abutment, Zirconia abutment
|
|
|
- Joleen Rosamund Porter
- 6 years ago
- Views:
Transcription
1 Alberto Sicilia Marc Quirynen Alain Fontolliet Helena Francisco Anton Friedman Tomas Linkevicius Rainer Lutz Henny J. Meijer Eric Rompen Roberto Rotundo Frank Schwarz Massimo Simion Wim Teughels Ann Wennerberg Otto Zuhr Long-term stability of peri-implant tissues after bone or soft tissue augmentation. Effect of zirconia or titanium abutments on peri-implant soft tissues. Summary and consensus statements. The 4th EAO Consensus Conference 2015 Authors affiliations: Alberto Sicilia, University of Oviedo, Oviedo, Spain Marc Quirynen, Wim Teughels, Catholic University of Leuven, Leuven University Hospital, Leuven, Belgium Alain Fontolliet, University of Zurich, Zurich, Switzerland Helena Francisco, University of Lisbon, Lisbon, Portugal Anton Friedman, Witten-Herdecke University, Witten, Germany Tomas Linkevicius, University of Vilnius, Vilnius, Lithuania Rainer Lutz, University of Erlangen-Nuremberg, Erlangen, Germany Henny J. Meijer, University of Groningen, Groningen, Netherlands Eric Rompen, University of Liege, Liege, Belgium Roberto Rotundo, University of Florence, Florence, Italy Frank Schwarz, Heinrich Heine University, D usseldorf, Germany Massimo Simion, University of Milan, Milan, Italy Ann Wennerberg, University of Malm o, Malm o, Sweden Otto Zuhr, Private Practice in Munich, University of Frankfurt, Frankfurt, Germany *Corresponding author: Alberto Sicilia University of Oviedo. Faculty of Medicine and Health Sciences University Clinic of Dentistry, Section of Periodontology Catedratico Jose Serrano sn Oviedo, Spain asicilia@clinicasicilia.es Key words: hard tissue augmentation, peri-implant tissues, soft tissue augmentation, titanium abutment, Zirconia abutment Abstract Introduction: Several surgical techniques and prosthetic devices have been developed in the last decades, aiming to improve aesthetic, hygienic and functional outcomes that may affect the periimplant tissues, such as procedures of bone and soft tissue augmentation and the use of custommade abutments of titanium and zirconium. Materials and methods: Three systematic reviews, based on randomized clinical trials and prospective studies covering the above reported topics were analysed, and the detected evidence was exposed to interactive experts discussion during the group s and general assembly s meetings of the 4th EAO Consensus Conference. The results are reported using the following abbreviations: S- T: short-term evidence, M-T: medium-term evidence; L-T: long-term evidence; LE: limited evidence. Results: Soft tissue augmentation procedures may be indicated for the increase of soft tissue thickness and keratinized tissue, the reduction of interproximal peri-implant bone loss, and the coverage of shallow peri-implant soft tissue recessions (S-T, LE), L-T is lacking. Guided bone regeneration approaches (GBR) showed efficacy when used for ridge reconstruction after the complete healing of the soft tissues (S-T & L-T), and the stability of the augmented bone may play a role in the maintenance of the soft tissue position and dimensions (LE). No significant differences were observed between titanium and zirconia abutments when evaluating probing pocket depth, bleeding on probing, marginal bone levels and mucosal recessions. Zirconia abutments were associated with more biological complications but demonstrated superiority in terms of achieving natural soft tissue colour (S-T). Date: Accepted 18 May 2015 To cite this article: Sicilia A, Quirynen M, Fontolliet A, Francisco H, Friedman A, Linkevicius T, Lutz R, Meijer HJ, Rompen E, Rotundo R, Schwarz F, Simion M, Teughels W, Wennerberg A, Zuhr O. Long-term stability of peri-implant tissues after bone or soft tissue augmentation. Effect of zirconia or titanium abutments on peri-implant soft tissues. Summary and consensus statements. The 4th EAO Consensus Conference Clin. Oral Impl. Res. 26 (Suppl. 11), 2015, doi: /clr The task of this working group was to analyse the effect of soft or hard tissue augmentation on the peri-implant tissues, including the long-term stability of the observed results, as well as to analyse the effect on the peri-implant tissues of the use of zirconia and titanium abutments. Three systematic reviews were evaluated, and the findings reported were exposed to interactive experts discussion within the group and general assembly meetings of the 4th European Association for Osseointegration Consensus Conference (4th EAO- CC): Long-term outcomes of soft tissue augmentation around dental implants on soft and hard tissue stability. A systematic review. (Rotundo et al. 2015) 148
2 Long-term outcomes of bone augmentation on soft and hard tissue stability. A systematic review. (Lutz et al. 2015) The effect of zirconia or titanium as abutment material on soft tissues. A systematic review and meta-analysis. (Linkevicius & Vaitelis 2015) Using this methodology, three consensus report were elaborated containing the summaries of the reviews, which included the group s analysis of the information obtained from the tables and references in each review, as well analysis of additional references discovered during the group s discussion. Along with this condensed information, a translational effort was made, including experts opinions on clinical criteria, to elaborate the consensus statements, clinical recommendations and implications for research. Long-term outcomes of soft tissue augmentation around dental implants on soft and hard tissue stability. A systematic review To investigate the long-term outcomes, in terms of peri-implant soft tissue height and thickness, on bone levels, when soft tissue augmentation has been performed. There is no long-term evidence to suggest that soft tissue augmentation may have an effect on peri-implant soft tissue thickness and keratinized tissue width (KTW) or on the stability of peri-implant bone levels. The available results, summarized below, are limited to short and medium-term evaluation and are based on 10 papers, mainly with a 1-year follow up period. Two studies reported medium-term data (4 9 years), both at high risk of bias (Bianchi & Sanfilippo 2004; Bruschi et al. 2014). Eight of them reported on soft tissue augmentation performed at the time of implant placement or at the second stage surgery. The other two dealt with treatment of peri-implant soft tissue dehiscences after prosthetic rehabilitation (both with 1 year of follow up). These two papers were eligible and used for meta-analysis. Effect of soft tissue augmentation on soft tissue thickness and keratinized tissue width Data from two studies were analysed. The first of these was a randomized clinical trial (RCT) evaluating the use of a connective tissue graft (CTG) during the first stage of implant placement in 10 patients (Wiesner et al. 2010). The second was a prospective case series study (PCS) evaluating the treatment of peri-implant recession coverage in 20 patients (Zucchelli et al. 2012). The data from these studies suggested that the use of a CTG is related with an increase of soft tissue thickness of between 1.2 and 1.6 mm at 1 year. It is difficult to summarize data on KTW from the available information due to the heterogeneity of the procedures. In cases of soft tissue augmentation performed at the time of implant placement, a PCS study (split-thickness apically repositioned flaps ARF- with 85 patients at 4 years) (Bruschi et al. 2014) reported an average increase of 5.1 mm. In cases of soft tissue augmentation performed after the prosthetic rehabilitation, a RCT at 1 year (free gingival graft or vestibuloplasty in 64 patients) (Basegmez et al. 2012) reported an increase of KTW between 1.2 and 2.4 mm. In cases where soft tissue dehiscences were present, a PCS study (CAF+CTG on 20 patients at 1 year) (Zucchelli et al. 2012), showed an increase of KTW of 0.6 mm. Effect of soft tissue augmentation on peri-implant bone levels Three studies were identified which used two different approaches: Autogenous connective tissue applied buccally: Data from 1 RCT (CTG on the buccal side, or not, at the first stage of implant placement 10 patients/split mouth) showed no differences between connective tissue grafted and non-grafted areas in terms of mean marginal bone levels (mmbls) at 1 year (Wiesner et al. 2010). Allogenic connective tissue substitutes (ACTS) applied over the crest: Two PCTs (ACTS placed over the crest at implant placement, or not), which involved in total 144 patients, reported significantly lower interproximal marginal peri-implant bone resorption in the grafted areas at 1 year (about 0.2 vs. 1.5 mm) (Linkevicius et al. 2013; Puisys & Linkevicius 2013). Effect of soft tissue augmentation on implant/ abutment coverage Data from two PCSs at 1 year (Zucchelli et al. 2012; Roccuzzo et al. 2013) involving the treatment of shallow peri-implant soft tissue dehiscences by means of CAF+CTG, showed positive results, reporting a complete defect coverage in 56% to 75% of the cases. The related Bayesian meta-analysis indicated a mean implant/abutment coverage of mm (CrI:1.4;1.9). Effect of soft tissue augmentation on aesthetic evaluation Only one study (CS of 20 patients on abutment coverage) reported data on aesthetic evaluation from the patient s point of view, showing that the patients perceived a significant aesthetic improvement up to 1 year after the procedure (Zucchelli et al. 2012). Data from two studies with 1-year followup (1 RCT on implant placement +CTG in the posterior area, and 1 PCS on implant/ abutment coverage in the anterior area) evaluating the aesthetic results from the practitioner s point of view showed a significant aesthetic improvement after both treatments (Wiesner et al. 2010; Roccuzzo et al. 2013). Group s consensus At short and medium-time observation periods there exists limited evidence that: 1. Soft tissue augmentation procedures are able to increase the peri-implant soft tissue thickness and the width of keratinized tissue. 2. In posterior mandibular areas with thin crestal soft tissue, marginal peri-implant bone loss may be reduced by means of vertical soft tissue thickening procedures (ACTS). 3. The coverage of exposed implant/abutment surfaces related to shallow marginal soft tissue recessions may be achieved by means of CAF+CTG. 4. Subjective and objective aesthetic results may be improved by means of soft tissue augmentation procedures. However, due to the lack of studies, there is no long-term evidence that the soft tissue augmentation may have an effect on peri-implant soft tissue thickness, keratinized tissue width, soft tissue marginal levels and on the stability of peri-implant bone levels. The group s opinion, based on limited data, is that soft tissue augmentation procedures may be performed to increase the peri-implant soft tissue thickness, the width of keratinized tissue, and to reduce marginal peri-implant bone loss in areas with thin soft tissues. In the presence of peri-implant soft tissue dehiscences, it may be possible to cover the exposed implant/abutment surface by means of a CAF+CTG. So far, long-term evidence is too limited to strongly recommend peri-implant soft tissue augmentation procedures. The decision must at this stage be left to clinician judgement after a thorough patient evaluation. 149 Clin. Oral Impl. Res. 26 (Suppl. 11), 2015 /
3 There is a need for studies evaluating, at least over a medium and long-term period (5 10 or more years), the repercussions of peri-implant soft tissue augmentation on the stability of the soft and hard peri-implant tissues, as well as the aesthetic aspects and patient-related outcome measures. Future studies must include the following clinical and radiological evaluations as a minimum: 1. Assessment of peri-implant tissue health. 2. Peri-implant keratinized tissue width changes (KTW). 3. Peri-implant marginal soft tissue level changes (PSL). 4. Peri-implant soft tissue thickness changes (KTT). 5. Peri-implant marginal bone level changes (MBL). 6. Professional aesthetic evaluation. 7. Patient reported outcome measures (PROMS). New validated technologies should be used to further improve the accuracy and reproducibility of the measurements. Long-term outcomes of bone augmentation on soft and hardtissue stability. A systematic review This review analysed the current literature regarding medium- and long-term data concerning the stability of peri-implant tissues after hard-tissue augmentation, prior to or at the same time as implant placement. Twenty-seven prospective studies were identified, dealing with guided bone regeneration procedures (21), socket grafting (4) and bone stability around implants that were placed in previously augmented bone (2). Only six were randomized clinical trials (RCTs) that were designed to compare different augmentation techniques. These had a follow-up of between 1 and 5 years. One RCT included a negative control group evaluating bone changes around implants placed into pristine alveolar bone. The studies evaluated bone regeneration associated with implant placement in three different scenarios: guided bone regeneration plus delayed implant placement, guided bone regeneration plus simultaneous implant placement, and socket preservation with graft simultaneous to implant placement. Several prospective studies considered bone augmentation using different techniques. The follow-up period ranged from 1 to 12.5 years. Twenty-three studies evaluated two-dimensional interproximal bone level changes by calculating mean marginal bone loss by means of peri-apical radiographs (5 RCTs and 18 PCTs). They included 725 patients and 1358 implants. Only six studies evaluated the bone levels three-dimensionally by means of a cone beam computer tomographic examination (CBCT). These were made up of two RCTs and four controlled clinical trials (CCTs). All of them dealt with different modalities of guided bone regeneration (GBR) associated with dental implant treatments. They evaluated 141 patients and 188 implants, with follow-up periods ranging from 1 to 7 years. Thirteen studies evaluated soft tissue levels by measuring soft tissue recession using either a periodontal probe or calibrated photographs. These included 518 patients and 849 implants. Two studies used a radiopaque marker to evaluate soft tissue dimensions in CBCT scans (46 patients and 46 implants). Stability of augmented bone After an augmentation procedure the characteristics of the regenerated tissue depend on the materials used within the graft (among other factors). Hence, it cannot always be considered as vital bone. However, to be consistent with the current literature the words bone, bone levels, bone gain and similar terms, are used in the present consensus report. GBR procedures for bone reconstruction, performed simultaneously with the placement of dental implants, in situations in which adequate soft tissue healing was accomplished before the surgery, obtained significant bone gain (as evaluated by means as a CBCT examination) and interproximal bone levels were reported as being stable over the medium-term period. However, no comparison was available between CBCTs taken at different time points after the implant placement (Jung et al. 2015; Buser et al. 2013a, 2013b; Miyamoto et al. 2011). The group was, however, able to make the general observation that following the use of GBR techniques, marginal bone levels (mmbl), assessed by means of periapical radiographs, seemed to be stable over years, with bone loss ranging from 0.1 to 0.8 mm (Mejndert et al. 2007; Merli et al. 2010; Buser et al. 2013a; Amorfini et al. 2013; Jung et al. 2013). Only one study (CCT) examined the use of GBR techniques simultaneously with implant placement, immediately after tooth extraction. This reported that at 7 years 36% of the implants treated showed almost a nondetectable buccal plate (Benic et al. 2012). There is a lack of data in the present review about the stability of the augmented bone using surgical techniques other then GBR, mainly because the type of studies available were generally case reports or retrospective studies. Only two prospective clinical studies were detected. These dealt with the use of autogenous bone, particulated or blocks, associated to DBBM and fibrin glue, or to a titanium mesh, with a follow-up of 2 and 3 years. They evaluated bone loss and demonstrated a mean marginal bone reduction of between 0.3 and 1.1 mm (Von Arx et al. 1998; Hellem et al. 2003). Effect of bone augmentation on soft tissue stability Long-term soft tissue stability was difficult to evaluate with the information retrieved from the reviewed papers, as the baseline reference point and measurements were unclear and not applied consistently in many studies. However, limited data exist to evaluate whether following GBR the soft tissue profile is maintained over time. Two studies (PCTs), dealing with GBR procedures simultaneous to early implant placement, clinically evaluated the distance between the implant shoulder of bone-level implants and the mucosal margin (DIM) at two time points with a 4 and 5 years interval, showing that DIM increased with time. The increment ranged from 0.3 to 0.4 mm, indicating stability or soft tissue coverage of the implant-supported crown (Buser et al. 2013a, 2013b). A few studies show a relationship between the position of the soft tissue margins and the level of the peri-implant bone (Benic et al. 2012; Miyamoto et al. 2011; Dahlin et al. 2010). Consensus statements GBR procedures have been shown to be effective in augmenting the alveolar bone - when performed after completion of soft tissue healing. The regenerated bone seems to be stable over time. There is limited evidence to indicate that the remodelling pattern is similar to that of native bone. Stability of the augmented bone was also reported, in the short-term, with techniques using autogenous bone, with or without DBBM, and titanium mesh or fibrin glue acting as stabilizers of the graft. 150 Clin. Oral Impl. Res. 26 (Suppl. 11), 2015 /
4 GBR performed at the time of tooth extraction together with immediate implant placement has been associated with significant loss of the buccal bone plate. Limited information exists regarding the relation between the stability of the soft tissue margin and that of the regenerated bone, even though a small number of studies may indicate a positive relationship between the underlying bone level and the soft tissue margin position. When aiming at early implant placement, i.e. 4 8 weeks after the tooth extraction, or at the placement of an implant in a healed ridge performing a simultaneous hard tissue augmentation, GBR is a reliable method to reconstruct the ridge and ends-up with increased and stable bone volume. However, ridge augmentation with GBR techniques associated to immediate implants performed immediately after tooth extraction may not be recommendable, as further loss of the buccal plate may occur. Consistent bone ridge reconstructions obtained by means of GBR procedures may facilitate the maintenance of a stable buccal soft tissue contour. Based on the limited evidence and on experts opinions, the group consents that residual marginal defects which lead to the exposure of the implant surface must be avoided by clinicians when using moderately rough surfaced implants in combination with GBR procedures, since these areas may be prone to the development of peri-implant diseases on the long-term (Schwarz et al. 2012; Schwarz et al. 2014; Fontana et al. 2015). There is a lack of information about threedimensional hard and soft tissue evolution following the use of other kinds of hard tissue augmentation techniques. The great variation in the way outcomes are reported, the lack of consistency between the methods of evaluation during follow-up, as well as the difficulty of establishing adequate baseline reference points, makes it very difficult to summarize data and make comparisons among different studies. Additionally, the outcome of bone regeneration procedures should be evaluated in all three dimensions. Therefore, further research should concentrate on a more precise evaluation of hard and soft tissue reconstruction by means of a three-dimension analysis, either using CBCT (respecting EURATOM regulations) or using alternative approaches based on intraoral or lab-based optical scanner technology, or ultrasonic devices. Although short-term studies (1 year) provide very valuable information of the treatment outcomes, to assess hard and soft tissue stability medium and long-term evaluation is recommended (more than 5 years). The impact of implant characteristics on the long-term outcome of bone augmentation has still to be explored. Measurements for bone loss evaluation Mean marginal bone loss (mmbl) measured on periapical radiographs is the most frequently used method to assess interproximal bone loss. Using this technique the distance from the implant shoulder to the bone to implant contact point can be identified. However, no information about the buccal bone level can be obtained. Frequency distribution of the MBL should also be reported. Bone levels and the thickness of the buccal plate can be evaluated by means of a CBCT examination using the appropriate technique. If a CBCT examination is included in the study protocol it should be performed at least at baseline and at the end of follow-up. From this examination the following information should be obtained: the distance from the gingival margin to the implant shoulder (radiopaque marker) (DIM). the thickness of the buccal and lingual walls at 2, 4 and 6 mm of the implant or abutment shoulders. the percentage of cases with no detectable buccal/lingual plate, as well as the frequency distribution of the buccal/lingual bone changes. The evaluation of the DIM could also be achieved, in four points per implant, using a clinical examination with the help of a periodontal probe, after the removal of the implant-supported prosthesis. This technique should also be considered during the follow-up, if multiple evaluations have to be made, to reduce patient exposure to radiation. The use of optical scanners to obtain precise and non-invasive ridge and soft tissues volume information, associated with the clinical measurement of the DIM by means of a periodontal probe, could allow us to estimate the level of buccal and interproximal hard tissue, allowing us to reduce patients exposure to radiation. There is a need to evaluate the impact of the loss of the buccal plate on peri-implant health and its repercussions on the quality of life of the patient. The effect of zirconia or titanium as abutment material on soft tissues. A systematic review and meta-analysis The objective of the review was to analyse the literature with regard to the effect of zirconia or titanium as abutment materials on soft peri-implant tissues. Nine studies (11 papers) were included: four RCTs and five prospective studies (CCTs) with at least 10 patients, with a follow-up 1 year, and with a direct comparison (splitmouth) between titanium oxide (Ti) and zirconium oxide (Zr) abutments. Clinical parameters (PPD, BOP, REC, MBL and additional biological complications) and aesthetic outcome variables (soft tissue colour, patientreported outcomes and aesthetic indices) were analysed. Effect of Zr or Ti as abutment material on soft tissues. Clinical parameters Probing pocket depth (PPD) PPD was recorded in three studies (five papers: Sailer et al. 2009; Zembic et al. 2009, 2012; Lops et al. 2013; Carrillo et al. 2014) and none of them showed statistically significant difference between Ti and Zr abutments, neither in absolute values nor in changes over time. A meta-analysis was not feasible due to heterogeneity of the reported outcomes. Bleeding on probing (BOP) Five studies (seven papers: Sailer et al. 2009; Zembic et al. 2009; Zembic et al. 2012; Lops et al. 2013; Hosseini et al. 2011; Hosseinni et al. 2013; Payer et al. 2012) compared bleeding on probing around Zr or Ti abutments. None of them found statistically significant differences at 1, 3 and 5 years follow-up. There was also no difference in plaque indices. The latter were not considered because they were primarily assessed at the restoration rather than at the abutment level. Marginal bone level (MBL) Six studies (eight papers: Sailer et al. 2009; Zembic et al. 2009, 2012; Lops et al. 2013; Hosseini et al. 2011; Hosseinni et al. 2013; Payer et al. 2012; Carrillo et al. 2014) reported on interproximal marginal bone 151 Clin. Oral Impl. Res. 26 (Suppl. 11), 2015 /
5 level changes, and did not show any statistical significant differences. Additional biological complications Biological complications (suppuration, swelling, fistula, implant loss) were reported in four studies (Hosseini et al. 2011; Hosseinni et al. 2013; Zembic et al. 2012; Lops et al. 2013). Three of them showed a higher frequency of biological complications at implants with Zr abutments. A meta-analysis was not meaningful due to the heterogeneity of the criteria. Soft tissue recession Peri-implant mucosal recession was recorded in three studies (Zembic et al. 2012; Lops et al. 2014; Carrillo et al. 2014) and again no significant differences were observed. Effect of Zr or Ti as abutment material on soft tissues. Aesthetics Soft tissue colour Colour characteristics of the peri-implant mucosa were evaluated in five studies (six papers: Sailer et al. 2009; Zembic et al. 2009; Hosseini et al. 2011; Hosseinni et al. 2013; Cosgarea et al. 2014; Bressan et al. 2011), of which three used spectrophotometry and these were included in a meta-analysis. The outcome was found to be significantly superior for Zr abutments. Patient-reported outcome The evaluation by the patients themselves was reported in two studies (Hosseini et al. 2011; Carrillo et al. 2014). Both applied visual analogue scale (VAS). No significant difference was seen. Aesthetic indices The aesthetic outcomes were reported in four studies (six papers: Sailer et al. 2009; Zembic et al. 2009, 2012; Hosseini et al. 2011; Payer et al. 2012; Carrillo et al. 2014). Only one study used an index restricted to soft tissues (Pink aesthetic score) and showed a significant difference in favour of Zr abutments. The other three studies implemented a combined index which also included the restoration or focused on the papillae only. Consensus statement The literature evaluated in this systematic review revealed no significant differences in clinical outcomes in terms of PPD, BOP, MBL and mucosal recessions, when comparing zirconia and titanium as abutment materials. Zr abutments may be associated with more biological complications, whereas they showed significant superiority in achieving natural soft tissue colour. Based on the available data, both zirconia and titanium abutments have been successfully used in the anterior and posterior regions up to the premolar area of both jaws. In particular, the reported clinical outcomes (PPD, BOP, MBL and REC) were not significantly different between either material. Accordingly, the clinician may choose either Zr or Ti abutments for single-tooth restorations. There is no clinical evidence for a reduced plaque accumulation on Zr abutments. Therefore, maintenance care should be similar for both materials. In aesthetically demanding areas, especially with thin buccal soft tissues, the use of Zr abutments may offer aesthetic advantages. Some reports show a higher incidence of biological complications at implants with Zr abutments, however, a correlation with the abutment material could not be identified. These complications could instead be associated with submucosal cement remnants. Therefore, irrespective of the material used, the abutment must be designed with easy to access cementation margins. Future studies should consider a more uniform definition of biological complications and should also report on changes, as well as absolute values, relating to primary and secondary outcomes. Radiographic assessments of MBL should be based on standardized periapical radiographs with a clear definition of the baseline reference. The influence of the nano-, micro- and macro-structures, as well as the cleaning (chemical composition of the surface) of the trans-mucosal components should be evaluated clinically (e.g. in relation to the stability of the soft tissue). Future studies should address indications other than single-tooth restorations. It would be interesting to compare the aesthetic outcome of Zr abutments with other materials such as: colour-modified Zr or Ti abutments. References Linkevicius, T. & Vaitelis, J. (2015) The effect of zirconia or titanium as abutment material on soft peri-implant tissues: a systematic review and meta-analysis. Clinical Oral Implants Research 26 (Suppl. 11): Lutz, R., Neukam, F.W. & Schmitt, C.M. (2015) Long-term outcomes of bone augmentation on soft and hard tissue stability: a systematic review. Clinical Oral Implants Research 26 (Suppl. 11): Rotundo, R., Pagliaro, U., Bendinelli, E., Esposito, M. & Buti, J. (2015) Long-term outcomes of soft tissue augmentation around dental implants on soft and hard tissue stability: a systematic review. Clinical Oral Implants Research 26 (Suppl. 11): Clin. Oral Impl. Res. 26 (Suppl. 11), 2015 /
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012
 Alberto Sicilia Daniele Botticelli on behalf of Working Group 3 Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012 Authors affiliations: Alberto
Alberto Sicilia Daniele Botticelli on behalf of Working Group 3 Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012 Authors affiliations: Alberto
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Immediate Implant Placement:
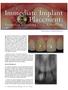 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Conventional immediate implant placement and immediate placement with socket-shield technique Which is better
 International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
University of Groningen. Immediate dental implant placement in the aesthetic zone Slagter, Kirsten
 University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Digital registration of peri-implant transmucosal portion and pontic area in the esthetic zone
 Digital registration of peri-implant transmucosal portion and pontic area in the esthetic zone P. Venezia 1, F. Torsello 2, R. Cavalcanti 3, E. Casiello 4, M. Chiapasco 5 1 DDS Private Practice, Bari,
Digital registration of peri-implant transmucosal portion and pontic area in the esthetic zone P. Venezia 1, F. Torsello 2, R. Cavalcanti 3, E. Casiello 4, M. Chiapasco 5 1 DDS Private Practice, Bari,
Consensus Statements and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry
 Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
GUIDED BONE & TISSUE REGENERATION 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Peri-implant health and peri-implant bone stability after immediate implant placement
 2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Short implants in the posterior maxilla to avoid sinus augmentation procedure: 5-year results from a retrospective cohort study
 Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
Lorenz et al. International Journal of Implant Dentistry (2019) 5:3 https://doi.org/10.1186/s40729-018-0155-1 International Journal of Implant Dentistry RESEARCH Open Access Short implants in the posterior
HÄMMERLE, Christoph, et al. Abstract
 Article Digital technologies to support planning, treatment, and fabrication processes and outcome assessments in implant dentistry. Summary and consensus statements. The 4th EAO consensus conference 2015
Article Digital technologies to support planning, treatment, and fabrication processes and outcome assessments in implant dentistry. Summary and consensus statements. The 4th EAO consensus conference 2015
Implant restoration in the aesthetic zone using guided surgery and immediate functional loading
 Prachatipat Hospital Prathumtani Province Dr. Nawakamon Suriyan Implant restoration in the aesthetic zone using guided surgery and immediate functional loading Digital Workflow: clinical patient information
Prachatipat Hospital Prathumtani Province Dr. Nawakamon Suriyan Implant restoration in the aesthetic zone using guided surgery and immediate functional loading Digital Workflow: clinical patient information
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
GUIDED BONE & TISSUE REGENERATION 2-DAY LIVE COURSE DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
2017 WORLD WORKSHOP. Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March DOI: /jcpe.12957
 Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Socket grafting and ridge preservation using Bond Apatite. Cases 1. Surgery Dr. David Baranes D.M.D
 Socket grafting and ridge preservation using Bond Apatite Cases 1 Case 1 description In this case the two inferiors hopeless molars 37 38 was removed.the socket and the ridge was preserve by augmenting
Socket grafting and ridge preservation using Bond Apatite Cases 1 Case 1 description In this case the two inferiors hopeless molars 37 38 was removed.the socket and the ridge was preserve by augmenting
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
TOPICS. T O P I C S Day 2. Introduction Surgical challenges to treat esthetic implant failures Treatment options & case reports Conclusions
 T O P I C S Day 2 Implant placement post extraction with simultaneous contour augmentation using GBR: When immediate, when early, when late? CAD-CAM technology and zirconia: new opportunities for esthetic
T O P I C S Day 2 Implant placement post extraction with simultaneous contour augmentation using GBR: When immediate, when early, when late? CAD-CAM technology and zirconia: new opportunities for esthetic
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
CASE REPORT MEGAGEN IMPLANT. AnyRidge. CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP
 AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Soft-Tissue Success with the. Clinical Success. Proven Matrix. with the Proven. Geistlich Mucograft Geistlich Mucograft Seal
 Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Movement
 Journal of Dental Health, Oral Disorders & Therapy Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Abstract Introduction: Adult orthodontics is rapidly expanding primarily due
Journal of Dental Health, Oral Disorders & Therapy Alveolar Bone Remodeling and Development after Immediate Orthodontic Root Abstract Introduction: Adult orthodontics is rapidly expanding primarily due
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Screw retained implant crown restoration with digital workflow using scan body and surgical guide
 Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
Implant Studio Patient Case
 Melbourne Bayside Dental Specialists Dr. Philip Tan Implant Studio Patient Case Benefits of guided surgery Case information Dr. Tan presents three different types of cases. Each case uses 3Shape Implant
Melbourne Bayside Dental Specialists Dr. Philip Tan Implant Studio Patient Case Benefits of guided surgery Case information Dr. Tan presents three different types of cases. Each case uses 3Shape Implant
Ankylos. Scientific Summary
 Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
JMSCR Vol 06 Issue 07 Page July 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
Peri-Implant Augmentation
 Indication Sheet PIR - Special Edition Peri-Implant ugmentation Long-term stability KEY TO SUCCESS 3.5-year follow-up by Dr. Paul Stone, University of Edinburgh Dental Institute and lackhills Specialist
Indication Sheet PIR - Special Edition Peri-Implant ugmentation Long-term stability KEY TO SUCCESS 3.5-year follow-up by Dr. Paul Stone, University of Edinburgh Dental Institute and lackhills Specialist
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Fueling innovation in the premium dental market
 Fueling innovation in the premium dental market Francisco Faoro Head Product Development BUSurgical 8 October 2012 Straumann a global leader in replacement, restorative and regenerative dentistry A pioneer
Fueling innovation in the premium dental market Francisco Faoro Head Product Development BUSurgical 8 October 2012 Straumann a global leader in replacement, restorative and regenerative dentistry A pioneer
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Astra Tech Implant System. Scientific Summary
 Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Natural preservation of the emergence profile
 case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
Smile Line Rehabilitation with Dental Implants. Agenda. Agenda. Smile line revitalization with implants Priest Prosthodontics, LLC 1
 Smile Line Rehabilitation with Dental Implants Board Certified Prosthodontist Hilton Head Island, SC Agenda Implant placement and esthetic potential Single immediate implant placement Soft tissue preservation
Smile Line Rehabilitation with Dental Implants Board Certified Prosthodontist Hilton Head Island, SC Agenda Implant placement and esthetic potential Single immediate implant placement Soft tissue preservation
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Foundation for Oral Rehabilitation (FOR) consensus text on The Rehabilitation of Missing Single Teeth
 CONSENSUS STATEMENTS S173 Foundation for Oral Rehabilitation (FOR) consensus text on The Rehabilitation of Missing Single Teeth Methodology used for establishing the consensus text The Foundation for Oral
CONSENSUS STATEMENTS S173 Foundation for Oral Rehabilitation (FOR) consensus text on The Rehabilitation of Missing Single Teeth Methodology used for establishing the consensus text The Foundation for Oral
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Soft-Tissue Solutions from The Collagen Expert. Clinical Success with the Proven. Geistlich Mucograft Geistlich Mucograft Seal Geistlich Fibro-Gide
 Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Consensus Report Biomechanics/risk management (Working Group 2)
 Mariano Sanz Ignace Naert Consensus Report Biomechanics/risk management (Working Group 2) Members of Working Group: Klaus Gotfredsen Flemming Isidor Franck Renouard Phoebus Madianos Carlos Madrid Pascal
Mariano Sanz Ignace Naert Consensus Report Biomechanics/risk management (Working Group 2) Members of Working Group: Klaus Gotfredsen Flemming Isidor Franck Renouard Phoebus Madianos Carlos Madrid Pascal
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Gum Graft? Patient Need a. Does My. 66 JANUARY 2017 // dentaltown.com. by Dr. Brian S. Gurinsky
 by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction?
 C L I N I C A L Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction? Johan Hartshorne 1 Summary Systematic review conclusion:
C L I N I C A L Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction? Johan Hartshorne 1 Summary Systematic review conclusion:
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
MINI System CASE REPORT. Name: Dr. Achraf Souayah Na<on: Tunisia
 MINI System SE REPORT Name: Dr. chraf Souayah Na
MINI System SE REPORT Name: Dr. chraf Souayah Na
