Combined multichannel intraluminal impedance and. Characteristics of Consecutive Esophageal Motility Diagnoses After a Decade of Change
|
|
|
- Harvey Cain
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Characteristics of Consecutive Esophageal Motility Diagnoses After a Decade of Change Katherine Boland, BS,* Mustafa Abdul-Hussein, MD,* Radu Tutuian, MD,w and Donald O. Castell, MD* Background and Aims: Combined multichannel intraluminal impedance and esophageal manometry (MII-EM) measures concomitantly bolus transit and pressure changes allowing determination of the functional impact of esophageal motility abnormalities. Ten years ago our laboratory reported MII-EM results in 350 consecutive patients. Since then high-resolution impedance manometry (HRIM) became available and the definitions of ineffective esophageal motility (IEM) and nutcracker esophagus were revised. The aim of this study was to assess the impact of these developments on esophageal function testing. Methods: From August 2012 through May 2013, HRIM was performed in 350 patients referred for esophageal function testing. Each patient received 10 liquid and 10 viscous swallows. While taking advantage of the new technology and revised criteria, HRIM findings were classified according to the conventional criteria to allow more appropriate comparison with our earlier analysis. Results: Compared with the study performed 10 years ago, the prevalence of normal manometry (36% vs. 35%), achalasia (7% vs. 8%), scleroderma (1% vs. 1%), hypertensive lower esophageal sphincter (LES) (7% vs. 7%), and hypotensive LES (1% vs. 2%) remained the same, whereas the prevalence of distal esophageal spasm (9% vs. 3%), nutcracker esophagus (9% vs. 3%), and poorly relaxing LES (10% vs. 3%) decreased and the prevalence of IEM increased (20% vs. 31%) significantly. Compared with the early study, normal liquid bolus transit was significantly different in patients with hypertensive LES (96% vs. 57%) and poorly relaxing LES (55% vs. 100%). Conclusions: This study brings to light the increase in prevalence of IEM. In addition, it suggests that the hypertensive LES and poorly relaxing LES may each affect bolus transit in about half of these patients. Key Words: esophagus, motility, ineffective esophageal motility (J Clin Gastroenterol 2016;50: ) Combined multichannel intraluminal impedance and manometry (MII-EM) is a test of esophageal function that provides concomitant evaluation of bolus transit and pressure changes. First described by Silny in 1991, MII uses differences in resistance to alternating currents among air, Received for publication November 13, 2014; accepted July 21, From the *Department of Gastroenterology and Hepatology, Medical University of South Carolina, Charleston, SC; and wbern University Hospital, Bern, Switzerland. R.T.: Educational programs: MMS International, Sandhill Sci Inc., Almirall, Abbott and Advisory Board (Switzerland): Almirall, Sucampo, Diagnoplex. The remaining authors declare that they have nothing to disclose. Reprints: Katherine Boland, BS, 150 Bee Street, Apt 301, Charleston, SC ( bolandk@musc.edu). Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved. esophageal mucosa, and esophageal liquid bolus to detect bolus movement within the esophagus without the use of radiation. 1 Impedance is a useful addition to traditional esophageal liquid manometry testing as it provides bolus transit information in addition to pressure data, and normal values have been established for MII-EM. 2 The classification of esophageal motility abnormalities has evolved since Spechler and Castell s original classification based on manometry alone in 2001, 3 specifically the diagnostic criteria of ineffective esophageal motility (IEM) and the nutcracker esophagus have become more stringent. 4,5 Furthermore, high-resolution impedance manometry (HRIM), through more closely spaced pressure sensors along the catheter, allows more detailed measurements of the intraluminal pressures and through the color-coded pressure topography, provides a more accurate evaluation of the lower esophageal sphincter (LES) dynamics following deglutition. The interpretation of HRIM is still being refined. Because the data gathered from the pressure topography is user dependent, many clinicians convert the topography display back to convention line tracings. Thus, using all the tools available with this exciting technique allows for a more standardized measurement and ease in establishing a diagnosis. Ten years ago, 350 consecutive patients were evaluated in the Medical University of South Carolina esophageal motility laboratory for functional abnormalities using combined conventional MII-EM with intraluminal transducers at 5-cm intervals. 6 The aim of the current study was to evaluate and update the demographics and prevalence of the various manometric disorders with the updated definitions of IEM and the nutcracker esophagus, in addition to the increased accuracy provided by HRIM technology. METHODS This study retrospectively examined 350 consecutive prospectively collected HRIM studies performed in the esophageal laboratory at the Medical University of South Carolina from August 3, 2012 to May 15, Approval was obtained from our Institutional Review Board to review and analyze these studies and to publish the information obtained from them. All patients included in the study provided informed consent, giving the investigators permission to use their data for database research studies. Esophageal function testing was performed using a UNI-ESO-WG1A1 High-Resolution Impedance Manometry Probe (Sandhill Scientific Inc., Highlands Ranch, CO). The UNI-ESO-WG1A1 HRIM catheter has a 4 mm diameter and includes 32 circumferential pressure channels and 16 impedance channels. Solid state intraluminal pressure transducers are located at 6, 4, 3, 2, 1, 0, 1, J Clin Gastroenterol Volume 50, Number 4, April
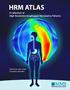
2 Boland et al J Clin Gastroenterol Volume 50, Number 4, April , 3, 4, 5, 6, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 19, 20, 21, 23, 24, 25, 26, 27, 28, 29, and 30 cm and impedance-measuring segments at 5, 3, 1, 1, 3, 5, 7, 9, 11, 13, 15, 17, 19, 21, 23, and 25 cm. The catheter was passed transnasally so that the zero point on the catheter was aligned with the maximal high-pressure zone of the LES. In the supine position, patients received 10 swallows of 5 ml normal saline and 10 swallows of 5 ml viscous (apple sauce like consistency) material each 20 to 30 seconds apart. The HRIM software can display data in either color-coded pressure topography Clouse plots or traditional waveform line plots. In this study, all data were acquired and visually assessed by HRIM, but numerically analyzed using conventional waveform line plots and interpreted using conventional manometry normals to standardize data analysis for comparison with our prior study of diagnostic distribution a decade earlier. 6 Manometric parameters used to characterize swallows included: (1) contraction amplitude at 5 and 10 cm above the LES; (2) distal esophageal amplitude (DEA) as the average of contraction amplitude at 5 and 10 cm above the LES; and (3) onset velocity of esophageal contractions in the distal part of the esophagus (ie, contraction velocity between 10 and 5 cm above the LES). Mid-respiratory resting pressure and LES residual pressure during swallowing were used to assess LES function. Impedance parameters included (1) bolus entries and exits 5, 10, 15, and 20 cm above the LES; and (2) total bolus transit time (TBTT), the time elapsed between bolus entry at 20 cm above the LES and bolus exit at 5 cm above the LES. Swallows were classified by manometry as (1) normal, if the contraction amplitudes 5 and 10 cm above the LES were each Z30 mm Hg and the distal-onset velocity was <8 cm/s; (2) ineffective, if either of the contraction amplitudes at 5 or 10 cm above the LES was <30 mm Hg; or (3) simultaneous, if the contraction amplitudes at 5 and 10 cm above the LES were each Z30 mm Hg and the distal-onset velocity was >8 cm/s. Swallows were classified by MII as showing complete bolus transit if bolus entry occurred at 20 cm above the LES; bolus exit points were recorded in the 3 distal impedance-measuring sites at 15, 10, and 5 cm above the LES, and the TBTT was <15 seconds. A swallow was classified as incomplete bolus transit if bolus exit was not identified at any of the 3 distal impedance-measuring sites, if bolus entry was not identified at 20 cm above the LES, or if the TBTT was >15 s. Overall, esophageal transit was defined as normal liquid transit if at least 80% of liquid swallows had complete bolus transit and as normal viscous transit if at least 70% of viscous swallows had complete bolus transit. 2 Manometry was evaluated for liquid swallows only because that has been standard worldwide for many years. Bolus transit, however, was evaluated for both liquid and viscous swallows. Diagnoses of manometric motility abnormalities for 8 named entities were established using the original criteria published by Spechler and Castell, 3 along with the more recently suggested changes in diagnostic criteria for IEM 4 and the nutcracker esophagus. 5 Achalasia was defined by absent esophageal body peristalsis and if present, poorly relaxing LES (residual pressure >8 mm Hg). The occasional hypertensive resting LES pressure reinforced this diagnosis. Scleroderma (SSc) was defined based on an appropriate clinical diagnosis and confirmed by low-amplitude contractions in the distal esophagus with or without a low LES pressure. Distal esophageal spasm (DES) was defined as Z20% simultaneous contractions. IEM was defined as Z50% swallows with contraction amplitude of <30 mm Hg in either of the 2 distal sites located at 5 and 10 cm above the LES. Mild IEM was defined by associated normal bolus transit for both liquid and viscous swallows, moderate IEM by abnormal bolus transit for either liquid or viscous swallows, and severe IEM by abnormal bolus transit for both liquid and viscous swallows. Nutcracker esophagus was defined as normal peristalsis of the esophageal body with an average DEA exceeding 220 mm Hg. Poorly relaxing LES was defined as average LES residual pressure exceeding 8 mm Hg associated with normal esophageal body contractions. Hypertensive LES was defined as an LES mid-respiratory resting pressure exceeding 45 mm Hg with normal esophageal body contractions. Normal esophageal manometry was defined as no more than 40% ineffective swallows, no more than 10% simultaneous swallows, a DEA < 220 mm Hg, and a normal LES resting and residual pressures. In patients having both esophageal body and LES abnormalities, the final diagnosis was based on the esophageal body finding. Major motility abnormality (MMA) is a MII-EM diagnosis that has evolved in our laboratory over the past 10 years; that is, since our prior report on diagnostic findings in the initial group of 350 patients. It is reserved for patients whose motility study is clearly abnormal but difficult to simply categorize into one of the 8 named motility abnormalities. It is also intended to inform the referring physician that the study is definitely abnormal. The final diagnosis on the report reads as Major motility abnormality with features of and and may include any combination of the following: achalasia, SSc, IEM, DES, or nutcracker esophagus. It is intended to be used sparingly. Figure 1 is a pressure tracing in which 90% of swallows show failed peristalsis, 10% of swallows are ineffective, and there is a normal residual pressure. This reading was read as MMA with features of achalasia and IEM. In this case, barium esophagram failed to reveal the classic features of achalasia. Patients were asked to fill out a questionnaire in which they described their major symptom, which was the reason for undergoing MII-EM. The symptoms included heartburn, dysphagia, regurgitation, chronic cough, chest pain or pressure, epigastric pain, hoarseness, throat clearing, and recurrent asthma attacks. Simple statistics were used to describe manometric and impedance characteristics in this group of patients. w 2 tests were used to assess differences in proportion of patients and/or swallows. Unpaired t tests were used to compare mean values of different diagnostic groups. For statistical significance a was set at RESULTS Three hundred and fifty patients (223 female, 116 male, mean age: 57.3 y, range 16 to 84 y) underwent esophageal function testing using HRIM between August 2012 and May While all patients received liquid swallows, 46 patients (10 normal manometry, 10 achalasia, 2 DES, 2 nutcracker, 13 IEM, 2 SSc, 3 hypertensive LES, 1 hypotensive LES, 3 MMA) requested discontinuation of the study before receiving viscous swallows. The primary symptoms for which patients were referred for esophageal function testing were: dysphagia (28%), chronic cough Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved.
3 J Clin Gastroenterol Volume 50, Number 4, April 2016 Characteristics of Consecutive Esophageal Motility FIGURE 1. Major motility abnormality with features of achalasia and ineffective esophageal motility. (15%), chest pain/pressure (12%), heartburn (11%), regurgitation (11%), epigastric pain (6%), throat clearing (6%), hoarseness (3%), asthma (3%), and other (6%). Dysphagia was the primary presenting symptom for patients diagnosed with achalasia (68%), nutcracker esophagus (33%), SSc (80%), DES (44%), and hypertensive LES (42%). The primary presenting symptom of IEM was cough (18%), hypotensive LES was regurgitation (33%) and cough (33%), and poorly relaxing LES was chest pain (22%) and cough (22%). Of the 76 patients presenting with dysphagia who had both liquid and viscous swallows performed, 28 (37%) had normal bolus transit, 2 FIGURE 2. A, Manometric diagnoses 2012 to B, Manometric diagnoses 2002 to DES indicates distal esophageal spasm; IEM, ineffective esophageal motility; LES, lower esophageal sphincter; MMA, major motility abnormality; SSc, scleroderma. FIGURE 3. Percentage of patients with normal bolus transit for liquid swallows based on manometric diagnoses. DES indicates distal esophageal spasm; IEM, ineffective esophageal motility; LES, lower esophageal sphincter; MMA, major motility abnormality; SSc, scleroderma. Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved
4 Boland et al J Clin Gastroenterol Volume 50, Number 4, April 2016 (3%) had abnormal bolus transit for liquid swallows, 4 (5%) had abnormal bolus transit for viscous swallows, and 42 (55%) had abnormal bolus transit for both liquid and viscous swallows. Detailed demographic features of all patients are shown in Table 1. Patients with IEM, nutcracker, hypertensive LES, and normal manometry were more frequently women (67%, 92%, 69%, 76%). However, only the prevalence of females with nutcracker esophagus was significantly different from the prevalence of females diagnosed with other esophageal abnormalities at the laboratory (P < 0.03). Patients across all categories were more frequently white; however, no single diagnosis was significantly different when compared with patients with other esophageal abnormalities. Manometric Findings Using Liquid Swallows 2012 to 2013 Of the 350 patients receiving liquid swallows, 121 (35%) had normal EM. On the basis of the above-mentioned manometric criteria, 28 (8%) had achalasia, 5 (1%) SSc, 110 (31%) IEM, 9 (3%) DES, 12 (3%) nutcracker esophagus, 26 (7%) hypertensive LES, 6 (2%) hypotensive LES, 9 (3%) poorly relaxing LES, and 24 (7%) MMA (Fig. 2A). Manometric Findings Using Liquid Swallows 2002 to 2003 Ten years ago, of the 350 patients who received liquid swallows from our laboratory, 125 (36%) had normal EM, 24 (7%) achalasia, 4 (1%) SSc, 71 (20%) IEM, 33 (9%) DES, 30 (9%) nutcracker esophagus, 25 (7%) hypertensive LES, 5 (1%) hypotensive LES, and 33 (9%) poorly relaxing LES (Fig. 2B). Combined Manometry and Impedance Findings 2012 to 2013 Figure 3 depicts the percentage of patients for each manometric diagnosis that had normal bolus transit for liquid swallows. Combined MII-EM for liquid swallows revealed that none of the patients with achalasia, SSc, or DES had normal bolus transit. Fifteen percent of patients with IEM had normal bolus transit, whereas a little over half of patients with hypertensive LES (57%), hypotensive LES (60%), and poorly relaxing LES (55%) had normal liquid bolus transit. Most patients with normal manometry (83%) and nutcracker esophagus (90%) had normal bolus transit for liquids. Combined Manometry and Impedance Findings 2002 to 2003 Our laboratory s previous study of combined MII-EM information for liquid swallows showed that none of the patients with achalasia or SSc had normal bolus transit. Fifty-one percent of patients with IEM and 55% of patients with DES had normal bolus transit, whereas almost all patients with normal EM (95%), nutcracker esophagus (97%), poorly relaxing LES (100%), hypertensive LES (96%), and hypotensive LES (100%) had normal liquid bolus transit. MMA Twenty-four patients were diagnosed with MMA. Of these 24 patients, 9 patients had characteristics of achalasia and IEM, 7 with achalasia and DES, 3 with SSc and IEM, 2 with achalasia and SSc, 2 with DES and IEM, and 1 with nutcracker esophagus and DES. IEM Demographics and Prevalence One hundred and ten patients with IEM were assessed using HRIM. Of these patients, 80 (73%) were white and 74 (67%) were female. Of the 97 patients receiving both liquid and viscous swallows, 11 (11%) patients had mild IEM, that is, normal bolus transit for liquid and viscous, 24 (25%) patients had moderate IEM with either abnormal liquid or abnormal viscous bolus transit, and 62 (64%) patients had severe IEM with abnormal liquid and viscous bolus transit. The primary symptoms for which IEM patients were referred for esophageal function testing were diverse and included: dysphagia (13%), chronic cough (18%), chest pain/pressure (12%), heartburn (14%), regurgitation (15%), epigastric pain (8%), throat clearing (5%), asthma (4%), and other (12%). DISCUSSION The results of this study using the HRIM catheter with the newer conventional diagnostic criteria for IEM and the nutcracker esophagus update the prevalence of esophageal abnormalities previously reported from our laboratory 10 years ago. 6 Despite the advent of the Chicago Classification System, this study used the conventional diagnostic criteria to standardize data analysis with our previous study. In the past decade, the prevalence of normal manometry, achalasia, SSc esophagus, hypertensive LES, and hypotensive LES have remained the same. However, nutcracker esophagus, poorly relaxing LES, IEM, and DES show TABLE 1. Demographic Parameters of all Patients Diagnosis Patients [n (%)] Female Patients [n (%)] Mean Age Age Range White [n (%)] Black [n (%)] Normal manometry 121 (35) 91 (76) (72) 22 (25) Achalasia 28 (8) 14 (50) (79) 6 (21) SSc 5 (1) 3 (60) (40) 3 (60) IEM 110 (31) 74 (67) (73) 29 (26) DES 9 (3) 4 (44) (100) 0 (0) Nutcracker 12 (3) 11 (92) (67) 3 (25) Hypertensive LES 26 (7) 18 (69) (73) 5 (19) Hypotensive LES 6 (2) 4 (67) (100) 0 (0) Poorly relaxing LES 9 (3) 4 (44) (56) 3 (33) MMA 24 (7) 12 (50) (67) 7 (29) DES indicates distal esophageal spasm; IEM, ineffective esophageal motility; LES, lower esophageal sphincter; MMA, major motility abnormality; SSc, scleroderma Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved.
5 J Clin Gastroenterol Volume 50, Number 4, April 2016 Characteristics of Consecutive Esophageal Motility significant changes in prevalence. Likewise, MMA as a diagnostic category has emerged and accounts for 7% of diagnoses made from this laboratory. The data show a decrease in the prevalence of the nutcracker esophagus from 9% ten years ago to 3% now (P < 0.002). This comes as no surprise as the manometric criteria for the diagnosis of nutcracker esophagus used in our laboratory became more stringent in the past 10 years from an average DEA > 180 mm Hg to an average DEA > 220 mm Hg for the 10 liquid swallows. However, it should be noted that of our 12 patients diagnosed with nutcracker esophagus, only 9 were diagnosed by conventional manometry standards. Three patients had DEAs slightly <220 mm Hg, but met Chicago Classification version high-resolution manometry requirements for nutcracker (mean DCI > 5000 mm Hg s cm). These observations suggest that perhaps the criteria for hypercontractile esophagus by HRIM have been set too low and are consistent with the most recent criterion suggested by the International Working Group 8 as well as a recent study from our laboratory. 9 Likewise, the prevalence of poorly relaxing LES decreased from 9% to 3% (P < ). With the advent of high-resolution manometry catheters, the closely spaced pressure sensors provide a more complete and accurate assessment of the LES, which essentially eliminates errors because of sensor placement or LES movement. Consequently, we believe that 3% is a more accurate assessment of the prevalence of poorly relaxing LES; however, 22 of the 26 patients diagnosed with hypertensive LES had a poorly relaxing LES, which could account for the decrease in prevalence. Surprisingly, we found an increase in the prevalence of IEM over the last decade (2004 IEM in 20% of patients, 2014 IEM in 31%; P < 0.001) despite the manometric criteria for IEM becoming more stringent, that is, requiring 5 of 10 instead of 3 of 10 contractions with an amplitude of <30 mm Hg in the distal esophagus. One would have expected the prevalence to decrease in a similar manner as the nutcracker esophagus findings. In addition, in comparing the rates of mild, moderate, and severe IEM to a study from our laboratory done 5 years ago, 10 the prevalence of severe IEM has increased from 47% to 63% (P < 0.01) among patients found to have IEM. These findings suggest that there is an increase in the prevalence as well as the severity of IEM. IEM is a frequent motility disorder in patients with gastroesophageal reflux disease (GERD) 11 and has been shown to increase in prevalence as the severity of reflux disease progresses from nonerosive reflux disease to erosive esophagitis to Barrett esophagus. 12 The most recent National Ambulatory Medical Care Survey documented that the rate of GERD-related doctor visits has nearly doubled from 1995 to Although it remains unclear whether GERD is a cause of IEM or vice versa, it is tempting to consider that the 2 increases in prevalence may be related. Diabetes, specifically diabetic autonomic neuropathy, has also been associated with esophageal dysmotility, decreased amplitudes of contraction, and abnormal wave forms. 14,15 As diabetes has increased in prevalence, especially in older adults, 16 within the past decade, it is also another possible explanation for the increase in IEM prevalence. Finally, the prevalence of DES has decreased from 9% to 3% (P < ), whereas neither the manometric criteria nor the technology have changed in making this diagnosis. Difficult to catch on manometry testing due to its sporadic and infrequent occurrence, DES is hard to diagnose and even harder to rule out of a differential. Furthermore, our laboratory has implemented rule #1, by which we believe that it is better to underdiagnose than to overdiagnose motility abnormalities. Clinical experience suggests that the term distal esophageal spasm in particular can often cloud other diagnoses. Consequently, tracings that suggest DES are examined with additional care to confirm that every DES diagnosis is strong (ie, borderline cases are adjusted to normal). Finally, the addition of the MMA category has captured some of the prior DES diagnoses. To compare bolus transit for liquid swallows to the earlier analysis completed 10 years ago, patients from the current study who had normal liquid impedance are shown in Figure 3. These results differ from the data gathered from our laboratory 10 years ago in 2 ways. First, the earlier study demonstrated that normal EM, nutcracker esophagus, poorly relaxing LES, hypertensive LES, and hypotensive LES all had normal bolus transit for liquid swallows in 95% of patients or greater. Although liquid bolus transit in nutcracker esophagus and hypotensive LES are not significantly different from 10 years ago, hypertensive LES, poorly relaxing LES, and normal manometry are all significantly different (P < 0.002). Consequently, this study s data do not support the conclusion made in our laboratory that esophageal body pressures are the main determinants of complete bolus transit. Instead, the data suggest that hypertensive LES and poorly relaxing LES can impair bolus transit in about half of patients. It has been known that when combined with an esophageal body dysfunction, the patients symptoms stem primarily from the abnormality in LES relaxation and that inadequate LES relaxation causes delayed esophageal clearance. 3 As the majority of patients from this study who were grouped under hypertensive LES also had a poorly relaxing LES, further analysis is needed as to whether both LES abnormalities result in bolus transit delay. Although the bolus transit for liquid swallows for patients with normal manometry is significantly different compared with 10 years ago, we believe this is skewed by the effects of GERD. A recent study by Savarino et al 12 found that some patients with severe reflux disease presented with normal manometry and abnormal bolus transit. As 13 of the 18 (72%) patients with abnormal bolus transit for liquid swallows and normal manometry had abnormal reflux studies completed in our laboratory as well, we feel that this supports Savarino and colleague s study and deserves future analysis. Secondly, the prior study showed that half of patients with IEM (51%) had normal bolus transit for liquids. We believe the drastic decrease in this number to 15% (P < ) is indicative of both the change in the IEM definition and the rise in prevalence of severe IEM. In addition, normal bolus transit for liquids in patients with DES dropped from 55% ten years ago to 0% in the current study (P < 0.01). Consequently, we believe that the manometric parameters and patterns do not overestimate the functional defect caused by IEM and DES. This study is limited by the lack of comparison of the HRIM to barium studies that could have possibly confirmed or clarified the diagnosis for many of the patients categorized as MMA. Therefore, we cannot comment on Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved
6 Boland et al J Clin Gastroenterol Volume 50, Number 4, April 2016 the diagnostic accuracy and advantages of MMA as a diagnostic term. Further analysis of these findings is the focus of a subsequent study from our laboratory. In addition, one could regard the use of conventional manometry criteria as a further limitation arguing that we missed out on the chance to use the Chicago classification with the HRIM recordings. As the study published 10 years ago used the conventional Spechler-Castell classification system, we considered it more appropriate to use the same system when evaluating changes in prevalence of manometric findings over time. In summary, although most of the named esophageal motility disorders have not changed in prevalence or have fluctuated in a predictable manner, IEM has significantly increased in prevalence and severity. Further studies are needed to evaluate possible causes for this and to better clarify the IEM, GERD, and diabetes relationship. A suggestion is made in support for a new small subclass of MMA, which we feel has been helpful in our laboratory to identify the occasional poorly defined but definitely abnormal study. The findings of this investigation also suggest that a change in the classification of esophageal motility abnormalities which better blends the manometry and bolus transit may be needed. Further analysis of the dynamics of the LES in relation to esophageal functional defects likely defined by HRIM is also needed. REFERENCES 1. Silny J. Intraluminal multiple electric impedance procedure for measurement of gastrointestinal motility. J Gastrointest Motil. 1991;3: Tutuian R, Vela MF, Balaji NS, et al. Esophageal function testing with combined multichannel intraluminal impedance and manometry: multicenter study in healthy volunteers. Clin Gastroenterol Hepatol. 2003;1: Spechler SJ, Castell DO. Classification of oesophageal motility abnormalities. Gut. 2001;49: Tutuian R, Castell DO. Clarification of the esophageal function defect in patients with manometric ineffective esophageal motility: studies using combined impedance-manometry. Clin Gastroenterol Hepatol. 2004;2: Agrawal A, Hila A, Tutuian R, et al. Clinical relevance of the nutcracker esophagus: suggested revision of criteria for diagnosis. J Clin Gastroenterol. 2006;40: Tutuian R, Castell DO. Combined multichannel intraluminal impedance and manometry clarifies esophageal function abnormalities: study in 350 patients. Am J Gastroenterol. 2004;99: Bredenoord A, Fox M, Kahrilas P, et al. Chicago classification criteria of esophageal motiligy disorders defined in high resolution esophageal pressure topography. Neurogastroenterol Motil ;14: Kahrilas P, Bredenoord A, Fox M, et al. The Chicago classification of esophageal motility disorders. Neurogastroenterol Motil. 2015;27: Hiestand M, Castell DO. Ineffective esophageal motility (IEM) has two clinically distinct subtypes. Gastroenterology. 2014; 146: Blonski W, Vela M, Safder A, et al. Revised criterion for diagnosis of ineffective esophageal motility is associated with more frequent dysphagia and greater bolus transit abnormalities. Am J Gastroenterol. 2008;103: Ho SC, Chang CS, Wu CY, et al. Ineffective esophageal motility is a primary motility disorder in gastroesophageal reflux disease. Dig Dis Sci. 2002;47: Savarino E, Gemignani L, Pohl D, et al. Oesophageal motility and bolus transit abnormalities increase in parallel with the severity of gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2011;34: Friedenberg FK, Hanlon A, Vanar V, et al. Trends in gastroesophageal reflux disease as measured by the National Ambulatory Medical Care Survey. Dig Dis Sci. 2010;55: Hollis JB, Castell DO, Braddom RL. Esophageal function in diabetes mellitus and its relation to peripheral neuropathy. Gastroenterology. 1977;73: Zhao J, Frokjaer JB, Drewes AM, et al. Upper gastrointestinal sensory-motor dysfunction in diabetes mellitus. World J Gastroenterol. 2006;12: Cheng YJ, Imperatore G, Geiss LS, et al. Secular changes in the age-specific prevalence of diabetes among US adults: Diabetes Care. 2013;36: Copyright r 2015 Wolters Kluwer Health, Inc. All rights reserved.
CHAPTER 3. J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1
 CHAPTER 3 Multichannel ntraluminal impedance monitoring in the evaluation of patients with non-obstructive dysphagia J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1 1 Department
CHAPTER 3 Multichannel ntraluminal impedance monitoring in the evaluation of patients with non-obstructive dysphagia J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1 1 Department
127 Chapter 1 Chapter 2 Chapter 3
 CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
High Resolution Impedance Manometry (HRiM ) Swallow Atlas
 High Resolution Impedance Manometry (HRiM ) Swallow Atlas Normal Esophageal Function Bolus Transit UES Esophageal Body LES Complete bolus transit Peristaltic contractions with pressure amplitude of at
High Resolution Impedance Manometry (HRiM ) Swallow Atlas Normal Esophageal Function Bolus Transit UES Esophageal Body LES Complete bolus transit Peristaltic contractions with pressure amplitude of at
Journal of. Gastroenterology and Hepatology Research. Major Motility Abnormality (MMA): A Needed But Unusual Category of Esophageal Dysmotiliy
 Journal of Gastroenterology and Hepatology Research Online Submissions: http: //www.ghrnet.org/index./joghr/ doi: 10.17554/j.issn.2224-3992.2016.05.634 Journal of GHR 2016 June; 5(3): 2082-2087 ISSN 2224-3992
Journal of Gastroenterology and Hepatology Research Online Submissions: http: //www.ghrnet.org/index./joghr/ doi: 10.17554/j.issn.2224-3992.2016.05.634 Journal of GHR 2016 June; 5(3): 2082-2087 ISSN 2224-3992
Esophageal Impedance: Role in the Evaluation of Esophageal Motility
 TZ CHI MED J June 2009 Vol 21 No 2 available at http://ajws.elsevier.com/tcmj Tzu Chi Medical Journal Review Article Esophageal Impedance: Role in the Evaluation of Esophageal Motility Chien-Lin Chen*
TZ CHI MED J June 2009 Vol 21 No 2 available at http://ajws.elsevier.com/tcmj Tzu Chi Medical Journal Review Article Esophageal Impedance: Role in the Evaluation of Esophageal Motility Chien-Lin Chen*
What can you expect from the lab?
 Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis.
 Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Esophageal Manometry. John M. Wo, M.D. October 1, 2009
 Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Apple Sauce Improves Detection of Esophageal Motor Dysfunction During High-Resolution Manometry Evaluation of Dysphagia
 Dig Dis Sci (2011) 56:1723 1728 DOI 10.1007/s10620-010-1513-x ORIGINAL ARTICLE Apple Sauce Improves Detection of Esophageal Motor Dysfunction During High-Resolution Manometry Evaluation of Dysphagia Benjamin
Dig Dis Sci (2011) 56:1723 1728 DOI 10.1007/s10620-010-1513-x ORIGINAL ARTICLE Apple Sauce Improves Detection of Esophageal Motor Dysfunction During High-Resolution Manometry Evaluation of Dysphagia Benjamin
Esophageal Motor Abnormalities
 Esophageal Motor Abnormalities Brooks D. Cash, MD, FACP, AGAF, FACG, FASGE Professor of Medicine Gastroenterology Division University of South Alabama Mobile, AL High Resolution Manometry Late Ray Clouse,
Esophageal Motor Abnormalities Brooks D. Cash, MD, FACP, AGAF, FACG, FASGE Professor of Medicine Gastroenterology Division University of South Alabama Mobile, AL High Resolution Manometry Late Ray Clouse,
J Neurogastroenterol Motil, Vol. 25 No. 1 January, 2019
 JNM J Neurogastroenterol Motil, Vol. 25 No. 1 January, 2019 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm18054 Original Article High-resolution Manometry Findings During Solid Swallows
JNM J Neurogastroenterol Motil, Vol. 25 No. 1 January, 2019 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm18054 Original Article High-resolution Manometry Findings During Solid Swallows
Abstract. Abnormal peristaltic waves like aperistalsis of the esophageal body, high amplitude and broader waves,
 Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Minimum sample frequency for multichannel intraluminal impedance measurement of the oesophagus
 Neurogastroenterol Motil (2004) 16, 713 719 doi: 10.1111/j.1365-2982.2004.00575.x Minimum sample frequency for multichannel intraluminal impedance measurement of the oesophagus A. J. BREDENOORD,* B. L.
Neurogastroenterol Motil (2004) 16, 713 719 doi: 10.1111/j.1365-2982.2004.00575.x Minimum sample frequency for multichannel intraluminal impedance measurement of the oesophagus A. J. BREDENOORD,* B. L.
A collection of High Resolution Esophageal Manometry Patterns
 A collection of High Resolution Esophageal Manometry Patterns Distinctive color maps of motility disorders Table of contents Introduction... 3 Normal HRM [B.1]... 4 Achalasia... 5 Classic Achalasia with
A collection of High Resolution Esophageal Manometry Patterns Distinctive color maps of motility disorders Table of contents Introduction... 3 Normal HRM [B.1]... 4 Achalasia... 5 Classic Achalasia with
Pressure topography metrics
 Aim: The Chicago Classification (CC) categorizes esophageal motility disorders in high-resolution manometry (HRM) depicted with color pressure topography plots, also known as Clouse plots in honor of Ray
Aim: The Chicago Classification (CC) categorizes esophageal motility disorders in high-resolution manometry (HRM) depicted with color pressure topography plots, also known as Clouse plots in honor of Ray
Motility characteristics in the transition zone in Gastroesophageal Reflux Disease (GORD) patients
 Li et al. BMC Gastroenterology (2016) 16:106 DOI 10.1186/s12876-016-0525-1 RESEARCH ARTICLE Open Access Motility characteristics in the transition zone in Gastroesophageal Reflux Disease (GORD) patients
Li et al. BMC Gastroenterology (2016) 16:106 DOI 10.1186/s12876-016-0525-1 RESEARCH ARTICLE Open Access Motility characteristics in the transition zone in Gastroesophageal Reflux Disease (GORD) patients
CHAPTER 2. N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M. Conchillo 2, A.J.P.M. Smout 2, R.H. Holloway 1
 CHAPTER 2 Assessment of esophageal motor function using combined perfusion manometry and multichannel intraluminal impedance measurement in normal subjects N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M.
CHAPTER 2 Assessment of esophageal motor function using combined perfusion manometry and multichannel intraluminal impedance measurement in normal subjects N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M.
Two Distinct Types of Hypercontractile Esophagus: Classic and Spastic Jackhammer
 Brief communication Gut and Liver, Vol. 10, No. 5, September 2016, pp. 859-863 Two Distinct Types of Hypercontractile Esophagus: Classic and Spastic Jackhammer Yun Soo Hong, Yang Won Min, and Poong-Lyul
Brief communication Gut and Liver, Vol. 10, No. 5, September 2016, pp. 859-863 Two Distinct Types of Hypercontractile Esophagus: Classic and Spastic Jackhammer Yun Soo Hong, Yang Won Min, and Poong-Lyul
Esophageal Manometry: Assessment of Interpreter Consistency
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:218 224 ORIGINAL ARTICLES Esophageal Manometry: Assessment of Interpreter Consistency DEVJIT S. NAYAR, FARAH KHANDWALA, EDGAR ACHKAR, STEVEN S. SHAY, JOEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:218 224 ORIGINAL ARTICLES Esophageal Manometry: Assessment of Interpreter Consistency DEVJIT S. NAYAR, FARAH KHANDWALA, EDGAR ACHKAR, STEVEN S. SHAY, JOEL
Slide 4. Slide 5. Slide 6
 Slide 1 Slide 4 Measure Pressures within the Esophagus Evaluate Coordination of Muscles Presented by: Donna Dickinson, RN, Clin II, Manometry Specialist Bon Secours Richmond Health System Slide 2 Slide
Slide 1 Slide 4 Measure Pressures within the Esophagus Evaluate Coordination of Muscles Presented by: Donna Dickinson, RN, Clin II, Manometry Specialist Bon Secours Richmond Health System Slide 2 Slide
Achalasia: Inject, Dilate, or Surgery?
 Achalasia: Inject, Dilate, or Surgery? John E. Pandolfino, MD, MSCI, FACG Professor of Medicine Feinberg School of Medicine Northwestern University Chief, Division of Gastroenterology and Hepatology Northwestern
Achalasia: Inject, Dilate, or Surgery? John E. Pandolfino, MD, MSCI, FACG Professor of Medicine Feinberg School of Medicine Northwestern University Chief, Division of Gastroenterology and Hepatology Northwestern
High-Resolution Manometry Correlates of Ineffective Esophageal Motility
 nature publishing group ORIGINAL CONTRIBUTIONS 1647 see related editorial on page x High-Resolution Manometry Correlates of Ineffective Esophageal Motility Yinglian Xiao, MD, PhD 1, 2, Peter J. Kahrilas,
nature publishing group ORIGINAL CONTRIBUTIONS 1647 see related editorial on page x High-Resolution Manometry Correlates of Ineffective Esophageal Motility Yinglian Xiao, MD, PhD 1, 2, Peter J. Kahrilas,
Manometry Conundrums
 Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
INSIGHT HRiM. Simplify the Complexities of. High Resolution Impedance Manometry System
 INSIGHT HRiM High Resolution Impedance Manometry System Simplify the Complexities of Esophageal Function Testing HRIM is a leading edge, comprehensive test of both esophageal pressure and bolus transit
INSIGHT HRiM High Resolution Impedance Manometry System Simplify the Complexities of Esophageal Function Testing HRIM is a leading edge, comprehensive test of both esophageal pressure and bolus transit
Color Atlas of High Resolution Manometry
 Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Health-related quality of life and physiological measurements in achalasia
 Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
NIH Public Access Author Manuscript J Clin Gastroenterol. Author manuscript; available in PMC 2010 June 30.
 NIH Public Access Author Manuscript Published in final edited form as: J Clin Gastroenterol. 2008 ; 42(5): 627 635. doi:10.1097/mcg.0b013e31815ea291. Esophageal Motility Disorders in Terms of Pressure
NIH Public Access Author Manuscript Published in final edited form as: J Clin Gastroenterol. 2008 ; 42(5): 627 635. doi:10.1097/mcg.0b013e31815ea291. Esophageal Motility Disorders in Terms of Pressure
Classifying Esophageal Motility by Pressure Topography Characteristics: A Study of 400 Patients and 75 Controls
 American Journal of Gastroenterology ISSN 0002-9270 C 2007 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01532.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Classifying Esophageal
American Journal of Gastroenterology ISSN 0002-9270 C 2007 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01532.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Classifying Esophageal
Refractory GERD : case presentation and discussion
 Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
A CURIOUS CASE OF HYPERTENSIVE LES. Erez Hasnis Department of Gastroenterology Rambam Health Care Campus
 A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
Clinical Usefulness of High-Resolution Manometry
 Korean J Neurogastroenterol Motil 2009;15:107-115 Review Article Clinical Usefulness of High-Resolution Manometry Moo In Park, M.D. Department of Internal Medicine, Kosin University College of Medicine,
Korean J Neurogastroenterol Motil 2009;15:107-115 Review Article Clinical Usefulness of High-Resolution Manometry Moo In Park, M.D. Department of Internal Medicine, Kosin University College of Medicine,
An Overview on Pediatric Esophageal Disorders. Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II
 An Overview on Pediatric Esophageal Disorders Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II Case report F.C. 3 year old boy Preterm born from emergency
An Overview on Pediatric Esophageal Disorders Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II Case report F.C. 3 year old boy Preterm born from emergency
pissn: eissn: Journal of Neurogastroenterology and Motility
 JNM J Neurogastroenterol Motil, Vol. 21 No. 3 July, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm15002 Journal of Neurogastroenterology and Motility Original Article Supragastric
JNM J Neurogastroenterol Motil, Vol. 21 No. 3 July, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm15002 Journal of Neurogastroenterology and Motility Original Article Supragastric
High Resolution Manometry: A new perspective on esophageal motility disorders. Chris Andrews & Bill Paterson
 High Resolution Manometry: A new perspective on esophageal motility disorders Chris Andrews & Bill Paterson CDDW/CASL Meeting Session: CanMEDS Roles Covered in this Session: Medical Expert (as Medical
High Resolution Manometry: A new perspective on esophageal motility disorders Chris Andrews & Bill Paterson CDDW/CASL Meeting Session: CanMEDS Roles Covered in this Session: Medical Expert (as Medical
Reproducibility of multichannel intraluminal electrical impedance monitoring of gastroesophageal reflux
 3 Reproducibility of multichannel intraluminal electrical impedance monitoring of gastroesophageal reflux A.J. Bredenoord B.L.A.M. Weusten R. Timmer A.J.P.M. Smout Dept. of Gastroenterology, St. Antonius
3 Reproducibility of multichannel intraluminal electrical impedance monitoring of gastroesophageal reflux A.J. Bredenoord B.L.A.M. Weusten R. Timmer A.J.P.M. Smout Dept. of Gastroenterology, St. Antonius
Surgical Evaluation for Benign Esophageal Disease. Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018
 Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
The effect of sildenafil on segmental oesophageal motility and gastro-oesophageal reflux
 Alimentary Pharmacology & Therapeutics The effect of sildenafil on segmental oesophageal motility and gastro-oesophageal reflux H.S.KIM*,J.L.CONKLIN &H.PARK* *Department of Internal Medicine, Brain Korea
Alimentary Pharmacology & Therapeutics The effect of sildenafil on segmental oesophageal motility and gastro-oesophageal reflux H.S.KIM*,J.L.CONKLIN &H.PARK* *Department of Internal Medicine, Brain Korea
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
NIH Public Access Author Manuscript Am J Gastroenterol. Author manuscript; available in PMC 2010 June 21.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Gastroenterol. 2010 May ; 105(5): 981 987. doi:10.1038/ajg.2010.43. Esophageal Motor Disorders in Terms of High-Resolution Esophageal
NIH Public Access Author Manuscript Published in final edited form as: Am J Gastroenterol. 2010 May ; 105(5): 981 987. doi:10.1038/ajg.2010.43. Esophageal Motor Disorders in Terms of High-Resolution Esophageal
Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India
 Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Intraesophageal Impedance Monitoring Clinical Studies. J.M. Conchillo
 Intraesophageal Impedance Monitoring Clinical Studies J.M. Conchillo Intraesophageal Impedance Monitoring: Clinical Studies Conchillo Armendáriz, José Maria Thesis, University Utrecht, with summary in
Intraesophageal Impedance Monitoring Clinical Studies J.M. Conchillo Intraesophageal Impedance Monitoring: Clinical Studies Conchillo Armendáriz, José Maria Thesis, University Utrecht, with summary in
Ineffective esophageal motility: clinical, manometric, and outcome characteristics in patients with and without abnormal esophageal acid exposure
 Diseases of the Esophagus (2017) 30, 1 8 DOI: 10.1093/dote/dox012 Original Article Ineffective esophageal motility: clinical, manometric, and outcome characteristics in patients with and without abnormal
Diseases of the Esophagus (2017) 30, 1 8 DOI: 10.1093/dote/dox012 Original Article Ineffective esophageal motility: clinical, manometric, and outcome characteristics in patients with and without abnormal
Gastroesophageal reflux disease (GERD) is a common chronic
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:743 748 Efficacy of Esophageal Impedance/pH Monitoring in Patients With Refractory Gastroesophageal Reflux Disease, on and off Therapy JASON M. PRITCHETT,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:743 748 Efficacy of Esophageal Impedance/pH Monitoring in Patients With Refractory Gastroesophageal Reflux Disease, on and off Therapy JASON M. PRITCHETT,*
Systematic comparison of conventional oesophageal manometry with oesophageal motility while eating. bread ALIMENTARY TRACT
 1264 Gut, 1991,32, 1264-1269 ALIMENTARY TRACT Department of Medicine, Royal Infirmary of Edinburgh, Edinburgh EH3 9YW P J Howard L Maher A Pryde R C Heading Correspondence to: Dr P J Howard. Accepted for
1264 Gut, 1991,32, 1264-1269 ALIMENTARY TRACT Department of Medicine, Royal Infirmary of Edinburgh, Edinburgh EH3 9YW P J Howard L Maher A Pryde R C Heading Correspondence to: Dr P J Howard. Accepted for
Manometry is a technique commonly used to evaluate. Value of Spatiotemporal Representation of Manometric Data. Methods Subjects
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:525 530 Value of Spatiotemporal Representation of Manometric Data CLAUDIA GRÜBEL,* RICHARD HISCOCK, and GEOFF HEBBARD* *Department of Gastroenterology, The
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:525 530 Value of Spatiotemporal Representation of Manometric Data CLAUDIA GRÜBEL,* RICHARD HISCOCK, and GEOFF HEBBARD* *Department of Gastroenterology, The
Achalasia is diagnosed by showing dysfunction of lower
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
Comparison of oesophageal function tests between Chinese non-erosive reflux disease and reflux hypersensitivity patients
 Gao et al. BMC Gastroenterology (2017) 17:67 DOI 10.1186/s12876-017-0624-7 RESEARCH ARTICLE Comparison of oesophageal function tests between Chinese non-erosive reflux disease and reflux hypersensitivity
Gao et al. BMC Gastroenterology (2017) 17:67 DOI 10.1186/s12876-017-0624-7 RESEARCH ARTICLE Comparison of oesophageal function tests between Chinese non-erosive reflux disease and reflux hypersensitivity
Oro-pharyngeal and Esophageal Motility and Dysmotility John E. Pandolfino, MD, MSci
 Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
High Resolution Esophageal Manometry
 High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux
 Alimentary Pharmacology and Therapeutics The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux K. Ravi*, D. L. Francis*, J. A. See, D. M. Geno* & D. A. Katzka*
Alimentary Pharmacology and Therapeutics The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux K. Ravi*, D. L. Francis*, J. A. See, D. M. Geno* & D. A. Katzka*
Clinical Study Comparison of Esophageal Function Tests in Chinese Patients with Functional Heartburn and Reflux Hypersensitivity
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3596148, 8 pages https://doi.org/10.1155/2017/3596148 Clinical Study Comparison of Esophageal Function Tests in Chinese Patients with
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3596148, 8 pages https://doi.org/10.1155/2017/3596148 Clinical Study Comparison of Esophageal Function Tests in Chinese Patients with
Findings of impedance ph-monitoring in patients with atypical gastroesophageal reflux symptoms
 Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Findings of impedance ph-monitoring in patients with atypical
Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Findings of impedance ph-monitoring in patients with atypical
Gender, medication use and other factors associated with esophageal motility disorders in non-obstructive dysphagia
 Gastroenterology Report, 6(3), 2018, 177 183 doi: 10.1093/gastro/goy018 Advance Access Publication Date: 2 June 2018 Original article ORIGINAL ARTICLE Gender, medication use and other factors associated
Gastroenterology Report, 6(3), 2018, 177 183 doi: 10.1093/gastro/goy018 Advance Access Publication Date: 2 June 2018 Original article ORIGINAL ARTICLE Gender, medication use and other factors associated
9/18/2015. Disclosures. Objectives. Dysphagia Sherri Ekobena PA-C. I have no relevant financial interests to disclose I have no conflicts of interest
 Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ang D, Misselwitz B, Hollenstein M, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ang D, Misselwitz B, Hollenstein M, et al.
Achalasia esophagus, a major motility disorder, results
 GASTROENTEROLOGY 2010;139:102 111 A Unique Esophageal Motor Pattern That Involves Longitudinal Muscles Is Responsible for Emptying in Achalasia Esophagus SU JIN HONG,* VALMIK BHARGAVA, YANFEN JIANG, DEBBIE
GASTROENTEROLOGY 2010;139:102 111 A Unique Esophageal Motor Pattern That Involves Longitudinal Muscles Is Responsible for Emptying in Achalasia Esophagus SU JIN HONG,* VALMIK BHARGAVA, YANFEN JIANG, DEBBIE
Dysphagia. Conflicts of Interest
 Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Gastroesophageal Reflux Disease in Infants and Children
 Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
NIH Public Access Author Manuscript Arch Surg. Author manuscript; available in PMC 2013 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
ORIGINAL ARTICLE. in which elements of the abdominal cavity herniate. Anatomic disruption of the esophagogastric junction (EGJ), phrenoesophageal
 ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
Characteristics of gastroesophageal reflux in patients with and without excessive gastroesophageal acid exposure
 13 Characteristics of gastroesophageal reflux in patients with and without excessive gastroesophageal acid exposure A.J. Bredenoord B.L.A.M. Weusten R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
13 Characteristics of gastroesophageal reflux in patients with and without excessive gastroesophageal acid exposure A.J. Bredenoord B.L.A.M. Weusten R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
Title: Comparison of esophageal motility in gastroesophageal reflux disease with and without globus sensation
 Title: Comparison of esophageal motility in gastroesophageal reflux disease with and without globus sensation Authors: Yuming Tang, Jia Huang, Ying Zhu, Aihua Qian, Bin Xu, Weiyan Yao DOI: 10.17235/reed.2017.4449/2016
Title: Comparison of esophageal motility in gastroesophageal reflux disease with and without globus sensation Authors: Yuming Tang, Jia Huang, Ying Zhu, Aihua Qian, Bin Xu, Weiyan Yao DOI: 10.17235/reed.2017.4449/2016
Myogenic Control. Esophageal Motility. Enteric Nervous System. Alimentary Tract Motility. Determinants of GI Tract Motility.
 Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Esophageal Motility. Alimentary Tract Motility
 Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Achalasia: Classic View
 Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
Review article: the measurement of non-acid gastro-oesophageal reflux
 Alimentary Pharmacology & Therapeutics Review article: the measurement of non-acid gastro-oesophageal reflux A. J. P. M. SMOUT Department of Gastroenterology, University Medical Center Utrecht, Utrecht,
Alimentary Pharmacology & Therapeutics Review article: the measurement of non-acid gastro-oesophageal reflux A. J. P. M. SMOUT Department of Gastroenterology, University Medical Center Utrecht, Utrecht,
Comparison of esophageal motility in gastroesophageal reflux disease with and without globus sensation
 1130-0108/2017/109/12/850-855 Revista Española de Enfermedades Digestivas Copyright 2017. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2017, Vol. 109, N.º 12, pp. 850-855 ORIGINAL PAPERS Comparison of
1130-0108/2017/109/12/850-855 Revista Española de Enfermedades Digestivas Copyright 2017. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2017, Vol. 109, N.º 12, pp. 850-855 ORIGINAL PAPERS Comparison of
Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease
 Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
David Markowitz, MD. Physicians and Surgeons
 Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
ManOSCan ESO HigH Resolution ManoMetRy
 ManoScan ESO High Resolution Manometry Normal Swallow with 3D Visualization ManoScan ESO ManoScan ESO provides a complete physiological mapping of the esophageal motor function, from the pharynx to the
ManoScan ESO High Resolution Manometry Normal Swallow with 3D Visualization ManoScan ESO ManoScan ESO provides a complete physiological mapping of the esophageal motor function, from the pharynx to the
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.42 Original Article Observations
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.42 Original Article Observations
High-resolution Manometry in Patients with Gastroesophageal Reflux Disease Before and After Fundoplication
 JNM J Neurogastroenterol Motil, Vol. 23 No. 1 January, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/.5056/jnm16062 Original Article High-resolution Manometry in Patients with Gastroesophageal
JNM J Neurogastroenterol Motil, Vol. 23 No. 1 January, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/.5056/jnm16062 Original Article High-resolution Manometry in Patients with Gastroesophageal
Baclofen decreases acid and non-acid post-prandial gastro-oesophageal reflux measured by combined multichannel intraluminal impedance and ph
 Aliment Pharmacol Ther 23; 17: 243 21. doi: 1.146/j.136-236.23.1394.x decreases acid and non-acid post-prandial gastro-oesophageal reflux measured by combined multichannel intraluminal impedance and ph
Aliment Pharmacol Ther 23; 17: 243 21. doi: 1.146/j.136-236.23.1394.x decreases acid and non-acid post-prandial gastro-oesophageal reflux measured by combined multichannel intraluminal impedance and ph
JNM Journal of Neurogastroenterology and Motility
 ㅋ JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 17 No. 1 January, 2011 DOI: 10.5056/jnm.2011.17.1.48 Original Article Achalasia Cardia Subtyping by High-Resolution
ㅋ JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 17 No. 1 January, 2011 DOI: 10.5056/jnm.2011.17.1.48 Original Article Achalasia Cardia Subtyping by High-Resolution
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Radiology. Gastrointestinal. Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact. Farooq P. Agha
 Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
ORIGINAL ARTICLE. Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease
 ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Esophageal Motility Disorders. Disclosures
 Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Chicago Classification of Esophageal Motility Disorders: Lessons Learned
 Curr Gastroenterol Rep (2017) 19: 37 DOI 10.1007/s11894-017-0576-7 NEUROGASTROENTEROLOGY AND MOTILITY DISORDERS OF THE GASTROINTESTINAL TRACT (S RAO, SECTION EDITOR) Chicago Classification of Esophageal
Curr Gastroenterol Rep (2017) 19: 37 DOI 10.1007/s11894-017-0576-7 NEUROGASTROENTEROLOGY AND MOTILITY DISORDERS OF THE GASTROINTESTINAL TRACT (S RAO, SECTION EDITOR) Chicago Classification of Esophageal
Treating Achalasia. When to consider surgery and New options for therapy
 Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Available Online at International Journal of Pharmaceutical & Biological Archives 2013; 4(5): ORIGINAL RESEARCH ARTICLE
 ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 968-972 ORIGINAL RESEARCH ARTICLE Existence of Oesophageal Dysmotility and Autonomic
ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 968-972 ORIGINAL RESEARCH ARTICLE Existence of Oesophageal Dysmotility and Autonomic
Prevalence and Clinical Characteristics of Refractoriness to Optimal Proton Pump Inhibitor Therapy in Non-erosive Reflux Disease
 www.medscape.com Prevalence and Clinical Characteristics of Refractoriness to Optimal Proton Pump Inhibitor Therapy in Non-erosive Reflux Disease Mentore Ribolsi; Michele Cicala; Patrizia Zentilin; Matteo
www.medscape.com Prevalence and Clinical Characteristics of Refractoriness to Optimal Proton Pump Inhibitor Therapy in Non-erosive Reflux Disease Mentore Ribolsi; Michele Cicala; Patrizia Zentilin; Matteo
ORIGINAL ARTICLES ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:379 384 ORIGINAL ARTICLES ALIMENTARY TRACT Baclofen Improves Symptoms and Reduces Postprandial Flow Events in Patients With Rumination and Supragastric
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:379 384 ORIGINAL ARTICLES ALIMENTARY TRACT Baclofen Improves Symptoms and Reduces Postprandial Flow Events in Patients With Rumination and Supragastric
Refractory GERD: What s a Gastroenterologist To Do?
 Refractory GERD: What s a Gastroenterologist To Do? Philip O. Katz, MD, FACG Chairman, Division of Gastroenterology Einstein Medical Center Clinical Professor of Medicine Jefferson Medical College Philadelphia,
Refractory GERD: What s a Gastroenterologist To Do? Philip O. Katz, MD, FACG Chairman, Division of Gastroenterology Einstein Medical Center Clinical Professor of Medicine Jefferson Medical College Philadelphia,
Survey of findings in patients having persistent heartburn on proton pump inhibitor therapy
 Diseases of the Esophagus (2014) (2016), 29, 27 33 DOI: 10.1111/dote.12293 Original article Survey of findings in patients having persistent heartburn on proton pump inhibitor therapy R. Mandaliya, 1 A.
Diseases of the Esophagus (2014) (2016), 29, 27 33 DOI: 10.1111/dote.12293 Original article Survey of findings in patients having persistent heartburn on proton pump inhibitor therapy R. Mandaliya, 1 A.
Can the upper esophageal sphincter contractile integral help classify achalasia?
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Can the upper esophageal sphincter contractile integral help classify achalasia? Tania Triantafyllou a, Charalampos Theodoropoulos a, Apostolos
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Can the upper esophageal sphincter contractile integral help classify achalasia? Tania Triantafyllou a, Charalampos Theodoropoulos a, Apostolos
The Chicago Classification of esophageal motility disorders, v3.0
 Neurogastroenterology & Motility Neurogastroenterol Motil (2014) doi: 10.1111/nmo.12477 The Chicago Classification of esophageal motility disorders, v3.0 P. J. KAHRILAS, A. J. BREDENOORD, M. FOX, C. P.
Neurogastroenterology & Motility Neurogastroenterol Motil (2014) doi: 10.1111/nmo.12477 The Chicago Classification of esophageal motility disorders, v3.0 P. J. KAHRILAS, A. J. BREDENOORD, M. FOX, C. P.
Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression*
 Original Research SLEEP MEDICINE Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression* William C. Orr, PhD; Andrea Craddock, PhD; and Suanne Goodrich, PhD Background:
Original Research SLEEP MEDICINE Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression* William C. Orr, PhD; Andrea Craddock, PhD; and Suanne Goodrich, PhD Background:
Gastroesophageal reflux disease (GERD) is a common ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1110 1116 ALIMENTARY TRACT Use of Direct, Endoscopic-Guided Measurements of Mucosal Impedance in Diagnosis of Gastroesophageal Reflux Disease ELIF SARITAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1110 1116 ALIMENTARY TRACT Use of Direct, Endoscopic-Guided Measurements of Mucosal Impedance in Diagnosis of Gastroesophageal Reflux Disease ELIF SARITAS
Buspirone, a new drug for the management of patients with ineffective esophageal motility?
 Editorial Buspirone, a new drug for the management of patients with ineffective esophageal motility? United European Gastroenterology Journal 2015, Vol. 3(3) 261 265! Author(s) 2015 Reprints and permissions:
Editorial Buspirone, a new drug for the management of patients with ineffective esophageal motility? United European Gastroenterology Journal 2015, Vol. 3(3) 261 265! Author(s) 2015 Reprints and permissions:
The most widely accepted tool for the diagnosis of
 Evaluation of Gastroesophageal Reflux Events in Children Using Multichannel Intraluminal Electrical Impedance Tobias G. Wenzl, MD The majority of gastroesophageal reflux (GER) episodes in infants and children
Evaluation of Gastroesophageal Reflux Events in Children Using Multichannel Intraluminal Electrical Impedance Tobias G. Wenzl, MD The majority of gastroesophageal reflux (GER) episodes in infants and children
Rapid Drink Challenge in high-resolution manometry: an adjunctive test for detection of esophageal motility disorders
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2017 Rapid Drink Challenge in high-resolution manometry: an adjunctive test
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2017 Rapid Drink Challenge in high-resolution manometry: an adjunctive test
Classification of oesophageal motility abnormalities
 Gut 2001;49:145 151 145 Review Classification of oesophageal motility abnormalities Summary Manometric examination of the oesophagus frequently reveals abnormalities whose cause is unknown and whose physiological
Gut 2001;49:145 151 145 Review Classification of oesophageal motility abnormalities Summary Manometric examination of the oesophagus frequently reveals abnormalities whose cause is unknown and whose physiological
ORIGINAL PAPERS. Esophageal motor disorders are frequent during pre and post lung transplantation. Can they influence lung rejection?
 ORIGINAL PAPERS Esophageal motor disorders are frequent during pre and post lung transplantation. Can they influence lung rejection? Constanza Ciriza-de-los-Ríos 1, Fernando Canga-Rodríguez-Valcárcel 1,
ORIGINAL PAPERS Esophageal motor disorders are frequent during pre and post lung transplantation. Can they influence lung rejection? Constanza Ciriza-de-los-Ríos 1, Fernando Canga-Rodríguez-Valcárcel 1,
Normal Values of Pharyngeal and Esophageal 24-Hour ph Impedance in Individuals on and off Therapy and Interobserver Reproducibility
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:366 372 ALIMENTARY TRACT Normal Values of Pharyngeal and Esophageal 24-Hour ph Impedance in Individuals on and off Therapy and Interobserver Reproducibility
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:366 372 ALIMENTARY TRACT Normal Values of Pharyngeal and Esophageal 24-Hour ph Impedance in Individuals on and off Therapy and Interobserver Reproducibility
