Differential benefits of amoxicillin-metronidazole in different phases of periodontal therapy Randomized controlled crossover clinical trial
|
|
|
- Gyles Stafford
- 5 years ago
- Views:
Transcription
1 Article Differential benefits of amoxicillin-metronidazole in different phases of periodontal therapy Randomized controlled crossover clinical trial MOMBELLI, Andrea, et al. Abstract Background: The specific advantage of administering systemic antibiotics during initial, nonsurgical therapy, or in the context of periodontal surgery is unclear. This study assessed the differential outcomes of periodontal therapy supplemented with amoxicillin-metronidazole during either the non-surgical or the surgical treatment phase. Methods: Single center, randomized placebo controlled crossover clinical trial with a one- year follow-up. Eighty participants with Aggregatibacter actinomycetemcomitans-associated moderate to advanced periodontitis were randomized into two treatment groups. A: Antibiotics (3/d 500 mg metronidazole plus 375 mg amoxicillin for 7 days) during the first, non-surgical phase of periodontal therapy (T1), and placebo during the second, surgical phase (T2). B: Placebo during T1, and antibiotics during T2. Number of sites with PD >4 mm and BOP per patient was the primary outcome. Results: sites were clinically monitored on 1870 teeth. T1 with antibiotics decreased the number of sites with PD >4 mm and BOP per patient significantly more than without (A: from 34.5 to 5.7, 84%; B: from 28.7 [...] Reference MOMBELLI, Andrea, et al. Differential benefits of amoxicillin-metronidazole in different phases of periodontal therapy Randomized controlled crossover clinical trial. Journal of Periodontology, 2015, vol. 86, no. 3, p DOI : /jop Available at: Disclaimer: layout of this document may differ from the published version.
2 J Periodontol March 2015 Differential Benefits of Amoxicillin Metronidazole in Different Phases of Periodontal Therapy in a Randomized Controlled Crossover Clinical Trial Andrea Mombelli,* Adnan Almaghlouth, Norbert Cionca,* Delphine S. Courvoisier, and Catherine Giannopoulou* Background: The specific advantage of administering systemic antibiotics during initial, non-surgical therapy or in the context of periodontal surgery is unclear. This study assesses the differential outcomes of periodontal therapy supplemented with amoxicillin metronidazole during either the non-surgical or the surgical treatment phase. Methods: This is a single-center, randomized placebo-controlled crossover clinical trial with a 1-year follow-up. Eighty participants with Aggregatibacter actinomycetemcomitans associated moderate to advanced periodontitis were randomized into two treatment groups: group A, antibiotics (500 mg metronidazole plus 375 mg amoxicillin three times per day for 7 days) during the first, non-surgical phase of periodontal therapy (T1) and placebo during the second, surgical phase (T2); and group B, placebo during T1 and antibiotics during T2. The number of sites with probing depth (PD) >4 mm and bleeding on probing (BOP) per patient was the primary outcome. Results: A total of 11,212 sites were clinically monitored on 1,870 teeth. T1 with antibiotics decreased the number of sites with PD >4 mm and BOP per patient significantly more than without (group A: from 34.5 to 5.7, 84%; group B: from 28.7 to 8.7, 70%; P <0.01). Twenty patients treated with antibiotics, but only eight treated with placebo, achieved a 10-fold reduction of diseased sites (P = 0.007). Consequently, fewer patients of group A needed additional therapy, the mean number of surgical interventions was lower, and treatment time in T2 was shorter. Six months after T2, the mean number of residual pockets (group A: ; group B: ) was not significantly different and was sustained over 12 months in both groups. Conclusion: Giving the antibiotics during T1 or T2 yielded similar long-term outcomes, but antibiotics in T1 resolved the disease quicker and thus reduced the need for additional surgical intervention. J Periodontol 2015;86: KEY WORDS Amoxicillin; case management; metronidazole; periodontitis; randomized controlled trial. *DepartmentofPeriodontology,UniversityofGeneva,Geneva,Switzerland. Previously, Department of Periodontology, University of Geneva; currently, Department of Dentistry, King Fahad Medical City, Riyadh, Saudi Arabia. Center for Clinical Research and Division of Clinical Epidemiology, University of Geneva. doi: /jop
3 Sequence of Antibiotic Treatments Volume 86 Number 3 Contemporary periodontal treatment aims at the removal of subgingival bacterial deposits (plaque and calculus) through a mechanical cleaning method called scaling and root planing (SRP). To facilitate SRP and to allow direct visual control in deep pockets, the gums can be lifted back surgically for better access. In clinical practice, periodontal therapy is usually performed in two stages. An attempt to remove a maximum of bacterial deposits is made first without elevating a flap. After 3 to 6 months, the case is reevaluated, and, if deemed necessary, additional root surface instrumentation follows, this time in the context of a local surgical intervention. The benefit of systemically administered adjunctive antibiotics, notably the combination of amoxicillin plus metronidazole, is well documented. 1-3 However, their specific indication and the optimal time point for administration are controversial. 4,5 An early study, indicating that systemic metronidazole as an adjunct to non-surgical debridement could reduce the need for subsequent surgical therapy, 6 and a later publication from the same authors claiming sustained benefits over 5 years, 7 were met with disapproval by distinguished members of the professional community. 8 Postponing antibiotic therapy to the second, surgical treatment phase may be advocated for two reasons. 9 First, because it is known that SRP alone is able to resolve a considerable amount of periodontal pathology on its own, especially in shallow and moderately deep lesions, this strategy may help to constrain the prescription of antibiotics to situations in which non-surgical mechanical therapy alone is evidently insufficient. Second, given the limited effects of antibiotics on intact biofilm and the challenge to remove such bacterial deposits from deep lesions, surgical access may provide a better opportunity for thorough debridement and thus improve the conditions for the antimicrobial agent to work. As much as this reasoning seems to make sense, data from specifically designed controlled trials are unavailable to support the recommendation. Contrary to this view, the vast majority of trials have tested antibiotics as adjuncts to SRP. A systematic review in 2008 that tried to assess the relative benefit of prescribing antibiotics either during the non-surgical phase or the surgical phase of therapy remained inconclusive. 10 However, two studies, not included in this review, showed better clinical outcomes if patients with generalized aggressive periodontitis (AgP) were given amoxicillin and metronidazole immediately after initial SRP than at a later stage of therapy. 11,12 The combination of amoxicillin plus metronidazole has been recommended in the past specifically for the treatment of Aggregatibacter actinomycetemcomitans positive patients. 13 For the present trial, this recommendation is followed. The exclusive advantage of these antibiotics in such patients was questioned later, but specific evidence 14,15 was not available when this study was designed. A systematic review determined that, on average, 62% of patients diagnosed with AgP and 28% of patients diagnosed with chronic periodontitis (CP) are A. actinomycetemcomitans positive. 16 The main purpose of this study is to evaluate the influence of timing of adjunctive systemic antibiotics on the outcomes of periodontal therapy in A. actinomycetemcomitans positive patients in a controlled randomized clinical trial (RCT). MATERIALS AND METHODS This was a single-center, double-masked, placebocontrolled RCT. Using a crossover design for antibiotic administration, 80 participants were distributed randomly into two groups: 1) group A received the antibiotics during the first stage of periodontal therapy (T1); and 2) group B received the antibiotics during the subsequent surgical phase of periodontal therapy (T2). The Ethical Committee of the University Hospitals of Geneva, Geneva, Switzerland, approved the protocol. The study was authorized by the Swiss Agency for Therapeutic Products (Swissmedic), Bern, Switzerland and is registered at ClinicalTrials.gov as NCT Research was conducted according to the principles outlined in the Declaration of Helsinki on human medical experimentation. Written informed consent was obtained from all participants. Patients By screening 319 individuals seeking treatment at the University of Geneva School of Dental Medicine between April 2009 and August 2012, 80 systemically healthy patients (41 males and 39 females, aged 26.1 to 68.8; mean age: 47.3 years) with untreated moderate to advanced periodontitis were included on the basis of the following criteria: 1) aged 25 to 70 years; 2) the presence of 12 scorable teeth (not including third molars, teeth with orthodontic appliances, bridges, crowns, or implants); 3) diagnosis of periodontitis with the presence of at least four teeth with a probing depth (PD) >4 mm; 4) clinicalattachmentloss 2 mm; 5) radiographic evidence of bone loss; and 6) detection of A. actinomycetemcomitans in a pooled sample from the deepest pocket of each quadrant (as determined with oligonucleotide probe technology 17 ). Exclusion criteria were as follows: 1) systemic illnesses (i.e., diabetes mellitus, cancer, human immunodeficiency virus, bone metabolic diseases, or disorders that compromise wound healing, radiation, or immunosuppressive therapy); 2) pregnancy or lactation; 3) systemic antibiotics taken within the previous 2 months; 4) use of non-steroid anti-inflammatory drugs; 5) confirmed or suspected intolerance to 5-nitroimidazole derivatives or amoxicillin; and 6) subgingival SRP or surgical periodontal therapy in the 368
4 J Periodontol March 2015 Mombelli, Almaghlouth, Cionca, Courvoisier, Giannopoulou past year. Smoking history was recorded, but smoking was not an exclusion criterion. Using the 1999 international classification scheme, cases might be diagnosed clinically as CP and 15 as AgP. Test Products and Randomization The test medication consisted of 500 mg metronidazole and 375 mg amoxicillin to be taken three times per day for 7 days. The control medication was a similar-looking placebo. The capsules containing the test or control medication were packaged in identical neutral boxes. The pharmacy of the Geneva University Hospital prepared the products and randomly allocated the participants to one of two treatment groups using a simple computergenerated randomization list with a random block size of 20. The therapist (NC) gave the package to the participant on the day specified by the study protocol. The treatment group was concealed to the therapist, the patient, and the clinical examiner (AA). The therapist was not involved in any clinical measurements and was unaware of the recorded data, except for the periodontal pocket chart that he needed to provide the treatment. Clinical Protocol The clinical examiner recorded the medical history and obtained informed consent. He removed all supragingival hard and soft bacterial deposits. He gave instructions in proper oral hygiene to enable the patients to keep 80% of tooth surfaces plaque free. The patients were recalled, and, if necessary, additional instructions were provided. Once the appropriate level of plaque control was reached, they were scheduled to receive subgingival treatment by the therapist (T1) within 1 month. Immediately before the therapist started, the examiner recorded the following clinical parameters on six sites of all teeth except third molars: 1) gingival index (GI); 19 2) PD; 3) recession (REC) (positive if the gingival margin was located apical to the cemento-enamel junction [CEJ] and negative if it was located coronal to the CEJ); 4) bleeding on probing (BOP); and 5) suppuration. In addition, the presence or absence of plaque (plaque score [PS]) was recorded on six sites of all teeth by running a probe across the site. The therapist then cleaned all tooth surfaces and treated the periodontally diseased teeth with thorough SRP to the depth of the pocket under local anesthesia. He first used ultrasonic instruments and then curets and finally irrigated the pockets with a 0.1% aqueous solution of chlorhexidine. SRP was completed within 48 hours and usually required two sessions. After completion, the therapist gave the medication to the participants with the instructions to start with the drug regimen on the evening of the same day, to continue three times daily for 7 days, to rinse the mouth twice daily during the next 10 days with 0.2% chlorhexidine, and to come back after 1 week, returning any medication that may have remained. Using a structured questionnaire, the examiner recorded any concomitant medication and all adverse events 1 week and 1 month after SRP. Three months after SRP, the examiner recorded the same clinical parameters as at baseline. In T2, a surgical access was provided for open-flap debridement of all teeth with residual PD 6 mm and all furcation-involved teeth with residual pockets 5 mm. A full-thickness flap was elevated, granulation tissue was removed, and the root surfaces were treated with ultrasonic and hand instruments and low-abrasive diamond burs. Non-surgical retreatment by SRP was given to any other sites with residual PD of 4 to 5 mm. Treatments were performed under local anesthesia and were accomplished in one or two sessions within 1 week. Participants were instructed to rinse the mouth twice daily during the next 10 days with 0.2% chlorhexidine. At the end of treatment, each patient received the medication and was advised to start with the drug regimen on the evening of the same day. One week after treatment, the operator removed the sutures and gave specific individualized instructions for oral hygiene after surgery. The examiner collected any remaining medication and recorded any concomitant treatment and all adverse events. The examiner saw the patients again 1, 3, 6, and 12 months after T2. At 6 and 12 months after T2, the examiner recorded the same clinical parameters as at baseline. Statistical Analyses Sites with PD 5 mmthatshowboparecommonly viewed as diseased, and persistence of these signs represents an incomplete treatment outcome with an increased risk for tooth loss. 20 Thus, in the present study, the number of sites per patient with PD >4 mmandthat had BOP was the primary outcome. Secondary outcomes included longitudinal changes of PD, BOP, REC, and clinical attachment level (CAL) (calculated as PD + REC) at sites with baseline PD >4 mm.patientaverages were computed for all measures recorded at multiple sites. Adverse events were summarized by treatment group and treatment phase for all evaluable patients. The sample size was determined on the basis of a previous study comparing SRP with or without adjunctive amoxicillin and metronidazole, with a mean difference in the number of residual pockets with PD >4 mm and BOP, 3 months after therapy, of The difference in the number of residual pockets may decrease after crossover because everyone will have been treated with the antibiotics. Thus, 37 patients per treatment arm would provide 80% power to detect a true difference of 2.0 in the number of residual pockets after therapy, assuming that the common standard deviation is 3.0 and a is Consequently, 40 participants per arm were included to compensate for 10% possible dropout. Gracey curets, Hu-Friedy, Chicago, IL. 369
5 Sequence of Antibiotic Treatments Volume 86 Number 3 Figure 1. Diagram of the different phases of the study. All analyses were done according to intention to treat by including in the analysis all patients randomized into their allocated group. The effect of treatment group on patient-level categorical variables was estimated using Fisher exact test. Linear regression (t test) was used for the patient-level continuous variables. With respect to site-level outcome, multilevel regressions considered sites as nested within teeth, themselves nested within patients. To compare the effect of treatment group over time, the treatment and the time variables, as well as their interaction, were included in the model. The effect of treatment group on the reduction of the number of sites with PD >4 mmandbop,at6monthsaftert2, was further analyzed by linear regression, using sex, age, and smoking as moderating factors. For all continuous outcomes, normality and homoscedasticity was checked using residual plots. A statistical computing program i was used for all analyses. P values <0.05 were accepted for statistical significance. RESULTS The clinical procedures and evaluations were performed from April 2009 to March Figure 1 shows the flow diagram for the different phases of the study. Seventy-one of the 80 initially recruited participants completed all visits of the study. One was lost before receiving the first intervention, two were lost after T1, two did not participate in T2, two were lost before 6 months, and two more were lost before 12 months. In addition, one participant was unavailable for the evaluation 6 months after T2. All patients completed the course of systemic medication as allocated. Table 1 displays the baseline characteristics of the participants. A total of 11,212 sites (six per tooth on a total of 1,870 teeth; eight sites were inaccessible) were clinically monitored. Pockets >4 mm had a mean PD of 6.46 mm. Table 2 shows the clinical results at the 3-month follow-up after T1 by treatment group. The non-surgical treatments provided in T1 with adjunctive antibiotics according to protocol A reduced the number of sites with PD >4 mm and BOP per patient by 83.5% (from 34.5 to 5.7) and with adjunctive placebo (protocol B) by 69.7% (from 28.7 to 8.7), with the difference in reduction being significant (P <0.01). Twenty patients (52.6%) treated with antibiotics, but only eight (20.5%) treated with placebo, achieved a 10-fold reduction of diseased sites, with the differences being significant (P = 0.007). Consequently, fewer patients of group A than group B received additional therapy in T2 (Table 3). Only three patients of group B had no sites with PD >4 mm and BOP and therefore required no additional mechanical therapy (they still received the allocated medication according to protocol). The treatment time in T2 was >30 minutes shorter for patients of group A compared with group B, although this difference was not significant because of the large variability in treatment times between patients. The mean number of surgical interventions per patient, performed according to preset rules (open-flap debridement in case of the presence of residual PD 6 mm or furcation involvement with residual PD 5 mm), was lower in patients of group A than group B. i R v.3.1.1, R Foundation for Statistical Computing, Vienna, Austria. 370
6 J Periodontol March 2015 Mombelli, Almaghlouth, Cionca, Courvoisier, Giannopoulou Table 1. Baseline Characteristics by Treatment Group (group A, n 5 40; group B, n 5 40) Variable Group A* Group B* P Age, years Females, n (%) 21 (52.5) 18 (45.0) 0.65 Smokers, n (%) 16 (40.0) 17 (42.5) 1.00 PD, mm REC, mm CAL, mm BOP, % GI score PS, % PD >4 and BOP, n sites per participant *Mean SD or number of participants (percentage). Differencebetweengroups. Table 2. Clinical Status by Treatment Group 3 Months After the Initial Therapy (group A, n 5 38; group B, n 5 39) Variable Group A* Group B* P PD; mm REC; mm CAL; mm BOP; % GI score PS; % PD >4 and BOP; n sites per participant Participants achieving a 10-fold reduction of PD >4 and BOP; n (%) Participants with persistence of sites with PD >4 and BOP; n (%) *Mean SD or number of participants (percentage). Differencebetweengroups (52.6) 8 (20.5) (64.1) 34 (89.5) 0.01 Table 4 shows the clinical results at follow-up by treatment group, 6 months after T2. The mean number of sites with PD >4 mm and BOP per patient was significantly lower than at baseline (P <0.001) in both groups, with the difference between groups in the final result not being significant. Figure 2A shows the reduction in the number of sites per participant with PD >4 mm and BOP. At 6 months after T2, it was noted that the protocol with antibiotics in T1 had reduced the number of sites with PD >4 mm and BOP more than the protocol with the antibiotics in T2, but when using the patient as the unit of analysis, the difference (31.7 versus 26.5 sites per patient less) was not significant (P = 0.36). The treatment results obtained at 6 months after T2 remained stable over 12 months. Figure 2B shows the reduction of PD (full-mouth average of sites with baseline PD >4mm).Similartothe number of sites with PD >4 mmandbop,therewas a significantly greater initial decrease of PD in the participants of group A than in those of group B (P <0.01). Six and 12 months after T2, the reductions in PD were alike (P = 0.77 and P = 0.37, respectively). The evolution of CALs (PD + REC) followed the same trend (Fig. 2C). Linear regression analysis of the reduction in the numbers of sites with PD >4 mmandbopat6months after T2 revealed that smokers benefitted from being treated according to protocol A more than nonsmokers, although this difference did not reach significance (P = 0.07). In this analysis, sex and age are not found to be significant moderating factors. Given the trend of a lower number of surgical interventions performed in the patients of group A, the effect of surgery on REC was the subject of a supplementary analysis. It was found that each surgical intervention increased REC by 0.1 mm. However, this effect was not statistically significant. There were no serious adverse events. After T1, four participants treated with antibiotics (group A) and one treated with placebo (group B) reported stomach upset (nausea, vomiting). Four patients of group A and four of group B reported gastrointestinal problems (abdominal pain, diarrhea), and one participant treated with placebo reported a headache. One of these patients, reporting abdominal pain after placebo, was a dropout at month 3. After T2, three participants treated with antibiotics (group B) and one treated with placebo (group A) reported a stomach upset. Three patients treated with antibiotics and one treated with placebo reported gastrointestinal problems. Two patients treated with placebo reported constipation and one loss of appetite. DISCUSSION In the vast majority of trials evaluating systemic antibiotics for the treatment of periodontal disease, 371
7 Sequence of Antibiotic Treatments Volume 86 Number 3 Table 3. Treatments in T2 (group A, n 5 38; group B, n 5 37) Variable Group A* Group B* P Participants needing additional mechanical therapy in T2; n (%) Participants needing more than one session to treat; n (%) Treatment time, minutes per participant Surgical interventions, n per participant 28 (73.7) 33 (89.2) (26.3) 15 (40.5) *Mean SD or number of participants (%). Differencebetweengroups. Table 4. Clinical Characteristics 6 Months After Completion of T2 (group A, n 5 37; group B, n 5 35) Variable Group A* Group B* P PD, mm REC, mm CAL, mm BOP, % GI, score PS, % PD >4 and BOP, n sites per participant Participants achieving a 10-fold reduction of PD >4 and BOP; n (%) Participants with persistence of sites with PD >4 and BOP; n (%) *Mean SD or number of participants (percentage). Differencebetweengroups (86.5) 29 (82.9) (29.7) 15 (42.9) 0.33 Figure 2. Reduction of the number of sites with PD >4 mm and BOP per patient (A), reduction of PD as full-mouth average of sites with baseline PD >4 mm (B), and CAL (PD + REC) gain as full-mouth average of sites with baseline PD >4 mm (C) by treatment group. Values were computed as the difference from baseline to months 3 after T1 and from baseline to 6 and 12 months after T2. Significance of the difference between groups is indicated. the drugs were administered as adjunct to SRP, and the participants were monitored without additional intervention over several months. This does not correspond to common practice, because clinical signs of disease occasionally persist after non-surgical debridement, and additional therapy may thus be indicated. The influence of the timing of antibiotic therapy in a sequential protocol that corresponds better to current practice was evaluated. In the present study, giving amoxicillin plus metronidazole in T1 or T2 had no influence on the long-term outcome: 6 or 12 months after therapy, the mean number of sites with PD >4 mm and BOP per patient was significantly lower than at baseline in both groups, with no significant difference between the two. However, fewer patients treated with adjunctive antibiotics in T1 received additional therapy, the treatment time in T2 was shorter, 372
8 J Periodontol March 2015 Mombelli, Almaghlouth, Cionca, Courvoisier, Giannopoulou and the mean number of surgical interventions was lower. The present findings are in line with recent trials also suggesting that SRP with amoxicillin plus metronidazole can reduce the need for surgical interventions. 22,23 Given the debate about the discriminatory significance of the 1999 classification system, 24 recruitment of participants followed practical rules to identify patients with periodontal disease irrespective of the presumed disease class. So far, the specific moderating effect of disease class on the benefit of amoxicillin and metronidazole has not been determined in an accurately conducted trial. Because amoxicillin plus metronidazole was advocated in the past, especially for the treatment of A. actinomycetemcomitans-associated periodontitis, 13 apositivetestforthismicroorganismwasrequired for inclusion. Recent research refutes claims about an exclusive advantage of these antibiotics in A. actinomycetemcomitans positive patients, 14,25,26 but this was not yet recognized when the study started. The benefit of the first part of the clinical protocol of the present study full-mouth SRP completed within 48 hours in T1 has been evaluated in a previous independent trial. 21,27 Allowing 48 hours to deliver full-mouth SRP gives the clinical staff some leeway for scheduling and permits avoiding anesthesia at both sides of the dentition on the same day. A systematic review concluded that the specific modus of delivering SRP, for example quadrant-wise SRP compared with full-mouth SRP within 24 hours, had little effect on the outcome. 28 The selection of efficacy endpoints for clinical trials on periodontal therapy is a subject of debate. 29 Mean CAL changes have been used as endpoint measures; however, in clinical practice, the most consequential outcome is the disappearance of deep pockets with signs of inflammation. Sites with PD >4 mm and BOP are considered commonly to be in need of additional care and thus were the focus of this investigation. Assuming that pockets >4 mm with BOP need additional therapy, treatment needs can be estimated by the number of residual pockets. However, multiple residual pockets can sometimes be treated in a single intervention, so the number of surgeries also depends on the location and distribution of the lesions. The data collected in this trial allow not only an estimation of treatment needs but also permit a comparison of the interventions actually performed. AcomplicatedRCTcomparedtreatmentoutcomes of SRP, with or without adjunctive amoxicillin plus metronidazole and/or local tetracycline therapy and/or followed by periodontal surgery. 30 Eight groups of 30 patients were assigned to eight imaginable permutations of these elements and were followed over 24 months. PD reduction was seen to a greater extent in patients receiving periodontal surgery. Patients treated with adjunctive antibiotics continued to gain CAL and showed continuous decrease of PD up to 6 months after therapy. The plateau reached at that point in time was kept throughout the remainder of the observation period. Systemic amoxicillin and metronidazole enhanced mean CAL gains by 0.5 mm. PD was reduced to a similar degree by antibiotics or surgery (0.5 or 0.4 mm, respectively). In the present study, similar outcomes 6 and 12 months after therapy according to either protocol A or B indicate that the clinical improvements obtained from non-surgical treatment were as stable as results obtained by surgical intervention. Studies monitoring patients over longer periods after various treatments have repeatedly identified three crucial factors for long-term stability: 1) the level of selfperformed oral hygiene; 2) the inclusion in a maintenance program; and 3) not smoking The results from the present study suggest that smokers may have a specific advantage from being treated with the combination of amoxicillin and metronidazole in the non-surgical phase. This is in line with a study showing good results of therapy especially with SRP plus amoxicillin and metronidazole in smokers. 36 In contrast, an earlier trial reported poorer treatment response to SRP in smokers than nonsmokers, regardless of the application of either systemic or locally applied adjunctive metronidazole alone, 37 and a recent study suggested that smokers do not respond as well as non-smokers. 38 The incidence and nature of adverse events observed in this study correspond to observations made in previous studies. 2,3 Adverse events were generally minor, sporadic, and without a particular association with one group. The specific design of the trial (all participants were treated with antibiotics in either T1 or T2) precludes an evaluation of all aspects of adverse events. CONCLUSIONS In patients with moderate to advanced periodontitis, systemic amoxicillin plus metronidazole significantly enhanced the effects of full-mouth SRP. Consequently, fewer patients of this group received additional therapy in T2. Differences in the final results between groups were not significant. ACKNOWLEDGMENTS This work was supported by Swiss National Science Foundation Grant and a scholarship from the Royal Saudi Arabian Government (to AA). The Institute for Applied Immunology, Zuchwil, Switzerland, analyzed the microbiologic samples taken for the purpose of screening free of charge. The help of Céline Nicole-Ippolito (Department of Periodontology, University of Geneva, Geneva, Switzerland) in data acquisition is greatly appreciated. The authors report no conflicts of interest related to this study. 373
9 Sequence of Antibiotic Treatments Volume 86 Number 3 REFERENCES 1. Zandbergen D, Slot DE, Cobb CM, Van der Weijden FA. The clinical effect of scaling and root planing and the concomitant administration of systemic amoxicillin and metronidazole: A systematic review. J Periodontol 2013;84: Sgolastra F, Gatto R, Petrucci A, Monaco A. Effectiveness of systemic amoxicillin/metronidazole as adjunctive therapy to scaling and root planing in the treatment of chronic periodontitis: A systematic review and metaanalysis. J Periodontol 2012;83: Sgolastra F, Petrucci A, Gatto R, Monaco A. Effectiveness of systemic amoxicillin/metronidazole as an adjunctive therapy to full-mouth scaling and root planing in the treatment of aggressive periodontitis: A systematic review and meta-analysis. J Periodontol 2012;83: Zandbergen D, Slot DE, Cobb CM, Van der Weijden FA. Letter to the editor: Authors response. J Periodontol 2014;85: Preus HR, Scheie AA, Baelum V. Letter to the editor: Re: The clinical effect of scaling and root planing and the concomitant administration of systemic amoxicillin and metronidazole: A systematic review; Re: Effectiveness of systemic amoxicillin/metronidazole as adjunctive therapy to scaling and root planing in the treatment of chronic periodontitis: A systematic review and metaanalysis; Re: Effectiveness of systemic amoxicillin/ metronidazole as an adjunctive therapy to full-mouth scaling and root planing in the treatment of aggressive periodontitis: A systematic review and meta-analysis. J Periodontol 2014;85: Loesche WJ, Giordano JR, Hujoel P, Schwarcz J, Smith BA. Metronidazole in periodontitis: Reduced need for surgery. J Clin Periodontol 1992;19: Loesche WJ, Giordano JR, Soehren S, Kaciroti N. The nonsurgical treatment of patients with periodontal disease: Results after five years. J Am Dent Assoc 2002;133: Robbins J. Experts debate the best way to fix ailing gums. The New York Times. January 21, Mombelli A. Antimicrobial advances in treating periodontal diseases. Front Oral Biol 2012;15: Herrera D, Alonso B, León R, Roldán S, Sanz M. Antimicrobial therapy in periodontitis: The use of systemic antimicrobials against the subgingival biofilm. J Clin Periodontol 2008;35(Suppl. 8): Kaner D, Christan C, Dietrich T, Bernimoulin JP, Kleber BM, Friedmann A. Timing affects the clinical outcome of adjunctive systemic antibiotic therapy for generalized aggressive periodontitis. J Periodontol 2007;78: Griffiths GS, Ayob R, Guerrero A, et al. Amoxicillin and metronidazole as an adjunctive treatment in generalized aggressive periodontitis at initial therapy or retreatment: A randomized controlled clinical trial. J Clin Periodontol 2011;38: van Winkelhoff AJ, Winkel EG. Microbiological diagnostics in periodontics: Biological significance and clinical validity. Periodontol ;39: Mombelli A, Cionca N, Almaghlouth A, Décaillet F, Courvoisier DS, Giannopoulou C. Are there specific benefits of amoxicillin plus metronidazole in Aggregatibacter actinomycetemcomitans-associated periodontitis? Double-masked, randomized clinical trial of efficacy and safety. J Periodontol 2013;84: Guerrero A, Nibali L, Lambertenghi R, et al. Impact of baseline microbiological status on clinical outcomes in generalized aggressive periodontitis patients treated with or without adjunctive amoxicillin and metronidazole: An exploratory analysis from a randomized controlled clinical trial. JClinPeriodontol2014;41: Mombelli A, Casagni F, Madianos PN. Can presence or absence of periodontal pathogens distinguish between subjects with chronic and aggressive periodontitis? A systematic review. J Clin Periodontol 2002;29(Suppl. 3):10-21, discussion Dix K, Watanabe SM, McArdle S, et al. Species-specific oligodeoxynucleotide probes for the identification of periodontal bacteria. J Clin Microbiol 1990;28: Armitage GC. Development of a classification system for periodontal diseases and conditions. Ann Periodontol 1999;4: Löe H, Silness J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand 1963;21: Matuliene G, Pjetursson BE, Salvi GE, et al. Influence of residual pockets on progression of periodontitis and tooth loss: Results after 11 years of maintenance. J Clin Periodontol 2008;35: Cionca N, Giannopoulou C, Ugolotti G, Mombelli A. Amoxicillin and metronidazole as an adjunct to fullmouth scaling and root planing of chronic periodontitis. J Periodontol 2009;80: Mestnik MJ, Feres M, Figueiredo LC, et al. The effects of adjunctive metronidazole plus amoxicillin in the treatment of generalized aggressive periodontitis: A1-yeardouble-blinded,placebo-controlled, randomized clinical trial. JClinPeriodontol2012;39: Feres M, Soares GM, Mendes JA, et al. Metronidazole alone or with amoxicillin as adjuncts to non-surgical treatment of chronic periodontitis: A 1-year doubleblinded, placebo-controlled, randomized clinical trial. J Clin Periodontol 2012;39: Armitage GC. AAP centennial commentary: Theme 3: Evolution and application of classification systems for periodontal diseases A retrospective commentary. J Periodontol 2014;85: Socransky SS, Haffajee AD, Teles R, et al. Effect of periodontal therapy on the subgingival microbiota over a 2-year monitoring period. I. Overall effect and kinetics of change. J Clin Periodontol 2013;40: Soares GM, Mendes JA, Silva MP, et al. Metronidazole alone or with amoxicillin as adjuncts to non-surgical treatment of chronic periodontitis: A secondary analysis of microbiological results from a randomized clinical trial. J Clin Periodontol 2014;41: Cionca N, Giannopoulou C, Ugolotti G, Mombelli A. Microbiologic testing and outcomes of full-mouth scaling and root planing with or without amoxicillin/ metronidazole in chronic periodontitis. J Periodontol 2010;81: Eberhard J, Jepsen S, Jervøe-Storm PM, Needleman I, Worthington HV. Full-mouth disinfection for the treatment of adult chronic periodontitis. Cochrane Database Syst Rev 2008;(1):CD Hujoel PP. Endpoints in periodontal trials: The need for an evidence-based research approach. Periodontol ;36:
10 J Periodontol March 2015 Mombelli, Almaghlouth, Cionca, Courvoisier, Giannopoulou 30. Goodson JM, Haffajee AD, Socransky SS, et al. Control of periodontal infections: A randomized controlled trial I. The primary outcome attachment gain and pocket depth reduction at treated sites. J Clin Periodontol 2012;39: Eickholz P, Krigar DM, Pretzl B, Steinbrenner H, Dörfer C, Kim TS. Guided tissue regeneration with bioabsorbable barriers. II. Long-term results in infrabony defects. J Periodontol 2004;75: Cortellini P, Tonetti MS. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004;75: Axelsson P, Nyström B, Lindhe J. The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J Clin Periodontol 2004;31: Axelsson P, Lindhe J. The significance of maintenance care in the treatment of periodontal disease. J Clin Periodontol 1981;8: Lindhe J, Westfelt E, Nyman S, Socransky SS, Haffajee AD. Long-term effect of surgical/non-surgical treatment of periodontal disease. J Clin Periodontol 1984; 11: Matarazzo F, Figueiredo LC, Cruz SE, Faveri M, Feres M. Clinical and microbiological benefits of systemic metronidazole and amoxicillin in the treatment of smokers with chronic periodontitis: A randomized placebo-controlled study. J Clin Periodontol 2008;35: Palmer RM, Matthews JP, Wilson RF. Non-surgical periodontal treatment with and without adjunctive metronidazole in smokers and non-smokers. J Clin Periodontol 1999;26: Faveri M, Rebello A, de Oliveira Dias R, et al. Clinical and microbiologic effects of adjunctive metronidazole plus amoxicillin in the treatment of generalized chronic periodontitis: Smokers versus non-smokers. J Periodontol 2014;85: Correspondence: Dr. Andrea Mombelli, School of Dental Medicine, University of Geneva, Rue Barthélemy-Menn 19, CH-1205 Geneva, Switzerland. Fax: ; Andrea.Mombelli@unige.ch. Submitted August 18, 2014; accepted for publication October 21,
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS
 Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
DUAL ANTIBIOTIC SYSTEMIC THERAPY IN THE TREATMENT OF PERIODONTAL DISEASES AND THE ROLE OF METRONIDAZOLE
 DUAL ANTIBIOTIC SYSTEMIC THERAPY IN THE TREATMENT OF PERIODONTAL DISEASES AND THE ROLE OF METRONIDAZOLE BesianABAZI¹,JoanaMIHANI² Abstract INTRODUCTION: OBJECTIVE: MATERIALSANDMETHODS: RESULTS: CONCLUSIONS:
DUAL ANTIBIOTIC SYSTEMIC THERAPY IN THE TREATMENT OF PERIODONTAL DISEASES AND THE ROLE OF METRONIDAZOLE BesianABAZI¹,JoanaMIHANI² Abstract INTRODUCTION: OBJECTIVE: MATERIALSANDMETHODS: RESULTS: CONCLUSIONS:
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
Non-surgical periodontal therapy with systemic antibiotics in patients with untreated aggressive periodontitis: a systematic review and meta-analysis
 J Periodont Res 2014 All rights reserved Review Article Non-surgical periodontal therapy with systemic antibiotics in patients with untreated aggressive periodontitis: a systematic review and meta-analysis
J Periodont Res 2014 All rights reserved Review Article Non-surgical periodontal therapy with systemic antibiotics in patients with untreated aggressive periodontitis: a systematic review and meta-analysis
The International Journal of Periodontics & Restorative Dentistry
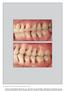 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The ultimate goal in periodontal
 Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS
 THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
Journal of Dentistry, Tehran University of Medical Sciences
 Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester
 Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report
 Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
XIV CONGRESSO INTERNAZIONALE
 Società Italiana di Parodontologia Adjunctive effect of neridronate in non-surgical periodontal therapy: a randomized clinical trial Effetti aggiuntivi del neridronato alla terapia parodontale non chirurgica:
Società Italiana di Parodontologia Adjunctive effect of neridronate in non-surgical periodontal therapy: a randomized clinical trial Effetti aggiuntivi del neridronato alla terapia parodontale non chirurgica:
Research Article Full Mouth Disinfection Versus Scaling and Root Planing per Quadrant in Aggressive Periodontitis: A Systematic Review
 Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Full Mouth Disinfection Versus Scaling and Root Planing per Quadrant in Aggressive Periodontitis: A Systematic Review Maísa Casarin 1 *, Danilo Antonio
Cronicon OPEN ACCESS EC DENTAL SCIENCE Research Article Full Mouth Disinfection Versus Scaling and Root Planing per Quadrant in Aggressive Periodontitis: A Systematic Review Maísa Casarin 1 *, Danilo Antonio
Periodontal Patient Management
 Periodontal Patient Management Area Dental Meeting Day 3 Tim Ricks, DMD, MPH, ADO Presentation Purposes Show steps in the diagnosis of disease Reiterate sequence of care in patients with periodontal disease
Periodontal Patient Management Area Dental Meeting Day 3 Tim Ricks, DMD, MPH, ADO Presentation Purposes Show steps in the diagnosis of disease Reiterate sequence of care in patients with periodontal disease
Antimicrobial Treatment for Advanced Periodontal Disease
 Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Quadrant root planing versus same-day full-mouth root planing I. Clinical findings
 J Clin Periodontol 24; 31: 132 14 Copyright r Blackwell Munksgaard 24 Printed in Denmark. All rights reserved Quadrant root planing versus same-day full-mouth root planing I. Clinical findings D. A. Apatzidou
J Clin Periodontol 24; 31: 132 14 Copyright r Blackwell Munksgaard 24 Printed in Denmark. All rights reserved Quadrant root planing versus same-day full-mouth root planing I. Clinical findings D. A. Apatzidou
Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis
 CLINICAL AND RESEARCH REPORTS Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis Takeo Fujii, Pao-Li Wang, Yoichiro Hosokawa, Shinichi Shirai, Atsumu Tamura, Kazuhiro
CLINICAL AND RESEARCH REPORTS Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis Takeo Fujii, Pao-Li Wang, Yoichiro Hosokawa, Shinichi Shirai, Atsumu Tamura, Kazuhiro
effect of surgical debridement vs. non-surgical debridement for the treatment of chronic periodontitis.
 J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
There are three referral categories used in the dental referral system:
 Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
The dentogingival junction to the
 Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
12-Months Clinical Comparison between Osteoinductal and Emdogain for the Treatment of Intrabony Defects
 Seite 1 von 5 Int Poster J Dent Oral Med 2007, Vol 9 No 01, Poster 348 12-Months Clinical Comparison between and Emdogain for the Treatment of Intrabony Defects Language: English Authors: Assist. Prof.
Seite 1 von 5 Int Poster J Dent Oral Med 2007, Vol 9 No 01, Poster 348 12-Months Clinical Comparison between and Emdogain for the Treatment of Intrabony Defects Language: English Authors: Assist. Prof.
EXCEEDS, SATISFACTORY, DOES NOT MEET GRADING CRITERIA FOR PREDOCTORAL PERIODONTICS CASES AND REEVALUATION
 A. For prophylaxis, periodontal maintenance, and SRP cases: 1. Charting accuracy a. Exceeds Expectations - Student has accurately charted the patient's oral condition. The charting includes O Leary plaque
A. For prophylaxis, periodontal maintenance, and SRP cases: 1. Charting accuracy a. Exceeds Expectations - Student has accurately charted the patient's oral condition. The charting includes O Leary plaque
PERIODONTAL CASE PRESENTATION - 1
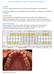 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Oral hygiene reinforcement in the simplified periodontal treatment of 1 hour
 J Clin Periodontol 2014; 41: 149 156 doi: 10.1111/jcpe.12200 Oral hygiene reinforcement in the simplified periodontal treatment of 1 hour Danae A. Apatzidou, Penelope Zygogianni, Dimitra Sakellari and
J Clin Periodontol 2014; 41: 149 156 doi: 10.1111/jcpe.12200 Oral hygiene reinforcement in the simplified periodontal treatment of 1 hour Danae A. Apatzidou, Penelope Zygogianni, Dimitra Sakellari and
Additive or Synergistic Antimicrobial Effects of Amoxicillin and Metronidazole on Whole Plaque Samples: A Preliminary Report
 Journal of the International Academy of Periodontology 2011 13/1: 11 16 Additive or Synergistic Antimicrobial Effects of Amoxicillin and Metronidazole on Whole Plaque Samples: A Preliminary Report Clemens
Journal of the International Academy of Periodontology 2011 13/1: 11 16 Additive or Synergistic Antimicrobial Effects of Amoxicillin and Metronidazole on Whole Plaque Samples: A Preliminary Report Clemens
Reimbursement Guide. ATRIDOX Insurance Reimbursement Guide for the submission of insurance claims
 Reimbursement Guide Insurance Reimbursement Guide f the submission of insurance claims General reimbursement & submission infmation Reimbursement infmation Submission of insurance claims Pre-determination
Reimbursement Guide Insurance Reimbursement Guide f the submission of insurance claims General reimbursement & submission infmation Reimbursement infmation Submission of insurance claims Pre-determination
Mechanical Non Surgical Therapy: An Indispensable Tool
 IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
FACULTY OF HEALTH SCIENCES INSTITUTE OF CLINICAL DENTISTRY
 Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Khosropanah H., et al J Dent Shiraz Univ Med Scien June; 13(2): 44-48
 Original Article The Clinical Effectiveness of Subgingival Irrigation with Povidone-Iodine and Hydrogen Peroxide in Treatment of Moderate to Severe Chronic Periodontitis Khosropanah H. a, Koohpeima F.
Original Article The Clinical Effectiveness of Subgingival Irrigation with Povidone-Iodine and Hydrogen Peroxide in Treatment of Moderate to Severe Chronic Periodontitis Khosropanah H. a, Koohpeima F.
JMSCR Volume 2 Issue 7 Page July
 www.jmscr.igmpublication.org Impact Factor 1.1147 ISSN (e)-2347-176x Clinical Evaluation of Locally Delivered 10% Doxycycline Hyclate Gel as An Adjunct to Scaling and Root Planing in the Treatment of Chronic
www.jmscr.igmpublication.org Impact Factor 1.1147 ISSN (e)-2347-176x Clinical Evaluation of Locally Delivered 10% Doxycycline Hyclate Gel as An Adjunct to Scaling and Root Planing in the Treatment of Chronic
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
What s new for the clinician? Summaries of and excerpts from recently published papers
 http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Full-mouth treatment concepts for chronic periodontitis: a systematic review
 J Clin Periodontol 2008; 35: 591 604 doi: 10.1111/j.1600-051X.2008.01239.x Full-mouth treatment concepts for chronic periodontitis: a systematic review Eberhard J, Jervøe-Storm P-M, Needleman I, Worthington
J Clin Periodontol 2008; 35: 591 604 doi: 10.1111/j.1600-051X.2008.01239.x Full-mouth treatment concepts for chronic periodontitis: a systematic review Eberhard J, Jervøe-Storm P-M, Needleman I, Worthington
Initial Therapy. Alessan"o Geminiani, DDS, MS. Oral sulcular epithelium. Oral. epithelium. Junctional. epithelium. Connective tissue.
 Oral sulcular epithelium Junctional epithelium E Oral epithelium Initial Therapy Connective tissue Bone Alessan"o Geminiani, DDS, MS Non-surgical Therapy Scaling: Instrumentation of the crown and root
Oral sulcular epithelium Junctional epithelium E Oral epithelium Initial Therapy Connective tissue Bone Alessan"o Geminiani, DDS, MS Non-surgical Therapy Scaling: Instrumentation of the crown and root
Osseous surgery in periodontal treatment
 SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
SCIENTIFIC SESSION Osseous surgery in periodontal treatment Essayist: Roberto Pontoriero Introduction In periodontally involved patients, periodontal therapy usually results in various degrees of soft-tissue
CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY
 204 CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY Supportive Periodontal Therapy CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY DEFINITION Supportive Periodontal Treatment (Periodontal Maintenance, Preventive
204 CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY Supportive Periodontal Therapy CHAPTER 10. SUPPORTIVE PERIODONTAL THERAPY DEFINITION Supportive Periodontal Treatment (Periodontal Maintenance, Preventive
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Dina Zandbergen 1, Dagmar Else Slot 1*, Richard Niederman 2 and Fridus A. Van der Weijden 1,3
 Zandbergen et al. BMC Oral Health DOI 10.1186/s12903-015-0123-6 RESEARCH ARTICLE Open Access The concomitant administration of systemic amoxicillin and metronidazole compared to scaling and root planing
Zandbergen et al. BMC Oral Health DOI 10.1186/s12903-015-0123-6 RESEARCH ARTICLE Open Access The concomitant administration of systemic amoxicillin and metronidazole compared to scaling and root planing
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
[4] Loe H, Theilade E, Jensen SB. Experimental gingivits in man. J Periodontol May-Jun;36:
![[4] Loe H, Theilade E, Jensen SB. Experimental gingivits in man. J Periodontol May-Jun;36: [4] Loe H, Theilade E, Jensen SB. Experimental gingivits in man. J Periodontol May-Jun;36:](/thumbs/82/86455625.jpg) PNC 1 (11) 2017, S. 6-12 Timing in der systematischen Parodontitistherapie Prof. Dr. Peter Hahner, Prof. Dr. Georg Gaßmann Literatur [1] McGuire MK. Prognosis versus actual outcome: a long-term survey
PNC 1 (11) 2017, S. 6-12 Timing in der systematischen Parodontitistherapie Prof. Dr. Peter Hahner, Prof. Dr. Georg Gaßmann Literatur [1] McGuire MK. Prognosis versus actual outcome: a long-term survey
Home care. Home care. Core Values for Treating Patients in Practice. Professional care. BSP Roadshows 2008/9
 3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Influence of different post-interventional maintenance concepts on periodontal outcomes: an evaluation of three systematic reviews
 Gartenmann et al. BMC Oral Health (017) 17:19 DOI 10.1186/s1903-016-044-6 RESEARCH ARTICLE Open Access Influence of different post-interventional maintenance concepts on periodontal outcomes: an evaluation
Gartenmann et al. BMC Oral Health (017) 17:19 DOI 10.1186/s1903-016-044-6 RESEARCH ARTICLE Open Access Influence of different post-interventional maintenance concepts on periodontal outcomes: an evaluation
- BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis
 Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology
 A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology Christine M. Blue, BSDH, MS; Patricia Lenton, RDH, MA; Scott Lunos, MS; Kjersta Poppe, RDH, MS; Joy Osborn,
A Pilot Study Comparing the Outcome of Scaling/Root Planing With and Without Perioscope Technology Christine M. Blue, BSDH, MS; Patricia Lenton, RDH, MA; Scott Lunos, MS; Kjersta Poppe, RDH, MS; Joy Osborn,
2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd
 J Clin Periodontol 2014; 41: 890 899 doi: 10.1111/jcpe.12282 Metronidazole and amoxicillin as adjuncts to scaling and root planing for the treatment of type 2 diabetic subjects with periodontitis: 1-year
J Clin Periodontol 2014; 41: 890 899 doi: 10.1111/jcpe.12282 Metronidazole and amoxicillin as adjuncts to scaling and root planing for the treatment of type 2 diabetic subjects with periodontitis: 1-year
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
ARESTIN (minocycline hcl) subgingival powder
 ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Clinical efficacy of phase I therapy combined with a triclosan/copolymer dentifrice on generalized chronic periodontitis
 Journal of Dental Sciences (2010) 5, 216e220 available at www.sciencedirect.com journal homepage: www.e-jds.com Original Article Clinical efficacy of phase I therapy combined with a triclosan/copolymer
Journal of Dental Sciences (2010) 5, 216e220 available at www.sciencedirect.com journal homepage: www.e-jds.com Original Article Clinical efficacy of phase I therapy combined with a triclosan/copolymer
Have you been diag nosed with PERIODONTAL DISEASE
 Have you been diag nosed with PERIODONTAL DISEASE What you need to know about Periodontal Disease? Periodontal disease (also called gum disease) is a chronic, bacterial infection of the gums that can destroy
Have you been diag nosed with PERIODONTAL DISEASE What you need to know about Periodontal Disease? Periodontal disease (also called gum disease) is a chronic, bacterial infection of the gums that can destroy
An intriguing case of gingival enlargement associated with generalised aggressive periodontitis
 CLINICAL REPORT 295 Ajay Mahajan, Jaya Dixit, Umesh Verma An intriguing case of gingival enlargement associated with generalised aggressive periodontitis KEY WORDS antimicrobial therapy, clinical findings,
CLINICAL REPORT 295 Ajay Mahajan, Jaya Dixit, Umesh Verma An intriguing case of gingival enlargement associated with generalised aggressive periodontitis KEY WORDS antimicrobial therapy, clinical findings,
Periodontal Treatment Guide
 Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
THE AMERICAN ACADEMY OF PERIODONTOLOGY
 THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
Clinical Management of an Unusual Case of Gingival Enlargement
 Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
Subject: Periodontal Maintenance Guideline #: Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/05/2018
 Dental Policy Subject: Periodontal Maintenance Guideline #: 04-901 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/05/2018 Description This document addresses periodontal maintenance. Note:
Dental Policy Subject: Periodontal Maintenance Guideline #: 04-901 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/05/2018 Description This document addresses periodontal maintenance. Note:
TITLE: Periostat for Periodontal Disease: A Review of the Clinical Effectiveness, Cost Effectiveness and Guidelines
 TITLE: Periostat f Periodontal Disease: A Review of the Clinical Effectiveness, Cost Effectiveness and Guidelines DATE: 10 May 2012 CONTEXT AND POLICY ISSUES Periodontal disease is a common condition which
TITLE: Periostat f Periodontal Disease: A Review of the Clinical Effectiveness, Cost Effectiveness and Guidelines DATE: 10 May 2012 CONTEXT AND POLICY ISSUES Periodontal disease is a common condition which
Volume 27 No. 11 August New Information and Reminders for Dental Services
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 27 No. 11 August 2017 To: Subject: Dental Providers - For Action Managed Care Organizations For
Screenings, Indices Their influence on the treatment plan (Berne concept)
 Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Transient Tooth Discoloration After Periodontal Instrumentation of an Aggressive Periodontitis. A Case Report
 Transient Tooth Discoloration After Periodontal Instrumentation of an Aggressive Periodontitis. A Case Report Julio C Rincon A*, Zahida Oakley*, Paul Abbott *Department of Periodontology and Implant Dentistry.
Transient Tooth Discoloration After Periodontal Instrumentation of an Aggressive Periodontitis. A Case Report Julio C Rincon A*, Zahida Oakley*, Paul Abbott *Department of Periodontology and Implant Dentistry.
Show biofilm the red card
 Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93.
 Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Periodontal Case Report
 Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
Systemic Chemotherapeutic Agents as Adjunctive Periodontal Therapy: A Narrative Review and Suggested Clinical Recommendations
 Journal of the International Academy of Periodontology 2015 17/4: 123 134 Systemic Chemotherapeutic Agents as Adjunctive Periodontal Therapy: A Narrative Review and Suggested Clinical Recommendations Rachel
Journal of the International Academy of Periodontology 2015 17/4: 123 134 Systemic Chemotherapeutic Agents as Adjunctive Periodontal Therapy: A Narrative Review and Suggested Clinical Recommendations Rachel
Predictors of clinical outcomes after periodontal treatment of aggressive periodontitis: 12-month randomized trial
 Original Research; Periodontology Predictors of clinical outcomes after periodontal treatment of aggressive periodontitis: 12-month randomized trial Alex Nogueira HAAS (a) Carina Maciel SILVA-BOGHOSSIAN
Original Research; Periodontology Predictors of clinical outcomes after periodontal treatment of aggressive periodontitis: 12-month randomized trial Alex Nogueira HAAS (a) Carina Maciel SILVA-BOGHOSSIAN
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera
 Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Optimization of the periodontal attachment before orthodontic treatment
 DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
DOI: 10.1051/odfen/2017008 J Dentofacial Anom Orthod 2017;20:307 The authors Optimization of the periodontal attachment before orthodontic treatment S. Mouraret 1, J.-P. Forestier 2 1 Private practice
Periodontitis is characterized by
 Journal of Oral Health & Community Dentistry original article Povidone Iodine vs Tetracycline Fibers- To Analyse the Therapeutic Effect Suchetha A 1, Garg A 2, Lakshmi P 3,Sapna N 4, Mundinamane DB 5,
Journal of Oral Health & Community Dentistry original article Povidone Iodine vs Tetracycline Fibers- To Analyse the Therapeutic Effect Suchetha A 1, Garg A 2, Lakshmi P 3,Sapna N 4, Mundinamane DB 5,
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
HDS PROCEDURE CODE GUIDELINES
 D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
Implementing Hygiene Systems for Increased Productivity
 Implementing Hygiene Systems for Increased Productivity Rachel Wall, RDH, BS Phone 704-541-0995 Fax 866-645-4469 Rachel@inspiredhygiene.com www.inspiredhygiene.c Copyright 2014. Revised 2017 Inspired Hygiene
Implementing Hygiene Systems for Increased Productivity Rachel Wall, RDH, BS Phone 704-541-0995 Fax 866-645-4469 Rachel@inspiredhygiene.com www.inspiredhygiene.c Copyright 2014. Revised 2017 Inspired Hygiene
Giovanpaolo Pini-Prato, MD, DDS, PhD1 Cristina Magnani, DDS1 Roberto Rotundo, DDS2
 55 T r e a tm e n t o f A c u te P e r io d o n ta l A b s c e s s e s U s in g th e B io film D e c o n ta m in a tio n A p p r o a c h : A C a s e R e p o rt S tu d y Giovanpaolo Pini-Prato, MD, DDS,
55 T r e a tm e n t o f A c u te P e r io d o n ta l A b s c e s s e s U s in g th e B io film D e c o n ta m in a tio n A p p r o a c h : A C a s e R e p o rt S tu d y Giovanpaolo Pini-Prato, MD, DDS,
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus
 Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
2017 Oregon Dental Conference Course Handout
 2017 Oregon Dental Conference Course Handout Kimberly Miller, RDH Course 8123: Principle Based Periodontal Therapy and Treatment Planning! Thursday, April 6 9 am - 4:30 pm Principle Based Periodontal Therapy
2017 Oregon Dental Conference Course Handout Kimberly Miller, RDH Course 8123: Principle Based Periodontal Therapy and Treatment Planning! Thursday, April 6 9 am - 4:30 pm Principle Based Periodontal Therapy
Introduction to Periodontal and Implant Surgery
 Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
2018 Oregon Dental Conference Course Handout
 2018 Oregon Dental Conference Course Handout James Kohner, DDS Course 9147: Beating Up on Your Patients Periodontal Disease: A Minimally Invasive Approach Friday, April 6 2 pm 5 pm James S. Kohner, D.D.S.
2018 Oregon Dental Conference Course Handout James Kohner, DDS Course 9147: Beating Up on Your Patients Periodontal Disease: A Minimally Invasive Approach Friday, April 6 2 pm 5 pm James S. Kohner, D.D.S.
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
THE NATU R R E A G L E N P E R R O A M TI O O T N ER OF
 Hyaluronic Acid THE NATURAL PROMOTER OF 1 HYADENT BG & HYADENT HYALURONIC ACID-MODE OF ACTION ATTRACTS BLOOD THE NATURAL PROMOTER OF HYADENT BG, a highly concentrated and cross-linked hyaluronic acid gel,
Hyaluronic Acid THE NATURAL PROMOTER OF 1 HYADENT BG & HYADENT HYALURONIC ACID-MODE OF ACTION ATTRACTS BLOOD THE NATURAL PROMOTER OF HYADENT BG, a highly concentrated and cross-linked hyaluronic acid gel,
Your Pet s Dentistry Procedure
 Your Pet s Dentistry Procedure Does your pets breath smell? Periodontal disease is the most common disease in dogs and cats. Without adequate care and attention, periodontal disease can result in pain,
Your Pet s Dentistry Procedure Does your pets breath smell? Periodontal disease is the most common disease in dogs and cats. Without adequate care and attention, periodontal disease can result in pain,
For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT)
 For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT) Dear Dental Care Provider, Thank you for your contribution
For Dentists and Other Dental Professionals: Dental Screening Program for Patients Who May Need Hematopoietic Stem Cell Transplantation (HSCT) Dear Dental Care Provider, Thank you for your contribution
Ortho Hygiene. #2078, Tuscany Blvd. NW, Calgary, AB T3L 2V7 Phone: Fax:
 Ortho Hygiene You already know that maintaining good oral hygiene is important for everyone but when you re having orthodontic treatment, it s even more critical. Why? Because, while the appliances (such
Ortho Hygiene You already know that maintaining good oral hygiene is important for everyone but when you re having orthodontic treatment, it s even more critical. Why? Because, while the appliances (such
Periodontal Screening and Scoring Of Patients Attended Periodontal Clinic of School Of Dentistry at University Of Sulaimani
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 8 Ver. I (Aug. 2015), PP 71-75 www.iosrjournals.org Periodontal Screening and Scoring Of Patients
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 8 Ver. I (Aug. 2015), PP 71-75 www.iosrjournals.org Periodontal Screening and Scoring Of Patients
Dental Research Journal
 Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Periodontal Maintenance
 Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Essentials of Periodontal Management in General Practice
 Essentials of Periodontal Management in General Practice Phil Ower MSc BDS MGDSRCS Specialist in Periodontics Briars Dental Centre, Newbury and www.periocourses.co.uk Introduction Effective management
Essentials of Periodontal Management in General Practice Phil Ower MSc BDS MGDSRCS Specialist in Periodontics Briars Dental Centre, Newbury and www.periocourses.co.uk Introduction Effective management
GOALS FOR THE PERIODONTAL PATIENT
 1 Goals for the Periodontal Patient: 1. Modify Risk Factors a. Overall goal is total health. b. Research shows that oral health is related to total health c. #1 preventable risk fact is tobacco use d.
1 Goals for the Periodontal Patient: 1. Modify Risk Factors a. Overall goal is total health. b. Research shows that oral health is related to total health c. #1 preventable risk fact is tobacco use d.
policy update bulletin
 November 2018 policy update bulletin Dental Clinical Policy & Coverage Guideline Updates UnitedHealthcare respects the expertise of the physicians, health care professionals, and their staff who participate
November 2018 policy update bulletin Dental Clinical Policy & Coverage Guideline Updates UnitedHealthcare respects the expertise of the physicians, health care professionals, and their staff who participate
Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease
 Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease Dental Caries The current understanding of the caries process supports the shift in caries management from a restorative-only
Examination and Treatment Protocols for Dental Caries and Inflammatory Periodontal Disease Dental Caries The current understanding of the caries process supports the shift in caries management from a restorative-only
