Medicare Star Ratings and the Shift to Quality- Based Payment Models. David Nau, RPh, PhD, FAPhA PQS President
|
|
|
- Maria Terry
- 6 years ago
- Views:
Transcription
1 Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President
2 The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based purchasing or value-driven healthcare Value is the balance of quality and costs, thus we can optimize value by improving quality while reducing costs One of the biggest challenges in driving better quality is that we can t always agree on how to define and measure quality PQA takes the lead on development of medication-related quality measures for evaluation of health plans, PBMs and pharmacies, and EQuIPP allows pharmacies to track their performance on quality metrics
3 Medicare Star Ratings Annual ratings of Medicare plans that are made available on Medicare Plan Finder and CMS website Ratings are displayed as 1 to 5 stars Stars are calculated for each measure, as well as each domain, summary, and overall (applies to MA-PDs) level Two-year lag between year of service and reporting year for PQA measures in Star Ratings (e.g., 2013 drug claims for 2015 Ratings) Star Ratings were released in October 2014 to inform beneficiaries who were enrolling for 2015
4 Part D Stars Medicare drug plans receive a summary rating on quality as well as four domain, and individual measure, scores (13 individual measures) Five measures are from PQA: - 2 measures of medication safety >High risk medications in the elderly >Appropriate treatment of blood pressure in persons with diabetes - 3 measures of medication adherence >Oral diabetes medications >Cholesterol medication (statins) >Blood pressure (renin-angiotensin system antagonists) Due to the higher weighting of clinically-relevant measures, the PQA measures account for 50% of Part D summary ratings for 2015
5 2015 Medicare Part D: Display Measures Display measures are not a part of the Star Ratings, but are used to provide benchmarks and feedback to plans CMS also monitors display measures to assess plan performance; poor performance can lead to compliance actions by CMS Display measures (from PQA): Drug-Drug Interactions Excessive doses of oral diabetes medications Comprehensive Medication Review (CMR) Completion Rate HIV antiretroviral medication adherence (only in safety reports) New Display measure (NOT from PQA) Use of atypical antipsychotics
6 *New* Star Ratings Measure for 2016 Medication Therapy Management Program Completion Rate for Comprehensive Medication Reviews (Part D Measure). Highlights: - PQA-endorsed measure - Measures the percentage of beneficiaries who met eligibility criteria for the MTM program and who received a CMR with a written summary in the CMS standardized format score will be based on 2014 measurement period - This measure will be assigned a weight of 1 - For complete measure details, please see the PQA measure listing on the website
7 2017 and Beyond Potential new measures: Statin Therapy in Diabetes - As of November 21, 2014, PQA has endorsed Statin Use in Persons with Diabetes measure. CMS stated that if the measure is endorsed by PQA in 2014, the measure would be considered as a new 2017 Display Measure and a 2018 Star Rating. Asthma Measure Suite - NCQA is currently testing three asthma measures, all for members 5-64 years of age. The three measures are: > Use of Appropriate Medications for People with Asthma > Medication Management for People with Asthma > Asthma Medication Ratio Opioid Overutilization - PQA is currently developing 3 measures evaluating multi-provider, high dosage opioid use among individuals 18 years and older without cancer and excluding hospice
8 Part D Stars Table G-2: Part D Measure Weights Measure ID Measure Name Part D Summary MA-PD Overall D01 Appeals Auto-Forward D02 Appeals Upheld D03 Complaints about the Drug Plan D04 Members Choosing to Leave the Plan D05 Drug Plan Quality Improvement 5 5 D06 Rating of Drug Plan D07 Getting Needed Prescription Drugs D08 MPF Price Accuracy 1 1 D09 High Risk Medication 3 3 D10 Diabetes Treatment 3 3 D11 Medication Adherence for Diabetes Medications 3 3 D12 Medication Adherence for Hypertension (RAS antagonists) 3 3 D13 Medication Adherence for Cholesterol (Statins) 3 3 From CMS 2015 Star Ratings Technical Notes
9 Part D Star Thresholds Change
10 Improvement in Adherence Rates Part D Measure MA-PD PDP PDC - Diabetes 73.0% 73.7% 75 % 77 % 74.4% 75.8% 77 % 79 % PDC - Hypertension 72.2% 73.9% 76 % 78 % 74.3% 76.8% 78 % 81 % PDC - Cholesterol 68.0% 69.0% 71 % 74 % 69.1% 71.0% 73 % 77 % Average across all contracts for each year
11 High Stakes for Part D Stars Enrollment Implications Quality Bonus Payments (MA-PD) Poor performers identified by CMS - Low-performer icon Removal from Medicare for continued poor overall performance (< 3 stars for 3 years in a row) - For 2014, CMS chose not to execute its authority to terminate poor-performing plans since these plans were showing signs of improvement - Still maintains this authority in future years
12 How are MA-PD plans responding? Formularies, clinical strategies, network contracts, marketing/promotions, aligning with star measures Significant investments in drive to 5 Contract strategies for pharmacy networks Pay for Performance (P4P) pharmacies may be eligible for bonus payment based on star performance Preferred pharmacies based partly on star performance
13 Pharmacy Pay-for-Performance Programs Using EQuIPP Inland Empire Health Plan (IEHP) - Launched in October 2013 based on Star measures plus asthma and GDR - Pharmacies will receive bonus depending on their performance on each measure: > 3-star attainment = small bonus > 5-star attainment = large bonus Caremark-SilverScript - Ongoing program in 2014 based on PDC-adherence and ACE/ARB in Diabetes measures - Combination of payment for gap closures delivered through Mirixa and bonus on reaching performance goals as measured by EQuIPP Healthfirst of NY - Program launching October 2014 based on PDC-adherence measures - Combination of payment for program commitment and for reaching performance goals as measured by EQuIPP
14 Pharmacy Quality Ratings PQA, PQS and the University of Arizona are exploring whether an Overall Rating of a pharmacy can be created from the individual PQA measures in way that is scientifically valid as well as efficient Project is funded by the Community Pharmacy Foundation Stakeholder input and consumer input are being solicited EQuIPP data will be used to pilot-test various models for the ratings Many issues will need to be addressed to determine how this rating system would be appropriately implemented. Stay tuned
15 Partnering for Quality How does your pharmacy use quality metrics today? What information do you need to help with conversations about quality of medication use with both physicians, patients, AND your pharmacists? Is your pharmacy positioned to play a role in moving quality forward? Is your pharmacy positioned to participate in qualitybased preferred networks?
16 EQuIPP Performance Measurement and Assessment for Pharmacy & Health Plans Pharmacy Health Plans How do we compare vs. peers? How do we compare vs. state? How can we compete to participate in value based, shared risk or tiered networks? How is my network performing? How do we compare as a plan? How can we create networks to properly share value based on high performance? Overview PQS is a Joint Venture (for profit) between CECity and Pharmacy Quality Alliance (non profit), trusted licensor of medication use quality measures CECity platform leveraged to present unbiased performance at provider, organization, state, national and payor network level Includes core measures that matter Medicare Stars (Part D) Major health plans and Chain Pharmacies are all in
17 Participants Existing Plans - Humana - Aetna - Coventry - Wellcare - Cigna HealthSpring - Caremark: > Silverscript > More to come in Inland Empire Health Plan (CA) - UPMC Health Plan (PA) - Gateway Health Plan (PA) - Healthfirst of NYC EQuIPP Statistics: Over 15 million lives in dataset Over 55,000 participating pharmacies New for Tenet Health Plans - BCBS of Michigan - Express Scripts > Highmark BCBS > Others TBD - Prime Therapeutics > Florida Blue > Capital Health Plan (FL) > Horizon BCBS (NJ) > BCBS Alabama > BCBS North Carolina > BCBS South Carolina > BCBS Arkansas > BCBS Minnesota > HCSC Blues plans TX, OK, MT, NM, IL
18 Store Dashboard
19 Patient Outlier Capability Outliers are patients who represent improvement opportunities Outliers can be identified from a standard EQuIPP data feed or based on supplemental file provided by clients Include a brief documentation function to allow pharmacists to track outreach - Outlier documentation can be provided to clients to help determine future interventions
20
21 Click on Medication Adherence: READ MORE
22 Click on FAQ tab
23 Tactics Check your EQuIPP scores every month (data are updated on the 15 th of each month). Identify your biggest opportunity for improvement Which measure has the biggest gap with Top 20% or State Average? Which plans have created incentives for improvement? How can you find some easy wins to start? Pick one quality measure to get started and talk with your staff about ways to impact that measure Come up with an improvement plan then orient all your staff and pick a day to start
24 Adherence Ideas Focus on Medicare patients with diabetes Many will also be on statins and ACE inhibitors Connection of adherence to outcomes is strong Implement refill synch program Start with a few high priority patients (e.g., diabetics enrolled in Medicare plans that have a P4P program) Use technology to help you scale up Screen high-priority patients to identify non-adherence risk Talk to your Medicare patients on diabetes, ACEI, or cholesterol meds Can take 10 seconds to ask if they have any concerns about: Side effects Costs Lack of effectiveness (i.e., isn t really helping me)
25 High Risk Med (HRM) Ideas Make sure that all pharmacy staff know the common HRMs - Glyburide, Zolpidem, or whatever else is common with your physicians - If you re not sure which ones are common, have a tech/intern run usage reports on some of the HRMs - Identify physicians who are top prescribers of specific HRMs Anytime an older patient (>65yo) presents a NEW prescription for a HRM, the technician should flag this script for review by RPh - Consider use of HRM Fax form within EQuIPP resources Where available, use the EQuIPP Outlier list to identify specific patients who have received an HRM Pick an easy win for your first initiative; then talk with a physician about a change in future Rxs, or conversion of existing patients - Easy win: glyburide conversion to glipizide or glimepiride; or if already on metformin, consider a combo product
26 Summary Quality metrics are driving action amongst health plans and PBMs A growing number of prescription drug plans are implementing performance-based incentives for network pharmacies, such as: - Pay-for-performance models that include bonus payments to topperforming pharmacies - Preferred networks that include star-performance as a criterion for inclusion as a preferred pharmacy EQuIPP continues to expand the number of plans and pharmacies who use this platform as a neutral intermediary for calculation of pharmacy quality scores Pharmacies need to track their quality to compete in a value-based contracting environment and will need clinical decision support tools that prompt efficient, effective action.
27 Questions?
116th Annual Convention
 116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
116th Annual Convention Date: Tuesday, October 21, 2014 Time: 8:30 am 10:00 am Location: Austin Convention Center, Room 17AB, Level 4 Title: Activity Type: Speaker: Medicare Part D Star Ratings What They
9/25/15. Pharmacy Quality Measures: Financial Support. Learning Objectives. Speaker Disclosure. Access to Preferred Networks and Clinical Performance
 Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES
 USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
USING MTM TO IMPROVE STAR RATINGS : CASE STUDIES Sept 13, 2015 Amanda Applegate, PharmD, BCACP Disclosures Nothing to disclose Learning Objectives Describe how MTM can improve star ratings Discuss strategies
Capital Health Plan CMS Star Ratings Strategies for Improvement
 Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Understanding Your Patient Care Opportunity Report (PCOR)
 Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Legislative & Regulatory Update Brad Young, RxPlus Government Affairs
 Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
Legislative & Regulatory Update 2018 Brad Young, RxPlus Government Affairs Disclosures Brad Young reports no actual or potential conflicts of interest associated with this presentation. 2 Learning Objectives
How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses
 How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses We are in a new, changing healthcare environment that is affecting every stakeholder in the market hospitals, doctors,
How Independent Pharmacies Can Use Medicare Star Ratings to Improve Their Businesses We are in a new, changing healthcare environment that is affecting every stakeholder in the market hospitals, doctors,
6/18/2015. Disclosure. Objectives. Star Ratings. Understand the current climate of healthcare reform
 Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director jgaldo@samford.edu Disclosure I do not have (nor does any immediate
Star Ratings John A. Galdo, Pharm.D., BCPS, CGP (Jake) Assistant Professor of Pharmacy Practice Community Practice Residency Director jgaldo@samford.edu Disclosure I do not have (nor does any immediate
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights
 Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
Patient-Centered Measurement: Innovation Challenge Series
 Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
PATIENT-IMPACT SCORECARD
 UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star
 Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
ACO Congress Conference Pre Session Clinical Performance Measurement
 ACO Congress Conference Pre Session Clinical Performance Measurement Lynne Rothney-Kozlak, MPH Interim VP, ACO Collaborative (Independent Consultant) October 25, 2010 Agenda for Presentation 1. The Framework
ACO Congress Conference Pre Session Clinical Performance Measurement Lynne Rothney-Kozlak, MPH Interim VP, ACO Collaborative (Independent Consultant) October 25, 2010 Agenda for Presentation 1. The Framework
Measuring and Improving Quality in Accountable Care Organizations
 Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT
 2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
Member-centered cancer care In Georgia
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Member-centered cancer care In Georgia Ira Klein, MD, MBA, FACP GASCO Annual Meeting September 5, 2015 > One
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Member-centered cancer care In Georgia Ira Klein, MD, MBA, FACP GASCO Annual Meeting September 5, 2015 > One
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
 COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
Medication Therapy Management: Improving Health and Saving Money
 Medication Therapy Management: Improving Health and Saving Money Ed Staffa, RPh Vice President, Pharmacy Mirixa Corporation estaffa@mirixa.com July 23, 2008 MTM At A Glance The U.S. health care system
Medication Therapy Management: Improving Health and Saving Money Ed Staffa, RPh Vice President, Pharmacy Mirixa Corporation estaffa@mirixa.com July 23, 2008 MTM At A Glance The U.S. health care system
PHARMACY BENEFITS MANAGER SELECTION FAQ FOR PRODUCERS
 PHARMACY BENEFITS MANAGER SELECTION FAQ FOR PRODUCERS For Producer Audience Only - Please Do Not Distribute Regence has selected Prime Therapeutics as the Pharmacy benefits manager for its health plans.
PHARMACY BENEFITS MANAGER SELECTION FAQ FOR PRODUCERS For Producer Audience Only - Please Do Not Distribute Regence has selected Prime Therapeutics as the Pharmacy benefits manager for its health plans.
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
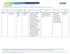 Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC South Carolina Primary Health Care Association September 19, 2015
 Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Quality Metrics & Immunizations
 Optimizing Patients' Health by Improving the Quality of Medication Use Quality Metrics & Immunizations Hannah Fish, PharmD, CPHQ Discussion Objectives 1. Describe the types and distribution of quality
Optimizing Patients' Health by Improving the Quality of Medication Use Quality Metrics & Immunizations Hannah Fish, PharmD, CPHQ Discussion Objectives 1. Describe the types and distribution of quality
Your Prescription Card. Your guide for savings.
 CVS Caremark 620 Epsilon Drive Pittsburgh, PA 15238 4750-_PM 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 Your Prescription Card. Your guide for savings. Dear Plan Member, Welcome to your new benefits. Attached
CVS Caremark 620 Epsilon Drive Pittsburgh, PA 15238 4750-_PM 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 Your Prescription Card. Your guide for savings. Dear Plan Member, Welcome to your new benefits. Attached
How pharmacy and retail health can support health and wellness. Nancy Gagliano Chief Medical Officer, MC September, 2014
 How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
3/17/2017. Innovative Opportunities for Pharmacists in the Evolving World of Healthcare. Elderly represent about of our emergency medical services:
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS)
 2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS) Overview Value Partnerships, in conjunction with the Blue Cross Pharmacy team, has created the Electronic Prescribing of Controlled
2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS) Overview Value Partnerships, in conjunction with the Blue Cross Pharmacy team, has created the Electronic Prescribing of Controlled
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Medicaid s Role in Combating the Opioid Crisis
 1 Medicaid s Role in Combating the Opioid Crisis September 23, 2016 Deborah Bachrach Partner Manatt Health Assessing Innovations in Medicaid 1 Medicaid Started as Adjunct to Welfare Programs 2 Eligibility
1 Medicaid s Role in Combating the Opioid Crisis September 23, 2016 Deborah Bachrach Partner Manatt Health Assessing Innovations in Medicaid 1 Medicaid Started as Adjunct to Welfare Programs 2 Eligibility
Value Based Pay for Performance Results & Highlights Measurement Year September 2017
 Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
PRESENTATION. Conference Proceedings. RAND Medicare Advantage (MA) and Part D Contract Star Ratings Technical Expert Panel May 31st 2018 Meeting
 Conference Proceedings RAND Medicare Advantage (MA) and Part D Contract Star Ratings Technical Expert Panel May 31st 2018 Meeting PRESENTATION Cheryl L. Damberg and Susan M. Paddock For more information
Conference Proceedings RAND Medicare Advantage (MA) and Part D Contract Star Ratings Technical Expert Panel May 31st 2018 Meeting PRESENTATION Cheryl L. Damberg and Susan M. Paddock For more information
Tools for Targeting High Risk Patients in Your Practice. Statement of Disclosure
 Tools for Targeting High Risk Patients in Your Practice Joseph Vande Griend, PharmD, BCPS, CGP Assistant Professor, University of Colorado Departments of Clinical Pharmacy and Family Medicine Skaggs School
Tools for Targeting High Risk Patients in Your Practice Joseph Vande Griend, PharmD, BCPS, CGP Assistant Professor, University of Colorado Departments of Clinical Pharmacy and Family Medicine Skaggs School
Mail Service Pharmacy
 Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
2016 Drug Trends Series
 Drug Trends Series Part 3: Assessing opioids and compounds Published August 2017 1 Drug Trends Series Opioids & Compounds First Script Introduction As with the first two editions in Coventry s Drug Trends
Drug Trends Series Part 3: Assessing opioids and compounds Published August 2017 1 Drug Trends Series Opioids & Compounds First Script Introduction As with the first two editions in Coventry s Drug Trends
Getting started with Prime
 Getting started with Prime How does a pharmacy plan work? When you visit your doctor, he or she may prescribe medicine for you. Here's how the plan works: Take your prescription and member ID card to the
Getting started with Prime How does a pharmacy plan work? When you visit your doctor, he or she may prescribe medicine for you. Here's how the plan works: Take your prescription and member ID card to the
Beneficiary and Pharmacy Outreach: Lessons Learned in Part D
 Beneficiary and Pharmacy Outreach: Lessons Learned in Part D Terri Swanson Aetna John Wells Aetna September 10, 2015 Agenda Aetna s Part D Pharmacy Networks in 2015 Pharmacy and Beneficiary Communication
Beneficiary and Pharmacy Outreach: Lessons Learned in Part D Terri Swanson Aetna John Wells Aetna September 10, 2015 Agenda Aetna s Part D Pharmacy Networks in 2015 Pharmacy and Beneficiary Communication
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015
 Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medication Adherence
 Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
Successes in Regional Collaboration to Achieve the Triple Aim Oregon. Pay for Performance Summit San Francisco March 24, 2014
 Successes in Regional Collaboration to Achieve the Triple Aim Oregon Pay for Performance Summit San Francisco March 24, 2014 Agenda Oregon Health Care Quality Corporation (Q Corp) Background Priority Projects
Successes in Regional Collaboration to Achieve the Triple Aim Oregon Pay for Performance Summit San Francisco March 24, 2014 Agenda Oregon Health Care Quality Corporation (Q Corp) Background Priority Projects
Your Prescription Card. Your guide for savings.
 3 Paragon Drive Montvale, NJ 07645 >00001 00001 001 P50708 _PM 7873 GROUP JOHN Q SAMPLE 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 APDNCLDJDKDIFPAKHPANEMFK AJCLLKEBEKNJJBNMPKGOKIKK AMBPIBPEAKHEIOBKFGFBOMMK
3 Paragon Drive Montvale, NJ 07645 >00001 00001 001 P50708 _PM 7873 GROUP JOHN Q SAMPLE 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 APDNCLDJDKDIFPAKHPANEMFK AJCLLKEBEKNJJBNMPKGOKIKK AMBPIBPEAKHEIOBKFGFBOMMK
Affordable Solutions
 Affordable Solutions For the Under & Un-Insured Don t Miss Out Dental Office Guide to DentalPlans.com Free Gift Inside Get to Know DentalPlans.com DentalPlans.com, a Henry Schein One Company, helps people
Affordable Solutions For the Under & Un-Insured Don t Miss Out Dental Office Guide to DentalPlans.com Free Gift Inside Get to Know DentalPlans.com DentalPlans.com, a Henry Schein One Company, helps people
Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants. April 23, 2014
 Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants April 23, 2014 Center on Budget and Policy Priorities Our Plan For Today Description of the Option and why its important:
Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants April 23, 2014 Center on Budget and Policy Priorities Our Plan For Today Description of the Option and why its important:
2017 Drug Trends Series
 2017 Drug Trends Series Part 1 Evaluating the traditional view Retail and mail-order prescriptions Published April 2018 1 2017 Drug Trends Series Traditional View First Script A year of important progress
2017 Drug Trends Series Part 1 Evaluating the traditional view Retail and mail-order prescriptions Published April 2018 1 2017 Drug Trends Series Traditional View First Script A year of important progress
New Mexico Retiree Health Care Authority Medicare Part D Prescription Drug Program Express Scripts Holding Company. All Rights Reserved.
 New Mexico Retiree Health Care Authority Medicare Part D Prescription Drug Program 1 About Express Scripts Express Scripts is RHCA s chosen partner for administering your prescription plan We are a leading
New Mexico Retiree Health Care Authority Medicare Part D Prescription Drug Program 1 About Express Scripts Express Scripts is RHCA s chosen partner for administering your prescription plan We are a leading
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT
 HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
HEADED FOR HEDIS AND REACHING FOR THE STARS: THE PHARMACIST S ROLE IN POPULATION HEALTH MANAGEMENT Desola Davis, PharmD, BCPS, BCACP Dalia Zall, PharmD 1 Copyright 2017 Kaiser Foundation Health Plan, Inc.
Medication Therapy Management program
 Medication Therapy Management program Your one-on-one review of your medicines Be safe Feel good Save money Safe and sound never felt so good Get the most from your medicine therapy with a personal medicine
Medication Therapy Management program Your one-on-one review of your medicines Be safe Feel good Save money Safe and sound never felt so good Get the most from your medicine therapy with a personal medicine
Lessons Learned from Meaningful Use Implementation. Cynthia L. Bero, MPH Partners HealthCare May 19, 2011
 Lessons Learned from Meaningful Use Implementation Cynthia L. Bero, MPH Partners HealthCare May 9, 20 Meaningful Use Plan of Action Learn the HITECH program Certified EHR Technology. Analyze gap between
Lessons Learned from Meaningful Use Implementation Cynthia L. Bero, MPH Partners HealthCare May 9, 20 Meaningful Use Plan of Action Learn the HITECH program Certified EHR Technology. Analyze gap between
September 22, National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC Prescription Opioid Epidemic
 National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC 20036 RE: Prescription Opioid Epidemic On behalf of America s Health Insurance Plans (AHIP), thank you for your leadership
National Association of Attorneys General 1850 M Street, NW, 12 th Floor Washington, DC 20036 RE: Prescription Opioid Epidemic On behalf of America s Health Insurance Plans (AHIP), thank you for your leadership
Pharmacy Benefit Management
 Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Q1 Is your software capable of generating ICD-10 test claims?
 Q1 Is your software capable of generating ICD-10 test claims? Answered: 55 Skipped: 0 85.45% 47 14.55% 8 Total 55 # If no, is there a scheduled month when it will be ready? (If it is not scheduled, please
Q1 Is your software capable of generating ICD-10 test claims? Answered: 55 Skipped: 0 85.45% 47 14.55% 8 Total 55 # If no, is there a scheduled month when it will be ready? (If it is not scheduled, please
A COMPREHENSIVE APPROACH TO MANAGING DIABETES
 A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
Uroplasty, Inc. Investor Update Canaccord Genuity Conference December 6, 2011
 Uroplasty, Inc. Investor Update Canaccord Genuity Conference December 6, 2011 Forward Looking Statement This presentation includes forward-looking statements, including financial projections, relating
Uroplasty, Inc. Investor Update Canaccord Genuity Conference December 6, 2011 Forward Looking Statement This presentation includes forward-looking statements, including financial projections, relating
Drug Therapy Management
 Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
Measures At A Glance Updated: 11/01/2018 2018 Page 1 of 9 Mandatory Measures (10) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to on an annual
MEASURE STEWARD Pharmacy Quality Alliance (PQA) D ATA SOURCE Enrollment; U R A C DOMAIN Engagement & Experience of Care
 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DM2012-12 DTM2015-01 Portion of Days Covered (PDC) Adherence
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help
 Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Title: Antipsychotic Use in Persons with Dementia CMS ID: ARCO3 NQF #: N/A
 Source(s) Pharmacy Quality Alliance (PQA). Technical specifications for PQA approved measures. Springfield (VA): Pharmacy Quality Alliance (PQA); 2015 Jul. 66 p. Measure Domain Clinical Quality Measures:
Source(s) Pharmacy Quality Alliance (PQA). Technical specifications for PQA approved measures. Springfield (VA): Pharmacy Quality Alliance (PQA); 2015 Jul. 66 p. Measure Domain Clinical Quality Measures:
RECEIVING YOUR PERMANENT
 00001 JOHN Q SAMPLE 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 3118-00001_PM City of Savannah 132 E. Broughton Street Savannah, GA 31401 THIS IS A ONE-TIME CARD TO BE USED UNTIL YOUR PERMANENT CARD ARRIVES
00001 JOHN Q SAMPLE 9501 E. Shea Blvd SCOTTSDALE, AZ 85260 3118-00001_PM City of Savannah 132 E. Broughton Street Savannah, GA 31401 THIS IS A ONE-TIME CARD TO BE USED UNTIL YOUR PERMANENT CARD ARRIVES
The Pharmacy Quality Alliance Optimizing Health by Advancing the Quality of Medication Use
 Optimizing Health by Improving the Quality of Medication Use Adult Immunization Measure Development Update The Optimizing Health by Advancing the Quality of Medication Use Lisa Hines, PharmD Senior Director,
Optimizing Health by Improving the Quality of Medication Use Adult Immunization Measure Development Update The Optimizing Health by Advancing the Quality of Medication Use Lisa Hines, PharmD Senior Director,
Thank you for your continued engagement and member support of the Pharmacy Quality Alliance.
 Optimizing Health by Advancing the Quality of Medication Use November 14, 2017 FROM: Jacqueline Green, Chief Operating Officer, Pharmacy Quality Alliance SUBJECT: PQA Headlines & Highlights as we head
Optimizing Health by Advancing the Quality of Medication Use November 14, 2017 FROM: Jacqueline Green, Chief Operating Officer, Pharmacy Quality Alliance SUBJECT: PQA Headlines & Highlights as we head
16 th Annual IHA Stakeholders Meeting Session 2C
 16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
Fifth Annual National ACO Summit
 Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Telligen Quality Innovation Network Quality Improvement Organization
 Telligen Quality Innovation Network Quality Improvement Organization PQA Patient Safety Measures for Inappropriate Prescription Opioid Use August 29, 2017 Optimizing Patients' Health by Improving the Quality
Telligen Quality Innovation Network Quality Improvement Organization PQA Patient Safety Measures for Inappropriate Prescription Opioid Use August 29, 2017 Optimizing Patients' Health by Improving the Quality
NCPA LTC Division Newsletter
 March 2016 NCPA LTC Division Newsletter NCPA Offers FDA Additional Information on Repackaging Draft Guidance NCPA recently joined with the American Society of Consultant Pharmacists (ASCP) in a follow
March 2016 NCPA LTC Division Newsletter NCPA Offers FDA Additional Information on Repackaging Draft Guidance NCPA recently joined with the American Society of Consultant Pharmacists (ASCP) in a follow
How Mail-Servi. Prepared for
 How Mail-Servi ice Pharmacies Will Save $46.6 Billion Over the Next Decade and the Cost of Proposed Restrictions Prepared for February 2012 Table of Contents I. Executive Summary... 3 Major Findings on
How Mail-Servi ice Pharmacies Will Save $46.6 Billion Over the Next Decade and the Cost of Proposed Restrictions Prepared for February 2012 Table of Contents I. Executive Summary... 3 Major Findings on
Performance Measurement: HEDIS, STARS and More. Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016
 Performance Measurement: HEDIS, STARS and More Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016 Defining Quality & Performance Trends The Triple Aim and National Priorities Partnership
Performance Measurement: HEDIS, STARS and More Margaret E. O Kane NCQA President CAPG Educational Series October 27, 2016 Defining Quality & Performance Trends The Triple Aim and National Priorities Partnership
2017 Medicare CAHPS At-A-Glance Report
 2017 Medicare CAHPS At-A-Glance Report CMS MA PD Contract: H9207 Project Number(s): 30120117 and 10123759 Current data as of: 07/10/2017 1965 Evergreen Boulevard Suite 100, Duluth, Georgia 30096 2017 At-A-Glance
2017 Medicare CAHPS At-A-Glance Report CMS MA PD Contract: H9207 Project Number(s): 30120117 and 10123759 Current data as of: 07/10/2017 1965 Evergreen Boulevard Suite 100, Duluth, Georgia 30096 2017 At-A-Glance
A&M Care Prescription Drug Program Express Scripts Holding Company. All Rights Reserved.
 A&M Care 2018 2019 Prescription Drug Program 1 Prescription Drug Benefits Annual Deductible Out of Pocket Maximum Access Options Retail 30 Day Supply: Refills allowed as prescribed. (Good option for new
A&M Care 2018 2019 Prescription Drug Program 1 Prescription Drug Benefits Annual Deductible Out of Pocket Maximum Access Options Retail 30 Day Supply: Refills allowed as prescribed. (Good option for new
Amy Larrick Chavez-Valdez, Director, Medicare Drug Benefit and C & D Data Group
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, Maryland 21244-1850 CENTER FOR MEDICARE TO: FROM: SUBJECT: All Part D Sponsors Amy Larrick
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, Maryland 21244-1850 CENTER FOR MEDICARE TO: FROM: SUBJECT: All Part D Sponsors Amy Larrick
January 16, Dear Administrator Verma:
 Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
Ms. Seema Verma Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services Attention: CMMI New Direction P.O. Box 8011 Baltimore, MD 21244-1850 Re: (CMS-4182-P) Medicare
INFLUENZA & PNEUMOCCOCAL VACCINATIONS
 INFLUENZA & PNEUMOCCOCAL VACCINATIONS ONE HEALTH PLAN S PERSPECTIVE Paige Reichert, MD Senior Medical Director of Quality May 2015 THE CIGNA-HEALTHSPRING FOOTPRINT o Cigna-HealthSpring serves the senior
INFLUENZA & PNEUMOCCOCAL VACCINATIONS ONE HEALTH PLAN S PERSPECTIVE Paige Reichert, MD Senior Medical Director of Quality May 2015 THE CIGNA-HEALTHSPRING FOOTPRINT o Cigna-HealthSpring serves the senior
Atrius Health Pioneer ACO: Structure, Activities and Results
 Atrius Health Pioneer ACO: Structure, Activities and Results Emily Brower Executive Director Accountable Care Programs Emily_Brower@AtriusHealth.org March 2014 1 Atrius Health. 2 Atrius Health Structure
Atrius Health Pioneer ACO: Structure, Activities and Results Emily Brower Executive Director Accountable Care Programs Emily_Brower@AtriusHealth.org March 2014 1 Atrius Health. 2 Atrius Health Structure
The Value of Walgreens
 The Value of Walgreens How Walgreens improves employer health plans through access, quality and lower costs Why millions of patients choose Walgreens And your options to move forward with Walgreens Walgreens
The Value of Walgreens How Walgreens improves employer health plans through access, quality and lower costs Why millions of patients choose Walgreens And your options to move forward with Walgreens Walgreens
comparisons and helped about 30 patients sign up for First Health Value Plus thinking they would have zero copays on generics. Two days before the dea
 I helped several hundred patients evaluate the best plan for them this year and Coventry s First Health Value Plus was the very best for many of them. I used the Medicare.gov website and put in my pharmacy
I helped several hundred patients evaluate the best plan for them this year and Coventry s First Health Value Plus was the very best for many of them. I used the Medicare.gov website and put in my pharmacy
Quality Innovation Network - Quality Improvement Organization Adult Immunization Task. May 14, Agenda
 Quality Innovation Network - Quality Improvement Organization Adult Immunization Task National Adult and Influenza Immunization Summit Centers for Medicare & Medicaid Services 1 May 14, 2015 Agenda Quick
Quality Innovation Network - Quality Improvement Organization Adult Immunization Task National Adult and Influenza Immunization Summit Centers for Medicare & Medicaid Services 1 May 14, 2015 Agenda Quick
Making Diabetes Prevention a Reality: The National Diabetes Prevention Program
 Making Diabetes Prevention a Reality: The National Diabetes Prevention Program Ann Albright, PhD, RD Director, Division of Diabetes Translation Centers for Disease Control and Prevention National Center
Making Diabetes Prevention a Reality: The National Diabetes Prevention Program Ann Albright, PhD, RD Director, Division of Diabetes Translation Centers for Disease Control and Prevention National Center
Paying for Genomic Testing and Associated Care. Scott Ramsey, MD, PhD FRED HUTCHINSON CANCER RESEARCH CENTER
 Paying for Genomic Testing and Associated Care Scott Ramsey, MD, PhD FRED HUTCHINSON CANCER RESEARCH CENTER Cost of Cancer Genome Sequencing Will vary with: Approach Whole genome, exome, transcriptome
Paying for Genomic Testing and Associated Care Scott Ramsey, MD, PhD FRED HUTCHINSON CANCER RESEARCH CENTER Cost of Cancer Genome Sequencing Will vary with: Approach Whole genome, exome, transcriptome
2012 Chronic Respiratory. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2012 Chronic Respiratory Program Evaluation Our mission is to improve the health and quality of life of our members 2012 Chronic Respiratory Program Evaluation Program Title: Chronic Respiratory Program
2012 Chronic Respiratory Program Evaluation Our mission is to improve the health and quality of life of our members 2012 Chronic Respiratory Program Evaluation Program Title: Chronic Respiratory Program
BENEFITS ASSISTANCE PROGRAM 2015 ARIZONA PRESCRIPTION DRUG PLANS (PDP) Area Agency on Aging, Region One - 1 -
 AARP MedicareRx Saver Plus S5921-380 Plan rating: 2.5 stars AARP MedicareRx Preferred S5820-027 Plan rating: United Healthcare P.O. Box 29300 Hot Springs, AR 71903 1-888-867-5575 (Members) 1-888-867-5564
AARP MedicareRx Saver Plus S5921-380 Plan rating: 2.5 stars AARP MedicareRx Preferred S5820-027 Plan rating: United Healthcare P.O. Box 29300 Hot Springs, AR 71903 1-888-867-5575 (Members) 1-888-867-5564
Safe, effective, affordable drug choices: online tool for payers and patients.
 Executive summary: Rising healthcare costs and greater access to medical information drive patients to seek options for their drug therapy. The MedAlternatives database by Gold Standard/Elsevier empowers
Executive summary: Rising healthcare costs and greater access to medical information drive patients to seek options for their drug therapy. The MedAlternatives database by Gold Standard/Elsevier empowers
Medicaid in South Carolina. South Carolina Medicaid in /19/2018. > FY 2017 Appropriation: $7.2 billion > Full benefit Membership: 1.
 Medicaid in South Carolina > FY 2017 Appropriation: $7.2 billion > Full benefit Membership: 1.04 million South Carolina Medicaid in 2018 Bryan Amick SC Chapter, American Academy of Pediatrics 2018 CATCH
Medicaid in South Carolina > FY 2017 Appropriation: $7.2 billion > Full benefit Membership: 1.04 million South Carolina Medicaid in 2018 Bryan Amick SC Chapter, American Academy of Pediatrics 2018 CATCH
Challenges for U.S. Attorneys Offices (USAO) in Opioid Cases
 Challenges for U.S. Attorneys Offices (USAO) in Opioid Cases Overview On August 2, 2017, U.S. Attorney General Jeff Sessions announced a pilot program whereby a new federal data analysis program is being
Challenges for U.S. Attorneys Offices (USAO) in Opioid Cases Overview On August 2, 2017, U.S. Attorney General Jeff Sessions announced a pilot program whereby a new federal data analysis program is being
Medicaid Care Management: The Advanced Medical Home (AMH) Program OB Care Management (OBCM) Care Coordination for Children (CC4C) March 2018
 Medicaid Care Management: The Advanced Medical Home (AMH) Program OB Care Management (OBCM) Care Coordination for Children (CC4C) March 2018 Advanced Medical Home Overview The Advanced Medical Home (AMH)
Medicaid Care Management: The Advanced Medical Home (AMH) Program OB Care Management (OBCM) Care Coordination for Children (CC4C) March 2018 Advanced Medical Home Overview The Advanced Medical Home (AMH)
ADMINISTRATIVE POLICY AND PROCEDURES MedStar Family Choice Medicare Advantage Plans
 ADMINISTRATIVE POLICY AND PROCEDURES MedStar Family Choice Medicare Advantage Plans DEPARTMENT: Medicare Compliance POLICY TITLE: RELATED DEPARTMENTS: All POLICY #: 706 C VERSION #: 4 REVISION DATE: Identifying
ADMINISTRATIVE POLICY AND PROCEDURES MedStar Family Choice Medicare Advantage Plans DEPARTMENT: Medicare Compliance POLICY TITLE: RELATED DEPARTMENTS: All POLICY #: 706 C VERSION #: 4 REVISION DATE: Identifying
Free Yourself Tips for living without back pain
 spring 2010 Free Yourself Tips for living without back pain - Log on to live healthier - Diabetes do s and don ts - How to appeal a claim best friends enjoying Idaho's city of rocks one TO one newsletter
spring 2010 Free Yourself Tips for living without back pain - Log on to live healthier - Diabetes do s and don ts - How to appeal a claim best friends enjoying Idaho's city of rocks one TO one newsletter
STEP THERAPY IN MEDICARE PART D
 STEP THERAPY IN MEDICARE PART D Sarkis Kavarian, PharmD Candidate 15 Preceptor Dr. Craig Stern Pro Pharma Pharmaceutical Consultants, Inc. May 1 st, 2015 Objectives Why is this important? Medicare Part
STEP THERAPY IN MEDICARE PART D Sarkis Kavarian, PharmD Candidate 15 Preceptor Dr. Craig Stern Pro Pharma Pharmaceutical Consultants, Inc. May 1 st, 2015 Objectives Why is this important? Medicare Part
Part D PDE Data and the Opioid Epidemic
 Part D PDE Data and the Opioid Epidemic State Data Resource Center Acumen, LLC August 30, 2017 3:30-4:30pm ET Outline Background Information on Opioid Use Helpful Part D Elements for Analysis How to Perform
Part D PDE Data and the Opioid Epidemic State Data Resource Center Acumen, LLC August 30, 2017 3:30-4:30pm ET Outline Background Information on Opioid Use Helpful Part D Elements for Analysis How to Perform
Monitoring Psychotropic Use Among Foster Children EMPAA
 State Plans for Monitoring Psychotropic Use Among Foster Children EMPAA October 30, 2012 Child and Family Services Improvement and Innovation Act of 2011 Required Components of Psychotropic Oversight and
State Plans for Monitoring Psychotropic Use Among Foster Children EMPAA October 30, 2012 Child and Family Services Improvement and Innovation Act of 2011 Required Components of Psychotropic Oversight and
Gathering and Using Member Feedback in Plan Governance
 Gathering and Using Member Feedback in Plan Governance Credit Information If you are a social worker in a National Association of Social Workers (NASW) state and would like to receive CE credits through
Gathering and Using Member Feedback in Plan Governance Credit Information If you are a social worker in a National Association of Social Workers (NASW) state and would like to receive CE credits through
American Joint Replacement Registry s Orthopaedic Quality Resource Center a CMS approved Qualified Clinical Data Registry (QCDR)
 American Joint Replacement Registry s Orthopaedic Quality Resource Center a CMS approved Qualified Clinical Data Registry (QCDR) American Joint Replacement Registry s Orthopaedic Quality Resource Center
American Joint Replacement Registry s Orthopaedic Quality Resource Center a CMS approved Qualified Clinical Data Registry (QCDR) American Joint Replacement Registry s Orthopaedic Quality Resource Center
PQA Measure Development Update: June 2017
 PQA Measure Development Update: June 2017 The Measure Development Teams and Task Forces have been meeting monthly via webinar, and the Stakeholder Advisory Panels had their first meetings in March. Additionally,
PQA Measure Development Update: June 2017 The Measure Development Teams and Task Forces have been meeting monthly via webinar, and the Stakeholder Advisory Panels had their first meetings in March. Additionally,
QBPC PI CME Performance Dashboards Reference Guide
 QBPC PI CME Performance Dashboards Reference Guide QBPC PI-CME has been designed to enhance knowledge, competency and performance in the management of patients with cardiovascular (CV) metabolic risk factors.
QBPC PI CME Performance Dashboards Reference Guide QBPC PI-CME has been designed to enhance knowledge, competency and performance in the management of patients with cardiovascular (CV) metabolic risk factors.
Diabetes Care begins with Diabetes Prevention. Neha Sachdev, MD Janet Williams, MA
 Diabetes Care begins with Diabetes Prevention Neha Sachdev, MD Janet Williams, MA Objectives Describe the clinical practice burden and trends in type 2 diabetes Review evidence for diabetes prevention
Diabetes Care begins with Diabetes Prevention Neha Sachdev, MD Janet Williams, MA Objectives Describe the clinical practice burden and trends in type 2 diabetes Review evidence for diabetes prevention
Medication Therapy Management Solution
 Medication Therapy Management Solution A Medicaid Case Report It s often challenging to include evidencebased clinical programs that offer financial benefits. However, pharmacotherapy is central to the
Medication Therapy Management Solution A Medicaid Case Report It s often challenging to include evidencebased clinical programs that offer financial benefits. However, pharmacotherapy is central to the
EXAMPLE ONLY. RxBIN Issuer (80840) ID NAME Drew Zehnder. Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030
 Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030 00001 RxBIN 004336 RxPCN ADV RxGRP RX3151 Issuer (80840) 9151014609 ID NAME 111111111 Drew Zehnder Present this Prescription Card to fill your
Houston Methodist 6565 Fannin Street, GB164 Houston, TX 77030 00001 RxBIN 004336 RxPCN ADV RxGRP RX3151 Issuer (80840) 9151014609 ID NAME 111111111 Drew Zehnder Present this Prescription Card to fill your
Your Prescription Card. Your guide for savings.
 Kent State University P.O. Box 5190 Kent, OH 44242-0001 13578-00001_PM JOHN Q SAMPLE 2215 SANDERS RD NBT 2215-5 NORTHBROOK, IL 60062 Your Prescription Card. Your guide for savings. 00001 Dear Plan Member,
Kent State University P.O. Box 5190 Kent, OH 44242-0001 13578-00001_PM JOHN Q SAMPLE 2215 SANDERS RD NBT 2215-5 NORTHBROOK, IL 60062 Your Prescription Card. Your guide for savings. 00001 Dear Plan Member,
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
The MetroHealth System. Creating the HIT Organizational Culture at MetroHealth. Creating the HIT Organizational Culture
 CASE STUDY CASE STUDY The MetroHealth System Optimizing Health Information Technology to Increase Vaccination Rates The MetroHealth System in Cleveland, Ohio, was the first safety-net health care system
CASE STUDY CASE STUDY The MetroHealth System Optimizing Health Information Technology to Increase Vaccination Rates The MetroHealth System in Cleveland, Ohio, was the first safety-net health care system
