Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial
|
|
|
- Kevin Henry
- 5 years ago
- Views:
Transcription
1 J Clin Periodontol 2013; 40: doi: /jcpe Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial Ronald E. Jung 1, Alexander Philipp 2,3, Beat M. Annen 3, Luca Signorelli 3, Daniel S. Thoma 1, Christoph H.F. Hämmerle 1, Thomas Attin 2 and Patrick Schmidlin 2 1 Clinic of Fixed and Removable Prosthodontics and Dental Material Science, University of Zurich, Zurich, Switzerland; 2 Clinic of Preventive Dentistry, Periodontology and Cariology, Center of Dental Medicine, University of Zurich, Zurich, Switzerland; 3 Private Practice, Zurich, Switzerland Jung RE, Philipp A, Annen BM, Signorelli L, Thoma DS, Ha mmerle CHF, Attin T, Schmidlin P. Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial. J Clin Periodontol 2013; 40: doi: /jcpe Abstract Objective: To evaluate the radiographic changes of the alveolar ridge following application of different ridge preservation techniques 6 months after tooth extraction. Materials and Methods: Four treatment modalities were randomly assigned in 40 patients: b-tricalcium-phosphate-particles with polylactid coating (b-tcp), demineralized bovine bone mineral with 10% collagen covered with a collagen matrix (DBBM-C/CM), DBBM-C covered with an autogenous soft-tissue graft (DBBM-C/PG) and spontaneous healing (control). Cone-beam computed tomography scans were performed after treatment and 6 months later. Results: After 6 months, the vertical changes ranged between 0.6 mm ( 10.2%) for control and a gain of 0.3 mm (5.6%) for DBBM-C/PG on the lingual side, and between 2.0 mm ( 20.9%) for b-tcp and a gain of 1.2 mm (8.1%) for DBBM-C/PG on the buccal side. The most accentuated ridge width changes were recorded 1 mm below the crest: 3.3 mm ( 43.3%, C), 6.1 mm ( 77.5%, b-tcp), 1.2 mm ( 17.4%, DBBM-C/CM) and 1.4 mm ( 18.1%, DBBM-C/ PG). At all three levels, DBBM-C with either CM or PG was not significantly differing (p > 0.05), while most other differences between the groups reached statistical significance (p < 0.05). Conclusions: Application of DBBM-C, covered with CM or PG, resulted in less vertical and horizontal changes of the alveolar ridge as compared with controls 6 months after extraction. Key words: bone regeneration; bone substitute; cone-beam CT; graft material; human; RCT; socket preservation Accepted for publication 21 September 2012 Conflict of interest and source of funding statement This study was predominantly supported by the Clinic of Fixed and Removable Prosthodontics and Dental Material Science, the Clinic of Preventive Dentistry, Periodontology and Cariology, both Center of Dental Medicine, University of Zurich, Zurich, Switzerland and in part by research grants of Geistlich Pharma AG, Wolhusen, Switzerland and Degradable Solutions AG, Schlieren, Switzerland. All patients were treated and all analyses performed at the Clinic of Fixed and Removable Prosthodontics and Dental Material Science, the Clinic of Preventive Dentistry, Periodontology and Cariology, both Center of Dental Medicine, University of Zurich, Zurich, Switzerland. The authors declare that they have no conflicts of interests. 90
2 Rx-evaluation of ridge preservation 91 After tooth extraction, a variety of soft and hard tissue alterations are initiated and lead to a reduced alveolar ridge contour (Amler et al. 1960, Pietrokovski & Massler 1967). The resorption processes responsible for the dimensional changes following tooth extraction have been studied in different animal models (Kuboki et al. 1988, Lin et al. 1994, Cardaropoli et al. 2003, Araujo et al. 2005, 2008, Fickl et al. 2008a,b). Dimensional and contour changes in post-extraction AR have been described by serial study cast measurements (Lam 1960, Pietrokovski & Massler 1967, Watt & Likeman 1974, Schropp et al. 2003), lateral cephalograms, (Carlsson & Persson 1967, Atwood & Coy 1971), radiographic analyses (Atwood 1957, Carlsson & Persson 1967, Tallgren 1969, Schropp et al. 2003) and direct measurements of the ridge following surgical re-entry procedures (Lekovic et al. 1997, 1998, Barone et al. 2008). The dimensional changes of the alveolar ridge following tooth extraction were recently assessed in a systematic review (Van der Weijden et al. 2009). Clinically, a mean resorption of the buccal bone contour of approximately 50% taking place mainly within the first 3 months after tooth extraction was observed (Schropp et al. 2003). The possible consequences of these resorption processes may significantly hamper implant placement without additional bone regeneration techniques and may yield an inadequate aesthetic outcome due to the ridge deficiencies. A variety of pre-clinical and clinical studies have evaluated the effect of using immediate implants, of placing bone substitute materials with and without application of membranes or soft tissue coverage for their ability to maintain the alveolar ridge contour (Iasella et al. 2003, Barone et al. 2008, Mardas et al. 2010, Horvath et al. 2012, Vignoletti et al. 2012). They revealed that none of the tested treatments was able to completely preserve the buccal bone plate. However, biomaterials placed into the extraction sockets promoted bone modelling and partially compensated, at least temporarily, for the marginal ridge contraction in an animal model (Araujo et al. 2008). A recent review article evaluated the techniques and outcomes of postextraction ridge preservation procedures (Darby et al. 2009). They reported a large heterogeneity of the studies describing many different techniques, methodologies, durations and materials making direct comparison very difficult. Hence, there is a lack of controlled clinical studies evaluating different techniques for alveolar ridge preservation. The aim of this study was to evaluate the radiographic changes of different techniques for ridge preservation compared with spontaneous healing within the first 6 months after tooth extraction. Materials and Methods Study design This study was a prospective, controlled, randomized, clinical investigation according to the Helsinki protocol. All procedures and materials were submitted and approved by the local ethical committee (Ethikkommission des Kanton Zu rich, Ref. Nr. StV 06/12). Informed consent was obtained from all patients prior to the start of the study. Regarding the randomization, a computer-generated list was prepared and concealed randomization envelopes were stored by an independent person unaware of the study protocol. Participants and treatment protocol Forty patients requiring extraction of at least one upper or lower asymptomatic front tooth or premolar were recruited. The diagnosed indications for tooth extractions were caries, endodontic complications (e.g. root fracture), periodontitis, orthodontic and prosthetic reasons. Only healthy patients with an adequate oral hygiene (bleeding on probing 20%; Plaque index 20%) were included. As a prerequisite for inclusion in the study, patients had to be systemically healthy and not smoking more than 20 cigarettes/day. The demographic data of all patients and sites are presented in Table 1. Tooth extraction was performed with great care to preserve the buccal bone plate and the surrounding soft and hard tissues. Subsequently, the height of the buccal and lingual bone plate was clinically measured to the nearest 0.5 mm at the midbuccal and midlingual aspect using a periodontal probe. In addition, the height of the socket was measured to the base, which allowed calculating the vertical loss of the buccal plate compared with the lingual bone plate. Participants were excluded if more than 50% of the buccal bone height was not present. Patients not meeting all inclusion criteria were excluded from the study. After tooth extraction, careful removal of the granulation tissue with hand instruments and rinsing with sterile saline, the patients were randomly assigned to one of three test ridge preservation techniques or the control group according to an opaque, concealed, continuously numbered randomization envelope (n = 10 per group): b-tricalcium-phosphate-particles (500 lm), with a poly(lactideco-glycolide) coating (easy-graft, Degradable Solutions AG, Schlieren, Switzerland) 1 2 mm below the bone crest without any further treatment at the soft tissue level (b-tcp) Demineralized bovine bone mineral with 10% collagen (DBBM-C; Bio-Oss Collagen, Geistlich Table 1. Demographic data of included patients and sites Patient parameters Control b-tcp DBBM-C/CM DBBM-C/PG Age (years) Mean ± SD 48 ± ± ± ± 14 Male/female 6/4 6/4 4/7 2/8 Smoker/Non-smoker 1/9 1/9 2/9 7/3 Anterior/posterior 3/7 3/7 5/6 7/3 Mandible/maxilla 0/10 1/9 4/7 3/7 Reason for extraction orthodontic/chronic periapical lesion/fracture of tooth or lack of tooth substance 1/5/4 0/4/6 0/2/8 0/4/6 DBBM, demineralized bovine bone mineral.
3 92 Jung et al. Pharma AG, Wolhusen, Switzerland) at the bone level and application of a collagen matrix (CM; Mucograft Geistlich Pharma AG, Wolhusen, Switzerland) at the soft tissue level (DBBM-C/ CM) DBBM-C (Bio-Oss Collagen, Geistlich Pharma AG) at the bone level and application of an autogenous soft tissue punch graft (PG) at the soft tissue level (DBBM-C/PG). For the control group (iv; control), no further treatment was applied and the coagulum within the socket was left open for spontaneous healing. In brief, the regenerative materials were applied as follows: In the b-tcp group, the bone substitute material was prepared according to the manufacturer s instructions. The material was delivered in a syringe. An N-methylpyrrolidone/water mixture (NMP) was added to the material before application and mixed for 15 s. The material was then placed within the bony envelope and was slightly compressed. The material was rinsed with 40 ml of sterile saline to remove the NMP and to allow for in situ hardening and stabilization of the material. No further treatment was applied at the soft tissue level, that is, the socket was left open. For group DBBM-C/PG, a previously described technique was used (Jung et al. 2004). This technique was slightly modified for the DBBM-C/CM group. In brief, for both latter groups, a bone substitute material (Bio-Oss Collagen) was placed within the bony envelope at least to the level of the palatal/ lingual bone plate. Subsequently, the soft tissue borders of the alveole were de-epithelialized using a diamond drill under copious irrigation with water. For the DBBM-C/PG group, an autogenous soft tissue graft was harvested from the patient s palate using a soft tissue punch (Biopsy Punch, Stiefel Laboratorien, Munich, Germany) with a similar dimension as the respective alveole (diameter 6 8 mm). With this selected punch, a free gingival graft of 2 3 mm thickness was cut and gently dissected using a sharp tissue elevator. Finally, the harvested graft was placed on top of the filler material, adapted and sutured to the marginal gingiva of the extracted tooth with 6 10 single interrupted sutures (Dafilon No. 6/0; Braun Aesculap, Tuttlingen, Germany). In group applying DBBM-C/ CM, instead of an autogenous graft, a collagen matrix (Mucograft ) with similar dimensions was prepared using a punch biopsy with a diameter of 6 mm and adapted to the soft tissue borders again using single interrupted sutures (Dafilon No. 6/0, Braun Aesculap). Subsequently, a cone-beam computed tomography (CBCT) scan was taken with a resolution of 0.3 mm (scan time: 8.5 s, exposure time: 4 s, 120 KV, 5 ma) using a KaVo 3D exam (KaVo, Biberach an der Riss, Germany). Patients were instructed to rinse twice a day with 0.2% Chlorhexidine (Kantonsapotheke Zu rich, Zurich, Switzerland), and received pain killer medication (Mefenacid, Streuli Pharma, Uznach, Switzerland) and antibiotics (Amoxicillin Sandoz, Sandoz, Basel, Switzerland) for 5 days. All patients were recalled at 7 10 days for a check-up and suture removal (groups DBBM-C/PG and DBBM-C/ CM). Patients then followed their individual maintenance programme according to the individual periodontal and caries risk assessment. Follow-up Six months post-extraction, all patients were recalled and a second CBCT scan was taken using the same settings as described above. Analyses Clinical measurements at baseline The height of the alveole after tooth extraction was measured at the lingual and buccal aspect using a periodontal probe to the nearest millimetre. The difference between the buccal and lingual height was expressed in mm either in positive values (buccal bone plate more coronal than lingual bone plate) or in negative values (buccal plate more apical than lingual bone plate). CBCT measurements To perform radiographic measurements, CBCT scans at baseline and at 6 months were processed using an open source software package (Slicer For superimposition of the original DICOM data (Digital Imaging and Communications in Medicine) of the two CBCT scans, a computer-assisted superimposition was done in selected areas of the data set, where no changes had taken place during the 6 months (e.g. the cranial base in the maxilla or the lower border and angle in the mandible respectively). By this step, the two data sets were aligned and were, thereafter, manually checked for perfect match. Subsequently, the measurements were made at baseline and at 6 months using the same reference points and lines. To set a reference, the most apical point of the extraction socket was defined in the baseline image and two reference lines were subsequently drawn. The vertical reference line was drawn in the centre of the extraction socket crossing the apical reference point. The horizontal reference line was drawn perpendicular to the vertical line crossing the apical reference point. The following measurements with respect to these reference points and lines were then performed in the centre of the extraction socket (Fig 1): thickness of the buccal bone plate at three levels (1 mm, 3 mm and 5 mm below the lingual bone crest) (BBP-1, BBP-3, BBP-5) (only at baseline). height of the alveole at the midbuccal (BH) and midlingual (LH) aspect: for groups b-tcp, DBBM-C/CM and DBBM-C/ PG, the height was measured with (BHgraft/LHgraft) or without grafting material (BHplate/ LHplate), whereas in the control group only BHplate/LHplate was calculated. the horizontal ridge width measured at three levels (at 1 mm, 3 mm, 5 mm) below the most coronal aspect of the crest (HW-1, HW-3, HW-5). In addition, dimensional changes over time were assessed based on the measurements performed at baseline and at 6 months. This encompassed the following parameters (expressed both in percentages and in mm): i) changes in ridge height at the buccal and lingual aspect (BHgraftC/ LHgraftC, BHplateC/LHplateC); ii) changes in ridge width at three levels below the crest (HW-1C, HW-3C, HW-5C).
4 Rx-evaluation of ridge preservation 93 No post-operative complications were recorded at any included site. All patients completed the study and passed the 6-month follow-up. Clinical baseline measurements Of 40 extraction sockets in the upper and lower jaw, 23 were premolars, eight laterals incisors, six central incisors and three canines. As the treatments were randomly assigned, the sites were equally distributed among the four treatment modalities and were not suspected to influence the treatment outcomes. The clinically measured difference between the buccal and lingual height of the bone plate ranged between 0.9 mm (b-tcp) and 2.0 mm (control). Overall, no statistically significant differences in mean defect dimensions were observed among the four treatment modalities (p > 0.05) (Table 2). Fig. 1. Cone-beam computed tomography (CBCT) slice section of demineralized bovine bone mineral (DBBM)-C/CM site at baseline. HW-1 (at 1 mm), HW-3 (at 3 mm) and HW-5 (at 5 mm) represent measurements performed at three levels below the bone crest. In a vertical dimension, the most coronal aspects on the buccal and lingual side of the socket were measured being the bone crest (BHplate, LHplate) or the graft material (BHgraft; LHgraft). Statistical analysis For the pooled data set as well as for each treatment group, the sample distributions of all variables were described univariately by showing means, medians, standard deviations, quartiles and extreme values. To test the working hypothesis of systematic differences between treatment groups, for each variable, a Kruskal Wallis non-parametric one-way analysis of variance was performed, each at a level of Due to the exploratory nature of the analysis, no Bonferroni correction for multiple testing was applied. For variables with significant differences between treatment groups, approximate partial F-tests were used to verify the test decisions under consideration of the potential confounders plate loss and central thickness using linear models. Each non-parametric ANOVA was followed by two-sided Wilcoxon s rank sum tests for pairwise comparisons including Bonferroni correction: A comparison of four groups produces six pairwise tests, thus a more conservative significance level of 0.05/6 = was used. Similarly, if three groups were compared with each other, three tests at a level of 0.05/3 = were calculated. The analysis was performed using R version (R Development Core Team 2010). Results Patients All treatments were performed according to the clinical protocol. CBCT analyses Representative CBCTs of all four treatments modalities are presented in Fig. 2. At baseline, the thickness of the buccal bone plate at the three measured levels ranged from a minimum of 0.6 mm to a maximum of 1.8 mm, but did not reveal any statistically significant differences between the treatments (p > 0.005). All measured outcome variables with means and standard deviations are presented in Table 2. The dimensional changes after 6 months are presented in Table 3a and b and Fig. 3a,b. Table 2. Baseline measurements for height differences between buccal and lingual bone crest (clinically assessed using a periodontal probe) and for thickness of buccal bone plate (radiographically using baseline CBCT) Baseline measurements (mm) Control b-tcp DBBM-C/ CM DBBM-C/ PG Mean SD Mean SD Mean SD Mean SD Clinical measurements (periodontal probe) Difference in vertical bone height between lingual and buccal bone Radiographic measurements (thickness of buccal bone plate) Buccal bone plate 1 mm Buccal bone plate 3 mm Buccal bone plate 5 mm Buccal bone plate 1 to 5 mm mean CBCT, cone-beam computed tomography; DBBM, demineralized bovine bone mineral.
5 94 Jung et al. (a) (c) (e) (g) The mean height changes at the lingual aspect (LHplateC) over 6 months amounted to 0.6 mm (±0.6 mm) for control sites, 0.4 mm (±1.4 mm) for b-tcp, 0.4 mm (±1.4 mm) for DBBM-C/CM and 0.3 mm (±1.1 mm) for DBBM-C/PG. The (b) Fig. 2. Representative cone-beam computed tomography (CBCT) of all four treatment modalities at baseline and at 6 months. *buccal side. (a) b-tcp site at baseline. (b) b- TCP site at 6 months. (c) Demineralized bovine bone mineral (DBBM)-C/CM site at baseline. (d) DBBM-C/CM site at 6 months. (e) DBBM-C/PG site at baseline. (f) DBBM-C/PG site at 6 months. (g) Control site at baseline. (h) Control site at 6 months. (d) (f) (h) differences between the groups reached statistical significance for DBBM-C/PG versus b-tcp (p < 0.005). At the buccal aspect, the respective height changes (BHplateC) were 0.5 mm (±0.9 mm) for control sites, 2.0 mm (±2.4 mm) for b-tcp, 0.0 mm (±1.2 mm) for DBBM-C/CM and 1.2 mm (±2.9 mm) for DBBM-C/PG. The differences between the four groups were not statistically significantly different between the groups (p > 0.005). When the various bone graft materials in groups b-tcp, DBBM-C/CM and DBBM-C/ PG were taken into consideration and the most coronal aspect of the graft materials served as reference points, the respective values demonstrated a height loss ranging between 3.5 mm (±1.1 mm) for b-tcp, 1.3 mm (±0.9 mm) for DBBM-C/CM and 0.5 mm (±0.9 mm) for DBBM-C/PG on the lingual side (LHgraftC). A height loss was also observed on the buccal side (BHgraftC), with values ranging between 3.9 mm (±2.4 mm) for b-tcp, 1.5 mm (±1.2 mm) for DBBM-C/CM and 0.5 mm (±1.0 mm) for DBBM- C/PG. The differences reached statistical significance between DBBM-C/ PG and b-tcp on the buccal aspect, and between on the lingual aspect for the two DBBM groups versus b-tcp (p < 0.005) (Tables 3a,b and 4; Fig. 3a). The mean ridge width changes at the three levels below the crest (HW-1C, HW-3C, HW-5C) amounted to 3.3 mm (±2.0 mm), 1.7 mm (±0.8 mm), 0.8 mm (±0.5 mm) for control sites, 6.1 mm (±2.5 mm), 3.1 mm (±1.6 mm), 5.7 mm (±3.0 mm) for b-tcp, 1.2 mm (±0.8 mm), 0.6 mm (±0.6 mm), 0.1 mm (±0.2 mm) for DBBM-C/CM and 1.4 mm (±1.0 mm), 0.6 mm (±0.5mm), 0.6 mm (±0.9 mm) for DBBM-C/PG. At all three levels, DBBM-C/CM and DBBM-C/PG were not significantly differing (p > 0.005), while many other differences between the groups reached statistical significance (p < 0.005) (Tables 3a,b and 4; Fig. 3b). The statistical analysis of potentially confounding factors confirmed the systematic treatment differences under simultaneous consideration of the extent of the initial bone loss of the buccal bone plate (clinical measurements) and the initial thickness of the buccal bone plate (CBCT measurements) except for the variables LHplateC and HW-5C. Discussion This study demonstrated that the application of DBBM-C into the extraction socket, covered with either
6 Rx-evaluation of ridge preservation 95 a collagen matrix (CM) or an autogenous soft tissue punch graft (PG), resulted in significantly less vertical and horizontal resorption compared with the control group in the majority of the assessed parameters 6 months after tooth extraction. Broad evidence exists in the dental literature for studies reporting on dimensional changes of the alveolar ridge following tooth extraction. A very recent systematic review with a total of 20 included studies demonstrated a percentage of vertical bone loss at the buccal aspect of 11 22% ( mm, weighted mean 1.24 mm at 6 months) (Tan et al. 2012). The outcomes of the latter meta-analysis can be compared with the values obtained in the control group (spontaneous healing) of this study revealing a mean vertical bone loss of the buccal bone plate of 5.5% and of the lingual bone plate of 10.2%. This slightly less pronounced vertical bone loss in this study might be explained by the fact that no flap elevation was performed neither during extraction nor for the measurements. In contrast, some studies included in that systematic review measured the vertical dimensional changes by elevating a flap at the time of extraction and at reentry (Lekovic et al. 1997, 1998, Camargo et al. 2000, Iasella et al. 2003, Serino et al. 2003, Barone et al. 2008, Pelegrine et al. 2010). A previous pre-clinical study in dog mandibles demonstrated a significant difference in the extent of bone resorption comparing flapless extractions and extractions with flap elevation (Fickl et al. 2008a). The flapless surgery reduced the volumetric alterations on the buccal aspect irrespective whether a grafting material was used. In the same pre-clinical study, it was also concluded that the treatment of the extraction socket with DBBM with 10% collagen and a free gingival graft (corresponding to the DBBM-C/PG group in this study) was beneficial in limiting bone resorption (Fickl et al. 2008c). It is important to mention that in this study also the lingual bone plate revealed vertical changes. Therefore, studies, using the lingual bone plate as a vertical reference to measure the buccal resorption, should be interpreted with caution in future studies. Table 3. (a) Changes in ridge height and width between 6 months and baseline based on CBCT measurements expressed in mm. (b) Changes in ridge height and width between 6 months and baseline based on CBCT measurements expressed in % CBCT analysis Control b-tcp DBBM-C/CM DBBM-C/PG Mean SD Mean SD Mean SD Mean SD (a) BHgraftC NA NA LHgraftC NA NA LHplateC BHplateC HW-1C HW-3C HW-5C (b) BHgraftC NA NA LHgraftC NA NA LHplateC BHplateC HW-1C HW-3C HW-5C CBCT, cone-beam computed tomography; DBBM, demineralized bovine bone mineral. Change in ridge height (%) (a) Control β-tcp DBBM C/CM DBBM C/PG HW 1C HW 3C HW 5C LHplateC BHplateC DBBM C/PG DBBM C/CM ß TCP Control (b) Change in ridge width (%) Fig. 3. (a) Changes in ridge height (%) over 6 months based on cone-beam computed tomography (CBCT) measurements. Most coronal aspects of the extraction sockets serve as reference points on the buccal (BHplate) and lingual (LHplate) side. (b) Changes in ridge width (%) over 6 months based on CBCT measurements. Measurements performed at three levels below the bone crest ( 1 mm= HW-1C; 3 mm= HW-3C; 5 mm= HW-5C).
7 96 Jung et al. Table 4. Calculated statistical differences for changes in ridge height and width over 6 months among the four treatment modalities Variable Group b-tcp DBBM-C/CM DBBM-C/PG LHgraftC DBBM-C/CM DBBM-C/PG LHplateC DBBM-C/CM DBBM-C/PG Control BHgraftC DBBM-C/CM DBBM-C/PG BHplateC DBBM-C/CM DBBM-C/PG Control HW-1C DBBM-C/CM DBBM-C/PG Control HW-3C DBBM-C/CM DBBM-C/PG Control HW-5C DBBM-C/CM DBBM-C/PG Control Bold values represent statistical differences after Bonferroni correction. DBBM, demineralized bovine bone mineral. The application of a slowly resorbing grafting material (DBBM + 10% collagen) covered either with a collagen matrix (CM) or an autogenous soft tissue punch graft (PG) resulted in a reduced amount of vertical bone loss at the buccal and the lingual aspect. In this study, the vertical changes have been analysed on the level of the bone plate and on the level of the most coronal point of the graft material. The results from the graft materials (BHgraftC and LHgraftC) demonstrated that it was not possible to mineralize the amount of graft material at the most coronal portion of the graft material. This was documented by a vertical loss ranging from 4.4% to 15.6% of the original augmentation height. However, part of the vertical bone loss of the plates could be partially compensated or even overcompensated by using the DBBM-C material. This was predominantly evident in the PG group revealing a gain of the reduced bone plates of up to 1.2 mm at the buccal aspect. This observation corroborates histological outcomes of a clinical study using either HA/TCP or DBBM following tooth extraction (Mardas et al. 2010). In that study, the most coronal portion of the graft material (DBBM) was not mineralized (Mardas et al. 2010). In a recent systematic review on surgical protocols for alveolar ridge preservation a statistically significantly reduced contraction of the alveolar crest was demonstrated for sites with grafting procedures compared with sites with spontaneous healing (Vignoletti et al. 2012). This was in agreement with this study. However, this is not true for the alternative treatment modality (b-tcp with open for healing). The latter test group was not able to preserve the bone plate. In contrast, the resorption of the ß-TCP seemed more pronounced compared with spontaneous healing. Different reasons may explain these findings: (i) The shorter degradation time of TCP and a subsequent higher turnover of the remodelling process in the extraction socket. This finding is supported by the latest recommendations to use slowly resorbing bone graft substitutes for socket preservation (Ha mmerle et al. 2012), (ii) An additional reason might be the influence of the polylactid coating and the respective degradation products. However, previous pre-clinical data did not reveal an inflammatory reaction to the PLGA-coated calcium phosphate materials (Nair et al. 2006, Rothamel et al. 2007, Schmidlin et al. 2011), (iii) The third possible explanation might be attributed to the open healing (i.e. lack of sealing towards the oral cavity). Due to this missing seal, material might have been lost during healing. This speculation is supported by the more favourable outcomes of the two groups with a socket seal (DBBM-C/CM, DBBM- C/PG) and by a pre-clinical study in dogs (Fickl et al. 2008c). When it comes to dimensional alterations after tooth extraction the horizontal bone loss is in general more pronounced than the aforementioned vertical bone loss (Darby et al. 2009, Tan et al. 2012). Tooth extraction without the use of grafting material leads to a percentage of horizontal dimensional changes of 29 63% after 6 7 months (Tan et al. 2012). This is in agreement with this study demonstrating a mean ridge width reduction at the level 1 mm below the crest of 43.3% for control sites with spontaneous healing. By using a slowly resorbing grafting material (DBBM-C), the amount of horizontal bone loss could be significantly reduced to 17.4% for DBBM- C/CM and 18.1% for DBBM-C/PG. This fits to a number of pre-clinical and clinical studies reporting that no grafting material was able to completely preserve the alveolar ridge after tooth extraction, but could preserve the buccal bone volume to a certain extent (Chen et al. 2007, Araujo et al. 2008, Fickl et al. 2008c). This finding mainly derives from studies where no flap was elevated at the time of extraction and the grafting procedure. Hence, grafting only within the former extraction socket may not allow maintaining 100% of the original dimensions. In contrast, elevating the flap at the time of tooth extraction offers the opportunity to over-augment the socket by placing grafting material also to the outside of the buccal bone plate. Interestingly, a current systematic review demonstrated in a subgroup analysis a significant difference in favour of the flapped group in regards to the horizontal ridge changes (Vignoletti et al. 2012). From a practical point of view, a flapless approach would simplify the entire clinical procedure (tooth extraction with an alveolar ridge preservation technique). The majority of clinical studies reported on horizontal bone loss at the level of the alveolar crest only (Lekovic et al. 1997, 1998, Camargo et al. 2000, Iasella et al. 2003, Pelegrine et al. 2010). The radiographic analysis of this study has the opportunity to perform the measurements also more apically at 3 and 5 mm
8 Rx-evaluation of ridge preservation 97 below the alveolar crest. In general, the horizontal bone loss decreased in all groups with an increasing distance to the alveolar crest. Therefore, the horizontal changes 1 mm below the crest have been the ones, which benefited most from the alveolar ridge preservation techniques. The present RCT failed to identify an influence of prognostic factors (i.e. location of tooth extraction, initial buccal bone defect; initial thickness of the buccal bone plate), on the majority of the radiographic outcome measurements. This is in contrast to recent studies in humans showing the influence of the location and the thickness of the socket walls in the ensuing modelling and remodelling processes after tooth extraction (Ferrus et al. 2010, Januario et al. 2011). This may also be explained in part by the small sample size analysed in the current investigation and differences between the tooth sites and conditions. However, a power analysis revealed a minimum sample size of approximately 240 patients to be included aiming to achieve 81% power to detect a 0.5 mm difference with standard deviations of 1 mm. This is far beyond the scope and the feasibility of this study. In addition, one could also argue that even more groups would have been necessary to be included, namely the evaluation of DBBM-C without collagen matrix or autogenous graft, or coronal wound closure approaches alone, to discern between different regenerative approaches. Considering that despite these limitations statistically significant differences were detected after Bonferroni correction, some clinically relevant conclusionscanbedrawnandtheresults may serve as a basis for future studies. Conclusions The application of DBBM-C into an extraction socket, covered either with a collagen matrix (CM) or an autogenous soft tissue punch graft (PG), resulted in less vertical and horizontal changes compared with spontaneous healing or the use of TCP alone without primary closure 6 months after tooth extraction. However, none of the techniques was able to completely preserve the alveolar ridge contour. The possible influence of these techniques on the long-term outcomes of implant therapy or conventional prosthodontics remains unknown. Acknowledgements The authors thank Dr. Michael Mayer, Consult AG, Bern, Switzerland for performing the statistical analysis. References Amler, M. H., Johnson, P. L. & Salman, I. (1960) Histological and histochemical investigation of human alveolar socket healing in undisturbed extraction wounds. Journal of the American Dental Association 61, Araujo, M., Linder, E., Wennstrom, J. & Lindhe, J. (2008) The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. The International journal of periodontics & restorative dentistry 28, Araujo, M. G., Sukekava, F., Wennstrom, J. L. & Lindhe, J. (2005) Ridge alterations following implant placement in fresh extraction sockets: an experimental study in the dog. Journal of Clinical Periodontology 32, Atwood, D. A. (1957) A cephalometric study of the clinical rest position of the mandible. Part II. The variability in the rate of bone loss following the removal of occlusal contacts. Journal of Prosthetic Dentistry 7, Atwood, D. A. & Coy, W. A. (1971) Clinical, cephalometric, and densitometric study of reduction of residual ridges. Journal of Prosthetic Dentistry 26, Barone, A., Aldini, N. N., Fini, M., Giardino, R., Calvo Guirado, J. L. & Covani, U. (2008) Xenograft versus extraction alone for ridge preservation after tooth removal: a clinical and histomorphometric study. Journal of Periodontology 79, Camargo, P. M., Lekovic, V., Weinlaender, M., Klokkevold, P. R., Kenney, E. B., Dimitrijevic, B., Nedic, M., Jancovic, S. & Orsini, M. (2000) Influence of bioactive glass on changes in alveolar process dimensions after exodontia. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology and Endodontics 90, Cardaropoli, G., Araujo, M. & Lindhe, J. (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. Journal of Clinical Periodontology 30, Carlsson, G. E. & Persson, G. (1967) Morphologic changes of the mandible after extraction and wearing of dentures. A longitudinal, clinical, and x-ray cephalometric study covering 5 years. Odontologisk Revy 18, Chen, S. T., Darby, I. B. & Reynolds, E. C. (2007) A prospective clinical study of non-submerged immediate implants: clinical outcomes and esthetic results. Clinical Oral Implants Research 18, Darby, I., Chen, S. T. & Buser, D. (2009) Ridge preservation techniques for implant therapy. International Journal of Oral and Maxillofacial Implants 24(Suppl), Ferrus, J., Cecchinato, D., Pjetursson, E. B., Lang, N. P., Sanz, M. & Lindhe, J. (2010) Factors influencing ridge alterations following immediate implant placement into extraction sockets. Clinical Oral Implants Research 21, Fickl, S., Zuhr, O., Wachtel, H., Bolz, W. & Huerzeler, M. (2008a) Tissue alterations after tooth extraction with and without surgical trauma: a volumetric study in the beagle dog. Journal of Clinical Periodontology 35, Fickl, S., Zuhr, O., Wachtel, H., Bolz, W. & Huerzeler, M. B. (2008b) Hard tissue alterations after socket preservation: an experimental study in the beagle dog. Clinical Oral Implants Research 19, Fickl, S., Zuhr, O., Wachtel, H., Stappert, C. F., Stein, J. M. & Hurzeler, M. B. (2008c) Dimensional changes of the alveolar ridge contour after different socket preservation techniques. Journal of Clinical Periodontology 35, Ha mmerle, C. H. F., Araujo, M. & Simion, M. (2012) Osteology Consensus Report Evidencebased knowledge on the biology and treatment of extraction sockets. Clinical Oral Implants Research 23, Horvath, A., Mardas, N., Mezzomo, L. A., Needleman, I. G. & Donos, N. (2012) Alveolar ridge preservation. A systematic review. Clinical Oral Investigations doi: /s Iasella, J. M., Greenwell, H., Miller, R. L., Hill, M., Drisko, C., Bohra, A. A. & Scheetz, J. P. (2003) Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. Journal of Periodontology 74, Januario, A. L., Duarte, W. R., Barriviera, M., Mesti, J. C., Araujo, M. G. & Lindhe, J. (2011) Dimension of the facial bone wall in the anterior maxilla: a cone-beam computed tomography study. Clinical Oral Implants Research 22, Jung, R. E., Siegenthaler, D. W. & Hammerle, C. H. (2004) Postextraction tissue management: a soft tissue punch technique. The International journal of periodontics & restorative dentistry 24, Kuboki, Y., Hashimoto, F. & Ishibashi, K. (1988) Time-dependent changes of collagen crosslinks in the socket after tooth extraction in rabbits. Journal of Dental Research 67, Lam, R. V. (1960) Contour Changes of the Alveolar Processes Following Extractions. Journal of Prosthetic Dentistry 10, Lekovic, V., Camargo, P. M., Klokkevold, P. R., Weinlaender, M., Kenney, E. B., Dimitrijevic, B. & Nedic, M. (1998) Preservation of alveolar bone in extraction sockets using bioabsorbable membranes. Journal of Periodontology 69, Lekovic, V., Kenney, E. B., Weinlaender, M., Han, T., Klokkevold, P., Nedic, M. & Orsini, M. (1997) A bone regenerative approach to alveolar ridge maintenance following tooth extraction. Report of 10 cases. Journal of Periodontology 68, Lin, W. L., McCulloch, C. A. & Cho, M. I. (1994) Differentiation of periodontal ligament fibroblasts into osteoblasts during socket healing after tooth extraction in the rat. Anatomical Record 240, Mardas, N., Chadha, V. & Donos, N. (2010) Alveolar ridge preservation with guided bone regeneration and a synthetic bone substitute or a bovine-derived xenograft: a randomized, controlled clinical trial. Clinical Oral Implants Research 21, Nair, P. N., Luder, H. U., Maspero, F. A., Fischer, J. H. & Schug, J. (2006) Biocompatibility of Beta-tricalcium phosphate root replicas in porcine tooth extraction sockets - a correla-
9 98 Jung et al. tive histological, ultrastructural, and x-ray microanalytical pilot study. Journal of Biomaterials Applications 20, Pelegrine, A. A., da Costa, C. E., Correa, M. E. & Marques, J. F., Jr (2010) Clinical and histomorphometric evaluation of extraction sockets treated with an autologous bone marrow graft. Clinical Oral Implants Research 21, Pietrokovski, J. & Massler, M. (1967) Alveolar ridge resorption following tooth extraction. Journal of Prosthetic Dentistry 17, R Development Core Team. (2010) R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing. Rothamel, D., Schwarz, F., Herten, M., Chiriac, G., Pakravan, N., Sager, M. & Becker, J. (2007) Dimensional ridge alterations following tooth extraction. An experimental study in the dog. [Article in German] Mund-, Kiefer- und Gesichtschirurgie 11, Schmidlin, P. R., Nicholls, F., Kruse, A., Zwahlen, R. A. & Weber, F. E. (2011) Evaluation of moldable, in situ hardening calcium phosphate bone graft substitutes. Clinical Oral Implants Research doi: /j x. Schropp, L., Wenzel, A., Kostopoulos, L. & Karring, T. (2003) Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. The International journal of periodontics & restorative dentistry 23, Serino, G., Biancu, S., Iezzi, G. & Piattelli, A. (2003) Ridge preservation following tooth extraction using a polylactide and polyglycolide sponge as space filler: a clinical and histological study in humans. Clinical Oral Implants Research 14, Tallgren, A. (1969) Positional changes of complete dentures. A 7-year longitudinal study. Acta Odontologica Scandinavica 27, Tan, W. L., Wong, T. L., Wong, M. C. & Lang, N. P. (2012) A systematic review of postextractional alveolar hard and soft tissue dimensional changes in humans. Clinical Oral Implants Research 23(Suppl 5), Van der Weijden, F., Dell Acqua, F. & Slot, D. E. (2009) Alveolar bone dimensional changes of post-extraction sockets in humans: a systematic review. Journal of Clinical Periodontology 36, Vignoletti, F., Matesanz, P., Rodrigo, D., Figuero, E., Martin, C. & Sanz, M. (2012) Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clinical Oral Implants Research 23(Suppl 5), Watt, D. M. & Likeman, P. R. (1974) Morphological changes in the denture bearing area following the extraction of maxillary teeth. British Dental Journal 136, Address: Ronald E. Jung Clinic of Fixed and Removable Prosthodontics and Dental Material Science Center of Dental Medicine, University of Zurich Plattenstrasse 11 CH-8032 Zurich, Switzerland ronald.jung@zzm.uzh.ch Clinical Relevance Scientific rationale for the study: A variety of clinical, histological and morphological changes occur following tooth extraction. These changes may complicate potential implant therapy. Clinicians and patients may therefore benefit from effective ridge preservation techniques. Principal findings: The dimensional changes following tooth extraction and subsequent ridge preservation varied extensively in both, horizontal and a vertical direction. The application of a slowly resorbing biomaterial covered with either autogenous soft tissue punch or a collagen matrix revealed the least contraction of the extraction socket over 6 months. Practical implications: Ridge preservation without raising a flap and using a biomaterial with a socket seal can substantially limit the dimensional changes of the extraction socket compared with spontaneous healing. However, complete preservation of the original anatomical borders still seems unpredictable.
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction?
 C L I N I C A L Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction? Johan Hartshorne 1 Summary Systematic review conclusion:
C L I N I C A L Is alveolar ridge preservation (socket grafting) an effective therapy to preserve physiologic bone loss after tooth extraction? Johan Hartshorne 1 Summary Systematic review conclusion:
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
SOCKET PRESERVATION AND TECHNIQUES AN EVALUATION OF THE LITERATURE
 SOCKET PRESERVATION AND TECHNIQUES AN EVALUATION OF THE LITERATURE Raghav Khandelwal, DMD Highland General Hospital Assistant Program Director: Ben Shimel, DDS Program Director/Chair: Chan Park, DDS,MD
SOCKET PRESERVATION AND TECHNIQUES AN EVALUATION OF THE LITERATURE Raghav Khandelwal, DMD Highland General Hospital Assistant Program Director: Ben Shimel, DDS Program Director/Chair: Chan Park, DDS,MD
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Dimensional ridge alterations following tooth extraction. An experimental study in the dog
 J Clin Periodontol 2005; 32: 212 218 doi: 10.1111/j.1600-051X.2005.00642.x Copyright r Blackwell Munksgaard 2005 Dimensional ridge alterations following tooth extraction. An experimental study in the dog
J Clin Periodontol 2005; 32: 212 218 doi: 10.1111/j.1600-051X.2005.00642.x Copyright r Blackwell Munksgaard 2005 Dimensional ridge alterations following tooth extraction. An experimental study in the dog
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Clinical cases by Dr. Fernando Rojas-Vizcaya. botiss. dental bone & tissue regeneration. biomaterials. strictly biologic
 Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
The Socket Shield Technique A case Report
 The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012
 Alberto Sicilia Daniele Botticelli on behalf of Working Group 3 Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012 Authors affiliations: Alberto
Alberto Sicilia Daniele Botticelli on behalf of Working Group 3 Computer-guided implant therapy and soft- and hard-tissue aspects. The Third EAO Consensus Conference 2012 Authors affiliations: Alberto
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
Pressure Bearing Device Affects Extraction Socket Remodeling of Maxillary Anterior Tooth. A Prospective Clinical Trial
 Pressure Bearing Device Affects Extraction Socket Remodeling of Maxillary Anterior Tooth. A Prospective Clinical Trial Xi Jiang, DMD;* Yu Zhang, DMD; Bo Chen, DMD; Ye Lin, DMD ABSTRACT Background: Extraction
Pressure Bearing Device Affects Extraction Socket Remodeling of Maxillary Anterior Tooth. A Prospective Clinical Trial Xi Jiang, DMD;* Yu Zhang, DMD; Bo Chen, DMD; Ye Lin, DMD ABSTRACT Background: Extraction
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Conventional immediate implant placement and immediate placement with socket-shield technique Which is better
 International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
Saudi Journal of Oral and Dental Research. DOI: /sjodr ISSN (Print)
 Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online) A Clinical and Histomorphometric
Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online) A Clinical and Histomorphometric
Ridge preservation in a case of severe periodontitis
 Ridge preservation in a case of severe periodontitis Roberto Rossi, Ulf Nannmark, Andrea Pilloni and Nino Squadrito demonstrate how to preserve and condition the soft tissue with a combined approach Periodontal
Ridge preservation in a case of severe periodontitis Roberto Rossi, Ulf Nannmark, Andrea Pilloni and Nino Squadrito demonstrate how to preserve and condition the soft tissue with a combined approach Periodontal
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Dental Research Journal
 Dental Research Journal Original Article Clinical and biometrical evaluation of socket preservation using demineralized freeze dried bone allograft with and without the palatal connective tissue as a biologic
Dental Research Journal Original Article Clinical and biometrical evaluation of socket preservation using demineralized freeze dried bone allograft with and without the palatal connective tissue as a biologic
It is now well-known that tooth loss results in a loss of
 CASE LETTER Sliding Full-Thickness Pedicle Flap for Primary Wound Closure of the Socket Preservation Site Shane J. J. McCrea, MMedSci, MSc, BDS INTRODUCTION It is now well-known that tooth loss results
CASE LETTER Sliding Full-Thickness Pedicle Flap for Primary Wound Closure of the Socket Preservation Site Shane J. J. McCrea, MMedSci, MSc, BDS INTRODUCTION It is now well-known that tooth loss results
Effect of Single and Contiguous Teeth Extractions on Alveolar Bone Remodeling: A Study in Dogscid_
 Effect of Single and Contiguous Teeth Extractions on Alveolar Bone Remodeling: A Study in Dogscid_403 1..7 Mansour Al-Askar, MSc;* Rory O Neill, MS; Paul C. Stark, ScD; Terrence Griffin, DMD; Fawad Javed,
Effect of Single and Contiguous Teeth Extractions on Alveolar Bone Remodeling: A Study in Dogscid_403 1..7 Mansour Al-Askar, MSc;* Rory O Neill, MS; Paul C. Stark, ScD; Terrence Griffin, DMD; Fawad Javed,
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
Clinical and histological. evaluation of a flapless socket preservation procedure:
 Clinical and histological evaluation of a flapless socket preservation procedure: A prospective single cohort study Abstract Objective Valentina Borgia, * Fortunato Alfonsi, Paolo Tonelli, Lorenzo Bertelli,
Clinical and histological evaluation of a flapless socket preservation procedure: A prospective single cohort study Abstract Objective Valentina Borgia, * Fortunato Alfonsi, Paolo Tonelli, Lorenzo Bertelli,
Benefits of CBCT in Implant Planning
 10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Surgical soft tissue improvement in the course of implant therapy
 C L I N I C A L Surgical soft tissue improvement in the course of implant therapy Daniel Bäumer 1, Otto Zuhr 2, Markus Hürzeler 3 Abstract Soft tissue management has become a crucial part of implant therapy
C L I N I C A L Surgical soft tissue improvement in the course of implant therapy Daniel Bäumer 1, Otto Zuhr 2, Markus Hürzeler 3 Abstract Soft tissue management has become a crucial part of implant therapy
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Early implant placement: 3D radiographic study on the fate of buccal wall
 Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
DDS, resident of Periodontology, School of Dentistry, Isfahan University of Medical Sciences, Isfahan, Iran INTRODUCTION
 A comparative study of ridge preservation using calcium sulfate and collagen membrane with and without freeze-dried bone allograft following tooth extraction REZA AMIRZARGAR 1, GHOLAMREZA SHIRANI 2, HAMID
A comparative study of ridge preservation using calcium sulfate and collagen membrane with and without freeze-dried bone allograft following tooth extraction REZA AMIRZARGAR 1, GHOLAMREZA SHIRANI 2, HAMID
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
SIdP Sessione Premio H.M. Goldman 2019 SIdP H.M. Goldman Award 2019 Session 19 th International Congress
 THE EFFECT OF IMMEDIATE IMPLANT PLACEMENT ON AL VEOLAR RIDGE PRESERVATION: RADIOGRAPHIC RESULTS OF A RANDOMIZED CONTROLLED CLINICAL TRIAL COM PARING THESE TWO TREATMENT MODALITIES AND NATU RAL HEALING
THE EFFECT OF IMMEDIATE IMPLANT PLACEMENT ON AL VEOLAR RIDGE PRESERVATION: RADIOGRAPHIC RESULTS OF A RANDOMIZED CONTROLLED CLINICAL TRIAL COM PARING THESE TWO TREATMENT MODALITIES AND NATU RAL HEALING
Limited bone availability makes implant placement challenging
 Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
Ridge preservation: what is it and when should it be considered
 REVIEW Australian Dental Journal 2008; 53: 11 21 doi:10.1111/j.1834-7819.2007.00008.x Ridge preservation: what is it and when should it be considered I Darby,* S Chen,* R De Poi* *School of Dental Science,
REVIEW Australian Dental Journal 2008; 53: 11 21 doi:10.1111/j.1834-7819.2007.00008.x Ridge preservation: what is it and when should it be considered I Darby,* S Chen,* R De Poi* *School of Dental Science,
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement
 Guy Huynh-Ba Bjarni E. Pjetursson Mariano Sanz Denis Cecchinato Jorge Ferrus Jan Lindhe Niklaus P. Lang Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant
Guy Huynh-Ba Bjarni E. Pjetursson Mariano Sanz Denis Cecchinato Jorge Ferrus Jan Lindhe Niklaus P. Lang Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Identification and Efficacy Ranking of Allograft and Xenograft for Extraction and Ridge Preservation Procedures
 e253 Identification and Efficacy Ranking of and for and Ridge Preservation Procedures 1 Department of Dental Public Health, Faculty of Dentistry, King Abdulaziz University, Jeddah, Saudi Arabia. Zuhair
e253 Identification and Efficacy Ranking of and for and Ridge Preservation Procedures 1 Department of Dental Public Health, Faculty of Dentistry, King Abdulaziz University, Jeddah, Saudi Arabia. Zuhair
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
Clinical Success. with the Proven. Clinical Success. with the Proven Bone Substitute Products
 Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
The alternative to connective tissue grafts. Geistlich Fibro-Gide
 The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
SOLUTIONS AFTER TOOTH EXTRACTION
 SOLUTIONS AFTER TOOTH EXTRACTION CONTENT GEISTLICH EXPERTISE FOR EASY AND PREDICTABLE REGENERATIVE DENTISTRY The alveolar ridge loses volume in conventional therapy 4 Geistlich Biomaterials offer a predictable
SOLUTIONS AFTER TOOTH EXTRACTION CONTENT GEISTLICH EXPERTISE FOR EASY AND PREDICTABLE REGENERATIVE DENTISTRY The alveolar ridge loses volume in conventional therapy 4 Geistlich Biomaterials offer a predictable
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
easy-graft TM CRYSTAL
 1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction.
 Biomedical Research 2017; 28 (12): 5402-5407 ISSN 0970-938X www.biomedres.info Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction. Tao Wang
Biomedical Research 2017; 28 (12): 5402-5407 ISSN 0970-938X www.biomedres.info Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction. Tao Wang
The International Journal of Periodontics & Restorative Dentistry
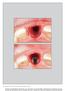 The International Journal of Periodontics & Restorative Dentistry 401 Guidelines for Selecting the Implant Diameter During Immediate Implant Placement of a Fresh Extraction Socket: A Case Series Ariádene
The International Journal of Periodontics & Restorative Dentistry 401 Guidelines for Selecting the Implant Diameter During Immediate Implant Placement of a Fresh Extraction Socket: A Case Series Ariádene
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Extraction socket preservation using β tricalcium phosphate bone graft plug and platelet rich fibrin membrane A case series
 2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
PROSPECTIVE, COMPARATIVE VOLUMETRIC ASSESSMENT OF ALVEOLAR RIDGE PRESERVATION UTILIZING DIFFERENT BONE GRAFTING MATERIALS. David Paul Semeniuk
 PROSPECTIVE, COMPARATIVE VOLUMETRIC ASSESSMENT OF ALVEOLAR RIDGE PRESERVATION UTILIZING DIFFERENT BONE GRAFTING MATERIALS David Paul Semeniuk A thesis submitted to the faculty at the University of North
PROSPECTIVE, COMPARATIVE VOLUMETRIC ASSESSMENT OF ALVEOLAR RIDGE PRESERVATION UTILIZING DIFFERENT BONE GRAFTING MATERIALS David Paul Semeniuk A thesis submitted to the faculty at the University of North
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
We want to keep you smiling. Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Original Article Conventional extraction vs. enucleation in anterior maxillary sites: a pilot study in humans
 Int J Clin Exp Med 2017;10(2):2147-2155 www.ijcem.com /ISSN:1940-5901/IJCEM0018259 Original Article Conventional extraction vs. enucleation in anterior maxillary sites: a pilot study in humans Oscar A
Int J Clin Exp Med 2017;10(2):2147-2155 www.ijcem.com /ISSN:1940-5901/IJCEM0018259 Original Article Conventional extraction vs. enucleation in anterior maxillary sites: a pilot study in humans Oscar A
TOPICS. T O P I C S Day 1. Implant Locations. Implant Placement in the Posterior Maxilla. Anatomy and risk factors Option 1: Short implants
 T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Workshop 1 - Ideal time for implant placement: immediate, early or delayed. Adriana Ramos Yannuzzi 1
 Workshop 1 - Ideal time for implant placement: immediate, early or delayed Adriana Ramos Yannuzzi 1 1 Assistant Prof. Department of Occlusion and Prosthodontics. Professor at the Specialization Course
Workshop 1 - Ideal time for implant placement: immediate, early or delayed Adriana Ramos Yannuzzi 1 1 Assistant Prof. Department of Occlusion and Prosthodontics. Professor at the Specialization Course
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Soft-Tissue Solutions from The Collagen Expert. Clinical Success with the Proven. Geistlich Mucograft Geistlich Mucograft Seal Geistlich Fibro-Gide
 Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
original article Abstract
 original article A Review on Alveolar Ridge Preservation Following Tooth Extraction Robert Horowitz, DDS, 1 Danny Holtzclaw, DMD, MS, 2 Paul S. Rosen, DMD, MS 3 Abstract Context The question that clinicians
original article A Review on Alveolar Ridge Preservation Following Tooth Extraction Robert Horowitz, DDS, 1 Danny Holtzclaw, DMD, MS, 2 Paul S. Rosen, DMD, MS 3 Abstract Context The question that clinicians
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Dimensional changes of the alveolar ridge contour after different socket preservation techniques
 J Clin Periodontol 2008; 35: 906 913 doi: 10.1111/j.1600-051X.2008.01305.x Dimensional changes of the alveolar ridge contour after different socket preservation techniques Fickl S, Zuhr O, Wachtel H, Stappert
J Clin Periodontol 2008; 35: 906 913 doi: 10.1111/j.1600-051X.2008.01305.x Dimensional changes of the alveolar ridge contour after different socket preservation techniques Fickl S, Zuhr O, Wachtel H, Stappert
