C LINICAL A RTICLE. The sacrifice of motion to achieve spinal stability and pain relief has been practised since the early 20 th
|
|
|
- Gwendoline Daniels
- 5 years ago
- Views:
Transcription
1 Page 8 / SA ORTHOPAEDIC JOURNAL Autumn 2008 C LINICAL A RTICLE Lumbar fusion indications and surgical options RN Dunn, MBChB(UCT), MMed(UCT)Orth, FCS(SA)Orth Head of Spinal Services, Division of Orthopaedic Surgery, University of Cape Town Reprint requests: Dr RN Dunn Head of Spinal Services Division of Orthopaedic Surgery University of Cape Town PO Box Tokai, 7966 Tel: (021) Fax: robdunn@mweb.co.za The sacrifice of motion to achieve spinal stability and pain relief has been practised since the early 20 th century by means of iatrogenically induced ankylosis or fusion. Initially this was practised in the management of Pott s disease and indications have been expanded over the years to include trauma, deformity and degenerative conditions. In the last few decades there has been a proliferation of options as regards surgical technique and instrumentation. This often overwhelms the surgeon where more is perceived to be better, yet there is limited evidence that this is in fact so. Surgical indications for lumbar fusion Indications for surgery in traumatic and infective pathologies are relatively clear. Once spinal stability is threatened fusion is indicated. This is based on the assessment of the anatomical structures and the appreciation of the Denis three-column or AO two-column systems. Denis describes the anterior, middle and posterior columns whereas the AO system limits their classification to the anterior and posterior columns only, suggesting that the middle column per se does not add much value in decision-making. Once two or more columns in the Denis, or both columns in the AO classification are disrupted, an unstable situation is diagnosed. Should this involve a ligamentous injury (e.g. flexion distraction injury), spontaneous healing to a stable state is not expected and surgical fusion is indicated. Should the injury be purely bony (e.g. Chance fracture), non-operative care can be considered as spontaneous fracture healing will occur. The particular patient s circumstances need to be taken into account. Should there be a polytrauma situation with chest injury, early surgical spinal stabilisation may be beneficial to allow early mobilisation and safe nursing care. In spinal deformity, fusion may be indicated to correct or arrest the progression of kyphosis or scoliosis. This is typically in the growing spine where the underlying pathology is expected to cause progressive deformity. Most lumbar fusions are performed for degenerative conditions. Should the current or expected deformity threaten respiratory or neurological status, surgery should be undertaken. On occasion the effect on cosmesis and resultant psychological consequences is a driver to undertake surgery. Examples would be congenital abnormalities with significant abnormal growth potential such as a posterior hemivertebrae causing kyphosis or a lumbar sacral hemivertebrae with severe progressive scoliosis. More commonly the deformity is in the form of adolescent idiopathic scoliosis which presents during the pubertal growth spurt. Curves with Cobb angles approaching 45 and beyond would be considered for fusion surgery.
2 SA ORTHOPAEDIC JOURNAL Autumn 2008 / Page 9 This is where the clarity ends. Most lumbar fusions are performed for degenerative conditions. The rationale for this is that the pain generator causes pain in response to mechanical stress, i.e. movement, which may be more than normal. The pain generator may be musculature, the facets or disc. There is an increasing focus on the disc as the source of lumbar pain. This still provides many challenges as all discs degenerate with age, yet only a few cause significant debilitating pain. It remains difficult to correlate degeneration with axial back pain in a highly predictable manner. This opens the way for excessive spinal surgery in degenerative conditions and demands firm clinical indications to achieve the best outcomes. A recent review of randomised trials comparing lumbar fusion surgery to non-operative care in chronic back pain concluded that although surgery may be more efficacious than unstructured non-surgical care it may not be more efficacious than cognitive behaviour therapy. 1 The use of may indicates that the outcome of surgery in this context is still not proven despite widespread use. Essentially the mainstream indication for fusion in axial back pain is significant pain unresponsive to active nonoperative care for a period of 6 months, where the pain generator has been determined by imaging and possible provocative discography. This is extremely broad and open to varied interpretation which explains the different approaches among surgeons. Significant pain to one patient (and surgeon) is different from another and is influenced by many factors. Patients with associated severe sciatica for more than 6 weeks or reduced neurological function would be considered for surgery earlier. Other considerations would be patients where decompression for stenosis would result in instability, e.g. foraminectomy and pars resection. The presence of a neural arch defect, such as a bilateral spondylolysis, with radicular and axial pain is a good indication. The presence of symptomatic and radiological instability is an indication. Instability itself is a difficult concept in degenerative conditions. White 2 describes it as a loss of ability of the spine under physiological loads to maintain relationships between vertebrae It is this loss that leads to nerve root irritation and pain from structural changes. Translation of greater than 3 mm on flexion/extension or an angulation greater than 10 can be considered pathological. The evidence of the vacuum sign, viz. the evidence of intra-discal gas on the X-ray and traction osteophytes (2-3 mm away from the endplate) suggests instability. Fusion options There are multiple fusion options which can be divided by technique and approach. The lumbar spine can be fused by means of posterior or posterolateral fusions, or interbody (via the disc space). The latter can be achieved via the anterior or posterior surgical approach. In addition, the procedures can be performed with or without the use of instrumentation, and a variety of bone graft options. Posterior/posterolateral fusion Posterior fusions, where graft was placed directly on the lamina, are largely historical. Posterolateral fusions have however remained a commonly utilised technique. After sub-periosteal exposure and decortication of the lamina, pars interarticularis, facet joints and transverse processes, bone graft is applied. Although superficially simple, it is a demanding procedure especially in the male pelvis with narrow space between the posterior crests and large erector spinae muscle bulk. This may explain the wide variation of reported fusion rates from 60 90%. 3,4 This technique demands visualisation of the bony elements and retraction/removal of the intervening muscles and tendons. With a meticulous technique fusion rates of 90% and above can be achieved. 3 This posterolateral space provides for a large volume of graft which when mature provides good stability as it is closer to the compression side of the spine than the previously used posterior on lay fusions. The advantages are that although meticulous attention to detail is required, it is a simple and low cost technique with high fusion rates. It does not require the lamina to be intact and is thus useful as an adjunct to a decompression. There is no violation to the neurological structures with a low risk approach. The disadvantages are that extensive muscular dissection is required. This is technically demanding in the muscular patient, especially male. This can be avoided by the muscle splitting (Wiltse) technique where through a midline incision, the lumbar fascia is exposed and a plane developed laterally. The fascia is opened longitudinally about 2.5 cm lateral to the midline, where there is a palpable groove in the erector muscles indicative of the gap between multifidus and longissmus. Blunt dissection with an educated finger tip locates the facet and transverse process. This is easiest at L4/5 as distally the fascia inserts into the crest. However once the plane is identified at L4/5 it can be extended distally and the muscle detached appropriately. This is bloodless and prevents the muscle bulk being retracted against the iliac crest. Through this approach the transverse processes, facets and pars are easily visible allowing easy decortication and bone grafting. Criticism of the posterolateral technique is that it does not change or improve the sagittal profile and does not directly address the pain generator. The degenerate disc remains and is unloaded once fusion occurs. Should there be instability such as a spondylolisthesis, brace wear may be required and patients may be slower to mobilise than other fusion options.
3 Page 10 / SA ORTHOPAEDIC JOURNAL Autumn 2008 Instrumented posterolateral fusion The addition of instrumentation to provide immediate rigidity has been shown to accelerate fusion as well as increase fusion rates in the animal model. 5,6 Historically spinous process wiring, Steffee plates and facet screws have been tried, but presently the mainstay of posterior instrumentation is the pedicle screw. It allows three-dimensional control of the vertebral body with the passage of screw from the base of the junction of the transverse process, superior articular process and pars down the pedicle into the body. With the large pedicles in the lumbar spine this is technically easy in trained hands although there is still a reported incidence of misplacement in the region of 10%. Many of these are minor cortical violations which are clinically insignificant. Zdeblick 4 compared cohorts undergoing uninstrumented, pedicle screw plate and newer pedicle screw rod procedures. He found a 65% fusion rate in the former and 95% in the latter. It has been suggested that instrumented patients have a lower postoperative analgesic requirement, and are more rapidly mobilised with a reduced hospital stay. This has not been the author s experience and one wonders whether this has more to do with the surgeon s confidence than patient factors. There is no doubt that more exposure, i.e. muscle stripping, is required to insert the screws safely, which must have an adverse effect on the patient. This adds operative time and blood loss. Despite the reported improved radiographic fusion rates, this does not necessarily follow through to enhanced clinical outcome. Andersen 7 reports on a five-year outcome comparing instrumented and uninstrumented posterolateral fusions. Although there are the usual methodological problems inherent in these papers, they found no difference in the pain drawings, Dallas Pain Questionnaire and Low Back Pain rating scale. Overall 79% had some residual back pain and 69% leg pain. Sixty-two per cent of the pain drawings were classified as organic and 38% nonorganic. This message was confirmed by Van Tulder 8 in his meta-analysis of eight trials with improved fusion rates but not statistically or clinically significant improvement in clinical outcomes. Posterior and transforaminal lumbar interbody fusion The posterior lumbar interbody fusion (PLIF) is performed via the spinal canal. More extensive posterior canal exposure is required but the facets are left intact. Bilateral annulotomies are done, first one then the other. This requires significant medial retraction of the thecal sac which is the major concern. This is responsible for the postoperative neuritis and frequent CSF leaks seen. The disc space is cleared and prepared for fusion. Bone graft and usually a cage is passed bilaterally into the disc space. The proposed advantages are that the pain generator (disc) is removed. The cage supports the anterior column where 80% of the force is transmitted. Figure 1: 30-year-old patient with lytic listhesis, back and leg pain Figure 2: MRI scan confirming foraminal stenosis This allows foraminal height improvement without being kyphogenic such as simply distracting pedicle screws. Higher fusion rates have been demonstrated by PLIFs compared to posterolateral fusions, although only achieving the best reported results of PL fusions. The literature is varied on PLIF versus PL. Although there is a higher fusion rate in PLIFs, this is not borne out in clinical outcome studies. In addition PLIFs carry a higher complication rate (30% vs 5.6%). 9
4 SA ORTHOPAEDIC JOURNAL Autumn 2008 / Page 11 Figure 3: Postoperative lateral view indicating TLIF cage in situ with reduction of slip and disc height The transforaminal lumbar interbody fusion (TLIF) reduces some of the neurological risk as less retraction is required. One facet is resected and the annulotomy done more laterally in the foramen where there is far more space. It requires only one side to be done. The author usually approaches via the symptomatic side so should there be some transient postoperative neuritis, it is not in the asymptomatic leg. The disc is cleared. Bone graft is placed anteriorly in the disc space and a C-shaped cage inserted and rotated round, before being impacted as far forward as possible. As with the PLIF technique, pedicle screws are a mandatory adjunct. Fusion rates of up to 100% have been reported. 9 The interbody techniques are useful when sagittal plane correction is desired. A good indication is the patient with a lysis where, after decompression, there is minimal posterolateral bony surface available for fusion. There is the situation of a degenerative disc with foraminal stenosis. Here the TLIF cage will provide interbody distraction opening the foramina and facilitate interbody fusion with a large surface area from the endplates. The author finds this his primary indication for the TLIF technique. A less frequent indication is augmenting the L5/S1 level when applying a long posterior construct. In the older patient L5/S1 non-union is frequently seen with S1 screw lucency. The addition of the TLIF cage supports them without the need for an additional surgical approach (Figures 1 3). Figure 4: 38-year-old woman with back and leg pain; lateral X-ray indicating instability of L4/5 on erect view Anterior lumbar interbody fusion (ALIF) The ALIF is performed via the anterior approach. Thus it avoids opening the spinal canal but places the abdominal structures at risk. The retroperitoneal approach reduces the visceral problems but the vascular structures remain the concern. Although the L4/5 level can be approached from laterally, the ascending lumbar vein may be at risk. From directly anterior the vessel needs to be divided to allow medial mobilisation of the left iliac to allow access to the disc space if covered by the bifurcation. Both direct vascular injury and thrombosis have been reported. 10
5 Page 12 / SA ORTHOPAEDIC JOURNAL Autumn 2008 We therefore owe it to our axial back pain patients to be extremely conservative both in offering surgery and the technique employed. No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article. This article is free of plagiarism. Figure 5: Postoperative posterior decompression and fusion with an ALIF cage in situ The rationale for ALIF is that the disc (pain generator) is removed, and foraminal height and sagittal balance can be restored. In the author s opinion this can be achieved with the posterior options although proponents argue that ALIF is superior in this regard but equal in clinical outcome. 11 It may still be indicated in management of discogenic pain only, i.e. when decompression is not required. Stand-alone ALIFs, i.e. without posterior fixation, have a risk of non-union and generally they involve a circumferential fusion. Newer anterior plates may obviate the need for posterior fixation but results have yet to be seen (Figures 4 5). Summary Fusion of the lumbar spine is fraught with problems both in the indications and choice of fusion technique. The vast majority of surgery of the lumbar spine is for degenerative complaints where indications are vague and depend on the individual surgeon and patient s threshold. Furthermore there are many options in surgical technique. Although they may offer intuitive and radiographic benefits these do not seem to translate to predictably improved patient outcomes. This may simply be because of the poor patient selection due to the available indications. References 1. Mirza SK, Deyo RA. Systematic review of randomised trials comparing lumbar fusion surgery to non-operative care for the treatment of chronic back pain. Spine 2007 Apr 1; 32(7): White AA, Panjabi MM. Clinical biomechanics of the spine. Philadelphia. Lippincott 1978 p McCulloch JA. Uninstrumented posterolateral lumbar fusion for single level isolated disc resorption and/or degenerative disc disease. J Spinal Disorder 1999;12(1): Zdeblick TA. A prospective randomised study of lumbar fusions. Spine 1993;18: Kanayama M, Cunningham BW, Sefter JC et al. Does spinal instrumentation influence the healing process of posterolateral fusion? Spine 1999 Jun 1;24(11): McAfee P, Forey ID, Suttlin CE et al. Device related osteoporosis with spinal instrumentation. Spine Sept. 7. Andersen T, Christiansen FB, Hansen ES, Bunger C. Pain 5 years after instrumented and non-instrumented posterolateral lumbar fusion. Eur Spine J 2003; 12(4): Van Tulder MW, Koes B, Seitsalo, Malmivaara A. Outcome of invasive treatment modalities on back pain and sciatica: an evidence-based review. Eur Spine J Jan;Supp 1:S Wang JC, Mummaneni PV, Haid RW. Current treatment strategies of the painful lumbar motion segment. Posterolateral fusion versus interbody fusion. Spine 2005;30(165):S Kulkarni SS, Lowery GL, Ross RE et al. Arterial complications following ALIF: report of 8 cases. Eur Spine J 2003 Feb 12;(1): Hseih PC, Koski TR, O Shaughnessy BA. ALIF in comparison with TLIF: implications for restoration of foraminal height, local disc angle, lumbar lordosis and sagittal balance. J Neurosurg Spine 2007;7(4): SAOJ
Spondylolytic spondylolisthesis:
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Spondylolysis. Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down.
 Spondylolysis Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down. Thomas J Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Spondylolysis Defect in the
Spondylolysis Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down. Thomas J Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Spondylolysis Defect in the
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Introduction. CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2011 Vol 10 No 1 / Page 25
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 211 Vol 1 No 1 / Page 25 C L I N I C A L A RT I C L E Cervical PEEK cage standalone fusion the issue of subsidence RN Dunn, MBChB(UCT), FCS(SA)Orth, MMed(Orth)
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 211 Vol 1 No 1 / Page 25 C L I N I C A L A RT I C L E Cervical PEEK cage standalone fusion the issue of subsidence RN Dunn, MBChB(UCT), FCS(SA)Orth, MMed(Orth)
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
PARADIGM SPINE. Brochure. coflex-f Minimally Invasive Lumbar Fusion
 PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Classification of Thoracolumbar Spine Injuries
 Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
C LINICAL A RTICLE. Page 26 / SA ORTHOPAEDIC JOURNAL Autumn 2009
 Page 26 / SA ORTHOPAEDIC JOURNAL Autumn 2009 CLINICAL ARTICLE C LINICAL A RTICLE Transforaminal lumbar interbody fusion (TLIF): assessment of clinical and radiological outcome MJD Jacobsohn MBChB, FCS(Neuro)SA
Page 26 / SA ORTHOPAEDIC JOURNAL Autumn 2009 CLINICAL ARTICLE C LINICAL A RTICLE Transforaminal lumbar interbody fusion (TLIF): assessment of clinical and radiological outcome MJD Jacobsohn MBChB, FCS(Neuro)SA
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Spinal Deformity Pathologies and Treatments
 Spinal Deformity Pathologies and Treatments Scoliosis Spinal Deformity 3-dimensional deformity affecting all 3 planes Can be difficult to visualize with 2-dimensional radiographs Kyphosis Deformity affecting
Spinal Deformity Pathologies and Treatments Scoliosis Spinal Deformity 3-dimensional deformity affecting all 3 planes Can be difficult to visualize with 2-dimensional radiographs Kyphosis Deformity affecting
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Lumbar Spinal Fusion Corporate Medical Policy
 Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
ILIF Interlaminar Lumbar Instrumented Fusion. Anton Thompkins, M.D.
 ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Adult Spinal Deformity: Principles of Surgical Correction
 Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
The imaging features of spondylolisthesis : what the clinician needs to know
 The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Spinal fusion for paediatric lumbosacral spondylolisthesis
 South African Orthopaedic Journal http://journal.saoa.org.za Horn A et al. SA Orthop J 2018;17(4) DOI 10.17159/2309-8309/2018/v17n4a5 SPINE TRAUMA Spinal fusion for paediatric lumbosacral spondylolisthesis
South African Orthopaedic Journal http://journal.saoa.org.za Horn A et al. SA Orthop J 2018;17(4) DOI 10.17159/2309-8309/2018/v17n4a5 SPINE TRAUMA Spinal fusion for paediatric lumbosacral spondylolisthesis
DEGENERATIVE SPONDYLOLISTHESIS
 AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
The vault bones Frontal Parietals Occiput Temporals Sphenoid Ethmoid
 The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
Disclosures 5/27/2016. Narrowing of the spinal canal or neuroforamina causing a symptomatic compression of the neural element.
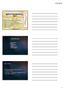 Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
L5-S1 Spondylolysis/listhesis in children & adolescents: When is surgery indicated? Hubert Labelle, MD
 L5-S1 Spondylolysis/listhesis in children & adolescents: When is surgery indicated? Hubert Labelle, MD Wiltse, Newman and Macnab Classification Clin Orthop 1976;117:23-29 Type I: Congenital spondylolisthesis
L5-S1 Spondylolysis/listhesis in children & adolescents: When is surgery indicated? Hubert Labelle, MD Wiltse, Newman and Macnab Classification Clin Orthop 1976;117:23-29 Type I: Congenital spondylolisthesis
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Management of fractures of the pedicle after instrumentation with transpedicular screws
 Management of fractures of the pedicle after instrumentation with transpedicular screws A REPORT OF THREE PATIENTS F. Lattig, T. F. Fekete, D. Jeszenszky From the Schulthess Clinic, Zürich, Switzerland
Management of fractures of the pedicle after instrumentation with transpedicular screws A REPORT OF THREE PATIENTS F. Lattig, T. F. Fekete, D. Jeszenszky From the Schulthess Clinic, Zürich, Switzerland
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
The Fusion of. Strength, Design. Performance. and
 The Fusion of Strength, Design and Performance Interbody Fusion Platform Interbody Fusion Platform The DePuy Spine Interbody Fusion platform is designed to provide an open architecture implant in a load-sharing
The Fusion of Strength, Design and Performance Interbody Fusion Platform Interbody Fusion Platform The DePuy Spine Interbody Fusion platform is designed to provide an open architecture implant in a load-sharing
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
L8 Spine System SURGICAL TECHNIQUE. Add: No.1-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China
 Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
CLINICAL ARTICLE. Abstract. History. Pathological process. Reprint requests: Prof GJ Vlok Tel: (021) Fax: (021)
 Page 50 / SA ORTHOPAEDIC JOURNAL Autumn 2008 C L I N I C A L A RT I C L E Degenerative spondylolisthesis: part of the normal ageing process Prof GJ Vlok, MBChB, MMed(Orth), FC(Orth)(SA) Professor and Head,
Page 50 / SA ORTHOPAEDIC JOURNAL Autumn 2008 C L I N I C A L A RT I C L E Degenerative spondylolisthesis: part of the normal ageing process Prof GJ Vlok, MBChB, MMed(Orth), FC(Orth)(SA) Professor and Head,
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Regions of the Spine
 Anatomy The spine is a very complex mechanical structure that is highly flexible yet very strong and stable. In the normal spine, regardless of your position or activity, including sleeping, there is always
Anatomy The spine is a very complex mechanical structure that is highly flexible yet very strong and stable. In the normal spine, regardless of your position or activity, including sleeping, there is always
Functional Anatomy and Exam of the Lumbar Spine. Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation
 Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN
 ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN Consultant Musculoskeletal Radiologist Royal National Orthopaedic Hospital Stanmore,UK. INTRODUCTION 2 INTRODUCTION 3 INTRODUCTION Spinal
ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN Consultant Musculoskeletal Radiologist Royal National Orthopaedic Hospital Stanmore,UK. INTRODUCTION 2 INTRODUCTION 3 INTRODUCTION Spinal
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF)
 Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose
 Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
4.5 System. Surgical Technique. This publication is not intended for distribution in the USA.
 4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES
 AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy. Christian Etter, MD, Spine Surgeon Zürich, Switzerland
 The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy Christian Etter, MD, Spine Surgeon Zürich, Switzerland WW Fusion Volume by Disorder 2004E % Tumor/Trauma 11% Deformity 15% Degeneration
The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy Christian Etter, MD, Spine Surgeon Zürich, Switzerland WW Fusion Volume by Disorder 2004E % Tumor/Trauma 11% Deformity 15% Degeneration
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Original Investigation. Peng Luo 1*, Rong-Xue Shao 2*, Ai-Min Wu 1, Hua-Zi Xu 1, Yong-Long ChI 1, Yan LIn 1 ABSTRACT
 DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Thoracolumbar Spine Fractures
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Professor of Radiology Adjunct Professor of Health Services Harborview Injury Prevention and Research Center University of Washington Outline Who
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Professor of Radiology Adjunct Professor of Health Services Harborview Injury Prevention and Research Center University of Washington Outline Who
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar
 BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
Related Policies None
 Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Corporate Medical Policy
 Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Apache Cervical Interbody Fusion Device. Surgical Technique. Page of 13. LC-005 Rev F
 LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Bony framework of the vertebral column Structure of the vertebral column
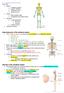 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
PACH PLATE 2 OR 4 HOLE FIXATION
 2 OR 4 HOLE FIXATION The Science of Fusion PACH_v6.indd 1 6/03/2015 7:10 am PACH Plate Design Rationale The PACH Plate has been designed to be used as an anterior or lateral fixation plate for the thoracolumbar,
2 OR 4 HOLE FIXATION The Science of Fusion PACH_v6.indd 1 6/03/2015 7:10 am PACH Plate Design Rationale The PACH Plate has been designed to be used as an anterior or lateral fixation plate for the thoracolumbar,
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Spinal Terminology Basics
 Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
