Continuing Anti-thrombotic Medication During Low-to-Intermediate Risk Spinal Procedures: A Retrospective Evaluation
|
|
|
- Brianna Chapman
- 6 years ago
- Views:
Transcription
1 Pain Physician 2017; 20: ISSN Retrospective Study Continuing Anti-thrombotic Medication During Low-to-Intermediate Risk Spinal Procedures: A Retrospective Evaluation Noud van Helmond, MD 1, Wesley Day 1, and Kenneth B. Chapman, MD 1,2 From: 1 Spine & Pain Institute of New York, New York City, New York; 2 Department of Anesthesiology, New York University Langone Medical Center, New York City, New York Address Correspondence: Kenneth B. Chapman, MD Spine & Pain Institute of New York 860 5th Ave New York, NY chapmanken@spinepainny. com Disclaimer: There was no external funding in the preparation of this manuscript. Conflict of interest: Each author certifies that he or she, or a member of his or her immediate family, has no commercial association (i.e., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted manuscript. Manuscript received: Revised manuscript received: Accepted for publication: Free full manuscript: Background: The current American Society of Regional Anesthesia (ASRA) guidelines recommend discontinuing anti-thrombotic therapy prior to any interventional spine procedures to decrease the incidence of bleeding complications. However, discontinuing anti-thrombotics may pose considerable danger in terms of cerebrovascular and cardiovascular events. Recent evidence suggests that some spinal interventions may still be performed safely with antithrombotics on board and some practitioners thus elect to continue certain anti-thrombotics for these procedures. Objective: To assess the rate of adverse events in patients undergoing spine procedures that are currently classified by the ASRA guidelines as low-to-intermediate bleeding risk, while being on continued anti-thrombotic therapy. Study Design: Retrospective cohort study. Setting: Interventional pain management practice. Methods: A retrospective chart review was performed on patients who underwent lowto-intermediate risk spine procedures with variable anti-thrombotic medications continued throughout the course of treatment. Results: Between October 2015 and May 2016, out of 2,204 patients who underwent low-tointermediate risk spine procedures, we identified 490 patients on anti-thrombotic medications. These included aspirin (N = 275), P2Y 12 inhibitors (N = 129), warfarin (N = 62), heparin (N = 10), factor Xa inhibitors (N = 55), and dipyridamole (N = 1). Forty-two patients were on multiple anti-thrombotics. Anti-thrombotics were continued throughout the procedure for 467 of 490 patients (88%). One bleeding complication (injection site bleeding) occurred in a patient that continued clopidogrel and aspirin during a lumbar radiofrequency ablation. We encountered no bleeding complications attributable to anti-thrombotics in the other 466 procedures in which anti-thrombotics were continued during lumbar (N = 260), thoracic (N = 18), and cervical (N = 40) medial branch injections, sacroiliac injections (N = 47), and during lumbar (N = 87) thoracic (N = 2), and cervical (N = 12) medial branch radiofrequency ablations. Limitation: The retrospective nature of the study and its reliance on electronic medical records are potential limitations. Conclusion: Continuing anti-thrombotic medication during medial branch and sacroiliac injections may be possible. Key words: Interventional pain management, thrombotic complications, hemostasis, anticoagulation, bleeding complications Pain Physician 2017; 20:
2 Pain Physician: July/August 2017; 20: The level of bleeding risk one spinal procedure holds over another is poorly understood. In 2015, the American Society of Regional Anesthesia (ASRA) (1) published guidelines rating the level of risk imposed by variable, commonly performed interventional pain procedures. Those considered intermediate risk for bleeding complications included epidural injections (interlaminar and transforaminal), facet blocks, sympathetic block, radiofrequency neurotomy, and lumbar intradiscal injections. The authors recommend discontinuing anti-thrombotic medications for these procedures and further delineate the length of time certain medications must be stopped in advance to limit the risk of complications such as an epidural hematoma. This is contrary to a 2013 Spine Intervention Society guideline (2) which suggested that lumbar transforaminal epidural, posterior-approach facet joint, radiofrequency neurotomy, sacroiliac, lumbar sympathetic, and lumbar intradiscal injections may be performed safely while continuing certain anti-thrombotic agents. In addition, in 2013 Manchikanti et al (3) performed a comprehensive systematic review on periprocedural antithrombotic management and provided recommendations specific for interventional pain techniques, which were adapted for the 2013 American Society of Interventional Pain Physicians (ASIPP) guidelines (4). The ASIPP guidelines distinguish high risk (interlaminar epidural injections, percutaneous adhesiolysis, disc decompression, sympathetic blocks, placement of implantables) and low risk (caudal epidural injection, paravertebral interventional techniques, peripheral joint injections) interventional techniques, and contrary to the ASRA guidelines do not include an intermediate risk category. The ASIPP guidelines recommend continuing non-steroidal anti-inflammatory drugs (NSAIDs), aspirin, and phosphodiesterase inhibitors for any procedure and provide more room for choice for the physician to continue or stop other anti-thrombotics for high risk and low risk procedures. They also provide a higher INR requirement (2.0) for low risk procedures (4). The practice of discontinuing anti-thrombotic medication prior to spinal interventions is mostly based on several case reports of epidural hematomas in patients undergoing spine procedures under continued anti-thrombotic medications (5-7). However, discontinuing anti-thrombotics may pose considerable danger in terms of cerebrovascular and cardiovascular events (8). The risk of epidural hematomas or other bleeding complications would appear to be low in patients undergoing procedures that are currently classified as low-to intermediate risk for bleeding by ASRA guidelines (8,9). As a result, some practitioners elect to continue certain anti-thrombotics for these procedures (8,10). It has been suggested to modify the latest ASRA guidelines to recommend continuation of most anti-thrombotics for low-to-intermediate risk procedures (9). The aim of this study was to assess the risk of bleeding complications in patients undergoing several low-to-intermediate risk spine interventions during which anti-thrombotic medications were continued. Methods Study Population The study was conducted in a private practice in which some practitioners routinely continued antithrombotics while others discontinued anti-thrombotics in keeping with the currently accepted ASRA guidelines for spine interventions. To assess the risks associated with continuation of anti-thrombotic therapy, we performed a retrospective chart review on all patients who underwent certain low-to-intermediate risk spine interventions between October 1, 2015, and May 31, We chose this time window because we estimated from a preliminary analysis that this would include ~400 patients on anti-thrombotics in our analysis. A previous study on bleeding risk associated with spine interventions and antithrombotics reached reliable results including ~200 patients (9). We included medial branch blocks (lumbar, thoracic, and cervical), sacroiliac joint injections, and medial branch radiofrequency ablations (lumbar, thoracic, and cervical). Medial branch blocks and medial branch radiofrequency ablations are currently classified as intermediate-risk by the ASRA guidelines (1), whereas sacroiliac joint injections are classified as low risk. We did not include epidural injections because all practitioners in our office discontinue antithrombotics prior to epidural injections. This study was approved by the Northwell Institutional Ethical Review Board (number: ) on September 13, Requirement of informed consent and HIPAA authorization was waived. All spinal procedures were performed under fluoroscopic guidance. Most injections were performed with 25 gauge spinal needles. For radiofrequency medial branch ablations, 20 gauge or 22 gauge needles were used
3 Continuing Anti-thrombotic Medication during Spinal Procedures Anti-thrombotic Medications The following medications were considered antithrombotic medications: aspirin (Ecotrin), warfarin (Coumadin or Jantoven), dabigatran etexilate (Pradaxa), apixaban (Eliquis), rivaroxaban (Xarelto), clopidogrel (Plavix), prasugrel (Effient), ticagrelor (Brilinta), heparin, enoxaparin (Lovenox), and dipyridamole (Persantine). Data Retrieval Patient characteristics, medication information, performed interventions, and past complications were collected retrospectively from medical records. We checked for complications from procedures by looking at the notes of follow-up telephone calls 48 hours postprocedure, or notes from a follow-up appointment (~2 to 4 weeks post-procedure). During follow-up calls and follow-up visits patients are specifically asked whether they have experienced any complications as a result of the procedure. Study Outcome Bleeding complication from a spine procedure was the main outcome of this study. We screened medical records for clinically evident bleeding complications such as a hematoma or injection site bleeding. Statistical Analysis Patients with incomplete follow-up were excluded from the analysis. Continuous data are displayed as mean ± standard deviation. Outcome incidences are reported with adjusted Wald confidence intervals within 95% (11). Analysis was performed using JMP version 12 (SAS Institute Inc., Cary, NC, USA). Results During the study period, 2,204 of the predetermined low-to-intermediate risk spinal procedures were performed; 53 patients did not return for a follow-up visit nor could they be reached by phone. Of the 2,151 patients with complete data, 490 patients (260 men, and 230 women) were found to be on anti-thrombotic medication. The mean age of patients on ant-thrombotic medication was 69 ± 11 years. In 467 patients, anti-thrombotic therapy was continued throughout the procedure Table 1. If anti-thrombotic medication was discontinued for the procedure, it was halted for the duration recommended in the 2015 ASRA guidelines (1). Study Outcome A 59-year-old woman developed injection site bleeding after undergoing a lumbar radiofrequency ablation while on aspirin and clopidogrel throughout the procedure. She presented at the emergency department where the bleeding was stopped by applying pressure. Of note, no bleeding complications occurred in 466 other patients in which anti-thrombotics were continued during the different low-to-intermediate risk interventional spine procedures Table 2. The corresponding 95%-confidence intervals for bleeding complications were % for medial branch injections, % for medial branch radiofrequency ablations, and % for sacroiliac injections Table 2. No clinically evident bleeding events were observed in the 1,661 patients not on anti-thrombotics. Discussion This retrospective cohort study describes a significant number of chronic pain patients that underwent low-to-intermediate risk spinal interventions under continued anti-thrombotics. We observed one bleeding complication in this cohort of 467 patients that were on anti-thrombotics throughout their procedure. The 95% confidence intervals of bleeding risk were %, %, and % for medial branch injections, sacroiliac injections, and medial branch radiofrequency ablations, respectively. Bleeding Risk of Continuing Anti-thrombotics for Spine Interventions Currently Classified as Low-to-Intermediate Risk by ASRA Guidelines Management of anti-thrombotics during procedures requires balancing the risk of bleeding complications vs. thromboembolic events. The ASRA consensus guidelines recommend discontinuing most anti-thrombotic medications for low-to-intermediate risk procedures (1), but are mostly based on circumstantial evidence from spinal anesthesia for surgical procedures because no better evidence was available at the time the guidelines were adopted. Recently several studies were conducted in attempts to address this dilemma. A study by Endres et al (8) reported no bleeding complications after 1,836 medial branch injections and 261 sacroiliac injections in patients continuing anti-thrombotics. Similarly, another study (9) found no hemorrhagic complications in patients continuing anti-thrombotics undergoing 62 medial branch injections, 5 sacroiliac injections, and 26 medial branch radiofrequency ablations. These results confirmed an earlier study by 439
4 Pain Physician: July/August 2017; 20: Table 1. Periprocedural anti-thrombotic therapy. Procedure Aspirin LMB Inj. TMB Inj. CMB Inj. Sacroiliac Inj. LMB RFA TMB RFA CMB RFA Total Discontinued 1 (1) 0 2 (7) 1 (3) 5 (9) 2 (66) 3 (33) 14 (5) Continued 136 (99) 11 (100) 28 (93) 29 (97) 50 (91) 1 (33) 6 (67) 261 (95) Clopidogrel Discontinued 15 (21) 0 2 (33) 5 (45) 6 (25) (23) Continued 58 (79) 4 (100) 4 (67) 6 (55) 18 (75) 1 (100) 1 (100) 92 (77) Ticagrelor Discontinued Continued 2 (100) 0 1 (100) 1 (100) (100) Prasugrel Discontinued Continued 3 (100) (100) (100) Dipyridamole Discontinued Continued 1 (100) (100) Warfarin Discontinued 4 (12) 1 (100) 1 (14) 2 (20) 1 (10) (15) Continued 28 (88) 0 6 (86) 8 (80) 9 (90) 0 2 (100) 53 (85) Rivaroxaban Discontinued 4 (29) (25) (26) Continued 10 (71) (100) 3 (75) (74) Dabigatran Discontinued (50) (8) Continued 4 (100) 2 (100) 1 (50) 1 (100) 3 (100) (92) Apixaban Discontinued 3 (18) (50) (21) Continued 14 (82) 1 (100) 0 1 (100) 2 (50) 0 1 (100) 19 (79) Heparin Discontinued 1 (100) 1 (100) (40) Continued 3 (100) (60) Enoxaparin Discontinued (100) (20) Continued 1 (100) (100) 0 2 (100) 4 (80) Total Discontinued 28 (9) 2 (10) 7 (15) 8 (15) 15 (15) 2 (50) 3 (20) 65 (12) Continued 260 (91) 18 (90) 40 (85) 47 (85) 88 (85) 2 (50) 12 (80) 467 (88) L, lumbar, T, thoracic, C, cervical, MB, medial branch, Inj., injection, RFA, radiofrequency ablation Manchikanti et al (10) that found no serious bleeding complications in patients continuing anti-thrombotics undergoing 1,116 facet joint interventions. Our study adds to this fund of safety data for interventional spine procedures. After combining our data with the data from these earlier studies, the upper 95% CI limits for bleeding complications rates with continued antithrombotics during medial branch injections, sacroiliac injections, and medial branch radiofrequency ablations are 0.15%, 1.0%, and 4.7%, respectively. Previous stud
5 Continuing Anti-thrombotic Medication during Spinal Procedures ies that declared epidural or spinal anesthesia safe in patients taking anti-platelet drugs did so on the basis of a zero percent prevalence of complications in 386 (12) and 383 (13) patients, respectively. In those studies the upper confidence limits of 0% were reported as 1.1% (12) and 0.96% (13), which are greater than or relatively equal to the upper limits that are observed with medial branch injections (0.15% upper limit of complication risk) and sacroiliac injections (1.0% upper limit of complication risk). Applying the same safety standard to the present study means that medial branch injections and sacroiliac injections can be regarded as safe in patients on anti-thrombotics. The upper limit of complication risk for radiofrequency ablations is substantially greater (4.7%) than previously used safety thresholds and further research is needed to reliably estimate its associated bleeding risk under continued anti-thrombotics. In the current study, we did not include epidural injections because all practitioners in our office discontinue anti-thrombotics prior to epidural injections. Manchikanti et al (10) described patients continuing anti-thrombotics during 466 interlaminar epidurals, 630 caudal epidurals, and 170 lumbar transforaminal epidurals. Surprisingly, when they combined data for all epidurals they found an increased risk of local bleeding for the patients that discontinued anti-thrombotics vs. the patients that continued anti-thrombotics (68.3% vs. 60.2%) and no differences regarding intravascular entry, profuse bleeding, local hematoma, oozing, and bruising. Of note, they encountered no epidural hematomas in patients continuing anti-thrombotics, which is consistent with the studies by Endres et al (8) and Goodman et al (9) that found no epidural hematomas in 1,633 and 90 patients, respectively, undergoing transforaminal epidural injections under continued anti-thrombotics. Continuing antithrombotics during epidural injections may thus be safe in selected patients. However, in our office all practitioners choose to discontinue anti-thrombotics before epidural injections given the potential serious consequences if an epidural hematoma were to occur, and we were thus unable to assess an event rate in the current study. Studies with very significant sample size are needed to assess whether the risk of epidural hematoma following epidural injection under continued anti-thrombotics is acceptably low in selected patients (8). Table 2. Low- and intermediate-risk spine interventions and incidence of bleeding complications. Bleeding complications % (95CI) Anti-thrombotic continued Procedure LMB Inj. 0 ( ) 260 (91) TMB Inj. 0 (0.0 15) 18 (90) CMB Inj. 0 ( ) 40 (85) Total MB Inj. 0 ( ) 318 (90) LMB RFA 1.1 ( ) 88 (85) TMB RFA 0 (0.0 63) 2 (50) CMB RFA 0 (0.0 22) 12 (80) Total MB RFA 1.0 ( ) 102 (80) Sacroiliac Inj. 0 ( ) 47 (85) Total 0.2 ( ) 467 (88) L, lumbar, T, thoracic, C, cervical, MB, medial branch, Inj., injection, RFA, radiofrequency ablation Thromboembolic Risk with Discontinuing Antithrombotics We did not encounter any thromboembolic complications in the 63 patients who discontinued their anti-thrombotics in our study (Table 1). However in the study by Endres et al (8), 9 out of 4,766 patients in which anti-thrombotics were discontinued as recommended by guidelines (1) suffered thromboembolic complications (myocardial infarction, stroke, pulmonary embolism). Two patients in that study died as a result of these complications. Although small, this prevalence of serious complications (0.4%, 95% CI: %) means that there is a risk associated with temporary discontinuation of anti-thrombotics. Outside the current study period of interest, we have previously also experienced a complication of discontinuation of antithrombotics in our practice. In that case, a patient undergoing an epidural injection died as a result of an acute myocardial infarction after Plavix was discontinued. Clinical Implications Practicing interventional pain management physicians face a dilemma when they need to choose between discontinuing and continuing anti-thrombotics for interventional spine procedures. As mentioned earlier, both choices carry risks: discontinuing anti-thrombotics is associated with a slight increased risk of thromboembolic events such as myocardial infarction and stroke while continuing antithrombotics may render patients more vulnerable to bleeding complications. The decision of continuing or discontinu
6 Pain Physician: July/August 2017; 20: ing anti-thrombotics will always need to be made on a case-by-case basis by factoring in individual patient characteristics and the planned procedure. The risks of discontinuing anti-thrombotics should also be discussed with the prescribing physician. In the case of medial branch injections and sacroiliac injections, it may be advisable to continue anti-thrombotics in a majority of patients given the apparent low incidence of bleeding complications with these interventions, and the greater risk of serious thromboembolic complications occurring when anti-thrombotics are discontinued. Of note, the bleeding complications that can occur with these procedures are relatively minor (bruising, injection site bleeding) compared to the potential thromboembolic complications (stroke, myocardial infarction) when anti-thrombotics are discontinued. Methodological Considerations Several limitations pertain to this study. First, the retrospective nature of this study means that a small number of patients were lost to follow-up. Second, we did not analyze INR values for this study, which could have provided some more insight into the physiological effects of discontinuation of coumadin. Third, continuation and discontinuation of NSAIDs other than aspirin and selective serotonin reuptake inhibitors were not monitored. However, the ASRA guidelines (1) recommend continuing both NSAIDs and selective serotonin reuptake inhibitors medications during the procedures we investigated in this study. Fourth, we did not analyze bleeding risk for individual anti-thrombotic medications because our sample size did not allow for such an analysis. However, it is safe to assume that some anti-thrombotic medications will convey a higher bleeding risk than others. Fifth, this study utilized a patient sample from a large private practice in which each interventional pain management physician performs large volumes of the studied interventions each year. Additionally, most injections were performed with 25 gauge spinal needles and for radiofrequency medial branch ablations 20 gauge or 22 gauge needles were used to minimize the risk of bleeding. Some physicians use 22 gauge and 18 gauge for these respective procedures instead and bleeding complication rates may thus be different in a different setting. Continued multicenter studies on this topic are therefore warranted to further improve patient safety. Conclusion Medial branch injections and sacroiliac joint injections appear to be safe to perform in patients who continue anti-thrombotics throughout the procedure. Continuing anti-thrombotics during these spine interventions will likely prevent the increased risk of thromboembolic complications that might otherwise occur as the result of their discontinuation. References 1. Narouze S, Benzon HT, Provenzano DA, Buvanendran A, De Andres J, Deer TR, Rauck R, Huntoon MA. Interventional spine and pain procedures in patients on antiplatelet and anticoagulant medications: Guidelines from the American Society of Regional Anesthesia and Pain Medicine, the European Society of Regional Anaesthesia and Pain Therapy, the American Academy of Pain Medicine, the International Neuromodulation Society, the North American Neuromodulation Society, and the World Institute of Pain. Reg Anesth Pain Med 2015; 40: Bogduk N. Practice Guidelines for Spinal Diagnostic and Treatment Procedures. International Spine Intervention Society, San Francisco, Manchikanti L, Falco FJ, Benyamin RM, Caraway DL, Kaye AD, Helm S, 2nd, Wargo BW, Hansen H, Parr AT, Singh V, Swicegood JR, Smith HS, Schultz DM, Malla Y, Hirsch JA. Assessment of bleeding risk of interventional techniques: A best evidence synthesis of practice patterns and perioperative management of anticoagulant and antithrombotic therapy. Pain Physician 2013; 16:S261-S Manchikanti L, Abdi S, Atluri S, Benyamin RM, Boswell MV, Buenaventura RM, Bryce DA, Burks PA, Caraway DL, Calodney AK, Cash KA, Christo PJ, Cohen SP, Colson J, Conn A, Cordner H, Coubarous S, Datta S, Deer TR, Diwan S, Falco FJ, Fellows B, Geffert S, Grider JS, Gupta S, Hameed H, Hameed M, Hansen H, Helm S, 2nd, Janata JW, Justiz R, Kaye AD, Lee M, Manchikanti KN, McManus CD, Onyewu O, Parr AT, Patel VB, Racz GB, Sehgal N, Sharma ML, Simopoulos TT, Singh V, Smith HS, Snook LT, Swicegood JR, Vallejo R, Ward SP, Wargo BW, Zhu J, Hirsch JA. An update of comprehensive evidence-based guidelines for interventional techniques in chronic spinal pain. Part II: Guidance and recommendations. Pain Physician 2013; 16:S49- S Tam NL, Pac-Soo C, Pretorius PM. Epidural haematoma after a combined spinal-epidural anaesthetic in a patient treated with clopidogrel and dalteparin. Br J Anaesth 2006; 96: Benzon HT, Wong HY, Siddiqui T, Ondra S. Caution in performing epidural injections in patients on several antiplatelet drugs. Anesthesiology 1999; 91: Maier C, Gleim M, Weiss T, Stachetzki U, Nicolas V, Zenz M. Severe bleeding following lumbar sympathetic blockade in two patients under medication with irreversible platelet aggregation inhibitors. Anesthesiology 2002; 97: Endres S, Shufelt A, Bogduk N. The risks of continuing or discontinuing anticoagulants for patients undergoing common interventional pain procedures. Pain Med 2017;18: Goodman BS, McLean House L, Vallabhaneni S, Mallempati S, Willey MR, 442
7 Continuing Anti-thrombotic Medication during Spinal Procedures Smith MT. Anticoagulation and antiplatelet management for spinal procedures: A prospective, descriptive study and interpretation of guidelines. Pain Med 2016; in press. 10. Manchikanti L, Malla Y, Wargo BW, Cash KA, McManus CD, Damron KS, Jackson SD, Pampati V, Fellows B. A prospective evaluation of bleeding risk of interventional techniques in chronic pain. Pain Physician 2011; 14: Agresti A, Coull B. Approximate is better than exact for interval estimation of binomial proportions. Am Statistician 1998; 52: Horlocker TT, Wedel DJ, Schroeder DR, Rose SH, Elliott BA, McGregor DG, Wong GY. Preoperative antiplatelet therapy does not increase the risk of spinal hematoma associated with regional anesthesia. Anesth Analg 1995; 80: Horlocker TT, Bajwa ZH, Ashraf Z, Khan S, Wilson JL, Sami N, Peeters-Asdourian C, Powers CA, Schroeder DR, Decker PA, Warfield CA. Risk assessment of hemorrhagic complications associated with nonsteroidal antiinflammatory medications in ambulatory pain clinic patients undergoing epidural steroid injection. Anesth Analg 2002; 95: , table of contents
8
CLINICAL GUIDELINES. Update Summary
 CLINICAL GUIDELINES CDI Quality Institute Anticoagulation and Antiplatelet Guidelines for Patients Undergoing Percutaneous Image-Guided Needle Procedures: An Update Concerning Facet Joint Injections, Medial
CLINICAL GUIDELINES CDI Quality Institute Anticoagulation and Antiplatelet Guidelines for Patients Undergoing Percutaneous Image-Guided Needle Procedures: An Update Concerning Facet Joint Injections, Medial
The Risks of Continuing or Discontinuing Anticoagulants for Patients Undergoing Common Interventional Pain Procedures
 Pain Medicine 2017; 18: 403 409 doi: 10.1093/pm/pnw108 SPINE SECTION Original Research Article The Risks of Continuing or Discontinuing Anticoagulants for Patients Undergoing Common Interventional Pain
Pain Medicine 2017; 18: 403 409 doi: 10.1093/pm/pnw108 SPINE SECTION Original Research Article The Risks of Continuing or Discontinuing Anticoagulants for Patients Undergoing Common Interventional Pain
Sacroiliac Joint Intraarticular Injection in True Anteroposterior View: Description of a New C-Arm Guided Method
 Pain Physician 2018; 21:61-66 ISSN 1533-3159 Case Series Sacroiliac Joint Intraarticular Injection in True Anteroposterior View: Description of a New C-Arm Guided Method Arman Taheri, MD 1, Mahbod Lajevardi,
Pain Physician 2018; 21:61-66 ISSN 1533-3159 Case Series Sacroiliac Joint Intraarticular Injection in True Anteroposterior View: Description of a New C-Arm Guided Method Arman Taheri, MD 1, Mahbod Lajevardi,
A Prospective Randomized Noninferiority Trial Comparing Upper and Lower One-Third Joint Approaches for Sacroiliac Joint Injections
 Pain Physician 2018; 21:251-257 ISSN 1533-3159 Randomized Trial A Prospective Randomized Noninferiority Trial Comparing Upper and Lower One-Third Joint Approaches for Sacroiliac Joint Injections Sang Hyun
Pain Physician 2018; 21:251-257 ISSN 1533-3159 Randomized Trial A Prospective Randomized Noninferiority Trial Comparing Upper and Lower One-Third Joint Approaches for Sacroiliac Joint Injections Sang Hyun
Post-procedure dose ok after hours. 12 hours (q 24h dosing only) assuming surgical hemostasis; second dose 24 hours after first dose.
 Medication Time to wait after last dose Post-procedure dose ok after hours Can pull catheter hours after last dose Can give next dose hours after pulling catheter Enoxaparin (Lovenox) Prophylactic dose
Medication Time to wait after last dose Post-procedure dose ok after hours Can pull catheter hours after last dose Can give next dose hours after pulling catheter Enoxaparin (Lovenox) Prophylactic dose
CLINICAL GUIDELINES. CMM-207: Epidural Adhesiolysis. Version Effective February 15, 2019
 CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
Maximizing Safety During Spine Interventions: Technique, Steroid Selection, and Anticoagulation Management
 Maximizing Safety During Spine Interventions: Technique, Steroid Selection, and Anticoagulation Management Byron J Schneider, MD, Assistant Professor PM&R Vanderbilt University Medical Center AOCPMR 2018
Maximizing Safety During Spine Interventions: Technique, Steroid Selection, and Anticoagulation Management Byron J Schneider, MD, Assistant Professor PM&R Vanderbilt University Medical Center AOCPMR 2018
Antiplatelet and Anticoagulant Therapy Management Surrounding Regional Anesthesia
 1 Antiplatelet and Anticoagulant Therapy Management Surrounding Regional Anesthesia Key Points: Neuraxial complications are extremely rare. Epidural hematomas are one possible complication of neuraxial
1 Antiplatelet and Anticoagulant Therapy Management Surrounding Regional Anesthesia Key Points: Neuraxial complications are extremely rare. Epidural hematomas are one possible complication of neuraxial
Anticoagulation Management Around Endoscopy: GI Perspective. Nathan Landesman, DO FACOI Flint Gastroenterology Associates October 11, 2017
 Anticoagulation Management Around Endoscopy: GI Perspective Nathan Landesman, DO FACOI Flint Gastroenterology Associates October 11, 2017 EDUCATIONAL OBJECTIVES Understand risks of holding anticoagulation
Anticoagulation Management Around Endoscopy: GI Perspective Nathan Landesman, DO FACOI Flint Gastroenterology Associates October 11, 2017 EDUCATIONAL OBJECTIVES Understand risks of holding anticoagulation
Fluoroscopically Guided Infiltration of the Cervical Nerve Root: An Indirect Approach Through the Ipsilateral Facet Joint
 Pain Physician 2014; 17:291-296 ISSN 1533-3159 Non-Randomized Study Fluoroscopically Guided Infiltration of the Cervical Nerve Root: An Indirect Approach Through the Ipsilateral Facet Joint Alexios Kelekis,
Pain Physician 2014; 17:291-296 ISSN 1533-3159 Non-Randomized Study Fluoroscopically Guided Infiltration of the Cervical Nerve Root: An Indirect Approach Through the Ipsilateral Facet Joint Alexios Kelekis,
Author Information. Case Information
 Author Information Full Names: Jonathan M. Hagedorn, MD Susan M. Moeschler, MD Affiliation: Mayo Clinic, Rochester, MN Email Contacts: jonhagedornmd@yahoo.com Moeschler.susan@mayo.edu Case Information
Author Information Full Names: Jonathan M. Hagedorn, MD Susan M. Moeschler, MD Affiliation: Mayo Clinic, Rochester, MN Email Contacts: jonhagedornmd@yahoo.com Moeschler.susan@mayo.edu Case Information
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Prostate Biopsy Alerts
 Prostate Biopsy Alerts Saskatchewan Prostate Assessment Pathway Guidelines for the Primary Care Provider for Patient Preparation and the Management of Medications and Complications September 2016 Table
Prostate Biopsy Alerts Saskatchewan Prostate Assessment Pathway Guidelines for the Primary Care Provider for Patient Preparation and the Management of Medications and Complications September 2016 Table
The Institute of Medicine report on relieving pain in America (1,2) showed the magnitude of pain in the
 Pain Physician 2013; 16:177-184 ISSN 1533-3159 Editorial Refinement in Evidence Synthesis of Percutaneous Adhesiolysis Standiford Helm II, MD 1, Ramsin M. Benyamin, MD 2, and Frank J.E. Falco, MD 3 The
Pain Physician 2013; 16:177-184 ISSN 1533-3159 Editorial Refinement in Evidence Synthesis of Percutaneous Adhesiolysis Standiford Helm II, MD 1, Ramsin M. Benyamin, MD 2, and Frank J.E. Falco, MD 3 The
A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case
 Pain Physician 2010; 13:145-150 ISSN 1533-3159 Medical-Legal Review A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case Standiford
Pain Physician 2010; 13:145-150 ISSN 1533-3159 Medical-Legal Review A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case Standiford
Comparison of 3 Approaches to Percutaneous Epidural Adhesiolysis and Neuroplasty in Post Lumbar Surgery Syndrome
 Pain Physician 2018; 21:E501-E508 ISSN 2150-1149 Case-Control Study Comparison of 3 Approaches to Percutaneous Epidural Adhesiolysis and Neuroplasty in Post Lumbar Surgery Syndrome Mert Akbas, MD 1, Abdel
Pain Physician 2018; 21:E501-E508 ISSN 2150-1149 Case-Control Study Comparison of 3 Approaches to Percutaneous Epidural Adhesiolysis and Neuroplasty in Post Lumbar Surgery Syndrome Mert Akbas, MD 1, Abdel
Key words: Rhizotomy, radiofrequency neurotomy, 2 needles, facet joint pain, low back pain, cadaveric tissue. Pain Physician 2010; 13:43-49
 Pain Physician 2010; 13:43-49 ISSN 1533-3159 Cadaveric Study The Efficacy of Two Electrodes Radiofrequency Technique: Comparison Study Using a Cadaveric Interspinous Ligament and Temperature Measurement
Pain Physician 2010; 13:43-49 ISSN 1533-3159 Cadaveric Study The Efficacy of Two Electrodes Radiofrequency Technique: Comparison Study Using a Cadaveric Interspinous Ligament and Temperature Measurement
Clinical Course of Cervical Percutaneous Epidural Neuroplasty in Single-Level Cervical Disc Disease with 12-Month Follow-up
 Pain Physician 2017; 20:E941-E949 ISSN 2150-1149 Retrospective Study Clinical Course of Cervical Percutaneous Epidural Neuroplasty in Single-Level Cervical Disc Disease with 12-Month Follow-up Chang Hyun
Pain Physician 2017; 20:E941-E949 ISSN 2150-1149 Retrospective Study Clinical Course of Cervical Percutaneous Epidural Neuroplasty in Single-Level Cervical Disc Disease with 12-Month Follow-up Chang Hyun
Medical Affairs Policy
 Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
Radiology guided treatment for spinal pain. Dr Paul O Connell
 Radiology guided treatment for spinal pain Dr Paul O Connell Image guided treatment for back pain Management of Acute radicular pain Chronic low back pain Facetal Sacro-iliac joint Cervicogenic headaches
Radiology guided treatment for spinal pain Dr Paul O Connell Image guided treatment for back pain Management of Acute radicular pain Chronic low back pain Facetal Sacro-iliac joint Cervicogenic headaches
Breast Biopsy on Therapeutic Anticoagulation. Dr Jillian Gardner MBBS, FRACGP, MPH&TM, CCFP, DCH Senior Medical Officer Head of Unit BreastScreen SA
 Breast Biopsy on Therapeutic Anticoagulation Dr Jillian Gardner MBBS, FRACGP, MPH&TM, CCFP, DCH Senior Medical Officer Head of Unit BreastScreen SA Outline: Breast biopsy on therapeutic anticoagulation
Breast Biopsy on Therapeutic Anticoagulation Dr Jillian Gardner MBBS, FRACGP, MPH&TM, CCFP, DCH Senior Medical Officer Head of Unit BreastScreen SA Outline: Breast biopsy on therapeutic anticoagulation
Increased Dose of Betamethasone for Transforaminal Epidural Steroid Injections Is Not Associated with Superior Pain Outcomes at 4 Weeks
 Pain Physician 2015; 18:E355-E361 ISSN 2150-1149 Retrospective Evaluation Increased Dose of Betamethasone for Transforaminal Epidural Steroid Injections Is Not Associated with Superior Pain Outcomes at
Pain Physician 2015; 18:E355-E361 ISSN 2150-1149 Retrospective Evaluation Increased Dose of Betamethasone for Transforaminal Epidural Steroid Injections Is Not Associated with Superior Pain Outcomes at
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/ /01/ /17/2017
 MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
5/31/2013. Disclosures. Lumbar Facet Joint Pain: Evidence. I have nothing to disclose
 Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011
 Pain Physician 2014; 17:E129-E139 ISSN 2150-1149 Health Policy Review Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011 Laxmaiah
Pain Physician 2014; 17:E129-E139 ISSN 2150-1149 Health Policy Review Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011 Laxmaiah
Coagulation management in epidural steroid injection
 PRACE POGLĄDOWE Anestezjologia Intensywna Terapia 2014, tom 46, numer 3, 209 213 ISSN 0209 1712 www.ait.viamedica.pl Coagulation management in epidural steroid injection Martina Bellini, Massimo Barbieri
PRACE POGLĄDOWE Anestezjologia Intensywna Terapia 2014, tom 46, numer 3, 209 213 ISSN 0209 1712 www.ait.viamedica.pl Coagulation management in epidural steroid injection Martina Bellini, Massimo Barbieri
A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up
 Pain Physician 2015; 18:79-92 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up Laxmaiah
Pain Physician 2015; 18:79-92 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up Laxmaiah
The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of Follow-up
 Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
NEURAXIAL BLOCKADE AND ANTICOAGULANTS
 Soli Deo Gloria NEURAXIAL BLOCKADE AND ANTICOAGULANTS Lecture 4 Developing Countries Regional Anesthesia Lecture Series Daniel D. Moos CRNA, Ed.D. U.S.A. moosd@charter.net Disclaimer Every effort was made
Soli Deo Gloria NEURAXIAL BLOCKADE AND ANTICOAGULANTS Lecture 4 Developing Countries Regional Anesthesia Lecture Series Daniel D. Moos CRNA, Ed.D. U.S.A. moosd@charter.net Disclaimer Every effort was made
The Role of Gabapentin in the Prevention of Postoperative Neuritis following Radiofrequency Ablation of Cervical and Lumbar Medial Branch Nerves
 Original article: The Role of Gabapentin in the Prevention of Postoperative Neuritis following Radiofrequency Ablation of Cervical and Lumbar Medial Branch Nerves *Sean W. Welsh, MD, Susan Varner, NP,
Original article: The Role of Gabapentin in the Prevention of Postoperative Neuritis following Radiofrequency Ablation of Cervical and Lumbar Medial Branch Nerves *Sean W. Welsh, MD, Susan Varner, NP,
Clinical Policy: Lysis of Epidural Lesions Reference Number: CP.MP.116
 Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Antiplatelets and Anticoagulants. Helen Leung, PharmD PGY1 Pharmacy Resident Memorial Hermann-Texas Medical Center
 Antiplatelets and Anticoagulants Helen Leung, PharmD PGY1 Pharmacy Resident Memorial Hermann-Texas Medical Center Mechanism 2 http://www.medicinehack.com/2011/07/virchows-triad.html Mechanism 3 http://drtedwilliams.net/kb/index.php?pagename=coagulation%20cascade
Antiplatelets and Anticoagulants Helen Leung, PharmD PGY1 Pharmacy Resident Memorial Hermann-Texas Medical Center Mechanism 2 http://www.medicinehack.com/2011/07/virchows-triad.html Mechanism 3 http://drtedwilliams.net/kb/index.php?pagename=coagulation%20cascade
FACET JOINT INJECTIONS Version 18.0; Effective
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Guideline for Patients on antiplatelet agents undergoing Elective, Non-cardiac
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Guideline for Patients on antiplatelet agents undergoing Elective, Non-cardiac
Disclosures. Overview. Have you ever. The Perioperative Management of Anticoagulants. No financial conflicts of interest to disclose
 Disclosures No financial conflicts of interest to disclose The Perioperative Management of Anticoagulants Margaret C. Fang, MD, MPH Associate Professor of Medicine UCSF Division of Hospital Medicine Medical
Disclosures No financial conflicts of interest to disclose The Perioperative Management of Anticoagulants Margaret C. Fang, MD, MPH Associate Professor of Medicine UCSF Division of Hospital Medicine Medical
CLINICAL GUIDELINES. CMM-201 ~ Facet Joint Injections. Version 19.0 Effective August 11, 2017
 CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
ADVOCATE HEALTHCARE GUIDELINE FOR ANTITHROMBOTIC REVERSAL
 Minimal clinical evidence exists to support the efficacy of nonspecific procoagulant therapies that promote thrombin formation and antifibrinolytics in the setting of antithrombotic-related bleeding. Hemostatic
Minimal clinical evidence exists to support the efficacy of nonspecific procoagulant therapies that promote thrombin formation and antifibrinolytics in the setting of antithrombotic-related bleeding. Hemostatic
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14, 06/18/15, 05/25/16, 05/18/17
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
SPECIAL REPORT. Deepak Gupta 1
 SPECIAL REPORT The American Society of Regional Anesthesia and Pain Medicine Guidelines for patients receiving medications that affect hemostasis: A clinical perspective Deepak Gupta 1 Abstract It is always
SPECIAL REPORT The American Society of Regional Anesthesia and Pain Medicine Guidelines for patients receiving medications that affect hemostasis: A clinical perspective Deepak Gupta 1 Abstract It is always
The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations
 Pain Physician 2010; 13:527-534 ISSN 1533-3159 Retrospective Study The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations Stephan Klessinger, MD From: Nova Clinic, Biberach, Germany
Pain Physician 2010; 13:527-534 ISSN 1533-3159 Retrospective Study The Benefit of Therapeutic Medial Branch Blocks after Cervical Operations Stephan Klessinger, MD From: Nova Clinic, Biberach, Germany
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Asif Serajian DO FACC FSCAI
 Anticoagulation and Antiplatelet update: A case based approach Asif Serajian DO FACC FSCAI No disclosures relevant to this talk Objectives 1. Discuss the indication for antiplatelet therapy for cardiac
Anticoagulation and Antiplatelet update: A case based approach Asif Serajian DO FACC FSCAI No disclosures relevant to this talk Objectives 1. Discuss the indication for antiplatelet therapy for cardiac
Title: RN Specialty Practice: RN Procedure: Epidural Catheter Removal. I.D. Number: 1080
 Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
Antithrombotics 201: Aspirin and USPSTF. Presented by: Craig Williams, PharmD., BCPS., FNLA; November, Conflicts of Interest: None
 Antithrombotics 201: Aspirin and USPSTF Presented by: Craig Williams, PharmD., BCPS., FNLA; November, 2016 Conflicts of Interest: None 1 What percent of patients who die within 30 days of an MI die before
Antithrombotics 201: Aspirin and USPSTF Presented by: Craig Williams, PharmD., BCPS., FNLA; November, 2016 Conflicts of Interest: None 1 What percent of patients who die within 30 days of an MI die before
UP TO AMA PRA CATEGORY 1 CREDITS
 EXCELLENCE IN EDUCATION FOR INTERVENTIONAL PAIN PHYSICIANS CADAVER WORKSHOP AND ONLINE VIDEO LECTURES BASIC, INTERMEDIATE, AND ABIPP PREPARATION FEBRUARY 1-2, 2014 IMAGING, FLUOROSCOPY, AND RADIATION SAFETY
EXCELLENCE IN EDUCATION FOR INTERVENTIONAL PAIN PHYSICIANS CADAVER WORKSHOP AND ONLINE VIDEO LECTURES BASIC, INTERMEDIATE, AND ABIPP PREPARATION FEBRUARY 1-2, 2014 IMAGING, FLUOROSCOPY, AND RADIATION SAFETY
Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
 Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians EXHIBITOR PROSPECTUS INTERVENTIONAL TECHNIQUES LUMBAR ENDOSCOPIC SPINAL DECOMPRESSION REGENERATIVE MEDICINE IN MUSCULOSKELTAL
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians EXHIBITOR PROSPECTUS INTERVENTIONAL TECHNIQUES LUMBAR ENDOSCOPIC SPINAL DECOMPRESSION REGENERATIVE MEDICINE IN MUSCULOSKELTAL
Lysis of Epidural Adhesions
 Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Contractor Information. LCD Information. FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836)
 FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
Antiplatelet and Anti-Thrombotic Therapy. Ivan Anderson, MD RIHVH Cardiology
 Antiplatelet and Anti-Thrombotic Therapy Ivan Anderson, MD RIHVH Cardiology Outline Anti-thrombotic therapy Risk stratification of stroke with atrial fibrillation DVT and PE treatment Pharmacology Anti-platelet
Antiplatelet and Anti-Thrombotic Therapy Ivan Anderson, MD RIHVH Cardiology Outline Anti-thrombotic therapy Risk stratification of stroke with atrial fibrillation DVT and PE treatment Pharmacology Anti-platelet
Laxmaiah Manchikanti, MD, Sneha Pampati, and Kimberly A. Cash, RT
 Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Preoperative Management of Patients Receiving Antithrombotics
 Preoperative Management of Patients Receiving Antithrombotics Bleeding complications remain an important concern for most surgical procedures. Attempts to minimize the risk of these complications by removing
Preoperative Management of Patients Receiving Antithrombotics Bleeding complications remain an important concern for most surgical procedures. Attempts to minimize the risk of these complications by removing
Oral anti-thrombotic therapy-management in patients requiring endoscopy
 Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Interventional Techniques
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians Interventional Techniques Comprehensive Review Course Up to 8 AMA PRA Category 1 Credits (Plus Free Online Lectures)
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians Interventional Techniques Comprehensive Review Course Up to 8 AMA PRA Category 1 Credits (Plus Free Online Lectures)
DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
 Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
Phillip Weidner, DO, DABA, BCPM May 20th, 2014
 Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
INTERVENTIONAL TECHNIQUES
 ASIPP EDUCATIONAL SERVICES EXCELLENCE IN THE EDUCATION OF INTERVENTIONAL PAIN PHYSICIANS INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE 7 AMA PRA Category 1 Credits (Plus Free Online Lectures) AND
ASIPP EDUCATIONAL SERVICES EXCELLENCE IN THE EDUCATION OF INTERVENTIONAL PAIN PHYSICIANS INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE 7 AMA PRA Category 1 Credits (Plus Free Online Lectures) AND
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians EXHIBITOR PROSPECTUS INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE AND CADAVER WORKSHOP LUMBAR ENDOSCOPIC
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians EXHIBITOR PROSPECTUS INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE AND CADAVER WORKSHOP LUMBAR ENDOSCOPIC
Xarelto (rivaroxaban) Prescriber Guide
 Xarelto (rivaroxaban) Prescriber Guide October 2018 PP-XAR-IE-0031 Contents Patient Alert Card 4 Dosing Recommendations 4 Stroke prevention in adult patients with non-valvular atrial fibrillation 4 Patients
Xarelto (rivaroxaban) Prescriber Guide October 2018 PP-XAR-IE-0031 Contents Patient Alert Card 4 Dosing Recommendations 4 Stroke prevention in adult patients with non-valvular atrial fibrillation 4 Patients
Peri-Procedural Management of Antithrombotic Agents
 u Peri-Procedural Management of Antithrombotic Agents An Integrated Care Pathway of the Collaborative Care Network Subject Matter Experts: Will Maxted, MD Veronica Kerner, PharmD Pathway Custodian: Pat
u Peri-Procedural Management of Antithrombotic Agents An Integrated Care Pathway of the Collaborative Care Network Subject Matter Experts: Will Maxted, MD Veronica Kerner, PharmD Pathway Custodian: Pat
CLINICAL GUIDELINES. CMM-201: Facet Joint Injections/Medial Branch Blocks. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
Cigna Medical Coverage Policies Musculoskeletal Facet Joint Injections/Medial Branch Blocks
 Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
CERVICAL DIAGNOSTIC MBB CERVICAL RF (RADIOFREQUENCY ABLATION)
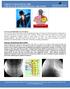 Overview and indications for procedures: Cervical Facet joints (also known as the Zygapophysial joints or Z-joints) are paired structures on both side of your spine that allows movement between two vertebrae.
Overview and indications for procedures: Cervical Facet joints (also known as the Zygapophysial joints or Z-joints) are paired structures on both side of your spine that allows movement between two vertebrae.
MEDICAL POLICY SUBJECT: RADIOFREQUENCY FACET DENERVATION
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Funding: The ASRA Consensus Conference was funded by unrestricted educational grants from: Pharmacia & Upjohn Company and Aventis Pharmaceuticals
 Regional Anesthesia in the Anticoagulated Patient - Defining the Risks Published by the American Society of Regional Anesthesia and Pain Medicine This document has been developed by a Consensus Conference
Regional Anesthesia in the Anticoagulated Patient - Defining the Risks Published by the American Society of Regional Anesthesia and Pain Medicine This document has been developed by a Consensus Conference
INTERVENTIONAL TECHNIQUES
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE (Plus Free Online Lectures) AND CADAVER WORKSHOP OCTOBER 5-7,
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE (Plus Free Online Lectures) AND CADAVER WORKSHOP OCTOBER 5-7,
Safety of Arthrocentesis and Joint Injection in Patients Receiving Anticoagulation at Therapeutic Levels
 CLINICAL RESEARCH STUDY Safety of Arthrocentesis and Joint Injection in Patients Receiving Anticoagulation at Therapeutic Levels Imdad Ahmed, MBBS, a,b Elie Gertner, MD a,b a Department of Internal Medicine,
CLINICAL RESEARCH STUDY Safety of Arthrocentesis and Joint Injection in Patients Receiving Anticoagulation at Therapeutic Levels Imdad Ahmed, MBBS, a,b Elie Gertner, MD a,b a Department of Internal Medicine,
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA Mailstop: CA
 To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
Regional anaesthesia and antithrombotic drugs
 Regional anaesthesia and antithrombotic drugs G Davies FRCA MR Checketts FRCA Matrix references 1A02, 2G01 Key points Vertebral canal haematoma is a rare but potentially devastating complication of central
Regional anaesthesia and antithrombotic drugs G Davies FRCA MR Checketts FRCA Matrix references 1A02, 2G01 Key points Vertebral canal haematoma is a rare but potentially devastating complication of central
Nanik Hatsakorzian Pharm.D/MPH
 Pharm.D/MPH 2014 1 Therapeutics FDA indication & Dosing Clinical Pearls Anticoagulants Heparin Antiphospholipid antibody syndrome Cerebral thromboembolism Prosthetic heart valve Acute coronary syndrome
Pharm.D/MPH 2014 1 Therapeutics FDA indication & Dosing Clinical Pearls Anticoagulants Heparin Antiphospholipid antibody syndrome Cerebral thromboembolism Prosthetic heart valve Acute coronary syndrome
Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain Caused by Spinal Stenosis
 Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
A Prospective Evaluation of Psychotherapeutic and Illicit Drug Use in Patients Presenting with Chronic Pain at the Time of Initial Evaluation
 Pain Physician 2013; 16:E1-E13 ISSN 2150-1149 Prospective Evaluation A Prospective Evaluation of Psychotherapeutic and Illicit Drug Use in Patients Presenting with Chronic Pain at the Time of Initial Evaluation
Pain Physician 2013; 16:E1-E13 ISSN 2150-1149 Prospective Evaluation A Prospective Evaluation of Psychotherapeutic and Illicit Drug Use in Patients Presenting with Chronic Pain at the Time of Initial Evaluation
Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal Stenosis
 Pain Physician 2013; 16:E531-E536 ISSN 2150-1149 Retrospective Evaluation Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal
Pain Physician 2013; 16:E531-E536 ISSN 2150-1149 Retrospective Evaluation Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal
Change from lovenox to pradaxa
 P ford residence southampton, ny Change from lovenox to pradaxa 14-11-2017 We wanted to put out a friendly reminder that the Ask 3 Teach 3 (A3T3) initiative is indeed full swing. This is an multidisciplinary
P ford residence southampton, ny Change from lovenox to pradaxa 14-11-2017 We wanted to put out a friendly reminder that the Ask 3 Teach 3 (A3T3) initiative is indeed full swing. This is an multidisciplinary
VENOUS THROMBOEMBOLISM PHARMACOLOGY. University of Hawai i Hilo DNP Program NURS 603 Advanced Clinical Pharmacology Danita Narciso Pharm D
 VENOUS THROMBOEMBOLISM PHARMACOLOGY University of Hawai i Hilo DNP Program NURS 603 Advanced Clinical Pharmacology Danita Narciso Pharm D LEARNING OBJECTIVES Know what factors anticoagulant medications
VENOUS THROMBOEMBOLISM PHARMACOLOGY University of Hawai i Hilo DNP Program NURS 603 Advanced Clinical Pharmacology Danita Narciso Pharm D LEARNING OBJECTIVES Know what factors anticoagulant medications
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
OUTPATIENT ANTITHROMBOTIC MANAGEMENT POST NON-ST ELEVATION ACUTE CORONARY SYNDROME. TARGET AUDIENCE: All Canadian health care professionals.
 OUTPATIENT ANTITHROMBOTIC MANAGEMENT POST NON-ST ELEVATION ACUTE CORONARY SYNDROME TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To review the use of antiplatelet agents and oral
OUTPATIENT ANTITHROMBOTIC MANAGEMENT POST NON-ST ELEVATION ACUTE CORONARY SYNDROME TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To review the use of antiplatelet agents and oral
Medial Branch Blocks
 Medial Branch Blocks What are medial branch blocks? Medial branch nerves are locates on the back of the spine on each side next to each facet joints. They send sensory signals to the brain regarding the
Medial Branch Blocks What are medial branch blocks? Medial branch nerves are locates on the back of the spine on each side next to each facet joints. They send sensory signals to the brain regarding the
Facet Joint Denervation. Populations Interventions Comparators Outcomes Individuals: With suspected facet joint pain
 Protocol Facet Joint Denervation (701116) Medical Benefit Effective Date: 01/01/16 Next Review Date: 11/18 Preauthorization Yes Review Dates: 09/09, 09/10, 07/11, 07/12, 05/13, 05/14, 01/15, 11/15, 11/16,
Protocol Facet Joint Denervation (701116) Medical Benefit Effective Date: 01/01/16 Next Review Date: 11/18 Preauthorization Yes Review Dates: 09/09, 09/10, 07/11, 07/12, 05/13, 05/14, 01/15, 11/15, 11/16,
Xarelto (rivaroxaban)
 Xarelto (rivaroxaban) Policy Number: 5.01.575 Last Review: 7/2018 Origination: 6/2014 Next Review: 7/2019 LoB: ACA Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Xarelto
Xarelto (rivaroxaban) Policy Number: 5.01.575 Last Review: 7/2018 Origination: 6/2014 Next Review: 7/2019 LoB: ACA Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Xarelto
Contractor Information. Proposed/Draft LCD Information
 PROPOSED/DRAFT Local Coverage Determination (LCD): Surgery: Epidural Steroid Injections (DL34364) Please note: This is a Proposed/Draft policy. Proposed/Draft LCDs are works in progress that are available
PROPOSED/DRAFT Local Coverage Determination (LCD): Surgery: Epidural Steroid Injections (DL34364) Please note: This is a Proposed/Draft policy. Proposed/Draft LCDs are works in progress that are available
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
CERVICAL EPIDURAL INJECTION
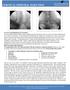 Overview and Indications for Procedure: Cervical epidural injection helps with a radiating pain from the neck to the arm often associated with herniated disc in the cervical spine. Cervical Epidural Steroid
Overview and Indications for Procedure: Cervical epidural injection helps with a radiating pain from the neck to the arm often associated with herniated disc in the cervical spine. Cervical Epidural Steroid
Conflicts of Interest: None. Aspirin, primary prevention and USPSTF. Primary prevention of ASCVD is important
 Aspirin, primary prevention and USPSTF Presented by: Craig Williams, PharmD., BCPS., FNLA; February 2017 Conflicts of Interest: None Primary prevention of ASCVD is important Myocardial Infarction Incidence
Aspirin, primary prevention and USPSTF Presented by: Craig Williams, PharmD., BCPS., FNLA; February 2017 Conflicts of Interest: None Primary prevention of ASCVD is important Myocardial Infarction Incidence
Technician Training Tutorial: Dispensing Oral Blood Thinners
 (Page 1 of 5) Technician Training Tutorial: Dispensing Oral Blood Thinners Warfarin (Coumadin, Jantoven-U.S., others) is an oral anticoagulant blood thinner used to help prevent blood clots that can lead
(Page 1 of 5) Technician Training Tutorial: Dispensing Oral Blood Thinners Warfarin (Coumadin, Jantoven-U.S., others) is an oral anticoagulant blood thinner used to help prevent blood clots that can lead
Section 12: Nerve damage associated with a spinal or epidural injection
 Risks associated with your anaesthetic Section 12: Nerve damage associated with a spinal or epidural injection Summary This leaflet explains the possibility of nerve damage occurring with your spinal or.
Risks associated with your anaesthetic Section 12: Nerve damage associated with a spinal or epidural injection Summary This leaflet explains the possibility of nerve damage occurring with your spinal or.
Effect of Cervical Interlaminar Epidural Steroid Injection: Analysis According to the Neck Pain Patterns and MRI Findings
 Original Article Korean J Pain 2016 April; Vol. 29, No. 2: 96-102 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.2.96 Effect of Cervical Interlaminar Epidural Steroid Injection:
Original Article Korean J Pain 2016 April; Vol. 29, No. 2: 96-102 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.2.96 Effect of Cervical Interlaminar Epidural Steroid Injection:
GENICULAR NERVE ABLATION
 Overview and Indications for Procedure: Osteoarthritis (OA) of the knee is the leading cause of knee pain in adults. Knee OA results in the thinning of the covering cartilage and remodeling of the knee
Overview and Indications for Procedure: Osteoarthritis (OA) of the knee is the leading cause of knee pain in adults. Knee OA results in the thinning of the covering cartilage and remodeling of the knee
3/23/2017. Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate Europace Oct;14(10): Epub 2012 Aug 24.
 Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Rhizolysis. Exceptional healthcare, personally delivered
 Rhizolysis Exceptional healthcare, personally delivered Your Doctor has requested that you have a rhizolysis procedure. We hope the following information will answer some of the questions you may have
Rhizolysis Exceptional healthcare, personally delivered Your Doctor has requested that you have a rhizolysis procedure. We hope the following information will answer some of the questions you may have
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017
 Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Outpatient Treatment of Deep Vein Thrombosis with Low Molecular Weight Heparin (LMWH) Clinical Practice Guideline August 2015
 Outpatient Treatment of Deep Vein Thrombosis with Low Molecular Weight Heparin (LMWH) Clinical Practice Guideline August 2015 General Principles: There is compelling data in the medical literature to support
Outpatient Treatment of Deep Vein Thrombosis with Low Molecular Weight Heparin (LMWH) Clinical Practice Guideline August 2015 General Principles: There is compelling data in the medical literature to support
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections
 Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
INTERVENTIONAL TECHNIQUES
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE (Plus Free Online Lectures) AND CADAVER WORKSHOP VENUE Loews
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians INTERVENTIONAL TECHNIQUES COMPREHENSIVE REVIEW COURSE (Plus Free Online Lectures) AND CADAVER WORKSHOP VENUE Loews
Survey of European Pain Medicine Practice
 Pain Physician 2012; 15:E983-E994 ISSN 2150-1149 Survey Survey of European Pain Medicine Practice Sanjeeva Gupta, MD, FRCA, FFPMRCA 1, Manish Gupta, FRCA 2, Sherdil Nath, MD, FRCA 3, and G. Michael Hess,
Pain Physician 2012; 15:E983-E994 ISSN 2150-1149 Survey Survey of European Pain Medicine Practice Sanjeeva Gupta, MD, FRCA, FFPMRCA 1, Manish Gupta, FRCA 2, Sherdil Nath, MD, FRCA 3, and G. Michael Hess,
October 22 Orlando, Florida
 ASIPP Educational Services Excellence in the education of Interventional Pain Physicians Interventional Techniques Cadaver Workshop Up to 8 AMA PRA Category 1 Credits Basic, Intermediate, and ABIPP Exam
ASIPP Educational Services Excellence in the education of Interventional Pain Physicians Interventional Techniques Cadaver Workshop Up to 8 AMA PRA Category 1 Credits Basic, Intermediate, and ABIPP Exam
Radiofrequency Ablation
 Radiofrequency Ablation Information for patients and families Read this booklet to learn: what radiofrequency ablation is how to prepare what to expect who to contact if you have any questions Your radiofrequency
Radiofrequency Ablation Information for patients and families Read this booklet to learn: what radiofrequency ablation is how to prepare what to expect who to contact if you have any questions Your radiofrequency
