DI D V I E V R E T R I T C I U C LA L R DI D S I EA E SE Dr Förhécz Zsolt
|
|
|
- Gerard Caldwell
- 6 years ago
- Views:
Transcription
1 DIVERTICULARDISEASE Dr Förhécz Zsolt
2 Diverticula: the formation of small bulging pouches out from the colon wall. The diverticula usually range in diameter from 5-10 mm, but it can exceed 2 cm. The medical condition that refers to the presence of diverticula is known as diverticulosis
3
4
5 Diet low in fiber results in low stool volume, which prolongs transit time. This low stool volume also causes an increase in intraluminal pressure based on LaPlace slaw (P [pressure] = kt[wall tension]/r[radius]), which states that there is an inverse relationship between intraluminal pressure and lumen diameter. This increased intraluminal pressure can in turn cause herniation of the colonic mucosa in areas of weakness such as the penetration point of vasa recta that supplies the submucosa and mucosa. This might explain the reason why diverticula are usually present in parallel rows.
6 RISK FACTORS ENVIRONMENTAL AND LIFESTYLE FACTORS ARE IMPORTANT RISK FACTORS FOR DIVERTICULAR DISEASE. Fiber The role of fiber in the development of diverticulosis is unclear. the risk of diverticular disease was significantly increased with diets that were low in fiber and were high in total fat or red meat Nut, corn, and popcorn consumption arenotassociated with an increase in risk of diverticulosis, diverticulitis or diverticular bleeding. Physical activity It is unclear if lack of vigorous exercise is a risk factor for diverticular disease. However, vigorous physical activity appears to reduce the risk of diverticulitis and diverticular bleeding. Obesity Obesity has been associated with an increase in risk of both diverticulitis and diverticular bleeding. Other Current smokers appear to be at increased risk for perforated diverticulitis and a diverticular abscess as compared with nonsmokers Caffeine and alcohol are not associated with an increased risk for symptomatic diverticular diseas Several medications are associated with an increased risk of diverticulitis and diverticular bleeding including nonsteroidal antiinflammatorydrugs, steroids, and opiates. In contrast, statins may be associated with a decreased risk of diverticular perforation
7
8 As a diverticulum herniates, the penetrating vessel responsible for the wall weakness at that point becomes draped over the dome of the diverticulum, separated from the bowel lumen only by mucosa.over time, the vasa recta is exposed to injury along its luminal aspect, leading to eccentric intimal thickening and thinning of the media. These changes may result in segmental weakness of the artery, predisposing to rupture into the lumen. DIVERTICULAR BLEEDING
9 The management of colonic diverticular bleeding includes resuscitation and, if the bleeding does not stop spontaneously, treatment of the bleeding site. If active bleeding or a visible vessel (similar to stigmata of ulcer hemorrhage) can be localized to a particular diverticulum during colonoscopy, endoscopic therapy can be attempted. Angiography is an alternative to colonoscopy for treatment in cases where the bleeding site cannot be identified with colonoscopy or if a bleeding site is identified but attempts to stop the bleeding endoscopically are unsuccessful. If the bleeding cannot be controlled with endoscopic or angiographic therapy, or if there is persistent instability despite aggressive resuscitation, surgery is typically required.
10 The underlying cause of diverticulitis is micro-or macroscopic perforation of a diverticulum. It was previously believed that obstruction of diverticula (eg, by fecaliths) increased diverticular pressure and caused perforation. However, such obstruction is now thought to be rare. The primary process is thought to be erosion of the diverticular wall by increased intraluminal pressure or inspissated food particles.inflammation and focal necrosis ensue, resulting in perforation DIVERTICULITIS
11 CLINICAL MANIFESTATIONS The clinical presentation of acute diverticulitis depends on the severity of the underlying inflammatory process and the presence of associated complications. The mean age at admission for acute diverticulitis is 63 years. While the incidence of acute diverticulitis is lower in younger individuals, approximately 16 percent of admissions for acute diverticulitis are in patients under 45 years of age
12 CLINICAL MANIFESTATIONS Abdominal pain is the most common complaint in patients with acute diverticulitis. The pain is usually in the left lower quadrant due to involvement of the sigmoid colon. However, patients may have right lower quadrant or suprapubic pain due to the presence of a redundant inflamed sigmoid colon or, much less commonly, right-sided (cecal) diverticulitis which has a higher incidence in Asian populations The pain is usually constant and is often present for several days prior to presentation.approximately 50 percent of patients have had one or more prior episodes of similar pain.
13 Nausea and vomiting (20 to 62 percent)due to a bowel obstruction or an ileus due to peritoneal irritation low grade fever Hemodynamic instability with hypotension and shock are rare and are associated with perforation and peritonitis. A tender mass is palpable in approximately( 20%) due to pericolonic inflammation or a peridiverticular abscess. localized peritoneal signs with localized guarding, rigidity, and rebound tenderness Rectal examination may reveal a mass or tenderness to palpation in the presence of a distal sigmoid abscess. Stool may be positive for occult blood change in bowel habits, with constipation reported in approximately 50% and diarrhea in 25 to 35 % Approximately 10 to 15 percent of patients with acute diverticulitis have urinary urgency, frequency, or dysuria due to irritation of the bladder from an inflamed sigmoid colon
14
15 A diverticular abscess may be noted on abdominal CT scan at initial presentation or may develop subsequently. A diverticular abscess should therefore be suspected in patients with uncomplicated diverticulitis who have no improvement in abdominal pain or a persistent fever despite three days of antibiotic treatment. DIVERTICULAR ABSCESSES OCCUR IN APPROXIMATELY 17 PERCENT OF PATIENTS HOSPITALIZED WITH ACUTE DIVERTICULITIS
16 because of relative luminal narrowing due to pericolonicinflammation or compression from a diverticular abscess. However, high-grade colonic obstruction is rare in the acute setting and is usually associated with the subsequent development of a stricture due to chronic diverticular inflammation also cause a small bowel obstruction if a loop of small intestine becomes incorporated in a pericolonic inflammatory mass OBSTRUCTION DURING AN ATTACK OF ACUTE DIVERTICULITIS, PARTIAL COLONIC OBSTRUCTION CAN OCCUR
17 colovesical fistula may have pneumaturia, fecaluria, or dysuria. colovaginal fistula may report vaginal passage of feces or flatus. FISTULA INFLAMMATION FROM ACUTE DIVERTICULITIS MAY RESULT IN THE FORMATION OF A FISTULA BETWEEN THE COLON AND ADJACENT VISCERA. FISTULAS MOST COMMONLY INVOLVE THE BLADDER
18 In patients with a free perforation, the abdomen is distended and diffusely tender to light palpation. There is diffuse guarding, rigidity, and rebound tenderness, and bowel sounds are absent. ALTHOUGH ONLY 1 TO 2 PERCENT OF PATIENTS WITH ACUTE DIVERTICULITIS HAVE A PERFORATION WITH PURULENT OR FECAL PERITONITIS, MORTALITY RATES APPROACH 20 PERCENT
19 mild leukocytosis. However, the white count may be normal in up to 45 percent of patients Serum amylase and lipase may be normal or mildly elevated, especially in patients with a free perforation and peritonitis. Urinalysis may reveal sterile pyuria due to adjacent inflammation. The presence of colonic flora on urine culture suggests the presence of a colovesical fistula LABORATORY FINDINGS
20 Computed tomography scan Computed tomography (CT) findings suggestive of acute diverticulitis include the presence of localized bowel wall thickening (>4 mm), an increase in soft tissue density within the pericolonicfat secondary to inflammation or fat stranding, and the presence of colonic diverticula IMAGING
21 Ultrasound features suggestive of acute diverticulitis include: A hypoechoic peridiverticular inflammatory reaction Mural and peridiverticular abscess formation with or without gas bubbles Bowel wall thickening(segmental mural thickening greaterthan4 mm) atthepointof maximaltenderness Presence of diverticula in the surrounding segments ABDOMINAL ULTRASOUND
22 Magnetic resonance imaging Abdominal magnetic resonance imaging (MRI) findings suggestive of acute diverticulitis include colonic wall thickening, presence of diverticula, and pericolonic exudates and edema Abdominal and chest radiographs Nonspecific abnormalities can be seen on abdominal radiographs in 30 to 50 percent of patients with acute diverticulitis. These findings include air-fluid levels with small or large intestinal dilation due to an ileus or obstruction and soft tissue densities due to the presence of an abscess.an upright chest radiograph may demonstrate the presence of pneumoperitoneumwith air under the diaphragm in 3 to 12 percent of patients with acute diverticulitis
23 Colorectalcancer Acuteappendicitis Inflammatory bowel disease Infectiouscolitis Ischemiccolitis DIFFERENTIAL DIAGNOSIS
24 Colonoscopy has no role in establishing the diagnosisof acute diverticulitis, as the inflammation is peridiverticular. Endoscopic evaluation of the colon should be avoided in the acute setting due to the risk of perforation or exacerbation of the existing inflammation. After the complete resolution of symptoms associated with acute diverticulitis (typically in six to eight weeks), a colonoscopy is performed, except for those who have had a colonoscopy within the previous yea EXCLUSION OF AN UNDERLYING MALIGNANCY
25 In patients with acute diverticulitis, mortality rates vary depending on the presence of complications and patient comorbidities. In patients with acute uncomplicated diverticulitis, conservative treatment is successful in 70 to 100 percent of patients and mortality is negligible In patients with complicated diverticulitis undergoing an operation,the mortality rate is approximately 0.6 to 5 percent Although mortality rates are up to 20 percent in patients with perforated diverticulitis with purulent or fecal peritonitis, these complications are rare in the absence of diffuse peritoniti MORTALITY
26 Patients with acute diverticulitis should receive inpatient treatment if CT showscomplicateddiverticulitisdefinedbythepresenceof perforation, abscess, obstruction, or fistulization. CT shows uncomplicated diverticulitis but the patient has one or more of the following characteristics: Sepsis Immunosuppression(eg, poorlycontrolleddiabetes mellitus, chronichigh-dosecorticosteroiduse, useof other immunosuppressive agents, advanced HIV infection, B or T cell leukocyte deficiency) High fever(>102.5 F/39 C) Significant leukocytosis Severe abdominal pain or diffuse peritonitis Advanced age Significant comorbidities Intolerance of oral intake Noncompliance/unreliability for return visits/lack of support system Failed outpatient treatment CRITERIA FOR INPATIENT TREATMENT
27 Antibiotics used to treat diverticulitis must cover the usualgastrointestinalfloraof Gram-negativerodsand anaerobes, particularly E. coli and B. fragilis We use one of the following outpatient antibiotic regimensin adultpatientswithnormalrenaland hepatic function: Ciprofloxacin(500 mg PO every12 hours) plusmetronidazole(500 mg PO every8 hours) Trimethoprim-sulfamethoxazole(1 double-strengthtablet [sulfamethoxazole800 mg;trimethoprim160 mg] every12 hours) plus metronidazole(500 mg PO every 8 hours) Amoxicillin-clavulanate(1 tablet [875 mgamoxicillin; 125 mg clavulanic acid] every 8 hours) or Augmentin XR (2 tablets[each tablet containing1 g amoxicillin; 62.5 mg clavulanicacid] every12 hours) Moxifloxacin(400 mg PO daily; usein patientsintolerantof both metronidazole and beta lactam agents) INITIAL OUTPATIENT CARE
28 The outpatient treatment of acute colonic diverticulitis typically consists of oral antibiotics for 7 to 10 days. Patients are reassessed clinically two to three days after the initiation of antibiotic therapy and weekly thereafter until the complete resolution of all symptoms. Repeat imaging studies arenotindicated unless the patient fails to improve clinically. Patients who fail outpatient treatment are admitted for inpatient treatment. OUTPATIENT TREATMENT
29 There is no evidence for dietary restrictions in acute uncomplicated diverticulitis. Some guidelines allow regular diet in patients who can tolerate it while others endorse a "modified" diet One approach is to limit patients to a clear liquid diet until they can be reassessed in two to three days, after which their diet can be liberalized to soft or regular if they demonstrate clinical improvement. OUTPATIENT DIET
30 Acute diverticulitis that presents with frank perforation is lifethreatening and mandates emergency surgery Microperforationshould be treated with intravenous antibiotics in a fashion that is similar to patients with uncomplicated diverticulitis. CT-guided drainage is typically performed for abscesses that are amenable to percutaneous drainage Abscesses not amenable to percutaneous drainage-patients who fail to improve after two to three days of antibiotic therapy will require surgery. Obstruction-surgicalresection of the involved bowel segment is mandatory to rule out cancer. Diverticular fistulas rarely close spontaneously, and a resection of the affected bowel segment is generally required. INPATIENTTREATMENTOF COMPLICATIONS
31 typically begins with administration of intravenous antibiotics, fluids, and pain medications. Patients are discharged with oral antibiotics to complete a course of 10 to 14 days Failure of inpatient medical treatment Surgery is indicated at any point during admission INPATIENTTREATMENTOF DIVERTICULITIS
32 After successful out-or inpatient treatment of acute diverticulitis, patients are reassessed in six to eight weeks. Those who have persistent symptoms may have chronic smoldering diverticulitis and are referred for surgical evaluation. Those who are symptom-free should undergo colonoscopy to rule out colon cancer. Patients who have had complicated diverticulitis or who are immunosuppressed should be referred for elective surgery, while others may be observed with dietary and behavioral modifications to reduce the risk of recurrence. Additionally, patients who reside in or frequently travel to remote areas that lack medical resources may benefit from elective surgery to reduce the risk of recurrences.
33 After nonoperative management of acute diverticulitis, patients have a 16 to 42 percent risk of developing recurrent diverticulitis. However, prior uncomplicated attacks do not predict a higher incidence nor a higher severity of recurrence. Thus, the number of prior attacks is no longer used as a sole criterion for surgery. Overall, approximately 20 percent of patients with acute diverticulitis will require surgical intervention at some time during the course of their disease because of symptoms, nearly all of whom have had either a complicated episode or several uncomplicated episodes of diverticulitis
34 COLONIC ISCHEMIA is the most frequent form of intestinal ischemia, most often affecting older adults. It is due to a reduction in blood flow to a level that is insufficient for the delivery of oxygen and nutrients needed for cellular metabolism. It can be related to acute arterial occlusion (embolic, thrombotic), venous thrombosis, or hypoperfusionof the mesenteric vasculature causing nonocclusive ischemia. The incidence is estimated at 16 cases per 100,000 person-years, which has increased over time The majority of patients have transient, nongangrenousischemia, which resolves without sequelae. Some patients develop colonic necrosis and gangrene, which can be lifethreatening. Long-term complications include persistent segmental colitis and the development of a stricture
35
36 of colonic ischemia vary depending upon the clinical setting and the extent and duration of the ischemia. Patients with acute colonic ischemia usually present with rapid onset of mild abdominal pain and tenderness over the affected bowel, most often the left colon. Mild-to-moderate amounts of rectal bleeding or bloody diarrhea usually develop within 24 hours of the onset of abdominal pain. Approximately 20 percent of patients develop chronic ischemic colitis. THE CLINICAL MANIFESTATIONS
37 Three progressive clinical stages have been described: Hyperactive phase Soon after occlusion or hypoperfusion, severe pain dominates with frequent passage of bloody, loose stools. Blood loss is usually mild without the need for transfusion. Paralytic phase The pain usually diminishes, becomes more continuous, and diffuses. The abdomen becomes more tender and distended without bowel sounds. Shock phase Massive fluid, protein, and electrolytes start to leak through a damaged, gangrenous mucosa. Severe dehydration with shock and metabolic acidosis may develop, requiring rapid surgical intervention. Fortunately, this most severe form affects only 10 to 20 percent of patients.
38 Laboratory studies are routinely obtained during the initial evaluation of the patient with abdominal pain or gastrointestinal bleeding, including complete blood count, metabolic panel, and coagulation studies. Although these are not diagnostic for colonic ischemia, they may aid the assessment of disease severity There are no specific laboratory markers for ischemia, although an increased serum lactate, lactate dehydrogenase (LDH), creatine phosphokinase (CPK), or amylase may indicate advanced tissue damage. Decreased hemoglobin levels may reflect intestinal blood loss LABORATORY STUDIES
39 Plain abdominal radiography A plain abdominal radiograph is frequently nonspecific signs such as signs such as thumbprinting (indicating submucosal edema) and hemorrhage could be identified in only 30 percent of patients with mesenteric infarction
40 Chronicischemiccolitis A protractedtimecourseand less severe symptoms distinguish these patients from those with acute colonic ischemia. Patients with episodes of chronic recurrent colonic ischemia can present with recurrent abdominal pain, bloody diarrhea, weightlossfromprotein-losingenteropathy, recurrent bacteremia, persistent sepsis, or symptomatic colonic strictures.
41
42 DIAGNOSIS A diagnosis of colonic ischemia is usually suspected based upon the history, physical examination, and clinical setting. It is confirmed with imaging when possible, typically with computed tomography (CT) of the abdomen. Suspicion for colonic ischemiashould be increased in patients (particularly in older adults) with any of the risk factors and with lower abdominal pain with bloody diarrhea or hematochezia; however, these symptoms are nonspecific, the presence of four or more risk factors (ie, older than 60, hemodialysis, hypertension, hypoalbuminemia, diabetes mellitus, constipation-inducing medications) was 100 percent predictive of colonic ischemia.
43 For patients who present with fulminant gangrenous colonic ischemia with peritonitisand/orcolon perforation, a definitive diagnosis will necessarily be made in the operating room. In certain acute settings and for those with chronic symptoms, lower endoscopy (sigmoidoscopy or colonoscopy) or arteriography may be used in an effort to identify colonic ischemia and differentiate it from other causes of abdominal pain and bloody stools
44 TREATMENT Supportive care Supportive care with bowel rest and observation is appropriate provided there is no evidence of colon perforation, necrosis, or gangrene. Intravenous fluids/infusioshould be given to ensure adequate colonic perfusion. A nasogastric tube should be inserted if an ileus is present. Any precipitating conditions should be treated, and medications known to promote intestinal ischemia (eg, vasopressors, digitalis) should be promptly discontinued if feasible. Cardiac function and oxygenation should be optimized.
45 Antibiotics There is no strong evidence supporting the routine use of antibiotics for the treatment of all patients with colonic ischemia. However, we agree with major society guidelines that suggest empiric broad-spectrum antibiotics for most patients with colonic ischemia, except possibly those with mild disease and no evidence for bleeding from ulceration
46 Antithrombotic therapy Antithrombotic therapy is not indicated for most patients with colonic ischemia, as the majority have nonocclusive ischemia. However, anticoagulant therapy is indicated for patients who develop ischemia due to mesenteric venous thrombosis or from cardiac thromboembolism
47 Surgery is required in up to 20 percent of cases Patients with colon infarction and necrosis require urgent surgical intervention, which can be life-saving Clinical suspicion of ischemia (eg, ongoing pain that is out of proportion to clinical examination, hemodynamic instability) is a common indication for surgical exploration. Other indications for abdominal exploration include endoscopic evidence of full-thickness irreversible necrosis of the colonic muscularisor lesser degrees of ischemia in patients who do not respond appropriately to nonsurgical supportive care Abdominal exploration
48 Prior to abdominal exploration (open or laparoscopic), bowel preparation should not be used, as it can precipitate perforation or toxic dilation of the colon. Once the abdomen is exposed (open or laparoscopic), the bowel should be systematically inspected from the ligament of Treitz to the peritoneal reflection overlying the rectum Second-look procedure In most cases following exploration or colonic resection, repeat exploration (ie, "second-look" operation [open or laparoscopic]) should be performed within 12 to 24 hours to assess the viability of the remaining bowel and integrity of any anastomose
49 Among patients with embolic or thrombotic arterial occlusion, pharmacomechanical thrombolysis with or without vascular angioplasty and stenting may be indicated. unlike mesenteric ischemia, embolectomy, bypass graft, or endarterectomy is not performed in cases of primary colonic ischemia, which is not generally related to large artery obstruction VASCULAR INTERVENTION
50 IRRITABLE BOWEL SYNDROME (IBS) Irritable bowel syndrome (IBS) is a functional disorder of the gastrointestinal tract characterized by chronic abdominal pain and altered bowel habits. The estimated prevalence of IBS globally is approximately 11 percent with a higher prevalence in younger individuals and in women. IBS is associated with other conditions including fibromyalgia, chronic fatigue syndrome(also known as systemic exertionintolerancedisease), gastroesophagealreflux disease, functional dyspepsia, non-cardiac chest pain, and psychiatric disorders including major depression, anxiety, and somatization
51 PATHOPHYSIOLOGY OF IRRITABLE BOWEL SYNDROME Although motor abnormalities of the gastrointestinal tract (increased frequency and irregularity of luminal contractions, abnormal transit time) are detectable in some patients with IBS, no predominant pattern of motor activity has emerged as a marker for IBS. Selective hypersensitization of visceral afferent nerves in the gut has been observed in patients with IBS and is one explanation for IBS symptoms. Immunohistologicinvestigation has revealed mucosal immune system activation characterized by alterations in particular immune cells and markers in some patients with IBS.
52 The development of IBS following infectious gastroenteritis has been suspected clinically based upon a history of an acute diarrheal illness preceding the onset of irritable bowel symptoms in some patients. The cause of bowel symptoms following acute infection is uncertain although several theories (malabsorption, increased enteroendocrinecells/lymphocytes,and antibiotic use) have been proposed. The complex ecology of the fecal microflora has led to speculation whether changes in its composition could be associated with IBS. An association between IBS and small intestinal bacterial overgrowth has been conflicting. The role of food in the pathophysiology of IBS is not clear. Investigations have centered on the development of food specific antibodies, carbohydrate malabsorption, and gluten sensitivity. A genetic susceptibility to IBS is suggested by several twin studies, although familial patterns may also reflect underlying social factors. Associations between specific genes and IBS are under investigation. Psychosocial factors may influence the expression of IBS symptoms.
53 CLINICAL MANIFESTATIONS Abdominal pain in IBS is usually described as a cramping sensation with variable intensity and periodic exacerbations. The pain is frequently related to defecation. While in some patients abdominal pain is relieved with defecation, a substantial portion of patients report worsening of pain with defecation. Symptoms of IBS include diarrhea, constipation, alternating diarrhea and constipation, or normal bowel habits alternating with either diarrhea and/or constipation. Diarrhea is usually characterized as frequent loose stools of small to moderate volume. Bowel movements generally occur during waking hours, most often in the morning or after meals. Patients may have constipation with interludes of diarrhea or normal bowel function.
54 DIAGNOSTIC CRITERIA IN THE ABSENCE OF A BIOLOGIC DISEASE MARKER, SEVERAL SYMPTOM-BASED CRITERIA HAVE BEEN PROPOSED TO STANDARDIZE THE DIAGNOSIS OF IBS. Rome IV criteria for IBS IBS is defined as recurrent abdominal pain, on average, at least one day per week in the last three months, associated with two or more of the following criteria: Related to defecation Associated with a change in stool frequency Associated with a change in stool form (appearance)
55 IBS subtypes Subtypes of IBS are recognized based on the patient's reported predominant bowel habit on days with abnormal bowel movements. The Bristol stool form scale (BSFS) should be used to record stool consistency. IBS subtypes are defined for clinical practice as follows: IBS with predominant constipation: Patient reports that abnormal bowel movements are usually constipation (type 1 and 2 in the BSFS) IBS with predominant diarrhea: Patient reports that abnormal bowel movements are usually diarrhea (type 6 and 7 in the BSFS) IBS with mixed bowel habits: Patient reports that abnormal bowel movements are usually both constipation and diarrhea (more than one-fourth of all the abnormal bowel movements were constipation and more than one-fourth were diarrhea) IBS unclassified: Patients who meet diagnostic criteria for IBS but cannot be accurately categorized into one of the other three subtypes.
56 INITIAL EVALUATION in all patients with suspected IBS includes a history and physical examination, and limited testing to evaluate for the presence of alarm features concerning for organic disease(medical history!) In all patients with suspected IBS, we perform a complete blood count and age appropriate colorectal cancer screening. In patients with diarrhea, we perform the following: -C-reactive protein or fecal calprotectin -Serologic testing for celiac disease
57 ALARM FEATURES CONCERNING FOR UNDERLING ORGANIC DISEASE INCLUDE: Age of onset after age 50 years Rectal bleeding or melena Nocturnal diarrhea Progressive abdominal pain Unexplained weight loss Laboratory abnormalities (iron deficiency anemia, elevated C-reactive protein or fecal calprotectin) Family history of inflammatory bowel disease or colorectal cancer In patients who meet diagnostic criteria for IBS and have no alarm features, we do not routinely perform any additional testing beyond the initial evaluation In patients with alarm features, we perform additional evaluation to exclude other causes of similar symptoms. The diagnostic evaluation is based on the clinical presentation and usually includesendoscopic evaluation in all patients and imaging in selected cases
58 Most patients with IBS have chronic symptoms that vary in severity over time. Patients may also experience a change in IBS subtype over time with the most frequent change being from predominant constipation or diarrhea to mixed bowel habits
59 Establishment of a clinician-patient relationship and continuity of care are critical to the management of all patients with irritable bowel syndrome (IBS). In patients with mild and intermittent symptoms that do not impair quality of life, we initially recommend lifestyle and dietary modification alone rather than specific pharmacologic agents INITIAL THERAPY
60 A careful dietary history may reveal patterns of symptoms related to specific foods. Patients with IBS may benefit from exclusion of gas-producing foods; a diet low in fermentable oligo-, di-, and monosaccharides and polyols (FODMAPs); and in select cases, lactose and gluten avoidance. Food allergy testing The role of food allergy in IBS is unclear Physical activity Physical activity should be advised DIETARY MODIFICATION
61 ADJUNCTIVE PHARMACOLOGIC THERAPY WE TREAT PATIENTS WITH MODERATE TO SEVERE SYMPTOMS OF IRRITABLE BOWEL SYNDROME (IBS) THAT IMPAIR QUALITY OF LIFE WITH PHARMACOLOGIC AGENTS Constipation In patients with IBS with constipation(ibs-c) who have failed a trial of soluble fiber(eg, psyllium/ispaghula), we suggest polyethylene glycol(peg)/osmotic laxatives. We treat patients with persistent constipation despite treatment with PEG with lubiprostone or linaclotide. Diarrhea we use antidiarrheals(eg,loperamide) as initial treatment and use bile acid sequestrants as second-line therapy Abdominal pain and bloating In patients with abdominal pain due to IBS, we use antispasmodicson an as-needed basis. In patients with IBS with constipation, we initiate antispasmodics only if the abdominal pain persists despite treatment of constipation. In patients with persistent abdominal pain despite antispasmodics, we recommend a trial of antidepressants. In patients with moderate to severe IBS without constipation, particularly those with bloating, who have failed to respond to other therapies, we suggest a two-week trial of rifaximin Probiotics Probiotics are not routinely recommended in patients with IBS
62
8/29/2016 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW. LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES
 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULOSIS MEDICAL AND SURGICAL MANAGEMENT. Simon Radley Consultant Surgeon March 2013
 DIVERTICULOSIS MEDICAL AND SURGICAL MANAGEMENT Simon Radley Consultant Surgeon March 2013 Definitions Diverticulosis: presence of diverticulae Diverticular disease: diverticulae associated with symptoms
DIVERTICULOSIS MEDICAL AND SURGICAL MANAGEMENT Simon Radley Consultant Surgeon March 2013 Definitions Diverticulosis: presence of diverticulae Diverticular disease: diverticulae associated with symptoms
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Colon ischemia. ACG Clinical Guideline; Am J Gastroenterol 2015
 Colon ischemia ACG Clinical Guideline; Am J Gastroenterol 2015 Manifestations Acute, reversible Irreversible : gangrene, fulminant colitis/stricture formation, chronic ischemic colitis Recurrent sepsis
Colon ischemia ACG Clinical Guideline; Am J Gastroenterol 2015 Manifestations Acute, reversible Irreversible : gangrene, fulminant colitis/stricture formation, chronic ischemic colitis Recurrent sepsis
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
12 Blueprints Q&A Step 2 Surgery
 12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
Colon ischemia. Bible class 12 September Stefan Christen. ACG Clinical Guideline: Am J Gastroenterol 2015
 Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
General Data. 王 X 村 78 y/o 男性
 General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #10 Acute GI Bleeds
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #10 Acute GI Bleeds Gastrointestinal bleeding is a very common problem in emergency medicine. Between
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #10 Acute GI Bleeds Gastrointestinal bleeding is a very common problem in emergency medicine. Between
When should we operate for recurrent diverticulitis. Savvas Papagrigoriadis MD MSc FRCS Consultant Colorectal Surgeon King's College Hospital
 When should we operate for recurrent diverticulitis Savvas Papagrigoriadis MD MSc FRCS Consultant Colorectal Surgeon King's College Hospital ASCRS Practice parameters for the Treatment of Acute Diverticulitis
When should we operate for recurrent diverticulitis Savvas Papagrigoriadis MD MSc FRCS Consultant Colorectal Surgeon King's College Hospital ASCRS Practice parameters for the Treatment of Acute Diverticulitis
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
Irritable Bowel Syndrome Now. George M. Logan, MD Friday, May 5, :35 4:05 PM
 Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
Always keep it in the differential
 Acute Appendicitis Lissa C. Sakata and Lindsey Perea 2 Always keep it in the differential Learning Objectives 1. The learner should be able to describe the etiology of acute appendicitis. 2. The learner
Acute Appendicitis Lissa C. Sakata and Lindsey Perea 2 Always keep it in the differential Learning Objectives 1. The learner should be able to describe the etiology of acute appendicitis. 2. The learner
Spectrum of Diverticular Disease. Outline
 Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
3/22/2011. Inflammatory Bowel Disease. Inflammatory Bowel Disease Objectives: Appendicitis. Lemone and Burke Chapter 26
 Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
A Trip Through the GI Tract: Common GI Diseases and Complaints. Jennifer Curtis, MD
 A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
Management of Diverticulitis. Sanjay Adusumilli MBBS MS FRACS
 Management of Diverticulitis Sanjay Adusumilli MBBS MS FRACS 0411 051 281 Trained by CSSANZ in Oxford (UK) and Perth Appointments at BMDH, HSS, Norwest Private and SAN Hospital Surgery performed: Laparoscopic
Management of Diverticulitis Sanjay Adusumilli MBBS MS FRACS 0411 051 281 Trained by CSSANZ in Oxford (UK) and Perth Appointments at BMDH, HSS, Norwest Private and SAN Hospital Surgery performed: Laparoscopic
The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix.
 The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix is located in the lower right portion of the abdomen. It has no known
The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix is located in the lower right portion of the abdomen. It has no known
Diverticular Disease Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
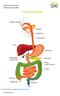 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS
 GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
The term inflammatory bowel disease is used to designate two related inflammatory intestinal disorders:
 3. Disorders of the Small and Large Intestines a. Irritable Bowel Syndrome: The term irritable bowel syndrome is used to describe a functional gastrointestinal disorder characterized by a variable combination
3. Disorders of the Small and Large Intestines a. Irritable Bowel Syndrome: The term irritable bowel syndrome is used to describe a functional gastrointestinal disorder characterized by a variable combination
ACUTE ABDOMEN. Dr. M Asadi. Surgical Oncology Research Center MUMS. Assistant Professor of General Surgery
 ACUTE ABDOMEN Dr. M Asadi Assistant Professor of General Surgery Surgical Oncology Research Center MUMS Definition I. The term Acute Abdomen refers to signs & symptoms of abdominal pain and tenderness,
ACUTE ABDOMEN Dr. M Asadi Assistant Professor of General Surgery Surgical Oncology Research Center MUMS Definition I. The term Acute Abdomen refers to signs & symptoms of abdominal pain and tenderness,
3/20/2009. Julio Garcia-Aguilar Chair, Department of Surgery City of Hope, Duarte, California
 Ischemic Colitis Ischemic Colitis Julio Garcia-Aguilar Chair, Department of Surgery City of Hope, Duarte, California Ischemic colitis (IC) represents greater than 50% of all intestinal ischemia IC most
Ischemic Colitis Ischemic Colitis Julio Garcia-Aguilar Chair, Department of Surgery City of Hope, Duarte, California Ischemic colitis (IC) represents greater than 50% of all intestinal ischemia IC most
What Is Diverticulitis?
 What Is Diverticulitis? By age 50, about half of people have diverticulosis, a health issue in which pockets (or diverticula) form in the wall of the large bowel. In about 5 percent of people, these pockets
What Is Diverticulitis? By age 50, about half of people have diverticulosis, a health issue in which pockets (or diverticula) form in the wall of the large bowel. In about 5 percent of people, these pockets
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider
 Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
Inflammatory Bowel Disease When is diarrhea not just diarrhea?
 Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Lower Gastrointestinal Tract KNH 406
 Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Diarrhoea on the AMU. Dr Chris Roseveare
 Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Surgical Education Series
 Surgical Education Series The Acute Abdomen Ahmad kachooei, MD MPH Assistant Professor Division of General Surgery Department of Surgery University of Qom Outline Definitions What causes an acute abdomen
Surgical Education Series The Acute Abdomen Ahmad kachooei, MD MPH Assistant Professor Division of General Surgery Department of Surgery University of Qom Outline Definitions What causes an acute abdomen
Irritable Bowel Syndrome. Mustafa Giaffer March 2017
 Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Colon Ischemia (CI): New Developments and Guidelines for Management. Spectrum of CI
 Colon Ischemia (CI): New Developments and Guidelines for Management Lawrence J. Brandt, MD, MACG Professor of Medicine and Surgery Albert Einstein College of Medicine Emeritus Chief of Gastroenterology
Colon Ischemia (CI): New Developments and Guidelines for Management Lawrence J. Brandt, MD, MACG Professor of Medicine and Surgery Albert Einstein College of Medicine Emeritus Chief of Gastroenterology
Surgery ~ Current Problems in. Colonic Diverticular Disease
 Current Problems in Surgery ~ Volume 37 Number 7 July 2000 Colonic Diverticular Disease II Foreword In Brief Biographic InFormation Introduction Epidemiologic and Pathophysiologic Features and Natural
Current Problems in Surgery ~ Volume 37 Number 7 July 2000 Colonic Diverticular Disease II Foreword In Brief Biographic InFormation Introduction Epidemiologic and Pathophysiologic Features and Natural
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
Is one of the most common chronic disorders. causing patients to seek medical treatment.
 ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
Historical perspective
 Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
IBS-D: The Role of Pathophysiology in Assessment and Treatment ReachMD Page 1 of 7
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
An Approach to Abdominal Pain
 An Approach to Abdominal Pain objectives Should know the different types of abd pain Is acute or chronic? Hx taking skills with knowing the key questions Important abdominal pain signs A good differential
An Approach to Abdominal Pain objectives Should know the different types of abd pain Is acute or chronic? Hx taking skills with knowing the key questions Important abdominal pain signs A good differential
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary
 Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
Lower GI bleeding. Aliu Sanni, MD Long Island College Hospital 17 th June, 2010
 Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University.
 Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
DIVERTICULAR DISEASE HANDS OFF OR HANDS ON?
 DIVERTICULAR DISEASE HANDS OFF OR HANDS ON? TE MADIBA AND M NAIDOO TE MADIBA MMed, LLM, PhD, FCS (SA), FASCRS Emeritus Professor of Surgery & Director of the Gastrointestinal Cancer Research Centre, University
DIVERTICULAR DISEASE HANDS OFF OR HANDS ON? TE MADIBA AND M NAIDOO TE MADIBA MMed, LLM, PhD, FCS (SA), FASCRS Emeritus Professor of Surgery & Director of the Gastrointestinal Cancer Research Centre, University
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
A Population-Based Analysis of the Clinical Course of Colonic Diverticulitis and its Evolving Management
 A Population-Based Analysis of the Clinical Course of Colonic Diverticulitis and its Evolving Management by Debbie Li A thesis submitted in conformity with the requirements for the degree of Masters of
A Population-Based Analysis of the Clinical Course of Colonic Diverticulitis and its Evolving Management by Debbie Li A thesis submitted in conformity with the requirements for the degree of Masters of
Clostridium Difficile Infection in Adults Treatment and Prevention
 Clostridium Difficile Infection in Adults Treatment and Prevention Definition: Clostridium Difficile colonizes the human intestinal tract after the normal gut flora has been altered by antibiotic therapy
Clostridium Difficile Infection in Adults Treatment and Prevention Definition: Clostridium Difficile colonizes the human intestinal tract after the normal gut flora has been altered by antibiotic therapy
Imaging abdominal vascular emergencies. V.Stoynova
 Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY
 Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY 15 FEB 2018 Sources Sources Sources Initial evaluation History Physical examination Laboratory evaluation Obtained at
Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY 15 FEB 2018 Sources Sources Sources Initial evaluation History Physical examination Laboratory evaluation Obtained at
Presenter. Irritable Bowel Syndrome. Objectives. Introduction. Rome Criteria. Irritable Bowel Syndrome 2/28/2018
 Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
X-Plain Sigmoidoscopy Reference Summary
 X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois
 ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 13:40-14:00
ENTEROCOLITIDES CAN YOU TELL THEM APART ON MDCT? Richard M. Gore, MD North Shore University Medical Center University of Chicago Evanston, Illinois SCBT/MR 2010 San Diego, California March 8, 2010 13:40-14:00
Christopher Lau Kings County Hospital SUNY Downstate Medical Center February 24, 2011
 Christopher Lau Kings County Hospital SUNY Downstate Medical Center February 24, 2011 37 year old male presented with 1 day history of abdominal pain Pain was diffuse but worst in the epigastric area No
Christopher Lau Kings County Hospital SUNY Downstate Medical Center February 24, 2011 37 year old male presented with 1 day history of abdominal pain Pain was diffuse but worst in the epigastric area No
Hits and Myths of Diverticulosis. JR Gray Gastoenterology UBC
 Hits and Myths of Diverticulosis JR Gray Gastoenterology UBC Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
Hits and Myths of Diverticulosis JR Gray Gastoenterology UBC Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
Gastroenterology Fellowship Program
 Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Chronic Abdominal Pain. Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016
 Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Nursing diagnosis for diverticular disease
 P ford residence southampton, ny Nursing diagnosis for diverticular disease Oct 18, 2010. Nursing Interventions: Diverticular Disease Administer antibiotics, stool softeners, and antispasmodics, as ordered.
P ford residence southampton, ny Nursing diagnosis for diverticular disease Oct 18, 2010. Nursing Interventions: Diverticular Disease Administer antibiotics, stool softeners, and antispasmodics, as ordered.
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Diagnosis and Management of Enterovesical Fistula
 Società Italiana di Chirurgia ColoRettale www.siccr.org 2009; 23: 200-210 Diagnosis and Management of Enterovesical Fistula Gitana Scozzari, Mario Morino Digestive Surgery and Center for Minimal Invasive
Società Italiana di Chirurgia ColoRettale www.siccr.org 2009; 23: 200-210 Diagnosis and Management of Enterovesical Fistula Gitana Scozzari, Mario Morino Digestive Surgery and Center for Minimal Invasive
Prof. Dr. Ahmed ElGeidie Professor of General surgery GEC Dr. Ahmed Abdelrafee
 Prof. Dr. Ahmed ElGeidie Professor of General surgery GEC Dr. Ahmed Abdelrafee Diverticulosis of the colon is the presence of pockets in the wall of the colon called diverticula which may, or may not,
Prof. Dr. Ahmed ElGeidie Professor of General surgery GEC Dr. Ahmed Abdelrafee Diverticulosis of the colon is the presence of pockets in the wall of the colon called diverticula which may, or may not,
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
GENI Program: GI and Abdominal Chief Complaints. Kim Macfarlane Clinical Nurse Specialist, Critical Care February 2008
 GENI Program: GI and Abdominal Chief Complaints Kim Macfarlane Clinical Nurse Specialist, Critical Care February 2008 Dehydration Common acute and chronic problem Recognition is critically important to
GENI Program: GI and Abdominal Chief Complaints Kim Macfarlane Clinical Nurse Specialist, Critical Care February 2008 Dehydration Common acute and chronic problem Recognition is critically important to
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
9/21/15. Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015
 Unless they prove otherwise. ~Every ED attending ever Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015 AAA with rupture Mesenteric
Unless they prove otherwise. ~Every ED attending ever Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015 AAA with rupture Mesenteric
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
COPYRIGHTED MATERIAL. 1 Approach to the patient with gross gastrointestinal bleeding. Grace H. Elta, Mimi Takami
 1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
F A M N O P R S ! D !
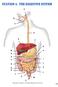 A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
CLINICAL VIGNETTE 2016; 2:1
 CLINICAL VIGNETTE 2016; 2:1 Editor-in-Chief: Olufemi E. Idowu. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria. MANAGEMENT OF APPENDICITIS Ibrahim NA, Njokanma
CLINICAL VIGNETTE 2016; 2:1 Editor-in-Chief: Olufemi E. Idowu. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria. MANAGEMENT OF APPENDICITIS Ibrahim NA, Njokanma
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review
 Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE
 ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
Cecal Volvulus: Case Presentation and Review of CT Findings
 August 2011 Cecal Volvulus: Case Presentation and Review of CT Findings Omar Pardesi, Harvard Medical School Year III Our Patient LD: History & Physical HPI: 28 y.o. female presents with diffuse abdominal
August 2011 Cecal Volvulus: Case Presentation and Review of CT Findings Omar Pardesi, Harvard Medical School Year III Our Patient LD: History & Physical HPI: 28 y.o. female presents with diffuse abdominal
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
INTRODUCTION TO DIAGNOSTIC ENDOSCOPY
 INTRODUCTION TO DIAGNOSTIC ENDOSCOPY EGD & Colonoscopy Procedure Kolegium Ilmu Bedah Indonesia B. Parish Budiono Sub Bagian Bedah Digestif FK UNDIP/RSUP Dr. Kariadi Semarang GI Endoscopy GI Endoscopy is
INTRODUCTION TO DIAGNOSTIC ENDOSCOPY EGD & Colonoscopy Procedure Kolegium Ilmu Bedah Indonesia B. Parish Budiono Sub Bagian Bedah Digestif FK UNDIP/RSUP Dr. Kariadi Semarang GI Endoscopy GI Endoscopy is
Diverticulosis Diverticulitis
 Diverticulosis Diverticulitis 28.02.2018 Ioannis Kapoglou/Riad Sarraj Universitätsklinik für Viszerale Medizin Gastroenterologie Epidemiology Diverticulosis / Diverticulitis 2 Epidemiology
Diverticulosis Diverticulitis 28.02.2018 Ioannis Kapoglou/Riad Sarraj Universitätsklinik für Viszerale Medizin Gastroenterologie Epidemiology Diverticulosis / Diverticulitis 2 Epidemiology
Case Presentation: Mr. S
 Case Presentation: Mr. S History Seen as inpatient in May, but has significant prior history and is a poor historian 53 y.o. Male no PMH, has been out of contact with medicine for years aside from hernia
Case Presentation: Mr. S History Seen as inpatient in May, but has significant prior history and is a poor historian 53 y.o. Male no PMH, has been out of contact with medicine for years aside from hernia
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
GASTROINESTINAL BLEEDING. Dr.Ammar I. Abdul-Latif
 GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
ONE of the most severe complications of diverticulitis of the sigmoid
 CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Colonic diverticulitis with perforation to region of left hip: a rare complication Report
CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Colonic diverticulitis with perforation to region of left hip: a rare complication Report
Gastroenterology Tutorial
 Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Clinical Questions. Clinical Questions. Clinical Questions. Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen
 Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen 1. What is an operational concept of acute abdomen? any abdominal condition of acute onset from various causes involving the intraabdominal
Health-Process-Evidencebased Clinical Practice Guidelines Acute Abdomen 1. What is an operational concept of acute abdomen? any abdominal condition of acute onset from various causes involving the intraabdominal
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Diverticulosis / Diverticulitis
 Diverticulosis / Diverticulitis Endoscopy Department Patient information leaflet You will only be given this leaflet if you have been diagnosed with Diverticulosis and / or Diverticulitis. The information
Diverticulosis / Diverticulitis Endoscopy Department Patient information leaflet You will only be given this leaflet if you have been diagnosed with Diverticulosis and / or Diverticulitis. The information
