Emergent Intrathecal Baclofen Withdrawal After Pseudomeningocele Aspiration
|
|
|
- George Stewart
- 6 years ago
- Views:
Transcription
1 Pain Physician 2013; 16:E113-E118 ISSN Case Report Emergent Intrathecal Baclofen Withdrawal After Pseudomeningocele Aspiration Timothy R. Smith, MD, PhD, Divakar S. Mithal, PhD, Anne Park, MD, Angela Bohnen, MD, Joseph Adel, MD, and Joshua M. Rosenow, MD From: Department of Neurological Surgery, Northwestern University, Feinberg School of Medicine, Chicago, IL Address Correspondence: Timothy R. Smith, MD, PhD Department of Neurological Surgery Northwestern University Feinberg School of Medicine 676 N. St. Clair St., Suite 2210 Chicago, IL northwestern.edu Disclaimer: There was no external funding in the preparation of this manuscript. Conflict of interest: None. Manuscript received: Revised manuscript received: Accepted for publication: Intrathecal baclofen (ITB) infusion has become a common treatment for severe spasticity. Many complications of these drug delivery systems have been reported such as those related to improper dosing, mechanical failure of the implanted pump or catheter, or postoperative wound issues. We report a case of ITB withdrawal after pseudomeningocele aspiration. A 21 year-old male with spastic quadriparesis due to traumatic brian injury (TBI) presented with a pseudomeningocele surrounding an ITB pump (215 mcg/day, continuous) implanted in the abdomen. The pseudomeningocele was percutaneously aspirated and approximately 15 hours later the patient developed signs and symptoms of acute baclofen withdrawal. As a result, the patient underwent an exploration of the ITB infusion system with an intraoperative epidural blood patch. The symptoms of ITB withdrawal improved over the next 18 hours. The subcutaneous cerebrospinal fluid (CSF) collection partially recurred 48 hours later, but this resolved after a second epidural blood patch. The case illustrates a unique presentation of a serious complication of ITB infusion. This underscores that timely diagnosis and treatment of acute baclofen withdrawal is key to optimal outcomes. Key words: Intrathecal baclofen, baclofen withdrawal, intrathecal baclofen pump complications, pseudomeningocele, cerebrospinal fluid leak, case report Pain Physician 2013; 16:E113-E118 Free full manuscript: Intrathecal baclofen (ITB) is a common modality employed in the management of severe spasticity when oral medications and botulinum toxin injections are not sufficiently therapeutic or cause unacceptable side effects (1-9). Historically, oral baclofen has been used to treat spasticity; however, intrathecal administration of baclofen delivers a significantly higher drug concentration to the spinal cord, the area of therapeutic action of the drug. There is also a 4 to one post-infusion drug concentration gradient from the caudal to the rostral aspect of the spinal cord. This gradient focuses the beneficial effect at the spinal level and reduces the unwanted cranial side effects (10). The most common indications for ITB therapy include cerebral palsy, traumatic brain injury, spinal cord injury, diffuse anoxic brain injury, multiple sclerosis, stroke, and dystonia (4,7,11-16). ITB therapy has been shown to improve quality of life and optimize daily care, as well as be cost effective (17-20). ITB therapy, however, is not without risk (18). Complications can be varied, but can be categorized as relating to dosing, mechanical failure of catheter or pump, or wound issues such as infection (5,9,11,21,22). In particular, any complication resulting in abrupt cessation of ITB delivery may result in a severe baclofen withdrawal syndrome, which can be life threatening
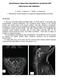
2 Pain Physician: March/April 2013; 16:E113-E118 (9,11,18,21). As a result, recognition of ITB withdrawal is an important component of managing patients with ITB delivery systems (9). In this study, we present a case of a young patient with an ITB pump complicated by acute baclofen withdrawal after pseudomeningocele aspiration. Case Report History The patient is a 21-year-old man who suffered a severe traumatic brain injury (TBI) due to a motorcycle accident. This left him with severe spastic quadriparesis. A bolus trial of 50 mcg of ITB provided excellent relief of his spasticity and improvement in his dysautonomia. Based on this, he underwent implantation of an intrathecal catheter (model 8731 SC, Medtronic Neurological, Minneapolis, MN) and subcutaneous programmable pump (215 mcg/day, continuous, Synchromed II, Medtronic Neurological, Minneapolis, MN). The patient was placed under general anesthesia and access to the cerebrospinal fluid (CSF) was obtained in a single pass. A catheter was placed via a standard oblique trajectory from a fascial entry point over the right L3 pedicle to a puncture of the thecal sac in the midline at the L1-2 interspace. The catheter tip was positioned at approximately the T4 level (Fig. 1). To complete the case, each layer (deep dermal, dermal, and subcutaneous) was brought together with absorbable sutures. The skin was closed with interrupted vertical mattress 3.0 nylons. No intraoperative complications were noted, and no sign of leak was noted at the time of closure. The patient did well post-operatively, and he was discharged back to inpatient rehabilitation on postoperative day (POD) #1. He was seen again on POD #8. At that time there was a small soft subcutaneous collection at the abdominal site, but none at the lumbar wound site. He had been in an abdominal binder Fig. 1. Plain radiographs of the abdomen demonstrating ITB pump catheter system with entrance into the spinal canal on the right at L1-L2, and pump position in the right lower abdominal quadrant. A. The anterior-posterior view denotes catheter continuity at both proximal and distal connections. B. Lateral view verifies entrance level at L1-L2. E114
3 Emergent Intrathecal Baclofen Withdrawal After Pseudomeningocele Aspiration since surgery. The staples were removed on POD #10, still with no sign of leak at the lumbar wound. The following day, clear fluid was noted to leak from the abdominal wound and the patient was transferred that night to the emergency room (ER) for evaluation. In the ER, it was noted that there was a large tense, fluid collection around the pump. Radiographs of the abdomen were obtained which revealed the catheter system to be in continuity. The fluid collection was sterilely aspirated at the bedside, removing 80 ml of clear fluid (sent for cell count, gram stain, and culture). The lateral margin of the wound was oversewn with 3-0 nylon, and the patient was sent back to rehabilitation in an abdominal binder. The following day, POD #12, he was noted to have increased muscular spasms and mild tachycardia, both of which were unresponsive to morphine. Later in the day, he also developed a temperature of 104 o F, tachycardia in the 140s, and tachypnea of breaths per minute, in addition to severe twitching, diaphoresis, and further increased spasticity. He returned to the ER at that time. The subcutaneous collection at the abdominal site had not only recurred since the aspiration the previous evening, but it exceeded the prior collection in size. Given that his presentation was consistent with acute ITB withdrawal, he was taken emergently to the operating room for exploration and possible revision of the catheter system. The patient was placed in a lateral decubitus position on a beanbag. When the abdominal incision was opened, clear fluid was noted to surround the pump without evidence of infection. There was an obvious flow of fluid into the abdominal site around the catheter where it entered the abdominal wound from its subcutaneous tunnel around the flank. After opening the back incision, clear fluid was seen to egress around the entrance site of the catheter into the fascia. A 2-0 silk suture was used in a purse-string fashion to fasten the soft tissue firmly around the exiting catheter without obstructing CSF flow. Good spontaneous flow of CSF was visualized throughout the entire catheter system prior to closing the incisions. Under fluoroscopic guidance and using the loss of resistance to air technique, a 22G spinal needle was placed into the epidural space at L2-3 and 20 ml of autologous blood was infused in a cranial direction. Upon completion of the case, the wound was closed in typical fashion, bringing together 3 layers with absorbable sutures (deep, dermal, and subcutaneous), and the skin was closed with interrupted vertical mattress 3.0 nylons. Two post-operative baclofen boluses were administered through the functioning catheter system to overcome the ITB deficit. The patient was admitted to the ICU for monitoring and flat bed rest for 24 hours. The following day, the patient s fever resolved, the spasms improved, and his vitals stabilized. On POD #2 following the revision, the subcutaneous fluid collection was noted to partially recur. A second blood patch was performed, this time with 30 ml of autologous blood. The small recurrent collection resolved within 24 hours after this and no further issues were noted. From the patient s original admission, the specter of meningitis was raised and subsequently evaluated. We found no clinical evidence of infection. The patient did not have clinical evidence of meningismus at any time. All procedures were undertaken in a sterile fashion. CSF and subcutaneous fluid were sent for infectious workup, as well as CBC with differential, ESR/CRP, and blood cultures, and were all found to be negative. As such, only standard 24-hour antibiotics were used upon presentation, and the patient never developed any infectious issues throughout his course. Discussion ITB is widely used for treating severe spasticity, resulting in significant increases in these patients overall ease of care and quality of life (3,4,8,12,18,20,23-25). ITB therapy has shown to be efficacious by numerous studies; however, this therapy carries certain risks (5,9,11,21). Approximately 20 30% of patients with implanted pumps experience a complication (5,9,24-27). Complications are varied, but can be trichotomized as relating to dosing (overdose or withdrawal), mechanical failure of catheter or pump (malfunction, leaks), or infection (wound, hardware, and meningitis) (5,9,11,21,22). The most frequent complications are infections, CSF leaks, and catheter malfunctions (22-24,28). Rarely, either baclofen withdrawal or overdose can also occur (11,21,29,30). For patients physiologically dependent on ITB for spasticity control, sudden disruption of ITB delivery can precipitate acute ITB withdrawal syndrome, a potentially life-threatening complication (5,7,11,18,21,27,29-37). In a review of the literature, Watve et al (38) observed that ITB withdrawal is frequently due to catheter dysfunction and often occurs close to a patient s scheduled pump refill date. The syndrome of ITB withdrawal is characterized by reflex spasticity, hyperthermia, autonomic dysregulation, pruritus, seizures, central nervous system (CNS) depression, with eventual progression to rhabdomyolysis, disseminated intravascular coagulation, and E115
4 Pain Physician: March/April 2013; 16:E113-E118 multisystem organ failure (11,21,30,31,33,35-37). When baclofen delivery by any route of administration is stopped, withdrawal may begin within the first 3 days, initially presenting with severe rebound hyperspasticity and pruritic symptoms (31,37-41). These symptoms are likely due to a sudden removal of baclofen-mediated GABAB inhibitory tone in the CNS (37-39). Severe withdrawal may present with broader, systemic symptoms mimicking other disseminated neurological syndromes such as autonomic dysreflexia, post-anesthetic malignant hyperthermia, and neuroleptic malignant syndrome (37-40). Salazar and Eiland (40) reported a case of ITB withdrawal with features resembling serotonin syndrome (SS). Clinical suspicion for withdrawal was indicated due to the presence of an ITB pump that was due for refill, and because clinical history revealed no serotonergic medications (40). The ITB withdrawal syndrome is often refractory to oral baclofen therapy alone, and in rare situations can last for weeks (11,21). Definitive treatment of acute ITB withdrawal is restoration of intrathecal baclofen infusion (38). Severe cases of withdrawal may require adjuvant treatment with benzodiazepines as their activity at GABAa receptors bypasses baclofen regulation of GABAb, providing supportive autonomic regulation (39). Given the similarities to SS, Meythaler et al (41) initiated a case series using the potent anti-serotonergic drug cyproheptadine to improve symptoms of acute ITB withdrawal. While promising results have been reported (37,41) evidence for use of anti-serotonergics remains limited (38). The frequency of ITB pump complications resulting from surgical technique is not known. Awaad et al (9) reviewed their own complications from baclofen pump implantations and found that over a 4 year period they performed 33 additional revision surgeries on half the patients studied (22/44). Of the 22 patients requiring revision surgery, only one patient had an occult CSF leak that resulted in an abdominal fluid collection. A pump injection study revealed a catheter leak at the pump connector site, which was revised. He continued to have an abdominal fluid collection, even with negative dye studies, and eventually he was taken back to place an entirely new catheter which solved the problem (9). Haranhalli and colleagues (5) reported implanting 87 ITB pumps over a 10-year period at their institution. Just over 17% of their patients had complications, representing 25 complications in 13 patients. They found that the first complication occurred around 2 years from the first surgery. Five patients had a subcutaneous fluid collection, only one of which required surgical correction, the rest were treated with abdominal binders. In the case requiring surgical correction, a recurrent pseudomeningocele was related to an increased CSF pressure and moderate hydrocephalus. They theorized that early CSF diversion could have eliminated the need for further surgeries (5). One of the most common complications of ITB pump implantations is a spinal fluid leak resulting in spinal headache (3,5,9,27,37). For this straightforward complication, an epidural blood patch can be utilized (42). For refractory cases of spinal headache, a lumbar drain can also be inserted for CSF diversion (43). The most invasive approach for repair is an open laminectomy and primary dural closure (43). In our case there was no initial CSF leak noted at the time of closure and even 10 days postoperatively no CSF was noted at the lumbar surgical site, a result of pseudomeningocele formation. In the case of laminectomy or discectomy pseudomeningocele formation rates can range from % (43). In the case of minimally invasive spinal surgery such as ITB catheter placement, the rate of pseudomeningocele appears to be lower (5,9). Vender et al (22) draw an important distinction between adult and pediatric populations with regards to CSF complications. They found that wound-related complications were almost twice as prevalent in children (46%) than in adults (25%) (22). The varied complications in children included infections, CSF fistulae, pseudomeningoceles, wound dehiscence, and granuloma formation, whereas adult complications were primarily infections. In their case series, pseudomeningoceles were related to CSF leakage at the catheter insertion site (22), without mechanical malfunction of the catheter itself. They note that children are more susceptible to pseudomeningocele formation secondary to decreased amount of muscle and soft tissue to resist formation or to protect against wound breakdown (22). In 2 pediatric patients without implanted catheters, Fridley et al (44) demonstrate that symptomatic pseudomeningocele aspiration can be augmented with placement of an epidural blood patch to address the causative CSF leak. Their technique is ultrasound guided giving the benefit of noninvasive evaluation of the pseudomeningocele, but does not allow for direct inspection of the pump and catheter as was required in our case. Meticulous care must be applied to the implantation of ITB pumps and associated catheters. We routinely placed a purse-string, non-absorbable sutures around the catheter exiting from the fascia (45). However, in E116
5 Emergent Intrathecal Baclofen Withdrawal After Pseudomeningocele Aspiration this case that suture prevented CSF flow through the catheter and was removed at the time of pump implant. With the suture removed, CSF flowed through the catheter implantation site down the catheter track and into the abdomen. As published in prior case reports, a prophylactic epidural blood patch can also be considered in the instance of a CSF leak (42,44,46,47), but this method will not allow direct visualization of a pump system. In this case of severe ITB withdrawal it was imperative to determine whether the system was functioning and confirm that the leak was not the result of a fracture in the catheter. Therefore the decision to surgically explore the ITB system was made. A new purse-string suture was placed at the time of revision, a method that has been reported for repairing a CSF leak around an intrathecal catheter (45,48). If there is intra-operative concern for leakage of CSF around the catheter, we recommend careful inspection while the anesthetic team induces a valsalva maneuver to induce intra-abdominal pressures of 40 cm water for seconds. If a leak is visualized, we recommend verifying that the retention suture around the catheter is properly fastened (45). This is the first reported case of iatrogenic baclofen withdrawal secondary to pseudomeningicele aspiration of which the authors are aware. We hypothesize that the patient developed a CSF fistula around the catheter, which extended to the pump pocket in the abdomen. Much of the ITB was shunted from the thecal sac into the subcutaneous pseudomeningocele. Combined with the known vertical concentration gradient for ITB, the shunting likely led to a significant loss of drug outside the thecal sac. However, because the initial collection developed over several days, the loss of ITB was gradual. Moreover, the collection likely provided some backpressure against further loss of CSF and ITB. Once the pseudomeningocele was aspirated (~80 ml of fluid), the result was an immediate evacuation of both CSF and ITB, leading to acute baclofen withdrawal. Sealing the CSF fistula with both a new purse string and blood patch stanched the extra-thecal flow of CSF and improved the patient s symptoms. Importantly, this case highlights that severe ITB withdrawal can develop within days of the initial delivery of ITB. Conclusion While ITB pumps are efficacious for patients with severe spasticity, they are not without risk. The diagnosis and treatment of ITB withdrawal is vital to the health of patients who have implanted pumps. This case highlights the importance of recognizing potential baclofen stores that can precipitate ITB withdrawal when drained or aspirated. Treatment of ITB withdrawal may require surgical intervention, including binders, blood patches, catheter revision, and placement of a pursestring suture. Furthermore, when the cause of ITB delivery failure cannot be easily ascertained, urgent surgical exploration is indicated. References 1. Albright AL. Neurosurgical treatment of spasticity: Selective posterior rhizotomy and intrathecal baclofen. Stereotact Funct Neurosurg 1992; 58: Albright AL. Baclofen in the treatment of cerebral palsy. J Child Neurol 1996; 11: Albright AL, Gilmartin R, Swift D, Krach LE, Ivanhoe CB, McLaughlin JF. Longterm intrathecal baclofen therapy for severe spasticity of cerebral origin. J Neurosurg 2003; 98: Coffey JR, Cahill D, Steers W, Park TS, Ordia J, Meythaler J, Herman R, Shetter AG, Levy R, Gill B, Smith R, Wilberger J, Loeser JD, Chabal C, Feler C, Robertson JT, Penn RD, Clarke A, Burchiel KJ, Leibrock LG Intrathecal baclofen for intractable spasticity of spinal origin: Results of a long-term multicenter study. J Neurosurg 1993; 78: Haranhalli N, Anand D, Wisoff JH, Harter DH, Weiner HL, Blate M, Roth J. Intrathecal baclofen therapy: Complication avoidance and management. Childs Nerv Syst 2011; 27: Penn RD, Kroin JS. Intrathecal baclofen alleviates spinal cord spasticity. Lancet 1984; 1: Richard I, Menei P. Intrathecal baclofen in the treatment of spasticity, dystonia and vegetative disorders. Acta Neurochir Suppl 2007; 97: Van Schaeybroeck P, Nuttin B, Lagae L, Schrijvers E, Borghgraef C, Feys P. Intrathecal baclofen for intractable cerebral spasticity: A prospective placebo-controlled, double-blind study. Neurosurgery 2000; 46: ; discussion Awaad Y, Rizk T, Siddiqui I, Roosen N, McIntosh K, Waines GM. Complications of intrathecal baclofen pump: Prevention and cure. ISRN Neurol 2012; 2012: Sallerin B, Lazorthes Y. Intrathecal baclofen. Experimental and pharmacokinetic studies. Neurochirurgie 2003; 49: Douglas AF, Weiner HL, Schwartz DR. Prolonged intrathecal baclofen withdrawal syndrome. Case report and discussion of current therapeutic management. J Neurosurg 2005; 102: Korenkov AI, Niendorf WR, Darwish N, Glaeser E, Gaab MR. Continuous intrathecal infusion of baclofen in patients with spasticity caused by spinal cord injuries. Neurosurg Rev 2002; 25: Albright AL. Intraventricular baclofen infusion for dystonia. Report of two cases. E117
6 Pain Physician: March/April 2013; 16:E113-E118 J Neurosurg 2006; 105: Albright AL, Barry MJ, Shafton DH, Ferson SS. Intrathecal baclofen for generalized dystonia. Dev Med Child Neurol 2001; 43: Narayan RK, Loubser PG, Jankovic J, Donovan WH, Bontke CF. Intrathecal baclofen for intractable axial dystonia. Neurology 1991; 41: Sanger TD, Delgado MR, Gaebler-Spira D, Hallett M, Mink JW. Classification and definition of disorders causing hypertonia in childhood. Pediatrics 2003; 111:e89-e Bensmail D, Ward AB, Wissel J, Motta F, Saltuari L, Lissens J, Cros S, Beresniak A. Cost-effectiveness modeling of intrathecal baclofen therapy versus other interventions for disabling spasticity. Neurorehabil Neural Repair 2009; 23: Dario A, Tomei G. A benefit-risk assessment of baclofen in severe spinal spasticity. Drug Saf 2004; 27: de Lissovoy G, Matza LS, Green H, Werner M, Edgar T. Cost-effectiveness of intrathecal baclofen therapy for the treatment of severe spasticity associated with cerebral palsy. J Child Neurol 2007; 22: Hoving MA, Evers SM, Ament AJ, van Raak EP, Vles JS. Intrathecal baclofen therapy in children with intractable spastic cerebral palsy: A cost-effectiveness analysis. Dev Med Child Neurol 2008; 50: Hansen CR, Gooch JL, Such-Neibar T. Prolonged, severe intrathecal baclofen withdrawal syndrome: A case report. Arch Phys Med Rehabil 2007; 88: Vender JR, Hester S, Waller JL, Rekito A, Lee MR. Identification and management of intrathecal baclofen pump complications: A comparison of pediatric and adult patients. J Neurosurg 2006; 104: Albright AL, Ferson SS. Intraventricular baclofen for dystonia: Techniques and outcomes. Clinical article. J Neurosurg Pediatr 2009; 3: Motta F, Buonaguro V, Stignani C. The use of intrathecal baclofen pump implants in children and adolescents: Safety and complications in 200 consecutive cases. J Neurosurg 2007; 107: Hoving MA, van Raak EP, Spinc le GH, Palmans LJ, Becher JG, Vles JS. Efficacy of intrathecal baclofen therapy in children with intractable spastic cerebral palsy: A randomised controlled trial. Eur J Paediatr Neurol 2009; 13: Borowski A, Littleton AG, Borkhuu B, Presedo A, Shah S, Dabney KW, Lyons S, McMannus M, Miller F. Complications of intrathecal baclofen pump therapy in pediatric patients. J Pediatr Orthop 2010; 30: Gooch JL, Oberg WA, Grams B, Ward LA, Walker ML. Complications of intrathecal baclofen pumps in children. Pediatr Neurosurg 2003; 39: Ward A, Hayden S, Dexter M, Scheinberg A. Continuous intrathecal baclofen for children with spasticity and/or dystonia: Goal attainment and complications associated with treatment. J Paediatr Child Health 2009; 45: Bellinger A, Siriwetchadarak R, Rosenquist R, Greenlee JD. Prevention of intrathecal baclofen withdrawal syndrome: Successful use of a temporary intrathecal catheter. Reg Anesth Pain Med 2009; 34: Alden TD, Lytle RA, Park TS, Noetzel MJ, Ojemann JG. Intrathecal baclofen withdrawal: A case report and review of the literature. Childs Nerv Syst 2002; 18: Zuckerbraun NS, Ferson SS, Albright AL, Vogeley E. Intrathecal baclofen withdrawal: Emergent recognition and management. Pediatr Emerg Care 2004; 20: Siegfried RN, Jacobson L, Chabal C. Development of an acute withdrawal syndrome following the cessation of intrathecal baclofen in a patient with spasticity. Anesthesiology 1992; 77: Mohammed I, Hussain A. Intrathecal baclofen withdrawal syndrome- a lifethreatening complication of baclofen pump: A case report. BMC Clin Pharmacol 2004; 4: Miracle AC, Fox MA, Ayyangar RN, Vyas A, Mukherji SK, Quint DJ. Imaging evaluation of intrathecal baclofen pumpcatheter systems. AJNR Am J Neuroradiol 2001; 32: Kao LW, Amin Y, Kirk MA, Turner MS. Intrathecal baclofen withdrawal mimicking sepsis. J Emerg Med 2003; 24: Greenberg MI, Hendrickson RG. Baclofen withdrawal following removal of an intrathecal baclofen pump despite oral baclofen replacement. J Toxicol Clin Toxicol 2003; 41: Coffey RJ, Edgar TS, Francisco GE, Graziani V, Meythaler JM, Ridgely PM, Sadiq SA, Turner MS. Abrupt withdrawal from intrathecal baclofen: Recognition and management of a potentially life-threatening syndrome. Arch Phys Med Rehabil 2002; 83: Watve SV, Sivan M, Raza WA, Jamil FF. Management of acute overdose or withdrawal state in intrathecal baclofen therapy. Spinal Cord 2012; 50: Ross JC, Cook AM, Stewart GL, Fahy BG. Acute intrathecal baclofen withdrawal: A brief review of treatment options. Neurocrit Care 2011; 14: Salazar ML, Eiland LS. Intrathecal baclofen withdrawal resembling serotonin syndrome in an adolescent boy with cerebral palsy. Pediatr Emerg Care 2008; 24: Meythaler JM, Roper JF, Brunner RC. Cyproheptadine for intrathecal baclofen withdrawal. Arch Phys Med Rehabil 2003; 84: Dominguez E, Latif O, Rozen D, Sahinler B, Orbegozo M, Edmunds A, Lou L, Day M, Racz G, Raj P. Subdural blood patch for the treatment of persistent CSF leak after permanent intrathecal catheter implantation: A report of two cases. Pain Pract 2001; 1: Hawk MW, Kim KD. Review of spinal pseudomeningoceles and cerebrospinal fluid fistulas. Neurosurg Focus 2000; 9:e Fridley JS, Jea A, Glover CD, Nguyen KP. Symptomatic postsurgical cerebrospinal fluid leak treated by aspiration and epidural blood patch under ultrasound guidance in 2 adolescents. J Neurosurg Pediatr 2013;11: Rosenow JM. Surgical technique for intrathecal medication delivery system implantation.in: Rezai AR, Peckham H, Krames E (eds). Neuromodulation 2009; Boston, MA, Elsevier. pp Hardy PA. Extradural blood patch of a cerebrospinal fluid cutaneous fistula in the presence of an intrathecal drug delivery system. Anesthesiology 1994; 81: Chauhan C, Francis GA, Kemeny AA. The avoidance of surgery in the treatment of subarachnoid cutaneous fistula by the use of an epidural blood patch: Technical case report. Neurosurgery 1995; 36: ; discussion Singh PK, Jain R, Mishra S, Kumar S, Bhatnagar S, Deo S. Management of pericatheter cerebrospinal fluid leak after intrathecal implantation of a drug delivery system. Am J Hosp Palliat Care 2008; 25: E118
PEDIATRICS J Neurosurg Pediatr 16: , Amer Dastgir, MD, Nathan J. Ranalli, MD, Theresa L. MacGregor, PhD, and Philipp R.
 PEDIATRICS case report J Neurosurg Pediatr 16:335 339, 2015 Baclofen pump catheter leakage after migration of the abdominal catheter in a pediatric patient with spasticity Amer Dastgir, MD, Nathan J. Ranalli,
PEDIATRICS case report J Neurosurg Pediatr 16:335 339, 2015 Baclofen pump catheter leakage after migration of the abdominal catheter in a pediatric patient with spasticity Amer Dastgir, MD, Nathan J. Ranalli,
A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative
 A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative Kathryn M. Wagner, Virendra R. Desai, Jeffrey S. Raskin, Arvind Mohan, JoWinsyl Montojo, Valentina
A Standardized Protocol to Reduce Pediatric Baclofen Pump Infections: A Quality Improvement Initiative Kathryn M. Wagner, Virendra R. Desai, Jeffrey S. Raskin, Arvind Mohan, JoWinsyl Montojo, Valentina
In June 1996, the US Food and Drug Administration
 Clinical article J Neurosurg Pediatr 18:493 498, 2016 Comparison between an Ascenda and a silicone catheter in intrathecal baclofen therapy in pediatric patients: analysis of complications Francesco Motta,
Clinical article J Neurosurg Pediatr 18:493 498, 2016 Comparison between an Ascenda and a silicone catheter in intrathecal baclofen therapy in pediatric patients: analysis of complications Francesco Motta,
Intrathecal Baclofen for Spasticity. Dr. M. Mehra Dr. A. Kumar
 Intrathecal Baclofen for Spasticity Dr. M. Mehra Dr. A. Kumar Goals of Spasticity: Management Decrease spasticity Improve functional ability and independence Decrease pain associated with spasticity Prevent
Intrathecal Baclofen for Spasticity Dr. M. Mehra Dr. A. Kumar Goals of Spasticity: Management Decrease spasticity Improve functional ability and independence Decrease pain associated with spasticity Prevent
BOTULINUM TOXIN AND INTRATHECAL BACLOFEN. Spencer Cotterell DO Mercy Rehabilitation Hospital June 30, 2018
 BOTULINUM TOXIN AND INTRATHECAL BACLOFEN Spencer Cotterell DO Mercy Rehabilitation Hospital June 30, 2018 INJECTABLES MEDICAL MANAGEMENT OF SPASTICITY Leonard, J In: Botulinum toxin: 2009 A protein and
BOTULINUM TOXIN AND INTRATHECAL BACLOFEN Spencer Cotterell DO Mercy Rehabilitation Hospital June 30, 2018 INJECTABLES MEDICAL MANAGEMENT OF SPASTICITY Leonard, J In: Botulinum toxin: 2009 A protein and
Introduction. Conflict of Interest Disclosure. Author s conflicts of interest: Kimberly Gonzalez, RN, BSN, no conflict of interest
 Kimberly Gonzalez, RN, BSN September 15, 2017 ASPMN Annual Conference Introduction Kimberly A. Gonzalez, B.S.N., Critical Care Unit, Content Expert, Clin III BSN, University of Texas at Arlington, May
Kimberly Gonzalez, RN, BSN September 15, 2017 ASPMN Annual Conference Introduction Kimberly A. Gonzalez, B.S.N., Critical Care Unit, Content Expert, Clin III BSN, University of Texas at Arlington, May
Role of Intrathecal Baclofen. Mr. Chirag Patel Consultant Paediatric Neurosurgeon Children s Hospital for Wales, Cardiff.
 Role of Intrathecal Baclofen Mr. Chirag Patel Consultant Paediatric Neurosurgeon Children s Hospital for Wales, Cardiff. History of Intrathecal Baclofen therapy 1978: First used in guinea pigs by Wilson.
Role of Intrathecal Baclofen Mr. Chirag Patel Consultant Paediatric Neurosurgeon Children s Hospital for Wales, Cardiff. History of Intrathecal Baclofen therapy 1978: First used in guinea pigs by Wilson.
Pharmacokinetics and pharmacodynamics of intrathecal baclofen therapy Heetla, Herre Wigger
 University of Groningen Pharmacokinetics and pharmacodynamics of intrathecal baclofen therapy Heetla, Herre Wigger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Pharmacokinetics and pharmacodynamics of intrathecal baclofen therapy Heetla, Herre Wigger IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Intrathecal baclofen (ITB) therapy has been used to. Risk factors for baclofen pump infection in children: a multivariate analysis
 clinical article J Neurosurg Pediatr 17:756 762, 2016 Risk factors for baclofen pump infection in children: a multivariate analysis Heather S. Spader, MD, Robert J. Bollo, MD, MS, Christian A. Bowers,
clinical article J Neurosurg Pediatr 17:756 762, 2016 Risk factors for baclofen pump infection in children: a multivariate analysis Heather S. Spader, MD, Robert J. Bollo, MD, MS, Christian A. Bowers,
CATHETER MIGRATION AFTER IMPLANTATION OF
 CATHETER MIGRATION AFTER IMPLANTATION OF AN INTRATHECAL BACLOFEN INFUSION PUMP FOR SEVERE SPASTICITY: A CASE REPORT Tung-Chou Li, 1 Mei-Hsiu Chen, 2 Jing-Shan Huang, 3 Jun-Yeen Chan, 3 Yaun-Kai Liu, 3
CATHETER MIGRATION AFTER IMPLANTATION OF AN INTRATHECAL BACLOFEN INFUSION PUMP FOR SEVERE SPASTICITY: A CASE REPORT Tung-Chou Li, 1 Mei-Hsiu Chen, 2 Jing-Shan Huang, 3 Jun-Yeen Chan, 3 Yaun-Kai Liu, 3
Research Article Complications of Intrathecal Baclofen Pump: Prevention and Cure
 International Scholarly Research Network ISRN Neurology Volume 2012, Article ID 575168, 6 pages doi:10.5402/2012/575168 Research Article Complications of Intrathecal Baclofen Pump: Prevention and Cure
International Scholarly Research Network ISRN Neurology Volume 2012, Article ID 575168, 6 pages doi:10.5402/2012/575168 Research Article Complications of Intrathecal Baclofen Pump: Prevention and Cure
Intrathecal Baclofen. Val Stevenson
 Intrathecal Baclofen Val Stevenson Plan What is it, how does it work? Who is it for? How is it done? Evidence base Pros and cons Case study Baclofen GABA derivative (inhibitory neurotransmitter) Presynaptic
Intrathecal Baclofen Val Stevenson Plan What is it, how does it work? Who is it for? How is it done? Evidence base Pros and cons Case study Baclofen GABA derivative (inhibitory neurotransmitter) Presynaptic
Acute Intrathecal Baclofen Withdrawal: A Brief Review of Treatment Options
 Neurocrit Care (2011) 14:103 108 DOI 10.1007/s12028-010-9422-6 PRACTICAL PEARL Acute Intrathecal Baclofen Withdrawal: A Brief Review of Treatment Options James C. Ross Aaron M. Cook Gary L. Stewart Brenda
Neurocrit Care (2011) 14:103 108 DOI 10.1007/s12028-010-9422-6 PRACTICAL PEARL Acute Intrathecal Baclofen Withdrawal: A Brief Review of Treatment Options James C. Ross Aaron M. Cook Gary L. Stewart Brenda
An algorithmic approach to the management of unrecognized hydrocephalus in pediatric candidates for intrathecal baclofen pump implantation
 OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original Article An algorithmic approach
OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original Article An algorithmic approach
Intrathecal Baclofen in Spinal Spasticity: Frequency and Severity of Withdrawal Syndrome. Pain Physician 2015; 18:E633-E641
 Pain Physician 2015; 18:E633-E641 ISSN 2150-1149 Case Study Intrathecal Baclofen in Spinal Spasticity: Frequency and Severity of Withdrawal Syndrome Ivana Stetkarova, MD, PhD 1, Karel Brabec, MD 1, Peter
Pain Physician 2015; 18:E633-E641 ISSN 2150-1149 Case Study Intrathecal Baclofen in Spinal Spasticity: Frequency and Severity of Withdrawal Syndrome Ivana Stetkarova, MD, PhD 1, Karel Brabec, MD 1, Peter
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY. Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery
 INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery Intrathecal Therapy Insertion of a drug into CSF space, commonly
INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery Intrathecal Therapy Insertion of a drug into CSF space, commonly
INTRATHECAL BACLOFEN THERAPY
 INTRATHECAL BACLOFEN THERAPY Michael Saulino, MD/PhD Associate professor Department of Rehabilitation Medicine Thomas Jefferson University Adjuvant Assistant Professor Temple University Staff Physiatrist
INTRATHECAL BACLOFEN THERAPY Michael Saulino, MD/PhD Associate professor Department of Rehabilitation Medicine Thomas Jefferson University Adjuvant Assistant Professor Temple University Staff Physiatrist
Review the enclosed Urgent: Medical Device Correction Complete and return the Reply Card
 July 2011 Dear Healthcare Professional, Enclosed is an update regarding the potential for reduced battery performance that can lead to sudden loss of therapy in a small percentage of SynchroMed II pumps.
July 2011 Dear Healthcare Professional, Enclosed is an update regarding the potential for reduced battery performance that can lead to sudden loss of therapy in a small percentage of SynchroMed II pumps.
ITB therapy, first described in 1984 by Penn and Kroin 1 for the
 Published November 24, 2010 as 10.3174/ajnr.A2211 REVIEW ARTICLE A.C. Miracle M.A. Fox R.N. Ayyangar A. Vyas S.K. Mukherji D.J. Quint Imaging Evaluation of Intrathecal Baclofen Pump-Catheter Systems SUMMARY:
Published November 24, 2010 as 10.3174/ajnr.A2211 REVIEW ARTICLE A.C. Miracle M.A. Fox R.N. Ayyangar A. Vyas S.K. Mukherji D.J. Quint Imaging Evaluation of Intrathecal Baclofen Pump-Catheter Systems SUMMARY:
THERAPY Baclofen Pump Program at Boston Children s Hospital
 BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
IMPLANTABLE INTRATHECAL DRUG DELIVERY SYSTEMS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Intrathecal Opioid Therapy for Management of Chronic Pain
 Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE
 ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
Intrathecal baclofen infusion and subsequent orthopedic surgery in patients with spastic cerebral palsy
 Neurosurg Focus 4 (1):Article 3, 1998 Intrathecal baclofen infusion and subsequent orthopedic surgery in patients with spastic cerebral palsy Peter C. Gerszten, M.D., A. Leland Albright, M.D., and Graham
Neurosurg Focus 4 (1):Article 3, 1998 Intrathecal baclofen infusion and subsequent orthopedic surgery in patients with spastic cerebral palsy Peter C. Gerszten, M.D., A. Leland Albright, M.D., and Graham
A Patient s Guide to Pain Management: Pain Pumps
 A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Rising Complication Rates after Intrathecal Catheter and Pump Placement in the Pediatric Population: Analysis of National Data Between 1997 and 2006
 Pain Physician 2012; 15:65-74 ISSN 1533-3159 Observational Study Rising Complication Rates after Intrathecal Catheter and Pump Placement in the Pediatric Population: Analysis of National Data Between 1997
Pain Physician 2012; 15:65-74 ISSN 1533-3159 Observational Study Rising Complication Rates after Intrathecal Catheter and Pump Placement in the Pediatric Population: Analysis of National Data Between 1997
Infusion Pump Surgery: Achievements and Limitation. Yasir MH. Hamandi FIBMS, Abdulameer J. Al-Khafaji FIBMS, Haider A.
 Iraqi JS Published by Al-Nahrain College of edicine ISSN 1681-6579 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-nahrain.edu.iq Infusion Pump Surgery: Achievements and Limitation Yasir H. Hamandi
Iraqi JS Published by Al-Nahrain College of edicine ISSN 1681-6579 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-nahrain.edu.iq Infusion Pump Surgery: Achievements and Limitation Yasir H. Hamandi
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Intrathecal baclofen use in adults with cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Intrathecal baclofen use in adults with cerebral palsy LINDA E KRACH MD Department of Physical Medicine and Rehabilitation, University of Minnesota, Minneapolis,
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Intrathecal baclofen use in adults with cerebral palsy LINDA E KRACH MD Department of Physical Medicine and Rehabilitation, University of Minnesota, Minneapolis,
LV-EBP: Record-setting large volume epidural blood patch
 LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems
 Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans
Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans
Intrathecal drug therapy using the Codman Model 3000 Constant Flow Implantable Infusion Pumps: experience with 17 cases
 (2005) 43, 214 218 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Original Article Intrathecal drug therapy using the Codman Model 3000 Constant Flow Implantable
(2005) 43, 214 218 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Original Article Intrathecal drug therapy using the Codman Model 3000 Constant Flow Implantable
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Overview. Spasticity. Spasticity. Oral Medications. Spasticity 3/10/2012. Medication Management of Spasticity in the Traumatic Brain Injured Patient
 Medication Management of in the Traumatic Brain Injured Patient 6 th Annual Northern Kentucky TBI Conference March 23, 2012 www.bridgesnky.org Chad Walters, D.O. Medical Director Radical Rehab Solutions
Medication Management of in the Traumatic Brain Injured Patient 6 th Annual Northern Kentucky TBI Conference March 23, 2012 www.bridgesnky.org Chad Walters, D.O. Medical Director Radical Rehab Solutions
Guidelines for longterm intrathecal infusions (Analgesics/adjuvants/antispasmodics)
 PM06 PM2 2012 2018 Faculty of Pain Medicine Australian and New Zealand College of Anaesthetists Guidelines for longterm intrathecal infusions (Analgesics/adjuvants/antispasmodics) 1. INTRODUCTION 1.1 Persistent
PM06 PM2 2012 2018 Faculty of Pain Medicine Australian and New Zealand College of Anaesthetists Guidelines for longterm intrathecal infusions (Analgesics/adjuvants/antispasmodics) 1. INTRODUCTION 1.1 Persistent
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
INTRODUCTION METHODS. Original Article. Singapore Med J 2015; 57(1): 8-12 doi: /smedj
 Singapore Med J 2015; 57(1): 8-12 doi: 10.11622/smedj.2016005 Treatment of severe, disabling spasticity with continuous intrathecal baclofen therapy following acquired brain injury: the experience of a
Singapore Med J 2015; 57(1): 8-12 doi: 10.11622/smedj.2016005 Treatment of severe, disabling spasticity with continuous intrathecal baclofen therapy following acquired brain injury: the experience of a
Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch
 J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
Dr. Park s SDR Publication
 Dr. Park s SDR Publication Journal Papers 1. Phillips LH, Park TS: Electrophysiological mapping of the segmental anatomy of the muscles of the lower extremity. Muscle and Nerve 1991; 14:1213-121 2. Harris
Dr. Park s SDR Publication Journal Papers 1. Phillips LH, Park TS: Electrophysiological mapping of the segmental anatomy of the muscles of the lower extremity. Muscle and Nerve 1991; 14:1213-121 2. Harris
Incidental durotomy during spine surgery occurs in. Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks
 J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
Dystonia. The condition can vary from very mild to severe. Dystonia may get worse over time or it may stay the same or get better.
 Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
CONTINUAL INFUSION OF INTRATHECAL BACLOFEN (ITB): LONG TERM EFFECT ON SPASTICITY
 CONTINUAL INFUSION OF INTRATHECAL BACLOFEN (ITB): LONG TERM EFFECT ON SPASTICITY Dhafir Al Khudhairi *, Abdulrahman Shug a Aldin **, Yousef Hamdan ***, Abdullah Rababah ****, Mona Hafez Matthana *****,
CONTINUAL INFUSION OF INTRATHECAL BACLOFEN (ITB): LONG TERM EFFECT ON SPASTICITY Dhafir Al Khudhairi *, Abdulrahman Shug a Aldin **, Yousef Hamdan ***, Abdullah Rababah ****, Mona Hafez Matthana *****,
Coding and Reimbursement for
 Coding and Reimbursement for The material referenced and provided is based upon research of current Medicare reference sources. The final decision of billing for any product or procedure must be made by
Coding and Reimbursement for The material referenced and provided is based upon research of current Medicare reference sources. The final decision of billing for any product or procedure must be made by
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT. Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
SynchroMed EL Pump Motor Stall Due To Gear Shaft Wear
 Aug 2007 Important Patient Management Information SynchroMed EL Pump Motor Stall Due To Gear Shaft Wear Pumps with Motors Manufactured Beginning September 1999 Models Affected: 8626-10, 8626L-10, 8626-18,
Aug 2007 Important Patient Management Information SynchroMed EL Pump Motor Stall Due To Gear Shaft Wear Pumps with Motors Manufactured Beginning September 1999 Models Affected: 8626-10, 8626L-10, 8626-18,
The Role of the Neuromodulation in Management of Chronic Pain
 The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
Mri with baclofen pump
 Mri with baclofen pump 830 South Main St Suite 2 Orrville, OH 44667. 1207 W. State St. Suite N Alliance, OH 44601. NeuroCare Orrville Hours: W & TH 7AM-4:30PM (subject to change). var r = [99, 104, 101,
Mri with baclofen pump 830 South Main St Suite 2 Orrville, OH 44667. 1207 W. State St. Suite N Alliance, OH 44601. NeuroCare Orrville Hours: W & TH 7AM-4:30PM (subject to change). var r = [99, 104, 101,
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
About 70% of brachial plexus injuries are of. Neuromodulation in the Management of Pain from Brachial Plexus Injury. Case Report
 Pain Physician 2008; 11:81-85 ISSN 1533-3159 Case Report Neuromodulation in the Management of Pain from Brachial Plexus Injury Silviu Brill, MD, and Itay Goor Aryeh, MD From: Pain Clinic, Department of
Pain Physician 2008; 11:81-85 ISSN 1533-3159 Case Report Neuromodulation in the Management of Pain from Brachial Plexus Injury Silviu Brill, MD, and Itay Goor Aryeh, MD From: Pain Clinic, Department of
Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai. Interventional Options
 10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
Case Report. Ilioinguinal Peripheral Nerve Stimulation. Juan A. Ramos, MD 1, Andrew J. McNeil, DO 2, Ted F. Gingrich, MD 3
 Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Sales of Intrathecal Baclofen Therapy Products Begin
 For Immediate Release Company name: DAIICHI SANKYO COMPANY, LIMITED Representative: Takashi Shoda, President and Representative Director (Code no.: 4568, First Section, Tokyo, Osaka and Nagoya Stock Exchanges)
For Immediate Release Company name: DAIICHI SANKYO COMPANY, LIMITED Representative: Takashi Shoda, President and Representative Director (Code no.: 4568, First Section, Tokyo, Osaka and Nagoya Stock Exchanges)
Advanced Treatment of Spasticity 14 th Jan 2017
 About the Society of Rehabilitation Medicine (Singapore) Advanced Treatment of Spasticity 14 th Jan 2017 Dr Geoffrey S Samuel Consultant Department of Rehabilitation Medicine Singapore General Hospital
About the Society of Rehabilitation Medicine (Singapore) Advanced Treatment of Spasticity 14 th Jan 2017 Dr Geoffrey S Samuel Consultant Department of Rehabilitation Medicine Singapore General Hospital
ICD-9-CM Diagnosis Code options
 ICD-9-CM Diagnosis Code options Diagnosis codes are used by both physicians and facilities to document the indication for the procedure. Intrathecal drug delivery is directed at managing chronic, intractable
ICD-9-CM Diagnosis Code options Diagnosis codes are used by both physicians and facilities to document the indication for the procedure. Intrathecal drug delivery is directed at managing chronic, intractable
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY. Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group
 IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
SINGAPORE GUIDED LUMBAR PROCEDURES WORKSHOP ULTRASOUND AND FLUOROSCOPIC OCTOBER 29-30, 2016 ACADEMIA, SINGAPORE GENERAL HOSPITAL PRESENTED BY:
 ULTRASOUND AND FLUOROSCOPIC GUIDED LUMBAR PROCEDURES WORKSHOP ACADEMIA, SINGAPORE GENERAL HOSPITAL SINGAPORE OCTOBER 29-30, 2016 CORPORATE SUPPORT: PRESENTED BY: Ultrasound and Fluoroscopic Guided Lumbar
ULTRASOUND AND FLUOROSCOPIC GUIDED LUMBAR PROCEDURES WORKSHOP ACADEMIA, SINGAPORE GENERAL HOSPITAL SINGAPORE OCTOBER 29-30, 2016 CORPORATE SUPPORT: PRESENTED BY: Ultrasound and Fluoroscopic Guided Lumbar
Urgent: Medical Device Correction
 January 2008 Urgent: Medical Device Correction Updated Information - Inflammatory Mass (granuloma) At or Near the Distal Tip of Intrathecal Catheters Dear Healthcare Professional, This letter is an update
January 2008 Urgent: Medical Device Correction Updated Information - Inflammatory Mass (granuloma) At or Near the Distal Tip of Intrathecal Catheters Dear Healthcare Professional, This letter is an update
Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
 International Journal of Health Sciences, Qassim University, Vol. 8, No. 1 (January-March 2014) Case Report Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
International Journal of Health Sciences, Qassim University, Vol. 8, No. 1 (January-March 2014) Case Report Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
Lumbar CSF Drains for Thoracic Aortic Surgery
 Lumbar CSF Drains for Thoracic Aortic Surgery John C. Klick, MD CASE CAG Why do them? Open descending thoracic aortic aneurysm repair (still the gold standard) has an incidence of postoperative paraplegia
Lumbar CSF Drains for Thoracic Aortic Surgery John C. Klick, MD CASE CAG Why do them? Open descending thoracic aortic aneurysm repair (still the gold standard) has an incidence of postoperative paraplegia
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Implantable Infusion Pump for Pain and Spasticity
 Implantable Infusion Pump for Pain and Spasticity Policy Number: 7.01.41 Last Review: 6/2018 Origination: 1/1988 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Implantable Infusion Pump for Pain and Spasticity Policy Number: 7.01.41 Last Review: 6/2018 Origination: 1/1988 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Life Care Plan. Eric Henderson Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
STANDARDIZED PROCEDURE REPROGRAMMING AND REFILLING INTRATHECAL BACLOFEN PUMPS and ACCESSING THE CATHETER ACCESS PORT (Adult,Peds)
 I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
Katherine Gibson-Corley DVM, PhD, DACVP. Pathology Grand Rounds March 27, 2014
 Katherine Gibson-Corley DVM, PhD, DACVP Pathology Grand Rounds March 27, 2014 Outline Introduction to spinal cord stimulation (SCS) Current SCS devices The Iowa-Patch TM (I-Patch) Post-surgical pathologies
Katherine Gibson-Corley DVM, PhD, DACVP Pathology Grand Rounds March 27, 2014 Outline Introduction to spinal cord stimulation (SCS) Current SCS devices The Iowa-Patch TM (I-Patch) Post-surgical pathologies
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
10 Years of Experience with Intrathecal Baclofen a review of safety and adverse events
 10 Years of Experience with Intrathecal Baclofen a review of safety and adverse events Romain Briest 1, Remo (Ray) Russo 1,2, Felicity Baker 1, James Rice 1 1. Women's and Children's Health Network 2.
10 Years of Experience with Intrathecal Baclofen a review of safety and adverse events Romain Briest 1, Remo (Ray) Russo 1,2, Felicity Baker 1, James Rice 1 1. Women's and Children's Health Network 2.
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
While some patients with SIH recover without intervention
 ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Department of Anesthesiology and Pain Medicine, School of Medicine, Catholic University of Daegu, Daegu, Korea
 Original Article Korean J Pain 2013 January; Vol. 26, No. 1: 32-38 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.1.32 Continuous Intrathecal Morphine Administration for Cancer Pain
Original Article Korean J Pain 2013 January; Vol. 26, No. 1: 32-38 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.1.32 Continuous Intrathecal Morphine Administration for Cancer Pain
 Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Surgical Privileges Form: "Neurosurgery" Clinical Privileges Request. Requested (To be completed by the applicant) Not Recommended (For committee use)
 Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Spinal Cord Stimulation for Multiple Sclerosis and Spinal Cord Injury
 Spinal Cord Stimulation for Multiple Sclerosis and Spinal Cord Injury R. Davis Neural Engineering Clinic, PO Box 480, Rockport, Maine, 04856, U.S.A. Introduction Since 1973, spinal cord stimulation (SCS)
Spinal Cord Stimulation for Multiple Sclerosis and Spinal Cord Injury R. Davis Neural Engineering Clinic, PO Box 480, Rockport, Maine, 04856, U.S.A. Introduction Since 1973, spinal cord stimulation (SCS)
Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management
 S20 Journal of Pain and Symptom Management Vol. 31 No. 4S April 2006 Special Article Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management Michael Stanton-Hicks
S20 Journal of Pain and Symptom Management Vol. 31 No. 4S April 2006 Special Article Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management Michael Stanton-Hicks
DELINEATION OF PRIVILEGES - NEUROSURGERY
 KALEIDA HEALTH Name Date DELINEATION OF PRIVILEGES - NEUROSURGERY PLEASE NOTE: Please check the box for each privilege requested. Do not use an arrow or line to make selections. We will return applications
KALEIDA HEALTH Name Date DELINEATION OF PRIVILEGES - NEUROSURGERY PLEASE NOTE: Please check the box for each privilege requested. Do not use an arrow or line to make selections. We will return applications
Catheter Obstruction of Intrathecal Drug Administration System
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 47-51 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.47 Catheter Obstruction of Intrathecal Drug Administration System -A
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 47-51 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.47 Catheter Obstruction of Intrathecal Drug Administration System -A
STANDARDIZED PROCEDURE LUMBAR PUNCTURE (Adult, Peds)
 I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
Visualization of Sacral Nerve Roots via Percutaneous Intraspinal Navigation (PIN) V
 AJNR Am J Neuroradiol 26:2420 2424, October 2005 Technical Note Visualization of Sacral Nerve Roots via Percutaneous Intraspinal Navigation (PIN) V Takuya Fujimoto, Brian P. Giles, Robert E. Replogle,
AJNR Am J Neuroradiol 26:2420 2424, October 2005 Technical Note Visualization of Sacral Nerve Roots via Percutaneous Intraspinal Navigation (PIN) V Takuya Fujimoto, Brian P. Giles, Robert E. Replogle,
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Life Care Plan. Hannah Sayne Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
C ontinuous intrathecal baclofen infusion using a subcutaneously
 PAPER Long term effect (more than five years) of intrathecal baclofen on impairment, disability, and quality of life in patients with severe spasticity of spinal origin A Zahavi, J H B Geertzen, B Middel,
PAPER Long term effect (more than five years) of intrathecal baclofen on impairment, disability, and quality of life in patients with severe spasticity of spinal origin A Zahavi, J H B Geertzen, B Middel,
LUMBAR PUNCTURE. Multimedia Health Education
 LUMBAR PUNCTURE Disclaimer This film is an educational resource only and should not be used to make a decision on. All such decisions must be made in consultation with a physician or licensed healthcare
LUMBAR PUNCTURE Disclaimer This film is an educational resource only and should not be used to make a decision on. All such decisions must be made in consultation with a physician or licensed healthcare
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Anesthesia Processing Guidelines
 Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
Image-guided intrathecal baclofen pump catheter implantation: a technical note and case series
 CLINICAL ARTICLE J Neurosurg Spine 26:621 627, 2017 Image-guided intrathecal baclofen pump catheter implantation: a technical note and case series Shenandoah Robinson, MD, 1,2 Faith C. Robertson, BS, 2
CLINICAL ARTICLE J Neurosurg Spine 26:621 627, 2017 Image-guided intrathecal baclofen pump catheter implantation: a technical note and case series Shenandoah Robinson, MD, 1,2 Faith C. Robertson, BS, 2
Durotomies with CSF leakage are one of the most
 CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
PAAQS Reference Guide
 Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
PHYSICIAN CODING AND PAYMENT GUIDE
 Targeted Drug Delivery PHYSICIAN CODING AND PAYMENT GUIDE 2018 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Targeted Drug Delivery PHYSICIAN CODING AND PAYMENT GUIDE 2018 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
LIVE LIFE WITH LESS PAIN
 LIVE LIFE WITH LESS PAIN Medtronic Pain Therapies Medtronic Inc. 710 Medtronic Pkwy. Minneapolis, MN 55432 USA Tel. 1-763-505-5000 medtronic.com 2017 Medtronic. UC201502755c EN Living with pain can be
LIVE LIFE WITH LESS PAIN Medtronic Pain Therapies Medtronic Inc. 710 Medtronic Pkwy. Minneapolis, MN 55432 USA Tel. 1-763-505-5000 medtronic.com 2017 Medtronic. UC201502755c EN Living with pain can be
Hydrocephalus 1/16/2015. Hydrocephalus. Functions of Cerebrospinal fluid (CSF) Flow of CSF
 Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
