TOTAL HIP REPLACEMENT Doug Thompson, MD PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with
|
|
|
- Aldous Rodgers
- 6 years ago
- Views:
Transcription
1 PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. An incision is made along the side or front of the hip, and a deeper incision is made longitudinally to expose the joint surfaces. The hip is dislocated, and the ball end of the thigh bone (ie femoral head) is cut near the base of the femoral neck, then reamed and shaped to accept a metal stem. The metal stem can be secured with cement or by press-fit and bone ingrowth. In most instances, I will use metal components with a porous coating to allow bone ingrowth, avoiding the potential problems with cement which can break down and create an abrasive which accelerates plastic wear and component loosening. However, bone quality and medical conditions can often require the stem to be cemented. The size of the metal stem is selected to provide the best pressfit inside the bony femoral canal and to maintain leg length and hip geometry as close as possible to normal. During this part of the procedure, bony spurs are also removed, and any excessive soft tissue is removed or released to allow optimum motion and eliminate deforming contractures or impingement. The cup socket of the hip is then reamed, and a metal cup is then secured into the hip socket. The choice of bearing material then determines the type of head and liner. In most instances a plastic liner will be secured inside the cup, and a large polished metal ball will impacted on the femoral stem. The plastic liner provides a similar function as normal cartilage In some instances, ie for metal-on-metal bearing surfaces, a polished metal liner will be secured inside the metal cup, and a large polished head impacted on the stem. A newer type of bearing surface, ie bipolar, allows a polished metal liner to be secured inside the metal cup, and a bipolar head composed of a polished metal ball pressed inside a larger plastic ball. The plastic pieces will slowly wear, but with the latest technological advancements, should last 20 years or more. With optimum positioning and size of the components, the risk of dislocation is reduced through proper soft tissue tension. A manual test of stability throughout its range of motion is used to assess stability and avoidance of impingement. An xray is used during surgery to make sure the components are positioned correctly. Prior to implantation of the components, the hip is thoroughly irrigated with antibiotic solution. After implantation of the components, the deep soft tissues are closed, the skin closed with a watertight suture, and an impermeable dressing applied to prevent secondary infection until the wound is healed. A drain may or may not be used.
2 POSTOPERATIVE CARE AND REHABILITATION Most people can expect to spend 3 days in the hospital, going home or to an inpatient rehabilitation facility on Thursday. During the acute hospital stay, you will participate in group physical therapy in the Joint Replacment gym on the orthopedic floor twice a day. Therapy will focus on on walking with a walker, exercises to maintain and improve the motion in your leg, and exercises to strengthen your leg muscles. It is important that you actively use your muscles to bend and straighten your knees while in bed to avoid stiffness. You will also be instructed to pump your ankles to exercise your calf muscles which also helps prevent blood clots in the legs. A medical doctor will provide management of your other medical problems while in the hospital. You will receive antibiotics, pain medications, laxatives, and blood thinners while in the hospital You will also continue with medications at home. We will give you prescriptions for these prior to your surgery date so that they are available once you get home. A case manager will visit with you in the hospital to arrange for your home equipment needs and facilitate your continued rehabilitation needs with either home health, outpatient physical therapy, or inpatient rehabilitation at one of the rehabilitation hospitals or a skilled nursing facilities. Some insurances allow inpatient rehabilitation at either St Michaels Rehab Hospital or HealthSouth Rehab Hospital, but many do not. If you require continued inpatient rehabilitation and your insurance does not approve a rehabilitation hospital setting, we will arrange for inpatient care at a skilled nursing facility. We will determine your preferences and family support situation for rehab during your preoperative visit. If you are transferred to an inpatient rehabilitation facility (ie either rehab hospital or skilled nursing facility) you will continue to receive physical therapy about 3 hours per day. You can generally expect to stay an additional 7-14 days in the inpatient rehabilitation facility before being discharged home. If you go home, we will arrange home health to visit you 5 times a week (or whatever your insurance allows) or outpatient physical therapy at a facility near your home. We want you to leave the dressing in place until seen in the office at your two week followup visit. A waterproof dressing will be used to allow you to take a shower, but you are to avoid baths during the time the dressing is in place. The first couple of weeks are a little rough, but you will be walking farther with less pain every day. By your two week postoperative appointment in the office, you can generally expect to be close to transitioning from a walker to a cane. By 6 weeks postop, you can generally expect to be doing well, walking without a cane and without pain. By 3 months postop, you will generally be back to normal. Most patients, depending on their job duties, can be back to work by 4-6 weeks after surgery. Some jobs may require a longer time off.
3 PAIN CONTROL Multiple modalities for pain control to allow comfort, early ambulation, and shorter hospital stay. By controlling the pain immediately after surgery, less pain medication is needed in the following days because the pain pathway sensitization is delayed. Local Injection. To help control pain, a local anesthetic will be injected into the soft tissues inside the hip. Anti-Inflammatories. Unless contraindicated, you will be given IV NSAIDs and IV Tylenol before leaving the operating room, and the IV NSAIDs will continue during your stay in the hospital. By inhibiting the inflammatory response to surgery, the pain can be significantly reduced. Oral Pain Medication. For further breakthrough pain, oral narcotics will also be used. Typically, only low does hydrocodone is needed, and will be given on a scheduled basis unless you become nauseous or tired or confused. PCA pump. A patient controlled anesthetic (PCA) pump will be available for severe episodes of breakthrough pain. When the patient pushes a button, a small dose of narcotic will be pumped intravenously for fast pain control. The dose and interval of medicine are controlled. With the above pain modalities in use, the PCA pump use is seldom needed. The oral and IV narcotics can cause constipation and nausea. Laxatives will be given to minimize the effects of the narcotics on the bowels, and anti-nausea medicine will be given at the end of surgery and as needed thereafter.
4 RISKS AND PREVENTION In general, you can expect 95-97% chance that your surgery will do well without complications. However, there is a possibility of a complication despite all of the precautions we take. We take precaution to minimize the risk of complications, as detailed below (these are the most common complications, but there may be others): Medical Complications Your unique medical conditions are best known by your primary care physician and other medical subspecialists. Prior to surgery, we will obtain labs and send you to your primary care physician and other indicated subspecialists to evaluate your medical condition, determine the medical risks of surgery, and provide medical clearance for surgery. They will assess your risk of cardiopulmonary or other medical complications and develop a coordinated plan for your perioperative medical management to minimize those potential risks. They will help fine tune your medical condition in preparation for surgery. If your have diabetes, renal disease, rheumatalogical problems, pulmonary problems, or cardiovascular problems, your risk of complications is increased. It is important to keep your blood pressure under control during the perioperative period. If your blood pressure is too high, you can have a stroke in the perioperative period. You should take your blood pressure medications with just a sip of water on the morning of surgery. For diabetics, blood sugar may be managed with a sliding scale insulin protocol. If you take methotrexate or TNFa antagonists, you should generally stop them one cycle before surgery and not restart them until after the wound is healed at the first postoperative visit to facilitate bone and soft tissue healing. Cardiac complications can occur despite preoperative evaluation and clearance, including myocardial infarction, congestive heart failure, arrythmia, and even death. A cardiologist evaluation and perioperative management will be used as indicated. Constipation or Bowel Immobility can develop after surgery and will be treated with laxatives and other means as needed. Urinary retention is common after surgery. You will have a foley catheter placed prior to surgery, and it will be discontinued typically on the first or second day after surgery. In some instances, it may have to stay in place longer. Anesthesia Complications Aspiration Pneumonia. To prevent aspiration of your stomach contents, please do not eat or drink anything other than your blood pressure medicines and a sip of water after midnight before surgery. Atelectasis. When you undergo general anesthesia, a machine will breath for you, inflating your lungs. When that inflation pressure is removed after surgery, a small amount of inflammation and fluid can collect in the small sacs in the lungs. It is important to drive that fluid away by breathing deeply every hour to avoid pneumonia and reduce postoperative fever. You will be given an incentive spirometer while in the hospital help with the deep breathing, and we will use oxygen and breathing treatments if needed. Your anesthesiologist will do a thorough evaluation of your medical condition and plan for your anesthesia requirements during your preoperative registration visit
5 at the hospital, and review that once again on the day of surgery. They can explain the options, recommendations, procedures, and risks in more detail. Infection Infection is a very serious problem that is taken seriously. The implants we place can get infected at the time of surgery or at any time after surgery from bloodborn bacteria from dental procedures, urinary tract infections, etc. If they get infected, it is often necessary to remove the components to treat the infection, and later reimplantation after the infection is cured. This is a disastrous condition which we want to avoid and take every precaution to try to prevent. Your teeth and mouth can be a source of infection at the time of surgery and at any time thereafter. We will evaluate your dental health and refer you to your dentist for any concerning dental issues and clearance prior to surgery if needed. Any dental issues must be resolved prior to a joint replacement, and surgery may be canceled if not resolved to our satisfaction. At any time after your joint replacement, it is important to take antibiotics prior to and following any dental procedures. If your dentist cannot provide prophylactic antibiotics, ask our office and we will prescribe them for you. Your nose can also be a source of bacteria that can cause infection. We will culture your nose and determine if difficult bacteria are present. We will also prescribe mupirocin antibiotic ointment which you will use 5 days prior to surgery to eradicate any nasal bacteria, particularly MSSA and MRSA. Your skin can carry a multitude of bacteria, including difficult to treat MRSA strains. You will be instructed to take a whole body bath or shower with Hibiclens antibacterial soap for 5 days prior to surgery, including the morning of surgery You will also be prepped upon arrival at the hospital on the day of surgery with Hibiclens. You will also be prepped again in the operating room and a sealant iodine barrier used to wrap around the operative site. Contamination during surgery can occur, but its risks are minimized by the use of clean spacesuit hoods, meticulous sterile technique, antibiotic irrigation, and IV antibiotics before, during, and after surgery for 24 hours. Secondary infection from a draining wound after surgery can also occur. To minimize this risk, we use a watertight suture closure on the skin and apply an impermeable dressing while in the operating room. That dressing provides a barrier to secondary infection and will stay in place until removed in our office at your 2 week followup appointment. We may also prescribe an oral antibiotic at the time of your preop visit to be taken at home after surgery. If you have an active urinary tract infection, it must be treated prior to surgery. We will collect a urine sample in our lab in preparation for surgery and treat accordingly. Steroids delay wound healing. We prefer that oral steroids be stopped or reduced below 7.5mg/day to avoid wound complications. Methotrexate and other rheumatological medications also delay healing and can lead to increased risk of secondary infection or immunosuppression of your own body s defense mechanism. Your should stop methotrexate preferably 7 days before surgery, and not restart until 2 weeks after surgery. Other medications
6 such as TNFa antagonists and SERMS should also be stopped at least one cycle prior to surgery. Blood Clots (DVT) and Pulmonary Embolism With reduced mobility after a joint replacement, you are at risk of developing a blood clot in your legs. If blood clots form in the deep veins of the legs (DVT), they can dislodge and travel to the lungs where they can cause a serious and possibly deadly condition called a pulmonary embolism. Therefore, it is very important to try to prevent a blood clot from forming. If you have had a DVT before, you are at increased risk of having one develop again, and we may recommend a filter be placed in your main vein to catch any clots before they reach your lungs. The best way to prevent a blood clot is to have you walk as quickly as possible after surgery, using the normal muscular pumping motion of your body to increase the flow in the veins. We will have physical therapy begin to work with you on the day of surgery if possible, and definitely on the first day after surgery to get you walking as quickly as possible. You will be instructed to also perform active motion exercises hourly while in bed, including toe curls, ankle pumps, and bending and straightening the knee. These motions simulate walking motion of the muscles, but without the weight. We will also implement passive means to help with blood clot prevention, including plexipulses or sequential compression devices, TED hose, and blood thinners. Plexipulses/SCDs are attached to the feet/calves, and a pneumatic pump inflates them to create a pressure gradient and flow in the veins of your legs, preventing blood stagnation. You will have these on while in bed during your hospital stay. TED hose are compression stockings which help compress the legs and minimize the amount of blood that can pool in the veins of the legs. We will apply TED hose or a compression dressing during surgery, and you will wear them for 6 weeks after surgery. Unless contraindicated, we will use blood thinners starting the day after surgery and continue for 10 days, until you become increasingly mobile. If you already take coumadin prior to surgery, we will resume your coumadin after surgery. For others, we will give Lovenox injections or an oral medicine called Xarelto. We will give these medications to you while in the hospital, and give you a prescription for an additional week for home use during your preop visit. After completion of 10 days of blood thinner, we will have you take 81mg of aspirin each day for an additional month. Bleeding/Blood Loss You will lose blood during and after surgery which may require a blood transfusion based on your clinical symptoms. We may place a drain during surgery to collect blood and prevent a hematoma from forming. The drain, if used, will typically be discontinued on the first or second day after surgery. During surgery, we will lower your blood pressure (ie hypotensive anesthesia) to a minimize bleeding.
7 We use electrocautery during surgery to coagulate small vessels to minimize blood loss. During surgery we also use a local injection that contains epinephrine to constrict small vessels and minimize blood loss. Unless contraindicated, you will be given a dose at the start of surgery and at the end of surgery of a medicine which will help reduce bleeding. We will have you discontinue aspirin, Plavix or like drugs, coumadin, NSAIDS, and any other medication that can thin your blood 5-7 days prior to surgery. These will be resumed 10 days after surgery, or sooner based on your medical condition. We will check your blood level prior to surgery to see if you are anemic. If you are, we may start you on a medication called Procrit to improve your anemia prior to surgery. Although not typically needed, an optional predonation of blood by the patient a few weeks prior to surgery allows their own blood to be given back after surgery. During the period between predonation and surgery, the patients body can generally build back up the normal blood volume, allowing the predonated blood to replace the blood lost during and after surgery. Dislocation Recent technological advancements have allowed much bigger heads to be used, which significantly reduces dislocation risk. With optimum positioning and size of the components, the risk of dislocation is reduced through proper soft tissue tension. A manual test of stability throughout its range of motion is used to assess stability and avoidance of impingement. An xray is used during surgery to make sure the components are positioned correctly. Heterotopic Ossification Some patients form excessive bone around the hip, which can lead to stiffness and pain. Nerve Injury Although nerves are typically never lacerated, they may occasionally be stretched during surgery due to stiffness or correction of deformities. In most instances, a nerve injury is temporary and may require bracing until the nerve recovers. Fracture Patients with weak bone (osteoporosis) are at increased risk of fracture during the perioperative period. If a fracture occurs, it will be treated appropriately and may require additional procedures at the time of surgery or later. Vascular Injury Very low risk, but has been reported in the literature. Loosening or Mechanical Failure The implant can fail to have complete bone ingrowth into its porous coating, particularly in patients who take certain medications, have adverse medical conditions, have metal allergies, or have reduced bone formation from any cause. Although rare with modern technological components, implants can fail.
8 Continued Pain TOTAL HIP REPLACEMENT Although the purpose of the procedure is to reduce or eliminate pain, in some rare cases, chronic pain of unknown etiology can continue.
TOTAL KNEE REPLACEMENT Doug Thompson, MD PROCEDURE The purpose of the total knee replacement procedure is to replace diseased worn joint cartilage
 PROCEDURE The purpose of the total knee replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. An
PROCEDURE The purpose of the total knee replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. An
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
TOTAL HIP ARTHROPLASTY (hip replacement)
 TOTAL HIP ARTHROPLASTY (hip replacement) The condition The hip is a ball and socket joint. The ball is formed by the head of the thighbone (femur) which fits snugly into the cup shaped bone in the pelvis
TOTAL HIP ARTHROPLASTY (hip replacement) The condition The hip is a ball and socket joint. The ball is formed by the head of the thighbone (femur) which fits snugly into the cup shaped bone in the pelvis
While complications from surgery are uncommon some can be serious and may include:
 PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
The time required for surgery will vary depending upon the procedure recommended. The surgery may last 3 8 hours.
 PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
Patient Education GANZ PERIACETABULAR OSTEOTOMY
 GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GEORGETOWN ORTHOPAEDIC SPINE SURGERY. Lumbar Decompression
 Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
introduction jointunderstanding benefits of knee-replacement surgery
 introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
Your Care Team. Therapy staff (PT, PTA, OT, tech) Orthopedic surgeon. Case management staff (RN, social worker) Physician s assistant.
 Your Care Team You are not alone as you consider total joint replacement surgery. You are part of a team of dedicated health professionals who will be on your side throughout the entire process. You may
Your Care Team You are not alone as you consider total joint replacement surgery. You are part of a team of dedicated health professionals who will be on your side throughout the entire process. You may
Total Hip Replacement Surgery
 Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
KNEE ARTHROSCOPY SURGERY
 KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide
 Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
Patient Education Shoulder Arthroplasty
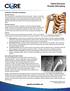 Explanation of Procedure and Diagnosis Shoulder Arthritis The shoulder joint is essentially a ball and socket joint. However, unlike the ball and socket joint of the hip, the shoulder has much greater
Explanation of Procedure and Diagnosis Shoulder Arthritis The shoulder joint is essentially a ball and socket joint. However, unlike the ball and socket joint of the hip, the shoulder has much greater
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions
 Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Total Shoulder Replacement Patient Guide
 About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction
 Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
POSTERIOR CERVICAL LAMINECTOMY AND FUSION
 PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
The Shoulder. The Shoulder Joint:
 The Shoulder The board certified physicians and surgeons at Orthopaedic Associates of Central Texas (OACT) are leaders in caring for the joints of the body. The shoulder joint is a complex and dynamic
The Shoulder The board certified physicians and surgeons at Orthopaedic Associates of Central Texas (OACT) are leaders in caring for the joints of the body. The shoulder joint is a complex and dynamic
ADULT SPINAL DEFORMITY SURGERY
 PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
ANTERIOR CERVICAL DISCECTOMY AND FUSION
 PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Table of Contents: What is a laparoscopic nissen fundoplication?...3. Where will surgery be performed?...3
 Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Patient Education Total Knee Arthroplasty
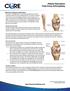 Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Patient Education Total Hip Arthroplasty
 Explanation of Diagnosis and Procedure Whether you have just begun exploring treatment options or have already decided with your orthopedic surgeon to undergo hip replacement surgery, this information
Explanation of Diagnosis and Procedure Whether you have just begun exploring treatment options or have already decided with your orthopedic surgeon to undergo hip replacement surgery, this information
Total Hip Replacement
 PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
TOTAL KNEE REPLACEMENT. Surgical Treatment for Advanced Pain due to Arthritis. Dr. Adam S. Rosen
 TOTAL KNEE REPLACEMENT Surgical Treatment for Advanced Pain due to Arthritis Dr. Adam S. Rosen What is Arthritis? How do you treat Arthritis? Arthritis is an inflammation of the joint due to loss of cartilage.
TOTAL KNEE REPLACEMENT Surgical Treatment for Advanced Pain due to Arthritis Dr. Adam S. Rosen What is Arthritis? How do you treat Arthritis? Arthritis is an inflammation of the joint due to loss of cartilage.
ANTERIOR LUMBAR INTERBODY FUSION (ALIF)
 PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Dr. Clark s Frequently Asked Questions
 Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components.
 Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
Jonathan T. Bravman, M.D.
 Total Shoulder Arthroplasty Patient Information Packet When planning for a total shoulder arthroplasty (TSA) procedure many questions arise concerning surgery, pain management, post-operative care, and
Total Shoulder Arthroplasty Patient Information Packet When planning for a total shoulder arthroplasty (TSA) procedure many questions arise concerning surgery, pain management, post-operative care, and
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
POSTERIOR LATERAL FUSION LUMBAR
 PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION
 UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty
![Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty](/thumbs/90/102636395.jpg) Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
PSOAS RELEASE DISCHARGE INSTRUCTIONS. Dr. Andrew Wolff
 Dr. Andrew Wolff 5215 Loughboro Road St. 200 Washington DC, 20815 Phone: 202-787-5601 ext 616 Fax: 202-787-5606 E-Mail: drwolff.ma@wosm.com Web: andrewwolffmd.com PSOAS RELEASE DISCHARGE INSTRUCTIONS page
Dr. Andrew Wolff 5215 Loughboro Road St. 200 Washington DC, 20815 Phone: 202-787-5601 ext 616 Fax: 202-787-5606 E-Mail: drwolff.ma@wosm.com Web: andrewwolffmd.com PSOAS RELEASE DISCHARGE INSTRUCTIONS page
PERCUTANEOUS NEPHROLITHOTRIPSY
 PERCUTANEOUS NEPHROLITHOTRIPSY Date of Surgery Please bring this booklet the day of your surgery. QHC#48 Percutaneous Nephrolithotripsy is a surgical procedure to remove kidney stones. The surgeon will
PERCUTANEOUS NEPHROLITHOTRIPSY Date of Surgery Please bring this booklet the day of your surgery. QHC#48 Percutaneous Nephrolithotripsy is a surgical procedure to remove kidney stones. The surgeon will
GEORGETOWN ORTHOPAEDIC SPINE SURGERY POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION)
 POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D.
 OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total hip replacement, there is a great deal of information that is important
OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total hip replacement, there is a great deal of information that is important
TOTAL KNEE REPLACEMENT
 TOTAL KNEE REPLACEMENT Patient Information Realistic Expectations about Knee Replacement Surgery An important factor in deciding whether to have total knee replacement surgery is understanding what the
TOTAL KNEE REPLACEMENT Patient Information Realistic Expectations about Knee Replacement Surgery An important factor in deciding whether to have total knee replacement surgery is understanding what the
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
A Patient s Guide to Artificial Joint Replacement of the Ankle
 A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
Patient Information for Consent
 Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT HANDBOOK AND JOURNAL FAQ
 PATIENT HANDBOOK AND JOURNAL FAQ FREQUENTLY ASKED QUESTIONS What is the recovery time for a total hip replacement? This generally takes about three months. Everyone heals at a different pace so this time
PATIENT HANDBOOK AND JOURNAL FAQ FREQUENTLY ASKED QUESTIONS What is the recovery time for a total hip replacement? This generally takes about three months. Everyone heals at a different pace so this time
Patient s guide to surgery
 Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
ABOUT YOUR KNEE SURGERY
 JOINT REPLACEMENT PROGRAM ABOUT YOUR KNEE SURGERY Center for Special Surgery is a state-of-the art outpatient surgical facility with fully equipped operating rooms and comfortable recovery areas. The professional
JOINT REPLACEMENT PROGRAM ABOUT YOUR KNEE SURGERY Center for Special Surgery is a state-of-the art outpatient surgical facility with fully equipped operating rooms and comfortable recovery areas. The professional
Patient Information for Consent
 Patient Information for Consent OS01 Total Hip Replacement Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI hospital on:...... Get
Patient Information for Consent OS01 Total Hip Replacement Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI hospital on:...... Get
Table of Contents. What is Spinal Fusion? Pre-Register for Surgery How Do I Prepare for Surgery?... 3
 www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
Subcapital hip fracture surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
TOTAL HIP REPLACEMENT GUIDE
 TOTAL HIP REPLACEMENT GUIDE This manual was made by physical therapists and Patient, Family and Community Education at City of Hope. Your physical therapist is: who can be reached at 626-256-HOPE (4673),
TOTAL HIP REPLACEMENT GUIDE This manual was made by physical therapists and Patient, Family and Community Education at City of Hope. Your physical therapist is: who can be reached at 626-256-HOPE (4673),
Total Hip Replacement
 AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
Arthroscopic Surgery. What is Arthroscopic Surgery?
 Arthroscopic Surgery The physicians and surgeons at Orthopaedic Asssociates of Central Texas (OACT) are leaders in caring for the joints of the body. We service patients in Williamson and surrounding Counties,
Arthroscopic Surgery The physicians and surgeons at Orthopaedic Asssociates of Central Texas (OACT) are leaders in caring for the joints of the body. We service patients in Williamson and surrounding Counties,
What is a total knee replacement?
 What is a total knee replacement? If you and your surgeon have exhausted all non-surgical measures for treating your knee pain and inflammation, you might be a candidate for total knee replacement. This
What is a total knee replacement? If you and your surgeon have exhausted all non-surgical measures for treating your knee pain and inflammation, you might be a candidate for total knee replacement. This
ACL Reconstruction. Role of the Anterior Cruciate Ligament. Treatment of ACL tears. ACL Reconstruction
 Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Preparing for your Laparoscopic Myotomy
 Preparing for your Laparoscopic Myotomy Pre and post-operative information Department of Table of Contents: What is a Laparoscopic Myotomy...3 Planning for surgery...3 Preparing for surgery/bowel prep.4
Preparing for your Laparoscopic Myotomy Pre and post-operative information Department of Table of Contents: What is a Laparoscopic Myotomy...3 Planning for surgery...3 Preparing for surgery/bowel prep.4
Anterior Cervical Discectomy and Fusion (ACDF)
 Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Activities After Knee Replacement
 Activities After Knee Replacement After undergoing knee replacement, you may expect your lifestyle to be a lot like it was before surgery but without the pain. In many ways, you are right, but returning
Activities After Knee Replacement After undergoing knee replacement, you may expect your lifestyle to be a lot like it was before surgery but without the pain. In many ways, you are right, but returning
Patient Information for Consent
 Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
Total Knee Replacement
 Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
A Patient's Guide to Cervical Laminectomy
 Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
ACL RECONSTRUCTION. Date of Surgery. Please bring this booklet the day of your surgery. QHC#65
 ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Hip Fracture Orthopaedic Department Patient Information Leaflet
 riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
About Your Thoracic Surgery
 About Your Thoracic Surgery Thoracic refers to your chest, which includes your heart, lungs, airways, ribs, esophagus, and thymus gland. In order for you to recover as quickly and painlessly as possible,
About Your Thoracic Surgery Thoracic refers to your chest, which includes your heart, lungs, airways, ribs, esophagus, and thymus gland. In order for you to recover as quickly and painlessly as possible,
In some cases, a medical evaluation may be needed, to be performed by your primary care physician about 2-4 weeks prior to surgery.
 Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY?
 ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY? GET TO KNOW HOW THIS LATEST-GENERATION BLOOD THINNER HELPS PROTECT YOU FROM BLOOD CLOTS. Once I got the facts, my doctor and I chose XARELTO Do not stop
ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY? GET TO KNOW HOW THIS LATEST-GENERATION BLOOD THINNER HELPS PROTECT YOU FROM BLOOD CLOTS. Once I got the facts, my doctor and I chose XARELTO Do not stop
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Anterior Approach to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Femoral shaft fracture surgery (femoral nailing)
 Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Total hip replacement
 Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
[PREPARING FOR TOTAL HIP REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS]
![[PREPARING FOR TOTAL HIP REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] [PREPARING FOR TOTAL HIP REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS]](/thumbs/90/101378966.jpg) X 2012 US CENTER FOR SPORTS MEDICINE DR. COREY G. SOLMAN, JR. [PREPARING FOR TOTAL HIP REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] Information regarding the expectations before, during and after surgery
X 2012 US CENTER FOR SPORTS MEDICINE DR. COREY G. SOLMAN, JR. [PREPARING FOR TOTAL HIP REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] Information regarding the expectations before, during and after surgery
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Robot Assisted Laparoscopic Radical Prostatectomy
 Robot Assisted Laparoscopic Radical Prostatectomy Robot Assisted Laparoscopic Radical Prostatectomy is an alternative to Open Radical Prostatectomy. It will be performed by your Consultant Urologist at
Robot Assisted Laparoscopic Radical Prostatectomy Robot Assisted Laparoscopic Radical Prostatectomy is an alternative to Open Radical Prostatectomy. It will be performed by your Consultant Urologist at
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Pre-Operative Patient Instruction Form for a Robotic Partial Knee Replacement
 Pre-Operative Patient Instruction Form for a Robotic Partial Knee Replacement What s Next: You will schedule a visit with your Primary Care Physician for a pre-operative history and physical to make sure
Pre-Operative Patient Instruction Form for a Robotic Partial Knee Replacement What s Next: You will schedule a visit with your Primary Care Physician for a pre-operative history and physical to make sure
Guide to Knee Surgery
 Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
