Management of benign vulval dermatoses in primary care
|
|
|
- Ferdinand Robbins
- 5 years ago
- Views:
Transcription
1 PRESCRIBING IN PRACTICE Management of benign vulval dermatoses in primary care MITESH PATEL AND DAVID NUNNS SPL Vulval dermatoses can be difficult to manage in primary care, and GPs need to be aware of the risk of malignancy. This article describes the most common types of benign vulval dermatoses encountered in primary care and their management, and discusses when referral to secondary care is required. Figure 1. Allergic contact dermatitis of the vulva T he management of vulval dermatoses can be difficult for the GP, as many patients have complex needs and clinical signs may be subtle.1 This article discusses the common benign, pruritic skin conditions affecting the vulva in adults (see Table 1). In this review, we focus on the pharmacological and non-pharmacological treatment of these dermatoses in primary care and explain when patients should be referred to secondary care (see Figure 2).2 Vulval dermatitis Vulval dermatitis is an inflammatory skin condition with a reported incidence of up 18 Prescriber May 2018 to 30% in vulval clinics.3 The main symptoms are vulval soreness and pruritus.4 Vulval dermatitis can be classified into eczematous or contact subtypes (see below), but the signs are similar. On examination, there is often symmetrically inflamed, erythematous, weepy skin with satellite lesions and poorly-defined edges. Lichenification may be present if the condition is long term. Secondary candidiasis is not uncommon, so a swab to exclude infection is suggested. Eczematous subtype more commonly seen in patients with a history of atopy, although sweat, warmth and rubbing are non-atopic-related triggers.1 prescriber.co.uk
2 Vulval dermatoses l PRESCRIBING IN PRACTICE Vulval dermatitis atopic eczema and contact dermatitis Vulval psoriasis Vulval lichen planus Vulval lichen sclerosus Vulval lichen simplex Table 1. Common benign vulval dermatoses Contact dermatitis arises secondary to an allergen or irritant. Allergic contact dermatitis (see Figure 1) is a delayed response following prior sensitisation, commonly to antifungals, nickel, topical antibiotics or preservatives in products. 5 Allergic contact dermatitis is diagnosed by patch testing. Irritant dermatitis occurs minutes to hours after contact with triggers including urine, hygienic products, douches and lubricants, 5 but should also be considered in patients with incontinence or a significant hygiene habit, eg overwashing. 1 A general approach is to restore the skin barrier, provide symptom relief, treat co-existing infection (see Table 2) 1 and reduce inflammation with steroids. Importantly, patients must avoid any allergens or irritants. A moderate topical steroid can be applied once daily (see Box 1), 2 or a potent topical steroid if the condition is more severe, for 7 10 days until the symptoms resolve. 6 The patient s serum ferritin should be checked, as iron-deficiency anaemia is found in 20% of cases. 3 In treatment-resistant dermatitis or if atypical characteristics or lesions emerge, then a referral to secondary care is required. 7 Consider a two-week wait referral for patients with suspected vulval cancer. The most common symptom of vulval cancer is chronic pruritus or pain. The most common sign is a vulvar mass or lump, which can be ulcerated or warty in appearance. 8 Vulval psoriasis Vulval psoriasis affects 5% of women with vulvar symptoms, 9 presenting with pruritus and a burning sensation, made worse by friction and irritants. Classically in psoriasis, well demarcated, scaly erythematous plaques are seen, but vulval psoriatic plaques are smooth, glossy and often salmon pink in colour. Often no scale in vulval creases are seen but surrounding skin may have the typical scaly lesions of psoriasis. There is no scarring or loss of anatomy 1 (see Figure 3). Encourage general vulval care (see Table 2), but most patients require referral to secondary care for management. 2 For acute care or when there is a delay in referral, a moderate topical steroid can be used, or a potent steroid in severe cases (see Box 1). As the skin folds can become particularly macerated, there is a chance of secondary bacterial or fungal infection. A combination topical preparation (eg clobetasone butyrate 0.05%/ oxytetracycline 3%/nystatin cream) may be helpful. 10 Most patients should to be managed in secondary care or referred if the diagnosis is uncertain. The disease is often Vulval itch Vaginal discharge or weeping of skin Suspicious features (consider cancer/vin*) Take biopsy Swab and treat Is there candidiasis? Normal architecture? Eczema/psoriasis Vulval care regimen; moderate potency topical steroid yes no Lichen sclerosis/ lichen planus Vulval care regimen; treat if confident with very potent topical steroid If inadequate response Refer for diagnosis, ongoing investigation and treatment if not confident (if cancer suspected, refer via appropriate pathway) *VIN = vulval intraepithelial neoplasia, a precancerous skin condition (not discussed in this article) Figure 2. Management of vulval pruritus in primary care and when to refer to secondary care prescriber.co.uk Prescriber May
3 PRESCRIBING IN PRACTICE l Vulval dermatoses Provide written information on the diagnosis and treatment of vulval conditions - See the British Society for the Study of Vulval Disease website for more information (bssvd.org) Re-stablish the skin barrier: - Wash the vulva with water and use fingertips only - Do not rub or scrub the genital skin while bathing and gently pat the skin dry - Avoid soaps, shampoos, bubble bath and scented wipes. Instead, use a soap substitute such as Hydromol ointment or aqueous cream (the latter needs to be washed off) - Avoid using sponges and flannels to clean the vulva - Wear light-coloured cotton or loose-fitting silk underwear - Avoid wearing sanitary pads or panty liners frequently - Avoid using nail varnish and cut nails if you scratch the skin Symptom control: - Educate the patient on the itch-scratch cycle - Gel packs or cooled washcloths can reduce symptoms - If symptoms are worse at night, use a tricyclic antidepressant such as amitriptyline starting at 5 10mg or doxepin starting at 25mg and increase based on response, rather than using a sedating antihistamine Treat co-existing infection: - Take appropriate swabs if an infection is suspected - Treat weepy, discharging skin that may indicate secondary bacterial infection with antibiotics such as flucloxacillin - Candidiasis can occur with any dermatoses, especially when using topical steroids and if present, treat with an oral antifungal such as fluconazole twice daily - Think about co-existing herpes simplex virus infection, which may need oral antiviral treatment Table 2. General vulval care chronic so there is a role for primary care in long-term management. Vulval lichen simplex chronicus Vulval lichen simplex chronicus is a chronic inflammatory dermatosis, with the key symptom of severe pruritus leading to vulval pain through skin fissuring (via the itch/scratch cycle). 11 Pruritus can be triggered as a result of dermatitis, an irritant or secondary to a systemic or psychological disorder. 12 A localised eczematous patch can be observed, which can become lichenified with erosions and might be more marked on the side of the vulva opposite the dominant hand. Skin excoriation and pubic hair loss can be seen. Usually, no loss of anatomy is seen but it can result in thick leathery skin. General vulval care should be encouraged (see Table 2). Treatment with a very potent topical steroid and an emollient is suggested. Once control of symptoms is achieved, a moderate potency topical steroid may be required intermittently. 7 The patient should be referred to secondary care if the diagnosis is indeterminate, where a biopsy may be required. For coinciding psychiatric symptoms, a referral for psychological therapy may provide benefit. 11 Vulval lichen sclerosus Lichen sclerosus is a chronic inflammatory condition, with an autoimmune link 13 and an approximate prevalence of 3% in older patients. 14 Key symptoms are pruritus, soreness and dyspareunia. 12 Typically, pearly white papules are observed in a figure-of-eight pattern around the vulva, perineal body and perianal skin, and purpura can be seen. This can progress to erosions, hyperkeratosis, ulcers and fissures after prolonged scratching 13 (see Figure 3. Vulval psoriasis showing ill-defined erythema and a lack of scale Figure 4). There may be fusion of the clitoral hood from scarring, resulting in sexual dysfunction. 15 It is important to note that the risk of development to squamous cell carcinoma (SCC) is up to 5%. 16 All patients need to be notified of the risk of squamous cell carcinoma, and ideally self-examine once a month and present for immediate review if any changes arise. If any clinical findings are indicative, an autoimmune thyroid and pernicious anaemia screen are suggested. 7 A very potent topical steroid (such as clobetasol propionate 0.05% ointment) daily for one month (see Box 1), then on alternate days for one month and finally twice a week for a month is suggested. 17 The minimum topical steroid required to maintain remission should be used as maintenance, with 30 60g topical ster- Figure 4. Vulval lichen sclerosus with fusion of the clitoral hood 20 Prescriber May 2018 prescriber.co.uk
4 Vulval dermatoses l PRESCRIBING IN PRACTICE The mucosal skin of the vulva is somewhat resistant to steroids and therefore very potent steroids can be used for a longer duration. 1 However, hair-bearing areas of the vulva are prone to atrophy and require close monitoring. Topical steroids are safe to use in pregnancy and breastfeeding. 9 Topical steroids should be used once daily and an ointment is preferred to reduce irritation. Review all patients using a potent steroid after one month. 7 The amount of topical steroid required for treatment is measured in fingertip units (FTU), measured from the first crease of the finger to the very tip. 2 The number of FTUs required is usually one to two but is specifically tailored to the patient depending upon surface area affected by the condition. Examples of topical steroids and their potency Moderate potency: Clobetasone butyrate 0.05%, betamethasone valerate 0.025% Potent: Mometasone furoate 0.1%, betamethasone valerate 0.1%, betamethasone dipropionate 0.05% Very potent: Clobetasol propionate 0.05%, diflucortolone valerate 0.3% Box 1. Topical steroid options for vulval dermatoses oid normally needed per year for maintenance treatment. 18 In one study, 23% of patients using very potent steroids experienced a reversion to normal skin and 96% found an improvement in their symptoms. 19 The importance of maintenance treatment has been demonstrated in a study showing that no compliant patients developed SCC, compared with 4.7% of partially compliant patients. 20 Patients need to be reviewed after three and nine months and then annually if their condition is stable and uncomplicated. 7 If the diagnosis is indeterminate, a lesion is observed or there is a worry about vulval intraepithelial neoplasia or malignancy, then a biopsy is required. This referral may be urgent or via a two-week wait pathway, depending on the findings. At each review, if any pseudocyst of the clitoris is observed, if the patient has dysaesthesia or psychosexual prob-
5 PRESCRIBING IN PRACTICE l Vulval dermatoses Figure 5. Erosive vulval lichen planus with vestibular erosions lems, or if there are scarring issues, then a referral is indicated. At the annual review, if the patient remains symptomatic despite treatment, is using a very potent steroid greater than three times a week or greater than 30g in six months, or suspect lesions are observed, then they should be referred. 21 Patients also require referral if systemic or other topical treatments are indicated, with trials showing positive effects with oral retinoids 22 and topical calcineurin inhibitors. 23 However oral retinoids are highly teratogenic and therefore pregnancy must be avoided for two years after finishing treatment. 10 Topical calcineurin inhibitors are not licenced for vulval lichen sclerosus, can cause irritation, and have been linked to malignancy. 10 Intralesional steroids can be used for thick plaques. 24 Vulval lichen planus Vulval lichen planus is a chronic inflammatory, autoimmune dermatosis, commonly seen in the fifth and sixth decade KEY POINTS sof life. 25 Patients may have coinciding oral lichen planus in a syndrome called vulvovaginal gingival syndrome. 26 The key symptoms include dyspareunia, pruritus, pain and vaginal discharge. The main feature distinguishing lichen planus from lichen sclerosus is the involvement of the vagina in a third of cases of lichen planus. 16 The risk of development to SCC is approximately 3%. 25 Vulval lichen planus can be classified into two subtypes: Erosive The most common subtype with pain as the main symptom. Wickham striae may be seen at the edges of vestibular erosions 27 (see Figure 5). The vestibular erosions are strikingly obvious when the inner labia are parted. There is an overlap with vulval lichen sclerosus. Classical Violaceous papules are observed in the anogenital region alongside lacy, reticular white Wickham striae, resulting in itch as the main symptom. 28 All patients need to be notified of the small risk of squamous cell carcinoma, and ideally self-examine frequently and present for immediate review if any changes arise. An autoimmune thyroid screen has been suggested. 29 No gold-standard treatment routine is known; however, a very potent topical steroid (see Box 1), parallel to the management of lichen sclerosus, is favoured. 21 Very potent steroids have been shown to improve symptoms in 75% of cases. 25 Delivery of topical steroids into the vagina can be difficult and preparations with an applicator such as prednisolone suppositories can be used. 10 Stable disease should be reviewed annually. Most patient should have an initial Inform all patients of general vulval care (see Table 2), including maintaining a protective skin barrier with emollients and treating secondary infection, and provide written information In treatment-resistant dermatoses, if the diagnosis is unclear, new lesions appear or if there are any concerns about malignancy then refer the patient to secondary care For lichen sclerosus and lichen planus, a three-month reducing regimen of a very potent topical steroid can be used prior to review if confident about clinical assessment and prescribing review by a vulval clinic team and a management plan should be arranged. If the diagnosis is unclear, a lesion is observed or there is a worry about vulval intraepithelial neoplasia or malignancy, then referral for a biopsy is required. This referral may be urgent or via a twoweek wait pathway, depending on the findings. Patients with erosive disease need referral as they require long-term follow-up. Referral is also required if systemic treatments are needed, including oral prednisolone or retinoids, 7 or immunosuppressants such as methotrexate or azathioprine. 30 Summary A variety of benign vulval diseases can present to the primary care physician that are sometimes difficult to diagnose and often require careful management. All patients should be encouraged to undertake general vulval care. If a qualified healthcare professional is confident in prescribing, then potent or very potent steroids can be offered to the patient to be used on the vulva and applied once a day but cases must be reviewed after a month. If the diagnosis is not known, in treatment resistant cases or if there is concern about malignancy, then always refer to secondary care for assessment. Acknowledgements We would like to thank DermNet New Zealand for their permission to use their Figures 3 and 5 in this article (licence available from No changes were made to the original images. We also thank the patient for consent to use Figure 4 in this article. References 1. Stewart MAS. Vulvar dermatoses: a practical approach to evaluation and management. JCOM 2005;19(5): Simpson R, Nunns D. Skin diseases affecting the vulva. Obstet Gynaecol Reprod Med 2017;27(3): Crone AM, et al. Aetiological factors in vulvar dermatitis. J Eur Acad Dermatol Venereol 2000;14(3): Connor CJ, Eppsteiner EE. Vulvar contact dermatitis. Proc Obstet Gynecol 2014;4(2): Prescriber May 2018 prescriber.co.uk
6 Vulval dermatoses l PRESCRIBING IN PRACTICE 5. Bauer A, et al. Vulvar dermatoses irritant and allergic contact dermatitis of the vulva. Dermatology 2005;210(2): van der Meijden WI, et al European guideline for the management of vulval conditions. J Eur Acad Dermatol Venereol 2017;31;6: Edwards SK, et al, BASHH UK national guideline on the management of vulval conditions. Int J STD AIDS 2015;26(9): Hunter DJ. Carcinoma of the vulva: a review of 361 patients.gynecol Oncol 1975; 3(2): Selim MA, Hoang MP. A Histologic review of vulva inflammatory dermatoses and intraepithelial neoplasm. Dermatol Clin 2010;28: Royal College of Obstetricians and Gynaecologists. Vulval skin disorders, management. Green-top Guideline No. 58. February Lynch PJ. Lichen simplex chronicus (atopic/neurodermatitis) of the anogenital region. Dermatol Ther 2004;17(1): Moyal-Barracco M, Wendling J. Vulvar dermatosis. Best Pract Res Clin Obstet Gynaecol 2014;28(7): Fistarol SK, Itin PH. Diagnosis and treatment of lichen sclerosus: an update. Am J Clin Dermatol 2013;14(1): Leibovitz A, et al. Vulvovaginal examinations in elderly nursing home women residents. Arch Gerontol Geriatr 2000;31(1): McPherson T, Cooper S. Vulval lichen sclerosus and lichen planus. Dermatol Ther 2010;23(5): Wallace HJ. Lichen sclosus et atrophicus. Trans St John s Hosp Dermatol Soc 1971;57(1): Schlosser BJ, Mirowski GW. Approach to the patient with vulvovaginal complaints. Dermatol Ther 2010;23(5): Simpson RC, et al. Real-life experience of managing vulval erosive lichen planus: a case-based review and UK multicentre case note audit. Br J Dermatol 2012;167(1): Cooper SM, et al. Does treatment of vulvar lichen sclerosus influence its prognosis? Arch Dermatol 2004;140: Lee A, et al. Long-term management of adult vulvar lichen sclerosus: A prospective cohort study of 507 women. JAMA Dermatol 2015;151(10): Nunns D. Guideline for the assessment, referral and initial management of adult vulval lichen sclerosus Available from: doc=docm93jijm4n895.pdf&ver= Nissi R, et al. Pimecrolimus cream 1% in the treatment of lichen sclerosus. Gynecol Obstet Invest 2007;63(3): Bousema MT, et al. Acitretin in the treatment of severe lichen sclerosus et atrophicus of the vulva: a double-blind, placebo controlled study. J Am Acad Dermatol 1994;30(2): Mazdisnian F, et al. Intralesional injection of triamcinolone in the treatment of lichen sclerosus. J Reprod Med 1999;44(4): Cooper SM, Wojnarowska F. Influence of treatment of erosive lichen planus of the vulva on its prognosis. Arch Dermatol 2006;142(3): Pelisse M, et al. A new vulvovaginogingival syndrome. Plurimucous erosive lichen planus. Ann Dermatol Venereol 1982;109(9): Lewis FM. Vulval lichen planus. Br J Dermatol 1998;138(4): Guerrero A, Venkatesan A. Inflammatory vulvar dermatoses. Clin Obstet Gynecol 2015;58(3): Meyrick-Thomas RH, et al. Lichen sclerosus and autoimmunity a study of 350 women. Br J Dermatol 1988;118(1): Guerrero A, Venkatesan A. Inflammatory vulvar dermatoses. Clin Obstet Gynecol 2015;58(3): Declaration of interests None to declare. Mitesh Patel is an ST3 Academic Clinical Fellow, Division of Primary Care, Nottingham and David Nunns is a Consultant Gynaecological Oncologist, Nottingham City Hospital, Nottingham prescriber.co.uk Prescriber May
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Access from the University of Nottingham repository:
 Simpson, Rosalind C. and Nunns, David (2017) Skin diseases affecting the vulva. Obstetrics, Gynaecology and Reproductive Medicine, 27 (3). pp. 77-85. ISSN 1879-3622 Access from the University of Nottingham
Simpson, Rosalind C. and Nunns, David (2017) Skin diseases affecting the vulva. Obstetrics, Gynaecology and Reproductive Medicine, 27 (3). pp. 77-85. ISSN 1879-3622 Access from the University of Nottingham
What are the symptoms of a vulval skin condition?
 Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Disorders of the vulva
 Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Kelly H. Tyler, MD, FACOG, FAAD S052 Gender Dermatology: Diagnosis and Treatment of Genital Skin Disorders Vulvar Dermatitis
 Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Lichen sclerosus. Lichen planus
 Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Conflicts of interest
 Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Disclosures Dr. Lynette Margesson
 Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
sclerosus, lichen simplex, or threadworm infestation (particularly if combined with peri-anal itch).
 Pruritus vulvae - Management View full scenario How should I assess a woman with pruritus vulvae? There is an identifiable cause for pruritus vulvae in most women. Confirm that the woman is experiencing
Pruritus vulvae - Management View full scenario How should I assess a woman with pruritus vulvae? There is an identifiable cause for pruritus vulvae in most women. Confirm that the woman is experiencing
4/3/2017 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS BACTERIAL VAGINOSIS EPIDEMIOLOGY OBJECTIVES
 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
OCCG SERVICE SPECIFICATION (2017/18)
 OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera?
 DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
Eczema & Dermatitis Clinical features: Histopathological features: Classification:
 Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Diagnosis and Management of Vulvar Disorders
 Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
Vaginal involvement in genital erosive lichen planus
 Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
MALE GENITAL (PENIS) LICHEN SCLEROSUS
 MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
Lichen planus. Information for patients Gynaecology
 Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
WHITE PAPER SmartXide 2 V 2 LR. MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy
 WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
Vulvodynia and vestibulectomy
 Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
The use of CO2 laser for patients with Lichen sclerosus
 The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
Lichen sclerosus. Information for patients Gynaecology
 Lichen sclerosus Information for patients Gynaecology page 2 of 8 What is lichen sclerosus? Lichen sclerosus is a skin condition that most often affects the vulva (the outer folds of skin around your vagina).
Lichen sclerosus Information for patients Gynaecology page 2 of 8 What is lichen sclerosus? Lichen sclerosus is a skin condition that most often affects the vulva (the outer folds of skin around your vagina).
Asymptomatic Undiagnosed Lichen Sclerosus
 Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Children s Hospital Of Wisconsin
 Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
15 minute eczema consultation
 THERAPY WORKSHOP 15 minute eczema consultation History Current treatments Examination Treatment Plan Written action plan Soap substitute/bath oil Antiseptic baths Emollients Topical steroids Other treatments
THERAPY WORKSHOP 15 minute eczema consultation History Current treatments Examination Treatment Plan Written action plan Soap substitute/bath oil Antiseptic baths Emollients Topical steroids Other treatments
CANDIDIASIS (WOMEN) Single Episode. Clinical Features. Diagnosis. Management
 CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! **
 ** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Cholestatic jaundice Chronic kidney disease Iron deficiency +/-anaemia. Hepatoma Diabetes Leukaemia
 Pruritis Introduction Pruritis can cause discomfort, frustration, poor sleep, anxiety and depression. Itch may be localised or due to systemic disease. Pruritis in systemic disease is often worse at night.
Pruritis Introduction Pruritis can cause discomfort, frustration, poor sleep, anxiety and depression. Itch may be localised or due to systemic disease. Pruritis in systemic disease is often worse at night.
VIN/VAIN O C T O B E R 3 RD J M O R G A N
 VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
Review Article Vulvar Skin Disorders throughout Lifetime: About Some Representative Dermatoses
 Hindawi Publishing Corporation BioMed Research International Volume 2014, Article ID 595286, 6 pages http://dx.doi.org/10.1155/2014/595286 Review Article Vulvar Skin Disorders throughout Lifetime: About
Hindawi Publishing Corporation BioMed Research International Volume 2014, Article ID 595286, 6 pages http://dx.doi.org/10.1155/2014/595286 Review Article Vulvar Skin Disorders throughout Lifetime: About
Recommended management of eczema in older patients
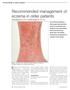 Recommended management of eczema in older patients Victoria Sherman MA, MRCP and Daniel Creamer BSc, MD, FRCP Our series Prescribing in older people gives practical advice for successful management of
Recommended management of eczema in older patients Victoria Sherman MA, MRCP and Daniel Creamer BSc, MD, FRCP Our series Prescribing in older people gives practical advice for successful management of
STUDY. Influence of Treatment of Erosive Lichen Planus of the Vulva on Its Prognosis
 STUDY Influence of Treatment of Erosive Lichen Planus of the Vulva on Its Prognosis Susan M. Cooper, MRCP; Fenella Wojnarowska, DM, FRCP Objective: To record the clinical features, symptomatic response
STUDY Influence of Treatment of Erosive Lichen Planus of the Vulva on Its Prognosis Susan M. Cooper, MRCP; Fenella Wojnarowska, DM, FRCP Objective: To record the clinical features, symptomatic response
Atopic Eczema with detail on how to apply wet wraps
 Atopic Eczema with detail on how to apply wet wraps Dr Carol Hlela Consultant Dermatologist Head of Unit, Department of Dermatology, Paediatrics Red Cross Children s Hospital, UCT Red Cross War Memorial
Atopic Eczema with detail on how to apply wet wraps Dr Carol Hlela Consultant Dermatologist Head of Unit, Department of Dermatology, Paediatrics Red Cross Children s Hospital, UCT Red Cross War Memorial
Common Superficial Fungal Infections
 How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
Vulvodynia. Information for patients Gynaecology
 Vulvodynia Information for patients Gynaecology page 2 of 8 What is vulvodynia? Vulvodynia is a chronic (long term) condition of vulval pain. It is the term used to describe women who experience the sensation
Vulvodynia Information for patients Gynaecology page 2 of 8 What is vulvodynia? Vulvodynia is a chronic (long term) condition of vulval pain. It is the term used to describe women who experience the sensation
Anne Arundel Medical Center Informed Consent
 Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
Conflicts of interest. Genital Lichen Planus. Objectives. Lichen Planus. Genital Lichen Planus. Author Up To Date. Vulvar Lichen Planus Patterns
 Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Vulval intraepithelial neoplasia. Information for patients Gynaecology
 Vulval intraepithelial neoplasia Information for patients Gynaecology page 2 of 8 What is vulval intraepithelial neoplasia? Vulval intraepithelial neoplasia (VIN) is not cancer. VIN is a disease of the
Vulval intraepithelial neoplasia Information for patients Gynaecology page 2 of 8 What is vulval intraepithelial neoplasia? Vulval intraepithelial neoplasia (VIN) is not cancer. VIN is a disease of the
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level
 Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Case 1. Case Studies in Vulvovaginal Disease. Disclosures. What is your diagnosis? Case 1. Lichen sclerosus 10/19/2018
 Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Summary. Accepted for publication 18 May Key words genital lichen planus, oral lichen planus, vulval lichen planus
 CLINICAL AND LABORATORY INVESTIGATIONS DOI 10.1111/j.1365-2133.2006.07480.x Prevalence of vulval lichen planus in a cohort of women with oral lichen planus: an interdisciplinary study P. Belfiore, O. Di
CLINICAL AND LABORATORY INVESTIGATIONS DOI 10.1111/j.1365-2133.2006.07480.x Prevalence of vulval lichen planus in a cohort of women with oral lichen planus: an interdisciplinary study P. Belfiore, O. Di
Vulvodynia What a Health Practitioner Should Know
 Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
The Normal Vulva: Overview of Basic Dermatology Treatment
 The Normal Vulva: Overview of Basic Dermatology Treatment 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor
The Normal Vulva: Overview of Basic Dermatology Treatment 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor
Professor Rohan Ameratunga Clinical Immunologist and Allergist Auckland
 Professor Rohan Ameratunga Clinical Immunologist and Allergist Auckland 16:30-17:25 WS #170: Eczema Management 17:35-18:30 WS #182: Eczema Management (Repeated) Managing ECZEMA A/Prof Rohan Ameratunga
Professor Rohan Ameratunga Clinical Immunologist and Allergist Auckland 16:30-17:25 WS #170: Eczema Management 17:35-18:30 WS #182: Eczema Management (Repeated) Managing ECZEMA A/Prof Rohan Ameratunga
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
GROUP 15 TOPICAL PREPARATIONS
 - 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
- 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
PACKAGE LEAFLET: INFORMATION FOR THE USER. Flutarzole 0,05% w/w cream, Fluticasone propionate
 PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Clinically Microscopically Pathogenesis: autoimmune not lifetime
 Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
An All Too Familiar Story
 All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
My Algorithm. Questions to ask. Do you or your family have a history of?... Allergic rhinitis, Sensitive skin, Asthma Skin Cancer
 Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
ATOPIC ECZEMA. What are the aims of this leaflet?
 ATOPIC ECZEMA What are the aims of this leaflet? This leaflet has been written to help you understand more about atopic eczema. It tells you what it is, what causes it, what can be done about it, and where
ATOPIC ECZEMA What are the aims of this leaflet? This leaflet has been written to help you understand more about atopic eczema. It tells you what it is, what causes it, what can be done about it, and where
New Medicine Report. Pimecrolimus. RED- Hospital only Date of Last Revision 6 th March 2003
 New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
Topics in Women s Health. Ann Laros, MD University of Iowa
 Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
Vulvovaginal Complaints
 Curr Treat Options Peds (2016) 2:209 215 DOI 10.1007/s40746-016-0062-8 Pediatric Gynecology (L Breech and K Stambough, Section Editors) Vulvovaginal Complaints Chelsea Bayer, MD Laura Parks, MD * Address
Curr Treat Options Peds (2016) 2:209 215 DOI 10.1007/s40746-016-0062-8 Pediatric Gynecology (L Breech and K Stambough, Section Editors) Vulvovaginal Complaints Chelsea Bayer, MD Laura Parks, MD * Address
Pharmacologic Treatment of Atopic Dermatitis
 J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
Medication Policy Manual. Topic: Dupixent, dupilumab Date of Origin: March 10, Committee Approval: March 10, 2017 Next Review Date: May 2018
 Independent licensees of the Blue Cross and Blue Shield Association Medication Policy Manual Policy No: dru493 Topic: Dupixent, dupilumab Date of Origin: March 10, 2017 Committee Approval: March 10, 2017
Independent licensees of the Blue Cross and Blue Shield Association Medication Policy Manual Policy No: dru493 Topic: Dupixent, dupilumab Date of Origin: March 10, 2017 Committee Approval: March 10, 2017
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California.
 Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
The Genital Skin During Menopause in Health and Disease
 The Genital Skin During Menopause in Health and Disease 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of
The Genital Skin During Menopause in Health and Disease 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of
Topical Doxepin Prior Authorization with Quantity Limit Program Summary
 Topical Doxepin Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1-3 Agent(s) Indication(s) Dosage & Administration Doxepin 5% cream Prudoxin (doxepin) cream 5% KS_PS_Topical_Doxepin_PAQL_ProgSum_AR1018
Topical Doxepin Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1-3 Agent(s) Indication(s) Dosage & Administration Doxepin 5% cream Prudoxin (doxepin) cream 5% KS_PS_Topical_Doxepin_PAQL_ProgSum_AR1018
Vulvar Disease Clinical Cases
 Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation
 Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
The Itch That Rashes. Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah
 The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
Vulval disease in children
 Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Dermatitis (inflammatory skin condition) Nonallergic. dermatitis. Non-atopic eczema (non- IgE mediated)
 Atopic Eczema Dermatitis (inflammatory skin condition) Allergic dermatitis -eczema Nonallergic dermatitis Atopic eczema (IgE mediated) Non-atopic eczema (non- IgE mediated) Pathophysiology of Eczema Allergy
Atopic Eczema Dermatitis (inflammatory skin condition) Allergic dermatitis -eczema Nonallergic dermatitis Atopic eczema (IgE mediated) Non-atopic eczema (non- IgE mediated) Pathophysiology of Eczema Allergy
Dr Emmy Babor GPSI Dermatology
 Dr Emmy Babor GPSI Dermatology Wrinkles Sagging Thin skin (not all areas think about soles of feet) Loss of elasticity Pigmentary changes Dryness Loss of luminosity Baldness/ grey hair Increased nose
Dr Emmy Babor GPSI Dermatology Wrinkles Sagging Thin skin (not all areas think about soles of feet) Loss of elasticity Pigmentary changes Dryness Loss of luminosity Baldness/ grey hair Increased nose
Non-Venereal Female Genital Dermatoses A Clinical Study
 JMSCR Volume 2 Issue 11 Page 2864-2873 November-2014 2864-2902 November-2014 2014 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x ABSTRACT Non-Venereal Female Genital Dermatoses A Clinical
JMSCR Volume 2 Issue 11 Page 2864-2873 November-2014 2864-2902 November-2014 2014 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x ABSTRACT Non-Venereal Female Genital Dermatoses A Clinical
過敏病科中心. Allergy Centre. Eczema. Allergy Centre 過敏病科中心. Allergy Centre. For enquiries and appointments, please contact us at:
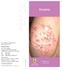 Allergy Centre 過敏病科中心 Eczema For enquiries and appointments, please contact us at: Allergy Centre 9/F, Li Shu Pui Block Hong Kong Sanatorium & Hospital 2 Village Road, Happy Valley, Hong Kong Tel: 2835
Allergy Centre 過敏病科中心 Eczema For enquiries and appointments, please contact us at: Allergy Centre 9/F, Li Shu Pui Block Hong Kong Sanatorium & Hospital 2 Village Road, Happy Valley, Hong Kong Tel: 2835
TCIs are only available on prescription and are usually started by a dermatology specialist.
 (TCIs) What are topical calcineurin inhibitors? Topical calcineurin inhibitors are treatments that alter the immune system and have been developed for controlling eczema. There are two types available:
(TCIs) What are topical calcineurin inhibitors? Topical calcineurin inhibitors are treatments that alter the immune system and have been developed for controlling eczema. There are two types available:
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
Vision Health: Conditions, Disorders & Treatments EYELID DISORDERS
 Vision Health: Conditions, Disorders & Treatments EYELID DISORDERS There are a number of disorders that can affect the eyelid. Entropion Entropion is an inward turning of the eyelid and lashes toward the
Vision Health: Conditions, Disorders & Treatments EYELID DISORDERS There are a number of disorders that can affect the eyelid. Entropion Entropion is an inward turning of the eyelid and lashes toward the
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Patient Satisfaction of Surgical Treatment of Clitoral Phimosis and Labial Adhesions Caused by Lichen Sclerosus
 ORIGINAL RESEARCH WOMEN S SEXUAL HEALTH Patient Satisfaction of Surgical Treatment of Clitoral Phimosis and Labial Adhesions Caused by Lichen Sclerosus Anne N. Flynn, MD,* Michelle King, MSc, Mollie Rieff,
ORIGINAL RESEARCH WOMEN S SEXUAL HEALTH Patient Satisfaction of Surgical Treatment of Clitoral Phimosis and Labial Adhesions Caused by Lichen Sclerosus Anne N. Flynn, MD,* Michelle King, MSc, Mollie Rieff,
Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream DO NOT DUPLICATE
 The Journal of Reproductive Medicine Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream Claudia Marchitelli, M.D., Graciela Secco, M.D., Myriam Perrotta, M.D.,
The Journal of Reproductive Medicine Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream Claudia Marchitelli, M.D., Graciela Secco, M.D., Myriam Perrotta, M.D.,
PRESCRIBING INFORMATION. Cream 0.025% Topical Corticosteroid
 PRESCRIBING INFORMATION Pr PROPADERM (beclomethasone dipropionate) Cream 0.025% Topical Corticosteroid Valeant Canada LP 2150 St-Elzear Blvd. West, Laval, Quebec, Canada H7L 4A8 Date of preparation: October
PRESCRIBING INFORMATION Pr PROPADERM (beclomethasone dipropionate) Cream 0.025% Topical Corticosteroid Valeant Canada LP 2150 St-Elzear Blvd. West, Laval, Quebec, Canada H7L 4A8 Date of preparation: October
What is atopic dermatitis?
 What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Dr Lilianne Scholtz (MBBCh)
 Dr Lilianne Scholtz (MBBCh) I have a discharge. It s itchy and it burns. My urine burns too. Diagnosis based on symptoms alone is accurate in ~34 % of women because symptoms are very non-specific Sobel
Dr Lilianne Scholtz (MBBCh) I have a discharge. It s itchy and it burns. My urine burns too. Diagnosis based on symptoms alone is accurate in ~34 % of women because symptoms are very non-specific Sobel
Dermatology elective for yr. 5. Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015
 Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Core Module 13: Gynaecological Problems
 Core Module 13: Gynaecological Problems Learning outcomes: To understand and demonstrate appropriate knowledge, skills and attitudes in relation to common gynaecological disorders To understand paediatric
Core Module 13: Gynaecological Problems Learning outcomes: To understand and demonstrate appropriate knowledge, skills and attitudes in relation to common gynaecological disorders To understand paediatric
11/1/18. Age and Vulvar Pathology ANATOMY. Prepuce Clitoris Vestibule Hart line. Labia. minora. Labia. majora. Fourchette.
 Age and Vulvar Pathology Maria Angelica Selim, MD Professor of Pathology and Dermatology Director Dermatopathology Unit Duke University Medical Center Labia minora Labia majora Bartholin s duct Prepuce
Age and Vulvar Pathology Maria Angelica Selim, MD Professor of Pathology and Dermatology Director Dermatopathology Unit Duke University Medical Center Labia minora Labia majora Bartholin s duct Prepuce
What you need to know about ECZEMA
 What you need to know about ECZEMA The Irish Skin Foundation is a national charity with a mission to improve quality of life for people with skin conditions, promote skin health and the prevention of skin
What you need to know about ECZEMA The Irish Skin Foundation is a national charity with a mission to improve quality of life for people with skin conditions, promote skin health and the prevention of skin
British Association of Dermatologists Undergraduate Award Essay Prize Who should look after genital skin disease in the 21 st century?
 Who should look after genital skin disease in the 21 st century? Sethuparvathy Jayakumar, 4 th year medical student, King s College London GKT School of Medical Education Genital skin disease is a broad
Who should look after genital skin disease in the 21 st century? Sethuparvathy Jayakumar, 4 th year medical student, King s College London GKT School of Medical Education Genital skin disease is a broad
Gunasundari October 15, :57 PM 13:57 4 Color Fig(s):0 Art: GOX-D
 Original Article Reconstructive Use of Platelet-rich Plasma for Vulvovaginal Autoimmune Conditions Like Lichen Sclerosus AQ1 AQ2 Fariba Behnia-Willison, MBBS, MIS, FRANZCOG* Nina R. Pour, O&G SRMO-DRANZCOG
Original Article Reconstructive Use of Platelet-rich Plasma for Vulvovaginal Autoimmune Conditions Like Lichen Sclerosus AQ1 AQ2 Fariba Behnia-Willison, MBBS, MIS, FRANZCOG* Nina R. Pour, O&G SRMO-DRANZCOG
Advanced Training Skills Module August Vulval Disease
 Introduction Vulval Disease This module is designed to provide training in all aspects of vulval disease. Successful completion of the ATSM will equip an individual to develop this aspect of care in their
Introduction Vulval Disease This module is designed to provide training in all aspects of vulval disease. Successful completion of the ATSM will equip an individual to develop this aspect of care in their
Oral & Vulvovaginal GVHD. Rachel Kornik, MD Assistant Professor of Dermatology University of Wisconsin Hospital and Clinics
 Oral & Vulvovaginal GVHD Rachel Kornik, MD Assistant Professor of Dermatology University of Wisconsin Hospital and Clinics DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rachel Kornik, MD S001 Advanced Medical
Oral & Vulvovaginal GVHD Rachel Kornik, MD Assistant Professor of Dermatology University of Wisconsin Hospital and Clinics DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rachel Kornik, MD S001 Advanced Medical
What s Topical About Topicals?
 What s Topical About Topicals? Megha M. Tollefson, MD Associate Professor of Dermatology and Pediatrics July 29, 2017 2015 MFMER 3513105-1 Disclosures None 2015 MFMER 3513105-2 Outline Topical steroids
What s Topical About Topicals? Megha M. Tollefson, MD Associate Professor of Dermatology and Pediatrics July 29, 2017 2015 MFMER 3513105-1 Disclosures None 2015 MFMER 3513105-2 Outline Topical steroids
What you need to know about ECZEMA
 What you need to know about ECZEMA The Irish Skin Foundation is a national charity with a mission to improve quality of life for people with skin conditions, promote skin health and the prevention of skin
What you need to know about ECZEMA The Irish Skin Foundation is a national charity with a mission to improve quality of life for people with skin conditions, promote skin health and the prevention of skin
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions
 Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD)
 Diagnosis: ATOPIC DERMATITIS (AD) Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD) PATIENT ADVICE: Unfortunately, there is no cure for atopic dermatitis, so
Diagnosis: ATOPIC DERMATITIS (AD) Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD) PATIENT ADVICE: Unfortunately, there is no cure for atopic dermatitis, so
Allergic versus Contact
 Allergic versus Contact Dermatitis Julie Sterbank, DO Assistant Clinical Professor Allergy/Immunology MetroHealth Medical Center/Case Western Reserve University Disclosure I have no financial disclosures
Allergic versus Contact Dermatitis Julie Sterbank, DO Assistant Clinical Professor Allergy/Immunology MetroHealth Medical Center/Case Western Reserve University Disclosure I have no financial disclosures
Anal intraepithelial neoplasia. Information for patients Gynaecology
 Anal intraepithelial neoplasia Information for patients Gynaecology What is anal intraepithelial neoplasia? Anal intraepithelial neoplasia (AIN) is not cancer. AIN describes the presence of abnormal cells
Anal intraepithelial neoplasia Information for patients Gynaecology What is anal intraepithelial neoplasia? Anal intraepithelial neoplasia (AIN) is not cancer. AIN describes the presence of abnormal cells
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
Address: 1. What is your vulvar diagnosis (if known)? 2. What is the main symptom for which you are coming to the Vulvar Mucosal Specialty Clinic?
 Referring Physician Address: Phone: Fax: Requirements before your appointment: All records from previous physicians participating in your current condition must be received by the time of your appointment.
Referring Physician Address: Phone: Fax: Requirements before your appointment: All records from previous physicians participating in your current condition must be received by the time of your appointment.
Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial
 European Journal of General Practice. 2009; 15: 2933 ORIGINAL ARTICLE Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial ANTOINE L. M. LAGRO-JANSSEN
European Journal of General Practice. 2009; 15: 2933 ORIGINAL ARTICLE Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial ANTOINE L. M. LAGRO-JANSSEN
What is Psoriasis? Common Areas Affected. Type Who Does it Affect Characteristics
 What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
Cases of Non-Infectious Vulvovaginitis
 Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
LRI Children s Hospital
 Atopic Eczema Care LRI Children s Hospital Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: May 2017 Version: V 4 Revision due: May 2020 Written by: K.
Atopic Eczema Care LRI Children s Hospital Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: May 2017 Version: V 4 Revision due: May 2020 Written by: K.
