Epidermolysis Bullosa Acquisita: A Retrospective Clinical Analysis of 30 Cases
|
|
|
- Elwin Mills
- 5 years ago
- Views:
Transcription
1 Acta Derm Venereol 2011 Epub ahead of print CLINICAL REPORT Epidermolysis Bullosa Acquisita: A Retrospective Clinical Analysis of 30 Cases Jong Hoon Kim 1, Yeon Hee Kim 2 and Soo-Chan Kim 1 1 Department of Dermatology and Cutaneous Biology Research Institute, Yonsei University College of Medicine, Seoul, Korea, and 2 Department of Biostatistics, University of Pittsburgh, Pittsburgh, USA Epidermolysis bullosa acquisita (EBA) is an acquired, autoimmune blistering disorder caused by autoantibody production against type VII collagen. The aim of this study was to examine the clinical types, treatments, and outcomes of 30 patients with EBA. In our cohort, the median age of onset was 44.0 years, with a similar incidence for both genders (46.7% male, 53.3% female). The majority of patients had classic type (36.7%) and bullous pemphigoid (BP)-like type (46.7%) EBA. The remaining patients had mucous membrane pemphigoid-like (6.7%), Brunsting-Perry pemphigoid-like (6.7%), and linear IgA bullous dermatosis-like type (3.3%) EBA. All patients were treated initially with a combination of methylprednisolone, dapsone and colchicine. No significant differences in time to remission were identified between patients with classic vs. BP-like EBA. In a second subset analysis of 19 patients, a group treated with high-dose (> 8 mg) methylprednisolone achieved remission earlier (median time to remission: 3 months) than a group treated with low-dose ( 8 mg) methylprednisolone (median time to remission: 12 months), irrespective of clinical type (p = 0.003). Key words: epidermolysis bullosa acquisita; retrospective study, clinical study remission. (Accepted November 10, 2010.) Acta Derm Venereol 2011; 91: XX XX. Soo-Chan Kim, Department of Dermatology, Yonsei University College of Medicine, Gangnam Severance Hospital, 712 Eonjuro, Gangnam-gu, Seoul , Korea. kimsc@yuhs.ac Epidermolysis bullosa acquisita (EBA) is a blistering disease associated with autoantibody production against type VII collagen, the major component of the anchoring fibrils that connect the basement membrane zone to the papillary dermis (1, 2). Although the exact pathophysiologic process in EBA remains unclear, circulating autoantibodies against type VII collagen in patients with EBA ultimately result in subepidermal blister formation with concomitant inflammation, milia and scarring (3). The mucocutaneous lesions of EBA can be quite varied and mimic other types of autoimmune bullous disease. Currently, 5 clinical presentations of EBA have been identified: (i) classic (4); (ii) bullous pemphigoid (BP)-like (5); (iii) mucous membrane pemphigoid (MMP)-like (6); (iv) Brunsting-Perry pemphigoid-like (7); and (v) linear lga bullous dermatosis (LAD)-like type (Table I) (8). The classic form of EBA is a noninflammatory mechanobullous disease primarily involving trauma-prone areas of skin, such as the hands, elbows, knees, and feet, and in some cases the oral mucosa. BP-like EBA is an inflammatory vesiculobullous eruption that mainly involves the trunk, central body, extremities, skin folds and, in some cases, the oral mucosa. Individuals with disease that primarily affects mucosal surfaces are defined as having the MMP-like EBA, while Brunsting-Perry pemphigoid-like EBA is a chronic, recurrent blistering disease confined to the head and neck. LAD-like type presents with linear IgA deposits in the basement membrane zone that can be observed with direct immunofluorescence (9). EBA is a chronic disease that is often refractory to many treatment modalities. Generally, patients with EBA require supportive care, such as wound management and education regarding trauma prevention, especially in individuals with the classic mechanobullous type of the disease. However, while some patients with EBA respond well to treatment with dapsone (10), colchicines (11) and cyclosporine, many patients, particularly those with Table I. Clinical types of epidermolysis bullosa acquisita (EBA) Clinical type Classic EBA Bullous pemphigoid-like type EBA Mucous membrane pemphigoid-like type EBA Brunsting-Perry pemphigoid-like type EBA Linear IgA dermatosis-like type EBA A non-inflammatory mechanobullous disease primarily involving trauma-prone areas of skin, such as the hands, elbows, knees, and feet, and in some cases the oral mucosa An inflammatory vesiculobullous eruption that mainly involves the trunk, central body, extremities, skin folds, and in some cases the oral mucosa A disease that primarily affects mucosal surfaces A chronic, recurrent blistering disease confined to the head and neck A disease that presents with linear IgA deposits in the basement membrane zone that can be observed with direct immunofluorescence 2011 The Authors. doi: / Journal Compilation 2011 Acta Dermato-Venereologica. ISSN
2 2 J. H. Kim et al. classic mechanobullous disease, respond poorly to systemic corticosteroids and immunosuppressive agents (e.g. azathioprine, methotrexate and cyclophosphamide) (9). More recently, both extracorporeal photochemotherapy (12) and intravenous immunoglobulin (13) have also been reported to be effective in some patients with EBA. To date, only a few clinical studies of EBA have been conducted, presumably because EBA is a relatively rare disease (14). No significant etiologic factors for EBA have been identified in the previous clinical studies, although one study did report an association between the HLA-DR2 allele and EBA (15). Most estimates indicate the prevalence of EBA to be 1 case per 1.3 million people in Germany and 4 cases per 3.6 million people in France (16, 17). Here, we conducted a retrospective clinical analysis of 30 patients with EBA to determine the clinical manifestations of the disease and evaluate treatment outcomes. Statistical analyses were employed to evaluate any differences in treatment outcome between classic and BP-like type EBA and to identify any correlations between systemic corticosteroid dose and therapeutic efficacy. MATERIALS AND METHODS All data for this study were collected retrospectively from the medical records of 30 patients diagnosed with EBA over a 16- year period ( ) in the Department of Dermatology of Gangnam Severance Hospital, Seoul, Korea. In all individuals, diagnosis was made by clinical and histologic features, and later confirmed through immunofluorescence and immunoblot analyses (Table II). In the present study, we evaluate age of onset, clinical type, duration of follow-up, medical treatments, comorbidities, and time to remission. Here, we used the definitions of remission for EBA by modification of definition of remission for pemphigus suggested by the International Pemphigus Committee (18). Complete remission (CR) off therapy was defined as the absence of new and/ or established lesions for at least two months with out treatment. Complete remission on therapy was defined as the absence of new lesions while the patient is receiving minimal therapy. Minimal therapy was defined as less than or equal to 8 mg/day of methylprednisolone with or without adjuvant therapy including dapsone and colchicines for at least two months. Partial remission (PR) off therapy was defined as the presence of transient new lesions that heal within one week without treatment for at least two months. Partial remission on minimal therapy was defined as the presence of transient new lesions that heal within one week while the patient is receiving minimal therapy. The treatment protocol for patients with EBA is described below. Initially, all patients were treated with combination therapy of low-dose methylprednisolone, dapsone and colchicine. Patients with mild clinical features (less than 10% of body involvement) initially were prescribed 8 mg/day of methylprednisolone, while patients with severe clinical features (more than 10% of body involvement) were prescribed > 8 mg/day of methylprednisolone. Systemic corticosteroid dosage was later adjusted by therapeutic response. For dapsone, patients were initially prescribed a dose of 25 mg/day, which Table II. Patient characteristics Patient No. Sex/age (years) a Clinical type DIF Salt-split DIF Salt-split IIF IIF Western blot 1 F/78 1 IgG, IgA, C3 Dermal Dermal 1:40 ND 2 F/24 1 IgG, IgA, C3 Dermal Negative 0 ND 3 F/37 1 IgG, IgA Dermal Negative 0 ND 4 F/66 1 IgG, C3 Dermal Dermal 1:20 Positive 5 F/68 1 IgG, C3 Dermal Dermal 1:160 ND 6 F/41 1 Negative ND Dermal 1:40 Positive 7 M/59 1 Negative ND Dermal 1:160 Positive 8 F/83 1 C3 Dermal Dermal 1:5 Positive 9 M/73 1 IgG Dermal Dermal 1:10 Positive 10 M/60 1 IgG Dermal Negative 0 Positive 11 M/45 1 IgG, IgA Dermal Negative 0 ND 12 F/74 2 IgG, IgA, C3 Dermal Negative 0 ND 13 F/45 2 IgG, IgA, IgM, C3 Dermal Negative 0 Positive 14 F/55 2 IgG, IgA Dermal Negative 0 ND 15 F/35 2 IgG, C3 Dermal Dermal 1:20 ND 16 M/72 2 IgG, C3 Dermal Dermal 1:640 Positive 17 M/39 2 IgG, IgA, C3 Dermal Dermal 1:160 Positive 18 M/52 2 IgG, C3 Dermal Dermal 1:40 ND 19 M/31 2 IgG, IgA, C3 Dermal Dermal 1:16 Positive 20 F/47 2 IgG, C3 Dermal Negative 0 Negative 21 F/39 2 IgG, IgA, C3 Dermal Negative 0 ND 22 F/67 2 IgG, C3 Dermal Dermal 1:640 Positive 23 M/35 2 IgG, C3 Dermal Dermal 1:80 ND 24 M/70 2 IgG, IgA, C3 Dermal Negative 0 ND 25 M/55 2 IgG, C3 Dermal Dermal 1:20 Positive 26 F/66 3 Negative ND Dermal 1:320 Positive 27 M/66 3 IgG, C3 Dermal Negative 0 Negative 28 M/55 4 IgG, C3 Demral Negative 0 Negative 29 F/27 4 IgG, C3 Dermal Dermal 1:160 ND 30 M/29 5 IgA Dermal Negative 0 ND a Age at time of writing. Clinical type: 1 = classic type; 2 = bullous pemphigoid-like type; 3 = mucous membrane pemphigoid-like type; 4 = Brunsting-Perry pemphigoid-like type; 5 = linear IgA dermatosis-like type; ND: not done; DIF: direct immunofluoroscence; IIF: indirect immunofluoroscence
3 Clinical analysis of EBA 3 was gradually increased up to 100 mg/day as tolerated. For colchicine, patients were maintained on a dose of 1.2 mg/day. Other immunosuppressive medications, such as cyclophosphamide, mycophenolate mofetil, cyclosporine and azathioprine, were considered if patients did not respond to the combination therapy of methylprednisolone, dapsone and colchicine. To assess the relationship between systemic corticosteroid dose and therapeutic efficacy, we stratified the patients into two groups: a high-dose steroid (HDS) group that received > 8 mg/day of methylprednisolone for at least one month; and a low-dose steroid (LDS) group that received 8 mg/day of methylprednisolone for at least one month. We performed a subset analysis of 19 patients with EBA treated with methylprednisolone, dapsone and colchicine by a single physician. Patients who were prescribed other immunosuppressive agents, including systemic corticosteroid pulse therapy, cyclophosphamide, mycophenolate mofetil, cyclosporine or azathioprine, were excluded from this subgroup. Baseline characteristics were summarized by EBA type using descriptive statistics. All descriptive summaries are presented with a median and range for continuous variables and a count and percentage for categorical variables. Fisher s exact test and Wilcoxon rank-sum test were performed to compare the clinical features between two groups (classic vs. BP-like type and HDS vs. LDS group). Comparison of time to remission was done by log-rank test. All analyses were performed with SAS (version 9.1, SAS institute, North Carolina, USA) using an alpha level of RESULTS In our cohort, the median age at disease onset was 44.0 (range 21 79) years, with 14 (46.7%) male patients and 16 (53.3%) female patients. The median length of follow-up period was 23.0 (range ) months. Classification by clinical phenotype revealed 11 (36.7%) individuals with classic, 14 (46.7%) with BP-like, 2 (6.7%) with MMP-like, 2 (6.7%) with Brunsting-Perry pemphigoid-like, and 1 (3.3%) with LAD-like type. The clinical features of the varying EBA patient types are shown in Table III. No significant differences were identified between patients with classic and BP-like types in terms of sex (male 36.4% vs. 50%, p = ), age of onset (median age 58.0 years vs years, p = ), duration of follow-up (median duration 25.0 vs months, p = ), maximum methylprednisolone dose over a one-month period (median dose 8.0 vs mg, p = ) and oral involvement (7 of 11 patients vs. 6 of 14 patients). All patients were initially treated with combination therapy of methylprednisolone, dapsone and colchicine. Other immunosuppressive therapies, including cyclophosphamide, mycophenolate mofetil, cyclosporine or azathioprine, were prescribed for 6 (20%) patients who did not respond to the initial regimen (Table IV). Treatment was well tolerated in most patients, with the exception of one 37-year-old patient who developed a cataract after 10 years of corticosteroid therapy. After analyzing our database, the following diseases were considered as co-morbid disease associated with EBA: 3 patients with diabetes mellitus, two patients with systemic lupus erythematosus. Another patient died approximately one year after diagnosis as a result of an esophageal stricture secondary to mucosal involvement. The median time to remission for the 30 patients with EBA was 9 months. From a cross-sectional point of view, complete remission was observed in 33.3% of individuals (8/24), and partial remission in 20.8% (5/24) at one year after treatment initiation. Complete remission was achieved in 33.3% (5/15) of patients at 3 years after diagnosis, and 45.5% (5/11) at 6 years after diagnosis. Partial remission was seen in 33.3% of individuals (5/15) at 3 years after diagnosis and 45.5% (5/11) at 6 years after diagnosis (Fig. 1). We also compared median time to remission between patients with classic EBA (n = 11) and BP-like EBA (n = 14). The median time to remission was 10 months in classic patients with EBA and 18 months in BP-like patients with EBA (Table II). No statistical differences were identified between two types in time to remission (p = ) and complete remission (p = ) (Fig. 2). According to the treatment dosage of methylprednisolone, patients were stratified into the HDS group (6 patients), and the LDS group (13 patients). The resulting Kaplan Meier curves demonstrate that significantly better responses to treatment were achieved in the HDS group irrespective of clinical types. The median time to remission was 3 months in the HDS group and 12 months in LDS group (p = 0.003) (Fig. 3). Table III. Clinical features of epidermolysis bullosa acquisita (EBA) patients. No statistical differences were observed in age, sex, maximal dose of corticosteroid or oral involvement between classic and bullous pemphigoid (BP)-like EBA Clinical type Classic BP-like MMP-like Brunsting-Perry pemphigoid-like LAD-like Total Number of patients (M/F) 11 (4/7) 14 (7/7) 2 (1/1) 2 (1/1) 1 (1/0) 30 (14/16) Median age of onset, years (range) 58.0 (21 79) 43.0 (28 67) 56.5 (49 64) 24.5 (24 25) (21 79) Median follow-up duration, months (range) 25.0 (1 96) 23.0 ( ) 86.5 (21 152) 20.5 (13 28) ( ) Maximum dose of MPD at least 1 month, mg (range) 8.0 (0 48) 16.0 (4 72) (0 4) (0 72) Oral involvement, n (%) 7 (63.6) 6 (42.9) 2 (100) (50) Time to remission a, months, n a Complete remission plus partial remission. MMP: mucous membrane pemphigoid; LAD: linear IgA bullous dermatosis; MPD: methylprednisolone.
4 4 J. H. Kim et al. Table IV. Six patients who were treated with other immunosuppressive drugs Duration of treatment before the beginning of Sex/age Clinical other immunosuppressive Remission Pat. No. (years) types Immunosuppressive drugs drugs time 1 F/78 Classic Methylprednisolone pulse therapy (methylprednisolone 500 mg for 3 days) 1 month 3 months 3 F/37 Classic Mycophenolate mofetil 2000 mg 1 month 10 months Methylprednisolone pulse therapy (methylprednisolone 500 mg for 3 days) 13 F/45 BP-like Mycophenolate mofetil 1500 mg 36 months 72 months Pulse therapy with methylprednisolone and cyclophosphamide (methylprednisolone 500 mg for 3 days and cyclophosphamide 500 mg for 1 day) 17 M/39 BP-like Cyclosporine 100 mg 30 months 63 months 25 M/55 BP-like Azathioprine 100 mg 1 month No remission 26 F/66 MMP-like Pulse therapy with methylprednisolone and cyclophosphamide (methylprednisolone 500 mg for 3 days and cyclophosphamide 500 mg for 1 day) 1 month 23 months BP: bullous pemphigoid; MMP: mucous membrane pemphigoid. DISCUSSION Our results show that the classic and BP-like presentations are the two most common clinical types of this disease. In our cohort, generalized inflammatory BP-like EBA was slightly more common than the classic form, which primarily affects trauma-prone extensor skin surfaces. No comparisons between the other subtypes, including MMP-like, Brunsting-Perry pemphigoid-like, and LAD-like EBA, could be made due to the small number of patients in our cohort. We did not find the classic type to be statistically different from the BP-like type in terms of age of onset, sex, maximum prescribed dose of systemic corticosteroids and oral involvement. In our clinic, we used a combination of a low-dose systemic steroids, dapsone, and colchicine as a first-line therapy. Colchicine is often used as a first-line drug because of its low incidence of serious side-effects (11), and, in this study, all patients were prescribed colchicine at a dose of 1.2 mg/day. Dapsone is another safe and effective medication used in the treatment of EBA (10). In this study, all patients with EBA were initially prescribed dapsone at a dose of 25 mg/day, which was gradually increased up to 100 mg/day as tolerated. Although some previous reports recommend the use of high-dose systemic corticosteroids in EBA (19, 20), we use relatively low doses (8 mg for the classic type and 16 mg for BP-like type as median maximum methylprednisolone doses) to avoid the side-effects often associated with long-term corticosteroid use. Notably, we were able to achieve favorable outcomes (9 months of time to remission) without serious side-effects with this regimen. Although some data has linked EBA with inflammatory bowel disease (IBD) (21 23), none of the patients in our cohort had EBA with comorbid IBD. The incidence and prevalence of IBD in Korea are lower than that in North America and Europe, although they are increasing. In addition, IBD patients in Korea are associated with different genomics from those in Western countries (24). These reasons may explain the low incidence of IBD among our patients with EBA. Also, EBA has been reported to be associated with systemic diseases, including rheumatoid arthritis, diabetes mellitus, cryoglobulinaemia, psoriasis and systemic lupus erythematosus (9, 25). There were three patients with diabetes mellitus and two with systemic lupus erythematosus in our study. The most severe complication Fig. 1. Time to remission for 30 patients with epidermolysis bullosa acquisita (EBA). (A) Kaplan Meier curve of remission in EBA. Median time to remission was 9 months. (B) Cumulative remission rate of patients with EBA by treatment duration. One year after therapy initiation, partial remission (PR) was achieved in 20.8% (5/24 patients) and complete remission (CR) in 33.3% (8/24 patients).
5 Clinical analysis of EBA 5 Fig. 2. Comparison of time to remission between classic and bullous pemphigoid (BP)-like epidermolysis bullosa acquisita (EBA) (n = 25). (A) Kaplan Meier curve of remission (partial remission (PR) plus complete remission (CR)) in two different types: classic and BP-like type. No statistical differences were identified in the time to remission between classic (n = 11) and BP-like (n = 14) EBA (10 months vs. 18 months, p = ). (B) Kaplan Meier curve of CR showed that there were no statistical differences in the time to CR between classic and BP-like EBA (p = 0.94). (C), (D) Cumulative remission rate of classic and BP-like type by treatment duration. Rates of PR and CR between classic and BP-like type were assessed after the first year of treatment (PR; 11.1% vs. 30% CR; 44.4% vs. 20%) and the third year of treatment (PR; 50% vs. 50% CR; 50% vs. 33.3%). Time to CR was not different between classic and BP-like types (p = ). that developed in our patients with EBA was esophageal stricture, which correlated with severe mucosal involvement (26). Other minor common problems were secondary skin infections, milia, scarring and fibrosis. We also compared the demographics and clinical course of classic EBA with BP-like EBA. The classic presentation appears to convey a more favorable outcome, with faster median times to remission than the BP-like presentation. However, we did not find any statistical differences between the two types. In our comparison of the groups treated with low- and high-dose systemic corticosteroids, we were unable Fig. 3. Comparison of time to remission between high-dose steroid (HDS) and low-dose steroid (LDS) group (n = 19). A HDS group (n = 6) demonstrated better outcomes than a comparable LDS group (n = 13) (3 months vs. 12 months, p = 0.003). High dose: > 8 mg of methylprednisolone for at least one month; low dose: 8 mg of methylprednisolone for at least one month. to identify any differences in baseline demographics, including sex ratio, clinical types and median age of onset (Table V). However, the HDS group did show significantly shorter times to remission compared with the LDS group, irrespective of clinical type. Moreover, while the clinical disease activity of the HDS group was more severe at baseline, relatively better outcomes were nevertheless achieved in this group. These data suggest that higher doses of systemic corticosteroids (specifically > 8 mg/day of methylprednisolone) not only treat Table V. Demographics by high-dose steroid (HDS) and low-dose steroid (LDS) group. No statistical differences were observed in sex, clinical types, or age of onset between the HDS and LDS group (p = , and for each variable) LDS group HDS group p-value Male to female ratio 6:7 2: Clinical type, n (%) Classic 5 (71.4) 2 (28.6) BP-like 5 (62.5) 3 (37.5) MMP-like 1 (100) 0 (0) Brunsting-Perry pemphigoid-like 2 (100) 0 (0) LAD-like 0 (0) 1 (100) Age at onset, years, median (min, max) 44.0 (21.0, 79.0) 37.5 (28.0, 61.0) Time to remission, months BP: bullous pemphigoid; MMP: mucous membrane pemphigoid; LAD: linear IgA bullous dermatosis.
6 6 J. H. Kim et al. patients with EBA more effectively, but also expedite the time to remission. In conclusion, the median time to remission for EBA was 9 months in our cohort. No significant differences were identified between classic-type and BP-like type EBA in terms of age of onset, sex, treatment intensity, median time to remission and oral involvement. A group of patients treated with higher doses of corticosteroids (> 8 mg/day of methylprednisolone for at least one month) showed more favorable outcomes than individuals treated with lower doses of corticosteroids ( 8 mg/day of methylprednisolone for at least one month). REFERENCES 1. Woodley DT, Briggaman RA, O Keefe EJ, Inman AO, Queen LL, Gammon WR. Identification of the skin basement-membrane autoantigen in epidermolysis bullosa acquisita. N Engl J Med 1984; 310: Woodley DT, Burgeson RE, Lunstrum G, Bruckner- Tuderman L, Reese MJ, Briggaman RA. Epidermolysis bullosa acquisita antigen is the globular carboxyl terminus of type VII procollagen. J Clin Invest 1988; 81: Woodley DT, Chang C, Saadat P, Ram R, Liu Z, Chen M. Evidence that anti-type VII collagen antibodies are pathogenic and responsible for the clinical, histological, and immunological features of epidermolysis bullosa acquisita. J Invest Dermatol 2005; 124: Roenigk HH Jr., Ryan JG, Bergfeld WF. Epidermolysis bullosa acquisita. Report of three cases and review of all published cases. Arch Dermatol 1971; 103: Gammon WR, Briggaman RA, Woodley DT, Heald PW, Wheeler CE Jr. Epidermolysis bullosa acquisita a pemphigoid-like disease. J Am Acad Dermatol 1984; 11: Dahl MG. Epidermolysis bullosa acquisita a sign of cicatricial pemphigoid? Br J Dermatol 1979; 101: Kurzhals G, Stolz W, Meurer M, Kunze J, Braun-Falco O, Krieg T. Acquired epidermolysis bullosa with the clinical feature of Brunsting-Perry cicatricial bullous pemphigoid. Arch Dermatol 1991; 127: Hashimoto T, Ishiko A, Shimizu H, Tanaka T, Dodd HJ, Bhogal BS, et al. A case of linear IgA bullous dermatosis with IgA anti-type VII collagen autoantibodies. Br J Dermatol 1996; 134: Remington J, Chen M, Burnett J, Woodley DT. Autoimmunity to type VII collagen: epidermolysis bullosa acquisita. Curr Dir Autoimmun 2008; 10: Hughes AP, Callen JP. Epidermolysis bullosa acquisita responsive to dapsone therapy. J Cutan Med Surg 2001; 5: Cunningham BB, Kirchmann TT, Woodley D. Colchicine for epidermolysis bullosa acquisita. J Am Acad Dermatol 1996; 34: Miller JL, Stricklin GP, Fine JD, King LE, Arzubiaga MC, Ellis DL. Remission of severe epidermolysis bullosa acquisita induced by extracorporeal photochemotherapy. Br J Dermatol 1995; 133: Meier F, Sonnichsen K, Schaumburg-Lever G, Dopfer R, Rassner G. Epidermolysis bullosa acquisita: efficacy of high-dose intravenous immunoglobulins. J Am Acad Dermatol 1993; 29: Delgado L, Aoki V, Santi C, Gabbi T, Sotto M, Maruta C. Clinical and immunopathological evaluation of epidermolysis bullosa acquisita. Clin Exp Dermatol 2010; 36: Gammon WR, Heise ER, Burke WA, Fine JD, Woodley DT, Briggaman RA. Increased frequency of HLA-DR2 in patients with autoantibodies to epidermolysis bullosa acquisita antigen: evidence that the expression of autoimmunity to type VII collagen is HLA class II allele associated. J Invest Dermatol 1988; 91: Bernard P, Vaillant L, Labeille B, Bedane C, Arbeille B, Denoeux JP, et al. Incidence and distribution of subepidermal autoimmune bullous skin diseases in three French regions. Bullous Diseases French Study Group. Arch Dermatol 1995; 131: Zillikens D, Wever S, Roth A, Weidenthaler-Barth B, Hashimoto T, Brocker EB. Incidence of autoimmune subepidermal blistering dermatoses in a region of central Germany. Arch Dermatol 1995; 131: Murrell DF, Dick S, Ahmed AR, Amagai M, Barnadas MA, Borradori L, et al. Consensus statement on definitions of disease, end points, and therapeutic response for pemphigus. J Am Acad Dermatol 2008; 58: Engineer L, Ahmed AR. Emerging treatment for epidermolysis bullosa acquisita. J Am Acad Dermatol 2001; 44: Hallel-Halevy D, Nadelman C, Chen M, Woodley DT. Epidermolysis bullosa acquisita: update and review. Clin Dermatol 2001; 19: Chen M, O Toole EA, Sanghavi J, Mahmud N, Kelleher D, Weir D, et al. The epidermolysis bullosa acquisita antigen (type VII collagen) is present in human colon and patients with crohn s disease have autoantibodies to type VII collagen. J Invest Dermatol 2002; 118: Ray TL, Levine JB, Weiss W, Ward PA. Epidermolysis bullosa acquisita and inflammatory bowel disease. J Am Acad Dermatol 1982; 6: Raab B, Fretzin DF, Bronson DM, Scott MJ, Roenigk HH Jr., Medenica M. Epidermolysis bullosa acquisita and inflammatory bowel disease. JAMA 1983; 250: Kim ES, Kim WH. Inflammatory bowel disease in Korea: epidemiological, genomic, clinical, and therapeutic characteristics. Gut Liver 2010; 4: Ishii N, Hamada T, Dainichi T, Karashima T, Nakama T, Yasumoto S, et al. Epidermolysis bullosa acquisita: what s new? J Dermatol 2010; 37: Hughes BR, Horne J. Epidermolysis bullosa acquisita and total ulcerative colitis. J R Soc Med 1988; 81:
Epidermolysis Bullosa Acquisita
 Introduction Epidermolysis Bullosa Acquisita Pages with reference to book, From 192 To 194 Nasser Rashid Dar ( Departments of Dermatology, Combined Military Hospital, Peshawar. ) Ahsan Hameed, Ashfaq Ahmad
Introduction Epidermolysis Bullosa Acquisita Pages with reference to book, From 192 To 194 Nasser Rashid Dar ( Departments of Dermatology, Combined Military Hospital, Peshawar. ) Ahsan Hameed, Ashfaq Ahmad
Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis
 Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis A. España C. Sitaru* M. Pretel L. Aguado J. Jimenez# Department of Dermatology, University
Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis A. España C. Sitaru* M. Pretel L. Aguado J. Jimenez# Department of Dermatology, University
Citation for published version (APA): Buijsrogge, J. J. A. (2011). Unusual variants of subepidermal autoimmune bullous diseases. Groningen: s.n.
 University of Groningen Unusual variants of subepidermal autoimmune bullous diseases Buijsrogge, Jacqueline Johanna Angela IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Unusual variants of subepidermal autoimmune bullous diseases Buijsrogge, Jacqueline Johanna Angela IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Introduction to Pemphigoid: Spectrum of Disease & Treatment
 Introduction to Pemphigoid: Spectrum of Disease & Treatment A Razzaque Ahmed, MD Center for Blistering Diseases Boston, MA A.Razzaque.Ahmed@tufts.edu centerforblisteringdiseases.com SPECTRUM OF PEMPHIGOID
Introduction to Pemphigoid: Spectrum of Disease & Treatment A Razzaque Ahmed, MD Center for Blistering Diseases Boston, MA A.Razzaque.Ahmed@tufts.edu centerforblisteringdiseases.com SPECTRUM OF PEMPHIGOID
Background information of DIF
 Napa Dermatopathology Meeting 2018: Immunobullous Disease Whitney A. High, MD, JD, MEng whitney.high@ucdenver.edu Professor of Dermatology & Pathology Vice-Chairman, Dermatology Director of Dermatopathology
Napa Dermatopathology Meeting 2018: Immunobullous Disease Whitney A. High, MD, JD, MEng whitney.high@ucdenver.edu Professor of Dermatology & Pathology Vice-Chairman, Dermatology Director of Dermatopathology
Title. CitationBritish Journal of Dermatology, 155(5): Issue Date Doc URL. Rights. Type. File Information
 Title Childhood epidermolysis bullosa acquisita with autoa collagen : case report and review of the literature Author(s)Mayuzumi, M.; Akiyama, M.; Nishie, W.; Ukae, S.; Abe CitationBritish Journal of Dermatology,
Title Childhood epidermolysis bullosa acquisita with autoa collagen : case report and review of the literature Author(s)Mayuzumi, M.; Akiyama, M.; Nishie, W.; Ukae, S.; Abe CitationBritish Journal of Dermatology,
Autoimmune Diseases with Oral Manifestations
 Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
A case of bullous pemphigoid following pemphigus foliaceus
 #2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
#2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
Interesting Case Series. Linear IgA Bullous Dermatosis
 Interesting Case Series Linear IgA Bullous Dermatosis Sean Chen, BA, a Peter Mattei, MD, a Max Fischer, MD, MPH, a Joshua D. Gay, PA-C, b Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS, b and Leigh Ann
Interesting Case Series Linear IgA Bullous Dermatosis Sean Chen, BA, a Peter Mattei, MD, a Max Fischer, MD, MPH, a Joshua D. Gay, PA-C, b Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS, b and Leigh Ann
Bullous Pemphigoid with Lymphocytic Colitis: A Case Report and Short Literature Review
 Dermatol Ther (Heidelb) (2016) 6:437 441 DOI 10.1007/s13555-016-0135-4 CASE REPORT Bullous Pemphigoid with Lymphocytic Colitis: A Case Report and Short Literature Review Alexandra Sperl. Johann W. Bauer.
Dermatol Ther (Heidelb) (2016) 6:437 441 DOI 10.1007/s13555-016-0135-4 CASE REPORT Bullous Pemphigoid with Lymphocytic Colitis: A Case Report and Short Literature Review Alexandra Sperl. Johann W. Bauer.
Quality of Life Assessment in Korean Patients with Pemphigus
 Ann Dermatol Vol. 27, No. 5, 2015 http://dx.doi.org/10.5021/ad.2015.27.5.492 ORIGINAL ARTICLE Quality of Life Assessment in Korean Patients with Pemphigus Jae Yong Sung, Mi Ryung Roh, Soo-Chan Kim Department
Ann Dermatol Vol. 27, No. 5, 2015 http://dx.doi.org/10.5021/ad.2015.27.5.492 ORIGINAL ARTICLE Quality of Life Assessment in Korean Patients with Pemphigus Jae Yong Sung, Mi Ryung Roh, Soo-Chan Kim Department
STUDY. High Risk of Death in Elderly Patients With Extensive Bullous Pemphigoid
 STUDY High Risk of Death in Elderly Patients With Extensive Bullous Pemphigoid Jean-Claude Roujeau, MD; Catherine Lok, MD; Sylvie Bastuji-Garin, MD; Sami Mhalla, MD; Véronique Enginger, MD; Philippe Bernard,
STUDY High Risk of Death in Elderly Patients With Extensive Bullous Pemphigoid Jean-Claude Roujeau, MD; Catherine Lok, MD; Sylvie Bastuji-Garin, MD; Sami Mhalla, MD; Véronique Enginger, MD; Philippe Bernard,
Rituximab in refractory autoimmune bullous diseases
 Clinical dermatology Review article doi: 10.1111/j.1365-2230.2006.02151.x Rituximab in refractory autoimmune bullous diseases E. Schmidt, N. Hunzelmann,* D. Zillikens, E.-B. Bröcker and M. Goebeler Departments
Clinical dermatology Review article doi: 10.1111/j.1365-2230.2006.02151.x Rituximab in refractory autoimmune bullous diseases E. Schmidt, N. Hunzelmann,* D. Zillikens, E.-B. Bröcker and M. Goebeler Departments
A cross-sectional study of clinical, histopathological and direct immmunofluorescence diagnosis in autoimmune bullous diseases
 Original Article A cross-sectional study of clinical, histopathological and direct immmunofluorescence diagnosis in autoimmune bullous diseases Anchal Jindal, MD 1 Rushikesh Shah, MBBS 2 Neela Patel, MD
Original Article A cross-sectional study of clinical, histopathological and direct immmunofluorescence diagnosis in autoimmune bullous diseases Anchal Jindal, MD 1 Rushikesh Shah, MBBS 2 Neela Patel, MD
Treatment with steroids and immunosuppressants
 Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Acquired and Inherited Bullous Diseases
 Acquired and Inherited Bullous Diseases Erin Wei MD Brigham and Women s Hospital, Department of Dermatology Instructor, Harvard Medical School Director, Bullous Disease Clinic No disclosures Conflict of
Acquired and Inherited Bullous Diseases Erin Wei MD Brigham and Women s Hospital, Department of Dermatology Instructor, Harvard Medical School Director, Bullous Disease Clinic No disclosures Conflict of
NIH Public Access Author Manuscript Immunol Allergy Clin North Am. Author manuscript; available in PMC 2014 February 18.
 NIH Public Access Author Manuscript Published in final edited form as: Immunol Allergy Clin North Am. 2012 May ; 32(2): 317 vii. doi:10.1016/j.iac.2012.04.011. Dapsone in the management of the autoimmune
NIH Public Access Author Manuscript Published in final edited form as: Immunol Allergy Clin North Am. 2012 May ; 32(2): 317 vii. doi:10.1016/j.iac.2012.04.011. Dapsone in the management of the autoimmune
Original Contribution
 Direct Immunofluorescence Test of Skin Biopsy Samples Results of 204 Cases Kabir AN, 1 Das RK, 2 Kamal M 3 Direct immunofluorescence (DIF) test of skin and renal biopsy specimens is being done on regular
Direct Immunofluorescence Test of Skin Biopsy Samples Results of 204 Cases Kabir AN, 1 Das RK, 2 Kamal M 3 Direct immunofluorescence (DIF) test of skin and renal biopsy specimens is being done on regular
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
Clinical spectrum and therapeutic approach in pemphigus vulgaris
 Clinical spectrum and therapeutic approach in pemphigus vulgaris Michael Hertl Department of Dermatology and Allergology Philipps University, Marburg, Germany F125: Bullous Diseases: Diagnostic and Management
Clinical spectrum and therapeutic approach in pemphigus vulgaris Michael Hertl Department of Dermatology and Allergology Philipps University, Marburg, Germany F125: Bullous Diseases: Diagnostic and Management
Autoimmune bullous dermatoses
 Autoimmune bullous dermatoses Overview of serological diagnostics in autoimmune blister-forming diseases of the skin Pemphigoid diseases Pemphigus diseases Epidermolysis bullosa acquisita Dermatitis herpetiformis
Autoimmune bullous dermatoses Overview of serological diagnostics in autoimmune blister-forming diseases of the skin Pemphigoid diseases Pemphigus diseases Epidermolysis bullosa acquisita Dermatitis herpetiformis
Pemphigus in younger age group in Bangladeshi population
 ORIGINAL ARTICLE in younger age group in Bangladeshi population Abdul Wahab 1, MD, Lubna Khondker 1, MD, Jamal Uddin 1, MD, Ishrat Bhuiyan 2, MD Shirajul Islam Khan 3, MD, Zafrul Islam 1, MD, Rahmat Ali
ORIGINAL ARTICLE in younger age group in Bangladeshi population Abdul Wahab 1, MD, Lubna Khondker 1, MD, Jamal Uddin 1, MD, Ishrat Bhuiyan 2, MD Shirajul Islam Khan 3, MD, Zafrul Islam 1, MD, Rahmat Ali
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Dr Saleem Taibjee. Consultant Dermatologist & Dermatopathologist
 Dr Saleem Taibjee saleem.taibjee@dchft.nhs.uk Consultant Dermatologist & Dermatopathologist Case S14-10797 and S15-4023 F50. Previous blistering, now marked milia on dorsum of hands. 4mm punch biopsy The
Dr Saleem Taibjee saleem.taibjee@dchft.nhs.uk Consultant Dermatologist & Dermatopathologist Case S14-10797 and S15-4023 F50. Previous blistering, now marked milia on dorsum of hands. 4mm punch biopsy The
Bullous Eruption: A Manifestation of Lupus Erythematosus
 CONTINUING MEDICAL EDUCATION : A Manifestation of Lupus Erythematosus CPT Ronea Harris-Stith, USAF, MC; CPT Quenby L. Erickson, USAF, MC; Dirk M. Elston, MD; COL Kathleen David-Bajar, MC, USA GOAL To gain
CONTINUING MEDICAL EDUCATION : A Manifestation of Lupus Erythematosus CPT Ronea Harris-Stith, USAF, MC; CPT Quenby L. Erickson, USAF, MC; Dirk M. Elston, MD; COL Kathleen David-Bajar, MC, USA GOAL To gain
AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE
 AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE Ron Feldman, MD, PhD Assistant Professor of Dermatology Emory University ron.j.feldman@emory.edu Disclosures I have no conflict of interest to
AUTOIMMUNE BLISTERING DISEASES; WINDOW TO SYSTEMIC DISEASE Ron Feldman, MD, PhD Assistant Professor of Dermatology Emory University ron.j.feldman@emory.edu Disclosures I have no conflict of interest to
B. Autoimmune blistering diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details formation immediately above the basal layer. The dermal papillae, which are covered by basal cells in the single layer that is left in
Go Back to the Top To Order, Visit the Purchasing Page for Details formation immediately above the basal layer. The dermal papillae, which are covered by basal cells in the single layer that is left in
Current concepts of autoimmune bullous diseases Advances in pathogenesis. Luca Borradori
 Current concepts of autoimmune bullous diseases Advances in pathogenesis Luca Borradori Dept. of Dermatology Inselspital, University Hospital of Berne Switzerland Luca.Borradori@insel.ch Autoimmune bullous
Current concepts of autoimmune bullous diseases Advances in pathogenesis Luca Borradori Dept. of Dermatology Inselspital, University Hospital of Berne Switzerland Luca.Borradori@insel.ch Autoimmune bullous
BJD British Journal of Dermatology. Summary REVIEW ARTICLE
 REVIEW ARTICLE BJD British Journal of Dermatology International Bullous Diseases Group: consensus on diagnostic criteria for epidermolysis bullosa acquisita C. Prost-Squarcioni id, 1,2,3 F. Caux, 1 E.
REVIEW ARTICLE BJD British Journal of Dermatology International Bullous Diseases Group: consensus on diagnostic criteria for epidermolysis bullosa acquisita C. Prost-Squarcioni id, 1,2,3 F. Caux, 1 E.
Sarolta Kárpáti. Technology Transfer in Diagnostic Pathology, 5th Central European Regional Meeting May 1, 2010, Siófok
 Blistering diseases Sarolta Kárpáti SEMMELWEIS UNIVERSITY, BUDAPEST Technology Transfer in Diagnostic Pathology, 5th Central European Regional Meeting May 1, 2010, Siófok Blistering diseases Autoimmune
Blistering diseases Sarolta Kárpáti SEMMELWEIS UNIVERSITY, BUDAPEST Technology Transfer in Diagnostic Pathology, 5th Central European Regional Meeting May 1, 2010, Siófok Blistering diseases Autoimmune
BULLOUS SYSTEMIC lupus erythematosus
 OBSERVATION Bullous Systemic Lupus Erythematosus With Autoantibodies Recognizing Multiple Skin Basement Membrane Components, Bullous Pemphigoid Antigen 1, Laminin-5, Laminin-6, and Type VII Collagen Lawrence
OBSERVATION Bullous Systemic Lupus Erythematosus With Autoantibodies Recognizing Multiple Skin Basement Membrane Components, Bullous Pemphigoid Antigen 1, Laminin-5, Laminin-6, and Type VII Collagen Lawrence
Egyptian Dermatology Online Journal Vol. 8 No 2: 6, December Yasmeen J Bhat*, Iffat Hasan*, Atiya Yaseen*, Hina Altaf*, Shylla Mir**
 Pemphigoid gestationis in a multigravida Yasmeen J Bhat*, Iffat Hasan*, Atiya Yaseen*, Hina Altaf*, Shylla Mir** * Department of Dermatology, STD & Leprosy; Government Medical College, Srinagar ** Department
Pemphigoid gestationis in a multigravida Yasmeen J Bhat*, Iffat Hasan*, Atiya Yaseen*, Hina Altaf*, Shylla Mir** * Department of Dermatology, STD & Leprosy; Government Medical College, Srinagar ** Department
OBSERVATION. (EBA) is a chronic subepidermal bullous disease
 OBSERVATION Clinical Response of Severe Mechanobullous Epidermolysis Bullosa Acquisita to Combined Treatment With Immunoadsorption and Rituximab (Anti-CD2 Monoclonal Antibodies) Andrea Niedermeier, MD;
OBSERVATION Clinical Response of Severe Mechanobullous Epidermolysis Bullosa Acquisita to Combined Treatment With Immunoadsorption and Rituximab (Anti-CD2 Monoclonal Antibodies) Andrea Niedermeier, MD;
Guidelines for the management of bullous pemphigoid
 British Journal of Dermatology 2002; 147: 214 221. GUIDELINES Guidelines for the management of bullous pemphigoid F.WOJNAROWSKA, G.KIRTSCHIG, A.S.HIGHET,* V.A.VENNING AND N.P.KHUMALO Department of Dermatology,
British Journal of Dermatology 2002; 147: 214 221. GUIDELINES Guidelines for the management of bullous pemphigoid F.WOJNAROWSKA, G.KIRTSCHIG, A.S.HIGHET,* V.A.VENNING AND N.P.KHUMALO Department of Dermatology,
Pharmacologyonline 1: 1-6 (2010) Case Report Ravishankar and Hiremath CIPROFLOXACIN INDUCED BULLOUS PEMPHIGOID: A CASE REPORT
 CIPROFLOXACIN INDUCED BULLOUS PEMPHIGOID: A CASE REPORT Ravishankar AC 1*, Hiremath SV 1 1 Dept of Pharmacology and Pharmacotherapeutics, JN Medical College, Belgaum, India. Summary Bullous pemphigoid
CIPROFLOXACIN INDUCED BULLOUS PEMPHIGOID: A CASE REPORT Ravishankar AC 1*, Hiremath SV 1 1 Dept of Pharmacology and Pharmacotherapeutics, JN Medical College, Belgaum, India. Summary Bullous pemphigoid
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease:
 Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
atorvastatin 10mg, amlodipine 5mg and dilitazem 60mg. He had unexplained iron deficiency anaemia (hemoglobin-8.4gm/dl, ferritin- 4.73ng/ml, total iron
 Pemphigus herpetiformis : A rare clinical variant of pemphigus Shrestha P 1, Tajhya RB 2, Pokharel A 3 1,2 Consultant Dermatologist, Department of Dermatology, Vayodha Hospital Pvt. Ltd, Balkhu, Kathmandu,
Pemphigus herpetiformis : A rare clinical variant of pemphigus Shrestha P 1, Tajhya RB 2, Pokharel A 3 1,2 Consultant Dermatologist, Department of Dermatology, Vayodha Hospital Pvt. Ltd, Balkhu, Kathmandu,
EPIDERMOLYSIS BULLOSA
 EPIDERMOLYSIS BULLOSA Definition Epidermolysis bullosa (EB) is a term used to describe a group of rare mainly hereditary, chronic, non-inflammatory diseases of skin and mucous membranes. EB is characterized
EPIDERMOLYSIS BULLOSA Definition Epidermolysis bullosa (EB) is a term used to describe a group of rare mainly hereditary, chronic, non-inflammatory diseases of skin and mucous membranes. EB is characterized
Bullous colon lesions in a patient with bullous pemphigoid
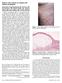 Bullous colon lesions in a patient with bullous pemphigoid Evelyn Maria Sachsenberg-Studer, MD, Ulf Runne, MD, Till Wehrmann, MD, Manfred Wolter, MD, Susanne Kriener, MD, Knut Engels, MD, Thomas Elshorst-
Bullous colon lesions in a patient with bullous pemphigoid Evelyn Maria Sachsenberg-Studer, MD, Ulf Runne, MD, Till Wehrmann, MD, Manfred Wolter, MD, Susanne Kriener, MD, Knut Engels, MD, Thomas Elshorst-
Immunobullous Diseases: Review and Update. May P. Chan, MD Associate Professor of Pathology and Dermatology University of Michigan
 Immunobullous Diseases: Review and Update May P. Chan, MD Associate Professor of Pathology and Dermatology University of Michigan Diagnosis of Immunobullous Diseases Clinical H&E DIF DIAGNOSIS IIF ELISA
Immunobullous Diseases: Review and Update May P. Chan, MD Associate Professor of Pathology and Dermatology University of Michigan Diagnosis of Immunobullous Diseases Clinical H&E DIF DIAGNOSIS IIF ELISA
Importance of serological tests in diagnosis of autoimmune blistering diseases
 doi: 10.1111/1346-8138.12703 Journal of Dermatology 2015; 42: 3 10 REVIEW ARTICLE Importance of serological tests in diagnosis of autoimmune blistering diseases Ken ISHII Department of Dermatology, Toho
doi: 10.1111/1346-8138.12703 Journal of Dermatology 2015; 42: 3 10 REVIEW ARTICLE Importance of serological tests in diagnosis of autoimmune blistering diseases Ken ISHII Department of Dermatology, Toho
Clinicopathological correlation of blistering diseases of skin
 Bangladesh Med Res Counc Bull 2008; 34: 48-53 Copyright 2008 by Bangladesh Medical Research Council Clinicopathological correlation of blistering diseases of skin A.K.M. Nurul Kabir 1, Mohammed Kamal 1
Bangladesh Med Res Counc Bull 2008; 34: 48-53 Copyright 2008 by Bangladesh Medical Research Council Clinicopathological correlation of blistering diseases of skin A.K.M. Nurul Kabir 1, Mohammed Kamal 1
Ann Dermatol Vol. 24, No 1,
 Ann Dermatol Vol. 24, No 1, 2012 http://dx.doi.org/10.5021/ad.2012.24.1.45 ORIGINAL ARTICAL Usefulness of Enzyme-linked Immunosorbent Assay Using Recombinant BP180 and BP230 for Serodiagnosis and Monitoring
Ann Dermatol Vol. 24, No 1, 2012 http://dx.doi.org/10.5021/ad.2012.24.1.45 ORIGINAL ARTICAL Usefulness of Enzyme-linked Immunosorbent Assay Using Recombinant BP180 and BP230 for Serodiagnosis and Monitoring
Original Article ABSTRACT
 Original Article doi: 10.5146/tjpath.2015.01345 Utility of Direct Immunofluorescence Studies in Subclassification of Autoimmune Sub-Epidermal Bullous Diseases: A 2-Year Study in a Tertiary Care Hospital
Original Article doi: 10.5146/tjpath.2015.01345 Utility of Direct Immunofluorescence Studies in Subclassification of Autoimmune Sub-Epidermal Bullous Diseases: A 2-Year Study in a Tertiary Care Hospital
CLINCOPATHOLOGICAL CASE
 CLINCOPATHOLOGICAL CASE Generalized vesiculo-bullous and pustular eruption in an adult man Hassab El-Naby H, MD, El-Khalawany M, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt CLINICAL
CLINCOPATHOLOGICAL CASE Generalized vesiculo-bullous and pustular eruption in an adult man Hassab El-Naby H, MD, El-Khalawany M, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt CLINICAL
Department of Dermatology, Nippon Medical School, 1-1-5, Sendagi, Bunkyo-ku, Tokyo , Japan 2
 Dermatology Research and Practice Volume 2010, Article ID 931340, 5 pages doi:10.1155/2010/931340 Case Report Paraneoplastic Pemphigus Presenting as Mild Cutaneous Features of Pemphigus Foliaceus and Lichenoid
Dermatology Research and Practice Volume 2010, Article ID 931340, 5 pages doi:10.1155/2010/931340 Case Report Paraneoplastic Pemphigus Presenting as Mild Cutaneous Features of Pemphigus Foliaceus and Lichenoid
Mucous membrane pemphigoid in a patient with hypertension treated with atenolol: a case report
 Kanjanabuch et al. Journal of Medical Case Reports 2012, 6:373 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Mucous membrane pemphigoid in a patient with hypertension treated with atenolol: a
Kanjanabuch et al. Journal of Medical Case Reports 2012, 6:373 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Mucous membrane pemphigoid in a patient with hypertension treated with atenolol: a
السكري للداء مرافقة فقاعات diabeticorum= Bullosis
 1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae
 H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
Pemphigus foliaceus: a clinical study of 32 cases in Hong Kong 32
 H.K. Dermatol. Venereol. Bull. (2004) 12, 126-132 Original Article Pemphigus foliaceus: a clinical study of 32 cases in Hong Kong 32 This is a cross-sectional, retrospective study of 32 Hong Kong Chinese
H.K. Dermatol. Venereol. Bull. (2004) 12, 126-132 Original Article Pemphigus foliaceus: a clinical study of 32 cases in Hong Kong 32 This is a cross-sectional, retrospective study of 32 Hong Kong Chinese
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
To Correlate Clinical Diagnosis with Histopathology and DIF Pattern of Autoimmune Based Vesiculobullous Disorders In A Tertiary Teaching Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 7 Ver. 2 (July. 2018), PP 01-06 www.iosrjournals.org To Correlate Clinical Diagnosis with Histopathology
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 7 Ver. 2 (July. 2018), PP 01-06 www.iosrjournals.org To Correlate Clinical Diagnosis with Histopathology
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Autoimmune Blistering Disease
 life. science. discovery. life. science. discovery. Autoimmune Blistering Disease - Diagnostic Methodology for Pemphigus and Pemphigoid - Pemphigus Epidermal cell-cell junction EBA Epidermal side Epidermal
life. science. discovery. life. science. discovery. Autoimmune Blistering Disease - Diagnostic Methodology for Pemphigus and Pemphigoid - Pemphigus Epidermal cell-cell junction EBA Epidermal side Epidermal
Management of Pyoderma Gangrenosum Mentoring in IBD XVII
 Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
and Isolation of Antibody in Linear Immunoglobulin A Bullous Dermatosis
 Identification of the Cutaneous Basement Membrane Zone Antigen and Isolation of Antibody in Linear Immunoglobulin A Bullous Dermatosis John J. Zone, Ted B. Taylor, Donald P. Kadunce, and Laurence J. Meyer
Identification of the Cutaneous Basement Membrane Zone Antigen and Isolation of Antibody in Linear Immunoglobulin A Bullous Dermatosis John J. Zone, Ted B. Taylor, Donald P. Kadunce, and Laurence J. Meyer
Indian Journal of Dermatopathology and Diagnostic Dermatology
 Volume 1 Issue 1 Jan-Jun 2014 Online full text at www.ijdpdd.com Indian Journal of Dermatopathology and Diagnostic Dermatology DSI IADVL Karnataka Branch Official Publication of Dermatopathology Society
Volume 1 Issue 1 Jan-Jun 2014 Online full text at www.ijdpdd.com Indian Journal of Dermatopathology and Diagnostic Dermatology DSI IADVL Karnataka Branch Official Publication of Dermatopathology Society
Glistening, Skin-Colored Nodule
 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
Paul K. Shitabata, M.D. Dermatopathology Institute
 Paul K. Shitabata, M.D. Dermatopathology Institute Technical Considerations Storage of slides at room temperature
Paul K. Shitabata, M.D. Dermatopathology Institute Technical Considerations Storage of slides at room temperature
Citation for published version (APA): Meijer, J. M. (2018). Diagnosis of pemphigoid diseases. [Groningen]: Rijksuniversiteit Groningen.
![Citation for published version (APA): Meijer, J. M. (2018). Diagnosis of pemphigoid diseases. [Groningen]: Rijksuniversiteit Groningen. Citation for published version (APA): Meijer, J. M. (2018). Diagnosis of pemphigoid diseases. [Groningen]: Rijksuniversiteit Groningen.](/thumbs/94/122280961.jpg) University of Groningen Diagnosis of pemphigoid diseases Meijer, Joost Martien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Diagnosis of pemphigoid diseases Meijer, Joost Martien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Studies on clinical symptoms, diagnosis and treatment in pemphigoid diseases Terra, Jorrit
 University of Groningen Studies on clinical symptoms, diagnosis and treatment in pemphigoid diseases Terra, Jorrit IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Studies on clinical symptoms, diagnosis and treatment in pemphigoid diseases Terra, Jorrit IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Case 1. Debridement Cultures Keflex Silvadene
 The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
Novel and recurrent COL7A1 mutations in Chinese patients with dystrophic epidermolysis bullosa pruriginosa
 Case Report Novel and recurrent COL7A1 mutations in Chinese patients with dystrophic epidermolysis bullosa pruriginosa K.J. Zhu*, C.Y. Zhu*, Y. Zhou and Y.M. Fan Department of Dermatology, Affiliated Hospital
Case Report Novel and recurrent COL7A1 mutations in Chinese patients with dystrophic epidermolysis bullosa pruriginosa K.J. Zhu*, C.Y. Zhu*, Y. Zhou and Y.M. Fan Department of Dermatology, Affiliated Hospital
Prognostic factors in pemphigus vulgaris and pemphigus foliaceus M. Saha, 1 B. Bhogal, 1 M.M. Black, 1 D. Cooper, 2 R.W. Vaughan 3 and R.W.
 CLINICAL AND LABORATORY INVESTIGATIONS BJD British Journal of Dermatology Prognostic factors in pemphigus vulgaris and pemphigus foliaceus M. Saha, 1 B. Bhogal, 1 M.M. Black, 1 D. Cooper, 2 R.W. Vaughan
CLINICAL AND LABORATORY INVESTIGATIONS BJD British Journal of Dermatology Prognostic factors in pemphigus vulgaris and pemphigus foliaceus M. Saha, 1 B. Bhogal, 1 M.M. Black, 1 D. Cooper, 2 R.W. Vaughan
Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis
 Accepted Manuscript Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis Maglie Roberto, MD, Antiga Emiliano, MD, PhD, Caproni Marzia, MD, PhD PII: S0190-9622(17)32812-8
Accepted Manuscript Comment on Association of bullous pemphigoid with malignancy: A systematic review and meta-analysis Maglie Roberto, MD, Antiga Emiliano, MD, PhD, Caproni Marzia, MD, PhD PII: S0190-9622(17)32812-8
Immunofluorescence in Oral Dermatological Disorders- No Shiny Matter
 Journal of Academy of Dental Education Journal of Academy of Dental Education, 24-28, DOI: 10.18311/jade/2015-2016/15951 ISSN (Print): 2348-1595 ISSN (Online) : 2348-2621 Immunofluorescence in Oral Dermatological
Journal of Academy of Dental Education Journal of Academy of Dental Education, 24-28, DOI: 10.18311/jade/2015-2016/15951 ISSN (Print): 2348-1595 ISSN (Online) : 2348-2621 Immunofluorescence in Oral Dermatological
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
Bullous pemphigoid (BP) is the most common autoimmune. ActaDV ActaDV
 6 CLINICAL REPORT Diagnostic Value of Linear Fluorescence Along the Basement Membrane of Sweat Gland Ducts in Bullous Pemphigoid Işın SINEM BAĞCI,, Orsolya N. HORVÁTH, Enno SCHMIDT,, Thomas RUZICKA and
6 CLINICAL REPORT Diagnostic Value of Linear Fluorescence Along the Basement Membrane of Sweat Gland Ducts in Bullous Pemphigoid Işın SINEM BAĞCI,, Orsolya N. HORVÁTH, Enno SCHMIDT,, Thomas RUZICKA and
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Drug Class Prior Authorization Criteria Immune Globulins
 Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Autoimmune bullous disorders 1)
 Clin Chem Lab Med 2006;44(2):144 149 2006 by Walter de Gruyter Berlin New York. DOI 10.1515/CCLM.2006.027 2006/39 Review Autoimmune bullous disorders 1) Rüdiger Eming* and Michael Hertl for the members
Clin Chem Lab Med 2006;44(2):144 149 2006 by Walter de Gruyter Berlin New York. DOI 10.1515/CCLM.2006.027 2006/39 Review Autoimmune bullous disorders 1) Rüdiger Eming* and Michael Hertl for the members
Mucous membrane pemphigoid presenting as bleeding gums and burning sensation of mouth: a case report
 Archives of Orofacial Sciences www.dental.usm.my/aos/ Penerbit Universiti Sains Malaysia. 2018 print ISSN: 1823-8602 e-issn: 2231-7163 Case Report Arch Orofac Sci (2018), 13(1): 45-49. Mucous membrane
Archives of Orofacial Sciences www.dental.usm.my/aos/ Penerbit Universiti Sains Malaysia. 2018 print ISSN: 1823-8602 e-issn: 2231-7163 Case Report Arch Orofac Sci (2018), 13(1): 45-49. Mucous membrane
STUDY. the most frequent autoimmune blistering skin disease. 1,2 It is most common in
 STUDY Prediction of Survival for Patients With Bullous Pemphigoid A Prospective Study Pascal Joly, MD, PhD; Jacques Benichou, MD, PhD; Catherine Lok, MD, PhD; Marie France Hellot, ScD; Philippe Saiag,
STUDY Prediction of Survival for Patients With Bullous Pemphigoid A Prospective Study Pascal Joly, MD, PhD; Jacques Benichou, MD, PhD; Catherine Lok, MD, PhD; Marie France Hellot, ScD; Philippe Saiag,
University of Groningen. Acantholysis in pemphigus van der Wier, Gerda
 University of Groningen Acantholysis in pemphigus van der Wier, Gerda IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Acantholysis in pemphigus van der Wier, Gerda IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
The incidence of internal malignancies in autoimmune bullous diseases
 Tokai J Exp Clin Med., Vol. 32, No. 1, pp. 42-47, 2007 The incidence of internal malignancies in autoimmune bullous diseases Kenichi IWASHITA, Takashi MATSUYAMA, Emiko AKASAKA, Kimihiko MIZUTANI, Kozo
Tokai J Exp Clin Med., Vol. 32, No. 1, pp. 42-47, 2007 The incidence of internal malignancies in autoimmune bullous diseases Kenichi IWASHITA, Takashi MATSUYAMA, Emiko AKASAKA, Kimihiko MIZUTANI, Kozo
Discovering potential drug-targets for personalized treatment of autoimmune disorders - what we learn from epidermolysis bullosa acquisita
 Expert Opinion on Therapeutic Targets ISSN: 1472-8222 (Print) 1744-7631 (Online) Journal homepage: http://www.tandfonline.com/loi/iett20 Discovering potential drug-targets for personalized treatment of
Expert Opinion on Therapeutic Targets ISSN: 1472-8222 (Print) 1744-7631 (Online) Journal homepage: http://www.tandfonline.com/loi/iett20 Discovering potential drug-targets for personalized treatment of
Persistence of Autoreactive IgA-Secreting B Cells Despite Multiple Immunosuppressive Medications Including Rituximab
 Research Case Report/Case Series Persistence of Autoreactive IgA-Secreting B Cells Despite Multiple Immunosuppressive Medications Including Rituximab Yong He, MD; Michiko Shimoda, PhD; Yoko Ono, MD; Itzel
Research Case Report/Case Series Persistence of Autoreactive IgA-Secreting B Cells Despite Multiple Immunosuppressive Medications Including Rituximab Yong He, MD; Michiko Shimoda, PhD; Yoko Ono, MD; Itzel
Vesiculobullous Diseases
 Vesiculobullous Diseases Larkin Community Hospital/NSU-COM Presenters: Yuri Kim, DO, Sam Ecker, DO, Jennifer David, DO, MBA Program Director: Stanley Skopit, DO, MSE, FAOCD, FAAD We have no relevant disclosures
Vesiculobullous Diseases Larkin Community Hospital/NSU-COM Presenters: Yuri Kim, DO, Sam Ecker, DO, Jennifer David, DO, MBA Program Director: Stanley Skopit, DO, MSE, FAOCD, FAAD We have no relevant disclosures
STUDY. A Comparison of Oral Methylprednisolone Plus Azathioprine or Mycophenolate Mofetil for the Treatment of Bullous Pemphigoid
 STUDY A Comparison of Oral Methylprednisolone Plus Azathioprine or Mycophenolate Mofetil for the Treatment of Bullous Pemphigoid Stefan Beissert, MD; Thomas Werfel, MD; Uta Frieling, MD; Markus Böhm, MD;
STUDY A Comparison of Oral Methylprednisolone Plus Azathioprine or Mycophenolate Mofetil for the Treatment of Bullous Pemphigoid Stefan Beissert, MD; Thomas Werfel, MD; Uta Frieling, MD; Markus Böhm, MD;
Reliability and validity of the Chinese version of the autoimmune bullous disease quality of life (ABQOL) questionnaire
 Yang et al. Health and Quality of Life Outcomes (2017) 15:31 DOI 10.1186/s12955-017-0594-z RESEARCH Open Access Reliability and validity of the Chinese version of the autoimmune bullous disease quality
Yang et al. Health and Quality of Life Outcomes (2017) 15:31 DOI 10.1186/s12955-017-0594-z RESEARCH Open Access Reliability and validity of the Chinese version of the autoimmune bullous disease quality
A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients
 Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Diagnostic performance of the MESACUP anti-skin profile TEST
 Investigative report Eur J Dermatol 216; 26(1): 56-63 Orsolya N. HORVÁTH 1,2 Rita VARGA 1 Makoto KANEDA 3 Enno SCHMIDT 4 Thomas RUZICKA 1 Miklós SÁRDY 1 1 Department of Dermatology, Allergology, Ludwig
Investigative report Eur J Dermatol 216; 26(1): 56-63 Orsolya N. HORVÁTH 1,2 Rita VARGA 1 Makoto KANEDA 3 Enno SCHMIDT 4 Thomas RUZICKA 1 Miklós SÁRDY 1 1 Department of Dermatology, Allergology, Ludwig
Understanding Myositis Medications
 Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Epitope Spreading: Lessons From Autoimmune Skin Diseases
 Epitope Spreading: Lessons From Autoimmune Skin Diseases REVIEW Lawrence S. Chan,* Carol J. Vanderlugt, Takashi Hashimoto, Takeji Nishikawa, John J. Zone,** Martin M. Black, Fenella Wojnarowska, Seth R.
Epitope Spreading: Lessons From Autoimmune Skin Diseases REVIEW Lawrence S. Chan,* Carol J. Vanderlugt, Takashi Hashimoto, Takeji Nishikawa, John J. Zone,** Martin M. Black, Fenella Wojnarowska, Seth R.
Case Report Ocular Involvement and Blindness Secondary to Linear IgA Dermatosis
 Ophthalmology Volume 2010, Article ID 280396, 4 pages doi:10.1155/2010/280396 Case Report Ocular Involvement and Blindness Secondary to Linear IgA Dermatosis Cinthya Ramos-Castellón, 1 Gabriela Ortiz-Nieva,
Ophthalmology Volume 2010, Article ID 280396, 4 pages doi:10.1155/2010/280396 Case Report Ocular Involvement and Blindness Secondary to Linear IgA Dermatosis Cinthya Ramos-Castellón, 1 Gabriela Ortiz-Nieva,
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adhesion and migration, the diverse functions of the laminin a3 subunit, 79 87 Alopecia in epidermolysis bullosa, 165 169 Amblyopia and inherited
Note: Page numbers of article titles are in boldface type. A Adhesion and migration, the diverse functions of the laminin a3 subunit, 79 87 Alopecia in epidermolysis bullosa, 165 169 Amblyopia and inherited
pemphigoid. a clinical and immunopathological study
 British Journal of Ophthalmology, 1989, 73, 52-56 Conjunctival involvement in cicatricial and bullous pemphigoid. a clinical and immunopathological study PEGGY A FRITH,' AND A J BRON' V A VENNING,2 F WOJNAROWSKA,2
British Journal of Ophthalmology, 1989, 73, 52-56 Conjunctival involvement in cicatricial and bullous pemphigoid. a clinical and immunopathological study PEGGY A FRITH,' AND A J BRON' V A VENNING,2 F WOJNAROWSKA,2
Serologic Markers CONVENTIONAL ANTIBODIES ANTIBODIES UNCONVENTIONAL. AIH Type I
 Autoimmune Hepatitis By Thomas Frazier Objective What we need to know about AIH Diagnosis Treatment Difficulties in both Liver transplantation concerns AASLD Guidelines: Hepatology. 2010 Jun;51(6):2193-213.
Autoimmune Hepatitis By Thomas Frazier Objective What we need to know about AIH Diagnosis Treatment Difficulties in both Liver transplantation concerns AASLD Guidelines: Hepatology. 2010 Jun;51(6):2193-213.
When your patient complains of
 WILLIAM LAWSON, MD, DDS Mount Sinai School of Medicine ABSTRACT: Certain clues can help you identify the cause of bullous oral lesions. Diffuse oral and labial bullous erosions, sometimes accompanied by
WILLIAM LAWSON, MD, DDS Mount Sinai School of Medicine ABSTRACT: Certain clues can help you identify the cause of bullous oral lesions. Diffuse oral and labial bullous erosions, sometimes accompanied by
Definitive and Differential Diagnosis of Desquamative Gingivitis Through Direct Immunofluorescence Studies
 Volume 83 Number 10 Definitive and Differential Diagnosis of Desquamative Gingivitis Through Direct Immunofluorescence Studies Lakshmanan Suresh* and Mirdza E. Neiders* Background: Desquamative gingivitis
Volume 83 Number 10 Definitive and Differential Diagnosis of Desquamative Gingivitis Through Direct Immunofluorescence Studies Lakshmanan Suresh* and Mirdza E. Neiders* Background: Desquamative gingivitis
Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States
 Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States Sergey Rekhtman MD, PharmD, MPH Amit Garg, MD Department of Dermatology Zucker
Risk of Pneumocystosis among Patients Receiving Immunosuppressive Therapies: a population based analysis in the United States Sergey Rekhtman MD, PharmD, MPH Amit Garg, MD Department of Dermatology Zucker
Immunofluorescence in Oral Pathology Part III: Pathology and Immunofluorescent Patterns in Intraepithelial Immunobullous Disorders
 10.5005/jp-journals-10015-1157 Roopa S Rao et al REVIEW ARTICLE Immunofluorescence in Oral Pathology Part III: Pathology and Immunofluorescent Patterns in Intraepithelial Immunobullous Disorders Roopa
10.5005/jp-journals-10015-1157 Roopa S Rao et al REVIEW ARTICLE Immunofluorescence in Oral Pathology Part III: Pathology and Immunofluorescent Patterns in Intraepithelial Immunobullous Disorders Roopa
Recent Advances in the Molecular Pathology of Bullous Skin Disorders
 1 Bahrain Medical Bulletin, Vol. 27, No. 2, June 2005 Recent Advances in the Molecular Pathology of Bullous Skin Disorders John A McGrath* Maintenance of an intact epidermis depends on secure adhesion
1 Bahrain Medical Bulletin, Vol. 27, No. 2, June 2005 Recent Advances in the Molecular Pathology of Bullous Skin Disorders John A McGrath* Maintenance of an intact epidermis depends on secure adhesion
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
10/25/2018. Autoimmunity and how to treat it. Disclosure. Why do we get autoimmunity? James Verbsky MD/PhD Pediatric Rheumatology/Immunology
 Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Review Article Clinical Relevance of Autoantibodies in Patients with Autoimmune Bullous Dermatosis
 Clinical and Developmental Immunology Volume 2012, Article ID 369546, 9 pages doi:10.1155/2012/369546 Review Article Clinical Relevance of Autoantibodies in Patients with Autoimmune Bullous Dermatosis
Clinical and Developmental Immunology Volume 2012, Article ID 369546, 9 pages doi:10.1155/2012/369546 Review Article Clinical Relevance of Autoantibodies in Patients with Autoimmune Bullous Dermatosis
