Follow this and additional works at:
|
|
|
- Howard Marsh
- 5 years ago
- Views:
Transcription
1 Washington University School of Medicine Digital Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed ERCP for malignant distal biliary obstruction Jason G. Bill Michael Darcy Larissa L. Fuijii-Lau Daniel K. Mullady Srinivas Gaddam See next page for additional authors Follow this and additional works at: Recommended Citation Bill, Jason G.; Darcy, Michael; Fuijii-Lau, Larissa L.; Mullady, Daniel K.; Gaddam, Srinivas; Murad, Faris M.; Early, Dayna S.; Edmundowicz, Steven A.; and Kushnir, Vladimir M.,,"A comparison between endoscopic ultrasound-guided rendezvous and percutaneous biliary drainage after failed ERCP for malignant distal biliary obstruction." Endoscopy International Open.4,9. E980-E985. (2016). This Open Access Publication is brought to you for free and open access by Digital Commons@Becker. It has been accepted for inclusion in Open Access Publications by an authorized administrator of Digital Commons@Becker. For more information, please contact engeszer@wustl.edu.
2 Authors Jason G. Bill, Michael Darcy, Larissa L. Fuijii-Lau, Daniel K. Mullady, Srinivas Gaddam, Faris M. Murad, Dayna S. Early, Steven A. Edmundowicz, and Vladimir M. Kushnir This open access publication is available at Digital
3 E980 A comparison between endoscopic ultrasound-guided rendezvous and percutaneous biliary drainage after failed ERCP for malignant distal biliary obstruction Authors Jason G. Bill 1, Michael Darcy 2, Larissa L. Fujii-Lau 1, Daniel K. Mullady 1, Srinivas Gaddam 1, Faris M. Murad 1, Dayna S. Early 1, Steven A. Edmundowicz 1, Vladimir M. Kushnir 1 Institutions 1 Division of Gastroenterology, Washington University School of Medicine in St Louis, Missouri, United States 2 Division of Interventional Radiology, Washington University School of Medicine in St Louis, Missouri, United States submitted 13. February 2016 accepted after revision 5. July 2016 Bibliography DOI /s Published online: Endoscopy International Open 2016; 04: E980 E985 Georg Thieme Verlag KG Stuttgart New York E-ISSN Corresponding author Jason G. Bill, MD Division of Gastroenterology Washington University School of Medicine 660 South Euclid Ave Campus Box 8124 St Louis, Missouri Phone: Fax: jbill@dom.wustl.edu License terms Background and study Aims: Selective biliary cannulation is unsuccessful in 5% to 10 % of patients undergoing endoscopic retrograde cholangiopancreatography (ERCP) for malignant distal biliary obstruction (MDBO). Percutaneous biliary drainage (PBD) has been the gold standard, but endoscopic ultrasound guided rendezvous (EUSr) have been increasingly used for biliary decompression in this patient population. Our aim was to compare the initial success rate, long-term efficacy, and safety of PBD and EUSr in relieving MDBO after failed ERC Patients and methods: A retrospective study involving 50 consecutive patients who had an initial failed ERCP for MDBO. Twenty-five patients undergoing EUSr between were compared to 25 patients who underwent PBD immediately prior to the introduction of EUSr at our center ( ). Comparisons were made between the two groups with regard to technical success, duration of hospital stay and adverse event rates after biliary decompression. Results: The mean age at presentation was 66.5 (± 12.6 years), 28 patients (54.9 %) were female. The etiology of MDBO was pancreaticobiliary malignancy in 44 (88 %) and metastatic disease in 6 (12 %) cases. Biliary drainage was technically successful by EUSr in 19 (76 %) cases and by PBD in 25 (100 %) (P=0.002). Median length of hospital stay after initial drainage was 1 day in the EUSr group vs 5 days in PBD group (P = 0.02). Repeat biliary intervention was required for 4 patients in the EUSr group and 15 in the PBD group (P =0.001). Conclusions: Initial technical success with EUSr was significantly lower than with PBD, however when EUSr was successful, patients had a significantly shorter post-procedure hospital stay and required fewer follow-up biliary interventions. Meeting presentations: Annual Digestive Diseases Week 2015 Introduction Malignant distal biliary obstruction (MDBO) is a frequent complication of pancreaticobiliary and metastatic malignancy. Endoscopic retrograde cholangiopancreatography (ERCP) is the current gold standard for decompressing the biliary tree in this population [1 4]. However, ERCP can be unsuccessful in 5% to 10 % of patients with MDBO due to tumor-related alterations in the periampullary anatomy, as well as physician and patient factors [1]. Traditionally, unsuccessful ERCP has been followed by percutaneous biliary drainage (PBD) or surgical intervention to obtain biliary decompression [1]. PBD is a well-established and effective method for biliary decompression in the setting of malignant obstruction. However, in most cases, at least temporary external drainage and repeated interventions for drain maintenance are often required following PBD; leading to potential treatment interruptions and lower quality of life [5]. Over the past decade, advances in technology and development of new techniques have allowed endoscopic ultrasound guided biliary drainage (EUS-BD) to be used as an alternative in patients with MDBO. Various techniques of EUS-BD have been described, including EUS-guided choledochoduodenostomy, EUS-guided rendezvous (EUSr), and EUS-guided antegrade stent placement. Early data have demonstrated that in expert hands, EUS-BD is superior to PBD in regards to success of internal biliary drainage and complications and may overall improve a patient s quality of life [4]. The overall technical and clinical success rates of EUS-BD is approximately 80 % with a complication rate of approximately 10 % [6]. Only a few studies have attempted to compare the safety and efficacy of EUS-BD to PBD. In the most recent report, Khashab et al. found that EUS-BD was a Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
4 E981 safer and potentially more efficacious alternative to PBD [2]. However, in this study a variety of EUS-BD methods were employed and PBD was only performed after a failed attempt at EUS-BD. Because EUS-BD techniques and their role in treating MDBO are still evolving, it remains unclear how outcomes compare to the current gold standard in this setting, PBD. The aim of this study was to compare the initial success rate, long- term efficacy and safety of PBD and EUSr in relieving MDBO after failed initial ERC Patients and Methods This was a retrospective comparative study involving 50 consecutive patients with MDBO in whom biliary decompression could not be achieved via ERCP at a single academic tertiary referral center. Patients were identified from a manual search of the institutional endoscopic database (Provation MD, Minneapolis, MN). A manual chart review was performed and the clinical and endoscopic data were extracted from each patient s electronic medical record including demographics (age, gender), type of malignancy (pancreaticobiliary, metastatic), laboratory data, complications, number of repeat biliary interventions, and length of hospitalization. Twenty-five consecutive patients who underwent EUSr between 2008 and 2014 were compared to a cohort of 25 patients who underwent PBD immediately prior to the introduction of EUSr at our center ( ). All EUSr procedures performed at our institution between 2008 and 2014 were included in this study. Patients with surgically altered anatomy (Roux-En-Y gastric bypass, pancreaticoduodenectomy, hepaticojejunostomy) were excluded from the study. The Institutional Review Board of Washington University School of Medicine/Barnes Jewish Hospital approved review of clinical data for the purpose of this study. EUSr was performed at the university hospital endoscopy unit by 1 of 5 experienced endoscopists expert in EUS, ERCP, and interventional EUS. All patients were under monitored anesthesia care and received antibiotics during the procedure and for 3 to 5 days thereafter. The number of failed ERCP attempts prior to attempting EUSr or PBD was recorded. The definition of failed biliary cannulation with ERCP was not standardized in this study and the decision to use an alternative method of biliary cannulation was determined by the attending endoscopist. During the time of the study, our group s approach to EUS-BD was to attempt EUSr rather than other techniques after failed ERC All EUSr were performed using a trans-duodenal approach with the echoendoscope seated in the duodenal bulb. Primarily this decision is based on the risk of complications, primarily bile leak, with other EUS-BD methods. After failed ERCP at our center, EUSr was attempted during the same endoscopy session. If EUSr was unsuccessful, the decision to use an alternative method of EUS-BD, refer a patient to PBD, or perform ERCP at a later date was at the discretion of the attending endoscopist. All EUSr procedures were performed using a therapeutic linear echoendoscope (GF-UC140P or GF-UCT140; Olympus Medical Systems, Center Valley, PA). Once the scope was seated in the duodenal bulb, the bile duct was identified and color flow Doppler was used to confirm the lack of intervening vessels. Next, the bile duct was accessed, prior to 2009, using a 19-gauge FNA needle and then using an access needle (EchoTip Access Needle, Cook Medical Inc., Bloomington, IN) thereafter. The needle was advanced the lumen of the extrahepatic bile duct, the stylet was removed, and bile was aspirated to verify positioning within the bile duct. Next, contrast was injected and a cholangiogram was obtained. Following the cholangiogram, a long guidewire [0.035 inch Jagwire (Boston Scientific Corporation, Natick, MA) or inch angled Visiglide wire (Olympus America, Center Valley, PA)] was then passed through the access needle the bile duct. The guidewire was manually manipulated to advance through the major papilla and was coiled within the. The access needle and echoendoscope were then removed, leaving the wire in place. Alongside the wire, a duodenoscope (TJF ; Olympus Medical Systems, Center Valley, PA) was inserted to the level of the papilla. The biliary tree was then deeply cannulated with a sphinctertome using the guidewire placed via EUSr as a guide to where the biliary opening lay. If cannulation was unsuccessful using this technique, then the luminal end of the guidewire was grasped with a snare or forceps and pulled through the duodenoscope so that both ends of the guidewire exited the patient s mouth and were under the control of the endoscopist. This allowed a sphinctertome or balloon catheter to be advanced over the wire directly the biliary tree. Subsequently, a biliary stent was placed across the stricture. Technical success of EUSr was defined by the wire being advanced the via the major papilla and a stent placed in a retrograde manner ( " Fig. 1). Patients were not routinely admitted to the hospital for observation following EUSr if the procedure was performed on an outpatient basis. PBD was performed by experts in Interventional Radiology under moderate sedation using well established techniques [7]. Most patients initially received external biliary drainage which at the discretion of the attending radiologist could be converted to a metallic biliary stent when clinically appropriate [7]. Patients were monitored in the hospital for a minimum of 23 hours following PBD placement. Following PBD placement, any repeated procedure (stent/tube exchange) was recorded as repeated interventions. Procedure-related adverse events (AEs) were divided early (within 7 days) and late (greater than 7 days) from the index procedure. AE recorded included recurrent biliary obstruction, bleeding (defined as an acute>3 g/dl drop in Hgb requiring PRBC transfusion or overt bleeding outside of what is typically accepted post procedure that required further medical/surgical management), pancreatitis, bile leak and cholecystitis. Statistical analysis Data are reported as mean ± standard deviation (SD) for normally distributed data, and median and range for skewed data. Grouped continuous variable data were compared using two-tailed Student s t test and Mann-Whitney U test where appropriate. Intergroup and categorical comparisons were made using the Chisquare and Fisher s exact tests. A p value of<0.05 was required for statistical significance. All statistical analyses were performed using PASW 19.1 (SPSS, Inc., Chicago, IL). Results During the 12-year study period, 1076 patients underwent an initial ERCP for malignant distal biliary obstruction at our medical center, biliary access via ERCP was unsuccessful in 54 (5.0 %). Four patients elected to pursue hospice care after failed ERCP, and further attempts at biliary decompression were not made. Fifty patients [mean age 66.5 ±12.6 years, 28 (54.9 %) females] were included in this study. The etiology of MDBO was pancreaticobili- Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
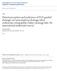
5 E982 Fig. 1 EUS-guided rendezvous in an 84-year-old patient with obstructive jaundice due to an ampullary cancer. a Endoscopic examination revealed a large mass, which made identification of the biliary orifice impossible. b Endosonographic examination revealed marked biliary ductal dilation and due to direct extension of the tumor the bile duct lumen. c Under endosonographic guidance the bile duct was punctured and a cholangiogram was obtained, confirming findings observed on EUS examination. d,e Next, a guide wire was advanced the and via the EUS needle. f Finally a covered metal biliary stent was placed in a retrograde manner. ary malignancy in 44 (88 %) and metastatic malignancy in 6 (12 %) cases. In the EUSr group, pancreaticobiliary malignancies included pancreatic adenocarcinoma in 20 (80 %), neuroendocrine tumor in 1 (4 %), and ampullary/duodenal cancer in 3 (12 %) patients. Patients underwent a median of 1 (range 1 3) unsuccessful ERCP attempts. The reason for failed biliary cannulation at time of ERCP was tumor-related ampullary deformity in 34 (68 %) cases and inability to cannulate a normal appearing ampulla in 16 (32 %). There were no significant differences in any of the baseline characteristics between the EUSr and PBD groups ( " Table 1). Biliary drainage was technically successful by EUSr in 19 (76 %) cases and by PBD in 25 (100 %) (P =0.002, " Table2). Median length of hospital stay after initial drainage was 1 day (range 0 26) in the EUSr group vs 5 days (range 1 20 days) in the PBD group (P = 0.02). The median length of hospital stay following successful EUSr was 1 day (range 0 13), significantly shorter than the PBD group (P=.002). Nine patients in the EUSr group underwent the procedure on an outpatient basis and were not admitted to the hospital within the subsequent 14 days. Clinical success, defined as a 50 % drop in bilirubin within 7 days of the index procedure was obtained in 24 (96 %) in the EUSr group and 20 (80 %) of those in the PTC grou Five patients in the EUSr and 5 patients in the PBD group underwent a pancreaticoduodenectomy at a median of 12 days (range 7 165) following biliary drainage; there were no intraoperative of postoperative biliary complications. EUSr was unsuccessful in 6 cases (24 %); summarized in " Table3. Reasons for failed EUSr included inability to pass the guidewire antegrade (n = 5), inability to locate a safe window EUS for biliary puncture due to duodenal deformity (n = 1). In cases where EUSr was unsuccessful, biliary drainage was obtained by PBD (n = 3), repeat ERCP (n=2), and EUS-guided choledochoduodenostomy (n =1). Both patients who had biliary access obtained through repeat ERCP underwent the procedure within 24 hours after EUSr was attempted. The median time to PBD following failed ERCP was 1 (range 0 3) day. The median hospital length of stay for failed EUSr was 4 days (range 0 26), which was similar to the primary PBD group (5 days, P=0.64). Table1 Baseline demographics. EUSr (n = 25) PBD (n =25) P value Age(years;mean±SD) 65.4± ± Gender (female) Etiology of biliary obstruction Pancreatobiliary malignancy Metastatic malignancy 1 5 Unsuccessful ERCP attempts 1(1 3) 1 (1 2) 0.26 (median, range) Reason for failed ERCP Tumor invasion/ deformity Normal ampulla 16 9 Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
6 E983 Table2 Post-procedure, per protocol analysis. EUSr (n=25) PBD (n = 25) P value Initial technical success Clinical success (reduction in bilirubin > 50 % 24/25 (96 %) 20/25 (80%) Mean pre-eus-bd bilirubin Mean post-eus-bd bilirubin Length of hospital stay following initial drainage (median, range) 1 day (0 26) 5 days (1 20) Follow-up duration after initial drainage (median, range) 37 days (5 476) 11 (1 272) Repeat procedure Number repeat procedures (median, range) 0 (0 1) 1 (0 10) Table3 Patients who failed EUSr. Patient Age Year of Study Endoscopist (1 5) Primary cancer Reason EUSr failed Method of biliary decompression Length of hospital stay Clinical success Early adverse event(s) Repeat biliary intervention Pancreatic Wire did Pancreatic Could not access bile duct by EUS due to duodenal deformity Ampullary Wire did Pancreatic Wire did Breast Wire did Pancreatic Wire did PBD 4 days Yes Bleeding from PBD tract, treated with PBD replacement ERCP 4 days Yes None yes EUS-BD 26 days * yes None no PBD 2 days yes None no ERCP 0 days Yes None no PBD 7 days Yes None no yes EUSr, endoscopic ultrasound-guided rendezvous Early AEs occurred in 4 (16 %) patients in the EUSr group and 3 (12 %) in the PBD groups (P =0.68, " Table 3). Early AEs included recurrent biliary obstruction (2 PBD), bleeding (2 EUSr, 1 PBD), pancreatitis (1 EUSr), and bile leak (1 EUSr). In the EUSr group, bleeding was related to a gastroduodenal artery pseudoaneurysm in 1 patient and was successfully treated with percutaneous embolization; a second patient developed hemobilia from a PBD after a failed EUSr, this was successfully treated by re-positioning of the PBD. In the PBD group one patient developed hemobilia; this was successfully treated with PBD repositioning and did not require vascular intervention. Delayed AE occurred in 3 (12 %) patients in the EUSr group and 6 (5 %) in the PBD group (P = 0.27) ( " Table 4). Repeat biliary intervention was required for 3 patients in the EUSr group and 14 in the PBD group (P=0.001). Scheduled biliary interventions, including drain and stent changes were required in 14 patients in the PBD group, a median of 19 days (range 1 33) following initial drainage and in 3 patients in the EUSr group, a median of 5 days (range 1 105) later (P< 0.001). Conversion of PBD to metal biliary stent was successful in 10 (40 %) patients following initial PBD placement. Recurrent biliary obstruction, requiring intervention occurred in 4 patients in the PBD group, at a median of 237 days (range 1 272) after initial drainage and in one patient in the EUSr group, 476 days after stent placement ( " Fig. 2, Log Rank P = 0.01). Discussion Since being first reported in 2001 by Giovannini et al., EUS-BD has been increasingly used as an alternative in patients with MDBO who fail ERCP [8]. Numerous techniques have been and are being developed with growing data supporting its use and efficacy [1 5, 9 14]. In our study, EUSr was found to be a safe and effective method of biliary drainage in patients with MDBO after failed initial ERC It was associated with shorter post-procedure Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
7 E984 Table4 Adverse events. Adverse events EUSr PBD Early (<7 days) Biliary obstruction 0 2 Bleeding 2 1 Pancreatitis 1 0 Bile leak 1 0 Late (>7 days) Biliary obstruction 2 5 Cholecystitis 1 1 EUSr, endoscopic ultrasound-guided rendezvous; PBD, percutaneous biliary drainage Cum Survival Fig. 2 Rendezvous PTC Rendezvous-censored PTC-censored Time (days) Kaplan Meyer Estimate of time to biliary obstruction. hospital stay and required fewer follow-up biliary interventions than PBD. Three techniques have been developed including EUS-guided antegrade transluminal drainage (stenting using a transgastric or transduodenal approach without accessing the papilla), EUSguided antegrade transpapillary stent placement, and EUSr. From a large analysis of EUS-guided biliary techniques, the overall success rate of EUSr is estimated to be 81 % with a complication rate about 10 % of cases [6]. We recognize that there has been a more recent push for utilizing a protocol based approach to different rendezvous techniques, with some endoscopists favoring step wise attempts at biliary access starting with the trans-intrahepatic approach [15]. However, our standard approach to EUS-guided biliary access during the study period was EUSr, specifically utilizing the transduodenal approach with the echoendoscope seated in the duodenal bulb. This decision was based primarily on the concern for occurrence of bile leak, peritonitis and bleeding associated with creation of a fistula between the lumen of the gastrointestinal tract and the biliary tree when the antegrade approach is used or transluminal stenting is performed [6]. While these complications are relatively uncommon, there consequences can be devastating; particularly in the 20 % of patients with potentially resectable pancreaticobiliary tumors. With the recent introduction of lumen opposing stents, EUSguided choledochoduodenosotmy has become an attractive alternative to EUS-guided biliary decompression.[16] However, the currently available lumen opposing stents were not designed specifically for the biliary tree and may pose a risk of cholecystitis in patients with a gallbladder in situ as well as stent erosion or migration. Thus, we feel that if EUS guided biliary drainage is attempted rendezvous should remain the preferred first line approach, given the fact that it preserves the anatomic integrity of the biliary tree and avoid creation of a fistula. It remains unclear whether EUS techniques are superior in efficacy, safety, and cost when compared to PBD in patients with MDBO who have failed ERC It is well known that PBD is highly successful but generally requires repeat procedures and periprocedural adverse events are not infrequent rates ranging from 10 % to 32 % in the modern literature [6]. In a recent study, Khashab et al studied a group of 73 patients with MDBO who failed repeat ERCP and found that technical success was higher in the PBD group but the adverse event rate was higher in the latter group of patients. Regarding successful biliary drainage, defined as reduction in total bilirubin by 50 % in 2 weeks, the groups were not statistically different [2]. However, a major critique of the study is patients were enrolled to the PBD group only after failed ERCP and EUS-BD; potentially biasing the study against PBD. In our study AE rates were similar between the EUSr and PBD groups. However, recurrent biliary obstruction occurred more frequently and repeated procedures were required more often in the PBD grou Repeated biliary manipulation may lead to further complications and requires the patient to have repeated hospital visits for catheter checks and changes. Recurrent biliary obstruction is a major source of morbidity and treatment interruption in patients undergoing chemotherapy. Given the fact that EUSr is associated with a lower rate of recurrent biliary obstruction it stands to reason that this approach would be preferable in patients receiving neoadjunct or palliative chemotherapy [17, 18]. Moreover, the length of hospital stay was significantly shorter in the EUSr group, landing another advantage to EUSr; particularly in cases where the initial ERCP is performed on an outpatient basis and if EUSr is performed in the same endoscopic session. Finally, we hypothesize that patients would experience a lower quality of life following PBD when compared to EUSr as external drainage catheters typically repeated interventions. It cannot be understated however, that there are important advantages of PBD. First, PBD is more widely available and the techniques of PBD are well established and standardized. Furthermore, complications of PBD are typically minor and do not require surgical backup that may only be available at tertiary medical centers. That being said, EUS techniques have a key advantage of being performed at the same session of ERC However, if initial EUSr fails, it could be argued that PBD is a safer therapeutic option given no need for repeat anesthesia and its almost universal technical success. Technology, ie stents and guidewires, that focus solely on EUS-BD are needed and currently in development [19, 20]. With the development of technology and as experience by interventional endoscopists is gained, the technical success rates of EUS-BD are likely to improve. The major limitation of our study is its retrospective nature and limitations inherent to this design. The use of historical controls may have introduced some degree of bias; however there were no significant differences in the baseline characteristics and the protocol (minimum of 23 hours inpatient observation) following PBD placement remains the same at our institution. We also de- Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
8 E985 tected no difference in the rate of adverse events comparing EUSr and PBD, however our sample size may be insufficient to detect a meaningful difference in this regard. Additionally, this was a single-center study; results may not be applicable to institutions with different practice patterns for endoscopic and percutaneous biliary drainage. Finally, we focused our study on patients with malignant distal biliary obstruction and we cannot comment on the efficacy and safety of EUS guided biliary drainage in the treatment of hilar biliary structures or benign biliary disease. Conclusions In summary, EUSr is a safe and effective method of biliary drainage in patients with MDBO after failed ERC Initial technical success with EUSr was significantly lower than with PBD, however when EUSr was successful patients had a significantly shorter post-procedure hospital stay and required fewer follow-up biliary interventions than those undergoing PBD. Competing interests: None References 1 Sarkaria S, Lee HS, Gaidhane M et al. Advances in endoscopic ultrasound-guided biliary drainage: a comprehensive review. Gut Liver 2013; 7: Khashab MA, Valeshabad AK, Afghani E et al. A comparative evaluation of EUS-guided biliary drainage and percutaneous Drainage in patients with distal malignant biliary obstruction and failed ERC. Dig Dis Sci 2015; 60: Iwashita T, Lee JG, Shinovia S et al. Endoscopic ultrasound-guided rendezvous for biliary access after failed cannulation. Endoscopy 2012; 44: Artifon EL, Aparicio D, Paione JB et al. Biliary drainage in patients with unresectable, malignant obstruction where ERCP fails: endoscopic ultrasonography-guided choledochoduodenostomy versus percutaneous drainage. J Clin Gastroenterol 2012; 46: Hara K, Yamao K, Mizuno N et al. Endoscopic ultrasound-guided choledochoduodenostomy. Dig Endosc 2010; 22: Iwashita T, Doi S, Yasuda I. Endoscopic ultrasound-guided biliary drainage: a review. Clin J Gastroenterol 2014; 7: Covey AM, Brown KT. Percutaneous transhepatic biliary drainage. Tech Vasc Interv Radiol 2008; 11: Giovannini M, Moutardier V, Pesenti C et al. Endoscopic ultrasoundguided bilioduodenal anastomosis: a new technique for biliary drainage. Endoscopy 2001; 33: Gupta K, Mallery S, Hunter D et al. Endoscopic ultrasound and percutaneous access for endoscopic biliary and pancreatic drainage after initially failed ERC. Rev Gastroenterol Disord 2007; 7: Khashab MA, Dewitt J. EUS-guided biliary drainage: is it ready for prime time? Yes Gastrointest Endosc 2013; 78: Mallery S, Matlock J, Freeman ML. EUS-guided rendezvous drainage of obstructed biliary and pancreatic ducts: Report of 6 cases. Gastrointest Endosc 2004; 59: Iwashita T, Lee JG. Endoscopic ultrasonography-guided biliary drainage: rendezvous technique. Gastrointest Endosc Clin N Am 2012; 22: Liu YD, Wang ZQ, Wang XD et al. Stent implantation through rendezvous technique of PTBD and ERCP: the treatment of obstructive jaundice. J Dig Dis 2007; 8: Barkay O, Sherman S, McHenry L et al. Therapeutic EUS-assisted endoscopic retrograde pancreatography after failed pancreatic duct cannulation at ERC. Gastrointest Endosc 2010; 71: Park do H, Jeong SU et al. Prospective evaluation of a treatment algorithm with enhanced guidewire manipulation protocol for EUS-guided biliary drainage after failed ERCP (with video). Gastrointest Endosc 2013; 78: Itoi T, Binmoeller K, Itowkawa F et al. Endoscopic ultrasonographyguided cholecystogastrostomy using a lumen-apposing metal stent as an alternative to extrahepatic bile duct drainage in pancreatic cancer with duodenal invasion. Dig Endosc 2013; 25: Boulay BR, Gardner TB, Gordon SR. Occlusion rate and complications of plastic biliary stent placement in patients undergoing neoadjuvant chemoradiotherapy for pancreatic cancer with malignant biliary obstruction. J Clin Gastroenterol 2010; 44: Sut M, Kennedy R, McNamee J et al. Long-term results of percutaneous transhepatic cholangiographic drainage for palliation of malignant biliary obstruction. J Palliat Med 2010; 13: Itoi T, Binmoeller KF, Shah J et al. Clinical evaluation of a novel lumenapposing metal stent for endosonography-guided pancreatic pseudocyst and gallbladder drainage (with videos). Gastrointest Endosc 2012; 75: Itoi T, Itokawa F, Uraoka T et al. Novel EUS-guided gastrojejunostomy technique using a new double-balloon enteric tube and lumen-apposing metal stent (with videos). Gastrointest Endosc 2013; 78: Bill Jason G et al. Endoscopic ultrasounduided rendezvous Endoscopy International Open 2016; 04: E980 E985
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches
 E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
Jintao Guo, Siyu Sun, Xiang Liu, Sheng Wang, Nan Ge, and Guoxin Wang. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable Metal Stent for Malignant Biliary Obstruction
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Endoscopic ultrasound guided biliary drainage: a comprehensive review
 Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis
 Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or
 Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
ORIGINAL PAPERS. Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP
 ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A Literature Review
 Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction
 CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
efficacy. Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience
 E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy
 Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Endoscopic ultrasound-guided anterograde cholangiopancreatography
 J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
Gastrointestinal Intervention
 Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases
 Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures
 E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Gastrointestinal Intervention
 Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
EUS Guided Pancreatic Duct Drainage: When? How?
 PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Review Article EUS-Guided Biliary Drainage
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2018 Patient perception and preference of EUS-guided drainage over percutaneous drainage when endoscopic transpapillary
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2018 Patient perception and preference of EUS-guided drainage over percutaneous drainage when endoscopic transpapillary
Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents
 REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Introduction. Patients and methods. Patients. Background and study aims Failure to recognize the
 A simple and novel marking method for correctly identifying the precutting direction to achieve safe and efficacious precut sphincterotomy (with video) Authors Kazumasa Nagai, Akio Katanuma, Kuniyuki Takahashi,
A simple and novel marking method for correctly identifying the precutting direction to achieve safe and efficacious precut sphincterotomy (with video) Authors Kazumasa Nagai, Akio Katanuma, Kuniyuki Takahashi,
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic Stents
 Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Endoscopic Ultrasound-Guided Biliary Drainage
 Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s74 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S74-S82 Endoscopic Ultrasound-Guided Biliary Drainage Everson L.A. Artifon, MD, PhD,
Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s74 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S74-S82 Endoscopic Ultrasound-Guided Biliary Drainage Everson L.A. Artifon, MD, PhD,
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Introduction E1111. Background and study aim Gallbladder drainage in patients
 Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
ERCP in altered anatomy. Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway
 ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden
 Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Performing forward-viewing endoscopy at time of pancreaticobiliary EUS and ERCP may detect additional upper gastrointestinal lesions
 E193 Performing forward-viewing endoscopy at time of pancreaticobiliary EUS and ERCP may detect additional upper gastrointestinal lesions Authors Ashby Thomas 1, *, Arunan S Vamadevan 1, *, Eoin Slattery
E193 Performing forward-viewing endoscopy at time of pancreaticobiliary EUS and ERCP may detect additional upper gastrointestinal lesions Authors Ashby Thomas 1, *, Arunan S Vamadevan 1, *, Eoin Slattery
Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal Stent for Acute Cholecystitis: A Systematic Review
 REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas
 ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
910 Dumonceau Jean-Marc et al. Endoscopic biliary stenting: Endoscopy 2018; 50:
 Endoscopic biliary stenting: indications, choice of stents, and results: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline Updated October 2017 Authors Jean-Marc Dumonceau 1,AndreaTringali
Endoscopic biliary stenting: indications, choice of stents, and results: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline Updated October 2017 Authors Jean-Marc Dumonceau 1,AndreaTringali
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without papillotomy
 E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
E806 THIEME Clinical features of gallstone impaction at the ampulla of Vater and the effectiveness of endoscopic biliary drainage without Authors Yuichi Takano 1, Masatsugu Nagahama 1, Naotaka Maruoka
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Urgent endoscopic ultrasound-guided choledochoduodenostomy for acute obstructive suppurative cholangitis-induced sepsis
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i16.4264 World J Gastroenterol 2016 April 28; 22(16): 4264-4269 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i16.4264 World J Gastroenterol 2016 April 28; 22(16): 4264-4269 ISSN 1007-9327
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Early Infectious Complications of Percutaneous Metallic Stent Insertion for Malignant Biliary Obstruction
 Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
ERCP complications and challenges in their diagnosis and management.
 ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) Fax- (760) Preparation for ERCP
 Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for ERCP Patient Name- Procedure Date and Time- Please do not
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for ERCP Patient Name- Procedure Date and Time- Please do not
Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline
 Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Chronic pancreatitis is a fibroinflammatory disease of the
 Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Index. Springer Nature Singapore Pte Ltd K.-H. Lai et al. (eds.), Biliopancreatic Endoscopy,
 A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
Endoscopic Ultrasound-Guided Pancreatobiliary Endoscopy in Surgically Altered Anatomy
 FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
Introduction E275 ABSTRACT. Original article
 International multicenter comparative trial of endoscopic ultrasonography-guided gastroenterostomy versus surgical gastrojejunostomy for the treatment of malignant gastric outlet obstruction Authors Mouen
International multicenter comparative trial of endoscopic ultrasonography-guided gastroenterostomy versus surgical gastrojejunostomy for the treatment of malignant gastric outlet obstruction Authors Mouen
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
 Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
