The Impact of Brief Parental Anxiety Management on Child Anxiety Treatment Outcomes: A Controlled Trial
|
|
|
- Moris Casey
- 5 years ago
- Views:
Transcription
1 Journal of Clinical Child & Adolescent Psychology, 43(3), , 2014 Published with license by Taylor & Francis ISSN: print= online DOI: / The Impact of Brief Parental Anxiety Management on Child Anxiety Treatment Outcomes: A Controlled Trial Jennifer L. Hudson, Carol Newall, Ronald M. Rapee, Heidi J. Lyneham, Carolyn C. Schniering, Viviana M. Wuthrich, Sophie Schneider, Elizabeth Seeley-Wait, Susan Edwards, and Natalie S. Gar Centre for Emotional Health, Department of Psychology, Macquarie University Parental anxiety is a risk to optimal treatment outcomes for childhood anxiety disorders. The current trial examined whether the addition of a brief parental anxiety management (BPAM) program to family cognitive behavioral therapy (CBT) was more efficacious than family CBT-only in treating childhood anxiety disorders. Two hundred nine children (aged 6 13 years, 104 female, 90% Caucasian) with a principal anxiety disorder were randomly allocated to family CBT with a five-session program of BPAM (n ¼ 109) or family CBT-only (n ¼ 100). Family CBT comprised the Cool Kids program, a structured 12-week program that included both mothers and fathers. Overall, results revealed that the addition of BPAM did not significantly improve outcomes for the child or the parent compared to the CBT-only group at posttreatment or 6-month follow-up. Overall, however, children with nonanxious parents were more likely to be diagnosis free for any anxiety disorder compared to children with anxious parents at posttreatment and 6-month follow-up. BPAM did not produce greater reductions in parental anxiety. The results support previous findings that parent anxiety confers poorer treatment outcomes for childhood anxiety disorders. Nevertheless the addition of BPAM anxiety management for parents in its current format did not lead to additional improvements when used as an adjunct to family CBT in the treatment of the child s anxiety disorder. Future benefits may come from more powerful methods of reducing parents anxiety. Empirical data support the efficacy of cognitive behavioral therapy (CBT) for anxious youth (Cartwright- Hatton, Roberts, Chitsabesan, Fothergill, & Harrington, 2004). Despite its efficacy, the remission rate following CBT is 56.5% in anxious youth, and it is clear that a # Jennifer L. Hudson, Carol Newall, Ronald M. Rapee, Heidi J. Lyneham, Carolyn C. Schniering, Viviana M. Wuthrich, Sophie Schneider, Elizabeth Seeley-Wait, Susan Edwards, and Natalie S. Gar We are with the Centre for Emotional Health, Department of Psychology, Macquarie University. This research was supported by the National Health and Medical Research Council (382008). We thank Dr Alan Taylor for assisting with the statistical analyses. We also thank the staff and therapists at the Emotional Health Clinic in collecting these data. Clinical trial registration information Australian New Zealand Clinical Trials Registry URL: Correspondence should be addressed to Jennifer L. Hudson, Centre for Emotional Health, Department of Psychology, Macquarie University, NSW 2109, Australia. jennie.hudson@mq.edu.au significant proportion of children and adolescents do not respond to CBT. An important challenge for clinical researchers is the identification of risk factors that impede optimal treatment response, and in targeting these factors, enhance outcomes for anxious youth. There has been growing interest in the contribution of parental anxiety to treatment outcomes of the anxious child. This interest has been guided by studies implicating a significant positive association between child and parent anxiety (Last, Hersen, Kazdin, Francis, & Grubb, 1987; Rapee, Schniering, & Hudson, 2009; Silverman, Kurtines, Jaccard, & Pina, 2009). Moreover, there has been some evidence that the presence of untreated parental anxiety poses a significant risk to the successful short-term outcome of child-focused CBT for anxiety disorders. For example, in a large-scale clinical trial, only 38.9% of children were diagnosis free if they had one anxious parent compared to 82.4% of children without
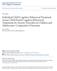
2 BRIEF PARENTAL ANXIETY MANAGEMENT 371 anxious parents who were diagnosis free at the end of treatment (Cobham, Dadds, & Spence, 1998). Another study also demonstrated that maternal anxiety obstructed optimal treatment outcomes for the child at 1-year follow-up (Kendall, Hudson, Gosch, Flannery- Schroeder, & Suveg, 2008). A small number of studies have emerged that have concurrently targeted parental anxiety in the treatment of anxious youth (Creswell, Willetts, Murray, Singhal, & Cooper, 2008). Cobham et al. (1998) demonstrated that the addition of Parent Anxiety Management (PAM) to child CBT enhanced posttreatment diagnostic outcomes compared to child CBT without PAM, but only for children with at least one anxious parent. Of interest, this favorable result for the inclusion of PAM was not maintained at 6- and 12-month follow-up and was not apparent on any measure aside from diagnostic status. However, at the 3-year follow-up, the provision of PAM conferred significant benefits regardless of parental anxiety status. That is, children in the PAM þ CBT group were more likely to be diagnosis free compared to children in the CBT-only group even if their parent was not anxious. A key limitation of this study was the reliance on self-report questionnaire measures to determine parental anxiety. The use of self-report measures is problematic for a number of reasons: (a) Parents of anxious children tend to underreport their own anxiety symptoms, potentially due to feelings of guilt that is associated with feeling responsible for the child s anxiety (Kendall & Suveg, 2006), and (b) self-report measures of anxiety tend to be less objective than clinical interviews (Bogels & Brechman-Toussaint, 2006). The current study investigated whether adding a brief treatment for parent anxiety would enhance the efficacy of standard family CBT for anxious children. We hypothesized that the inclusion of a brief PAM (BPAM) would enhance treatment outcomes only for anxious children with at least one clinically anxious parent. The current study included the following improvements on previous studies: (a) the sample allowed sufficient power to detect a moderate effect size difference between groups, and (b) parent anxiety was determined through diagnostic interviews at pretreatment, posttreatment, and 6month follow-up. The addition of BPAM to family CBT was expected to be superior to family CBT alone in terms of (a) diagnostic outcomes and clinical severity gleaned from posttreatment diagnostic status and (b) symptom change based on parent- and child-reported anxiety symptoms. METHOD Participants Participants in the study were 209 children and their parents seeking psychological treatment for the child s anxiety. Eligible children were aged 6 to 13 years and met criteria for a principal (most impairing) anxiety disorder according to Diagnostic and Statistical Manual of Mental Disorders (4th ed. [DSM IV]). Anxiety disorders were assessed using the Anxiety Disorders Interview Schedule for DSM-IV, Child and Parent Versions (Silverman & Albano, 1996). Exclusion criteria included intellectual and developmental disability, psychoses, disabling medical conditions, and concurrent psychological treatment. Parents who were identified during the assessment as having a psychological disorder were asked to delay any treatment until after the study was complete. Children on medication for anxiety or depression were included (n ¼ 12) if the dose was stable for 2 weeks during treatment. Adolescents (12 13 years) with comorbid major depression were referred to an alternate program (n ¼ 3). Children with comorbid behavioral disorders who had a clinical severity rating (CSR) of 6 or more were excluded. Figure 1 presents the flow of participants through the study. Measures Child Psychopathology Structured interview. Children and parents were interviewed using the Anxiety Disorder Interview Schedule for Children Child and Parent version (ADIS-IV-C=P; Silverman & Albano, 1996). Diagnoses and CSRs (on a scale of 0 to 8) were assigned by graduate students in clinical psychology or qualified clinical psychologists based on composite parent and child report. A severity of 4 or more on the CSR indicated that diagnostic criteria were met at a clinically interfering level. 1 Clinicians were trained to match anxiety diagnoses within one severity rating of each other. Fifteen participants were double coded for reliability purposes. The intraclass correlation for the total CSR among clinicians was.83. Interrater reliability (kappa) for the presence of a disorder in the child s profile was.84 for the presence of a principal anxiety diagnosis and.82 for any anxiety diagnosis. Anxiety symptoms. The Spence Children s Anxiety Scale (Spence, 1998) was used to assess child- and motherreported anxiety symptoms. This measure contains 38 items that load on a single factor (range ¼ 0 114). Internal consistency and retest reliability are good (Nauta et al., 2004; Spence, 1998). The measure distinguishes anxious and nonclinical children and has adequate convergent validity. The internal consistency in the current 1 The or rule was used, that is, a diagnosis was assigned when reported by either parent or child (unless the rule would result in duplicating symptoms in two diagnoses, in which case clinical judgment was used).
3 372 HUDSON ET AL. FIGURE 1 Flow of participants through the clinical trial. Note: CBT ¼ child and family cognitive-behavioral therapy; BPAM ¼ CBT and parental anxiety management program. sample was good to excellent (mother report a ¼.88; child report a ¼.91). Parent Psychopathology Structured interview. Parental anxiety was assessed using the ADIS-IV (Brown, Di Nardo, & Barlow, 1994). The ADIS-IV is a semistructured clinical interview for assessing anxiety disorders and other diagnoses in adults according to DSM-IV criteria. Again, a CSR of 4 or more indicated the presence of a clinical disorder. The child was considered to have an anxious parent if one or both parents met criteria for an anxiety disorder. A total of 16 parents were double coded for reliability purposes. The intraclass correlation for the total CSR was.93. Interrater reliability (kappa) for the presence of a disorder in the parent s profile was.85 for the presence of a principal anxiety diagnosis and.85 for any anxiety diagnosis. Depression anxiety stress scales 21 items (DASS-21; lovibond & lovibond, 1995). Parents completed the DASS-21 to assess for current parental anxiety symptoms via the anxiety subscale (scores 7 and below are considered within the range of normal). The DASS-21 has demonstrated good internal consistency and concurrent validity (Antony, Bieling, Cox, Enns, & Swinson, 1998). The internal consistency for the current sample of mothers and fathers on the DASS Anxiety subscale were moderate (mother report a ¼.77; father report a ¼.71). Treatment Conditions Treatments for child anxiety were conducted in groups in ten 2-hr, weekly sessions. In each session, the therapist spent roughly equal time with the children, parent(s), and parents and children together. Children (n ¼ 5 7) were allocated to a group based on age, resulting in groups of children with a range of different anxiety disorders. All treatment sessions were audiotaped for reliability purposes. The primary therapist for each group (n ¼ 10) was a paid clinical psychologist or a postgraduate clinical
4 BRIEF PARENTAL ANXIETY MANAGEMENT 373 student. Training and weekly supervision was provided by the clinic director or the first author. CBT Group The CBT condition used the Cool Kids program, which has established efficacy (e.g., Hudson et al., 2009). The manual-based program is designed for the management of broad-based childhood anxiety disorders and includes psychoeducation, cognitive restructuring, gradual exposure, child management skills, and assertiveness training. The primary focus of most sessions is on the development and evaluation of the gradual exposure and use of other strategies to support exposure. With the exception of one therapist-assisted in-group session of in vivo exposure, children completed gradual exposure under the direction of their parents for homework. Any discussion of parental anxiety was removed from the treatment manual and all treatment focused on the child s anxiety and not on the parent s. BPAM Group The BPAM group completed the Cool Kids program in an identical format to the CBT group and in addition received five 45-min sessions of BPAM training. The parental anxiety management program comprised of a bibliotherapy program supplemented with five therapistled group-based sessions. 2 Parents received extensive printed materials describing strategies and were encouraged by therapists to engage in extensive home practices. The program included psychoeducation about anxiety, cognitive restructuring, gradual exposure, assertiveness, problem-solving skills, and time management. The main aim of the BPAM component was to teach parents to manage their anxiety via CBT techniques. Three of the BPAM sessions focused on gradual exposure. Parents were given individualized attention in planning exposures at home. Therapist time spent treating the child s anxiety was matched for both treatment conditions. BPAM parents received additional therapist time focused on their own anxiety (with a different therapist). BPAM sessions were held during the time the Cool Kids therapist was working with the children and parents would usually be in the waiting room (45 55 min). Treatment Integrity Treatment integrity was assessed in a random sample of 20% of therapy sessions using the observer-rated Protocol Adherence Checklist Modified (Southam-Gerow & Kendall, 2002), adapted for each condition. Therapists demonstrated an average of 96% adherence to the manual for Cool Kids and 92% in the BPAM program. 2 The manual is available from the authors. Procedure The ethical procedures of this study were approved by the Macquarie University Human Ethics Committee. After a brief telephone screen, parents signed consent forms at assessment, and the children provided verbal assent. Children who met criteria for inclusion and agreed to participate were allocated to a group based on the child s age. The first author used a schedule from a random number generator to assign each group to CBT (19 groups) or BPAM (19 groups) and to therapists. We encouraged both parents to attend wherever possible and provided child-minding services for siblings. Families completed a post- and 6-month follow-up assessment (ADIS-IV-C=P, ADIS-IV, and symptom measures for children and parents). Structured interviews were conducted by diagnosticians masked to condition. Postand follow-up diagnoses with a CSR less than 4 were considered remitted. Data Analyses Based on treatment allocation and parent diagnostic status, the study consisted of four groups as follows: BPAM þ Anxious Parent (n ¼ 74), CBT þ Anxious Parent (n ¼ 70), BPAM þ Non-anxious Parents (n ¼ 21), CBT þ Nonanxious Parents (n ¼ 24). The Anxious Parent groups comprised children who had two parents with an anxiety disorder (32%), an anxious mother only (55%), or an anxious father only (13%). Due to administrative error, 27% of parental attendance of treatment sessions in the BPAM condition was not recorded. However, of the mothers (n ¼ 68) and fathers (n ¼ 70) whose session attendance was recorded in the BPAM condition, 66 mothers (97%) and 57 fathers (81%) completed both the BPAM and CBT program. Missing diagnostic data for intent-to-treat was handled via the last-point-carried-forward method. Continuous data were analyzed using a stacked database (each line represented one observation for one participant). This method ensured that missing observation did not result in deletion of the participant (Peugh & Enders, 2005). Participants in the completer sample (N ¼ 189) included families in which the child and at least one parent completed a minimum of six sessions of the Cool Kids program, and for BPAM at least one of the parents must also have completed at least three sessions. 3 This yielded a final distribution of 94 children in the CBT group and 95 children in BPAM group. From the 3 As noted earlier, a portion of parental session attendance of treatment programs was not recorded. To manage this missing data without losing a substantial portion of our overall sample, parents whose session attendance was not recorded (n ¼ 61, about 29% of overall sample) but completed ADISes across all three time points were also considered treatment completers (n ¼ 45).
5 374 HUDSON ET AL. completer sample, 98% of anxious mothers (48 of 49) and 92% of anxious fathers (22 of 24) completed the BPAM program. The proportion of participants who no longer met criteria for the principal anxiety diagnosis and any anxiety diagnosis, at post- and 6-month follow-up in the two conditions, was examined using chi-square tests of independence. Mixed models containing random factors for subject and fixed effects for treatment group, parental anxiety status at pre-, and time (including two- and three-way interactions) were fitted to measures of childand mother-reported symptoms and diagnostic severity. RESULTS Attrition Treatment completers were compared to attrition cases on sociodemographic, diagnostic, and pretreatment measures. Children who dropped out of treatment were older than treatment completers (completers: M ¼ 9.5 years, SD ¼ 2.0; attrition cases: M ¼ 10.47, SD ¼ 1.84), t(202) ¼ 2.01, p <.05. No other significant differences between attrition cases and completers were detected (p <.05). Pretreatment Comparisons The treatment groups were examined for pretreatment differences on demographic variables via a series of chisquare tests and 2 (anxious vs. nonanxious parents) 2 (BPAM vs. CBT) univariate analyses of variance. There were no significant pretreatment differences between the groups on family sociodemographic variables (see Table 1). Results showed that there were significantly more children with externalizing disorders among nonanxious parents (17 of 45, or 37.8%) compared to anxious parents (29 of 144, or 20.1%; v 2 (1, N ¼ 189) ¼ 5.79, p <.05. There were no other pretreatment differences for the children between groups (Table 1). Pretreatment scores on questionnaires were examined via two-way analysis of variance. There was a main effect of parental anxiety status at pretreatment on the maternal DASS Anxiety subscale, F(1, 181) ¼ 7.71, p <.05. No other significant main effects or interactions were observed for any of the remaining questionnaires at pretreatment. Mixed-model analyses were conducted to determine whether therapy group 4 and therapist were significant sources of variation on the main outcome variables. 4 Note that therapy group refers to the group to which the child was allocated based on age and not the treatment condition. Hence age was entered as a covariate when examining cluster effects. Results revealed that there was no clustering (all ps >.05) and the median intraclass correlation was zero, ranging from 0 to.06. Thus therapy group and therapist were not a significant source of variation and could be disregarded. Diagnostic Changes at Posttreatment and Follow-Up Across Conditions Child Diagnostic Status The proportion of children who were free of their principal anxiety disorder and any anxiety disorders at posttreatment and follow-up is shown in Table 2. At posttreatment, no significant main effects for treatment condition (CBT vs. BPAM) or parental anxiety status (anxious vs. nonanxious parents at pretreatment) were found for principal anxiety diagnosis. That is, there were no differences in remission rates of principal diagnoses at posttreatment between CBT and BPAM and no difference in remission rates for children with anxious and nonanxious parents. When any anxiety diagnosis was taken into consideration at posttreatment, there was a main effect for parental anxiety status. That is, the percentage of children who were free of any anxiety diagnosis was significantly greater in the nonanxious parents group (14 of 45, or 31.1%) than in the anxious parents group (24 of 138, or 17.4%), v 2 (1, N ¼ 183) ¼ 3.88, p <.05. No other significant differences were found for any anxiety diagnosis at posttreatment. A similar picture was found at the 6-month follow-up. No main effects were found for treatment group (CBT vs. BPAM) or parental anxiety status (anxious vs. nonanxious parents) for principal anxiety diagnosis. Again, when any anxiety diagnosis was taken into account at 6-month follow-up, children with nonanxious parents were significantly more likely to be diagnosis free (19 of 43, or 44.2%) compared to children with anxious parents (35 of 126, 27.8%) at follow-up, v 2 (1, N ¼ 190) ¼ 3.97, p <.05. No other significant effects for principal diagnosis or any anxiety diagnoses were found at follow-up. Intent-to-treat analyses produced comparable results for all chi-square analyses previously reported, with the exception that the main effect of parental anxiety status at the 6-month follow-up for any anxiety diagnosis revealed a trend rather than significance, v 2 (1, N ¼ 204) ¼ 3.67, p ¼.058. Parental Diagnostic Status We examined whether treatment group affected maternal and paternal anxiety diagnostic status at postand 6-month follow-up for anxious parents. Anxious parents were defined as parents with any anxiety
6 BRIEF PARENTAL ANXIETY MANAGEMENT 375 TABLE 1 Demographic Data Across Conditions (Standard Deviations) in Treatment Completers Demographic Anxious Parent þ BPAM a Anxious Parent þ CBT b Nonanxious Parent þ BPAM c Non-Anxious Parent þ CBT d Child Sex, % Female Children s M Age 9.2 (2.0) 9.6 (2.0) 9.6 (2.0) 9.5 (2.0) Family Income, % > $80, $40,000 80, $20, , $0 20, No. of Siblings 1.6 (0.9) 1.3 (0.9) 1.3 (0.7) 1.4 (.9) Ethnicity e,% Australian Asian=Asian Australian European=European Australian American=American Australian Other Family Makeup, % Two Parent Single Parent Stepparents=Blended Mothers M Age 41.2 (5.0) 41.1 (5.2) 41.8 (5.5) 42.6 (5.4) Mothers Education Level, % School Certificate Higher School Certificate TAFE=Apprenticeship Certificate=Diploma Undergraduate Degree Postgraduate Degree Mothers Employment Status Stay-at-Home Parent Full-Time Student Unemployed=Illness Part-Time Work Full-Time Work Retired Fathers M Age 43.2 (5.2) 42.7 (6.7) 44.6 (6.7) 45 (4.0) Fathers Education Level Primary School School Certificate Higher School Certificate TAFE=Apprenticeship Certificate=Diploma Undergraduate Degree Postgraduate Degree Fathers Employment Status Stay-at-Home Parent Unemployed=Illness Part-Time Work Full-Time Work Retired Children s Principal Diagnoses, % GAD SOC SAD PD OCD SPEC PTSD ADNOS Children s Comorbid Diagnoses (%) f (Continued )
7 376 HUDSON ET AL. TABLE 1 Continued Demographic Anxious Parent þ BPAM a Anxious Parent þ CBT b Nonanxious Parent þ BPAM c Non-Anxious Parent þ CBT d Anxiety Externalizing Mood Disorders Other g No Comorbidity No. of Comorbid Diagnoses 3.0 (1.7) 2.7 (1.6) 2.3 (1.4) 2.8 (1.6) Maternal Principal Diagnoses, % GAD NA NA SOC NA NA PD NA NA OCD NA NA SPEC NA NA PTSD NA NA Mood Disorder Paternal Principal Diagnoses, % GAD NA NA SOC NA NA SPEC NA NA OCD NA NA Mood Disorder Other h Note: BPAM ¼ parent anxiety management and cognitive-behavioral therapy; CBT ¼ cognitive-behavioral therapy; GAD ¼ generalized anxiety disorder; OCD ¼ obsessive-compulsive disorder; PD ¼ panic disorder; SAD ¼ separation anxiety disorder; SOC ¼ social phobia; SPEC ¼ specific phobia; PTSD ¼ post-traumatic stress disorder; ADNOS ¼ anxiety disorder not otherwise specified. a n ¼ 74. b n ¼ 70. c n ¼ 21. d n ¼ 24. e Parents were asked to record their ethnicity in an open-ended question. The majority of our participants identify as Australian. A smaller portion of families identify as Northwest, Southern, or Eastern European (e.g., Italian, Croatian Australian) or Southeast, Northeast, Southern, or Central Asian (Thai, Chinese Australian) heritage. f Comorbid diagnoses represent all secondary disorders with a CSR of 4 or greater in the child s diagnostic profile. g Other childhood disorders included selective mutism (n ¼ 1), developmental disability (n ¼ 1), and enuresis (n ¼ 3). h Other paternal disorders included adjustment disorder (n ¼ 2), hypochondriasis (n ¼ 1), ADHD (n ¼ 1), alcohol abuse=dependence (n ¼ 1), obsessive compulsive personality disorder (n ¼ 1), and insomnia (n ¼ 1). TABLE 2 The Proportion of Children No Longer Meeting Criteria for Principal Anxiety Diagnosis and Any Anxiety Diagnoses at Posttreatment and Follow-Up Across the Two Conditions in the Treatment Completer Sample Posttreatment Follow-Up Anxious Parent Nonanxious Parent Anxious Parent Nonanxious Parent BPAM a CBT b BPAM c CBT d BPAM e CBT f BPAM g CBT h Principal Diagnosis 33 (45.8) 22 (33.3) 9 (42.9) 13 (54.2) 35 (53.0) 31 (51.7) 11 (55.0) 13 (56.5) Any Anxiety Diagnoses 14 (19.4) 10 (15.2) 7 (33.3) 7 (29.2) 17 (25.8) 18 (30.0) 7 (35.0) 12 (52.2) Note: BPAM ¼ parent anxiety management and cognitive-behavioral therapy; CBT ¼ cognitive-behavioral therapy. a n ¼ 72. b n ¼ 66. c n ¼ 21. d n ¼ 24. e n ¼ 66. f n ¼ 60. g n ¼ 20. h n ¼ 23.
8 BRIEF PARENTAL ANXIETY MANAGEMENT 377 TABLE 3 Proportion of Anxious Parents No Longer Meeting Criteria for Principal Anxiety Diagnosis and Any Anxiety Diagnoses at Posttreatment and Follow-Up Across the Two Conditions in the Completer Sample Posttreatment Follow-Up Maternal Paternal Maternal Paternal BPAM a CBT b BPAM c CBT d BPAM e n (%) CBT f BPAM g CBT h Principal Anxiety Diagnosis 22 (35.5) 18 (32.7) 15 (51.7) 11 (34.4) 23 (45.1) 18 (36.0) 15 (57.7) 15 (51.7) Any Anxiety Diagnoses 16 (26.2) 11 (20.0) 6 (20.7) 6 (18.8) 12 (23.5) 12 (24.0) 8 (30.8) 11 (37.9) Note: BPAM ¼ parent anxiety management and cognitive-behavioral therapy; CBT ¼ cognitive-behavioral therapy. a n ¼ 61. b n ¼ 55. c n ¼ 29. d n ¼ 32. e n ¼ 51. f n ¼ 50. g n ¼ 26. h n ¼ 29. diagnosis (CSR >4) at pretreatment. The proportion of anxious mothers and fathers who were diagnosis free at posttreatment and follow-up is shown in Table 3. Results indicated that anxious mothers and fathers assigned to the BPAM treatment group were not significantly different from those in the CBT group at posttreatment or follow-up on principal or any anxiety diagnosis (ps >.05). Symptoms Measures and Diagnostic Severity Across Time and Condition Mixed-model analyses were fitted to clinical severity ratings (principal diagnosis, any anxiety diagnoses) and symptoms (child and mother report). The CSR for any anxiety diagnosis was summed across all anxiety diagnoses to give a total anxiety severity. As can be seen in Table 4, there was a significant main effect for time. All measures observed a significant improvement from pre- to posttreatment and from pretreatment to 6mth follow-up. Only the CSR (principal) showed continued improvements from posttreatment to follow-up. In addition, there was a significant parent anxiety status effect for maternal anxiety (Table 4): Maternal anxiety was higher in the anxious parent groups than the nonanxious parent groups regardless of time or condition. 5 DISCUSSION The results of the current study indicate that the addition of a specific treatment component aimed at 5 Intent-to-treat analyses produced comparable results for all outcomes reported in this section. parents anxiety to a standard family-based treatment for child anxiety did not enhance treatment outcomes for children, even among children who had a parent with an anxiety disorder. The diagnostic outcome for parental anxiety at posttreatment and follow-up provides the most parsimonious explanation for the results. Specifically, among anxious fathers and mothers, the provision of BPAM did not improve parental anxiety diagnoses at posttreatment and 6-month follow-up compared to anxious parents who did not receive BPAM, indicating that BPAM did not have its intended effects of reducing parental anxiety. Consistent with the diagnostic patterns, there were no differences in self-reported symptoms of parental anxiety between parents who received BPAM and those that did not, nor did BPAM interact with parental anxiety status to predict child anxiety treatment outcomes. These results are consistent with the finding from Cobham et al. (1998), who also failed to show significant reductions in parents anxiety following their anxiety management program. The lack of effects on parents anxiety is surprising given the extensive evidence that self-help programs augmented with therapist contact can provide highly efficacious treatment for adult anxiety disorders (Hirai & Clum, 2006). Although the current effects may reflect an insufficient dose of BPAM, it is also possible that they reflect additional complications in integrating parent and child treatment. Is it possible that parents were reluctant to work on their own anxiety when seeking treatment for their child, or were they too focused on helping their child to work on their own fears? These questions need to be examined in future studies. The lack of a significant benefit of BPAM is largely consistent with previous research (Cobham et al., 1998; Creswell et al., 2008). An apparent exception
9 TABLE 4 Means for Pretreatment, Posttreatment, and Follow-Up Data Across the Four Conditions in the Completer Sample CBT þ Anxious Parent CBT þ Non-Anxious Parent BPAM þ Anxious Parent BPAM þ Non-Anxious Parent Measure Pre M Post M 6-Month FU M Pre M Post M 6-Month FU M Pre M Post M 6-Month FU M Pre M Post M 6-Month FU M F and t Values CSR (Principal) 6.49 (.18) CSR (Anxiety Diagnosis) (.91) SCAS (Child) (1.77) SCAS (Mother) (1.43) DASS Anxiety Subscale (Mother) DASS Anxiety Subscale (Father) 7.31 (.65) 4.09 (.58) 4.36 (.18) (.92) (1.85) (1.52) 5.00 (.69) 3.21 (.60) 3.66 (.19) (.95) (1.93) (1.58) 5.06 (.71) 3.68 (.63) 6.46 (.30) (1.55) (3.04) (2.46) 3.56 (1.11) 4.69 (1.02) 3.71 (.30) (1.55) (3.08) (2.46) 2.97 (1.11) 3.21 (1.06) 3.08 (.31) 9.80 (1.56) (3.08) (2.50) 2.90 (1.13) 3.08 (1.08) 6.37 (.17) (.88) (1.72) (1.38) 6.38 (.63) 5.45 (.55) 3.78 (.17) (.89) (1.75) (1.41) 5.33 (.64) 4.17 (.56) 3.65 (.18) (.91) (1.87) (1.51) 4.04 (.68) 3.63 (.58) 6.10 (.32) (1.62) (3.25) (2.63) 4.13 (1.19) 2.19 (1.06) 4.05 (.32) (1.65) (3.21) (2.63) 2.14 (1.19) 1.65 (1.05) 3.45 (.33) (1.67) (3.36) (2.73) 1.96 (1.23) 1.56 (1.08) Time effect F (2, 352) ¼ , p <.01; t (349) ¼ 16.05, p ¼.00a; t (353) ¼ 19.30, p ¼.00b; t (353) ¼ 3.44, p ¼.00c Time effect F (2, 348) ¼ 92.50, p ¼.00; t (347) ¼ 10.74, p ¼.00a; t (348) ¼ 12.54, p ¼.00b; t (348) ¼ 2.01, nsc Time effect F (2, 311) ¼ 59.28, p ¼.00; t (310) ¼ 7.94, p ¼.00a, t (313) ¼ 10.35, p ¼.00b; t (311) ¼ 2.71, p ¼.01c Time effect F (2, 314) ¼ 86.88, p ¼.00; t (313) ¼ 10.24, p ¼.00a; t (317) ¼ 11.93, p ¼.00b; t (311) ¼ 2.33, p ¼.02c Time effect F (2, 316) ¼ 9.25, p ¼.00; t (316) ¼ 3.32, p ¼.00a; t (319) ¼ 4.01, p ¼.00b; t (314) ¼.08, nsc; Parental anxiety status effect, F (1, 179) ¼ 10.73, p ¼.00. Time effect F (2, 273) ¼ 6.37, p ¼.00;t (273) ¼ 3.03, p ¼.00a; t (276) ¼ 3.11, p ¼.00b; t (271) ¼.19, nsc Note: Pre ¼ pretreatment; Post ¼ posttreatment; FU ¼ follow-up; CSR principal ¼ Clinical Severity Rating for the child s principal diagnosis; CSR anxiety diagnosis ¼ summed Clinical Severitty for all anxiety diagnoses for the child; CBT ¼ cognitive-behavioral therapy condition; BPAM ¼ cognitive-behavioral therapy and brief parental anxiety management condition; SCAS ¼ Sp- Spence Children s Anxiety Scale; DASS ¼ Depression Anxiety Stress Scale; SMF ¼ Short Mood and Feelings Questionnaire. a Pretreatment to posttreatment. b Pretreatment to 6-month follow-up. c Posttreatment to 6-month follow-up. Note that significance is set at p <.017 for time main effect follow-up comparisons (pretreatment to posttreatment, pretreatment to 6-month follow-up, and posttreatment to 6-month follow-up) to adjust for multiple simple comparison. 378
10 BRIEF PARENTAL ANXIETY MANAGEMENT 379 was demonstrated by Cobham et al. (1998) on only a single measure, and this effect disappeared by 6-month follow-up. Therefore the current state of evidence appears to indicate that adding parent anxiety treatment to treatment for child anxiety results in little, if any improvements. As previously noted, however, research to date has failed to alter parents anxiety and so this conclusion must be tempered by the caveat that the fundamental significant benefits of BPAM emerged after 3 years (Cobham, Dadds, Spence, & McDermott, 2010), despite the lack of initial anxiety reduction among parents and regardless of whether parents were anxious initially. Thus, it is possible that BPAM provides some additional components that are not necessarily related to the parent s anxiety. If parental anxiety disorders did not reduce in the current BPAM because of insufficient dose, it will mean that future BPAM programs may need to increase the intensity, duration, and=or number of BPAM sessions (Barlow, 2007). It is worth noting that there was a reduction in parental anxiety symptoms in our study for all groups. However, given the significant number of parental anxiety disorders present at the end of treatment, it is unlikely that this reduction in symptoms was of clinical significance. The improvements in parental anxiety for the family-focused CBT groups may have been due to spontaneous recovery and the alleviation of family stress as a consequence of improvements in the child s anxiety. One possibility to consider is that improvements in parental anxiety may also have been due to parental deployment of strategies discussed in family-focused CBT, even without the provision of BPAM. Specifically, it is very likely that anxious parents in the family-focused CBT groups also used cognitive therapy and exposure therapy to manage his or her anxiety. The reduction of parental anxiety symptoms across time for both the CBT and BPAM group could explain the absence of group differences: All children may have benefited from the universal reduction of parental anxiety. Furthermore, the changes in child anxiety resulting from the child components of the Cool Kids program may have led to changes in parental anxiety and parental behaviors (Silverman et al., 2009). As there was not a waitlist control, it is unclear whether parental anxiety symptoms declined as a consequence of spontaneous recovery or having received CBT directly (BPAM groups) and indirectly (CBT groups) for parental anxiety. It is also worth noting that unlike Cobham et al., we did not conduct a stratified randomization (i.e., have a separate randomization list for children with and without anxious parents). Nevertheless, our randomization procedures did not result in an unbalanced design and thus the absence of stratification does not appear to have resulted in any material difference. A finding of theoretical and practical importance in the current study was that the presence of parental anxiety diagnosis conferred poorer treatment efficacy for the child. This finding was consistent across posttreatment and 6-month follow-up, and reflects the elevated risk for child anxiety by having an anxious parent (Rapee et al., 2009). This consistent finding provides impetus to continue to search for methods to reduce parents anxiety within the context of treatment for childhood anxiety disorders. Implications for Research, Policy, and Practice The current study suggests that the inclusion of BPAM to family CBT did not enhance child treatment outcomes. The study results, however, continue to emphasize the merit of addressing parental anxiety in interventions for childhood anxiety disorders because the children in our study were less likely to be diagnosis free if they had a parent who also had an anxiety disorder. This large-scale study strongly suggests that five sessions of BPAM did not lead to an enhanced decline in parental anxiety over and above the decline observed across time for children receiving CBT. The presence of parent anxiety is clearly a risk factor that therapists working with anxious children need to consider. To date, neither our BPAM program nor Cobham et al. s program was sufficient in reducing parental anxiety disorder in conjunction with treatment for the child. A more intensive BPAM program for parents may be needed. REFERENCES Antony, M. M., Bieling, P. J., Cox, B. J., Enns, M. W., & Swinson, R. P. (1998). Psychometric properties of the 42-item and 21-item version of the Depression Anxiety Stress Scales (DASS) in clinical groups and a community sample. Psychological Assessment, 10, Barlow, D. H. (2007). Clinical handbook of psychological disorders: A step-by-step treatment manual. New York, NY: Guilford. Bogels, S. M., & Brechman-Toussaint, M. L. (2006). Family issues in child anxiety: attachment, family functioning, parental rearing and beliefs. Clinical Psychology Review, 26, Brown, T. A., Di Nardo, P. A., & Barlow, D. H. (1994). Anxiety Disorders Inverview Schedule for DSM IV (ADIS IV) [Computer software]. San Antonio, TX: GPOWER. Cartwright-Hatton, S., Roberts, C., Chitsabesan, P., Fothergill, C., & Harrington, R. (2004). Systematic review of the efficacy of cognitive behaviour therapies for childhood and adolescent anxiety disorders. British Journal of Clinical Psychology, 43, Cobham, V. E., Dadds, M. R., & Spence, S. H. (1998). The role of parental anxiety in the treatment of childhood anxiety. Journal of Consulting and Clinical Psychology, 66, Cobham, V. E., Dadds, M. R., Spence, S. H., & McDermott, B. (2010). Parental anxiety in the treatment of childhood anxiety: A different story three years later. Journal of Clinical Child & Adolescent Psychology, 39,
11 380 HUDSON ET AL. Creswell, C., Willetts, L., Murray, L., Singhal, M., & Cooper, P. (2008). Treatment of child anxiety: An exploratory study of the role of maternal anxiety and behaviours in treatment outcome. Clinical Psychology and Psychotherapy, 15, Hirai, M., & Clum, G. A. (2006). A meta-analytic study of self-help interventions for anxiety problems. Behavior Therapy, 37, Hudson, J. L., Rapee, R. M., Deveney, C., Schneiring, C. A., Lyneham, H. J., & Bovopoulos, N. (2009). Cognitive-behavioral treatment versus an active control for children and adolescents with anxiety disorders: A randomized trial. Journal of the American Academy of Child and Adolescent Psychiatry, 48, Kendall, P. C., Hudson, J. L., Gosch, E., Flannery-Schroeder, E., & Suveg, C. (2008). Cognitive-behavioral therapy for anxiety disordered youth: A randomized clinical trial evaluating child and family modalities. Journal of Consulting and Clinical Psychology, 76, Kendall, P. C., & Suveg, C. (2006). Treating anxiety disorders in youth. Child and Adolescent Therapy: Cognitive-Behavioral Procedures, 3, Last, C. G., Hersen, M., Kazdin, A., Francis, G., & Grubb, H. J. (1987). Psychiatric illness in the mothers of anxious children. American Journal of Psychiatry, 144, Lovibond, P. F., & Lovibond, S. H. (1995). The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behaviour Research and Therapy, 33, Nauta, M. H., Scholing, A., Rapee, R. M., Abbott, M., Spence, S. H., & Waters, A. (2004). A parent-report measure of children s anxiety: Psychometric properties and comparisons with child-report in a clinic and normal sample. Behaviour Research and Therapy, 42, Peugh, J. L., & Enders, C. K. (2005). Using the SPSS mixed procedure to fit cross-sectional and longitudinal multilevel models. Educational and Psychological Measurement, 65, Rapee, R. M., Schniering, C. A., & Hudson, J. L. (2009). Anxiety disorders during childhood and adolescence: Origins and treatment. Annual Review of Clinical Psychology, 5, Silverman, W. K., & Albano, A. M. (1996). The Anxiety Disorders Interview Schedule for Children for DSM IV: Child and Parent Versions. San Antonio, TX: Psychological Corporation. Silverman, W. K., Kurtines, W. M., Jaccard, J., & Pina, A. A. (2009). Directionality of change in youth anxiety treatment involving parents: An initial examination. Journal of Consulting and Clinical Psychology, 77, doi: =a Southam-Gerow, M., & Kendall, P. C. (2002). Manual for the Protocol Adherence Checklist - Modified. Philadelphia, PA: Temple University. Spence, S. H. (1998). A measure of anxiety symptoms among children. Behaviour Research and Therapy, 36,
Patterns and Predictors of Subjective Units of Distress in Anxious Youth
 Behavioural and Cognitive Psychotherapy, 2010, 38, 497 504 First published online 28 May 2010 doi:10.1017/s1352465810000287 Patterns and Predictors of Subjective Units of Distress in Anxious Youth Courtney
Behavioural and Cognitive Psychotherapy, 2010, 38, 497 504 First published online 28 May 2010 doi:10.1017/s1352465810000287 Patterns and Predictors of Subjective Units of Distress in Anxious Youth Courtney
Behaviour Research and Therapy
 Behaviour Research and Therapy 72 (2015) 30e37 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat Comparing outcomes for children with
Behaviour Research and Therapy 72 (2015) 30e37 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat Comparing outcomes for children with
Can Parents Treat their Anxious Child using CBT? A Brief Report of a Self-Help Program
 Research Article imedpub Journals http://www.imedpub.com Acta Psychopathologica DOI: 10.4172/2469-6676.100036 Can Parents Treat their Anxious Child using CBT? A Brief Report of a Self-Help Program Abstract
Research Article imedpub Journals http://www.imedpub.com Acta Psychopathologica DOI: 10.4172/2469-6676.100036 Can Parents Treat their Anxious Child using CBT? A Brief Report of a Self-Help Program Abstract
A randomized controlled trial of online versus clinic-based CBT for adolescent anxiety
 A randomized controlled trial of online versus clinic-based CBT for adolescent anxiety Author Spence, Sue, Donovan, Caroline, March, Sonja, Gamble, Amanda, E. Anderson, Renee, Prosser, Samantha, Kenardy,
A randomized controlled trial of online versus clinic-based CBT for adolescent anxiety Author Spence, Sue, Donovan, Caroline, March, Sonja, Gamble, Amanda, E. Anderson, Renee, Prosser, Samantha, Kenardy,
Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study
 Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark ABSTRACT
 The Anxiety Disorder Clinic for Children and Adolescents (TADCCA) 115 The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark MIKAEL THASTUM a,b a Department
The Anxiety Disorder Clinic for Children and Adolescents (TADCCA) 115 The Anxiety Disorders Clinic for Children and Adolescents (TADCCA) at Aarhus University in Denmark MIKAEL THASTUM a,b a Department
NIH Public Access Author Manuscript J Am Acad Child Adolesc Psychiatry. Author manuscript; available in PMC 2012 August 26.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2008 September ; 47(9): 1039 1047. doi:10.1097/ CHI.ob013e31817eecco. School-Based Interventions
NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2008 September ; 47(9): 1039 1047. doi:10.1097/ CHI.ob013e31817eecco. School-Based Interventions
Improving access to treatment for anxiety disorders in children through low intensity interventions
 School of Psychology and Clinical Language Sciences Improving access to treatment for anxiety disorders in children through low intensity interventions Cathy Creswell 29 January 2015 University of Reading
School of Psychology and Clinical Language Sciences Improving access to treatment for anxiety disorders in children through low intensity interventions Cathy Creswell 29 January 2015 University of Reading
Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
 The Cognitive Behaviour Therapist: page 1 of 10 doi:10.1017/s1754470x08000160 ORIGINAL RESEARCH Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
The Cognitive Behaviour Therapist: page 1 of 10 doi:10.1017/s1754470x08000160 ORIGINAL RESEARCH Using a structured treatment, Friends for Life, in Norwegian outpatient clinics: results from a pilot study
No differences between group
 2 2 No differences between group No differences between group versus individual versus treatment individual of treatment childhood anxiety of childhood disorders in anxiety a randomized disorders clinical
2 2 No differences between group No differences between group versus individual versus treatment individual of treatment childhood anxiety of childhood disorders in anxiety a randomized disorders clinical
An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A)
 Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
A Retrospective Examination of the Similarity Between Clinical Practice and Manualized Treatment for Childhood Anxiety Disorders
 Available online at www.sciencedirect.com Cognitive and Behavioral Practice 17 (2010) 322 328 www.elsevier.com/locate/cabp A Retrospective Examination of the Similarity Between Clinical Practice and Manualized
Available online at www.sciencedirect.com Cognitive and Behavioral Practice 17 (2010) 322 328 www.elsevier.com/locate/cabp A Retrospective Examination of the Similarity Between Clinical Practice and Manualized
COGNITIVE-BEHAVIORAL GROUP TREATMENT FOR ANXIETY SYMPTOMS IN CHILDREN WITH HIGH-FUNCTIONING AUTISM SPECTRUM DISORDERS. Judy Reaven and Susan Hepburn
 COGNITIVE-BEHAVIORAL GROUP TREATMENT FOR ANXIETY SYMPTOMS IN CHILDREN WITH HIGH-FUNCTIONING AUTISM SPECTRUM DISORDERS Judy Reaven and Susan Hepburn Anxiety disorders are among the most common psychiatric
COGNITIVE-BEHAVIORAL GROUP TREATMENT FOR ANXIETY SYMPTOMS IN CHILDREN WITH HIGH-FUNCTIONING AUTISM SPECTRUM DISORDERS Judy Reaven and Susan Hepburn Anxiety disorders are among the most common psychiatric
Understanding anxiety disorders in children
 What questions will be covered? Anxiety in Children: What GPs need to know PROFESSOR JENNIE HUDSON, Department of Psychology Understanding anxiety disorders in children Are Anxiety Disorders something
What questions will be covered? Anxiety in Children: What GPs need to know PROFESSOR JENNIE HUDSON, Department of Psychology Understanding anxiety disorders in children Are Anxiety Disorders something
Predictors of Treatment Effectiveness for Youth with ASD and Comorbid Anxiety Disorders: It all Depends on the Family?
 DOI 10.1007/s10803-016-2956-5 ORIGINAL PAPER Predictors of Treatment Effectiveness for Youth with ASD and Comorbid Anxiety Disorders: It all Depends on the Family? F. J. A. van Steensel 1 V. M. Zegers
DOI 10.1007/s10803-016-2956-5 ORIGINAL PAPER Predictors of Treatment Effectiveness for Youth with ASD and Comorbid Anxiety Disorders: It all Depends on the Family? F. J. A. van Steensel 1 V. M. Zegers
The Efficacy of an Internet-Based Cognitive-Behavioral Therapy Intervention for Child Anxiety Disorders
 The Efficacy of an Internet-Based Cognitive-Behavioral Therapy Intervention for Child Anxiety Disorders Sonja March, 1 B Psych Hons, Susan H. Spence, 2 PHD, MBA, and Caroline L. Donovan, 2 PHD 1 School
The Efficacy of an Internet-Based Cognitive-Behavioral Therapy Intervention for Child Anxiety Disorders Sonja March, 1 B Psych Hons, Susan H. Spence, 2 PHD, MBA, and Caroline L. Donovan, 2 PHD 1 School
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Children and Adolescents: A Review and Meta-Analyses
 Phobic and Anxiety Disorders 1 Running head: TREATMENTS FOR PHOBIC AND ANXIETY DISORDERS Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Children and Adolescents: A Review and
Phobic and Anxiety Disorders 1 Running head: TREATMENTS FOR PHOBIC AND ANXIETY DISORDERS Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Children and Adolescents: A Review and
An analysis of the RCMAS lie scale in a clinic sample of anxious children $
 Anxiety Disorders 15 (2001) 443 457 An analysis of the RCMAS lie scale in a clinic sample of anxious children $ Armando A. Pina, Wendy K. Silverman*, Lissette M. Saavedra, Carl F. Weems Child and Family
Anxiety Disorders 15 (2001) 443 457 An analysis of the RCMAS lie scale in a clinic sample of anxious children $ Armando A. Pina, Wendy K. Silverman*, Lissette M. Saavedra, Carl F. Weems Child and Family
Research in child anxiety disorders indicates
 A Longitudinal Study of Developmental Differences in Universal Preventive Intervention for Child Anxiety Sally Lock and Paula M. Barrett Griffith University, Australia The present paper presents the results
A Longitudinal Study of Developmental Differences in Universal Preventive Intervention for Child Anxiety Sally Lock and Paula M. Barrett Griffith University, Australia The present paper presents the results
Heidi Clayards Lynne Cox Marine McDonnell
 Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Author. Published. Journal Title DOI. Copyright Statement. Downloaded from. Griffith Research Online
 Cognitive Behavioural Therapy Combined with an Interpersonal Skills Component in the Treatment of Generalized Anxiety Disorder in Adolescent Females: A Case Series. Author Waters, Allison, Donaldson, Jillian,
Cognitive Behavioural Therapy Combined with an Interpersonal Skills Component in the Treatment of Generalized Anxiety Disorder in Adolescent Females: A Case Series. Author Waters, Allison, Donaldson, Jillian,
Macquarie University ResearchOnline
 Macquarie University ResearchOnline This is the author version of an article published as: Wuthrich, V. M., Rapee, R. M., Cunningham, M. J., Lyneham, H. J., Hudson, J. L., & Schniering, C. A. (2012). A
Macquarie University ResearchOnline This is the author version of an article published as: Wuthrich, V. M., Rapee, R. M., Cunningham, M. J., Lyneham, H. J., Hudson, J. L., & Schniering, C. A. (2012). A
The treatment of child anxiety disorders
 The treatment of child anxiety disorders via guided parent delivered cognitivebehavioural therapy: a randomised controlled trial Article Published Version Creative Commons: Attribution 3.0 (CC BY) Open
The treatment of child anxiety disorders via guided parent delivered cognitivebehavioural therapy: a randomised controlled trial Article Published Version Creative Commons: Attribution 3.0 (CC BY) Open
Since the publication of Ollendick and King's (1998) initial status report on the efficacy of psychosocial
 Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Childr... Page 1 of 40 Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Children and Adolescents Authors:
Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Childr... Page 1 of 40 Evidence-Based Psychosocial Treatments for Phobic and Anxiety Disorders in Children and Adolescents Authors:
SUMMARY AND DISCUSSION
 Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Cognitive, affective and behavioural characteristics of mothers with anxiety disorders in the context of child anxiety disorder
 Cognitive, affective and behavioural characteristics of mothers with anxiety disorders in the context of child anxiety disorder Article Accepted Version Creswell, C., Apetroaia, A., Murray, L. and Cooper,
Cognitive, affective and behavioural characteristics of mothers with anxiety disorders in the context of child anxiety disorder Article Accepted Version Creswell, C., Apetroaia, A., Murray, L. and Cooper,
The development of cognitivebehavioral. A Cognitive-Behavioral Group for Patients With Various Anxiety Disorders
 A Cognitive-Behavioral Group for Patients With Various Anxiety Disorders David H. Erickson, Ph.D. Amy S. Janeck, Ph.D. Karen Tallman, Ph.D. Objective: Cognitive-behavioral therapy (CBT) protocols for each
A Cognitive-Behavioral Group for Patients With Various Anxiety Disorders David H. Erickson, Ph.D. Amy S. Janeck, Ph.D. Karen Tallman, Ph.D. Objective: Cognitive-behavioral therapy (CBT) protocols for each
WHY TRANSDIAGNOSTIC TREATMENTS?
 TRANSDIAGNOSTIC TREATMENTS FOR ANXIETY DISORDERS Martin M. Antony, PhD, ABPP Professor of Psychology, Ryerson University, Toronto Outline Why Transdiagnostic Treatments? Transdiagnostic Treatment Protocols
TRANSDIAGNOSTIC TREATMENTS FOR ANXIETY DISORDERS Martin M. Antony, PhD, ABPP Professor of Psychology, Ryerson University, Toronto Outline Why Transdiagnostic Treatments? Transdiagnostic Treatment Protocols
Metacognitive therapy for generalized anxiety disorder: An open trial
 Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M.
 UvA-DARE (Digital Academic Repository) Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M. Link to publication Citation
UvA-DARE (Digital Academic Repository) Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M. Link to publication Citation
Comorbidity and the Treatment of Principal Anxiety Disorders in a Naturalistic Sample
 Available online at www.sciencedirect.com Behavior Therapy 41 (2010) 296 305 www.elsevier.com/locate/bt Comorbidity and the Treatment of Principal Anxiety Disorders in a Naturalistic Sample Lissa Davis
Available online at www.sciencedirect.com Behavior Therapy 41 (2010) 296 305 www.elsevier.com/locate/bt Comorbidity and the Treatment of Principal Anxiety Disorders in a Naturalistic Sample Lissa Davis
Transdiagnostic Approaches to the Treatment of Anxiety and Emotional Disorders:
 Transdiagnostic Approaches to the Treatment of Anxiety and Emotional Disorders: Peter J. Norton, Ph.D. Disclosures Funded by grants and awards from: American Psychological Association National Institute
Transdiagnostic Approaches to the Treatment of Anxiety and Emotional Disorders: Peter J. Norton, Ph.D. Disclosures Funded by grants and awards from: American Psychological Association National Institute
Symptoms of social anxiety, depression and stress in parents of children with social anxiety disorder
 Symptoms of social anxiety, depression and stress in parents of children with social anxiety disorder Article Accepted Version Halldorsson, B., Draisey, J., Cooper, P. and Creswell, C. (2017) Symptoms
Symptoms of social anxiety, depression and stress in parents of children with social anxiety disorder Article Accepted Version Halldorsson, B., Draisey, J., Cooper, P. and Creswell, C. (2017) Symptoms
Types of Parental Involvement in CBT With Anxious Youth: A Preliminary Meta-Analysis
 Journal of Consulting and Clinical Psychology 2014 American Psychological Association 2014, Vol. 82, No. 6, 1163 1172 0022-006X/14/$12.00 http://dx.doi.org/10.1037/a0036969 Types of Parental Involvement
Journal of Consulting and Clinical Psychology 2014 American Psychological Association 2014, Vol. 82, No. 6, 1163 1172 0022-006X/14/$12.00 http://dx.doi.org/10.1037/a0036969 Types of Parental Involvement
No differences between group versus individual treatment of childhood anxiety disorders in a randomised clinical trial
 Journal of Child Psychology and Psychiatry 49:8 (2008), pp 886 893 doi:10.1111/j.1469-7610.2008.01877.x No differences between group versus individual treatment of childhood anxiety disorders in a randomised
Journal of Child Psychology and Psychiatry 49:8 (2008), pp 886 893 doi:10.1111/j.1469-7610.2008.01877.x No differences between group versus individual treatment of childhood anxiety disorders in a randomised
FIU Digital Commons. Florida International University. Jessica Dahan Florida International University,
 Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 10-23-2013 Individual Child Cognitive Behavioral Treatment versus Child-Parent Cognitive
Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 10-23-2013 Individual Child Cognitive Behavioral Treatment versus Child-Parent Cognitive
Interpretation and Expectation in Childhood Anxiety Disorders: Age Effects and Social Specificity
 J Abnorm Child Psychol (2014) 42:453 465 DOI 10.1007/s10802-013-9795-z Interpretation and Expectation in Childhood Anxiety Disorders: Age Effects and Social Specificity Cathy Creswell & Lynne Murray &
J Abnorm Child Psychol (2014) 42:453 465 DOI 10.1007/s10802-013-9795-z Interpretation and Expectation in Childhood Anxiety Disorders: Age Effects and Social Specificity Cathy Creswell & Lynne Murray &
Generalized Anxiety Disorder
 Generalized Anxiety Disorder Carl F. Weems and R. Enrique Varela The Treatment of Generalized Anxiety Disorder in Youth This chapter reviews the literature on the treatment of Generalized Anxiety Disorder
Generalized Anxiety Disorder Carl F. Weems and R. Enrique Varela The Treatment of Generalized Anxiety Disorder in Youth This chapter reviews the literature on the treatment of Generalized Anxiety Disorder
The Role of Control in Childhood Anxiety Disorders
 Cognitive Therapy and Research, Vol. 27, No. 5, October 2003 ( C 2003), pp. 557 568 The Role of Control in Childhood Anxiety Disorders Carl F. Weems, 1,4 Wendy K. Silverman, 2 Ronald M. Rapee, 3 and Armando
Cognitive Therapy and Research, Vol. 27, No. 5, October 2003 ( C 2003), pp. 557 568 The Role of Control in Childhood Anxiety Disorders Carl F. Weems, 1,4 Wendy K. Silverman, 2 Ronald M. Rapee, 3 and Armando
Online CBT in the Treatment of Child and Adolescent Anxiety Disorders: Issues in the Development of BRAVE ONLINE and Two Case Illustrations
 Behavioural and Cognitive Psychotherapy, 2008, 36, 411 430 Printed in the United Kingdom First published online 25 June 2008 doi:10.1017/s135246580800444x Online CBT in the Treatment of Child and Adolescent
Behavioural and Cognitive Psychotherapy, 2008, 36, 411 430 Printed in the United Kingdom First published online 25 June 2008 doi:10.1017/s135246580800444x Online CBT in the Treatment of Child and Adolescent
Family treatment of child anxiety: outcomes, limitations and future directions
 Family treatment of child anxiety: outcomes, limitations and future directions Article Accepted Version Creswell, C. and Cartwright Hatton, S. (00) Family treatment of child anxiety: outcomes, limitations
Family treatment of child anxiety: outcomes, limitations and future directions Article Accepted Version Creswell, C. and Cartwright Hatton, S. (00) Family treatment of child anxiety: outcomes, limitations
Effects of psychotherapy for anxiety in children and adolescents: A metaanalytic
 Accepted Manuscript Effects of psychotherapy for anxiety in children and adolescents: A metaanalytic review Shirley Reynolds, Charlotte Wilson, Jo Austin, Lee Hooper PII: S0272-7358(12)00021-9 DOI: doi:
Accepted Manuscript Effects of psychotherapy for anxiety in children and adolescents: A metaanalytic review Shirley Reynolds, Charlotte Wilson, Jo Austin, Lee Hooper PII: S0272-7358(12)00021-9 DOI: doi:
Version of record first published: 15 Jun 2010.
 This article was downloaded by: [Bond University] On: 15 March 2013, At: 04:52 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer House,
This article was downloaded by: [Bond University] On: 15 March 2013, At: 04:52 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer House,
Examining Outcome Variability: Correlates of Treatment Response in a Child and Adolescent Anxiety Clinic
 Journal of Clinical Child Psychology Copyright 2001 by 2001, Vol. 30, No. 3, 422 436 Lawrence Erlbaum Associates, Inc. Examining Outcome Variability: Correlates of Treatment Response in a Child and Adolescent
Journal of Clinical Child Psychology Copyright 2001 by 2001, Vol. 30, No. 3, 422 436 Lawrence Erlbaum Associates, Inc. Examining Outcome Variability: Correlates of Treatment Response in a Child and Adolescent
Social performance predicts
 4 4 Social performance predicts Social performance predicts treatment treatment outcome in children outcome in with children anxiety disorders with anxiety Leeden, Elisabeth M. W. J. Utens, Philip D.A.
4 4 Social performance predicts Social performance predicts treatment treatment outcome in children outcome in with children anxiety disorders with anxiety Leeden, Elisabeth M. W. J. Utens, Philip D.A.
Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive Disorder: A Preliminary Investigation
 Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
De Los Reyes and Kazdin (2009, Behavior Modification)
 RPC Model Coding Manual 1 De Los Reyes and Kazdin (2009, Behavior Modification) Manual for Range of Possible Changes Meta-Analysis Andres De Los Reyes University of Maryland at College Park Alan E. Kazdin
RPC Model Coding Manual 1 De Los Reyes and Kazdin (2009, Behavior Modification) Manual for Range of Possible Changes Meta-Analysis Andres De Los Reyes University of Maryland at College Park Alan E. Kazdin
Assessing the Impact of Group-based Cognitive Behaviour Therapy with Children and Adolescents Presenting with Anxiety or Depression
 PEG-171 Assessing the Impact of Group-based Cognitive Behaviour Therapy with Children and Adolescents Presenting with Anxiety or Depression Joan Nandlal, PhD & John Robinson, MA Bennett Research and Evaluation
PEG-171 Assessing the Impact of Group-based Cognitive Behaviour Therapy with Children and Adolescents Presenting with Anxiety or Depression Joan Nandlal, PhD & John Robinson, MA Bennett Research and Evaluation
Accepted Manuscript. Susan H. Spence, Caroline L. Donovan, Sonja March, Justin Kenardy, Cate Hearn
 Accepted Manuscript Generic versus disorder specific cognitive behavior therapy for social anxiety disorder in youth: A randomized controlled trial using internet delivery Susan H. Spence, Caroline L.
Accepted Manuscript Generic versus disorder specific cognitive behavior therapy for social anxiety disorder in youth: A randomized controlled trial using internet delivery Susan H. Spence, Caroline L.
A new Intervention Program for children with problematic school absenteeism
 A new Intervention Program for children with problematic school absenteeism Daniel Bach Johnsen Clinical psychologist, MSc, PhD. Student The Anxiety Clinic for Children and Adolescents Department of Psychology
A new Intervention Program for children with problematic school absenteeism Daniel Bach Johnsen Clinical psychologist, MSc, PhD. Student The Anxiety Clinic for Children and Adolescents Department of Psychology
A Meta-Analysis of Transdiagnostic Cognitive Behavioural Therapy in the
 A Meta-Analysis of Transdiagnostic Cognitive Behavioural Therapy in the Treatment of Child and Young Person Anxiety Disorders Donna L. Ewing a, Jeremy J. Monsen b, Ellen J. Thompson a, Sam Cartwright-Hatton
A Meta-Analysis of Transdiagnostic Cognitive Behavioural Therapy in the Treatment of Child and Young Person Anxiety Disorders Donna L. Ewing a, Jeremy J. Monsen b, Ellen J. Thompson a, Sam Cartwright-Hatton
Transdiagnostic treatment for posttraumatic stress and alcohol use behaviours and cognitions: An RCT
 Transdiagnostic treatment for posttraumatic stress and alcohol use behaviours and cognitions: An RCT Janine V. Olthuis, Margo C. Watt, Sean P. Mackinnon, & Sherry H. Stewart PTSD Conference at MUN July/August
Transdiagnostic treatment for posttraumatic stress and alcohol use behaviours and cognitions: An RCT Janine V. Olthuis, Margo C. Watt, Sean P. Mackinnon, & Sherry H. Stewart PTSD Conference at MUN July/August
Anxiety Instruments Summary Table: For more information on individual instruments see below.
 1 Anxiety Instruments Summary Table: For more information on individual instruments see below. Measure Anxiety Specific Instrument Age Range Assesses total anxiety and different anxiety subtypes Both a
1 Anxiety Instruments Summary Table: For more information on individual instruments see below. Measure Anxiety Specific Instrument Age Range Assesses total anxiety and different anxiety subtypes Both a
Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual
 Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual Anxiety likely contributes to poorer adaptive functioning, quality of life, and Using CBT to treat depression after stroke was first
Cognitive Behavioral Therapy For Late Life Depression A Therapist Manual Anxiety likely contributes to poorer adaptive functioning, quality of life, and Using CBT to treat depression after stroke was first
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Age as factor in selective mutism, 623 as factor in social phobia, 623 Agoraphobia, 593 600 described, 594 596 DSM-V changes related to,
Index Note: Page numbers of article titles are in boldface type. A Age as factor in selective mutism, 623 as factor in social phobia, 623 Agoraphobia, 593 600 described, 594 596 DSM-V changes related to,
Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A.
 UvA-DARE (Digital Academic Repository) Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A. Link to publication Citation for
UvA-DARE (Digital Academic Repository) Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A. Link to publication Citation for
The role of the family in child and adolescent posttraumatic stress following attendance at an. emergency department
 The role of the family in child and adolescent posttraumatic stress following attendance at an emergency department Key words: PTSD, children, parents. Running Head: FAMILY INFLUENCES ON CHILD PTSD Abstract
The role of the family in child and adolescent posttraumatic stress following attendance at an emergency department Key words: PTSD, children, parents. Running Head: FAMILY INFLUENCES ON CHILD PTSD Abstract
Laura Christine Skriner ALL RIGHTS RESERVED
 2015 Laura Christine Skriner ALL RIGHTS RESERVED TRAJECTORIES AND PREDICTORS OF TREATMENT RESPONSE IN CBT FOR YOUTH ANXIETY: AN INTEGRATIVE DATA ANALYSIS APPROACH By LAURA CHRISTINE SKRINER, M.S. A dissertation
2015 Laura Christine Skriner ALL RIGHTS RESERVED TRAJECTORIES AND PREDICTORS OF TREATMENT RESPONSE IN CBT FOR YOUTH ANXIETY: AN INTEGRATIVE DATA ANALYSIS APPROACH By LAURA CHRISTINE SKRINER, M.S. A dissertation
COGNITIVE BEHAVIOR THERAPY (CBT) & DIALECTICAL BEHAVIOR THERAPY (DBT)
 COGNITIVE BEHAVIOR THERAPY (CBT) & DIALECTICAL BEHAVIOR THERAPY (DBT) Kim Bullock, MD Clinical Associate Professor, Director of Neurobehavioral Clinic Director of Virtual Reality Therapy Lab Department
COGNITIVE BEHAVIOR THERAPY (CBT) & DIALECTICAL BEHAVIOR THERAPY (DBT) Kim Bullock, MD Clinical Associate Professor, Director of Neurobehavioral Clinic Director of Virtual Reality Therapy Lab Department
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES
 APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes
 MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
Journal of Cognitive Psychotherapy: An International Quarterly Volume 29, Number
 Journal of Cognitive Psychotherapy: An International Quarterly Volume 29, Number 3 2015 With Obsessive-Compulsive Disorder: Examining Maternal Influences Lara J. Farrell, PhD Donna Hourigan, DPsych (Clin)
Journal of Cognitive Psychotherapy: An International Quarterly Volume 29, Number 3 2015 With Obsessive-Compulsive Disorder: Examining Maternal Influences Lara J. Farrell, PhD Donna Hourigan, DPsych (Clin)
DBT Modification/ Intervention
 Table 2. Published Studies Examining Application of Inpatient DBT (alphabetical listing) Citation Inpatient Setting DBT Sample Comparison Sample DBT Modification/ Intervention Outcome Measures Results
Table 2. Published Studies Examining Application of Inpatient DBT (alphabetical listing) Citation Inpatient Setting DBT Sample Comparison Sample DBT Modification/ Intervention Outcome Measures Results
The Relation of Severity and Comorbidity to Treatment Outcome with Cognitive Behavioral Therapy for Childhood Anxiety Disorders
 DOI 10.1007/s10802-010-9394-1 The Relation of Severity and Comorbidity to Treatment Outcome with Cognitive Behavioral Therapy for Childhood Anxiety Disorders Juliette Margo Liber & Brigit M. van Widenfelt
DOI 10.1007/s10802-010-9394-1 The Relation of Severity and Comorbidity to Treatment Outcome with Cognitive Behavioral Therapy for Childhood Anxiety Disorders Juliette Margo Liber & Brigit M. van Widenfelt
Parental psychopathology and treatment outcome for anxious youths: Roles of family functioning and caregiver strain
 Parental psychopathology and treatment outcome for anxious youths: Roles of family functioning and caregiver strain Jessica L. Schleider, Golda S. Ginsburg, Courtney P. Keeton, John R. Weisz, Boris Birmaher,
Parental psychopathology and treatment outcome for anxious youths: Roles of family functioning and caregiver strain Jessica L. Schleider, Golda S. Ginsburg, Courtney P. Keeton, John R. Weisz, Boris Birmaher,
Testing the Efficacy of Theoretically Derived Improvements in the Treatment of Social Phobia
 Journal of Consulting and Clinical Psychology 2009 American Psychological Association 2009, Vol. 77, No. 2, 317 327 0022-006X/09/$12.00 DOI: 10.1037/a0014800 Testing the Efficacy of Theoretically Derived
Journal of Consulting and Clinical Psychology 2009 American Psychological Association 2009, Vol. 77, No. 2, 317 327 0022-006X/09/$12.00 DOI: 10.1037/a0014800 Testing the Efficacy of Theoretically Derived
DESIGN TYPE AND LEVEL OF EVIDENCE: Randomized controlled trial, Level I
 CRITICALLY APPRAISED PAPER (CAP) Hasan, A. A., Callaghan, P., & Lymn, J. S. (2015). Evaluation of the impact of a psychoeducational intervention for people diagnosed with schizophrenia and their primary
CRITICALLY APPRAISED PAPER (CAP) Hasan, A. A., Callaghan, P., & Lymn, J. S. (2015). Evaluation of the impact of a psychoeducational intervention for people diagnosed with schizophrenia and their primary
Parent-Child Interaction Therapy for Treatment of Separation Anxiety Disorder in Young Children: A Pilot Study
 126 Parent-Child Interaction Therapy for Treatment of Separation Anxiety Disorder in Young Children: A Pilot Study Molly L. Choate, Donna B. Pincus, Sheila M. Eyberg, and David H. Barlow, Center for Anxiety
126 Parent-Child Interaction Therapy for Treatment of Separation Anxiety Disorder in Young Children: A Pilot Study Molly L. Choate, Donna B. Pincus, Sheila M. Eyberg, and David H. Barlow, Center for Anxiety
Clinical Psychology Review
 Clinical Psychology Review 32 (2012) 251 262 Contents lists available at SciVerse ScienceDirect Clinical Psychology Review Effects of psychotherapy for anxiety in children and adolescents: A meta-analytic
Clinical Psychology Review 32 (2012) 251 262 Contents lists available at SciVerse ScienceDirect Clinical Psychology Review Effects of psychotherapy for anxiety in children and adolescents: A meta-analytic
"Online mindfulness approaches to promote wellbeing in the community
 "Online mindfulness approaches to promote wellbeing in the community Day: Wednesday 11th July 2018 Time: 3.30 4.45 pm Track: Clinical applications Interest in mindfulness-based practices has increased
"Online mindfulness approaches to promote wellbeing in the community Day: Wednesday 11th July 2018 Time: 3.30 4.45 pm Track: Clinical applications Interest in mindfulness-based practices has increased
Parental Psychopathology & Childhood Treatment Response
 Parental Psychopathology & Childhood Treatment Response Mary A. Fristad, PhD, ABPP Professor, Psychiatry, Psychology & Human Nutrition The Ohio State University Division of Child & Adolescent Psychiatry
Parental Psychopathology & Childhood Treatment Response Mary A. Fristad, PhD, ABPP Professor, Psychiatry, Psychology & Human Nutrition The Ohio State University Division of Child & Adolescent Psychiatry
Anxiety in Youth: Identification, Management, & Referral
 Anxiety in Youth: Identification, Management, & Referral Martin E. Franklin, Ph.D. Associate Professor of Psychiatry University of Pennsylvania School of Medicine Prelude to the Talk: Anxiety & Its Disorders
Anxiety in Youth: Identification, Management, & Referral Martin E. Franklin, Ph.D. Associate Professor of Psychiatry University of Pennsylvania School of Medicine Prelude to the Talk: Anxiety & Its Disorders
Child Anxiety Treatment: Outcomes in Adolescence and Impact on Substance Use and Depression at 7.4-Year Follow-Up
 Journal of Consulting and Clinical Psychology Copyright 2004 by the American Psychological Association 2004, Vol. 72, No. 2, 276 287 0022-006X/04/$12.00 DOI: 10.1037/0022-006X.72.2.276 Child Anxiety Treatment:
Journal of Consulting and Clinical Psychology Copyright 2004 by the American Psychological Association 2004, Vol. 72, No. 2, 276 287 0022-006X/04/$12.00 DOI: 10.1037/0022-006X.72.2.276 Child Anxiety Treatment:
NICE Guidelines in Depression. Making a Case for the Arts Therapies. Malcolm Learmonth, Insider Art.
 1 NICE Guidelines in Depression. Making a Case for the Arts Therapies. Malcolm Learmonth, Insider Art. These notes are derived from a review of the full Guidelines carried out by Malcolm Learmonth, May
1 NICE Guidelines in Depression. Making a Case for the Arts Therapies. Malcolm Learmonth, Insider Art. These notes are derived from a review of the full Guidelines carried out by Malcolm Learmonth, May
Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A.
 UvA-DARE (Digital Academic Repository) Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A. Link to publication Citation for
UvA-DARE (Digital Academic Repository) Anxiety disorders in children with autism spectrum disorders: A clinical and health care economic perspective van Steensel, F.J.A. Link to publication Citation for
Journal of Clinical Psychology Practice
 Journal of Clinical Psychology Practice Content and Diagnostic Specificity of Fear Hierarchy Items of Youth with Anxiety Disorders Kimberly D. Becker University of Maryland School of Medicine Ashley M.
Journal of Clinical Psychology Practice Content and Diagnostic Specificity of Fear Hierarchy Items of Youth with Anxiety Disorders Kimberly D. Becker University of Maryland School of Medicine Ashley M.
Treatment Moderation and Secondary Outcomes: Results from a Randomized Clinical Trial
 Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 6-28-2012 Treatment Moderation and Secondary Outcomes: Results from a Randomized
Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 6-28-2012 Treatment Moderation and Secondary Outcomes: Results from a Randomized
Establishing the Link: Assessment and Intervention of Children and Adults October 23, 2018
 Mental Health Aspects in Persons with Intellectual/Developmental Disabilities: Assessment and Diagnostic Practices (Keynote Speaker) Robert J. Fletcher, DSW, ACSW, LCSW, NADD-CC NADD Founder & CEO Emeritus
Mental Health Aspects in Persons with Intellectual/Developmental Disabilities: Assessment and Diagnostic Practices (Keynote Speaker) Robert J. Fletcher, DSW, ACSW, LCSW, NADD-CC NADD Founder & CEO Emeritus
Anxiogenic Patterns in Mother-Child Interactions
 Anxiogenic Patterns in Mother-Child Interactions Kyle W. Harvison L. Kevin Chapman Natalie G. Ballash Janet Woodruff-Borden ABSTRACT. The current study examined psychosocial variables associated with the
Anxiogenic Patterns in Mother-Child Interactions Kyle W. Harvison L. Kevin Chapman Natalie G. Ballash Janet Woodruff-Borden ABSTRACT. The current study examined psychosocial variables associated with the
Early Maladaptive Schemas And Personality. Disorder Symptoms An Examination In A Nonclinical
 Early Maladaptive Schemas And Personality Disorder Symptoms An Examination In A Non-clinical Sample Objective: This study examined whether some early maladaptive schema (EMS) domains, Results: Findings
Early Maladaptive Schemas And Personality Disorder Symptoms An Examination In A Non-clinical Sample Objective: This study examined whether some early maladaptive schema (EMS) domains, Results: Findings
This is the published version of a paper published in Behavioural and Cognitive Psychotherapy.
 http://www.diva-portal.org This is the published version of a paper published in Behavioural and Cognitive Psychotherapy. Citation for the original published paper (version of record): Norell Clarke, A.,
http://www.diva-portal.org This is the published version of a paper published in Behavioural and Cognitive Psychotherapy. Citation for the original published paper (version of record): Norell Clarke, A.,
A parent-report measure of children s anxiety: psychometric properties and comparison with child-report in a clinic and normal sample
 Behaviour Research and Therapy 42 (2004) 813 839 www.elsevier.com/locate/brat A parent-report measure of children s anxiety: psychometric properties and comparison with child-report in a clinic and normal
Behaviour Research and Therapy 42 (2004) 813 839 www.elsevier.com/locate/brat A parent-report measure of children s anxiety: psychometric properties and comparison with child-report in a clinic and normal
Do Treatment Manuals Undermine Youth Therapist Alliance in Community Clinical Practice?
 Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 4, 427 432 0022-006X/11/$12.00 DOI: 10.1037/a0023821 Do Treatment Manuals Undermine Youth Therapist
Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 4, 427 432 0022-006X/11/$12.00 DOI: 10.1037/a0023821 Do Treatment Manuals Undermine Youth Therapist
CBT for Hypochondriasis
 CBT for Hypochondriasis Ahmad Alsaleh, MD, FRCPC Assistant Professor of Psychiatry College of Medicine, KSAU-HS, Jeddah Agenda Types of Somatoform Disorders Characteristics of Hypochondriasis Basic concepts
CBT for Hypochondriasis Ahmad Alsaleh, MD, FRCPC Assistant Professor of Psychiatry College of Medicine, KSAU-HS, Jeddah Agenda Types of Somatoform Disorders Characteristics of Hypochondriasis Basic concepts
Jamie A. Micco, PhD APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS
 APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS Jamie A. Micco, PhD Director, Intensive Outpatient Service Child and Adolescent Cognitive Behavioral Therapy Program Massachusetts General
APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS Jamie A. Micco, PhD Director, Intensive Outpatient Service Child and Adolescent Cognitive Behavioral Therapy Program Massachusetts General
EVALUATING A COGNITIVE BEHAVIORAL THERAPY GROUP PROGRAM FOR ANXIOUS FIVE TO SEVEN YEAR OLD CHILDREN: A PILOT STUDY
 DEPRESSION AND ANXIETY 26:243 250 (2009) Research Article EVALUATING A COGNITIVE BEHAVIORAL THERAPY GROUP PROGRAM FOR ANXIOUS FIVE TO SEVEN YEAR OLD CHILDREN: A PILOT STUDY Suneeta Monga, M.D, Arlene Young,
DEPRESSION AND ANXIETY 26:243 250 (2009) Research Article EVALUATING A COGNITIVE BEHAVIORAL THERAPY GROUP PROGRAM FOR ANXIOUS FIVE TO SEVEN YEAR OLD CHILDREN: A PILOT STUDY Suneeta Monga, M.D, Arlene Young,
2. How do different moderators (in particular, modality and orientation) affect the results of psychosocial treatment?
 Role of psychosocial treatments in management of schizophrenia: a meta-analytic review of controlled outcome studies Mojtabai R, Nicholson R A, Carpenter B N Authors' objectives To investigate the role
Role of psychosocial treatments in management of schizophrenia: a meta-analytic review of controlled outcome studies Mojtabai R, Nicholson R A, Carpenter B N Authors' objectives To investigate the role
When the Evidence Says, Yes, No, and Maybe So
 CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE When the Evidence Says, Yes, No, and Maybe So Attending to and Interpreting Inconsistent Findings Among Evidence-Based Interventions Yale University ABSTRACT
CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE When the Evidence Says, Yes, No, and Maybe So Attending to and Interpreting Inconsistent Findings Among Evidence-Based Interventions Yale University ABSTRACT
Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M.
 UvA-DARE (Digital Academic Repository) Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M. Link to publication Citation
UvA-DARE (Digital Academic Repository) Anxiety disorders in young children: Parent and child contributions to the maintenance, assessment and treatment van der Sluis, C.M. Link to publication Citation
A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change
 A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change William R. Beardslee, MD* ; Tracy R. G. Gladstone, PhD* ; Ellen J. Wright, MA*;
A Family-Based Approach to the Prevention of Depressive Symptoms in Children at Risk: Evidence of Parental and Child Change William R. Beardslee, MD* ; Tracy R. G. Gladstone, PhD* ; Ellen J. Wright, MA*;
Interpretation Bias in Childhood Social Anxiety Disorder
 Berkshire Child Anxiety Clinic The Winnicott Research Unit Interpretation Bias in Childhood Social Anxiety Disorder 20 April 2012 University of Reading 2008 www.reading.ac.uk Anxiety: Interpretation of
Berkshire Child Anxiety Clinic The Winnicott Research Unit Interpretation Bias in Childhood Social Anxiety Disorder 20 April 2012 University of Reading 2008 www.reading.ac.uk Anxiety: Interpretation of
Sticking to the recipe: How do adherence and differentiation to a CBT protocol affect client outcomes in youths with anxiety?
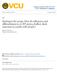 Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2017 Sticking to the recipe: How do adherence and differentiation to a CBT protocol affect client outcomes
Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2017 Sticking to the recipe: How do adherence and differentiation to a CBT protocol affect client outcomes
Cognitive-Behavioral Assessment of Depression: Clinical Validation of the Automatic Thoughts Questionnaire
 Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
Child-Parent Psychotherapy Research Fact Sheet OVERVIEW
 Child-Parent Psychotherapy Research Fact Sheet OVERVIEW Child-Parent Psychotherapy (CPP) is an intervention model for children aged 0-5 who have experienced traumatic events and/or are experiencing mental
Child-Parent Psychotherapy Research Fact Sheet OVERVIEW Child-Parent Psychotherapy (CPP) is an intervention model for children aged 0-5 who have experienced traumatic events and/or are experiencing mental
Experiential Avoidance in Individuals with Hoarding Disorder
 Cogn Ther Res (2013) 37:779 785 DOI 10.1007/s10608-012-9511-2 BRIEF REPORT Experiential Avoidance in Individuals with Hoarding Disorder Michael G. Wheaton Laura E. Fabricant Noah C. Berman Jonathan S.
Cogn Ther Res (2013) 37:779 785 DOI 10.1007/s10608-012-9511-2 BRIEF REPORT Experiential Avoidance in Individuals with Hoarding Disorder Michael G. Wheaton Laura E. Fabricant Noah C. Berman Jonathan S.
What Do Youth Referred for Anxiety Problems Worry About? Worry and Its Relation to Anxiety and Anxiety Disorders in Children and Adolescents
 Journal of Abnormal Child Psychology, Vol. 28, No. 1, 2000, pp. 63 72 What Do Youth Referred for Anxiety Problems Worry About? Worry and Its Relation to Anxiety and Anxiety Disorders in Children and Adolescents
Journal of Abnormal Child Psychology, Vol. 28, No. 1, 2000, pp. 63 72 What Do Youth Referred for Anxiety Problems Worry About? Worry and Its Relation to Anxiety and Anxiety Disorders in Children and Adolescents
INDEX. P. 2 Provisional List of Potentially Harmful Therapies (Adapted from Lilienfeld, 2007)
 Comprehensive List of Currently-Identified Potentially Harmful (PHTs) and Empirically Supported Psychological Treatments (ESTs) for Adults, Adolescents, and Children INDEX P. 2 Provisional List of Potentially
Comprehensive List of Currently-Identified Potentially Harmful (PHTs) and Empirically Supported Psychological Treatments (ESTs) for Adults, Adolescents, and Children INDEX P. 2 Provisional List of Potentially
Positive Parenting for Healthy Living: A randomised controlled trial of a brief group program for parents of children with asthma or eczema
 Positive Parenting for Healthy Living: A randomised controlled trial of a brief group program for parents of children with asthma or eczema Alina Morawska PhD Amy Mitchell PhD Parenting and Family Support
Positive Parenting for Healthy Living: A randomised controlled trial of a brief group program for parents of children with asthma or eczema Alina Morawska PhD Amy Mitchell PhD Parenting and Family Support
Social Anxiety Disorder. Operational Definition. Operational Definition 5/5/2012
 Social Anxiety Disorder Operational Definition A. Marked fear or anxiety about one or more social situations in which the person is exposed to possible scrutiny by others. B. The individual fears that
Social Anxiety Disorder Operational Definition A. Marked fear or anxiety about one or more social situations in which the person is exposed to possible scrutiny by others. B. The individual fears that
