Five-Year Experience Comparing Resorbable to Titanium Miniplate Osteosynthesis in Cleft Lip and Palate Orthognathic Surgery
|
|
|
- Hugo Harrison
- 6 years ago
- Views:
Transcription
1 Five-Year Experience Comparing Resorbable to Titanium Miniplate Osteosynthesis in Cleft Lip and Palate Orthognathic Surgery Constantin A. Landes, M.D., D.M.D., Alexander Ballon, D.M.D. Objective: To evaluate 5-year outcome stability and complications in orthognathic surgery using resorbable versus titanium osteofixation. Patients, Methods: Twenty-two cleft lip and palate maxillary retrognathia cases were operated on using either poly (70L-lactide-co-30DL-lactide) or titanium miniplate osteofixation. All had two-piece Le Fort I maxillary advancement osteotomy, 11 had simultaneous mandibular setback, and 13 had alveolar bone grafts. Results: Average operative movement and postoperative instability recorded for maxillary horizontal movement (A-point-) were 2.5 mm and 2.1 mm for the study group, compared with 6.3 mm and 1.9 mm for the control group. For maxillary vertical movement (ANS-), measured values were 4.9 and mm for the study group and and 0.9 mm for the controls. For mandibular horizontal movement, measured values were 10.7 mm and 2.8 mm for the study group and 1.9 mm and mm for the controls. Gonial angle measures were 7.1 and 3.5 for the study group and 6.7 and 3.1 for the controls. Foreign body granuloma and fistulation occurred in 1 (9%) member of the study group, but was treated successfully with debridement; implant palpability subsided after 24 months. Three (27%) controls required plate removal, but the remaining plates were palpable. Conclusion: In the study group, horizontal maxillary stability appeared inferior to vertical stability, but mandibular stability was more reliable. Because groups were not matched for magnitude or direction of movement, the results of this study are preliminary and should be interpreted cautiously. KEY WORDS: maxillary retrognathia, midfacial hypoplasia, miniplate osteosynthesis, occlusal relapse, orthognathic surgery, poly (70L-lactideco-30DL-lactide), resorbable plates, skeletal relapse Le Fort I osteotomies became standard procedures during the last half of the 20th century and were definitive treatment for conditions such as vertical maxillary excess, midfacial hypoplasia, and anterior open-bite (Poole et al., 1986; Houston and James, 1989; Posnick and Ewing, 1990; Posnick and Tompson, 1995). In cleft lip and palate (CLP) patients, the basic etiology responsible for maxillary retrognathia and class III occlusion is the developmental embryological malformation of oral, palatal, and pharyngeal tissues, combined with scarring after surgical procedures (Adlam et al., 1989; Witzel, 1989; Hochban et al., 1993). Over the course of development, CLP patients also can develop abnormal structural relationships in the oral cavity due to the incomplete alveolar ridge and palate, Dr. Landes is Consultant and Dr. Ballon is Research Fellow, Department of Maxillofacial and Plastic Facial Surgery, Johann-Wolfgang Goethe University Medical Center, Frankfurt, Germany. Submitted November 2004; Accepted March Address correspondence to: Dr. Constantin A. Landes, Kiefer und Plastische Gesichtschirurgie, Haus 21 G, Theodor Stern Kai 7, Frankfurt am Main, Germany. c.landes@lycos.com. oronasal fistulae, a constricted maxillary arch, and crossbite. These structural abnormalities create a combination of specific problems found in CLP patients before orthognathic surgery. These factors may contribute to the difficulties in achieving a stable result (Witzel, 1989; Posnick and Taylor, 1994; Posnick, 2000). erative relapse is a known phenomenon in orthognathic surgery, and depending on its magnitude, may compromise the operative result. This phenomenon is more common in patients with CLP than in other patients with dento-facial deformities (Epker and Wolford, 1976; Freihofer, 1977; Champy, 1980). Plate-fixation and bone grafting to the osteotomy gap have therefore been recommended for better stability in maxillary advancements (Champy, 1980; Adlam et al., 1989; Posnick and Ewing, 1990; Posnick and Taylor, 1994). Resorbable plate osteosyntheses, frequently applied in otherwise dysgnathic collectives (Haers and Sailer, 1998; Edwards et al., 2001a, 2001b; Turvey et al., 2002; Laine et al., 2004) were reported only in a small previous sample that comprised CLP and other malformations with a 2-year follow-up (Landes and Kriener, 2003). These alternative osteosyntheses were not ap- 67
2 68 Cleft Palate Craniofacial Journal, January 2006, Vol. 43 No. 1 plied out of concern for pronounced relapses. The previous report (Landes and Kriener, 2003) neither differentiated relapse-patterns, dependent on operative movement direction and dimension, nor included a control group. The goal of this pilot study was to evaluate maxillary and mandibular stability in patients with CLP who had undergone resorbable fixation of maxillary and mandibular osteotomies. The outcomes were compared with those of a control group that had undergone a similar procedure with titanium fixation. PATIENTS AND METHODS This study compared preoperative, postoperative, and follow-up maxillary and mandibular craniofacial conformation in 22 dysgnathic CLP patients who required orthognathic surgery. All patients underwent maxillary advancement and some simultaneous mandibular setback between 1993 and All received preoperative and postoperative orthodontic treatment for several years. Nine individuals had left-sided unilateral CLP (UCLP), 4 had bilateral CLP (BCLP), and 9 had rightsided UCLP; none had isolated cleft palate or submucous cleft palate. The assignment for resorbable (study group) or titanium (control group) osteosynthesis after 1999, when resorbable implants were available, was exclusively patient-driven. It was mandatory to inform every patient of the two options and to allow a free decision. This approach was decided upon with our institution s board of ethics, because resorbables had proven reliable in other orthognathic surgery cases but were to be first applied to a pilot collective of dysgnathic CLP patients. All patients were thoroughly informed of the benefits (avoidance of metal exposure and removal) and risks (clinically apparent foreign body reaction, instability and relapse, or incomplete disintegration) of resorbable osteosyntheses. All patients except those with severe maxillary retrognathia ( 10-mm sagittal incisal distance) were invited to participate (beginning in 1999), but some preferred standard titanium. Only those patients who accepted the risks were treated with resorbable osteosyntheses; all others received standard titanium miniplates. All patients were available for follow-up; 12 were male (6 in each group) and 10 female (5 in each group). Patient ages ranged from 16 to 37 years at surgery. Eleven (50%) patients had two-piece Le Fort I maxillary advancement only, and 11 (50%) received simultaneous mandibular setback, according to occlusal and esthetic facial proportion. Nine patients received late alveolar bone grafting from resected mandibular cortex, four from the iliac crest. Resorbable Maxillary Osteosynthesis Resorbable maxillary osteosynthesis was accomplished with poly (70L-lactide-co-30DL-lactide) resorbable plates and 2- mm strong screws (3 patients: MacroSorb, MacroPore, San Diego, CA; 8 patients: PolyMax, Synthes, Oberdorf, Switzerland). The brand was changed due to availability problems when the first manufacturer changed distribution politics. Both brands have identical copolymer-basis, identical dimensions, tensile strength, and elastic modulus (see Claes et al., 1996). Alternatively, titanium miniplates and 2-mm strong screws (Leibinger-mini, Tuttlingen, Germany) were used. The operative procedure was performed with 4- to 6-hole L-plates paranasal and at the bilateral infrazygomatic crest, fixed to each segment with two to three 6-mm screws. Two-piece advancement in the study group was supported by an infranasal horizontal plate as a cross-brace with one or two 6-mm-long screws retaining the bone transplant (Fig. 1A through 1D). Mandibular osteosyntheses were fixed by a single plate, proximally with two to three 6-mm screws and distally with 8-mm screws. After the fifth patient, the protocol for mandibular osteosynthesis was changed. The revised protocol entailed the use of two plates rather than one. This change took place because the investigators had noted clinical instability in a different group of patients with dento-facial deformities who had undergone a similar procedure. No bone transplants will further bridge osteotomy gaps as these may falsify the retentive force evinced by the osteosyntheses. Simultaneous late alveolar bone-grafts may, however, be performed. Titanium-osteosynthesis Titanium-osteosynthesis was accomplished with the use of four 4-hole miniplates. The plates were placed at paranasal areas and infrazygomatic crests bilaterally, and fastened with 6-mm screws. MacroSorb included a battery-powered, sterile, single-use heating pen for local plate molding in situ. Sterile warming saline basins (55 C/131 F MacroSorb; 70 C/158 F PolyMax) were used to bend entire plates. These remained flexible for 5 to 7 seconds at glass temperature (50 C/125 F to 70 C/158 F). Burholes were drilled conventionally with a 2.0 mm-diameter burr, and a thread was tapped. Thread and screw diameter were 2.0 mm, plate thickness was 1.2 mm, and plate width was 6 mm. Though the PolyMax tap can be self-drilling in upper and midface craniofacial osteosyntheses, this did not work with the mandibular cortex. Titanium plates were plied for passive fit and fixated conventionally. Patients were left with a soft diet for 6 weeks. From the 7th week, all kinds of food that did not require intense mastication were allowed. No rigid intermaxillary fixation was applied. From the second postoperative day, two to four rubber bands were suspended between canine brackets over an occlusal wafer, to maintain guided occlusion for 4 weeks. Cephalometric analyses compared the preoperative craniofacial conformation (Burstone et al., 1978) with the postoperative situation, 6 months thereafter and every subsequent year (see Figs. 2 through 4). Standard landmarks (Sella,, Porion, Orbitale, Anterior Nasal Spine, Posterior Nasal Spine [the most dorsal projection from the bilateral hard-palate ending, due to absence of a spine and two-piece osteotomy a rather insecure landmark], A-point, B-point, Pogonion, Gnathion, Gonion, Articulare) were defined. For horizontal measurements, landmarks were projected perpendicular to the facial horizontal and their distances measured parallel to the facial horizontal in milli-
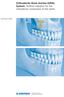
3 Landes and Ballon, RESORBABLE OSTEOSYNTHESES IN CLEFT-ASSOCIATED ORTHOGNATHIC SURGERY 69 FIGURE 1 A: Two-piece Le-Fort I advancement with four L-plates bridging the advancement gap at the anterior maxillary sinus wall, with an additional infranasal plate bridging the alveolar defect as a cross-brace in this BCLP situation that was considerably wider on the right side. On the left side, earlier alveolar grafting was successful and the alveolus is continuous. B: Another advancement, similar to 1A. An additional infranasal plate bridged the bilateral alveolar defect as a cross-brace in a wide BCLP situation. C: Identical situation with the transversal plate retaining bilateral cortical bone grafts. D: Lateral aspect of the patient in 1B and 1C showing the right osteosynthesis at the infrazygomatic crest before bone grafting to the alveolar defect. meters. Vertical measurements were performed from the specific landmark parallel to the facial vertical, perpendicular to the facial horizontal. All cephalometries were performed by the second author, who did not perform the surgery, to avoid observer bias. Retest reliability (absolute and relative error in intraindividual measurement) was assessed by having the second author measure all cephalograms twice in a single blind evaluation. The measurement averages were used for further calculation; 20 cephalograms were evaluated by both authors for interindividual absolute and relative error assessments. Effective operative maxillary horizontal movement was defined as the absolute difference between the pre- and postoperative A-point- distance. erative effective instability was assessed from the absolute difference between the followup and the postoperative value. This was done also for PNS- in the dorsal maxilla. For assessment of vertical maxillary movement (impaction or elongation), vertical ANS- and PNS- were used; for horizontal mandibular movement, B-point- and Pogonion- were used; and for change in intrinsic mandibular bend and postoperative assessment of the angular instability, Articulare-Gonion-Gnathion (Gonial angle) was used. All radiograms were made with the identical cephalostat (Phillips Medical Systems, The Netherlands). The analysis software used was OrthoPlan (Orthognathic Treatment Planner, Pacific Coast Software, Moreno Valley, CA) and spreadsheet analyses were performed with Excel RESULTS Eleven bimaxillary procedures (9 study, 2 control group) and 11 isolated Le Fort I osteotomies (9 control, 2 study group) have been followed. Intraindividual standard and relative errors in cephalometric analysis were 1.2 mm and 3.6%, respectively, whereas interindividual errors were 1.6 mm and 4.9%, respectively. Because transversal jaw rotation in lateral cephalograms is difficult to evaluate and does not lend itself to comprehensive data collection, jaw movements were reduced to four two-dimensional vectors. Operative movements for the study group are shown in Table 1, with corresponding values for the control group shown in Table 2.
4 70 Cleft Palate Craniofacial Journal, January 2006, Vol. 43 No. 1 FIGURE 2 Superpositioned serial cephalograms, oriented by anterior cranial base alignment. Although made with the identical equipment, superpositioning interferences and landmark definition insecurities prevailed. These come from minor posture differences, in spite of head-positioning accessories. Posterior nasal spine (PNS) served the projection of the dorsal hard palate margin. FIGURE 3 Superpositioned pre- and postoperative cephalogram-blueprint, with cephalometrics for orthognathic surgery-relevant landmarks (abbreviations), distances, and the outlined Frankfort horizontal. Adequate experience rendered the handling of templates and resorbables as uncomplicated as the bending of titanium miniplates. Unlike the conventional adaptation of titanium miniplates, no extra time was required. Though the resorbable plate diameter was bigger, wound closure was unproblematic and no periosteal incisions were necessary. Screws initially broke 5% of the time, when the thread was not completely cut or was cut oblique to the plate. If a screw head broke during the insertion due to overtightening, a new burhole and thread could be cut easily into the partly inserted screw body and a replacement screw could be tightened. Both systems provided 2.4-mm emergency screws. With three patients, resorbable osteosyntheses were fixed over an osteotomy gap of 5 to 10 mm due to bone elongation and loss of continuity in cortical bend. As an additional cross-brace between the alveolar segments, the infranasal plate proved practical to retain a late alveolar graft, as well. Follow-up ranged from 6 to 137 months (average 31 months). In the study group, radiographic follow-up was (range 6 to 50) months, and clinical follow-up was (range 6 to 62) months. In the control group, radiographic follow-up was (range 12 to 73) months, and clinical follow-up was (range 14 to 137) months. All patients were available for follow-up, but due to geographical mobility and patients schedules, recall was not always regularly possible. Thus, 100% of patients attended 1-year recall; 27%, 2- year recall; 45%, 5-year recall. Patients were radiographed a maximum of 4 times to minimize individual radiation exposure. Clinical examination always took place. All of the patients had pre- and postoperative radiographs; 50% were scheduled 6 months postoperatively; 50%, 1 year postoperatively; and 50% each subsequent year. The study group had absolute postoperative instability as shown in Table 1. Resorbable osteosyntheses appeared less stable in the anterior maxillary horizontal and dorsal maxillary vertical dimension. The dorsal horizontal, anterior vertical maxillary, and the mandibular resorbable fixation appeared more reliable. The control group s corresponding values are shown in Table 2. In the controls, the dorsal maxillary horizontal and vertical position were less reliable. Because PNS is an insecure landmark, the dorsal maxillary movements have to be interpreted with caution. The Pogonion- values were influenced by a genioplasty in four individuals. Foreign body reaction, swelling and fistulation occurred in one (9%) patient with resorbable osteosynthesis, but was successfully treated with curettage and debridement, and plate palpability subsided after 24 months. Titanium plate removal due to infection, palpability, and temperature sensitivity was required in 3 (27%) patients, but remaining plates were palpable at the end of follow-up. DISCUSSION This study evaluated, within a pilot collective, whether upto-date resorbables yield comparable or acceptable outcomes in segment stability when compared with the standard method. Patients with CLP and maxillary hypoplasia are known to have
5 Landes and Ballon, RESORBABLE OSTEOSYNTHESES IN CLEFT-ASSOCIATED ORTHOGNATHIC SURGERY 71 FIGURE 4 Preoperative view of the patient from Figures 2 and 3. A: Lateral. B: Frontal occlusion. C: Six-month postoperative lateral. D: Frontal occlusion. more postoperative relapses than other patients with Angle s Class III conditions. This is due to the scars produced by previous operations (Houston and James, 1989; Posnick and Ewing, 1990; Posnick and Tompson, 1995; Hirano and Suzuki, 2001). In spite of current advances in surgery and timing of orthodontics, maxillary hypoplasia cannot be avoided completely (Ross, 1987). Although resorbable osteosyntheses have been used in orthognathic surgery since 1991 (Laine et al., 2004), detailed study of segmental instability in orthognathic surgery of CLP patients has not been published (Landes and Kriener, 2003). Due to the limited number of patients, the authors were unable to create homogenous groups regarding BCLP or UCLP, age, sex, CLP width, or other similar variables. In spite of this, this small group of patients with CLP represents the typical distribution of patients regarding gender and cleft type
6 72 Cleft Palate Craniofacial Journal, January 2006, Vol. 43 No. 1 TABLE 1 Study Collective Dimension of Absolute Intraoperative Movement and erative ; Differences Between A-point and PNS Movement Come From Maxillary Rotation and Insecurity in PNS Definition; Differences Between B-point and Pg Come from Genioplasty* Gonial Angle ( ) Horizontal Mandibular Movement (mm) Vertical Maxillary Movement (mm) Horizontal Maxillary Movement (mm) Articulare- Gonion- Gnathion Pogonion- B-point- PNS- ANS- PNS- A-point- Patient Number Average *PNS Posterior Nasal Spine; Pg Pogonion; ANS Anterior Nasal Spine. and should allow the authors to obtain preliminary results regarding stability, biocompatibility, and possible untoward effects. Current resorbable osteofixations are made of copolymers, mainly poly L-lactide with poly DL-lactide or polyglycolide. Thus, crystallinity thought to cause very slow resorption and long-standing osteolyses (Suuronen et al., 1998; Kallela et al., 1999) is reduced. Concern regarding sufficient stability concentrated on mandibular osteofixation. In vitro (Maurer et al., 2002) and clinical reports of poly (70L-lactide-co-30DL-lactide), abbreviated P(L/DL)LA (Landes and Kriener, 2003; Laine et al., 2004), and poly (L-lactide-co-glycolide) or PLGA (Edwards et al., 2001) use demonstrated adequate stability without detailed postoperative stability analysis according to operative movement dimension and direction. This study, therefore, measured linear segmental millimeter movements. Although measurement technique is not perfectly comparable, Hirano and Suzuki (2001) advanced A-point 7 mm (range 2 to 13 mm), with a mean relapse of 1.5 mm (range, 7 mm backward relapse to 1.5 mm additional drift ; i.e., postoperative movement in the direction of operative positioning). Houston and James (1989), Hochban et al. (1993), and Posnick and Tompson (1995) reported similar results, emphasizing that instability is related to the magnitude and direction of the surgical movement. The current study group had 2.5 mm (range, to 5mm) A-point advancement and 2.1 mm average instability( 4 mm relapse to 3.8 mm drift), whereas the controls had 6.3 mm (1.4 to 11.6 mm) advancement with 1.9 mm mean instability ( 4.7 mm relapse to 3.8 mm drift). Hirano and Suzuki (2001) reported vertical operative A- point movement from 5 mm intrusion to 7 mm elongation, with 8 mm relapse to 2 mm drift. Resorbables in the current study had 4.9 mm ( 5.8 mm intrusion to 14.2 mm elongation) absolute vertical movement and mm average instability ( 6 to 2 mm), compared with the controls with mm ( 4.9 mm intrusion to 4.5 mm elongation) movement and 0.9 mm ( 0.9 to 3.4 mm) instability. Thus, maxillary advancement in resorbables was less stable than vertical elongation. Other dentofacial deformity samples using titanium osteosyntheses had 7 mm (Hoffmann and Brennan, 2004) and 10 mm (Waite et al., 1996) average maxillary advancement with less relapse: 0.7 to 1.8 mm. P(L/DL)LA osteosyntheses and mm average maxillary advancement (Haers and Sailer, 1998), with less postoperative instability ( mm), and mm average elongation, mm mean relapse, mm average impaction, and 1.2 mm additional intrusion. Similar maxillary advancements were osteosynthesized in vitro in identical manner with P(L/DL)LA (MacroSorb) plates upon polyurethane skulls; advancement gaps were not bridged (Araujo et al., 2001). Retrograde compressive relapse force was simulated by progressive loading through a material-testing machine and disclosed higher elastic resistance in the inferior-superior than the anterioposterior direction (i.e., compression after maxillary elongation was more stable than sagittal compression after advancement, as clinically seen within
7 Landes and Ballon, RESORBABLE OSTEOSYNTHESES IN CLEFT-ASSOCIATED ORTHOGNATHIC SURGERY 73 TABLE 2 Control Collective Dimension of Absolute Intraoperative Movement and erative ; Differences Between A-point and PNS Movement Come From Maxillary Rotation and Insecurity in PNS Definition; Differences Between B-point and Pg Come from Genioplasty* Gonial Angle ( ) Horizontal Mandibular Movement (mm) Vertical Maxillary Movement (mm) Horizontal Maxillary Movement (mm) Articulare- Gonion- Gnathion Pogonion- B-point- PNS- ANS- PNS- A-point- Patient Number Average *PNS Posterior Nasal Spine; Pg Pogonion; ANS Anterior Nasal Spine. this study). P(L/DL)LA revealed lower elastic stiffness compared to titanium, however, it provided adequate maxillary fixation to withstand the force of mastication, according to the authors. Bilateral double plates fixed with 2 to 3 screws in the anterior and posterior mandibular segment maintained reliable stability. In 7 resorbable mandibular osteofixations of 10.7 mm ( 23.4 mm to 4.7 mm) average operative movement at B- point, 2.8 mm ( 4 mm to 4.9 mm) instability occurred, comparable to previous reports in other dentofacial deformities mandibular setbacks (Mobarak et al., 2000); 2 controls with 2.7 mm and 1.2 mm movement did show 1.2 mm and mm relapse. P(L/DL)LA osteosyntheses in other dentofacial deformities (Haers and Sailer, 1998) showed after mm advancement at B-point mm instability. Because the resorbable and control groups were significantly different regarding the magnitude and direction of the surgical movement, differences between the groups regarding instability may be due to the differences in surgical movements. We tried to account for these differences by calculating the ratio between the instability and the surgical movement, but because the surgical movements were small for many patients, this ratio misrepresented a fairly stable clinical result; calculating ratios or percentages appeared inadequate. A statistical test could have been designed to compare instability between the groups while accounting for differences in surgical movement. One possible approach would have been to perform an analysis of covariance adjusting for pre- versus postoperative changes. Another approach would have been to assign a threshold creating two or three categories of surgical movements (e.g., minimal, moderate, large) and then to look at differences between these subgroups. Finally, another method would involve a nonparametric analysis of covariance. Although it might have been possible to develop such a test, the groups were so small that the result most likely would not have been valid. Therefore, only the absolute instability has been reported and the results of this study should be interpreted with caution, because the groups were not matched for such variables as magnitude or direction of movement, age, sex, UCLP, or BCLP. Freihofer (1977), Champy (1980), Houston and James (1989) and Hochban et al. (1993) suggest that sufficient mobilization, albeit scarring, from previous operations in the palate and retromaxillary region may be a preventive measure against relapse. Adequate mobilization and advance with little resistance that did not proportionally increase with the dimension of movement was intended, but maxillary rigidity could not be estimated preoperatively. In contrast to an alternative splint, if a planned advancement could not be reached with little resistance (Hirano and Suzuki, 2001), simultaneous mandibular setback was performed. High resistance was clinically considered to be overstrain to resorbable osteofixations, and therefore, the study group had more bimaxillary procedures. In a noncleft 10-year poly-l-lactide (abbreviated PLLA) and P(L/DL)LA review (Laine et al., 2004), 9% minor complications occurred, including infection (1%), insufficient fixation (2%), granuloma (3%), and fistulation with hyperplasic mu-
8 74 Cleft Palate Craniofacial Journal, January 2006, Vol. 43 No. 1 cosa that subsided after curettage. The current study had 1 (9%) case of foreign body granuloma, sufficiently treated with curettage, evincing sound osseous union upon inspection. Three (27%) controls had plate exposure, temperature sensitivity, or infection and had consecutive metal removal. Palpability of resorbable plates subsided after 2 years; titanium plates were palpable at the end of follow-up. Based upon the principle of orthognathic surgery improving maxillomandibular relationship and occlusion, 9 of 11 (82%) of both groups were clinical successes; 18% did not visibly improve, yet were content with the resulting incisal edge-toedge-occlusion. Hirano and Suzuki (2001) reported 4 (6%) cases, 2 BCLP and 2 UCLP, that relapsed. All had had bimaxillary surgery and relapsed within months; 3 were reoperated and later partially relapsed. Resorbable osteofixation permitted minor elastic jaw mobility up to 6 weeks postoperatively and allowed faster occlusal settling and potentially better condylar repositioning (Edwards et al., 2001; Norholt et al., 2004). Though the study group was small and a preliminary experience, the results encourage further evaluation in a bigger study for more definite instability assessment. Resorbable osteosynthesis horizontal maxillary stability appeared inferior to vertical stability and to other dysgnathic groups without CLP, whereas mandibular stability was more reliable. Because groups were not matched for magnitude or direction of movement, the results of this study should be interpreted with caution. Two-jaw surgery showed more effective relapse prevention, sound postoperative overbite, and better aesthetics. The earlier control group had more isolated Le Fort I osteotomies, whereas the recent study group had more bimaxillary procedures, reducing the direct compatibility of results, indicating a different clinical proceeding when resorbable plates are used, especially considering potential anterioposterior maxillary relapse. REFERENCES Adlam DM, Yau CK, Banks P. A retrospective study of the stability of midface osteotomies in cleft lip and palate patients. Br J Oral Maxillofac Surg. 1989; 27: Araujo MM, Waite PD, Lemons JE. Strength analysis of Le Fort I osteotomy fixation: titanium versus resorbable plates. J Oral Maxillofac Surg. 2001; 59: Burstone CJ, James RB, Legan H, Murphy GA, Norton LA. Cephalometrics for orthognathic surgery. J Oral Surg. 1978;36: Champy M. Surgical treatment of midface deformities. Head Neck Surg. 1980; 2: Claes LE, Ignatius AA, Rehm KE, Scholz C. New bioresorbable pin for the reduction of small bony fragments: design, mechanical properties and in vitro degradation. Biomaterials. 1996;17: Edwards RC, Kiely KD, Eppley BL. The fate of resorbable poly-l-lactic/polyglycolic acid (LactoSorb) bone fixation devices in orthognathic surgery. J Oral Maxillofac Surg. 2001a;59: Edwards RC, Kiely KD, Eppley BL. Fixation of bimaxillary osteotomies with resorbable plates and screws: experience in 20 consecutive cases. J Oral Maxillofac Surg. 2001b;59: Epker BN, Wolford LM. Middle-third facial osteotomies: the use in the correction of congenital dentofacial and craniofacial deformities. J Oral Surg. 1976;34: Freihofer HP. Results of osteotomies of the facial skeleton in adolescence. J Maxillofac Surg. 1977;5: Haers PE, Sailer HF. Biodegradable self reinforced poly-l/dl-lactide screws and plates in bimaxillary orthognathic surgery: short-term skeletal stability and material related failures. J Craniomaxillofac Surg. 1998;26: Hirano A, Suzuki H. Factors related to relapse after Le Fort I osteotomy in patients with cleft lip and palate. Cleft Palate Craniofac J. 2001;38:1 10. Hochban W, Ganss C, Austermann KH. Long-term results after maxillary advancements in patients with clefts. Cleft Palate Craniofac J. 1993;30: Hoffman GR, Brennan PA. The skeletal stability of one-piece Le Fort I osteotomy to advance the maxilla. Part I. Stability resulting from non bone grafted rigid fixation. Br J Oral Maxillofac Surg. 2004;42: Houston JB, James DR. Le Fort I maxillary osteotomies in cleft palate cases surgical changes and stability. J Craniomaxillofac Surg. 1989;17:9 15. Kallela I, Laine P, Suuronen R, Ranta P, Iizuka T, Lindqvist C. Osteotomy site healing following mandibular sagittal split osteotomy and rigid fixation with polylactide biodegradable screws. Int J Oral Maxillofac Surg. 1999;28: Laine P, Kontio R, Lindqist C, Suuronen R. Are there any complications with bioabsorbable fixation devices? A 10-year review in orthognathic surgery. Int J Oral Maxillofac Surg. 2004;33: Landes CA, Kriener S. Resorbable plate osteosynthesis of sagittal split osteotomies with major bone movement. Plast Reconstr Surg. 2003;111: Maurer P, Holweg S, Knoll WD, Schubert J. Study by finite element method of the mechanical stress of selected biodegradable osteosynthesis screws in sagittal ramus osteotomy. Br J Oral Maxillofac Surg. 2002;40: Mobarak KA, Krogstad O, Espeland L, Lyberg T. Long-term stability of mandibular setback surgery: a follow-up of 80 bilateral sagittal split osteotomy patients. Int J Adult Orthod Orthognath Surg. 2000;15: Norholt SE, Pedersen TK, Jensen J. Le Fort I miniplate osteosynthesis: a randomized, prospective study comparing resorbable PLLA/PGA with titanium. Int J Oral Maxillofac Surg. 2004;3: Poole MD, Robinson PR, Nunn ME. Maxillary advancement in cleft palate patients a modification of the Le Fort I osteotomy and preliminary results. J Maxillofac Surg. 1986;14: Posnick JC. The staging of cleft lip and palate reconstruction Infancy through adolescence. In: Posnick JC, ed. Craniofacial and Maxillofacial Surgery in Children and Young Adults. St. Louis: Elsevier; 2000: Posnick JC, Ewing MP. Skeletal stability after Le Fort I maxillary advancement in patients with unilateral cleft lip and palate. Plast Reconstr Surg. 1990; 85: Posnick JC, Taylor M. Skeletal stability and relapse patterns after Le fort I osteotomy using miniplate fixation in patients with isolated cleft palate. Plast Reconstr Surg. 1994;94: Posnick JC, Tompson B. Cleft-orthognathic surgery complications and longterm results. Plast Reconstr Surg. 1995;96: Ross RB. Treatment variables affecting facial growth in complete unilateral cleft lip and palate. Part 7: an overview of treatment and facial growth. Cleft Palate J. 1987;24: Suuronen R, Pohjonen T, Hietanen J, Lindquist C. A 5-year in vitro and in vivo study of the biodegradation of polylactide plates. J Oral Maxillofac Surg. 1998;56: Turvey TA, Bell RB, Tejera TJ, Proffit WR. The use of self-reinforced biodegradable bone plates and screws in orthognathic surgery. J Oral Maxillofac Surg. 2002;60: Waite PD, Tejera TJ, Anucul B. The stability of maxillary advancement using Le Fort I osteotomy with and without genial bone grafting. Int J Oral Maxillofac Surg. 1996;25: Witzel M. The effects of Le Fort I osteotomy with maxillary movement on articulation, resonance, and velopharyngeal function. Cleft Palate J. 1989; 26:199.
The Skeletal Stability of Maxillary Advancement in Combination with Bilateral Sagittal Split Ramus Osteotomy. Mohamed Diaa Z.
 The Skeletal Stability of Maxillary Advancement in Combination with Bilateral Sagittal Split Ramus Osteotomy Mohamed Diaa Z. Ismail Associate Professor of Oral and Maxillofacial Surgery, Faculty of Dentistry,
The Skeletal Stability of Maxillary Advancement in Combination with Bilateral Sagittal Split Ramus Osteotomy Mohamed Diaa Z. Ismail Associate Professor of Oral and Maxillofacial Surgery, Faculty of Dentistry,
RapidSorb Resorbable Tacks. Resorbable Fixation System.
 RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Patients with cleft lip and palate (CLP) usually
 Comparison of Treatment Outcome and Stability Between Distraction Osteogenesis and LeFort I Osteotomy in Cleft Patients With Maxillary Hypoplasia Seung-Hak Baek, DDS, MSD, PhD,* Jin-Kyung Lee, DDS, 1 Jong-Ho
Comparison of Treatment Outcome and Stability Between Distraction Osteogenesis and LeFort I Osteotomy in Cleft Patients With Maxillary Hypoplasia Seung-Hak Baek, DDS, MSD, PhD,* Jin-Kyung Lee, DDS, 1 Jong-Ho
Changes in soft tissue thickness after Le Fort I osteotomy in different cleft types
 Arja Heliövaara, DDS, PhD Orthodontist Jyri Hukki, MD, PhD Senior Consultant in Plastic Surgery Reijo Ranta, DDS, PhD Docent and Senior Orthodontist Aarne Rintala, MD, PhD Assistant Professor of Plastic
Arja Heliövaara, DDS, PhD Orthodontist Jyri Hukki, MD, PhD Senior Consultant in Plastic Surgery Reijo Ranta, DDS, PhD Docent and Senior Orthodontist Aarne Rintala, MD, PhD Assistant Professor of Plastic
Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients
 Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS
 POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY
 PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
PREDICTING LOWER LIP AND CHIN RESPONSE TO MANDIBULAR ADVANCEMENT WITH GENIOPLASTY A CEPHALOMETRIC STUDY Dr. Deepthi T. Amanna Authors : Dr. Deepthi T. Amanna Assistant Professor Dr. E.T. Roy Professor
The use of a LeFort I osteotomy to correct
 ORIGINAL ARTICLE LeFort I maxillary advancement: 3-year stability and risk factors for relapse Paul A. Dowling, a Lisen Espeland, b Leiv Sandvik, c Karim A. Mobarak, d and Hans Erik Hogevold e Dublin,
ORIGINAL ARTICLE LeFort I maxillary advancement: 3-year stability and risk factors for relapse Paul A. Dowling, a Lisen Espeland, b Leiv Sandvik, c Karim A. Mobarak, d and Hans Erik Hogevold e Dublin,
Advances in skeletal stabilization techniques have
 ORIGINAL ARTICLE Comparison of titanium and resorbable copolymer fixation after Le Fort I maxillary impaction Walinder S. Dhol, a Johan P. Reyneke, b Bryan Tompson, c and George K. B. Sándor d Johannesburg,
ORIGINAL ARTICLE Comparison of titanium and resorbable copolymer fixation after Le Fort I maxillary impaction Walinder S. Dhol, a Johan P. Reyneke, b Bryan Tompson, c and George K. B. Sándor d Johannesburg,
Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy
 Original Article Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy M. Bayat 1,2, M. Ja'farian 3, O. Ghassemi Habashi 4 1 Assistant Professor, Department
Original Article Correlation between Gonial Angle and Different Variables after Bilateral Sagittal Split Ramus Osteotomy M. Bayat 1,2, M. Ja'farian 3, O. Ghassemi Habashi 4 1 Assistant Professor, Department
UNCORRECTED PROOF. G.R. Hoffman a,1, P.A. Brennan b,c, * Introduction. Patients and methods 40
 British Journal of Oral and Maxillofacial Surgery (2004) xxx, xxx xxx The skeletal stability of one-piece Le Fort 1 osteotomy to advance the maxilla Part 2. The influence of uncontrollable clinical variables
British Journal of Oral and Maxillofacial Surgery (2004) xxx, xxx xxx The skeletal stability of one-piece Le Fort 1 osteotomy to advance the maxilla Part 2. The influence of uncontrollable clinical variables
MAHP Orthognathic Surgery Guidelines. Medical Policy Statement. Criteria
 Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system
 J Med Dent Sci 2004; 51: 27 33 Original Article Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system Eduardo Yugo Suzuki, Nobuyoshi Motohashi
J Med Dent Sci 2004; 51: 27 33 Original Article Longitudinal dento-skeletal changes in UCLP patients following maxillary distraction osteogenesis using RED system Eduardo Yugo Suzuki, Nobuyoshi Motohashi
Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report
 Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Case Report Ortho-surgical Management of Severe Vertical Dysplasia: A Case Report 1 Vinni Arora, 2 Rekha Sharma, 3 Sachin Parashar 1 Senior Resident, 2 Professor and Head of Department, 3 Former Resident
Surgical Treatment of the Nasal-Maxillary Complex in Adolescents With Cleft Lip and Palate
 Surgical Treatment of the Nasal-Maxillary Complex in Adolescents With Cleft Lip and Palate Fernando D. Burstein MD, FACS, FAAP Atlanta, Georgia, USA Rather than treating nasal, maxillary, and soft tissue
Surgical Treatment of the Nasal-Maxillary Complex in Adolescents With Cleft Lip and Palate Fernando D. Burstein MD, FACS, FAAP Atlanta, Georgia, USA Rather than treating nasal, maxillary, and soft tissue
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM. A new resorbable approach to Alveolar bone augmentation
 RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM A new resorbable approach to Alveolar bone augmentation RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM Bone Graft Containment The RapidSorb Rapid Resorbable Fixation
RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM A new resorbable approach to Alveolar bone augmentation RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM Bone Graft Containment The RapidSorb Rapid Resorbable Fixation
Stability and Relapse in Orthognathic Surgery
 Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
Stability and Relapse in Orthognathic Surgery Neeraj Panchal, DDS, MD, MA Christine Ellis, DDS, MSD Paul Tiwana, DDS, MD, MS, FACS INTRODUCTION The long-term success of orthognathic reconstructive surgery
Stability of maxillary advancement using rigid fixation and porous-block hydroxyapatite grafting: Cleft palate versus non-cleft patients
 Pushkar Mehra, BDS, DMD Formerly,Fellow Oral and Maxillofacial Currently, Assistant Professor Oral and Maxillofacial Boston University School of Dental Medicine Director Boston Medical Center Boston, Massachusetts
Pushkar Mehra, BDS, DMD Formerly,Fellow Oral and Maxillofacial Currently, Assistant Professor Oral and Maxillofacial Boston University School of Dental Medicine Director Boston Medical Center Boston, Massachusetts
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Original Research. This appraisal is based on a system of cephalometric analysis that was developed at Indiana University by Burstone and Legan.
 Received: 08 th June 2015 Accepted: 13 th September 2015 Conflicts of Interest: None Source of Support: Nil Original Research Hard Tissue Cephalometric Norms for Orthognathic Surgery in Karnataka Population
Received: 08 th June 2015 Accepted: 13 th September 2015 Conflicts of Interest: None Source of Support: Nil Original Research Hard Tissue Cephalometric Norms for Orthognathic Surgery in Karnataka Population
Postoperative Evaluation on SSRO performed by Short Lingual Osteotomy and IVRO
 140 J Meikai Dent Med 43 2, 140 147, 2014 Short Lingual Osteotomy SSRO IVRO 1 1 1 1 1 1 2 2 1 2 1 1 2 SSRO SSRO IVRO SSRO short lingual osteotomy SL SL IVRO SL 4 6 IVRO SL IVRO SL 1 IVRO SL short lingual
140 J Meikai Dent Med 43 2, 140 147, 2014 Short Lingual Osteotomy SSRO IVRO 1 1 1 1 1 1 2 2 1 2 1 1 2 SSRO SSRO IVRO SSRO short lingual osteotomy SL SL IVRO SL 4 6 IVRO SL IVRO SL 1 IVRO SL short lingual
How predictable is orthognathic surgery?
 European Journal of Orthodontics 26 (2004) 303 309 European Journal of Orthodontics vol. 26 no. 3 European Orthodontic Society 2004; all rights reserved. How predictable is orthognathic surgery? Charlotte
European Journal of Orthodontics 26 (2004) 303 309 European Journal of Orthodontics vol. 26 no. 3 European Orthodontic Society 2004; all rights reserved. How predictable is orthognathic surgery? Charlotte
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis
 Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Orthognathic treatment of facial asymmetry due to temporomandibular joint ankylosis Ayse Gulsen 1, Serhat Sibar 2, Selahattin Ozmen 3 1 Department of Plastic, Reconstructive, and Aesthetic Surgery, Gazi
Technique Guide. Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Suuronen R, Pohjonen T, Hietanen J. A 5-year in vitro and in vivo study of biodegradation of polylactide plates J Oral Maxillofac Surg 56:604, 1998
 Reabsorbible J. Hoffmann, C. Adam, D. Troitzsch, S. Reinert Bioresorbable Fixation in Craniomaxillofacial Surgery, Poster Cutright DE, Hunsuck EE, Beasley JD Fracture reduction using a biodegradable material,
Reabsorbible J. Hoffmann, C. Adam, D. Troitzsch, S. Reinert Bioresorbable Fixation in Craniomaxillofacial Surgery, Poster Cutright DE, Hunsuck EE, Beasley JD Fracture reduction using a biodegradable material,
Topic: Orthognathic Surgery Date of Origin: October 5, Section: Surgery Last Reviewed Date: December 2013
 Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Orthognathic Surgery Date of Origin: October 5, 2004 Section: Surgery Last Reviewed Date: December 2013 Policy No: 137 Effective Date: March 1, 2014 IMPORTANT REMINDER Medical
Orthodontics-surgical combination therapy for Class III skeletal malocclusion
 [Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
[Downloaded free from http://www.contempclindent.org on Tuesday, July 16, 2013, IP: 164.100.31.82] Click here to download free Android application for this jou Orthodontics-surgical combination therapy
Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures
 Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Treatment of severe unilateral open bite and crossbite in cleft lip and palate patients
 European Journal of Orthodontics 6 (1984) 294-3(12 1984 European Orthodontic Society Treatment of severe unilateral open bite and crossbite in cleft lip and palate patients Hans Enemark Aarhus, Denmark
European Journal of Orthodontics 6 (1984) 294-3(12 1984 European Orthodontic Society Treatment of severe unilateral open bite and crossbite in cleft lip and palate patients Hans Enemark Aarhus, Denmark
Original Research. Figure 1: (a) Unilateral complete cleft of the lip and palate, (b) unilateral complete skeletal cleft with a Simonart s band.
 Received: 14 th August 2015 Accepted: 19 th November 2015 Conflicts of Interest: None Source of Support: Nil Original Research Simonart s Bands and Facial Growth in Unilateral Cleft Lip and Palate Patients:
Received: 14 th August 2015 Accepted: 19 th November 2015 Conflicts of Interest: None Source of Support: Nil Original Research Simonart s Bands and Facial Growth in Unilateral Cleft Lip and Palate Patients:
DISTRACTION PRODUCT OVERVIEW. For a wide variety of facial applications
 DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery
 University of Connecticut DigitalCommons@UConn SoDM Masters Theses School of Dental Medicine June 1991 Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery Gregory A. Hack
University of Connecticut DigitalCommons@UConn SoDM Masters Theses School of Dental Medicine June 1991 Long Term Stability and Prediction of Soft Tissue Changes Following LeFort I Surgery Gregory A. Hack
Bio-degradable osteosynthesis system in treatment of mandibular parasymphysis fractures
 Al Am een J Med Sci 2012; 5(4): 371-375 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Bio-degradable osteosynthesis system in treatment of mandibular
Al Am een J Med Sci 2012; 5(4): 371-375 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Bio-degradable osteosynthesis system in treatment of mandibular
Surgically assisted rapid palatal expansion (SARPE) prior to combined Le Fort I and sagittal osteotomies: A case report
 200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
200 Carlos Alberto E. Tavares, DDS, MS, DOrth Professor Department of Orthodontics Associação Brasileira de Odontologia - RS Porto Alegre, Brazil Miguel Scheffer, DDS, MS Chairman Department of Oral and
Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy
 Original Article Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy H. Mohajerani 1, M. Mehdizadeh 2, A. Khalighi Sigaroodi 3 1 Assistant Professor,
Original Article Skeletal Relapse after Correction of Mandibular Prognathism by Bilateral Sagittal Split Ramus Osteotomy H. Mohajerani 1, M. Mehdizadeh 2, A. Khalighi Sigaroodi 3 1 Assistant Professor,
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
AESTHETIC ORTHOGNATHIC SURGERY
 c0435 ESTHETIC ORTHOGNTHIC SURGERY Stephen. aker, MD, DDS, and Harvey Rosen, MD, DMD CHPTER 87 s0010 p0010 s0020 p0015 s0025 p0020 s0030 p0025 s0035 p0030 s0040 p0035 s0045 p0040 1. What is orthognathic
c0435 ESTHETIC ORTHOGNTHIC SURGERY Stephen. aker, MD, DDS, and Harvey Rosen, MD, DMD CHPTER 87 s0010 p0010 s0020 p0015 s0025 p0020 s0030 p0025 s0035 p0030 s0040 p0035 s0045 p0040 1. What is orthognathic
Inion CPS. Biodegradable Fixation System. Product Overview
 Inion CPS Biodegradable Fixation System Product Overview Material advantage What are the Inion biodegradable implants made from? All Inion CPS implants are based on Inion biodegradable polymer blends and
Inion CPS Biodegradable Fixation System Product Overview Material advantage What are the Inion biodegradable implants made from? All Inion CPS implants are based on Inion biodegradable polymer blends and
Cleft Lip and Palate: The Effects on Speech and Resonance
 Ann W. Kummer, PhD, CCC-SLP Cincinnati Children s Cleft lip and/or palate can have a negative impact on both speech and resonance. The following is a summary of normal anatomy, the types and causes of
Ann W. Kummer, PhD, CCC-SLP Cincinnati Children s Cleft lip and/or palate can have a negative impact on both speech and resonance. The following is a summary of normal anatomy, the types and causes of
Class II. Bilateral Cleft Lip and Palate. Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Cleft Lip and Palate.
 Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
For over 30 years, orthognathic surgery has
 ORIGINAL ARTICLE The predictability of maxillary repositioning in LeFort I orthognathic surgery Ron Jacobson, DDS, MS, a and David M. Sarver, DMD, MS b Chicago, Ill, and Birmingham, Ala Our ability to
ORIGINAL ARTICLE The predictability of maxillary repositioning in LeFort I orthognathic surgery Ron Jacobson, DDS, MS, a and David M. Sarver, DMD, MS b Chicago, Ill, and Birmingham, Ala Our ability to
ORAL AND CRANIOFACIAL CHARACTERISTICS OF UNTREATED ADULT UNILATERAL CLEFT LIP AND PALATE INDIVIDUALS
 Short Communication ORAL AND CRANIOFACIAL CHARACTERISTICS OF UNTREATED ADULT UNILATERAL CLEFT LIP AND PALATE INDIVIDUALS M. S. Ravi Professor, Dept. of Orthodontics, A. B. Shetty Memorial Institute of
Short Communication ORAL AND CRANIOFACIAL CHARACTERISTICS OF UNTREATED ADULT UNILATERAL CLEFT LIP AND PALATE INDIVIDUALS M. S. Ravi Professor, Dept. of Orthodontics, A. B. Shetty Memorial Institute of
Mixed-reality simulation for orthognathic surgery
 Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Fushima and Kobayashi Maxillofacial Plastic and Reconstructive Surgery (2016) 38:13 DOI 10.1186/s40902-016-0059-z METHODOLOGY Mixed-reality simulation for orthognathic surgery Kenji Fushima 1* and Masaru
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion
 Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
Dental Medicine Research 30 2) 161 166, 2010 161 Case Report Orthodontic and Orthognathic Surgical Correction of a Skeletal Class III Malocclusion Tetsutaro Yamaguchi, Yoko Tomoyasu, Tatsuo Shirota*, Masashi
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob
 University of Groningen Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
University of Groningen Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy
 1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
Chapter 2. Material and methods
 Chapter 2 Material and methods Material and methods Summary This chapter describes the subjects and methods being used in this study. Between 1986 and 1997 9 expeditions were undertaken in remote areas
Chapter 2 Material and methods Material and methods Summary This chapter describes the subjects and methods being used in this study. Between 1986 and 1997 9 expeditions were undertaken in remote areas
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area.
 Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
New innovations in craniomaxillofacial fixation: the 2.0 lock system
 LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
Stability after Mandibular Advancement using Bilateral Sagittal Split Osteotomy
 Stability after Mandibular Advancement using Bilateral Sagittal Split Osteotomy Authors Erica Larsson Ellinore Jacobsson Tutors Mats Sjöström Jan Ahlqvist ABSTRACT The bilateral sagittal split osteotomy
Stability after Mandibular Advancement using Bilateral Sagittal Split Osteotomy Authors Erica Larsson Ellinore Jacobsson Tutors Mats Sjöström Jan Ahlqvist ABSTRACT The bilateral sagittal split osteotomy
SURGICAL MODEL ACCURACY DEVICE. 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution
 SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
SURGICAL MODEL ACCURACY DEVICE 25 years - manufacturing and distribution - around the globe research - design - manufacturing - distribution 2 SMAD - SURGICAL MODEL ACCURACY DEVICE SMAD has be designed
Midline Mandibular Osteotomy in an Asymmetric Patient
 Case Report Midline Mandibular Osteotomy in an Asymmetric Patient M. L. Anghinoni a ; A. S. Magri b ; A. Di Blasio c ; L. Toma d ; E. Sesenna e ABSTRACT This case report shows the possibility of the application
Case Report Midline Mandibular Osteotomy in an Asymmetric Patient M. L. Anghinoni a ; A. S. Magri b ; A. Di Blasio c ; L. Toma d ; E. Sesenna e ABSTRACT This case report shows the possibility of the application
Maxillary Growth Control with High Pull Headgear- A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 01 Ver. X January. (2018), PP 09-13 www.iosrjournals.org Maxillary Growth Control with High
A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery.
 SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
/aedj EVALUATION OF THE CHANGES IN THE SOFT AND HARD TISSUE PROFILE AFTER ANTERIOR SEGMENTAL OSTEOTOMY OF MAXILLA AND MANDIBLE.
 10.5368/aedj.2017.9.3.1.4 EVALUATION OF THE CHANGE IN THE OFT AND HARD TIUE PROFILE AFTER ANTERIOR EGMENTAL OTEOTOMY OF MAXILLA AND MANDIBLE. 1 sudhakar Gudipalli 2 urekha.k 3 Anil Budumuru 4 Praveen Peramulla
10.5368/aedj.2017.9.3.1.4 EVALUATION OF THE CHANGE IN THE OFT AND HARD TIUE PROFILE AFTER ANTERIOR EGMENTAL OTEOTOMY OF MAXILLA AND MANDIBLE. 1 sudhakar Gudipalli 2 urekha.k 3 Anil Budumuru 4 Praveen Peramulla
Surgical technique. IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
 Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital,
 Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Technique Guide. Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth.
 Technique Guide Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth. Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and
Technique Guide Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth. Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults
 Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
Evaluation of maxillary protrusion malocclusion treatment effects with prosth-orthodontic method in old adults Peicheng Xu, DDS, MSD, a and Honghu Liu, DDS, PhD b a Shanghai Xuhui Dental Hospital and b
Orthognathic surgery for a patient with trichorhinophalangeal syndrome type I: A case report
 Orthognathic surgery for a patient with trichorhinophalangeal syndrome type I: A case report Kentaro Kunimori, DDS, a Kiyoshi Harada, DDS, PhD, b Yutaka Maruoka, DDS, PhD, c and Ken Omura, DDS, PhD, d
Orthognathic surgery for a patient with trichorhinophalangeal syndrome type I: A case report Kentaro Kunimori, DDS, a Kiyoshi Harada, DDS, PhD, b Yutaka Maruoka, DDS, PhD, c and Ken Omura, DDS, PhD, d
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Medartis Product Overview MODUS
 Medartis Product Overview MODUS Content 3 Clinical Benefits MODUS 4 5 Technology 6 Clip System 7 0.9 / 1.2, Trauma 0.9 / 1.2 8 1.5, Trauma 1.5 9 Orbital Plating System OPS 1.5 9 Neuro 1.5 10 Trauma 2.0
Medartis Product Overview MODUS Content 3 Clinical Benefits MODUS 4 5 Technology 6 Clip System 7 0.9 / 1.2, Trauma 0.9 / 1.2 8 1.5, Trauma 1.5 9 Orbital Plating System OPS 1.5 9 Neuro 1.5 10 Trauma 2.0
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch
 Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
Case Report An Adult Case of Skeletal Open Bite with a Severely Narrowed Maxillary Dental Arch Michiru Takeuchi, DDS a ; Eiji Tanaka, DDS, PhD b ; Daisuke Nonoyama, DDS c ; Junko Aoyama, DDS d ; Kazuo
Author(s) Fujimura, Kazuma; Bessho, Kazuhisa.
 Title Rigid fixation of intraoral mandibular prognathism. vertico Author(s) Fujimura, Kazuma; Bessho, Kazuhisa Citation Journal of oral and maxillofacial s 1173 Issue Date 2012-05 URL http://hdl.handle.net/2433/155855
Title Rigid fixation of intraoral mandibular prognathism. vertico Author(s) Fujimura, Kazuma; Bessho, Kazuhisa Citation Journal of oral and maxillofacial s 1173 Issue Date 2012-05 URL http://hdl.handle.net/2433/155855
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis CASE REPORT
 Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
Effects of different surgical procedures on the pharyngeal space with mandibular prognathism
 J Osaka Dent Univ 2015 (October) ; 49 (2) : 143 148. Effects of different surgical procedures on the pharyngeal space with mandibular prognathism Yutaka Yamada and Naoyuki Matsumoto Department of Orthodontics,
J Osaka Dent Univ 2015 (October) ; 49 (2) : 143 148. Effects of different surgical procedures on the pharyngeal space with mandibular prognathism Yutaka Yamada and Naoyuki Matsumoto Department of Orthodontics,
UCL Repair: Emphasis on Muscle Dissection and Reconstruction
 UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures.
 Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures. Surgical Technique MR Safe Radiolucent Table of Contents System Description 3 Indications and Contraindications 4 Fixation Components
Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures. Surgical Technique MR Safe Radiolucent Table of Contents System Description 3 Indications and Contraindications 4 Fixation Components
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Postoperative mandibular stability after orthognathic surgery in patients with mandibular protrusion and mandibular deviation
 Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Wenli Lai, DDS, PhD Lecturer Department of Orthodontics West China College of Stomatology Sichuan University Chengdu, China Kazuhiro Yamada, DDS, PhD Lecturer Division of Orthodontics Department of Oral
Low Profile Neuro Plating System. Surgical Technique
 Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Intraoperative measurement of maxillary repositioning in a series of 30 patients with maxillomandibular vertical asymmetries
 Giancarlo Renzi, MD Andrea Carboni, MD Maurizio Perugini, MD Fellow Maxilllofacial Surgery Department University La Sapienza Rome, Italy Roberto Becelli, PhD, MDS Professor Maxillofacial Surgery Teaching
Giancarlo Renzi, MD Andrea Carboni, MD Maurizio Perugini, MD Fellow Maxilllofacial Surgery Department University La Sapienza Rome, Italy Roberto Becelli, PhD, MDS Professor Maxillofacial Surgery Teaching
Bioabsorbable osteofixation for orthognathic surgery
 Park Maxillofacial Plastic and Reconstructive Surgery (2015) 37:6 DOI 10.1186/s40902-015-0003-7 REVIEW Bioabsorbable osteofixation for orthognathic surgery Young-Wook Park Open Access Abstract Orthognathic
Park Maxillofacial Plastic and Reconstructive Surgery (2015) 37:6 DOI 10.1186/s40902-015-0003-7 REVIEW Bioabsorbable osteofixation for orthognathic surgery Young-Wook Park Open Access Abstract Orthognathic
Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient
 Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
 Evaluation of the maxillary morphological changes following distraction in CLP patients decrease in the Ul to NF except for Case 6. me [35] instance,血e small maxillary advancement of 2.4 mm and maxillary
Evaluation of the maxillary morphological changes following distraction in CLP patients decrease in the Ul to NF except for Case 6. me [35] instance,血e small maxillary advancement of 2.4 mm and maxillary
Technique Guide Small Bone Fusion System
 Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
KJLO. A Sequential Approach for an Asymmetric Extraction Case in. Lingual Orthodontics. Case Report INTRODUCTION DIAGNOSIS
 KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
KJLO Korean Journal of Lingual Orthodontics Case Report A Sequential Approach for an Asymmetric Extraction Case in Lingual Orthodontics Ji-Sung Jang 1, Kee-Joon Lee 2 1 Dream Orthodontic Clinic, Gimhae,
DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI Page 1 Page 2 rigid fixation for maxillofacial surgery rigid fixation for maxillofacial pdf rigid fixation for maxillofacial
DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI Page 1 Page 2 rigid fixation for maxillofacial surgery rigid fixation for maxillofacial pdf rigid fixation for maxillofacial
CLEFT LIP and PALATE. Sahlgrenska University Hospital Göteborg, Sweden. Information about Cleft Lip and Palate. English version
 CLEFT LIP and PALATE Sahlgrenska University Hospital Göteborg, Sweden Information about Cleft Lip and Palate English version 1 TABLE OF CONTENTS page What are cleft lip and palate? 3 Which children can
CLEFT LIP and PALATE Sahlgrenska University Hospital Göteborg, Sweden Information about Cleft Lip and Palate English version 1 TABLE OF CONTENTS page What are cleft lip and palate? 3 Which children can
Maxillary Advancement Surgery and Nasolabial Soft Tissue Changes
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. VIII (March. 2017), PP 23-29 www.iosrjournals.org Maxillary Advancement Surgery and
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 3 Ver. VIII (March. 2017), PP 23-29 www.iosrjournals.org Maxillary Advancement Surgery and
