Aims. Background. Definition
|
|
|
- Horace Ellis
- 5 years ago
- Views:
Transcription
1 REVIEW ARTICLE BJD British Journal of Dermatology How not to get scar(r)ed: pointers to the correct diagnosis in patients with suspected primary cicatricial alopecia M.J. Harries,* R.M. Trueb,à A. Tosti, A.G. Messenger, I. Chaudhry,** D.A. Whiting, C.E.M. Griffiths* and R. Paus* *Dermatological Sciences, The University of Manchester, Salford Royal Hospital, Manchester M6 8HD, U.K. Department of Dermatology, University of Lübeck, D Lübeck, Germany àdepartment of Dermatology, University Hospital of Zurich, Zurich, Switzerland Department of Dermatology, University of Bologna, Bologna, Italy Department of Dermatology, University of Sheffield, Hallamshire Hospital, Sheffield, U.K. **Department of Histopathology, Manchester Royal Infirmary, Manchester, U.K. Baylor Hair Research and Treatment Centre, Dallas, TX, U.S.A. ààdepartment of Dermatology, University of Melbourne, Melbourne, Australia Summary R. Sinclair,àà Correspondence Matthew Harries. Accepted for publication 21 October 2008 Key words alopecia, diagnosis, review Conflicts of interest None declared. DOI /j x Primary cicatricial alopecias (PCAs) are a rare, but important, group of disorders that cause irreversible damage to hair follicles resulting in scarring and permanent hair loss. They may also signify an underlying systemic disease. Thus, it is of paramount importance that clinicians who manage patients with hair loss are able to diagnose these disorders accurately. Unfortunately, PCAs are notoriously difficult conditions to diagnose and treat. The aim of this review is to present a rational and pragmatic guide to help clinicians in the professional assessment, investigation and diagnosis of patients with PCA. Illustrating typical clinical and histopathological presentations of key PCA entities we show how dermatoscopy can be profitably used for clinical diagnosis. Further, we advocate the search for loss of follicular ostia as a clinical hallmark of PCA, and suggest pragmatic strategies that allow rapid formulation of a working diagnosis. Scalp hair is an important component of body self-image in humans. Hair styles are commonly used to express individuality and increase sexual attractiveness. Therefore, it is no surprise that hair loss can have a marked impact on a person s psychological status, quality of life and social interaction, 1 3 not just through concern about the impact it may have on their appearance, but also whether it may signify a serious underlying disease. While this is true for essentially all forms of cosmetically disturbing hair loss, in cicatricial alopecias the situation is aggravated by the usually irreversible and often progressive nature of the condition. Cicatricial alopecias are a rare, but important, group of disorders that cause irreversible damage to hair follicles resulting in scarring and permanent hair loss. 3 8 In some situations they may also be associated with an underlying systemic disease. 7 For these reasons it is: (i) a priority to exclude or confirm the presence of a cicatricial alopecia, and (ii) of paramount importance that every clinician who manages patients with hair loss is able to diagnose these disorders accurately. Unfortunately, as this review will highlight, the latter is often more difficult than it sounds. Aims The aim of this review is to present a rational and pragmatic guide which allows clinicians to assess, investigate and ultimately diagnose patients with cicatricial alopecia. This paper is the second in a series of reviews that attempt to offer a comprehensive overview of cicatricial alopecias, focusing on primary cicatricial alopecia (PCA). The current review of the diagnosis of PCA complements our published, evidence-based account of treatment options in PCA. 4 Background Definition Cicatricial alopecia may be diagnosed on both clinical and histopathological grounds. In the clinical setting, the normally visible follicular ostia are lost, often, but not invariably, within an area of visible scarring. In many cases, this is concomitant with at least some degree of epidermal atrophy and other textural skin architecture changes. On histological examination 482
2 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 483 Fig 1. Cardinal signs of primary cicatricial alopecia (PCA). (a) Loss of visible follicular ostia. (b) Loss of visible follicular ostia (dermatoscopy view). (c) Histological hallmark of PCA showing follicle loss with replacement by fibrous tissue (haematoxylin and eosin; original manification 20). the hair follicles are destroyed and replaced with scar-like fibrous tissue (Fig. 1). 7,9 14 Primary vs. secondary cicatricial alopecia In PCA the hair follicle itself is the main target of the disease. In contrast, secondary cicatricial alopecias (e.g. skin cancer, thermal burns, sarcoidosis, or a consequence of ionizing radiotherapy) develop follicular damage coincidently as part of a more generalized destructive process within the skin, which ultimately destroys the hair follicle s stem cell-based capacity for repeated regeneration. 2,5,6,10 This review will focus on PCA. Epidemiology Data from various specialist hair centres in North America suggest that PCAs are relatively uncommon, even considering the highly selected cohort of patients studied At one centre the frequency of cicatricial alopecias seen was 3Æ2% between 1997 and 2001, while another reported a cicatricial alopecia frequency of 7Æ3% over a 10-year period. 14,15 Although the exact prevalence within the general population remains unknown, it is likely to be substantially lower than the figures reported above. Pathogenesis The exact pathogenesis of any of the PCAs is currently unknown. However, all forms of PCA probably result from irreversible damage to the epithelial hair follicle stem cells that reside in a protected area of the outer root sheath called the bulge. 17,18 The bulge is located in the upper third of the hair follicle at the level of the insertion of the arrector pili muscle (Fig. 2a,b). Morphologically, in some patients, this often Fig 2. (a) Hair follicle anatomy (from Whiting, 106 courtesy of Canfield Publishing). (b) Hair follicle anatomy showing the bulge region (haematoxylin and eosin; original magnification 20). (c) The follicular trochanter 19 (arrows) may be a useful morphological marker of the bulge region in humans (haematoxylin and eosin; original magnification 100).
3 484 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. markers remain to be identified for any of the currently recognized PCA entities. 6,23 4 The PCA literature is often confusing due to inconsistent use of terminology and poor disease definition. 7,21 These problems are compounded by our poor knowledge of the natural history of the different PCA diseases, the lack of good quality evidence for treatment 4 and our current inability to monitor disease progression objectively and effectively over time. Fig 3. The pattern of inflammatory infiltrate typically seen in permanent and reversible alopecias. Red dots = inflammatory infiltrate. (Adapted from Cotsarelis and Millar 107 ). difficult to identify bulge can be recognized by searching for a peculiar protrusion of the outer root sheath, for which the term follicular trochanter has been suggested (Fig. 2c). 19 It is thought that inflammation in the area of the bulge somehow destroys the epithelial hair follicle stem cells located here and, in so doing, removes the follicle s potential for regeneration. 5,6,20,21 It is interesting to compare the pattern of inflammation in PCA with that of the prototypical nonscarring inflammatory hair disorder, alopecia areata. 2,21 Despite the often marked peribulbar inflammation seen in alopecia areata, the follicles are not permanently destroyed, presumably because the bulge region is unaffected by the disease process (Fig. 3). The fact that mutant mice with a targeted deletion of keratin 15-expressing hair follicle epithelial progenitor cells show a striking loss of hair follicles, yet fail to develop signs of scarring, 20 suggests that the loss of epithelial stem cells is not the only element of PCA pathogenesis. Classification The North American Hair Research Society (NAHRS) has attempted to address some of these difficult issues by organizing a workshop on PCA. By consensus opinion, a working classification was produced that is based primarily on the predominant inflammatory infiltrate found on scalp biopsy. Once a patient had been classified into a specific histological subgroup, the disease could be identified based on the salient clinical features (Table 1). 25 Recommendations for both clinical and histological minimum datasets were also proposed so as to improve diagnosis and management, as well as facilitate research collaboration. Clinical assessment When approaching a patient with suspected scarring hair loss, it is prudent to follow a few simple rules, as follows. 1 Take a careful history. Particularly concentrate on the disease onset and progression, local and systemic symptoms, and other skin, nail or mucous membrane changes. A history of lupus erythematosus (LE), other autoimmune diseases or lichen planus (LP) should be sought and previous hair-care Problems with diagnosis of primary cicatricial alopecias Primary cicatricial alopecias are notoriously difficult to diagnose. While the observant clinician will soon notice clinical signs that point to the presence of some form of cicatricial alopecia, accurate classification is less straightforward, or (rarely) cannot be made at all. This difficulty results from the following factors: 1 The clinical and histological features may change over time as the disease evolves. At the time of examination the PCA may have already progressed to an advanced stage of hair follicle and skin degeneration, thereby eliminating any of the key diagnostic indicators. PCAs appear to follow a final common pathway in end-stage disease, characterized by complete follicular destruction, replacement with fibrous tissue and absence of an inflammatory infiltrate. At this stage specific disease classification may be impossible Overlapping clinical and pathological features make distinguishing one condition from another difficult, and at times impossible. 13,14 3 No single clinical or pathological feature is diagnostic for a particular form of PCA. 7 Conclusive and specific molecular Table 1 The North American Hair Research Society classification of primary cicatricial alopecias 25 Inflammatory infiltrate Lymphocytic Neutrophilic Mixed Nonspecific (end-stage) Diagnosis Chronic cutaneous lupus erythematosus Lichen planopilaris Classic lichen planopilaris Frontal fibrosing alopecia Graham Little syndrome Classic pseudopelade of Brocq Central centrifugal cicatricial alopecia Alopecia mucinosa Keratosis follicularis spinulosa decalvans Folliculitis decalvans Dissecting cellulitis folliculitis (perifolliculitis abscedens et suffodiens) Folliculitis (acne) keloidalis Folliculitis (acne) necrotica Erosive pustular dermatosis
4 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 485 Table 2 Dermatoscopy features of primary cicatricial alopecias Diagnosis Lichen planopilaris Chronic cutaneous lupus erythematosus Folliculitis decalvans Dermatoscopy features Absent follicular openings; follicular plugging; hair casts; peripilar white dots (dark-skinned patients); interfollicular simple red loops; arborizing red lines; honeycomb pigment; patchy deep pigmentation Absent follicular openings; red dot pattern of follicular openings (early disease); follicular plugging; hyperkeratotic perifollicular scaling; arborizing red lines Scalp oedema; crusts; peripilar casts; coiled dilated capillaries; tufted hairs; twisted red loops practices (e.g. use of hot combs, excessive traction) documented. 2 2 Carefully examine the scalp skin. Close inspection of the area of hair loss is mandatory, aided by a magnifying lens or dermatoscope, to appreciate the disappearance of the normal follicular ostia and identify any associated changes in skin texture (Table 2) As dermatoscopy offers very fast and highly instructive clues to PCA diagnosis, it is strongly recommended for the clinical examination of every case of PCA. 28 Irregularly spaced hair shafts and hair tufting ( doll s hair ) are additional clues to a scarring process. 2 Erythema, scaling and perifollicular hyperkeratosis should be recorded along with any signs of atrophy, dyspigmentation, pustules or crusting. The pattern of hair loss (e.g. central, multifocal, frontal) and the extent of scalp involvement should be estimated and monitored. 25 TIP Patient symptoms (e.g. pruritus, scalp tenderness) can often be used to guide the clinician to active areas of disease that may otherwise have been overlooked and often represent a particularly fruitful area to biopsy. 7 For example, scalp itching is a typical early sign of lichen planopilaris (LPP) and may be associated with minimal signs of scarring at disease onset. 3 Look for tufted hairs. These are multiple hairs emerging from a single follicular ostium. Hair tufting in PCA probably results from upper dermal inflammation destroying the distal follicle. As the skin heals the hairs are then pulled together to emerge through a common follicular ostium. 29,30 Hair tufting is commonly seen in folliculitis decalvans (FD) tufted folliculitis but is not pathognomonic of this disorder and may be seen in other PCA entities. 29 CAUTION A small number of hairs emerging through the same follicular ostium is often a normal finding Perform a hair pull test. Active hair loss (i.e. disease activity) can be assessed reliably, quickly and easily on different areas of the scalp during clinical assessment. Grip approximately 20 hairs near to the scalp, gently pulling upwards and away from the skin. The extraction of anagen hairs with thickened root sheaths strongly suggests cicatricial alopecia, even if Fig 4. Positive pull test revealing anagen bulbs with attached inner and outer root sheaths. the pull test does not reveal increased hair loss (Fig. 4). Therefore, even though only a few hairs may be extracted, the pull test is always regarded as pathological if anagen hairs are present. 5 Examine the rest of the skin. Particularly look for evidence of LE (e.g. face, ear lobes) or LP (e.g. oral cavity, genitalia, nails) in other anatomical regions besides the scalp. 6 Photograph the scalp. Photographic documentation allows objective assessment of disease extent and progression with time. 25 In practice, however, this may be difficult as patches of alopecia are often irregular and look very different, depending on how the remaining hair is parted. It is best to choose a target area and standardize the image (i.e. light, angle, distance). 7 Take samples for microscopy, culture and sensitivity (bacterial and fungal) if crusting, pustules, bogginess or scale are present. Fungal infections may induce a secondary cicatricial alopecia that may mimic various recognized PCA entities Remember, pustules can also be seen in normal scalps, fungal infections, LPP and discoid LE, 37,38 and are not pathognomonic for FD. 8 Arrange a skin biopsy of the scalp. 9 Follow the flowcharts (Figs 5, 6) to reach a provisional diagnosis. 10 Consider referral to a hair loss specialist for advice and or incorporation into an ongoing research study clinical trial. The scalp biopsy Scalp biopsy is a vital component of the assessment in PCA as it will not only determine the predominant inflammatory infiltrate used for disease classification (Table 1), 25 but can also be used to confirm scarring (if doubt exists) and helps to identify secondary causes of cicatricial alopecia. Unfortunately, scalp biopsies are often inadequate so that even the most expert pathologist cannot possibly reach a
5 486 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Fig 5. Flowchart 1. Clinical probability flowchart for primary cicatricial alopecia (PCA). LPP, lichen planopilaris; CCLE, chronic cutaneous lupus erythematosus; FFA, frontal fibrosing alopecia; AM, alopecia mucinosa; KFSD, keratosis follicularis spinulosa decalvans; PB, pseudopelade of Brocq; CCCA, central centrifugal cicatricial alopecia; DCS, dissecting cellulitis of the scalp; FD, folliculitis decalvans; AKN, acne keloidalis nuchae; ANV, acne necrotica varioliformis; EPDS, erosive pustular dermatosis of the scalp. diagnosis. Common errors include too small or superficial samples, crush artefact, cross-cutting of follicles or poor selection of biopsy site. Two 4 6-mm punch biopsies should be taken from active lesions, usually at the edge of the bald patch that is clinically affected by the inflammatory process, yet still contains a reasonable number of follicles. To stand any chance of diagnosing PCA accurately, the type and pattern of inflammation affecting the follicle before it has been completely destroyed need to be seen. Do not biopsy a completely bald, atrophic end-stage area of alopecia as the pathologist will see only nonspecific scarring. The punch biopsy instrument should be orientated parallel to the direction of hair growth so as to avoid the blade cutting across the follicles within the specimen (Fig. 7 correct technique). If follicles are cross-cut it can significantly reduce the number of diagnostic follicles available to the pathologist and thereby sharply reduces the information gained from the procedure. 11 Histopathology assessment For optimal results, one biopsy should be processed for horizontal sectioning and the other for vertical sectioning. 11,39 42 The biopsy destined for vertical sectioning is then bisected, enabling one half to be formalin fixed and processed for paraffin embedding and routine histology (haematoxylin and eosin), and the other to be snap-frozen and processed for immunofluorescence studies. The latter technique is primarily advised when autoimmune disorders (e.g. LE, vesiculobullous diseases) are suspected or when the biopsy material is to be used for research purposes. Additional histochemical stains, besides haematoxylin and eosin, for elastin (Verhoeff van Gieson; VVG), mucin (alcian blue), mast cells (toluidine blue; Giemsa) and periodic acid Schiff may improve diagnostic yield (see below). 43 To optimize histopathological reporting the NAHRS workshop on PCA devised a pathology minimum dataset to be completed for every case of suspected cicatricial alopecia. 25 This dataset prompts the recognition and reporting of key features for diagnosis of PCA, including hair follicle density and structure, adnexal involvement, epithelial changes, type and distribution of inflammatory infiltrate, degree and location of fibrosis, and interstitial changes. Immunofluorescence may improve diagnostic yield in certain situations, particularly if standard histopathology is inconclusive and cutaneous LE or a bullous disorder are suspected on clinical grounds. 44 However, caution is required as false-positive results may be seen in chronically sun-damaged skin. 45 Elastin stains (VVG) may improve diagnostic yield, particularly in end-stage disease that no longer displays an identifiable inflammatory infiltrate. VVG staining patterns for each PCA entity are summarized in Table 3, which also summarizes salient histopathological features of the major PCA entities. Steps to diagnosis Step 1. Is this a scarring alopecia? Having assessed the patient, the first step is to identify if the hair loss is the result of scarring. This is not always easy. We
6 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 487 Fig 6. Flowchart 2. Histopathology diagnostic flowchart for primary cicatricial alopecia (PCA). LPP, lichen planopilaris; CCLE, chronic cutaneous lupus erythematosus; FFA, frontal fibrosing alopecia; AM, alopecia mucinosa; KFSD, keratosis follicularis spinulosa decalvans; PB, pseudopelade of Brocq; CCCA, central centrifugal cicatricial alopecia; DCS, dissecting cellulitis of the scalp; FD, folliculitis decalvans; AKN, acne keloidalis nuchae; ANV, acne necrotica varioliformis; EPD EPDS, erosive pustular dermatosis of the scalp; BMZ, basement membrane zone; IMF, immunofluorescence; PAS, periodic acid Schiff; ORS, outer root sheath. *Elastin staining pattern not known for AM and KFSD. recommend good lighting along with optical magnification from a hand-lens, plus use of a dermatoscope. 27,28 Thus armed, search for loss of visible follicular ostia and epidermal atrophy. Proceed to step 2 when these clinical indicators of PCA are positive, or if scarring cannot be definitely excluded, especially when other signs are present that can be associated with PCA (e.g. skin sclerosis, pustules, crust). If the hair loss is deemed to be nonscarring in nature, do not proceed, but follow available guides on how to assess and manage nonscarring hair loss. 5,9,46
7 488 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Fig 7. The punch biopsy direction (large arrow) must run parallel to the remaining visible hair shafts to avoid cross-cutting the follicles. The biopsy must also be deep enough to sample the whole terminal hair follicle (i.e. extend into the subcutaneous fat). Step 2. What is your provisional clinical diagnosis? Although the usefulness of clinical inspection in PCA can sometimes be limited, a provisional differential diagnosis can usually be formulated based on the clinical features expressed. Use the clinical probability flowchart (flowchart 1, Fig. 5), the disease summaries and diagnostic tips below to narrow the clinical diagnosis. Additional clues can be gained from photographs of each condition (Figs 8 19) and the additional clinical details listed in Table 3. TIP Answer the following questions: 1 What is the patient s ethnic origin? Some conditions appear disproportionately over-represented in certain racial groups. 47 Central centrifugal cicatricial alopecia (CCCA), 48,49 acne keloidalis nuchae (AKN) 50 and dissecting cellulitis of the scalp (DCS; perifolliculitis capitis abscedens et suffodiens) 51 are almost exclusively found in those of African descent. However, exceptions do occur, but rarely. 49, What is the patient s age? Erosive pustular dermatosis (EPD) is reported primarily in elderly patients Frontal fibrosing alopecia (FFA) is seen predominantly in postmenopausal women, while keratosis follicularis spinulosa decalvans (KFSD) has an onset in late childhood or adolescence What is the scalp distribution? Certain conditions have characteristic locations within the scalp. Lesions of AKN are typically located on the occipital scalp, whereas FFA displays a distinctive band-like recession of the frontal hairline. 7,14,50,59,60,68 4 Are other nonscalp regions involved? Eyebrow alopecia is commonly seen in FFA and KFSD. 59,60,66,67 Chronic cutaneous lupus erythematosus (CCLE) is rarely solely limited to the scalp, with reports suggesting that coexisting lesions occur at other body sites in 80 90% of cases. 37,69 Diagnostic confidence may be greatly increased when typical nonscalp lesions of LP coexist with LPP. Some papers report extrascalp LP in up to 50% patients with LPP at some point during the course of the disease. 38 However, in practice these figures appear too high. For example, of 167 patients with biopsy-proven classic LPP seen at one European centre, two had nail LP, seven cutaneous LP and 36 oral LP (A. Tosti, unpublished data). 5 What is the most likely diagnosis? Contrary to previously published reports 15 it is the experience of the coauthors of this review that LPP and its variants are by far the most commonly encountered forms of PCA seen in general dermatological practice. Unfortunately no reliable data on the incidence and prevalence of defined PCA entities are as yet available. Therefore, LPP represents a sensible starting point when formulating your diagnosis. Use of the enclosed simplified flowchart will help reach a provisional diagnosis (Flowchart 1, Fig. 5). If you still experience difficulties in reaching a provisional diagnosis, scan Table 3 and the following summaries of the major forms of PCA for additional clues. Lichen planopilaris and variants These are illustrated in Figures 8 and 9. Classical LPP is characterized by multifocal patches of permanent alopecia distributed over the central scalp. Lesional skin displays perifollicular erythema and follicular hyperkeratosis, usually within the hairbearing rim of inflammation that surrounds the expanding edge of hair loss. 7 Other variants of LPP include FFA and Graham Little syndrome. Additionally, the recently described entity fibrosing alopecia in a pattern distribution (FAPD) may also be a variant of LPP. 25,70 In FFA, a band-like symmetrical recession of the frontal hairline, with associated scarring, is seen. Perifollicular erythema and follicular hyperkeratosis within the hair-bearing margin indicate ongoing disease activity. The zone of hair loss is typically much paler than that of the sun-exposed facial skin and this can be used to indicate the position of the original hairline (Fig. 9a). 59,60 Associated alopecia of the eyebrows is common 60 and nonscarring hair loss of the axillae and limbs may also be seen. 61,62,64 The diagnosis of Graham Little syndrome is suggested by the clinical triad of patchy, progressive scarring alopecia, nonscarring alopecia of axillary and pubic hair and the presence of widespread horny follicular (keratosis pilarislike) papules on the trunk and limbs (Fig. 9b,c) FAPD is characterized by scarring hair loss within areas of androgenetic alopecia (Fig. 9d). Although it is unknown whether FAPD is a variant of LPP, it appears to represent a lichenoid tissue reaction directed against miniaturized scalp hair. 70 Chronic cutaneous lupus erythematosus Cicatricial alopecia is a common feature in CCLE (Fig. 10), with around a third of cases having scalp involvement. 37,77 Progression to systemic LE is uncommon (< 10%) in those presenting purely with skin lesions. 78 Clinical features include
8 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 489 Table 3 Summary of the main clinical and histopathologial characteristics for each primary cicatricial alopecia entity (Table adapted from Sellheyer and Bergfeld 9 ) Epidemiology Clinical features Investigations associations Histopathology Lymphocytic group Lichen planopilaris (LPP) More common in women; adults Chronic cutaneous lupus erythematosus (CCLE) More common in women; adults Central scalp location; multifocal patches or diffuse confetti-like pattern; perifollicular erythema and hyperkeratosis; predominant activity at EDGE of alopecia patch. Nonscalp lichen planus may coexist Central scalp location; solitary or multiple plaques with diffuse erythema, scale and follicular plugging followed by progressive atrophy, telangiectasia and dyspigmentation; predominant activity in CENTRE of alopecia patch. Nonscalp lesions in 80 90% cases. 37,69 Risk of systemic disease low (< 10%) in those initially presenting with CCLE 78 Consider LFT, hepatitis B & C serology Exclude drug-induced LPP ANA, ENA, dsdna, U&E, LFT, urinalysis, blood pressure Lymphocytic infiltrate centred on infundibulum and isthmus; interface dermatitis (lichenoid > vacuolar) present; prominent cytoid bodies; loss of sebaceous glands (early); superficial perivascular pattern of inflammation only mucinours perifollicular fibroplasia; 116 no peri-eccrine inflammation; no dermal mucin. VVG stain: Superficial, wedge-shaped scar; elastin fibres preserved in interfollicular dermis. 43 IMF: Globular IgM (± fibrinogen) on cytoid bodies Lymphocytic infiltrate involving the infundibulum, isthmus and interfollicular epidermis; interface dermatitis (vacuolar > lichenoid) present; superficial and deep perivascular and peri-eccrine inflammation; follicular plugging; thickened basement membrane; moderate dermal mucin. VVG stain: Diffuse dermal scarring with loss of elastin fibres. 43 IMF: Granular linear deposits of IgG and C3 along epidermal and follicular BMZ (lupus band); IMF positive in % cases 44,79,117 Pseudopelade of Brocq (PB) More common in women; adults Flesh-coloured (atrophic) patches; likened to footprints in the snow ; 82 no visible inflammation; may coalesce into larger irregular patches. Symptoms usually absent Usually none required Lymphocytic infiltrate around the infundibulum and isthmus (may be sparse or absent); no interface changes; superficial (or absent) perivascular pattern of inflammation; concentric lamellar fibroplasias often marked; absent sebaceous glands but arrector pili muscles remain intact. VVG stain: Thickened elastin fibres in hyalinized dermis; wide fibrous tracts with intact elastic sheath. 43 Central centrifugal cicatricial alopecia (CCCA) More common in women; adults; African descent Starts over vertex crown; slowly progressive centrifugal spread; skin noninflamed and flesh-coloured; individual or grouped hairs may survive within zones of scarring; papules or pustules may be present (particularly at the active MARGIN). Symptoms usually absent Possible association with traumatic hair-care practices. 118,119 IMF: Negative Lymphocytic infiltrate around the infundibulum and isthmus (may be sparse or absent); no interface changes; superficial (or absent) perivascular pattern of inflammation; concentric lamellar fibroplasias often marked; premature desquamation of the IRS (early); 48,120 absent sebaceous glands. VVG stain: same staining pattern as PB. 43 IMF: Negative
9 490 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Table 3 (Continued) Epidemiology Clinical features Investigations associations Histopathology Alopecia mucinosa (AM) All ages Polymorphous skin lesions erythematous papules, patches or plaques; follicular openings often prominent and devoid of hairs; patchy or diffuse alopecia; mucinous material may sometimes be expressed from follicular openings with firm pressure; initial hair loss may be nonscarring. May involve any part of integument; predilection for scalp and eyebrows Keratosis follicularis spinulosa decalvans (KFSD) More common in males; onset in childhood; X-linked 95 Onset of keratosis pilaris on face, trunk and limbs in infancy; patchy alopecia with perifollicular erythema and scale; progressive scarring alopecia during later childhood; reduced disease activity around puberty; 94 infective exacerbations (pustules) common; loss of eyebrows and eyelashes (early). Associated with photophobia, corneal dystrophy, palmoplantar keratoderma and atopy Neutrophilic and mixed groups Folliculitis decalvans (FD) Adults Single or multifocal patches; expanding rim of painful folliculitis; thickened hypertrophic scarring; hair tufting ( doll s hair ); follicular pustules and scale common; predominant activity at EDGE of alopecia patch Dissecting cellulitis of the scalp (DCS) More common in black males Multiple painful interconnecting scalp nodules with overlying alopecia; nodules often fluctuant and may discharge purulent material; sinus tracts present; initial hair loss nonpermanent due to switch in hair cycle from anagen to telogen; hypertrophic scarring (late). Associated with acne conglobata and hidradenitis suppurativa (follicular occlusion triad) and with arthritis. 51, Risk of SCC in long-standing cases; 126 tinea capitis may mimic DCS 34 Rule out associated malignancy. LONG-TERM FOLLOW-UP REQUIRED 88,89,91 Ophthalmology assessment; 121 genetic counselling Lymphocytic infiltrate involving entire follicle; no interface changes; superficial and deep perivascular inflammation; atypical lymphocytes and epidermotropism should prompt further evaluation to rule out malignancy; mucinous degeneration of sebaceous gland and ORS the entire follicle may be affected. VVG stain: Staining pattern unknown. IMF: Negative Acute lesions show epidermal oedema with neutrophils; replaced later by a lymphocytic mixed infiltrate involving the infundibulum and isthmus; no interface changes; superficial perivascular pattern of inflammation; some perifollicular deposition of mucin (late). VVG stain: Staining pattern unknown. IMF: Negative MC&S (bacterial and fungal) Neutrophilic infiltrate early in disease course, replaced later by lymphocytes and plasma cells; perifollicular and intrafollicular inflammation with developing abscess formation; no sinus tracts; variable dermal fibrosis; follicular plugging. VVG stain: Absent from fibrous tracts and interfollicular dermis (late). IMF: Negative MC&S (bacterial and fungal); Follicular occlusion; early neutrophilic infiltration skin biopsy culture 34 becoming mixed later on; infiltrate typically located deep in the perifollicular and interfollicular dermis and subcutis; deep abscess formation; sinus tracts are characteristic; fibrosis prominent around the fibrous tracts. VVG stain: Absent from fibrous tracts and interfollicular dermis (late). IMF: Negative
10 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 491 Table 3 (Continued) Epidemiology Clinical features Investigations associations Histopathology Acne keloidalis nuchae (AKN) More common in black males Characteristic location on occipital scalp and neck; firm follicular papules that may coalesce into fibrous nodules and plaques; secondary infection common (pustules and crusting). May be painful. Mechanical irritation suggested as possible predisposing factor; 127,128 tinea capitis may mimic AKN 32 MC&S (bacterial and fungal) Mixed infiltrate of lymphocytes and neutrophils located in the perifollicular dermis and within the follicle; granuloma formation; perifollicular abscess formation; no sinus tracts; perifollicular lamellar fibrosis seen early, with hypertrophic scarring later on; follicular plugging. (Note: in-growing hairs not a feature of AKN). 50 Acne necrotica varioliformis (ANV) Erosive pustular dermatosis of the scalp (EPDS) Adults Itchy and painful lesions found on the frontal hairline and parietal scalp; characteristic lesions are oedematous, umbilicated papulopustules that undergo central necrosis, occur in crops and heal with varioliform scars; lesions often quickly excoriated; exacerbated by stress. 129 The face, eyebrows, neck and chest (seborrhoeic areas) may also be involved Elderly Thick crust overlying erosions and pustules; vertex scalp location; balding and sun-damaged skin; often history of preceding scalp trauma. Lesions usually asymptomatic. Risk of secondary carcinoma; 130 fungal kerion may mimic EPDS. 36 Rule out cicatricial pemphigoid with IMF VVG stain: Absent from fibrous tracts and interfollicular dermis (late). IMF: Negative MC&S (bacterial and fungal) Early acneiform follicular dilatation, lymphocyte exocytosis, follicular spongiosis and perifollicular oedema with a mixed infiltrate of lymphocytes and neutrophils; no abscess formation; no sinus tracts; single cell necrosis progressing to confluent cell necrosis throughout the follicle. VVG stain: Absent from fibrous tracts and interfollicular dermis (late). IMF: Negative MC&S (bacterial and fungal) Histopathology nonspecific; mixed infiltrate of lymphocytes and neutrophils throughout epidermis, hair follicle, dermis and subcutis; epidermal atrophy; foreign-body giant cells; arrector pili muscles remain intact. VVG stain: Absent from fibrous tracts and interfollicular dermis (late). IMF: Negative VVG, Verhoeff van Gieson; IMF, immunofluorescence; BMZ, basement membrane zone; ANA, antinuclear antibodies; ENA, extractable nuclear antigens; dsdna, double-stranded DNA; U&E, urea and electrolytes; LFT, liver function tests, MC&S, microscopy, culture and sensitivities; IRS, inner root sheath; ORS, outer root sheath; SCC, squamous cell carcinoma.
11 492 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Fig 8. Classic lichen planopilaris (LPP). (a) Loss of follicular ostia with active disease at the expanding edge of the lesion. Perifollicular erythema and follicular hyperkeratosis are typical signs in active LPP. (b) Close-up view of perifollicular erythema and hyperkeratosis. (c) Dermatoscopy view showing loss of follicular ostia and follicular hyperkeratosis. (d, e) Horizontal and vertical histopathology sections showing a perifollicular lichenoid interface dermatitis involving the distal follicle. Haematoxylin and eosin; original magnification: (d) 200, (e) 100. (f) Cytoid bodies highlighted by direct immunofluorescence. Fig 9. Lichen planopilaris variants. (a) Band-like recession of frontal hairline in frontal fibrosing alopecia. Note the loss of eyebrows. (b) Close-up view showing the follicular rash of Graham Little syndrome (GLS). (c) Nonscarring axillary alopecia in GLS. (d) Fibrosing alopecia in a pattern distribution.
12 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 493 Fig 10. Chronic cutaneous lupus erythematosus (CCLE). (a) Scalp CCLE with predominant inflammation in the centre of the lesion. (b) Lesion of CCLE on the face. (c) Dermatoscopy of a 2-month old patch of CCLE showing erythematous dots within follicular openings. (d) Dense perifollicular lymphocytic infiltrate (haematoxylin and eosin; original magnification 20). (e) Horizontal section through deep dermis showing a vacuolar interface dermatitis, concentric lamellar fibrosis and peri-eccrine inflammation (haematoxylin and eosin; original magnification 200). (f) Lupus band on direct immunofluorescence. diffuse erythema and scale, followed by progressive atrophy, telangiectasia and dyspigmentation. 79 The most pronounced inflammatory activity is usually observed in the centre of the plaque of alopecia. Plaques may be either solitary or multiple and are often found in a central distribution on the scalp. In early CCLE dermatoscopy shows a typical red dot pattern of the follicular openings (Table 2; Fig. 10c). 27,28 Pseudopelade of Brocq Controversy exists as to whether pseudopelade of Brocq (PB; Fig. 11) is a disease entity in its own right or just the endstage appearance of a different scarring process (e.g. LPP, CCLE). 80,81 Plaques are usually ivory-white to flesh-coloured and slightly atrophic. Multiple, variably sized plaques, distributed mainly over the vertex, are typical ( footprints in the snow ) 82 and may fuse into larger, irregularly shaped areas of alopecia. Symptoms and clinically visible inflammation are usually absent. 80 Central centrifugal cicatricial alopecia CCCA (Fig. 12) is characterized by a noninflammatory scarring alopecia of the central scalp. It starts on the vertex and crown and spreads symmetrically and centrifugally. The hair loss of CCCA is often incomplete, with some individual or grouped hairs remaining unaffected within the area of scarring. The scalp skin is usually soft, flesh-toned 7 and without clinical evidence of inflammation. Symptoms are usually absent. 48,49 Alopecia mucinosa Alopecia mucinosa (AM; Fig. 13) may occur at any age and at any body site; however, AM has a predilection for the head and neck, and in particular the scalp and eyebrows. 83 Typical lesions include erythematous follicular papules and indurated plaques, with conspicuous follicular openings that are usually devoid of hairs. However, other morphologies have been described AM may be idiopathic (primary AM) or associated with an underlying lymphoproliferative disorder (secondary AM). 88 At present, the disease course and prognosis, and ultimately the differentiation of primary AM from secondary AM, cannot be predicted using current clinical and pathological criteria Long-term follow-up is therefore mandatory in all cases. Several authorities consider AM in adults almost always to indicate the presence of cutaneous T-cell lymphoma. 92 Keratosis follicularis spinulosa decalvans KFSD (Fig. 14) begins in infancy with progressive development of keratosis pilaris on the face, trunk and limbs. Loss of
13 494 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Fig 11. Pseudopelade of Brocq. (a) Characteristic noninflamed irregular patch of alopecia. (b) Histopathology examination reveals minimal absent inflammation and follicular scars (haematoxylin and eosin; original magnification 20). Fig 12. Central centrifugal cicatricial alopecia. Centrifugally spreading alopecia with no clinical signs of inflammation (from Whiting, 106 courtesy of Canfield Publishing). Fig 13. Alopecia mucinosa (AM). (a) Multiple plaques of AM on the scalp. (b, c) Histopathology shows intrafollicular mucin deposition. (b) Haematoxylin and eosin; original magnification 200; (c) alcian blue; original magnification 200. eyebrows is seen early in the course of the disease. A progressive scarring alopecia develops later in childhood. Variable degrees of inflammation, follicular hyperkeratosis and atrophy are seen within areas of either patchy or diffuse hair loss. Secondary bacterial infections are common and are heralded by the appearance of crops of new scalp pustules. Photophobia,
14 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 495 Fig 14. Keratosis follicularis spinulosa decalvans (KFSD). (a) Perifollicular hyperkeratosis is often prominent in KFSD. (b) Loss of eyebrows in KFSD. Fig 15. Folliculitis decalvans (FD). (a) Scarring, scale, follicular pustules and hair tufting characteristic of FD. (b) Hair tufting (tufted folliculitis). (c) Dermatoscopy view shows tufting and coiled capillaries. (d f) Histopathology reveals hair tufting and hair follicle destruction with a dense neutrophilic infiltrate and foreign-body giant cells. Haematoxylin and eosin; original magnification: (d) 20, (e) 100, (f) 200. corneal dystrophy, palmoplantar keratoderma and atopy are associated with KFSD. 93,94 Around puberty a reduction in disease activity is noted and hair loss slows or stops. 66,95,96 Folliculitis decalvans tufted folliculitis FD (Fig. 15) is characterized by a progressive scarring alopecia resulting from a destructive, purulent folliculitis 97 (N.B. Tufted folliculitis appears to represent a variant of FD and the term will be used synonymously with that of FD). 98,99 The vertex is the most commonly affected site. Patches may be single or multifocal and comprise an expanding rim of painful folliculitis that eventually reveals a central area of scarring. 97 This scarred zone is often hypertrophic, which contrasts with the usually atrophic scarring found in CCLE and LPP. Follicular pustules and crusting are prominent and tufts containing mul-
15 496 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Fig 17. Acne keloidalis nuchae (AKN). (a) Mild moderate AKN with numerous firm follicular papules over the occipital scalp. (b) Large keloid-like area of scarring seen in severe AKN. Fig 16. Dissecting cellulitis of the scalp. (a) Multiple fluctuant scalp nodules. (b) Dense neutrophilic inflammation with follicular destruction (haematoxylin and eosin; original magnification 20). tiple hairs are often seen emerging from a single dilated follicular orifice ( doll s hair ). 29, CAUTION Fungal infections may mimic PCA. Always take samples for culture if scale, pustules or discharge are present Dissecting cellulitis of the scalp DCS (Fig. 16) manifests as multiple enlarging painful and fluctuant nodules and abscesses on the scalp that interconnect via sinus tracts. A purulent material may be discharged either spontaneously, or with firm pressure over lesional skin. 11 The condition is associated with hidradenitis suppurativa and acne conglobata. It is thought that follicular occlusion is one element in the pathogenesis of all three disorders, although the genesis of the inflammatory focus remains obscure. 51 DCS tends to runs a progressive course that eventually results in marked hypertrophic scarring and permanent hair loss. Acne keloidalis nuchae A chronic inflammatory folliculitis, AKN (Fig. 17) commonly involves the occipital scalp resulting in permanent hair loss and scarring. The condition tends to occur preferentially in young black men, although AKN in black women 52 and white men has been described. Lesions start as firm follicular papules that coalesce into larger, keloid-like plaques. Secondary infection is common and is suggested by pustule formation, increased pain and discharge. 50 Acne necrotica varioliformis Acne necrotica varioliformis (Fig. 18) is characterized by crops of follicular lesions, usually involving the parietal scalp and frontal hair line, which heal with scarring. Other areas affected may include the face, eyebrows, neck and chest. The lesions typically comprise oedematous, umbilicated papulopustules that undergo central necrosis, crust over and then slowly heal, leaving varioliform scars. Most lesions are excoriated and may be painful or itchy Erosive pustular dermatosis Erosive pustular dermatosis (Fig. 19) was defined by Burton et al. as a chronic extensive pustulation confined to the scalp of an elderly person, and leading to erosion and scarring alopecia. 57 A typical patient with EPD is elderly, balding and shows signs of chronic sun damage to the scalp. Asymptomatic areas of thick crust are usually present that, when
16 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. 497 Fig 18. Acne necrotica varioliformis (ANV). (a) Moulage of ANV. (b, c) Typical lesions of ANV. Fig 19. Erosive pustular dermatosis of the scalp (EPD). (a) Crusted and eroded lesion of EPD on the bald scalp of an elderly patient. (b) Nonspecific histology showing eroded skin with a dense mixed inflammatory infiltrate (haematoxylin and eosin; original magnification 100). removed, reveal moist erosions, pustules and scarring hair loss. 56,58 Step 3. What does the histology show? See Flowchart 2, (Fig. 6), Figs 8 19 and Table 3. Once secondary causes of cicatricial alopecia have been excluded, the most important histopathological challenge is to identify the predominant inflammatory infiltrate. 9,12 14,25,105 This will aid disease classification and help to narrow the differential diagnosis. Flowchart 2 (Fig. 6) can be used as a rough guide to formulating a histological differential diagnosis. Table 3 can then be used to review specific histological features. CAUTION Some conditions classified into a certain histological subgroup may, at some point during the course of the disease, have a different predominant infiltrate to the main group to which it has been classified. For example, acute lesions of KFSD often show a neutrophil-predominant infiltrate early in the disease course (Table 3). This must be kept in mind when interpreting the pathologist s report.
17 498 Diagnosis of primary cicatricial alopecia, M.J. Harries et al. Histopathology tips in primary cicatricial alopecia 1 Most pathologists are unfamiliar with scalp histopathology. Do not be afraid to ask for an expert pathology review. 2 Within the lymphocyte-predominant subgroup the most common question asked is whether the diagnosis is that of CCLE or LPP. This is because these conditions are the two most commonly encountered diseases within the subgroup, and invite both common and distinct therapeutic approaches. Also, differentiating one disease from another on clinical grounds alone can be difficult. Important histopathological differences do exist and identification of these can usually secure a diagnosis: 44 CCLE displays both superficial and deep perivascular and peri-eccrine inflammation, and the dermis contains moderate amounts of mucin. In LPP, deep periadnexal inflammation and dermal mucin are absent. 9,14 Diagnostic power can be further increased by the addition of immunofluorescence studies (Figs 8f,10f; Table 3) Current histopathological techniques can readily differentiate between lymphocyte-predominant and neutrophil-predominant subgroups of PCA. However, Mirmirani et al. found that within these histopathological subgroups it was not possible to differentiate consistently clinically distinct disease (e.g. LPP, FFA, CCCA and PB in the lymphocyte-predominant subgroup) from the histopathology features alone. 22 Although this study was not a true representation of real life (i.e. it excluded cases of CCLE), it does highlight the importance of good clinicopathological correlation when formulating a diagnosis in PCA. Close communication between pathologist and clinician will maximize the chance of an accurate diagnosis in these disorders. Step 4. Have you reached a working diagnosis? By this point you should have: (i) confirmed that your patient has scarring hair loss; (ii) excluded secondary causes of scarring alopecia; (iii) determined the predominant inflammatory infiltrate on histopathology; (iv) reviewed the clinical and pathological findings and formulated a short-list of possible diagnoses; and (v) reviewed the specific features of each disease (Table 3; Figs 8 19) to determine the final diagnosis. You should now have an accurately diagnosed case of PCA. The next hurdle is how to treat the patient. For this, you may wish to consult our previous review on treatment options in PCA. 4 If you still cannot make a diagnosis, don t worry. Even for the most experienced clinicians, PCA can at times be impossible to diagnose. In this situation cicatricial alopecia of uncertain cause would be an entirely reasonable statement. If the hair loss is still active then follow-up assessment with repeated pathology examination is advised. Referral to a clinician with a specialist interest in hair disorders is a sensible option at any time throughout the diagnostic and treatment process as, for the hair follicle of your patient, rapid initiation of effective therapy is indeed a matter of life and death : any postponement of well-selected therapy (often because a clear-cut working diagnosis has not been reached quickly enough) will increase the level of irreversible hair follicle damage. Conclusion PCAs are an important group of disorders that result in scarring and permanent hair loss. Accurate diagnosis is the vital first step in their successful management. Although by the time most patients are seen permanent follicular damage has occurred; treatment is still required to stop ongoing inflammation and halt further hair loss. Also, the clinically visible extent of scarring is not always a reliable indicator of the actual level of irreversible stem cell damage and subsequent hair follicle destruction. Thus, early initiation of therapy, aided and encouraged by fast and accurate diagnosis, may sometimes still allow hair follicles with residual repair potential to recover from inflammatory damage. Only through correct diagnosis and appropriate management can we hope to minimize the often marked physical and psychological impact that these conditions have on our patients. Acknowledgments Writing of this review was made possible in part by the Geoffrey-Dowling Fellowship from the British Association of Dermatologists to M.J.H., a grant from the University of Lübeck Research Focus Programme on Autoimmunity to R.P. and a grant from the Cicatricial Alopecia Research Foundation (CARF) to M.J.N. and R.P. References 1 Hadshiew IM, Foitzik K, Arck PC et al. Burden of hair loss: stress and the underestimated psychosocial impact of telogen effluvium and androgenetic alopecia. J Invest Dermatol 2004; 123: Paus R, Olsen E, Messenger A. Hair growth disorders. In: Fitzpatrick s Dermatology in General Medicine (Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, eds), 7th edn. New York: McGraw-Hill, 2008; Williamson D, Gonzalez M, Finlay AY. The effect of hair loss on quality of life. J Eur Acad Dermatol Venereol 2001; 15: Harries MJ, Sinclair RD, MacDonald-Hull S et al. Management of primary cicatricial alopecias: options for treatment. Br J Dermatol 2008; 159: Paus R. Therapeutic strategies for treating hair loss. Drug Discov Today Ther Strateg 2006; 3: Stenn KS, Cotsarelis G, Price VH. Report from the cicatricial alopecia colloquium. J Invest Dermatol 2006; 126: Ross EK, Tan E, Shapiro J. Update on primary cicatricial alopecias. J Am Acad Dermatol 2005; 53: Sinclair RD. Aquired cicatricial alopecias. In: Rook s Textbook of Dermatology (Burns DA, Breathnach SM, Cox NH, Griffiths CEM, eds), 7th edn. Oxford: Blackwell Publishing, 2004; Sellheyer K, Bergfeld WF. Histopathologic evaluation of alopecias. Am J Dermatopathol 2006; 28: Headington JT. Cicatricial alopecia. Dermatol Clin 1996; 14: Sperling LC. Scarring alopecia and the dermatopathologist. J Cutan Pathol 2001; 28: Sperling LC, Cowper SE. The histopathology of primary cicatricial alopecia. Semin Cutan Med Surg 2006; 25:41 50.
Dermatopathology Workshop Summary, Berlin 2004
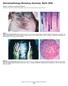 Dermatopathology Workshop Summary, Berlin 2004 David A. Whiting and Rolf Hoffmannw Baylor Hair Research and Treatment Center, Dallas, Texas, USA; wdermatology Practice, Freiburg, Germany Figure 1 Case
Dermatopathology Workshop Summary, Berlin 2004 David A. Whiting and Rolf Hoffmannw Baylor Hair Research and Treatment Center, Dallas, Texas, USA; wdermatology Practice, Freiburg, Germany Figure 1 Case
Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery
 Dermoscopy in the evaluation and treatment of hair loss Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD
Dermoscopy in the evaluation and treatment of hair loss Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD
Tips on Evaluation and Diagnosis of Scarring Alopecias. Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic
 Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Tips on getting the most from your alopecia pathology reports. D irector, H a ir C linic, Boston Medical C e n ter
 Tips on getting the most from your alopecia pathology reports Lynne J. Goldberg, MD J a g Bhawan Professor o f Dermatology a n d Pathology & Laboratory Medicine Boston U n iversity School of Medicine D
Tips on getting the most from your alopecia pathology reports Lynne J. Goldberg, MD J a g Bhawan Professor o f Dermatology a n d Pathology & Laboratory Medicine Boston U n iversity School of Medicine D
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia
 CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Lichen planopilaris and its variants. Antonella Tosti. Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery
 Lichen planopilaris and its variants Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S023 Lichen planopilaris
Lichen planopilaris and its variants Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S023 Lichen planopilaris
How to decipher a pathology report for alopecia
 How to decipher a pathology report for alopecia DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Lynne J. Goldberg, MD S063-Hair Disorders Made Easier DISCLOSURES I do not have any relationships with industry
How to decipher a pathology report for alopecia DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Lynne J. Goldberg, MD S063-Hair Disorders Made Easier DISCLOSURES I do not have any relationships with industry
New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology
 New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology Conflict of Interest No relevant conflicts Investigator for Samumed, Kythera, Incyte, Concert, Allergan Advisory
New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology Conflict of Interest No relevant conflicts Investigator for Samumed, Kythera, Incyte, Concert, Allergan Advisory
FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI
 FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI B D S B S M Department of Dermatology and Venereology, ed al a lty, ed al n er ty o a Summary. presence of several hairs
FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI B D S B S M Department of Dermatology and Venereology, ed al a lty, ed al n er ty o a Summary. presence of several hairs
Trichoscopic findings in cicatricial alopecias and hair shaft disorders and its application in histopathology
 International Journal of Research in Medical Sciences Khadatkar AS et al. Int J Res Med Sci. 2017 Dec;5(12):5254-5259 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175435
International Journal of Research in Medical Sciences Khadatkar AS et al. Int J Res Med Sci. 2017 Dec;5(12):5254-5259 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175435
Tufted folliculitis of the scalp: a distinctive clinicohistological variant of folliculitis decalvans
 British Journal of Dermatology 1998; 138: 799 805. Tufted folliculitis of the scalp: a distinctive clinicohistological variant of folliculitis decalvans G.ANNESSI Department of Dermatology and Dermatopathology,
British Journal of Dermatology 1998; 138: 799 805. Tufted folliculitis of the scalp: a distinctive clinicohistological variant of folliculitis decalvans G.ANNESSI Department of Dermatology and Dermatopathology,
FAST FACTS FOR BOARD REVIEW
 FAST FACTS FOR BOARD REVIEW Series Editor: William W. Huang, MD, MPH Common Hair Disorders Rita Pichardo-Geisinger, MD Dr. Pichardo-Geisinger is Associate Professor of Dermatology, Wake Forest Baptist
FAST FACTS FOR BOARD REVIEW Series Editor: William W. Huang, MD, MPH Common Hair Disorders Rita Pichardo-Geisinger, MD Dr. Pichardo-Geisinger is Associate Professor of Dermatology, Wake Forest Baptist
Dutasteride female pattern hair loss management 49, 50 male baldness management 41, 42 Dyeing, see Hair care
 Subject Index Acne keloidalis nuchae, ethnic patients 146, 147 Actinic keratosis, ultraviolet radiation exposure 108 Aging hair effects 4, 5 melanocyte aging 130 132 molecular mechanisms 5 7 pigment loss,
Subject Index Acne keloidalis nuchae, ethnic patients 146, 147 Actinic keratosis, ultraviolet radiation exposure 108 Aging hair effects 4, 5 melanocyte aging 130 132 molecular mechanisms 5 7 pigment loss,
Case Report DOI: /ourd Georgia Dermatopathology Associates, Atlanta, Georgia, USA 2
 Case Report DOI: 10.7241/ourd.20143.72 CENTRAL CENTRIFUGAL CICATRICIAL ALOPECIA AMALGAMATED WITH ALOPECIA AREATA: IMMUNOLOGIC FINDINGS Ana Maria Abreu Velez 1, Bruce R. Smoller 2, Michael S. Howard 1 Source
Case Report DOI: 10.7241/ourd.20143.72 CENTRAL CENTRIFUGAL CICATRICIAL ALOPECIA AMALGAMATED WITH ALOPECIA AREATA: IMMUNOLOGIC FINDINGS Ana Maria Abreu Velez 1, Bruce R. Smoller 2, Michael S. Howard 1 Source
Discoid Lupus Erythematosus
 S023 Hair and Scalp Dermoscopy Discoid Lupus Erythematosus Bruna Duque Estrada, M.D. Instituto de Dermatologia Prof. Rubem David Azulay Rio de Janeiro, Brazil. Disclosure of Relationship with Industry
S023 Hair and Scalp Dermoscopy Discoid Lupus Erythematosus Bruna Duque Estrada, M.D. Instituto de Dermatologia Prof. Rubem David Azulay Rio de Janeiro, Brazil. Disclosure of Relationship with Industry
SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS
 EUROPEAN JOURNAL OF INFLAMMATION Vol. 5, no. 1, 23-27 (2007) SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS G.I. ATHANASIADIS, E.
EUROPEAN JOURNAL OF INFLAMMATION Vol. 5, no. 1, 23-27 (2007) SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS G.I. ATHANASIADIS, E.
What Are the Different Forms?
 SCARRING/CICATRICIAL ALOPECIA Scarring alopecia also known as cicatricial alopecia, refers to a collection of hair loss disorders that may be diagnosed in up to 3% of hair loss patients. It occurs worldwide
SCARRING/CICATRICIAL ALOPECIA Scarring alopecia also known as cicatricial alopecia, refers to a collection of hair loss disorders that may be diagnosed in up to 3% of hair loss patients. It occurs worldwide
An Epidemiological Study of 198 Cases of Primary Cicatricial Alopecia in Iran
 British Journal of Medicine & Medical Research 20(4): 1-6, 2017; Article no.bjmmr.27476 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org An Epidemiological Study of
British Journal of Medicine & Medical Research 20(4): 1-6, 2017; Article no.bjmmr.27476 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org An Epidemiological Study of
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Psoriatic Scarring Alopecia
 Psoriatic Scarring Alopecia Ming-Hsiung Yeh 1 Tsen-Fang Tsai 2 Cheng-Hsiang Hsiao 3 Psoriasis affects approximately 0.123% of the population in China. Scalp is the first site of involvement in nearly 50%
Psoriatic Scarring Alopecia Ming-Hsiung Yeh 1 Tsen-Fang Tsai 2 Cheng-Hsiang Hsiao 3 Psoriasis affects approximately 0.123% of the population in China. Scalp is the first site of involvement in nearly 50%
Pimples and Boils!! Dr Nathan Harvey Anatomical Pathology, PathWest
 Pimples and Boils!! Dr Nathan Harvey Anatomical Pathology, PathWest Overview & Learning Objectives Review the cardinal signs/symptoms of acute inflammation Review the histological features of acute inflammation
Pimples and Boils!! Dr Nathan Harvey Anatomical Pathology, PathWest Overview & Learning Objectives Review the cardinal signs/symptoms of acute inflammation Review the histological features of acute inflammation
Alopecia. Antonella Tosti. Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami
 Alopecia Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S049
Alopecia Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S049
Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience
 Original article CED Clinical and Experimental Dermatology Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience F. Mardones 1 and J. Shapiro
Original article CED Clinical and Experimental Dermatology Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience F. Mardones 1 and J. Shapiro
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1416-1422 Trichoscopic Clues for Diagnosis of Patchy Scalp Alopecia in the Egyptian Patients Abd Elrauof Mohamed AL Mohsen, Mohamed
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1416-1422 Trichoscopic Clues for Diagnosis of Patchy Scalp Alopecia in the Egyptian Patients Abd Elrauof Mohamed AL Mohsen, Mohamed
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Clinicopathologic Self-Assessment
 Clinicopathologic Self-Assessment Handout Symposium (S003), July 27 th 2017 Maija Kiuru MD PhD Assistant Professor, Departments of Dermatology & Pathology University of California Davis CASE 1: History
Clinicopathologic Self-Assessment Handout Symposium (S003), July 27 th 2017 Maija Kiuru MD PhD Assistant Professor, Departments of Dermatology & Pathology University of California Davis CASE 1: History
Histologic Features of Alopecias: Part II: Scarring Alopecias
 Actas Dermosifiliogr. 2015;106(4):260-270 REVIEW Histologic Features of Alopecias: Part II: Scarring Alopecias C. Bernárdez, A.M. Molina-Ruiz, L. Requena Servicio de Dermatología, Fundación Jiménez Díaz,
Actas Dermosifiliogr. 2015;106(4):260-270 REVIEW Histologic Features of Alopecias: Part II: Scarring Alopecias C. Bernárdez, A.M. Molina-Ruiz, L. Requena Servicio de Dermatología, Fundación Jiménez Díaz,
Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp
 Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.214 ORIGINAL ARTICLE Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp Woo-Haing Shim 1, Seung-Wook Jwa
Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.214 ORIGINAL ARTICLE Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp Woo-Haing Shim 1, Seung-Wook Jwa
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
STUDY. Histopathologic Features of Alopecia Areata
 Histopathologic Features of Alopecia Areata A New Look David A. Whiting, MD, FRCP(Edin) STUDY Background: A peribulbar lymphocytic infiltrate is the expected histologic feature of alopecia areata, but
Histopathologic Features of Alopecia Areata A New Look David A. Whiting, MD, FRCP(Edin) STUDY Background: A peribulbar lymphocytic infiltrate is the expected histologic feature of alopecia areata, but
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Daniel Asz Sigall, MD MEXICO
 Daniel Asz Sigall, MD MEXICO Scalp dermoscopy 1) Hair shaft diameter heterogeneity 2) Short regrowing hairs 3) Single- hair pilosebaceous units 4) Yellow dots 5) peripilar sign 6) Honeycomb pigmentation
Daniel Asz Sigall, MD MEXICO Scalp dermoscopy 1) Hair shaft diameter heterogeneity 2) Short regrowing hairs 3) Single- hair pilosebaceous units 4) Yellow dots 5) peripilar sign 6) Honeycomb pigmentation
TUFTED FOLLICULITIS: AN EASILY MISSED ENTITY Sowmya Naga Dogiparthi 1, M. Krishnakanth 2, S. Adikrishnan 3, Adithya B 4, Sudha R 5
 TUFTED FOLLICULITIS: AN EASILY MISSED ENTITY Sowmya Naga Dogiparthi 1, M. Krishnakanth 2, S. Adikrishnan 3, Adithya B 4, Sudha R 5 HOW TO CITE THIS ARTICLE: Sowmya Naga Dogiparthi, M. Krishnakanth, S.
TUFTED FOLLICULITIS: AN EASILY MISSED ENTITY Sowmya Naga Dogiparthi 1, M. Krishnakanth 2, S. Adikrishnan 3, Adithya B 4, Sudha R 5 HOW TO CITE THIS ARTICLE: Sowmya Naga Dogiparthi, M. Krishnakanth, S.
Primary Scarring Alopecia: Clinical-Pathological Review of 72 Cases and Review of the Literature
 Original Article Skin Appendage Disord 217;:12 14 Received: January 1, 217 Accepted: February 28, 217 Published online: April 8, 217 Primary Scarring Alopecia: Clinical-Pathological Review of 72 Cases
Original Article Skin Appendage Disord 217;:12 14 Received: January 1, 217 Accepted: February 28, 217 Published online: April 8, 217 Primary Scarring Alopecia: Clinical-Pathological Review of 72 Cases
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123
 BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
Conflicts. Objectives. University of Texas Health Science Center at San Antonio. Pediatrics Grand Rounds 24 August Pediatric Dermatology 101
 Pediatric Dermatology 101 John C. Browning, MD, FAAD, FAAP Conflicts Investigator: ViroXis Advisor: ViroXis Advisory Board: TopMD Speaker: Galderma Objectives Understand the meaning and importance of cutaneous
Pediatric Dermatology 101 John C. Browning, MD, FAAD, FAAP Conflicts Investigator: ViroXis Advisor: ViroXis Advisory Board: TopMD Speaker: Galderma Objectives Understand the meaning and importance of cutaneous
This section covers the basic knowledge of normal skin structure and function required to help understand how skin diseases occur.
 Background Knowledge Functions of normal skin Background Knowledge This section covers the basic knowledge of normal skin structure and function required to help understand how skin diseases occur. Learning
Background Knowledge Functions of normal skin Background Knowledge This section covers the basic knowledge of normal skin structure and function required to help understand how skin diseases occur. Learning
Frontal fibrosing alopecia severity index (FFASI): a validated scoring system for assessing frontal fibrosing alopecia
 Received Date : 22-Jul-2015 Accepted Article Revised Date : 10-Jan-2016 Accepted Date : 11-Jan-2016 Article type : Research Letter Frontal fibrosing alopecia severity index (FFASI): a validated scoring
Received Date : 22-Jul-2015 Accepted Article Revised Date : 10-Jan-2016 Accepted Date : 11-Jan-2016 Article type : Research Letter Frontal fibrosing alopecia severity index (FFASI): a validated scoring
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
Hair disorders Antonella Tosti
 Hair disorders Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti,
Hair disorders Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti,
GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM
 GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM Telogen effluvium is a form of diffuse hair loss that occurs during the telogen or resting phase of the hair growth cycle. Telogen
GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM Telogen effluvium is a form of diffuse hair loss that occurs during the telogen or resting phase of the hair growth cycle. Telogen
A 40-year old male with follicular papule and pustule at central face area for 3 months
 A 40-year old male with follicular papule and pustule at central face area for 3 months GMS- Neg AFB-Neg Fite stain - neg HISTOPATHOLOGICAL DIFFERENTIAL DIAGNOSIS CASEOUS GRANULOMA INFECTION -MYCOBACTERIUM
A 40-year old male with follicular papule and pustule at central face area for 3 months GMS- Neg AFB-Neg Fite stain - neg HISTOPATHOLOGICAL DIFFERENTIAL DIAGNOSIS CASEOUS GRANULOMA INFECTION -MYCOBACTERIUM
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
B. Incorrect! The ectoderm does not produce the dermis. C. Incorrect! The dermis is derived from the mesoderm.
 Human Anatomy - Problem Drill 04: The Integumentary System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. From the inner cell
Human Anatomy - Problem Drill 04: The Integumentary System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. From the inner cell
OBSERVATION. Fibrosing Alopecia in a Pattern Distribution
 Fibrosing Alopecia in a Pattern Distribution Patterned Lichen Planopilaris or Androgenetic Alopecia With a Lichenoid Tissue Reaction Pattern? Martin S. Zinkernagel, Cand Med; Ralph M. Trüeb, MD OBSERVATION
Fibrosing Alopecia in a Pattern Distribution Patterned Lichen Planopilaris or Androgenetic Alopecia With a Lichenoid Tissue Reaction Pattern? Martin S. Zinkernagel, Cand Med; Ralph M. Trüeb, MD OBSERVATION
COPYRIGHTED MATERIAL. Introduction CHAPTER 1. Introduction
 CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
Diploma examination. Dermatopathology: First paper. Tuesday 21 March Candidates must answer FOUR questions ONLY. Time allowed: Three hours
 Dermatopathology: First paper Tuesday 21 March 2017 1. Discuss the role of fluorescent in-situ hybridization (FISH) and emerging molecular techniques in the diagnosis of cutaneous melanocytic lesions,
Dermatopathology: First paper Tuesday 21 March 2017 1. Discuss the role of fluorescent in-situ hybridization (FISH) and emerging molecular techniques in the diagnosis of cutaneous melanocytic lesions,
Nkanyezi Ferguson, MD, FAAD University of Iowa Hospital and Clinics Iowa City, IA
 Nkanyezi Ferguson, MD, FAAD University of Iowa Hospital and Clinics Iowa City, IA U030 - Hair Care Practices and Hair Disorders in Skin of Color DISCLOSURES No relevant relationships with industry To discuss
Nkanyezi Ferguson, MD, FAAD University of Iowa Hospital and Clinics Iowa City, IA U030 - Hair Care Practices and Hair Disorders in Skin of Color DISCLOSURES No relevant relationships with industry To discuss
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Strathprints Institutional Repository
 Strathprints Institutional Repository Holmes, S. and Ryan, T. and Young, D. and Harries, M. (2016) Frontal fibrosing alopecia severity index (FFASI) : a validated scoring system for assessing frontal fibrosing
Strathprints Institutional Repository Holmes, S. and Ryan, T. and Young, D. and Harries, M. (2016) Frontal fibrosing alopecia severity index (FFASI) : a validated scoring system for assessing frontal fibrosing
Hair and Scalp Changes in Cutaneous and Systemic Lupus Erythematosus
 Am J Clin Dermatol https://doi.org/10.1007/s40257-018-0363-8 REVIEW ARTICLE Hair and Scalp Changes in Cutaneous and Systemic Lupus Erythematosus Siriorn Udompanich 1 Kumutnart Chanprapaph 1 Poonkiat Suchonwanit
Am J Clin Dermatol https://doi.org/10.1007/s40257-018-0363-8 REVIEW ARTICLE Hair and Scalp Changes in Cutaneous and Systemic Lupus Erythematosus Siriorn Udompanich 1 Kumutnart Chanprapaph 1 Poonkiat Suchonwanit
Authors: Raja ni N a lluri A a nd M at t hew H a r rie s B. Hair follicles, the hair cycle and hair loss ABSTRACT. Introduction
 CME DERMATOLOGY Clinical Medicine 2016 Vol 16, No 1: 74 8 Alopecia in general medicine Authors: Raja ni N a lluri A a nd M at t hew H a r rie s B ABSTRACT Appreciation of different types of hair loss (alopecia)
CME DERMATOLOGY Clinical Medicine 2016 Vol 16, No 1: 74 8 Alopecia in general medicine Authors: Raja ni N a lluri A a nd M at t hew H a r rie s B ABSTRACT Appreciation of different types of hair loss (alopecia)
Lymphomatoid Papulosis 3 Case Reports
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
Table of Contents: Part 1 Medical Dermatology. Chapter 1 Acneiform Disorders. Acne. Acne Vulgaris. Pomade Acne. Steroid Acne
 Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
Table of Contents: Part 1 Medical Dermatology Chapter 1 Acneiform Disorders Acne Acne Vulgaris Pomade Acne Steroid Acne Infantile Acne Pediatric Perspectives Neonatal Acne (Acne Neonatorum) Pediatric Perspectives
Periocular skin cancer
 Periocular skin cancer Information for patients Skin cancer involving the skin of the eyelid or around the eye is called a periocular skin cancer. Eyelid skin cancers occur most often on the lower eyelid,
Periocular skin cancer Information for patients Skin cancer involving the skin of the eyelid or around the eye is called a periocular skin cancer. Eyelid skin cancers occur most often on the lower eyelid,
Skin Deep: Cutaneous Lupus. Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016
 Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
ISPUB.COM. A Case of Actinic Lichen Planus. K Choi, H Kim, H Kim, Y Park INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
Skin lesions The Good and the Bad. Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry
 Skin lesions The Good and the Bad Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry Case 1 32 year old woman Australian Lesion on back New hair growing
Skin lesions The Good and the Bad Dr Virginia Hubbard Ipswich Hospital NHS Trust Barts and the London School of Medicine and Dentistry Case 1 32 year old woman Australian Lesion on back New hair growing
Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady
 Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Update in deposition diseases
 Genoa, Italy Update in deposition diseases Prof. Franco Rongioletti, Section of Dermatology, Chair of Dermatopathology, University of Genoa,Italy Cutaneous deposition disorders Endogenous Exogenous Cutaneous
Genoa, Italy Update in deposition diseases Prof. Franco Rongioletti, Section of Dermatology, Chair of Dermatopathology, University of Genoa,Italy Cutaneous deposition disorders Endogenous Exogenous Cutaneous
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
Case No. 5; Slide No. B13/8956/2
 Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
Lichen planus along with Blaschko lines "Blaschkoian lichen planus"
 Original Article Lichen planus along with Blaschko lines "Blaschkoian lichen planus" Hossein Kavoussi, Mazaher Ramazani, Elias Salimi Dermatology Department, Kermanshah University of Medical Sciences,
Original Article Lichen planus along with Blaschko lines "Blaschkoian lichen planus" Hossein Kavoussi, Mazaher Ramazani, Elias Salimi Dermatology Department, Kermanshah University of Medical Sciences,
Histopathology: granulomatous inflammation, including tuberculosis
 Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
Egyptian Dermatology Online Journal Vol. 5 No 2:16, December Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris
 Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris Pathak D.* and Thapa A** Egyptian Dermatology Online Journal 5 (2): 16 * Consultant Dermatologist, Delhi Dermatology Group Kubba,
Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris Pathak D.* and Thapa A** Egyptian Dermatology Online Journal 5 (2): 16 * Consultant Dermatologist, Delhi Dermatology Group Kubba,
Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs
 Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs Classification of Body Membranes Epithelial membranes Cutaneous
Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs Classification of Body Membranes Epithelial membranes Cutaneous
Chapter 4 Opener Pearson Education, Inc.
 Chapter 4 Opener Introduction The integumentary system is composed of: Skin Hair Nails Sweat glands Oil glands Mammary glands The skin is the most visible organ of the body Clinicians can tell a lot about
Chapter 4 Opener Introduction The integumentary system is composed of: Skin Hair Nails Sweat glands Oil glands Mammary glands The skin is the most visible organ of the body Clinicians can tell a lot about
Test your knowledge with multiple-choice cases. What are these speckled spots?
 Test your knowledge with multiple-choice cases Case 1 What are these speckled spots? A speckled, pigmented lesion is noticed on the upper arm of a 10-year-old girl. Her mother says the lesion has been
Test your knowledge with multiple-choice cases Case 1 What are these speckled spots? A speckled, pigmented lesion is noticed on the upper arm of a 10-year-old girl. Her mother says the lesion has been
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
ABCD rule. apocrine glands. arrector pili. ceruminous glands. contact dermatitis
 ABCD rule assessing moles: asymmetric, broder irregularity, color, diameter (larger than 6mm) apocrine glands arrector pili sweat glands in the pubic and underarm areas that secrete thicker sweat, that
ABCD rule assessing moles: asymmetric, broder irregularity, color, diameter (larger than 6mm) apocrine glands arrector pili sweat glands in the pubic and underarm areas that secrete thicker sweat, that
Chapter 19 Hidradenitis Suppurativa
 1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease:
 Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
SEBACEOUS NEOPLASMS. Dr. Prachi Saraogi Clinical Fellow in Dermatology
 SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls
 Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
Integumentary System-Skin and Body Coverings
 Integumentary System-Skin and Body Coverings List the four types of epithelial or connective membranes. The epithelial cutaneous includes your and is exposed to the. Its function is to. An example is..
Integumentary System-Skin and Body Coverings List the four types of epithelial or connective membranes. The epithelial cutaneous includes your and is exposed to the. Its function is to. An example is..
family study of seven male cases and six female
 36 J Med Genet 1992; 29: 36-40 Netherlands Ophthalmic Research Institute, Department of Ophthalmogenetics, Amsterdam, The L D M van Osch E Veldman Department of Dermato-Venereology, Subdivision of Paediatric
36 J Med Genet 1992; 29: 36-40 Netherlands Ophthalmic Research Institute, Department of Ophthalmogenetics, Amsterdam, The L D M van Osch E Veldman Department of Dermato-Venereology, Subdivision of Paediatric
BSD SELF-ASSESSMENT CASES 21-24
 BSD SELF-ASSESSMENT CASES 21-24 EDINBURGH, 2 JULY 2018 LASZLO IGALI CASE 21 CLINICAL HISTORY Female, 43 years, nodule on left side of face/jaw angle area. Slow growth over years. MACRO (NOT GIVEN) Skin
BSD SELF-ASSESSMENT CASES 21-24 EDINBURGH, 2 JULY 2018 LASZLO IGALI CASE 21 CLINICAL HISTORY Female, 43 years, nodule on left side of face/jaw angle area. Slow growth over years. MACRO (NOT GIVEN) Skin
I have a skin lump doc! What s next? 12 th August 2017 Dr. Sue-Ann Ho Ju Ee
 I have a skin lump doc! What s next? 12 th August 2017 Dr. Sue-Ann Ho Ju Ee Some thoughts Is this skin cancer? How common is this? How likely is this in this patient? What happens next if it s something
I have a skin lump doc! What s next? 12 th August 2017 Dr. Sue-Ann Ho Ju Ee Some thoughts Is this skin cancer? How common is this? How likely is this in this patient? What happens next if it s something
أملس عضلي غرن = Leiomyosarcoma. Leiomyosarcoma 1 / 5
 Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
HOW TO BEST MANAGE ALOPECIA IN Kristen Fernandez, MD Department of Dermatology University of Missouri Harry S Truman VA
 HOW TO BEST MANAGE ALOPECIA IN 2018 Kristen Fernandez, MD Department of Dermatology University of Missouri Harry S Truman VA MOST COMMON TYPES OF ALOPECIA Non scarring Androgenetic alopecia Alopecia areata
HOW TO BEST MANAGE ALOPECIA IN 2018 Kristen Fernandez, MD Department of Dermatology University of Missouri Harry S Truman VA MOST COMMON TYPES OF ALOPECIA Non scarring Androgenetic alopecia Alopecia areata
Introduction. Skin and Body Membranes. Cutaneous Membranes Skin 9/14/2017. Classification of Body Membranes. Classification of Body Membranes
 Introduction Skin and Body Membranes Body membranes Cover surfaces Line body cavities Form protective and lubricating sheets around organs Classified in 5 categories Epithelial membranes 3 types- cutaneous,
Introduction Skin and Body Membranes Body membranes Cover surfaces Line body cavities Form protective and lubricating sheets around organs Classified in 5 categories Epithelial membranes 3 types- cutaneous,
Snapshot Dx Quiz: September 2018 Detailed Answers
 Snapshot Dx Quiz: September 2018 Detailed Answers Cynthia X. Wang, BA 1 Milan J. Anadkat, MD 1,2 1 Washington University School of Medicine, St. Louis, Missouri 2 Division of Dermatology, St. Louis, Missouri
Snapshot Dx Quiz: September 2018 Detailed Answers Cynthia X. Wang, BA 1 Milan J. Anadkat, MD 1,2 1 Washington University School of Medicine, St. Louis, Missouri 2 Division of Dermatology, St. Louis, Missouri
My Method for Approaching Skin Biopsies
 My Method for Approaching Skin Biopsies P A U L H A U N, MD, MS, F A A D A S S I S T A N T P R O F E S S O R D E R M A T O L O G Y A N D D E R M A T O P A T H O L O G Y D E P A R T M E N T O F D E R M
My Method for Approaching Skin Biopsies P A U L H A U N, MD, MS, F A A D A S S I S T A N T P R O F E S S O R D E R M A T O L O G Y A N D D E R M A T O P A T H O L O G Y D E P A R T M E N T O F D E R M
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges
 Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Rameshwar Gutte and Uday Khopkar
 Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Update on African American Hair and Scalp Disorders
 Update on African American Hair and Scalp Disorders Heather Woolery-Lloyd, M.D. Director of Ethnic Skin Care Voluntary Assistant Professor Miller/University of Miami School of Medicine Department of Dermatology
Update on African American Hair and Scalp Disorders Heather Woolery-Lloyd, M.D. Director of Ethnic Skin Care Voluntary Assistant Professor Miller/University of Miami School of Medicine Department of Dermatology
7/10/18. Introduction. Integumentary System. Physiology. Anatomy. Structure of the Skin. Epidermis
 Introduction Integumentary System Chapter 22 Skin is largest and heaviest organ of body (7% of body weight) Houses receptors for touch, heat, cold, movement, and vibration No other body system is more
Introduction Integumentary System Chapter 22 Skin is largest and heaviest organ of body (7% of body weight) Houses receptors for touch, heat, cold, movement, and vibration No other body system is more
Dermoscopic patterns in active and regressive lichen planus and lichen planus variants: a morphological study
 DERMTOLOGY PRCTICL & CONCEPTUL www.derm101.com Dermoscopic patterns in active and regressive lichen planus and lichen planus variants: a morphological study Şule Güngör 1, Ilteriş O. Topal 1, Emek K. Göncü
DERMTOLOGY PRCTICL & CONCEPTUL www.derm101.com Dermoscopic patterns in active and regressive lichen planus and lichen planus variants: a morphological study Şule Güngör 1, Ilteriş O. Topal 1, Emek K. Göncü
Porokeratosis: Introduction
 Porokeratosis: Introduction Benign epidermal proliferation Distinct clinical & histologic features 5 clinical subtypes Erroneously named porokeratosis CLINICAL SUBTYPES 1. Porokeratosis of Mibelli 2. Disseminated
Porokeratosis: Introduction Benign epidermal proliferation Distinct clinical & histologic features 5 clinical subtypes Erroneously named porokeratosis CLINICAL SUBTYPES 1. Porokeratosis of Mibelli 2. Disseminated
Dermatopathology Cytokeratin expression in pilonidal sinus
 British Journal of Dermatology 2002; 146: 409 413. Dermatopathology Cytokeratin expression in pilonidal sinus I.KUROKAWA, S.NISHIJIMA,* K.SUZUKI, K.KUSUMOTO, H.SENSAKI, N.SHIKATA AND A.TSUBURA Department
British Journal of Dermatology 2002; 146: 409 413. Dermatopathology Cytokeratin expression in pilonidal sinus I.KUROKAWA, S.NISHIJIMA,* K.SUZUKI, K.KUSUMOTO, H.SENSAKI, N.SHIKATA AND A.TSUBURA Department
