatory mini-incision microsurgical vasovasostomy under local anaesthesia using a specially designed double-ringed clamp that
Singapore Med J 2015; 56(4): 228-232 doi: 10.11622/smedj.2014191 A feasible ambulatory mini-incision microsurgical vasovasostomy under local anaesthesia using a specially designed double-ringed clamp that
A SUWRELESS TECHNIC FOR BIlATERAL PARTIAL VASECfOMY
 FERTIUTY AND STERILITY Copyright 1972 by The Williams & Wilkins Co. Vol. 23, No.1, January 1972 Printed in U.S.A. A SUWRELESS TECHNIC FOR BIlATERAL PARTIAL VASECfOMY WILLIAM M. MOSS, M.D., F.A.C.S. * Assistant
FERTIUTY AND STERILITY Copyright 1972 by The Williams & Wilkins Co. Vol. 23, No.1, January 1972 Printed in U.S.A. A SUWRELESS TECHNIC FOR BIlATERAL PARTIAL VASECfOMY WILLIAM M. MOSS, M.D., F.A.C.S. * Assistant
Lincolnshire Knowledge and Resource Service
 Lincolnshire Knowledge and Resource Service This search summary contains the results of a literature search undertaken by the Lincolnshire Knowledge and Resource Service librarians in; October 2013 All
Lincolnshire Knowledge and Resource Service This search summary contains the results of a literature search undertaken by the Lincolnshire Knowledge and Resource Service librarians in; October 2013 All
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
How-To Booklet: Pediatric Spay-Neuter. Surgical Techniques Pictorial
 How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy
 www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.782 Infection/Inflammation Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy Seung Hoon Cho, Seung Ki Min, Seung Tae
www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.782 Infection/Inflammation Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy Seung Hoon Cho, Seung Ki Min, Seung Tae
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
Preoperative Consultation
 Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Lincolnshire Knowledge and Resource Service
 Lincolnshire Knowledge and Resource Service This search summary contains the results of a literature search undertaken by the Lincolnshire Knowledge and Resource Service librarians in October 2011. All
Lincolnshire Knowledge and Resource Service This search summary contains the results of a literature search undertaken by the Lincolnshire Knowledge and Resource Service librarians in October 2011. All
Teche Regional Urology David C. Benson, MD, FACS 1302 Lakewood Drive Suite 100 Morgan City, La
 VASECTOMY PATIENT INFORMATION I. Purpose of the operation The intent of the operation, known as bilateral partial vasectomy, is to render you sterile (i.e. unable to cause a pregnancy in a female partner).
VASECTOMY PATIENT INFORMATION I. Purpose of the operation The intent of the operation, known as bilateral partial vasectomy, is to render you sterile (i.e. unable to cause a pregnancy in a female partner).
HALTON VASECTOMY CLINIC PATIENT MANUAL
 Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Georgetown Hospital
Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Georgetown Hospital
REVERSIBILITY OF STERILIZATION PRODUCED BY VAS OCCLUSION CLIP*
 FERTILITY AND STERILITY Copyright @ 1971 by The Williams & Wilkins Co. Vol. 22, No.4, April 1971 Printed in U.S.A. REVERSIBILITY OF STERILIZATION PRODUCED BY VAS OCCLUSION CLIP* P. s. JHAVER,t JOSEPH E.
FERTILITY AND STERILITY Copyright @ 1971 by The Williams & Wilkins Co. Vol. 22, No.4, April 1971 Printed in U.S.A. REVERSIBILITY OF STERILIZATION PRODUCED BY VAS OCCLUSION CLIP* P. s. JHAVER,t JOSEPH E.
THE PATIENT S GUIDE TO VASECTOMY REVERSAL
 The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
NO-SCALPEL VASECTOMY
 Dr William Lynch MRCGP MICGP Vasectomist & GP Surgeon FREEPHONE 1800 313 595 NO-SCALPEL VASECTOMY An affordable and permanent method of family planning for men. Advantages: Less Discomfort One small opening
Dr William Lynch MRCGP MICGP Vasectomist & GP Surgeon FREEPHONE 1800 313 595 NO-SCALPEL VASECTOMY An affordable and permanent method of family planning for men. Advantages: Less Discomfort One small opening
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY
 MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
No-Scalpel Vasectomy. Vasectomy
 No-Scalpel Vasectomy Vasectomy Once a man or a couple decides to not have more children, they usually consider permanent contraception. Vasectomy is a safe and very effective form of permanent birth control
No-Scalpel Vasectomy Vasectomy Once a man or a couple decides to not have more children, they usually consider permanent contraception. Vasectomy is a safe and very effective form of permanent birth control
STERILITY IN MALE ANIMALS INDUCED BY INJECTION OF CHEMICAL AGENTS INTO THE VAS DEFERENS*
 FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No. 11, November 1973 Printed in U.S.A. STERILITY IN MALE ANIMALS INDUCED BY INJECTION OF CHEMICAL AGENTS INTO THE VAS DEFERENS*
FERTILITY AND STERILITY Copyright 1973 by The Williams & Wilkins Co. Vol. 24, No. 11, November 1973 Printed in U.S.A. STERILITY IN MALE ANIMALS INDUCED BY INJECTION OF CHEMICAL AGENTS INTO THE VAS DEFERENS*
VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD
 Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Academic Script Surgical Techniques Like Ovariectomy, Orchidectomy, Adrenalectomy, Etc
 Academic Script Surgical Techniques Like Ovariectomy, Orchidectomy, Adrenalectomy, Etc Aim: To Study the Surgical Techniques like Ovariectomy, Orchidectomy, Adrenalectomy, Tubectomy and Vasectomy in Rodents
Academic Script Surgical Techniques Like Ovariectomy, Orchidectomy, Adrenalectomy, Etc Aim: To Study the Surgical Techniques like Ovariectomy, Orchidectomy, Adrenalectomy, Tubectomy and Vasectomy in Rodents
TORONTO WEST GTA. Vasectomy. vasectomía
 TORONTO WEST GTA Vasectomy vasectomía You are either considering or about to have a vasectomy. Patients who are informed and prepared for vasectomy can recover in less time and with less pain. This booklet
TORONTO WEST GTA Vasectomy vasectomía You are either considering or about to have a vasectomy. Patients who are informed and prepared for vasectomy can recover in less time and with less pain. This booklet
Vasectomy, which is one of the few contraceptive options
 Vasectomy in the United States, 2002 Mark A. Barone,* Paul L. Hutchinson, Christopher H. Johnson, Jason Hsia and Jennifer Wheeler From EngenderHealth (MAB), New York, New York, Department of International
Vasectomy in the United States, 2002 Mark A. Barone,* Paul L. Hutchinson, Christopher H. Johnson, Jason Hsia and Jennifer Wheeler From EngenderHealth (MAB), New York, New York, Department of International
THE PATIENT S GUIDE TO VARICOCELE
 The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES
 Nagoya J. Med. Sci. 60. 37-42, 1997 SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES MASANORI YAMAMOTO, HATSUKI HIBI, KEISUKE YOKOI, ATSUSHI MISHIMA and SATOSHI KATSUNO Department
Nagoya J. Med. Sci. 60. 37-42, 1997 SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES MASANORI YAMAMOTO, HATSUKI HIBI, KEISUKE YOKOI, ATSUSHI MISHIMA and SATOSHI KATSUNO Department
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
VASECTOMY COUNSELING If you are thinking of having a vasectomy, there are some important things you should know before the vasectomy is done.
 VASECTOMY COUNSELING If you are thinking of having a vasectomy, there are some important things you should know before the vasectomy is done.* Vasectomy is intended to be a permanent form of contraception.
VASECTOMY COUNSELING If you are thinking of having a vasectomy, there are some important things you should know before the vasectomy is done.* Vasectomy is intended to be a permanent form of contraception.
EZ (NO -SCALPEL, NO -NEEDLE) VASECTOMY
 EZ (NO -SCALPEL, NO -NEEDLE) VASECTOMY Vasectomy is a method of birth control chosen by more than 500,000 men each year in the United States. It is a simple, safe procedure that is more than 99% effective
EZ (NO -SCALPEL, NO -NEEDLE) VASECTOMY Vasectomy is a method of birth control chosen by more than 500,000 men each year in the United States. It is a simple, safe procedure that is more than 99% effective
THE BIPOLAR NEEDLE FOR VASECTOMY. I. EXPERIENCE WITH THE FIRST 1000 CASES*
 FERTILITY AND STERILITY Copyright 1978 The American Fertility Society Vol. 29, No.6, June 1978 Printed in U.SA. THE BIPOLAR NEEDLE FOR VASECTOMY. I. EXPERIENCE WITH THE FIRST 1000 CASES* STANWOOD S. SCHMIDT,
FERTILITY AND STERILITY Copyright 1978 The American Fertility Society Vol. 29, No.6, June 1978 Printed in U.SA. THE BIPOLAR NEEDLE FOR VASECTOMY. I. EXPERIENCE WITH THE FIRST 1000 CASES* STANWOOD S. SCHMIDT,
American Urological Association (AUA) Guideline
 1 (AUA) Guideline VASECTOMY: AUA GUIDELINE Ira D. Sharlip, Arnold M. Belker, Stanton Honig, Michel Labrecque, Joel L. Marmar, Lawrence S. Ross, Jay I. Sandlow, David C. Sokal Approved by the AUA Board
1 (AUA) Guideline VASECTOMY: AUA GUIDELINE Ira D. Sharlip, Arnold M. Belker, Stanton Honig, Michel Labrecque, Joel L. Marmar, Lawrence S. Ross, Jay I. Sandlow, David C. Sokal Approved by the AUA Board
VASECTOMY. Unit 9. Learning Objectives. Teaching Resources In This Unit
 Unit 9 VASECTOMY Learning Objectives By the end of this unit, learners should be able to: Define vasectomy List the types of surgical techniques used for vasectomy Explain how vasectomy works State the
Unit 9 VASECTOMY Learning Objectives By the end of this unit, learners should be able to: Define vasectomy List the types of surgical techniques used for vasectomy Explain how vasectomy works State the
CONSENT TO STERILIZATION OPERATION (SURGICAL VASECTOMY)
 CONSENT TO STERILIZATION OPERATION (SURGICAL VASECTOMY) I (Patient s Name) have been given the following information: Explanation of Sterilization: Vasectomy is a minor surgical procedure that can be performed
CONSENT TO STERILIZATION OPERATION (SURGICAL VASECTOMY) I (Patient s Name) have been given the following information: Explanation of Sterilization: Vasectomy is a minor surgical procedure that can be performed
UNDERSTANDING. Permanent Birth Control for Men
 UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
NO-SCALPEL VASECTOMY IN A CAMP APPROACH: FOLLOW-UP, COMPLICATIONS AND COMPLIANCE
 Original Article NO-SCALPEL VASECTOMY IN A CAMP APPROACH: FOLLOW-UP, COMPLICATIONS AND COMPLIANCE Patel Piyush R 1, Shah D K 2, Modi Anjali 3, Mistry Sunita N 4 Financial Support: None declared Conflict
Original Article NO-SCALPEL VASECTOMY IN A CAMP APPROACH: FOLLOW-UP, COMPLICATIONS AND COMPLIANCE Patel Piyush R 1, Shah D K 2, Modi Anjali 3, Mistry Sunita N 4 Financial Support: None declared Conflict
VASECTOMY INFORMATION AND CONSENT
 VASECTOMY INFORMATION AND CONSENT This information will help you understand more about the vasectomy: the indications for this procedure, the success and failure rates, the alternative forms of contraception,
VASECTOMY INFORMATION AND CONSENT This information will help you understand more about the vasectomy: the indications for this procedure, the success and failure rates, the alternative forms of contraception,
MICROSURGICAL VASECTOMY REVERSAL
 MICROSURGICAL VASECTOMY REVERSAL TECHNIQUES TO IMPROVE OUTCOME By Edward Karpman, MD, Daniel H. Williams IV, MD, and Larry I. Lipshultz, MD In the United States today, men are playing a greater role in
MICROSURGICAL VASECTOMY REVERSAL TECHNIQUES TO IMPROVE OUTCOME By Edward Karpman, MD, Daniel H. Williams IV, MD, and Larry I. Lipshultz, MD In the United States today, men are playing a greater role in
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
Surgery Illustrated Surgical Atlas Inguinal orchidectomy for testicular cancer
 Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
How Long To Heal After Vasectomy Reversal Can You Have Intercourse
 How Long To Heal After Vasectomy Reversal Can You Have Intercourse The recovery after vasectomy reversal is very important. If you can have help for a week, so that other person can do all the lifting,
How Long To Heal After Vasectomy Reversal Can You Have Intercourse The recovery after vasectomy reversal is very important. If you can have help for a week, so that other person can do all the lifting,
the liver and kidney function (both vital when dealing with anaesthetic drugs) and to rule out any unsuspected illnesses.
 Orchiectomy: Castration reduces overpopulation by inhibiting male fertility and decreases male aggressiveness, roaming, and undesirable urination behaviour. It helps prevent androgenrelated diseases, including
Orchiectomy: Castration reduces overpopulation by inhibiting male fertility and decreases male aggressiveness, roaming, and undesirable urination behaviour. It helps prevent androgenrelated diseases, including
Comparing three different surgical techniques used in adult bilateral varicocele
 Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Male Infertility Caused by Varicoceles
 What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration.
 Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Ambulatory Phlebectomy & Sclerotherapy. Dr. S. Kundu Medical Director The Vein Institute of Toronto
 Ambulatory Phlebectomy & Sclerotherapy Dr. S. Kundu Medical Director The Vein Institute of Toronto 1 Disclosures Consultant: Bard Canada Boston Scientific Canada Edwards Life Sciences Baylis Canada Sigmacon
Ambulatory Phlebectomy & Sclerotherapy Dr. S. Kundu Medical Director The Vein Institute of Toronto 1 Disclosures Consultant: Bard Canada Boston Scientific Canada Edwards Life Sciences Baylis Canada Sigmacon
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Recommended pre- and post-operative supplies for your No-Scalpel Vasectomy*
 Recommended pre- and post-operative supplies for your No-Scalpel Vasectomy* 1. Antibacterial wash: Wash your scrotum nightly for 3 days prior to your vasectomy and 2 days afterward. 2. Hospital razor:
Recommended pre- and post-operative supplies for your No-Scalpel Vasectomy* 1. Antibacterial wash: Wash your scrotum nightly for 3 days prior to your vasectomy and 2 days afterward. 2. Hospital razor:
حسام أبو عوض. -Dr. Mohammad Muhtasib. 1 P a g e
 5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA
 www.ivis.org Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA November 2-5, 2011 Hyderabad, India Reprinted in IVIS with the Permission of WEVA Organizers
www.ivis.org Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA November 2-5, 2011 Hyderabad, India Reprinted in IVIS with the Permission of WEVA Organizers
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Early experience of laparoscopic varicocelectomy in College
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Minimal Hydrocelectomy with the aid of scrotoscope: a ten-year experience
 ORIGINAL ARTICLE Vol. 40 (3): 384-389, May - June, 2014 doi: 10.1590/S1677-5538.IBJU.2014.03.13 Minimal Hydrocelectomy with the aid of scrotoscope: a ten-year experience Yan Bin, Wei Yong-bao, Yin Zhuo,Yang
ORIGINAL ARTICLE Vol. 40 (3): 384-389, May - June, 2014 doi: 10.1590/S1677-5538.IBJU.2014.03.13 Minimal Hydrocelectomy with the aid of scrotoscope: a ten-year experience Yan Bin, Wei Yong-bao, Yin Zhuo,Yang
acornsurgery Patient s Guide to Non-Scalpel Vasectomy (NSV) & Pre & Post Operative Care
 acornsurgery Patient s Guide to Non-Scalpel Vasectomy (NSV) & Pre & Post Operative Care Quick and simple procedure No scalpel involved No stitches necessary Less painful than scalpel technique Only a 1
acornsurgery Patient s Guide to Non-Scalpel Vasectomy (NSV) & Pre & Post Operative Care Quick and simple procedure No scalpel involved No stitches necessary Less painful than scalpel technique Only a 1
DEFINITION HX & PH/EX
 DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
What are Varicoceles?
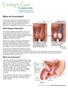 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT
 ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT Reproduct ion Physiology Section, Department of Zoology, University of Rajasthan, Jaipur-302004 Summary: Rats and mice were vasectomized
ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT Reproduct ion Physiology Section, Department of Zoology, University of Rajasthan, Jaipur-302004 Summary: Rats and mice were vasectomized
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
NUPAS HAVING A VASECTOMY. T: T: (01) (Eire) Your guide to advice & information for vasectomy
 NUPAS national unplanned pregnancy advisory service HAVING A VASECTOMY Your guide to advice & information for vasectomy T: 0333 004 6666 T: (01) 874 0097 (Eire) 2-3 HAVING A VASECTOMY AFTERCARE HELPLINE
NUPAS national unplanned pregnancy advisory service HAVING A VASECTOMY Your guide to advice & information for vasectomy T: 0333 004 6666 T: (01) 874 0097 (Eire) 2-3 HAVING A VASECTOMY AFTERCARE HELPLINE
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA
 PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
Vasectomy reversal: decision making and technical innovations
 Review Article Vasectomy reversal: decision making and technical innovations E. Will Kirby, Mark Hockenberry, Larry I. Lipshultz Baylor College of Medicine, Houston, Texas, USA Contributions: (I) Conception
Review Article Vasectomy reversal: decision making and technical innovations E. Will Kirby, Mark Hockenberry, Larry I. Lipshultz Baylor College of Medicine, Houston, Texas, USA Contributions: (I) Conception
THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS
 Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Penile implants What to expect and how to prepare
 Penile implants What to expect and how to prepare Penile implants can restore erectile function. Explore your choices and find out what to expect from this procedure. Penile implants are artificial devices
Penile implants What to expect and how to prepare Penile implants can restore erectile function. Explore your choices and find out what to expect from this procedure. Penile implants are artificial devices
Integra. SafeGuard Mini Carpal Tunnel Release System SURGICAL TECHNIQUE
 SafeGuard Mini Carpal Tunnel Release System SURGICAL TECHNIQUE SafeGuard Mini Carpal Release System Contents Surgical Technique...2 Description...2 The SafeGuard System...2 Indications...2 Contraindications...2
SafeGuard Mini Carpal Tunnel Release System SURGICAL TECHNIQUE SafeGuard Mini Carpal Release System Contents Surgical Technique...2 Description...2 The SafeGuard System...2 Indications...2 Contraindications...2
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM
 Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM 1) Other Names: Scrotum None Testicles Testes (Curry Tempkin, p. 236, 2/3/2) Ductus deferens spermatic cord (Tempkin, p. 279, Anatomy
Scrotum Kacey Morrison Amanda Baxter Sabrina Tucker July 18, 2006 SCROTUM 1) Other Names: Scrotum None Testicles Testes (Curry Tempkin, p. 236, 2/3/2) Ductus deferens spermatic cord (Tempkin, p. 279, Anatomy
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
Pre Vasectomy Consultation
 Pre Vasectomy Consultation Patient: Private/ GMS Date: D.o.B Tel. Occupation: GP: Number of children: Age of youngest child: General Health: Bleeding disorders: Medication: Allergies: Local Anaesthetics:
Pre Vasectomy Consultation Patient: Private/ GMS Date: D.o.B Tel. Occupation: GP: Number of children: Age of youngest child: General Health: Bleeding disorders: Medication: Allergies: Local Anaesthetics:
Dr Bruce Sutherland General Practitioner, Warkworth
 Dr Bruce Sutherland General Practitioner, Warkworth VASECTOMY Dr Bruce Sutherland Overview Embryology Anatomy Procedure Pre Op consultation Post Op care Pitfalls EMBRYOLOGY Fetus at age 7 weeks Fig.
Dr Bruce Sutherland General Practitioner, Warkworth VASECTOMY Dr Bruce Sutherland Overview Embryology Anatomy Procedure Pre Op consultation Post Op care Pitfalls EMBRYOLOGY Fetus at age 7 weeks Fig.
@DrAshBowen. ll Pain: Solving mysteries of the male scrotum
 @DrAshBowen ll Pain: Solving mysteries of the male scrotum On the Docket Good Hydrocele Epididymal cysts Varicocele Bad Testis Cancer/Tumor Epididymitis/Orchitis STI Torsion UGLY Chronic Orchalgia Post
@DrAshBowen ll Pain: Solving mysteries of the male scrotum On the Docket Good Hydrocele Epididymal cysts Varicocele Bad Testis Cancer/Tumor Epididymitis/Orchitis STI Torsion UGLY Chronic Orchalgia Post
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Instruction for the patient
 Instruction for the patient Your situation You are a 38-year-old, woman who is pregnant with her third child You and your partner agree that with this child your family is complete In the past, you used
Instruction for the patient Your situation You are a 38-year-old, woman who is pregnant with her third child You and your partner agree that with this child your family is complete In the past, you used
Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients
 Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
EVALUATION STUDY FOR AUTO-LIGATION OF VAS-DEFERENS METHOD TO TEASER BUCKS PREPARATION
 I.J.A..R, VOL. () 0: 06-0 ISSN 50 579 EVALUATION STUY FOR AUTO-LIGATION OF VAS-EFERENS METHO TO TEASER UKS PREPARATION Hussein Kareem Ibrahiem linical Sciences epartment/veterinary Medicine Faculty/University
I.J.A..R, VOL. () 0: 06-0 ISSN 50 579 EVALUATION STUY FOR AUTO-LIGATION OF VAS-EFERENS METHO TO TEASER UKS PREPARATION Hussein Kareem Ibrahiem linical Sciences epartment/veterinary Medicine Faculty/University
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
M. Al-Mohtaseb. Tala Saleh. Faisal Nimri
 4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
BENIGN & MALIGNANT TESTIS DISEASES. Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES
 BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
Effect of female partner age on pregnancy rates after vasectomy reversal
 MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
Temporary reappearance of sperm 12 months after vasectomy clearance
 British Journal of Urology ( 19 9 5), 76, 3 7 1-3 72 Temporary reappearance of sperm 12 months after vasectomy clearance T.S. O BRIEN, D. CRANSTON, P. ASHWIN, E. TURNER, 1.2. MAcKENZIE and J. GUILLEBAUD
British Journal of Urology ( 19 9 5), 76, 3 7 1-3 72 Temporary reappearance of sperm 12 months after vasectomy clearance T.S. O BRIEN, D. CRANSTON, P. ASHWIN, E. TURNER, 1.2. MAcKENZIE and J. GUILLEBAUD
Information for Patients. Vasectomy. English
 Information for Patients Vasectomy English Table of contents What is vasectomy?... 2 Are there any alternatives for vasectomy?... 2 The procedure... 2 How to prepare for the procedure... 2 On the day of
Information for Patients Vasectomy English Table of contents What is vasectomy?... 2 Are there any alternatives for vasectomy?... 2 The procedure... 2 How to prepare for the procedure... 2 On the day of
QUIETOUCH PODIATRY PRESENTATION
 QUIETOUCH PODIATRY PRESENTATION Flushing, New York 11373 USA Tel: +1 718 672 7150 Fax: +1 718 672 8501 On the Web at: http://www.ameditech.com Page 1 TABLE OF CONTENTS Page 3 Introduction & Description
QUIETOUCH PODIATRY PRESENTATION Flushing, New York 11373 USA Tel: +1 718 672 7150 Fax: +1 718 672 8501 On the Web at: http://www.ameditech.com Page 1 TABLE OF CONTENTS Page 3 Introduction & Description
BP and Heart Rate by Telemetry
 BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
The Varicocele as Related to Fertility
 The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
Microsurgical vasectomy reversal : results and predictors of success
 9 REVUE Andrologie 2005, 15, N~ 167-171 Microsurgical vasectomy reversal : results and predictors of success Gert R. DOHLE, Marij SMIT Andrology unit, Department of Urology, Erasmus University Medical
9 REVUE Andrologie 2005, 15, N~ 167-171 Microsurgical vasectomy reversal : results and predictors of success Gert R. DOHLE, Marij SMIT Andrology unit, Department of Urology, Erasmus University Medical
