Author's Accepted Manuscript
|
|
|
- Joseph Burns
- 5 years ago
- Views:
Transcription
1 Author's Accepted Manuscript Urologic Outcome of the Xiao Procedure in Children with Myelomeningocele and Lipomyelomeningocele Undergoing Spinal Cord Detethering: Results of A Randomized, Prospective, Double Blind Study Gerald F. Tuite, Yves Homsy, Ethan G. Polsky, Margaret A. Reilly, Carolyn M. Carey, S. Parrish Winesett, Luis F. Rodriguez, Bruce B. Storrs, Sarah J. Gaskill, Lisa L. Tetreault, Denise G. Martinez, Ernest K. Amankwah PII: S (16) DOI: /j.juro Reference: JURO To appear in: The Journal of Urology Accepted Date: 31 May 2016 Please cite this article as: Tuite GF, Homsy Y, Polsky EG, Reilly MA, Carey CM, Winesett SP, Rodriguez LF, Storrs BB, Gaskill SJ, Tetreault LL, Martinez DG, Amankwah EK, Urologic Outcome of the Xiao Procedure in Children with Myelomeningocele and Lipomyelomeningocele Undergoing Spinal Cord Detethering: Results of A Randomized, Prospective, Double Blind Study, The Journal of Urology (2016), doi: /j.juro DISCLAIMER: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our subscribers we are providing this early version of the article. The paper will be copy edited and typeset, and proof will be reviewed before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to The Journal pertain. Embargo Policy All article content is under embargo until uncorrected proof of the article becomes available online. We will provide journalists and editors with full-text copies of the articles in question prior to the embargo date so that stories can be adequately researched and written. The standard embargo time is 12:01 AM ET on that date. Questions regarding embargo should be directed to jumedia@elsevier.com.
2 1 2 3 Urologic Outcome of the Xiao Procedure in Children with Myelomeningocele and Lipomyelomeningocele Undergoing Spinal Cord Detethering: Results of A Randomized, Prospective, Double Blind Study Gerald F. Tuite, MD, 1,4,5 Yves Homsy, MD, 7 Ethan G. Polsky, MD, 7 Margaret A. Reilly, PT, 2 Carolyn M. Carey, MD, MBA, 1,5 S. Parrish Winesett, MD, 6 Luis F. Rodriguez, MD, 1,5 Bruce B. Storrs, MD, 1,5 Sarah J. Gaskill, MD, 5 Lisa L. Tetreault, RN, CCRP, 3 Denise G. Martinez, MPH, 3 and Ernest K. Amankwah, PhD 3 1 Division of Pediatric Neurosurgery, Neuroscience Institute, 2 Department of Occupational and Physical Therapy, and 3 Clinical and Translational Research Organization, Johns Hopkins All Children s Hospital, Saint Petersburg, Florida; 4 Department of Pediatrics, Johns Hopkins Medicine, Baltimore, Maryland; 5 Division of Pediatric Neurosurgery, Department of Neurosurgery and Brain Repair, 6 Division of Pediatric Neurology, Department of Pediatrics, and Department of Urology7, The University of South Florida, Tampa, Florida Correspondence Gerald Tuite, Institute for Brain Protection Sciences, Johns Hopkins All Children s Hospital, Division of Pediatric Neurosurgery, 601 5th St. S, Ste. 511, Saint Petersburg, Florida Tel: FAX: gtuite1@jhmi.edu. Running Head: Double Blinded RCT of the Xiao Procedure In Spina Bifida Key Words spina bifida; tethered spinal cord; urination; Xiao procedure; nerve transfer Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. This work was financially supported primarily by a research grant from the All Children s Hospital Foundation. Additional financial support was provided by the AANS/CNS Joint Section on Pediatric Neurosurgery and the AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves. 1
3 Abstract Purpose: Although previous studies have reported high success rates (70-85%) after an intradural somatic-to-autonomic nerve transfer procedure in children with spinal dysraphism, none of the studies had a control group or blinded observers. Herein we report on a rigorously designed study to investigate the effectiveness of the Xiao procedure. Materials and Methods: Children with neurogenic bladder dysfunction related to myelomeningocele or lipomyelomeningocele, who required spinal cord detethering (DT), were randomized between two groups at the time of surgery: half underwent only DT and half underwent the Xiao procedure (XP) in addition to spinal cord detethering (DT+X). Double blinded evaluations were performed at regular intervals during the 3-year follow-up. Results: 10 patients underwent only DT and 10 underwent DT+X. The XP did not result in voluntary voiding or continence in any patient, but patients in DT+X were more likely to have greater improvements in total bladder capacity, bladder over-activity and overall quality of life than those who only underwent DT. By the end of the study, none of the double blinded participants or evaluators were able to accurately predict to which group the patients had been assigned. Conclusions: The results of this RCT are in agreement with recently published, similarly disappointing results of the Xiao procedure in spinal cord injury. Improvements in bladder parameters observed in this study may be related to sacral nerve root section, a necessary portion of the XP, instead of reinnervation. Confirmatory animal studies are recommended before further clinical trials of the XP in humans are performed. 2
4 INTRODUCTION The Xiao Procedure (XP), which creates a skin-cns-bladder reflex through an intradural lumbosacral nerve transfer, has been reported to result in voluntary voiding in patients with neurogenic bladder dysfunction related to spinal cord injury and spina bifida. 1-6 However, recent studies of the XP in patients with spinal cord injury (SCI), by other investigators, did not result in measureable benefit to patients, raising concern about the reproducibility of Xiao s results. Our group recently published the initial results of a randomized, prospective, double blinded trial of the XP in 20 children undergoing spinal cord detethering. 11 In summary, all patients remained incontinent, wore pull-ups or diapers, and were unable to initiate or control their own urination in a meaningful way before and at all intervals during the three year follow-up. Urodynamic bladder contractions (Pdet > 10 cm H20) in response to scratching occurred in many patients who did and did not undergo the XP. No patient who underwent the XP had reliable, reproducible scratch-initiated bladder contractions or controlled voiding after surgery. 11 Here we report more detailed results pertaining to urologic outcomes and the patients perception of their results. METHODS Please refer to our previous publication for details regarding IRB approval (# ), methodological details and initial results. 11 Briefly, any patient less than 21 years of age, with neurogenic bladder dysfunction related to spina bifida, who was scheduled for spinal cord detethering for the usual reasons, was eligible for enrollment in the study. Patients underwent detailed evaluations at regular intervals throughout the three year follow-up. All patients and evaluators were blinded throughout the study to the surgical procedure that was performed. 11 Urodynamic testing was done with retrograde filling and patch EMG in accordance with the International Children s Continence Guidelines 12 using the Aquarius TT system (Laborie, Williston, Vermont). All urodynamic studies were performed by a urodynamic technologists along with the study nurse coordinator (LLT). A rectal catheter was used to measure abdominal pressure. The bladder was filled cc/min to the total bladder capacity (TBC), determined by a sensation of fullness or discomfort, signs of autonomic dysreflexia, a significant leak around the catheter or a major sustained spike in bladder pressure. Once the TBC was reached, 20% of the volume was released and systematic scratching of the lower extremities ensued. Patients underwent urodynamic studies before surgery and at 6, 9, 12, 18, 24 and 36 months after surgery. We report results at one year intervals because they are very similar to the results at the other time intervals All patients completed the same questionnaires utilized by Peters et al in their previous study of the Xiao procedure in patients with spina bifida. 4, 5 Clean intermittent catheterization (CIC) and all 3
5 bladder active medications (antispasmodics and anticholinergics, BAMs) were discontinued two weeks prior to surgery and were only reinstituted during the three year follow-up if the upper tracts were at risk, as defined by the protocol outlined in the supplement (Supp. Table 1). After patients completed the entire study, patients, both study urologists and the research coordinator all tried to predict the group to which the patient has been randomized. Decisions about reinstitution of CIC and BAMs after completion of the study were made based on typical clinical parameters. The management of bowel function was directed by the usual caregivers and health care providers, not by a specific protocol. RESULTS Summary of Baseline Characteristics and Surgical Details (Supp Tables 2,3 and 4) Of the 20 patients enrolled in the study, 10 underwent DT and 10 underwent DT+X. The distribution of baseline characteristics between the two groups were similar, except that patients in DT+X were younger and less likely to be utilizing CIC and taking BAMs prior to surgery when compared to DT. DT+X donor roots were as follows: L5=5, L4=2, S1=2, T11=1. Recipient roots in DT +X were as follows: S3/4=7, S2/3/4=1, S3=1, S2=1. Nerve grafts were utilized in two patients. 11 Five patients in DT+X had worsening urologic symptoms as their primary indication for detethering: Three developed LPP>40 cm H20 and two had a decline in TBC associated with frequent UTIs and leaking between catheterizations. Urge to Urinate, CIC, and Bladder Active Medications (Figure 1, Supp Table 3) Before surgery, 20% of DT+X and 50% of DT felt the urge to void. By one year after surgery, two additional patients in both groups felt the urge to void. Of the patients who did not have the urge to urinate before surgery, 3 of 8 (37%) in DT+X and 2 of 5 (40%) in DT felt to the urge to urinate at study completion. CIC was utilized before surgery in 40% of DT+X and 70% of DT. Most patients were able to stay off CIC throughout the study. After study completion, when patients and their urologists made decisions about catheterization based on clinical symptoms, 5 of 9 (56%) in DT+X and 5 of 8 (62%) in DT chose to utilize CIC. Before surgery, BAMs were used in 40% of DT+X and 50% of DT. Most patients in both groups were able to safely stay off BAMs during the study period, however, by the end of the study, 2 patients in both groups chose to return to BAMs. There were no statistically significant differences in the urge to urinate, the use of CIC or the use of BAMs when comparing the DT+X to DT group at any point in the study Total Bladder Capacity (Figure 2, Supp Table 4) Baseline TBC was lower in DT+X compared to DT (medians: 136 vs. 188 cc, p = 0.17). The median TBC, when compared to baseline, increased more in DT+X than DT (medians: 1 yr 59cc vs. 36cc, p = 0.36; 4
6 yrs 107cc vs. 78cc, p = 0.42; 3 yrs: 100cc vs. 66cc, p = 0.22). Overall there were no significant differences in TBC between the groups at the different time points; however, two patients in DT+X had large increases in TBC compared to baseline (179cc and 356cc), while the TBC decreased for three patients in DT by the end of the study. Patient 5 (DT+X) did not have her TBC included in the two and three year analyses because she had undergone bladder augmentation at 18 months. By comparing the actual change in TBC to the age related increase in TBC predicted by the Hjälmås formula (30+age in years X 30), there were greater improvements in TBC in DT+X compared to DT (p = 0.14). 13 Leak Point Pressure (Supp Table5) Prior to surgery, 3 patients in both groups had LPP > 40 cm H2O and one patient in each group did not leak at all during bladder filling. By one year, LPP increased in 4 patients in DT (< 40 cm H2O before surgery, > 40 cm H2O after), but none of those in DT+X had a similar increase. LPPs worsened with time in the DT+X group, but not as severely as those in the DT group: By 3 years, 90% of patients in DT had no leak or a LPP > 40 cm H2O, compared to 5 of 9 (56%) in DT+X. The bladders of six patients in DT transitioned from a LPP < 40 cm H2O before surgery to either no leak or a LPP > 40 cm H2O. However, only two patients in DT+X had a similar worsening in their LPP over three years. Uninhibited Detrusor Contractions (Supp Table 5) Prior to surgery, 90% of DT+X and 80% of DT had UDCs > 15cm H2O. By one year, 2 of 9 (22%) of DT+X had resolution of their previous UDCs, but none improved in DT. By three years, UDCs had resolved in 2 of 9 (22%) of DT+X and 1 of 8 (13%) of DT. Reactivity of Neurogenic Bladder (Supp Table 5) Prior to surgery, 80% of patients in each group were considered to have overactive neurogenic bladders. Over the three year study period, patients in DT+X more frequently experienced a decrease in bladder contractility than those in DT. 3 of 8 (38%) overactive bladders in DT+X and 1 of 8 (13%) in DT normalized their contractility at three years. Two patients in both groups transitioned from underactive neurogenic bladder prior to surgery to overactive bladders by three years. Global Questionnaires Related to Strength, Quality of Life, Bladder and Bowel Function (Figure 3, Supp Table6) Patients perception of their bladder, bowel, and lower extremity motor function throughout the study were not statistically different when comparing the two groups at every time point. 70% of DT+X felt their ability to void had improved by one year compared to 50% of DT. By three years, 67% of DT+X felt voiding had improved compared to 40% of DT. By three years, none of the DT+X patients felt their voiding ability had worsened, but 3 of 10 did in DT At one year, half the patients in both groups felt their ability to move their bowels had improved, without significant change throughout the remaining two years. At year 2 and 3, a higher proportion of patients in the DT compared to DT+X felt their ability to move their bowels had improved. 5
7 Patients in DT felt their lower extremity leg strength had declined more than those in the DT+X: by three years, four patients in the DT group and one patient in the DT+X group felt their legs were weaker at three years than they were before surgery Improvements in patients overall quality of life (QOL) at the end of the study was greater in DT+X than in DT. At one year, 80% of patients in DT+X and 70% of DT felt their QOL was better. By three years, all patients in DT+X felt their QOL was better, but only 30% of those in DT were better than before their surgery (p = 0.003). Review of the overall data for these 5 patients showed that 4 of 5 whose quality of life worsened also had a decline in the assessment of their lower extremity strength. Of note, all four of those patients were 13 years of age or older when they enrolled in the study. All patients in the DT+X were 9 years old or younger at enrollment, with the exception of one 16 year old. Accuracy of Predicting Which Patients Underwent the Xiao Procedure (Supp Table 7) 10 of 18 (56%) of patients and their parents thought they had been assigned to DT+X, however their predictions were only accurate 44% of the time (kappa = -0.1, p = 0.67). The blinded urologists only agreed on the group assignment in 6 of 20 (30%) of the cases and each one of them was correct only 55% of the time (kappa = 0.1, p = 0.65). The research nurse, who was most familiar with every aspect of the patient s assessment, only correctly predicted the treatment arm 50% of the time (kappa = 0, p >0.99). Resumption of CIC and BAMs After The Study Was Complete (Supp Table 3) One patient in each group utilized CIC before the study and did not need to use CIC after completion of the study. However, most patients in both groups who were using CIC before the study chose to return to CIC when the study was complete. 3 patients in DT+X who did not use CIC before the study were placed on CIC after the study was complete. Most patients resumed their pre-study use or lack of utilization of BAMs at the end of the study. Two patients in both groups who used BAMs prior to the study did not resume them at the end of the study. DISCUSSION Xiao et al have published extensively on the somatic-to-autonomic intradural anastomosis, taking the concept from bench to bedside in a series of studies involving animals, patients with spinal cord injury, and children with spina bifida. 6, 10, Their results, which suggested an 86.2% rate of bladder control 6, have not been reproducible by other investigators. 6 Two well-designed European studies of adults with spinal cord injury failed to produce reflex initiated bladder contractions or meaningful urination. 7, 8 CG Xiao, in an editorial regarding the 2014 study from Denmark that failed to show a positive outcome, attributed the lack of success by other investigators to the use of BAMs after surgery. 20 Our study reported here utilized very little or no BAMs in our patients after surgery. 9 6
8 Results of the procedure in patients with spina bifida are predictably more difficult to interpret due to the presence of partial bladder and bowel function in most patients. In their study of children with spina bifida who underwent the Xiao procedure, Peters et al found scratch initiated urodynamic contractions more similar to Xiao s results than ours, but they failed to reproduce the dramatic control of urination and continence described by Xiao et al and others. 4, 5 While the results of Peters et al were concerning for a lack of duplication of the spectacular results of Xiao et al, many were still encouraged by their results. 4, 5 Our studyshowed that many of the results attributed to the performance of the Xiao Procedure may have, in fact, been related to spinal cord detethering, placebo or the effect of sacral rhizotomy. 11 For example, the greater increase in TBC, the lessened likelihood of developing elevated LPPs, and the more frequent resolution of UDCs in DT+X patients could all be related to the effect of the sacral rhizotomy that is performed during the Xiao 21, 22 Procedure, instead of the effect of reinnervation. Patients in the DT+X group had a more significant improvement in QOL at years 2 and 3, which may be attributable to an outcome that we may not have measured as part of our study. We believe the greater improvement in patients who underwent the Xiao procedure is more likely attributable to the younger age, less decline in leg function and/or a greater imrprovment in TBC in patients in DT+X. Even though we employed a randomized, double blinded methodology, our results are limited by the small sample size and/or the inclusion of only patients undergoing detethering. The randomization of younger patients to DT+X, though likely the result of chance, may have also influenced our results. The questionnaires that form the basis of the subjective measures of outcome were the same as those used by Peters et al 5, but the reliability of these questionnaires has not been validated in separate studies. CONCLUSIONS Performance of the Xiao Procedure during spinal cord detethering in patients with spina bifida was more likely to lead to improvements in QOL, TBC, bladder over-activity, and leak point pressure, all of which may be attributable to the effect of sacral rhizotomy instead of bladder reinnervation. The Xiao procedure did not result in voluntary voiding or continence in any patient. These results, in combination with results of other recently published studies, suggest that further basic science/animal studies should be performed before further clinical trials of the Xiao Procedure are performed in humans. Figure Legends: Figure 1: Patients CIC use before, during and after completion of the study. Most patients were able to stay off CIC and BAMs (Supplemental Table 3) during the study, as recommended by Xiao et al. 6 7
9 Patients undergoing the Xiao procedure during spinal cord detethering were not more likely to stay off CIC than those who only underwent detethering at most time points Figure 2: Total bladder capacity (TBC)after surgery.. When comparing actual TBC to the expected TBC based on age, patients in DT+X had a greater improvement in TBC than those who underwent only DT. 13 Figure 3: Patient and family responses to the same global questionnaires utilized by Peters et al 4, 5, assessing their perceived changes in foot and leg strength (3a), and their overall quality of life (3b). There were no statistically significant differences in their responses to the questionnaires, except for a greater improvement in quality of life for patients who underwent the Xiao procedure ((p = 0.003). Patients in DT had more worsening in foot and leg strength than patients in DT+X. References: 1. Lin, H., Hou, C., Chen, A.: Reconstructed bladder innervation above the level of spinal cord injury to produce urination by abdomen-to-bladder reflex contractions. J Neurosurg Spine, 14: 799, Lin, H., Hou, C., Zhen, X. et al.: Clinical study of reconstructed bladder innervation below the level of spinal cord injury to produce urination by Achilles tendon-to-bladder reflex contractions. J Neurosurg Spine, 10: 452, Lin, H., Hou, C. L., Zhong, G. et al.: Reconstruction of reflex pathways to the atonic bladder after conus medullaris injury: preliminary clinical results. Microsurgery, 28: 429, Peters, K. M., Gilmer, H., Feber, K. et al.: US Pilot Study of Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida: 3-Year Experience. Adv Urol, 2014: , Peters, K. M., Girdler, B., Turzewski, C. et al.: Outcomes of lumbar to sacral nerve rerouting for spina bifida. J Urol, 184: 702, Xiao, C. G.: Xiao Procedure for Neurogenic Bladder in Spinal Cord Injury and Spina Bifida. Curr Bladder Dysfunct Rep, 7: 83, Rasmussen, M. M., Rawashdeh, Y. F., Clemmensen, D. et al.: The artificial somato-autonomic reflex arch does not improve lower urinary tract function in patients with spinal cord lesions. J Urol, Sievert, K. D., Amend, B., Roser, F. et al.: Challenges for Restoration of Lower Urinary Tract Innervation in Patients with Spinal Cord Injury: A European Single-center Retrospective Study with Long-term Follow-up. Eur Urol, Tuite, G. F., Storrs, B. B., Homsy, Y. L. et al.: Attempted bladder reinnervation and creation of a scratch reflex for bladder emptying through a somatic-to-autonomic intradural anastomosis. J Neurosurg Pediatr, 12: 80, Xiao, C. G., Du, M. X., Li, B. et al.: An artificial somatic-autonomic reflex pathway procedure for bladder control in children with spina bifida. J Urol, 173: 2112, Tuite, G. F., Polsky, E. G., Homsy, Y. L. et al.: Lack of efficacy of an intradural somatic-toautonomic nerve anastomosis (Xiao procedure) for bladder control in children with myelomeningocele and lipomyelomeningocele: results of a prospective, randomized, doubleblind study. J Neurosurg Pediatr, Schafer, W., Abrams, P., Liao, L. et al.: Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn, 21: 261,
10 Hjalmas, K.: Urodynamics in normal infants and children. Scand J Urol Nephrol Suppl, 114: 20, Dai, C. F., Xiao, C. G.: Electrophysiological monitoring and identification of neural roots during somatic-autonomic reflex pathway procedure for neurogenic bladder. Chin J Traumatol, 8: 74, Wang, H. Z., Li, S. R., Wen, C. et al.: Morphological changes of cholinergic nerve fibers in the urinary bladder after establishment of artificial somatic-autonomic reflex arc in rats. Neurosci Bull, 23: 277, Xiao, C. G.: Reinnervation for neurogenic bladder: historic review and introduction of a somaticautonomic reflex pathway procedure for patients with spinal cord injury or spina bifida. Eur Urol, 49: 22, Xiao, C. G., de Groat, W. C., Godec, C. J. et al.: "Skin-CNS-bladder" reflex pathway for micturition after spinal cord injury and its underlying mechanisms. J Urol, 162: 936, Xiao, C. G., Du, M. X., Dai, C. et al.: An artificial somatic-central nervous system-autonomic reflex pathway for controllable micturition after spinal cord injury: preliminary results in 15 patients. J Urol, 170: 1237, Xiao, C. G., Godec, C. J.: A possible new reflex pathway for micturition after spinal cord injury. Paraplegia, 32: 300, Xiao, C. G.: Re: The Artificial Somato-Autonomic Reflex Arch Does Not Improve Lower Urinary Tract Function in Patients with Spinal Cord Lesions: M. M. Rasmussen, Y. F. Rawashdeh, D. Clemmensen, H. Tankisi, A. Fuglsang-Frederiksen, K. Krogh and P. Christensen J Urol 2015;193: J Urol, 194: 1828, Schneidau, T., Franco, I., Zebold, K. et al.: Selective sacral rhizotomy for the management of neurogenic bladders in spina bifida patients: long-term followup. J Urol, 154: 766, Storrs, B. B.: Selective posterior rhizotomy for treatment of progressive spasticity in patients with myelomeningocele. Preliminary report. Pediatr Neurosci, 13: 135,
11 Supplementary Table 1: Discontinuation of Bladder Active Medications (BAMs) and Clean Intermittent Catheterization (CIC) New patients entered into the study All patients will have all BAMs and CIC discontinued at least two weeks prior to the preoperative urodynamic studies and the preoperative questionnaires BAMs and CIC will be reinstituted per protocol (see below) Protocol for ultrasound monitoring after cessation of CIC and BAMs All patients undergo routine renal ultrasounds (RUS), regardless of symptoms Once a month after CIC and BAMs stopped If stable or improved after three monthly RUS, perform RUS every three months If RUS stable or improved after one year, start RUS once a year Criteria for restarting CIC (do not start BAMs simultaneously) Symptomatic failure o Urinary retention o Two symptomatic urinary tract infections (UTIs)(T>101.5, catheter culture proven) within six months Ultrasound failure o Worsening or new hydronephrosis If CIC reinstituted, criteria for adding BAMs If UTIs persist despite reinstitution of CIC, restart BAMs If no improvement in RUS after reinstitution of CIC, restart BAMs If only CIC was reinstituted, criteria for cessation If CIC was reinstituted for retention or UTI: terminate CIC after three months if symptoms or UTIs resolved If CIC was reinstituted for RUS changes: terminate CIC after six weeks if the repeat RUS has improved If CIC and BAMs are reinstituted, terminate both and start the monthly RUS monitoring again If CIC and BAMs reinstituted for retention or UTIs: If RUS is stable or improved and no symptomatic UTIs develop, terminate CIC and BAMs and restart RUS monitoring monthly according to protocol upon entry into the study If CIC or BAMs reinstituted because of RUS changes: After three months, if RUS improves when compared to the RUS that prompted reintroduction of the CIC and BAMs, stop both CIC BAMs and restart RUS monthly according to protocol upon entry into the study. Urology Journal 1 6/8/ :52 AM
12 Supplementary Table 2: Baseline characteristics DT+X DT Variable N (%) N (%) p-value Gender > Male 6(60) 7(70) Female 4(40) 3(30) Age Mean + SD 7.3(4.4) 9.7(5.4) Median (range) 6.5(1-16) 9.5(1-18) Type of spina bifida > MM 8(80) 8(80) LMM 2(20) 2(20) In utero MM repair > No 7(87.5) 7(87.5) Yes 1(12.5) 1(12.5) Previous spinal cord surgery Mean + SD 1.3(0.5) 1.7(0.8) Median (range) 1(1-2) 2(0-3) Syrinx present No 6(60) 3(30) Yes 4(40) 7(70) Primary reason for spinal cord detethering.07 1 Back pain 2(20) 1(10) LE weakness 0(0) 4(40) Foot/leg deformity 2(20) 0(0) Urologic symptoms 5(50) 2(20) Scoliosis 1(10) 3(30) Ambulatory status > Walks, w/o devices 1(10) 1(10) Walks w/ devices 6(60) 6(60) Can t walk, can stand w/ 2(20) 1(10) devices Can t walk or stand 1(10) 2(20) 1 Fisher s exact test; 2 Independent t-test; 3 Mann-Whitney U-test Urology Journal 1 6/8/ :52 AM
13 Supplementary Table 3: Urologic outcomes: Urge to urinate, clean intermittent catheterization, bladder active medication Urge to Urinate On CIC On BAMs Pt. BL 1 yr 2 yr 3 yr BL 1 yr 2 yr 3 yr Post study BL 1 yr 2 yr 3 yr Post study DT+X = = = = = = = na na na + + na na na = + - na na na = = = = = na - = = = = = = Total % DT = na = na = = = = = = na = na = = = = = = = = = = = = = = = Total % DT= Detethering only, DT+X= Detethering plus Xiao, BL = Baseline, CIC = clean intermittent catheterization, BAM = bladder active medications, = change from baseline comparing results at three years to those before surgery, na = no data, ( ) = better, ( ) = worse, (=) = no change. Urology Journal 1 6/8/ :52 AM
14 Supplementary Table 4: Total bladder capacity (cc) Pt. Age BL 1 yr 2 yr 3 yr DT+X na na na na Mean (SD) 193 (160) 250(215) 271 (119) 286 (146) 84 (129) Median (Range) 136(74-600) 195 (50-775) 243 ( ) 236 (88-495) 79 ( ) DT Mean (SD) 245 (154) 242 (121) 271 (142) 262 (254) 18 (116) Median (Range) 188 (39-469) 224 (98-448) 266 ( ) 254 (90-500) 34 ( ) DT= Detethering only, DT+X= Detethering plus Xiao, BL = baseline, = change from base line: TBC at 3 years minus baseline Urology Journal 1 6/8/ :52 AM
15 Supplementary Table 5: Urodynamic outcomes: Leak point pressure, uninhibited detrusor contractions, type of neurogenic bladder. Uninhibited Detrusor Leak Point Pressure Contractions > 10 cm H 2 O Type of Neurogenic Bladder Pt. BL 1 yr 2 yr 3 yr BL 1 yr 2 yr 3 yr BL 1 yr 2 yr 3 yr DT+X 1 >40 NLk <40 < O O N N 2 <40 <40 <40 < O U N O 3 NLk >40 NLk NLk O O U N 4 >40 <40 <40 > O N N O 5 >40 <40 na na + + na na O O na na 12 <40 <40 <40 > U N O O 15 <40 <40 <40 < U O N O 16 <40 <40 <40 < O O O N 17 na NLk NLk NLk O N O O 19 <40 <40 >40 > O O O O Totals 90% 70% 56% 78% DT 6 <40 <40 <40 NLk O O O O 7 >40 >40 >40 NLk O O O O 8 >40 >40 >40 > O O N O 9 NLk <40 >40 < O O N O 10 >40 >40 >40 > O O O O 11 <40 >40 NLk NLk U O O O 13 <40 <40 NLk NLk U U N O 14 <40 >40 >40 NLk O O O O 18 <40 >40 >40 NLk O O O N 20 <40 >40 >40 > O O O O Totals 80% 100% 80% 90% DT= Dethethering only, DT+X= Detethering plus Xiao, NLk = no leak, O = overactive, U = underactive, N = neutral (neither overactive or hyperactive), ( ) = better, ( ) = worse, (=) = no change, (+) = yes, (-) = no, na = no data 40 and >40 = cmh2o Urology Journal 1 6/8/ :52 AM
16 Supplementary Table 6: Global follow-up questionnaires at one, two and three years Ability to move bowels Ability to void Foot and leg strength Quality of life Pt 1 yr 2 yr 3yr 1 yr 2 yr 3 yr 1 yr 2 yr 3 yr 1 yr 2 yr 3 yr DT+X 1 = 2 = = = 3 = = = = = 4 = = = 5 = na na = na na = na na = na na 12 = = = = = 15 = = = = = 16 na na na na = = = = = = = = DT 6 = = = = = = = = = = = = 7 = = = = = = 8 = 9 10 = 11 = = = = 13 = = = = = = = = = = = 20 = DT=Detethering only, DT+X= detethering plus Xiao, ( ) =improved, ( ) = worse, (=) = no change, na = no data Urology Journal 1 6/8/ :52 AM
17 Supplementary Table 7: End of study predictions by study subjects, their parents and other blinded investigators as to whether the Xiao procedure had been performed. Patient. & Family Study Nurse Urologist 1 Urologist 2 Pt. DT+X 1 DT+X DT+X DT DT+X 2 DT+X DT+X DT+X DT 3 DT+X DT+X DT+X DT 4 DT+X DT DT DT 5 DT DT DT DT 12 DT+X DT DT+X DT 15 DT DT DT DT 16 DT DT DT DT 17 DT+X DT+X DT+X DT 19 DT DT DT DT+X % correct 60% 40% 40% 20% DT 6 na DT DT+X DT 7 DT+X DT+X DT+X DT+X 8 DT DT DT DT 9 DT+X DT+X DT+X DT 10 na DT+X DT DT 11 DT DT DT DT+X 13 DT DT+X DT+X DT 14 DT+X DT DT DT 18 DT DT DT DT 20 DT+X DT DT+X DT+X % correct 50% 60% 50% 70% DT = detethering only, DT + X = detethering + Xiao procedure, na =not available Urology Journal 1 6/8/ :52 AM
18
19
20
21
22 Abbreviations: BAM = Bladder Active Medications (anticholinergics, antimuscurinics, antispasmodics), CIC = Clean Intermittent Catheterization, DT = Detethering only, DT+X =Detethering plus Xiao, LPP = Leak Point Pressure, Pdet = Detrusor Pressure measurement, QOL = Quality of Life, RUS = Renal Ultrasound, SCI = Spinal Cord Injury, TBC = Total Bladder Capacity, UDC = Uninhibited Detrusor Contractions, XP = Xiao procedure (intradural somatic-to-autonomic bladder reinnervation procedure)
Neurogenic bladder dysfunction related to spinal
 clinical article J Neurosurg Pediatr 18:150 163, 2016 Lack of efficacy of an intradural somatic-to-autonomic nerve anastomosis (Xiao procedure) for bladder control in children with myelomeningocele and
clinical article J Neurosurg Pediatr 18:150 163, 2016 Lack of efficacy of an intradural somatic-to-autonomic nerve anastomosis (Xiao procedure) for bladder control in children with myelomeningocele and
Clinical Study US Pilot Study of Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida: 3-Year Experience
 Advances in Urology, Article ID 863209, 7 pages http://dx.doi.org/10.1155/2014/863209 Clinical Study US Pilot Study of Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida:
Advances in Urology, Article ID 863209, 7 pages http://dx.doi.org/10.1155/2014/863209 Clinical Study US Pilot Study of Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida:
Original Paper. Urol Int DOI: /
 Urologia Internationalis Original Paper Received: May 17, 2016 Accepted after revision: August 3, 2016 Published online: October 28, 2016 Experimental Electrophysiological and Pressure Responses of Urinary
Urologia Internationalis Original Paper Received: May 17, 2016 Accepted after revision: August 3, 2016 Published online: October 28, 2016 Experimental Electrophysiological and Pressure Responses of Urinary
Disclosures. Background. Expanding the Xiao Concept to Spina Bifida
 Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal
Lumbar to Sacral Nerve Rerouting to Restore Voiding and Bowel Function in Spina Bifida Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele?
 Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele? Grace Yoshiba BS Chris Halline, BA Earl Y. Cheng MD Theresa A. Meyer RN Ilina Rosoklija MPH Robin Bowman MD Elizabeth
Lipomyelomeningocele for the Urologist: should we view it the same as myelomeningocele? Grace Yoshiba BS Chris Halline, BA Earl Y. Cheng MD Theresa A. Meyer RN Ilina Rosoklija MPH Robin Bowman MD Elizabeth
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Neurogenic Bladder. Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, Eric Levey, M.D.
 Neurogenic Bladder Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical Officer,
Neurogenic Bladder Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical Officer,
Evidence Summary: The inflow Urinary Prosthesis FDA De Novo Approval DEN130044
 Evidence Summary: The inflow Urinary Prosthesis FDA De Novo Approval DEN130044 Unique alternative to urinary catheters for women with permanent urinary retention Therapeutic benefits o Highly effective
Evidence Summary: The inflow Urinary Prosthesis FDA De Novo Approval DEN130044 Unique alternative to urinary catheters for women with permanent urinary retention Therapeutic benefits o Highly effective
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach)
 Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Brief Reports. Cystometric Evaluation of Voiding Dysfunctions
 Brief Reports Cystometric Evaluation of Voiding Dysfunctions Pawanindra Lal Navneet Kaur Anurag Krishna Not infrequently, in pediatric practice one is confronted by anxious parents of children with voiding
Brief Reports Cystometric Evaluation of Voiding Dysfunctions Pawanindra Lal Navneet Kaur Anurag Krishna Not infrequently, in pediatric practice one is confronted by anxious parents of children with voiding
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
2/9/2008. Men Women. Prevalence of OAB. Men: 16.0% Women: 16.9% Prevalence (%) < Age (years)
 Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
CHAPTER 1 INTRODUCTION
 Introduction 1 CHAPTER 1 INTRODUCTION 8 Introduction Spina bifida is a congenital defect of the spine in 1-3 out of 1000 live born children 1 and still is one of the most common serious congenital malformations.
Introduction 1 CHAPTER 1 INTRODUCTION 8 Introduction Spina bifida is a congenital defect of the spine in 1-3 out of 1000 live born children 1 and still is one of the most common serious congenital malformations.
Management of neurogenic bladder in children. In: Guidelines on paediatric urology.
 Complete Summary GUIDELINE TITLE Management of neurogenic bladder in children. In: Guidelines on paediatric urology. BIBLIOGRAPHIC SOURCE(S) Management of neurogenic bladder in children. In: Tekgul S,
Complete Summary GUIDELINE TITLE Management of neurogenic bladder in children. In: Guidelines on paediatric urology. BIBLIOGRAPHIC SOURCE(S) Management of neurogenic bladder in children. In: Tekgul S,
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Neuropathic bladder and spinal dysraphism
 Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
Elimination Patterns: Bladder
 Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
NON-Neurogenic Chronic Urinary Retention AUA White Paper
 NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Management of the Urinary Tract in Spina Bifida Cases Varies With Lesion Level and Shunt Presence
 Neuropathic Bladder Management of the Urinary Tract in Spina Bifida Cases Varies With Lesion Level and Shunt Presence Peter Metcalfe,* Darren Gray and Darcie Kiddoo From the Division of Pediatric Surgery,
Neuropathic Bladder Management of the Urinary Tract in Spina Bifida Cases Varies With Lesion Level and Shunt Presence Peter Metcalfe,* Darren Gray and Darcie Kiddoo From the Division of Pediatric Surgery,
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Robotic Appendicovesicostomy
 Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
NEUROPATHIC BLADDER DISORDERS
 NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
Department of Paediatric Surgery, All India Institute of Medical Sciences, New Delhi , India
 Original Article A Clinical and Urodynamic Study on the Effects of Oral Tolterodine on Serial Alterations in Neurogenic Detrusor Overactivity vis-à-vis Oral Oxybutynin in Children (Existing Oxybutynin
Original Article A Clinical and Urodynamic Study on the Effects of Oral Tolterodine on Serial Alterations in Neurogenic Detrusor Overactivity vis-à-vis Oral Oxybutynin in Children (Existing Oxybutynin
european urology 49 (2006) 22 29
 european urology 49 (2006) 22 29 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review - Neuro-urology Reinnervation for Neurogenic Bladder: Historic Review and Introduction
european urology 49 (2006) 22 29 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review - Neuro-urology Reinnervation for Neurogenic Bladder: Historic Review and Introduction
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME?
 URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
In Utero Closure of Myelomeningocele Does Not Improve Lower Urinary Tract Function
 In Utero Closure of Myelomeningocele Does Not Improve Lower Urinary Tract Function Nora G. Lee, Pablo Gomez, Vikrant Uberoi, Paul J. Kokorowski, Shahram Khoshbin, Stuart B. Bauer and Carlos R. Estrada*
In Utero Closure of Myelomeningocele Does Not Improve Lower Urinary Tract Function Nora G. Lee, Pablo Gomez, Vikrant Uberoi, Paul J. Kokorowski, Shahram Khoshbin, Stuart B. Bauer and Carlos R. Estrada*
URODYNAMICS. Your urodynamic study is scheduled at the Ambulatory Procedure Center. This is located at 4-South waiting room at the Altru Main Clinic.
 Altru HEALTH SYSTEM URODYNAMICS Your urodynamic study is scheduled at the Ambulatory Procedure Center. This is located at 4-South waiting room at the Altru Main Clinic. Arrival Time: Appointment Date:
Altru HEALTH SYSTEM URODYNAMICS Your urodynamic study is scheduled at the Ambulatory Procedure Center. This is located at 4-South waiting room at the Altru Main Clinic. Arrival Time: Appointment Date:
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Impact of urethral catheterization on uroflow during pressure-flow study
 Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Outcomes Primary Outcomes Secondary Outcomes Tertiary Outcomes
 Urology David Joseph, MD, Chair Hadley Wood, MD Elizabeth Yerkes, MD Dominic Frimberger, MD Michelle Baum, MD Rose Khavari, MD Rosalie Misseri, MD Stacey Tanaka, MD Sharon Baillie, RN Outcomes Primary
Urology David Joseph, MD, Chair Hadley Wood, MD Elizabeth Yerkes, MD Dominic Frimberger, MD Michelle Baum, MD Rose Khavari, MD Rosalie Misseri, MD Stacey Tanaka, MD Sharon Baillie, RN Outcomes Primary
Incontinence. When I was given this topic in urology to discuss with you today I
 Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
Male LUTS. Dr. Brian Ho. Division of Urology Department of Surgery Queen Mary Hospital
 Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Comparison of the Effects by Obybutynin and Tolterodine on Spina Bifida Patients: A Pilot Crossover Study
 LUTS (2011) 3, 99 103 ORIGINAL ARTICLE Comparison of the Effects by Obybutynin and Tolterodine on Spina Bifida Patients: A Pilot Crossover Study Akihiro KANEMATSU, 1,2 Kazuyoshi JOHNIN, 2,3 Koji YOSHIMURA,
LUTS (2011) 3, 99 103 ORIGINAL ARTICLE Comparison of the Effects by Obybutynin and Tolterodine on Spina Bifida Patients: A Pilot Crossover Study Akihiro KANEMATSU, 1,2 Kazuyoshi JOHNIN, 2,3 Koji YOSHIMURA,
Bladder Dysfunction in Multiple Sclerosis. by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN
 Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies. Dr. Boris Friedman May 2, 2012 OBJECTIVES
 Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Clinical Policy: Urodynamic Testing Reference Number: CP.MP.98
 Clinical Policy: Reference Number: CP.MP.98 Effective Date: 10/15 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.98 Effective Date: 10/15 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Posterior Tibial Nerve Stimulation
 Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Slide 1. Slide 2. Slide 3. Bladder Management and Preventing CAUTI. Bladder management CAUTI prevention standards
 Slide 1 Bladder Management and Preventing CAUTI Diana Weinel, MS RN James A. Haley Veterans Hospital & Clinics Tampa, FL Florida State Association of Rehabilitation Nurses Conference May, 2018 Slide 2
Slide 1 Bladder Management and Preventing CAUTI Diana Weinel, MS RN James A. Haley Veterans Hospital & Clinics Tampa, FL Florida State Association of Rehabilitation Nurses Conference May, 2018 Slide 2
Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic Study
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
THE vesical dysfunction which follows injury or disease of the spinal cord
 VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured Population
 Paraplegia 27 (1989) 364-369 0031-1758/89/0027-0364$10.00 ([j 1989 International Medical Society of Paraplegia The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured
Paraplegia 27 (1989) 364-369 0031-1758/89/0027-0364$10.00 ([j 1989 International Medical Society of Paraplegia The Effect ofverapamil on the Treatment of Detrusor Hyperreflexia in the Spinal Cord Injured
Incontinence in neurological disease
 nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
Posterior Tibial Nerve Stimulation for Voiding Dysfunction
 Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Intermittent Catheterisation What do we need to know? Workshop
 Intermittent Catheterisation What do we need to know? Workshop Hanny Cobussen-Boekhorst, PhD, MANP, RN Continence and Urostomy care Radboud University Medical Center Department of Urology Nijmegen, The
Intermittent Catheterisation What do we need to know? Workshop Hanny Cobussen-Boekhorst, PhD, MANP, RN Continence and Urostomy care Radboud University Medical Center Department of Urology Nijmegen, The
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Spinal dysraphism and neurogenic bladder: Still a relevant topic
 The Journal of Medical Research 2017; 3(5): 234-238 Research Article JMR 2017; 3(5): 234-238 September- October ISSN: 2395-7565 2017, All rights reserved www.medicinearticle.com Received: 28-09-2017 Accepted:
The Journal of Medical Research 2017; 3(5): 234-238 Research Article JMR 2017; 3(5): 234-238 September- October ISSN: 2395-7565 2017, All rights reserved www.medicinearticle.com Received: 28-09-2017 Accepted:
University of Alberta Reconstructive Urology Fellowship
 University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
LOYOLA UNIVERSITY MEDICAL CENTER MAYWOOD, ILLINOIS. Department of Urology INFORMED CONSENT. Patient s Name: Medical Record Number:
 1 IRB NUMBER: 107592072104 LOYOLA UNIVERSITY MEDICAL CENTER MAYWOOD, ILLINOIS Department of Urology INFORMED CONSENT Patient s Name: Medical Record Number: Project Title: A Multi-Center, Open-Label, Active-Controlled,
1 IRB NUMBER: 107592072104 LOYOLA UNIVERSITY MEDICAL CENTER MAYWOOD, ILLINOIS Department of Urology INFORMED CONSENT Patient s Name: Medical Record Number: Project Title: A Multi-Center, Open-Label, Active-Controlled,
Multiple Sclerosis. Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
 Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction?
 London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
Physiologic Anatomy and Nervous Connections of the Bladder
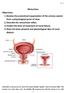 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
Re-evaluation of differential sacral rhizotomy for neurological bladder disease
 J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in children
 ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
Philadelphia College of Osteopathic Medicine. Victoria J. Kopec Philadelphia College of Osteopathic Medicine,
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
Geriatric Urinary Incontinence
 Geriatric Urinary Incontinence Neil M. Resnick, MD Thomas Detre Professor of Medicine Chief, Division of Geriatric Medicine University of Pittsburgh/UPMC UI: The Problem Prevalence in elderly 33% Morbidity
Geriatric Urinary Incontinence Neil M. Resnick, MD Thomas Detre Professor of Medicine Chief, Division of Geriatric Medicine University of Pittsburgh/UPMC UI: The Problem Prevalence in elderly 33% Morbidity
How to manage a patient with bladder dysfunction
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
