Symptoms, causes and treatment options of different IRDs
|
|
|
- Marian Warner
- 5 years ago
- Views:
Transcription
1 Symptoms, causes and treatment options of different IRDs While all IRDs affect the retina and visual function, the symptoms, onset, progression and cause of each varies. Here, we will give an overview of the different symptoms of the different IRDs in a PDF format that you can easily download. In our Focus On section on this website, you can find out more about certain diseases as this Toolkit develops. Usher Syndrome Leber Congenital Amaurosis Retinitis Pigmentosa Choroideremia Juvenile Macular Degeneration Stargardt Disease Best Disease Juvenile X-linked Retinoschisis Leber Hereditary Optic Neuropathy Cone-Rod Dystrophies Achromatopsia Gyrate Atrophy Kearns-Sayre syndrome 1 Back to contents Retina International 10/18
2 Usher syndrome Usher syndrome is a syndromic IRD that affects both hearing and vision. The symptoms of Usher syndrome consist of hearing loss (found at an early age), vision loss caused by a condition called retinitis pigmentosa (RP), and sometimes balance problems. While people with IRDs do have a higher risk of developing hearing issues late in life than the general population, Usher syndrome is characterised by hearing loss early-on in life. You can find more information on Usher Syndrome in our Focus on: Usher Syndrome section (link) Leber Congenital Amaurosis Leber congenital amaurosis (LCA) appears at birth or in very young children. It is an inherited disease that can result in quite severe vision loss. The level of vision loss varies between individuals; some people affected can have little or no light perception. Both rod and cone cells are affected by the mutations and both will degenerate and die. Retinitis Pigmentosa Retinitis pigmentosa (RP) is a term used to describe a group of diseases where vision loss gradually worsens due to progressive photoreceptor degeneration, resulting in legal blindness. Onset of the disease can vary widely, with some people starting to notice changes as children while others are diagnosed in adulthood. In general, RP affects both eyes similarly. The early symptoms noticed by people with RP usually include difficulties with seeing in dim light and moving between bright or dark environments, along with a gradual loss of peripheral vision These symptoms are due to the initial degeneration of the rod cells, which are responsible for seeing in dim light and are more concentrated at the edges of the retina. In the later stages of the disease, the disease can affect cones cells in the centre of the retina, resulting in loss of central vision and colour vision. This video gives an insight into loss of peripheral vision due to RP Video showing loss of peripheral vision with RP: While visual function will get progressively worse with time in people with RP, the rate of progression and the extent of vision loss can be very different between individuals affected, even varying between people from the same family. For this reason, it is very difficult to know how quickly or slowly the disease will progress in an affected individual. 2 Back to contents Retina International 10/18
3 What is the cause of RP and how is it inherited? RP is one of the most complicated genetic conditions of all, and over 50 different genes have been identified to be causative for various forms of RP. There are various inheritance patterns for RP, including autosomal dominant (30-40%), autosomal recessive (50-60%) and X-linked (5-15%). Approximately 50% of RP patients will have a history of at least one other family member being affected. Half of patients will not have a family history of the condition. While their RP is still caused by a gene alteration, it might not be possible to determine the inheritance pattern in these patients. The autosomal dominant form of disease tends to follow a milder course with maintenance of preserved vision well into late middle age. The X-linked form is the most severe and central vision may be lost by the third decade. RP is a genetic disease, but cases with no family history also commonly occur. If a family member is diagnosed with RP, it is strongly advised that other members of the family also have an eye exam by an eye doctor (ophthalmologist) who is specially trained to detect retinal diseases. What treatments are available for RP? Maximising the remaining vision that an individual has is a crucial first step to take. There are many new low vision aids including telescopic and magnifying lenses. The wide range of assistive technologies for people with visual impairments provides plenty of choice for users at all stages of sight loss, and this technology has also removed many barriers to education and employment. There are, as of yet, no proven or effective cures for RP, although research in this area has accelerated and potential therapies are in clinical trial stage. The term RP represents an extremely large and varied group of diseases, as scientists have now identified more than 200 genes that can have mutations causing RP. Typically, each person with RP only has a mutation in a single pair of genes. Gene therapy to replace defective genes by inserting healthy genes into the retina via harmless viruses is being explored in clinical trials for a small number of RP genes. Emerging gene therapy treatments are designed to specifically target the gene responsible for the individual patient s form of RP. Therefore, the importance of ensuring access to genetic testing to establish which form of RP a family or individual is affected by cannot be overemphasised. Another research area currently being explored is that of drug treatments which aim to preserve the function of the rod and cone photoreceptor cells, thereby keeping them alive for longer. Many of these drugs are re-purposed drugs, which may have already been approved for a different disease and are now being tested for their effectiveness in RP. It is estimated that as few as 5% of cone cells need to be preserved by such a treatment in order to have a significant impact on quality of life by the maintenance of a small but very useful amount of central vision. 3 Back to contents Retina International 10/18
4 Gene therapy and drug therapies hold huge promise to treat individuals at an early to mid-stage of disease progression, where there are still some viable rod and cone cells present. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. Stem Cell Technology Stem cell technology holds great potential to replace retinal cells that have already died due to degeneration. Scientists are currently working on replacing two different cell types by stem cell therapy - retinal pigment epithelium (RPE) cells and photoreceptor cells. RPE cells are a special type of cell that support the photoreceptor cells, but are not responsible for seeing, therefore it is hoped that replacement of RPE cells will help the retina function better, prevent further vision loss, and help nourish surviving retinal cells. This cell type would need to be replaced in time to help support a retina that is still working. Efforts at transplanting stem cell-derived photoreceptor cells are at an even earlier stage of research, however a number of recent animal studies have shown the potential to restore function in the eye, which may pave the way for human studies in the future. Retina Implants Retinal implants are a form of biomedical technology currently being developed for use by people affected by retinitis pigmentosa. A number of these implants have shown success in delivering a form of artificial vision to individuals with total vision loss due to RP. When all or most of the photoreceptor cells have died, they can theoretically be replaced by an electronic microchip that brings a visual image to the remaining cells of the retina. These microchips electronically signal the remaining retinal cells which pass the signal down the optic nerve for processing as a visual image by the brain. At the moment, these devices do not restore natural vision, but can be very useful in improving mobility, by allowing an individual to see a difference in light and dark to the point where they can tell how to walk through a doorway. A number of devices are now on the market in certain regions. See your Eye Doctor! Despite the lack of current treatments for RP, it is still very important to continue to have regular eye check-ups. This is because people with RP are still at risk for other kinds of eye problems that can affect the general population and may be treatable. RP patients tend to develop cataracts at an earlier age than the non-rp population and can do very well from cataract surgery, although the visual outcome obviously depends on the severity of the retinal degeneration. Regular visits to your eye doctor can also make you aware of current advances as we learn more about RP. 4 Back to contents Retina International 10/18
5 Choroideremia Choroideremia primarily occurs in men as it is caused by a genetic defect on the X-chromosome. Women can be carriers of choroideremia but rarely experience full symptoms. The first symptom of choroideremia is problems with seeing in low light (night-blindness), which is usually seen in childhood. Affected. As the disease progresses, peripheral vision deteriorates first and people with choroideremia may develop tunnel vision. By late adulthood, the remaining central vision is lost. Choroideremia is a rare disease, affecting an estimated 1 in 50,000 people. Choroideremia is sometimes misdiagnosed as other retinal conditions such as RP due to the similarity of symptoms. However, the family inheritance pattern of mainly males being affected and the characteristic pattern of the back of the eye help with diagnosis. What is the cause of choroideremia and how is it inherited? Unlike some other retinal degenerations, such as RP, cases of choroideremia are due to mutations in just one gene, known as CHM. The CHM gene makes an essential protein called REP-1, which is involved in escorting essential nutrients between cells in the back of the eye. However, about 20% of patients with a clinical diagnosis of choroideremia have been found not to have a mutation in the CHM gene. Choroideremia is genetically passed through families by an X-linked pattern of inheritance. The CHM gene is located on the X chromosome. Females have two X chromosomes, but generally only one of the chromosomes will carry a faulty copy of the gene and the other functioning copy will compensate. Therefore, females are carriers of the condition, but do not generally display the severe symptoms of the disease. In women, one or other of the two X chromosomes is randomly inactivated in every cell. Usually, in female carriers of X-linked disease genes, including CHM, this results in 50% of the retinal cells working on the altered CHM gene and the other 50% working on the normal copy of the CHM gene. These women will have very subtle, if any, symptoms of the disease. Inactivation, however, in some women may be skewed in favour of either the normal or the altered CHM gene copy. If more than 50% of the normal CHM copy is inactivated, the carrier female will have more symptoms. In rare, extreme cases of skewed inactivation the carrier female might be almost as severely affected as a male. Because males only have one X chromosome, they will become affected by the condition if they receive a faulty copy of the gene. Affected males cannot pass on the disease to their sons, because they pass on their Y chromosome. Men with choroideremia will pass on the disease gene to all of their daughters, who then become carriers of the gene. If a family member is diagnosed with choroideremia, it is strongly advised that other members of the family also have an eye exam by an eye doctor (ophthalmologist) who is specially trained to detect retinal diseases. 5 Back to contents Retina International 10/18
6 What treatments are available? For an individual affected by choroideremia, maximising the remaining vision that an individual has is a crucial first step to take, and there are many new low vision aids including telescopic and magnifying lenses. The wide range of assistive technologies for people with visual impairments provides plenty of choice for users at all stages of sight loss, and this technology has also removed many barriers to education and employment. At this time, there are no treatments available for choroideremia. However, in recent years there have been momentous leaps made in clinical research and development. Over the past twenty years, researchers have identified the causative CHM gene, explored gene therapy in mouse models of disease and performed necessary safety tests of this treatment approach. This has culminated in the authorisation of a small number of gene therapy clinical trials in people with choroideremia. In these gene therapy trials, the researchers engineer a small, non-toxic virus to deliver the correct version of the CHM gene into the light-sensing photoreceptor cells in the retina. The patient s retina is first detached and then the virus is injected underneath using a very fine needle. Early results from this trial have been positive, no safety issues have been reported and, in some cases, improvements in vision have been observed. The safety and effectiveness of this treatment is being monitored as a priority and there is great hope that a treatment will emerge in the future. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. Juvenile Macular Degeneration Juvenile macular degeneration is the term used to describe a series of inherited eye disorders that affect children and young adults. Juvenile macular degeneration is different from age-related macular degeneration, which occurs as part of the body s natural aging process. Juvenile macular degeneration is sometimes called macular dystrophy. Macular degeneration is a deterioration or breakdown of the eye's macula. The macula is a small area in the centre of the retina the light-sensitive tissue lining the back of the eye. The macula is the part of the retina that is responsible for your central vision, allowing you to see fine details clearly. The macula makes up only a small part of the retina, yet it is much more sensitive to detail than the rest of the retina (called the peripheral retina). The macula is what allows you to thread a needle, read small print, and read street signs. The peripheral retina gives you side (or peripheral) vision. If someone is standing off to one side of your vision, your peripheral retina helps you know that person is there by allowing you to see their general shape. The most common form of juvenile macular degeneration is Stargardt disease. Other types of juvenile macular degeneration include Best s disease (also called Best s vitelliform retinal dystrophy), and juvenile retinoschisis. All of these diseases are rare and cause central vision loss. Unfortunately, there is no treatment available to prevent vision loss. 6 Back to contents Retina International 10/18
7 Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. Stargardt Disease Stargardt disease, also referred to as fundus flavimaculatus, affects the functional, central area of the retina called the macula. It is the most common form of inherited juvenile macular degeneration. The macula is rich in cone cells, which give us colour vision and central vision for tasks such as reading. It is usually first diagnosed in the teenage years when decreased central vision is experienced. The progression of Stargardt disease varies between individuals. However, while central vision is lost, peripheral vision can often be preserved as this is reliant on rod cells rather than cone cells. Stargardt Disease Symptoms Usually, both eyes are affected to a similar extent. The initial symptom experienced is usually difficulty reading as central vision is impaired. This can be followed by the appearance of blind spots in the visual field that may increase with time. While it is usual for an individual with Stargardt disease to completely lose their sight, the disease can progress slowly and be degenerative. However, it is difficult to predict progression in the future as the disease can vary considerably between individuals, even affected members of the same family. The following videos address living with Stargardt disease: from Fighting Blindness and from MDF Australia What is the cause of Stargardt disease and how is it inherited? Stargardt disease is estimated to affect between 1 in 8,000 to 10,000 people worldwide. The majority of people with Stargardt disease have the recessive form of disease, involving mutations in the ABCA4 gene, which provides instructions to make the ABCA4 protein. If there is a faulty ABCA4 gene, it leads to the build-up of a toxic waste product known as A2E in the retinal pigment epithelium (RPE) and this can lead to macular degeneration and progressive loss of vision. A very rare form of Stargardt disease may be caused by mutations in the ELOVL4 gene, which follows an autosomal dominant form of inheritance. Mutations in the ELOVL4 gene can make dysfunctional ELOVL4 protein clumps that can interfere with photoreceptor cell functions leading to cell death. 7 Back to contents Retina International 10/18
8 If a family member is diagnosed with Stargardt disease, it is strongly advised that other members of the family also have an eye exam by an eye doctor (ophthalmologist) who is specially trained to detect retinal diseases. What treatments are available? At present, there are no effective treatments for Stargardt disease. There is research to suggest that UV sunlight can increase the toxicity of the waste products accumulating in the retina, therefore, it is recommended that people with Stargardt disease wear UV screening sunglasses when out in direct sunlight. Recent evidence also suggests that taking extra vitamin A, such as in a vitamin supplement, may have a negative effect on the condition and should be avoided. Gene therapy is currently being explored for the recessive form of Stargardt disease caused by ABCA4 gene mutations. The idea behind gene therapy is that a normal copy of the ABCA4 gene can be engineered in the laboratory. This can then be injected into the eye of an affected individual, delivering the correct copy of the gene and therefore stopping the degeneration of the sight of the individual. This safety and effectiveness of this treatment approach is currently being evaluated in early-stage clinical trials conducted in people with this form of Stargardt disease Stem cells are amazing cells that are produced in the body and have the remarkable potential to develop into many different cell types in the body during early life and growth. A number of groups worldwide are currently manipulating stem cells from various origins in order to produce retinal pigment epithelial (RPE) and these cells have been injected into a number of patients. The transplantation of these functional cells into patients may prevent the death of the remaining photoreceptors and may, therefore, help Stargardt patients avoid further sight loss. These early stage clinical trials are currently on-going. Efforts at transplanting stem cell-derived photoreceptor cells are at an even earlier stage of research, but a number of recent animal studies have shown the potential to restore function in the eye, which may pave the way for human studies in the future. Another interesting approach that is currently being studied as a therapy involves research into a modified form of vitamin A, called deuterated vitamin A. The researchers hope that this may help slow the accumulation of A2E by blocking its formation downstream in the visual cycle. They are currently testing the safety of this approach. Please note however that recent evidence suggests that taking extra normal vitamin A, such as in a vitamin supplement from a health shop, may have a negative effect on the condition and should be avoided as this can increase toxic levels of A2E. Despite the lack of current treatments for Stargardt disease, general eye check-ups are important. This is because people with Stargardt disease are still at risk for other kinds of eye problems that can affect the general population and may be treatable. Regular visits to your eye doctor can also make you aware of current advances and new treatments as we learn more about the condition. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. 8 Back to contents Retina International 10/18
9 Best Disease What Is Best Disease? Best disease, also known as vitelliform macular dystrophy, is an inherited form of retinal degeneration affecting the portion of the retina known as the macula. The macula is the central part of the retina containing the photoreceptor cells known as cone cells, which are responsible for fine visual detail and colour perception. Best disease is usually diagnosed during the teenage years, but vision does not generally deteriorate until later in life. The progression of visual loss varies between individuals but side or peripheral vision usually remains unaffected. Therefore, people with Best disease do not generally have issues with independent mobility. What are the symptoms of Best disease? The first symptoms of Best disease can vary from person to person but always involves the central vision. In the initial stages, a fatty yellow pigment builds up in the cells underneath the macula. Over time, the abnormal accumulation of this substance can damage the cone cells located in the macula, leading to a blurring or distortion of central vision. Best disease generally doesn t affect peripheral or side vision. It does not always affect both eyes equally and clearer vision is sometimes retained in one eye. What is the cause of Best disease and how is it inherited? Best disease is a genetic disease and is caused by mutations in the BEST1 gene which produces the protein Bestrophin-1. Best disease is passed down through families by an autosomal dominant pattern of inheritance. In this pattern of inheritance, an affected person has a mutated BEST1 gene paired with a normal copy of the BEST1 gene. When the affected person has children with an unaffected partner, there is a 50 percent chance that the affected parent will pass the mutated BEST1 gene to each child. The unaffected partner will only pass normal copies of BEST1 genes. A child who does not have a mutated BEST1 gene will not have the disease and cannot then pass the disease to his or her children. Owing to the variable expression of the BEST1-mutated gene, some people who have the mutation may have very mild, or in rare cases, no symptoms. What treatments are available? Currently, there is no treatment for Best disease. Genetic research identified the BEST1 gene as causative for Best disease in 1998 and researchers are now working on understanding the function of this gene in the retina. Recently, there have been encouraging gene therapy studies in preclinical models of Best disease. These findings mark the first clear steps to developing a therapy that could prevent vision loss. Using this approach, which has proven to be safe in other retinal conditions, researchers engineer small, non-toxic viruses to deliver the correct version of the BEST1 gene to the retina. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. 9 Back to contents Retina International 10/18
10 Juvenile X-linked Retinoschisis Juvenile X-linked retinoschisis is a rare genetic disease of the retina and primarily affects boys and young men. Retinoschisis is a condition in which an area of the retina (the tissue lining the inside of the back of the eye that transmits visual signals to the optic nerve and brain) has separated into two layers. The part of the retina that is affected by retinoschisis will have poorer vision, however very few people with retinoschisis lose all of their vision. Affected boys are usually diagnosed while at primary/middle school when poor vision and difficulty with reading become more apparent, but occasionally the disease is diagnosed in young infants. Most boys with retinoschisis present with a mild decrease in central vision that may be subtle and not perceptible. They may continue to lose vision into their teens. Once they are adults, their vision often stabilises until they are in their 50s or 60s. Retinoschisis patients are more susceptible to retinal detachment and eye haemorrhage (bleeding) than other people and they should have regular examinations with an eye doctor. When detected early, a complicating retinal detachment can be treated surgically. What is the cause of retinoschisis and how is it inherited? The exact prevalence of retinoschisis is currently unknown, but it is thought to affect between one in 5,000 to 20,000 people, and is therefore a rare condition. X-linked retinoschisis is usually caused by mutations (defects) in the RS1 (retinoschisin 1) gene, which is located, as the name suggests, on the X chromosome. Men have only one X chromosome, while women have two. Therefore, because women almost always have another functioning X chromosome, they typically retain normal vision, even as carriers. However, in rare circumstances, due to the phenomenon of non-random X chromosome inactivation some female carriers may have symptoms. Men, on the other hand, will develop sub-optimal vision if they have an affected X chromosome. Affected males cannot pass on the disease to their sons, because they pass on their Y chromosome. Men who have retinoschisis must pass on the disease gene to all of their daughters who in turn become carriers of the condition. What treatments are available? Maximising an individual s remaining vision is a crucial first step to take, and there are many new low vision aids including telescopic and magnifying lenses. Currently, there are no medical or surgical treatments available for retinoschisis. Glasses may improve the overall quality of vision in a patient with retinoschisis who is also near-sighted or farsighted but will not repair the nerve tissue damage from the retinoschisis. In 1997, researchers identified mutations in the RS1 gene on the X chromosome that cause retinoschisis. Scientists then studied the gene to determine its function in the retina and this work has greatly enhanced efforts to develop treatments for this condition. A number of groups 10 Back to contents Retina International 10/18
11 worldwide are now working on developing gene therapies for retinoschisis. These innovative therapies aim to deliver healthy copies of the RS1 gene by a non-toxic virus, therefore replacing defective copies at the back of the eye. General eye check-ups are important for people with retinoschisis, as these men and boys are still at risk for other kinds of eye problems that can affect the general population and may be treatable. They are also more vulnerable to retinal detachments and haemorrhages. Regular visits to your eye doctor can also make you aware of current advances as we learn more about retinoschisis. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. Leber Hereditary Optic Neuropathy Leber hereditary optic neuropathy (LHON) is a genetic disease that leads to sudden vision loss during young adult life. Men are more likely to be affected than women. LHON is a disorder caused by mutations in the genetic code of the mitochondria, which are small subunits that reside within the cell. Mitochondria are also known as the powerhouses of the cell as they constantly convert energy locked in our food into energy that the cell can use. Our eyes are our most energy hungry organs and a lack of energy production can lead to degeneration and death of retinal ganglion cells (RGCs), which are the nerve cells that communicate visual information to the brain. Loss of these cells leads to subsequent degeneration of the optic nerve and visual loss. However, it is worth noting that a significant percentage of people who possess a mutation that causes LHON do not develop any features of the disorder. Loss of vision due to LHON does not cause any eye pain, but it is quite an alarming experience as the loss of central vision presents suddenly and can progress quite quickly, leaving only peripheral vision. This means that the majority of people with LHON retain independent mobility but cannot focus on anything straight ahead or see fine detail. What are the symptoms of LHON? Affected individuals do not usually present any symptoms until they develop visual blurring affecting their central vision. These vision problems may begin in one eye or both simultaneously. If one eye is affected, then similar symptoms appear in the other eye on average eight weeks later. Over time, the vision in both eyes worsens with a severe loss of sharpness and a fading of colour vision. The vision loss mainly affects central vision, which is needed for tasks such as reading, driving and recognising faces. In a small percentage of cases, the central vision loss can improve; but in most cases loss of vision is permanent. The severity of symptoms may vary from one affected individual to another, even within the same family, due to a dosage effect. This is due to the fact that we have many mitochondria in each cell. 11 Back to contents Retina International 10/18
12 In one individual, if only a small proportion of mitochondria in each cell have the mutation, symptoms will be mild. In another individual, if a higher proportion of mitochondria in each cell carry the mutation, symptoms will be more severe. What is the cause of LHON and how is it inherited? LHON follows a mitochondrial pattern of inheritance, which is also known as maternal inheritance. Only egg cells and not sperm cells contribute mitochondria to a developing embryo, therefore only females can pass mitochondrial conditions to their children. Fathers affected by LHON or carrying LHON mutations do not pass the condition to their children. Often, people who develop LHON have no family history of the condition. However, it is currently impossible to predict which members of a family who carry a mutation will eventually develop vision loss. More than 50% of men and more than 85% of women with a mitochondrial mutation will never experience vision loss. LHON is a very rare condition. Research has revealed that three particular mutations in mitochondrial genes account for between 85% 90% of cases of LHON. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. 12 Back to contents Retina International 10/18
13 Cone-Rod Dystrophies Cone-rod dystrophies refer to a group of inherited diseases that affect the photoreceptor (light sensing) cells that are responsible for capturing images from the visual field. These cells line the back of the eye in the region known as the retina. Cone cells are present throughout the retina but are concentrated in the central region (the macula). They are useful for central (reading) vision. Rod cells are present throughout the retina except for the very centre and they help with night vision. In contrast to typical RP (known as the rod-cone dystrophies), which results from the loss of rod cells and later the cone cells, cone-rod dystrophies reflect the opposite sequence of events, where cone cells are primarily first affected with later loss of rods. What are the symptoms of cone-rod dystrophy? The cone cells are initially involved, as previously mentioned, and difficulty with the clarity of vision, colour vision problems and light sensitivity can be some of the earliest symptoms experienced. This is followed by a progressive loss of rod cells, which leads to night blindness and loss of side (peripheral) vision. The age of onset, progression and severity of cone-rod dystrophies can vary greatly from one person to another, even among individuals with the same type of cone-rod dystrophy. It is therefore very difficult to predict what an individual s vision will be like at a specific time in the future. Some forms of cone-rod dystrophy are inherited; other forms appear to occur spontaneously for no apparent reason (sporadically). Cone-rod dystrophies have many similarities to RP following varied inheritance patterns, including autosomal dominant, autosomal recessive, and X-linked. What treatments are available? Maximising an individual s remaining vision is a crucial first step to take. There are many new low vision aids, including telescopic and magnifying lenses, providing plenty of choice for users at all stages of sight loss. This technology has also removed many barriers to education and employment. There are, currently, no proven or effective cures for cone-rod dystrophies. However, scientists have identified more than 20 genes that can have mutations which cause these conditions. It is likely that many more mutations in many more genes will be identified in the coming years. Despite the lack of current treatments for cone-rod dystrophies, general eye check-ups are important. People with these conditions are still at risk for other kinds of eye problems that can affect the general population and may be treatable. Patients with cone rod dystrophies tend to develop cataracts at an earlier age than the overall population. Regular visits to your eye doctor can also make you aware of current advances as we learn more about these conditions. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. 13 Back to contents Retina International 10/18
14 Achromatopsia Achromatopsia is a rare hereditary vision disorder affecting the cone photoreceptor cells, resulting in an absence of colour vision along with additional visual problems. There are two main types of cells in the retina responsible for capturing the visual field; the rod cells and the cone cells. We use our rod cells at night time and in low light, but they are not sensitive to colour and do not provide detailed vision. We use our cone cells in bright light. They are responsible for our colour vision and for our central, reading vision. Genetic changes or mutations in genes that function in cone cells are responsible for achromatopsia. Individuals with achromatopsia have reduced visual acuity and are completely or almost fully colour blind; however, the condition is not progressive and it does not lead to blindness. What are the symptoms of achromatopsia? The condition is often first noticed in a young child by their parents, as children with achromatopsia may dislike bright lights and often avoid the daylight (known as photophobia). Nystagmus is another symptom of the condition, where their eyes may involuntary move and dance. Judging from their behaviour some parents may notice that their child s vision may be reduced or blurred. However, most children with achromatopsia have no problem with mobility or getting around. What is the cause of achromatopsia and how is it inherited? To date, mutations in one of five genes are known to cause achromatopsia. The condition is inherited in an autosomal recessive manner, which means that an affected individual inherits a mutated copy of an achromatopsia-linked gene from both parents. Most often, the parents of an individual with achromatopsia each carry one copy of the mutated gene, but do not show signs and symptoms of the condition. What treatments are available? The vision of people with achromatopsia decreases as the levels of light increase. In regular home lighting indoors, or outdoors just after dawn or just before dusk, some people with achromatopsia adapt to their reduced level of visual function without resorting to tinted lenses. Instead, they use visual strategies such as squinting or shielding their eyes or they position themselves in favourable light. Others sometimes wear medium tinted lenses in such settings. However, in full sunlight outdoors, or in very bright indoor spaces, almost all people with achromatopsia use very dark tinted lenses in order to function with a reasonable amount of vision, since they do not possess functioning cone photoreceptors needed in order to see well in these types of settings. Two of the most common genes linked to the condition (CNGB3 and CNGA3) account for 75% of achromatopsia cases, making this condition potentially amenable to gene therapy. Based on a number of successful results in animal models of achromatopsia, a number of groups have initiated human gene therapy clinical trials. These trials plan to deliver a normal copy of the mutated gene back to retina, in theory restoring cone function and visual function. Information about clinical trials that are currently being conducted worldwide can be found on and can be searched by condition and trial location. 14 Back to contents Retina International 10/18
15 Gyrate Atrophy Gyrate atrophy is an autosomal recessive dystrophy caused by mutations in the gene for ornithine aminotransferase (OAT), located on chromosome 10. Originally thought to be a subtype of choroideremia, the disorder is the result of ten-fold elevations of plasma ornithine, which is toxic to the RPE and choroid. Patients with gyrate atrophy have hyperpigmented fundi, with lobular loss of the RPE and choroid. The finding of generalised hyperpigmentation of the remaining RPE helps to clinically distinguish gyrate atrophy from choroideremia. In the early stages, patients have large, geographic peripheral paving-stone like areas of atrophy of the RPE and choriocapillaris, which gradually coalesce to form a characteristic scalloped border at the junction of normal and abnormal RPE. Affected patients usually develop night blindness during the first decade of life and experience progressive loss of visual field and visual acuity later in the disease course. The clinical diagnosis can be confirmed by measuring serum or plasma ornithine levels; molecular confirmation can be obtained by mutational analysis of the OAT gene. Occasionally, older patients present with an uncommon syndrome of peripheral chorioretinal atrophy that closely mimics gyrate atrophy; normal plasma ornithine levels in such patients exclude the diagnosis. What treatments are available? Although dietary restriction of arginine has been used to treat some gyrate atrophy patients, the diet is very difficult to maintain and must be monitored by paediatricians with experience in metabolic disease. Vitamin B6 treatment lowers the plasma ornithine levels in a small percentage of gyrate atrophy patients. Whether such a reduction improves the long-term visual outcome is unknown, but, unlike arginine restriction, vitamin supplementation is relatively easy to administer. Long-term vitamin therapy should be considered only for patients whose ornithine levels can be shown to drop in response to treatment. 15 Back to contents Retina International 10/18
16 Kearns-Sayre syndrome Kearns-Sayre syndrome is a condition that affects many parts of the body, especially the eyes. The features of Kearns-Sayre syndrome usually appear before the age of 20 years, and the condition is diagnosed by a few characteristic signs and symptoms. What are the symptoms of Kearns-Sayre Syndrome? People with Kearns-Sayre syndrome have progressive external ophthalmoplegia, which is weakness or paralysis of the eye muscles that impairs eye movement and causes drooping eyelids (ptosis). Affected individuals also have an eye condition called pigmentary retinopathy, which results from degeneration of the retina that gives it a speckled and streaked appearance. The retinopathy may cause loss of vision. People with Kearns-Sayre syndrome can often have abnormalities of the electrical signals that control the heartbeat (cardiac conduction defects), problems with coordination and balance that cause unsteadiness while walking (ataxia), or abnormally high levels of protein in the fluid that surrounds and protects the brain and spinal cord (the cerebrospinal fluid or CSF). They may also experience muscle weakness in their limbs, deafness, kidney problems, or a deterioration of cognitive functions (dementia). Affected individuals often have short stature. In addition, diabetes mellitus is occasionally seen in people with Kearns-Sayre syndrome. When the muscle cells of affected individuals are stained and viewed under a microscope, these cells usually appear abnormal. The abnormal muscle cells contain an excess of structures called mitochondria and are known as ragged-red fibers. A related condition called ophthalmoplegia-plus may be diagnosed if an individual has many of the signs and symptoms of Kearns-Sayre syndrome but not all the criteria are met. 16 Back to contents Retina International 10/18
How the eye works. Causes of retinitis pigmentosa
 Retinitis pigmentosa Retinitis pigmentosa (RP) is the name given to a diverse group of inherited eye disorders which affect a part of the eye called the retina. RP causes permanent changes to your vision
Retinitis pigmentosa Retinitis pigmentosa (RP) is the name given to a diverse group of inherited eye disorders which affect a part of the eye called the retina. RP causes permanent changes to your vision
Ophthalmology. Ophthalmology Services
 Ophthalmology Ophthalmology Services The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems
Ophthalmology Ophthalmology Services The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems
Understanding. Retinitis pigmentosa. and other inherited retinal dystrophies
 Understanding Retinitis pigmentosa and other inherited retinal dystrophies Contact us We re here to answer any questions you have about your eye condition or treatment. If you need further information
Understanding Retinitis pigmentosa and other inherited retinal dystrophies Contact us We re here to answer any questions you have about your eye condition or treatment. If you need further information
Let s Learn About. Visual Impairment
 Let s Learn About Visual Impairment Vision impairment and Blindness have many causes. Birth defects, eye disorders or injuries, and age-related diseases such as glaucoma and cataracts can lead to loss
Let s Learn About Visual Impairment Vision impairment and Blindness have many causes. Birth defects, eye disorders or injuries, and age-related diseases such as glaucoma and cataracts can lead to loss
Visual Conditions in Infants and Toddlers
 Visual Conditions and Functional Vision: Early Intervention Issues Visual Conditions in Infants and Toddlers Brief Overview of Childhood Visual Disorders Hatton, D.D. (2003). Brief overview of childhood
Visual Conditions and Functional Vision: Early Intervention Issues Visual Conditions in Infants and Toddlers Brief Overview of Childhood Visual Disorders Hatton, D.D. (2003). Brief overview of childhood
Advances in assessing and managing vision impairment
 Advances in assessing and managing vision impairment John Grigg Associate Professor and Head Discipline of Ophthalmology Consultant Ophthalmologist Sydney Eye Hospital and The Children s Hospital at Westmead
Advances in assessing and managing vision impairment John Grigg Associate Professor and Head Discipline of Ophthalmology Consultant Ophthalmologist Sydney Eye Hospital and The Children s Hospital at Westmead
LUXTURNA (voretigene neparovec-rzyl)
 LUXTURNA (voretigene neparovec-rzyl) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
LUXTURNA (voretigene neparovec-rzyl) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical
UKGTN Testing Criteria
 UKGTN Testing Criteria Approved name and symbol of disease/condition(s): Retinal Degeneration panel test Approved name and symbol of gene(s): a panel of 105 genes, variants of which have been shown to
UKGTN Testing Criteria Approved name and symbol of disease/condition(s): Retinal Degeneration panel test Approved name and symbol of gene(s): a panel of 105 genes, variants of which have been shown to
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Your guide to juvenile macular dystrophies
 Support throughout Your guide to juvenile macular dystrophies No one need face macular degeneration alone. For information and support call 0300 3030 111. Macular Society QR codes Throughout this leaflet
Support throughout Your guide to juvenile macular dystrophies No one need face macular degeneration alone. For information and support call 0300 3030 111. Macular Society QR codes Throughout this leaflet
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Corporate Medical Policy
 Corporate Medical Policy Voretigene Neparvovec-rzyl (Luxturna) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: voretigene_neparvovec_rzyl_luxturna 1/2018 N/A 6/2018 2/2018 Description
Corporate Medical Policy Voretigene Neparvovec-rzyl (Luxturna) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: voretigene_neparvovec_rzyl_luxturna 1/2018 N/A 6/2018 2/2018 Description
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
INHERITED RETINAL DISEASE. The Rod/Cone Dichotomy. Case History/Entrance Skills. Health Assessment 9/4/18. Hereditary Retinal Diseases Epidemiology
 Hereditary Retinal Diseases Epidemiology INHERITED RETINAL DISEASE Blair Lonsberry, MS, OD, MEd., FAAO Professor of Optometry Pacific University College of Optometry blonsberry@pacificu.edu HRDs affect
Hereditary Retinal Diseases Epidemiology INHERITED RETINAL DISEASE Blair Lonsberry, MS, OD, MEd., FAAO Professor of Optometry Pacific University College of Optometry blonsberry@pacificu.edu HRDs affect
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Age-related Macular Degeneration (AMD) and Diabetic Retinopathy (DR)
 Preserve Vision Information Age-related Macular Degeneration (AMD) and Diabetic Retinopathy (DR) Regular examination by your ophthalmologist will allow early detection and treatment. Age-related Macular
Preserve Vision Information Age-related Macular Degeneration (AMD) and Diabetic Retinopathy (DR) Regular examination by your ophthalmologist will allow early detection and treatment. Age-related Macular
Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease
 8:00 AM Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease Albert M. Maguire, MD OBJECTIVE Assess maintenance of functional vision/visual
8:00 AM Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease Albert M. Maguire, MD OBJECTIVE Assess maintenance of functional vision/visual
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Choroideremia OMIM number for disease 303100 Disease alternative names please
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Choroideremia OMIM number for disease 303100 Disease alternative names please
Diabetic Retinopathy Information
 http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
Age-Related Macular Degeneration (AMD)
 Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Thank you for taking the time to learn a little bit more about our organization.
 The Gavin R Stevens Foundation was inspired by two year old, Gavin. Gavin was diagnosed at four months of age, with Leber s Congenital Amaurosis (LCA), an inherited retina disease which causes blindness.
The Gavin R Stevens Foundation was inspired by two year old, Gavin. Gavin was diagnosed at four months of age, with Leber s Congenital Amaurosis (LCA), an inherited retina disease which causes blindness.
Age-Related. macular degeneration.
 Age-Related Macular Degeneration This pamphlet is designed to help people with age-related macular degeneration and their families better understand the disease. It describes the causes, symptoms, diagnosis,
Age-Related Macular Degeneration This pamphlet is designed to help people with age-related macular degeneration and their families better understand the disease. It describes the causes, symptoms, diagnosis,
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Leber congenital amaurosis OMIM number for disease 204000 Disease alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name Leber congenital amaurosis OMIM number for disease 204000 Disease alternative
Clinical Summaries. CLN1 Disease, infantile onset and others
 Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
An Introduction to mitochondrial disease.
 9 th September 2017 An Introduction to mitochondrial disease. Dr Andy Schaefer Consultant Neurologist and Clinical Lead NHS Highly Specialised Rare Mitochondrial Disease Service and Wellcome Trust Centre
9 th September 2017 An Introduction to mitochondrial disease. Dr Andy Schaefer Consultant Neurologist and Clinical Lead NHS Highly Specialised Rare Mitochondrial Disease Service and Wellcome Trust Centre
FOUNDATION OVERVIEW. Over the past four decades, the Foundation has raised $600 million to put an end to retinal degenerative diseases.
 FOUNDATION OVERVIEW Passion and Focus The Foundation Fighting Blindness was established in 1971 by a passionate group of individuals driven to overcome blinding eye diseases that were affecting themselves
FOUNDATION OVERVIEW Passion and Focus The Foundation Fighting Blindness was established in 1971 by a passionate group of individuals driven to overcome blinding eye diseases that were affecting themselves
Manual. Manual Welsh Eye Care Initiative. A Welsh Eye Care Initiative. Protocol. The Assessment and Management of Age-related Macular Degeneration
 A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz)
 PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Flashers and Floaters
 Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION GLAUCOMA GLAUCOMA
 GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
Specialist Referral Service Willows Information Sheets. Cataract surgery
 Specialist Referral Service Willows Information Sheets Cataract surgery An operating microscope in use A total cataract - the normally black pupil is bluish white Cataract surgery These notes do not cover
Specialist Referral Service Willows Information Sheets Cataract surgery An operating microscope in use A total cataract - the normally black pupil is bluish white Cataract surgery These notes do not cover
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
DIABETIC RETINOPATHY
 THE UK GUIDE DIABETIC RETINOPATHY Everything you need to know about diabetic retinopathy Jaheed Khan BSc (Hons) MBBS MD FRCOphth Fellow of the Royal College of Ophthalmologists Association for Research
THE UK GUIDE DIABETIC RETINOPATHY Everything you need to know about diabetic retinopathy Jaheed Khan BSc (Hons) MBBS MD FRCOphth Fellow of the Royal College of Ophthalmologists Association for Research
Chapter 32. Hearing, Speech, and Vision Problems. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 32 Hearing, Speech, and Vision Problems Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 32.1 Define the key terms and key abbreviations in this chapter. Describe the common ear, speech,
Chapter 32 Hearing, Speech, and Vision Problems Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 32.1 Define the key terms and key abbreviations in this chapter. Describe the common ear, speech,
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Happy New Year! Dan Roberts. International Low Vision Support Group NEWSLETTER. This Month. In This Issue
 In This Issue 1: This Month 2-4: News 5: A Message to Your Doctor Happy New Year! from Macular Degeneration Support The ILVSG is sponsored by MD Foundation www.eyesight.org 888-633-3937 ILVSG TeleSupport
In This Issue 1: This Month 2-4: News 5: A Message to Your Doctor Happy New Year! from Macular Degeneration Support The ILVSG is sponsored by MD Foundation www.eyesight.org 888-633-3937 ILVSG TeleSupport
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? WHAT CAUSES DIABETIC RETINOPATHY? WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
 Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
FROM CATARACTS TO CLARITY
 Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
Background. Financial disclaimer. The evaluation process. Objectives
 Background We are seeing the very early stages of a change in how we think about ophthalmic lenses. This is exciting stuff for optometrists and opticians! In addition to the traditional use of lenses for
Background We are seeing the very early stages of a change in how we think about ophthalmic lenses. This is exciting stuff for optometrists and opticians! In addition to the traditional use of lenses for
Managing eye health and vision loss in residential aged care facilities
 Managing eye health and vision loss in residential aged care facilities A resource for management and health professionals About this publication This resource is designed to provide residential aged care
Managing eye health and vision loss in residential aged care facilities A resource for management and health professionals About this publication This resource is designed to provide residential aged care
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
What You Should Know About Angioid Streaks By David J. Browning, MD, PhD
 What You Should Know About Angioid Streaks By David J. Browning, MD, PhD The eye wall has several layers, as shown in figure 1. Proceeding from the inside of the eye to the outside, the layers are as follows:
What You Should Know About Angioid Streaks By David J. Browning, MD, PhD The eye wall has several layers, as shown in figure 1. Proceeding from the inside of the eye to the outside, the layers are as follows:
Applying structure-function to solve clinical cases
 Applying structure-function to solve clinical cases Professor Michael Kalloniatis Centre for Eye Health, and, School of Optometry and Vision Science Acknowledgements Some material prepared by Nayuta Yoshioka
Applying structure-function to solve clinical cases Professor Michael Kalloniatis Centre for Eye Health, and, School of Optometry and Vision Science Acknowledgements Some material prepared by Nayuta Yoshioka
1.! Yes I do. 2.! No I don t. COPE Approved: COPE # PD! " !! What is electrodiagnostics testing? !! Visual Pathway Basic Understanding !!
 1.! Yes I do 2.! No I don t Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic COPE Approved: COPE # 3132-PD #$ #$! " 1.! Monthly
1.! Yes I do 2.! No I don t Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic COPE Approved: COPE # 3132-PD #$ #$! " 1.! Monthly
What is Alport s Syndrome? Why it is called Alport s Syndrome? What Causes Alport s Syndrome, and differences between men and women?
 ALPORT S SYNDROME What is Alport s Syndrome? Why is it called Alport s Syndrome? What causes Alport s Syndrome? How is Alport s Syndrome diagnosed? Is Alport s Syndrome common? Is there any treatment to
ALPORT S SYNDROME What is Alport s Syndrome? Why is it called Alport s Syndrome? What causes Alport s Syndrome? How is Alport s Syndrome diagnosed? Is Alport s Syndrome common? Is there any treatment to
Unravelling the genetic basis of simplex Retinitis Pigmentosa cases
 SUPPLEMENTARY INFORMATION Unravelling the genetic basis simplex Retinitis Pigmentosa cases Nereida Bravo-Gil 1,2#, María González-del Pozo 1,2#, Marta Martín-Sánchez 1, Cristina Méndez-Vidal 1,2, Enrique
SUPPLEMENTARY INFORMATION Unravelling the genetic basis simplex Retinitis Pigmentosa cases Nereida Bravo-Gil 1,2#, María González-del Pozo 1,2#, Marta Martín-Sánchez 1, Cristina Méndez-Vidal 1,2, Enrique
RETINITIS PIGMENTOSA A RARE GENETICAL DISORDER
 RETINITIS PIGMENTOSA A RARE GENETICAL DISORDER Retinitis pigmentosa (RP) is a group of inherited disorders affecting 1 in 3000-7000 people and characterized by abnormalities of the photoreceptors (rods
RETINITIS PIGMENTOSA A RARE GENETICAL DISORDER Retinitis pigmentosa (RP) is a group of inherited disorders affecting 1 in 3000-7000 people and characterized by abnormalities of the photoreceptors (rods
OAKLEIGH EYE CENTRE. THE EYE Before looking at diabetic retinopathy it is important to understand what the healthy eye looks like and how it works.
 ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
Charcot-Marie-Tooth Disease (CMT) Sometimes known as Hereditary Motor and Sensory neuropathy (HMSN) or Peroneal Muscular Atrophy (PMA)
 Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Patient Information Brochure. Cataract
 Patient Information Brochure Cataract Q: What is cataract? A: A cataract is an opacity (or cloudiness) in the lens of the eye. This cloudiness develops inside the lens and restricts light passing through
Patient Information Brochure Cataract Q: What is cataract? A: A cataract is an opacity (or cloudiness) in the lens of the eye. This cloudiness develops inside the lens and restricts light passing through
AgePage. Aging And Your Eyes. Steps To Protect Your Eyesight
 National Institute on Aging AgePage Aging And Your Eyes Are you holding the newspaper farther away from your eyes than you used to? Join the crowd age can bring changes that affect your eyesight. Some
National Institute on Aging AgePage Aging And Your Eyes Are you holding the newspaper farther away from your eyes than you used to? Join the crowd age can bring changes that affect your eyesight. Some
Patient AB. Born in 1961 PED
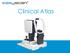 Clinical Atlas Patient AB Born in 1961 PED Autofluorescence Dilated 45 EasyScan Zero-dilation IR 45 Fundus Dilated 45 In the fundus photos (Canon CX1) the PED is not able to be seen. However, the extent
Clinical Atlas Patient AB Born in 1961 PED Autofluorescence Dilated 45 EasyScan Zero-dilation IR 45 Fundus Dilated 45 In the fundus photos (Canon CX1) the PED is not able to be seen. However, the extent
Cataract Surgery. Patient Information. How your care will be organised. Introduction
 Patient Information Cataract Surgery If you have any questions regarding your operation please contact Parkerswell Day Case Unit on 01392 406013. They are available between 09:00-17:30, Monday to Friday.
Patient Information Cataract Surgery If you have any questions regarding your operation please contact Parkerswell Day Case Unit on 01392 406013. They are available between 09:00-17:30, Monday to Friday.
Patient information. Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7
 Patient information Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7 Your eye specialist has advised you to have retinal detachment surgery. This leaflet gives you information that will help you
Patient information Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7 Your eye specialist has advised you to have retinal detachment surgery. This leaflet gives you information that will help you
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Myopia and pathological myopia. Fundus Photo, Right Eye (OD)
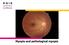 Myopia and pathological myopia Fundus Photo, Right Eye (OD) Contents 3 What is myopia and pathological myopia 3 How does the eye focus light? 3 What is myopia? 4 Development of myopia 4 What causes myopia?
Myopia and pathological myopia Fundus Photo, Right Eye (OD) Contents 3 What is myopia and pathological myopia 3 How does the eye focus light? 3 What is myopia? 4 Development of myopia 4 What causes myopia?
Macular Hole. Helpline
 Macular Hole The retina is a light-sensitive layer of tissue lining the back of the eye. The macula is a small area at the centre of the retina responsible for all of our central vision, most of our colour
Macular Hole The retina is a light-sensitive layer of tissue lining the back of the eye. The macula is a small area at the centre of the retina responsible for all of our central vision, most of our colour
C horoideraemia is an X linked, recessively inherited,
 658 CLINICAL SCIENCE Retrospective, longitudinal, and cross sectional study of visual acuity impairment in choroideraemia M Flynn Roberts, G A Fishman, D K Roberts, J R Heckenlively, R G Weleber, R J Anderson,
658 CLINICAL SCIENCE Retrospective, longitudinal, and cross sectional study of visual acuity impairment in choroideraemia M Flynn Roberts, G A Fishman, D K Roberts, J R Heckenlively, R G Weleber, R J Anderson,
Cataract Surgery Patient Information
 Cataract Surgery Patient Information www.ihg.org.uk Independent Health Group Patient Referral Centre T: 0330 3801362 E: ihg.referralsandenquiries@nhs.net Independent Health Group Limited is registered
Cataract Surgery Patient Information www.ihg.org.uk Independent Health Group Patient Referral Centre T: 0330 3801362 E: ihg.referralsandenquiries@nhs.net Independent Health Group Limited is registered
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Can mineral content in diet influence mineralization in Pseudoxanthoma Elasticum (PXE)?
 Can mineral content in diet influence mineralization in Pseudoxanthoma Elasticum (PXE)? Eliza Duvall September 2016 Abstract Pseudoxanthoma Elasticum (PXE) is a rare genetic disorder with no effective
Can mineral content in diet influence mineralization in Pseudoxanthoma Elasticum (PXE)? Eliza Duvall September 2016 Abstract Pseudoxanthoma Elasticum (PXE) is a rare genetic disorder with no effective
Genetics and the Macular Dystrophies. George Anadiotis D.O. Medical Director Clinical and Biochemical Genetics Randall Children s Hospital
 Genetics and the Macular Dystrophies George Anadiotis D.O. Medical Director Clinical and Biochemical Genetics Randall Children s Hospital Stargardt disease Best Vitelliform Macular Dystrophy North Carolina
Genetics and the Macular Dystrophies George Anadiotis D.O. Medical Director Clinical and Biochemical Genetics Randall Children s Hospital Stargardt disease Best Vitelliform Macular Dystrophy North Carolina
IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology
 IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to you so that you can make an informed
IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to you so that you can make an informed
Cataracts (1 of 7) What is a cataract? What can be done about a cataract? Lens
 i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
PATIENT INFORMATION LEAFLET MACULAR HOLE. What is the macula?
 What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film in a camera. Light is focused through the eye onto the retina, allowing us to see. The centre
What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film in a camera. Light is focused through the eye onto the retina, allowing us to see. The centre
Patient Information Cataract Surgery
 Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Understanding. Posterior vitreous detachment
 Understanding Posterior vitreous detachment Contact us We re here to answer any questions you have about your eye condition or treatment. If you need further information about posterior vitreous detachment
Understanding Posterior vitreous detachment Contact us We re here to answer any questions you have about your eye condition or treatment. If you need further information about posterior vitreous detachment
Major new Macular Degeneration Foundation research initiative
 Research Update 2010 Global research on the causes, genetics and treatment of Macular Degeneration continues at a hectic pace. In fact, no other area of ophthalmology is receiving as much attention at
Research Update 2010 Global research on the causes, genetics and treatment of Macular Degeneration continues at a hectic pace. In fact, no other area of ophthalmology is receiving as much attention at
Dan Roberts. International Low Vision Support Group NEWSLETTER. This Month. In This Issue. 1: This Month 2-5: News
 In This Issue 1: This Month 2-5: News Eye & Body Complete from Biosyntrx Extra Strength Protection Call for information 800-688-6815 The ILVSG is sponsored by MD Foundation www.eyesight.org 888-633-3937
In This Issue 1: This Month 2-5: News Eye & Body Complete from Biosyntrx Extra Strength Protection Call for information 800-688-6815 The ILVSG is sponsored by MD Foundation www.eyesight.org 888-633-3937
Understanding Albinism
 Understanding Albinism What is Albinism? People with Albinism are born with little or no pigment in their eyes, skin and hair, although in some cases the reduced pigmentation only affects the eyes. Albinism
Understanding Albinism What is Albinism? People with Albinism are born with little or no pigment in their eyes, skin and hair, although in some cases the reduced pigmentation only affects the eyes. Albinism
An Artificial Technique to Regain Vision Caused due to Retinal Impairment
 Current Development in Artificial Intelligence. ISSN 0976-5832 Volume 2, Number 1 (2011), pp. 21-26 International Research Publication House http://www.irphouse.com An Artificial Technique to Regain Vision
Current Development in Artificial Intelligence. ISSN 0976-5832 Volume 2, Number 1 (2011), pp. 21-26 International Research Publication House http://www.irphouse.com An Artificial Technique to Regain Vision
Macular Hole Surgery
 What is the macula? Macular Hole Surgery The macula is the part of the retina that enables us to make out things clearly and see colours. Rays of light enter the eye and are focused on the macular area
What is the macula? Macular Hole Surgery The macula is the part of the retina that enables us to make out things clearly and see colours. Rays of light enter the eye and are focused on the macular area
Phenotype Report. Num. Positions Not Called (Missing data) Num. Variants Assessed
 Report Date: August 19, 2015 Software Annotation Version: 8 Report Name: NA12144 NW European Genome : NA12144_S1 Sequencing Provider: Illumina Sequencing Type: Exome : Retinitis Pigmentosa Description:
Report Date: August 19, 2015 Software Annotation Version: 8 Report Name: NA12144 NW European Genome : NA12144_S1 Sequencing Provider: Illumina Sequencing Type: Exome : Retinitis Pigmentosa Description:
CATARACT & LENS SURGERY CATARACT SURGERY
 GENERAL INFORMATION CATARACT & LENS SURGERY CATARACT SURGERY WHAT IS A CATARACT? A cataract is not a growth, but rather a clouding of the normally transparent and flexible lens of the eye. This condition
GENERAL INFORMATION CATARACT & LENS SURGERY CATARACT SURGERY WHAT IS A CATARACT? A cataract is not a growth, but rather a clouding of the normally transparent and flexible lens of the eye. This condition
11/14/2013. Progressive Eye Conditions. Agenda. Review from Sessions 1 and 2 Session 1 Review of Eye Conditions. Objectives
 1 Progressive Eye Conditions Agenda 2:00 Introductions and Reconnect FIMC-VI Webinar Series Eye Conditions and Impact on Learning Session #3 of 3 November 13, 2013 Kay Ratzlaff Florida Instructional Materials
1 Progressive Eye Conditions Agenda 2:00 Introductions and Reconnect FIMC-VI Webinar Series Eye Conditions and Impact on Learning Session #3 of 3 November 13, 2013 Kay Ratzlaff Florida Instructional Materials
When Eyes Show Their Age
 When Eyes Show Their Age A guide to preserving the gift of sight for as long as possible with the compliments of Division of Health Services Diocese of Camden Expect Vision Changes Some loss of visual
When Eyes Show Their Age A guide to preserving the gift of sight for as long as possible with the compliments of Division of Health Services Diocese of Camden Expect Vision Changes Some loss of visual
Ophthamology Directorate. Eye Injection for Macular Disorders Information for Patients
 Ophthamology Directorate Eye Injection for Macular Disorders Information for Patients As discussed at your appointment today, please call the Medical Retinal Services Coordinator as soon as possible (within
Ophthamology Directorate Eye Injection for Macular Disorders Information for Patients As discussed at your appointment today, please call the Medical Retinal Services Coordinator as soon as possible (within
As with most body systems, there are vision changes that will occur for most of use these are typical or expected changes.
 1 As with most body systems, there are vision changes that will occur for most of use these are typical or expected changes. 2 Few parts to mention Pupil Lens 3 Question How do your eyes change with age?
1 As with most body systems, there are vision changes that will occur for most of use these are typical or expected changes. 2 Few parts to mention Pupil Lens 3 Question How do your eyes change with age?
Ophthalmology. Caring For Your Eyes. Jurong Medical Centre
 Ophthalmology Caring For Your Eyes Jurong Medical Centre Your eyes and you At Jurong Medical Centre, we have a dedicated team of ophthalmologists that specialise in treating a wide range of acute and chronic
Ophthalmology Caring For Your Eyes Jurong Medical Centre Your eyes and you At Jurong Medical Centre, we have a dedicated team of ophthalmologists that specialise in treating a wide range of acute and chronic
RPE65-associated Leber Congenital Amaurosis
 RPE65-associated Leber Congenital Amaurosis Brian Privett, MD, Edwin M. Stone, MD, PhD February 16, 2010 Chief Complaint: Poor fixation at 4 months of age History of Present Illness: This 7 year old female
RPE65-associated Leber Congenital Amaurosis Brian Privett, MD, Edwin M. Stone, MD, PhD February 16, 2010 Chief Complaint: Poor fixation at 4 months of age History of Present Illness: This 7 year old female
The Argus II Retinal Prosthesis System: Clinical Trials and Real World Experience
 The Argus II Retinal Prosthesis System: Clinical Trials and Real World Experience Usher Syndrome Coalition Conference Call November 20, 2014 Lisa C. Olmos de Koo, M.D., M.B.A. Mark Humayun, M.D., Ph.D.
The Argus II Retinal Prosthesis System: Clinical Trials and Real World Experience Usher Syndrome Coalition Conference Call November 20, 2014 Lisa C. Olmos de Koo, M.D., M.B.A. Mark Humayun, M.D., Ph.D.
Vitrectomy for diabetic vitreous haemorrhage
 Vitrectomy for diabetic vitreous haemorrhage Why have I been given this leaflet? If you have been given this leaflet it is likely that you have been asked to think about whether you want to go ahead with
Vitrectomy for diabetic vitreous haemorrhage Why have I been given this leaflet? If you have been given this leaflet it is likely that you have been asked to think about whether you want to go ahead with
Chapter 42 1/8/2018. Key Terms. Hearing & Vision. Cerumen Deafness Hearing loss Tinnitus Vertigo
 Chapter 42 Hearing, Speech, & Vision Problems Key Terms Cerumen Deafness Hearing loss Tinnitus Vertigo Hearing & Vision Sight and hearing allow communication, learning, and moving about. Important for
Chapter 42 Hearing, Speech, & Vision Problems Key Terms Cerumen Deafness Hearing loss Tinnitus Vertigo Hearing & Vision Sight and hearing allow communication, learning, and moving about. Important for
Ophthalmology. Glaucoma
 Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
3/14/2016. Fact. Nutrition for Your Eyes. Eyes are highly metabolic organs. Deep Green Vegetables & Bright Fruits. Lutein.
 Fact Good nutrition is essential for eye health Nutrition for Your Eyes Deborah Willcox, RD, LMNT Eyes are highly metabolic organs Deep Green Vegetables & Bright Fruits This means our eyes require a lot
Fact Good nutrition is essential for eye health Nutrition for Your Eyes Deborah Willcox, RD, LMNT Eyes are highly metabolic organs Deep Green Vegetables & Bright Fruits This means our eyes require a lot
Cataracts are a normal feature of aging. About half of adults aged 65 to 74 have cataracts.
 Cataract Mr Constable specialises in modern small incision phacoemulsification surgery for the treatment of cataracts using the latest microincision systems and implants. Most patients with cataracts can
Cataract Mr Constable specialises in modern small incision phacoemulsification surgery for the treatment of cataracts using the latest microincision systems and implants. Most patients with cataracts can
Macular hole. Information for patients Ophthalmology (Vitreal Retina) Large Print
 Macular hole Information for patients Ophthalmology (Vitreal Retina) Large Print page 2 of 16 What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film
Macular hole Information for patients Ophthalmology (Vitreal Retina) Large Print page 2 of 16 What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film
Factor XIII deficiency
 Factor XIII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XIII deficiency is a type of clotting disorder. A specific protein is missing from
Factor XIII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XIII deficiency is a type of clotting disorder. A specific protein is missing from
Diabetic Retinopathy. What should know
 Diabetic Retinopathy What should know Diabetic Retinopathy: What you should know This booklet is for people with diabetic retinopathy and their families and friends. It provides information about diabetic
Diabetic Retinopathy What should know Diabetic Retinopathy: What you should know This booklet is for people with diabetic retinopathy and their families and friends. It provides information about diabetic
INDEX. Genetics. French poodle progressive rod-cone degeneration,
 INDEX Acuity in Stargardt's macular dystrophy, 25-34 ADRP (Autosomal dominant retinitis pigmentosa), see Retinitis pigmentosa and Genetics afgf, 294, 296 Age-related maculopathy, see Macular degeneration
INDEX Acuity in Stargardt's macular dystrophy, 25-34 ADRP (Autosomal dominant retinitis pigmentosa), see Retinitis pigmentosa and Genetics afgf, 294, 296 Age-related maculopathy, see Macular degeneration
Cataract Surgery. This reference summary will help you understand what cataracts are and how they can be treated surgically.
 Cataract Surgery Introduction A cataract is a clouding of the eye s lens. Cataracts are a common eye condition that affect many people aged 65 or older. Your doctor may recommend cataract surgery to enhance
Cataract Surgery Introduction A cataract is a clouding of the eye s lens. Cataracts are a common eye condition that affect many people aged 65 or older. Your doctor may recommend cataract surgery to enhance
Understanding Cataracts
 Understanding Cataracts For more information, please contact T 0116 249 8839 E info@vistablind.org.uk W www.vistablind.org.uk 2 Contents 3 About cataracts 4 How your eye works 5 Causes 7 Symptoms 9 Treatment
Understanding Cataracts For more information, please contact T 0116 249 8839 E info@vistablind.org.uk W www.vistablind.org.uk 2 Contents 3 About cataracts 4 How your eye works 5 Causes 7 Symptoms 9 Treatment
