Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives
|
|
|
- Sharyl Wilkins
- 5 years ago
- Views:
Transcription
1 Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives
2 page 2
3 This booklet has been written to provide information about the surgical procedures that are commonly performed for pancreatic disorders. These procedures are used in the management of several conditions involving the pancreas, such as benign pancreatic growths, pancreatic cancers, and pancreatitis (acute or chronic). Much of the information in this booklet is about surgery for pancreatic cancers. The majority of surgical procedures performed on the pancreas will involve resection (removal) of the portion that is affected. The type of surgical operation for pancreatic tumours depends on the location of the tumour in the pancreas and on the type of the tumour. page 3
4 What is the pancreas? The pancreas is a gland that lies at the back of the upper abdomen, behind the stomach. It is shaped like a tadpole; the rounded head lies attached to the duodenum (a part of the intestine that forms the outlet of the stomach), while the body and tail extend across to the left side. The pancreas produces digestive juices and aids digestion of food. Pancreatic juice and bile mix with food in the intestine and help digestion. The pancreas also produces insulin, which controls the level of sugar in the blood. Lack of insulin causes diabetes. The pancreas and its location in the body Pancreas page 4
5 Types of operations The operation to remove the head of the pancreas is called pancreaticoduodenectomy. There are two types of pancreaticoduodenectomy: the Whipple s procedure and the pylorus preserving pancreaticoduodenectomy (PPPD). Your surgeon will decide on whether to carry out a Whipple s or PPPD operation, depending on the type of tumour that you have and what is seen during your operation. Whipple s procedure In the Whipple s operation the head of the pancreas, lower quarter of the stomach, common bile duct, gallbladder, duodenum (first part of the intestines) and surrounding lymph nodes are removed. The remaining pancreas, bile duct and stomach are then rejoined to the small intestine (jejunum). This allows pancreatic juice, bile and food to flow back into the small intestine, so that digestion can carry on as normal. The operation normally takes 4-7 hours. Reconstruction following a classical Whipple s procedure page 5
6 Pylorus-preserving pancreaticoduodenectomy (PPPD) The PPPD is a variation of the original Whipple s operation, but the lower end of the stomach is not removed. This leaves the valve (pylorus) which controls the flow of food from the stomach. It is otherwise a very similar procedure with similar risks. 1 page 6
7 Distal pancreatectomy If the problem is in the tail of the pancreas, your surgeon will recommend an operation called distal pancreatectomy (removal of the tail of the pancreas). Quite often this operation may also require removal of your spleen. This operation can often be carried out laparoscopically, through small holes in your abdomen (keyhole surgery), and this may be offered to you. Distal pancreatectomy page 7
8 Splenectomy Splenectomy is removal of the spleen. The spleen helps the body s defense against some infections. Without a spleen your immunity to those bacteria is reduced. If it is likely we will need to remove your spleen during surgery we will write to your GP to ask for you to have specific vaccinations beforehand, to protect you from the following bacteria. You will be given the following vaccinations: Streptococcus pneumoniae, Haemophilus influenzae type B and Neisseria meningitidis. In addition, you will need to take an antibiotic every day (usually penicillin) on a long term basis, to help prevent infection. Total pancreatectomy This operation involves the removal of the whole pancreas. It is essentially a combination of the pancreaticoduodenectomy and the distal pancreatectomy. You will become permanently diabetic following removal of the whole pancreas, as the pancreas is where the insulin for your body is produced. You will need to take insulin for the rest of your life. You will be given more information about being diabetic and will need on-going support from a diabetes nurse. This will usually be at your GP s surgery or you may be followed up by the diabetes specialist at your local hospital. In some cases, people who were expected to have a Whipple s procedure will need to have a total pancreatectomy. This is occasionally necessary if the tumour is more extensive than expected. page 8
9 Bypass procedure If your surgery is for suspected cancer, during the surgery your surgeon may find that it is not possible or advisable to remove the growth. Such a situation arises in 7 to 10 cases in 100 (7-10%). This may be because the tumour has spread to another location, like the liver. It could also be because the tumour has grown beyond the pancreas and become fixed to important blood vessels close by. In these circumstances your surgeon will not remove the tumour and may carry out a bypass procedure, to improve symptoms and prevent blockage of the bile duct or stomach in the future. This is done with a y shaped bowel reconstruction called a Roux en Y bypass. Roux en Y bypass procedure Duodenum Jejunal anastomosis (join) so gastric juices can enter the small intestine, to aid digestion page 9
10 What are the benefits of surgery? Without surgery, the average survival of people with pancreatic cancer is less than one year, and very few survive more than 2 years. The operation aims to completely remove the cancerous growth, and give the best chance of curing the problem. The chance of the cancer recurring depends on the type of tumour that you have. A successful operation can increase your chance of being cured to between 10-50%. This will only be accurately known after the operation, when the pathologist examines the removed pancreas. Your surgeon will receive the full pathology report 2-3 weeks after surgery. If you are having surgery for another condition, we will talk with you about the potential benefits. What alternative treatments are available? If you have cancer, chemotherapy may be able to shrink the cancer or delay its growth. If the cancerous tumour has not spread, but cannot be removed surgically because it is extending to nearby structures, then you may be recommended a combination of chemotherapy and radiotherapy. However, without surgery it is unlikely we will be able to cure this problem. If you do not have cancer, it is unlikely there will be any alternative treatments. page 10
11 What anaesthetic will I have? Our usual anaesthetic technique for pancreatic surgery is a combination of general and epidural anaesthesia. You are put completely to sleep, and a tube is put into your windpipe, so it is not uncommon to get a sore throat after the operation. You are likely to have several tubes attached to you after your surgery. These will include a narrow tube, called a catheter, for giving pain medication infusions into your back (epidural) or into your wound (local anaesthetic infusion). These tubes will stay in place for 3-5 days. They are very fine, so you will be able to lie on your back and sit and walk comfortably. This type of pain relief is very safe and helps you to breathe deeply. The risk of any permanent nerve damage is very rare, less than 1 in 10,000. After the operation, we will give you a PCEA (patient-controlled epidural analgesia) button to control the amount of painkiller that you get through the cannula. The pump is designed to prevent an overdose, so for a few minutes after you have pressed the button it will not deliver another dose. The team at the pre-assessment clinic can guide you and help with any questions that you have. They will also discuss with you our Enhanced Recovery After Surgery programme, known as ERAS, which can help you make a safe steady recovery as quickly as possible. It is known that starting to move around soon after surgery reduces the risk of complications. You will also have a chance to meet the anaesthetist on the day of the operation to ask them any questions you might have. You may need to be monitored in the Intensive Care Unit (ICU) after surgery, but most people will be transferred to the Churchill Overnight Recovery Unit (CORU) after the operation is complete. page 11
12 What are the risks and possible complications? Pancreatic operations are major procedures, with associated risks and complications. Nowadays, the operation has become much safer. This is mainly as a result of pancreatic surgery being carried out by a smaller number of surgeons, who have more experience in this type of surgery. At Oxford, over 70 pancreatic resections are performed annually, with less than 2.5% risk of death. If you have other medical problems, your risks may be higher than average. Complications following pancreatic surgery occur in in 100 patients, but the team at Oxford is experienced in managing these complications. Possible complications include: those related to general anaesthesia and the epidural chest infection and problems with breathing bleeding, which may result in blood transfusion wound infection blood clots forming in the legs anastomotic leak (1 in 10 patients): After the tumour is removed, the cut ends of the pancreas, bile duct and stomach are sewn to the intestine. Pancreatic juice or bile can leak into the abdomen (space around the organs). Your surgeon will leave a drain tube in your abdomen to remove any leaked pancreatic fluid. Most anastomotic leaks will heal on their own, but you will need longer to recover. If it does not stop leaking, you will need a further operation, and the entire pancreas may then need to be removed. delayed emptying of the stomach (1 in 10 patients): After the surgery, you will not be allowed to eat until your bowel function has returned. This usually takes 2-3 days. Sometimes the stomach may take longer to recover after surgery. During this time, you may need to receive nutrition through a feeding tube or intravenously (into a vein) for several weeks. page 12
13 delayed bleeding (2 to 5 in 10 patients): If there is an anastomotic leak, the fluid that leaks out can cause erosion of nearby blood vessels. This can cause internal bleeding, around 6-7 days after surgery. This is usually while you are still in hospital and would show as blood in your stool or vomiting blood, which may look like coffee grounds. This bleeding is usually treated using either tiny metal coils or foam to stop the bleeding. Very rarely, a second surgery is needed. What are long-term consequences of the operation? Malabsorption: The pancreas produces enzymes which help digest food. Removal of part of the pancreas decreases production of these enzymes. This can result in poor digestion of food, causing loose stools which are greasy and pale. You will need long-term treatment with pancreatic enzyme capsules and will be prescribed Creon capsules to be taken just before food. The usual dose is one capsule (25,000 units) with snacks and two capsules (50,000 units) with meals. You can vary the dose of enzyme that you take from one day to the next, depending on your diet. Foods that contain a large amount of fat will need more Creon. The dose of Creon can be increased if your stools remain loose and greasy. The enzyme is sourced from porcine (pork) products. Unfortunately there is currently no alternative to this, so please discuss this with the dietitian or doctor if you have any concerns. You will meet a dietitian on the ward, who will advise you on how to take the Creon capsules. Please see our information booklet A guide to eating and pancreatic enzyme supplements for more details. page 13
14 Loss of weight: It is normal to lose weight both before and after surgery. We would expect you to start regaining some of the lost weight 2-3 months after surgery. Alteration in diet: Though there are no specific restrictions to what you can eat, you may find your physical ability to eat is restricted. You may need to have small meals and snack between meals to minimise symptoms of bloating or discomfort. It will take several months for your ability to eat to return to normal. Diabetes: The pancreas produces insulin, which controls blood glucose. If you were not diabetic before your surgery, you are unlikely to develop diabetes after having half your pancreas removed. If you are already diabetic before your surgery, you are likely to need additional diabetic medication or insulin after surgery. Your blood glucose will be monitored very closely before you go home. Hernia: It is possible to develop a type of hernia called an incisional hernia after abdominal surgery. This is because of a weakness being created in the wall of the abdominal muscles, allowing a section of bowel to bulge through. This can usually be treated with an abdominal support bandage, but occasionally surgery may be required. page 14
15 How do I prepare for surgery? If you smoke, try to stop as soon as possible, to reduce the risk of any breathing problems during and after the operation. We will give you advice before surgery to help you prepare physically for the operation and optimise your level of fitness. You will also need to plan for any additional help you may need at home whilst recovering, particularly if you live alone. Please let us know about this in advance and we will do what we can to support you. You will be asked to come to the pre-assessment clinic at the Churchill Hospital before the operation. Please bring a list of your medication with you to the hospital. During this appointment our team will give you further instructions and explain what you can expect during your admission to hospital. What happens after the operation? After spending some time in the anaesthetic recovery area of the operating suite, you will be taken to either the ICU or CORU (recovery ward). If you are spending the first night on CORU you will usually be transferred back to the ward the next day. The nursing staff will monitor your progress and give you painkillers. You will be on intravenous drips to give you fluids and certain drugs and you will not be allowed to eat full meals for the first few days. After 2 days you should be able to try some soft foods. You will have a urine catheter in your bladder, a tube in your nose going to your stomach, and a tube coming from your abdomen (abdominal drain). After 3-5 days these tubes are usually removed, if we are confident you are making a good recovery and there is no evidence of internal leakage. It is important that we help you get out of bed and move about as soon as possible. Our physiotherapist will assist you with breathing exercises, which are important in order to prevent a chest infection. page 15
16 How long will I be in hospital after the operation? You are likely to be are able to go home 7-10 days after the operation, if there have been no complications. The ward nurses will give you painkillers to take at home as needed, and a follow-up appointment will be made for you in the surgical outpatient clinic. You will also be prescribed a course of injections to take home with you to take for once a day for a month, to thin your blood and reduce the risk of blood clots forming in your leg veins. We will show you how to this before you go home. When can I return to normal activities? On your return home, you will find movements and activity difficult for the first few weeks. You may also feel low in mood, but this will soon get better. It is important to keep as active as possible, but also to rest. You will need 2-3 months to return to normal activities. There are usually no restrictions on activities after that time, but please do discuss with us if you feel a particular problem is not settling. page 16
17 Will I need any further treatment or follow up? In some cases, the survival rate for people with pancreatic cancer can be improved by having chemotherapy. We will discuss the option of having chemotherapy with you and we will usually refer you to the oncologist, a cancer chemotherapy specialist, at your local hospital. You are likely to need continued monitoring for a few years, to check for any recurrence of cancer. We do not carry out routine scans, but will do if there is any evidence of a problem. Your check-ups may be shared between the surgeons at Oxford and your oncologist at your local hospital, so that the need for trips to Oxford is minimised. When should I call my doctor after surgery? Call your doctor if you: develop a fever (high temperature) notice your scar has become red and painful, or has a smelly discharge develop an unusual degree of pain develop nausea, vomiting or diarrhoea, or cannot eat properly become jaundiced (yellow eyes, dark urine). page 17
18 For further information Macmillan Cancer Support Website: Tel: Pancreatic Cancer UK Website: Tel: Maggie s Cancer Centre (Churchill Hospital, Oxford) Website: Tel: page 18
19 Useful contact numbers Hospital Switchboard: HPB (Hepatobiliary and Pancreatic) Unit Secretary: Specialist Cancer Nurses: or call the Hospital Switchboard and ask for bleep 1386/1891 Pre-assessment clinic Churchill Hospital: Churchill Overnight Recovery Unit (CORU): Oxford Upper GI Ward Churchill Hospital: Intensive Care Unit (ICU) Churchill Hospital: page 19
20 If you need an interpreter or would like this information leaflet in another format, such as Easy Read, large print, Braille, audio, electronically or another language, please speak to the department where you are being seen. You will find their contact details on your appointment letter. Clinical Nurse Specialist: Sue Wilner Consultant Hepatobiliary and Pancreatic Surgeons: Mr Michael Silva Mr Zahir Soonawalla Medical Illustrations by Julian King (Artist) December 2018 Review: December 2021 Oxford University Hospitals NHS Trust OMI 43171P
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon
 Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER
 INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
THE WHIPPLE PROCEDURE
 THE WHIPPLE PROCEDURE Patient Information AMEND Association for Multiple Endocrine Neoplasia Disorders Registered Charity No. 1099796 MEN SUPPORT Tel: 01892 516076 Email: info@amend.org.uk Membership is
THE WHIPPLE PROCEDURE Patient Information AMEND Association for Multiple Endocrine Neoplasia Disorders Registered Charity No. 1099796 MEN SUPPORT Tel: 01892 516076 Email: info@amend.org.uk Membership is
Distal pancreatectomy for pancreatic cancer. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Distal pancreatectomy for pancreatic cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Distal pancreatectomy for pancreatic cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Laparoscopic colon resection for colon cancer
 Laparoscopic colon resection for colon cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Laparoscopic colon resection for colon cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
The Whipple s procedure. Information for patients, families and carers
 Information for patients, families and carers Contents About your operation page 3 Before your operation page 9 On the day of your operation page 12 After your operation page 13 After you leave hospital
Information for patients, families and carers Contents About your operation page 3 Before your operation page 9 On the day of your operation page 12 After your operation page 13 After you leave hospital
University College Hospital. Subtotal and Total Gastrectomy. Gastrointestinal Services Division
 University College Hospital Subtotal and Total Gastrectomy Gastrointestinal Services Division If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
University College Hospital Subtotal and Total Gastrectomy Gastrointestinal Services Division If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
Treatment for early pancreatic cancer
 13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
To help you understand your operation, it is helpful to have a basic knowledge of how the body works (see Figure 1).
 Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Pancreatic Cancer (1 of 5)
 i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
Cholecystectomy (removal of the gallbladder) Patient Information
 Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
The Children s Hospital Intussusception and its treatment Information for parents
 The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
The Whipple (pancreatic and duodenal surgery)
 The Whipple (pancreatic and duodenal surgery) A guide for patients 1 Contents Introduction... 4 What is Whipple surgery?... 5 Pancreas... 7 Gallbladder... 7 Common bile duct... 7 Duodenum... 7 Lymph nodes...
The Whipple (pancreatic and duodenal surgery) A guide for patients 1 Contents Introduction... 4 What is Whipple surgery?... 5 Pancreas... 7 Gallbladder... 7 Common bile duct... 7 Duodenum... 7 Lymph nodes...
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Haematology and Surgery Departments Splenectomy
 Haematology and Surgery Departments Splenectomy This information sheet describes surgery for removal of the spleen (splenectomy) and what to expect before and after the operation. An operation to remove
Haematology and Surgery Departments Splenectomy This information sheet describes surgery for removal of the spleen (splenectomy) and what to expect before and after the operation. An operation to remove
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
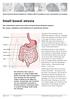 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Radical removal of the kidney (radical nephrectomy): procedure-specific information
 PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
The Children s Hospital, Tom s Ward. Hirschsprung Disease. Information for parents
 The Children s Hospital, Tom s Ward Hirschsprung Disease Information for parents What is Hirschsprung disease? Hirschsprung disease is a rare disorder of the bowels, most commonly the large bowel (colon).
The Children s Hospital, Tom s Ward Hirschsprung Disease Information for parents What is Hirschsprung disease? Hirschsprung disease is a rare disorder of the bowels, most commonly the large bowel (colon).
The Leeds Teaching Hospitals NHS Trust Adrenalectomy
 n The Leeds Teaching Hospitals NHS Trust Adrenalectomy Information for patients This leaflet provides information on having an adrenalectomy, reasons for the procedure and alternatives to surgery, along
n The Leeds Teaching Hospitals NHS Trust Adrenalectomy Information for patients This leaflet provides information on having an adrenalectomy, reasons for the procedure and alternatives to surgery, along
X-Plain Pancreatic Cancer Reference Summary
 X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
The organs and tissues of the body are made up of tiny building blocks called cells. Cancer is a disease of these cells.
 Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Informed Consent Gastrectomy
 Informed Consent Gastrectomy Department of Surgery, Nagasaki University Graduate School of Biomedical Sciences Important things you need to know Patient choice is an important part of your care. You have
Informed Consent Gastrectomy Department of Surgery, Nagasaki University Graduate School of Biomedical Sciences Important things you need to know Patient choice is an important part of your care. You have
Laparoscopic cholecystectomyy
 Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
Having a pancreas transplant alone (PTA)
 Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Laparotomy for large retroperitoneal mass:
 Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
Acute pancreatitis. Information for patients Hepatobiliary
 Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
ABDOMINAL PERINEAL RESECTION
 ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
LAPAROSCOPIC RADICAL REMOVAL OF THE KIDNEY INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts
 Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Abdominal surgery for Crohn's disease. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Partial Removal of the Kidney
 Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact Ward 4A, 4B or
Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact Ward 4A, 4B or
Appendectomy. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Appendectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Appendectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Epidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal
 Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Gall bladder cancer. Information for patients Hepatobiliary
 Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Open Radical Removal of the Kidney
 Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Retroperineal Lymph Node Dissection (RPLND)
 Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Pelvic exenteration. Information for patients and their families/carers
 Pelvic exenteration Information for patients and their families/carers Your doctor has recommended that you have an operation to remove your rectum, bladder and (if you are male) possibly your prostate.
Pelvic exenteration Information for patients and their families/carers Your doctor has recommended that you have an operation to remove your rectum, bladder and (if you are male) possibly your prostate.
Roboticassisted. laparoscopic nephrectomy
 Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Surgery. In this fact sheet. Surgery: English
 Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP. Patient Information
 ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon
 Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
University Hospitals Bristol NHS Foundation Trust NHS. Catheterisation using a Mitrofanoff
 University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Northumbria Healthcare NHS Foundation Trust. Laparoscopic Cholecystectomy. Issued by the Department of Upper Gastrointestinal Surgery
 Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Open repair of Abdominal Aortic Aneurysms (AAA)
 Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Surgery to remove the spleen (elective splenectomy)
 Surgery to remove the spleen (elective splenectomy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Surgery to remove the spleen (elective splenectomy) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Laparoscopic excision of a gastric gist. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Laparoscopic excision of a gastric gist Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Laparoscopic excision of a gastric gist Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Colon Cancer Surgery
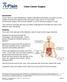 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Anti-reflux surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Anti-reflux surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Anti-reflux surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
This operation is necessary to remove the area of bowel that is diseased.
 PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
Undescended testes. Information for parents and carers
 Undescended testes Information for parents and carers The testes (or testicles) start developing high inside the tummy near the kidneys. At about 2 months before a boy is born they move down or descend
Undescended testes Information for parents and carers The testes (or testicles) start developing high inside the tummy near the kidneys. At about 2 months before a boy is born they move down or descend
Treatment for cancer of the gall bladder
 Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Further information You can get more information and share your experience at
 UG13 Elective Splenectomy Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from:......... Taunton and
UG13 Elective Splenectomy Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from:......... Taunton and
MB03 Laparoscopic Gastric Bypass
 Suite 1 Level 5, 123 Nerang Street, Southport Qld 4215 MB03 Laparoscopic Gastric Bypass Expires end of January 2019 Write questions or notes here: Further Information and Feedback: Tell us how useful you
Suite 1 Level 5, 123 Nerang Street, Southport Qld 4215 MB03 Laparoscopic Gastric Bypass Expires end of January 2019 Write questions or notes here: Further Information and Feedback: Tell us how useful you
B02 Mastectomy. Expires end of November Write questions or notes here:
 Practice Locations: St John of God Consulting Suites, 117 Anstruther Road, Mandurah Suite 50, Murdoch Medical Centre, 100 Murdoch Drive, Murdoch Tel: 08 6333 2800 Web: saudhamza.com.au B02 Mastectomy Expires
Practice Locations: St John of God Consulting Suites, 117 Anstruther Road, Mandurah Suite 50, Murdoch Medical Centre, 100 Murdoch Drive, Murdoch Tel: 08 6333 2800 Web: saudhamza.com.au B02 Mastectomy Expires
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Anterior Resection. Your Operation Explained. Delivering the best in care. UHB is a no smoking Trust
 Anterior Resection Your Operation Explained Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Anterior Resection Your Operation Explained Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Epidurals for pain relief after surgery Information for patients
 Epidurals for pain relief after surgery Information for patients Department of anaesthesia and pain medicine Epidurals for pain relief after surgery This information sheet explains what to expect when
Epidurals for pain relief after surgery Information for patients Department of anaesthesia and pain medicine Epidurals for pain relief after surgery This information sheet explains what to expect when
Head and neck cancer - patient information guide
 Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Information leaflet for parents/carers. Fundoplication
 Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
MB04 Laparoscopic Sleeve Gastrectomy
 Suite 1 Level 5, 123 Nerang Street, Southport Qld 4215 MB04 Laparoscopic Sleeve Gastrectomy Expires end of January 2019 Write questions or notes here: Further Information and Feedback: Tell us how useful
Suite 1 Level 5, 123 Nerang Street, Southport Qld 4215 MB04 Laparoscopic Sleeve Gastrectomy Expires end of January 2019 Write questions or notes here: Further Information and Feedback: Tell us how useful
PERCUTANEOUS NEPHROLITHOTOMY
 PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Open Incisional Hernia Repair
 www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
www.mogodaysurgery.com.au Mr. Sanjay Singh MBBS, MS, FRACS, FRCS (UK) Consultant Surgeon 2-4 Charles Street MOGO NSW 2536 Tel: 02 4474 3774 Fax: 02 4474 3775 Write questions or notes here: Open Incisional
Patient information. Breast Reconstruction using an Expander and Implant Breast Services Directorate PIF 110 V5
 Patient information Breast Reconstruction using an Expander and Implant Breast Services Directorate PIF 110 V5 You are going to have a breast reconstruction using an expander followed by an implant. This
Patient information Breast Reconstruction using an Expander and Implant Breast Services Directorate PIF 110 V5 You are going to have a breast reconstruction using an expander followed by an implant. This
Quick Facts about Ampullary Cancer
 Quick Facts about Ampullary Cancer What is the Ampulla of Vater? Princess Margaret The liver, gallbladder and pancreas produce important fluids to help you digest food. These fluids are carried through
Quick Facts about Ampullary Cancer What is the Ampulla of Vater? Princess Margaret The liver, gallbladder and pancreas produce important fluids to help you digest food. These fluids are carried through
Gastro-Oesophageal Reflux Disease Information Sheet
 Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
Patient & Family Guide. Bowel Surgery.
 Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Oesophageal, gastric and duodenal stents
 Oesophageal, gastric and duodenal stents Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Oesophageal, gastric and duodenal stents Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Information about liver tumours and surgery. - a guide for patients and relatives
 Information about liver tumours and surgery - a guide for patients and relatives About the liver The liver is a large organ, which lies in the upper part of the abdominal cavity, directly below the diaphragm.
Information about liver tumours and surgery - a guide for patients and relatives About the liver The liver is a large organ, which lies in the upper part of the abdominal cavity, directly below the diaphragm.
CONSENT FORM FOR ESOPHAGECTOMY. have and that this
 Page 1 of 11 CONSENT FORM FOR ESOPHAGECTOMY PROPOSED TREATMENT The doctor has explained that I, (name).., have and that this condition requires. About oesophagectomy You have been advised to have surgery
Page 1 of 11 CONSENT FORM FOR ESOPHAGECTOMY PROPOSED TREATMENT The doctor has explained that I, (name).., have and that this condition requires. About oesophagectomy You have been advised to have surgery
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
