Insulin sensitivity, and b-cell function in relation to hemoglobin A1C
|
|
|
- Dustin Blake
- 5 years ago
- Views:
Transcription
1 Nutrition, Metabolism & Cardiovascular Diseases (2014) 24, 27e33 Available online at journal homepage: Insulin sensitivity, and b-cell function in relation to hemoglobin A1C M.A. Marini a, S. Frontoni a, E. Succurro b, F. Arturi b, A. Sciacqua b, M.L. Hribal b, F. Perticone b, G. Sesti b, * a Department of Systems Medicine, University of Rome-Tor Vergata, Italy b Department of Medical and Surgical Sciences, University Magna Graecia of Catanzaro, Italy Received 17 November 2012; received in revised form 31 December 2012; accepted 25 January 2013 Available online 16 April 2013 KEYWORDS A1C; Insulin sensitivity; Insulin secretion Abstract Background and aims: The A1C diagnostic criterion for identifying individuals at increased risk for diabetes, introduced by the American Diabetes Association in 2010, was not defined on the basis of the principal pathophysiological abnormalities responsible for the development and progression of type 2 diabetes; we therefore wished to gain a deeper insight into the metabolic abnormalities characterizing the group of at risk individuals with an A1C value of 5.7e6.4%. Methods and results: As many as 338 non-diabetic offspring of type 2 diabetic patients were consecutively recruited. Insulin secretion was assessed using both indexes derived from oral glucose tolerance test (OGTT), and intravenous glucose tolerance test (IVGTT). Insulin sensitivity was measured by hyperinsulinemic euglycemic clamp. As compared with subjects with A1C <5.7%, individuals with A1C of 5.7e6.4% exhibited lower insulin sensitivity after adjusting for age, gender and body mass index (BMI). Insulin secretion estimated from the OGTT, did not differ between the two groups. By contrast, as compared with subjects with A1C <5.7%, the acute insulin response (AIR) during an IVGTT and both IVGTT-derived and OGTT-derived disposition indexes were reduced in individuals with A1C of 5.7e6.4% after adjusting for age, gender and BMI. As A1C increased to 5.7%, a sharp decrease in insulin sensitivity and b-cell function, measured as disposition index, was observed. Conclusions: Caucasian individuals with A1C 5.7% exhibit both core pathophysiological defects of type 2 diabetes i.e. insulin resistance and b-cell dysfunction. ª 2013 Elsevier B.V. All rights reserved. Abbreviations: AIR, acute insulin response; ADA, American Diabetes Association; AUC, area under the curve; BMI, body mass index; EASD, European Association for the Study of Diabetes; FPG, fasting plasma glucose; A1C, hemoglobin A1C; HOMA, homeostasis model assessment; IFG, impaired fasting glucose; IGT, impaired glucose tolerance; IDF, International Diabetes Federation; IVGTT, intravenous glucose tolerance test; M FFM, milligrams per minute per kilogram fat-free mass; OGTT, oral glucose tolerance test; PG, plasma glucose. * Corresponding author. Dipartimento di Scienze Mediche e Chirurgiche, Viale Europa, Catanzaro, Italy. Tel.: þ ; fax: þ address: sesti@unicz.it (G. Sesti) /$ - see front matter ª 2013 Elsevier B.V. All rights reserved.
2 28 M.A. Marini et al. Introduction Hemoglobin A1C (A1C) is an integrated measure of mean glycemia over the preceding 8e12 weeks, and is largely employed for monitoring metabolic control in subjects with diabetes [1]. In 2009, an International Expert Committee including representatives of the International Diabetes Federation (IDF), the American Diabetes Association (ADA), and the European Association for the Study of Diabetes (EASD) recommended the adoption of the A1C test for the diagnosis of diabetes with a cut-off of 6.5% in addition to the criteria based on either fasting plasma glucose (FPG) 126 mg/dl or 2-h 75-g oral glucose tolerance test (OGTT) plasma glucose (2-h PG) value 200 mg/dl [2]. This cut-off was mainly derived from an appraisal of epidemiological studies evaluating the association between A1C values and risk of retinopathy, a micro-vascular complication strongly related to chronic hyperglycemia [2]. In 2010, the ADA adopted this criterion for the diagnosis of diabetes, and revised the criteria for the diagnosis of increased risk for diabetes (pre-diabetes) with the inclusion, in addition to the preexisting groups of subjects with impaired fasting glucose (IFG) and/or impaired glucose tolerance (IGT), of the group of individuals with an A1C value ranging from 5.7% to 6.4% [3]. This cut-off was mainly derived from analyzes of prospective studies evaluating the association between A1C values and the future risk of type 2 diabetes [4]. However, the A1C diagnostic criterion for identifying individuals at increased risk for diabetes was not defined on the basis of the principal pathophysiological abnormalities responsible for the development and progression of type 2 diabetes, i.e. impaired tissue sensitivity to insulin and failure of pancreatic b-cells to compensate for the enhanced insulin demand. To gain a deeper insight into the metabolic abnormalities characterizing at risk individuals with an A1C value of 5.7e6.4%, we employed the hyperinsulinemiceeuglycemic clamp technique to evaluate insulin sensitivity as well as both OGTT and intravenous glucose tolerance test (IVGTT) to achieve a detailed analysis of b-cell function in a cohort of non-diabetic offspring of type 2 diabetic subjects. Methods The study group included 338 non-diabetic offspring consecutively recruited at the Department of Systems Medicine of the University of Rome-Tor Vergata and at the Department of Medical and Surgical Sciences of the University of Catanzaro-Magna Graecia [5]. All individuals were Caucasian and had one parent with type 2 diabetes and the other with no history of type 2 diabetes and a normal response to an OGTT. No subject was taking any medication know to affect glucose metabolism. After 12-h fasting, all individuals underwent anthropometrical evaluation including body composition evaluated by bioelectrical impedance, and a 75 g OGTT was performed with 0, 30, 60, 90 and 120 min sampling for plasma glucose and insulin. All non-diabetic individuals (FPG <126 mg/dl, 2 h post-load <200 mg/dl and A1C <6.5%) were characterized according to a previously validated protocol [5,6]. Briefly, after 12-h fasting, the subjects underwent an IVGTT and a hyperinsulinemic euglycemic clamp. After baseline blood collection, a bolus of glucose (300 mg/kg in a 50% solution) was given (within 30 s) into the antecubital vein to acutely increase blood glucose levels. Samples for the measurement of blood glucose and plasma insulin were drawn at 2, 4, 6, 8, 10, 20, 30, 40, 50, and 60 min. At 60 min after the glucose bolus, a continuous insulin infusion was initiated at the rate of 40 mu/m 2 of body surface area per min, after a priming dose, in order to reach and maintain a steady state plasma insulin of 85 9 mu/ml. Plasma glucose was assessed at 5 min intervals during the 2-h clamp study by a glucose analyzer. In the study subjects, mean plasma glucose concentration during the last hour of the clamp was 92 4 mg/dl. The study was approved by Institutional Ethics Committees and informed consent was obtained from each subject in accordance with principles of the Declaration of Helsinki. Analytical determinations A1C was measured with high performance liquid chromatography using a National Glycohemoglobin Standardization Program (NGSP) certified automated analyzer (Adams HA HbA1C analyzer, Menarini, Italy) (normal range 4.3e5.9%). Plasma insulin concentration was determined by a chemiluminescence-based assay (Immulite Ò, Siemens, Italy). Glucose, triglyceride, total and HDL-C concentrations were determined by enzymatic methods (Roche, Basel, Switzerland). Calculation Glucose disposal (M) was calculated as the mean rate of glucose infusion measured during the last 60 min of the clamp examination (steady-state) and is expressed as milligrams per minute per kilogram fat-free mass (M FFM ) measured with the use of electrical bioimpedance. Acute insulin response (AIR) during the IVGTT was calculated as the incremental area under the curve (AUC) for insulin during the first 10 min of the IVGTT using the trapezoidal rule. Two indexes of insulin secretion were calculated from the OGTT data: the incremental area under the curve of insulin (DIns[AUC]) was divided by the incremental area under the curve of glucose (DGluc[AUC]) during the 0- to 30-min of the OGTT as a measure of early insulin secretion, or by the DGluc[AUC] during the 0- to 120-min of the OGTT as a measure of total insulin secretion [7,8]. To evaluate b-cell function, two so-called disposition indexes were calculated as follows: AIR M FFM (IVGTT-derived disposition index) or DIns(AUC 0e120)/DGluc(AUC 0e120) M FFM (OGTT-derived disposition index) [9]. Statistical analysis Continuous variables are expressed as means SD. Categorical variables were compared by c 2 test. Metabolic differences among groups were tested after adjusting for gender, age, and BMI using a general linear model with post hoc Bonferroni correction for multiple comparisons. A P value <0.05 was considered nominally significant. All
3 A1C, insulin sensitivity, and b-cell function 29 analyzes were performed using SPSS software Version 16.0 for Windows. Results A total 77 of 338 (22.8%) subjects were at increased risk for diabetes according to ADA criteria (A1C 5.7e6.4%). Table 1 shows the metabolic characteristics of the two study groups i.e. subjects with A1C <5.7%. vs. subjects with A1C of 5.7e6.4%. Significant differences between the two groups were observed with respect to age (subjects with A1C of 5.7e6.4% were older than subjects with A1C <5.7%), and BMI (subjects with A1C of 5.7e6.4% were heavier than subjects with A1C <5.7%). A tendency toward a higher prevalence of men in the group with A1C of 5.7e6.4% was also observed. Therefore, all analyzes were adjusted for age, gender, and BMI. As expected, individuals at increased risk for diabetes (A1C 5.7e6.4%) had significantly higher A1C, FPG, and 2-h post-load plasma glucose and triglycerides levels as compared with subjects with A1C <5.7% (Table 1). A significant reduction in peripheral insulin sensitivity, evaluated by the hyperinsulinemic euglycemic clamp, was observed in individuals with A1C of 5.7e6.4% as compared with subjects with A1C <5.7% (P < after adjusting for age, gender, and BMI). Total insulin secretion during the 120-min OGTT, measured as DIns(AUC)/DGluc(AUC), and early insulin secretion, estimated as DIns AUC 0e30/DGluc AUC 0e30 did not differ between the two groups of individuals. By contrast, as compared with subjects with A1C <5.7%, the AIR during an IVGTT, a direct measure of insulin secretion from b-cells, was nominally reduced in individuals with A1C of 5.7e6.4% (P < 0.02 after adjusting for age, gender, and BMI). Since insulin secretion is dependent on actual insulin sensitivity, we compared the disposition indexes, derived either from the IVGTT or from the OGTT data in the two groups of subjects. Both disposition indexes were significantly lower in individuals with A1C of 5.7e6.4% as compared with subjects with A1C <5.7% (Table 1). After further adjustment for BMI in addition to age, and gender, both the IVGTT-derived and the OGTT-derived disposition indexes were significantly reduced in individuals with A1C of 5.7e6.4% (P < , and P Z 0.004, respectively). Stratification according to gender did not change results. Thus, men with A1C of 5.7e6.4% had lower insulinstimulated glucose disposal ( mg/min Kg FFM) as compared with men with A1C <5.7% ( mg/ min Kg FFM; P < after adjusting for age) as well as reduced IVGTT-derived disposition index ( vs for men with A1C <5.7% and 5.7e6.4%, respectively; P Z after adjusting for age). Accordingly, women with A1C of 5.7e6.4% had lower insulinstimulated glucose disposal ( mg/min Kg FFM) as compared with women with A1C <5.7% ( mg/ min Kg FFM; P < after adjusting for age) as well as reduced IVGTT-derived disposition index ( vs for women with A1C <5.7% and 5.7e6.4%, respectively; P Z after adjusting for age). Next, we stratified subjects with A1C <5.7% and those with A1C of 5.7e6.4% into two groups based on glucose tolerance during the OGTT: i) Normal glucose tolerant Table 1 Anthropometric and metabolic characteristics of the study subjects stratified according to A1C value. Variables Subjects with A1C <5.7% Subjects with A1C 5.7e6.4% P n (Male/Female) 261 (91/170) 77 (35/42) 0.09 Age (yr) <0.0001* BMI (kg/m 2 ) <0.0001** A1C (%) < Fasting glucose (mg/dl ) < h glucose (mg/dl) < Total cholesterol (mg/dl) HDL (mg/dl) Triglycerides (mg/dl) SBP (mmhg) DBP (mmhg) DInsAUC 0e30/DGluAUC 0e DInsAUC 0e120/DGluAUC 0e AIR (mu/ml min) Insulin-stimulated glucose disposal < (mg/min Kg FFM) Disposition index (AIR M FFM ) < Disposition index (DIns[AUC 0e120]/DGluc[AUC 0e120] M FFM ) IFG and/or IGT (%) 48 (18.4%) 41 (53.2%) < Data are means SD. Comparisons between the two groups were performed using a general linear model. P values refer to results after analyzes with adjustment for age, gender, and BMI. *P values refer to results after analyzes with adjustment for gender. **P values refer to results after analyzes with adjustment for age and gender. Categorical variables were compared by c 2 test. IFG Z Impaired fasting glucose; IGT Z Impaired glucose tolerance; AIR Z acute insulin response during IVGTT; SBP Z systolic blood pressure; DBP Z diastolic blood pressure.
4 30 M.A. Marini et al. (NGT) having fasting plasma glucose (FPG) < 100 mg/dl and 2-h plasma glucose <140 mg/dl; and ii) IFG and/or IGT having FPG Z 100e125 mg/dl or 2 h plasma glucose Z 140e199 mg/dl, and compared the metabolic characteristics of the four groups of individuals (Table 2). In the group of subjects having A1C <5.7%, IFG/IGT individuals exhibited significantly lower insulin-stimulated glucose disposal and IVGTT-derived disposition index as compared with NGT subjects. These differences remained significant after adjusting for age, gender, and BMI using a general linear model with post hoc Bonferroni correction for multiple comparisons. Accordingly, NGT subjects with A1C of 5.7e6.4% exhibited significantly lower insulin-stimulated glucose disposal and IVGTT-derived disposition index as compared with NGT subjects with A1C <5.7% even after adjusting for age, gender, and BMI. Then, all subjects were divided into categories based on 0.1% differences in A1C levels, and insulin sensitivity, OGTT-derived insulin secretion indexes, AIR, and disposition indexes were related to A1C values. Whole-body insulin sensitivity, measured with the hyperinsulinemic euglycemic clamp, remained unchanged up to an A1C value of 5.6%. However, as A1C increased to a value 5.7%, a sharp decrease in insulin sensitivity was observed (Fig. 1A). Insulin secretion during an OGTT, as measured by DIns(AUC 0e120)/DGluc(AUC 0e120) (Fig. 1B) and DInsAUC 0e30/DGluAUC 0e30 (Supplementary Fig. 1) indexes, did not change significantly up to A1C >6%. First phase insulin secretion measured as AIR during an IVGTT was nominally reduced as A1C increased to a value 5.9% (Supplementary Fig. 3). By contrast, the IVGTT-derived disposition index remained unchanged up to an A1C value of 5.6%, but it decreased as A1C increased to a value 5.7% (Fig. 1C). Discussion ADA has recently revised criteria for the diagnosis of type 2 diabetes and the categories at increased risk for diabetes, already including IFG and IGT, recommending the use of A1C assay as another diagnostic test option in addition to FPG or 2-h PG glucose values. The ADA criteria identify as individuals with high risk for future diabetes those with A1C ranging from 5.7 to 6.4% [3]. In the present study, we provide evidence that Caucasian individuals with A1C of 5.7e6.4% already exhibit abnormalities of the two main pathophysiological defects responsible for the development of type 2 diabetes, i.e. insulin resistance and b-cell dysfunction. We found that, as compared with subjects with A1C <5.7%, individuals with A1C of 5.7e6.4% exhibited a significant decrease ( 31%) in insulin sensitivity evaluated by Table 2 Anthropometric and metabolic characteristics of the study subjects stratified according to A1C value and glucose tolerance (NGT, IFG and/or IGT). Variables A1C <5.7% A1C 5.7e6.4% P NGT IFG and/or IGT NGT IFG and/or IGT n (%) 213 (63.0) 48 (14.2) 36 (10.7) 41 (12.1) Male/Female 65/148 26/22 14/22 21/ Age (yr) 34 10zzz*xxx xx <0.0001# BMI (kg/m 2 ) **xxx < A1C (%) ***xxx ***xxx < Fasting glucose (mg/dl) 85 8zzzxxx 98 11***xx 89 7xxx < h glucose (mg/dl) zzzxxx ***xxx xxx < Total cholesterol (mg/dl) HDL (mg/dl) 54 14* Triglycerides (mg/dl) x SBP (mmhg) *x DBP (mmhg) DInsAUC 0e30/DGluAUC 0e DInsAUC 0e120/DGluAUC 0e AIR (mu/ml min) Insulin-stimulated glucose disposal (mg/min Kg FFM) z**xxx xx < Disposition index (AIR M FFM ) z**xxx x < Disposition index (DIns[AUC 0e120]/DGluc[AUC 0e120] M FFM ) xxx x x Data are means SD. Comparisons between the four groups were performed using a general linear model with post hoc Bonferroni correction for multiple comparisons. P values refer to results after analyzes with adjustment for age, gender, and BMI. #P values refer to results after analyzes with adjustment for gender. Categorical variables were compared by c 2 test. NGT Z normal glucose tolerance; IFG Z Impaired fasting glucose; IGT Z Impaired glucose tolerance; AIR Z acute insulin response during IVGTT; BMI Z body mass index; SBP Z systolic blood pressure; DBP Z diastolic blood pressure. zp < 0.05; zzp < 0.01; zzzp < compared with subjects with A1C <5.7% and IFG/IGT after adjustment for age, and gender. *P < 0.05; **P < 0.01; ***P < compared with subjects with A1C 5.7e6.4% and NGT after adjustment for age, and gender. xp < 0.05; xxp < 0.01; xxxp < compared with subjects with A1C 5.7e6.4% and and IFG/IGT after adjustment for age, and gender.
5 A1C, insulin sensitivity, and b-cell function 31 Figure 1 Relationship between A1C and insulin-stimulated glucose disposal (A), DIns(AUC 0e120)/DGluc(AUC 0e120) (B), and OGTT-derived disposition index (C). Number of subjects according to A1C categories: A1C of 4.9 Z 44; A1C of 5 Z 24; A1C of 5.1 Z 31, A1C of 5.2 Z 30; A1C of 5.3 Z 33; A1C of 5.4 Z 25; A1C of 5.5 Z 41; A1C of 5.6 Z 33; A1C of 5.7 Z 24; A1C of 5.8 Z 10; A1C of 5.9 Z 15; and A1C of 6.0 Z 23. NS Z Not significant. the hyperinsulinemic euglycemic clamp, and a nominally significant reduction ( 13%) in first-phase insulin secretion assessed by IVGTT. Since the b-cell response to an increment in glucose levels is modulated by the severity of underlying insulin resistance, accounting for differences in insulin sensitivity is a critical point when evaluating b-cell function. Thus, adjusting insulin secretion, assessed by OGTT or IVGTT, for the degree of insulin sensitivity using the disposition index may be a better measure of b-cell function [9]. Using this approach, we observed that individuals with A1C of 5.7e6.4% exhibited a significantly reduction of both IVGTT-derived ( 38%) and OGTT-derived ( 22%) disposition indexes as compared with subjects with A1C <5.7% after adjusting for age, gender, and BMI indicating the presence of b-cell dysfunction. Although measurements of FPG, 2-h post-load glucose, and A1C are likely to reflect diverse pathophysiological feature of glucose metabolism, we observed that both individuals with IFG/IGT and A1C <5.7% and individuals with NGT and A1C value of 5.7e6.4% exhibited impairment in insulin sensitivity and b-cell function assessed by the disposition indexes. This observation suggests that IFG/IGT, and A1C-based diagnosis of pre-diabetes may capture at risk individuals with common underlying abnormalities in glucose metabolism. Interestingly, insulin sensitivity and b-cell function remained unchanged with the increase in A1C up to a value of 5.6%; thereafter, both insulin sensitivity and b-cell function steeply decreased with increasing A1C levels 5.7%. Consistent with the present data, a recent report including subjects of Mexican American descent who were part of the San Antonio Veterans Administration Genetic Epidemiology Study [10] has shown that insulin sensitivity (measured with an OGTT-derived index) remained unchanged up to a value of 5.5%, then decreasing, as A1C levels increased to 5.5%. However, b-cell function, measured with an OGTT-derived insulin secretion/insulin resistance disposition index, did not change significantly up to an A1C value of 5.7%, thereafter decreasing, as A1C levels increased to >5.7%. It is possible that the different A1C cut-point identifying subjects with reduced insulin sensitivity between the two studies may be due to differences in age or ethnicity since the Mexican Americans were older and had higher risk for type 2 diabetes as compared with the Caucasians participating to the present study. A recent systematic review of prospective studies that have examined the relationship of A1C to future diabetes incidence has reported that individuals with an A1C between 5.5 and 6.0% have an increased risk of diabetes with 5-year incidences ranging from 9 to 25% [4]. In consideration of the
6 32 M.A. Marini et al. expected increased use of A1C as a screening test to identify individuals with type 2 diabetes and pre-diabetic conditions [11,12], the findings of the present study showing that individuals with A1C of 5.7e6.4% already display abnormalities of insulin sensitivity and b-cell function may be clinically relevant in order to identify high-risk subjects who will benefit from lifestyle interventions [13e16] or even pharmaceutical treatment [16e20]. The current study has several strengths including the use of the gold standard hyperinsulinemic euglycemic clamp for assessment of insulin sensitivity, the measurement of insulin secretion by both OGTT and IVGTT, the collection of data by trained staff, following a standardized protocol [5], the use of a rigorously standardized A1C measurement, the exclusion of individuals with conditions that affect red cell turnover, such as anemia and major blood loss, the strict quality control of data collection and centralized laboratory analyzes. Nevertheless, the present study has some potential limitations. A first limitation is the availability of only single measures of each test including A1C, OGTT, IVGTT, euglycemic clamp study. A second limitation is the cross-sectional design, making causal interpretations of associations between underlying pathophysiological defects, i.e. insulin resistance and b-cell dysfunction and risk of type 2 diabetes difficult. Furthermore, the observed differences in insulin sensitivity and b- cell function may be, in part, due to differences in age and BMI between the groups with different A1C levels; however, all measures of insulin action and b-cell function were adjusted for these variables. Moreover, it can also be argued that the results of the current study might have been affected by the presence of a family history of type 2 diabetes. Nonetheless, type 2 diabetes is multifactorial disease arising from a complex interplay between environmental factors and genetic susceptibility, and many individuals who develop type 2 diabetes have a family history of diabetes. Additionally, it should be mentioned that insulin secretion and b-cell function indexes offer only an estimate of the underlying complex physiological phenomena; hence it is possible that where no differences were found, it was because of the lack of sensitivity and sophistication of the applied methods and, likewise, where differences were found, they could have been much greater with better methods. Moreover, although the present results are remarkably similar to those reported in Mexican Americans, they are only based on Caucasian subjects, and generalizing them to other ethnic groups must be done with caution because differences between ethnic groups in insulin resistance have been reported. In addition, because there is evidence that these ethnicities have higher A1C levels at any given level of FPG as compared with their Caucasian counterparts even after adjustment for confounding factors affecting glycemia, our results may not be generalizable to Hispanics, American Indians, Blacks, and Asian Americans [21]. Finally, it can also be argued that our results might have been influenced by the strong genetic predisposition to type 2 diabetes since all the individuals were offspring of type 2 diabetes patients. In conclusion, the results of the present study demonstrate that Caucasian individuals with A1C >5.7% exhibit both core pathophysiological defects of type 2 diabetes i.e. insulin resistance and b-cell dysfunction. These findings, together with the increased relative risk of incident type 2 diabetes in individuals with A1C ranging from 5.5 to 6.0% favor using an A1C value ranging from 5.7% to 6.4% to identify individuals at increased risk for diabetes in analogy to subjects with IFG or IGT as recommended by ADA. Acknowledgments The study was supported in part by the Ministry of University grant MERIT RBNE08NKH7 to G.S. Appendix A. Supplementary data Supplementary data related to this article can be found at References [1] Nathan DM, Kuenen J, Borg R, Zheng H, Schoenfeld D, Heine RJ, A1c-Derived Average Glucose Study Group. Translating the A1C assay into estimated average glucose values. Diabetes Care 2008;31:1473e8. [2] International Expert Committee. International Expert Committee report on the role of the A1C assay in the diagnosis of diabetes. Diabetes Care 2009;32:1327e34. [3] American Diabetes Association. Standards of medical care in diabetes Diabetes Care 2012;35(Suppl. 1):S11e63. [4] Zhang X, Gregg EW, Williamson DF, Barker LE, Thomas W, Bullard KM, et al. A1C level and future risk of diabetes: a systematic review. Diabetes Care 2010;33:1665e73. [5] Laakso M, Zilinskaite J, Hansen T, Boesgaard TW, Vänttinen M, Stancáková A, et al. Insulin sensitivity, insulin release and GLP-1 levels in subjects with IFG and/or IGT in the EUGENE2 study. Diabetologia 2008;51:502e11. [6] Succurro E, Andreozzi F, Marini MA, Lauro R, Hribal ML, Perticone F, et al. Low plasma insulin-like growth factor-1 levels are associated with reduced insulin sensitivity and increased insulin secretion in nondiabetic subjects. Nutr Metab Cardiovasc Dis 2009;19:713e /j.numecd [7] Stancakova A, Javorsky M, Kuulasmaa T, Haffner SM, Kuusisto J, Laakso M. Changes in insulin sensitivity and insulin release in relation to glycemia and glucose tolerance in 6,414 Finnish men. Diabetes 2009;58:1212e21. [8] Abdul-Ghani MA, Jenkinson CP, Richardson DK, Tripathy D, DeFronzo RA. Insulin secretion and action in subjects with impaired fasting glucose and impaired glucose tolerance: results from the Veterans Administration Genetic Epidemiology Study. Diabetes 2006;55:1430e5. [9] Kahn SE. The importance of b-cell failure in the development and progression of type 2 diabetes. J Clin Endocrinol Metab 2001;86:4047e58. [10] Kanat M, Winnier D, Norton L, Arar N, Jenkinson C, Defronzo RA, et al. The relationship between b-cell function and glycated hemoglobin: results from the veterans administration genetic epidemiology study. Diabetes Care 2001;34:1006e10. [11] Marini MA, Succurro E, Arturi F, Ruffo MF, Andreozzi F, Sciacqua A, et al. Comparison of A1C, fasting and 2-h postload plasma glucose criteria to diagnose diabetes in Italian Caucasians. Nutr Metab Cardiovasc Dis 2012;22:561e [12] Marini MA, Succurro E, Castaldo E, Cufone S, Arturi F, Sciacqua A, et al. Cardiometabolic risk profiles and carotid atherosclerosis in individuals with prediabetes identified by
7 A1C, insulin sensitivity, and b-cell function 33 fasting glucose, postchallenge glucose, and hemoglobin A1c criteria. Diabetes Care 2012;35:1144e9. [13] Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, et al. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance: the Da Qing IGT and Diabetes Study. Diabetes Care 1997;20:537e44. [14] Ramachandran A, Snehalatha C, Mary S, Mukesh B, Bhaskar AD, Vijay V, et al. The Indian Diabetes Prevention Programme shows that lifestyle modification and metformin prevent type 2 diabetes in Asian Indian subjects with impaired glucose tolerance (IDPP-1). Diabetologia 2006;49:289e97. [15] Tuomilehto J, Lindström J, Eriksson JG, Valle TT, Hämäläinen H, Ilanne-Parikka P, et al. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001;344:1343e50. [16] Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346:393e403. [17] Chiasson JL, Josse RG, Gomis R, Hanefeld M, Karasik A, Laakso M, the STOP-NIDDM Trail Research Group. Acarbose for prevention of type 2 diabetes mellitus: the STOP-NIDDM randomised trial. Lancet 2002;359:2072e7. org/ /s (02) [18] DREAM (Diabetes REduction Assessment with ramipril and rosiglitazone Medication) Trial Investigators, Gerstein HC, Yusuf S, Bosch J, Pogue J, Sheridan P, et al. Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomised controlled trial. Lancet 2006;368:1096e org/ /s (06) [19] DeFronzo RA, Tripathy D, Schwenke DC, Banerji M, Bray GA, Buchanan TA, et al. Pioglitazone for diabetes prevention in impaired glucose tolerance. N Engl J Med 2011;364:1104e15. [20] Zinman B, Harris SB, Neuman J, Gerstein HC, Retnakaran RR, Raboud J, et al. Low-dose combination therapy with rosiglitazone and metformin to prevent type 2 diabetes mellitus (CANOE trial): a double-blind randomised controlled study. Lancet 2010;376:103e11. [21] Herman WH, Ma Y, Uwaifo G, Haffner S, Kahn SE, Horton ES, et al. Differences in A1C by race and ethnicity among patients with impaired glucose tolerance in the Diabetes Prevention Program. Diabetes Care 2007;30:2453e7.
and Training Standards for Diabetes Prevention [IMAGE] project) to provide
![and Training Standards for Diabetes Prevention [IMAGE] project) to provide and Training Standards for Diabetes Prevention [IMAGE] project) to provide](/thumbs/94/120124786.jpg) Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Insulin Sensitivity, b-cell Function, and Incretin Effect in Individuals With Elevated 1-h Postload Plasma Glucose Levels MARIA A. MARINI,
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Insulin Sensitivity, b-cell Function, and Incretin Effect in Individuals With Elevated 1-h Postload Plasma Glucose Levels MARIA A. MARINI,
HbA1c is associated with intima media thickness in individuals with normal glucose tolerance
 Diabetes Care Publish Ahead of Print, published online October 6, 2009 Glucose metabolism and IMT HbA1c is associated with intima media thickness in individuals with normal glucose tolerance Thomas Bobbert,
Diabetes Care Publish Ahead of Print, published online October 6, 2009 Glucose metabolism and IMT HbA1c is associated with intima media thickness in individuals with normal glucose tolerance Thomas Bobbert,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study
 Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
T he prevalence of type 2 diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS
 FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
Inflammation markers and metabolic characteristics of subjects with onehour plasma glucose levels
 Diabetes Care Publish Ahead of Print, published online November 16, 2009 Inflammation markers and metabolic characteristics of subjects with onehour plasma glucose levels Gianluca Bardini, MD, PhD, Ilaria
Diabetes Care Publish Ahead of Print, published online November 16, 2009 Inflammation markers and metabolic characteristics of subjects with onehour plasma glucose levels Gianluca Bardini, MD, PhD, Ilaria
Diabetes Care Publish Ahead of Print, published online February 25, 2011
 Pathophysiology/Complications O R I G I N A L A R T I C L E Diabetes Care Publish Ahead of Print, published online February 25, 2011 The Relationship Between b-cell Function and Glycated Hemoglobin Results
Pathophysiology/Complications O R I G I N A L A R T I C L E Diabetes Care Publish Ahead of Print, published online February 25, 2011 The Relationship Between b-cell Function and Glycated Hemoglobin Results
Elevated 1 h postload plasma glucose levels identify adults with normal glucose tolerance but increased risk of non-alcoholic fatty liver disease
 Open Access Research Elevated 1 h postload plasma glucose levels identify adults with normal glucose tolerance but increased risk of non-alcoholic fatty liver disease Giorgio Sesti, Marta Letizia Hribal,
Open Access Research Elevated 1 h postload plasma glucose levels identify adults with normal glucose tolerance but increased risk of non-alcoholic fatty liver disease Giorgio Sesti, Marta Letizia Hribal,
Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study
 Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study Lifen Kuang, Zhimin Huang, Zhenzhen Hong, Ailing Chen, Yanbing Li* ORIGINAL ARTICLE Department of Endocrinology
Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study Lifen Kuang, Zhimin Huang, Zhenzhen Hong, Ailing Chen, Yanbing Li* ORIGINAL ARTICLE Department of Endocrinology
Discussion points. The cardiometabolic connection. Cardiometabolic Risk Management in the Primary Care Setting
 Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
A46-yr-old female is referred to you for an abnormal fasting
 SPECIAL FEATURE Approach to the Patient Approach to the Patient with Prediabetes Vanita R. Aroda and Robert Ratner Med Star Clinical Research Center, Washington, D.C. 20003 Prediabetes consists of impaired
SPECIAL FEATURE Approach to the Patient Approach to the Patient with Prediabetes Vanita R. Aroda and Robert Ratner Med Star Clinical Research Center, Washington, D.C. 20003 Prediabetes consists of impaired
Copyright 2017 by Sea Courses Inc.
 Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
Prevention of diabetes and its associated
 Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Clinical Study 1-Hour OGTT Plasma Glucose as a Marker of Progressive Deterioration of Insulin Secretion and Action in Pregnant Women
 Hindawi Publishing Corporation International Journal of Endocrinology Volume 2012, Article ID 460509, 5 pages doi:10.1155/2012/460509 Clinical Study 1-Hour OGTT Plasma Glucose as a Marker of Progressive
Hindawi Publishing Corporation International Journal of Endocrinology Volume 2012, Article ID 460509, 5 pages doi:10.1155/2012/460509 Clinical Study 1-Hour OGTT Plasma Glucose as a Marker of Progressive
Introduction ARTICLE. A. Ramachandran (*). C. Snehalatha. S. Mary. B. Mukesh. A. D. Bhaskar. V. Vijay. Indian Diabetes Prevention Programme (IDPP)
 Diabetologia (26) 49: 289 297 DOI 1.17/s125-5-97-z ARTICLE A. Ramachandran. C. Snehalatha. S. Mary. B. Mukesh. A. D. Bhaskar. V. Vijay. Indian Diabetes Prevention Programme (IDPP) The Indian Diabetes Prevention
Diabetologia (26) 49: 289 297 DOI 1.17/s125-5-97-z ARTICLE A. Ramachandran. C. Snehalatha. S. Mary. B. Mukesh. A. D. Bhaskar. V. Vijay. Indian Diabetes Prevention Programme (IDPP) The Indian Diabetes Prevention
G enetic and environmental factors
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Insulin Secretion and Its Determinants in the Progression of Impaired Glucose TolerancetoType2DiabetesinImpaired Glucose-Tolerant
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Insulin Secretion and Its Determinants in the Progression of Impaired Glucose TolerancetoType2DiabetesinImpaired Glucose-Tolerant
Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance
 CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
Type 2 Diabetes in Adolescents
 Type 2 Diabetes in Adolescents Disclosures Paid consultant, Eli Lilly, Inc, Pediatric Type 2 Diabetes Clinical Trials Outline The burden of diabetes Treatment and Prevention Youth Diabetes Prevention Clinic
Type 2 Diabetes in Adolescents Disclosures Paid consultant, Eli Lilly, Inc, Pediatric Type 2 Diabetes Clinical Trials Outline The burden of diabetes Treatment and Prevention Youth Diabetes Prevention Clinic
Prediabetes awareness, healthcare provider s advice, and lifestyle changes in American adults
 International Journal of Diabetes Mellitus (2015) 3, 11 18 Diabetes Science International International Journal of Diabetes Mellitus www.elsevier.com/locate/ijdm www.sciencedirect.com ORIGINAL ARTICLE
International Journal of Diabetes Mellitus (2015) 3, 11 18 Diabetes Science International International Journal of Diabetes Mellitus www.elsevier.com/locate/ijdm www.sciencedirect.com ORIGINAL ARTICLE
Glucose Challenge Test as a Predictor of Type 2 Diabetes
 Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health Fall 1-8-2016 Glucose Challenge Test as a Predictor of Type 2 Diabetes Rahsaan Overton Follow
Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health Fall 1-8-2016 Glucose Challenge Test as a Predictor of Type 2 Diabetes Rahsaan Overton Follow
Implementing Type 2 Diabetes Prevention Programmes
 Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population Years of Age
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
1472 Diabetes Care Volume 39, August 2016
 1472 Diabetes Care Volume 39, August 2016 Prediabetes : Are There Problems With This Label? No, We Need Heightened Awareness of This Condition! Diabetes Care 2016;39:1472 1477 DOI: 10.2337/dc16-1143 William
1472 Diabetes Care Volume 39, August 2016 Prediabetes : Are There Problems With This Label? No, We Need Heightened Awareness of This Condition! Diabetes Care 2016;39:1472 1477 DOI: 10.2337/dc16-1143 William
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
C-Reactive Protein Predicts the Deterioration of Glycemia in Chinese Subjects With Impaired Glucose Tolerance
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E C-Reactive Protein Predicts the Deterioration of Glycemia in Chinese Subjects With Impaired Glucose Tolerance KATHRYN C.B.
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E C-Reactive Protein Predicts the Deterioration of Glycemia in Chinese Subjects With Impaired Glucose Tolerance KATHRYN C.B.
Why Do We Care About Prediabetes?
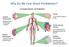 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Post-challenge hyperglycaemia is associated with premature death and macrovascular complications
 Diabetologia (2003) 46[Suppl1]:M17 M21 DOI 10.1007/s00125-002-0932-4 Post-challenge hyperglycaemia is associated with premature death and macrovascular complications Q. Qiao 1, 2, J. Tuomilehto 2, 3, K.
Diabetologia (2003) 46[Suppl1]:M17 M21 DOI 10.1007/s00125-002-0932-4 Post-challenge hyperglycaemia is associated with premature death and macrovascular complications Q. Qiao 1, 2, J. Tuomilehto 2, 3, K.
Lifestyle Intervention for Prevention of Type 2 Diabetes in Primary Health Care
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Lifestyle Intervention for Prevention of Type 2 Diabetes in Primary Health Care One-year follow-up of the Finnish National
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Lifestyle Intervention for Prevention of Type 2 Diabetes in Primary Health Care One-year follow-up of the Finnish National
PREVALENCE OF METABOLİC SYNDROME İN CHİLDREN AND ADOLESCENTS
 PREVALENCE OF METABOLİC SYNDROME İN CHİLDREN AND ADOLESCENTS Mehmet Emre Atabek,MD,PhD Necmettin Erbakan University Faculty of Medicine, Department of Pediatrics, Division of Pediatric Endocrinology and
PREVALENCE OF METABOLİC SYNDROME İN CHİLDREN AND ADOLESCENTS Mehmet Emre Atabek,MD,PhD Necmettin Erbakan University Faculty of Medicine, Department of Pediatrics, Division of Pediatric Endocrinology and
In the past 6 years, several randomized controlled
 Perspectives in Diabetes (How) Can We Prevent Type 2 Diabetes? Thomas A. Buchanan In the past 6 years, several randomized controlled trials have been conducted to test the impact of behavioral and pharmacological
Perspectives in Diabetes (How) Can We Prevent Type 2 Diabetes? Thomas A. Buchanan In the past 6 years, several randomized controlled trials have been conducted to test the impact of behavioral and pharmacological
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes!
 Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Introduction. Maria Adelaide Marini 1 Teresa Vanessa Fiorentino. Gaia Chiara Mannino 2 Maria Perticone. Giorgio Sesti 2
 DOI 10.1007/s00592-017-1004-z ORIGINAL ARTICLE Elevated 1-h post-challenge plasma glucose levels in subjects with normal glucose tolerance or impaired glucose tolerance are associated with whole blood
DOI 10.1007/s00592-017-1004-z ORIGINAL ARTICLE Elevated 1-h post-challenge plasma glucose levels in subjects with normal glucose tolerance or impaired glucose tolerance are associated with whole blood
Diabetes: Staying Two Steps Ahead. The prevalence of diabetes is increasing. What causes Type 2 diabetes?
 Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
The term impaired glucose tolerance
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk of Progression to Type 2 Diabetes Based on Relationship Between Postload Plasma Glucose and Fasting Plasma Glucose MUHAMMAD A. ABDUL-GHANI,
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk of Progression to Type 2 Diabetes Based on Relationship Between Postload Plasma Glucose and Fasting Plasma Glucose MUHAMMAD A. ABDUL-GHANI,
Development of type 2 diabetes is, to some
 Mode of Onset of Type 2 Diabetes from Normal or Impaired Glucose Tolerance Ele Ferrannini, 1 Monica Nannipieri, 1 Ken Williams, 2 Clicerio Gonzales, 3 Steve M. Haffner, 2 and Michael P. Stern 2 Fasting
Mode of Onset of Type 2 Diabetes from Normal or Impaired Glucose Tolerance Ele Ferrannini, 1 Monica Nannipieri, 1 Ken Williams, 2 Clicerio Gonzales, 3 Steve M. Haffner, 2 and Michael P. Stern 2 Fasting
The Effect of Lowering the Threshold for Diagnosis of Impaired Fasting Glucose
 Yonsei Med J 49(2):217-223, 2008 DOI 10.3349/ymj.2008.49.2.217 The Effect of Lowering the Threshold for Diagnosis of Impaired Fasting Glucose So Hun Kim, 1 Wan Sub Shim, 1 Eun A Kim, 1 Eun Joo Kim, 1 Seung
Yonsei Med J 49(2):217-223, 2008 DOI 10.3349/ymj.2008.49.2.217 The Effect of Lowering the Threshold for Diagnosis of Impaired Fasting Glucose So Hun Kim, 1 Wan Sub Shim, 1 Eun A Kim, 1 Eun Joo Kim, 1 Seung
Prevalence of Diabetes and High Risk for Diabetes Using A1C Criteria in the U.S. Population in
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Prevalence of Diabetes and High Risk for Diabetes Using A1C Criteria in the U.S. Population in 1988 2006 CATHERINE C. COWIE, PHD 1 KEITH
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Prevalence of Diabetes and High Risk for Diabetes Using A1C Criteria in the U.S. Population in 1988 2006 CATHERINE C. COWIE, PHD 1 KEITH
Association between arterial stiffness and cardiovascular risk factors in a pediatric population
 + Association between arterial stiffness and cardiovascular risk factors in a pediatric population Maria Perticone Department of Experimental and Clinical Medicine University Magna Graecia of Catanzaro
+ Association between arterial stiffness and cardiovascular risk factors in a pediatric population Maria Perticone Department of Experimental and Clinical Medicine University Magna Graecia of Catanzaro
Strategies for the prevention of type 2 diabetes and cardiovascular disease
 European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
Insulin-Resistant Prediabetic Subjects Have More Atherogenic Risk Factors Than Insulin-Sensitive Prediabetic Subjects
 Insulin-Resistant Prediabetic Subjects Have More Atherogenic Risk Factors Than Insulin-Sensitive Prediabetic Subjects Implications for Preventing Coronary Heart Disease During the Prediabetic State Steven
Insulin-Resistant Prediabetic Subjects Have More Atherogenic Risk Factors Than Insulin-Sensitive Prediabetic Subjects Implications for Preventing Coronary Heart Disease During the Prediabetic State Steven
Technical Information Guide
 Technical Information Guide This Guide provides information relating to the selection, utilization, and interpretation of the Quantose IR test. Information provided is based on peer-reviewed publications
Technical Information Guide This Guide provides information relating to the selection, utilization, and interpretation of the Quantose IR test. Information provided is based on peer-reviewed publications
Prediabetes Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Disclosures/Conflict of Interest.
 Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Pasta: A High-Quality Carbohydrate Food
 Pasta: A High-Quality Carbohydrate Food Cyril W.C. Kendall Department of Nutritional Sciences, Faculty of Medicine, University of Toronto; Clinical Nutrition & Risk Factor Modification Center, St. Michael
Pasta: A High-Quality Carbohydrate Food Cyril W.C. Kendall Department of Nutritional Sciences, Faculty of Medicine, University of Toronto; Clinical Nutrition & Risk Factor Modification Center, St. Michael
Prevention of diabetes type 2 by adjustment of lifestyle and diet
 International Journal of Community Medicine and Public Health Elahi AN et al. Int J Community Med Public Health. 2018 Sep;5(9):3697-3702 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Review Article
International Journal of Community Medicine and Public Health Elahi AN et al. Int J Community Med Public Health. 2018 Sep;5(9):3697-3702 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Review Article
Sex-specific differences in diabetes prevention: a systematic review and meta-analysis
 Diabetologia (2015) 58:242 254 DOI 10.1007/s00125-014-3439-x META-ANALYSIS Sex-specific differences in diabetes prevention: a systematic review and meta-analysis Anna Glechner & Jürgen Harreiter & Gerald
Diabetologia (2015) 58:242 254 DOI 10.1007/s00125-014-3439-x META-ANALYSIS Sex-specific differences in diabetes prevention: a systematic review and meta-analysis Anna Glechner & Jürgen Harreiter & Gerald
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead
 Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
The Metabolic Syndrome: Is It A Valid Concept? YES
 The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
Postchallenge Glucose, HbA 1c, and Fasting Glucose as Predictors of Type 2 Diabetes and Cardiovascular Disease: A 10-year Prospective Cohort Study
 Diabetes Care Publish Ahead of Print, published online June 23, 2010 A1C, Risk of Diabetes and CVD Postchallenge Glucose, HbA 1c, and Fasting Glucose as Predictors of Type 2 Diabetes and Cardiovascular
Diabetes Care Publish Ahead of Print, published online June 23, 2010 A1C, Risk of Diabetes and CVD Postchallenge Glucose, HbA 1c, and Fasting Glucose as Predictors of Type 2 Diabetes and Cardiovascular
Gestational Diabetes: Long Term Metabolic Consequences. Outline 5/27/2014
 Gestational Diabetes: Long Term Metabolic Consequences Gladys (Sandy) Ramos, MD Associate Clinical Professor Maternal Fetal Medicine Outline Population rates of obesity and T2DM Obesity and metabolic syndrome
Gestational Diabetes: Long Term Metabolic Consequences Gladys (Sandy) Ramos, MD Associate Clinical Professor Maternal Fetal Medicine Outline Population rates of obesity and T2DM Obesity and metabolic syndrome
Characteristicsof Glucose Disposal Index in General Population in China
 Characteristicsof Glucose Disposal Index in General Population in China QianRenM.D Department of Endocrinology and Metabolism, Peking University, People s Hospital Background We need to further characterize
Characteristicsof Glucose Disposal Index in General Population in China QianRenM.D Department of Endocrinology and Metabolism, Peking University, People s Hospital Background We need to further characterize
Type 2 diabetes mellitus and prediabetic dysglycemic
 ORIGINAL ARTICLE One-Hour ostload Hyperglycemia Confers Higher Risk of Hepatic Steatosis to HbA1c-Defined rediabetic Subjects Teresa Vanessa Fiorentino, Francesco Andreozzi, Gaia Chiara Mannino, Elisabetta
ORIGINAL ARTICLE One-Hour ostload Hyperglycemia Confers Higher Risk of Hepatic Steatosis to HbA1c-Defined rediabetic Subjects Teresa Vanessa Fiorentino, Francesco Andreozzi, Gaia Chiara Mannino, Elisabetta
Faculty. Identification and Treatment of Prediabetes to Prevent or Delay the Onset of T2DM. Learning Objectives. Disclosures
 Faculty Identification and Treatment of Prediabetes to Prevent or Delay the Onset of Sam Dagogo-Jack, MD, DM, FRCP A. C. Mullins Endowed Chair in Translational Research Professor of Medicine & Director
Faculty Identification and Treatment of Prediabetes to Prevent or Delay the Onset of Sam Dagogo-Jack, MD, DM, FRCP A. C. Mullins Endowed Chair in Translational Research Professor of Medicine & Director
Does the ticking clock go backward as well as forward?
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Singapore Impaired Glucose Tolerance Follow-Up Study Does the ticking clock go backward as well as forward? MOH-SIM
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Singapore Impaired Glucose Tolerance Follow-Up Study Does the ticking clock go backward as well as forward? MOH-SIM
programme. The DE-PLAN follow up.
 What are the long term results and determinants of outcomes in primary health care diabetes prevention programme. The DE-PLAN follow up. Aleksandra Gilis-Januszewska, Noël C Barengo, Jaana Lindström, Ewa
What are the long term results and determinants of outcomes in primary health care diabetes prevention programme. The DE-PLAN follow up. Aleksandra Gilis-Januszewska, Noël C Barengo, Jaana Lindström, Ewa
Should pregnant women be excluded from community based lifestyle intervention trial?- a case study
 Should pregnant women be excluded from community based lifestyle intervention trial?- a case study Elezebeth Mathews, Ph.D., MPH Assistant Professor Department of Public Health and Community Medicine Central
Should pregnant women be excluded from community based lifestyle intervention trial?- a case study Elezebeth Mathews, Ph.D., MPH Assistant Professor Department of Public Health and Community Medicine Central
Eugene Barrett M.D., Ph.D. University of Virginia 6/18/2007. Diagnosis and what is it Glucose Tolerance Categories FPG
 Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
It is well known that obesity, unbalanced
 D I A B E T E S P R O G R E S S I O N, P R E V E N T I O N, A N D T R E A T M E N T Nonpharmacologic Therapy and Exercise in the Prevention of Type 2 Diabetes JAAKKO TUOMILEHTO, MD, MPOLSC, PHD OBJECTIVE
D I A B E T E S P R O G R E S S I O N, P R E V E N T I O N, A N D T R E A T M E N T Nonpharmacologic Therapy and Exercise in the Prevention of Type 2 Diabetes JAAKKO TUOMILEHTO, MD, MPOLSC, PHD OBJECTIVE
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey
 Diabetes Care Publish Ahead of Print, published online December 15, 2008 Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey Valerie
Diabetes Care Publish Ahead of Print, published online December 15, 2008 Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey Valerie
2010 ADA Guidelines: 1. Diagnostic Criteria for DM 2. Categories of increased risk of DM. Gerti Tashko, M.D. DM Journal Club 1/21/2010
 2010 ADA Guidelines: 1. Diagnostic Criteria for DM 2. Categories of increased risk of DM Gerti Tashko, M.D. DM Journal Club 1/21/2010 NEW: Diagnosis with A1c 6.5% Cut point of A1c 6.5% diagnoses 33% less
2010 ADA Guidelines: 1. Diagnostic Criteria for DM 2. Categories of increased risk of DM Gerti Tashko, M.D. DM Journal Club 1/21/2010 NEW: Diagnosis with A1c 6.5% Cut point of A1c 6.5% diagnoses 33% less
Prediabetes & Type 2 Diabetes Prevention. Jacob M. Haus, PHD
 Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
Impact of Hemoglobin A1c Screening and Brief Intervention in a Medicare Population
 Impact of Hemoglobin A1c Screening and Brief Intervention in a Medicare Population Mary Jo Quinn DNP, ARNP-C, ACHPN Susan Schaffer PhD, ARNP, FNP-BC University of Florida College of Nursing, Gainesville,
Impact of Hemoglobin A1c Screening and Brief Intervention in a Medicare Population Mary Jo Quinn DNP, ARNP-C, ACHPN Susan Schaffer PhD, ARNP, FNP-BC University of Florida College of Nursing, Gainesville,
Treating Postprandial Hyperglycemia Does Not Appear to Delay Progression of Early Type 2 Diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Treating Postprandial Hyperglycemia Does Not Appear to Delay Progression of Early Type 2 Diabetes The Early Diabetes Intervention Program
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Treating Postprandial Hyperglycemia Does Not Appear to Delay Progression of Early Type 2 Diabetes The Early Diabetes Intervention Program
Asian Journal of Medical and Biological Research ISSN (Print) (Online)
 , 458-463; doi: 10.3329/ajmbr.v2i3.30118 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article Management and treatment patterns
, 458-463; doi: 10.3329/ajmbr.v2i3.30118 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article Management and treatment patterns
Prevention of diabetes in the modern era of affluent society and economic constraints
 Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
A high-risk phenotype associates with reduced improvement in glycaemia during a lifestyle intervention in prediabetes
 Diabetologia (215) 58:2877 2884 DOI 1.17/s125-15-376-z ARTICLE A high-risk phenotype associates with reduced improvement in glycaemia during a lifestyle intervention in prediabetes Norbert Stefan 1,2,3
Diabetologia (215) 58:2877 2884 DOI 1.17/s125-15-376-z ARTICLE A high-risk phenotype associates with reduced improvement in glycaemia during a lifestyle intervention in prediabetes Norbert Stefan 1,2,3
Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance Test in a Chinese Population
 Hindawi Diabetes Research Volume 2017, Article ID 3212814, 5 pages https://doi.org/10.1155/2017/3212814 Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance
Hindawi Diabetes Research Volume 2017, Article ID 3212814, 5 pages https://doi.org/10.1155/2017/3212814 Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance
Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes
 Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes Leigh Perreault, MD Associate Professor of Medicine Endocrinology, Metabolism and Diabetes University of Colorado Anschutz Medical
Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes Leigh Perreault, MD Associate Professor of Medicine Endocrinology, Metabolism and Diabetes University of Colorado Anschutz Medical
Diabetes and Obesity Sex- and Gender-differences!
 Oskar Kokoschka 1908 Das Mädchen Li und ich Diabetes and Obesity Sex- and Gender-differences! Alexandra Kautzky Willer IGM, Berlin 2015 Global Diabetes-Epidemic Increase (%) in age-standardised diabetes
Oskar Kokoschka 1908 Das Mädchen Li und ich Diabetes and Obesity Sex- and Gender-differences! Alexandra Kautzky Willer IGM, Berlin 2015 Global Diabetes-Epidemic Increase (%) in age-standardised diabetes
Long-term trends in cardiorespiratory fitness and the incidence of type 2. diabetes
 Diabetes Care Publish Ahead of Print, published online March 9, 2010 Long-term trends in fitness and diabetes Long-term trends in cardiorespiratory fitness and the incidence of type 2 diabetes Running
Diabetes Care Publish Ahead of Print, published online March 9, 2010 Long-term trends in fitness and diabetes Long-term trends in cardiorespiratory fitness and the incidence of type 2 diabetes Running
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden
 Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians VISWANATHAN MOHAN, MD, PHD 1 VENKATARAMAN VIJAYACHANDRIKA,
Epidemiology/Health Services Research O R I G I N A L A R T I C L E A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians VISWANATHAN MOHAN, MD, PHD 1 VENKATARAMAN VIJAYACHANDRIKA,
Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study. Arab Medical University. Benghazi, Libya
 Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Current Diabetes Care for Internists:2011
 Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
Primary Prevention of T2DM. KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009
 Primary Prevention of T2DM KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009 Primary Prevention of T2DM Why to intervene? When to intervene? Lifestyle intervention Pharmacological
Primary Prevention of T2DM KW Chan Endocrine & Diabetes Team Department of M&G, PMH 22 March 2009 Primary Prevention of T2DM Why to intervene? When to intervene? Lifestyle intervention Pharmacological
The Arab Risk (ARABRISK): Translation and Validation.
 Biomedical Research 2014; 25 (2): 271-275 ISSN 0970-938X http://www.biomedres.info The Arab Risk (ARABRISK): Translation and Validation. Alia Alghwiri a, Ahmad Alghadir b,c, Hamzeh Awad b* a Department
Biomedical Research 2014; 25 (2): 271-275 ISSN 0970-938X http://www.biomedres.info The Arab Risk (ARABRISK): Translation and Validation. Alia Alghwiri a, Ahmad Alghadir b,c, Hamzeh Awad b* a Department
Epidemiology of Diabetes, Impaired Glucose Homeostasis and Cardiovascular Risk. Eberhard Standl
 Epidemiology of Diabetes, Impaired Glucose Homeostasis and Cardiovascular Risk Eberhard Standl European Heart House Sophia Antipolis Thursday, June 17, 2010 IDF Diabetes Atlas 2009: Global Numbers Still
Epidemiology of Diabetes, Impaired Glucose Homeostasis and Cardiovascular Risk Eberhard Standl European Heart House Sophia Antipolis Thursday, June 17, 2010 IDF Diabetes Atlas 2009: Global Numbers Still
Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range.
 Diabetes Care Publish Ahead of Print, published online November 13, 2007 Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range. Rucha Jani, M.D., Marjorie
Diabetes Care Publish Ahead of Print, published online November 13, 2007 Decreased Non-Insulin Dependent Glucose Clearance Contributes to the Rise in FPG in the Non-Diabetic Range. Rucha Jani, M.D., Marjorie
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
DIABETES. A growing problem
 DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
PREVALENCE OF INSULIN RESISTANCE IN FIRST DEGREE RELATIVES OF TYPE-2 DIABETES MELLITUS PATIENTS: A PROSPECTIVE STUDY IN NORTH INDIAN POPULATION
 PREVALENCE OF INSULIN RESISTANCE IN FIRST DEGREE RELATIVES OF TYPE-2 DIABETES MELLITUS PATIENTS: A PROSPECTIVE STUDY IN NORTH INDIAN POPULATION Arvind Kumar, Poornima Tewari, Sibasis S. Sahoo and Arvind
PREVALENCE OF INSULIN RESISTANCE IN FIRST DEGREE RELATIVES OF TYPE-2 DIABETES MELLITUS PATIENTS: A PROSPECTIVE STUDY IN NORTH INDIAN POPULATION Arvind Kumar, Poornima Tewari, Sibasis S. Sahoo and Arvind
Type 2 diabetes is occurring in epidemic proportions
 The Natural History of Progression From Normal Glucose Tolerance to Type 2 Diabetes in the Baltimore Longitudinal Study of Aging James B. Meigs, 1 Denis C. Muller, 2 David M. Nathan, 3 Deirdre R. Blake,
The Natural History of Progression From Normal Glucose Tolerance to Type 2 Diabetes in the Baltimore Longitudinal Study of Aging James B. Meigs, 1 Denis C. Muller, 2 David M. Nathan, 3 Deirdre R. Blake,
Reducing cardiovascular risk factors in patients with prediabetes
 REVIEW Reducing cardiovascular risk factors in patients with prediabetes Jean-Louis Chiasson 1 & Sophie Bernard 1 Practice Points The prevalence of prediabetes is high and on the rise. Subjects with impaired
REVIEW Reducing cardiovascular risk factors in patients with prediabetes Jean-Louis Chiasson 1 & Sophie Bernard 1 Practice Points The prevalence of prediabetes is high and on the rise. Subjects with impaired
Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea
 https://doi.org/10.7180/kmj.2016.31.2.157 KMJ Original Article Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea Ju Won Lee, Nam Kyu Kim, Hyun Joon Park,
https://doi.org/10.7180/kmj.2016.31.2.157 KMJ Original Article Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea Ju Won Lee, Nam Kyu Kim, Hyun Joon Park,
The American Diabetes Association estimates
 DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range
 Pathophysiology/Complications O R I G I N A L A R T I C L E Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range RUCHA JANI, MD MARJORIE
Pathophysiology/Complications O R I G I N A L A R T I C L E Decreased Non Insulin-Dependent Glucose Clearance Contributes to the Rise in Fasting Plasma Glucose in the Nondiabetic Range RUCHA JANI, MD MARJORIE
Laboratory analysis of the obese child recommendations and discussion. MacKenzi Hillard May 4, 2011
 Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Diabete: terapia nei pazienti a rischio cardiovascolare
 Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
The use of A1C for the identification
 Reviews/Commentaries/ADA R E V I E W A R T I C L E Statements A1C Level and Future Risk of Diabetes: A Systematic Review XUANPING ZHANG, PHD 1 EDWARD W. GREGG, PHD 1 DAVID F. WILLIAMSON, PHD 2 LAWRENCE
Reviews/Commentaries/ADA R E V I E W A R T I C L E Statements A1C Level and Future Risk of Diabetes: A Systematic Review XUANPING ZHANG, PHD 1 EDWARD W. GREGG, PHD 1 DAVID F. WILLIAMSON, PHD 2 LAWRENCE
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
1/28/2014. The Metabolic Syndrome: Early History. Insulin Resistance: Early Diagnosis and Treatment to Prevent Cardiovascular Disease
 : Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
: Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
Diabetes Care 24:89 94, 2000
 Pathophysiology/Complications O R I G I N A L A R T I C L E Insulin Resistance and Insulin Secretory Dysfunction Are Independent Predictors of Worsening of Glucose Tolerance During Each Stage of Type 2
Pathophysiology/Complications O R I G I N A L A R T I C L E Insulin Resistance and Insulin Secretory Dysfunction Are Independent Predictors of Worsening of Glucose Tolerance During Each Stage of Type 2
The IDF consensus worldwide definition of the metabolic syndrome
 International Diabetes Federation Avenue Emile De Mot 19 B-1000 Brussels, Belgium Telephone +32-2-5385511 Telefax +32-2-5385114 info@idf.org www.idf.org VAT BE433.674.528 The IDF consensus worldwide definition
International Diabetes Federation Avenue Emile De Mot 19 B-1000 Brussels, Belgium Telephone +32-2-5385511 Telefax +32-2-5385114 info@idf.org www.idf.org VAT BE433.674.528 The IDF consensus worldwide definition
DPP-4 inhibitor. The new class drug for Diabetes
 DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
