FEVER ASSESSMENT SUMMARY
|
|
|
- James Walton
- 6 years ago
- Views:
Transcription
1 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care practices based upon the available medical literature and clinical expertise at the time of development. They should not be considered to be accepted protocol or policy, nor are intended to replace clinical judgment or dictate care of individual patients. FEVER ASSESSMENT SUMMARY The onset of fever in a patient in the ICU is a moment of opportunity for the physician. Appropriate evaluation of fever and institution of early, goal directed therapy where indicated is associated with a clear survival benefit for patients who are septic, experiencing endocrine emergencies or other causes of temperature disregulation. A shotgun approach to fever evaluation, however, may lead to unnecessary diagnostic tests and procedures, confusing or inconclusive data, and significant expense. It may also expose the patient to unnecessary discomfort, risk and even inappropriate therapies. RECOMMENDATIONS Level 1 ne Level 2 Core body temperature measurements (such as from an intravascular or urinary catheter) should be used whenever possible. Axillary and tympanic temperatures are unreliable. Two peripheral blood cultures should be obtained in the presence of a new fever (when clinical evaluation does not strongly suggest a non-infectious cause). If a central venous catheter is present, an additional culture should be drawn from the indwelling catheter. Intravascular catheters should not be routinely cultured during catheter guidewire exchange unless catheter-related infection is suspected. When indicated, the intracutaneous segment (as opposed to the catheter tip) should be sent for semi quantitative culture. Pulmonary secretions should be sent for Gram stain and culture only when a pulmonary etiology for the patient's fever is strongly suspected. Urine should be collected by clean catch or from the sampling port of the urinary catheter. If infection is suspected, surgical wounds should be opened with Gram stain and culture obtained from deep within the wound site. Cultures of the skin overlying a wound should not be performed. If there is sufficient clinical suspicion, a CT scan of the sinuses should be obtained. Evaluation for Clostridium difficile infection should begin with a C. difficile toxin enzyme immunoassay test. If this test is negative, a second test should be performed. Level 3 Fever is defined as a temperature elevation of greater than 38.3 C (101 F) New onset of fever should result in a careful physical examination and clinical assessment of the patient rather than automatic orders for costly radiologic and laboratory tests. Chest radiographs, urinalysis, or culture are not indicated in the first hours postoperatively unless history and clinical findings suggest a high probability of utility. The patient with postoperative fever should receive aggressive pulmonary toilet and careful evaluation of all operative wounds. ninfectious causes of fever should be carefully investigated. If fever is accompanied by altered consciousness or focal neurologic deficits, lumbar puncture or evaluation of CSF from an indwelling ventriculostomy should be considered. EVIDENCE DEFINITIONS Class I: Prospective randomized controlled trial. Class II: Prospective clinical study or retrospective analysis of reliable data. Includes observational, cohort, prevalence, or case control studies. Class III: Retrospective study. Includes database or registry reviews, large series of case reports, expert opinion. Technology assessment: A technology study which does not lend itself to classification in the above-mentioned format. Devices are evaluated in terms of their accuracy, reliability, therapeutic potential, or cost effectiveness. LEVEL OF RECOMMENDATION DEFINITIONS Level 1: Convincingly justifiable based on available scientific information alone. Usually based on Class I data or strong Class II evidence if randomized testing is inappropriate. Conversely, low quality or contradictory Class I data may be insufficient to support a Level I recommendation. Level 2: Reasonably justifiable based on available scientific evidence and strongly supported by expert opinion. Usually supported by Class II data or a preponderance of Class III evidence. Level 3: Supported by available data, but scientific evidence is lacking. Generally supported by Class III data. Useful for educational purposes and in guiding future clinical research. 1 Revised 10/7/07
2 INTRODUCTION Fever, a common problem in both the intensive care unit (ICU) and on the patient ward, is defined as an elevation in core body temperature. The Society of Critical Care Medicine (SCCM) defines fever as a temperature elevation of greater than 38.3 C (101 F) (1). The incidence of fever during a typical ICU stay has been reported to vary between 5-70% (Class II) (2,3). Fever represents the body's response to injury, inflammation, and infection. Temperature elevation has been shown to both enhance immune response and suppress certain bacterial species (1). Although it is widely agreed that fever has adaptive advantages as a response to infection, it is also clear that fever has deleterious effects (3). In an evaluation of fever in critically ill surgical patients published in 2004, Barie et al found that fever is associated with a higher incidence of organ failure and death and that peak temperature is a powerful predictor of mortality (Class II) (4). In certain patient groups, however, fever is a predictable aspect of their hospital course and diagnostic evaluation is not indicated; the empiric treatment of such temperature elevations may actually be detrimental. The presence of fever commonly leads to performance of diagnostic tests and procedures as well as institution of therapies that significantly increase patient care costs and expose the patient to unnecessary risks and discomfort. Prophylactic broad-spectrum antibiotic therapy is also commonly instituted placing the patient at risk for both drug reactions and development of resistant bacterial species. Fever should lead to a careful physical evaluation and clinical assessment of the patient rather than automatic orders for costly laboratory and radiologic studies that are commonly associated with a low diagnostic yield (Level 3) (1,3). LITERATURE REVIEW Review Articles In 1998, SCCM created a task force to establish guidelines for evaluating new fever in critically ill patients. O'Grady et al performed an extensive review of the literature regarding many aspects of fever evaluation (1). It is a well referenced and very practical document and is cited often throughout this guideline. Dr. Marik s review article from 2000 entitled Fever in the ICU includes a more basic science review of fever and its causes as well as an algorithmic approach to the assessment on fever (3). Measuring Temperature The first step in evaluating fever is to accurately assess temperature. The gold standard for temperature monitoring is central core temperature measurement using an intravascular device such as a pulmonary artery (PA) catheter thermistor. This invasive methodology has obvious disadvantages and impracticalities for some patients. Though the optimal method for measuring temperature is still debated, it is clear that the site and method of measurement should be recorded along with the measurement itself (Level 3) (1). Moran et al compared PA thermistor, axillary, tympanic membrane, and urinary bladder thermistor temperature assessments in 110 patients in a tertiary university-based hospital setting (5). The authors found that tympanic membrane measurements showed only modest correlation with PA (r=0.77), urinary (r=0.69), and axillary (r=0.76) temperatures. The average difference between PA and urinary temperature was small at -0.05, with a good correlation (p=0.92). This paper adds to a growing body of evidence that questions tympanic membrane measurements and suggests that urinary bladder temperature monitoring is the preferred alternative when PA catheter monitoring is not indicated and Foley catheter placement is indicated (Class II) (5). Evaluation of the Patient With the new onset of fever, a detailed search for possible etiologies should be performed. In addition to a careful physical examination and thorough review of the patient s medical record, this should include: Review of: Patient s injuries Previous cultures Prior antibiotic therapies All medications (to rule out drug-related fever) Recent chest radiograph (if available) Examination of: Pulmonary secretions All intravascular catheter insertion sites All drainage tubes and their output All wounds All extremities for swelling 2 Revised 10/7/07
3 Infectious vs. n-infectious Causes of Fever The initial goal in fever assessment should be to identify when an infectious vs. a non-infectious cause of fever is present. Some common non-infectious causes for fever are listed below. Many of these are diagnoses of exclusion and many patients will have risk factors for both infectious and non-infectious etiology of their fever. Unless there is strong evidence that the fever is non-infectious in nature, diagnostic tests to evaluate for a source of infection, chosen based on the clinical circumstances, should be initiated. Assuming the absence of pulmonary aspiration or breaks in sterile technique, the development of fever within the first hours postoperatively is usually non-infectious in origin (1). Alcohol / drug withdrawal Postoperative fever Post transfusion fever Drug fever Cerebral infarction Adrenal insufficiency Myocardial infarction Pancreatitis Acalculous cholecystitis Ischemic bowel Aspiration pneumonitis ARDS Subarachnoid hemorrhage n-infectious Causes of Fever Fat emboli Transplant rejection Deep venous thrombosis Pulmonary emboli Gout / pseudogout Hematoma / Solid organ injury Cirrhosis (without primary peritonitis) GI bleed Thrombophlebitis IV contrast reaction Neoplastic fevers Decubitus ulcers Blood Cultures Blood cultures should be obtained in patients with a new fever when clinical evaluation does not strongly suggest a non-infectious cause (Level 2) (1,3). Two peripheral blood cultures should be drawn after the initial temperature elevation. If a central venous catheter is present and considered to be a potential source of infection, a blood culture drawn through the catheter should also be sent. Following this, further blood cultures should be obtained based on clinical judgment rather than automatically with each temperature elevation (Level 2). Obtaining blood cultures more than every 24 hours is rarely helpful (1). Martinez and colleagues retrospectively reviewed the sensitivity and specificity of blood cultures drawn through a central venous or arterial catheter in comparison to those obtained from peripheral venipuncture (6). Sensitivity and specificity were determined using true bacteremia as the primary outcome measure. Paired blood cultures were used for analysis. difference in sensitivity was identified. Specificity, however, was significantly less for cultures obtained from indwelling catheters compared to peripheral venipunctures (95% vs. 98%; p=0.002). The positive predictive value of cultures obtained through a central venous line was significantly lower than that of peripheral venipuncture (61% vs. 82%; p=0.045) (Class III). Cultures should not be drawn from indwelling vascular catheters unless performed at the time of line placement or as part of the evaluation for intravascular catheter-related infection (Level 2) (1,3,7). Intravascular Catheters Intravascular catheters are a major source of nosocomial blood stream infections. Intravascular catheters should NOT be routinely cultured unless catheter-related infection is suspected. In a patient with a new fever and no other obvious source, it is reasonable to suspect catheter-related bloodstream infection. While negative blood cultures from a central line can help to exclude catheter related bloodstream infection (CRBSI), positive blood cultures drawn from the catheter may indicate either infection or colonization (7). One approach is to change the suspect line over a guidewire in which case the intracutaneous segment (as opposed to the catheter tip) should be sent for semi-quantitative culture (Class II) (8). If the culture returns with more than 15 colony forming units (CFU) of a specific pathogen, the catheter should be considered infected and removed with a new central venous catheter inserted at a new site. Quantitative blood cultures, drawn peripherally and from the central catheter, are another approach to diagnosis of CRBSI. If the colony count obtained from the central venous catheter is 5-fold 3 Revised 10/7/07
4 greater than that from the peripheral culture, the catheter should be considered infected (7). Intravascular catheter insertion sites should be cultured and Gram stained ONLY when there is expressible purulence or exudate from around the catheter (Level 2) (1). There has been a recent surge of work evaluating the maintenance of central venous catheters and prevention and management of CRBSI. These issues are addressed in greater detail in the Central Venous Catheter guideline and the Selection of Central Venous Catheter in the Surgical Patient guideline. A thorough discussion of the subject is also available in a 2001 consensus guideline by Mermel et al (7). Pulmonary Infections Chest radiographs and respiratory cultures are not indicated in the first hours post-operatively unless respiratory rate, auscultation, abnormal blood gas results, or pulmonary secretions suggest a high probability of utility (Level 3) (1,3). The patient with postoperative fever should receive aggressive pulmonary toilet (Level 3). Pulmonary secretions should be sent for Gram stain and culture only when a pulmonary etiology for the patient's fever is strongly suspected. An expectorated or suctioned specimen is adequate for initial evaluation (Level 2) (1). The quality of the sputum sample should be considered in the evaluation of the culture results. Specimens that demonstrate a preponderance of epithelial cells on initial Gram stain are not suitable and should be discarded (1). Saline should be instilled only when adequate specimens cannot be otherwise obtained. Bronchoscopy and bronchoalveolar lavage should be considered when initial sputum evaluations are nondiagnostic or in the presence of a discrete lobar infiltrate (Level 2) (1). A chest imaging study (plain radiograph or chest computed tomography if clinically indicated) should be obtained whenever a pulmonary etiology for fever is suspected (Level 3) (1). Pleural fluid should be obtained for evaluation only when there is an adjacent infiltrate or other reason to suspect infection and the fluid can be safely aspirated (Level 2) (1,3). Urinary Tract Infections Urinalysis or culture is not indicated in the first hours postoperatively unless there is reason to suspect infection (i.e., break in sterile technique) (Level 3) (1). Asymptomatic bacteruria is very common, especially in patients with indwelling urinary catheters. This typically implies colonization as opposed to true urinary tract infection with antibiotic therapy being indicated only for the latter. When a patient becomes febrile without another obvious source, a urine specimen should be collected by clean catch or from the sampling port of the urinary catheter, not from the collecting bag. Interpretation of urine culture in ICU patients may be difficult. If there is concordance of an organism in blood and urine cultures, fever can be attributed to a urinary tract infection (1). Gram-negative bacilli, Enterococci faecalis, and yeast are the most common organisms encountered (1). Patients with more than 10 5 CFU on quantitative urinary culture are usually treated with antibiotics based on work done by Platt et al in the 1980 s that demonstrated an increased mortality in these patients (Class II) (9). However, this level of bacteruria may occur in up to 30% of catheterized, hospitalized patients (Class II) (3). The significance of more than 10 5 CFU remains unclear as does the significance of pyuria in the specimen (1,3). Wound Evaluation Surgical and superficial wounds should be inspected daily for signs of infection (Level 3) (1). Superficial wound cultures are rarely indicated unless there is evidence of purulence or suspicious drainage. If infection is suspected, the wound should be opened and Gram stain and cultures should be performed from deep within the wound site (Level 2). Cultures of the skin overlying a wound should not be performed. In post-operative patients or trauma patients, evaluation of the surgical field or deep tissue wounds may be warranted based on clinical suspicion. Plain radiographs, CT, and ultrasound all have a role in evaluation of these patients based on clinical evaluation (Level 3). Sinusitis Sinusitis is most commonly caused by obstruction of the ostia draining the sinuses due to a nasotracheal or nasogastric tube. The evaluation of sinusitis is generally not part of the initial evaluation for fever and should be undertaken after the more likely etiologies for fever have been ruled out. Only 25% of ICU patients with sinusitis will have purulent nasal discharge (1). Gram-negative bacilli represent 60% of the bacterial isolates in nosocomial sinusitis with Pseudomonas aeruginosa being most common (1). Gram- 4 Revised 10/7/07
5 positive bacteria comprise one-third of the isolates with Staphylococcus aureus being most common. Fungi comprise the remaining 5-10% of isolates. If there is sufficient clinical suspicion, a CT scan of the sinuses should be obtained (Level 2). Clostridium difficile and Enteric Pathogens Clostridium difficile colitis is the most common cause of diarrhea-related fever. The majority of patients infected with C. difficile are asymptomatic with only one-third developing diarrhea (3). It should be suspected in any patient with fever, diarrhea, and a history of receiving antibacterial agents within the three weeks prior to the onset of diarrhea. The sensitivity of testing stool specimens for C. difficile colitis via the enzyme immunoassay test for C. difficile toxin is 72% for the first sample and 84% for the second sample. As a result, evaluation for C. difficile infection should begin with a C. difficile toxin enzyme immunoassay test (Level 2). If this test is negative, a second test should be performed (Level 2). Although direct visualization of pseudomembranes via endoscopy is highly specific, the sensitivity is only 23% for patients with mild disease and there is a risk for perforation of the colon during the procedure (Level 2) (3). The empiric administration of metronidazole or oral vancomycin is discouraged due to the risk of producing resistant pathogens (Level II). If severe illness is present, empiric metronidazole therapy may be considered while awaiting diagnostic studies. Stool evaluation for ova, parasites, and other pathogens should be performed only if the patient has recently traveled to an endemic area, was admitted to the hospital for diarrhea, or the patient is HIV infected (Level 2) (3). Evaluation of the CNS If fever is accompanied by altered consciousness or focal neurologic deficits, lumbar puncture (unless contraindicated) or evaluation of CSF from an indwelling ventriculostomy should be considered (Level 3). Gram stain and culture should be performed with further investigation for tuberculosis, fungal disease, neoplasm, etc as indicated by the clinical situation (1). Candida and Fungal Infections Candida is part of the normal intestinal flora of some 30% of healthy people (3). Antibiotic therapy increases the incidence to about 70% and most ICU patients probably become colonized. Though not all colonized patients become infected, Candida species and fungal infections are important opportunistic pathogens in the ICU population. Infection can be assessed from histologic evaluation of specimens or identification from sterile specimens. Tracheal aspirates (especially in neutropenic patients) and Candida found in specimens from indwelling urinary catheters likely represent colonization rather than infection (Level 2) (3). REFERENCES 1. O'Grady NP, Barie PS, Bartlett J, et al. Practice parameters for evaluating new fever in critically ill adult patients. Crit Care Med 1998; 26: Bota DP, Ferreira FL, Melot C, Vincent JL. Body temperature alterations in the critically ill. Intensive Care Med 2004; 30: Marik P. Fever in the ICU. Chest 2000; 117: Barie PS, Hydo LJ, Eachempati SR, Causes and Consequences of Fever Complicating Critical Surgical Illness. Surgical Infections 2004; 10/8/ Moran JL, Peter JV, Solomon PJ, et al: Tympanic temperature measurements: Are they reliable in the critically ill? A clinical study of measures of agreement. Crit Care Med 2007; 35: Martinez JA, DesJardin JA, Aronoff M, Supran S, Nasaraway SA, Snydman Dr. Clinical utility of blood cultures drawn from central venous or arterial cultures in critically ill patients. Crit Care Med 2002; 30: Mermel LA. Farr BM. Sherertz RJ. Raad II. O'Grady N. Harris JS. Craven DE. Infectious Diseases Society of America. American College of Critical Care Medicine. Society for Healthcare Epidemiology of America. Guidelines for the management of intravascular catheter-related infections. Infection Control & Hospital Epidemiology. 2001; 22: , 8. Maki DG, Weise CE, Sarafin HW. A semiquantitative culture method for identifying intravenous catheter related infection. N Engl J Med 1977; 296: Platt R, Polk BF, Murdock B, Rosner B. Mortality associated with nosocomial urinary-tract infection. N Engl J Med 1982; 307: Revised 10/7/07
6 APPENDIX 1: CULTURE TECHNIQUES (1) Blood Indication: Blood cultures should be obtained in patients with a new fever when clinical evaluation does not strongly suggest a noninfectious cause. The site of venipuncture should be prepped with 10% povidone iodine, 70% alcohol, or equivalent antiseptic (iodophors must dry to provide maximal antiseptic activity) (Level I). At least ml of blood should be drawn from a separate site for each culture (Level II). The injection port should be wiped with alcohol prior to injection (Level III). Needles should NOT be switched prior to inoculating blood culture bottles. The risk of needle stick injury during the switch in needles is currently felt to outweigh the risk of contamination. A pair of blood cultures should be drawn after the initial temperature elevation. Following this, further blood cultures should be obtained based on clinical judgment rather than automatically with each temperature elevation (Level II). Cultures should not be drawn from indwelling vascular catheters unless performed at the time of line placement (Level III). Intravascular catheters Indication: Intravascular catheters should be cultured when catheter-related infection is strongly suspected (Level II). See Invasive Catheter Guidelines Pulmonary Secretions Indication: Pulmonary secretions should be cultured when a febrile patient is suspected of having a lower respiratory tract infection by clinical and/or radiographic assessment (Level II). Expectorated sputum should be sterilely collected from nonintubated patients (Level II). Deep tracheal aspirates should be obtained without use of saline in intubated patients. Saline should be instilled only when adequate specimens cannot otherwise be obtained. (Level II). Bronchoalveolar lavage should be considered when a discrete lobar infiltrate is present on chest radiograph or when tracheal aspirate cultures have not been helpful (Level II). Sputum samples should be transported to the microbiology laboratory and processed within 2 hours from the time of collection (Level II). Urine Indication: Urine cultures should be sent in the presence of fever and sufficient clinical suspicion. A midstream clean catch specimen should be sent in patients without a Foley catheter. Aspiration of urine from the sampling port of the urinary collecting tubing should be performed in patients with a Foley catheter. Meticulous cleansing of the aspiration port should be performed. Specimens should be sent to the microbiology laboratory for processing within 1 hour or the specimen should be refrigerated (Level II). Wound Indication: Wound cultures should be sent in the presence of fever, purulent drainage or sufficient clinical suspicion. Wounds that are suspected of being infected should be opened (Level II). Gram stain and cultures that are sent should be from deep within the wound site (Level II). Stool Indication: Stool should be sent for C. difficile toxin assay in any patient with fever, diarrhea, and a history of antibiotic administration with the previous 3 weeks. Stool for ova and parasites should be sent only if the patient has recently traveled to an endemic area, was admitted to the hospital for diarrhea, or the patient is HIV infected (Level II). Day 1: Send one stool sample for C. difficile toxin assay (Level II). Day 2: If the first specimen is negative, send an additional sample for C. difficile toxin assay 6 Revised 10/7/07
7 FEVER ASSESSMENT GUIDELINES Review patient's medical record, previous cultures and studies. Perform physical examination. Is patient's temperature > 38.3 o C (101.0 o F)? END Is a clinically obvious source of infection present? Perform focused diagnostic tests and procedures Begin empiric antibiotics per guidelines. Await culture results. Does patient have a clear noninfectious etiology for fever? Treat cause for fever. fever workup indicated at this time. Observe patient for 48 hours Obtain blood cultures Reevaluate / examine patient for source of fever. Perform focused diagnostic tests and procedures based on findings. Persistent fever or progressive signs of infection? Central line in place > 72 hours? Guidewire exchange catheter & culture ICS OR remove catheter +/- culture ICS (if sufficient clinical suspicion) Nasogastric or nasoendotracheal tube in place? Remove tubes if possible. Replace with small bore feeding tube. Does patient have diarrhea and risk factors for C. difficile infection? Obtain C. difficile toxin assay Consider empiric therapy per guidelines if sufficient suspicion for infection. Await culture results. Fever source identified? Focused diagnostic tests and procedures Blood: Two peripheral blood cultures per 24 hour period +/- through central venous catheter Invasive Catheters: Consider culturing any expressed purulence, remove / exchange catheter Pulmonary: Chest radiograph, Sputum culture, Bronchoalveolar lavage Stool: C. difficile toxin assay (if diarrhea and antibiotic use within 3 weeks) Urine: Urine culture, remove / exchange urinary catheter(if strong suspicion) Sinuses: Sinus CT, puncture/aspirate sinuses (if strong suspicion) Wound: Open wound, consider Gram stain / culture any expressed purulence Central Nervous System: Lumbar puncture, CSF culture Treat infection source END 7 Revised 10/7/07
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Effective Date: SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOGENS QUICK REFERENCE
 1 of 9 Policy #: Subject: 611 (PLH-611-06) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOGENS QUICK REFERENCE Approved by: Laboratory Director, Jerry
1 of 9 Policy #: Subject: 611 (PLH-611-06) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOGENS QUICK REFERENCE Approved by: Laboratory Director, Jerry
CATHETER-ASSOCIATED URINARY TRACT INFECTIONS
 CATHETER-ASSOCIATED URINARY TRACT INFECTIONS Hamid Emadi M.D Associate professor of Infectious diseases Department Tehran university of medical science The most common nosocomial infection The urinary
CATHETER-ASSOCIATED URINARY TRACT INFECTIONS Hamid Emadi M.D Associate professor of Infectious diseases Department Tehran university of medical science The most common nosocomial infection The urinary
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
American College of Surgeons Critical Care Review Course 2012: Infection Control
 American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Collection and Transportation of Clinical Specimens
 Collection and Transportation of Clinical Specimens IDK II Faculty of Nursing Universitas Indonesia PDF Created with deskpdf PDF Writer - Trial :: http://www.docudesk.com The laboratory diagnosis of an
Collection and Transportation of Clinical Specimens IDK II Faculty of Nursing Universitas Indonesia PDF Created with deskpdf PDF Writer - Trial :: http://www.docudesk.com The laboratory diagnosis of an
Specimen Collection and Source Mapping
 Specimen Collection and Source Mapping October 4, 2016 Steve Renfroe MT(ASCP) Consultant, Clinical Specialty What is Your Culture? Does your urinalysis reflex to culture? Does Lab educate your Nursing
Specimen Collection and Source Mapping October 4, 2016 Steve Renfroe MT(ASCP) Consultant, Clinical Specialty What is Your Culture? Does your urinalysis reflex to culture? Does Lab educate your Nursing
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used
 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
ANWICU knowledge
 ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
Microbiology Collection
 Microbiology Collection Notify the Microbiology Laboratory at 920-738-6317 if any of the following etiological agents are suspected to be present in the specimens sent to the laboratory. Bacillius anthracis
Microbiology Collection Notify the Microbiology Laboratory at 920-738-6317 if any of the following etiological agents are suspected to be present in the specimens sent to the laboratory. Bacillius anthracis
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Key Definitions. Downloaded from
 Key Definitions In order to make sure that every member of the team is clear about the definitions that will be used, we have provided a list of key terms in the next few pages along with commonly used
Key Definitions In order to make sure that every member of the team is clear about the definitions that will be used, we have provided a list of key terms in the next few pages along with commonly used
The Clinical Significance of Blood Cultures. Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM
 The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE
 EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
Blood Culture Collection and Interpretation
 Blood Culture Collection and Interpretation Catherine Ernst, RN,PBT(ASCP) Blood Cultures Indications for blood culture collection Proper method for blood culture collection Interpreting a blood culture
Blood Culture Collection and Interpretation Catherine Ernst, RN,PBT(ASCP) Blood Cultures Indications for blood culture collection Proper method for blood culture collection Interpreting a blood culture
CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting
 CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting James T. Fields, MD Carolinas Center for Medical Excellence Columbia, South Carolina February
CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting James T. Fields, MD Carolinas Center for Medical Excellence Columbia, South Carolina February
5. Use of antibiotics, which disturbs balance of normal flora. 6. Poor nutritional status.
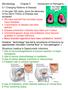 Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Candiduria in ICU : when and how to treat? Dr. Debashis Dhar Dept of Critical Care and Emergency Medicine Sir Ganga Ram Hospital
 Candiduria in ICU : when and how to treat? Dr. Debashis Dhar Dept of Critical Care and Emergency Medicine Sir Ganga Ram Hospital Introduction Nosocomial bacteriuria or candiduria develops in up to 25%
Candiduria in ICU : when and how to treat? Dr. Debashis Dhar Dept of Critical Care and Emergency Medicine Sir Ganga Ram Hospital Introduction Nosocomial bacteriuria or candiduria develops in up to 25%
320 MBIO Microbial Diagnosis. Aljawharah F. Alabbad Noorah A. Alkubaisi 2017
 320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Pathogens of the Urinary tract The urinary system is composed of organs that regulate the chemical composition and volume of
320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Pathogens of the Urinary tract The urinary system is composed of organs that regulate the chemical composition and volume of
Prevention of Important HAIs: Principle & Case Scenario in VAP/CAUTI. CPT. Pasri Maharom MD, MPH Dec 15, 2015
 Prevention of Important HAIs: Principle & Case Scenario in VAP/CAUTI CPT. Pasri Maharom MD, MPH Dec 15, 2015 Catheter Associated Urinary Tract Infection CAUTI CAUTI Epidemiology Key Principles of Preventing
Prevention of Important HAIs: Principle & Case Scenario in VAP/CAUTI CPT. Pasri Maharom MD, MPH Dec 15, 2015 Catheter Associated Urinary Tract Infection CAUTI CAUTI Epidemiology Key Principles of Preventing
MICROBIOLOGY SPECIMEN COLLECTION MANUAL
 Lee Memorial Health System Lee County, FL CLINICAL LABORATORY MICROBIOLOGY SPECIMEN COLLECTION MANUAL ACID FAST CULTURE Specimen Type see Specimen Chart ACID FAST STAIN see Specimen Chart Acid Fast stain
Lee Memorial Health System Lee County, FL CLINICAL LABORATORY MICROBIOLOGY SPECIMEN COLLECTION MANUAL ACID FAST CULTURE Specimen Type see Specimen Chart ACID FAST STAIN see Specimen Chart Acid Fast stain
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Scottish Surveillance of Healthcare Associated Infection Programme (SSHAIP) Health Protection Scotland (HPS) SSI Surveillance Protocol 7th Edition
 1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013
 Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013 Financial Disclosures No financial disclosures Objectives Review a case of recurrent Clostridium difficile infection
Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013 Financial Disclosures No financial disclosures Objectives Review a case of recurrent Clostridium difficile infection
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
Collection (Specimen Source Required on all tests) Sputum: >5 ml required. First morning specimen preferred.
 Type Acid Fast (Mycobacteria) Sputum: >5 ml required. First morning specimen preferred. For blood, sodium heparin tube preferred. Lithium heparin acceptable. Do not centrifuge.. delay. Swabs are not appropriate
Type Acid Fast (Mycobacteria) Sputum: >5 ml required. First morning specimen preferred. For blood, sodium heparin tube preferred. Lithium heparin acceptable. Do not centrifuge.. delay. Swabs are not appropriate
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Healthcare-associated infections acquired in intensive care units
 SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
There s More Than One Way to Skin a CAuTi:
 There s More Than One Way to Skin a CAuTi: A Multidisciplinary Approach to Prevent Catheter Associated Urinary Tract Infections & Treatment of Asymptomatic Bacteriuria Objectives Identify causes of CAUTI
There s More Than One Way to Skin a CAuTi: A Multidisciplinary Approach to Prevent Catheter Associated Urinary Tract Infections & Treatment of Asymptomatic Bacteriuria Objectives Identify causes of CAUTI
Urinary tract infection. Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine
 Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE
 ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Diagnosis and Management of UTI s in Care Home Settings. To Dip or Not to Dip?
 Diagnosis and Management of UTI s in Care Home Settings To Dip or Not to Dip? 1 Key Summary Points: Treat the patient NOT the urine In people 65 years, asymptomatic bacteriuria is common. Treating does
Diagnosis and Management of UTI s in Care Home Settings To Dip or Not to Dip? 1 Key Summary Points: Treat the patient NOT the urine In people 65 years, asymptomatic bacteriuria is common. Treating does
UTI IN ELDERLY. Zeinab Naderpour
 UTI IN ELDERLY Zeinab Naderpour Urinary tract infection (UTI) is the most frequent bacterial infection in elderly populations. While urinary infection in the elderly person is usually asymptomatic, symptomatic
UTI IN ELDERLY Zeinab Naderpour Urinary tract infection (UTI) is the most frequent bacterial infection in elderly populations. While urinary infection in the elderly person is usually asymptomatic, symptomatic
Clostridium difficile Infection (CDI) Management Guideline
 Clostridium difficile Infection (CDI) Management Guideline Do not test all patients with loose or watery stools for CDI o CDI is responsible for
Clostridium difficile Infection (CDI) Management Guideline Do not test all patients with loose or watery stools for CDI o CDI is responsible for
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
VAP Prevention bundles
 VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
Blood cultures in ED. Dr Sebastian Chang MBBS FACEM
 Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Sepsi: nuove definizioni, approccio diagnostico e terapia
 GIORNATA MONDIALE DELLA SEPSI DIAGNOSI E GESTIONE CLINICA DELLA SEPSI Giovedì, 13 settembre 2018 Sepsi: nuove definizioni, approccio diagnostico e terapia Nicola Petrosillo Società Italiana Terapia Antiinfettiva
GIORNATA MONDIALE DELLA SEPSI DIAGNOSI E GESTIONE CLINICA DELLA SEPSI Giovedì, 13 settembre 2018 Sepsi: nuove definizioni, approccio diagnostico e terapia Nicola Petrosillo Società Italiana Terapia Antiinfettiva
Pseudomonas aeruginosa
 JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela
 Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela Microbiology Department Medical Faculty, University of Indonesia Urinary Tract Infection
Diagnostic approach and microorganism resistance pattern in UTI Yeva Rosana, Anis Karuniawati, Yulia Rosa, Budiman Bela Microbiology Department Medical Faculty, University of Indonesia Urinary Tract Infection
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Preventing & Controlling the Spread of Infection
 Preventing & Controlling the Spread of Infection Contributors: Alice Pong M.D., Hospital Epidemiologist Chris Abe, R.N., Senior Director Ancillary and Support Services Objectives Review the magnitude of
Preventing & Controlling the Spread of Infection Contributors: Alice Pong M.D., Hospital Epidemiologist Chris Abe, R.N., Senior Director Ancillary and Support Services Objectives Review the magnitude of
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION
 HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
EXECUTIVE SUMMARY. General
 I D S A G U I D E L I N E S Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard
I D S A G U I D E L I N E S Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard
Bacteriemia and sepsis
 Bacteriemia and sepsis Case 1 An 80-year-old man is brought to the emergency room by his son, who noted that his father had become lethargic and has decreased urination over the past 4 days. The patient
Bacteriemia and sepsis Case 1 An 80-year-old man is brought to the emergency room by his son, who noted that his father had become lethargic and has decreased urination over the past 4 days. The patient
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
STANDARDIZED PROCEDURE LUMBAR PUNCTURE (Adult, Peds)
 I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
Fever Without a Source Age: 0-28 Day Pathway - Emergency Department Evidence Based Outcome Center
 Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Guideline for the Management of Fever and Neutropenia in Children with Cancer and/or Undergoing Hematopoietic Stem-Cell Transplantation
 Guideline for the Management of Fever Neutropenia in Children with Cancer /or Undergoing Hematopoietic Stem-Cell Transplantation COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive
Guideline for the Management of Fever Neutropenia in Children with Cancer /or Undergoing Hematopoietic Stem-Cell Transplantation COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Lab 4. Blood Culture (Media) MIC AMAL-NORA-ALJAWHARA 1
 Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
SAMPLE. Collecting a faeces specimen
 7. Perform steps 10 16 of the common steps (see pp. 39 43). Evidence base: PHE (2014a) To ensure that: the patient is safe and comfortable. the specimen has been correctly collected and documented in the
7. Perform steps 10 16 of the common steps (see pp. 39 43). Evidence base: PHE (2014a) To ensure that: the patient is safe and comfortable. the specimen has been correctly collected and documented in the
Diagnosis of Ventilator- Associated Pneumonia: Where are we now?
 Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
2046: Fungal Infection Pre-Infusion Data
 2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
STANDARDIZED PROCEDURE LUMBAR PUNCTURE/INTRATHECAL CHEMOTHERAPY (Adult, Peds)
 I. Definition The lumbar puncture (LP) may assist in diagnosis of central nervous system (CNS) infections, malignancies and subarachnoid hemorrhage after imaging studies. The LP also facilitates the administration
I. Definition The lumbar puncture (LP) may assist in diagnosis of central nervous system (CNS) infections, malignancies and subarachnoid hemorrhage after imaging studies. The LP also facilitates the administration
Infectious Diseases in Clinical Practice February 2011 Lisa G. Winston, MD
 Infectious Diseases in Clinical Practice February 2011 Lisa G. Winston, MD A 60 year old man was hospitalized 2 months ago for CABG. His course was uncomplicated, and he was discharged after 5 days. He
Infectious Diseases in Clinical Practice February 2011 Lisa G. Winston, MD A 60 year old man was hospitalized 2 months ago for CABG. His course was uncomplicated, and he was discharged after 5 days. He
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy.
 Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
URINARY TRACT INFECTIONS: Focus on CA UTIs
 URINARY TRACT INFECTIONS: Focus on CA UTIs William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University of North Carolina
URINARY TRACT INFECTIONS: Focus on CA UTIs William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University of North Carolina
Clostridium difficile Specimen Collection
 Clostridium difficile Specimen Collection Collect stool specimens into a clean, airtight container with no preservative. All stool specimens should be tested as soon as possible. Ideally, stool specimens
Clostridium difficile Specimen Collection Collect stool specimens into a clean, airtight container with no preservative. All stool specimens should be tested as soon as possible. Ideally, stool specimens
Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age
 Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
320 MBIO Microbial Diagnosis. Aljawharah F. Alabbad Noorah A. Alkubaisi 2017
 320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
Antibiotic Stewardship and the Misdiagnosis of UTI
 Antibiotic Stewardship and the Misdiagnosis of UTI Daniel J. Pallin, MD, MPH Director of Research, Department of Emergency Medicine Chairman, Clinical Investigation Committee Brigham and Women s Hospital
Antibiotic Stewardship and the Misdiagnosis of UTI Daniel J. Pallin, MD, MPH Director of Research, Department of Emergency Medicine Chairman, Clinical Investigation Committee Brigham and Women s Hospital
INFECTION PREVENTION AND CONTROL
 INFECTION PREVENTION AND CONTROL Health Care-Associated Infection (HAI) Definitions May 28, 2012 The Capital Health Infection Prevention Control (IPAC) department conducts ongoing surveillance reports
INFECTION PREVENTION AND CONTROL Health Care-Associated Infection (HAI) Definitions May 28, 2012 The Capital Health Infection Prevention Control (IPAC) department conducts ongoing surveillance reports
Getting the Point of Injection Safety
 Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association
 Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
Yes No Unknown. Major Infection Information
 Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Clinical Practice Management Guideline for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention
 Clinical for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention Background Ventilator-associated pneumonia (VAP), a pneumonia that develops 48hrs after initiation of mechanical ventilation,
Clinical for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention Background Ventilator-associated pneumonia (VAP), a pneumonia that develops 48hrs after initiation of mechanical ventilation,
Objec&ves. Clinical Presenta&on
 Michelle A. Barron, MD Associate Professor of Medicine Division of Infectious Diseases University of Colorado Denver Objec&ves Determine who is at risk for invasive candidiasis. Understand whether prophylaxis
Michelle A. Barron, MD Associate Professor of Medicine Division of Infectious Diseases University of Colorado Denver Objec&ves Determine who is at risk for invasive candidiasis. Understand whether prophylaxis
2018 CNISP HAI Surveillance Case definitions
 2018 CNISP HAI Surveillance Case definitions The following case definitions for the surveillance of healthcare-associated infections (HAIs) are used by all acute-care hospitals that participate in the
2018 CNISP HAI Surveillance Case definitions The following case definitions for the surveillance of healthcare-associated infections (HAIs) are used by all acute-care hospitals that participate in the
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review
 Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
Update in Hospital Medicine. Update in Hospital Medicine 2009
 2009 Bradley A. Sharpe, MD UCSF Division of Hospital Medicine PE in Acute COPD Exacerbations Question: What is the prevalence of PE in patients with COPD who need hospitalization? Design: Systematic review,
2009 Bradley A. Sharpe, MD UCSF Division of Hospital Medicine PE in Acute COPD Exacerbations Question: What is the prevalence of PE in patients with COPD who need hospitalization? Design: Systematic review,
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS.
 Page 1 The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS. Appendix TABLE E-1 Care-Module Trigger Events That May Indicate an Adverse
Page 1 The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS. Appendix TABLE E-1 Care-Module Trigger Events That May Indicate an Adverse
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Vascular Catheter Related Infections in a Tertiary Care Hospital A Microbiological Study
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 592-599 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.072
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 592-599 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.072
National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH
 National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion
National Healthcare Safety Network: Central Line-associated Bloodstream Case Studies Teresa C. Horan, MPH National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare Quality Promotion
The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH
 The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH Some history first Clostridium difficile, a spore-forming gram-positive (i.e., thick
The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH Some history first Clostridium difficile, a spore-forming gram-positive (i.e., thick
Asyntomatic bacteriuria, Urinary Tract Infection
 Asyntomatic bacteriuria, Urinary Tract Infection C. Infectious Diseases Society of America Guidelines for the Diagnosis and Treatment of Asyntomatic Bacteriuria in Adults (2005) Pyuria accompanying asymptomatic
Asyntomatic bacteriuria, Urinary Tract Infection C. Infectious Diseases Society of America Guidelines for the Diagnosis and Treatment of Asyntomatic Bacteriuria in Adults (2005) Pyuria accompanying asymptomatic
Clostridium difficile
 Clostridium difficile Care Homes IPC Study Day Sue Barber Infection Prevention & Control Lead AV & Chiltern CCG s Clostridium difficile A spore forming Bacterium. Difficult to grow in the laboratory hence
Clostridium difficile Care Homes IPC Study Day Sue Barber Infection Prevention & Control Lead AV & Chiltern CCG s Clostridium difficile A spore forming Bacterium. Difficult to grow in the laboratory hence
