MRCP in Patient Care: A Prospective Survey of Gastroenterologists
|
|
|
- Scot Evans
- 6 years ago
- Views:
Transcription
1 Gastrointestinal Imaging Original Research Akisik et al. MRCP Survey Gastrointestinal Imaging Original Research M. Fatih Akisik 1 S. Gregory Jennings 1 Alex M. Aisen 1 Stuart Sherman 2 Gregory A. Cote 2 Kumaresan Sandrasegaran 1 Temel Tirkes 1 Akisik MF, Jennings SG, Aisen AM, et al. Keywords: MRCP, practice patterns, survey DOI: /AJR Received August 21, 2012; accepted after revision January 7, Department of Radiology and Imaging Sciences, Indiana University School of Medicine, 550 N University Blvd, Rm 0615, Indianapolis, IN Address correspondence to M. F. Akisik (makisik@iupui.edu). 2 Department of Medicine, Division of Gastroenterology and Hepatology, Indiana University School of Medicine, Indianapolis, IN. AJR 2013; 201: X/13/ American Roentgen Ray Society MRCP in Patient Care: A Prospective Survey of Gastroenterologists OBJECTIVE. MRCP is increasingly used to evaluate pancreaticobiliary disease, yet its effect on patient care is unknown. The purpose of this study was to measure the effect of MRCP on referring physicians initial diagnoses, the physicians confidence in their diagnoses, and the influence of MRCP results on clinical management. SUBJECTS AND METHODS. We prospectively surveyed gastroenterologists who referred patients for nonurgent MRCP for pancreaticobiliary evaluation. Before MRCP, gastroenterologists reported the working diagnosis, confidence level (high, moderate, low), and next step in clinical management if MRCP was unavailable. MRCP was performed with standard protocols, including secretin enhancement. After reviewing MRCP findings and without referring to their previous assessment, gastroenterologists reported a revised diagnosis, confidence level, and next step in clinical management. They then compared pre- and post-mrcp management plans and rated the influence of MRCP on changing management from 1 (none) to 5 (major). Diagnostic confidence and frequency of common diagnoses and recommendation for an invasive next-step procedure (e.g., ERCP) or endoscopic ultrasound were compared between pre- and post-mrcp assessments. RESULTS. Survey data were analyzed on 171 patients (123 women, 48 men; mean age, 50 [SD, 17] years; range, years) undergoing MRCP for unexplained abdominal pain (42.9%), suspected pancreaticobiliary neoplasm (20%), recent acute (17.1%) or suspected chronic (14.9%) pancreatitis, and other indications (5.1%). Recommendations of ERCP and endoscopic ultrasound decreased after MRCP (from 49.1% to 35.1%, p=0.03, and from 26.9% to 13.5%, p 0.01). After MRCP, high confidence in diagnosis increased (from 72/171 to 100/171, p < 0.01), as did recommendations for noninvasive therapy (from 18/171 to 56/171, p < 0.01). A major or substantial change in clinical management was made in the care of 67 of 171 patients (39.2%). CONCLUSION. Use of MRCP significantly changes gastroenterologists treatment of patients with suspected pancreaticobiliary disease by increasing diagnostic confidence and reducing the frequency of invasive follow-up procedures. A patient with abdominal symptoms suggesting pancreaticobiliary disease poses a daunting clinical problem until an accurate diagnosis is made. Determining the cause of the symptoms often requires an invasive diagnostic procedure with sedation, such as ERCP or endoscopic sonography. ERCP has been the most commonly used diagnostic imaging method in the evaluation of these patients and continues to be so at many smaller medical centers. ERCP can also be used to provide therapy, such as sphincterotomy or stent placement, when a structural problem is identified. However, ERCP is associated with substantial morbidity, most commonly pancreatitis; bleeding; duode- nal perforations; and in rare instances death [1 3]. Although endoscopic ultrasound is considered a lower-risk procedure, complications are not infrequent. They are more common in association with fine-needle aspiration and endoscopic ultrasound-guided interventions such as pseudocyst drainage and biopsy [4]. In some patients, diagnostic pancreatobiliary endoscopy may be technically difficult or impossible, as in cases of postoperative anatomic changes. Although imaging of the pancreas and liver is possible with CT and conventional MRI [5], only limited evaluation of the pancreaticobiliary ductal system is possible with these studies, and no functional information about the pancreas is obtained. The introduction AJR:201, September
2 Akisik et al. of magnetic resonance cholangiopancreatography (MRCP) has revolutionized the ability to identify ductal anatomy noninvasively [6 9]. Injection of a synthetic secretin, which stimulates pancreatic exocrine function, has further improved MRCP by improving visualization of the pancreatic ductal system and enabling assessment of pancreatic exocrine function [10 12]. Secretin injection improves delineation of the pancreatic ducts and side branches and thus detection of pathologic conditions (e.g., chronic pancreatitis), anatomic variants (e.g., pancreas divisum) [13 15], and pancreatic cystic lesions [16]. MRCP is much less invasive than ERCP and endoscopic ultrasound and has become the front-line imaging technique at our medical center and elsewhere for evaluating patients with unexplained abdominal pain that may be related to pancreaticobiliary disease [17, 18]. Although gastroenterologists and other clinicians have embraced MRCP for initial imaging evaluation, few systematic data are available on the effect of MRCP on clinical decision making [19 21]. The purpose of this study was to measure the effect of MRCP on referring physicians initial diagnoses, their confidence in the diagnoses, and the degree to which MRCP results influence clinical management. Subjects and Methods Patient Population This prospective, single-institution, HIPAAcompliant study was approved by our institutional review board with waiver of the requirement for informed consent. On 95 dates between November 2009 and December 2010, we enrolled all patients who were referred by participating gastroenterologists at our tertiary-care hospital for secretin-enhanced MRCP in the evaluation of pancreaticobiliary disease and did not have a known history of ERCP, endoscopic ultrasound, or pancreaticobiliary surgery. The clinical indication for MRCP and the name of the referring gastroenterologist were recorded. After imaging was performed, an electronic folder containing all MRCP images and the radiologist s report of each study with no patient identifiers other than study number was created in the radiology image archive. The radiologic diagnosis of chronic pancreatitis was based on the Cambridge criteria for pancreatic ductal assessment and pancreatic atrophy [22] (Table 1). Acute pancreatitis was defined by a combination of pancreatic edema, fluid collections, and enhancement abnormalities. Survey Method Before MRCP, the requesting gastroenterologist was asked to complete a survey delineating the working diagnosis before MRCP, the level of confidence with this diagnosis (high, moderate, or low), and the next step in clinical management if MRCP were unavailable. The gastroenterologists were aware of all available clinical information, usually including previous imaging studies, as they formed their working diagnoses; this reflects routine clinical practice. After reviewing the results of MRCP and without referring to their pre- MRCP survey responses, the gastroenterologists were asked to provide a revised working diagnosis, level of confidence with this diagnosis, and the next step in clinical management after MRCP was completed. The physician then compared pre- and post-mrcp management plans and rated the influence of MRCP on changing clinical management from 1 (no change) to 5 (major change). MRCP All MRCP examinations were performed with a 1.5-T (Magnetom Avanto, Siemens Healthcare) or 3-T (Magnetom Verio, Siemens Healthcare) MRI system with standard MRCP imaging parameters and a multielement phased-array imaging coil. Similar imaging parameters were used for the 1.5-T and 3-T systems. A negative contrast agent consisting of up to 300 ml ferumoxsil oral suspension (GastroMARK, Covidien Pharmaceuticals) was administered orally approximately 30 minutes before the MRCP examination, after a fast of at least 4 hours. Both traditional imaging sequences and fluidsensitive MRCP sequences designed to depict the pancreatic and biliary ducts were used. Thin-slice, T1- and T2-weighted images were acquired. In addition, the protocol included fluid-sensitive, coronal or coronal oblique 2D, T2-weighted, breath-hold MRCP images obtained with both a thin-slice 3D technique and a thick-slab sequence with a half- Fourier single shot acquisition pulse sequence with a single 40-mm-thick coronal slab positioned over the pancreas (Table 2). All patients underwent secretin-enhanced MRCP. An image was acquired every 30 seconds over a 10-minute period after IV administration of 16 µg of synthetic human secretin (ChiRhostim, ChiRhoClin) injected over 1 minute. All examinations concluded with a threephase unenhanced and contrast-enhanced 3D T1- weighted fat-suppressed gradient-echo sequence. A standard of 0.1 mmol/kg gadobenate dimeglumine (MultiHance, Bracco Diagnostics) was administered at 2 ml/s via a power injector and followed by a 20-mL saline flush. The mean imaging time for secretin-enhanced MRCP at our facility is 1 hour. Data Analysis The proportion of patients with each of several common diagnoses and the proportion with highconfidence diagnoses before and after MRCP were compared by Fisher test. The frequencies of ERCP and endoscopic ultrasound as recommended nextstep procedures before and after MRCP were also compared by Fisher test. We divided all next-step procedures into invasive and noninvasive categories and compared their frequency of recommendation before and after MRCP by Fisher test. Invasive procedures included ERCP, endoscopic ultrasound, upper endoscopy, and surgical consultation. Noninvasive measures included outpatient medical therapy, dietary regimen, and follow-up with laboratory or other imaging tests, such as CT, ultrasound, and upper gastrointestinal examinations. Results At the end of enrollment, 196 patients were identified. Twenty-three patients were excluded from data analysis because of incomplete surveys, and two patients were later found to not meet the inclusion criteria. The other 171 patients (123 women, 48 men; mean age, 50 [SD, 17] years; range, years) composed the study group. The reasons for referral were unexplained abdominal pain of suspected pancreatobiliary origin (42.9%), suspected pancreatobiliary neoplasm (20%), recent TABLE 1: Cambridge Criteria for Chronic Pancreatitis Term Main Duct Side Branches Additional Features Normal Normal None Equivocal Normal < 3 Mild disease Normal 3 Moderate disease Abnormal > 3 Marked disease Abnormal > 3 One or more of large cavity, obstruction, filling defect, severe dilatation or irregularity Note Modified with permission from [22]. If pathologic changes are limited to one third or less of the gland, they are said to be local and designated as being in the head, body, or tail; if more than one third is affected, the changes are diffuse. 574 AJR:201, September 2013
3 MRCP Survey TABLE 2: MRCP Sequence Parameters Sequence Slice Thickness (mm) TE TR Flip Angle ( ) No. of Signals Acquired Bandwidth (Hz) Gradient-recalled echo Dixon T1-weighted 6 2.4/ HASTE axial and coronal T2-weighted STIR HASTE MRCP radial slab D MRCP HASTE MRCP coronal for secretin Volumetric interpolated breath-hold examination (VIBE) TABLE 3: Referring Gastroenterologists Working Diagnoses Before and After MRCP (n = 171) Working Diagnosis Before MRCP After MRCP p Pancreatitis 52 (30.4) 52 (30.4) 1.00 Acute 27 (15.8) 15 (8.8) 0.07 Chronic 21 (12.2) 33 (19.2) 0.10 Acute on chronic 4 (2.3) 4 (2.3) 1.00 Sphincter of Oddi dysfunction 36 (21.1) 29 (17.0) 0.41 Pancreaticobiliary disease 17 (9.9) 17 (9.9) 1.00 Neoplasm 34 (19.9) 33 (19.3) 1.00 Other diagnoses 32 (18.7) 40 (23.4) 0.59 TABLE 4: Proposed Next Step by Referring Gastroenterologists (n = 171) Next Step Before MRCP After MRCP p ERCP 84 (49.1) 63 (36.8) 0.03 Endoscopic ultrasound 46 (26.9) 23 (13.5) < 0.01 Conservative therapy a 22 (12.9) 56 (32.7) < 0.01 Further imaging 15 (8.8) 18 (10.5) 0.59 Surgical consultation 4 (2.3) 9 (5.3) 0.26 a Medical therapy, diet, laboratory workup, or follow-up. acute pancreatitis (17.1%), suspected chronic pancreatitis (14.9%), and other indications (5.1%). Six referring gastroenterologists participated in the survey. MRCP examinations were interpreted by one of four abdominal radiologists, each with at least 11 years of body MRI experience. Diagnoses before and after MRCP are summarized in Table 3. The most frequent working diagnoses before MRCP were pancreatitis (52 of 171 patients, 30.4%), including acute (n = 27), chronic (n = 21), and a mix of acute and chronic (n = 4) disease. After MRCP, the most frequent diagnosis continued to be pancreatitis (52 of 171 patients, 30.4%), including acute (n = 15), chronic (n = 33), and a mix of acute and chronic (n = 4) disease. Although these changes in diagnosis were not significant, confidence in diagnosis increased after the results of MRCP were known. High-confidence diagnoses increased from 72 of 171 patients (42.1%) before MRCP to 100 of 171 patients (58.5% after MRCP) (p < 0.01). Only four patients had low-confidence diagnoses after MRCP, compared with 12 before MRCP. Treatment strategy changed significantly once the MRCP results were available (Table 4). Before MRCP, gastroenterologists would have recommended ERCP to 84 of the 171 patients (49.1%) or endoscopic ultrasound in 46 patients (26.9%) compared with 63 (36.8%) and 23 patients (13.5%) after MRCP (p = 0.03 for ERCP, p < 0.01 for endoscopic ultrasound) (Table 4). Thus the need for these invasive procedures to evaluate pancreaticobiliary disease significantly decreased after MRCP interpretation. Noninvasive or conservative management was significantly more likely to be recommended after MRCP results were known. Without MRCP, only 22 of 171 patients (12.9%) would have been treated conservatively. After MRCP this proportion increased to 56 of 171 patients (32.7%) (p < 0.01). Overall, physicians reported a major or substantial change in clinical management after MRCP for 67 of 171 patients (39.2%) (Table 5). Discussion MRCP has been frequently used to evaluate the pancreaticobiliary ductal system for biliary diseases, such as ductal stones, strictures, and postsurgical complications. In this study, we found that an optimized MRCP examination reduces the need for invasive testing for the diagnosis of pancreatic diseases and that the findings increase the referring physician s confidence in the working diagnosis. Few data have been published about how MRCP changes clinical practice. In 1997 in a prospective study that included 40 patients, Sahai et al. [19] evaluated the efficacy of MRCP in supplanting ERCP. The patients had working diagnoses of jaundice, abnormal liver enzyme concentration, abdominal pain, recurrent acute pancreatitis, and suspected complications of chronic pancreatitis. Those investigators concluded that MRCP findings did not significantly affect clinicians decision making and that adding results of MRCP to other clinical information would have prevented less than 3% of diagnostic and therapeutic ERCP procedures. The results of the study by Sahai et al. [19] differ from ours for a number of reasons. The patient selection processes differed substantially. We entered only patients referred for MRCP, whereas Sahai et al. selected patients scheduled for ERCP. This is a crucial methodologic difference, resulting in different patient populations. The technology underlying MRCP has improved substantially in the 15 years between the studies. Modern MRI sys- AJR:201, September
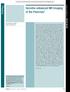
4 Akisik et al. tems can generate 3D, high-resolution MRCP images that can show tiny ductal stones, abnormal side branches, and ductal strictures. In addition, visualization of the pancreatic duct can be significantly enhanced with IV secretin [10 15, 18, 23]. In a 2001 study, Parnaby et al. [20] collected data suggesting that in a suitably selected subgroup of patients, MRCP could obviate ERCP, a result similar to ours. In a retrospective study including 1148 patients, Farrell et al. [21] concluded, initial MRCP in patients referred with abdominal pain would potentially have avoided ERCP in 44% of cases, and significantly reduced patient morbidity and mortality. These studies approached the problem from different vantage points, yet both concluded that MRCP was useful in reducing the need for ERCP. However, they did not test the clinical value of MRCP in defining TABLE 5: Effect of MRCP Results on Clinical Management by Gastroenterologists (n = 171) Degree of Change Clinical Decision No. of Patients 1, None No change in management 73 (42.7) 2, Minor Nonpharmaceutical, discharge with instructions (e.g., avoid fatty food) 23 (13.5) 3, Moderate Additional noninvasive diagnostic procedure (e.g., CT, ultrasound of abdomen) or upper gastrointestinal examination 8 (4.7) 4, Substantial Change in pharmaceutical management, invasive procedure (ERCP or endoscopic ultrasound), referral to additional specialist 55 (32.2) 5, Major Change in recommendation for surgery, for invasive endoscopic procedure (e.g., sphincterotomy), major change in diagnosis (e.g., benign versus malignant lesion) 12 (7.0) A C B D the cause of symptoms. Moreover, the MRCP protocols were mainly heavily T2 weighted. In other words, they could be classified as MR ductography. At our institution, we generally incorporate MRCP in a complete MRI study, which includes anatomic soft-tissue imaging and the use of IV gadolinium contrast medium in addition to MRCP with secretin. Contrast enhancement yields invaluable information about parenchymal organs, including the pancreas. In some cases, high-grade pancreatic ductal strictures can be caused by an obstructive mass, and thus contrast media may be useful for excluding malignancy. Secretin enhancement provides information about pancreatic exocrine function and improves visualization of the main duct, its side branches, and pancreatic cystic lesions and their relation to the main duct in differentiation of side-branch intrapapillary mucinous neoplasms. Use of secretin also facilitates delineation of complete versus incomplete pancreas divisum and pseudostrictures [11 15, 23]. Our results show that in a patient population representative of that seen for evaluation of suspected pancreaticobiliary disease at a tertiary care center, MRCP had a significant effect on clinical decision making. Gastroenterologists would have recommended endoscopic procedures for 76% of patients (ERCP, 49.1%; endoscopic ultrasound, 26.9%) without MRCP findings compared with 48.6% (ERCP, 35.1%; endoscopic ultrasound, 13.5%) when MRCP results were available. Although unproven, preprocedure MRCP may also help in planning for subsequent ERCP in patients in whom it is necessary, as for confirming the presence of complete pancreas divisum and thereby eliminating efforts to cannulate the ventral pancreatic duct. Fig year-old woman with constant abdominal pain referred for further evaluation. A, MRCP image obtained before secretin injection shows normal-caliber main pancreatic duct without obvious abnormal side branches, dilatation, or luminal strictures. B, MRCP image obtained 4 minutes after secretin injection shows dilated duct with multiple abnormal side branches (arrows) consistent with mild chronic pancreatitis. C, Axial unenhanced T1-weighted fat-suppressed gradient-recalled echo image shows normal signal intensity of pancreas. D, Axial contrast-enhanced T1-weighted fatsuppressed gradient-recalled echo image obtained 45 seconds after C shows normal-size pancreatic gland with homogeneous enhancement. Without secretin administration, diagnosis of chronic pancreatitis would not have been possible. 576 AJR:201, September 2013
5 MRCP Survey The decreased need for invasive procedures resulted largely from confirmation of suspected chronic pancreatitis and exclusion of structural abnormalities that might have required intervention (Fig. 1). This alone may justify the value of diagnostic MRCP in the evaluation of many abdominal disorders. Another important result is in the increased confidence level of gastroenterologists after MRCP examination. Chronic abdominal pain related to pancreaticobiliary disease is most commonly due to pancreatitis (acute or chronic), sphincter of Oddi dysfunction, pancreatic cysts and pseudocysts, and mass effect from pancreatic neoplasms, including intraductal pancreatic mucinous neoplasms. In our tertiary care hospital, we currently perform approximately 1200 MRCP examinations each year to evaluate pancreaticobiliary abnormalities. Although ERCP and endoscopic ultrasound are still common procedures ( 3000 ERCP and 2400 endoscopic ultrasound examinations were performed in 2011), MRCP has reduced the need for purely diagnostic ERCP at our institution [24]. MRCP can be performed in both inpatient and outpatient settings, does not require sedation or extra nursing staff other than MRI technologists, and can be performed relatively quickly, often within 1 hour. The only major limitation of MRI and MRCP is that some patients cannot undergo MRI because of preexisting conditions such as claustrophobia and the presence of devices such as cardiac pacemakers, aneurysm clips, and certain types of aortic grafts. The limitations of this study include performance in a single tertiary care referral facility. Our patient population was representative of patients referred for further evaluation for suspected pancreaticobiliary disease. The patients had varying clinical presentations and had undergone differing initial workups at the referring institutions. The number of patients was reduced somewhat by the need for exclusion of patients who had undergone previous invasive procedures. Several patients had to be excluded because of incomplete surveys. We found that knowledge of MRCP results improves diagnostic confidence among gastroenterologists and decreases the need for invasive procedures to confirm or establish a diagnosis. The high sensitivity of MRCP for evaluating the pancreatobiliary tree has led to the evolution of ERCP as a purely therapeutic procedure in many cases and obviates purely diagnostic endoscopic ultrasound in many patients. References 1. Cotton PB, Garrow DA, Gallagher J, Romangnuolo J. Risk factors for complications after ERCP: a multivariate analysis of 11,497 procedures over 12 years. Gastrointest Endosc 2009; 70: Male R, Lehman G, Sherman S, et al. Severe and fatal complications from diagnostic and therapeutic ERCPs. Gastrointest Endosc 1994; 40(P):A29 3. Loperfido S, Angelini G, Benedetti G, et al. Major early complications from diagnostic and therapeutic ERCP: a prospective multicenter study. Gastrointest Endosc 1998; 48: Adler DG, Jacobson BC, Davila RE, et al. ASGE guideline: complications of EUS. Gastrointest Endosc 2005; 61: Balci NC, Alkaade S, Magas L, Momtahen AJ, Burton FR. Suspected chronic pancreatitis with normal MRCP: findings on MRI in correlation with secretin MRCP. J Magn Reson Imaging 2008; 27: Wallner BK, Schumacher KA, Weidenmaier W, Friedrich JM. Dilated biliary tract evaluation with MR cholangiography with a T2-weighted contrast enhanced fast sequence. Radiology 1991; 181: Outwater E. MR cholangiography with a fast spin-echo sequence. (abstract) J Magn Reson Imaging 1993; 3(P): Barish MA, Yucel EK, Soto JA, Chuttani R, Ferrucci JT. MR cholangiopancreatography: efficacy of three-dimensional turbo spin-echo technique. AJR 1995; 165: Sahni VA, Mortele KJ. Magnetic resonance cholangiopancreatography: current use and future applications. Clin Gastroenterol Hepatol 2008; 6: Fukukura Y, Fujiyoshi F, Sasaki M, Nakajo M. Pancreatic duct: morphologic evaluation with MR cholangiopancreatography after secretin stimulation. Radiology 2002; 222: Matos C, Metens T, Deviere J, et al. Pancreatic duct: morphological and functional evaluation with dynamic MR pancreatography after secretin stimulation. Radiology 1997; 203: Akisik MF, Sandrasegaran K, Aisen AM, Maglinte DD, Sherman S, Lehman GA. Dynamic secretinenhanced MR cholangiopancreatography. Radio Graphics 2006; 26: Monill J, Pernas J, Clavero J, et al. Pancreatic duct after pancreatoduodenectomy: morphologic and functional evaluation with secretin-stimulated MR pancreatography. AJR 2004; 183: Manfredi R, Costamagna G, Brizi MG, et al. Severe chronic pancreatitis versus suspected pancreatic disease: dynamic MR cholangiopancreatography after secretin stimulation. Radiology 2000; 214: Matos C, Winant C, Delhaye M, Devière J. Functional MRCP in pancreatic and periampullary disease. Int J Gastrointest Cancer 2001; 30: Waters JA, Schmidt CM, Pinchot JW, et al. CT vs MRCP: optimal classification of IPMN type and extent. J Gastrointest Surg 2008; 12: Hekimoglu K, Ustundag Y, Dusak A, et al. MRCP vs. ERCP in the evaluation of biliary pathologies: review of current literature. J Dig Dis 2008; 9: Sandrasegaran K, Lin C, Akisik FM, Tann M. Stateof-the-art pancreatic MRI. AJR 2010; 195: Sahai AV, Devonshire D, Yeoh KG, et al. The decision-making value of magnetic resonance cholangiopancreatography in patients seen in a referral center for suspected biliary and pancreatic disease. Am J Gastroenterol 2001; 96: Parnaby CN, Jenkins JT, Ferguson JC, Williamson BW. Prospective validation study of an algorithm for triage to MRCP or ERCP for investigation of suspected pancreatico-biliary disease. Surg Endosc 2008; 22: Farrell RJ, Noonan N, Mahmud N, Morrin MM, Kelleher D, Keeling PW. Potential impact of magnetic resonance cholangiopancreatography on endoscopic retrograde cholangiopancreatography workload and complication rate in patients referred because of abdominal pain. Endoscopy 2001; 33: Axon AT, Classen M, Cotton PB, Cremer M, Freeny PC, Lees WR. Pancreatography in chronic pancreatitis: international definitions. Gut 1984; 25: Hellerhoff KJ, Helmberger H 3rd, Rösch T, Settles MR, Link TM, Rummeny EJ. Dynamic MR pancreatography after secretin administration: image quality and diagnostic accuracy. AJR 2002; 179: Coté GA, Singh S, Bucksot LG, et al. Association between volume of endoscopic retrograde cholangiopancreatography at an academic medical center and use of pancreatobiliary therapy. Clin Gastroenterol Hepatol 2012; 10: AJR:201, September
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, conta
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. M. Fatih Akisik,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. M. Fatih Akisik,
MRI Abdomen Protocol Pancreas/MRCP with Contrast
 MRI Abdomen Protocol Pancreas/MRCP with Contrast Reviewed By: Brett Mollard, MD; Anna Ellermeier, MD Last Reviewed: July 2018 Contact: (866) 761-4200 Standard uses: 1. Characterization of cystic and solid
MRI Abdomen Protocol Pancreas/MRCP with Contrast Reviewed By: Brett Mollard, MD; Anna Ellermeier, MD Last Reviewed: July 2018 Contact: (866) 761-4200 Standard uses: 1. Characterization of cystic and solid
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION
 IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
ENDOSCOPY IN COMPETITION DIAGNOSTICS. Dr. med. Dirk Hartmann Klinikum Ludwigshafen
 Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Chronic pancreatitis is characterized by continued inflammation
 Diagn Interv Radiol 2011; 17:249 254 Turkish Society of Radiology 2011 ABDOMINAL IMAGING REVIEW MRI assessment of chronic pancreatitis Cem Balcı ABSTRACT Magnetic resonance imaging (MRI) plays an important
Diagn Interv Radiol 2011; 17:249 254 Turkish Society of Radiology 2011 ABDOMINAL IMAGING REVIEW MRI assessment of chronic pancreatitis Cem Balcı ABSTRACT Magnetic resonance imaging (MRI) plays an important
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, by Am. Coll. of Gastroenterology ISSN /01/$20.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion
 Acta Med Kindai Univ Vol.43, No.1 1-8, 2018 1 MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion Shojiro Hidaka 1,2,
Acta Med Kindai Univ Vol.43, No.1 1-8, 2018 1 MR cholangiopancreatography; Predicting imaging findings for differentiation of malignant bile ductal obstruction versus benign lesion Shojiro Hidaka 1,2,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Secretin-Enhanced MRCP: Review of Technique and Application With Proposal for Quantification of Exocrine Function
 Gastrointestinal Imaging Original Research Sanyal et al. Secretin-Enhanced MRCP Gastrointestinal Imaging Original Research Rupan Sanyal 1 Tyler Stevens 2 Eric Novak 3 Joseph C. Veniero 1 Sanyal R, Stevens
Gastrointestinal Imaging Original Research Sanyal et al. Secretin-Enhanced MRCP Gastrointestinal Imaging Original Research Rupan Sanyal 1 Tyler Stevens 2 Eric Novak 3 Joseph C. Veniero 1 Sanyal R, Stevens
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic pancreatitis is a fibroinflammatory disease of the
 Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
MR CHOLANGIOPANCREATOGRAPHY: PROSPECTIVE COMPARISON OF 3-DIMENSIONAL TURBO SPIN ECHO AND SINGLE-SHOT TURBO SPIN ECHO WITH ERCP
 R.C. Chen, K.Y. Lin, J.M. Lii, et al MR CHOLANGIOPANCREATOGRAPHY: PROSPECTIVE COMPARISON OF 3-DIMENSIONAL TURBO SPIN ECHO AND SINGLE-SHOT TURBO SPIN ECHO WITH ERCP Ran-Chou Chen, 1,2 Kuang-Yang Lin, 3
R.C. Chen, K.Y. Lin, J.M. Lii, et al MR CHOLANGIOPANCREATOGRAPHY: PROSPECTIVE COMPARISON OF 3-DIMENSIONAL TURBO SPIN ECHO AND SINGLE-SHOT TURBO SPIN ECHO WITH ERCP Ran-Chou Chen, 1,2 Kuang-Yang Lin, 3
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Secretin-Stimulated MRCP
 Gastrointestinal Imaging Original Research Mensel et al. Secretin-Stimulated MRCP Gastrointestinal Imaging Original Research Birger Mensel 1 Philip Messner 1 Julia Mayerle 2 Gabriele Fluhr 2 Henry Völzke
Gastrointestinal Imaging Original Research Mensel et al. Secretin-Stimulated MRCP Gastrointestinal Imaging Original Research Birger Mensel 1 Philip Messner 1 Julia Mayerle 2 Gabriele Fluhr 2 Henry Völzke
Index words : Bile duct radiography, technology Bile ducts MR Bile ducts surgery Liver, transplantation
 Hilar Branching Anatomy of Living Adult Liver Donors: Comparison of T2-MR Cholangiography and Contrast Enhanced T1-MR Cholangiography in Terms of Diagnostic Utility 1 Joon Seok Lim, M.D. 1, Myeong-Jin
Hilar Branching Anatomy of Living Adult Liver Donors: Comparison of T2-MR Cholangiography and Contrast Enhanced T1-MR Cholangiography in Terms of Diagnostic Utility 1 Joon Seok Lim, M.D. 1, Myeong-Jin
Usefulness of the Navigator-echo triggering Technique for Free-Breathing 3D MRCP
 Usefulness of the Navigator-echo triggering Technique for Free-Breathing 3D MRCP Poster No.: C-1257 Congress: ECR 2012 Type: Scientific Exhibit Authors: K. Matsunaga, G. Ogasawara, K. Fujii, T. Irie, T.
Usefulness of the Navigator-echo triggering Technique for Free-Breathing 3D MRCP Poster No.: C-1257 Congress: ECR 2012 Type: Scientific Exhibit Authors: K. Matsunaga, G. Ogasawara, K. Fujii, T. Irie, T.
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis
 MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Cause of Acute Pancreatitis in A Case
 2008 19 531-535 Pancreas Divisum An Infrequent Cause of Acute Pancreatitis in A Case Cheuk-Kay Sun 1, Jui-Hao Chen 1, Kuo-Ching Yang 1, and Chin-Chu Wu 2 1 Division of Gastroenterology, Department of Internal
2008 19 531-535 Pancreas Divisum An Infrequent Cause of Acute Pancreatitis in A Case Cheuk-Kay Sun 1, Jui-Hao Chen 1, Kuo-Ching Yang 1, and Chin-Chu Wu 2 1 Division of Gastroenterology, Department of Internal
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Secretin-enhanced MR Imaging of the Pancreas 1
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Riccardo Manfredi, MD, MBA, Roberto Pozzi Mucelli, MD Secretin-enhanced MR Imaging of the Pancreas 1 Secretin is a
This copy is for personal use only. To order printed copies, contact reprints@rsna.org Riccardo Manfredi, MD, MBA, Roberto Pozzi Mucelli, MD Secretin-enhanced MR Imaging of the Pancreas 1 Secretin is a
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Magnetic resonance cholangiopancreatography: the ABC of MRCP
 Insights Imaging (2012) 3:11 21 DOI 10.1007/s13244-011-0129-9 PICTORIAL REVIEW Magnetic resonance cholangiopancreatography: the ABC of MRCP Nyree Griffin & Geoff Charles-Edwards & Lee Alexander Grant Received:
Insights Imaging (2012) 3:11 21 DOI 10.1007/s13244-011-0129-9 PICTORIAL REVIEW Magnetic resonance cholangiopancreatography: the ABC of MRCP Nyree Griffin & Geoff Charles-Edwards & Lee Alexander Grant Received:
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Magnetic resonance cholangiopancreatography (MRCP) is
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:967 977 CLINICAL IMAGING Magnetic Resonance Cholangiopancreatography: Current Use and Future Applications VIKRAM A. SAHNI and KOENRAAD J. MORTELE Division
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:967 977 CLINICAL IMAGING Magnetic Resonance Cholangiopancreatography: Current Use and Future Applications VIKRAM A. SAHNI and KOENRAAD J. MORTELE Division
stents she/he is providing appropriate or inappropriate care?
 Pancreatic Stents Are They Now State of the Art Care? To Help Limit Post ERCP Pancreatitis Glen A. Lehman, M.D. Professor of Medicine and Radiology Division of Gastroenterology/Hepatology Indiana University
Pancreatic Stents Are They Now State of the Art Care? To Help Limit Post ERCP Pancreatitis Glen A. Lehman, M.D. Professor of Medicine and Radiology Division of Gastroenterology/Hepatology Indiana University
Imaging and Treatment Features of Idiopathic Pancreatitis and Pancreas Divisum in a Young Man: A Case Report
 Case Report Elmer Press Imaging and Treatment Features of Idiopathic Pancreatitis and Pancreas Divisum in a Young Man: A Case Report Sari Venesmaa a, e, Markku Heikkinen b, Sakari Kainulainen c, Hannu
Case Report Elmer Press Imaging and Treatment Features of Idiopathic Pancreatitis and Pancreas Divisum in a Young Man: A Case Report Sari Venesmaa a, e, Markku Heikkinen b, Sakari Kainulainen c, Hannu
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
MRI of the Hepatobiliary System
 BODY APPLICATIONS OF MRI 51 Chapter Four C H A P T E R F O U R MRI of the Hepatobiliary System After completing this chapter, the reader will be able to: Develop a protocol for liver MRI Identify benign
BODY APPLICATIONS OF MRI 51 Chapter Four C H A P T E R F O U R MRI of the Hepatobiliary System After completing this chapter, the reader will be able to: Develop a protocol for liver MRI Identify benign
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Role of magnetic resonance cholangiopancreatography in diagnosing pancreatobiliary pathologies: a prospective study
 International Surgery Journal Nirhale DS et al. Int Surg J. 2018 Jun;5(6):2233-2237 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182228
International Surgery Journal Nirhale DS et al. Int Surg J. 2018 Jun;5(6):2233-2237 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182228
Evidence based imaging of the pancreas
 Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
To describe normal anatomy and common variants in biliary tree anatomy including the prevalence of these.
 Up for debate: Should 3.0T magnetic resonance pancreatography (MRCP) become a routine part of preoperative planning for patients undergoing laparoscopic cholecystectomy? Poster No.: C-0196 Congress: ECR
Up for debate: Should 3.0T magnetic resonance pancreatography (MRCP) become a routine part of preoperative planning for patients undergoing laparoscopic cholecystectomy? Poster No.: C-0196 Congress: ECR
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013
 Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
UTILITY OF THREE DIMENSIONAL MAGNETIC RESONANCE CHOLANGIOPANCREATOGRAPHY IN EVALUATION OF BILIARY OBSTRUCTION IN ADULTS
 - 842 - UTILITY OF THREE DIMENSIONAL MAGNETIC RESONANCE CHOLANGIOPANCREATOGRAPHY IN EVALUATION OF BILIARY OBSTRUCTION IN ADULTS Moanes M. Enaba MD *Tarek H. ELKammash**MD,, Mansour M. Morsy ***MD * Department
- 842 - UTILITY OF THREE DIMENSIONAL MAGNETIC RESONANCE CHOLANGIOPANCREATOGRAPHY IN EVALUATION OF BILIARY OBSTRUCTION IN ADULTS Moanes M. Enaba MD *Tarek H. ELKammash**MD,, Mansour M. Morsy ***MD * Department
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Cystic Pancreatic Lesions: Approach to Diagnosis
 Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Sphincter of Oddi Dysfunction: What s the Verdict in 2014?
 SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
Magnetic Resonance Cholangiopancreatography (MRCP)
 Magnetic Resonance Cholangiopancreatography (MRCP) What is Magnetic Resonance Cholangiopancreatography (MRCP)? What are some common uses of the procedure? How should I prepare for the procedure? What does
Magnetic Resonance Cholangiopancreatography (MRCP) What is Magnetic Resonance Cholangiopancreatography (MRCP)? What are some common uses of the procedure? How should I prepare for the procedure? What does
THE DIAGNOSTIC ACCURACY OF RAISED SERUM AMYLASE LEVEL AT 4 HOURS POST ERCP IN PREDICTING ACUTE PANCREATITIS
 ORIGINAL ARTICLE THE DIAGNOSTIC ACCURACY OF RAISED SERUM AMYLASE LEVEL AT 4 HOURS POST ERCP IN PREDICTING ACUTE PANCREATITIS UMBREEN ASLAM KHAN, SABEEN FARHAN, MUHAMMAD ARIF NADEEM, SIDRA RASHEED Department
ORIGINAL ARTICLE THE DIAGNOSTIC ACCURACY OF RAISED SERUM AMYLASE LEVEL AT 4 HOURS POST ERCP IN PREDICTING ACUTE PANCREATITIS UMBREEN ASLAM KHAN, SABEEN FARHAN, MUHAMMAD ARIF NADEEM, SIDRA RASHEED Department
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating Symptoms Suggestive of Common Bile Duct Stones
 Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Hepatobiliary investigations
 Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
INTRODUCTION. Jpn J Clin Oncol1999;29(6)
 Jpn J Clin Oncol1999;29(6)294-298 Clinical Significance of Magnetic Resonance Cholangiopancreatography for the Diagnosis of Cystic Tumor of the Pancreas Compared with Endoscopic Retrograde Cholangiopancreatography
Jpn J Clin Oncol1999;29(6)294-298 Clinical Significance of Magnetic Resonance Cholangiopancreatography for the Diagnosis of Cystic Tumor of the Pancreas Compared with Endoscopic Retrograde Cholangiopancreatography
Normal anatomy and anatomic variants of the biliary tree and pancreatic ductal system at MRCP - what the clinicians want to know
 Normal anatomy and anatomic variants of the biliary tree and pancreatic ductal system at MRCP - what the clinicians want to know Poster No.: C-1696 Congress: ECR 2014 Type: Educational Exhibit Authors:
Normal anatomy and anatomic variants of the biliary tree and pancreatic ductal system at MRCP - what the clinicians want to know Poster No.: C-1696 Congress: ECR 2014 Type: Educational Exhibit Authors:
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Newcastle HPB MDM updated radiology imaging protocol recommendations. Author Dr John Scott. Consultant Radiologist Freeman Hospital
 Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
The role of Magnetic Resonance Cholangiopancreatography in the evaluation of biliary tree: A pictorial review
 The role of Magnetic Resonance Cholangiopancreatography in the evaluation of biliary tree: A pictorial review Poster No.: C-0522 Congress: ECR 2013 Type: Educational Exhibit Authors: E. Alvarez-Hornia,
The role of Magnetic Resonance Cholangiopancreatography in the evaluation of biliary tree: A pictorial review Poster No.: C-0522 Congress: ECR 2013 Type: Educational Exhibit Authors: E. Alvarez-Hornia,
Aims and objectives. Page 2 of 10
 Diagnostic performance of automated breast volume scanner (ABVS) versus hand-held ultrasound (HHUS) as second look for breast lesions detected only on magnetic resonance imaging. Poster No.: C-1701 Congress:
Diagnostic performance of automated breast volume scanner (ABVS) versus hand-held ultrasound (HHUS) as second look for breast lesions detected only on magnetic resonance imaging. Poster No.: C-1701 Congress:
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
EVALUATION OF MRCP IN BILIARY OBSTRUCTION WITH ERCP, HISTOPATHOLOGICAL CORRELATION
 EVALUATION OF MRCP IN BILIARY OBSTRUCTION WITH ERCP, HISTOPATHOLOGICAL CORRELATION DISSERTATION SUBMITTED TO THE TAMIL NADU Dr. M.G.R MEDICAL UNIVERSITY, CHENNAI IN PARTIAL FULFILLMENT OF THE REGULATIONS
EVALUATION OF MRCP IN BILIARY OBSTRUCTION WITH ERCP, HISTOPATHOLOGICAL CORRELATION DISSERTATION SUBMITTED TO THE TAMIL NADU Dr. M.G.R MEDICAL UNIVERSITY, CHENNAI IN PARTIAL FULFILLMENT OF THE REGULATIONS
Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum
 ORIGINAL ARTICLE: Clinical Endoscopy Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum Lyssa N. Chacko, MD, Yang K. Chen, MD,
ORIGINAL ARTICLE: Clinical Endoscopy Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum Lyssa N. Chacko, MD, Yang K. Chen, MD,
Pancreatoscopy-Directed Electrohydraulic Lithotripsy for Pancreatic Ductal Stones in Painful
 Pancreatoscopy-Directed Electrohydraulic Lithotripsy for Pancreatic Ductal Stones in Painful Chronic Pancreatitis Using SpyGlass Short title: EHL for Pancreatic Ductal Stones Noor LH Bekkali 1, MD, PhD;
Pancreatoscopy-Directed Electrohydraulic Lithotripsy for Pancreatic Ductal Stones in Painful Chronic Pancreatitis Using SpyGlass Short title: EHL for Pancreatic Ductal Stones Noor LH Bekkali 1, MD, PhD;
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Case Report (1) Sphincter of Oddi Dysfunction. Case Report (3) Case Report (2) Case Report (4) Case Report (5)
 Dr David Westaby Imperial NHS Trust Imperial College Medical School London Case Report (1)! TD 33yr old male! Feb May 2010: Recurrent episodes of abdominal pain! June 2010 Episode severe abdominal pain
Dr David Westaby Imperial NHS Trust Imperial College Medical School London Case Report (1)! TD 33yr old male! Feb May 2010: Recurrent episodes of abdominal pain! June 2010 Episode severe abdominal pain
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Prevention and management of complications
 Prevention and management of complications Endoscopic retrograde cholangiopancreatography (ERCP) H.-J. Schulz, H. Schmidt Oskar-Ziethen-Hospital Sana Clinic Lichtenberg Teaching Hospital of Charité Humboldt
Prevention and management of complications Endoscopic retrograde cholangiopancreatography (ERCP) H.-J. Schulz, H. Schmidt Oskar-Ziethen-Hospital Sana Clinic Lichtenberg Teaching Hospital of Charité Humboldt
Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT
 O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Sphincter of Oddi Dysfunction: Where do we stand in 2015?
 IU GI Motility Conference August 5, 2015 Sphincter of Oddi Dysfunction: Where do we stand in 2015? Evan L. Fogel, M.D. Professor of Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology
IU GI Motility Conference August 5, 2015 Sphincter of Oddi Dysfunction: Where do we stand in 2015? Evan L. Fogel, M.D. Professor of Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology
Differential Diagnosis of Benign and Malignant Intraductal Papillary Mucinous Tumors of the Pancreas: MR Cholangiopancreatography
 Differential Diagnosis of Benign and Malignant Intraductal Papillary Mucinous Tumors of the Pancreas: MR Cholangiopancreatography and MR Angiography Byung Se Choi, MD 1 Tae Kyoung Kim, MD 1 Ah Young Kim,
Differential Diagnosis of Benign and Malignant Intraductal Papillary Mucinous Tumors of the Pancreas: MR Cholangiopancreatography and MR Angiography Byung Se Choi, MD 1 Tae Kyoung Kim, MD 1 Ah Young Kim,
Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
 Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected Pancreatic Cancer
 Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation?
 What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation? John Baillie Division of Gastroenterology, Duke University Medical Center. Durham, NC, USA
What Should Be Done with Idiopathic Recurrent Pancreatitis That Remains Idiopathic after Standard Investigation? John Baillie Division of Gastroenterology, Duke University Medical Center. Durham, NC, USA
Diagnostic performance of endoscopic ultrasound-guided fine-needle aspiration in pancreatic lesions
 European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
ACCURACY OF MRCP COMPARED WITH ERCP IN THE DIAGNOSIS OF BILE DUCT STONES
 ejpmr, 2016,3(8), 27-32 SJIF Impact Factor 3.628 Research Article EUROPEAN JOURNAL OF European PHARMACEUTICAL Journal of Pharmaceutical and Medical Research AND MEDICAL RESEARCH ISSN 2394-3211 www.ejpmr.com
ejpmr, 2016,3(8), 27-32 SJIF Impact Factor 3.628 Research Article EUROPEAN JOURNAL OF European PHARMACEUTICAL Journal of Pharmaceutical and Medical Research AND MEDICAL RESEARCH ISSN 2394-3211 www.ejpmr.com
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Original Report. Duodenal Diverticula Mimicking Cystic Neoplasms of the Pancreas: CT and MR Imaging Findings in Seven. Patients
 Downloaded from www.ajronline.org by 46.3.198.217 on 12/11/17 from IP address 46.3.198.217. Copyright RRS. For personal use only; all rights reserved Michael Macari 1 Dawn Lazarus Gary Israel lec Megibow
Downloaded from www.ajronline.org by 46.3.198.217 on 12/11/17 from IP address 46.3.198.217. Copyright RRS. For personal use only; all rights reserved Michael Macari 1 Dawn Lazarus Gary Israel lec Megibow
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC)
 Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC) Poster No.: C-0051 Congress: ECR 2010 Type: Scientific Exhibit Topic: Abdominal
Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC) Poster No.: C-0051 Congress: ECR 2010 Type: Scientific Exhibit Topic: Abdominal
Endoscopic Ultrasound (EUS) Be the difference between maybe and definitely.
 (EUS) Be the difference between maybe and definitely. Maybe? Definitely. EUS lets you be certain in uncertain cases. Why EUS? EUS combines ultrasound technology with endoscopy to gain an internal vantage
(EUS) Be the difference between maybe and definitely. Maybe? Definitely. EUS lets you be certain in uncertain cases. Why EUS? EUS combines ultrasound technology with endoscopy to gain an internal vantage
Having an ERCP (endoscopic retrograde cholangio pancreatogram)
 Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
