Similarities Between Interstitial Cystitis and Male Chronic Pelvic Pain Syndrome
|
|
|
- Ashley Douglas
- 6 years ago
- Views:
Transcription
1 Similarities Between Interstitial Cystitis and Male Chronic Pelvic Pain Syndrome Robert M. Moldwin, MD, FACS Address Department of Urology, Long Island Jewish Medical Center, th Avenue, New Hyde Park, NY 11040, USA. Current Urology Reports 2002, 3: Current Science Inc. ISSN Copyright 2002 by Current Science Inc. Few clinical conditions encountered by the urologist cause more patient and clinician frustration than interstitial cystitis and male chronic pelvic pain syndrome, also know as nonbacterial prostatitis. This frustration is fueled by the chronicity of often disabling urogenital (and often associated systemic) symptoms coupled with delayed care, misdiagnosis, and suboptimal clinical responses. Basic research and therapeutic trials for these syndromes have historically taken two separate paths. However, mounting evidence suggests that significant overlap may exist between them in epidemiology, pathophysiology, and even therapy. This discussion reviews some of the common features of these clinical problems and makes a case that they might in fact represent different manifestations of the same disease process. Introduction Epidemiology Interstitial cystitis (IC) and male chronic pelvic pain syndrome (MCPPS) are highly prevalent in the general population. Recent epidemiologic studies suggest that approximately 700,000 females in the United States are afflicted with IC [1 ]. If males were considered, this estimate might be as high as 1 million! National Ambulatory Medical Care Surveys demonstrate nearly 2 million physician visits per year with prostatitis listed as the diagnosis, the vast majority of those encounters likely due to National Institutes of Health (NIH) category IIIA MCPPS. Prostatitis was listed as a diagnosis in 8% and 1% of urologic and primary care visits, respectively [2 ]. In addition, 16% of 31,681 health care professionals surveyed in the United States (all without prostate cancer) selfreported a history of prostatitis [3 ]. Impact on the quality of life Perhaps more significant than the high prevalence of IC and MCPPS is the often devastating impact that these conditions have on the quality of life. Chronic pain and irritative voiding symptoms can have a profound impact on employment status, sexuality, and activities of daily living. In 1987, Held et al. [4] reported that patients with IC were three to four times more likely to report thoughts of suicide than the general population. Additionally, patients with IC were five times more likely to have been treated for emotional problems. Quality-of-life evaluations were rated lower for these patients than patients receiving hemodialysis for endstage renal disease. In a 1993 study by Koziol et al. [5], 93.4% of patients with IC found it difficult or impossible to travel. Leisure activities, sleep, and employment were adversely affected in 89.9%, 88.2%, and 84.4% of patients, respectively. Family relationships and responsibilities were adversely affected in 69.7% of patients. The National IC Database Study (sponsored by the National Institute of Diabetes, Digestive, and Kidney Diseases [NIDDK]) found interference with work and social activities in 54% and 71.7% of respondents, respectively [6]. Unfortunately, less attention has been given to the patient with MCPPS with regard to its impact on quality of life, however, completed studies have showed startling disturbances. In 1996, Wenninger et al. [7] noted that sickness impact profiles of patients with prostatitis were comparable with those of patients suffering from myocardial infarction, angina, or Crohn s disease. Quality-of-life scores related to mental health have been found to be lower in patients with MCPPS than in patients with severe congestive heart failure and diabetes mellitus [8 ]. Theories of Pathogenesis A review of literature compiled over the past 20 years demonstrates that investigations related to IC and MCCPS IIIA have taken separate but parallel paths. Interestingly, in many instances these paths have led to similar theories of etiology and pathogenesis, ranging from atypical organisms to aberrant neuronal function. Some investigated findings are discussed below. Occult infection Although Category IIIA MCPPS is not characteristically associated with bacteria found within expressed prostatic secretions (EPS), urine voided after prostatic massage, or semen, infection with atypical or fastidious organisms has been proposed by numerous investigators [9 12]. Krieger et al. [13] demonstrated bacterial DNA sequences
2 314 Prostatitis (Urinary Tract Infections) to be significantly more common in the prostate biopsy tissue of patients with chronic prostatitis/chronic pelvic pain syndrome (46.4%) versus patients with prostate cancer (19.6%). Using 16S rrna polymerase chain reaction (PCR) technique, Shoskes and Shahed [14] found bacterial DNA in as many as 70% of EPS specimens from patients with MCPPS IIIA. Fifty-one percent of those patients were also found to have gram-positive bacteria EPS cultures, bacteria that are often assumed to be commensals. Only 14% of those patients without prostatic inflammation (NIH MCPPS IIB) had bacterial DNA in their EPS. Interestingly, 57% of the total patients who had PCR positive for bacterial DNA improved with antibiotic therapy, while no patient with a negative PCR for bacterial DNA improved on antibiotic therapy. This study certainly suggests that PCR may aid in selecting patients for antibiotic therapy, but also suggests that occult bacteria may participate in the genesis of patient symptoms in a subpopulation of patients with MCPPS IIIA. These findings have prompted treatment algorithms to include an initial trial of antibiotic therapy without laboratory evidence of overt infection [15,16]. In contrast to these studies, Keay et al. [17] demonstrated bacterial DNA to be present in the transperineal biopsies of 89% of patients diagnosed with prostate cancer, a higher percentage than seen in the MCPPS IIIA groups of other studies. These conflicting data, difficulties in the determination of commensal versus virulent organisms, the focal nature of prostatitis, and the added variable of bacterial protection in the form of prostatic calculi and biofilms continue to impair investigative efforts. Similar controversies exist regarding an infectious etiology for IC. Sophisticated culture techniques that identify fastidious or unusual bacterial forms, Mycoplasma species, fungi, and viruses have failed to consistently demonstrate a causative organism [18]. Likewise, PCR technique has failed to demonstrate differences in bacterial forms between bladder biopsies of patients with IC and control subjects [19,20]. Interestingly, occasional reports are published that stir up conventional wisdom. Such a study was published in 2000 by Potts et al. [21] who identified Ureaplasma urealyticum in 48% of patients: patients who would have been otherwise diagnosed with IC. Ninety-one percent of these patients treated with antibiotics had improvement in their symptoms. Many patients with IC have had a documented urinary tract infection with consequent chronic bladder-based symptoms. This has lead many investigators to speculate that the episode of cystitis might have caused permanent bladder injury and the subsequent development of irritative voiding symptoms [22]. This scenario certainly might fit the patient with prostatitis as well. Leaky epithelium The healthy bladder surface is coated by a thin mucinous substance, termed bladder surface mucin (BSM), which is composed of numerous sulfonated glycosaminoglycans and glycoproteins. BSM is thought to function as a bladder protectant, decreasing the ability of organisms to bind to the underlying urothelial cells. Qualitative changes have been noted in BSM between IC patients and control subjects, and in some animal models of IC [23 26]. It has been speculated that these qualitative changes in BSM may cause permeability alterations, with the permeability changes ultimately resulting in bladder inflammation and/ or hyperalgesia [25]. Although prostatic acini are lined by columnar epithelium rather than transitional cells, the prostatic surface does elaborate mucus [27,28]. Could changes of the prostatic epithelial surface or its elaborated mucin, when exposed to the common occurrence of intraprostatic urinary reflux [29 ], be responsible for patient symptoms in MCPPS? The potassium sensitivity test was developed by Parsons [30] as a relatively simple office procedure to help diagnose patients with IC. Patients with IC will typically have a worsening of pelvic pain and/or irritative voiding symptoms after the instillation of a potassium chloride solution, presumably due to enhanced absorption of the salt through a defective bladder surface. Preliminary data collected by Parsons (Personal communication) demonstrated that 84% of 43 patients (18% with increased frequency only) with MCPPS IIIA tested positive with the potassium sensitivity test, thereby suggesting a common etiology for symptoms between the IC and MCPPS groups. Pentosan polysulfate sodium (PPS) is a common medication used for the treatment of IC. Its presumed mechanism of action is its binding to the urothelial surface, thereby augmenting an abnormally permeable bladder surface. Recent preliminary uncontrolled studies suggest that this medication may improve the symptoms of patients suffering from MCPPS IIIA [31]. Although further studies are clearly needed to determine the efficacy of PPS for the treatment of MCPPS, perhaps this similarity in clinical response reflects similarities in pathogenesis. Neurogenic inflammation Neurogenic inflammation is a well-described phenomenon that occurs in the patient with IC. In this paradigm, sensory nerves may secrete inflammatory mediators, resulting in local inflammation and/or hyperalgesia. A central component of this process is Substance P, a short chain peptide that functions as a nociceptive neurotransmitter in the central and peripheral nervous system, as well as an inflammatory mediator. When released by peripheral nerves (C-fibers or fibers associated with pain transmission) an inflammatory cascade occurs that results in processes such as mast cell degranulation and the activation of nearby nerve terminals. Supporting this pathogenic mechanism is the finding of increased numbers of substance P- containing nerves in the bladders of IC patients [32,33]. Additionally, increased concentrations of substance P have been found in the urine of patients with IC, the concentration of substance P being affected by the patient s degree of
3 Similarities Between IC and Male CPPS Moldwin 315 pain [34]. No investigations have yet been performed to detail the role of neurogenic inflammation in MCPPS IIIA, however, symptomatic improvements observed in patients after intravesicular instillation of dimethyl sulfoxide [35], a gold standard therapy for IC and a depleter of substance P [36], suggest that neurogenic inflammation may play a role in symptom exacerbation in some patients. Additionally, an animal model of spontaneous nonbacterial prostatitis has demonstrated an increased number of sensory C-fibers with progression of inflammation [37]. Mast cell activation Mast cells contain cytoplasmic granules, which themselves contain substances such as histamine, leukotrienes, prostaglandins, and tryptases: all of these agents are capable of stimulating inflammation. These granules may be released into the interstitium (degranulation) as part of an immunoglobulin E-mediated hypersensitivity reaction or in response to multiple other stimuli including neurotransmitters (substance P), cytokines, anaphylatoxins (complement: C3a, 4a, 5a), bacterial toxins, hypoxia, physical factors, lectins, various allergens, toxins, stress, and others [38 41]. Mastocytosis has been reported in the bladders of 30% to 65% of patients with IC [42,43]. This is probably an underestimation due to technical difficulties in identifying mast cells that have already degranulated (become activated ) [44]. Indirect evidence of the mast cell as an active participant in the pathogenesis of IC comes from increased levels of histamine found in the bladder walls of patients with IC [45] and increased urinary excretion of 1,4-methyl-imidazole-acetic-acid, a histamine metabolite [46,47], by these same patients. Although little work has been conducted to determine the role of the mast cell in MCPPS IIIA, case reports such as that submitted by Theoharides et al. [48] suggest that mastocytosis and elevated urinary histamine levels might be observed in some patients with prostatitis. This correlates well with an estrogen-induced model of prostatitis where increased numbers of degranulated mast cells were noted [49]. Increasing mast cell degranulation appeared in the previously discussed rat model of spontaneous prostatitis with prostatitis progression [37]. Autoimmunity The interest in autoimmunity as a possible cause of IC dates back to 1938, when Fister [50] noted similarities between IC and systemic lupus erythematosus. Indeed, IC has many of the features of an autoimmune disease: symptom chronicity with exacerbations and remissions; frequent organ-specific mononuclear cell infiltrates; the lack of a clearly defined pathogen; occasional clinical response to steroids or other immunosuppressants [51]; the high prevalence of antinuclear antibodies; and associations with well-described autoimmune syndromes. Further studies investigating the role of autoimmunity in IC are far from conclusive and often conflicting. High levels of bladderspecific autoantigens have been identified in some patients [52], however, this has not been a consistent finding [53,54]. In fact, some investigators suggest that this phenomenon is simply an indirect response to local cellular damage [38]. The same type of controversy exists for autoimmunity in the patient with MCPPS. Evidence suggests that autoimmunity may be responsible for symptoms in some patients suffering from MCPPS III. Alexander et al. [55] demonstrated that three of 10 men with MCPPS had an autoimmune response to prostatic proteins, as evidenced by a T lymphocytic response to seminal plasma. Although some patients with MCPPS appear to have evidence of autoimmunity-related pathogenesis, autoimmunity may also be present in conditions as common as benign prostatic hyperplasia (BPH) [56]. Similarities in Presentation Between Interstitial Cystitis and Male Chronic Pelvic Pain Syndrome A significant overlap of presenting signs and symptoms exists between IC and MCPPS. In some instances, this overlap can be so impressive as to make the distinction between these two entities quite blurry. Additionally, confusion and misdiagnosis between IC, MCPPS category IIIA, MCPPS category II (chronic bacterial prostatitis), and BPH [57] is very common. In 1969, Hanash and Pool [58] reported that 55% of 123 male patients had undergone at least one transurethral resection of the prostate (TURP) before being diagnosed with IC. In 1977, DeJuana and Everett [59] reported on 11 male patients with IC, five of whom underwent TURP and two who underwent open prostatectomy prior to their final diagnosis. Incorrect surgical procedures are performed less frequently today, most likely because of an increased awareness of the potential for sensory dysfunction and a more widespread use of urodynamic evaluation. Nevertheless, the diagnosis of IC can be confounded by the fact that only 7% of patients initially present with the entire complement of symptoms that they will ultimately develop. Driscoll and Teichman [60 ] reported that the median time for total symptom manifestation was 2 years, and not all patients manifest the entire spectrum of described complaints. It is quite likely that this same progression of symptoms is occurring in the patient with MCPPS, a condition whose symptoms may afflict up to 9.7% of the total community [61]. Typical symptoms of IC include urinary frequency, urinary urgency, and pelvic pain. Pain is typically worsened with bladder filling. Urethral syndrome, a condition thought by many to be an IC variant, is often diagnosed when dysuria is associated with other irritative voiding symptoms. Common complaints associated with prostatitis parallel those of IC, but may also include dysuria, perineal or penile pain, and pain with ejaculation. Pain with bladder filling, a classic feature of IC, is described in 45% of patients with MCPPS. This is consistent with a
4 316 Prostatitis (Urinary Tract Infections) report by Mayo et al. [62] who found bladder hypersensitivity in 30% of patients with MCPPS. Detrusor instability is relatively uncommon in the patient with IC, present between 0% and 14.6% of patients [63 66]: this condition is seen in 3% of our patient population. A high prevalence of instability (30%) was noted in only one study that selected out patients with relatively severe inflammatory disease [67]. Although few large studies are available for review, bladder instability like IC appears to be uncommon in the patient with MCPPS [62]. A common complaint among patients with IC and MCPPS is that of urinary hesitancy. The National IC Database Study noted this symptom in 78% of patients [66]. This, in addition to complaints of poor urinary flow rates, constipation, dyspareunia, and generalized pelvic pain, have been attributed to associated pelvic floor pseudodyssynergia or spasm, broadly termed pelvic floor dysfunction [65,68,69,70 ]. We retrospectively reviewed the charts of 100 consecutive female patients meeting NIDDK criteria for IC, noting other associated complaints including decreased force of the urinary stream (75%), urinary hesitancy (75%), a sensation of incomplete voiding (73%), the need to strain with urination (70%), and dyspareunia (45%). Likewise, voiding dysfunction in the patient with MCPPS appears to be quite common. Although Mayo et al. [62] found little evidence of pseudodyssynergia in MCPPS, most literature has demonstrated a high incidence of bladder neck and/or pelvic floor spasm associated with this condition, particularly within the MCPPS IIIB variant (prostatodynia) [71,72,73 ]. This similarity between MCPPS IIIB and IC is seen again in studies where both groups have been found to develop significant glomerulations (petechial hemorrhages of the bladder surface) upon bladder hydrodistention [74]. Conclusions In 1987, Messing [75] suggested that many men who initially received a diagnosis of nonbacterial prostatitis or prostatodynia might actually have had IC. This thought was based upon often striking similarities in clinical presentation between these syndromes. Supporting this hypotheses, other investigators noted the frequent misdiagnosis of IC as MCPPS [73,60 ]. Although no direct comparative studies have been performed, further investigations detailing similar epidemiology, pathophysiology, and even response to various therapies for IC and MCPPS begs the question whether these two syndromes are in fact different points in a spectrum of the same disease. References and Recommended Reading Papers of particular interest, published recently, have been highlighted as: Of importance Of major importance 1. Curhan GC, Speizer FE, Hunter DJ, et al.: Epidemiology of interstitial cystitis: a population based study. J Urol 1999, 161: This study demonstrates a strikingly high prevalance of medical conditions that have historically received little investigation. 2. Collins MM, Stafford RS, O Leary MP, et al.: How common is prostatitis? A national survey of physician visits. J Urol 1998, 159: This study also demonstrates a strikingly high prevalance of medical conditions that have historically received little investigation. 3. Collins MM, Meigs JB, Barry MJ, et al.: Prevalence and correlates of prostatitis in the health professionals follow-up study cohort. J Urol 2002, 167: Like the preceding two studies, this study demonstrates a strikingly high prevalence of medical conditions that have historically received little investigative attention. The amassed data of these three studies have fueled significant clinical and political support for these conditions. 4. Held PJ, Hanno PM, Wein AJ, et al.: Epidemiology of interstitial cystitis. In Interstitial Cystitis. Edited by Hanno PM, Staskin DR, Krane RJ, Wein AJ. New York: Springer-Verlag; 1990: Koziol JA, Clark DC, Gittes RF, Tan EM: The natural history of interstitial cystitis: a survey of 374 patients. J Urol 1993, 149: Simon LJ, Landis JR, Erickson DR, et al.: The interstitial cystitis data base study: concepts and preliminary baseline descriptive statistics. Urology 1997, 49(Suppl 5A): Wenninger K, Heiman JR, Rothman I, et al.: Sickness impact of chronic nonbacterial prostatitis and its correlates. J Urol 1996, 155: McNaughton CM, Pontari MA, O Leary MP, et al.: Quality of life is impaired in men with chronic prostatitis: the Chronic Prostatitis Collaborative Research Network. J Gen Int Med 2001, 16: An excellent study demonstrating the profound effects of prostatitis upon health-related quality-of-life issues. 9. Jarvi K, Wang W, Korithoski B, et al.: Identification of unusual bacteria in the semen and urine of men with NIH type III prostatitis. J Urol 2001, 165 (Suppl): Hochreiter WW, Duncan JL, Schaeffer AJ: Evaluation of the bacterial flora of the prostate using a 16S rrna gene based polymerase chain reaction. J Urol 2000, 163: Shortliffe LM, Sellers RG, Schachter J: The characterization of nonbacterial prostatitis: search for an etiology. J Urol 1992, 148: Berger RE, Krieger JN, Rothman I, et al.: Bacteria in the prostate tissue of men with idiopathic prostatic inflammation. J Urol 1997, 157: Krieger JN, Riley DE, Vesella RL, et al.: Bacterial DNA sequences in prostatic tissue from patients with prostate cancer and chronic prostatitis. J Urol 2000, 164: Shoskes DA, Shahed AR: Detection of bacterial signal by 16S rrna polymerase chain reaction in expressed prostatic secretions predicts response to antibiotic therapy in men with chronic pelvic pain syndrome. Tech Urol 2000, 6: Nickel JC: Effective office management of chronic prostatitis. Urol Clin North Am 1998, 25: An excellent review detailing practical management approaches for the patient with MCPPS.
5 Similarities Between IC and Male CPPS Moldwin Nickel JC, Downey J, Johnston B, et al.: Predictors of patient response to antibiotic therapy for the chronic prostatitis/ chronic pelvic pain syndrome: a prospective multicenter trial. J Urol 2001, 165: Keay S, Zhang CO, Baldwin BR, Alexander RB: Polymerase chain reaction amplification of bacterial 16s rrna genes in prostate biopsies from men without chronic prostatitis. Urology 1999, 53: Duncan JL, Schaeffer AJ: Do infectious agents cause interstitial cystitis? Urology 1997, 49(Suppl 5A): Keay S, Zhang CO, Baldwin BR, et al.: Polymerase chain reaction amplification of bacterial 16S rrna genes in interstitial cystitis and control patient bladder biopsies. J Urol 1998, 159: Warren JW: Interstitial cystitis as an infectious disease. Urol Clin North Am 1994, 21: Potts JM, Ward AM, Rackley RR: Association of chronic urinary symptoms in women and ureaplasma urealyticum. Urology 2000, 55: Elgavish A, Robert B, Lloyd K, et al.: Evidence for a mechanism of bacterial toxin action that may lead to the onset of urothelial injury in the interstitial cystitis bladder. J Urol 1995, 153:329A. 23. Moskowitz M, Byrne DS, Callahan HJ, et al.: Decreased expression of a glycoproteins component of bladder surface mucin (GP1) in interstitial cystitis. J Urol 1994, 151: Sant GR, Ucci AA, Jr, Alroy J: Bladder surface glycosaminoglycans (GAGs) in interstitial cystitis. J Urol 1986, 135:175A. 25. Lilly JD, Parsons CL: Bladder surface glycosaminoglycans is a human epithelial permeability factor. Surg Gynecol Obstet 1990, 171: Press SM, Moldwin R, Kushner L, et al.: Decreased expression of GP-51 glycosaminoglycan in cats afflicted with feline interstitial cystitis. J Urol 1995, 153:288A. 27. McNeal JE: Normal histology of the prostate. Am J Surg Pathol 1988, 12: Jones EG, Harper ME: Studies on the proliferation, secretory activities, and epidermal growth factor expression in benign prostatic hyperplasia explant cultures. Prostate 1992, 20: Kirby RS, Lowe D, Bultitude MI, Shuttleworth KE: Intra-prostatic urinary reflux: an aetiological factor in abacterial prostatitis. Br J Urol 1982, 54: This classic article details the common reflux of carbon particles into the prostatic ducts during TURP. Reflux of urine could potentiate the development of infection or possibly cause symptoms by enabling urine to elicit a local inflammatory response. 30. Parsons CL: Potassium sensitivity test. Tech Urol 1996, 2: Nickel JC, Johnston B, Downey J, et al.: Pentosan polysulfate therapy for chronic nonbacterial prostatitis (chronic pelvic pain syndrome category IIIA): a prospective multicenter clinical trial. Urology 2000, 56: Hohenfellner M, Nunues L, Schmidt RA, et al.: Interstitial cystitis: increased sympathetic innervation and related neuropeptide synthesis. J Urol 1992, 147: Pang X, Marchand J, Sant GR, et al.: Increased number of substance P positive fibers in interstitial cystitis. Br J Urol 1995, 75: Chen Y, Varghese R, Chiu P, et al.: Urinary substance P is elevated in women with interstitial cystitis. J Urol 1999, 161: Shirley SW, Stewart BH, Mirelman S: Dimethyl sulfoxide in the treatment of inflammatory genitourinary disorders. Urology 1978, 11: Kushner L, Chiu PY, Brettschneider N, et al.: Urinary substance P concentration correlates with urinary frequency and urgency in interstitial cystitis patients treated with intravesical dimethyl sulfoxide and not intravesical anesthetic cocktail. Urology 2001, 57(Suppl 1): Keith IM, Jin J, Neal D, Jr, et al.: Cell relationship in a Wistar rat model of spontaneous prostatitis. J Urol 2001, 166: Elbadawi A: Interstitial cystitis: a critique of current concepts with a new proposal for pathologic diagnosis and pathogenesis. Urology 1997, 49(Supp 5A): Theoharides TC, Sant GR: Bladder mast cell activation in interstitial cystitis. Semin Urol 1991, 9: Lagunoff D, Martin TW, Read G: Agents that release histamine from mast cells. Ann Rev Pharmacol Toxicol 1983, 23: Spanos C, Pang X, Ligris K, et al.: Stress-induced bladder mast cell activation: implications for interstitial cystitis. J Urol 1997, 157: Feltis JT, Perez-Marrero R, Emerson LE: Increased mast cells of bladder in suspected cases of interstitial cystitis: possible disease marker. J Urol 1987, 138: Lynes WL, Flynn SD, Shortliffe LD, et al.: Mast cell involvement in interstitial cystitis. J Urol 1987, 138: Theoharides T, Duraisamy K, Sant G: Mast cell involvement in interstitial cystitis: a review of human and experimental evidence. Urology 2001, 57(Suppl 6A): Kastrup J, Hald T, Larsen S, et al.: Histamine content and mast cell count of detrusor muscle in patients with interstitial cystitis and other types of chronic cystitis. Br J Urol 1983, 55: Holm-Bentzen M, Sondergaard I, Hald T: Urinary excretion of a metabolite of histamine (1,4-methyl-imidazole-acetic-acid) in painful bladder disease. Br J Urol 1987, 59: El-Mansoury M, Boucher W, Sant GR, et al.: Increased urine histamine and methylhistamine in interstitial cystitis. J Urol 1994, 153: Theoharides TC, Flaris N, Cronin CT, et al.: Mast cell activation in sterile bladder and prostate inflammation. Int Arch Allergy Appl Immunol 1990, 92: Seethalakshmi L, Bala RS, Malhotra RK, et al.: 17 beta-estradiol induced prostatitis in the rat is an autoimmune disease. J Urol 1996, 156: Fister GM: Similarity of interstitial cystitis to lupus erythematosus. J Urol 1938, 40: Moran PA, Dwyer PL, Carey MP, et al.: Oral methotexate in the management of refractory interstitial cystitis. Aust N Z J Obstet Gynaecol 1999, 39: Silk MR: Bladder antibodies in interstitial cystitis. J Urol 1970, 103: Jokinen E, Alfthan S, Oravisto K: Antitissue autoantibodies in interstitial cystitis. Clin Exp Immunol 1972, 11: Anderson JB, Parivar F, Lee G, et al.: The enigma of interstitial cystitis: an autoimmune disease? Br J Urol 1989, 63: Alexander RB, Brady F, Ponniah S: Autoimmune prostatitis: evidence of T cell reactivity with normal prostastic proteins. Urology 1997, 50: Zisman A, Zisman E, Lindner A, et al.: Autoantibodies to prostate specific antigen in patients with benign prostatic hyperplasia. Urology 1995, 154: Collins MM, Stafford RS, O Leary MP, Barry MJ: Distinguishing chronic prostatitis and benign prostatic hyperplasia symptoms: results of a national survey of physician visits. Urology 1999, 53: Hanash KA, Pool TL: Interstitial cystitis in men. J Urol 1969, 102: DeJuana CP, Everett JC, Jr: Interstitial cystitis, experience and review of recent literature. Urology 1977, 10: Driscoll A, Teichman JMH: How do patients with interstitial cystitis present? J Urol 2001, 166: This investigation demonstrates that the symptoms of IC may progress and describes the chronology of progression. This often slow progression of symptoms may in part account for the frequent misdiagnosis of IC, particularly among the male population. 61. Nickel JC, Downey J, Hunter D, et al.: Prevalence of prostatitislike symptoms in a population based study using the National Institutes of Health chronic prostatitis symptom index. J Urol 2001, 165: Mayo ME, Ross SO, Krieger JN: Few patients with "chronic prostatitis" have significant bladder outlet obstruction. Urology 1998, 52:
6 318 Prostatitis (Urinary Tract Infections) 63. Siroky MB: Is it interstitial cystitis? Diagnostic distinctions in reduced bladder capacity. Contemp Urol 1994, 6: Hanno PM, Landis JR, Matthews-Cook Y, et al.: The diagnosis of interstitial cystitis revisited: lessons learned from the National Institutes of Health Interstitial Cystitis Database Study. J Urol 1999, 161: Schmidt RA, Vapnek JM: Pelvic floor behavior and interstitial cystitis. Sem Urol 1991, 9: Kirkemo A, Peabody M, Diokno AC, et al.: Associations among urodynamic findings and symptoms in women enrolled in the Interstitial Cystitis Database (ICDB) Study. Urology 1997, 49(Suppl 5A): Holm-Bentzen M, Jacobsen F, Nerstrøm B, et al.: Painful bladder disease: clinical and pathoanatomical differences in 115 patients. J Urol 1987, 138: Moldwin RM, Mendelowitz F: Pelvic floor dysfunction and interstitial cystitis. Paper presented at the Research Symposium on Interstitial Cystitis, A Century of Awareness, A Decade of Progress. Orlando, FL. October 8 9, Lilius HG, Oravisto KJ, Valtonen EJ: Origin of pain in interstitial cystitis. Scand J Urol Nephrol 1973, 7: Weiss JM: Pelvic floor myofascial trigger points: manual therapy for interstitial cystitis and the urgency-frequency syndrome. J Urol 2001, 166: An excellent article detailing the frequent coexistence of pelvic floor dysfunction and IC. The article details symptom improvement with simple manual therapy techniques. 71. Segura JW, Opitz JL, Greene LF: Prostatitis, prostatosis or pelvic floor muscle tension myalgia? J Urol 1979, 122: Siroky MB, Goldstein I, Krane RJ: Functional voiding disorders in men. J Urol 1981, 126: Forrest JB, Vo Q: Observations on the presentation, diagnosis, and treatment of interstitial cystitis in men. Urology 2001, 57(Suppl 6A): The symptoms of IC often overlap with those of prostatitis and BPH. This article suggests keeping the diagnosis of IC in the differential diagnosis when evaluating the patient with lower urinary tract symptoms. 74. Miller JL, Rothman I, Bavendam TG, Berger RE: Prostatodynia and interstitial cystitis: one and the same? Urology 1995, 45: Messing EM: The diagnosis of interstitial cystitis. Urology 1987, 29(Suppl 4):4 7.
In evaluating a patient with lower urinary tract symptoms (LUTS), urologists
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
DELAYED DIAGNOSIS. Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >60%
 DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence?
 Rev Article CHRONIC PROSTATITIS THERAPY NICKEL The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence? J. CURTIS NICKEL Department of Urology,
Rev Article CHRONIC PROSTATITIS THERAPY NICKEL The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence? J. CURTIS NICKEL Department of Urology,
In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective?
 Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria. Michel Pontari IMMPACT-XX Meeting July 13, 2017
 Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria Michel Pontari IMMPACT-XX Meeting July 13, 2017 NIDDK Classification of Prostatitis 1 Type I: Acute Bacterial
Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria Michel Pontari IMMPACT-XX Meeting July 13, 2017 NIDDK Classification of Prostatitis 1 Type I: Acute Bacterial
Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation
 Client HMSA: PQSR 2009 Measure Title DIAGNOSTIC WORKUP OF CHRONIC PROSTATITIS Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation B Organizations Providing
Client HMSA: PQSR 2009 Measure Title DIAGNOSTIC WORKUP OF CHRONIC PROSTATITIS Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation B Organizations Providing
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
The four categories of prostatitis: A practical approach to treatment
 MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY The four categories of prostatitis: A practical approach to treatment JEANNETTE M. POTTS, MD Department of Urology,
MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY The four categories of prostatitis: A practical approach to treatment JEANNETTE M. POTTS, MD Department of Urology,
Clinical Significance of National Institutes of Health Classification in Patients With Chronic Prostatitis/Chronic Pelvic Pain Syndrome
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.276 Original Article - Infection/Inflammation http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.276&domain=pdf&date_stamp=2014-04-17
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.276 Original Article - Infection/Inflammation http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.276&domain=pdf&date_stamp=2014-04-17
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Rawal Medical Journal
 Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Original Article Role of alpha blockers
Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Original Article Role of alpha blockers
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
CHRONIC PELVIC PAIN SYNDROME. Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary
 CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
BPS/IC: evolution of definition and prevalence
 BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
Interstitial Cystitis. Dr. Gerard Testa
 Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC Department of Surgery, Division of Urology,
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC Department of Surgery, Division of Urology,
1 Olsson CA, Willscher MK, Austen G Jr, Siroky MB and Krane RJ. Management of prostatic fistulas. Urol Surv 1976;25:135.
 Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
J.C. NICKEL, J. DOWNEY, M.A. PONTARI*, D.A. SHOSKES
 Original Article FINASTERIDE TREATMENT OF CHRONIC PELVIC PAIN SYNDROME J.C. NICKEL et al. A randomized placebo-controlled multicentre study to evaluate the safety and efficacy of finasteride for male chronic
Original Article FINASTERIDE TREATMENT OF CHRONIC PELVIC PAIN SYNDROME J.C. NICKEL et al. A randomized placebo-controlled multicentre study to evaluate the safety and efficacy of finasteride for male chronic
Abstract. Key words Trial without catheter, Acute urinary retention, Benign prostatic hyperplasia, Introduction
 The role of sustained-released alfuzosin in the treatment of acute urinary retention Mohamed Fawzi Ahmed. Department of Surgery, Ninevah College of Medicine, University of Mosul. Abstract To see whether
The role of sustained-released alfuzosin in the treatment of acute urinary retention Mohamed Fawzi Ahmed. Department of Surgery, Ninevah College of Medicine, University of Mosul. Abstract To see whether
The term prostatitis refers to an inflammatory condition of the prostate gland in men.
 Edith Cavell Hospital Department of Urology Prostatitis What is prostatitis The term prostatitis refers to an inflammatory condition of the prostate gland in men. What types of prostatitis are there? Prostatitis
Edith Cavell Hospital Department of Urology Prostatitis What is prostatitis The term prostatitis refers to an inflammatory condition of the prostate gland in men. What types of prostatitis are there? Prostatitis
Bladder pain syndrome / Interstitial cystitis
 Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
PROSTATE BIOPSY CULTURE FINDINGS OF MEN WITH CHRONIC PELVIC PAIN SYNDROME DO NOT DIFFER FROM THOSE OF HEALTHY CONTROLS
 0022-5347/03/1692-0584/0 Vol. 169, 584 588, February 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000045673.02542.7a PROSTATE BIOPSY
0022-5347/03/1692-0584/0 Vol. 169, 584 588, February 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000045673.02542.7a PROSTATE BIOPSY
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
BJUI. Mini Reviews. Urological Oncology. Lower Urinary Tract. Sexual Medicine. Laparoscopic and Robotic Urology. Reconstructive and Paediatric Urology
 BJUI BJU INTERNATIONAL Mini Reviews Urological Oncology Sexual Medicine Lower Urinary Tract Laparoscopic and Robotic Urology Reconstructive and Paediatric Urology Investigative Urology 8 The Authors Original
BJUI BJU INTERNATIONAL Mini Reviews Urological Oncology Sexual Medicine Lower Urinary Tract Laparoscopic and Robotic Urology Reconstructive and Paediatric Urology Investigative Urology 8 The Authors Original
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Symptom Improvement and Transrectal Ultrasound-Documented Reduction of Prostate Size after Repetitive Prostatic Massage and Antimicrobial Therapy
 Symptom Improvement and Transrectal Ultrasound-Documented Reduction of Prostate Size after Repetitive Prostatic Massage and Antimicrobial Therapy Hennenfent BR, Garcia BS, Feliciano Jr. AE: Symptom Improvement
Symptom Improvement and Transrectal Ultrasound-Documented Reduction of Prostate Size after Repetitive Prostatic Massage and Antimicrobial Therapy Hennenfent BR, Garcia BS, Feliciano Jr. AE: Symptom Improvement
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy
 European Urology European Urology 44 (2003) 106 110 Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy Petr Hruz, Hansjörg Danuser, Urs E. Studer, Werner W. Hochreiter
European Urology European Urology 44 (2003) 106 110 Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy Petr Hruz, Hansjörg Danuser, Urs E. Studer, Werner W. Hochreiter
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Chronic nonbacterial prostatitis or chronic pelvic
 A REVIEW OF THE DEVELOPMENT AND VALIDATION OF THE NATIONAL INSTITUTES OF HEALTH CHRONIC PROSTATITIS SYMPTOM INDEX MARK S. LITWIN ABSTRACT Chronic nonbacterial prostatitis or chronic pelvic pain syndrome
A REVIEW OF THE DEVELOPMENT AND VALIDATION OF THE NATIONAL INSTITUTES OF HEALTH CHRONIC PROSTATITIS SYMPTOM INDEX MARK S. LITWIN ABSTRACT Chronic nonbacterial prostatitis or chronic pelvic pain syndrome
A Review on Interstitial Cystitis Syndrome (ICS)
 31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
ISSN: (Print) (Online) Journal homepage:
 Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 CHANGE IN INTERNATIONAL PROSTATE SYMPTOM SCORE AFTER TRANSURETHRAL
Archives of Andrology Journal of Reproductive Systems ISSN: 0148-5016 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iaan19 CHANGE IN INTERNATIONAL PROSTATE SYMPTOM SCORE AFTER TRANSURETHRAL
CURRENT CONTROVERSIES THAT ADVERSELY AFFECT INTERSTITIAL CYSTITIS PATIENTS VICKI RATNER
 CURRENT CONTROVERSIES THAT ADVERSELY AFFECT INTERSTITIAL CYSTITIS PATIENTS VICKI RATNER ABSTRACT Interstitial cystitis (IC) remains a diagnosis of exclusion, based on the symptoms of urinary urgency, frequency,
CURRENT CONTROVERSIES THAT ADVERSELY AFFECT INTERSTITIAL CYSTITIS PATIENTS VICKI RATNER ABSTRACT Interstitial cystitis (IC) remains a diagnosis of exclusion, based on the symptoms of urinary urgency, frequency,
Prostate Health PHARMACIST VIEW
 Prostate Health PHARMACIST VIEW Prostate Definition Prostate is a gland made of fibromuscular tissue. It is about 4 cm and surrounds the neck of the bladder and the urethra. It produces seminal fluid.
Prostate Health PHARMACIST VIEW Prostate Definition Prostate is a gland made of fibromuscular tissue. It is about 4 cm and surrounds the neck of the bladder and the urethra. It produces seminal fluid.
Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy?
 Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
WHAT IS INTERSTITIAL CYSTITIS?
 Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Some prostatic diseases
 Some prostatic diseases Benign Prostatic Hyperplasia (Nodular Hyperplasia) Extremely common Present in a significant number of men by the age of 40 & its frequency rises progressively with age, reaching
Some prostatic diseases Benign Prostatic Hyperplasia (Nodular Hyperplasia) Extremely common Present in a significant number of men by the age of 40 & its frequency rises progressively with age, reaching
UroToday International Journal. Volume 2 - October 2009
 UroToday International Journal Robert J. Evans, 1 Jeffrey Proctor, 2 Robert M. Moldwin 3 1 Alliance Urology Specialists, Greensboro, NC; 2 Georgia Urology, Cartersville, GA; 3 The Arthur Smith Institute
UroToday International Journal Robert J. Evans, 1 Jeffrey Proctor, 2 Robert M. Moldwin 3 1 Alliance Urology Specialists, Greensboro, NC; 2 Georgia Urology, Cartersville, GA; 3 The Arthur Smith Institute
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Mini-Reviews. Interstitial Cystitis in Adolescents and Children: A Review
 J Pediatr Adolesc Gynecol (2004) 17:7 11 Mini-Reviews Interstitial Cystitis in Adolescents and Children: A Review T.F. Mattox, MD, FACOG Department of Obstetrics and Gynecology, Division of Urogynecology,
J Pediatr Adolesc Gynecol (2004) 17:7 11 Mini-Reviews Interstitial Cystitis in Adolescents and Children: A Review T.F. Mattox, MD, FACOG Department of Obstetrics and Gynecology, Division of Urogynecology,
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
INTERNATIONAL PROSTATE SYMPTOM SCORE IPSS - AUA AS DISCRIMINAT SCALE IN 400 MALE PATIENTS WITH LOWER URINARY TRACT SYMPTOMS (LUTS)
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology IPSS IN MALE PATIENTS WITH LUTS Vol. 30 (2): 135-141, March - April, 2004 INTERNATIONAL PROSTATE SYMPTOM
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology IPSS IN MALE PATIENTS WITH LUTS Vol. 30 (2): 135-141, March - April, 2004 INTERNATIONAL PROSTATE SYMPTOM
Infection/Inflammation. A Randomized, Double-Blind, Placebo Controlled Trial of Adalimumab for Interstitial Cystitis/Bladder Pain Syndrome
 Infection/Inflammation A Randomized, Double-Blind, Placebo Controlled Trial of Adalimumab for Interstitial Cystitis/Bladder Pain Syndrome Philip C. Bosch*, From the Department of Urology, Palomar Medical
Infection/Inflammation A Randomized, Double-Blind, Placebo Controlled Trial of Adalimumab for Interstitial Cystitis/Bladder Pain Syndrome Philip C. Bosch*, From the Department of Urology, Palomar Medical
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
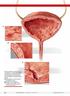 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China
 DOI: 10.1111/j.1745-7262.2008.00416.x. Clinical Experience. Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China Long-Fei Liu 1, Jin-Rui Yang 1, David A.Ginsberg
DOI: 10.1111/j.1745-7262.2008.00416.x. Clinical Experience. Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China Long-Fei Liu 1, Jin-Rui Yang 1, David A.Ginsberg
RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA
 American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
A SURVEY ON LOWER URINARY TRACT SYMPTOMS (LUTS) AMONG PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA (BPH) IN HOSPITAL UNIVERSITI SAINS MALAYSIA (HUSM)
 Malaysian Journal of Medical Sciences, Vol. 14, No. 2, July 2007 (67-71) SHORT COMMUNICATION A SURVEY ON LOWER URINARY TRACT SYMPTOMS (LUTS) AMONG PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA (BPH) IN HOSPITAL
Malaysian Journal of Medical Sciences, Vol. 14, No. 2, July 2007 (67-71) SHORT COMMUNICATION A SURVEY ON LOWER URINARY TRACT SYMPTOMS (LUTS) AMONG PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA (BPH) IN HOSPITAL
Review of treatments for interstitial cystitis
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy
 Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA
 PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA E.O. Stakhovsky, PhD, MD, Professor, Head of the Scientific and Research Department of Plastic and Reconstructive Oncourology,
PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA E.O. Stakhovsky, PhD, MD, Professor, Head of the Scientific and Research Department of Plastic and Reconstructive Oncourology,
Interstitial cystitis: bladder pain and beyond
 Interstitial cystitis: bladder pain and beyond Review 1. Introduction 2. Methods 3. Presentation 4. Other invasive approaches 5. Conclusion 6. Expert opinion Theoharis C Theoharides, Kristine Whitmore,
Interstitial cystitis: bladder pain and beyond Review 1. Introduction 2. Methods 3. Presentation 4. Other invasive approaches 5. Conclusion 6. Expert opinion Theoharis C Theoharides, Kristine Whitmore,
Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012
 Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012 J. Curtis Nickel Professor of Urology, Queen s University Canada CIHR Canada Research
Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012 J. Curtis Nickel Professor of Urology, Queen s University Canada CIHR Canada Research
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007)
 4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
Benign Prostatic Hyperplasia (BPH):
 Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
Benign Prostatic Hyperplasia (BPH): Evidence Based Guidelines for Primary Care Providers Jeanne Martin, DNP, ANP-BC Objectives 1. Understand the pathophysiology and prevalence of BPH 2. Select the appropriate
INTRODUCTION. Original Article - Lower Urinary Tract Dysfunction. Aram Kim 1, Kyeong-Ok Hoe 2, Jung Hyun Shin 2, Myung-Soo Choo 2 1
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Proof of Concept Trial of Tanezumab for the Treatment of Symptoms Associated With Interstitial Cystitis
 Proof of Concept Trial of Tanezumab for the Treatment of Symptoms Associated With Interstitial Cystitis R. J. Evans,*, R. M. Moldwin, N. Cossons, A. Darekar, I. W. Mills and D. Scholfield From the Department
Proof of Concept Trial of Tanezumab for the Treatment of Symptoms Associated With Interstitial Cystitis R. J. Evans,*, R. M. Moldwin, N. Cossons, A. Darekar, I. W. Mills and D. Scholfield From the Department
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital
 LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Addendum 1: International Consultation
 Reprinted with Permission of the International Consultation on Urological Diseases and the International Continence Society Hanno PM, Cervigni M, Dinis P, Lin A, Nickel JC, Nordling J, van Ophoven A, Ueda
Reprinted with Permission of the International Consultation on Urological Diseases and the International Continence Society Hanno PM, Cervigni M, Dinis P, Lin A, Nickel JC, Nordling J, van Ophoven A, Ueda
MODULE 5: HEMATURIA LEARNING OBJECTIVES DEFINITION. KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer
 MODULE 5: HEMATURIA KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer LEARNING OBJECTIVES At the end of this clerkship, the learner will be able to: 1. Define microscopic hematuria.
MODULE 5: HEMATURIA KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer LEARNING OBJECTIVES At the end of this clerkship, the learner will be able to: 1. Define microscopic hematuria.
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
DOWNLOAD OR READ : URINARY ANALYSIS AND DIAGNOSIS BY MICROSCOPICAL AND CHEMICAL EXAMINATION CLASSIC REPRINT PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : URINARY ANALYSIS AND DIAGNOSIS BY MICROSCOPICAL AND CHEMICAL EXAMINATION CLASSIC REPRINT PDF EBOOK EPUB MOBI Page 1 Page 2 urinary analysis and diagnosis pdf ORIGINAL REPORT COMPARISON
DOWNLOAD OR READ : URINARY ANALYSIS AND DIAGNOSIS BY MICROSCOPICAL AND CHEMICAL EXAMINATION CLASSIC REPRINT PDF EBOOK EPUB MOBI Page 1 Page 2 urinary analysis and diagnosis pdf ORIGINAL REPORT COMPARISON
The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III
 European Urology European Urology 47 (2005) 607 611 The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III Erik B. Cornel a, *, Ernst P. van Haarst b, Ria W.M. Browning-Groote
European Urology European Urology 47 (2005) 607 611 The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III Erik B. Cornel a, *, Ernst P. van Haarst b, Ria W.M. Browning-Groote
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department Outpatients
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.5.330 Voiding Dysfunction The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.5.330 Voiding Dysfunction The Prevalence and Characteristic Differences in Prostatic Calcification between Health Promotion Center and Urology Department
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Interstitial cystitis
 Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Interstitial Cystitis:
 Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study
 Singapore Med J 2002 Vol 43(4) : 189-193 O r i g i n a l A r t i c l e Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study J K Tan, D J C Png, L C H Liew, M K Li, M L Wong ABSTRACT
Singapore Med J 2002 Vol 43(4) : 189-193 O r i g i n a l A r t i c l e Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study J K Tan, D J C Png, L C H Liew, M K Li, M L Wong ABSTRACT
Asociación Mexicana de Médicos Veterinarios Especialistas en Pequeñas Especies
 Asociación Mexicana de Médicos Veterinarios Especialistas en Pequeñas Especies XXXI CONGRESO NACIONAL DE LA ASOCIACIÓN MEXICANA DE MÉDICOS VETERINARIOS ESPECIALISTAS EN PEQUEÑAS ESPECIES, A.C. DRA. IRENE
Asociación Mexicana de Médicos Veterinarios Especialistas en Pequeñas Especies XXXI CONGRESO NACIONAL DE LA ASOCIACIÓN MEXICANA DE MÉDICOS VETERINARIOS ESPECIALISTAS EN PEQUEÑAS ESPECIES, A.C. DRA. IRENE
Successful treatment of prostatitis syndrome with a mucolyticum
 1 This paper was submitted to : World Journal of Urology November 11, 2005 and not accepted See Comment in Laborjournal, 3, 14-18, 2007 Titel Successful treatment of prostatitis syndrome with a mucolyticum
1 This paper was submitted to : World Journal of Urology November 11, 2005 and not accepted See Comment in Laborjournal, 3, 14-18, 2007 Titel Successful treatment of prostatitis syndrome with a mucolyticum
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Dr. Krithika Doshi. Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical?
 Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical? Dr Kritika Doshi Introduction: Chronic pelvic and urogenital pain syndromes have recently been recognized as a
Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical? Dr Kritika Doshi Introduction: Chronic pelvic and urogenital pain syndromes have recently been recognized as a
Shrestha A, Chalise PR, Sharma UK, Gyawali PR, Shrestha GK, Joshi BR. Department of Surgery, TU Teaching Hospital, Maharajgunj, Kathmandu, Nepal
 Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Chapter 47 1/8/2018. Urinary System Disorders. Urinary Tract Infections. Treatment
 Chapter 47 Urinary System Disorders Urinary Tract Infections Urinary tract infections (UTIs) are common Infection in one area can involve the entire system Microbes enter through the urethra. Catheterization,
Chapter 47 Urinary System Disorders Urinary Tract Infections Urinary tract infections (UTIs) are common Infection in one area can involve the entire system Microbes enter through the urethra. Catheterization,
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
chronic pelvic pain Determination of IL-10 levels in syndrome patients Serdar Arısan *, Murat Can Kiremit, Turhan Çaşkurlu, Erbil Ergenekon
 (2): 87-91, 2008 istanbul Kultur University, Printed in Turkey www.advmolbiol.org Determination of IL-10 levels in syndrome patients Serdar Arısan *, Murat Can Kiremit, Turhan Çaşkurlu, Erbil Ergenekon
(2): 87-91, 2008 istanbul Kultur University, Printed in Turkey www.advmolbiol.org Determination of IL-10 levels in syndrome patients Serdar Arısan *, Murat Can Kiremit, Turhan Çaşkurlu, Erbil Ergenekon
Prostate Gland Disorders
 Prostate Gland Disorders THE PROSTATE GLAND A male s prostate gland is located in the floor of the pelvis surrounding the urethra between the bladder and the penis. The prostate is positioned immediately
Prostate Gland Disorders THE PROSTATE GLAND A male s prostate gland is located in the floor of the pelvis surrounding the urethra between the bladder and the penis. The prostate is positioned immediately
Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome
 CHRONIC THE IRAQI POSTGRADUATE CYSTITIS /PAINFUL MEDICAL BLADDER JOURNAL SYNDROME VOL., NO., Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome Issam
CHRONIC THE IRAQI POSTGRADUATE CYSTITIS /PAINFUL MEDICAL BLADDER JOURNAL SYNDROME VOL., NO., Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome Issam
Excessive Antibiotic Use in Men with Prostatitis
 CLINICAL RESEARCH STUDY Excessive Antibiotic Use in Men with Prostatitis Brent C. Taylor, PhD, MPH, a,b Siamak Noorbaloochi, PhD, a,b Mary McNaughton-Collins, MD, MPH, c Christopher S. Saigal, MD, MPH,
CLINICAL RESEARCH STUDY Excessive Antibiotic Use in Men with Prostatitis Brent C. Taylor, PhD, MPH, a,b Siamak Noorbaloochi, PhD, a,b Mary McNaughton-Collins, MD, MPH, c Christopher S. Saigal, MD, MPH,
Graminex G63 Flower Pollen Extract for Benign Prostatic Hyperplasia in Men
 Made in USA WHITE PAPER Graminex G63 Flower Pollen Extract Table of Contents Benign Prostatic Hyperplasia 2 Alternative Medicine 2 Chemical Composition 3 Modes of Action 3 Efficacy 4 Dosage 5 Conclusion
Made in USA WHITE PAPER Graminex G63 Flower Pollen Extract Table of Contents Benign Prostatic Hyperplasia 2 Alternative Medicine 2 Chemical Composition 3 Modes of Action 3 Efficacy 4 Dosage 5 Conclusion
INJ. Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory Agents in the Treatment of Chronic Pelvic Pain Syndrome
 Original Article Int Neurourol J 2011;15:92-96 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory
Original Article Int Neurourol J 2011;15:92-96 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
CAnnually, about 3 million patient visits to doctors in the
 UDC 1.2 002.2:15.032.2 ACTUAL TOPICS The modern approach to intravesical therapy of chronic cystitis O.D. Nikitin Bogomolets National Medical University Kyiv The difficulty of treating patients with chronic
UDC 1.2 002.2:15.032.2 ACTUAL TOPICS The modern approach to intravesical therapy of chronic cystitis O.D. Nikitin Bogomolets National Medical University Kyiv The difficulty of treating patients with chronic
Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer
 Bladder Cancer 3 (2017) 45 49 DOI 10.3233/BLC-160068 IOS Press Research Report 45 Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer Richard S. Matulewicz a,b,, John Oliver DeLancey
Bladder Cancer 3 (2017) 45 49 DOI 10.3233/BLC-160068 IOS Press Research Report 45 Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer Richard S. Matulewicz a,b,, John Oliver DeLancey
Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela
 Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela Microbiology Department Medical Faculty, University of Indonesia Urinary Tract Infection
Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela Microbiology Department Medical Faculty, University of Indonesia Urinary Tract Infection
